Abstract
The COVID-19 pandemic has had a massive and unprecedented impact on the mental health of individuals worldwide. Quarantine hotel employees not only endured enormous upheavals when providing service to quarantine guests during obligatory quarantine periods, but also experienced the high mental stress that comes with the risk of exposure and contagion of themselves, their friends, and their families. This study investigated the impact of the fear of COVID-19 on mental health problems. The moderating roles of self-compassion and psychological resilience were also examined. Data was collected from 360 employees from thirteen “Alternative State Quarantine” hotels in Thailand. The results suggested that fear of COVID-19 positively influenced mental health problems. Self-compassion and psychological resilience at work buffered the detrimental impact of fear of COVID-19 on mental health. This three-way interaction demonstrated that employees with high self-compassion and high resilience coped better. The theoretical and practical implications for hospitality managers are discussed.
Keywords: Fear of COVID-19, Mental health, Self-compassion, Psychological resilience, Quarantine hotels
1. Introduction
COVID-19 and its ramifications sparked fears, worries, and anxieties across the globe. After months of strict travel restrictions, Thailand geared up for a return to normalcy by easing some travel restrictions. To mitigate the spread of COVID-19 from overseas, the Thai government imposed stringent protection measures, including a mandatory 14-day quarantine at designated quarantine hotels (Department of Foreign Affairs, 2021). In many countries, hotels have been commandeered by governments to serve as isolation or quarantine accommodations (Teng et al., 2021). These temporarily adjusted hotels are called “quarantine hotels.” Additionally, many individuals require isolation from immediate family members due to the strict quarantine measures implemented globally. Quarantine hotels have proven to be a viable solution for addressing the need for temporary quarantine accommodation. However, hosting quarantine guests can impact the physical and mental well-being of quarantine hotel frontline employees, as they face a higher risk of infection.
Due to the COVID-19 outbreak, the stress and anxiety of hospitality employees, already recognized to be greater compared to other industries due to the long anti-social working hours and frequent interaction with clients (Haldorai et al., 2019), may be further exacerbated. Similar to health care employees, frontline employees of quarantine hotels are in direct contact with quarantine guests, thus increasing their exposure to respiratory droplets. These employees not only experience an increased workload due to new operating procedures and sanitation protocols in quarantine hotels, but also mental health issues such as depression, anxiety, and stress. High stress and anxiety can be detrimental to mental health if experienced for a long period of time. Thus, fear of COVID-19 is amplified among frontline employees in the hospitality industry (Chen and Eyoun, 2021), particularly those employed in quarantine hotels. This observation is supported by the research of Lin et el. (2020), which reported on the fear of contacting people who may be infected by COVID-19. Additionally, during the pandemic outbreak, individuals suffered from “infobesity,” or an overload of information. Due to the widespread media coverage of the pandemic outbreak and the known lethality of the infection, individuals became overly concerned about the virus’ consequences, affecting their mental health (Hamouche, 2020) and leading to reduced quality of life, psychological distress, depression, and anxiety. Past research and recent studies suggested that epidemics and pandemics caused by infectious diseases can be extremely distressing events for some people, even resulting in post-traumatic stress disorder and chronic psychological distress (Boyraz and Legros, 2020). A person’s mental health plays an important role in their well-being and is absolutely vital for leading a productive and satisfying life. In the workplace, mental health problems are associated with a wide range of detrimental consequences, such as low efficiency, drops in productivity, and increased absenteeism (Karatepe et al., 2021). In several conceptual works, COVID-19 has been implicated in aggravating mental health problems among hospitality employees, such as agitation, anxiety disorders, depression, insomnia, and anger (Sönmez et al., 2020), and accordingly Sigala (2020) has called for further empirical investigation on whether hospitality employees suffer from mental health problems due to fear of COVID-19 as a focal stressor. Hence, the primary purpose of this research is to conduct an empirical investigation into whether or not the fear of COVID-19 influences the mental health of quarantine hotel employees.
Given the adverse impacts of mental health problems on workplace outcomes, it is of great importance to investigate those factors that can buffer the effect of the fear of COVID-19 on mental health problems, since employee reactions to the psychological distress caused by traumatizing experiences, such as the COVID-19 pandemic, may differ. Mainstream research has documented that employees’ personal resources, such as psychological resilience (Hu et al., 2015) and self-compassion (Kyeong, 2013), can help combat stress and anxiety. Psychological resilience is the ability to adapt to difficult or problematic situations in life and the ability to thrive in times of fear and precariousness (Fletcher and Sarkar, 2013). Individuals with high resilience recover more quickly from trauma than individuals with low resilience (Schaubroeck et al., 2011). However, there exists a wide gap in the literature on the buffering role of psychological resilience during the pandemic period (Bozdağ & Ergün, 2020). Hence, the present study investigated the moderating role of psychological resilience in the positive relationship between fear of COVID-19 and mental health problems. Furthermore, a trend to integrate Buddhist concepts such as “mindfulness” with Western psychological approaches has led to a growing interest in the construct of self-compassion. Despite its long history in religion, medicine, and sociology, the study of compassion in organizations is relatively new (Lilius et al., 2008). Self-compassion is defined as “a warm, kind and non-judgmental attitude to oneself during setbacks” (Neff, 2003, p. 224) and has shown a positive association with well-being and mental health (MacBeth and Gumley, 2012). In addition to enabling emotional regulation, self-compassion has the ability to buffer adverse mental health outcomes due to stressful experiences, maladaptive beliefs, and negative self-related cognitions (Lau et al., 2020). Hence, we expect self-compassion to buffer the positive link between fear of COVID-19 and mental health problems among quarantine hotel employees. Taken together, the study aims to investigate the impact of the fear of COVID-19 on the mental health of quarantine hotel employees. The study further investigates the moderating roles of psychological resilience and self-compassion at work at the individual level as personal qualities that help individuals to thrive in the face of adversity.
2. Literature review and hypotheses development
2.1. Conservation of resources (COR) theory
COR theory can provide insight into how frontline employees experience mental health issues like emotional exhaustion and depression due to their fear of COVID-19. COR theory has often been adopted in studies examining the impact of stress during crisis situations and has been referenced as a framework for understanding stress in various investigations (Chen and Eyoun, 2021, Karatepe et al., 2021). COR theory proposes that individuals strive to acquire, maintain, and safeguard resources that they consider valuable. These resources can be lost or threatened by stressful events, and individuals try to minimize any threat of resource loss (Hobfoll, 1989). The theory further asserts that individuals are motivated to preserve their resources, and that the loss or threatened loss of resources can lead to stress reactions, such as anxiety, depression, and even physical illness. According to COR theory, individuals will try to cope with stress in ways that help them preserve their resources, such as seeking social support, engaging in problem-solving, or avoiding situations that could lead to further loss of resources. COR theory has been widely used to explain how individuals respond to stress, and how they can preserve their resources and cope with challenging situations.
Viewed through the lens of COR theory, mental health problems like anxiety, depression, and emotional exhaustion can occur when resources are threatened or depleted, or when the expected benefits of investing in resources fail to materialize. In other words, individuals may experience mental health problems when they believe that their emotional resources are inadequate to manage workplace stressors. The fear of COVID-19 is a workplace stressor that can deplete employee resources (Karatepe et al., 2021). The principle that resource investment can aid stress resistance, developed from COR theory (Hobfoll, 2002), forms a solid foundation for understanding the moderating roles of self-compassion and psychological resilience. Studies have demonstrated that personal resources can help individuals deal better with stress-inducing and resource depleting situations (Chen and Eyoun, 2021). Based on these theoretical underpinnings, self-compassion and psychological resilience are expected to moderate the relationship between fear of COVID-19 and mental health problems.
2.2. Fear of COVID-19 and mental health problems
According to COR theory, emotional exhaustion can arise in individuals when they perceive the threat of losing resources or experience an actual loss of resources, and are unable to replenish those resources after investing in them (Hobfoll, 1989, Hobfoll, 2002). Resources refer to anything that is valued by an individual or serves as a means to achieve their goals (Hobfoll, 1989). During the pandemic, frontline employees in the hospitality industry needed to invest both their physical and psychological resources to cope with their fear of contracting COVID-19, which can result in resource depletion and increased stress at work. Furthermore, Karatepe et al. (2021) contended that losing limited resources, while coping with COVID-19 as a stressor, can lead to the experience of mental health problems. Additionally, Lee and Ashforth (1996) asserted that when employees lose their limited resources, do not have enough resources, or do not receive expected returns, it creates emotional strain in employees. Similarly, prior studies and theories have shown that fear can lead to a multitude of mental health problems including depression, anxiety, stress, sleep problems, mental health-related factors, and impaired mental well-being (Alimoradi et al., 2022).
