Abstract
Background
The aim of this study was to evaluate the use of patient reported experience measures (PREMs) in humeral shaft fractures managed with or without surgery against patient reported outcome measures (PROMs).
Methods
Adult patients treated for a humeral shaft fracture between June 2015 and August 2017 were included in non-surgery and surgery (early and late surgery) groups. The PREM questionnaire was based on patient and clinician feedback obtained during focus groups and was posted to patients. PROMs included the short form-12 (SF-12) and visual analogue scale (VAS) for pain, stiffness, function and satisfaction.
Results
Eighty-one patients responded, 54 patients were treated in a brace and 27 with surgery (13 early, 14 late). There was moderate positive correlation between PREM and VAS satisfaction and function and moderate negative correlation with VAS pain and stiffness. There was also moderate positive correlation between PREM and SF-12 mental and weak positive correlation with SF-12 physical. The late surgery group had poorer PREMs (expectations, p = 0.002 and friends & family test, p = 0.0001) and PROMs (VAS satisfaction, p = 0.005) compared to the early surgery group.
Conclusions
PREMs can be used in conjunction with PROMs to improve the patient's quality of care and as a means of identifying, at an early stage, those patients not doing well and to offer surgery.
Keywords: patient reported experience measure, PREM, PROM, non-surgical, surgical, humeral shaft fractures
Introduction
Patient experience and satisfaction is an important and commonly used indicator for measuring quality in health care. 1 It affects clinical outcomes and facilitates the timely, efficient, and patient-centred delivery of good health care. 2 In the literature much emphasis has been given to PROMs which ascertain perceptions of the patient's health status, perceived impairment, disability, and health-related quality of life. 3 A tool scarcely used in orthopaedics is PREMs. These gather information on patient's views of their experience whilst receiving care and are an indicator of the quality of patient care although they do not measure it directly. 4 Patient experience surveys elicit feedback on the process of care rather than its effects, focusing on issues such as communication with health professionals, information provision, and involvement in decisions, physical comfort, emotional support, and care transitions. 5 The British Medical Journal states “PREMs and PROMs are set to become the new currency for comparative performance assessment”. 5
Patient experience during the management of any fracture in plaster, a sling or with surgery can be distressing and lead to complications.6,7 PREMs may lead to changes that improve the delivery of services in the treatment of fractures. 8 A literature review performed found multiple papers reporting PROMs in patients sustaining a neck of femur fracture,9–13 but a scarcity of reporting PREMs in patients sustaining upper limb fractures14,15 or vertebral/hip fractures. 8 To date, there are no published studies analysing PREMs in patients sustaining humeral shaft fractures.
The aim of this study was to present our experience with the use of PREM questionnaires in the management of humeral shaft fractures and compare the experiences and satisfaction between patients treated with or without surgery (in plaster or a brace) against PROMs.
Methods
The study received approval from the institution's audit department (number 9554e). Patients over the age of 16 sustaining a fracture to the humeral shaft and treated conservatively (with a brace) or with surgery, between June 2015 and August 2017, were included. All but 3 patient's fractures had radiologically healed at their latest follow up. Fracture healing was determined by radiographs when bone continuity in 3 cortices was detected between the main fracture fragments in both planes. 16 Those who failed to respond, refused consent for inclusion in the study, were under the age of 16, were unable to provide informed consent and, finally, those who were not fluent in English were excluded. Patients were divided into non-surgical and surgical groups.
Patients were sent the following questionnaires by post:
Figure 1.
Patient reported experience measure (PREM) questionnaire posted to patients sustaining a humerus shaft fracture.
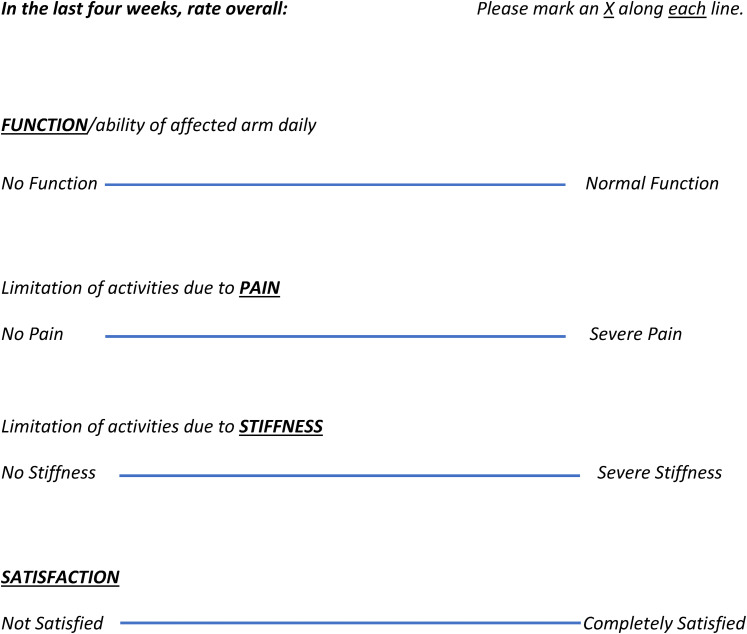
Figure 2.
