Abstract
Background
Cardiovascular disease burden is decreasing, but these reductions have not been distributed equally amongst socioeconomic groups.
Objectives
The aim of this study was to define the relationships between different domains of socioeconomic health, traditional cardiovascular risk factors and cardiovascular events.
Methods
This was a cross-sectional study of local government areas (LGAs) in Victoria, Australia. We used data from a population health survey combined with cardiovascular event data derived from hospital and government data. Four socioeconomic domains: educational attainment, financial wellbeing, remoteness, and psychosocial health, were generated from 22 variables. The primary outcome was a composite of non-STEMI, STEMI, heart failure and cardiovascular deaths per 10,000 persons. Linear regression and cluster analysis were used to assess the relationships between risk factors and events.
Results
Across 79 LGAs there were 33,654 interviews conducted. All socioeconomic domains were associated with burden of traditional risk factors, including hypertension, smoking, poor diet, diabetes, and obesity. Financial wellbeing, educational attainment and remoteness were all correlated with cardiovascular events on univariate analysis. After multivariate adjustment for age and sex, financial wellbeing, psychosocial wellbeing, and remoteness were associated with cardiovascular events, while educational attainment was not. After including traditional risk factors only financial wellbeing and remoteness remained correlated with cardiovascular events.
Conclusions
Financial wellbeing and remoteness independently be associated with cardiovascular events, while educational attainment and psychosocial wellbeing are attenuated by traditional cardiovascular risk factors. Poor socioeconomic health is clustered in certain areas, which have high cardiovascular event rates.
Keywords: Coronary artery disease, Epidemiology, Delivery of health care, Heart failure, Risk factors
1. Introduction
The burden of cardiovascular disease has decreased significantly in Australia over the past half century. Cardiovascular disease was responsible for 55% of all Australian deaths in the 1960s. That proportion has decreased to 29% of deaths in 2015 [1]. However, the population level improvements in cardiovascular disease have not been distributed equally amongst economic and cultural groups [2,3]. Disparities in outcomes are evident across income, education, and geographic groups [4].
Much of this disparity relates to the varying prevalence and control of traditional risk factors (such as diabetes, hypertension and dyslipidaemia) which are, in large part, governed by structural and social determinants of health [5,6]. These effects are even witnessed at a neighbourhood level, with studies demonstrating an association between living in a disadvantaged area and an increasing likelihood of coronary disease after accounting for individual-specific factors [7].
However, even after adjusting for the prevalence of traditional risk factors, residual risk persists across a socioeconomic gradient suggesting more research is required to understand the construct and determinants of these complex biopsychosocial relationships. Such factors may be both biological (such as physiological responses to chronic stress) and societal (such as structural barriers to healthcare) [8,9].
There is a paucity of data evaluating the impact and relationships between different categories of socioeconomic risk factors (e.g. education, income, employment) and cardiovascular risk. The 2015 American Heart Association Scientific Statement on the Social Determinants of Risk and Outcomes for Cardiovascular Disease highlighted the need for studies examining the interactions between different socioeconomic factors and cardiovascular disease [10]. Thus, our aims were to a) determine whether varying degrees of socioeconomic inequality are associated with adverse cardiovascular outcomes within local government areas, b) understand whether these associations were confounded by traditional risk factors and c) to understand the correlation and distribution of socioeconomic risk factors to identify areas of high need and thus inform policy levers and programs.
2. Methods
2.1. Study design and setting
We performed a cross-sectional study at the level of local government areas (LGAs) in the state of Victoria, Australia during 2015. We used data collected by the government via a population health survey in addition to outcome data derived from coding of all hospital admissions in Victoria. Using this data, we examined the relationship between socioeconomic risk factor domains and cardiovascular events at an LGA level. LGAs are an administrative subdivision of the state similar to a municipality. The state of Victoria has 79 LGAs which vary in population and geographic size. The function of LGA administration includes management of infrastructure, community facilities (such as parks and libraries), child-care and community health services. The study was approved by the Victorian Department of Health and Human Services ethical review panel. The protocol complies with the declaration of Helsinki. Participant consent was sought during survey collection.
2.2. Participants and data sources
Risk factor data was gathered in a state-wide survey from all adults (>18 years old) living in Victoria, Australia using a modified random digit dialling process, which included both landline and mobile phone numbers. Trained interviewers conducted computer-assisted telephone interviews, with the ability to conduct interviews in any of the nine most popular languages in Victoria. A single respondent was randomly selected from within a household and each respondent was treated as representing the whole household. The overall response rate (number of households contacted that completed an interview) was 69.6%. A total of 33,654 interviews (with 426 respondents per LGA) were completed including 940 interviews in non-English languages.
