Abstract
Background
Orthopaedic surgery is the least-diverse surgical specialty based on race and ethnicity. To our knowledge, the impact of this lack of diversity on discriminatory or noninclusive experiences perceived by Black orthopaedic surgeons during their residency training has never been evaluated. Racial microaggressions were first defined in the 1970s as “subtle verbal, behavioral, and environmental indignities, whether intentional or unintentional, that communicate hostile, derogatory, or negative racial slights and insults to the target person or group.” Although the term “microaggression” has long been established, more recently, as more workplaces aim to improve diversity, equity, and inclusion, it has entered the medical profession’s lexicon as a means of describing the spectrum of racial discrimination, bias, and exclusion in the healthcare environment.
Question/purposes
(1) What is the extent of discrimination that is perceived by Black orthopaedic surgeons during residency? (2) What subtypes of racial microaggressions (which encompasses racial discrimination, bias, and exclusion) do Black orthopaedic surgeons experience during residency training, and who are the most common initiators of these microaggressions? (3) What feedback statements could be perceived as racially biased to Black orthopaedic surgeons in residency training? (4) Are there gender differences in the reported types of racial microaggressions recalled by Black respondents during residency training?
Methods
An anonymous survey was administered between July 1, 2020, and September 1, 2020, to practicing orthopaedic surgeons, residents, and fellows in the J. Robert Gladden Orthopaedic Society database who self-identify as Black. There were 455 Black orthopaedic surgeons in practice and 140 Black orthopaedic residents or fellows in the database who met these criteria. Fifty-two percent (310 of 595) of participants responded. Fifty-three percent (243 of 455) were practicing surgeons and 48% (67 of 140) were current residents or fellows. Respondents reported their perception of discrimination in the residency workplace using a modified version of the single-item Perceived Occupational Discrimination Scale and were asked to recall any specific examples of experiences with racial discrimination, bias, or exclusion during their training. Examples were later categorized as different subtypes of racial microaggressions and were quantified through a descriptive analysis and compared by gender.
Results
Among survey respondents, 34% (106 of 310) perceived a lot of residency workplace discrimination, 44% (137 of 310) perceived some residency workplace discrimination, 18% (55 of 310) perceived a little residency workplace discrimination, and 4% (12 of 310) perceived no residency workplace discrimination. Categorized examples of racial microaggressions experienced in residency were commonly reported, including being confused for a nonphysician medical staff (nurse or physician’s assistant) by 87% (271 of 310) of respondents or nonmedical staff (janitorial or dietary services) by 81% (250 of 310) of respondents. Racially explicit statements received during residency training were reported by 61% (190 of 310) of respondents. Thirty-eight percent (117 of 310) of such statements were reportedly made by patients and 18% (55 of 310) were reportedly made by attending faculty. Fifty percent (155 of 310) of respondents reported receiving at least one of nine potentially exclusionary or devaluing feedback statements during their residency training. Among those respondents, 87% (135 of 155) perceived at least one of the statements to be racially biased in its context. The three feedback statements that, when received, were most frequently perceived as racially biased in their context was that the respondent “matched at their program to fulfill a diversity quota” (94% [34 of 36]), the respondent was unfriendly compared with their peers (92% [24 of 26]), or that the respondent was “intimidating or makes those around him/her uncomfortable” (88% [51 of 58]). When compared by gender, Black women more frequently reported being mistaken for janitors and dietary services at 97% (63 of 65), compared with Black men at 77% (187 of 244; p < 0.01). In addition, Black women more frequently reported being mistaken as nurses or physician assistants (100% [65 of 65]) than Black men did (84% [205 of 244]) during orthopaedic residency training (p < 0.01). Black women also more frequently reported receiving potentially devaluing or exclusionary feedback statements during residency training.
Conclusion
Perception of workplace discrimination during orthopaedic residency training is high (96%) among Black orthopaedic surgeons in the United States. Most respondents reported experiencing discrimination, bias, and exclusion that could be categorized as specific subtypes of racial microaggressions. Several different examples of racial microaggressions were more commonly reported by Black women. Certain feedback statements were frequently perceived as racially biased by recipients.
Clinical Relevance
To better understand barriers to the successful recruitment and retention of Black physicians in orthopaedics, the extent of racial discrimination, bias, and exclusion in residency training must be quantified. This study demonstrates that racial discrimination, bias, and exclusion during residency, wholly categorized as racial microaggressions, are frequently recalled by Black orthopaedic surgeons. A better understanding of the context of these experiences of Black trainees is a necessary starting point for the development of a more inclusive workplace training environment in orthopaedic surgery.
Introduction
Data from the American Association of Medical Colleges reveal that the proportion of Black orthopaedic surgery residents has never surpassed 4.7% of the resident population, and this population has actually decreased in the past decade [15]. Part of the challenge to improving the recruitment and retention of Black orthopaedic surgery residents is understanding the residency environment they face and determining whether racial discrimination, bias, and exclusion have affected the residency experience of current and graduated Black orthopaedic trainees.