VAS score: patients asked to mark an X along each line of the corresponding VAS category (function, pain, stiffness, and satisfaction) VAS, visual analogue scale.
A second letter was re-posted if there was no reply, followed by a structured telephone interview if that also failed. 19 The PREM questionnaire was produced using an informal composite qualitative method that combined patient opinion (gathered at focus group meetings), the opinions of experienced clinicians and a validated patient experience questionnaire already in use. 20 This feedback provided perspectives on the salient points of a patient's experience during treatment for their humeral shaft fracture. The questionnaire is a combination of the patient experience questionnaire (PEQ) and the patient satisfaction questionnaire (PSQ) (Figure 1). The PEQ relays information about the presence of stiffness, residual deformity (and acceptance of it), the return of function (to pre-injury level), and any occurring complications. The PSQ relays information about the quality of treatment received, the willingness to undergo the same treatment, expectations met, and friends and family test (FFT). These questionnaires were first applied to six patients to ensure that the wording, comprehension and volume of questions were fit for purpose. The refined PEQ and PSQ were then combined to form the patient experience and satisfaction questionnaire (PESQ) score (Figure 3). All categories except for one had a binary answer (yes/no). A point was given for each good outcome. No point was given for a bad outcome. The remaining question regarding the overall experience received gave 1 to 5 points giving a total maximum PESQ score of 12 with a minimum score of 1. Those questions with no response were given the lowest score. Each patient accrued a final PESQ score.
Figure 3.
PREM (PESQ 1–12) scoreboard: scores from PEQ 1–4 and PSQ 1–4 are added to form the PREM (PESQ) score for each patient.
PROMs collected included patient's VAS 18 scores (regarding overall function, limitation of activity due to pain, limitation of activity due to stiffness and overall satisfaction) (Figure 2) and the SF-12. 17 The SF-12 is a validated health questionnaire 21 that gives an indication of the patient's mental and physical functioning and overall health-related quality of life. It is divided into a mental component score (MCS) and a physical component score (PCS).
Additional data collected included patient's free text answers on the recovery process essential features, and treatment modality received. The questions in this section offered patients the opportunity to voice their opinion and in doing so, provided qualitative data regarding their treatment (See Appendices 1–3).
All statistical calculations were done with the use of SPSS for Windows 2000 (version 11.0; SPSS, Chicago, Illinois). Statistical methods included the t-test and two-tailed test. A p < 0.05 was considered to be the threshold for significance. The SF-12 scores were calculated using an online score calculator. 22
Pearson's correlation coefficient (r) was used to evaluate the correlation between the PESQ and PROMs (VAS for function, pain, stiffness, satisfaction and SF-12). The strength of negative correlation was classified as strong (r = −1.0 to −0.7), moderate (r = −0.7 to −0.3) and weak (r = −0.3 to −0.1). The strength of positive correlation was classified as strong (r = 0.7 to 1.0), moderate (r = 0.3 to 0.7) and weak (r = 0.1 to 0.3).
Results
The study achieved a 39% return rate, with 81 of the 208 patients responding to the questionnaire. After excluding 40 patients who had died, 82 were not contactable (by letter or phone), 3 denied participation and 2 were unable to consent. The mean age of patients at the time of treatment was 66 (range, 22–98) years with a 1:1.7 ratio of male to female (30:51) (Table 1). 54 patients were treated without surgery and 27 with surgery. Of the 27 who had surgery, 13 had their operation within six weeks (early surgery group). The mean time to surgery for this group was 1.5 (range, 0–4) weeks. Indications for early surgery included unstable fracture configurations pragmatically assessed by surgeons to require early surgery and open fractures. 14 of the 27 surgical patients had failed initial conservative management in a brace and underwent surgery due to non-union (late surgery group). The mean time to surgery for this group was 19.4 (range, 11–37) weeks.
Table 1.
Comparison of patient characteristics based on treatment modality.
| Total (N = 81) | Non-surgery group (N = 54) | Surgery group (N = 27) | Late surgery group (N = 14) | |
|---|---|---|---|---|
| Mean age at the time of treatment Years (range) |
66 (22–98) | 67 (25–98) | 64 (22–84) | 69 (29–83) |
| Male/Female (ratio) |
30 / 51 (1:1.7) |
20 / 34 (1:1.7) |
10 / 17 (1:1.7) |
4 / 10 (1:2.5) |
N, Number.
