Abstract
Objective
To describe the impact of the 10-valent pneumococcal conjugate vaccine on the pediatric burden of pneumococcal infections, carriage, serotype replacement, and antimicrobial resistance in Brazil since its introduction in 2010.
Data source
A narrative review of English, Spanish, and Portuguese articles published in online databases and in Brazilian epidemiological surveillance databases was performed. The following keywords were used: Streptococcus pneumoniae, pneumococcal disease, conjugate vaccine, PCV10, antimicrobial resistance, and meningitis.
Summary of the findings
Declines in hospitalization rates of all-cause pneumonia occurred in the target age groups and some age groups not targeted by vaccination early after the use of PCV10. Large descriptive studies of laboratory-confirmed pneumococcal meningitis and hospital-based historical series of hospitalized children with IPD have evidenced a significant impact on disease burden, in-hospital fatality rates, and admission to the intensive care unit before and after the inclusion of the vaccine. Impact data on otitis media is limited and inconsistent; the main benefit remains the prevention of complicated diseases. During the late post-vaccine years, a significant and progressive increase in high-level penicillin non-susceptibility pneumococci has been described. Since 2014 serotype 19A has been the leading serotype in all ages and was responsible for 28.2%–44.6% of all IPD in children under 5 yrs.
Conclusions
PCV10 has performed a significant impact on IPD in Brazil since 2010, however, progress has been continuously hampered by replacement. Broader spectrum PCVs could provide expanded direct and indirect protection against ST19A and other additional serotypes of increasing importance if administered to children in the Brazilian National Immunization Program.
Keywords: Streptococcus pneumoniae, Pneumococcus, Pneumococcal disease, IPD, Serotypes, PCV10
Introduction
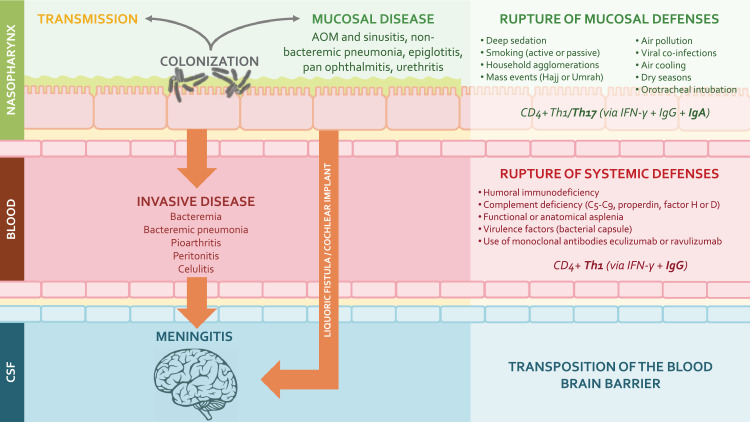
Streptococcus pneumoniae (pneumococcus) is a leading cause of community-acquired pneumonia (CAP), meningitis, and bacteremia (considered high-priority vaccine-preventable diseases) in children, the elderly, and high-risk populations.1,2 According to the World Health Organization, more than 318 000 children under 5 die each year worldwide, with the highest mortality burden in resource-poor regions.1,3 Pneumococcus, a common transient colonizer of the human nasopharynx in young children, has more than 100 serotypes, but a relatively small number are responsible for most of the disease.4,5 Invasive disease (IPD: bacteremic pneumonia, meningitis, and sepsis) and non-invasive/mucosal disease (acute otitis media and non-bacteremic pneumonia) are rare events compared with the frequency of asymptomatic nasopharyngeal colonization – a mandatory precondition for transmission and disease (Figure 1).5, 6, 7
Figure 1.
Host and environmental factors affecting encapsulated bacteria (including S. pneumoniae) shedding and disease forms. Conjugate vaccines interfere with colonization and disease progression by eliciting robust mucosal immunity (CD4+ Th1/Th17, IgG and IgA) and systemic immunity (CD4+ Th1 and IgG) (developed by the authors, adapted from Supplemental references #60–63). Abbreviations: AOM – acute otitis media; CSF – cerebrospinal fluid.
Following the successful development of the Haemophilus B conjugated vaccine in the 1980 s, the first pneumococcal conjugate vaccines (PCVs) were developed in the 1990s by covalently conjugating capsular serotypes to carrier proteins.8 PCVs have proved to be adequately immunogenic in young children and highly effective against infection: from 2000 to 2015, the use of PCVs has led to near 40% reduction in pediatric cases of pneumococcal pneumonia worldwide.1
However, despite this unquestionable achievement in different settings, successful implementation has been followed by replacement disease – an increase in the incidence of pneumococcal disease caused by non-vaccine serotypes (NVT).6,9,10 In a mature PCV vaccination program, such a phenomenon can erode the impact seen initially after vaccine introduction. Therefore, this review will cover some historical aspects and the essential concepts that significantly reduced the burden of pneumococcal disease in infants and children under 5 years of age in Brazil. Also, by describing the extent of residual IPD in the post-vaccine era, the potential effect of a switch to higher-valency PCVs concerning serotype 19A and other emerging serotypes will be discussed.
Search sources and strategy
The authors have performed a narrative review of English, Spanish, and Portuguese articles published in the following online databases: Medline (via PubMed), Web of Science, Scopus, Scientific Electronic Library Online (SciELO), and Latin American & Caribbean Health Sciences Literature (LILACS). Epidemiological surveillance databases were also analyzed, when available, from local surveillance systems such as Sistema de Informação de Agravos de Notificação (SINAN) (via the Brazilian Ministry of Health´s open-access public health database system [DATASUS]),11 Centro de Vigilância Epidemiológica da Secretaria de Estado da Saúde de São Paulo (CVE/SP), and Sistema de Informação do Programa Nacional de Imunizações (please refer to Supplemental references).
Historical perspective of IPD in Brazil
Early in the 1980 s, penicillin-resistant pneumococci began to be described in South Africa, Europe, and the USA.12 Taunay et al. serotyped meningitis strains in the early 1990s in Brazil,13 and a few years later, Berezin et al. evaluated pediatric patients with pneumonia and meningitis caused by Spn.14 The most prevalent serotypes in these studies were 1, 5, 6B, and 14 – the former was considered the leading serotype in pediatric IPD in Brazil at that time. Other evaluations performed in the same period resulted in similar serotypes distribution.15
At the end of the decade, led by this public health priority and to strengthen the scientific and technological capacity of the countries of Latin America and the Caribbean, the Pan American Health Organization (PAHO) established the Regional Vaccine System for Latin America (Sistema Regional de Vacunas para América Latina - SIREVA)16 as a source for basic research and to promote the development of affordable vaccines with appropriate serotype formulation for the region. In 1993, with financial support from the Government of Canada, a pilot laboratory surveillance study to evaluate the serotype distribution and antimicrobial resistance of S. pneumoniae causing invasive disease in children under 5 years began.16
The era of universal pneumococcal vaccination in Brazil
The 23-valent pneumococcal polysaccharide vaccine (PPV23; Pneumovax™, Merck Sharp & Dohme Corp.) was among the first vaccines commercialized to address the pneumococcal disease burden in 1983. This vaccine was able to protect against most of the serotypes associated with pneumococcal infections at that moment. However, due to its T-cell-independent mechanisms of action, it results in poor responses in children under 2 years of age, induces short-lasting immunity, lacks anamnestic/booster response upon subsequent challenge, and has no impact on the pneumococcal carriage (as with all unconjugated vaccines). Despite these limitations, PPV23 has been widely recommended for three decades for the direct protection of persons ≥ 2 years of age with selected chronic comorbidities that increase the risk of IPD, such as immunocompromising conditions, and in adults ≥ 65 years of age (Figure 2).
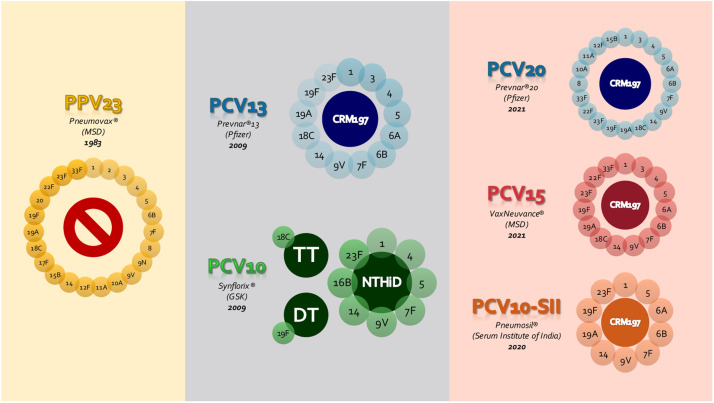
Figure 2.