Varying types of racial discrimination can be encompassed under the term “microaggressions.” Microaggressions were first described by Pierce [14] in 1970 as minor humiliations and indignities experienced by Black Americans. This term was later expanded by Sue et al. [17] in 2007 to describe “subtle snubs, slights, and insults directed toward minorities, women, and other historically stigmatized groups that implicitly communicate hostility.” Sue et al. further categorized microaggression into four subtypes: Microassaults are intentional verbal or nonverbal attacks clearly intended to offend the recipient; microinsults are subtle snubs or humiliations that convey a demeaning message to the recipient in a way that may be unintentional to the perpetrator; microinvalidations are exclusion, dismissal, or denial of the personal thoughts, feelings, or experiential reality of a person; and environmental microaggressions are when “microassaults, microinsults, and microinvalidations are reflected in the imagery, culture, processes, and climate of the workplace” [17]. In short, the term microaggression encapsulates the spectrum of discrimination, bias, and exclusion that historically has been experienced by minoritized populations.
Experiencing microaggressions has been proven to predict low self-esteem [11], increase stress and depressive symptoms [18], and increase binge drinking events with subsequent alcohol-related consequences [3]. Our understanding of the concept of microaggressions and its frequency in orthopaedic surgery is burgeoning. Recently, Samora et al. [16] published a survey on the prevalence of microaggressions experienced by women orthopaedic surgeons during different phases of their career (residency, fellowship, and attending practice). In addition, we published an article on the workplace experiences of practicing Black orthopaedic surgeons, which revealed that more than 97% of surveyed Black orthopaedic surgeons reported discrimination in the workplace [12]. Eighty-nine percent of those surveyed reported personally experiencing some form of racial discrimination in clinical practice, although in that survey, the term “racial microaggression” was not explicitly queried. Given the potential psychologic and physical sequelae of microaggressions, the current study aimed to take a step further to understand the extent to which Black orthopaedic surgeons recall experiences during their orthopaedic training that could be categorized as a racial microaggressions.
We asked: (1) What is the extent of discrimination that is perceived by Black orthopaedic surgeons during residency? (2) What subtypes of racial microaggressions (which encompasses racial discrimination, bias, and exclusion) do Black orthopaedic surgeons experience during residency training, and who are the most common initiators of these microaggressions? (3) What feedback statements could be perceived as racially biased to Black orthopaedic surgeons in residency training? (4) Are there gender differences in the reported types of racial microaggressions recalled by Black respondents during residency training?
Materials and Methods
Questionnaire Design
We developed a 23-item, anonymous survey to solicit experiences of racial bias, discrimination, and exclusion in the orthopaedic residency training environment (Supplemental Digital Content 1; http://links.lww.com/CORR/A966). In 2021, we published the results of a different 38-item anonymous survey designed to evaluate experiences of racial bias and microaggressions in the workplace of practicing orthopaedic surgeons [12].
Development and Pretesting
The first nine questions of the 23-item survey collected demographic and educational background data only. Questions 10 through 14 of the survey were developed to elucidate the frequency of three microaggression subtypes (microassaults, microinsults, and environmental microaggressions) experienced by respondents during their orthopaedic training experience. Racially explicit statements directed toward the recipient were queried as an example of a microassault, while being mistaken for a nurse or janitor is a commonly reported example of a microinsult in medicine [19]. Witnessing of racially explicit imagery (such as pictures, videos, and other media) in the residency workplace is an example of an environmental microaggression. To elucidate which feedback statements provided by superiors in the workplace environment could be perceived as racially biased, questions 19 to 21 were developed. Given the potential lack of familiarity with the definitions of microaggression and microaggression subtypes, the specific scenarios outlined in these questions were intended to quantify experiences with racial microaggressions without coercing the participant to define the context of their experiences with discrimination, bias, and exclusion as an explicit racial microaggression. To answer our first study question related to perceived discrimination in the residency workplace, Question 22 of the survey included a modified version of the single-item Perceived Occupational Discrimination Scale (PODS) [6], which was developed to assess Black Americans’ perceptions of access and treatment in the workplace and perception of discrimination in 26 different occupations including law, medicine, and accounting. The PODS uses a 4-point Likert-type scale: no (1), a little (2), some (3), and a lot (4), to quantify the extent of discrimination that a Black American perceives would exist for those in the selected occupation. Therefore, a higher mean PODS score equates to a higher perception of workplace discrimination. The PODS has been found to have good internal consistency and test-retest reliability in Black students [4] but has not been evaluated in professional populations.
Recruitment Process
The target population for this study was practicing Black orthopaedic surgeons and Black orthopaedic residents and fellows. This cohort was recruited from the database maintained by the J. Robert Gladden Orthopaedic Society. The survey was distributed electronically to 100% (455 of 455) of the practicing orthopaedic surgeons and 100% (140 of 140) of the orthopaedic residents and fellows in the database who self-identify as Black (which encompasses African American, Caribbean-American, Black African, and Black). According to the American Academy of Orthopaedic Surgeons 2018 census, there are approximately 573 practicing orthopaedic surgeons in the United States who identify as Black [1].
Survey Administration
This voluntary survey was administered and managed using the online REDCap software, hosted at Prisma Health [9]. The survey was emailed to participants between July 1, 2020, and September 1, 2020, and participants received a reminder every 14 days to complete the survey (total of three reminders) during this period. No incentives were offered for completing the survey, and participants could not change their responses after survey submission.