Also, Lazarus and Folkman’s (1984) “transactional theory of stress and coping” states “Psychological stress is a particular relationship between the person and the environment that is appraised by the person as taxing or exceeding his or her resources and endangering his or her well-being” (Lazarus and Folkman, 1984, p.19). That is, an individual’s perception of how well he or she can cope with a particular situation determines whether the event will be experienced as a stressor. A perceived lack of resources signifies a stressful situation. Accordingly, stress is viewed as a subjective experience shaped by perceived resources and demands. Havnen et al. (2020) noted that as research on stress has evolved, the research focus has shifted from examining potential vulnerability factors to the innate ability that many individuals seem to possess that allows them to cope with stressful situations. The “transactional theory of stress and coping” (Lazarus and Folkman, 1984) is also a good fit because it highlights that “it is the perception that the event is stressful, rather than the event itself, that determines whether coping strategies are initiated and whether the stressor is ultimately resolved” (Biggs et al., 2017, p. 352), which aligns with our focus on the fear of COVID-19 among quarantine hotel employees. Drawing on these theories, we hypothesize that quarantine hotel employees who perceive a high risk of acquiring COVID-19 consider this fear a threat that drains their psychological resources, eventually leading to mental health problems. Additionally, prior studies (e.g., Hall et al., 2008) have indicated that during an outbreak, people are fearful of infection, resulting in stress, anxiety, and depression. Besides experiencing stress resulting from long and irregular work hours, quarantine hotel employees may also have high stress and anxiety due to the uncertainty they experience in their work environment. Therefore, we hypothesize the following:
H1: “Fear of COVID-19 is positively related to mental health problems among quarantine hotel employees.”
2.3. Moderating role of self-compassion
Many psychologists have looked for elements that might help people cope with various types of psychological discomfort. A substantial amount of research has shown that employee personal resources are helpful in reducing stress (Li et al., 2021). Compassion is usually considered a positive social emotion and organizational researchers often see compassion as observing and empathizing with others’ suffering and then acting to reduce it (e.g., Kanov et al., 2017). Compassion is considered useful during organizational change and development initiatives and compassionate acts at work can also positively affect the giver (Worline and Dutton, 2017). Although compassion manifests itself in a variety of ways, it is primarily an emotion, concept, or process that is oriented toward others, whether at its very essence or in the context of work. In contrast, self-compassion is directed toward oneself. As of yet, however, there is limited knowledge on the possible role of self-compassion at work in reducing employees’ stress and anxiety (Lefebvre et al., 2020). Neff (2003) considered self-compassion to be critical for effective psychological and behavioral functioning and defined it as the capability to perceive difficulties as a normal aspect of life and to accept them with warmth, connection, and concern. The concept of self-compassion encompasses the following three aspects: mindfulness, defined as “being present and recognizing intrapersonal reactions to difficulties,” self-kindness, defined as “being kind and gentle with oneself rather than being critical of oneself,” and common humanity, defined as “the idea that all humans go through struggles as part of their lives” (Lefebvre et al., 2020, p.440). Studies have suggested that there is growing evidence that self-compassion can benefit individuals and groups equally in the workplace (Horan and Taylor, 2018, Kaurin et al., 2018).
According to COR theory, individuals are driven to accumulate and utilize resources as a means of coping with stressful situations (Hobfoll, 1989). Based on COR theory, it is argued that, to survive and thrive, humans have an innate urge to gather and maintain various types of resources such as object resources, personal resources, and energy resources. This theory posits that individuals employ their accumulated resources to address stressful situations. The accumulation of personal resources by being more self-compassionate fits well with the basic tenet of COR theory which argues for the conservation and accumulation of resources through “gain spirals” (Hobfoll, 2002). Individuals who possess a greater number of resources are more capable of resource gain, as these resources travel in a “caravan of resources” (Hobfoll et al., 2018). Recently, self-compassion as a personal resource has been recognized as a constructive mechanism to cope with stress in the workplace (Sinclair et al., 2017). Individuals with high self-compassion show enhanced emotional well-being and mental health (Gilbert and Procter, 2006). Studies have demonstrated that self-compassion helps individuals to envisage emotional and cognitive responses to negative events in everyday life, as well as buffering people from negative self-feelings while experiencing stressful events (Leary et al., 2007). Lau et al. (2020) suggested that self-compassion may moderate how people respond to challenges by promoting adaptive coping strategies. Individuals with high levels of self-compassion have better positive emotional regulation (e.g. emotional clarity, control of the desire for immediate gratification, and acceptance of emotional responses), which leads to improved mental health (Inwood and Ferrari, 2018). Similarly, Bluth et al. (2018) showed that self-compassion moderated the impact of stressors on psychological well-being in a “laboratory-induced” stressful setting. Accordingly, we hypothesize the following:
H2: “Self-compassion moderates the positive relationship between fear of COVID-19 and mental health problems among quarantine hotel employees such that the relationship is weaker at higher levels of self-compassion.”
2.4. Moderating role of psychological resilience
Psychological resilience is defined as the ability of an individual to withstand adversity and bounce back from difficult life events. The American Psychological Association (2017) defined resilience as “adapting well in the face of adversity, trauma, tragedy, threats or significant sources of stress—such as family and relationship problems, serious health problems, or workplace and financial stressors.” Block and Block (1980) originally conceptualized psychological resilience as a “personality trait.” They assumed that individuals’ adaptation to negative experiences or stressors varies over domains and time. Accordingly, an individual with a high level of resilience would adjust effectively to pressures in the workplace, their personal life, and so on. Although this trait approach is common and considers psychological resilience to be a “stable” characteristic, Den Hartigh and Hill (2022) noted that it is unclear if this trait aids in resisting stresses, recovering from stressors, changing or growing as a result of stressors, or a combination of these. Recent conceptualizations (e.g., Bryan et al., 2019) are clearer about what resilience, or being resilient, means, and have classified it into three types: the ability to (i) “resist stressors,” (ii) “bounce back from stressors,” or (iii) “grow from stressors.” Accordingly, psychological resilience is defined as the ability to resist change and maintain high levels of well-being despite encountering stressors. According to this definition, psychological resilience is the ability to maintain well-being after a stressful experience. This study conceptualizes psychological resilience as the ability to “return to a previous or original state” following a stressor.
According to COR theory, individuals tend to strive to acquire, maintain, nurture, and protect the resources they value (Hobfoll, 1989). That is, individuals rely on the critical resources at their disposal to manage stressful circumstances in their present surroundings, while also proactively building and safeguarding their existing resource reserves in preparation for possible future stressful situations. COR theory suggests that an individual’s coping abilities can be enhanced by their personal resources, such as resilience, which can provide energy or safeguard against the maladaptive psychological states that may be triggered by a stressor (Shin et al., 2012). Drawing on COR theory, Gong et al. (2022) found resilience is a protective resource in coping with the pandemic. Psychological resilience is a protective mechanism that operates in the face of negative stresses, and it is consistently linked to psychological well-being and a decreased risk of mental illness (Aguiar-Quintana et al., 2021). It is well-documented in the literature that those who have great psychological resilience are less likely to suffer from mental illnesses (e.g., Kavčič et al., 2021). People with high psychological resilience have a number of interpersonal and intrapersonal qualities, including more flexibility and the ability to use more suitable coping mechanisms than less resilient people (Song et al., 2021). Gloria and Steinhardt (2016) examined the moderating role of psychological capital and found that those with high levels of psychological resilience are more resistant to stress and have fewer anxiety and depression symptoms than those with low levels of resilience. Similarly, studies have found that an individual’s psychological resilience moderates the effect of stress on anxiety and depression (Pinquart, 2009, Wingo et al., 2010). Accordingly, this study suggests that, at the individual level, quarantine hotel employees’ psychological resilience can act as a protective mechanism against the negative effects of stress resulting from the fear of COVID-19, and that it has had a positive influence on mental health during the COVID-19 pandemic. Therefore, we hypothesize the following:
H3: “Psychological resilience moderates the positive relationship between fear of COVID-19 and mental health problems among quarantine hotel employees such that the relationship is weaker for individuals with high resilience.”
2.5. Three-way interaction
Working in quarantine hotels poses several challenges to employees. Cultivating coping techniques to deal with these challenges, such as increasing psychological resilience and self-compassion, will facilitate an individual to traverse this phase with greater ease. Although prior studies (e.g., Sinclair et al., 2017) have demonstrated that self-compassion mitigates the adverse implications of these emotional challenges, there have been limited studies on the relationship between strengths-based attributes like self-compassion and psychological resilience. Recent research is unclear on how inter-individual variations in self-compassion generate resilience in the wake of stressful events (Kaurin et al., 2018). According to COR theory, self-compassion as a psychological protective resource may work in tandem with psychological resilience to collectively reduce the impact of stressors on mental health problems. Based on arguments that self-compassion enhances psychological resilience (Neff and McGehee, 2010) and evidence that self-compassion regulates mental health problems (Inwood and Ferrari, 2018), we hypothesize that higher levels of self-compassion would amplify the buffering effect of psychological resilience on the relationship between fear of COVID-19 and mental health problems. Individuals who are resilient and self-compassionate employ adaptive coping strategies and typically have a positive self-perception. Individuals who are self-compassionate have a well-balanced attitude and do not engage in harsh self-criticism, which allows them to “bounce back” from life’s adversities (Warren et al., 2016). Self-compassion helps individuals recognize their shortcomings and motivates them to seek help (Dev et al., 2020). Those who adopt a self-compassionate mindset are more inclined to use positive coping mechanisms, develop emotional intelligence, and engage in health-promoting behaviors, all of which contribute to psychological resilience (Lefebvre et al., 2020). Individuals high in self-compassion tend to generate greater levels of resilience due to effective emotion regulation. Furthermore, it is documented that stressors exert less of an impact on those with high self-compassion and resilience than on those with low self-compassion and resilience (Smith, 2015). Additionally, individuals with higher levels of self-compassion display higher adaptive behaviors that require resilience (Shebuski et al., 2020). That is, self-compassion may interact with psychological resilience to influence mental health problems. Based on these considerations, we predict a three-way interaction between fear of COVID-19, self-compassion, and psychological resilience. Furthermore, the interaction postulated is based on the “transactional theory of stress and coping” (Lazarus and Folkman, 1984), which states that psychological resilience buffers the negative effect of stressors on strain and will hold good for individuals with high levels of self-compassion. In particular, the following hypothesis can be drawn:
H4: “Self-compassion will moderate the conditional influence of psychological resilience on the relationship between fear of COVID-19 and mental health problems. The positive relationship between fear of COVID-19 and mental health problems will be weaker for those employees who are high on self-compassion and psychological resilience.”