There was moderate positive correlation between PREM (PESQ 1–12) score and VAS satisfaction (r = 0.558, p = 0.0001) and VAS function (r = 0.423, p = 0.0001) (Table 2).
Table 2.
Correlations between PREM (PESQ) and PROM scores.
| PREM (PESQ 1–12) | ||
|---|---|---|
| VAS Pain | Pearson Correlation | −0.443 a |
| Sig. (2-tailed) | 0.0001 | |
| N | 73 | |
| VAS Stiffness | Pearson Correlation | −0.389 a |
| Sig. (2-tailed) | 0.001 | |
| N | 75 | |
| VAS Function | Pearson Correlation | 0.423 a |
| Sig. (2-tailed) | 0.0001 | |
| N | 74 | |
| VAS Satisfaction | Pearson Correlation | 0.558 a |
| Sig. (2-tailed) | 0.0001 | |
| N | 75 | |
| SF-12 (PCS) | Pearson Correlation | 0.169 |
| Sig. (2-tailed) | 0.131 | |
| N | 81 | |
| SF-12 (MCS) | Pearson Correlation | 0.320 a |
| Sig. (2-tailed) | 0.004 | |
| N | 81 |
Correlation is significant at the 0.01 level (2-tailed).
N, Number; PREM, patient reported experience measure; PESQ, patient experience and satisfaction questionnaire; PROM, patient reported outcome measure; VAS, visual analogue scale; SF-12, Short form-12; PCS, physical component score; MCS, mental component score .
There was moderate negative correlation between PREM score and VAS pain (r = -0.443, p = 0.0001) and VAS stiffness (r = -0.389, p = 0.001) i.e., patients who had more pain and stiffness had poorer experience (PREM) scores.
In addition, there was moderate positive corelation between PREM (PESQ 1–12) score and SF-12 MCS (r = 0.320, p = 0.004) and weak positive correlation for SF-12 PCS (r = 0.169, p = 0.131).
The non-surgery group achieved less favourable results in PROM scores when compared to the surgery group in the SF-12 PCS (p = 0.02) whereas, the surgery group sustained more complications (p = 0.001) and was less likely to recommend the same treatment (p = 0.01) (Tables 3 & 4). It is worthwhile noting that although no significant differences were found between groups for the rest of the categories, the surgery group had a better experience (p = 0.21) and expectation score (p = 0.17) than the non-surgery group despite not gaining pre-injury function (p = 0.83). They also developed less residual deformity (p = 0.63) and stiffness (p = 0.07) than the non-surgery group yet were less inclined to accept this deformity (p = 0.57). Most complications occurred in the surgical group (p = 0.001) with 14 of the 17 patients belonging to the late surgery group (p = 0.13) (Tables 3, 5 and 6). If we exclude non-union as a complication, the late surgery group had very few complications (2 out of 14, 14%) when compared to the other two groups (13% and 23% for non-surgery and early surgery respectively).
Table 3.
Comparing PREM results in Non-surgery and surgery groups.
| Outcome | Total (N = 81) N (%) |
Non-surgery group (N = 54) N (%) |
Surgery group (N = 27) N (%) |
p-value* |
|---|---|---|---|---|
| PEQ Stiffness | ||||
| Developed | 27 (33.3%) | 18 (33.3%) | 9 (33.3%) | 0.07 |
| Did not develop | 46 (56.8%) | 29 (53.7%) | 17 (63%) | |
| No response | 8 (9.9%) | 7 (13%) | 1 (3.7%) | |
| PEQ Residual deformity | ||||
| Developed | 45 (55.5%) | 33 (61.1%) | 12 (44.4%) | 0.63 |
| Not developed | 34 (42%) | 19 (35.2%) | 15 (55.6%) | |
| No response | 2 (2.5%) | 2 (3.7%) | ||
| Developed and accepted | 22/45 (48.9%) | 17/33 (51.5%) | 5/12 (41.7%) | |
| Developed but not accepted | 23/45 (51.1%) | 16/33 (48.5%) | 7/12 (58.3%) | 0.57 |
| PEQ Preinjury function | ||||
| Gained | 36 (44.4%) | 26 (48.1%) | 10 (37%) | |
| Not gained | 43 (53.1%) | 27 (50%) | 16 (59.3%) | 0.83 |
| No response | 2 (2.5%) | 1 (1.9%) | 1 (3.7%) | |
| PEQ Complications | ||||
| Developed | 24 (29.6%) | 7 (13%) | 17 (63%) | 0.001 |
| Did not develop | 57 (70.4%) | 47 (87%) | 10 (37%) | |
| PSQ Experience | 0.21 | |||
| Good/Excellent | 73 (90.1%) | 47 (87%) | 26 (96.3%) | |
| Neutral | 2 (2.5%) | 2 (3.7%) | - | |
| Poor/Very poor | 6 (7.4%) | 5 (9.3%) | 1 (3.7%) | |
| PSQ Recommend same treatment | ||||
| Would | 70 (86.4%) | 49 (90.7%) | 21 (77.8%) | 0.01 |
| Would not | 9 (11.1%) | 4 (7.4%) | 5 (18.5%) | |
| No response | 2 (2.5%) | 1 (1.9%) | 1 (3.7%) | |
| PSQ Expectations met | ||||
| Yes | 69 (85.2%) | 44 (81.5%) | 25 (92.6%) | 0.17 |
| No | 9 (11.1%) | 7 (13%) | 2 (7.4%) | |
| No response | 3 (3.7%) | 3 (5.5%) | - | |
| PSQ F&F test | ||||
| Yes | 70 (86.4%) | 48 (88.9%) | 22 (81.5%) | 0.31 |
| No | 10 (12.3%) | 6 (11.1%) | 4 (14.8%) | |
| No response | 1 (1.3%) | - | 1 (3.7%) |
* Group means were compared with an independent-samples t-test.