Response Rates
Fifty-two percent (310 of 595) of surveyed Black orthopaedic surgeons, fellows, and residents responded to the survey. Among them, 53% (243 of 455) were practicing orthopaedic surgeons and 48% (67 of 140) were residents or fellows (Table 1).
Table 1.
Demographics of 243 Black orthopaedic surgeons and 67 fellows and residents
| Parameter | Residents/fellows, % (n) |
Attending, % (n) |
| Gender | ||
| Men | 82 (55) | 78 (189) |
| Women | 18 (12) | 22 (53) |
| Declined to answer | 0 (0) | 0.4 (1) |
| Age group in years | ||
| 20 to 29 | 24 (16) | 0 (0) |
| 30 to 39 | 75 (50) | 27 (66) |
| 40 to 49 | 1.5 (1) | 29 (71) |
| 50 to 59 | 0 (0) | 26 (64) |
| 60 to 69 | 0 (0) | 12 (29) |
| 70 to 79 | 0 (0) | 5 (13) |
| Ethnicity | ||
| Non-Hispanic | 87 (58) | 98 (239) |
| Hispanic | 9 (6) | 0.8 (2) |
| Unknown or not reported | 4.5 (3) | 0.8 (2) |
| Nationality | ||
| United States citizen (by birth) | 87 (58) | 82 (199) |
| United States citizen (by naturalization) | 12 (8) | 16 (38) |
| Non–United States citizen, permanent resident (that is, green card) | 1.5 (1) | 2 (5) |
| Non–United States citizen, temporary resident | 0 (0) | 0.4 (1) |
| Geographic location of residencya | ||
| Northeast: New England (ME, NH, VT, MA, RI, CT) | 6 (4) | 8 (19) |
| Northeast: mid-Atlantic (NY, NJ, PA) | 25 (17) | 27 (66) |
| South: south Atlantic (DE, MD, DC, VA, WV, NC, SC, GA, FL) | 27 (18) | 30 (73) |
| South: east south central (KY, TN, AL, MS) | 0 (0) | 2.5 (6) |
| South: west south central (AR, LA, OK, TX) | 10.4 (7) | 6 (15) |
| Midwest: east north central (OH, MI, IN, IL, WI) | 9 (6) | 14 (34) |
| Midwest: west north central (MN, IA, MO, ND, SD, NE, KS) | 7 (5) | 1.2 (3) |
| West: mountain (WY, MT, CO, NM, ID, UT, AZ, NV) | 1.5 (1) | 0.8 (2) |
| West: pacific (WA, OR, CA, AK, HI) | 13 (9) | 9 (23) |
| Unknown or not reported | 0 (0) | 0.8 (2) |
| Attended a majority Black residency program (n = 308) | 1 (4 of 308) | 13 (41 of 308) |
Based on United States Census description.
Preventing Multiple Entries From the Same Individual
The survey was specifically designed in REDCap to include the quality control measure that prevents individuals from submitting multiple entries. The survey used a closed format, so participants could not complete the survey with an email address that was not already previously added into the REDCap system.
Statistical Analysis
Only completed surveys were included for analysis, and no statistical correction such as weighting or propensity scores were used. SPSS Statistics for Mac, version 28 (IBM Corp) was used for all statistical analyses. To answer the question regarding the extent of discrimination perceived against Black orthopaedic surgeons during residency, we used frequency statistics and an independent-samples t-test to compare PODS scores. The subtypes and initiators of microaggressions are reported using simple frequency statistics. The feedback statements recalled by surgeons are also reported using simple frequency statistics. To answer the question on how perceived microaggressions differed based on gender, we compared PODS scores using an independent-samples t-test. The difference in perceived microaggression subtypes and racial bias of feedback statements between genders were compared using the Pearson chi-square test.
Results
Extent of Perceived Discrimination Against Black Orthopaedic Surgeons During Residency
For all 310 respondents, the mean PODS score was 3.09 ± 0.82 of a maximum score of 4 points. There was no difference in PODS score among orthopaedic surgeons currently in practice (3.13 ± 0.79) and those currently in residency or fellowship (2.94 ± 0.90; p = 0.10). According to the 4-point Likert scale for the PODS instrument, 34% (106 of 310) perceived a lot of residency workplace discrimination, 44% (137 of 310) perceived some residency workplace discrimination, 18% (55 of 310) perceived a little residency workplace discrimination, and 4% (12 of 310) perceived no residency workplace discrimination.
Subtypes and Initiators of Microaggressions Reported During Residency Training
Sixty-one percent (190 of 310) of Black respondents reported that racially explicit statements (microassaults) were directed at them during their orthopaedic residency training. Respondents reported that patients were the most common initiators of these microassaults, with attending faculty being the second most common initiators (Table 2). Microinsults were the most common microaggressions reported by respondents, with 87% (271 of 310) being mistaken for a nonphysician staff member by patients and fellow employees and 81% (250 of 310) being mistaken for a nonclinical staff member such as a janitor or nutritional services employee. Environmental microaggressions, such as witnessing racially explicit comments or imagery in the residency workplace, was reported by most respondents (56% [173 of 310]).
Table 2.
