Abstract
Being immune privileged, the central nervous system (CNS) is constituted by unique parenchymal and non-parenchymal tissue-resident macrophages, namely, microglia and border-associated macrophages (BAMs), respectively. BAMs are found in the choroid plexus, meningeal and perivascular spaces, playing critical roles in maintaining CNS homeostasis while being phenotypically and functionally distinct from microglial cells. Although the ontogeny of microglia has been largely determined, BAMs need comparable scrutiny as they have been recently discovered and have not been thoroughly explored. Newly developed techniques have transformed our understanding of BAMs, revealing their cellular heterogeneity and diversity. Recent data showed that BAMs also originate from yolk sac progenitors instead of bone marrow-derived monocytes, highlighting the absolute need to further investigate their repopulation pattern in adult CNS. Shedding light on the molecular cues and drivers orchestrating BAM generation is essential for delineating their cellular identity. BAMs are receiving more attention since they are gradually incorporated into neurodegenerative and neuroinflammatory disease evaluations. The present review provides insights towards the current understanding regarding the ontogeny of BAMs and their involvement in CNS diseases, paving their way into targeted therapeutic strategies and precision medicine.
Keywords: CNS border-associated macrophages, tissue-resident macrophages, origin, yolk sac, molecular cues, development, disease
1. Introduction
The central nervous system (CNS) is considered immune-privileged as the blood–brain barrier (BBB) prevents its overexposure to external pathogens [1]. The CNS homeostasis is also maintained by immune cells, such as tissue-resident macrophages neutralizing noxious factors that are potentially harmful due to neurons’ limited capacity for renewal [2,3]. For a long time, microglia were referred to as the main and only innate immune cells of the CNS [4]. Recently, another population of tissue-resident macrophages was distinguished from the parenchymal macrophages of the CNS [5]. These cells are called CNS border-associated macrophages (BAMs) or CNS-associated macrophages (CAMs), first described as perivascular phagocytes in rats, and are located in the non-parenchymal region of CNS [6,7]. Specifically, the meninges, choroid plexus and perivascular spaces of the brain are populated by BAMs [8].
The single-cell analysis and fate-mapping in transgenic animal models facilitate the detection of microglia and BAMs, shedding light on the cells’ molecular identity without the need for irradiation in the experimental protocols [5,9,10,11,12,13]. Indeed, BAMs were clustered in different groups depending on their anatomical positions, revealing each subset’s heterogeneity [14,15]. Specifically, ΒAMs are divided into subdural/leptomeningeal macrophages (sdΜΦ), dural macrophages (dmΜΦ), stromal choroid plexus macrophages (cpΜΦ), choroid epiplexus macrophages (cpepiΜΦ), also known as Kolmer’s cells, and perivascular macrophages (pvΜΦ) [14]. The subpopulations of BAMs generally vary in morphology, motility, and function. Although BAMs display differences in their transcriptional profiles and dynamics, their functional diversity in each anatomical location has yet to be fully elucidated [16].
The overview of the origin of CNS macrophages has radically evolved during the last decades. In the past, all tissue-specific macrophages were considered to be derived from bone marrow progenitors [17,18,19]. However, according to recent data from studies that have utilized new genetic tools, the early perception that tissue-resident macrophages derive solely from adult blood circulating monocytes is no longer prevalent [8,11,20,21,22,23,24]. Although several studies have investigated the role of microglia in neuroinflammation and neurodegenerative diseases, such as Alzheimer’s disease, Parkinson’s disease and multiple sclerosis, little is known about the contribution of BAMs in these pathophysiological patterns [25,26,27,28,29,30]. There are apparent limitations to elucidating the contribution of BAMs in neurological disease; the exact pathophysiological role of BAMs and other CNS-innate immune cells cannot be interpreted by the majority of available tools; therefore, the distinction of BAMs from microglia under disease remains challenging [12,31]. Nevertheless, data obtained via contemporary technologies indicate their potential involvement and miscellaneous phenotypes in neurodegenerative and neuroinflammatory CNS diseases [5,12,32,33,34,35,36].
This review primarily aims to present the origin of BAMs in the fetal and postnatal period, the molecular cues which drive BAM generation, the principal distinction from microglia, and the implication of BAMs in various CNS disease conditions.
2. Origin of BAMs during Embryogenesis and Adulthood
The BAM embryonic origin was first investigated in rodents using bone marrow chimeras and whole-body irradiation, proposing that BAMs are bone marrow-derived [37,38]. In 2016, Goldmann et al., performing fate mapping analysis, observed that BAMs originate from the mouse yolk sac’s early erythro-myeloid progenitors (EMPs) during embryogenesis [8]. A tamoxifen-inducible Runx1CreERR26YFPfate-mapping mouse model confirmed that BAMs originate from early EMPs in the yolk sac, which gave rise to two different macrophage populations, namely, CD206+ (BAM progenitors) and CD206− (microglial progenitors) without the contribution of fetal liver or definitive hematopoiesis [20]. Interestingly, the mannose receptor C-type 1 (MRC1 or CD206) is a unique marker for BAMs [8,12,14]. The expression of Mrc1 is upregulated from E8.5 when the primitive macrophages, originating from EMPs, prepare to invade the embryonic tissues [39]. Recently, Masuda et al. investigated the progenitors of BAMs utilizing single-cell RNA sequencing and fate mapping analysis in the Mrc1CreERT2 mouse model. Although flow cytometry confirmed the presence of a CD206+ subpopulation within the A2 cells (CD45+ c-kit− CX3CR1+ cells), meningeal macrophages and microglia were found to originate from common CD206+ A2 progenitors in contrast with previous results [20,40]. The pvΜΦ were generated postnatally from sdΜΦ, requiring integrin-signaling and vascular smooth muscle cells (VSMCs) [40].
Regarding the repopulation pattern of BAMs in adulthood, there is a great heterogeneity between BAM clusters; specifically, the sdΜΦ, pvMΦ and cpepiΜΦ exhibit similar longevity with microglial cells as being self-maintained in the CNS independently from blood monocytes’ contribution [8,14]. The cpepiΜΦ were solely derived from local SALL1+ macrophages [14]. In Ccr2-deficient mice, the number of cpMΦ decreased, revealing their replenishment from Ly6Chi monocytes and shorter turnover [8]. In accordance with these results, Van Hove et al., combining single-cell RNA sequencing with complementary approaches in mice, suggested that dmΜΦ and cpΜΦ were gradually replenished by bone marrow-derived monocytes [14]. As dura mater and choroid plexus stroma are more accessible brain regions than (i) subdural space, (ii) the apical surface of the choroid plexuses, and (iii) brain parenchyma, the tissue permeability may be considered a crucial factor for brain macrophage ontogeny. However, the ablation of BAMs through CSF1R blockade led to the replenishment of cpΜΦ and dmΜΦ via local expansion, indicating their self-renewal capacity, while sdΜΦ presented difficulties in their repopulation [14].
By utilizing the Cx3cr1CreER:R26tdTomato fate mapping system in an experimental autoimmune encephalomyelitis (EAE) mouse model, Jordão et al. proposed that BAMs remained stable and locally self-renewed in addition to the recruitment of bone marrow-derived progenitors [12]. In Cx3cr1gfpCcr2rfp bone marrow chimeric mice, CD169+ BAMs proliferated after ischemia, while a small proportion of BAMs was bone marrow-derived, populating the perivascular and ischemic regions [36]. Both in homeostasis and disease, skull and vertebrae bone marrow constitute a pool of myeloid cells that can invade non-parenchymal and parenchymal CNS regions, transforming into tissue-resident macrophages [41]. A fate-mapping analysis in a mouse model of Alzheimer’s disease (AD) revealed that BAMs are a stable cell population with an unaffected turnover rate and a minimal replenishment from bone marrow-derived cells during this neurodegenerative disease [42].