Schematic of the pneumococcal vaccines available in 2022, including serotype composition (light colored circles), protein carrier (dark colored central circles), and year of licensure (developed by the authors, adapted from products packages insert). Abbreviations: PPV23 – 23-valent pneumococcal polysaccharide vaccine; PCV10 – 10-valent pneumococcal conjugate vaccine; PCV13 – 13-valent pneumococcal conjugate vaccine; PCV15 – 15-valent pneumococcal conjugate vaccine; PCV20 – 20-valent pneumococcal conjugate vaccine; PCV10-SII – 10-valent pneumococcal conjugate vaccine produced by Serum Institute of India; NTHiD – non-typeable Haemophilus influenzae protein D; TT – tetanus toxoid; DT – diphtheria toxoid; CRM197 – diphtheria toxoid variant CRM197 (Corynebacterium diphtheria cross-reactive material 197).
Based on the success of the recently developed vaccine conjugation system against Haemophilus influenzae b, the reports of increasing frequency of penicillin non-susceptible pneumococci, and the necessity to address the unmet needs of PPV23 in the pediatric population, the first pneumococcal conjugate vaccine was licensed.8 It included serotypes 4, 6B, 9V, 14, 18C, 19F, and 23F (PCV7; Prevenar™, Wyeth Pharmaceuticals LLC, a subsidiary of Pfizer Inc.) and was first authorized in the USA for use in children in 2000. In Brazil, PCV7 was introduced into its National Immunization Program (NIP) in 2007 to high-risk groups only, offering no or limited herd protection.
A decade after PCV7 approval, two second-generation, higher-valent conjugate vaccines that included additional serotypes were licensed based on immunogenicity data and replaced PCV7: a 10-valent (PCV10, Synflorix™, GlaxoSmithKline) and a 13-valent vaccine (PCV13, Prevnar™13, Wyeth Pharmaceuticals LLC, a subsidiary of Pfizer Inc.). They diverge in the number of serotypes included (ten serotypes in PCV10 and thirteen serotypes in PCV13) (Figure 2), polysaccharide concentration (more than double in PCV13 for seven of the ten shared serotypes), conjugation methods, and carrier protein – eight of the serotypes in PCV10 are conjugated to protein D, a surface lipoprotein of non-typeable Haemophilus influenzae (NTHi), and tetanus and diphtheria toxoids for the remaining two. In contrast, all serotypes in PCV13 are conjugated to diphtheria toxoid variant CRM197 (Corynebacterium diphtheria cross-reactive material 197).8
In March 2010, Brazil became the first country to introduce PCV10 into its routine childhood immunization program, free of charge, to all children under 2 years old. The recommended schedule included a 3+1 dose schedule (at 2, 4, and 6 months of age plus a booster at 12–18 months),17 which shifted to a 2+1 program (at 2 and 4 months plus a booster at 12–18 months) in 2016. Following the routine PCV vaccination, those at increased risk for IPD were additionally offered PPV23 after their second birthday (PCV-prime and PPV-boost schedule), and since September 2019, PCV13 was also provided to selected high-risk populations that did not receive PCV10: patients living with HIV/AIDS, hematopoietic stem cell transplant recipients, solid organ transplant recipients, and cancer patients).
Pneumococcal vaccine uptake in Brazil
Post-routine PCV introduction studies have demonstrated a substantial direct effect on vaccinated children but also on unvaccinated age groups.9 Such a highly desirable additional benefit from PCVs comprises an extension of this effect to those not targeted to receive the vaccine.18,19 Observational studies suggest that significant indirect (herd) effects can be achieved at 60%–75% coverage,20,21 while elimination or near-elimination of vaccine-type (VT) carriage and disease can only be achieved when PCV is given at sustained high rates (usually greater than 90%).22,23 By reducing VT carriage in the nasopharynx among vaccinees, conjugate vaccines interrupt the transmission of pneumococci to vaccine-ineligible groups, including the very young, older adults, and high-risk population7,24,25 (Figure 3).
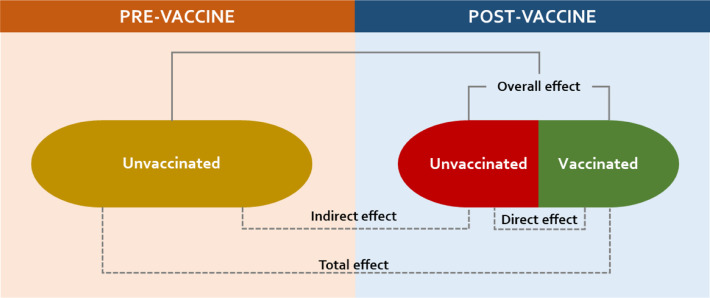
Figure 3.
Schematic of the varied vaccine effects in two populations, before and after national introduction, if high uptake is sustained through time (developed by the authors, adapted from Supplemental reference #64).
In Brazil, comprehensive national data on vaccine uptake are available on persons who receive publicly funded healthcare. These accounted for approximately 80% of the population, with heterogenous regional distribution.26 Early in the post-vaccine period in Brazil (the first 2-3 years after the implementation of PCV10), for example, significant declines in hospitalizations for all-cause pneumonia were described in major capitals but not in others with lower vaccination rates.27 After this period the average primary series uptake was 93.1% (range: 88.4–95.2%) and 85.3% (range: 76.3–93.1%) for the booster dose until 2018 nationally (http://tabnet.datasus.gov.br/cgi/deftohtm.exe?pni/cnv/cpniuf.def).11 However, since 2019 and fueled by the COVID-19 pandemic, fake news, politically-driven misinformation, and weakening of public health leadership, overall vaccine uptake declined dramatically in relation to previous years (Figure 4).28,29 Until the acceptance of this review, the year 2022 has reached the lowest historical vaccination rates for PCV10 following the first transition years: 53.6% for primary series and 45.5% for booster dose (http://tabnet.datasus.gov.br/cgi/deftohtm.exe?pni/cnv/cpniuf.def).11
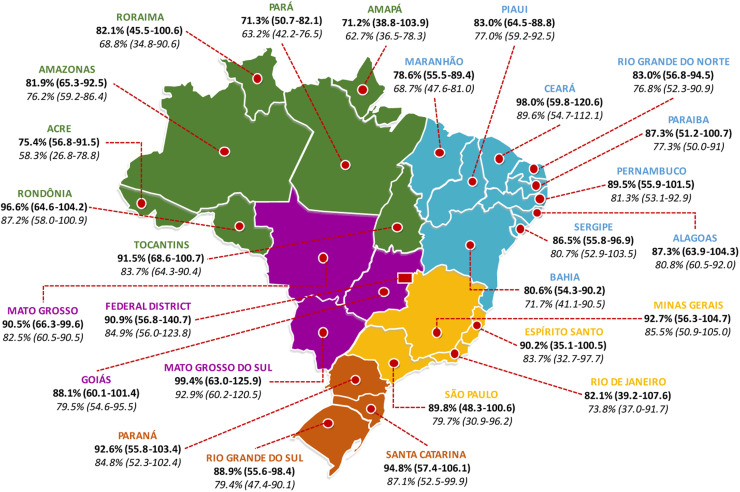
Figure 4.
Average PCV10 uptake (with range) for primary doses (in bold) and booster doses (in Italic), per Brazilian state, during late post-vaccine period (January 2012 – August 2022) National coverage data for full PCV10 vaccination among children (developed by the authors, data obtained from reference11 and adapted from reference29).