Initiators of microassaults for Black orthopaedic surgeons during residency training
| Initiator | % (n) |
| Patient | 62 (117) |
| Attending faculty | 29 (55) |
| Residents | 8 (15) |
| Nurses/nurse practitioners/physician assistants | 11 (20) |
| Office staff | 8 (15) |
| Surgical staff | 13 (24) |
| Other | 7 (14) |
The microassaults reportedly received by 190 respondents were sometimes initiated by more than one person; thus, 260 initiators of microassaults are listed.
Feedback Statements Recalled by 310 Black Orthopaedic Surgeons During Residency Training
Fifty percent (155 of 310) of respondents reported receiving at least one of nine potentially devaluing or exclusionary feedback statements during their residency training (Table 3). Among those respondents, 87% (135 of 155) perceived at least one of the statements to be racially biased in its context. The three most frequently reported statements recalled by the respondents were that the respondent was “at an inferior surgical skill level compared to their peers” (23% [70 of 310]), was “intimidating or made others around them feel uncomfortable” (19% [58 of 310]), or was “at an inferior intellectual level compared to their peers” (17% [53 of 310]). The three feedback statements that were the most frequently perceived as racially biased in their context was that the respondent “matched at their program to fulfill a diversity quota” (94% [34 of 36]), the respondent was unfriendly compared with their peers (92% [24 of 26]), or that the respondent was “intimidating or makes those around him/her uncomfortable” (88% [51 of 58]).
Table 3.
Residency feedback statements recalled by 310 Black orthopaedic surgeons during training
| Received example statement | Perceived statement as racially biased | ||
| Example statements | Overall, % (n) | Yes, % (n) | No, % (n) |
| Do not “fit in” at your program/do not match the “culture” of your program | 15 (47) | 87 (41 of 47) | 13 (6 of 47) |
| Matched at your program to fulfill a diversity quota | 12 (36) | 94 (34 of 36) | 6 (2 of 36) |
| Demonstrated inferior communication skills to your peers | 11 (34) | 79 (27 of 34) | 21 (7 of 34) |
| Demonstrated inferior bedside manners to your peers | 1.9 (6) | 50 (3 of 6) | 50 (3 of 6) |
| At an inferior intellectual level compared with your peers | 17 (53) | 66 (35 of 53) | 34 (18 of 53) |
| At an inferior surgical skill level compared with your peers | 23 (70) | 63 (44 of 63) | 37 (26 of 63) |
| Not cooperative, difficult, or “not a team player” | 13 (41) | 66 (27 of 41) | 34 (14 of 41) |
| Intimidating or make those around you uncomfortable | 19 (58) | 88 (51 of 58) | 12 (7 of 58) |
| Unfriendly compared with your peers | 8 (26) | 92 (24 of 26) | 8 (1 of 26) |
| Any of the above | 50 (155) | 87 (135 of 155) | 13 (20 of 155) |
| None of the above | 50 (155) | ||
Differences in Perceived Microaggressions and Racially Biased Statements Based on Gender
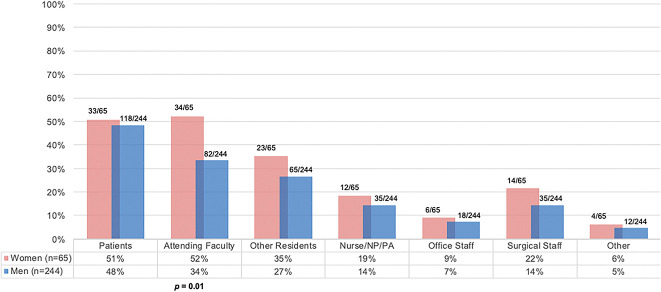
When compared by gender, Black women had a higher mean PODS score (2.89 ± 0.31) (higher perceived workplace discrimination in orthopaedic residency) than Black men did (2.71 ± 0.55; p = 0.01); however, this is unlikely to represent a contextual difference. There was no difference in the frequency of reported microassaults or environmental microaggressions during residency training when survey results were compared between men and women (Table 4). When microinsults were compared based on gender, 100% (65 of 65) of Black women reported being mistaken for a nurse or physician assistant during residency training compared with only 84% (205 of 244) of Black men (p < 0.01). In addition, 97% (63 of 65) of Black women were more likely to report being mistaken for janitorial or nutrition services staff during their residency training (p < 0.01). The initiators of racial microassaults were compared based on gender, showing that for Black women respondents, attending faculty are most often the initiators of racial microassaults (52% [34 of 65]) compared with Black men (34% [82 of 244]; p = 0.01). There were no other differences in the initiators of racial microassaults based on respondent gender (Fig. 1). Black women more frequently recalled receiving seven of the nine listed example statements given during their residency training (Fig. 2). The perception of racial bias in these statements was similar among women and men (Fig. 3).
Table 4.
