Abstract
Objectives
This study aimed to measure (1) the proportion of children who continue to receive specialist care (rheumatology/ophthalmology) as adults, (2) the characteristics associated with continuing specialist care, and (3) the frequency of specialist care appointments in both paediatric and adult services.
Methods
A retrospective cohort of young people with JIA was identified from UK primary care electronic health records (Clinical Practice Research Datalink) between 1 April 2003 and 31 December 2018. To be included in the study, cases needed to have at least 1 year of registration at their general practice beyond age 18 and linkage to Hospital Episodes Statistics data for secondary care information. All specialist care outpatient visits were identified from Hospital Episodes Statistics outpatient data.
Results
There were 666 young people included in the study. Of these, 427 (64%) received specialist care beyond age 18, 90 (13%) had their last recorded contact at 16–17 years and 149 (22%) did not continue after 16 years. Older age at diagnosis, female gender, less deprivation and a childhood diagnosis of uveitis were associated with continuing specialist care beyond age 18. Of those continuing beyond 18, 35% (n = 153) were subsequently discharged by the study end date. Of all those discharged, 32% had a missed appointment recorded after the last attended visit, suggesting failure to attend.
Conclusions
Two-thirds of young people with JIA continue to receive specialist care beyond age 18. This is useful information for children and young people with JIA and their families planning for their future, and for clinicians planning health-care services.
Keywords: JIA, healthcare utilization, epidemiology, outcomes research, adolescent medicine
Rheumatology key messages.
Two in three young people with JIA continue to attend hospital services beyond age 18.
Female gender, less deprivation and comorbid uveitis were associated with ongoing specialist care beyond age 18.
This study provides unique estimates of health-care utilization in young people with JIA.
Introduction
JIA describes inflammatory arthritis that occurs in one or more joints prior to age 16 [1]. While a proportion of children will achieve drug-free remission during childhood, others will continue to have active disease or require long-term anti-rheumatic medications and require specialist care as adults. Estimates of the proportion continuing under specialist care as adults vary and may be outdated, with many studies now >20 years old [2–4]; notably, classification, treatment and management of JIA has changed significantly in this time. These studies have typically focused on clinical measures such as clinical remission, often at a single time point in a select group of adults with JIA, rather than specifically around the time of transfer to adult services [2–8].
A young person transfers from paediatric to adult rheumatology services by age 18 in the UK. This therefore occurs simultaneously with a number of other well-recognized major developmental changes in a young person’s life, including physical, psychological and social changes (such as going on to college, university or work and leaving home) [9]. Alongside this, the way health care is delivered may differ between paediatric and adult care. As recommended by the EULAR/Paediatric Rheumatology European Society (PReS), young people need guidance to ensure they can manage their condition independently as an adult, addressing not only their medical needs but also their psychosocial, educational and vocational needs [10]. There have been studies indicating that many young people are not seen by an adult rheumatologist despite referral from paediatric rheumatology, potentially resulting in worse outcomes [11, 12]. Studies often focus on young people who are still under specialist care at the time of transfer to adult services, rather than understanding the proportion of all patients diagnosed with JIA who continue into adult services, thus biasing any results towards a more extreme phenotype. It is unknown how frequently young people with JIA in the UK continue under specialist care into adulthood or how their engagement with health-care services changes. To address this evidence gap, this study aimed to measure (1) the proportion of children with JIA who continue to receive specialist care (rheumatology/ophthalmology) as adults, (2) identify the characteristics associated with continuing specialist care and (3) determine the frequency of specialist care appointments in both paediatric and adult services.
Methods
Design
This investigation was a retrospective cohort study of young people with JIA in the UK.
Setting
Data was obtained from the Clinical Practice Research Datalink (CPRD), a large research database of primary care electronic health records. The CPRD database has two sections: CPRD GOLD, which contains data collected from primary care practices using Vision® software [13], and CPRD Aurum which contains data collected from primary care practices using EMIS® software [14]; combined, these sections contain information for 15 million patients as of November 2021. Twenty percent of practices in GOLD switched from Vision to EMIS software over the course of the study, so their patients would appear in both the GOLD and Aurum databases, resulting in duplicate records. When this occurred, only the practice data from Aurum was used, because the follow-up is generally longer in this database. For practices in the UK that consented to linkage, the CPRD data was linked to Hospital Episode Statistics (HES) data—a dataset that includes coded data on admissions and diagnoses (for inpatients) as a well as medical specialty, and attendence at any outpatient specialty hospital appointments. Although rheumatology and ophthalmology care in the UK is typically delivered through outpatient clinics in hospital settings, all diagnoses are recorded in a patient’s primary care record using Read codes. The study period was from 1 April 2003 (when HES outpatient data became available) to 31 December 2018. The study was approved by the CPRD Independent Scientific Advisory Committee (Protocol no. 19_060).
