Abstract
Cervical cerclages are associated with improved live birth rates and have low short- and long-term risks. However, there have been reports of fistula formation or erosion of cerclage into the surrounding tissue. Those complications are uncommon and yet are serious. The risk factors associated with its development are still unclear. The purpose of our study was to evaluate the incidence of fistula formation or erosion following transvaginal cervical cerclage and the associated clinical and sociodemographic factors. We conducted a systematic search of PubMed, Medline, and Embase databases to retrieve articles related to transvaginal or transabdominal cervical cerclage. Databases were searched up to July 2021. The study protocol was registered (PROSPERO ID 243542). A total of 82 articles were identified describing cervical cerclage and erosion or fistula formation. A total of 9 full-text articles were included. There were seven case reports and series that described 11 patients who experienced late complications following cervical cerclage. Many of the cerclage procedures were done electively (66.7%). The most common type of cerclage was McDonald (80%). While all cases reported fistula formation, the main location was vesicovaginal fistulas (63.6%). One patient (9.1%) had erosion of their cerclage and another (9.1%) had bladder calculi. Of 75 patients who underwent cerclage in two retrospective case reviews, the overall incidence of fistula was 1.3% and abscess was also 1.3%. Although rare, the most common long-term complication of cervical cerclage placement is fistula formation, particularly vesicovaginal fistulas.
Keywords: Cervical cerclage, complications, erosion, fistula, vesicovaginal fistula
INTRODUCTION
Preterm birth (PTB) is the delivery of a fetus between 20 and 36 + 6 weeks of gestation, and it is the main cause of neonatal morbidity and mortality.[1] While many of these births are due to preterm labor or preterm prelabor rupture of membranes, in some cases, it can be caused by cervical insufficiency. Cervical cerclage has been performed to treat cervical insufficiency, and subsequently reduces the occurrence of PTB.[2] Cervical cerclages are associated with improved live birth rates and have low short- and long-term risks. However, there have been reports of fistula formation or erosion of cerclage into the surrounding tissue. Those complications are uncommon and yet are serious. The risk factors associated with its development are still unclear.
Given the sparse publications on this topic, our objective was to evaluate the incidence of erosion or fistula formation following the placement of a cervical cerclage and to determine factors associated with this type of complication.
MATERIALS AND METHODS
The study protocol was registered with PROSPERO (ID 243542) and the analysis was reported as per the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guideline.[3] No amendments were required. Using EMBASE, PubMed, Ovid Medline, Google Scholar, and Cochrane Library, studies that were related to transvaginal cervical cerclages and their complications were evaluated using the following terms: “cervical cerclage” OR “cerclage” AND “erosion,” “cerclage” AND “fistula formation,” “transvaginal cerclage” AND “fistula formation,” “fistula” OR “erosion.” To assess risk of bias due to missing results, we did a quick search through Google Scholar and most articles overlapped with other electronic searches or the full-text were inaccessible.
We included articles published in the English language up to December 2021. Once duplicate articles were removed from our list, the abstracts were screened independently by two co-authors (SA and JW) to ensure relevance. In the event of disagreement, a third co-author (TT) acted as an adjudicator. This preliminary step was based on whether the title or abstract could possibly answer four questions applicable to our study. The four questions were related to the incidence of cerclage-related fistula formation, the type of suture material used for cerclage, and clinical and sociodemographic factors. Abdominal cerclage could be done by laparotomy or laparoscopy. In those performed by laparoscopy, we stated as laparoscopic abdominal cerclage.
Data extracted from each selected article included age of the patient, whether the cerclage was placed electively or emergently, gravidity and parity of the patient, whether they had a prior history of cerclage placement, the type of cerclage placed, pre- or postconceptional placement, the gestational age at the time of placement, the gestational age at time of delivery, the route of delivery (vaginal vs. cesarean), and the type of complication (erosion, fistula formation and abscess) and treatment. As all our articles were case reports, series or reviews, a quality assessment was performed using the National Heart, Lung, and Blood Institute Study Quality Assessment Tools.[4]
Statistical analysis
The pooled frequencies and percentages were presented for categorical variables. The pooled mean and standard deviations (SD) or median and interquartile range were calculated for continuous variables when appropriate. Data were analyzed using IBM SPSS Statistics version 27.0 (IBM Corp, Armonk, NY).
RESULTS
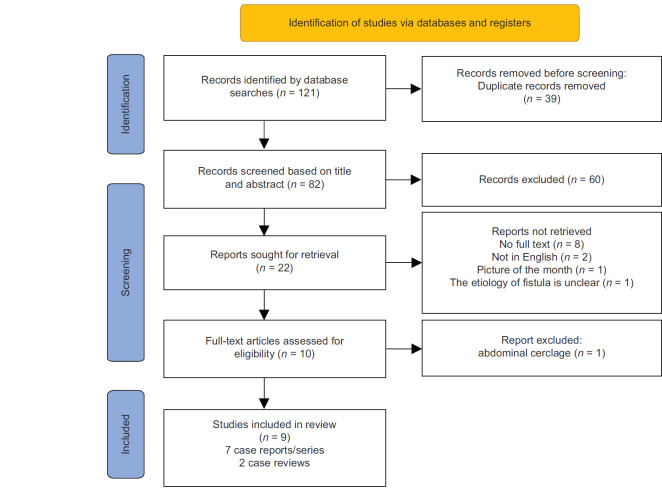
After the removal of duplicates, 82 articles were identified from the database search. We included all case series and case reports that described transvaginal cervical cerclage and erosion or fistula formation. Screening the titles and abstracts narrowed this down to 22 articles. A total of 10 full-text articles were included [Figure 1], including 8 case reports and case series,[5,6,7,8,9,10,11] and 2 case reviews.[2,12] The descriptions of the included case reports and case series are shown in Table 1, while the retrospective case reviews are shown in Table 2. The list of excluded studies is presented in Supplementary Table 1.