N, Number; PREM, patient reported experience measure; PEQ = patient experience questionnaire; PSQ, patient satisfaction questionnaire; F&F, friends & family.
Table 4.
Comparing PROM results in Non-surgery and surgery groups.
| Outcome | Total (N = 81) mean (SD) |
Non-surgery group (N = 54) mean (SD) |
Surgery group (N = 27) mean (SD) |
p-value* |
|---|---|---|---|---|
| VAS Pain (8 not responded) | 1.93 (2.68) | 1.54 (2.41) | 2.59 (3.03) | 0.15 |
| VAS Stiffness (6 not responded) | 2.27 (2.92) | 1.94 (2.68) | 2.85 (3.27) | 0.15 |
| VAS Function (6 not responded) | 7.62 (2.45) | 7.49 (2.59) | 7.85 (2.21) | 0.21 |
| VAS Satisfaction (6 not responded) |
7.85 (2.71) | 7.69 (2.86) | 8.15 (2.43) | 0.61 |
| SF-12 PCS | 42.11 (11.86) | 40.89 (12.73) | 44.55 (9.63) | 0.02 |
| SF-12 MCS | 48.97 (11.69) | 47.98 (12.41) | 50.95 (10.04) | 0.17 |
* Group means were compared with an independent-samples t-test.
N, number; SD, standard deviation; PROM, patient reported outcome measure; VAS, visual analogue scale; SF-12, Short form-12; PCS, physical component score; MCS, mental component score.
Table 5.
Comparing PREM results in early and late surgery groups.
| Outcome | Early surgery (N = 13) N (%) |
Late surgery (N = 14) N (%) |
p-value* |
|---|---|---|---|
| PEQ Stiffness | |||
| Developed | 4 (30.8%) | 5 (35.7%) | |
| Did not develop | 8 (61.5%) | 9 (64.3%) | 0.23 |
| No response | 1 (7.7%) | - | |
| PEQ Residual deformity | |||
| Developed | 7 (53.8%) | 5 (35.7%) | |
| Not developed | 6 (46.2%) | 9 (64.3%) | 0.64 |
| Developed and accepted | 3/7 (42.9%) | 2/5 (40%) | |
| Developed but not accepted | 4/7 (57.1%) | 3/5 (60%) | 0.53 |
| PEQ Preinjury function | |||
| Gained | 4 (30.8%) | 6 (42.9%) | |
| Not gained | 8 (61.5%) | 8 (57.1%) | |
| No response | 1 (7.7%) | - | 0.34 |
| PEQ Complications | |||
| Developed | 3 (23.1%) | 14 (100%)** | |
| Did not develop | 10 (76.9%) | - | 0.13 |
| PSQ Experience | |||
| Good/Excellent | 13 (100%) | 13 (92.9%) | 0.50 |
| Neutral | - | - | |
| Poor/Very poor | - | 1 (7.1%) | |
| PSQ Recommend treatment | |||
| Would | 10 (76.9%) | 11 (78.6%) | 0.68 |
| Would not | 2 (15.4%) | 3 (21.4%) | |
| No response | 1 (7.7%) | - | |
| PSQ Expectations met | |||
| Yes | 13 (100%) | 12 (85.7%) | 0.002 |
| No | - | 2 (14.3%) | |
| No response | - | - | |
| PSQ F&F test | |||
| Yes | 13 (100%) | 9 (64.3%) | 0.0001 |
| No | - | 4 (28.6%) | |
| No response | - | 1 (7.1%) |
* Group means were compared with an independent-samples t-test.
* * 100% due to all fractures resulting in Non-union.
N, number; PREM, patient reported experience measure; PEQ, patient experience questionnaire; PSQ, patient satisfaction questionnaire; F&F, friends & family.
Table 6.
