Abstract
Purpose
The aim of this systematic review was to evaluate the effectiveness of the socket shield technique (SST), an innovative surgical method introduced in 2010, for reducing buccal bone plate resorption.
Methods
The review was conducted following the PRISMA guidelines. Clinical studies conducted in humans and investigating the SST were searched on PubMed (MEDLINE), Embase, Web of Knowledge, and Google Scholar in November and December 2021. The implant survival rate, percentage of complications, and clinical parameters (marginal bone loss [MBL], pink esthetic score [PES], and buccal bone plate resorption [BBPR]) were analyzed using the collected data.
Results
The initial search resulted in 132 articles. After article screening, the full texts of 19 studies were read and 17 articles were finally included in the review. In total, 656 implants were installed with the SST. Nine of the 656 implants experienced failure, resulting in an implant survival rate of 98.6%. The percentage of complications was about 3.81%. The analysis of clinical parameters (MBL, PES, and BBPR), showed favorable results for the SST. The mean MBL in implants placed with the SST was 0.39±0.28 mm versus 1.00±0.55 mm in those placed without the SST. PES had a better outcome in the SST group, with an average of 12.08±1.18 versus 10.77±0.74. BBPR had more favorable results in implants placed with the SST (0.32±0.10 mm) than in implants placed with the standard technique (1.05±0.18 mm).
Conclusions
The SST could be considered beneficial for preserving the buccal bone plate. However, since only 7 of the included studies were long-term randomized controlled trials comparing the SST with the standard implant placement technique, the conclusions drawn from this systematic review should be interpreted with caution.
Trial Registration
PROSPERO Identifier: CRD42020180637
Keywords: Bone transplantation, Dental implants, Immediate dental implant loading, Oral surgery, Systematic review
INTRODUCTION
There is now a growing demand for implants placed immediately following extraction in the maxillary esthetic region. Implantology in the visible frontal region demands extreme precision due to patients’ high long-term requirements. Tooth loss results in physiological volume changes of the alveolar bone [1,2]. Alveolar bone resorption is more pronounced in the buccal plate than in the lingual plate [3]. During the 4-month interval following tooth extraction, the buccal bone dimension undergoes horizontal resorption that amounts to about 56%. The corresponding reduction of the lingual/palatal bone wall is 30% [4]. The marked alterations after tooth extraction appear to be attributable to the loss of the periodontal ligament and the subsequent trauma, in particular at the buccal bone plate. Alveolar bone resorption could compromise implant insertion, especially in esthetic areas such as the anterior maxilla. In order to resolve the negative impact of tooth loss, various techniques have been proposed, such as immediate implants, socket preservation with biomaterials [5,6], or alveolar ridge preservation with bioabsorbable membranes [7]. Immediate implant placement after tooth extraction is a well-known and successful treatment option with a comparable success rate to that of delayed implant techniques, and it reduces costs, the number of surgical procedures, and time to rehabilitation. The literature confirms that these techniques avoid ridge collapse, even if complete preservation of the bone crest is not documented. In 2010, Hurzeler et al. [8] proposed the socket shield technique (SST), which involves partial buccal root retention, in order to preserve the buccal bone plate, with an immediate implant placed palatal to the root fragment. They demonstrated the formation of cementum and osteointegration on implant surfaces placed in contact with intentionally retained roots. The surgical procedure of the SST (Figure 1) can be suggested for the stabilization of soft and hard tissues at the extraction site. The major indications for SST are maxillary anterior teeth in the esthetic areas that cannot be restored. SST can also be performed in the posterior region along with immediate implant placement [9,10]. SST is not recommended in teeth with widening of the periodontal ligament, periodontal disease or mobility, or horizontal or vertical root fractures [11,12,13,14,15,16].
Figure 1. Surgical procedures of the socket shield technique with immediate implant placement.