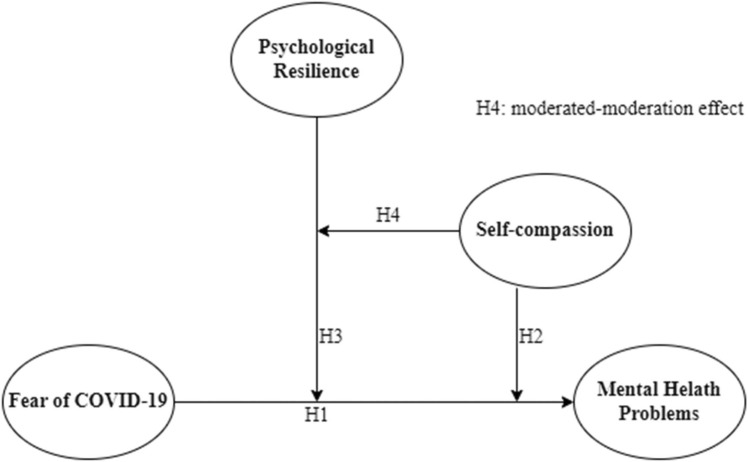
The proposed relationships are shown in Fig. 1.
Fig. 1.
Proposed model.
3. Methodology
3.1. Participants and procedure
The study was conducted among the frontline employees from “Alternative State Quarantine” hotels in Thailand. “Alternative State Quarantine” is a mandatory quarantine process that takes place in “government-approved hotels” in Bangkok at the expense of the guest. Many hotels, in collaboration with hospitals, have created “Alternative State Quarantine Packages” for non-Thai nationals returning from abroad. Thailand’s Ministry of Public Health and Ministry of Defense has approved these hotels. Quarantine hotel frontline employees were recruited because they are more likely to feel emotionally stressed at work (Han et al., 2016) and are at greater risk during the COVID-19 pandemic. Thirteen “Alternative State Quarantine” hotels volunteered to participate in this research endeavor. Among the thirteen hotels, five are luxury, and eight are upper-upscale hotels. A self-reported questionnaire was developed originally in English and was translated to Thai by two translators with survey knowledge and linguistic experience. The two translators made a parallel translation from English to Thai and the translated questionnaires were pre-tested and modified accordingly. The cover letter explained the study background, procedures, and purpose. The anonymity and confidentiality of personal information were ensured for the survey respondents. Data was collected in 2021, from June to September. The sample size was calculated using the sample size to free parameter ratio (Bentler and Chou, 1987), which should be between 5:1 and 10:1. A sample size of 205–410 would be adequate to estimate the 41 free parameters. We conducted a cross-sectional study and used an online survey to gather information from hotel staff. This method was considered necessary to comply with COVID-19 guidelines during the pandemic. Initially, we obtained 398 filled-in responses. We eliminated surveys with incomplete responses. Furthermore, a timer recorded the time it took for the participants to finish the survey. Participants who completed it in an unusually quick time were eliminated based on the recommendations of Wise and Kong (2005). We obtained 360 usable questionnaires for analysis.
3.2. Survey design and measurement scales
The survey had two sections. The first section had measures for “fear of COVID-19,” “mental health,” “self-compassion,” and “psychological resilience.” The second section consisted of demographic variables, including gender, age, education qualification, years of experience in the current organization and in the hotel industry, and department affiliation.
Fear of COVID-19: Seven items from the “Fear of Covid-19 scale (FCV-19S)” (Ahorsu et al., 2020) were used to assess this construct. A sample item includes: “My heart races or palpitates when I think about getting coronavirus-19.” The items were measured on a five-point Likert scale ranging from “1-strongly disagree” to “5-strongly agree.” The Cronbach alpha was 0.813.
Mental health: The short, five-item version of the “Mental Health Inventory (MHI-5)” from Berwick et al. (1991) was used to assess the mental health status of the frontline employees in quarantine hotels. The MHI-5 focused on anxiety, general positive affect, depression, and behavioral/emotional control. Each of the items was introduced by the question, “Working in a quarantine hotel, how much of the time, have you…?” A sample item includes: “….been a nervous person?” The items were scored on a five-point Likert scale ranging from “1-none of the time” to “5-all the time.” The higher the total score, the higher the level of mental health issues. This scale yielded a reliability score of 0.708.
Self-compassion: Twelve items from the “Self-Compassion Scale-Short Form” (Raes et al., 2011) were used to measure self-compassion. This scale is used when the focus is on self-compassion rather than its subscale scores (Lefebvre et al., 2020). The 12-item measure examines the three subscales of self-compassion: self-kindness (“When I’m going through a very hard time, I give myself the caring and tenderness I need.”), common humanity (“When I feel inadequate in some way, I try to remind myself that feelings of inadequacy are shared by most people.”), and mindfulness (“When something painful happens I try to take a balanced view of the situation.”). The respondents responded to a five-point Likert scale running from “1-almost never” to “5-almost always.” The reliability of this scale was 0.775.
Psychological resilience: The new ten-item “Connor-Davidson Resilience Scale (CD-RISC-10)” (Campbell‐Sills and Stein, 2007) is a self-report scale that assesses an individual’s ability to bounce back from negative events, and was derived from the original 25-item CD-RISC (Connor and Davidson, 2003). This uni-dimensional scale is designed as a Likert-type additive scale with five response options (“1-not true at all” and “5-true nearly all the time”). Higher scores reflect higher levels of resilience. The Cronbach alpha was 0.789.
The complete list of items is included in Table 1.
Table 1.
Reliability and validity.
| Constructs | Loadings | AVE | Composite reliability |
|---|---|---|---|
| Fear of COVID-19 | 0.735 | 0.951 | |
| “I am afraid of coronavirus-19.” | 0.874 | ||
| “It makes me uncomfortable to think about coronavirus-19.” | 0.892 | ||
| “My hands become clammy when I think about coronavirus-19.” | 0.883 | ||
| “I am afraid of losing my life because of coronavirus-19.” | 0.825 | ||
| “When watching news and stories about coronavirus-19 on social media, I become nervous or anxious.” | 0.825 | ||
| “I cannot sleep because I’m worrying about getting coronavirus-19.” | 0.891 | ||
| “My heart races or palpitates when I think about getting coronavirus-19.” | 0.805 | ||
| Mental health problems | 0.648 | 0.901 | |
| “Working in a quarantine hotel, how much of the time, have you…” | |||
| “…been a very nervous person?” | 0.708 | ||
| “…felt calm and peaceful?” | 0.788 | ||
| “…felt downhearted and blue?” | 0.752 | ||
| “…been a happy person?” | 0.869 | ||
| “…felt so down in the dumps that nothing could cheer you up?” | 0.891 | ||
| Self-compassion | 0.698 | 0.965 | |
| “When I fail at something important to me I become consumed by feelings of inadequacy.” | 0.701 | ||
| “I try to be understanding and patient toward the aspects of my personality I don’t like.” | 0.933 | ||
| “When something painful happens I try to take a balanced view of the situation.” | 0.938 | ||
| “When I’m feeling down, I tend to feel like most other people are probably happier than I am.” | 0.759 | ||
| “I try to see my failings as part of the human condition.” | 0.709 | ||
| “When I’m going through a very hard time, I give myself the caring and tenderness I need.” | 0.702 | ||
| “When something upsets me I try to keep my emotions in balance.” | 0.704 | ||
| “When I fail at something that’s important to me, I tend to feel alone in my failure.” | 0.935 | ||
| “When I’m feeling down I tend to obsess and fixate on everything that’s wrong.” | 0.935 | ||
| “When I feel inadequate in some way, I try to remind myself that feelings of inadequacy are shared by most people.” | 0.940 | ||
| “I’m disapproving and judgmental about my own flaws and inadequacies.” | 0.755 | ||
| “I’m intolerant and impatient toward those aspects of my personality I don’t like.” | 0.931 | ||
| Psychological resilience | 0.639 | 0.946 | |
| “I am able to adapt to change.” | 0.781 | ||
| “I can deal with whatever comes.” | 0.862 | ||
| “I try to see the humorous side of problems.” | 0.785 | ||
| “Coping with stress can strengthen me.” | 0.778 | ||
| “I tend to bounce back after illness or hardship.” | 0.789 | ||
| “I can achieve my goals despite obstacles.” | 0.858 | ||
| “I can stay focused under pressure.” | 0.702 | ||
| “I am not easily discouraged by failure.” | 0.771 | ||
| “I think of myself as strong person.” | 0.859 | ||
| “I can handle unpleasant feelings.” | 0.857 | ||
3.3. Analysis strategy
The partial least-squares (PLS) model was employed to analyze the data since it places stipulations on measurement scales, sample size, and distribution of residual scores to the bare minimum (Hair et al., 2017). To test the proposed hypotheses, we adopted the two-step approach. It first examined the measurement model’s reliability and validity. Second, it assessed the structural model. PROCESS macro model 3 (Hayes, 2013) was used to examine the three-way interaction. Based on previous research on mental health during the COVID-19 pandemic (Yan et al., 2021), we controlled for age, gender, education, experience, and department affiliation.