2.3. Public and patient involvement
The study was designed in consultation with the Victorian Department of Health and Human Services as representative of the public. No individual participant was involved in the design or assessment of the study. Findings will be disseminated to the Victorian public via publication in scientific journals and updates through the Victorian Department of Health and Human Services newsletters.
2.4. Variables
Traditional cardiovascular risk factor data for the proportion of adults with hypertension, obesity, insufficient physical activity, insufficient fruit and vegetable intake, smoking habits and diabetes mellitus was gathered through questions in the survey.
Cardiovascular events were based on hospital admissions in Victoria in 2017. The Victorian Department of Health and Human Services collects coded admission data for all hospital admissions in Victoria. Multiple codes relating to the outcome variables of heart failure, ST-elevation myocardial infarction (STEMI) and non-STEMI were included to define admissions during 2017. Additionally, cardiovascular mortality was ascertained using data from the government's death registry.
2.5. Socioeconomic score creation
All socioeconomic data was gathered through the government population health survey. Additionally, ‘remoteness’ a variable describing relative access to goods and services, was defined for each LGA using the Australian government classification. This classification provides 5 different classes: major cities, inner regional, outer regional, remote and very remote. Further information on the derivation of remoteness category is available on the Australian Bureau of Statistics website [11]. All Victorian LGAs fall into one of the three categories of major city, inner regional and outer regional.
We established four socioeconomic domains: educational attainment, financial wellbeing, remoteness (as a marker of access to healthcare) and psychosocial health. The variables comprised within these domains are found in Table 1. To summarise each domain for the LGAs, we ranked LGAs from 1 to 79 for each variable where lower ranks were associated with undesirable qualities (eg, rank 1 has the highest family violence rate). We averaged the LGA ranks for each variable and thus, numerically higher domain scores were associated with preferable characteristics in that socioeconomic domain. LGAs were then separated into tertiles based on their socioeconomic domain score.
Table 1.
Socioeconomic domain definitions.
| Educational Attainment | Financial Wellbeing | Psychosocial Wellbeing | Remoteness |
|---|---|---|---|
| Completion of Year 12 | Index of relative socioeconomic disadvantage | Recreational drug use | Major Cities of Australia |
| Higher education attainment | Food insecurity | Family violence rate | Inner Regional Australia |
| Mortgage stress | Gambling losses | Outer Regional Australia | |
| Median house price | Soft drink consumption | ||
| Proportion living in social housing | Good work-life balance | ||
| Homelessness | |||
| Disability support pension rate | |||
| Aged pension rate | |||
| Private health insurance | |||
| Missed consults due to finances | |||
| Missed medications due to finances |
2.6. Outcomes
The primary outcome was a composite of myocardial infarction admission, heart failure admission and cardiovascular death per 10,000 people.
2.7. Statistical analysis
Socioeconomic domain score tertiles were ordinal variables. Traditional cardiovascular risk factor proportions for each LGA were continuous variables. Remoteness was treated as a categorical variable. Cardiovascular outcome rates were analysed as a continuous variable measured as a rate per 10,000 persons per year. We performed univariate linear regression to assess the association of socioeconomic domains, traditional cardiovascular risk factors and remoteness. We then performed multiple linear regression with a progressive modelling technique to evaluate the significance of each socioeconomic domain after adjustment for other variables. The first models adjusted for demographic differences by including LGA median age and the proportion of males in the LGA in order to understand the relationship of socioeconomic domains after accounting for the effect of age and sex on cardiovascular events. The second model adjusted for demographics as well as traditional cardiovascular risk factors by including LGA median age, proportion of males and the individual prevalence of diabetes, hypertension, obesity, insufficient fruit and vegetable intake and insufficient physical exercise. The second model allows for assessment of confounding by traditional risk factors when considering the relationship between socioeconomic domains and cardiovascular events. To assess the distribution and relationships of different socioeconomic risk factor domains, we undertook a k-means cluster analysis using the continuous variables of financial wellbeing score, education score and psychosocial health score. These clusters were displayed on a heatmap. Significance was defined as a p < 0.05. All analysis was undertaken in R version 4.1.3 (R Foundation, Vienna, Austria).
3. Results
A total of 33,654 interviews were conducted across 79 LGAs in Victoria (426 respondents per LGA). Nine-hundred and forty interviews (2.8%) were conducted in non-English languages. The aggregate baseline characteristics for the LGAs by tertile of socioeconomic risk domain are shown in Table 2. The median age across LGAs was 41 years (IQR: 9.5) with a mean of 49.3 ± 1.1% males. Thirty-two percent (n = 25) of the LGAs were classified as ‘Major Cities of Australia’, while 43% (n = 34) were classified ‘Inner Regional Australia’ and 25% (n = 20) were ‘Outer Regional Australia’.
Table 2.