Summarizing, the origin of BAMs has been extensively studied in the last few years using new genetic tools, e.g., fate mapping analysis. It has been proposed that BAMs originate from early EMPs in the yolk sac during embryogenesis. Although specific BAMs are replenished by peripherally-derived monocytes postnatally, some remain solely derived from the local pool. BAMs have been shown to remain stable and locally self-renewed in both homeostasis and disease. Further investigation is needed to (i) confirm BAM origin, (ii) detect the precise embryonic progenitors of BAMs, especially of the dura mater and choroid plexus macrophages, (iii) determine the timing of each BAM subpopulation’s generation, and (iv) delineate their repopulation pattern.
3. Molecular Drives Orchestrating BAM Development
The transcription factor PU.1 (or SFPI) could be essential for the BAM generation during embryonic development since research has showed that in mice with deletion of the Sfpi1 gene, pvMΦ, sdMΦ, and cpMΦ were ablated [8]. Progenitors of BAMs express the runt-related transcription factor 1 (RUNX1), which regulates the expression of PU.1 during embryogenesis [20,43]. The impairment of PU.1 factor in mice results in a reduced number of A1 (CD45+ c-kitlo CX3CR1− immature cells) and A2 (CD45+ c-kit− CX3CR1+ cells) progenitor cells of the yolk sac, from which both microglial cells and BAMs originate. In contrast, the lack of interferon regulatory factor 8 (IRF8) exclusively decreased the number of A2 cells [44]. Furthermore, the colony-stimulating factor 1 receptor (CSF1R) signaling could be essential for BAM development [5,11,14]. In a zebrafish model carrying the panther mutation, a loss-of-function mutation in the fms gene orthologue which encodes CSF1R, primitive macrophages of the yolk sac could not colonize the embryonic tissues [45].
After progenitors’ migration and invasion in the CNS, BAM generation is initiated (Figure 1). The BAMs may be developed independently of transforming growth factor beta receptor (TGF-βR) signaling. In Tgfbr2-deficient mice, no alteration in cell numbers of BAMs occurred, while transforming growth factor beta (TGF-β) is required for the generation of microglial cells [20,46]. Three main brain border regions are filled with BAMs, namely, meninges, choroid plexus, and perivascular spaces. The postnatal expansion of sdMΦ was influenced by IRF8 and MAFB [40]. Indeed, in Irf8-deficient mice, a reduction of sdMΦ was observed [8]. The lack of integrin subunit beta 1 (ITGB1) in mice resulted only in a minor change in the numbers of sdΜΦ [40]. Similarly, the absence of insulin-like growth factor 1 (IGF1R) induces transcriptomic changes in BAMs via its implication in RNA processing, growth, migration and intracellular signaling [47]. The MYB, BATF3, and NR4A1 transcription factors were not necessary for BAM development [8].
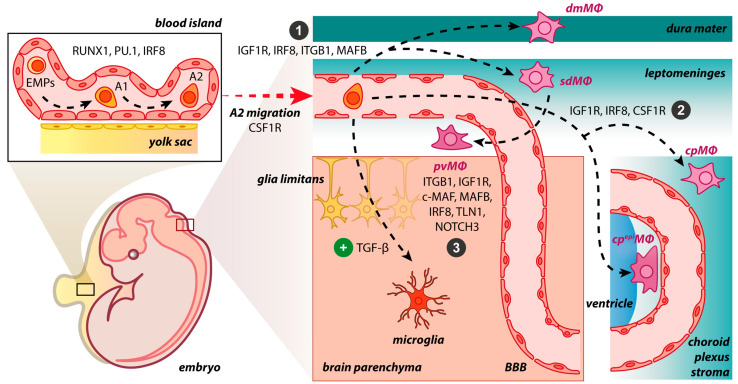
Figure 1.
BAM origin and propagation in the developing mouse brain. The early differentiation of macrophage progenitors is regulated by the expression of RUNX1, PU.1, and IRF8 in the yolk sac, where the primitive erythro-myeloid progenitors (EMPs) give rise to CD45+ c-kitlo CX3CR1− immature (A1) cells and subsequently to CD45+ c-kit− CX3CR1+ (A2) cells. In the presence of TGF-β, A2 cells initiate a microgliogenesis program upon settlement in the brain parenchyma. In the absence of the TGF-β, A2 cells do not enter the brain parenchyma, populate the abutting connective tissue, and may follow distinct developmental pathways: (1) IGF1R, IRF8, ITGB1, and MAFB restrict progenitors to the meninges, either dura or the subdural mesenchymal niche; (2) IGF1R, IRF8, and CSF1R dictate progenitors’ residency within the choroid plexus; (3) ITGB1, IGF1R, c-MAF, MAFB, IRF8, TLN1, and NOTCH3 stimulate pvΜΦ generation postnatally from sdΜΦ. However, it is not yet fully understood if the dmΜΦ share common progenitors and drivers with sdΜΦ during embryogenesis. dmΜΦ: dural macrophages; sdΜΦ: subdural macrophages; pvΜΦ: perivascular macrophages; cpΜΦ: stromal choroid plexus macrophages; cpepiΜΦ: choroid epiplexus macrophages; BBB: blood–brain barrier.
Specific molecular cues may also regulate the development of choroid plexus macrophages. Colony stimulating factor 1 (CSF1 or M-CSF), produced by stromal and epithelial cells, is crucial for macrophages’ ontogeny, orchestrating their proliferation and differentiation [48]. CSF1 binds to its receptor, namely, CSF1R, a homodimeric type III receptor tyrosine kinase [49]. Fms-intronic regulatory element (FIRE) is a highly conserved enhancer found in the second intron of the Csf1r gene [50]. In mutant mice with deletion of FIRE, the production and maintenance of cpMΦ were partially impaired [51]. On the contrary, Rojo et al. demonstrated that in FIRE-deficient mice, microglial cells were absent from the brain, whereas BAMs were retained [52]. Interestingly, cpMΦ remained unaltered in a study with Irf8-deficient mice [8], while other research considered IRF8 as a regulator of cpMΦ maturation since the gene ablation suppressed the transcriptional programme of cpMΦ [14,53].
The transcription factor c-MAF, a member of Maf family transcription factors, could be crucial for regulating the pvMΦ transcriptional programme as the deletion of c-Maf in macrophage lineages resulted in the ablation of pvMΦ in the mouse brain [54]. The postnatal expansion of pvΜΦ was also influenced by IRF8 and MAFB [40]. Moreover, VSMCs have a potential role in the distribution of the pvMΦ during development. In Notch3-deficient mice, VSMCs are reduced similarly to the pvMΦ, while the number of sdΜΦ was maintained [40,55]. The distribution of pvMΦ is also controlled by integrin signaling. Talin 1 (Tln1) is an integrin-related gene which encodes a cytoskeletal protein. In Tln1−/− mice, a significantly lower number of pvMΦ was observed, while microglia and sdΜΦ were not affected in the developing brain, underscoring the impaired vascularization as the cause of pvMΦ reduction [40]. Nevertheless, the absence of integrin subunit beta 1 (ITGB1) in mice resulted only in a minor change in the numbers of pvΜΦ [40]. All the aforementioned molecular cues involved in BAM development are presented in Table 1.