Complications sustained in each treatment group.
| Non-surgery group (N = 54) |
Early surgery group (N = 13) |
Late surgery group (N = 14) |
|
|---|---|---|---|
| Number of patients sustaining a complication (%) | 7 (13%) | 3 (23%) | 14 (100%) |
| Complications developed (outcome) | 3 Non-unions 1 Unfit 1 Asymptomatic 1 Declined surgery 1 Radial nerve palsy (Not recovered, declined tendon transfer) 2 Skin issues (Settled) 1 Arm swelling (Settled) |
3 Radial nerve palsies 2 Preoperative 1 Postoperative (All fully recovered) |
14 Non-unions (All united following surgery) 1 Postoperative Radial nerve palsy (Fully recovered) 1 Postoperative CRPS (Fully recovered) |
N, number; CRPS, Complex regional pain syndrome.
The late surgery cohort had poorer outcomes for PREM and PROM scores (Tables 5 and 7, respectively) including expectations not being met (p = 0.002), F&F test (p = 0.0001), VAS satisfaction (p = 0.005). However, no significant differences were found between groups for the rest of the categories.
Table 7.
Comparing PROM results in early surgery and late surgery group.
| Outcome | Early surgery (N = 13) mean (SD) |
Late surgery (N = 14) mean (SD) |
p-value* |
|---|---|---|---|
| VAS Pain (8 not responded) |
2.62 (3.25) | 2.57 (2.93) | 0.59 |
| VAS Stiffness (6 not responded) |
2.85 (3.31) | 2.86 (3.35) | 0.84 |
| VAS Function (6 not responded) |
8.31 (1.60) | 7.43 (2.65) | 0.52 |
| VAS Satisfaction (6 not responded) |
9.08 (1.12) | 7.29 (3.00) | 0.005 |
| SF-12 PCS | 45.13 (10.51) | 44.02 (9.11) | 0.94 |
| SF-12 MCS | 46.37 (10.04) | 55.21 (8.25) | 0.35 |
*Group means were compared with an independent-samples t-test.
N, number; SD, standard deviation; PROM, patient reported outcome measure; VAS, visual analogue scale; SF-12, Short form 12; PCS: physical component score; MCS, mental component score.
Analysis of the qualitative data from the free text question exercises (Appendices 1–3) established four clear themes, including treatment, process, service quality and end result. Each theme was further divided into subthemes according to comments made. These questions were intended to enable the patient to voice their opinion on what they considered were the essential features of their recovery, in a way that a PREM or PROM does not allow. When patients were asked what was important regarding their recovery, the most quoted comments included regaining function, independence and use of physiotherapy (Appendix 1). When asked what would be important for a health care professional to ask - regarding how well they recovered; return of function, range of movement and pain management were highlighted (Appendix 2). Finally, when asked to write freehand, some patients stated they “should have had the operation sooner” or “should have had surgery” (Appendix 3). This has identified a wide range of lived experiences of people who have suffered a humeral shaft fracture. The data could be utilised to improve patients journey in the long term.
Discussion
This study attempts to apply and compare a patient experience and satisfaction questionnaire with PROMs, to a cohort of patients with a humeral shaft fracture treated with or without surgery. We identified a positive correlation between PREM (PESQ) score and VAS satisfaction, VAS function and SF-12, and a negative correlation with VAS pain and VAS stiffness. Patients in the surgical cohort had similar PREM and VAS scores to the non-surgical group. However, patients in the late surgery cohort had poorer PREM and PROM scores than those in the early surgery group. This could be due to delay in treatment and incomplete recovery of function. It needs to be further explored whether operating earlier would improve PREM and PROM scores in this cohort. Further research is needed to identify humeral fractures at risk of non-union so early surgery could be offered to improve the patient outcome.
We also found contradicting results, with the surgery group having a better experience and expectation score than the non-surgery group despite not gaining more pre-injury function than the non-surgery group. They also developed less residual deformity and stiffness than the non-surgery group yet were less inclined to accept this deformity (p = 0.57). This may be due to higher expectations patients’ undergoing surgery have and shows the complexity of treating these fractures.
This study highlights that PREMs can be utilised in conjunction with PROMs to improve the patient's quality of care. By enabling patients voice their experiences and opinions, it can also be used as a surrogate to identify those patients who are not doing well early, to offer prompt surgery. In that way, patients are offered the chance to take an active part in their treatment and feel valued.
The National Institute for Health and Care Excellence (NICE) has published a quality standard that focuses on the patient experience 23 stating that “people using NHS services should be supported in shared decision making”. Patient's experiences have been investigated and utilised to identify disease processes that attenuate patient experience, 8 assess the relationship with validated PROMs 15 and validate predictors of health outcomes. 14
A PREM questionnaire for major trauma patients was created and validated by Bobrovitz et al. 1 They suggested that variation in patient and family experiences could be used as a tool to establish quality of care benchmarks, flag potential problem areas or successes, and to follow trends over time.