Study population
Young people with a Read code for JIA were identified from the CPRD data (see Supplementary Table S1, available at Rheumatology online) and, in line with previous research on this dataset [15], were considered validated cases for inclusion if they met either of the following criteria:
Attended ≥3 HES outpatient specialist care appointments, where specialist care refers to paediatric rheumatology, rheumatology or ophthalmology only, prior to age 16
HES inpatient admission with a JIA ICD-10 code, prior to age 16.
Further, cases needed to have: (1) registration at the same general practice (GP) from prior to age 16 years until at least 1 year beyond age 18 and (2) at least one outpatient specialist care appointment at any time. Both incident and prevalent cases were included. Cases were considered incident if they had at least 1 year of registration at their GP prior to their first JIA Read code (unless they were under 2 years old) and their first code was within the study period; otherwise, they were considered prevalent. Incident cases entered the study at the first Read code. Prevalent cases entered at: (1) start of GP registration if the first Read code was prior to this, due to their diagnosis being prior to registration at that GP practice, (2) the start of the study period, or (3) the first Read code if this was within 1 year of GP registration. For those cases for whom the first HES specialist care appointment occurred prior to these dates, the study entry date was the first HES specialist care appointment. HES data was checked to ensure there were no duplicate patients appearing at different GP practices. All cases were followed until leaving their GP, death or 31 December 2018, whichever occurred first.
Specialist care variables
All specialist care outpatient appointments were identified from HES outpatient data. The age at each appointment and the number of (1) rheumatology and (2) ophthalmology appointments per year of age was determined. Continuity of specialist care was categorized into three groups by age of last specialist care appointment: prior to 16 years, 16–17 years, and 18 years and beyond. Young people were considered discharged from specialist care (a proxy for disease remission) if they had >1 year between the last specialist appointment attended and the end of study follow-up. Young people were considered to have a gap in care if there was at least 1 year between specialist care appointments attended, with care restarting.
Demographic and comorbidity variables
Age and gender at first JIA code were identified. To determine whether patients with JIA and other chronic diseases were more likely to stay under specialist care, the following comorbidities were also identified if they had ≥1 Read code for the condition prior to age 18: asthma, inflammatory bowel disease, psoriasis, depression/anxiety and/or uveitis (codes listed in Supplementary Tables S2–S11, available at Rheumatology online). Deprivation was measured through patient level linkage to Indices of Multiple Deprivation (IMD) 2015 quintiles data [16], and IMD quintiles were further categorized as 1 (most deprived) vs 2/3 vs 4/5 (least deprived). The Indices of Deprivation are a measure of relative deprivation at a small local area level across the UK, based on seven different domains: income; employment; education, skills and training; health and disability; crime; housing and services; environment. Young people were also classified as living in a rural or urban neighbourhood based on a rural–urban classification of their GP practice location. Ethnicity was identified from HES data; for those young people for whom multiple ethnicities were recorded, the most frequent ethnicity recorded was used.
Analysis
The baseline characteristics were described, stratified by continuing specialist care category. A multinomial logistic regression model was used to assess whether any demographic or comorbidity variables were associated with the continuing specialist care category. The number of appointments per year of age was plotted in a box plot. Appointments attended, appointments missed, discharges, and gaps in specialist care attendance were described. For incident cases, time to discharge, stratified by age at diagnosis category, was plotted in a Kaplan–Meier curve.
Results
There were 666 young people eligible for this study (118 GOLD and 548 Aurum) (Fig. 1). The young people in this cohort were most frequently diagnosed between the ages of 9 and 15 years, 60% were female, 89% were Caucasian, and comorbidities were uncommon. The cohort was followed until a median age of 22 years, with a range of 19–30 years (Table 1).
Figure 1.
Flowchart of case definition in CPRD GOLD and Aurum. aValidation = either ≥3 Hospital Episode Statistics (HES) outpatient specialist care (rheumatology/ophthalmology) appointments or a HES inpatient admission coded with JIA, prior to age 16 years
Table 1.