Differences in reported racial microaggressions based on gender
| Microaggression subtype | Associated survey question | % (n) men | % (n) women | p value |
| Microassaults | As an orthopaedic surgery resident, did you ever have racially explicit statements directed toward you in the workplace? | 60 (147 of 244) | 65 (42 of 65) | 0.59 |
| Microaggressions are characterized by verbal or nonverbal attacks clearly intended to offend the recipient; often conscious | ||||
| Environmental microaggressions | ||||
| Microaggressions that are more apparent on systemic and environmental levels | As an orthopaedic surgery resident, did you ever witness racially explicit comments or imagery (including pictures, videos, or other media) in the workplace? | 55 (133 of 244) | 62 (40 of 65) | 0.32 |
| Microinsults | ||||
| Subtle snubs or humiliations that convey a demeaning message to the recipient in a way that may be unintentional to the perpetrator | As an orthopaedic surgery resident, were you ever mistaken for a non-physician medical staff (physician assistant, nurse, etc.) by a patient or hospital staff? | 84 (205 of 244) | 100 (65 of 65) | 0.002 |
| As an orthopaedic resident, were you ever mistaken for nonclinical staff (janitorial services, nutritional services, etc.) by a patient or hospital staff? | 77 (187 of 244) | 97 (63 of 65) | < 0.001 |
Fig. 1.
This graph represents the source of racially explicit statements experienced by Black orthopaedic surgeons, compared by gender. Black women orthopaedic surgeons received more microassaults from attending faculty members during residency training than men did. A color image accompanies the online version of this article.
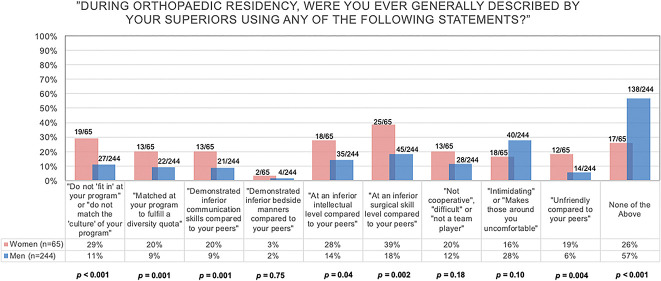
Fig. 2.
This figure shows potentially exclusionary and devaluing statements received by Black orthopaedic surgeons during residency training, compared by gender. Black women orthopaedic surgeons received more of these statements than Black men orthopaedic surgeons did. A color image accompanies the online version of this article.
Fig. 3.
This figure shows perception of racial bias among the potentially exclusionary and devaluing statements received by Black orthopaedic surgeons, compared by gender. A color image accompanies the online version of this article.
Discussion
The concept of microaggressions has been known since the 1970s [14], with deleterious effects including low self-esteem, increased stress, depressive symptoms, and increased alcoholic behavior [3, 11, 18]. Given the dearth of Black orthopaedic surgery residents training in the United States [15], we sought to understand whether this population experienced microaggressions during their residency training and how a respondent’s gender might affect his or her perceived experience with microaggressions. Using an instrument that specifically measures the perception of discrimination against Black Americans, we found that most respondents reported some level of workplace discrimination during their residency training. In addition, we found that most respondents reported receiving racially explicit statements during their residency training, with patients and attending faculty being the most common initiators of these statements. We also found that Black women respondents reported being mistaken more often for janitors, dietary services staff, nurses, or physician assistants than Black men respondents. When queried about common potentially devaluing or exclusionary feedback statements reportedly received during residency training, Black women more frequently reported receiving these example statements. This study highlights that microaggressions toward Black orthopaedic residents are not a rare phenomenon. More importantly, with patients and attending faculty most often initiating the microaggressions, Black orthopaedic residents may routinely experience these distressing interactions. Finally, given the intersectionality of being a gender and racial minority, Black women orthopaedic surgeons may be more susceptible to receiving different types of discriminatory, biased, or exclusionary statements during their training years.
Limitations
The most important limitation to our study relates to recall bias. Although some respondents were orthopaedic residents and fellows currently in training, most respondents were practicing orthopaedic surgeons recalling their experiences as residents. Some of the remembered details regarding their experiences with categorized microaggressions might become less accurate as the years progress. Second, as is common in all survey studies, there may be selection bias, given that a Black orthopaedic surgeon who faced discrimination and/or microaggressions may be more likely to respond to the survey than those who did not face these issues. However, based on the 2018 American Academy of Orthopaedic Surgeons census [1], the attending respondents represented 42% (243 of 573) of practicing Black orthopaedic surgeons in the United States. Additionally, there was no follow-up question asking whether the participant perceived an undertone of racial bias when being mistaken for nonphysician staff. The context of these experiences (whether these were rare or frequent) may provide greater clarity regarding the culture of discrimination in the work environment. The perception of pervasive workplace discrimination likely differs between the participant who recalls being mistaken for a nurse or a physician assistant only once during their training versus the participant who is not routinely assumed to be a physician and is mistaken for nonmedical staff on a weekly or daily basis. In addition, we did not have a control group of non-Black respondents to measure whether our results are specific to this cohort or experienced by orthopaedic residents of all races at similar frequencies. Finally, most respondents were trained in orthopaedic residency programs in the South, followed by the Northeast. A recent study created a map of racism by measuring Google searches for the “racial slur/N-word” stratified by geographic region [5]. Their data showed that racism was > 0.5 standard deviations above the mean in states in the South that are east of Texas, as well as in rural portions of the Northeast. Although outside of the scope of this study, the higher number of Black orthopaedic residents who trained in residency programs in the South may experience higher rates of racial discrimination, which may have influenced our survey results.