3.4. Common method bias
“Common method bias” needs to be investigated because the data was acquired using self-reported measures and both the independent and dependent variables were collected from the same individual (Podsakoff et al., 2012). Both procedural and statistical remedies were used to assess method bias. Procedural remedies were employed, such as protecting the participants’ anonymity and confidentiality, and notifying participants that there were no preferred or correct responses and that the research team wanted honest feedback on the items. Furthermore, we used the “measured latent marker variable” technique. The change in R2 value was relatively small when compared to the original model without the marker variable. The difference in variance was 0.014 upon adding the marker variable. Hence, common method bias has no significant impact on the conclusions drawn from this data.
4. Results
4.1. Demographic profile and descriptive statistics
Out of the 360 respondents, 37% are male and 63% are female. The average years of experience in the current hotel is 8 years and in the hotel industry, 11 years. Nearly half the respondents were aged 25–34 years and 36% were aged 35–44 years. More than half the respondents (59%) held a 4-year college degree. Regarding department affiliation, 31% belonged to the front office, 33% belonged to food and beverage, and 36% belonged to housekeeping. The mean (standard deviation) of the constructs is: Fear of COVID-19 = 4.757(1.072), mental health problems = 4.661(1.034), self-compassion = 3.989(0.805), and psychological resilience = 3.920(0.841).
4.2. Assessment of measurement model
The CFA with all the constructs demonstrated satisfactory results, with fit indices: χ2 = 1033.80, df = 363, χ2/df = 2.847, PNFI = 0.941, CFI = 0.935, IFI = 0.926, TLI = 0.907, SRMR = 0.045, and RMSEA = 0.071 (Bentler and Bonett, 1980). The indicator loadings ranged from 0.701 to 0.940 and are greater than the threshold value of 0.7, indicating that the indicators are reliable. The composite reliability varied from 0.901 to 0.964, exceeding the recommended value of 0.7. Thus, the model exhibited good internal consistency (Hair et al., 2017). The average variance extracted (AVE) values range from 0.639 to 0.735, well above the recommended threshold of 0.50. The convergent validity of all items is confirmed by these findings. Hence, the convergent validity is met, as indicated in Table 1. Furthermore, the square root of each construct’s AVE is greater than its correlation with other constructs, thus confirming discriminant validity (Fornell and Larcker, 1981). Also, the Chi-square difference test, which compares the Chi-square values of the constrained model (with the correlation coefficient between two factors constrained to 1) and the unconstrained model (with the correlation coefficient between two factors as freely estimated parameters), was used to determine whether or not the scale has good discriminant validity. The Chi-square value differences between constrained and unconstrained models for all the factors are above the critical indicator ꭓ2 0.05 = 3.841, thus exhibiting discriminant validity (Anderson and Gerbing, 1988). The results of discriminant validity are shown in Table 2.
Table 2.
Discriminant validity.
| Fear of COVID-19 | Mental health problems | Self-compassion | Psychological resilience | |
|---|---|---|---|---|
| Fear of COVID-19 | 0.858 | |||
| Mental health problems | 0.359 | 0.949 | ||
| Self-compassion | 0.406 | 0.931 | 0.982 | |
| Psychological resilience | 0.623 | 0.556 | 0.591 | 0.972 |
Note: The values in bold are the square root of the AVEs. Values below the diagonal are the correlations
4.3. Assessment of structural model
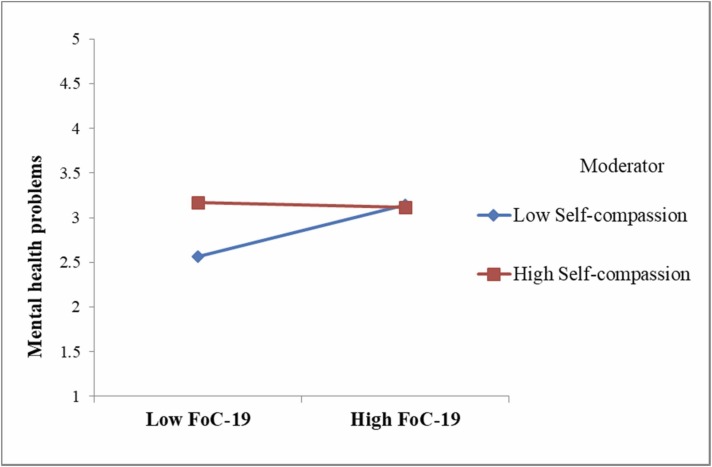
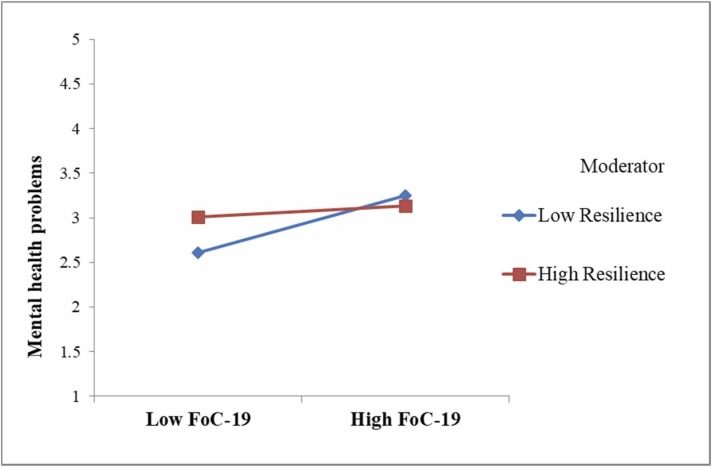
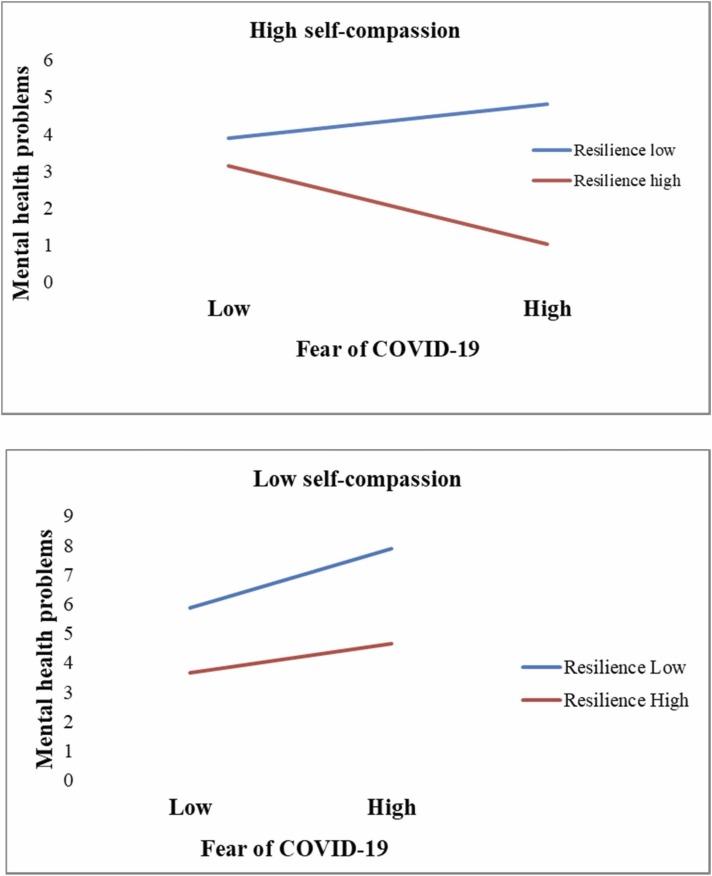
A preliminary analysis revealed that the control variables had no significant impact on the outcome variable. Therefore, these variables were excluded from further analysis. Following the suggestions of Hair et al. (2017), the path coefficients, t-values, and p-values for the structural model were calculated by employing a 5,000-sample re-sample bootstrapping approach. As indicated in Table 3, it is evident that the fear of COVID-19 positively influenced mental health problems (“β = 0.457, t = 11.335, p < 0.001″). R2 was 0.381, implying that the predictor explained 38.1% of the variance in mental health problems. Thus, H1 was supported. Second, the moderation effect of self-compassion was examined. Self-compassion moderated the positive effect between fear of COVID-19 and mental health problems (“β = −0.608, t = −4.779, p < 0.001″). The interaction accounted for significant incremental variance in mental health problems (ΔR2 = 0.029, p < 0.001). Tests of simple slopes ( Fig. 2) indicate that self-compassion dampened the positive link between fear of COVID-19 and mental health problems. Therefore, H2 is supported. Next, the moderating role of psychological resilience was investigated. As predicted, psychological resilience moderated the positive link between fear of COVID-19 and mental health problems (“β = −0.444, t = −3.685, p < 0.001″). The interaction accounted for significant incremental variance in mental health problems (ΔR2 = 0.017, p < 0.001). As indicated in Fig. 3, resilience weakened the positive link between fear of COVID-19 and mental health problems. Hence, H3 was supported. Finally, H4 predicted that the positive relationship between fear of COVID-19 and mental health problems would be weaker for individuals who have high self-compassion and high resilience than those with low self-compassion and low resilience. To test the three-way interaction between fear of COVID-19 with self-compassion and resilience on mental health problems, PROCESS macro Model 3 (Hayes, 2013) was employed. The three-way interaction of fear of COVID-19, self-compassion, and resilience was significant (“β = −0.239, t = −2.972, p < 0.05″), explaining an additional 3.8% of the variance. For a more specific test of the proposed hypothesis, we calculated the slope difference tests suggested by Dawson and Richter (2006). For an individual with high self-compassion, fear of COVID-19 was not related to mental health problems under conditions of high resilience (“β = −0.17, t = −1.183, p > 0.05″) but was positively related to mental health problems under conditions of low resilience. Moreover, these two slopes differed significantly (“t = 2.28, p < 0.05″). Similarly, for individuals with low self-compassion, fear of COVID-19 was strongly related to mental health problems under conditions of low resilience (“β = 0.355, t = 5.358, p < 0.001″), compared to under conditions of high resilience. The slope difference was significant (“t = 1.99, p < 0.05″). Hence, H4 was supported. Figs. 4a and 4b display the effect of fear of COVID-19 and resilience on mental health problems when individuals are high or low in self-compassion, respectively. The results of hypotheses testing are displayed in Table 3.