Vaccine impact on pneumonia and IPD hospitalization and childhood mortality
Systematic reviews have shown no evidence for differences in the effects of PCV10 and PCV13 against hospital admissions due to radiologically confirmed pneumonia and clinical pneumonia.17,30,31 In a recent systematic review including data from six Latin America and Caribbean countries, for example, PCV effectiveness against hospitalizations ranged from 7.4–20.6% for clinical pneumonia, 8.8–37.8% for radiographic confirmed pneumonia, 13.3–87.7% for meningitis, and 56–83.3% for IPD hospitalization.32 Attention should be drawn to the width of the 95% confidence intervals, as they may reveal imprecise estimates. Population-based studies using the Brazilian Unified Health System database (DATASUS) demonstrated significant declines in hospitalization rates of all-cause pneumonia, X-ray confirmed pneumonia and non-respiratory causes in children under 2 years of age in the early post-vaccination period.27,33, 34, 35 Five years after PCV10 introduction, similar reductions were described in the target age groups (17.4–26.5%; p < 0.01) and some age groups not targeted by vaccination (11.1–27.1%; p < 0.01), but no impact was seen among elderly over 65 years.36,37
From 1980 and 2010, pneumonia mortality in children younger than 5 years decreased by 10 times in Brazil (from 150 to 15 deaths per 100 000 children), a period during which the national Human Development Index rose substantially.38, 39, 40 Because randomized clinical trials generally do not have the power to detect significant mortality reductions from pneumococcal diseases, there are limited post-marketing PCV10 effectiveness studies in the country with such an endpoint.
Two long time-series studies used publicly available mortality data among Brazilian children younger than 5 years. The first was further stratified by socioeconomic status to address PCV-associated reduction in childhood pneumonia mortality.38 Although the introduction of PCV10 resulted only in a modest additional reduction at a national level (10%), substantially higher vaccine-related benefits occurred in the subpopulation living in extreme childhood poverty and low maternal education (point estimates of 16–24%) – particularly in younger children. Another research demonstrated consistent PCV10-associated declines in all-cause pneumonia hospitalizations in low- and high-income Brazilian populations.36
Finally, a third study compared the impact on pneumonia hospitalization rate following PCV10 implementation among the five administrative Brazilian regions (North, Northeast, Midwest, Southeast, and South)41 (Figure 4). The authors identified the largest hospitalization rate variation in the post-vaccine period in the North region of the country, where more significant increases were seen in the Human Development Index (very low in 2003; medium in 2010; high in 2017) and PCV10 coverage (from 58.79% in 2011 to 84.28% in 2017). In this administrative region, a significant decline that could be explained by vaccination was described only among age groups 0–4 years (12.5%; p = 0.01), 5–9 years (-38.5%; p < 0.01), and 10–14 years (-10.7%; p = 0.03).41 Putting these apparently low reductions in pneumonia mortality in perspective, even a modest benefit of the vaccine would translate into a large number of hospitalizations and deaths prevented annually in low-income and highly populated regions of Brazil.36,39, 40, 41
Like pneumonia, no randomized, head-to-head studies assessing the impact of both vaccines on IPD are available. Recent reports from Latin America have addressed the impact of PCV10 on IPD:42 Chile reported a significant decrease in invasive infections and mortality in children – attributed almost exclusively to meningitis cases43 but despite this initial success, PCV13 replaced PCV10 based on the increase of IPD caused by serotype 19A. A Brazilian group evaluated more than 14 400 episodes of laboratory-confirmed pneumococcal meningitis (PM) occurring between 2007 and 2021.44 In this descriptive study, PM incidence per 100 000 inhabitants was reduced from 2.5 during the pre-vaccine period (2007) to 1.5 in 2015, remained stable from 2016 through 2019 (1.11 cases/100 000 inhabitants), and then sharply declined to 0.33-0.39 during the COVID19 pandemic.
SIREVA, the largest and more reliable Brazilian database on IPD,16 relies on a passive surveillance network not designed to evaluate pneumococcal disease burden, disease incidence calculations, or vaccine impact. Alternatively, hospital-based historical series of hospitalized children with the pneumococcal disease have been used to assess the effect of PCV10 in severe disease.45 Berezin et al. described the changes in IPD episodes, in-hospital fatality rates, and admission to the intensive care unit before and after the inclusion of PCV10 in the Brazilian immunization program.45 Hospitalizations decreased from 20 cases to 5 cases per 10 000 pediatric admissions (p < 0.0001) and fatalities from 6.6 to 2.0 cases per 10 000 admissions (p < 0.0001) (driven mainly by meningitis and pneumonia). In contrast, 30% of cases required intensive care, with no percentual changes during the evaluation period. In addition, while IPD cases due to vaccine serotypes were reduced, infection rates caused by NVT increased.45
Another study evaluated the effect of PCV10 on hospitalizations, the need for intensive care, and outcomes in more than 700 cases of laboratory-confirmed pneumococcal infection at a large tertiary teaching hospital in Sao Paulo, Brazil.46 From 2000 to 2022, the annual IPD incidence rates in children under 5 years declined 69% (from 5.0 to 1.16 per 1 000 pediatric hospitalizations in the late post-vaccine period), while increases were evidenced in severe diseases among the high-risk population (from 36.3% to 47.2%) and case fatality rates also among healthy children (unpublished data).
Vaccine impact in non-invasive pneumococcal disease (nIPD)
Early and dense nasopharynx colonization with S. pneumoniae markedly increases the risk of acute otitis media (AOM).47 Following the completion of their primary PCV immunization, systemic immune responses are induced, and serotype-specific IgA and IgG antibodies are detected in saliva.9,48 Even higher antibody levels following subsequent booster vaccination lead to reduced vaccine-serotype-specific carriage.49 By reducing or eliminating nasopharyngeal colonization by VT pneumococcus, PCVs may ultimately reduce mucosal infections such as AOM.50 Additionally, by preventing early mucosal disease caused by VT, conjugate vaccines have the potential to disrupt the continuum of evolution from pneumococcal‐associated otitis media towards recurrent and chronic otitis media, thereby reducing the progression to subsequent and more complex disease caused by NVT and NTHi.51,52
Before the nationwide implementation of PCVs, the three leading bacterial pathogens isolated from the middle ear fluid of children with AOM were Streptococcus pneumoniae (up to 39%), non-typeable H. influenzae (up to 23%), and Moraxella catarrhalis (up to 15%).53,54 Despite limited and inconsistent data and extensive debate, recent evidence shows that successful implementation of pneumococcal vaccination has led to substantial reductions in ambulatory care visit rates for AOM, greater efficacy for more severe outcomes (such as complex otitis, tympanostomy tube placement, and recurrent otitis media), and near-elimination in the occurrence of such otopathogens included in the vaccine.52,55, 56, 57, 58, 59, 60 In addition, as expected for PCVs, colonization by vaccine serotypes decreased in the post-vaccine period among toddlers in Brazil, while, surprisingly, colonization by NTHi increased from 26% at baseline to 43.6%.61
No studies have evaluated the impact of PCV10 in pneumococcal OM in the Brazilian population, mainly due to limitations in obtaining middle ear fluid cultures for microbiologic diagnosis.52 Alternatively, case-based electronic data from the Outpatient Visits Information System of the Unified Health System have been used to measure the impact of PCV10 on all-cause pediatric OM. In an interrupted time-series analysis conducted in Goiania, Brazil, the estimated impact of PCV10 on all-cause OM was 43.0% (95% CI: 41.4–44.5%).62 When PCV10 was given to healthy infants during early infancy, the all-cause AOM risk varied from 6% (95% CI: −6% to 17%) to 15% (95%CI: −1% to 28%) – neither of these estimates reaching significance.50 Despite the encouraging data regarding the impact of PCV10 on the overall burden of otitis media, the main benefit of these vaccines remains the prevention of complicated disease.60
Vaccine impact in pneumococcal carriage, serotype replacement, and residual IPD burden
Conjugated vaccines have demonstrated a marked impact on the acquisition of vaccine-type serotypes in the nasopharynx.63 Significant geographical differences and redistribution of serotypes in the late post-vaccine period, driven by the selective pressure of PCVs (serotype replacement), have reduced the prevalence of serotypes included in the vaccine, but also a concerning emergence of NVT causing residual disease.6 All commercially available PCVs can result in a replacement. Still, there is insufficient evidence to direct comparisons of whether the changes in pneumococcal dynamics are more pronounced with one product or the other.55,64 After more than two decades of serotype replacement following the introduction of PCVs worldwide, the authors have learned that the population structure of pneumococci is reshaped due to the expansion of a limited number of NVT in carriage and disease.22
Pneumococcal carriage data can also predict reductions in VT and NVT following PCV introduction. Data on PCV10 impact on the nasopharyngeal carriage is limited in Brazil. An extensive carriage assessment among children living in São Paulo reported a 91% reduction in colonization by VT and a significant increase in NVT – mainly driven by serotype 6C – after 3 years of PCV10 use.61 An updated analysis compared the prevalence of nasopharyngeal colonization by VT between the pre-PCV10 survey (2010) and post-PCV10 survey (2017): carriage by vaccine type decreased 95.5% compared to that at baseline (19.8%), while NVT colonization increased by 185% in the late post-PCV10 survey – driven by serotype 6C (883.3% increase), NVT isolates (501% increase), non-PCV10 types (273.9% increase), and serotype 19A (233.3% increase).65
Despite the importance of bacterial carriage in the pathogenesis of the pneumococcal disease (Figure 1), data from the mucosa should not be fully extrapolated to symptomatic infection. For example, complete nasopharyngeal replacement of VT by non-VT after PCV implementation leads to incomplete replacement with less virulent serotypes in disease.55,66,67 While no randomized, head-to-head studies became available, a subnational Swedish study comparing regions using PCV10 and PCV13 in equivalent populations revealed a similar overall residual IPD burden. However, in areas using PCV10, the serotype share was taken up by 6A and 19A, while in those using PCV13, it was taken up by non-PCV13 serotypes.68
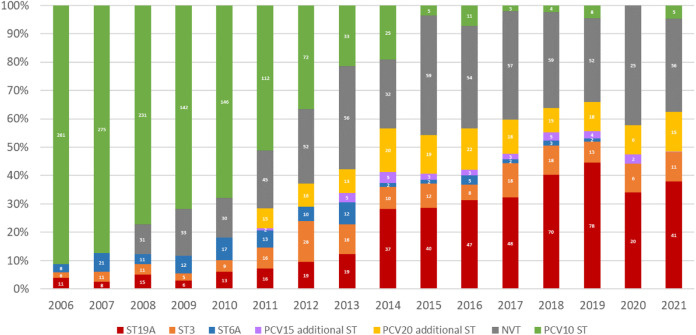
Similarly, in Brazil, serotype 19A in the vaccine-eligible group increased from an average of 3.5% (range: 1.4%–5.0%) in the pre-PCV10 period and early vaccine period to 39% on average from 2019 and 2021 (Figure 5). Serotype 3 (considered unique due to its abundant capsule, vaccine escape capabilities, and enhanced virulence69) showed a similar trend jumping from a 3.2% average in 2016 to 8.0% later in 2017, reaching two historical records of 10.2% in 2020 and 2021.70
Figure 5.