Baseline characteristics of LGAs.
| Financial Wellbeing |
Educational Attainment |
Psychosocial Wellbeing |
Remoteness |
|||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Tertile 1 | Tertile 2 | Tertile 3 | p-value | Tertile 1 | Tertile 2 | Tertile 3 | p-value | Tertile 1 | Tertile 2 | Tertile 3 | p-value | Outer Regional (n = 20) | Inner Regional (n = 34) | Major Cities (n = 25) | p-value | |
| Age, years Median (IQR) |
45 (10.5) | 44 (10.8) | 38.5* (4.8) | 0.009 | 47 (7) | 41* (7.8) | 38* (4.8) | <0.0001 | 42 (7.5) | 39 (12.8) | 42.5 (10) | 0.5 | 48 (4.8) | 42a (8.8) | 37a (3) | <0.0001 |
| Male Sex, % Mean (CI) |
49.7 (49.2,50.2) | 49.5 (49.2,49.8) | 48.8a (48.4,49.1) | 0.002 | 49.8 (49.4,50.2) | 49.4 (49.0,49.8) | 48.8a (48.4,49.2) | 0.0006 | 49.3 (48.9,49.7) | 49.5 (49.0,49.7) | 49.3 (48.8,49.9) | 0.9 | 50.1 (49.6,50.6) | 49.3a (48.9,49.7) | 48.8a (48.5,49.2) | 0.0002 |
| Hypertension, % Mean (CI) |
25.4 (24.0,26.9) | 24.7 (23.2,26.2) | 20.5a (19.1,22.0) | <0.001 | 25.6 (24.0,27.2) | 24.3 (23.0,25.6) | 20.7a (19.2,22.3) | <0.0001 | 25.7 (24.2,27.2) | 23.2a (21.7,24.6) | 21.8a (20.0,23.5) | 0.001 | 24.6 (23.1,26.2) | 24.8 (23.3,26.3) | 21.0a (19.5,22.6) | 0.0008 |
| Diabetes Mellitus Mean (CI) |
5.3 (4.9,5.7) | 5.3 (4.8,5.9) | 4.0a (3.5,4.4) | <0.001 | 5.0 (4.7,5.4) | 5.1 (4.6,5.6) | 4.5 (3.8,5.2) | 0.2 | 5.4 (4.9,5.9) | 4.9 (4.5,5.4) | 4.3a (3.7,4.8) | 0.008 | 4.9 (4.5,5.3) | 4.9 (4.4,5.4) | 4.9 (4.2,5.5) | 0.9 |
| Obesity, % Mean (CI) |
23.0 (21.2,24.8) | 21.5 (19.4,23.5) | 16.1* (14.3,17.9) | <0.001 | 23.2 (21.4,25.0) | 22.0 (20.1,23.8) | 15.4a (13.8,17.0) | <0.001 | 23.8 (22.1,25.6) | 18.4a (16.5,20.3) | 18.3a (16.1,20.5) | <0.0001 | 21.7 (19.8,23.6) | 22.3 (20.5,24.2) | 16.2a (14.3,18.1) | <0.0001 |
| Current Smokers, % Mean (CI) |
17.3 (15.9,18.6) | 14.6a (12.5,16.8) | 11.5a (10.0,13.0) | <0.0001 | 16.9 (14.9,18.9) | 14.7a (12.9,16.6) | 11.8a (10.4,13.2) | <0.0001 | 16.3 (14.4,18.2) | 14.5 (12.7,16.2) | 12.6a (10.7,14.5) | 0.005 | 15.5 (13.2,17.8) | 15.5 (13.7,17.2) | 12.3a (10.8,13.8) | 0.02 |
| Insufficient Fruit & Veg Intake, % Mean (CI) |
52.4 (51.0,53.9) | 48.9a (47.0,50.1) | 46.7a (44.0,49.4) | 0.0004 | 51.4 (49.6,53.2) | 50.5 (48.5,52.4) | 46.2a (43.8,48.7) | <0.0001 | 51.0 (49.2,52.7) | 49.7 (47.9,51.5) | 47.4a (44.5,50.2) | 0.06 | 51.7 (50.1,53.2) | 49.3 (47.0,51.6) | 47.6a (45.6,49.6) | 0.05 |
| Insufficient Physical Exercise, % Mean (CI) |
50.5 (48.9,52.1) | 51.0 (49.1,52.8) | 48.8 (46.7,50.9) | 0.22 | 51.1 (49.4,52.9) | 49.8 (48.3,51.4) | 39.2 (37.0,41.5) | 0.1 | 50.8 (49.0,52.7) | 51.8 (50.6,53.0) | 47.6a (45.5,49.6) | 0.007 | 49.4 (47.1,51.8) | 50.7 (49.1,52.4) | 49.7 (48.0,51.4) | 0.3 |
Table 2 – Distribution of traditional cardiovascular risk factors across different tertiles of socioeconomic domains.