Table 3.
Summary of results.
| Hypotheses | Path coefficients | SE | t-values | R2 & ΔR2 | Decision |
|---|---|---|---|---|---|
| H1: “Fear of COVID-19→ mental health problems” | 0.457 | 0.041 | 11.335 * * | R2: 0.381 | Supported |
| H2: “Fear of COVID-19 * self-compassion→ mental health problems” | -0.608 | 0.127 | -4.779 * * | ΔR2: 0.029 | Supported |
| H3: “Fear of COVID-19 * psychological resilience→ mental health problems” | -0.444 | 0.121 | -3.685 * * | ΔR2: 0.017 | Supported |
| H4: “Fear of COVID-19 * self-compassion * psychological resilience→ mental health problems” | -0.239 | 0.080 | -2.972 * | ΔR2: 0.038 | Supported |
Note: * p < 0.05, * * p < 0.001
Fig. 2.
Moderating effect of self-compassion.
Fig. 3.
Moderating role of psychological resilience.
Fig. 4.
Interactions between fear of COVID-19 and psychological resilience predicting mental health problems for individuals with (a) high self-compassion and (b) low self-compassion.
5. Discussion and implications
5.1. Discussion
First, fear of COVID-19 was positively associated with mental health problems. Sönmez et al. (2020) discussed in great detail the extent of occupational stress affecting hotel employees. Fear of COVID-19 exacerbates the stress of already-strained quarantine hotel employees and erodes their mental health. This result is consistent with the findings of Karatepe et al. (2021). In line with COR theory (Hobfoll, 1989), quarantine hotel employees who have a high chance of contracting COVID-19 regard this fear as a threat that consumes their psychological resources, eventually resulting in mental health problems. Consistent with the concept of the loss spiral in COR theory (Hobfoll, 2002), the results indicate that employees who are stressed because of their fear of COVID-19 will experience a decrease in mental well-being and mental health. Second, self-compassion moderated the positive link between fear of COVID-19 and mental health problems. This relationship was weaker for employees who were high in self-compassion. High levels of self-compassion attenuated the link between fear of COVID-19 and mental health problems. Grounded in COR theory (Hobfoll, 1989), self-compassion as a personal resource can influence the development of self-regulation, thus assisting individuals in effectively dealing with stressors. Therefore, individuals with higher degrees of self-compassion are more aware of their own needs and may be able to cope with the negative consequences of pandemic-related threats by being kinder to themselves and viewing the global threat as a shared experience with others. These results corroborate previous studies that report on the role of self-compassion in psychological well-being (Kyeong, 2013). Similarly, psychological resilience moderated the influence of fear of COVID-19 on mental health problems. The results of the moderation analysis revealed that for highly resilient employees, the link between fear of COVID-19 and mental health problems was weak compared to employees with low resilience. That is, highly resilient employees are better able to withstand the fear of COVID-19 and able to recover from its negative effects, whereas employees with low resilience are more likely to experience mental health problems. The findings imply that resilient employees are able to develope their abilities to cope and thrive when facing challenges and obstacles. According to the COR framework, employees who are resilient use their coping strategies to protect their personal resources when they face stressors in the workplace (Hobfoll, 2002). High resilience allows employees to approach situations with confidence, which is specifically important for employees working in challenging environments like quarantine hotels. The results support the findings of Chen et al. (2021). Finally, the three-way interaction demonstrated that the link between fear of COVID-19 and mental health problems is weakest among employees with high self-compassion and high resilience, and strongest for employees who have low self-compassion and resilience. The findings provide evidence that higher levels of self-compassion can significantly influence the reduction in mental health problems for highly resilient employees by reducing stress arising from fear of COVID-19. Thus, employing COR theory (Hobfoll, 1989), we demonstrated that the three-way interaction of two pertinent personal resources—self-compassion and psychological resilience—acts as a buffering resource that helps to lessen the harmful effects of fear of COVID-19 on mental health problems. For highly self-compassionate employees, high levels of resilience may act as an adaptive emotional regulation mechanism which guards against the activation of negative schemas triggered by stressful events (Trompetter et al., 2017).
5.2. Theoretical contributions
The study contributes to the current knowledge in the following ways. First, the present study is among the few that examine the mental health of frontline employees during a crisis, more specifically in quarantine hotels. This study responds to the call for further studies on the impact of COVID-19 on the mental health of frontline employees (Su et al., 2021). Due to the infectious volatility of COVID-19, frontline employees in quarantine hotels are at a higher risk of contracting COVID-19 and are more likely to have mental health issues (Karatepe et al., 2021, Sönmez et al., 2020). Unsurprisingly, these employees will be the most crucial players in the recovery of their firms once COVID-19 has been quelled. However, there are few studies in hospitality and tourism literature that show that COVID-19 exacerbates such employees’ mental health problems. This study attempted to fill this gap. Furthermore, the study applied COR theory (Hobfoll, 1989) to emphasize the buffering effect of self-compassion and psychological resilience in the positive relationship between fear of COVID-19 and mental health problems, furthering our understanding of the significance of employees’ self-compassion and psychological resilience in crisis situations. The findings also contribute to understanding the predictors of mental health problems during a pandemic, particularly during the COVID-19 outbreak. Understanding the impact of the pandemic on mental health is crucial for providing appropriate mental health interventions (Giallonardo et al., 2020).
Second, the findings reflect that high levels of self-compassion are linked to improved mental health. Therefore, self-compassion may be viewed as a distinct human strength and a foundation for better mental health. Kaurin et al. (2018) noted that research on self-compassion is still in its infancy, and thus more studies on the relationship between self-compassion and psychological well-being are required. Consequently, the results contribute to the small number of studies that examine the specific mechanism by which self-compassion in an organizational setting might serve as a protective factor against mental health problems. Previous research (e.g., Leary et al., 2007) has found a positive link between self-compassion and adaptive emotion regulation techniques like positive cognitive reappraisal and acceptance, and a negative link between self-compassion and dysfunctional emotion regulation techniques like “experience avoidance,” “thought suppression,” and “rumination.” This indicates that self-compassion allows stressors such as the fear of COVID-19 to be perceived as more transient, manageable, and less aversive, thus preventing mental health problems. Individuals high in self-compassion are more inclined to consider adversities in adaptive ways; they are realistic and unbiased, less likely to exaggerate and harshly condemn themselves, and more willing to perceive tough experiences as a normal part of life. Furthermore, instead of participating in self-criticism or self-blame in the midst of stressful situations, they respond to themselves with self-compassion—actively comforting themselves.