To recapitulate, the emergence of BAMs is considered a complex process tightly regulated by multiple molecular cues in a similar pattern to oligodendrogenesis and microgliogenesis [24,56]. Although some molecular drivers orchestrating BAM generation have been recently discovered, it remains a largely uncharted territory.
Table 1.
Molecular drivers and cues regulating the development of BAMs.
| Gene | Locus | Protein | Location | Tissue Specificity | Brain Specificity |
Molecular Function |
Species | Ref. |
|---|---|---|---|---|---|---|---|---|
| CSF1R | 5q32 | Colony stimulating factor 1 receptor |
Vesicles; Plasma membrane | Lymphoid tissue; Placenta | Low | Kinase; Receptor; Transferase |
Mice; Zebrafish | [5,11,14,45,51,52] |
| IGF1R | 15q26.3 | Insulin-like growth factor 1 receptor | Plasma membrane | Low | Low | Kinase; Receptor; Transferase |
Mice | [47] |
| IRF8 | 16q24.1 | Interferon regulatory factor 8 |
Nucleoplasm | Bone marrow; Lymphoid tissue | Low | Activator; DNA-binding; Repressor |
Mice | [8,14,40,44,53] |
| ITGB1 | 10p11.22 | Integrin subunit beta 1 | Plasma membrane; Focal adhesion sites; Endoplasmic reticulum | Low | Low | Virus entry; Integrin; Receptor |
Mice | [40] |
| MAF | 16q23.2 | MAF bZIP transcription factor |
Nucleoplasm; Nuclear bodies; Vesicles |
Low | Low | Activator; DNA-binding; Repressor |
Mice | [54] |
| MAFB | 20q12 | MAF bZIP transcription factor B |
Nucleoplasm; Nucleoli; Golgi apparatus; Cytosol | Parathyroid gland | Low | Activator; DNA-binding; Repressor |
Mice | [40] |
| NOTCH3 | 19p13.12 | Notch receptor 3 | Nucleoplasm; Cytosol; Actin filaments | Low | Low | Activator; Developmental protein; Receptor |
Mice | [40,55] |
| RUNX1 | 21q22.12 | RUNX family transcription factor 1 |
Nucleoplasm; Vesicles | Low | Low | Activator; DNA-binding; Repressor |
Mice | [20,43] |
| SPI1 | 11p11.2 | Spi-1 proto- oncogene |
Nucleoplasm | Bone marrow; Lung; Lymphoid tissue |
Low | Activator; DNA-binding; RNA-binding |
Mice | [8,44] |
| TGFB1 | 19q13.2 | Transforming growth factor beta 1 | Golgi apparatus; Cytosol | Low | Low | Growth factor; Mitogen | Mice | [20] |
| TLN1 | 9p13.3 | Talin 1 | Focal adhesion sites; Cytosol; Plasma membrane; Centriolar satellite | Low | Low | Cell-cell contact | Mice | [40] |
4. BAMs vs. Microglia
4.1. Differences in Morphology and Motility
The BAM subpopulations and microglia generally vary in morphology. Meningeal macrophages are flat, spindle-shaped cells with a few thick membrane projections from their cell body residing close to meningeal vessels [59,60]. Although sdΜΦ appeared elongated with a more amoeboid morphology than microglia, dmΜΦ was also suggested to be pleomorphic and dendriform-like cells [8,61]. In the same context, the pvΜΦ had elongated cell bodies permitting the embedding within vessel walls [8,59]. Regarding the choroid plexus, cpΜΦ display a star-like shape, while cpepiΜΦ seem more phenotypically diverse, varying from round to bipolar to stellate [8,61,62]. Under homeostatic conditions, microglia are ramified [8]. Inflammatory stimuli could shift microglial morphology from ramified to amoeboid by enlarging the cell body and retracting processes [24].
The BAMs and microglia appeared to slightly differ in motility as well. During homeostasis, pvΜΦ were non-motile, with only cellular processes extending through the blood vessel wall, whereas dmΜΦ and sdΜΦ exhibited limited motility in in vivo imaging [8,59]. Microglial cells are characterized by highly dynamic projections and a cell body with limited motility [8]. During inflammation, pvΜΦ extend dendritic-like processes along the perivascular space, indicating a potential chemotactic activation from surrounding cells, while meningeal macrophages prolongate their existing protrusions [63,64]. The amoeboid microglia exhibit a high phagocytic and proinflammatory phenotype [24]. As the in vivo imaging of choroid plexus remains challenging due to their deep localization in the ventricular system, the motility of cpΜΦ and cpepiΜΦ is yet unexplored [59].
4.2. Differences in Biological Role
Although microglia and BAMs are immune-competent cells of the CNS with common progenitors, their different localization may contribute to variations in their biological roles. The microglial populations’ functions have been reviewed in detail [65,66,67]. Concisely, microglial cells are involved in developmental processes, including cell positioning, survival, myelinogenesis, synaptic patterning, and axonal dynamics [68]. In adult CNS, microglia, as the regulators of acute and chronic immune responses, are implicated in removing pathogens and noxious particles, scavenging cellular debris and synapses, protecting neural tissue, and mediating neurogenesis in CNS injury [24,66,69].
The unique localization of BAMs between brain parenchyma and peripheral tissues pinpoint their pivotal role in the immune surveillance of pathological antigens [16]. Their antigen-presenting capacity is attributed to MHC II molecules on some BAM surfaces [12,32,70,71]. Furthermore, the pvΜΦ and dmΜΦ mainly phagocytose intruding pathogens and any foreign molecule or substance that can be detected in the bloodstream and cerebrospinal fluid [72,72]. The pvΜΦ also appear to regulate the accessibility of brain parenchyma to circulating cells and molecules by increasing the contractility of regional vessels and capillaries or diminishing the BBB permeability [73,74,75,76]. Interestingly, the latest approaches demonstrate the involvement of BAMs in ensuring a well-balanced metabolic environment for neurons, especially in the course of systemic perturbations [77,78].
4.3. Differences in Molecular and Genetic Profile
The distinction between parenchymal and non-parenchymal tissue-resident macrophages, namely, microglia and BAMs, respectively, remains challenging. Identifying specific surface protein expression patterns and the genetic signature of each cell’s population could assist in studying microglia and BAMs. Both microglia and BAMs share some common surface markers. Specifically, typical macrophage markers such as C-X3-C motif chemokine receptor 1 (CX3CR1), adhesion G protein-coupled receptor E1 (ADGRE1 or F4/80), Mer tyrosine kinase (MERTK), and CD11b are present in both cell populations [5,8]. Furthermore, CSF1R, allograft inflammatory factor 1 (AIF1 or IBA1) and protein tyrosine phosphatase receptor type C (PTPRC or CD45) constitute myeloid markers of these cells [8].
Although microglia and BAMs exhibit common surface markers, their discrimination may be based on their different expression levels. For instance, significantly higher levels of CD45 were observed in BAMs compared with microglial cells. However, the levels of CD45 are not a reliable marker regarding cells’ discrimination since a subset of BAMs has been found to express low levels of CD45 [5]. Microglia-specific markers are critical in identifying the parenchymal tissue-resident macrophages (Table 2). The purinergic receptor P2Y12 (P2RY12), the hexosaminidase subunit beta (HEXB), the siglech sialic acid binding Ig-like lectin H (SIGLEC-H), the transmembrane protein 119 (TMEM119), the annexin 3 (ANXA3), and the Spalt-like transcription factor 1 (SALL1) are present only in microglia and not in BAMs, allowing their unique distinction [5,8,12,36,79,80,81].