Baseline characteristics of the cohort (N = 666)
| Characteristics | Overall | Specialist care until age <16 years | Specialist care until age 16–17 years | Specialist care after ≥age 18 years | |
|---|---|---|---|---|---|
| N (%) | 666 (100%) | 149 (22.4%) | 90 (13.5%) | 427 (64.1%) | |
| Age at end of GP follow-up [median (IQR)] | 22.0 (20.0, 25.0) | 21.0 (20.0, 24.0) | 21.0 (20.0, 24.0) | 22.0 (20.0, 25.0) | |
| Number with GP follow-up beyond age 25 years (%) | 124 (18.6) | 20 (13.4) | 11 (12.2) | 93 (21.8) | |
| Demographics and comorbidities | |||||
| Age at first JIA codeb (%) | 0–3 years | 90 (13.5) | 22 (14.8) | 6 (6.7) | 62 (14.5) |
| 4–8 years | 167 (25.1) | 43 (28.9) | 18 (20.0) | 106 (24.8) | |
| 9–15 years | 409 (61.4) | 84 (56.4) | 66 (73.3) | 259 (60.7) | |
| Gender (%) | Male | 274 (41.1) | 76 (51.0) | 39 (43.3) | 159 (37.2) |
| Female | 392 (58.9) | 73 (49.0) | 51 (56.7) | 268 (62.8) | |
| Ethnicity (%) | Caucasian | 592 (88.9) | 131 (87.9) | 79 (87.8) | 382 (89.5) |
| IMD 2015 (%) | 1 (most deprived) | 143 (21.5) | 44 (29.5) | 14 (15.6) | 85 (19.9) |
| 2/3 | 254 (38.1) | 47 (31.5) | 34 (37.8) | 173 (40.5) | |
| 4/5 | 269 (40.4) | 58 (38.9) | 42 (46.7) | 169 (39.6) | |
| Urban-rural classification (%) | Urban | 591 (88.7) | 134 (89.9) | 76 (84.4) | 381 (89.2) |
| Rural | 75 (11.3) | 15 (10.1) | 14 (15.6) | 46 (10.8) | |
| Comorbidities prior to 18 (%) | Asthma | 130 (19.5) | 31 (20.8) | 28 (31.1) | 71 (16.6) |
| Inflammatory bowel disease | 12 (1.8) | ≤5a | ≤5a | 9 (2.1) | |
| Psoriasis | 28 (4.2) | ≤5a | ≤5a | 19 (4.4) | |
| Depression/anxiety | 45 (6.8) | 12 (8.1) | 8 (8.9) | 25 (5.9) | |
| Uveitis | 77 (11.6) | ≤5a | ≤5a | 61 (14.3) | |
| Discharge information | |||||
| Dischargedc (%) | No | 274 (41.1) | 0 (0.0) | 0 (0.0) | 274 (64.2) |
| Yes | 392 (58.9) | 149 (100.0) | 90 (100.0) | 153 (35.8) | |
| Of those considered discharged, n (%) who did not attend last scheduled appointment | 126 (32.1%) | 43 (28.9) | 33 (36.7) | 50 (32.7) | |
| Age at last rheumatology appointment attended if discharged (median [IQR]) | 16.8 [14.6, 18.9] | 14.0 [12.7, 15.2] | 16.8 [16.3, 17.4] | 19.7 [18.4, 22.2] | |
| Age at last ophthalmology appointment attended if discharged (median [IQR]) | 14.8 [12.9, 17.1] | 13.1 [11.3, 14.2] | 14.9 [13.4, 16.3] | 18.0 [15.6, 20.0] | |
| Age at last outpatient appointment attended if discharged (rheumatology or ophthalmology) (median [IQR]) | 17.0 [14.8, 19.0] | 14.0 [12.8, 15.2] | 16.9 [16.5, 17.4] | 20.2 [18.7, 22.5] | |
GP: general practice; IMD: Index of Multiple Deprivation; IQR: interquartile range.
Unable to present values for strata n ≤ 5 for ethical reasons.
As prevalent cases are included, the first JIA code may have occurred before 2003, if the patients subsequently met case definition criteria.
At least 1 year between last attended appointment and end of GP registration.