Tsehaie et al. 24 investigated patients undergoing trapeziometacarpal arthroplasty and found significant positive associations when comparing PREMs at 3 months with PROMs received at 12 months. Their PREMs predicted the outcome early where PROMs became available later during the study. The authors of this study recognised that their PREM questionnaire was not validated, may have omitted important aspects of treatment context, and may reach a ceiling effect.
Chao et al. 8 applied a PREM questionnaire to patients sustaining hip or vertebral fractures and assessed pain severity related to the fractures, the ability to take care of everyday needs, and the fullness of their daily activity using a 5-point Likert scale. These self-reported outcomes were validated against the EQ-5D-5L questionnaire. 11 They identified that chronic kidney disease attenuated the probability of PREM improvement in fracture patients. Limitations of this study include use of selected parts of the EQ-5D questionnaire which measures generic quality of life and cannot capture the entire spectrum of patient experiences. Also, the lack of recording of patients using NSAIDs may have been responsible for the relatively milder pain severity observed.
Jayakumar and colleagues 14 studied the association between engagement and experience in patients with upper limb fractures in the United Kingdom. PREMs used included a numerical rating scale for satisfaction with care providers (NRS-C) and satisfaction with services (NRS-S). The study concluded that patient engagement is positively correlated with health outcomes and patient experience. The different ways of obtaining data by telephone, online or in person, may however have introduced bias in the reported results. The same author 15 studied the relationship between a range of PROMs and the two PREMs mentioned above in patients with upper limb fractures. The study concluded that increasing alignment of PROMs and PREMs over the course of recovery after an upper-extremity fracture suggests that restored physical function may improve perceptions of satisfaction with care providers and hospital services over time. They advise that providers should pay close attention to the relationship between PROMs and PREMs if they are to be used as quality metrics in reimbursement programs.
Of the 81 patients in this study, 54 were managed conservatively, 13 had early surgery, and 14 had late surgery (due to non-union). All patients undergoing surgery went on to unite. The late surgery cohort had poorer outcomes for PREM and PROM scores which is in line with the existing literature.16,25–27 Most authors define delayed union as no radiographic signs of osseous union of a fracture of the humeral shaft or proximal humerus 4 months after injury and non-union as no radiographic signs of osseous union 6 months after injury. 28 Despite this, the recommended period before functional bracing is discontinued in favour of surgery varies widely in the literature. Toivanen et al. 29 operated on fractures that did not show clinical and radiological signs of consolidation at 6 weeks. The average time to delayed fixation after the injury for other studies include 28 weeks (range, 10–55 weeks), 30 6 months, 16 8 months 31 and 8.3 months (range 3–12 months). 32 Papasoulis et al. 33 performed a systematic review of 15 English language studies on outcomes of diaphyseal humeral fractures treated with a functional brace and showed a mean time to union of 10.7 weeks. These results suggest that patients with fractures that have not healed by 10–12 weeks, should undergo consultation, and offered the choice of surgery. Alternatively, it is recommended to maintain a high index of suspicion for non-union in humeral shaft fractures that demonstrate no interval healing on consecutive radiographs taken 6 to 8 weeks apart. 28 The mean time to surgery for the late surgery group in this study was 19.4 weeks (range, 11–37).
The increasing incidence of surgical management for humeral shaft fractures may represent a public health burden given the historical success of non-operative management. 34 Therefore, early identification of patients likely to develop non-union and offering them prompt surgery would not only improve their experience but also provides an opportunity to keep the financial burden of these fractures in check.
The limitations of this study include its retrospective nature and lack of complete recruitment, both of which introduce bias into the results. The cohort's size is relatively small (thus reducing the power of our analysis), and data was collected at a single time-point. Generic outcome measures like VAS and SF-12 were used to study patient outcome compared to disease-specific outcome measures. The generalizability of the findings may be challenged as it was performed at a single institution, (a level 2 trauma centre at a university teaching hospital in the UK). The different ways of obtaining data (i.e. postal or telephone) may have given rise to interviewer and responder bias but this approach is common, and other variations of this method have proven to be acceptable. 35 Also, the number of proxy responses were low overall and actively discouraged.
Conclusion
This study concludes that there is a positive correlation between patient experience and better function and outcome after humeral shaft fractures and a negative correlation with ongoing pain and stiffness. Patients in the surgical cohort had overall similar PREM and VAS scores to the non-surgical group but developed more complications and were less likely to recommend the same treatment. However, patients in the late surgery cohort had poorer PREM and PROM scores than the early surgery group. They were less satisfied and would not recommend the care they received to their family and friends due to delays in definitive treatment.