Indicates that the individual mean is significantly different from tertile 1 (reference group).
3.1. Socioeconomic domains and traditional cardiovascular risk factors
There were stepwise increases in the prevalence of most traditional cardiovascular risk factors with each worsening tertile of socioeconomic risk domain as demonstrated in Table 2. Particularly robust gradients were observed for hypertension, obesity, cigarette smoking and insufficient fruit and vegetable intake across each of the socioeconomic risk domain tertiles. In contrast, overall rates of insufficient physical activity were similar across financial well-being and remoteness strata while a monotonic relationship persisted across tertiles of educational attainment and psychosocial wellbeing. Of note, while diabetes was more common among those LGAs with overall lower psychosocial, financial wellbeing and educational attainment, there was no difference in prevalence by remoteness.
3.2. Traditional cardiovascular risk factors and cardiovascular events
All traditional cardiovascular risk factors apart from insufficient physical activity were associated with more cardiovascular events as demonstrated in Table 3. The strongest relationships were observed between cardiovascular events and male sex, median age and diabetes. Specifically, each percentage increase of males in an LGA was associated with an additional 6.4 cardiovascular events per 10,000 persons (95%CI 2.31 to 10.45, p = 0.003), an LGA median age increase of 1 year was associated with an additional 2.5 cardiovascular events per 10,000 persons (95%CI 2.05 to 3.03, p < 0.0001) and with each percentage increase in LGA diabetes prevalence there was an additional 3.6 cardiovascular events per 10,000 persons (95%CI 0.33 to 6.91, p = 0.03).
Table 3.
Univariate linear regression of risk factors and cardiovascular event rate per 10,000.
| Risk Factor | Regression Coefficient for Cardiovascular Events per 10,000 persons (95% CI) | p-value |
|---|---|---|
| LGA Population (per 1000 increase) | −0.17 (−0.22 to −0.11) | <0.0001 |
| Traditional Risk Factor Prevalence | ||
| Percentage of Males (per 1% increase) | 6.4 (2.31–10.45) | 0.003 |
| Median Age (per 1 year increase) | 2.5 (2.05–3.03) | <0.0001 |
| Diabetes Mellitus (per 1% increase) | 3.6 (0.33–6.91) | 0.03 |
| Hypertension (per 1% increase) | 1.6 (0.55–2.58) | 0.003 |
| Obesity (per 1% increase) | 1.5 (0.77–2.25) | 0.0001 |
| Current Smoking (per 1% increase) | 1.2 (0.41–2.16) | 0.005 |
| Insufficient Fruit and Vegetable Intake | 1.2 (0.39–1.99) | 0.004 |
| Insufficient Physical Activity | 0.6 (−0.42 to 1.54) | 0.3 |
3.3. Socioeconomic domains and cardiovascular outcomes
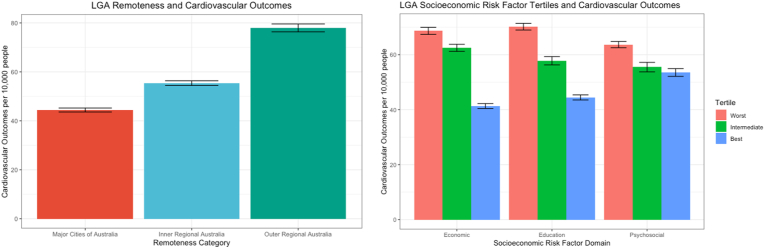
On univariate analysis there were monotonic relationships between worsening socioeconomic risk score and rate of cardiovascular events as shown in Fig. 1. For education, LGAs in the worst tertile had a cardiovascular event rate of 70.2 per 10,000 people (95%CI 63.8 to 76.6) compared to 44.4 per 10,000 people (95%CI 39.5 to 49.4) in the best tertile (p < 0.0001). For financial wellbeing, a similar magnitude of difference was seen (68.8 (95%CI 61.7 to 75.7) per 10,000 people in the worst tertile compared to 41.3 (95%CI 36.6 to 46.1) per 10,000 people in the best tertile, p < 0.0001) as demonstrated in Fig. 1. In contrast, LGA psychosocial wellbeing was not associated with adverse cardiovascular events (p = 0.13).
Fig. 1.
–Bar graphs of socioeconomic variables and cardiovascular outcomes.