To date, many heterogeneous clinical studies and reviews have been published in the literature on this technique, but there is still no consensus on its efficacy and its long-term and esthetic outcomes. Only a few clinical studies are randomized controlled trials, while there are more retrospective studies; nonetheless, even an analysis of randomized controlled trials, retrospective studies, and prospective clinical trials would be interesting, although such an analysis has not yet been performed. The SST, as with other immediate implant techniques, seems to have a survival rate comparable to that of the conventional implant technique. Long-term osteointegration is a milestone in a patient’s treatment [10], and like all techniques there is the possibility of complications and failure. The main goals of clinical trials are to determine the survival rate and to evaluate complications, but these are not the final endpoints; instead, the secondary outcomes to evaluate are the volume, health, and esthetics of the supporting tissues needed to maintain stability over the long term [10]. The aim of this systematic review was to establish the effectiveness of the SST. The primary outcome was to verify the implant survival rate and to determine which complications occur and how frequently they take place. The secondary outcome was to assess the long-term prognosis for the stabilization of buccal soft and hard tissues, especially the preservation of buccal crestal bone plate.
MATERIALS AND METHODS
Protocol
This systematic review was registered on PROSPERO (registration number: CRD42020180637). The review was based on the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines [17].
Eligibility criteria
The following population, intervention/exposure, comparison, outcome question was formulated to address the specific aim of the study (i.e., to evaluate the effectiveness of the SST):
1) Population: patients with a non-restorable tooth that required extraction.
2) Intervention: implants placed with the SST.
3) Comparison: implants with the conventional technique.
4) Outcomes: the implant survival rate with SST, which complications occur and how frequently they take place, and the long-term prognosis for the stabilization of buccal soft and hard tissues.
Inclusion criteria
This review included articles based on the socket-shield principle, in which implants are placed in close proximity or in contact with root fragments that are intentionally retained to preserve or promote buccal crestal bone. The studies eligible for inclusion were randomized controlled clinical studies, prospective cohort studies, and retrospective case series on humans, with a minimum follow-up of 6 months, published from 2010 to 2021.
Exclusion criteria
Studies in which root fragments were not retained intentionally or in which implants were unknowingly placed in proximity to the root fragment were excluded. Furthermore, case reports, studies on animals, and studies written in a language other than English were not included.
Search
A search was performed on PubMed (MEDLINE), Embase, Web of Knowledge, and Google Scholar in November and December 2021 including the following keywords: “socket,” “socket shield,” “socket shield technique,” “root membrane technique,” “implant placement,” “alveolar ridge preservation,” “implant proximity to teeth,” and “implant in contact with root.” A manual search was also performed of the last 5 years of publications in relevant dental journals (Clinical Implant Dentistry and Related Research, Clinical Oral Implants Research, Implant Dentistry, International Journal of Oral and Maxillofacial Implants, International Journal of Periodontics and Restorative Dentistry, Journal of Esthetic and Restorative Dentistry, Journal of Periodontal & Implant Science, International Journal of Prosthodontics, Journal of Cranio-Maxillofacial Surgery, and Journal of Periodontology), and the bibliographies of all eligible papers were scanned to find additional relevant studies. Clinical studies were chosen based on the title and abstract by 2 investigators.
Data collection
The data from each publication were analyzed, including complications, implant failure, the implant survival rate, and clinical parameters (marginal bone loss [MBL], the pink esthetic score [PES], buccal bone thickness, and buccal bone plate resorption [BBPR]). The authors independently collected the data and confirmed the results by comparison.
Statistical analysis
The weighted average mean was used for the analysis of the survival rate of implants in all 17 included articles. Randomized controlled trials were considered for comparisons of the mean values of MBL, PES, buccal bone thickness, and BBPR. The complication rate and implant survival rate were calculated as mean values.
Quality and risk of bias assessment of the included studies
The Cochrane Collaboration tool was used to assess the risk of bias in the human randomized controlled trials. To evaluate the risk of bias in non-randomized clinical trials, the ROBINS-I tool was used. The evaluated criteria were divided into pre-intervention, intervention, and post-intervention categories. The risk of bias was individually analyzed for each study and classified as low, moderate, serious, critical, and no information.
RESULTS
In total, 132 studies were found in the database search, from which 103 articles were screened after duplicates were removed. Articles that could not be found in English were discarded (n=2). After title and abstract screening, 82 records were excluded, and the full texts of the remaining 19 articles were read. Two of those articles were excluded from the systematic review because they involved a follow-up period shorter than 6 months. Seventeen studies were included in the quantitative and qualitative review. Figure 2 shows a flow diagram of the search results.