Table 2.
Morphology, motility, and specific surface markers of microglia and BAMs.
| Cell Type | Morphology | Motility | Cell-Specific Markers |
|---|---|---|---|
| Microglia | Ramified in homeostasis; Amoeboid in inflammation |
Cell bodies with limited-motility but highly dynamic processes in homeostasis; Highly phagocytic in inflammation |
SIGLEC-H+, P2RY12+, HEXB+, TMEM119+, ANXA3+, SALL1+ |
| pvΜΦ | Slightly elongated cell bodies | Non-motile cell bodies with extending and retracting projections through the blood vessel wall in homeostasis; Dendritic-like processes in inflammation |
CD206+, CD38+, LYVE1+, CD36+, CD163+, CD169+ |
| dmΜΦ | Elongated; Spindle-shaped cells; Few thick membrane projections; Dendriform |
Limited motility and highly dynamic protrusions in homeostasis; Extending projections in inflammation |
|
| sdΜΦ | Elongated; Amoeboid; Spindle-shaped cells; Few thick membrane projections |
Limited motility and highly dynamic protrusions in homeostasis; Extending projections in inflammation |
|
| cpΜΦ | Star-like shape | Unknown | |
| cpepiΜΦ | Round; Bipolar; Stellate | Unknown |
BAMs: border-associated macrophages; pvΜΦ: perivascular macrophages; dmΜΦ: dural macrophages; sdΜΦ: subdural macrophages; cpΜΦ: stromal choroid plexus macrophages; cpepiΜΦ: choroid epiplexus macrophages; SIGLEC-H: siglech sialic acid binding Ig-like lectin H; P2RY12: purinergic receptor P2Y12; HEXB: hexosaminidase subunit beta; TMEM119: transmembrane protein 119; ANXA3: annexin 3; SALL1: Spalt like transcription factor 1; CD206: Cluster of differentiation molecule 206; CD38: Cluster of differentiation molecule 38; CD36: Cluster of differentiation molecule 36; CD163: Cluster of differentiation molecule 163; CD169: Cluster of differentiation molecule 169; LYVE1: Lymphatic vessel endothelial hyaluronan receptor 1.
On the contrary, cell surface phenotyping has revealed distinctive BAM markers, which may be applied for their classification (Table 2). As already been pointed out, the BAMs can be localized to three main compartments: the meninges, perivascular space, and choroid plexus, with each macrophage population acquiring characteristic molecular and genetic profiles. The CD206 (or MRC1) constitutes a signature surface protein for BAMs [5,8,36]. Subsets of BAMs were distinguished through the different expression levels of major histocompatibility complex class II (MHCII), CD38, lymphatic vessel endothelial hyaluronan receptor 1 (LYVE1), and C-C motif chemokine receptor 2 (CCR2) [5]. The CD36, CD163, CD169, and LYVE1 have been detected in pvΜΦ [5,8,36,71,82,83,84]. The pvΜΦ manifested higher levels of CD45 and lower IBA1 in relation to microglia [8,83]. Only MHCII+ BAMs, which enriched choroid plexus and dura mater, were found to express CCR2, explaining the increased replacement and turnover rate of cpΜΦ and dmΜΦ [5]. In addition, CNS-resident macrophages may be distinguished from peripheral monocytes since the monocytes express the integrin subunit alpha 4 (ITGA4 or CD49d), integrin subunit alpha 5 (ITGA5 or CD49e), and cell division cycle 20 (CDC20) [8,85].
In terms of genetics, BAMs carry some specific genes such as Mrc1, platelet factor 4 (Pf4), membrane spanning 4-domains A7 (Ms4a7), stabilin 1 (Stab1), apolipoprotein E (Apoe), membrane-spanning 4-domains, subfamily A, member 6C (Ms4a6c), lysozyme 2 (Lyz2), and transforming growth factor beta induced (Tgfbi) [12,14]. Similarly, microglia-specific genes have been identified, forming a unique microglial transcriptional profile. These include P2ry12, Tmem119, secreted protein acidic and cysteine rich (Sparc), olfactomedin like 3 (Olfml3), HexB, Sall1, triggering receptor expressed on myeloid cells 2 (Trem2), Siglec-H, and solute carrier family 2 member 5 (Slc2a5) [5,8,12]. Although cpepiΜΦ constitute a subpopulation of BAMs located in the choroid plexus, they present significant similarities in their transcriptional profile with microglia expressing Sall1, a signature gene for the microglial population [14].
5. BAMs in Neurological Diseases and Promising Therapies
The implication of BAMs in the pathogenesis of CNS diseases, especially in neurodegeneration and neuroinflammation, is a rapidly emerging field of research. Although the precise role of BAMs in diseases is not yet elucidated, recent studies have addressed their potential involvement in several pathological conditions such as Alzheimer’s disease, Parkinson’s disease, multiple sclerosis, and stroke. Further experimental studies are needed to delineate the exact pathophysiological mechanism through which methodical manipulation of BAMs can halt or even reverse the progression of the aforementioned debilitating CNS diseases.
5.1. BAMs in Alzheimer’s Disease
AD is a brain disorder constituting a common cause of dementia, characterized by permanent neurodegeneration in specific brain areas [86]. However, the pathophysiology of the disease is not yet fully understood. The accumulation of amyloid beta (Aβ) protein in the brain has been implicated in AD. This protein forms sticky plaques that may disrupt the interaction between brain cells, leading to inflammation and neuronal death [87]. Additionally, AD is characterized by the accumulation of the tau protein, which forms neurofibrillary tangles [88]. Patients with Alzheimer’s disease (AD) could be affected by cerebral amyloid angiopathy (CAA), which involves the pathologic deposition of Aβ within the leptomeningeal and cortical blood vessels [89]. The role of pvΜΦ in CAA progression has been investigated in a TgCRND8 mouse model of AD [90]. Hawkes and McLaurin demonstrated that the stimulation of the pvΜΦ turnover decreased cerebral CAA load. Interestingly, the clearance of CAA load was not attributed to microglia or astrocytes. These findings indicate the importance of pvΜΦ in CAA progression, suggesting that their activation could be a useful therapeutic approach for removing vascular amyloid [90].
In Tg2576 mice, the clodronate-mediated depletion of pvΜΦ reduced the production of reactive oxygen species, thereby reversing cerebrovascular dysfunction induced by Aβ. Experiments utilizing bone marrow chimeras revealed that pvΜΦ are the primary cell expressing CD36 and NOX2, which are molecular substrates for inducing cerebrovascular oxidative stress [91]. The pvΜΦ play a significant role in upregulating secreted phosphoprotein 1 (SPP1), with perivascular fibroblasts contributing to a lesser extent. SPP1 assists microglia in engulfing synapses and increases the expression of phagocytic markers such as complement C1q A chain (C1QA), granulin precursor (GRN), and cathepsin B (CTSB) in the presence of Aβ oligomers. The deletion of Spp1 in AD mouse models prevented synaptic loss [34]. Finally, the minor replenishment of CD206+ BAMs and their stable turnover in a mouse AD model should be highlighted, as potential manipulations of these cells could lead to modification of AD pathology [42].