Distribution of IPD cases caused by additional PCV13 serotypes (3, 6A and 19A), PCV15 unique serotypes (22F and 33F), PCV20 exclusive serotypes (8, 10A, 11A, 12F, and 15B), and non-vaccine serotypes (NVT) in children under 5 years in Brazil, 2006-2021 (developed by the authors, adapted from Ref.70). Abbreviations: ST – serotype.
Vaccine impact in antibiotic-resistant pneumococci
Antimicrobial-resistant pneumococci were documented in humans as early as 1917 when optochin resistance was first described. In 1939, treatment-acquired sulfonamide resistance was reported in a case of meningitis, but it was not until 1965 that the first clinical penicillin-resistant pneumococci were reported in humans. During the 1970 s and 1980 s, pneumococcal resistance to penicillin, trimethoprim-sulfamethoxazole, and erythromycin increased and spread rapidly worldwide,12,18 while tetracycline and chloramphenicol resistances were also described with varied rates. In addition, multidrug-resistant strains (defined as reduced susceptibility to three or more chemical classes of antimicrobials) have become increasingly prevalent and are particularly associated with carriage and disease among young children.18
Consequently, pneumococcus has been a prominent cause of antibiotic consumption globally.71 As previously described, PCVs are considered a powerful strategy to reduce resistance,71, 72, 73 mainly by preventing the horizontal spread of non-susceptible strains within a community and reducing antibiotic use (thus alleviating selection pressure from broad-spectrum antibiotics).18,72 Multiple pneumococcal strains can concurrently colonize the same host (a phenomenon known as co-colonization or multiple serotype carriage).65 When associated with biofilm formation, it favors horizontal gene transfer – the primary evolutionary mechanism of Streptococcus species.5,74 Of the seven serotypes frequently associated with resistance (6A, 6B, 9V, 14, 19A, 19F, and 23F), serotype 19A is the only clinically significant, globally prevalent, highly multidrug-resistant, and not at all affected by PCV10.75
In Brazil, like other countries that have not incorporated PCV13 into their NIP, a combination of clonal expansion of NVT and capsule switch led to the development of serotype 19A lineages with high-level penicillin non-susceptibility.18,76,77 In a large study that evaluated 11 380 isolates from the SIREVA project,76 a reduction of infections due to penicillin (MIC ≥ 0.125 mg/l) and ceftriaxone (MIC ≥ 1.0 mg/l) non-susceptible pneumococcal strains was observed during the early post-vaccine period versus pre-PCV10 years in Brazil. From 2014 to 2019, this trend was followed by a significant and progressive increase in the proportion of Spn with higher MIC break points to penicillin (39.4%) and ceftriaxone (19.7%) – driven mainly by serotypes 19A, 6C, and 23A (Table 1). In addition, multidrug resistance reached an alarming 75% from 2018 to 2021.70
Table 1.
Penicillin susceptibility profile among meningeal and non-meningeal S. pneumoniae strains in children under 5 years in Brazil, 2006-2021. Prevalence of highly resistant serotype 19A (ST19A) is provided (adapted from reference70).
| Year | MENINGITIS STRAINS |
NON-MENINGITIS STRAINS |
ST19A | |||||
|---|---|---|---|---|---|---|---|---|
| Non-susceptible | Susceptible | n | Non-susceptible | Intermediate resistance | Susceptible | n | N (%) | |
| 2006 | 45.0% | 55.0% | 222 | 32.8% | 32.8% | 34.3% | 64 | 11 (3.8%) |
| 2007 | 48.6% | 51.4% | 220 | 0.0% | 17.9% | 82.1% | 75 | 8 (2.5%) |
| 2008 | 48.3% | 51.7% | 145 | 0.0% | 14.9% | 85.1% | 154 | 15 (5.0%) |
| 2009 | 46.5% | 53.5% | 129 | 0.0% | 18.8% | 81.2% | 69 | 6 (3.0%) |
| 2010 | 53.6% | 46.4% | 140 | 0.0% | 17.3% | 82.7% | 75 | 13 (6.0%) |
| 2011 | 35.7% | 64.3% | 126 | 0.0% | 9.7% | 90.3% | 93 | 16 (7.3%) |
| 2012 | 36.3% | 63.7% | 91 | 0.0% | 7.5% | 92.5% | 106 | 19 (9.6%) |
| 2013 | 32.3% | 67.7% | 62 | 0.0% | 10.9% | 89.1% | 92 | 19 (12.3%) |
| 2014 | 38.6% | 61.4% | 57 | 0.0% | 18.6% | 81.4% | 87 | 37 (28.2%) |
| 2015 | 40.0% | 60.0% | 55 | 0.0% | 20.0% | 80.0% | 85 | 40 (28.6%) |
| 2016 | 32.3% | 67.7% | 62 | 0.0% | 16.1% | 83.9% | 88 | 47 (31.3%) |
| 2017 | 48.0% | 52.0% | 58 | 0.0% | 9.0% | 91.0% | 91 | 48 (32.2%) |
| 2018 | 45.6% | 54.4% | 57 | 0.0% | 23.1% | 76.9% | 117 | 70 (40.2%) |
| 2019 | 65.0% | 35.0% | 80 | 1.1% | 28.7% | 70.2% | 94 | 78 (44.6%) |
| 2020 | 66.7% | 33.3% | 12 | 0.0% | 28.9% | 71.1% | 47 | 20 (33.9%) |
| 2021 | 66.7% | 33.3% | 29 | 0.0% | 28.9% | 71.1% | 79 | 41 (38.0%) |
Burden of pneumococcal disease due to serotypes included in the new PCVs
The constant shift in serotype distribution and pneumococcal disease led to the development of new vaccine platforms and products to solve unmet needs in varied settings. A new 10-valent PCV (PCV10-SII; Pneumosil™, Serum Institute of India, Pvt. Ltd) includes serotype 19A and other prevalent disease-causing serotypes in Latin America and the Caribbean, Africa, and Asia, conjugated to CRM197. The comparable performance to PCV10 and PCV13, unprecedented low cost, and WHO prequalification could make it an affordable and accessible option for LMICs. Broader spectrum PCVs have also been developed, and more formulations are in the pipeline for the next decade. The serotypes covered in these new PCVs are associated with a more significant disease burden in countries with mature PCV13 vaccination programs:78 a 15-valent vaccine (PCV15; VaxNeuvance™, Merck Sharp & Dohme Corp.) adds unique serotypes 22F and 33F and is approved for children and adults; a 20-valent vaccine (PCV20; Prevnar™20, Wyeth Pharmaceuticals LLC, a subsidiary of Pfizer Inc.) adds 5 additional serotypes compared to PCV15 (8, 10A, 11A, 12F, and 15B) and has been licensed for adults only, with approval to infants expected shortly.