Figure 1.
PRISMA 2020 flow diagram
Table 1.
Case reports and case series included in quantitative analysis
| Author | Age (years) |
Gravida | Para | Emergency versus elective | Prior history | Type of cerclage | Type of suture | GA at cerclage (weeks) | GA at delivery (weeks) | Fistula | Interval between cerclage- complication | Treatment | Treatment category |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Berchuck et al. | 26 | 8 | 5 | Emergency | Yes | Shirodkar | NA | 14 | 29 | Cervicovaginal | 0 | Conservative | Conservative |
| Grotegut et al. | 36 | 13 | 2 | Elective | Yes | McDonald | NA | 14 | 22 | Cervicovaginal | NA | Dilatation and evacuation | Surgical |
| Madueke- Laveaux et al. | 51 | 2 | 2 | Elective | No | Shirodkar | Polyethylene terephthalate tape | 16 | 35 | Vesico-cervical bladder calculi | 13 years | Hysteroscopy suture removal, cystolitholapaxy | Surgical |
| Massengill et al. | 32-35 | 1-6 | 1-3 | NA | Yes (3), No (2) |
McDonald | NA | NA | NA | Vesicovaginal | NA | Repair | Surgical |
| McKay et al. | 29 | 3 | 1 | Emergency | NA | McDonald | Silk horizontal mattress sutures | 20 | 33 | Vesicovaginal | 5 months | Transurethral cystorrhaphy repair | Surgical |
| Ng et al. | 30 | 6 | 2 | Elective | No | McDonald | Polyethylene terephthalate tape | 19 | 34 | Ureterovaginal | NA | Percutaneous nephrostomy | Surgical |
| Wall et al. | 38 | 3 | 0 | Elective | Yes | McDonald | Polyethylene terephthalate tape | 12.5 | 37.5 | Vesicovaginal | 12 weeks | Conservative | Conservative |
GA: Gestational age, NA: Not available
Table 2.
The clinical characteristics of patients who underwent cerclage from the case reports/series
| Characteristics | Missing | Descriptions | Value |
|---|---|---|---|
| Age | 0 | Mean (SD) | 35.1 (6.8) |
| Gravida | 0 | Median (IQR) | 3.0 (2.0-6.0) |
| Parity | 0 | Median (IQR) | 2.0 (1.3-2.0) |
| Timing of cerclage | 5 | Elective | 71.4 |
| Prior history | 1 | Presence | 63.6 |
| Type of cerclage | 1 | Shirodkar | 18.2 |
| McDonald | 72.7 | ||
| Location of cerclage | 0 | Vaginal | 66.7 |
| Cervical | 25.0 | ||
| Type of suture | 7 | Polyethylene terephthalate | 40.0 |
| GA when cerclage placed | 6 | Mean (SD) | 15.9 (3.0) |
| GA at delivery | 6 | Mean (SD) | 31.8 (5.5) |
| Route of delivery | 2 | Vaginal | 30.0 |
| C/S | 70.0 | ||
| Complication | 0 | Fistula | 91.7 |
| Erosion | 16.7 | ||
| Bladder calculi | 16.7 | ||
| Abscess | 8.3 | ||
| The most common fistula location | 0 | Vesicovaginal | 72.7 |
| Treatment category | 0 | Surgical | 75.0 |
| Conservative | 16.7 | ||
| None | 8.3 |
GA: Gestational age, SD: Standard deviation, IQR: Interquartile range, C/S: Cesarean section
Supplementary Table 1.