Further randomised control trials are needed to identify fractures at risk of non-union so that if early surgery is proven to be beneficial it can be offered to improve the patient experience.
This study shows promising results in the use of PREMs for humeral shaft fractures in conjunction with PROMs to improve the patient's quality of care.
They can also be utilised as a surrogate to identify those patients who are not doing well early, to offer prompt surgery.
Supplemental Material
Supplemental material, sj-docx-1-sel-10.1177_17585732211050224 for Use of patient reported experience measure and patient reported outcome measures to evaluate differences in surgical or non-surgical management of humeral shaft fractures by Lambros Athanatos, Darren P Sandean, Maitravaarun Burgula, Bethan Lee, Radhakant Pandey, and Harvinder P Singh in Shoulder & Elbow
Footnotes
Authors' Note: MaitraVaarun Burgula now works in East Suffolk and North Essex NHS Foundation Trust, Ipswich, England, UK. Darren P Sandean now works in Nottingham University Hospitals NHS Trust, Nottingham, England, UK. Bethan E Lee now works in NHS Highland, Inverness, Scotland, UK.
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding: The author(s) received no financial support for the research, authorship and/or publication of this article.
ORCID iD: Lambros Athanatos https://orcid.org/0000-0003-4514-6575
Supplemental Material: Supplemental material for this article is available online.
References
- 1.Bobrovitz N, Santana MJ, Kline T, et al. Multicenter validation of the quality of trauma care patient-reported experience measure (QTAC-PREM). J Trauma Acute Care Surg 2016; 80: 111–118. [DOI] [PubMed] [Google Scholar]
- 2.Jones EL, Wainwright TW, Foster JD, et al. A systematic review of patient reported outcomes and patient experience in enhanced recovery after orthopaedic surgery. Ann R Coll Surg Engl 2014; 96: 89–94. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Bailey A. A guide to patient reported measures– theory, landscape and uses. Monmouth Partners. 2016; 1–6. https://silo.tips/download/a-guide-to-patient-reported-measures-theory-landscape-and-uses(accessed 16 October 2021). [Google Scholar]
- 4.Kingsley C, Patel S. Patient-reported outcome measures and patient-reported experience measures. BJA Educ 2017; 17: 137–144. [Google Scholar]
- 5.Coulter A. Measuring what matters to patients. Br Med J 2017; 356: 1–2. [DOI] [PubMed] [Google Scholar]
- 6.Gagnier JJ, Morgenstern H, Kellam P. A retrospective cohort study of adverse events in patients undergoing orthopaedic surgery. Patient Saf Surg 2017; 11: 1–14. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Bakody E. Orthopaedic plaster casting: nurse and patient education. Nurs Stand 2009; 23: 49–56. [DOI] [PubMed] [Google Scholar]
- 8.Ter CC, Sen YR, Hung LW, et al. Chronic kidney disease predicts a lower probability of improvement in patient-reported experience measures among patients with fractures: a prospective multicenter cohort study. Arch Osteoporos 2018; 13: 1–10. [DOI] [PubMed] [Google Scholar]
- 9.Griffin XL, Parsons N, Achten J, et al. Recovery of health-related quality of life in a United Kingdom hip fracture population: the warwick hip trauma evaluation - A prospective cohort study. Bone Jt J 2015; 97–B: 372–382. [DOI] [PubMed] [Google Scholar]
- 10.Peeters CMM, Visser E, Van De Ree CLP, et al. Quality of life after hip fracture in the elderly: a systematic literature review. Injury 2016; 47: 1369–1382. [DOI] [PubMed] [Google Scholar]
- 11.Haywood KL, Brett J, Tutton E, et al. Patient-reported outcome measures in older people with hip fracture: a systematic review of quality and acceptability. Qual Life Res 2017; 26: 799–812. [DOI] [PubMed] [Google Scholar]
- 12.Orwig DL, Hochberg M, Yu-Yahiro J, et al. Delivery and outcomes of a yearlong home exercise program after hip fracture: a randomized controlled trial. Arch Intern Med 2011; 171: 323–331. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Lagergren J, Möller M, Rogmark C. Displaced femoral neck fractures in patients 60–69 years old – treatment and patient reported outcomes in a register cohort. Injury 2020; 51: 2652–2657. [DOI] [PubMed] [Google Scholar]
- 14.Jayakumar P, Teunis T, Vranceanu AM, et al. The impact of a patient's Engagement in their health on the magnitude of limitations and experience following upper limb fractures. Bone Jt J 2020; 102 B: 42–47. [DOI] [PubMed] [Google Scholar]