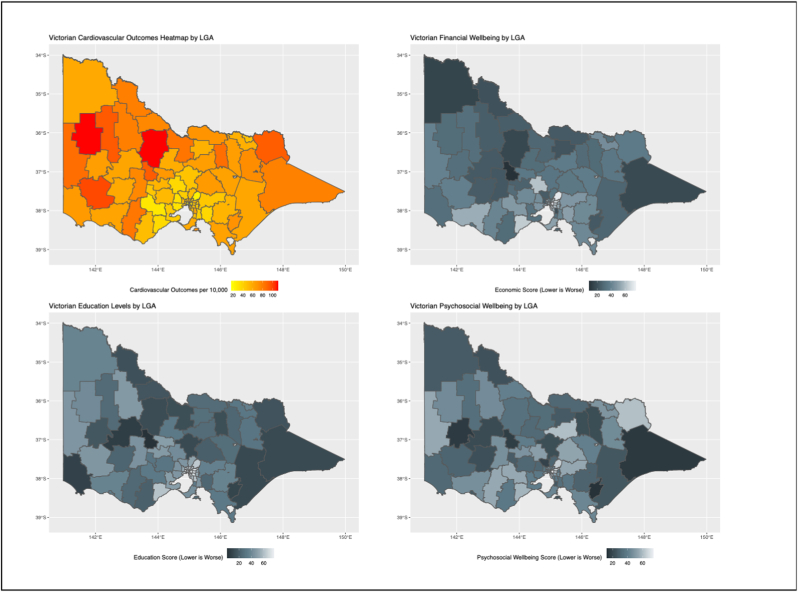
Remoteness was also highly associated with cardiovascular events. Cardiovascular event rates were worse in regional areas as compared to major city areas (an excess of 10.9 events per 10,000 people per year (95%CI 2.87 to 18.77) for inner regional areas and an excess of 33.5 events per 10,000 people per year (95%CI 24.55 to 42.55), p < 0.0001 for outer regional areas). A comparative heat map of socioeconomic risk factors and cardiovascular events across the LGAs is shown in Fig. 2.
Fig. 2.
Heatmaps of cardiovascular outcomes, financial wellbeing, education levels and psychosocial wellbeing by LGA.
3.4. Multivariate modelling
After adjusting for LGA demographic differences (age and proportion of males), financial wellbeing (p < 0001), psychosocial wellbeing (p = 0.001) and remoteness (p = 0.002) remained associated with cardiovascular event rates as shown in Table 4..
Table 4.
Multivariate modelling for LGA characteristics and cardiovascular events.
| Model 1: Sex and Age | Model 2: Sex and age + Traditional Risk Factors | ||
|---|---|---|---|
| Financial Wellbeing | T1 vs Ref | −16.7 (−23.8 to −9.7), p < 0.0001 | −10 (−18.7 to −1.3), p = 0.02 |
| T2 vs Ref | −2.9 (−9.1 to 3.4), p = 0.4 | −0.8 (−7.2 to 5.8), p = 0.7 | |
| Educational Attainment | T1 vs Ref | −9.7 (−18.1 to −1.2), p = 0.03 | −0.4 (−10.0 to 9.1), p = 0.3 |
| T2 vs Ref | −4.8 (−12.1 to 2.5), p = 0.2 | −3.3 (−10.0 to 9.1), p = 0.8 | |
| Psychosocial Wellbeing | T1 vs Ref | −12.6 (−19.2 to −6.0), p = 0.001 | −6 (−10.0 to 9.1), p = 0.8 |
| T2 vs Ref | −4.4 (−11.0 to 2.2), p = 0.2 | −0.4 (−10.0 to 9.1), p = 0.08 | |
| Remoteness | IR vs Major | −22.6 (−31.0 to −14.2), p < 0.0001 | −15.2 (−21.6 to −8.7), p = 0.05 |
| OR vs. Major | −33.5 (−42.5 to −24.6), p < 0.0001 | −8 (−17.0 to 1), p = 0.08 | |
After including traditional cardiovascular risk factors in addition to demographic differences, only financial wellbeing (p = 0.04) and remoteness (p < 0.0001) remained significantly associated with cardiovascular event rates.