Excluded articles
| Reason of exclusion | Reference |
|---|---|
| Title and/or abstract did not match | Aibinder WR, Schoch B, Schleck C, Sperling JW, Cofield RH. Revisions for aseptic glenoid component loosening after anatomic shoulder arthroplasty. J Shoulder Elbow Surg 2017;26:443-9. |
| Title and/or abstract did not match | Al-Badr A. Trends in the aetiology of urogenital fistula: A case of “retrogressive evolution”? Int Urogynecol J 2016;27:1443. |
| Title and/or abstract did not match | Al-Fifi S, Al-Binali A, Al-Shahrani M, Shafiq H, Bahar M, Almushait M, et al. Congenital anomalies and other perinatal outcomes in ICSI versus naturally conceived pregnancies: A comparative study. J Assist Reprod Genet 2009;26:377-81. |
| Title and/or abstract did not match | Amorese V, Corda M, Donadu M, Usai D, Pisanu F, Milia F, et al. Total hip prosthesis complication, periprosthetic infection with external fistulizing due to Enterobacter cloacae complex multiple drugs resistance: A clinical case report. Int J Surg Case Rep 2017;36:90-3. |
| Title and/or abstract did not match | Andaloro A, Santolini F. Septic pseudoarthrosis of femoral shaft after total hip prosthesis. A case report. Minerva Ortop Traumatol 1996;47:585-8. |
| Title and/or abstract did not match | Armstrong KL, Modest AM, Rosenblatt PL. Laparoscopic cerclage sacrohysteropexy: Comparing a novel technique for sacrohysteropexy to traditional supracervical hysterectomy and sacrocervicopexy. Female Pelvic Med Reconstr Surg 2021;27:e315-20. |
| Title and/or abstract did not match | Armstrong K, Rosenblatt PL, Modest AM. Comparing laparoscopic cerclage sacrohysteropexy to traditional laparoscopic supracervical hysterectomy and sacrocervicopexy: One year outcomes. Female Pelvic Med Reconstr Surg 2019;25 5 Suppl 1:S81. |
| Title and/or abstract did not match | Reinthal EK, Kirchhof B, Bartz-Schmidt KU. Preparation and after-care in vitreoretinal interventions. Klin Monbl Augenheilkd 2006;223:R1-14. |
| No access to full text | Ben-Baruch G, Rabinovitch O, Madjar I, Dor J, Mashiach S. Ureterovaginal fistula - A rare complication of cervical cerclage. Isr J Med Sci 1980;16:400-1. |
| Title and/or abstract did not match | Bentivegna E, Maulard A, Pautier P, Chargari C, Gouy S, Morice P. Fertility results and pregnancy outcomes after conservative treatment of cervical cancer: A systematic review of the literature. Fertil Steril 2016;106:1195-211.e5. |
| Not in English | Besio M, Fica A, Duque G. Transabdominal cerclage in the treatment of cervical incompetence. Rev Chil Obstet Ginecol 1991;56:415-8. |
| Title and/or abstract did not match | Breucking E, Mortier W, Lampert R, Brandt L. Anesthesia and intensive therapy for a patient with mitochondrial myopathy. Anaesthesist 1993;42:719-23. |
| Title and/or abstract did not match | Capello WN, Sallay PI, Feinberg JR. Omniflex modular femoral component. Two- to five-year results. Clin Orthop Relat Res 1994;(298):54-9. |
| Title and/or abstract did not match | Cheung KW, Seto MTY, Wang W, Lai CWS, Kilby MD, Ng EHY. Effect of delayed interval delivery of remaining fetus (es) in multiple pregnancies on survival: A systematic review and meta-analysis. Am J Obstet Gynecol 2020;222:306-19.e18. |
| Title and/or abstract did not match | Chon AH, Pham HQ, Chmait RH. Twin-twin transfusion syndrome complicated by proximate placental cord insertion sites: Endoscopic clip-assisted laser occlusion. Fetal Diagn Ther 2020;47:779-84. |
| Picture of the month | Cordoba Munoz MI, Acevedo-Alvarez M, Monteagudo A, Antoine C, Smilen S, Timor-Tritsch I. Three-dimensional sonographic virtual cystoscopy for diagnosis of cervical cerclage erosion into the bladder. Ultrasound Obstet Gynecol 2013;42:487-9. |
| Title and/or abstract did not match | Edwards TB, Stuart KD, Trappey GJ, O’Connor DP, Sarin VK. Utility of polymer cerclage cables in revision shoulder arthroplasty. Orthopedics 2011;34. [doi: 10.3928/01477447-20110228-13]. |
| Title and/or abstract did not match | Einarsson JI. Laparoscopic cerclage placement following a radical trachelectomy. Gynecological Surgery 2012;9 1 Suppl 1:S116. |
| Title and/or abstract did not match | Fleming ND, Ramirez PT, Soliman PT, Schmeler KM, Chisholm GB, Nick AM, et al. Quality of life after radical trachelectomy for early-stage cervical cancer: A 5-year prospective evaluation. Gynecol Oncol 2016;143:596-603. |
| Title and/or abstract did not match | Gellhaus PT, Bhandari A, Monn MF, Gardner TA, Kanagarajah P, Reilly CE, et al. Robotic management of genitourinary injuries from obstetric and gynaecological operations: A multi-institutional report of outcomes. BJU Int 2015;115:430-6. |
| No access to full text | Golomb J, Ben-Chaim J, Goldwasser B, Korach J, Mashiach S. Conservative treatment of a vesicocervical fistula resulting from Shirodkar cervical cerclage. J Urol 1993;149:833-4. |
| No access to full text | Goodacre TE. Complication of cervical cerclage. Trop Doct 1987;17:127-8. |