Figure 2. PRISMA 2009 flow diagram.
PRISMA: Preferred Reporting Items for Systematic Reviews and Meta-Analyses.
Study details and outcomes
Among the 17 studies involved in the review, 7 were retrospective studies [9,10,11,18,19,20,21], 7 were randomized controlled studies [22,23,24,25,26,27,28] and 3 were prospective studies [29,30,31]. All studies presented level III evidence. The mean follow-up period of the selected papers was 18 months.
Table 1 presents a quantitative description of all the studies included in the systematic review, along with the total sample size and complications associated with the SST. In the 17 human clinical studies, 575 patients were given 656 implants with the SST. Nine implants failed, and 25 implants had other complications such as exposure, infections, peri-implantitis, and migration. The mean complication rate was 3.81%, and the implant survival rate was 98.6% (Table 2).
Table 1. General characteristics of the included studies.
| Authors and year | Type of study | Follow-up period | Biological complications with no implant removal (%) | Implants failed and removed (survival rate) | No. of patients/total implants/SST |
|---|---|---|---|---|---|
| Bäumer et al., 2017 [9] | Retrospective case series | 51 months | No complications | 0 (100%) | 10/10/10 |
| Gluckman et al., 2017 [10] | Retrospective study | 1 year | 16 exposures, 3 infections, 1 migration (19.5%) | 5 (96.1%) | 128/128/128 |
| Siormpas et al., 2018 [11] | Retrospective study | 17 months (max 120 months of follow-up) | No complications (3 at 120 months of follow-up)a) | 3 (1.2%) (5 at 120 months of follow-up)b) | 182/250/250 |
| Mitsias et al., 2020 [12] | Retrospective cohort study | 3 years | No complications | 0 (100%) | 10/13/13 |
| Siormpas et al., 2014 [18] | Retrospective case series | 2 years | 1 periapical granulomatous defect (2.17%) | 0 (100%) | 46/46/46 |
| Abadzhiev et al., 2014 [19] | Retrospective case series | 2 years | No complications | 0 (100%) | 25/26/10 |
| Hana and Omar, 2020 [21] | Retrospective study | 12 months | 2 internal and other external shield exposures (20%) | 1 (95%) | 40/40/20 |
| Bramanti et al., 2018 [22] | Randomized controlled trial | 3 years | No complications | 0 (100%) | 40/40/20 |
| Sun et al., 2020 [23] | Randomized clinical study | 2 years | No complications | 0 (100%) | 30/30/15 |
| Tiwari et al., 2019 [24] | Randomized clinical study | 1 year | 1 apical resorption of the shield (12%) | 0 (100%) | 16/16/8 |
| Barakat et al., 2017 [25] | Randomized controlled clinical trial | 7 months | No complications | 0 (100%) | 20/20/10 |
| Atef et al., 2020 [26] | Randomized clinical study | 12 months | 0 | 0 (100%) | 42/42/21 |
| Abd-Elrahman et al., 2020 [27] | Randomized clinical study | 6 months | 1 internal shield exposure (10%) | 0 (100%) | 40/40/20 |
| Santhanakrishnan et al., 2021 [28] | Randomized clinical study | 6 months | 0 | 0 (100%) | 75/75/25 |
| Troiano et al., 2014 [29] | Prospective case study | 6 months | No complications | 0 (100%) | 7/10/10 |
| Han et al., 2018 [30] | Prospective study | 1 year | No complications | 0 (100%) | 30/40/40 |
| Fattouh, 2018 [31] | Prospective study | 12 months | 0 | 0 (100%) | 20/20/10 |
SST: socket-shield technique.
a)Root fragment infection and peri-implant mucositis at 113 months (n=1) and root fragment infections with fistula mucositis at 51 months and 83 months of follow-up (n=2), respectively. b)Failures of osseointegration.at 3 months (n=2) and peri-implantitis at 12, 36, and 59 months (n=3), respectively.