3.5. Cluster analysis of financial wellbeing, education and psychosocial wellbeing across LGAs
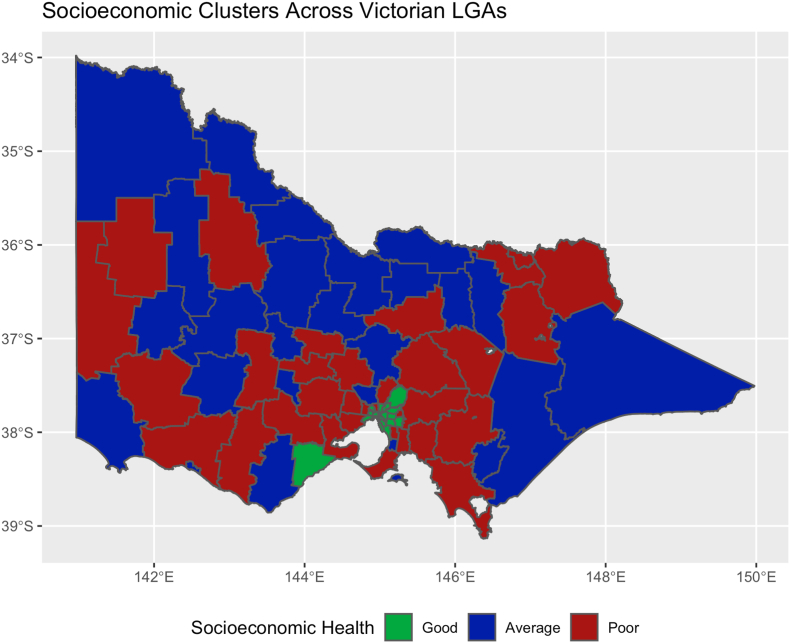
Cluster analysis including financial wellbeing, education and psychosocial wellbeing defined three separate LGA groups (between sum of squares/within sum of squares = 70%) with poor, average and good socioeconomic scores as demonstrated in Table 5. There was a strong association between worsening socioeconomic cluster and worsening cardiovascular event rates, with the worst cluster having an excess of 26.4 cardiovascular events per 10,000 people in comparison to the best cluster (p < 0.0001). A geographic heatmap of these clusters is demonstrated in Fig. 3.
Table 5.
Characteristics of socioeconomic clusters.
| Financial Wellbeing Score | Education Score | Psychosocial Score | Cardiovascular Event Rate (per 10,000 people) | |
|---|---|---|---|---|
| Good Socioeconomic Cluster | 59.3 | 66.9 | 52 | 41.3 (95% CI 36.0 to 46.8) |
| Average Socioeconomic Cluster | 39.3a | 39.4a | 43.8a | 59.7 (95% CI 53.2 to 63.4)a |
| Poor Socioeconomic Cluster | 25.7a | 20.1a | 25.6a | 67.7 (95% CI 61.0 to 74.3)a |
| p-value | <0.0001 | <0.0001 | <0.0001 | <0.0001 |
Table 5 – Cardiovascular event rates by socioeconomic cluster identified using K-means cluster analysis.
Indicates that the individual mean is different from the reference group which is good socioeconomic cluster.
Fig. 3.
Geographical distribution of clusters of socioeconomic health.
4. Discussion
This study demonstrates a strong association between cardiovascular event rates and worsening characteristics of financial wellbeing, educational attainment and remoteness at an LGA level. After adjustment for differences in LGA demographics (sex and age) educational attainment was no longer significantly associated with cardiovascular events, which suggests that the univariate effect of education may be attenuated by lower educational attainment in higher cardiovascular risk age groups and/or males. After further adjustment for traditional cardiovascular risk factors and demographic characteristics, only financial wellbeing and remoteness remained significantly associated with cardiovascular event rates. Poor psychosocial wellbeing was not associated with cardiovascular events on univariate analysis but became statistically significant after adjusting for age and proportion of male sex. After further adjustment for traditional cardiovascular risk factors psychosocial wellbeing was no longer statistically significant. These findings suggest that poor psychosocial wellbeing may be more common in lower risk age and sex groups, but that this relationship is attenuated by a poorer traditional cardiovascular risk profile. In contrast, it appears that independent of traditional risk factors, there remains a residual cardiovascular risk conferred by financial hardship and remoteness.
Furthermore, our findings suggest that socioeconomic risk factors are concentrated within certain ‘high-risk’ areas as demonstrated in the cluster analysis and geospatial mapping. Remoteness category is an Australian Bureau of Statistics defined marker of relative access to goods and services. Remoteness was found to be a significant predictor of LGA cardiovascular events after adjusting for both demographic differences and traditional cardiovascular risk factors. Increasing remoteness was associated with worse cardiovascular outcomes, with inner regional (+9.87 cases per 10,000 people, p = 0.004) and outer regional LGAs (+12.62 cases per 10,000 people, p < 0.0001) suffering poorer cardiovascular events than their major city counterparts. The relationship between remoteness and worse cardiovascular events likely occurs through multiple mechanisms. Previous work has demonstrated a lower likelihood of health seeking behaviour in rural communities compared to those in urban areas [12]. Additionally, remoteness correlates with lower measures of health literacy, which may add to this disparity [13,14]. By its very definition, increasing remoteness presents structural barriers to healthcare access. Importantly, our work suggests that the observed differences between metropolitan and remote communities are not simply a consequence of a higher traditional risk factor burden.