Finally, the findings provide a greater understanding of the interplay between individual-level variables in relation to mental health. Previous studies have examined the role of social support, loneliness, and prior mental health issues in affecting mental health during the pandemic (e.g., Keshavan, 2020). The findings contribute to this line of research by examining the moderating roles of self-compassion and psychological resilience. An understanding of the psychological factors that moderate the negative effects of stress and anxiety during a pandemic is particularly crucial for the development of effective intervention and preventive measures for stress, depression, and mental health related problems. It was found that employees with high levels of self-compassion and psychological resilience were more successful in managing the mental distress caused by COVID-19. The results indicate that an employee’s stress reactions to COVID-19 and stressors in general are impacted by a multiplex, dynamic process that involves concurrent interchange between the stressors and evaluation of the stressors. It also makes a significant contribution to “health protection theories” and understanding employees’ psychological well-being in the hospitality industry.
5.3. Practical implications
To alleviate mental health problems, quarantine hotel managers and operators may implement non-pharmaceutical interventions (Pillai et al., 2021) to lessen frontline employees’ apprehension during crises. First, the individuals’ soothing systems should be effectively activated by self-compassion, while their threat and resource systems are deactivated. As a result, self-compassion can assist people in achieving a positive state of resilience. Positive results are experienced when participating in self-compassion because it is an intrapersonal experience, independent of external factors (Neff, 2003). These principles imply that practicing self-compassion intentionally can calm the system, resulting in a feeling of peace, contentment, and well-being, as well as more emotional space to connect to resilient coping techniques (Gilbert et al., 2008). Hospitality HR managers can provide employees with access to resources on self-compassion, such as articles, videos, and books, all of which can help employees understand the benefits of self-compassion. Specifically, hotel HR departments can implement Neff and Germer’s (2013) “The Mindful Self-Compassion program (MSC).” This is a structured program intended to promote “self-compassion,” “mindfulness,” “life satisfaction,” “social connectivity,” and “happiness” while reducing negative consequences such as depression, stress, and anxiety. To improve self-compassion, both formal and informal self-compassionate meditations are utilized. Their strategy has been proven to increase self-compassion among individuals. This program includes lessons on meditation techniques such as (1) “nonjudgmental awareness of the sensations, thoughts, and emotions,” and (2) “noting and letting go of rumination and worries to cultivate adaptive coping skills for stress management” (Shapiro et al., 2005, p. 165).
Additionally, since self-compassion can be learned, offering training and a physical place to practice might be extremely beneficial in the long-term. Furthermore, self-compassion may be cultivated and improved through increasing attention and kindness toward oneself and others (Lefebvre et al., 2020). As a result, participating in community activities may encourage employees to volunteer to help those in need and may aid in the development of loving compassion for others and themselves. Hotel HR departments may offer workshops and training sessions to help employees develop self-compassion skills. This could include guided meditations, self-reflection exercises, or other activities that promote self-care and self-kindness. Self-compassion training can help employees develop vital qualities like tranquility, warmth and gentleness, forgiveness, expanded awareness, and feelings of interconnectedness with others. These characteristics will increase elements such as self-acceptance, excellent social relationships, and positive emotions, all of which are linked to good mental health. Such training and intervention can assist employees in recovering from mental stress. They may further encourage employees to use positive self-talk and to reframe negative self-talk in a compassionate way. It may act as a new tool to change the environment in which unpleasant events and stressful experiences occur in the future. This can help employees become more robust, as well as prevent them from subsequent remission or the emergence of new mental disorders (Neff and Germer, 2013). Protective factors, such as self-compassion and psychological resilience, may be learned through developing a meaningful purpose in life and believing that both positive and negative life experiences can be used to learn and grow. Previous research has indicated that Gestalt-based therapy procedures (such as the two-chair approach) can help people feel less self-critical and more compassionate toward themselves (see Neff et al., 2007, for a detailed procedure of the approach). Similarly, significant decreases in depression and associated symptoms are shown in employees who participate in “cognitive restructuring-based group therapy” that educates them to build the skills required to become more self-compassionate (Gilbert and Procter, 2006). Furthermore, hotel managers and supervisors can model self-compassion by demonstrating kindness, empathy, and compassion toward their employees and creating a culture of kindness and support.
Second, one of the most significant determinants of well-being is psychological resilience (Robertson et al., 2015). Prior studies have demonstrated that numerous psychological therapies, such as mindfulness, self-efficacy training, and cognitive behavioral therapy are beneficial in building psychological resilience. Hotel HR departments may improve their employees’ psychological resilience by strengthening social relationships within the organization, promoting physical and mental wellness, finding purpose by establishing and accomplishing realistic goals, and adopting positive thinking. HR departments may further provide training and workshops on stress management, coping skills, and resilience-building techniques. Specifically, training programs that focus on positive thinking, problem-solving, and self-care can provide employees with a comprehensive approach to building resilience and coping with stress. These resilience-building interventions can be used before, during, or after stressful or traumatic events. Individuals are better equipped to deal with adversity if interventions/training occurs prior to stressful events. Understanding the drivers of psychological resilience and integrating them into a framework that can advise HR managers is therefore crucial to identifying the developmental pathways that foster employees’ ability to successfully confront stressful and demanding work situations. Third, contact-less technology should be prioritized in the hospitality industry not just to decrease the fear of COVID-19, but also to improve employees’ psychological well-being (Pillai et al., 2021). Besides reducing human error, contactless technologies are safer from a health perspective. Suitable training programs on hygiene, cleanliness, and safety may also be implemented to help employees feel safer and more confident.
6. Limitations and directions for future research
The study’s findings are mitigated by certain limitations. To begin with, the study relied on self-reported measures, which are prone to common method bias (Podsakoff et al., 2012). Stress and well-being, on the other hand, are intrinsically subjective phenomena that may be best judged through self-reports. Therefore, the procedural and statistical remedies suggested by Podsakoff et al. (2012) were adopted. Future studies may however collect data from multiple sources to reduce the effect of common method bias. Second, the cross-sectional design of the study is an empirical restriction that precludes us from establishing stronger causal conclusions. The “transactional theory of stress and coping” (Lazarus and Folkman, 1984), which we applied, suggests that causation goes from external evaluation of situational cues to internal mood, not the other way around, which lends some credence to our study’s causal direction. Nonetheless, for better casual inferences future studies may adopt experimental and longitudinal studies (e.g., full-panel studies and diary studies). Third, the reported mental health problems were self-reported and were not based on clinical evaluations. Additionally, we did not go into detail on whether or not respondents had depressive conditions or related mental health concerns prior to the pandemic or at any time in their lives. Since the samples belonged to quarantine hotels in Thailand, the generalizability of our findings may be compromised. Future studies may extend the proposed framework to understand the impact of mental health problems on employees’ work and non-work outcomes. Future research may also examine the moderating role of other personal resource variables, such as psychological capital, that can mitigate the effects of the fear of COVID-19 on mental health problems.
Declaration of Competing Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Acknowledgements
This research was supported by the GuangDong Basic and Applied Basic Research Foundation (Grant Number: 2022A1515010376).
Data Availability
The data that has been used is confidential.
References
- Aguiar-Quintana T., Nguyen T.H.H., Araujo-Cabrera Y., Sanabria-Díaz J.M. Do job insecurity, anxiety and depression caused by the COVID-19 pandemic influence hotel employees’ self-rated task performance? The moderating role of employee resilience. Int. J. Hosp. Manag. 2021;94 doi: 10.1016/j.ijhm.2021.102868. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ahorsu D.K., Lin C.Y., Imani V., Saffari M., Griffiths M.D., Pakpour A.H. The fear of COVID-19 scale: development and initial validation. Int. J. Ment. Health Addict. 2020:1–9. doi: 10.1007/s11469-020-00270-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Alimoradi Z., Ohayon M.M., Griffiths M.D., Lin C.Y., Pakpour A.H. Fear of COVID-19 and its association with mental health-related factors: systematic review and meta-analysis. BJPsych Open. 2022;8(2) doi: 10.1192/bjo.2022.26. [DOI] [PMC free article] [PubMed] [Google Scholar]
- American Psychological Association. (2017). The road to resilience. Retrieved from http://www.apa.org/helpcenter/road-resilience.asp.