Table 2. Implant survival rate.
| Number of patients | Number of implants | Biological complications with no implant removal | Implant failure | Mean follow-up | Survival rate |
|---|---|---|---|---|---|
| 575 | 656 | 25 (3.81%) | 9 (1.37%) | 18 months | 98.6% |
As clinical parameters, MBL, PES, buccal bone thickness, and BBPR were analyzed from randomized controlled studies (Tables 3, 4, 5). MBL was lower in implants placed with the SST than in implants placed without the SST (0.39±0.28 mm vs. 1.00±0.55 mm). The SST likewise showed better outcomes for PES, with an average value of 12.08±1.18 versus 10.77±0.74. BBPR had more favorable results in implants placed with the SST (mean: 0.32±0.10 mm) than in implants placed with the standard technique (mean: 1.05±0.18 mm). Buccal bone thickness, in accordance with other results, showed better values in the SST group (1.14±0.2 mm) than in the control group (0.90±0.15 mm).
Table 3. Clinical parameters (mean ± standard deviation) of marginal bone loss, pink esthetic score, and buccal bone plate resorption of implants placed with the SST versus implants placed with other techniques in randomized controlled trials.
| Authors and year | SST implants | Control group and technique | Marginal bone loss (mm) | Pink esthetic score | Buccal bone plate resorption (mm) |
|---|---|---|---|---|---|
| Bramanti et al., 2018 [22] | 20 | Conventional immediate implant | SST: 0.60±0.06 | SST: 12.15±0.87 | Not evaluated |
| CG: 1.11±0.13 | CG: 10.3±1.59 | ||||
| Sun et al., 2020 [23] | 15 | Conventional immediate flap-less approach | SST: 0.28±0.22 (at 6 months) | SST: 12.07±1.62 | Not evaluated |
| CG: 0.87±0.29 (at 6 month) | CG: 11.33±1.76 | ||||
| Tiwari et.al., 2019 [24] | 8 | Conventional immediate implant | Not evaluated | Not evaluated | SST: 0.03±0.02 |
| CG: 0.18±0.013 | |||||
| Barakat et al., 2017 [25] | 10 | Conventional immediate implant | SST: 0.44±0.24 | Not evaluated | SST: 0.10±0.03 |
| CG: 1.61±0.78 | CG: 0.34±0.11 | ||||
| Atef et al., 2020 [26] | 21 | Conventional Immediate implant filling the buccal gap with xenograft | SST: 0.36±0.62 | SST: 12.12±0.64 | SST: 0.290±0.34 |
| CG: 0.71±1.02 | CG: 11.86±0.35 | CG: 1.45±0.72 | |||
| Abd-Elrahman et al., 2020 [27] | 20 | Conventional Immediate implant | SST: 0.31 | SST: 12±1.2 | SST: 0.15 |
| CG: 0.7 | CG: 8.85±1.81 | CG: 0.3 | |||
| Santhanakrishnan et al., 2021 [28] | 25 | I CG Conventional immediate implant placement | Not evaluated | SST: 12.1±1.6 | SST: 0.05±0.02 |
| II CG Delayed implant Placement | I CG: 12.2±1.9 | I CG: 0.4±0.01 | |||
| II CG: 10.9±1.5 | II CG: 0.2±0.2 |
Bold-faced values are statistically significant difference between groups.
SST: socket shield technique; CG: control group; SS: statistically significant difference.
Table 4. Buccal bone thickness of implants placed with the SST versus implants placed with the standard technique.
| Authors and year | No. of patients (implants) | Buccal bone thickness (mm) |
|---|---|---|
| Sun et al. 2020 [23] | 30 | 1.15±0.2 |
| 0.83±0.13 | ||
| Tiwari et al. 2019 [24] | 16 | 1.14±0.2 |
| 0.98±0.17 |
SST: socket shield technique.
Table 5. Weighted average values of clinical parameters.