Sixty-four percent (n = 427) continued to attend specialist care beyond age 18, 13.4% (n = 90) were discharged at age 16–17 years and 22.4% (n = 149) were discharged prior to the age of 16 years (Table 1). Initial inspection of the characteristics within each category indicated that, in those who continued specialist care beyond age 18, (i) their age at the first code had a similar distribution compared with those who were discharged prior to age 16, (ii) they were more frequently female (63% vs 49%) and (iii) they were more likely to have had a diagnosis of uveitis (14% vs <10%). Asthma and depression/anxiety were less common in those who continued specialist care beyond age 18 years (16.6% vs 24.7% and 5.9% vs 8.3%, respectively). Compared with those discharged prior to age 16 years, those who were discharged at age 16–17 years were more frequently older at diagnosis, had greater deprivation, more frequently lived in a rural location (16% vs 10%) and more frequently had asthma (31% vs 21%) (Table 1).
Characteristics associated with continuing specialist care into adulthood
In univariate multinomial logistic regression models, increasing age at diagnosis, female gender and less deprivation were associated with remaining under specialist care beyond age 18 years compared with those not remaining under specialist care beyond age 16 years. In adjusted multinomial logistic regression, these associations remained, with the addition of an association with a diagnosis of uveitis. Uveitis had the strongest association, with 2-fold higher odds of remaining under specialist care beyond age 18 years [odds ratio (OR) 2.23; 95% CI 1.14, 4.35] compared with those discharged prior to age 16 years. Age at diagnosis (OR 1.14 per year increase; 95% CI 1.07, 1.23) and less deprivation [OR for groups 4/5 vs 1 (most deprived) 2.4; 95% CI 1.14, 5.04] were associated with remaining under specialist care till age 16–17 years compared with those discharged prior to age 16 years (Table 2 and Fig. 2).
Table 2.
Multinomial logistic regression—factors associated with continuing specialist care category
| Model | Crude | Age and gender adjusted | Fully adjusted | |||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Outcome category | Specialist care until <16 years | Specialist care at ≥16 to <18 years | Specialist care until >18 years | Specialist care until <16 years | Specialist care at ≥16 to <18 years | Specialist care until age >18 years | Specialist care until age <16 years | Specialist care until age 16–17 years | Specialist care beyond age 18 years | |
| Age at first code | Reference | 1.14 (1.06, 1.22) | 1.04 (1, 1.09) | Reference | 1.14 (1.07, 1.22) | 1.05 (1, 1.1) | Reference | 1.14 (1.07, 1.23) | 1.07 (1.02, 1.12) | |
| Gender | Female | 1.36 (0.8, 2.3) | 1.75 (1.2, 2.56) | 1.49 (0.87, 2.54) | 1.83 (1.25, 2.68) | 1.48 (0.85, 2.56) | 1.84 (1.25, 2.72) | |||
| Comorbidities prior to age 18 | Asthma | 1.72 (0.95, 3.12) | 0.76 (0.47, 1.22) | 1.58 (0.85, 2.93) | 0.73 (0.45, 1.19) | |||||
| Depression/anxiety | 1.11 (0.44, 2.84) | 0.71 (0.35, 1.45) | 0.76 (0.28, 2.04) | 0.6 (0.28, 1.27) | ||||||
| Uveitis | 0.53 (0.17, 1.7) | 1.9 (0.99, 3.64) | 0.73 (0.22, 2.39) | 2.23 (1.14, 4.35) | ||||||
| IMD | 1 (Most deprived) | Reference | Reference | Reference | Reference | |||||
| 2 & 3 | 2.27 (1.08, 4.79) | 1.91 (1.17, 3.1) | 2.33 (1.09, 5) | 1.97 (1.2, 3.25) | ||||||
| 4 & 5 | 2.28 (1.11, 4.68) | 1.51 (0.94, 2.41) | 2.4 (1.14, 5.04) | 1.54 (0.95, 2.5) | ||||||
| Urban-rural | Urban | Reference | Reference | Reference | Reference | |||||
| Rural | 1.65 (0.75, 3.59) | 1.08 (0.58, 2) | 1.81 (0.79, 4.13) | 1.11 (0.58, 2.11) | ||||||
Figure 2.