- Anderson J.C., Gerbing D.W. Structural equation modeling in practice: a review and recommended two-step approach. Psychol. Bull. 1988;103(3):411–423. [Google Scholar]
- Bentler P.M., Bonett D.G. Significance tests and goodness of fit in the analysis of covariance structures. Psychol. Bull. 1980;88(3):588. [Google Scholar]
- Bentler P.M., Chou C.P. Practical issues in structural modeling. Sociol. Methods Res. 1987;16(1):78–117. [Google Scholar]
- Berwick D.M., Murphy J.M., Goldman P.A., Ware J.E., Barsky A.J., Weinstein M.C. Performance of a five-item mental health screening test. Med. Care. 1991;29(2):169–176. doi: 10.1097/00005650-199102000-00008. [DOI] [PubMed] [Google Scholar]
- Biggs A., Brough P., Drummond S. Lazarus and Folkman’s psychological stress and coping theory. Handb. Stress Health.: A Guide Res. Pract. 2017:351–364. [Google Scholar]
- Block J.H., Block J. In: Collins W.A., editor. Vol. 13. Lawrence Erlbaum; Hillsdale, NJ: 1980. The role of ego-control and ego-resiliency in the organization of behavior; pp. 39–101. (Development of cognition, affect, and social relations. The Minnesota symposia on child psychology). [Google Scholar]
- Bluth K., Mullarkey M., Lathren C. Self-compassion: a potential path to adolescent resilience and positive exploration. J. Child Fam. Stud. 2018;27(9):3037–3047. doi: 10.1007/s10826-018-1125-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Boyraz G., Legros D.N. Coronavirus disease (COVID-19) and traumatic stress: probable risk factors and correlates of posttraumatic stress disorder. J. Loss Trauma. 2020;25(6–7):503–522. [Google Scholar]
- Bryan C., O'Shea D., MacIntyre T. Stressing the relevance of resilience: a systematic review of resilience across the domains of sport and work. Int. Rev. Sport Exerc. Psychol. 2019;12(1):70–111. [Google Scholar]
- Campbell‐Sills L., Stein M.B. Psychometric analysis and refinement of the Connor– Davidson resilience scale (CD‐RISC): Validation of a 10–item measure of resilience. J. Trauma. Stress.: Off. Publ. Int. Soc. Trauma. Stress. Stud. 2007;20(6):1019–1028. doi: 10.1002/jts.20271. [DOI] [PubMed] [Google Scholar]
- Chen H., Eyoun K. Do mindfulness and perceived organizational support work? Fear of COVID-19 on restaurant frontline employees’ job insecurity and emotional exhaustion. Int. J. Hosp. Manag. 2021;94(August 2020) doi: 10.1016/j.ijhm.2020.102850. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Chen Y., Liu Y., Zhang Y., Li Z., Zhou T. The effect of fear of the COVID-19 on depression among chinese outbound students studying online in china amid the COVID-19 pandemic period: the role of resilience and social support. Front. Psychol. 2021;12(October):1–11. doi: 10.3389/fpsyg.2021.750011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Connor K.M., Davidson J.R.T. Development of a new resilience scale: the connor- davidson resilience scale (CD-RISC) Depress Anxiety. 2003;18(2):76–82. doi: 10.1002/da.10113. [DOI] [PubMed] [Google Scholar]
- Dawson J.F., Richter A.W. Probing three-way interactions in moderated multiple regression: development and application of a slope difference test. J. Appl. Psychol. 2006;91(4):917–926. doi: 10.1037/0021-9010.91.4.917. [DOI] [PubMed] [Google Scholar]
- Den Hartigh R.J.R., Hill Y. Conceptualizing and measuring psychological resilience: What can we learn from physics. N. Ideas Psychol. 2022;66(August 2021) doi: 10.1016/j.newideapsych.2022.100934. [DOI] [Google Scholar]
- Department of Foreign Affairs (2021). Alternative State Quarantine (ASQ) in Thailand. Alternative State Quarantine (ASQ) in Thailand | ThaiEmbassy.com.
- Dev V., Fernando A.T., Consedine N.S. Self-compassion as a stress moderator: a cross-sectional study of 1700 doctors, nurses, and medical students. Mindfulness. 2020;11(5):1170–1181. doi: 10.1007/s12671-020-01325-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Fletcher D., Sarkar M. Psychological resilience: a review and critique of definitions, concepts, and theory. Eur. Psychol. 2013;18(1):12. [Google Scholar]
- Fornell, C., & Larcker, D.F. (1981). Structural equation models with unobservable variables and measurement error: Algebra and statistics.
- Giallonardo V., Sampogna G., Del Vecchio V., Luciano M., Albert U., Carmassi C., Fiorillo A. The impact of quarantine and physical distancing following COVID- 19 on mental health: study protocol of a multicentric Italian population trial. Front. Psychiatry. 2020;11(June):1–10. doi: 10.3389/fpsyt.2020.00533. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gilbert P., Procter S. Compassionate mind training for people with high shame and self-criticism: overview and pilot study of a group therapy approach. Clin. Psychol. Psychother. 2006;13:353–379. [Google Scholar]
- Gilbert P., McEwan K., Mitra R., Franks L., Richter A., Rockliff H. Feeling safe and content: a specific affect regulation system? Relationship to depression, anxiety, stress, and self-criticism. J. Posit. Psychol. 2008;3(3):182–191. [Google Scholar]
- Gloria C.T., Steinhardt M.A. Relationships among positive emotions, coping, resilience and mental health. Stress Health. 2016;32(2):145–156. doi: 10.1002/smi.2589. [DOI] [PubMed] [Google Scholar]
- Gong Z., Lv Y., Jiao X., Liu J., Sun Y., Qu Q. The relationship between COVID- 19-related restrictions and fear of missing out, problematic smartphone use, and mental health in college students: the moderated moderation effect of resilience and social support. Front. Public Health. 2022;10 doi: 10.3389/fpubh.2022.986498. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hair J.F., Jr, Sarstedt M., Ringle C.M., Gudergan S.P. SAGE publications; 2017. Advanced Issues in Partial Least Squares Structural Equation Modeling. [Google Scholar]
- Haldorai K., Kim W.G., Pillai S.G., Park T.E., Balasubramanian K. Factors affecting hotel employees’ attrition and turnover: application of pull-push-mooring framework. Int. J. Hosp. Manag. 2019;83:46–55. [Google Scholar]
- Hall R.C., Hall R.C., Chapman M.J. The 1995 Kikwit Ebola outbreak: lessons hospitals and physicians can apply to future viral epidemics. Gen. Hosp. Psychiatry. 2008;30(5):446–452. doi: 10.1016/j.genhosppsych.2008.05.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hamouche S. COVID-19 and employees’ mental health: stressors, moderators and agenda for organizational actions. Emerald Open Res. 2020;2:15. doi: 10.35241/emeraldopenres.13550.1. [DOI] [Google Scholar]
- Han S.J., Bonn M.A., Cho M. The relationship between customer incivility, restaurant frontline service employee burnout and turnover intention. Int. J. Hosp. Manag. 2016;52:97–106. [Google Scholar]
- Havnen A., Anyan F., Hjemdal O., Solem S., Riksfjord M.G., Hagen K. Resilience moderates negative outcome from stress during the COVID-19 pandemic: a moderated mediation approach. Int. J. Environ. Res. Public Health. 2020;17(18):1–12. doi: 10.3390/ijerph17186461. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hayes A.F. Introduction to mediation, moderation, and conditional process analysis: A regression-based approach edn. Guilford Publications; New York: 2013. Mediation, Moderation, and Conditional Process Analysis; p. 120. [Google Scholar]
- Hobfoll S.E. Conservation of resources: a new attempt at conceptualizing stress. Am. Psychol. 1989;44(3):513. doi: 10.1037//0003-066x.44.3.513. [DOI] [PubMed] [Google Scholar]
- Hobfoll S.E. Social and psychological resources and adaptation. Rev. Gen. Psychol. 2002;6(4):307–324. [Google Scholar]
- Hobfoll S.E., Halbesleben J., Neveu J.-P., Westman M. Conservation of resources in the organizational context: the reality of resources and their consequences. Annu. Rev. Organ. Psychol. Organ. Behav. 2018;5:103–128. [Google Scholar]
- Horan K.A., Taylor M.B. Mindfulness and selfcompassion as tools in health behavior change: an evaluation of a workplace intervention pilot study. Journal of Contextual. Behav. Sci. 2018;8:8–16. [Google Scholar]
- Hu T., Zhang D., Wang J. A meta-analysis of the trait resilience and mental health. Personal. Individ. Differ. 2015;76:18–27. doi: 10.1016/j.paid.2014.11.039. [DOI] [Google Scholar]
- Inwood E., Ferrari M. Mechanisms of change in the relationship between self‐ compassion, emotion regulation, and mental health: a systematic review. Appl. Psychol.: Health Well‐Being. 2018;10(2):215–235. doi: 10.1111/aphw.12127. [DOI] [PubMed] [Google Scholar]
- Kanov J., Powley E.H., Walshe N.D. Is it ok to care? How compassion falters and is courageously accomplished in the midst of uncertainty. Hum. Relat. 2017;70(6):751–777. [Google Scholar]
- Karatepe O.M., Saydam M.B., Okumus F. COVID-19, mental health problems, and their detrimental effects on hotel employees’ propensity to be late for work, absenteeism, and life satisfaction. Curr. Issues Tour. 2021;24(7):934–951. doi: 10.1080/13683500.2021.1884665. [DOI] [Google Scholar]
- Kaurin A., Schönfelde S., Wessa M. Self-compassion buffers the link between self- criticism and depression in trauma-exposed fire fighters. J. Couns. Psychol. 2018;65(4):453–462. doi: 10.1037/cou0000275. [DOI] [PubMed] [Google Scholar]
- Kavčič T., Avsec A., Zager Kocjan G. Psychological functioning of slovene adults during the COVID-19 pandemic: does resilience matter? Psychiatr. Q. 2021;92(1):207–216. doi: 10.1007/s11126-020-09789-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Keshavan M.S. Pandemics and Psychiatry: Repositioning research in context of COVID- 19. Asian J. Psychiatry. 2020;51 doi: 10.1016/j.ajp.2020.102159. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kyeong L.W. Self-compassion as a moderator of the relationship between academic burn- out and psychological health in Korean cyber university students. Personal. Individ. Differ. 2013;54(8):899–902. doi: 10.1016/j.paid.2013.01.001. [DOI] [Google Scholar]
- Lau B.H.P., Chan C.L.W., Ng S.M. Self-compassion buffers the adverse mental health impacts of Covid-19-related threats: results from a cross-sectional Survey at the First Peak of Hong Kong’s outbreak. Front. Psychiatry. 2020;11(November):1–8. doi: 10.3389/fpsyt.2020.585270. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lazarus, R.S., & Folkman, S. (1984). Stress, appraisal, and coping. Springer publishing company.