| Parameters | Socket shield technique | Control group |
|---|---|---|
| Marginal bone loss (mm) | 0.39±0.28 | 1.00±0.55 |
| Pink esthetic score | 12.08±1.18 | 10.77±0.74 |
| Buccal bone plate resorption (mm) | 0.32±0.10 | 1.05±0.18 |
| Buccal bone thickness (mm) | 1.14±0.2 | 0.90±0.15 |
Quality assessment of the included studies
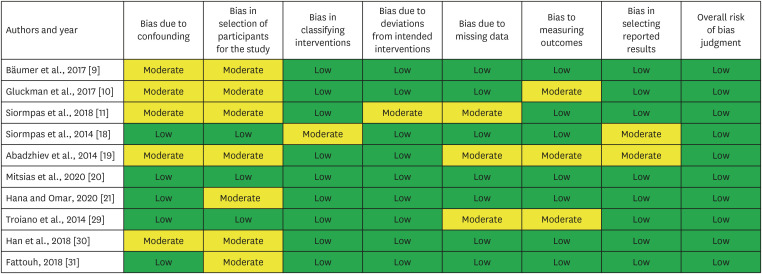
The Cochrane Collaboration’s tool was used to assess the risk of bias in the human randomized controlled trial, and the results are presented in Figure 3. All 7 studies had a low risk of bias, and any biases were deemed unlikely to alter the results of the systematic review. The ROBINS-I tool was used to evaluate the risk of bias in the non-randomized clinical trials. A detailed evaluation of the possible risk of bias for all categories is summarized in Figure 4.
Figure 3. Risk of bias of the included human randomized trials assessed using the Cochrane Collaboration’s tool.
Figure 4. Risk of bias of the included studies according to the ROBINS-I tool.
DISCUSSION
The present systematic review on the SST analyzed only human studies, particularly randomized controlled trials, retrospective case series, and prospective studies.
The primary aim of our review was to assess whether the SST has a favorable prognosis in terms of implant survival rate, which complications occur, and how frequently they take place. In the present review, the implant survival rate was found to be 98.6%, as we found that 9 implants failed out of 656 implants placed. This result seems to be in accordance with the implant survival rate reported in the literature (90%–95% at 10 years) [32]. The most frequent complications were shield exposure and infections. Exposure, internal or external, was found to account for 76% of complications. This complication could be related to a previous infection of the tooth fragment or a non-meticulous surgical technique. A scrupulous patient assessment, a dedicated surgical plan, and surgical experience on the part of clinicians are mandatory in order to reduce the probability of complications. In the study by Gluckman et al. [10], out of a total of 20 complications, 16 were exposures and 3 infections. The authors concluded “the likely cause is a lack of adequate space between the coronal edge of the shield and the subgingival contour of the crown.” In a retrospective study of 182 patients who received 250 implants, the 10-year cumulative implant success rate was 88.5% (implant-based) and 87.9% (patient-based). The complications were infection of the root portion, with suppuration and fistula formation, which occurred in 4 cases and infection of the root associated with preimplant mucositis in 1 case. However, the studies examined were relatively recent, so a longer period of follow-up will be necessary to obtain more accurate information on the implant survival rate.
The secondary aim of our review was to establish the effectiveness of the SST on clinical parameters, such as MBL, PES, and the ability of the technique on the capacity to reduce horizontal resorption of the buccal bone, which is the main reason why the SST was introduced. MBL has been considered among the major complications associated with maintenance and success in implant therapy. Various factors have been described as responsible for crestal bone resorption, such as biological width formation, surgical trauma and prosthetic problems including overload and fracture [33,34]. In randomized controlled studies, MBL was lower in implants placed with the SST than in implants placed without the SST. The PES evaluates the anterior esthetics of the implant-supported single crown at 7 points: the mesial and distal papilla, soft-tissue color, contour, level, texture, and deficiency of the alveolar ridge. Comparing 2 randomized controlled trials, by Sun et al. [23] and Bramanti et al. [22], PES had better outcomes in the SST group. PES is of remarkable importance because the SST is especially indicated in the anterior maxilla region, according to Hurzeler et al. [8]. MBL and PES had better results in the SST group in all the evaluated studies. We can consider the retained root-fragment as a barrier that was able to maintain the contour of the ridge, in order to preserve both hard and soft tissue. Our review also evaluated whether the retention of the root fragment could mitigate the horizontal resorption of buccal bone. Two parameters were evaluated: BBPR and buccal bone thickness. Tiwari et al. [24] and Barakat et al. [25], in their randomized controlled trials [22], both concluded that the SST group showed significantly less horizontal BBPR than implants placed in standard sockets.
This scientific evidence and the empirical experience of immediate implant placement in fresh extraction sockets have led to the proposal that by preserving the periodontal tissues on the buccal part of the socket, we could probably prevent bone resorption in this critical area, as no osteoclastic remodeling of the coronal part of the buccal plate.