Our work is consistent with previous findings of poor health amongst socially disadvantaged populations observed in many countries. Diez Roux et al. utilised the Atherosclerosis Risk in Community data to demonstrate an association between disadvantaged neighbourhoods in the United States and an increased incidence of coronary heart disease [7]. They utilised a summary score composed of wealth, income and occupation variables to represent the socioeconomic status of neighbourhoods. Individuals from disadvantaged neighbourhoods suffered a higher incidence of coronary disease, even after adjusting for an individual's own risk factors. This work demonstrates the impact of the broader socioeconomic environment in accounting for inequalities in cardiovascular outcomes.
Many previous studies have examined single markers of socioeconomic disadvantage and their relation to cardiovascular disease. An Asia-Pacific collaboration of cohort studies, which included Australian participants, demonstrated that primary education alone was associated with a hazard ratio of 2.47 for cardiovascular disease mortality compared to tertiary education [15]. This relationship persisted despite adjustment for traditional cardiovascular risk factors including body mass index, smoking, hypertension, and cholesterol. However, this study did not adjust for other socioeconomic confounders such as income and psychosocial factors. Similarly, Gerber et al. [16] demonstrated that, in an American population, each $10,000 increase in median neighbourhood annual income was associated with a 10% reduction in mortality risk. This study also found a similar relationship between education and cardiovascular outcomes. Both education and income were independent predictors in a multivariate model. However, this work offered only a limited assessment of the comparative relationship between education and annual income.
Given the complex causal chain of socioeconomic factors and cardiovascular disease it is unlikely that a single marker is sufficient in explaining the observed patterns. The interdependence of social determinants and traditional cardiovascular risk factors is apparent in our work given that the strength of effect was diminished in multivariate modelling. Indeed, only financial wellbeing and remoteness remained significantly associated with poor cardiovascular event rates after adjusting for demographics and the prevalence of traditional cardiovascular risk factors. While it is understandable that poor access to healthcare and other services may independently mediate poor cardiovascular event rates, the mechanism of financial wellbeing is less apparent. It seems likely that the relationship between LGA financial wellbeing and cardiovascular outcomes is complex and multifactorial. Possible explanations include structural barriers to accessing healthcare such as missed medications and missed healthcare consults in addition to the psychological stressors imposed by poverty which may result in chronic stress responses and poor health behaviours.
Our work suggests that socioeconomic factors are clustered densely in ‘high socioeconomic risk’ areas. This was demonstrated through an unsupervised cluster analysis that identified three separate groups with correlated scores across the three socioeconomic domains of financial wellbeing, education and psychosocial health. Furthermore, membership of one of these groups was strongly associated with cardiovascular events. These findings demonstrate the potential to guide interventions towards areas that have lower socioeconomic status across all domains by utilising such a clustered model approach.
These findings also highlight the potency of addressing social welfare as a means to improving cardiovascular outcomes at a state-wide level. Policy targeted at improving cardiovascular outcomes should consider how interventions will address socioeconomic factors – addressing risk factors without mitigating their upstream determinants is likely to be incomplete. Pragmatic modelling which uses areas bounded by a government body, such as in this study, may help identify a locus of control which can be used to effect change. Additionally, larger government units – such as states – may be too big to offer optimal local solutions based on community knowledge that allows acceptable and appropriate strategies to improve socioeconomic measures.
Our study has several limitations. Firstly, analysis was performed at an LGA rather than individual level. While this is useful in describing an area that is subject to a specific governing body, and ultimately for impacting policy, it also precludes a granular understanding of social determinants of health as they relate to the individual. Secondly, our study relies on self-reporting of many variables through computer assisted telephone interviews. This may result in bias in reporting, particularly around sensitive issues of psychosocial wellbeing and income. Our study also analysed hospital admissions at an LGA level which does not adjust for one individual having multiple hospital admissions. Additionally, we did not have detailed information on ethnicity in this study. Ethnicity could be an important factor in the determination of CV events and thus, the model may be incomplete. Lastly, the nature of our study design makes it difficult to infer causality based on our findings. Risk factors take many years to causally affect outcomes and thus a cross-sectional assessment such as this is unable to truly identify whether these socioeconomic domains will impact on future cardiovascular events.
Future work should focus on identifying the modifiable components of socioeconomic factors and effective strategies to improve these factors at a population level. Additionally, non-traditional social determinants such as privilege and institutionalized racism would likely add to the understanding of socioeconomic disadvantage and health. Lastly, ongoing work understanding the biological link between socioeconomic risk and cardiovascular disease is required.
5. Conclusion
In summary, our study demonstrates a strong association between the socioeconomic determinants of financial wellbeing, education levels, psychosocial wellbeing and remoteness and cardiovascular event rates at a local government area level. Additionally, we identified clustering of poor socioeconomic health factors amongst local government areas suggestive of ‘high-risk’ areas which may provide a blueprint for implementing interdisciplinary, policy interventions.