- Leary M.R., Tate E.B., Adams C.E., Allen A.B., Hancock J. Self-compassion and reactions to unpleasant self-relevant events: The implications of treating oneself kindly. J. Personal. Soc. Psychol. 2007;92:887–904. doi: 10.1037/0022-3514.92.5.887. [DOI] [PubMed] [Google Scholar]
- Lee R.T., Ashforth B.E. A meta-analytic examination of the correlates of the three dimensions of job burnout. J. Appl. Psychol. 1996;81(2):123. doi: 10.1037/0021-9010.81.2.123. [DOI] [PubMed] [Google Scholar]
- Lefebvre J.I., Montani F., Courcy F. Self-compassion and resilience at work: a practice-oriented review. Adv. Dev. Hum. Resour. 2020;22(4):437–452. doi: 10.1177/1523422320949145. [DOI] [Google Scholar]
- Li F., Luo S., Mu W., Li Y., Ye L., Zheng X., Chen X. Effects of sources of social support and resilience on the mental health of different age groups during the COVID-19 pandemic. BMC Psychiatry. 2021;21(1):1–14. doi: 10.1186/s12888-020-03012-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lilius J.M., Worline M.C., Maitlis S., Kanov J., Dutton J.E., Frost P. The contours and consequences of compassion at work. J. Organ. Behav. 2008;29(2):193–218. http://doi.org/dv4ch7. [Google Scholar]
- Lin J., Ren Y., Gan H., Chen Y., Huang Y., You X. Factors influencing resilience of medical workers from other provinces to Wuhan fighting against 2019 novel coronavirus pneumonia. BMC Psychiatry. 2020:1–15. doi: 10.21203/rs.3.rs-17931/v1. [DOI] [Google Scholar]
- MacBeth A., Gumley A. Exploring compassion: a meta-analysis of the association between self-compassion and psychopathology. Clin. Psychol. Rev. 2012;32(6):545–552. doi: 10.1016/j.cpr.2012.06.003. [DOI] [PubMed] [Google Scholar]
- Neff K.D. The development and validation of a scale to measure self-compassion. Self Identit-.-. 2003;2(3):223–250. [Google Scholar]
- Neff K.D., Germer C.K. A pilot study and randomized controlled trial of the mindful self‐compassion program. J. Clin. Psychol. 2013;69(1):28–44. doi: 10.1002/jclp.21923. [DOI] [PubMed] [Google Scholar]
- Neff K.D., McGehee P. Self-compassion and psychological resilience among adolescents and young adults. Self Identit-.-. 2010;9(3):225–240. [Google Scholar]
- Neff K.D., Kirkpatrick K.L., Rude S.S. Self-compassion and adaptive psychological functioning. J. Res. Personal. 2007;41(1):139–154. [Google Scholar]
- Pillai S.G., Haldorai K., Seo W.S., Kim W.G. COVID-19 and hospitality 5.0: redefining hospitality operations. Int. J. Hosp. Manag. 2021;94 doi: 10.1016/j.ijhm.2021.102869. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Pinquart M. Moderating effects of dispositional resilience on associations between hassles and psychological distress. J. Appl. Dev. Psychol. 2009;30(1):53–60. [Google Scholar]
- Podsakoff P.M., MacKenzie S.B., Podsakoff N.P. Sources of method bias in social science research and recommendations on how to control it. Annu. Rev. Psychol. 2012;63(1):539–569. doi: 10.1146/annurev-psych-120710-100452. [DOI] [PubMed] [Google Scholar]
- Raes F., Pommier E., Neff K.D., Van Gucht D. Construction and factorial validation of a short form of the self‐compassion scale. Clin. Psychol. Psychother. 2011;18(3):250–255. doi: 10.1002/cpp.702. [DOI] [PubMed] [Google Scholar]
- Robertson I.T., Cooper C.L., Sarkar M., Curran T. Resilience training in the workplace from 2003 to 2014: a systematic review. J. Occup. Organ. Psychol. 2015;88(3):533–562. [Google Scholar]
- Schaubroeck J.M., Riolli L.T., Peng A.C., Spain E.S. Resilience to traumatic exposure among soldiers deployed in combat. J. Occupat. Health Psychol. 16. 2011:18–37. doi: 10.1037/a0021006. [DOI] [PubMed] [Google Scholar]
- Shapiro S.L., Astin J.A., Bishop S.R., Cordova M. Mindfulness-based stress reduction for health care professionals: results from a randomized trial. Int. J. Stress Manag. 2005;12(2):164–176. [Google Scholar]
- Shebuski K., Bowie J.A., Ashby J.S. Self‐compassion, trait resilience, and trauma exposure in undergraduate students. J. Coll. Couns. 2020;23(1):2–14. [Google Scholar]
- Shin J., Taylor M.S., Seo M.-G. Resources for change: the relationships of organizational inducements and psychological resilience to employees’ attitudes and behaviors toward organizational change. Acad. Manag. J. 2012;55(3):727–748. [Google Scholar]
- Sigala M. Tourism and COVID-19: impacts and implications for advancing and resetting industry and research. J. Bus. Res. 2020;117:312–321. doi: 10.1016/j.jbusres.2020.06.015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sinclair S., Kondejewski J., Raffin-Bouchal S., King-Shier K.M., Singh P. Can self- compassion promote healthcare provider well-being and compassionate care to others? Results of a systematic review. Appl. Psychol.: Health Well-Being. 2017;9(2):168–206. doi: 10.1111/aphw.12086. [DOI] [PubMed] [Google Scholar]
- Smith J.L. Self-compassion and resilience in senior living residents. Sr. Hous. Care J. 2015;23(1):17–31. [Google Scholar]
- Song S., Yang X., Yang H., Zhou P., Ma H., Teng C., Chen H., Ou H., Li J., Mathews C.A., Nutley S., Liu N., Zhang X., Zhang N. Psychological resilience as a protective factor for depression and anxiety among the public during the outbreak of COVID-19. Front. Psychol. 2021;11 doi: 10.3389/fpsyg.2020.618509. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sönmez S., Apostolopoulos Y., Lemke M.K., Hsieh Y.C.J. Understanding the effects of COVID-19 on the health and safety of immigrant hospitality workers in the United States. Tour. Manag. Perspect. 2020;35 doi: 10.1016/j.tmp.2020.100717. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Su D.N., Tra D.L., Huynh H.M.T., Nguyen H.H.T., O’Mahony B. Enhancing resilience in the covid-19 crisis: lessons from human resource management practices in Vietnam. Curr. Issues Tour. 2021 doi: 10.1080/13683500.2020/1863930. [DOI] [Google Scholar]
- Teng Y.M., Wu K.S., Xu D. Vol. 9. 2021. The Association Between Fear of Coronavirus Disease 2019, Mental Health, and Turnover Intention Among Quarantine Hotel Employees in China. (Frontiers in Public Health). [DOI] [PMC free article] [PubMed] [Google Scholar]
- Trompetter H.R., de Kleine E., Bohlmeijer E.T. Why does positive mental health buffer against psychopathology? An exploratory study on self-compassion as a resilience mechanism and adaptive emotion regulation strategy. Cogn. Ther. Res. 2017;41(3):459–468. doi: 10.1007/s10608-016-9774-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Warren R., Smeets E., Neff K. Self-criticism and self-compassion: risk and resilience: Being compassionate to oneself is associated with emotional resilience and psychological well-being. Curr. Psych. 2016;15(12):18–28. [Google Scholar]
- Wingo A.P., Wrenn G., Pelletier T., Gutman A.R., Bradley B., Ressler K.J. Moderating effects of resilience on depression in individuals with a history of childhood abuse or trauma exposure. J. Affect. Disord. 2010;126(3):411–414. doi: 10.1016/j.jad.2010.04.009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wise S.L., Kong X. Response time effort: a new measure of examinee motivation in computer-based tests. Appl. Meas. Educ. 2005;18(2):163–183. doi: 10.1207/s15324818ame1802_2. [DOI] [Google Scholar]
- Worline M.C., Dutton J.E. Berrett-Koehler; Oakland, CA: 2017. Awakening Compassion at Work: The Quiet Power That Elevates People and Organizations. [Google Scholar]
- Yan J., Kim S., Zhang S.X., Foo M., Der, Alvarez-Risco A., Del-Aguila-Arcentales S., Yáñez J.A. Hospitality workers’ COVID-19 risk perception and depression: a contingent model based on transactional theory of stress model. Int. J. Hosp. Manag. 2021;95(April) doi: 10.1016/j.ijhm.2021.102935. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
The data that has been used is confidential.