| Title and/or abstract did not match | Grewal M, Pakzad MH, Hamid R, Ockrim JL, Greenwell TJ. The medium- to long-term functional outcomes of women who have had successful anatomical closure of vesicovaginal fistulae. Urol Ann 2019;11:247-51. |
| Title and/or abstract did not match | Hawkins E, Nimaroff M. Vaginal erosion of an abdominal cerclage 7 years after laparoscopic placement. Obstet Gynecol 2014;123:420-3. |
| No access to full text | Hines MR, Vakili B. Abdominal cerclage erosion into the bladder: Case report and description of surgical revision. Am J Obstet Gynecol 2017;216 3 Suppl 1:S624-5. |
| No access to full text | Hortenstine JS, Witherington R. Ulcer of the trigone: A late complication of cervical cerclage. J Urol 1987;137:109-10. |
| Title and/or abstract did not match | Hunter TJ, Abdus-Samee M, Balasubramanian S, Grocott N, McClelland D. Medium- to long-term results of acromioclavicular joint stabilisation using the Ligament Augmentation Reconstruction System (LARS) ligament. Shoulder Elbow 2020;12:163-9. |
| Title and/or abstract did not match | Iloabachie GC, Onah HE. Cervico-vaginal fistula from induced abortions causing subsequent spontaneous midtrimester abortions in Nigerians: Case report. Niger Postgrad Med J 2002;9:99-101. |
| Title and/or abstract did not match | Capmas P, Letendre I, Leray C, Deffieux X, Duminil L, Subtil D, et al. Vaginal cervico-isthmic cerclage versus McDonald cerclage in women with a previous failure of prophylactic cerclage: A retrospective study. Eur J Obstet Gynecol Reprod Biol 2017;216:27-32. |
| Title and/or abstract did not match | Johansen G, Lönnerfors C, Falconer H, Persson J. Reproductive and oncologic outcome following robot-assisted laparoscopic radical trachelectomy for early stage cervical cancer. Gynecol Oncol 2016;141:160-5. |
| Title and/or abstract did not match | Jones DG. Bone erosion beneath partridge bands. J Bone Joint Surg Br 1986;68:476-7. |
| No access to full text | Joyce JS, Chung CP, Yandell PM. Bladder erosion related to shirodkar cerclage placement: A case report. J Reprod Med 2017;62:675-7. |
| Title and/or abstract did not match | Kaldawy A, Ostrovsky L, Segev Y, Lavie O. Laparoscopic cerclage during radical trachelectomy - A novel technique: A case report and review of the literature.” J Gynecol Surg 2020;36:136-40. |
| Title and/or abstract did not match | Karaman Y, Bingol B, Gunenc Z. Laparoscopic transabdominal isthmic cerclage in a case of cervical agenesis and a successful pregnancy with ICSI. Gynecol Surg 2007;4:45-8. |
| Title and/or abstract did not match | Katz M, et al. Utility of routine cystoscopy during transvaginal cervico-isthmic cerclage. Female Pelvic Med Reconstr Surg 2015;21 5 Suppl 1:S130. |
| Title and/or abstract did not match | Wall LL, Khan F, Adams S. Vesicovaginal fistula formation after cervical cerclage mimicking premature rupture of membranes. Obstet Gynecol 2007;109:493-4. |
| Title and/or abstract did not match | Kim CH, Abu-Rustum NR, Chi DS, Gardner GJ, Leitao MM Jr., Carter J, et al. Reproductive outcomes of patients undergoing radical trachelectomy for early-stage cervical cancer. Gynecol Oncol 2012;125:585-8. |
| Title and/or abstract did not match | Kim JH, Chon MK, Lee S, Lee SY, Je HG. Choo KS. Mitral loop cerclage (MLC) as a variant form of ‘miral cerclage annuloplasty’ by adding an appliance (CSTV) for preventing its potential complications: A preclinical study with mature devices. J Am Coll Cardiol 2015;65 17 SUPPL 1:S62. |
| Title and/or abstract did not match | Kirchhoff C, et al. Periprosthetic humeral fractures: Strategies and techniques of revision arthroplasty. Unfallchirurg 2016;119:281-7. |
| Title and/or abstract did not match | Krwawicz T. Preventing scleral erosion after Arruga’s cerclage. Adv Ophthalmol 1978;36:180-6. |
| Title and/or abstract did not match | Krwawicz T. Prevention of scleral erosion following cerclage operation according to Arruga (preliminary communication). Klin Oczna 1978;48:397-8. |
| Title and/or abstract did not match | Leach M, Mohamed H, Sheuiebar H, Pickersgill A. A case of a missed cerclage, an unusual cause of postmenopausal bleeding. BJOG Int J Obstet Gynaecol 2013;120 Suppl 3:4. |
| Title and/or abstract did not match | Lee YK, Joung HY, Kim SH, Ha YC, Koo KH. Cementless bipolar hemiarthroplasty using a micro-arc oxidation coated stem in patients with displaced femoral neck fractures. J Arthroplasty 2014;29:2388-92. |
| Title and/or abstract did not match | Lincoff H, Ramirez V, Kreissig I, Baronberg N, Kaufman D. Encircling operations without drainage of subretinal fluid. Mod Probl Ophthalmol 1975;15:188-96. |
| Title and/or abstract did not match | Lincoff H, Kreissig I, Parver L. Limits of constriction in the treatment of retinal detachment. Arch Ophthalmol 1976;94:1473-7. |
| Title and/or abstract did not match | Machado I, Barini R, Nomura ML, DeCarvalho ECC. Pre-pregnancy transvaginal treatment of incompetent cervix. Int J Gynecol Obstet 2018;143 Suppl 3:275-6. |