With regard to buccal bone thickness at the crest, Sun et al. [23] and Tiwari et al. [24] found a statistically significant difference between the 2 groups. In the SST group, the average value was 1.15 mm, while in the control group, the average value was 0.90 mm.
All the studies included in this systematic review demonstrated better preservation of bone through the SST. Analyzing the complication and implant survival rates of the SST, we can consider this technique a successful alternative to post-extractive implant insertions in the esthetic zone. The presence of the “shield” establishes advantages for hard and soft tissues in terms of space maintenance. Thus, reduction of MBL, increased PES, and decreased buccal bone resorption are parameters that may encourage use of the SST. The reduction of both hard and soft tissue resorption results in a profile comparable to that of the natural teeth.
In conclusion, this systematic review showed encouraging results for the SST. Further long-term randomized controlled trials are required to establish the clinical safety and efficacy of this technique. Within the limits of this review, it may be concluded that the implant survival rate of the SST is in accordance with the standard implant survival rate.
The SST appears to be a safe technique to preserve alveolar bone, as it leads to less horizontal and vertical bone loss than conventional implantation. This technique may also induce more favorable esthetic outcomes than conventional implant placement. The greatest benefit of the SST seems to be preservation of the buccal bone plate, which protects implant placement and improves esthetic outcomes.
Nonetheless, there were few long-term randomized controlled trials comparing the SST with conventional immediate implants, and the conclusions drawn from the results of this systematic review should be interpreted with caution. Further randomized controlled trials with long-term follow-up have to be conducted in order to recommend the SST on a general basis and to establish stronger evidence for its success.
ACKNOWLEDGEMENTS
The authors thank Dr. Massimo Natale (private practice in Capo d’Orlando, Italy), for the clinical pictures.
Footnotes
Conflict of Interest: No potential conflict of interest relevant to this article was reported.
- Conceptualization: Stefano Oliva, Mario Capogreco, Maurizio D’Amario.
- Data curation: Stefano Oliva, Giovanna Murmura, Ettore Lupi, Di Carlo Mariachiara, Maurizio D’Amario.
- Formal analysis: Stefano Oliva, Mario Capogreco, Maurizio D’Amario.
- Methodology: Stefano Oliva, Giovanna Murmura, Maurizio D’Amario.
- Validation: Mario Capogreco, Maurizio D’Amario.
- Writing - original draft preparation: Stefano Oliva, Giovanna Murmura, Ettore Lupi, Di Carlo Mariachiara.
- Writing - review & editing: Mario Capogreco, Maurizio D’Amario.
References
- 1.Amler MH, Johnson PL, Salman I. Histological and histochemical investigation of human alveolar socket healing in undisturbed extraction wounds. J Am Dent Assoc. 1960;61:32–44. doi: 10.14219/jada.archive.1960.0152. [DOI] [PubMed] [Google Scholar]
- 2.Schropp L, Wenzel A, Kostopoulos L, Karring T. Bone healing and soft tissue contour changes following single-tooth extraction: a clinical and radiographic 12-month prospective study. Int J Periodontics Restorative Dent. 2003;23:313–323. [PubMed] [Google Scholar]
- 3.Araújo MG, Lindhe J. Dimensional ridge alterations following tooth extraction. An experimental study in the dog. J Clin Periodontol. 2005;32:212–218. doi: 10.1111/j.1600-051X.2005.00642.x. [DOI] [PubMed] [Google Scholar]
- 4.Botticelli D, Berglundh T, Lindhe J. Hard-tissue alterations following immediate implant placement in extraction sites. J Clin Periodontol. 2004;31:820–828. doi: 10.1111/j.1600-051X.2004.00565.x. [DOI] [PubMed] [Google Scholar]