Funding
There was no funding to undertake this study.
Author contribution statement
Drs. Muthalaly, Baradi, Nasis, Wilson and Mehta were responsible for hypothesis generation and study design. Dr. Muthalaly and Ms. O'Regan were responsible for data collection and organisation. Dr. Muthalaly was responsible for data analysis. Drs. Muthalaly and Nelson were responsible for manuscript preparation and submission. Dr. Muthalaly accepts overall responsibility for the manuscript.
Declaration of competing interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Acknowledgements
We would like to acknowledge Safer Care Victoria and the Victorian Department of Health and Human Services for their help in acquiring the data used in this project.
Handling Editor: D Levy
References
- 1.Trends in Cardiovascular Deaths. Australian Institute of Health and Welfare; Canberra: 2017. [Google Scholar]
- 2.Kavanagh A., Bentley R.J., Turrell G., Shaw J., Dunstan D., Subramanian S.V. Socioeconomic position, gender, health behaviours and biomarkers of cardiovascular disease and diabetes. Soc. Sci. Med. 2010;71(6):1150–1160. doi: 10.1016/j.socscimed.2010.05.038. [DOI] [PubMed] [Google Scholar]
- 3.Brown A. Addressing cardiovascular inequalities among indigenous Australians. Global. Cardiology. Science. and. Practice. 2012;2012(1) doi: 10.5339/gcsp.2012.2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Schultz W.M., Kelli H.M., Lisko J.C., et al. Socioeconomic status and cardiovascular outcomes: challenges and interventions. Circulation. 2018;137(20):2166–2178. doi: 10.1161/CIRCULATIONAHA.117.029652. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.The Economic Costs of Obesity: Report for Diabetes Australia. Canberra Access Economics; 2006. [Google Scholar]
- 6.Kestilä P., Magnussen C.G., Viikari J.S.A., et al. Socioeconomic status, cardiovascular risk factors, and subclinical Atherosclerosis in young adults. Arterioscler. Thromb. Vasc. Biol. 2012;32(3):815–821. doi: 10.1161/ATVBAHA.111.241182. [DOI] [PubMed] [Google Scholar]
- 7.Roux A.V.D., Merkin S.S., Arnett D., et al. Neighborhood of residence and incidence of coronary heart disease. N. Engl. J. Med. 2001;345(2):99–106. doi: 10.1056/NEJM200107123450205. [DOI] [PubMed] [Google Scholar]
- 8.Gruenewald T.L., Karlamangla A.S., Hu P., et al. History of socioeconomic disadvantage and allostatic load in later life. Soc. Sci. Med. 2012;74(1):75–83. doi: 10.1016/j.socscimed.2011.09.037. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Levesque J.-F., Harris M.F., Russell G. Patient-centred access to health care: conceptualising access at the interface of health systems and populations. Int. J. Equity. Health. 2013;12(1):18. doi: 10.1186/1475-9276-12-18. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Havranek E.P., Mujahid M.S., Barr D.A., et al. Social determinants of risk and outcomes for cardiovascular disease. Circulation. 2015;132(9):873–898. doi: 10.1161/CIR.0000000000000228. [DOI] [PubMed] [Google Scholar]
- 11.ABS Defining remoteness areas. 2018. https://www.abs.gov.au/ausstats/abs@.nsf/mf/1270.0.55.005
- 12.Thompson R., Miller N., Witter S. Health-seeking behaviour and rural/urban variation in Kazakhstan. Health. Econ. 2003;12(7):553–564. doi: 10.1002/hec.749. [DOI] [PubMed] [Google Scholar]
- 13.Golboni F., Nadrian H., Najafi S., Shirzadi S., Mahmoodi H. Urban-rural differences in health literacy and its determinants in Iran: a community-based study. Aust. J. Rural. Health. 2018;26(2):98–105. doi: 10.1111/ajr.12378. [DOI] [PubMed] [Google Scholar]
- 14.Zahnd W.E., Scaife S.L., Francis M.L. Health literacy skills in rural and urban populations. Am. J. Health. Behav. 2009;33(5):550–557. doi: 10.5993/ajhb.33.5.8. [DOI] [PubMed] [Google Scholar]
- 15.Woodward M., Peters S.A., Batty G.D., et al. Socioeconomic status in relation to cardiovascular disease and cause-specific mortality: a comparison of Asian and Australasian populations in a pooled analysis. BMJ Open. 2015;5(3) doi: 10.1136/bmjopen-2014-006408. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Gerber Y., Weston S.A., Killian J.M., et al. Neighborhood income and individual education: effect on survival after myocardial infarction. Mayo. Clin. Proc. 2008;83(6):663–669. doi: 10.4065/83.6.663. [DOI] [PMC free article] [PubMed] [Google Scholar]