Multinomial logistic regression—factors associated with continuing specialist care category
Discharge
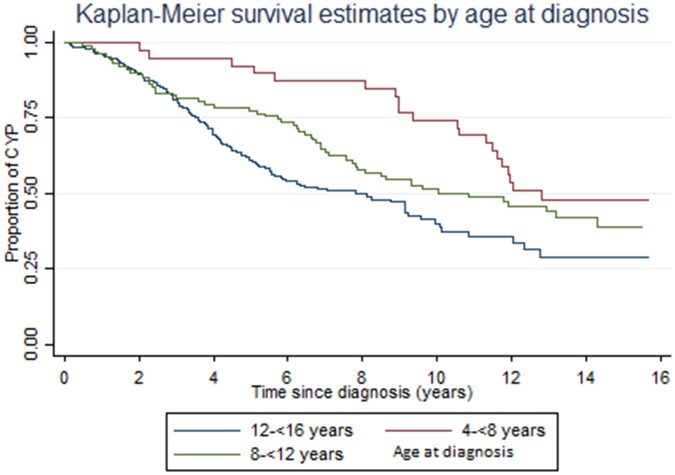
Of those who remained under specialist care beyond age 18 years, 35.8% (n = 153/427) were later identified as discharged prior to the end of follow-up, with an average age of 20 years at their last appointment prior to discharge. When incident cases were stratified by age at diagnosis, those diagnosed at an older age were discharged sooner than those diagnosed at a younger age, for example, it was 12 years until 50% were discharged in those diagnosed at age 4 to <8 years, compared with 7 years in those diagnosed at age 12 to <16 years (Fig. 3). Of those considered discharged, 126 (32.1%) had failed to attend an appointment after the last attended appointment.
Figure 3.
Kaplan–Meier survival curve for time in specialist care vs age at diagnosis. CYP: Children and Young People
Frequency of appointments and gaps in care
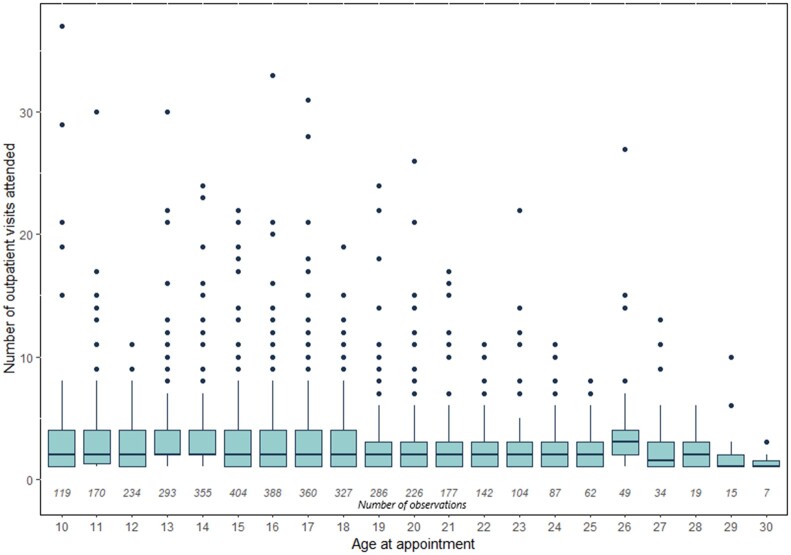
The number of appointments in rheumatology per year of age was similar across all ages, with a median of two appointments per year, but with a wider range below age 18 years (Fig. 4). Overall, young people failed to attend 11% of rheumatology appointments, and the proportion was slightly higher in those age ≥18 years. Gaps in care between appointments longer than 1 year were experienced by 354/666 (53%) young people during the study period. However, these were infrequent overall, affecting only 5% (n = 619/12 074) of all rheumatology appointments, meaning most young people only experienced such a long gap between appointments once. The median age at the end of a gap was 18 years (interquartile range: 15–21 years).
Figure 4.
Frequency of rheumatology appointments vs age
Discussion
This study found that two in three young people with JIA continued to be seen in specialist care beyond age 18 years. Factors associated with remaining under specialist care included female gender, greater deprivation, and a diagnosis of uveitis. Despite the high proportion of patients continuing to see a specialist after age 18 years, a third of those young people were subsequently discharged, with an average age of 20 years at their last appointment. Another important finding is that a large proportion, roughly one in three (36%), were discharged prior to age 18 years and were not seen again in specialist care.