In Brazil, the potential benefits of broader serotype coverage can be extrapolated from the distribution of such serotypes during post-PCV10 years (Figure 5). PCV15 unique serotypes accounted for 0.5% during the years 2011-2012, increasing to 2.5% on average (range: 0.3–3.8%) from 2013 to 2021. PCV20 additional serotypes were responsible for 7.5% of invasive diseases during the early vaccine period, increasing to 11.9% on average (range: 8.4–15.3%) during the late post-vaccine years. While PCV20 aims for wider coverage, PCV15 new conjugation technique resulted in improved immunologic responses against serotype 3 compared to PCV13. Real-world data is required to address the impact of this laboratory advantage on disease.
Further prospects on pneumococcal vaccination
In order to alleviate some of the limitations of the PCVs currently in use – particularly the issue of serotype replacement and the reduced immunogenicity and efficacy for serotype 3 – a new generation of pneumococcal vaccines is under development. New vaccine platforms aim for distinct pneumococcal proteic antigens (such as pneumococcal surface proteins A [PspA] and C [PspC], pneumolysin [Ply], pneumococcal histidine triad protein D [PhtD], elongation factor Tu [EF-Tu], and pneumococcal peptide 27 [Pep27]), new delivery system technologies, and enhanced immunogenicity (through conjugation to Toll-like receptors and reformulation into nanoparticle). Whole-cell vaccines can express all protein antigens without purification of individual proteins, conferring broader protection. Refer to Supplemental references for further reading.
Future perspectives for PCV vaccination in Brazil
Despite the significant impact of PCV10 on the pneumococcal disease since 2010, progress has been continuously hampered by serotype replacement. Given that (1) the once hypothesized PCV10 cross-protection against vaccine-related serotypes (mainly 19A) was not confirmed in clinical and epidemiologic studies from Brazil,45,46,65,79 and (2) PCV10 and PCV13 (and presumably PCV10-SII, PCV15, and PCV20) have a comparable impact on IPD, the authors believe that all PCVs that include serotype 19A can perform dramatic changes to the landscape of local serotype epidemiology. Moreover, considering the already discussed indirect effect of PCVs, these new vaccines can add additional protection to unvaccinated populations against other relevant serotypes if given to young children. That said, the country's choice between the available products will ultimately depend on vaccine cost, supply, and logistical factors.
Limitations
This manuscript was not intended as an exhaustive review PCVs comparability but rather as an overview of the impact of PCV10 in Brazil using local data. Consequently, a comprehensive systematic search was not performed, therefore some of the available evidence may have been missed. Although hospitalizations and PCV10 coverage data were obtained from administrative databases, the burden of community-acquired pneumonia shows similar estimates when compared to hospital primary data.80 Therefore, these sources are reliable to evaluate PCV10 vaccination as a pneumonia intervention. Similarly, surveillance information such as SIREVA can be used to assess circulating strains, support decision-making on vaccine introduction, and provide guidelines for antibiotic use. However, as reporting to laboratory-based systems is not compulsory in Latin America and the Caribbean (except for pneumococcal meningitis), such national passive surveillance systems are subject to under-reporting and lack of representativeness in IPD occurrence. The proportion of SIREVA-reported isolates, for example, in relation to the estimated expected cases varies considerably between the countries and is estimated to be less than 10% in Brazil.81 Therefore, such data require cautious interpretation due to timely and limited data availability, as well as heterogeneous case reporting and laboratory diagnosis of IPD.42,81 Additional references are provided as Supplemental references for further reading.
Conclusion
In a scenario of consistent improvements in healthcare delivery, socioeconomic status, and health interventions impacting childhood mortality in Brazil, PCV10 adds relatively modest reductions (but expressive in absolute terms) of hospitalization and mortality from pneumococcal diseases, especially in lower-income regions of the country. However, progress has been continuously hampered by replacement. Broader spectrum PCVs could provide expanded direct and indirect protection against ST19A and other additional serotypes of increasing importance if administered to children in the Brazilian NIP.
Disclaimer
The authors' findings and conclusions are those of the authors and do not necessarily represent the views of the institutions cited in the article.
Conflicts of interest
DJ has received grants to support research projects from Pfizer and Merck, Sharp & Dohme and honorary fees from Abbott, Pfizer, GlaxoSmithKline, Janssen, Cepheid, and Sanofi‐Pasteur. ENB declares no potential conflict of interest. The authors declare that the manuscript was conducted without any financial relationships that could be construed as a potential conflict of interest.
Footnotes
Supplementary material associated with this article can be found in the online version at doi:10.1016/j.jped.2022.11.003.
Appendix. Supplementary materials
References
- 1.Wahl B., O'Brien K.L., Greenbaum A., Majumder A., Liu L., Chu Y., et al. Burden of streptococcus pneumoniae and haemophilus influenzae type b disease in children in the era of conjugate vaccines: global, regional, and national estimates for 2000-15. Lancet Glob Health. 2018;6 doi: 10.1016/S2214-109X(18)30247-X. e744–e757. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Aliberti S., Dela Cruz C.S., Amati F., Sotgiu G., Restrepo M.I. Community-acquired pneumonia. Lancet. 2021;398:906–919. doi: 10.1016/S0140-6736(21)00630-9. [DOI] [PubMed] [Google Scholar]
- 3.Pneumococcal conjugate vaccines: WHO position paper [Internet]. Wkly Epidemiol Rec. 2019;94:85–104. [cited 2021 Nov 15]. Available from: https://apps.who.int/iris/rest/bitstreams/1209121/retrieve
- 4.Ganaie F., Saad J.S., McGee L., van Tonder A.J., Bentley S.D., Lo S.W., et al. A new pneumococcal capsule type, 10D, is the 100th serotype and has a large cps fragment from an oral streptococcus. mBio. 2020;11 doi: 10.1128/mBio.00937-20. e00937-20. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Weiser J.N., Ferreira D.M., Paton J.C. Streptococcus pneumoniae: transmission, colonization and invasion. Nat Rev Microbiol. 2018;16:355–367. doi: 10.1038/s41579-018-0001-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Devine V.T., Cleary D.W., Jefferies J.M., Anderson R., Morris D.E., Tuck A.C., et al. The rise and fall of pneumococcal serotypes carried in the PCV era. Vaccine. 2017;35:1293–1298. doi: 10.1016/j.vaccine.2017.01.035. [DOI] [PubMed] [Google Scholar]
- 7.Simell B., Auranen K., Käyhty H., Goldblatt D., Dagan R., O'Brien K.L., et al. The fundamental link between pneumococcal carriage and disease. Expert Rev Vaccines. 2012;11:841–855. doi: 10.1586/erv.12.53. [DOI] [PubMed] [Google Scholar]