Extent of Perceived Discrimination Against Black Orthopaedic Surgeons During Residency
Most Black respondents perceived that Black trainees experience workplace discrimination during orthopaedic residency training, with a mean PODS score of 3.13 for attending physicians and 2.94 for residents. In a preceding article [12], we showed that Black orthopaedic attending surgeons perceived high levels of discrimination in their current practices (PODS score of 3.02). Taken together with the results of the current study, the perception of workplace discrimination persists throughout the careers of Black orthopaedic surgeons. This perception of discrimination in the residency workplace is not unique to orthopaedics; in a randomized controlled trial, Khubchandani et al. [10] measured the perception of discrimination among residents from seven different general surgery training programs. Using the Every Day Discrimination Scale, and after controlling for socioeconomic and demographic factors, they found that Black general surgery residents were 4.2 times as likely to report discrimination in the workplace as White general surgery residents. A reader could possibly read these results, taken from a validated instrument, and conclude that the problem lies not in surgical training environment, but in the hypersensitive or misguided perceptions of Black trainees. This sentiment, however, is an apt example of the only microaggression subtype not measured in this current study, microinvalidations. Microinvalidations are defined as the dismissal or denial of the personal thoughts, feelings, or experiential reality of a person [17]. Therefore, for the reader who may reason that experiences with discrimination reported among this study cohort are an internal byproduct of a hypersensitivity or misguided perception of reality among the respondents, we argue that acceptance of and curiosity about the commonly reported experiences of this large cohort of medical professionals is an important first step in identifying factors that might be modified to make the residency workplace more inclusive and equitable.
Subtypes and Initiators of Microaggressions Reported During Residency Training
It is vital for orthopaedic leaders in residency training programs to understand the magnitude and breadth of microaggressions their Black trainees reportedly experience. We found that 61% of respondents reported receiving racially explicit statements (microassaults) during their residency training. In a similar study, Samora et al. [16] showed that 74% of 264 women orthopaedic surgeons and residents reportedly experienced some subtype of microaggression. In our study, respondents reported that patients were the most common initiators of these microaggressions, followed closely by attending faculty. This differs slightly from Samora et al.’s [16] study, which listed patients and their families as the most common initiators of microaggression, followed by men faculty members and women support staff. Of all microaggression subtypes, microinsults such as being mistaken for a nonphysician staff member or a nonclinical staff member were reported by more than 80% of respondents. Microinsults may appear to be a small slight; however, if they are received repeatedly in the training experience, it may foster the perception that the patients and supporting staff do not expect or believe that the Black trainee belongs in that work environment. This is further supported by the fact that most respondents reported witnessing racially explicit comments or imagery displayed in the residency workplace. Given the high frequency of these reported microaggressions toward Black trainees, orthopaedic residency leaders may inquire why they have not heard about these incidents occurring in their programs. A recent study by Alimi et al. [2] evaluating the prevalence and nature of microaggressions toward surgical trainees might answer this question. Of the surgical residents queried, 72% (1173 of 1624) reported experiencing microaggressions; however, only 7% (109 of 1624) reported these microaggression events to their program directors. Even more concerning is that 31% of the queried residents reported experiencing retaliation when they reported these microaggressions. These data should be used to implore leaders in orthopaedic residency training programs to implement systems and workflows that provide a safe space for residents to report the initiators of microaggressions, especially when the initiator is an orthopaedic faculty member.
Potentially Exclusionary or Devaluing Statements Recalled by 310 Black Orthopaedic Surgeons During Residency Training
Positive and negative feedback are common educational methods used to train competent orthopaedic surgeons. However, given the high frequency of reported workplace discrimination and microaggressions among Black trainees, readers may ask what statements given by residency superiors have a higher chance of being perceived as discriminatory, biased, or exclusionary. We sought to answer this question by using statement examples (Table 3). Only 50% of the respondents reported receiving these feedback statements, and only 44% of respondents perceived these statements as racially biased. Regardless, the feedback statements that were perceived ubiquitously as racially biased were statements that the respondent “did not fit the culture of the program” or they “matched at the program to fulfill a diversity quota.” Other statements that were almost universally perceived as racially biased were that the resident “looked intimidating or made those around them feel uncomfortable” and that the respondent was “less friendly than their peers.” The common theme in these example statements is that the respondent is seen as the “other”; they are regarded as dissimilar either culturally or visibly from their peers. The challenges of being perceived as “the other” was explored in a 2018 study [13]. In semistructured interviews of minority resident physicians, the authors asked about residents’ perceptions of how their racial identity affected their residency training. Minority trainees commonly reported that aspects of their cultural identity were ignored at work or they were perceived as threatening. They also often reported their residency programs made little effort to integrate aspects of minority culture into the educational environment, and these experiences intensified a sense of “otherness” among the trainees. The challenges that come with the perception of otherness often lead to the minority physician having difficulty reconciling their personal and professional identity, feeling pressure to assimilate socially, adopting a strategy of hypervigilance at work, and ultimately grappling with the negative consequence of social isolation in their work environment. Based on the potential negative consequences of perpetuating otherness among minority trainees, we argue that the mentioned example statements, which perpetuate this sense of otherness, do little to foster inclusion of minority residents or to improve their acumen as a surgeon. We recommend against providing this type of exclusionary feedback to any orthopaedic trainee. In contrast, the most commonly reported statements were ones that were also some of the least perceived as racially biased. These statements were that the trainee was at an inferior intellectual and/or surgical skill level compared with their peers. Despite having a lower perception of racial bias, these statements were still perceived as biased by at least two-thirds of recipients. The implications of these statements and any perceived racial bias in the example statements are complex. Feedback (positive and negative) regarding academic and surgical performance during surgical training is a critical component in the development of the orthopaedic workforce. It is certainly plausible that negative performance feedback received by a particular respondent was warranted and was not given with biased intent. However, the context in which bias was perceived in these statements was not queried in our survey. The respondent may have had other experiences of similar negative performance feedback from another superior and might not have recalled any racial bias from that particular individual. However, the study survey question asks the respondent to recall whether they have ever perceived a specific experience of bias with regard to these statements about intellect and surgical skill. The context could have been from a superior who had demonstrated bias or inequitable treatment toward that trainee or other trainees who were non-White. Alternatively, previous experiences of racial bias in the workplace environment may have contributed to hypervigilance toward bias that made it difficult for the respondent to determine whether the feedback was genuine or colored by implicit or explicit bias. The context behind each recollection of bias in these statements is unknown. However, in both scenarios, we ask, how does an orthopaedic faculty member provide candid feedback to their trainees across the racial divide without implying racial bias?