5.2. BAMs in Parkinson’s Disease
Parkinson’s disease (PD) is another common neurodegenerative disorder characterized by dopaminergic cell loss [92]. The accumulation of a-synuclein (α-SYN) is a distinct trait of degenerating dopaminergic neurons [93,94]. According to Guo et al., exosomes derived from microglia and CNS macrophages facilitated the transmission of α-SYN, leading to its aggregation in neurons and contributing to the development of PD [95]. Interestingly, BAMs may mediate the α-SYN related neuroinflammation by acting as antigen-presenting cells essential for initiating a CD4 T cell response [96]. The immune cell infiltration, recruitment, and antigen presentation were found to be greatly dependent on BAMs, framing their involvement in the pathogenesis of PD [96]. A JAK1/2 inhibitor, namely, AZD1480, has been considered a therapeutic option for PD by reducing α-SYN-related neuroinflammation via downregulation of the JAK/STAT pathway [97].
5.3. BAMs in Multiple Sclerosis
Multiple sclerosis (MS) is a debilitating neurodegenerative disease with a rising global prevalence in recent years [98]. MS features encompass neuroinflammation, demyelination, and axonal loss within the CNS [99,100]. Several mechanisms have been proposed to be implicated in the pathophysiology of MS [101,102,103]. Nevertheless, the potential role of BAMs in MS has been only recently investigated [47,104]. BAMs, as a CNS macrophage population, could potentially be involved in the MS course through the CNS-targeted autoimmunity or neurodegeneration leading to a secondary autoimmune response [105]. BAMs are presented with different phenotypes regarding their roles in each stage of the MS [106].
Particularly, Locatelli et al. identified various markers of BAMs, utilizing immunofluorescent techniques in a MS mouse model, as the neuroinflammatory lesions shifted from expansion to gradual resolution [107]. In EAE, the most widely used animal model for studying MS aspects [108,109], antigen presentation and T cell reactivation were found to be regulated by both meningeal macrophages and microglia, revealing the involvement of BAMs in the disease [110,111]. The pvΜΦ and sdΜΦ were found to be modestly increased in the EAE mouse model, with sdΜΦ population expanding during disease onset, suggesting their implication in the initial acute phase of EAE. On the contrary, the sdΜΦ population decreased during the chronic phase of the disease and pvΜΦ proliferation remained unaltered [12].
The BAMs could also exert miscellaneous functions in MS via interleukin 9 (IL9) upregulation. Donninelli et al. found that MS patients had higher IL9 levels in the cerebrospinal fluid obtained from post-mortem samples. Through flow cytometry of snap-frozen tissue blocks from the same patients’ brains, higher expression of IL9 was also observed in macrophages [112]. Additionally, the disease-mediated peroxisome injury in BAMs, leading to demyelination and axonal loss, may be prevented through treatment with 4-Phenylbutyrate, which serves as a potential therapeutic approach for halting inflammatory demyelination and the progression of MS [113]. Lastly, foamy macrophages are formed in brain regions during MS; by targeting lipophagy, remyelination can be promoted as some BAM subtypes may be involved in the aforementioned process [114,115].
5.4. BAMs in Other CNS Diseases
The BAMs have also been implicated in other CNS diseases, such as stroke. The study of Pedragosa et al. highlighted the major role of BAMs in different pathophysiological changes related to ischemic stroke, including the recruitment of granulocytes, increased expression of vascular endothelial growth factor (VEGF), and increased permeability of pial and cortical blood vessels [116]. The induction of ischemic stroke resulted in the proliferation and migration of CD163+ BAMs adopting a pro-inflammatory phenotype in the ischemic rat parenchyma. Although CD169+ perivascular macrophages were also observed to proliferate in response to ischemic stroke, they were replaced by infiltrating bone marrow-derived cells in mice. These findings were confirmed in a human model in which CD163+ cells were also accumulated in the ischemic region [36]. In the subarachnoid hemorrhage (SAH), sdΜΦ and pvΜΦ are involved in erythrocyte uptake affecting the outcome of hemorrhage. Specifically, their depletion led to the reduction of large arterioles’ inflammation and microthrombosis after SAH [117]. Ultimately, an induction of anti-inflammatory microglial/macrophage responses and subsequent neuroprotection could be achieved through the peripheral administration of interleukin 13 in cases of ischemic stroke [118].
6. Conclusions
Despite the fact that the origin of BAMs has been recently elucidated, the molecular drivers orchestrating their development still represent uncharted territory. Self-maintenance or even replenishment from bone marrow-derived monocytes serves as the most viable scenario behind the BAM repopulation pattern during adulthood. The precise role of BAMs in the pathogenesis of neurodegenerative and neuroinflammatory diseases should be further explored, nonetheless. Future research has to promptly focus on distinguishing between the unique properties of these cells as well as their synergistic actions and cross-reactivity with innate immune cells, especially in the context of disease. Lastly, after more BAM subtypes biomarkers have been popularized, lab-approached manipulations could target these specific populations according to disease course and progression.
Abbreviations
| α-SYN | a-synuclein |
| AD | Alzheimer disease |
| ADGRE1 | Adhesion G protein-coupled receptor E1 |
| AIF1 | Allograft inflammatory factor 1 |
| ANXA3 | Annexin 3 |
| APOE | Apolipoprotein E |
| Aβ | Amyloid beta |
| BAMs | Border-associated macrophages |
| BATF3 | Basic leucine zipper transcriptional factor ATF-like 3 |
| BBB | Blood–brain barrier |
| c-MAF | MAF bZIP transcription factor |
| C1QA | C1q A chain |
| CAA | Cerebral amyloid angiopathy |
| CAMs | CNS-associated macrophages |
| CCR2 | C-C Motif chemokine receptor type 2 |
| CD163 | Cluster of differentiation molecule 163 |
| CD169 | Cluster of differentiation molecule 68 |
| CD206 | Cluster of differentiation molecule 206 |
| CD36 | Cluster of differentiation molecule 36 |
| CDC20 | Cell division cycle 20 |
| CNS | Central nervous system |
| cpepiΜΦ | Choroid epiplexus macrophages |
| cpΜΦ | Stromal choroid plexus macrophages |
| CSF | Cerebrospinal fluid |
| CSF1 | Colony stimulating factor 1 |
| CSF1R | Colony stimulating factor 1 receptor |
| CTSB | Cathepsin B |
| CX3CR1 | C-X3-C motif chemokine receptor 1 |
| dmΜΦ | Dural macrophages |
| E | Embryonic day |
| EAE | Experimental autoimmune encephalomyelitis |
| EMPs | Erythro-myeloid progenitors |
| FIRE | Fms-intronic regulatory element |
| GRN | Granulin precursor |
| HEXB | Hexosaminidase subunit beta |
| IGF1R | Insulin-like growth factor 1 receptor |
| IL9 | Interleukin 9 |
| IRF8 | Interferon regulatory factor 8 |
| ITGA4 | Integrin subunit alpha 4 |
| ITGA5 | Integrin subunit alpha 5 |
| ITGB1 | Integrin subunit Beta 1 |
| JAK1/2 | Janus kinase 1/2 |
| LYVE1 | Lymphatic vessel endothelial hyaluronan receptor 1 |
| LYZ2 | Lysozyme 2 |
| MAFB | MAF bZIP transcription factor B |
| MERTK | Mer tyrosine kinase |
| MHCII | Major histocompatibility complex class II |
| MRC | Mannose receptor C-type 1 |
| MS | Multiple sclerosis |
| MS4A6C | Membrane-spanning 4-domains, subfamily A, member 6C |
| MS4A7 | Membrane spanning 4-domains A7 |
| MYB | MYB proto-oncogene, transcription factor |
| NR4A1 | Nuclear receptor subfamily 4 group A member 1 |
| OLFML3 | Olfactomedin like 3 |
| P2RY12 | Purinergic receptor P2Y12 |
| PD | Parkinson’s disease |
| PF4 | Platelet factor 4 |
| PTPRC | Protein tyrosine phosphatase receptor type C |
| pvΜΦ | Perivascular macrophages |
| RUNX1 | Runt-related transcription factor 1 |
| SAH | Subarachnoid hemorrhage |
| SALL1 | Spalt like transcription factor 1 |
| sdΜΦ | Subdural/leptomeningeal macrophages |
| SIGLEC-H | Siglech sialic acid binding Ig-like lectin H |
| SLC2A5 | Solute carrier family 2 member 5 |
| SPARC | Secreted protein acidic and cysteine rich |
| SPP1 | Secreted phosphoprotein 1 |
| STAB1 | Stabilin-1 |
| TGF-β | Transforming growth factor beta |
| TGF-βR | Transforming growth factor beta receptor |
| TGFBI | Transforming growth factor beta induced |
| TLN1 | Talin 1 |
| TMEM119 | Transmembrane protein 119 |
| TREM2 | Triggering receptor expressed on myeloid cells 2 |
| VEGF | Vascular endothelial growth factor |
| VSMCs | Vascular smooth muscle cells |
Author Contributions
Conceptualization, I.D., P.T and M.E.M.; writing—original draft preparation, I.D., P.T., P.E., E.D., N.E., A.C. and E.A.; writing—review and editing, M.E.M.; visualization, I.D. and P.T. All authors have read and agreed to the published version of the manuscript.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
Not applicable.