These data are somewhat in contrast with previous data on the proportion of patients whose disease persists into adulthood. For example, we showed that two-thirds of patients continue to attend specialist appointments after the age of 18 years; this is higher than the frequently cited figure that JIA continues into adulthood in at least one-third of patients [2]. However, that earlier estimate was based on studies describing the proportion of patients in clinical remission when followed up in adulthood, and the underlying estimates of remission vary considerably between 30% and 65% [2–5, 13–15]. In our study, patients may be in clinical remission as adults but, due to the nature of medications they are still receiving, such as biologics or MTX, they will require continued monitoring under a specialist. Others may have persistent inflammation, or persistent symptoms (e.g. pain) in the absence of inflammation, which still requires specialist input. Finally, our analyses also included ophthalmology, recognizing the importance of uveitis as an important comorbidity within JIA. Young people may therefore have continued with ophthalmology review due to previous damage or ongoing uveitis, even if their joints are in remission. However, only a small number of young people (n = 15) continued with adult ophthalmology services but no adult rheumatology input. In a similar study, Luque Ramos et al. described health-care utilization in early adulthood for patients with JIA in Germany, using electronic claims data. They found that 31% of patients were still seen in adult services at age 20 years [17]. This is slightly lower than our findings of 41% continuing to be seen in adult services at a median age of 22 years by the end of the study period. It is possible that patients in the UK are more likely to continue care due to the government-funded National Health Service than patients in Germany, where there is an insurance-based system.
The association with gender identified in this study may relate to differences in gender distribution within the JIA ILAR categories. For example, RF-positive polyarthritis is more common in female patients, has a later age of onset and is more likely to be associated with persistent disease [18]. Unfortunately, the ILAR category is not recorded in CPRD. Alternatively, there is some evidence for males having more gaps in care when moving from paediatric to adult care in chronic conditions more broadly [19], which could also explain this finding. Greater deprivation has been associated with persistent disease in childhood [20]; our study however our study suggests that YP from the least deprived backgrounds are most liekly to continue to access care into adulthood, though the strongest associations were seen in those discharged at age 16–17 years. There were similar findings in a study of young people with a range of chronic conditions, where higher income was associated with reduced odds of care gaps [19]. Interpretation is difficult with this data, as we do not know the reason for young people meeting our criteria of discharge; patients could be lost to follow-up, in remission, or have moved to another area and therefore changed their GP. Overall, 32% of those discharged did not attend their last appointment, indicating potential gaps in care. As mentioned above, late adolescence is characterized by significant educational and social transitions that young people have to navigate. Therefore, when young people with chronic conditions such as JIA also have to navigate health-care transitions, it is concerning, but perhaps not surprising, that challenges and loss to follow-up occur in some cases.
There were some indications in our study that young people with depression and anxiety were less likely to continue with specialist care into adult services. Of those who did continue under specialist care beyond age 18 years, just under 6% had a diagnosis of depression or anxiety recorded in their GP record; in contrast, it is estimated that in the general population 14.9% of 17–19-year-olds have an emotional disorder including depression and anxiety [21]. Within our cohort, those continuing under specialist care beyond 18 years had the least depression and anxiety compared with those leaving specialist care at the earlier ages, although the differences were relatively small and not statistically significant. Further, our study relied on Read codes to identify depression and anxiety; thus, there may have been some misclassification in this diagnosis. Nevertheless, this result warrants further investigation. In particular, it may suggest that young people with depression/anxiety are more frequently lost to follow-up as they enter adult services because their mental health problems make this transition more challenging. Due to the age of the cohort, there was limited follow-up beyond age 22 years, so it is unknown whether these same patients may re-present to rheumatology at a later date.
It was interesting to note that those diagnosed at a younger age were seen in specialist care for longer than those diagnosed at an older age. A review of the number of appointments by age did not indicate that patients were seen more frequently in paediatric care. This may suggest that establishing a relationship with young people is important for enhancing engagement with health-care services over the long term, and may increase the likelihood of young people continuing to engage with services as they move into the adult health-care sphere. As ILAR category was not recorded, it is also possible that some of the youngest patients were more likely to have polyarthritis that may be more likely to persist or require long-term medications.
This study has some limitations. Information on JIA subtypes, disease activity and clinical remission is not available within CPRD or HES, so we could not tell whether patients were lost to follow-up, patients were discharged due to being in drug-free remission, or whether ongoing active disease was the driver for young people staying in specialist care as seen in previous studies [18]. Although there is some treatment information within CPRD data, many treatments, such as biologics, are prescribed in secondary care and are not captured within HES data, and therefore we have not presented any treatment information. Also, although 96% of young people aged 16–24 years are registered with a GP [22], since we required patients to remain with the same GP until at least 19 years of age there is the possibility of selection bias, as these patients may represent a specific group who did not move location.