Cohen et al. [7] sought to answer this specific question by giving Black and White students at Stanford University an essay-writing assignment and then providing three different types of feedback. In the setting of “unbuffered feedback,” students received critical feedback on their essay with no additional comments. In the setting of what they coined as “wise feedback,” students received the same negative or critical feedback; however, this feedback was complemented by a statement that the faculty had extremely high standards and affirmation that despite the negative feedback, the student possessed the capacity and intellect to reach those high standards. Finally, in what the authors termed “positive buffer feedback,” students received negative feedback buffered only by standard praise of the student’s performance. Interestingly, more Black students who received unbuffered feedback rated the essay reviewer as biased than White students did. Positive buffer feedback did not result in a decreased perception of bias by Black students. This difference in the perception of bias disappeared only in the setting of negative feedback that was complemented by a statement of high standards and assurance that the student could reach those standards (“wise feedback”). This may serve as a framework for presenting negative formal and informal feedback to Black orthopaedic residents without perception of bias. We understand the feedback process can often be nuanced and requires a different approach for each individual resident based on their learning style and skill level. The list of potentially problematic statements provided (Table 3) is by no means exhaustive, but it may provide the concerned orthopaedic educator with broad categories of feedback statements they might consider avoiding or modifying because of the higher likelihood of those statements being received as biased.
Differences in Perceived Microaggressions and Racially Biased Statements Based on Gender
Given the high frequency of microaggressions and workplace discriminations reported by Samora et al. [16] among women orthopaedic surgeons and trainees, we sought to evaluate whether respondents who were both gender and racial minorities in orthopaedics would experience microaggressions at a higher rate. Although there was no difference in the frequency of microassaults or environmental microaggressions reported by women, we found that surveyed women received racial microassaults more frequently from attending faculty (52% [34 of 65]) than was reported by surveyed men (34% [82 of 244]) and more frequently received devaluing or exclusionary statements from their superiors. These data mirror those of Goulart et al. [8], who found that among trainees in plastic surgery, women residents received microaggressions more often from faculty who were men (62%) than men plastic surgery residents did (38%). As discussed previously, research has shown that these microaggressions are rarely reported to programs directors, likely because of the high rate of fear of faculty retaliation [2]. Given the hierarchal structure of many orthopaedic training environments, it is vital that department chairs and program directors provide safe spaces for women, and particularly minority women residents, to report these incidents. As an alternative, department leadership can also preemptively inform their women residents regarding who to speak with in the graduate medical education office if they are experiencing microaggressions from faculty.
Conclusion
Our study shows that perception of workplace discrimination during orthopaedic training is high among Black orthopaedic surgeons in the United States. Most respondents reported experiencing discrimination, bias, and exclusion that could be categorized as specific types of racial microaggressions, including microassaults, microinsults, and environmental microaggressions. The initiators of these microaggressions were most commonly patients and attending faculty. Black women respondents were more likely to report receiving racially explicit statements from attending faculty and more likely to report receiving devaluating or exclusionary feedback statements from their superiors. Reports from other surgical subspecialties show that microaggressions experienced by women and minority residents are rarely reported to program directors or department chairs because of fear of retaliation. Given this information, we recommend that orthopaedic residency leaders be proactive in providing residents with information on designated advocates in their department or the graduate medical education office to report conflict or experiences of racial bias or discrimination. Finally, although feedback from superiors is an important part of the trainee learning experience, certain feedback statements that focus on a trainee not fitting the culture of the program, filling a diversity quota, or being perceived as intimidating are often perceived as racially biased. We recommend that orthopaedic leadership consider educating teaching faculty on avoidance of statements that convey exclusion of the resident and consider further education on strategies to provide “wise” feedback to trainees.