- 8.Rappuoli R., De G.E., Costantino P. On the mechanisms of conjugate vaccines. Proc Natl Acad Sci USA. 2019;116:14–16. doi: 10.1073/pnas.1819612116. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Mackenzie G.A., Hill P.C., Jeffries D.J., Hossain I., Uchendu U., Ameh D., et al. Effect of the introduction of pneumococcal conjugate vaccination on invasive pneumococcal disease in The Gambia: a population-based surveillance study. Lancet Infect Dis. 2016;16:703–711. doi: 10.1016/S1473-3099(16)00054-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Ladhani S.N., Collins S., Djennad A., Sheppard C.L., Borrow R., Fry N.K., et al. Rapid increase in non-vaccine serotypes causing invasive pneumococcal disease in England and Wales, 2000-17: a prospective national observational cohort study. Lancet Infect Dis. 2018;18:441–451. doi: 10.1016/S1473-3099(18)30052-5. Erratum in: Lancet Infect Dis. 2018;18:376. [DOI] [PubMed] [Google Scholar]
- 11.Brazil. Ministry of Health, Informatics Department of the Brazilian Unified Health System. Informações de Saúde (TABNET) – DATASUS [Internet]. 2022 [cited 2022 Sep 1]. Available from: https://datasus.saude.gov.br/informacoes-de-saude-tabnet/
- 12.Chesney P.J. The escalating problem of antimicrobial resistance in Streptococcus pneumoniae. Am J Dis Child. 1992;146:912–916. doi: 10.1001/archpedi.1992.02160200034022. [DOI] [PubMed] [Google Scholar]
- 13.Taunay A.E., Austrian R., Landgraf I.M., Vieira M.F., Melles CE. Sorotipos de streptococcus pneumoniae isolados de líquido cefalorraquidiano no período de 1977-1988 na cidade de São Paulo, Brasil [Serotypes of Streptococcus pneumoniae isolated from cerebrospinal fluid in 1977-1988 in São Paulo City, Brazil] Rev Inst Med Trop Sao Paulo. 1990;32:11–15. doi: 10.1590/s0036-46651990000100003. [DOI] [PubMed] [Google Scholar]
- 14.Berezin E.N., Carvalho E.S., Casagrande S., Brandileone M.C., Mimica I.M., Farhat C.K. Streptococcus pneumoniae penicillin-nonsusceptible strains in invasive infections in Sao Paulo, Brazil. Pediatr Infect Dis J. 1996;15:1051–1053. doi: 10.1097/00006454-199611000-00027. [DOI] [PubMed] [Google Scholar]
- 15.Sessegolo J.F., Levin A.S., Levy C.E., Asensi M., Facklam R.R., Teixeira LM. Distribution of serotypes and antimicrobial resistance of Streptococcus pneumoniae strains isolated in Brazil from 1988 to 1992. J Clin Microbiol. 1994;32:906–911. doi: 10.1128/jcm.32.4.906-911.1994. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Di Fabio J.L., Agudelo C.I., Castañeda E. Sistema Regional de Vacunas (SIREVA), vigilancia por laboratorio y desarrollo de vacunas para Streptococcus pneumoniae: análisis bibliométrico, 1993-2019 [Regional System for Vaccines (SIREVA), laboratory surveillance and vaccine development for Streptococcus pneumoniae: bibliometric analysis, 1993-2019] Rev Panam Salud Publica. 2020;44:e80. doi: 10.26633/RPSP.2020.80. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Domingues C.M., Verani J.R., Montenegro Renoiner E.I., de Cunto Brandileone M.C., Flannery B., de Oliveira L.H., et al. Effectiveness of ten-valent pneumococcal conjugate vaccine against invasive pneumococcal disease in Brazil: a matched case-control study. Lancet Respir Med. 2014;2:464–471. doi: 10.1016/S2213-2600(14)70060-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Kim L., McGee L., Tomczyk S., Beall B. Biological and Epidemiological Features of Antibiotic-Resistant Streptococcus pneumoniae in Pre- and Post-Conjugate Vaccine Eras: a United States Perspective. Clin Microbiol Rev. 2016;29:525–552. doi: 10.1128/CMR.00058-15. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Pilishvili T., Lexau C., Farley M.M., Hadler J., Harrison L.H., Bennett N.M., et al. Sustained reductions in invasive pneumococcal disease in the era of conjugate vaccine. J Infect Dis. 2010;201:32–41. doi: 10.1086/648593. [DOI] [PubMed] [Google Scholar]
- 20.Loughlin A.M., Hsu K., Silverio A.L., Marchant C.D., Pelton SI. Direct and indirect effects of PCV13 on nasopharyngeal carriage of PCV13 unique pneumococcal serotypes in Massachusetts' children. Pediatr Infect Dis J. 2014;33:504–510. doi: 10.1097/INF.0000000000000279. [DOI] [PubMed] [Google Scholar]
- 21.Grant L.R., Hammitt L.L., O'Brien S.E., Jacobs M.R., Donaldson C., Weatherholtz R.C., et al. Impact of the 13-valent pneumococcal conjugate vaccine on pneumococcal carriage among American Indians. Pediatr Infect Dis J. 2016;35:907–914. doi: 10.1097/INF.0000000000001207. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Waight P.A., Andrews N.J., Ladhani S.N., Sheppard C.L., Slack M.P., Miller E. Effect of the 13-valent pneumococcal conjugate vaccine on invasive pneumococcal disease in England and Wales 4 years after its introduction: an observational cohort study. Lancet Infect Dis. 2015;15:535–543. doi: 10.1016/S1473-3099(15)70044-7. Erratum in: Lancet Infect Dis. 2015;15:629. [DOI] [PubMed] [Google Scholar]
- 23.Flasche S., Van Hoek A.J., Goldblatt D., Edmunds W.J., O'Brien K.L., Scott J.A., et al. The potential for reducing the number of pneumococcal conjugate vaccine doses while sustaining herd immunity in high-income countries. PLoS Med. 2015;12 doi: 10.1371/journal.pmed.1001839. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Ladhani S.N., Andrews N.J., Waight P., Borrow R., Slack M.P., Miller E. Impact of the 7-valent pneumococcal conjugate vaccine on invasive pneumococcal disease in infants younger than 90 days in England and Wales. Clin Infect Dis. 2013;56:633–640. doi: 10.1093/cid/cis934. [DOI] [PubMed] [Google Scholar]
- 25.Hanquet G., Krizova P., Valentiner-Branth P., Ladhani S.N., Nuorti J.P., Lepoutre A., et al. Effect of childhood pneumococcal conjugate vaccination on invasive disease in older adults of 10 European countries: implications for adult vaccination. Thorax. 2019;74:473–482. doi: 10.1136/thoraxjnl-2018-211767. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Schuck-Paim C., Taylor R.J., Simonsen L., Lustig R., Kürüm E., Bruhn C.A., et al. Challenges to estimating vaccine impact using hospitalization data. Vaccine. 2017;35:118–124. doi: 10.1016/j.vaccine.2016.11.030. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Afonso E.T., Minamisava R., Bierrenbach A.L., Escalante J.J., Alencar A.P., Domingues C.M., et al. Effect of 10-valent pneumococcal vaccine on pneumonia among children. Brazil Emerg Infect Dis. 2013;19:589–597. doi: 10.3201/eid1904.121198. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Daniels JP. Health experts slam Bolsonaro's vaccine comments. Lancet. 2021;397:361. doi: 10.1016/S0140-6736(21)00181-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Guzman-Holst A., de Barros E., Rubio P., DeAntonio R., Cintra O., Abreu A. Impact after 10-year use of pneumococcal conjugate vaccine in the Brazilian national immunization program: an updated systematic literature review from 2015 to 2020. Hum Vaccin Immunother. 2022;18 doi: 10.1080/21645515.2021.1879578. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Meeting of the Strategic Advisory Group of Experts on immunization October 2017 – conclusions and recommendations. Wkly Epidemiol Rec. 2017;92:729–747. [PubMed] [Google Scholar]
- 31.Loo J.D., Conklin L., Fleming-Dutra K.E., Deloria Knoll M., Park D.E., Kirk J., Goldblatt D., O'Brien K.L., Whitney C.G. Systematic review of the effect of pneumococcal conjugate vaccine dosing schedules on prevention of pneumonia. Pediatr Infect Dis J. 2014;33:S140–S151. doi: 10.1097/INF.0000000000000082. Suppl 2 Optimum Dosing of Pneumococcal Conjugate Vaccine For Infants 0 A Landscape Analysis of Evidence Supportin g Different Schedules. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.de Oliveira L.H., Camacho L.A., Coutinho E.S., Martinez-Silveira M.S., Carvalho A.F., Ruiz-Matus C., et al. Impact and effectiveness of 10 and 13-valent pneumococcal conjugate vaccines on hospitalization and mortality in children aged less than 5 years in Latin American countries: a systematic review. PLoS One. 2016;11 doi: 10.1371/journal.pone.0166736. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Scotta M.C., Veras T.N., Klein P.C., Tronco V., Polack F.P., Mattiello R., et al. Impact of 10-valent pneumococcal non-typeable Haemophilus influenzae protein D conjugate vaccine (PHiD-CV) on childhood pneumonia hospitalizations in Brazil two years after introduction. Vaccine. 2014;32:4495–4499. doi: 10.1016/j.vaccine.2014.06.042. [DOI] [PubMed] [Google Scholar]