Conclusions
This study provides a unique insight into health-care utilization in a large sample of young people with JIA in the UK. This important information will allow clinicians to communicate with young people with JIA and their families about the long-term future of their disease, and will be invaluable for health-care providers running, developing and planning developmentally appropriate adolescent and young adult services (including effective transitional care) in paediatric and adult rheumatology.
Supplementary data
Supplementary data are available at Rheumatology online.
Supplementary Material
Contributor Information
Ruth E Costello, Centre for Epidemiology Versus Arthritis, Division of Musculoskeletal Medicine and Dermatological Sciences, University of Manchester, Manchester Academic Health Sciences Centre, Manchester, UK.
Lianne Kearsley-Fleet, Centre for Epidemiology Versus Arthritis, Division of Musculoskeletal Medicine and Dermatological Sciences, University of Manchester, Manchester Academic Health Sciences Centre, Manchester, UK.
Janet E McDonagh, Centre for Epidemiology Versus Arthritis, Division of Musculoskeletal Medicine and Dermatological Sciences, University of Manchester, Manchester Academic Health Sciences Centre, Manchester, UK; NIHR Manchester Biomedical Research Centre, Manchester University Hospitals NHS Trust, Manchester, UK; Department of Paediatric and Adolescent Rheumatology, Royal Manchester Children’s Hospital, Manchester University Hospitals NHS Trust, Manchester, UK.
Kimme L Hyrich, Centre for Epidemiology Versus Arthritis, Division of Musculoskeletal Medicine and Dermatological Sciences, University of Manchester, Manchester Academic Health Sciences Centre, Manchester, UK; NIHR Manchester Biomedical Research Centre, Manchester University Hospitals NHS Trust, Manchester, UK; Kellgren Centre for Rheumatology, Manchester Royal Infirmary, Manchester University Hospitals NHS Trust, Manchester, UK.
Jenny H Humphreys, Centre for Epidemiology Versus Arthritis, Division of Musculoskeletal Medicine and Dermatological Sciences, University of Manchester, Manchester Academic Health Sciences Centre, Manchester, UK; Kellgren Centre for Rheumatology, Manchester Royal Infirmary, Manchester University Hospitals NHS Trust, Manchester, UK.
Data availability statement
The data used in this study were sourced from the Clinical Practice Research datalink, as part of CPRD protocol 19_060. This protocol can be found on their website (https://cprd.com/) where an application can be made to access the data.
Funding
This study was supported by an Academy of Medical Sciences Starter Grant for Clinical Lecturers (Ref: SGL020\1047). K.L.H. and J.E.M. are supported by the NIHR Manchester Biomedical Research Centre. J.E.M. and R.E.C. are supported by the Vs Arthritis Centre for Epidemiology (UK Grant No: 21755) and the NIHR Manchester Biomedical Research Centre.
Disclosure statement: K.L.H. has received non-personal speaker’s fees from Abbvie and grant income from BMS, UCB, and Pfizer, all unrelated to this manuscript. J.E.M. has received consultancy fees from Pfizer and CSL-Behring. R.E.C. has personal shares in AstraZeneca. All other authors have declared no conflicts of interest.