Acknowledgment
We thank the J. Robert Gladden Orthopaedic Society for providing access to their database of Black orthopaedic surgeons, fellows, and residents.
Footnotes
Each author certifies that there are no funding or commercial associations (consultancies, stock ownership, equity interest, patent/licensing arrangements, etc.) that might pose a conflict of interest in connection with the submitted article related to the author or any immediate family members.
All ICMJE Conflict of Interest Forms for authors and Clinical Orthopaedics and Related Research® editors and board members are on file with the publication and can be viewed on request.
This study was considered exempt from institutional review board approval.
This study was performed at the at the Texas Scottish Rite for Children, University of Texas-Southwestern, Dallas, TX, USA.
Contributor Information
Scott E. Porter, Email: scott.porter@prismahealth.org.
Kellie K. Middleton, Email: kelmd6@gmail.com.
Eric W. Carson, Email: carsonew@wustl.edu.
Gabriella E. Ode, Email: gabriellaode@gmail.com.
References
- 1.AAOS Orthopaedic Practice in the US 2018. Available at: https://www.aaos.org/quality/practice-management/aaos-orthopaedic-surgeon-census/orthopaedic-practice-in-the-u.s.-2018. Accessed October 1, 2021.
- 2.Alimi Y, Bevilacqua LA, Snyder RA, et al. Microaggressions and implicit bias in surgical training: an undocumented but pervasive phenomenon. Ann Surg. Published online April 9, 2021. DOI: 10.1097/SLA.0000000000004917. [DOI] [PubMed] [Google Scholar]
- 3.Blume AW, Lovato LV, Thyken BN, Denny N. The relationship of microaggressions with alcohol use and anxiety among ethnic minority college students in a historically White institution. Cultur Divers Ethnic Minor Psychol. 2012;18:45-54. [DOI] [PubMed] [Google Scholar]
- 4.Burkard AW, Boticki MA, Madson MB. Workplace discrimination, prejudice, and diversity measurement: a review of instrumentation. J Career Assess. 2002;10:343-361. [Google Scholar]
- 5.Chae DH, Clouston S, Hatzenbuehler ML, et al. Association between an internet-based measure of area racism and black mortality. PLoS One. 2015;10:e0122963. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Chung YB, Harmon LW. Assessment of perceived occupational opportunity for Black Americans. J Career Assess. 1999;7:45-62. [Google Scholar]
- 7.Cohen GL, Steele CM, Ross LD. The mentor’s dilemma: providing critical feedback across the racial divide. Pers Soc Psychol Bull . 1999;25:1302-1318. [Google Scholar]
- 8.Goulart MF, Huayllani MT, Balch Samora J, Moore AM, Janis JE. Assessing the prevalence of microaggressions in plastic surgery training: a national survey. Plast Reconstr Surg Glob Open . 2021;9:e4062. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Harris PA, Taylor R, Minor BL, et al. The REDCap consortium: building an international community of software platform partners. J Biomed Inform. 2019;95:103208. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Khubchandani JA Atkinson RB Ortega G. et al. Perceived discrimination among surgical residents at academic medical centers. J Surg Res. 2022;272:79-87. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Nadal KL, Wong Y, Griffin KE, et al. The adverse impact of racial microaggressions on college students’ self-esteem. J College Student Development. 2014;55:461-474. [Google Scholar]
- 12.Ode GE, Brooks JT, Middleton KK, Carson EW, Porter SE. Perception of racial and intersectional discrimination in the workplace is high among black orthopaedic surgeons: results of a survey of 274 black orthopaedic surgeons in practice. J Am Acad Orthop Surg. 2022;30:7-18. [DOI] [PubMed] [Google Scholar]
- 13.Osseo-Asare A, Balasuriya L, Huot SJ, et al. Minority resident physicians’ views on the role of race/ethnicity in their training experiences in the workplace. JAMA Netw Open. 2018;1:e182723. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Pierce CM. Black psychiatry one year after Miami. J Natl Med Assoc. 1970;62:471-473. [PMC free article] [PubMed] [Google Scholar]
- 15.Poon S, Kiridly D, Mutawakkil M, et al. Current trends in sex, race, and ethnic diversity in orthopaedic surgery residency. J Am Acad Orthop Surg. 2019;27:e725-e733. [DOI] [PubMed] [Google Scholar]
- 16.Samora JB, Denning J, Haralabatos S, Luong M, Poon S. Do women experience microaggressions in orthopaedic surgery? Current state and future directions from a survey of women orthopaedists. Curr Orthop Pract . 2020;31:503-507. [Google Scholar]
- 17.Sue DW, Capodilupo CM, Torino GC, et al. Racial microaggressions in everyday life: implications for clinical practice. Am Psychol. 2007;62:271-286. [DOI] [PubMed] [Google Scholar]
- 18.Torres L, Driscoll MW, Burrow AL. Racial microaggressions and psychological functioning among highly achieving African-Americans: a mixed-methods approach. J Soc Clin Psychol. 2010;29:1074-1099. [Google Scholar]
- 19.Torres MB, Salles A, Cochran A. Recognizing and reacting to microaggressions in medicine and surgery. JAMA Surg. 2019; 154:868-872. [DOI] [PubMed] [Google Scholar]