Conflicts of Interest
The authors declare no conflict of interest.
Funding Statement
This research received no external funding.
Footnotes
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content.
References
- 1.Mastorakos P., McGavern D. The Anatomy and Immunology of Vasculature in the Central Nervous System. Sci. Immunol. 2019;4:eaav0492. doi: 10.1126/sciimmunol.aav0492. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Li Q., Barres B.A. Microglia and Macrophages in Brain Homeostasis and Disease. Nat. Rev. Immunol. 2018;18:225–242. doi: 10.1038/nri.2017.125. [DOI] [PubMed] [Google Scholar]
- 3.Galloway D.A., Phillips A.E.M., Owen D.R.J., Moore C.S. Phagocytosis in the Brain: Homeostasis and Disease. Front. Immunol. 2019;10:790. doi: 10.3389/fimmu.2019.00790. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Casano A.M., Peri F. Microglia: Multitasking Specialists of the Brain. Dev. Cell. 2015;32:469–477. doi: 10.1016/j.devcel.2015.01.018. [DOI] [PubMed] [Google Scholar]
- 5.Mrdjen D., Pavlovic A., Hartmann F.J., Schreiner B., Utz S.G., Leung B.P., Lelios I., Heppner F.L., Kipnis J., Merkler D., et al. High-Dimensional Single-Cell Mapping of Central Nervous System Immune Cells Reveals Distinct Myeloid Subsets in Health, Aging, and Disease. Immunity. 2018;48:380–395.e6. doi: 10.1016/j.immuni.2018.01.011. [DOI] [PubMed] [Google Scholar]
- 6.Bechmann I., Kwidzinski E., Kovac A.D., Simbürger E., Horvath T., Gimsa U., Dirnagl U., Priller J., Nitsch R. Turnover of Rat Brain Perivascular Cells. Exp. Neurol. 2001;168:242–249. doi: 10.1006/exnr.2000.7618. [DOI] [PubMed] [Google Scholar]
- 7.Mato M., Ookawara S., Kurihara K. Uptake of Exogenous Substances and Marked Infoldings of the Fluorescent Granular Pericyte in Cerebral Fine Vessels. Am. J. Anat. 1980;157:329–332. doi: 10.1002/aja.1001570308. [DOI] [PubMed] [Google Scholar]
- 8.Goldmann T., Wieghofer P., Jordão M.J.C., Prutek F., Hagemeyer N., Frenzel K., Amann L., Staszewski O., Kierdorf K., Krueger M., et al. Origin, Fate and Dynamics of Macrophages at Central Nervous System Interfaces. Nat. Immunol. 2016;17:797–805. doi: 10.1038/ni.3423. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.McKinsey G.L., Lizama C.O., Keown-Lang A.E., Niu A., Santander N., Larpthaveesarp A., Chee E., Gonzalez F.F., Arnold T.D. A New Genetic Strategy for Targeting Microglia in Development and Disease. eLife. 2020;9:e54590. doi: 10.7554/eLife.54590. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Masuda T., Amann L., Sankowski R., Staszewski O., Lenz M., d’Errico P., Snaidero N., Costa Jordão M.J., Böttcher C., Kierdorf K., et al. Novel Hexb-Based Tools for Studying Microglia in the CNS. Nat. Immunol. 2020;21:802–815. doi: 10.1038/s41590-020-0707-4. [DOI] [PubMed] [Google Scholar]
- 11.Ginhoux F., Greter M., Leboeuf M., Nandi S., See P., Gokhan S., Mehler M.F., Conway S.J., Ng L.G., Stanley E.R., et al. Fate Mapping Analysis Reveals That Adult Microglia Derive from Primitive Macrophages. Science. 2010;330:841–845. doi: 10.1126/science.1194637. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Jordão M.J.C., Sankowski R., Brendecke S.M., Locatelli G., Tai Y.-H., Tay T.L., Schramm E., Armbruster S., Hagemeyer N., Groß O., et al. Single-Cell Profiling Identifies Myeloid Cell Subsets with Distinct Fates during Neuroinflammation. Science. 2019;363:eaat7554. doi: 10.1126/science.aat7554. [DOI] [PubMed] [Google Scholar]
- 13.Yona S., Kim K.-W., Wolf Y., Mildner A., Varol D., Breker M., Strauss-Ayali D., Viukov S., Guilliams M., Misharin A., et al. Fate Mapping Reveals Origins and Dynamics of Monocytes and Tissue Macrophages under Homeostasis. Immunity. 2013;38:79–91. doi: 10.1016/j.immuni.2012.12.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Van Hove H., Martens L., Scheyltjens I., De Vlaminck K., Pombo Antunes A.R., De Prijck S., Vandamme N., De Schepper S., Van Isterdael G., Scott C.L., et al. A Single-Cell Atlas of Mouse Brain Macrophages Reveals Unique Transcriptional Identities Shaped by Ontogeny and Tissue Environment. Nat. Neurosci. 2019;22:1021–1035. doi: 10.1038/s41593-019-0393-4. [DOI] [PubMed] [Google Scholar]
- 15.Zelco A., Börjesson V., de Kanter J.K., Lebrero-Fernandez C., Lauschke V.M., Rocha-Ferreira E., Nilsson G., Nair S., Svedin P., Bemark M., et al. Single-Cell Atlas Reveals Meningeal Leukocyte Heterogeneity in the Developing Mouse Brain. Genes Dev. 2021;35:1190–1207. doi: 10.1101/gad.348190.120. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Mildenberger W., Stifter S.A., Greter M. Diversity and Function of Brain-Associated Macrophages. Curr. Opin. Immunol. 2022;76:102181. doi: 10.1016/j.coi.2022.102181. [DOI] [PubMed] [Google Scholar]
- 17.van Furth R., Cohn Z.A., Hirsch J.G., Humphrey J.H., Spector W.G., Langevoort H.L. The Mononuclear Phagocyte System: A New Classification of Macrophages, Monocytes, and Their Precursor Cells. Bull. World Health Organ. 1972;46:845–852. [PMC free article] [PubMed] [Google Scholar]
- 18.Hoeffel G., Chen J., Lavin Y., Low D., Almeida F.F., See P., Beaudin A.E., Lum J., Low I., Forsberg E.C., et al. C-Myb+ Erythro-Myeloid Progenitor-Derived Fetal Monocytes Give Rise to Adult Tissue-Resident Macrophages. Immunity. 2015;42:665–678. doi: 10.1016/j.immuni.2015.03.011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Hickey W.F., Kimura H. Perivascular Microglial Cells of the CNS Are Bone Marrow-Derived and Present Antigen in Vivo. Science. 1988;239:290–292. doi: 10.1126/science.3276004. [DOI] [PubMed] [Google Scholar]
- 20.Utz S.G., See P., Mildenberger W., Thion M.S., Silvin A., Lutz M., Ingelfinger F., Rayan N.A., Lelios I., Buttgereit A., et al. Early Fate Defines Microglia and Non-Parenchymal Brain Macrophage Development. Cell. 2020;181:557–573.e18. doi: 10.1016/j.cell.2020.03.021. [DOI] [PubMed] [Google Scholar]