| No access to full text | Malmström H, Axelsson O. Results of cervical cerclage operations in pregnant women during a five-year period. Ann Chir Gynaecol 1981;70:75-8. |
| Title and/or abstract did not match | Martínez-Chapa A, Alonso-Reyes N, Luna-Macías M. Reprodcutive results of radical trachelectomy. Ginecol Obstet Mex 2015;83:770-5. |
| Title and/or abstract did not match | Miller JB. Cervicovaginal fistulas: Management of subsequent pregnancy. South Med J 1985;78:1358-60. |
| Title and/or abstract did not match | Nanni GS, Degli-Antoni, Camacho D, Wall T. Diagnosis of iatrogenic injury of the endometrium using duplex sonography. J Diagn Med Sonography 2016;32:168-72. |
| Title and/or abstract did not match | Nick AM, Frumovitz MM, Soliman PT, Schmeler KM, Ramirez PT. Fertility sparing surgery for treatment of early-stage cervical cancer: Open versus robotic radical trachelectomy. Gynecol Oncol 2012;124:276-80. |
| Title and/or abstract did not match | Orhan A, Kasapoglu I, Atalay A, Kosan B, Mert SN, Ozerkan K. A simple new method for laparoscopic sacrocervicopexy. J Turk German Gynecol Assoc 2017;18: S14-5. |
| Title and/or abstract did not match | Merolla G, Wagner E, Sperling JW, Paladini P, Fabbri E, Porcellini G. Revision of failed shoulder hemiarthroplasty to reverse total arthroplasty: Analysis of 157 revision implants. J Shoulder Elbow Surg 2018;27:75-81. |
| Title and/or abstract did not match | Pantazis K, Mikos T, Tzevelekis F, Theodoridis T, Tarlatzis B, Papameleteiou V. A case of an anti-incontinence surgery complication delayed by 12 years. Int Urogynecol J Pelvic Floor Dysfunct 2011;22 Suppl 3:S1990-1. |
| Title and/or abstract did not match | Pareja R, Rendon GJ, Angel GA, Echeverri LM, Ramirez PT. Retrospective analysis of 10 consecutive cases of laparoscopic radical trachelectomy in early cervical cancer. First American experience. J Minim Invasive Gynecol 2013;20 6 Suppl 1:S119. |
| Title and/or abstract did not match | Pareja R, Rendón GJ, Sanz-Lomana CM, Monzón O, Ramirez PT. Surgical, oncological, and obstetrical outcomes after abdominal radical trachelectomy - A systematic literature review. Gynecol Oncol 2013;131:77-82. |
| No access to full text | Popov A, Fedorov A, Manannikova T, Vrockaya V, Krasnopolskaya K, Barto R. Reproductive outcomes of cervical cerclage-6 year follow up. Gynecol Surg 2016;13 1 Suppl 1:S287. |
| Title and/or abstract did not match | Rebarber A, Sfakianaki A, Monteagudo A. Imaging of a cervicovaginal fistula using transvaginal saline contrast sonohysterography. Ultrasound Obstet Gynecol 2001;18:292-3. |
| Title and/or abstract did not match | Richter R, Bilek K. Differential diagnosis of varicose hemorrhage in pregnancy. Zentralbl Gynakol 1983;105:931-3. |
| Title and/or abstract did not match | Rizk A, Hamed M. The use of cerclage wire for surgical repair of unilateral rostral mandibular fracture in horses. Iran J Vet Res 2018;19:123-7. |
| Title and/or abstract did not match | Roed-Petersen B, Roed-Petersen J, Jørgensen KD. Nickel allergy and osteomyelitis in a patient with metal osteosynthesis of a jaw fracture. Contact Dermatitis 1979;5:108-12. |
| Title and/or abstract did not match | Rogers RG. Things sometimes happen. Obstet Gynecol 2007;109:481-2. |
| Not in English | Seban J. Fistula due to cerclage as a cause of recurrent vulvovaginal candidiasis. Cesk Gynekol 1988;53:586-8. |
| The etiology of fistula is unclear | Sifakis S, Kaminopetros P, Kappou D, Dimitriadis T. Successful term pregnancy in a patient with cervicovaginal fistula managed with transabdominal laparoscopic cervical cerclage. J Obstet Gynaecol 2012;32:700-1. |
| Title and/or abstract did not match | Takai N, Eto M, Sato F, Mimata H, Miyakawa I. Placenta percreta invading the urinary bladder. Arch Gynecol Obstet 2005;271:274-5. |
| Title and/or abstract did not match | Thayalan K, Parghi S, Krause H, Goh J. Vesicovaginal fistula following pelvic surgery: Our experiences and recommendations for diagnosis and prompt referral. Aust N Z J Obstet Gynaecol 2020;60:449-53. |
| Title and/or abstract did not match | Trovik J, Thornhill HF, Kiserud T. Incidence of obstetric fistula in Norway: A population-based prospective cohort study. Acta Obstet Gynecol Scand 2016;95:405-10. |
| Title and/or abstract did not match | Tsukahara I. Erosion of the sclera by cerclage equatorial (Arruga). Nihon Ganka Kiyo 1967;18:706-8. |
| Title and/or abstract did not match | Vieira MA, Rendón GJ, Munsell M, Echeverri L, Frumovitz M, Schmeler KM, et al. Radical trachelectomy in early-stage cervical cancer: A comparison of laparotomy and minimally invasive surgery. Gynecol Oncol 2015;138:585-9. |
| Title and/or abstract did not match | Witschel H, Faulborn J. Reaction of ocular tissues to scleral-implant and encircling material: Polyamide - Silicone - Polyester (author’s transl). Albrecht Von Graefes Arch Klin Exp Ophthalmol 1978;206:217-26. |