- 34.Sgambatti S., Minamisava R., Bierrenbach A.L., Toscano C.M., Vieira M.A., Policena G., et al. Early impact of 10-valent pneumococcal conjugate vaccine in childhood pneumonia hospitalizations using primary data from an active population-based surveillance. Vaccine. 2016;34:663–670. doi: 10.1016/j.vaccine.2015.12.007. [DOI] [PubMed] [Google Scholar]
- 35.Abrão W.M., Mello L.M., Silva A.S., Nunes A.A. Impact of the antipneumococcal conjugate vaccine on the occurrence of infectious respiratory diseases and hospitalization rates in children. Rev Soc Bras Med Trop. 2015;48:44–49. doi: 10.1590/0037-8682-0007-2015. [DOI] [PubMed] [Google Scholar]
- 36.Warren J.L., Shioda K., Kürüm E., Schuck-Paim C., Lustig R., Taylor R.J., et al. Impact of pneumococcal conjugate vaccines on pneumonia hospitalizations in high- and low-income subpopulations in Brazil. Clin Infect Dis. 2017;65:1813–1818. doi: 10.1093/cid/cix638. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Andrade A.L., Afonso E.T., Minamisava R., Bierrenbach A.L., Cristo E.B., Morais-Neto O.L., et al. Direct and indirect impact of 10-valent pneumococcal conjugate vaccine introduction on pneumonia hospitalizations and economic burden in all age-groups in Brazil: a time-series analysis. PLoS One. 2017;12 doi: 10.1371/journal.pone.0184204. Erratum in: PLoS One. 2017;12:e0189039. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Schuck-Paim C., Taylor R.J., Alonso W.J., Weinberger D.M., Simonsen L. Effect of pneumococcal conjugate vaccine introduction on childhood pneumonia mortality in Brazil: a retrospective observational study. Lancet Glob Health. 2019;7:e249–e256. doi: 10.1016/S2214-109X(18)30455-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Camargos P., Zhang L., Nascimento-Carvalho CM. Effect of pneumococcal conjugate vaccines on mortality from lower respiratory infections and pneumonia among under-fives. Hum Vaccin Immunother. 2021;17:537–545. doi: 10.1080/21645515.2020.1787071. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Camargos P., Nascimento-Carvalho C.M., Teixeira R., França E. Lower respiratory infections mortality among Brazilians under-five before and after national pneumococcal conjugate vaccine implementation. Vaccine. 2020;38:2559–2565. doi: 10.1016/j.vaccine.2020.01.084. [DOI] [PubMed] [Google Scholar]
- 41.Ferreira M.N., Netto E.M., Nascimento-Carvalho CM. The impact of 10-valent pneumococcal conjugate vaccine upon hospitalization rate of children with pneumonia in different Brazilian administrative regions. Vaccine. 2021;39:2153–2164. doi: 10.1016/j.vaccine.2021.02.051. [DOI] [PubMed] [Google Scholar]
- 42.Agudelo C.I., Castañeda-Orjuela C., Brandileone M.C., Echániz-Aviles G., Almeida S.C., Carnalla-Barajas M.N., et al. The direct effect of pneumococcal conjugate vaccines on invasive pneumococcal disease in children in the Latin American and Caribbean region (SIREVA 2006-17): a multicentre, retrospective observational study. Lancet Infect Dis. 2021;21:405–417. doi: 10.1016/S1473-3099(20)30489-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Diaz J., Terrazas S., Bierrenbach A.L., Toscano C.M., Alencar G.P., Alvarez A., et al. Effectiveness of the 10-valent pneumococcal Conjugate Vaccine (PCV-10) in children in chile: a nested case-control study using nationwide pneumonia morbidity and mortality surveillance data. PLoS One. 2016;11 doi: 10.1371/journal.pone.0153141. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Berezin E.N., Jarovsky D., Ribeiro C.M., Fátima S.F. The panorama of pneumococcal meningitis in Brazil, 2007-2021 (Abstract #286). Proceedings of the 12th International Symposium on Pneumococci and Pneumococcal Diseases (ISPPD); Toronto, Canada; 2022. [Internet]. E-poster presented at. Jun[cited 2021 Nov 15]. Available from: [Google Scholar]
- 45.Berezin E.N., Jarovsky D., Cardoso M.R., Mantese O.C. Invasive pneumococcal disease among hospitalized children in Brazil before and after the introduction of a pneumococcal conjugate vaccine. Vaccine. 2020;38:1740–1745. doi: 10.1016/j.vaccine.2019.12.038. [DOI] [PubMed] [Google Scholar]
- 46.Jarovsky D. Clinical and microbiological profiles of IPD in hospitalized patients in a tertiary Brazilian hospital, 2000-2021 (Abstract #507). Proceedings of the 12th International Symposium on Pneumococci and Pneumococcal Diseases (ISPPD); Toronto, Canada; 2022. [Internet]. Oral presentation presented at. Jun[cited 2021 Nov 15]. Available from: [Google Scholar]
- 47.Schilder A.G., Chonmaitree T., Cripps A.W., Rosenfeld R.M., Casselbrant M.L., Haggard M.P., et al. Otitis media. Nat Rev Dis Primers. 2016;2:16063. doi: 10.1038/nrdp.2016.63. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Korkeila M., Lehtonen H., Ahman H., Leroy O., Eskola J., Käyhty H. Salivary anti-capsular antibodies in infants and children immunised with Streptococcus pneumoniae capsular polysaccharides conjugated to diphtheria or tetanus toxoid. Vaccine. 2000;18:1218–1226. doi: 10.1016/s0264-410x(99)00393-x. [DOI] [PubMed] [Google Scholar]
- 49.Choo S., Zhang Q., Seymour L., Akhtar S., Finn A. Primary and booster salivary antibody responses to a 7-valent pneumococcal conjugate vaccine in infants. J Infect Dis. 2000;182:1260–1263. doi: 10.1086/315834. [DOI] [PubMed] [Google Scholar]
- 50.de Sévaux J.L., Venekamp R.P., Lutje V., Hak E., Schilder A.G., Sanders E.A., et al. Pneumococcal conjugate vaccines for preventing acute otitis media in children. Cochrane Database Syst Rev. 2020;11 doi: 10.1002/14651858.CD001480.pub6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Dagan R., Pelton S., Bakaletz L., Cohen R. Prevention of early episodes of otitis media by pneumococcal vaccines might reduce progression to complex disease. Lancet Infect Dis. 2016;16:480–492. doi: 10.1016/S1473-3099(15)00549-6. [DOI] [PubMed] [Google Scholar]
- 52.Ben-Shimol S., Givon-Lavi N., Leibovitz E., Raiz S., Greenberg D., Dagan R. Near-elimination of otitis media caused by 13-valent pneumococcal conjugate vaccine (PCV) serotypes in southern Israel shortly after sequential introduction of 7-valent/13-valent PCV. Clin Infect Dis. 2014;59:1724–1732. doi: 10.1093/cid/ciu683. [DOI] [PubMed] [Google Scholar]
- 53.Jacobs M.R., Dagan R., Appelbaum P.C., Burch DJ. Prevalence of antimicrobial-resistant pathogens in middle ear fluid: multinational study of 917 children with acute otitis media. Antimicrob Agents Chemother. 1998;42:589–595. doi: 10.1128/aac.42.3.589. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Heikkinen T., Thint M., Chonmaitree T. Prevalence of various respiratory viruses in the middle ear during acute otitis media. N Engl J Med. 1999;340:260–264. doi: 10.1056/NEJM199901283400402. [DOI] [PubMed] [Google Scholar]
- 55.Izurieta P., Nieto Guevara J. Exploring the evidence behind the comparable impact of the pneumococcal conjugate vaccines PHiD-CV and PCV13 on overall pneumococcal disease. Hum Vaccin Immunother. 2022;18 doi: 10.1080/21645515.2021.1872341. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56.Ben-Shimol S., Givon-Lavi N., Kotler L., Greenberg D., Dagan R. 2903. Post PCV13 dynamics of NonVaccine serotype (NVT): disproportionate increase of the additional PCV20 candidate serotypes in respiratory and invasive disease in young children. Open Forum Infect Dis. 2019;6:S83–S84. [Google Scholar]