- 5.Araújo M, Linder E, Wennström J, Lindhe J. The influence of Bio-Oss Collagen on healing of an extraction socket: an experimental study in the dog. Int J Periodontics Restorative Dent. 2008;28:123–135. [PubMed] [Google Scholar]
- 6.Araújo MG, Lindhe J. Socket grafting with the use of autologous bone: an experimental study in the dog. Clin Oral Implants Res. 2011;22:9–13. doi: 10.1111/j.1600-0501.2010.01937.x. [DOI] [PubMed] [Google Scholar]
- 7.Lekovic V, Camargo PM, Klokkevold PR, Weinlaender M, Kenney EB, Dimitrijevic B, et al. Preservation of alveolar bone in extraction sockets using bioabsorbable membranes. J Periodontol. 1998;69:1044–1049. doi: 10.1902/jop.1998.69.9.1044. [DOI] [PubMed] [Google Scholar]
- 8.Hürzeler MB, Zuhr O, Schupbach P, Rebele SF, Emmanouilidis N, Fickl S. The socket-shield technique: a proof-of-principle report. J Clin Periodontol. 2010;37:855–862. doi: 10.1111/j.1600-051X.2010.01595.x. [DOI] [PubMed] [Google Scholar]
- 9.Bäumer D, Zuhr O, Rebele S, Hürzeler M. Socket shield technique for immediate implant placement - clinical, radiographic and volumetric data after 5 years. Clin Oral Implants Res. 2017;28:1450–1458. doi: 10.1111/clr.13012. [DOI] [PubMed] [Google Scholar]
- 10.Gluckman H, Salama M, Du Toit J. A retrospective evaluation of 128 socket-shield cases in the esthetic zone and posterior sites: partial extraction therapy with up to 4 years follow-up. Clin Implant Dent Relat Res. 2018;20:122–129. doi: 10.1111/cid.12554. [DOI] [PubMed] [Google Scholar]
- 11.Siormpas KD, Mitsias ME, Kotsakis GA, Tawil I, Pikos MA, Mangano FG. The root membrane technique: a retrospective clinical study with up to 10 years of follow-up. Implant Dent. 2018;27:564–574. doi: 10.1097/ID.0000000000000818. [DOI] [PubMed] [Google Scholar]
- 12.Mitsias ME, Siormpas KD, Kotsakis GA, Ganz SD, Mangano C, Iezzi G. The root membrane technique: human histologic evidence after 5 years of function. BioMed Res Int. 2017;2017:7269467. doi: 10.1155/2017/7269467. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Kumar PR, Kher U. Shield the socket: procedure, case report and classification. J Indian Soc Periodontol. 2018;22:266–272. doi: 10.4103/jisp.jisp_78_18. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Gharpure AS, Bhatavadekar NB. Current evidence on the socket-shield technique: a systematic review. J Oral Implantol. 2017;43:395–403. doi: 10.1563/aaid-joi-D-17-00118. [DOI] [PubMed] [Google Scholar]
- 15.Mourya A, Mishra SK, Gaddale R, Chowdhary R. Socket-shield technique for implant placement to stabilize the facial gingival and osseous architecture: a systematic review. J Investig Clin Dent. 2019;10:e12449. doi: 10.1111/jicd.12449. [DOI] [PubMed] [Google Scholar]
- 16.Hinze M, Janousch R, Goldhahn S, Schlee M. Volumetric alterations around single-tooth implants using the socket-shield technique: preliminary results of a prospective case series. Int J Esthet Dent. 2018;13:146–170. [PubMed] [Google Scholar]
- 17.Shamseer L, Moher D, Clarke M, Ghersi D, Liberati A, Petticrew M, et al. Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015: elaboration and explanation. BMJ. 2015;350:g7647. doi: 10.1136/bmj.g7647. [DOI] [PubMed] [Google Scholar]
- 18.Siormpas KD, Mitsias ME, Kontsiotou-Siormpa E, Garber D, Kotsakis GA. Immediate implant placement in the esthetic zone utilizing the “root-membrane” technique: clinical results up to 5 years postloading. Int J Oral Maxillofac Implants. 2014;29:1397–1405. doi: 10.11607/jomi.3707. [DOI] [PubMed] [Google Scholar]
- 19.Abadzhiev M, Nenkov P, Velcheva P. Conventional immediate implant placement and immediate placement with socket-shield technique which is better. Int J Clin Med Res. 2014;1:176–180. [Google Scholar]