| Title and/or abstract did not match | Yao XX, Zhang D, Ji DG, Yang YS, Xie YJ, Ye YS, et al. Comparison of curative effects between two types of extensive devascularization around cardia in treatment of upper gastrointestinal hemorrhage of portal hypertension. J Jilin Univ Med Ed 2012;38:1008-12. |
| Title and/or abstract did not match | Zanconato G, Bergamini V, Baggio S, Cavaliere E, Franchi M. Successful pregnancy outcome after laparoscopic cerclage in a patient with cervicovaginal fistula. Case Rep Obstet Gynecol 2015;2015:784025. |
The case reports described 12 patients who experienced complications following cervical cerclage. In summary, the mean age of the patients was 34.3 SD 6.5 years [Table 3]. Most of the cerclages were placed in pregnancy and electively (66.7%). The most common type of cerclage was McDonald (80.0%). Fistula formation was reported in all cases with the most location was vesicovaginal fistulas (63.6%). In most cases the interval between the placement of the cerclage and the complication was not mentioned. However, Wall et al.[7] reported 12-week interval between cerclage placement and the development of a vesicovaginal fistula. Madueke-Laveaux et al.[8] reported erosion and fistula formation 13 years after placement of the cervical cerclage. Evaluating different types of suture material used, most articles did not state the type of sutures. However, it was conventionally performed with polyethylene terephthalate tape (Mersilene, New Brunswick, NJ).[7,8]
Table 3.
Case reviews included in quantitative analysis
| Author | n | Age | Parity | Emergency versus elective | Type of cerclage | Type of suture | GA when cerclage placed | GA at delivery | Route of delivery | Complication | Treatment | Treatment category |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Deffieux (2006)a | 24 | 32.1 (22-39) |
1.9 (1.6) | Elective | Cervico- isthmic | Polyethylene terephthalate | 12-16 weeks | Mean 37.1 (1.8) weeks | Caesarean 100% | Pelvic abscess (1/24=4.2%) |
Strip was removed and abscess was evacuated | Conservative |
| Wong (1993)b | 51 | No data | Multigravida (n=41) |
Emergency | Shirodkar (n=26) McDonald (n=25) |
Assumed polyethylene terephthalate | Mean 24.1 weeks | Mean 29.1 weeks | Vaginal (n=41) Caesarean (n=10) |
Cervicovaginal fistula (1/51=2.0%) |
No data | No data |
| Total | 75 | Vaginal 54.7% Caesarean 45.3% |
Abscess 1.3% Fistula 1.3% |
aPrior history: Pregnancy losses in 2nd trimester, failure of McDonald (n=16), absent portio vaginalis of cervix (n=4), premature delivery due to incompetence cervix (n=4), bPrior history: Premature babies (n=15), spontaneous abortions (n=30), terminations of pregnancy (n=28), ectopic pregnancies (n=3), cone biopsy (n=7). GA: Gestational age
In the retrospective case review [Table 2], Deffieux et al.[2] described 24 cases of elective cervico-isthmic cerclages. Only 1 of 24 (4.2%) had an abscess 6 months after delivery or 47.1 weeks after cerclage placement. Wong et al.[12] reviewed 51 cases of emergency placement of Shirodkar or McDonald cerclages. One patient developed cervicovaginal fistula formation (2%). There was no report of erosion or abscess formation. The interval between cerclage placement and complication was not mentioned. Among 75 patients underwent vaginal cerclage in both case reviews, the overall incidence of fistula was 1.3% and abscess formation was also 1.3%.
Quality of the studies
Using NIH quality evaluation tool, we found that all included ten case reports and series were of good quality [Table 4a]. Overall, both case reviews also had good quality [Table 4b].
Table 4a.
Quality assessment of case reports and case series using the National Institutes of Health tool
| Study | 1. Was the study question or objective clearly stated? | 2. Was the study population clearly and fully described, including a case definition? | 3. Were the cases consecutive? | 4. Were the subjects comparable? | 5. Was the intervention clearly described? | 6. Were the outcome measures clearly defined, valid, reliable, and implemented consistently across all study participants? | 7. Was the length of follow-up adequate? | 8. Were the statistical methods well- described? | 9. Were the results well described? | Overall: Poor, fair or good |
|---|---|---|---|---|---|---|---|---|---|---|
| Berchuck et al. | Yes | Yes | NA | NA | Yes | Yes | Yes | NA | Yes | Good |
| Grotegut et al. | Yes | Yes | NA | NA | Yes | Yes | Yes | NA | Yes | Good |
| Madueke- Laveaux et al. | Yes | Yes | NA | NA | Yes | Yes | Yes | NA | Yes | Good |
| Massengill et al. | Yes | Yes | Yes | Yes | Yes | Yes | NA | Yes | Yes | Good |
| McKay et al. | Yes | Yes | NA | NA | Yes | Yes | Yes | NA | Yes | Good |
| Ng et al. | Yes | Yes | NA | NA | Yes | Yes | Yes | NA | Yes | Good |
| Wall et al. | Yes | Yes | NA | NA | Yes | Yes | Yes | NA | Yes | Good |
NA: Not available
Table 4b.