- 21.Ginhoux F., Guilliams M. Tissue-Resident Macrophage Ontogeny and Homeostasis. Immunity. 2016;44:439–449. doi: 10.1016/j.immuni.2016.02.024. [DOI] [PubMed] [Google Scholar]
- 22.Shemer A., Grozovski J., Tay T.L., Tao J., Volaski A., Süß P., Ardura-Fabregat A., Gross-Vered M., Kim J.-S., David E., et al. Engrafted Parenchymal Brain Macrophages Differ from Microglia in Transcriptome, Chromatin Landscape and Response to Challenge. Nat. Commun. 2018;9:5206. doi: 10.1038/s41467-018-07548-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Stremmel C., Schuchert R., Wagner F., Thaler R., Weinberger T., Pick R., Mass E., Ishikawa-Ankerhold H.C., Margraf A., Hutter S., et al. Yolk Sac Macrophage Progenitors Traffic to the Embryo during Defined Stages of Development. Nat. Commun. 2018;9:75. doi: 10.1038/s41467-017-02492-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Dermitzakis I., Manthou M.E., Meditskou S., Tremblay M.-È., Petratos S., Zoupi L., Boziki M., Kesidou E., Simeonidou C., Theotokis P. Origin and Emergence of Microglia in the CNS—An Interesting (Hi)Story of an Eccentric Cell. Curr. Issues Mol. Biol. 2023;45:2609–2628. doi: 10.3390/cimb45030171. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Shao F., Wang X., Wu H., Wu Q., Zhang J. Microglia and Neuroinflammation: Crucial Pathological Mechanisms in Traumatic Brain Injury-Induced Neurodegeneration. Front. Aging Neurosci. 2022;14:825086. doi: 10.3389/fnagi.2022.825086. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Sims R., van der Lee S.J., Naj A.C., Bellenguez C., Badarinarayan N., Jakobsdottir J., Kunkle B.W., Boland A., Raybould R., Bis J.C., et al. Rare Coding Variants in PLCG2, ABI3, and TREM2 Implicate Microglial-Mediated Innate Immunity in Alzheimer’s Disease. Nat. Genet. 2017;49:1373–1384. doi: 10.1038/ng.3916. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Doorn K.J., Moors T., Drukarch B., van de Berg W.D., Lucassen P.J., van Dam A.-M. Microglial Phenotypes and Toll-like Receptor 2 in the Substantia Nigra and Hippocampus of Incidental Lewy Body Disease Cases and Parkinson’s Disease Patients. Acta Neuropathol. Commun. 2014;2:90. doi: 10.1186/s40478-014-0090-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Smajić S., Prada-Medina C.A., Landoulsi Z., Ghelfi J., Delcambre S., Dietrich C., Jarazo J., Henck J., Balachandran S., Pachchek S., et al. Single-Cell Sequencing of Human Midbrain Reveals Glial Activation and a Parkinson-Specific Neuronal State. Brain. 2022;145:964–978. doi: 10.1093/brain/awab446. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Prineas J.W., Kwon E.E., Cho E.-S., Sharer L.R., Barnett M.H., Oleszak E.L., Hoffman B., Morgan B.P. Immunopathology of Secondary-Progressive Multiple Sclerosis. Ann. Neurol. 2001;50:646–657. doi: 10.1002/ana.1255. [DOI] [PubMed] [Google Scholar]
- 30.Zrzavy T., Hametner S., Wimmer I., Butovsky O., Weiner H.L., Lassmann H. Loss of ‘Homeostatic’ Microglia and Patterns of Their Activation in Active Multiple Sclerosis. Brain. 2017;140:1900–1913. doi: 10.1093/brain/awx113. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Prinz M., Masuda T., Wheeler M.A., Quintana F.J. Microglia and Central Nervous System-Associated Macrophages-From Origin to Disease Modulation. Annu. Rev. Immunol. 2021;39:251–277. doi: 10.1146/annurev-immunol-093019-110159. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Bartholomäus I., Kawakami N., Odoardi F., Schläger C., Miljkovic D., Ellwart J.W., Klinkert W.E.F., Flügel-Koch C., Issekutz T.B., Wekerle H., et al. Effector T Cell Interactions with Meningeal Vascular Structures in Nascent Autoimmune CNS Lesions. Nature. 2009;462:94–98. doi: 10.1038/nature08478. [DOI] [PubMed] [Google Scholar]
- 33.Wasser B., Luchtman D., Löffel J., Robohm K., Birkner K., Stroh A., Vogelaar C.F., Zipp F., Bittner S. CNS-Localized Myeloid Cells Capture Living Invading T Cells during Neuroinflammation. J. Exp. Med. 2020;217:e20190812. doi: 10.1084/jem.20190812. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.De Schepper S., Ge J.Z., Crowley G., Ferreira L.S.S., Garceau D., Toomey C.E., Sokolova D., Rueda-Carrasco J., Shin S.-H., Kim J.-S., et al. Perivascular Cells Induce Microglial Phagocytic States and Synaptic Engulfment via SPP1 in Mouse Models of Alzheimer’s Disease. Nat. Neurosci. 2023;26:406–415. doi: 10.1038/s41593-023-01257-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Prinz M., Schmidt H., Mildner A., Knobeloch K.-P., Hanisch U.-K., Raasch J., Merkler D., Detje C., Gutcher I., Mages J., et al. Distinct and Nonredundant In Vivo Functions of IFNAR on Myeloid Cells Limit Autoimmunity in the Central Nervous System. Immunity. 2008;28:675–686. doi: 10.1016/j.immuni.2008.03.011. [DOI] [PubMed] [Google Scholar]
- 36.Rajan W.D., Wojtas B., Gielniewski B., Miró-Mur F., Pedragosa J., Zawadzka M., Pilanc P., Planas A.M., Kaminska B. Defining Molecular Identity and Fates of CNS-Border Associated Macrophages after Ischemic Stroke in Rodents and Humans. Neurobiol. Dis. 2020;137:104722. doi: 10.1016/j.nbd.2019.104722. [DOI] [PubMed] [Google Scholar]
- 37.Bechmann I., Priller J., Kovac A., Böntert M., Wehner T., Klett F.F., Bohsung J., Stuschke M., Dirnagl U., Nitsch R. Immune Surveillance of Mouse Brain Perivascular Spaces by Blood-Borne Macrophages. Eur. J. Neurosci. 2001;14:1651–1658. doi: 10.1046/j.0953-816x.2001.01793.x. [DOI] [PubMed] [Google Scholar]
- 38.Hickey W.F., Vass K., Lassmann H. Bone Marrow-Derived Elements in the Central Nervous System: An Immunohistochemical and Ultrastructural Survey of Rat Chimeras. J. Neuropathol. Exp. Neurol. 1992;51:246–256. doi: 10.1097/00005072-199205000-00002. [DOI] [PubMed] [Google Scholar]