References
- 1. Petty RE, Southwood TR, Manners P. et al. International League of Associations for Rheumatology classification of juvenile idiopathic arthritis: second revision, Edmonton, 2001. J Rheumatol 2004;31:390–2. [PubMed] [Google Scholar]
- 2. Zak M, Pedersen FK.. Juvenile chronic arthritis into adulthood: a long‐term follow‐up study. Rheumatology 2000;39:198–204. [DOI] [PubMed] [Google Scholar]
- 3. Oen K, Malleson PN, Cabral DA. et al. Disease course and outcome of juvenile rheumatoid arthritis in a multicenter cohort. J Rheumatol 2002;29:1989–99. [PubMed] [Google Scholar]
- 4. Koivuniemi R, Leirisalo-Repo M.. Juvenile chronic arthritis in adult life: a study of long-term outcome in patients with juvenile chronic arthritis or adult rheumatoid arthritis. Clin Rheumatol 1999;18:220–6. [DOI] [PubMed] [Google Scholar]
- 5. Selvaag AM, Aulie HA, Lilleby V. et al. Disease progression into adulthood and predictors of long-term active disease in juvenile idiopathic arthritis. Ann Rheum Dis 2016;75:190–5. [DOI] [PubMed] [Google Scholar]
- 6. Vidqvist KL, Malin M, Varjolahti-Lehtinen T. et al. Disease activity of idiopathic juvenile arthritis continues through adolescence despite the use of biologic therapies. Rheumatology 2013;52:1999–2003. [DOI] [PubMed] [Google Scholar]
- 7. Bertilsson L, Andersson-Gäre B, Fasth A. et al. Disease course, outcome, and predictors of outcome in a population-based juvenile chronic arthritis cohort followed for 17 years. J Rheumatol 2013;40:715–24. [DOI] [PubMed] [Google Scholar]
- 8. Chhabra A, Robinson C, Houghton K. et al. Long-term outcomes and disease course of children with juvenile idiopathic arthritis in the ReACCh-Out cohort: a two-centre experience. Rheumatology 2020;59:3727–30. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9. Christie D, Viner R.. Adolescent development. BMJ 2005;330:301–4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10. Foster HE, Minden K, Clemente D. et al. EULAR/PReS standards and recommendations for the transitional care of young people with juvenile-onset rheumatic diseases. Ann Rheum Dis 2017;76:639–46. [DOI] [PubMed] [Google Scholar]
- 11. Hazel E, Zhang X, Duffy CM. et al. High rates of unsuccessful transfer to adult care among young adults with juvenile idiopathic arthritis. Pediatr Rheumatol 2010;8:2–6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12. Hersh A, Von Scheven E, Yelin E.. Adult outcomes of childhood-onset rheumatic diseases. Nat Rev Rheumatol 2011;7:290–5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13. Herrett E, Gallagher AM, Bhaskaran K. et al. Data resource profile: Clinical Practice Research Datalink (CPRD). Int J Epidemiol 2015;44:827–36. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14. Wolf A, Dedman D, Campbell J. et al. Data resource profile: Clinical Practice Research Datalink (CPRD) Aurum. Int J Epidemiol 2019;48:1740–40g. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15. Costello R, McDonagh J, Hyrich KL. et al. Incidence and prevalence of juvenile idiopathic arthritis in the United Kingdom, 2000–2018: results from the Clinical Practice Research Datalink. Rheumatology 2021;61:2548–54. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16. Smith T, Noble M, Noble S. et al. The English Indices of Deprivation 2015: technical report. 2015. https://www.gov.uk/government/publications/english-indices-of-deprivation-2015-technical-report (January 2022, date last accessed).
- 17. Luque Ramos A, Hoffmann F, Albrecht K. et al. Transition to adult rheumatology care is necessary to maintain DMARD therapy in young people with juvenile idiopathic arthritis. Semin Arthritis Rheum 2017;47:269–75. [DOI] [PubMed] [Google Scholar]
- 18. Guzman J, Oen K, Tucker LB. et al. The outcomes of juvenile idiopathic arthritis in children managed with contemporary treatments: results from the ReACCh-Out cohort. Ann Rheum Dis 2015;74:1854–60. [DOI] [PubMed] [Google Scholar]
- 19. Goossens E, Bovijn L, Gewillig M. et al. Predictors of care gaps in adolescents with complex chronic condition transitioning to adulthood. Pediatrics 2016;137:e20152413. [DOI] [PubMed] [Google Scholar]
- 20. Shoop-Worrall SJW, Hyrich KL, Wedderburn LR. et al. ; CAPS the CLUSTER Consortium. Patient-reported wellbeing and clinical disease measures over time captured by multivariate trajectories of disease activity in individuals with juvenile idiopathic arthritis in the UK: a multicentre prospective longitudinal study. Lancet Rheumatol 2021;3:e111–21. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21. Sadler K, Vizard T, Ford T. et al. Mental Health of Children and Young People in England, 2017: Trends and characteristics. 2018. https://digital.nhs.uk/data-and-information/publications/statistical/mental-health-of-children-and-young-people-in-england/2017/2017 (7 January 2022, date last accessed).
- 22. Lifestyles Team, NHS Digital. Health Survey for England 2019. 2020. https://digital.nhs.uk/data-and-information/publications/statistical/health-survey-for-england/2019/main-findings#use-of-health-care-services (31 January 2022, date last accessed).
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Data Availability Statement
The data used in this study were sourced from the Clinical Practice Research datalink, as part of CPRD protocol 19_060. This protocol can be found on their website (https://cprd.com/) where an application can be made to access the data.