- 20.Mitsias MM, Bratos M, Siormpas K, Pikos MA, Kotsakis GA Root Membrane Group. Longitudinal soft tissue changes during periodontal ligament-mediated immediate implant placement with the root-membrane technique. Int J Oral Maxillofac Implants. 2020;35:379–385. doi: 10.11607/jomi.7245. [DOI] [PubMed] [Google Scholar]
- 21.Hana SA, Omar OA. Socket shield technique for dental implants in the esthetic zone, clinical and radiographical evaluation. J Duhok Univ. 2020;23:69–80. [Google Scholar]
- 22.Bramanti E, Norcia A, Cicciù M, Matacena G, Cervino G, Troiano G, et al. Postextraction dental implant in the aesthetic zone, socket shield technique versus conventional protocol. J Craniofac Surg. 2018;29:1037–1041. doi: 10.1097/SCS.0000000000004419. [DOI] [PubMed] [Google Scholar]
- 23.Sun C, Zhao J, Liu Z, Tan L, Huang Y, Zhao L, et al. Comparing conventional flap-less immediate implantation and socket-shield technique for esthetic and clinical outcomes: a randomized clinical study. Clin Oral Implants Res. 2020;31:181–191. doi: 10.1111/clr.13554. [DOI] [PubMed] [Google Scholar]
- 24.Tiwari S, Bedi RS, Wadhwani P, Aurora JK, Chauhan H. Comparison of immediate implant placement following extraction with and without socket-shield technique in esthetic region. J Maxillofac Oral Surg. 2020;19:552–560. doi: 10.1007/s12663-019-01272-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Barakat D, Hassan R, Eldibany R. Valuation of the socket shield technique for immediate implantation. Alexandria Dent J. 2017;42:155–161. [Google Scholar]
- 26.Atef M, El Barbary A, Dahrous MS, Zahran AF. Comparison of the soft and hard peri-implant tissue dimensional changes around single immediate implants in the esthetic zone with socket shield technique versus using xenograft: a randomized controlled clinical trial. Clin Implant Dent Relat Res. 2021;23:456–465. doi: 10.1111/cid.13008. [DOI] [PubMed] [Google Scholar]
- 27.Abd-Elrahman A, Shaheen M, Askar N, Atef M. Socket shield technique vs conventional immediate implant placement with immediate temporization. Randomized clinical trial. Clin Implant Dent Relat Res. 2020;22:602–611. doi: 10.1111/cid.12938. [DOI] [PubMed] [Google Scholar]
- 28.Santhanakrishnan M, Subramanian V, Ramesh N, Kamaleeshwari R. Radiographic and esthetic evaluation following immediate implant placement with or without socket shield and delayed implant placement following socket preservation in the maxillary esthetic region - a randomized controlled clinical trial. Clin Cosmet Investig Dent. 2021;13:479–494. doi: 10.2147/CCIDE.S332687. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Troiano M, Benincasa M, Sànchez P, Calvo-Guirado J. Bundle bone preservation with Root-T-Belt: case study. Ann Oral Maxillofac Surg. 2014;2:7. [Google Scholar]
- 30.Han CH, Park KB, Mangano FG. The modified socket shield technique. J Craniofac Surg. 2018;29:2247–2254. doi: 10.1097/SCS.0000000000004494. [DOI] [PubMed] [Google Scholar]
- 31.Fattouh H. Socket- shield technique versus guided bone regeneration technique for ridge preservation with immediate implant placement in the esthetic zone. Egypt Dent J. 2018;64:2047–2055. [Google Scholar]
- 32.Esposito M, Grusovin MG, Coulthard P, Thomsen P, Worthington HV. A 5-year follow-up comparative analysis of the efficacy of various osseointegrated dental implant systems: a systematic review of randomized controlled clinical trials. Int J Oral Maxillofac Implants. 2005;20:557–568. [PubMed] [Google Scholar]
- 33.Adell R, Lekholm U, Rockler B, Brånemark PI. A 15-year study of osseointegrated implants in the treatment of the edentulous jaw. Int J Oral Surg. 1981;10:387–416. doi: 10.1016/s0300-9785(81)80077-4. [DOI] [PubMed] [Google Scholar]
- 34.Jung YC, Han CH, Lee KW. A 1-year radiographic evaluation of marginal bone around dental implants. Int J Oral Maxillofac Implants. 1996;11:811–818. [PubMed] [Google Scholar]