Quality assessment of case reviews using National Institutes of Health tool
| Criteria | Deffieux | Wang |
|---|---|---|
| 1. Was the research question or objective in this paper clearly stated? | Yes | Yes |
| 2. Was the study population clearly specified and defined? | Yes (women with high risk of premature labor) | Yes (there is a table with the history of all patients) |
| 3. Was the participation rate of eligible persons at least 50%? | Yes | Yes |
| 4. Were all the subjects selected or recruited from the same or similar populations (including the same time period)? Were inclusion and exclusion criteria for being in the study prespecified and applied uniformly to all participants? | Yes (cerclage performed between week 12 and 16, between 2002 and 2005) | Yes (many of them had similar histories; study was between 1987 and 1990; the subjects were recruited from 22,000 people and had the meet inclusion criteria) |
| 5. Was a sample size justification, power description, or variance and effect estimates provided? | No | Yes |
| 6. For the analyses in this paper, were the exposure(s) of interest measured prior to the outcome(s) being measured? | Yes (cervico-isthmique cerclage performed in all patients) | Yes (patients either underwent MacDonald or Shirodkar cerclage) |
| 7. Was the timeframe sufficient so that one could reasonably expect to see an association between exposure and outcome if it existed? | No (although most patients gave birth, 3 were still pregnant) | Yes |
| 8. For exposures that can vary in amount or level, did the study examine different levels of the exposure as related to the outcome (e.g., categories of exposure, or exposure measured as continuous variable)? | Not applicable (everyone was exposed to cervico-isthmic cerclage) | Yes (patients underwent different types of cerclages: MacDonald or Shirodkar) |
| 9. Were the exposure measures (independent variables) clearly defined, valid, reliable, and implemented consistently across all study participants? | Yes (everyone was exposed to cervico-isthmic cerclage) | Yes (all patients either underwent MacDonald or Shirodkar cerclage) |
| 10. Was the exposure(s) assessed more than once over time? | Not applicable (all patients underwent cerclage once during the study) | Not applicable (all patients underwent cerclage once during the study) |
| 11. Were the outcome measures (dependent variables) clearly defined, valid, reliable, and implemented consistently across all study participants? | Yes (i.e., preterm birth rate, gestational age, etc., were evaluated for all) | Yes (outcome measures presented in tables [Table 2, 3, 4]) |
| 12. Were the outcome assessors blinded to the exposure status of participants? | No | No |
| 13. Was loss to follow-up after baseline 20% or less? | Yes (followed up all the patients they had) | Yes (followed up with all the patients in their study) |
| 14. Were key potential confounding variables measured and adjusted statistically for their impact on the relationship between exposure(s) and outcome(s)? | Not applicable (everyone underwent elective cervical cerclage with the same type of suture) | Not applicable (everyone underwent emergency cervical cerclage with the same type of suture) |
DISCUSSION
Complications related to cerclage placement are rare.[13] In one study, the incidence of fistula formation after cervical cerclage is <2%. Although the implications of transvaginal cervical cerclage are slightly different from that of abdominal cerclage, in a report of 16 studies of abdominal cerclage involving 678 cases, the authors did not encounter any vaginal erosion or fistulas.[7] We estimated that the actual incidence of erosion or fistula formation is 1/1000 cases of cervical cerclages.
Fistula formation was found mainly in multi-gravid women with a history of more than one cerclage placement. A McDonald's cerclage appears to be more likely to be associated with long-term complication than Shirodkar or abdominal cerclage. However, this could be due to the more frequent use of McDonald approaches. The latter is technically simpler than Shirodkar cerclage that needs bladder dissection off the cervix. Although not stated, most clinicians use polyethylene terephthalate tape (Mersilene).[13] Deffieux et al. reported having to remove the tape in a patient owing to vaginal erosion.[2]
In our study, we found that complication can occur as early as 12 weeks after transvaginal cerclage placement and could be up to 13 years. Ruan et al. reported bladder calculus around the cerclage 10 years after transvaginal cerclage suggesting the cerclage had eroded into the bladder.[14] Similarly, Tulandi et al. reported complete erosion of abdominal cerclage into the bladder with the formation of bladder calculi 5 years after laparoscopic abdominal cerclage.[15] Hawkins and Nimaroff reported vaginal erosion 7 years after laparoscopic abdominal cerclage.[16]
The main limitation of our study was the rare occurrence of long-term complications of cervical cerclage. There is no prospective cohort evaluating the occurrence of complications of cervical cerclage. However, to the best of our knowledge, this was the first systematic review evaluating long-term complications of cervical cerclage. The extraordinarily low incidence of late complications of cervical cerclage provides a reassurance to the patients requiring cervical cerclage.
CONCLUSIONS
Patients that may require multiple cerclages should be counseled that although the risk of developing a complication in the future may be rare, there is a possibility it may occur and, in that instance, surgical management is the most likely method of treatment. More data needs to be published to have a better understanding of specific risk factors that influence the development of a complication in this group of women such as the type of suture used.