- 15.Jayakumar P, Teunis T, Vranceanu A-M, et al. Relationship between magnitude of limitations and patient experience during recovery from upper-extremity fracture. JBJS Open Access 2019; 4: e0002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Matsunaga FT, Tamaoki MJS, Matsumoto MH, et al. Minimally invasive osteosynthesis with a bridge plate versus a functional brace for humeral shaft fractures: a randomized controlled trial. J Bone Jt Surg Am 2017; 99: 583–592. [DOI] [PubMed] [Google Scholar]
- 17.Ware JE, Kosinski M, Keller SD, et al. A 12-item short-form health survey of scales and preliminary construction tests of reliability and validity. Med Care 1996; 34: 220–233. [DOI] [PubMed] [Google Scholar]
- 18.Boonstra AM, Schiphorst Preuper HR, Reneman MF, et al. Reliability and validity of the visual analogue scale for disability in patients with chronic musculoskeletal pain. Int J Rehabil Res 2008; 31: 165–169. [DOI] [PubMed] [Google Scholar]
- 19.Dawson J, Rogers K, Fitzpatrick R, et al. The Oxford shoulder score revisited. Arch Orthop Trauma Surg 2009; 129: 119–123. [DOI] [PubMed] [Google Scholar]
- 20.Jenkinson C, Coulter A, Bruster S. The picker patient experience questionnaire: development and validation using data from in-patient surveys in five countries. Int J Qual Heal Care 2002; 14: 353–358. [DOI] [PubMed] [Google Scholar]
- 21.Gandek B, Ware JE, Aaronson NK, et al. Cross-validation of item selection and scoring for the SF-12 health survey in nine countries: results from the IQOLA project. J Clin Epidemiol 1998; 51: 1171–1178. [DOI] [PubMed] [Google Scholar]
- 22.Free online Short Form-12 (SF-12) score calculator. OrthoToolKit. http://orthotoolkit.com/sf-12/(accessed 16 October 2018).
- 23.National Clinical Guideline Centre. Patient experience in adult NHS services : improving the experience of care for people using adult NHS services. [PubMed]
- 24.Tsehaie J, van der Oest MJW, Poelstra R, et al. Positive experience with treatment is associated with better surgical outcome in trapeziometacarpal osteoarthritis. J Hand Surg Eur 2019; 44: 714–721. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Rämö L, Sumrein BO, Lepola V, et al. Effect of surgery vs functional bracing on functional outcome among patients with closed displaced humeral shaft fractures: the FISH randomized clinical trial. J Am Med Assoc 2020; 323: 1792–1801. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Harkin FE, Large RJ. Humeral shaft fractures: union outcomes in a large cohort. J Shoulder Elbow Surg 2017; 26: 1881–1888. [DOI] [PubMed] [Google Scholar]
- 27.Broadbent MR, Will E, McQueen MM. Prediction of outcome after humeral diaphyseal fracture. Injury 2010; 41: 572–577. [DOI] [PubMed] [Google Scholar]
- 28.Cadet ER, Yin B, Schulz B, et al. Proximal humerus and humeral shaft nonunions. J Am Acad Orthop Surg 2013; 21: 538–547. [DOI] [PubMed] [Google Scholar]
- 29.Toivanen JAK, Nieminen J, Laine HJ, et al. Functional treatment of closed humeral shaft fractures. Int Orthop 2005; 29: 10–13. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Rutgers M, Ring D. Treatment of diaphyseal fractures of the humerus using a functional brace. J Orthop Trauma 2006; 20: 597–601. [DOI] [PubMed] [Google Scholar]
- 31.Driesman AS, Fisher N, Karia R, et al. Fracture site mobility at 6 weeks after humeral shaft fracture predicts nonunion without surgery. J Orthop Trauma 2017; 31: 657–662. [DOI] [PubMed] [Google Scholar]
- 32.Ali E, Griffiths D, Obi N, et al. Nonoperative treatment of humeral shaft fractures revisited. J Shoulder Elbow Surg 2015; 24: 210–214. [DOI] [PubMed] [Google Scholar]
- 33.Papasoulis E, Drosos GI, Ververidis AN, et al. Functional bracing of humeral shaft fractures. A review of clinical studies. Injury 2010; 41: e21–e27. [DOI] [PubMed] [Google Scholar]
- 34.Schoch BS, Padegimas EM, Maltenfort M, et al. Humeral shaft fractures: national trends in management. J Orthop Traumatol 2017; 18: 259–263. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Bot AGJ, Becker SJE, Mol MF, et al. Validation of phone administration of short-form disability and psychology questionnaires. J Hand Surg Am 2013; 38: 1383–1387. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Supplemental material, sj-docx-1-sel-10.1177_17585732211050224 for Use of patient reported experience measure and patient reported outcome measures to evaluate differences in surgical or non-surgical management of humeral shaft fractures by Lambros Athanatos, Darren P Sandean, Maitravaarun Burgula, Bethan Lee, Radhakant Pandey, and Harvinder P Singh in Shoulder & Elbow