- 57.Kawai K., Adil E.A., Barrett D., Manganella J., Kenna MA. Ambulatory visits for otitis media before and after the introduction of pneumococcal conjugate vaccination. J Pediatr. 2018;201:122–127. doi: 10.1016/j.jpeds.2018.05.047. e1. [DOI] [PubMed] [Google Scholar]
- 58.Wiese A.D., Huang X., Yu C., Mitchel E.F., Kyaw M.H., Griffin M.R., et al. Changes in otitis media episodes and pressure equalization tube insertions among young children following introduction of the 13-valent pneumococcal conjugate vaccine: a birth cohort-based study. Clin Infect Dis. 2019;69:2162–2169. doi: 10.1093/cid/ciz142. [DOI] [PubMed] [Google Scholar]
- 59.Zhou X., de Luise C., Gaffney M., Burt C.W., Scott D.A., Gatto N., et al. National impact of 13-valent pneumococcal conjugate vaccine on ambulatory care visits for otitis media in children under 5 years in the United States. Int J Pediatr Otorhinolaryngol. 2019;119:96–102. doi: 10.1016/j.ijporl.2019.01.023. [DOI] [PubMed] [Google Scholar]
- 60.Sáfadi M.A., Jarovsky D. Acute otitis media in children: a vaccine-preventable disease? Braz J Otorhinolaryngol. 2017;83:241–242. doi: 10.1016/j.bjorl.2017.02.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Brandileone M.C., Zanella R.C., Almeida S.C., Brandao A.P., Ribeiro A.F., Carvalhanas T.M., et al. Effect of 10-valent pneumococcal conjugate vaccine on nasopharyngeal carriage of streptococcus pneumoniae and Haemophilus influenzae among children in São Paulo, Brazil. Vaccine. 2016;34:5604–5611. doi: 10.1016/j.vaccine.2016.09.027. [DOI] [PubMed] [Google Scholar]
- 62.Sartori A.L., Minamisava R., Bierrenbach A.L., Toscano C.M., Afonso E.T., Morais-Neto O.L., et al. Reduction in all-cause otitis media-related outpatient visits in children after PCV10 introduction in Brazil. PLoS One. 2017;12 doi: 10.1371/journal.pone.0179222. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63.Devine V.T., Jefferies J.M., Clarke S.C., Faust S.N. Nasopharyngeal bacterial carriage in the conjugate vaccine era with a focus on pneumococci. J Immunol Res. 2015;2015 doi: 10.1155/2015/394368. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.Balsells E., Guillot L., Nair H., Kyaw M.H. Serotype distribution of streptococcus pneumoniae causing invasive disease in children in the post-PCV era: a systematic review and meta-analysis. PLoS One. 2017;12 doi: 10.1371/journal.pone.0177113. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65.Brandileone M.C., Zanella R.C., Almeida S.C., Cassiolato A.P., Lemos A.P., Salgado M.M., et al. Long-term effect of 10-valent pneumococcal conjugate vaccine on nasopharyngeal carriage of Streptococcus pneumoniae in children in Brazil. Vaccine. 2019;37:5357–5363. doi: 10.1016/j.vaccine.2019.07.043. [DOI] [PubMed] [Google Scholar]
- 66.Hausdorff W.P., Hanage W.P. Interim results of an ecological experiment - Conjugate vaccination against the pneumococcus and serotype replacement. Hum Vaccin Immunother. 2016;12:358–374. doi: 10.1080/21645515.2015.1118593. Erratum in: Hum Vaccin Immunother. 2016;12:2478-81. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67.Weinberger D.M., Malley R., Lipsitch M. Serotype replacement in disease after pneumococcal vaccination. Lancet. 2011;378:1962–1973. doi: 10.1016/S0140-6736(10)62225-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Naucler P., Galanis I., Morfeldt E., Darenberg J., Örtqvist Å., Henriques-Normark B. Comparison of the impact of pneumococcal conjugate vaccine 10 or pneumococcal conjugate vaccine 13 on invasive pneumococcal disease in equivalent populations. Clin Infect Dis. 2017;65:1780–1789. doi: 10.1093/cid/cix685. Erratum in: Clin Infect Dis. 2019;68:534. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Luck J.N., Tettelin H., Orihuela C.J. Sugar-coated killer: serotype 3 pneumococcal disease. Front Cell Infect Microbiol. 2020;10 doi: 10.3389/fcimb.2020.613287. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Instituto Adolfo Lutz, Secretaria de Estado da Saúde. Boletim do Instituto Adolfo Lutz [Internet]. 2022. Available from: http://www.ial.sp.gov.br/ial/publicacoes/boletins
- 71.Buckley B.S., Henschke N., Bergman H., Skidmore B., Klemm E.J., Villanueva G., et al. Impact of vaccination on antibiotic usage: a systematic review and meta-analysis. Clin Microbiol Infect. 2019;25:1213–1225. doi: 10.1016/j.cmi.2019.06.030. [DOI] [PubMed] [Google Scholar]
- 72.Sempere J., Llamosí M., López Ruiz B., Del Río I., Pérez-García C., Lago D., et al. Effect of pneumococcal conjugate vaccines and SARS-CoV-2 on antimicrobial resistance and the emergence of streptococcus pneumoniae serotypes with reduced susceptibility in Spain, 2004-20: a national surveillance study. Lancet Microbe. 2022;3:e744–e752. doi: 10.1016/S2666-5247(22)00127-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73.Andrejko K., Ratnasiri B., Hausdorff W.P., Laxminarayan R., Lewnard J.A. Antimicrobial resistance in paediatric Streptococcus pneumoniae isolates amid global implementation of pneumococcal conjugate vaccines: a systematic review and meta-regression analysis. Lancet Microbe. 2021;2:e450–e460. doi: 10.1016/S2666-5247(21)00064-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 74.Valente C., Cruz A.R., Henriques A.O., Sá-Leão R. Intra-species interactions in streptococcus pneumoniae biofilms. Front Cell Infect Microbiol. 2022;11 doi: 10.3389/fcimb.2021.803286. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 75.Nisar M.I., Jehan F., Shahid S., Ahmed S., Shakoor S., Kabir F., et al. Serotype-specific effectiveness against pneumococcal carriage and serotype replacement after ten-valent Pneumococcal Conjugate Vaccine (PCV10) introduction in Pakistan. PLoS One. 2022;17 doi: 10.1371/journal.pone.0262466. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.M.C. Brandileone, S.C. Almeida, S. Bokermann, R. Minamisava, E.N. Berezin, L.H. Harrison, AL. Andrade Dynamics of antimicrobial resistance of streptococcus pneumoniae following PCV10 introduction in Brazil: nationwide surveillance from 2007 to 2019. Vaccine. 2021;39:3207–15. [DOI] [PubMed]
- 77.Almeida S.C., Lo S.W., Hawkins P.A., Gladstone R.A., Cassiolato A.P., Klugman K.P., et al. Genomic surveillance of invasive Streptococcus pneumoniae isolates in the period pre-PCV10 and post-PCV10 introduction in Brazil. Microb Genom. 2021;7 doi: 10.1099/mgen.0.000635. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 78.Huang L., Wasserman M., Grant L., Farkouh R., Snow V., Arguedas A., et al. Burden of pneumococcal disease due to serotypes covered by the 13-valent and new higher-valent pneumococcal conjugate vaccines in the United States. Vaccine. 2022;40:4700–4708. doi: 10.1016/j.vaccine.2022.06.024. [DOI] [PubMed] [Google Scholar]
- 79.Cassiolato A.P., Almeida S.C., Andrade A.L., Minamisava R., Brandileone MC. Expansion of the multidrug-resistant clonal complex 320 among invasive Streptococcus pneumoniae serotype 19A after the introduction of a ten-valent pneumococcal conjugate vaccine in Brazil. PLoS One. 2018;13 doi: 10.1371/journal.pone.0208211. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80.Sgambatti S., Minamisava R., Afonso E.T., Toscano C.M., Bierrenbach A.L., Andrade A.L. Appropriateness of administrative data for vaccine impact evaluation: the case of pneumonia hospitalizations and pneumococcal vaccine in Brazil. Epidemiol Infect. 2015;143:334–342. doi: 10.1017/S0950268814000922. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 81.Nieto Guevara J., Guzman-Holst A. Laboratory-based surveillance in Latin America: attributes and limitations in evaluation of pneumococcal vaccine impact. Hum Vaccin Immunother. 2021;17:4667–4672. doi: 10.1080/21645515.2021.1972709. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.