Financial support and sponsorship
Nil.
Conflicts of interest
Prof. Togas Tulandi, an editorial board member at Gynecology and Minimally Invasive Therapy, had no role in the peer review process of or decision to publish this article. The other authors declared no conflicts of interest in writing this paper.
REFERENCES
- 1.Abubakar II, Tillmann T, Banerjee A. Global, regional, and national age-sex specific all-cause and cause-specific mortality for 240 causes of death, 1990-2013: A systematic analysis for the Global Burden of Disease study 2013. Lancet. 2015;385:117–71. doi: 10.1016/S0140-6736(14)61682-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Deffieux X, de Tayrac R, Louafi N, Gervaise A, Sénat MV, Chauveaud-Lambling A, et al. Transvaginal cervico-isthmic cerclage using polypropylene tape: Surgical procedure and pregnancy outcome: Fernandez's procedure. J Gynecol Obstet Biol Reprod (Paris) 2006;35:465–71. doi: 10.1016/s0368-2315(06)76418-3. [DOI] [PubMed] [Google Scholar]
- 3.Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. Ann Intern Med. 2009;151 doi: 10.7326/0003-4819-151-4-200908180-00135. 264-9, W64. [DOI] [PubMed] [Google Scholar]
- 4.Quality Assessment Tool for Case Series Studies. [Last accessed on 2021 Nov 12]. Available from: https://www.nhlbi.nih.gov/health-topics/study-quality-assessment-tools .
- 5.Berchuck A, Sokol RJ. Cervicovaginal fistula formation: A new complication of Shirodkar cerclage. Am J Perinatol. 1984;1:263–5. doi: 10.1055/s-2007-1000016. [DOI] [PubMed] [Google Scholar]
- 6.Grotegut CA, Moore NL, Reddick KL, Canzoneri BJ, Boyd BK, Brown HL. Cervicovaginal fistula presenting during miscarriage. Ultrasound Obstet Gynecol. 2010;36:112–4. doi: 10.1002/uog.7581. [DOI] [PubMed] [Google Scholar]
- 7.Wall LL, Khan F, Adams S. Vesicovaginal fistula formation after cervical cerclage mimicking premature rupture of membranes. Obstet Gynecol. 2007;109:493–4. doi: 10.1097/01.AOG.0000247291.00155.88. [DOI] [PubMed] [Google Scholar]
- 8.Madueke-Laveaux OS, Platte R, Poplawsky D. Unique complication of a Shirodkar cerclage: Remote formation of a vesicocervical fistula in a patient with the history of cervical cerclage placement: A case report and literature review. Female Pelvic Med Reconstr Surg. 2013;19:306–8. doi: 10.1097/SPV.0b013e3182996cee. [DOI] [PubMed] [Google Scholar]
- 9.Massengill JC, Baker TM, Von Pechmann WS, Horbach NS, Hurtado EA. Commonalities of cerclage-related genitourinary fistulas. Female Pelvic Med Reconstr Surg. 2012;18:362–5. doi: 10.1097/SPV.0b013e318270aa7c. [DOI] [PubMed] [Google Scholar]
- 10.McKay HA, Hanlon K. Vesicovaginal fistula after cervical cerclage: Repair by transurethral suture cystorrhaphy. J Urol. 2003;169:1086–7. doi: 10.1097/01.ju.0000047516.32699.aa. [DOI] [PubMed] [Google Scholar]
- 11.Ng KL, Kale AS, Gosavi AT. Ureterovaginal fistula after insertion of a McDonald suture: Case report and review of published reports. J Obstet Gynaecol Res. 2015;41:1129–32. doi: 10.1111/jog.12671. [DOI] [PubMed] [Google Scholar]
- 12.Wong GP, Farquharson DF, Dansereau J. Emergency cervical cerclage: A retrospective review of 51 cases. Am J Perinatol. 1993;10:341–7. doi: 10.1055/s-2007-994757. [DOI] [PubMed] [Google Scholar]
- 13.Tulandi T, Alghanaim N, Hakeem G, Tan X. Pre and post-conceptional abdominal cerclage by laparoscopy or laparotomy. J Minim Invasive Gynecol. 2014;21:987–93. doi: 10.1016/j.jmig.2014.05.015. [DOI] [PubMed] [Google Scholar]
- 14.Ruan JM, Adams SR, Carpinito G, Ferzandi TR. Bladder calculus presenting as recurrent urinary tract infections: A late complication of cervical cerclage placement: A case report. J Reprod Med. 2011;56:172–4. [PubMed] [Google Scholar]
- 15.Tulandi T, Eiley D, Abenhaim H, Ziegler C. Complete Erosion of abdominal cerclage into the bladder. J Obstet Gynaecol Can. 2021;43:1083–5. doi: 10.1016/j.jogc.2021.03.017. [DOI] [PubMed] [Google Scholar]
- 16.Hawkins E, Nimaroff M. Vaginal erosion of an abdominal cerclage 7 years after laparoscopic placement. Obstet Gynecol. 2014;123:420–3. doi: 10.1097/AOG.0b013e3182a7114a. [DOI] [PubMed] [Google Scholar]