- 39.Mass E., Ballesteros I., Farlik M., Halbritter F., Günther P., Crozet L., Jacome-Galarza C.E., Händler K., Klughammer J., Kobayashi Y., et al. Specification of Tissue-Resident Macrophages during Organogenesis. Science. 2016;353:aaf4238. doi: 10.1126/science.aaf4238. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Masuda T., Amann L., Monaco G., Sankowski R., Staszewski O., Krueger M., Del Gaudio F., He L., Paterson N., Nent E., et al. Specification of CNS Macrophage Subsets Occurs Postnatally in Defined Niches. Nature. 2022;604:740–748. doi: 10.1038/s41586-022-04596-2. [DOI] [PubMed] [Google Scholar]
- 41.Cugurra A., Mamuladze T., Rustenhoven J., Dykstra T., Beroshvili G., Greenberg Z.J., Baker W., Papadopoulos Z., Drieu A., Blackburn S., et al. Skull and Vertebral Bone Marrow Are Myeloid Cell Reservoirs for the Meninges and CNS Parenchyma. Science. 2021;373:eabf7844. doi: 10.1126/science.abf7844. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Wu X., Saito T., Saido T.C., Barron A.M., Ruedl C. Microglia and CD206+ Border-Associated Mouse Macrophages Maintain Their Embryonic Origin during Alzheimer’s Disease. eLife. 2021;10:e71879. doi: 10.7554/eLife.71879. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Huang G., Zhang P., Hirai H., Elf S., Yan X., Chen Z., Koschmieder S., Okuno Y., Dayaram T., Growney J.D., et al. PU.1 Is a Major Downstream Target of AML1 (RUNX1) in Adult Mouse Hematopoiesis. Nat. Genet. 2008;40:51–60. doi: 10.1038/ng.2007.7. [DOI] [PubMed] [Google Scholar]
- 44.Kierdorf K., Erny D., Goldmann T., Sander V., Schulz C., Perdiguero E.G., Wieghofer P., Heinrich A., Riemke P., Hölscher C., et al. Microglia Emerge from Erythromyeloid Precursors via Pu.1- and Irf8-Dependent Pathways. Nat. Neurosci. 2013;16:273–280. doi: 10.1038/nn.3318. [DOI] [PubMed] [Google Scholar]
- 45.Herbomel P., Thisse B., Thisse C. Zebrafish Early Macrophages Colonize Cephalic Mesenchyme and Developing Brain, Retina, and Epidermis through a M-CSF Receptor-Dependent Invasive Process. Dev. Biol. 2001;238:274–288. doi: 10.1006/dbio.2001.0393. [DOI] [PubMed] [Google Scholar]
- 46.Butovsky O., Jedrychowski M.P., Moore C.S., Cialic R., Lanser A.J., Gabriely G., Koeglsperger T., Dake B., Wu P.M., Doykan C.E., et al. Identification of a Unique TGF-β–Dependent Molecular and Functional Signature in Microglia. Nat. Neurosci. 2014;17:131–143. doi: 10.1038/nn.3599. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Ivan D.C., Berve K.C., Walthert S., Monaco G., Borst K., Bouillet E., Ferreira F., Lee H., Steudler J., Buch T., et al. Insulin-like Growth Factor-1 Receptor Controls the Function of CNS-Resident Macrophages and Their Contribution to Neuroinflammation. Acta Neuropathol. Commun. 2023;11:35. doi: 10.1186/s40478-023-01535-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Hamilton J.A., Achuthan A. Colony Stimulating Factors and Myeloid Cell Biology in Health and Disease. Trends Immunol. 2013;34:81–89. doi: 10.1016/j.it.2012.08.006. [DOI] [PubMed] [Google Scholar]
- 49.Hamilton J.A. Colony-Stimulating Factors in Inflammation and Autoimmunity. Nat. Rev. Immunol. 2008;8:533–544. doi: 10.1038/nri2356. [DOI] [PubMed] [Google Scholar]
- 50.Sauter K.A., Bouhlel M.A., O’Neal J., Sester D.P., Tagoh H., Ingram R.M., Pridans C., Bonifer C., Hume D.A. The Function of the Conserved Regulatory Element within the Second Intron of the Mammalian Csf1r Locus. PLoS ONE. 2013;8:e54935. doi: 10.1371/journal.pone.0054935. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Munro D.A.D., Bradford B.M., Mariani S.A., Hampton D.W., Vink C.S., Chandran S., Hume D.A., Pridans C., Priller J. CNS Macrophages Differentially Rely on an Intronic Csf1r Enhancer for Their Development. Dev. Camb. Engl. 2020;147:dev194449. doi: 10.1242/dev.194449. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Rojo R., Raper A., Ozdemir D.D., Lefevre L., Grabert K., Wollscheid-Lengeling E., Bradford B., Caruso M., Gazova I., Sánchez A., et al. Deletion of a Csf1r Enhancer Selectively Impacts CSF1R Expression and Development of Tissue Macrophage Populations. Nat. Commun. 2019;10:3215. doi: 10.1038/s41467-019-11053-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.Hagemeyer N., Kierdorf K., Frenzel K., Xue J., Ringelhan M., Abdullah Z., Godin I., Wieghofer P., Costa Jordão M.J., Ulas T., et al. Transcriptome-Based Profiling of Yolk Sac-Derived Macrophages Reveals a Role for Irf8 in Macrophage Maturation. EMBO J. 2016;35:1730–1744. doi: 10.15252/embj.201693801. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Moura Silva H., Kitoko J.Z., Queiroz C.P., Kroehling L., Matheis F., Yang K.L., Reis B.S., Ren-Fielding C., Littman D.R., Bozza M.T., et al. C-MAF-Dependent Perivascular Macrophages Regulate Diet-Induced Metabolic Syndrome. Sci. Immunol. 2021;6:eabg7506. doi: 10.1126/sciimmunol.abg7506. [DOI] [PubMed] [Google Scholar]
- 55.Wang Q., Zhao N., Kennard S., Lilly B. Notch2 and Notch3 Function Together to Regulate Vascular Smooth Muscle Development. PloS ONE. 2012;7:e37365. doi: 10.1371/journal.pone.0037365. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56.Dermitzakis I., Manthou M.E., Meditskou S., Miliaras D., Kesidou E., Boziki M., Petratos S., Grigoriadis N., Theotokis P. Developmental Cues and Molecular Drivers in Myelinogenesis: Revisiting Early Life to Re-Evaluate the Integrity of CNS Myelin. Curr. Issues Mol. Biol. 2022;44:3208–3237. doi: 10.3390/cimb44070222. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.The Human Protein Atlas. [(accessed on 15 January 2023)]. Available online: https://www.proteinatlas.org/
- 58.Home-Gene-NCBI. [(accessed on 15 January 2023)]; Available online: https://www.ncbi.nlm.nih.gov/gene/
- 59.Nayak D., Zinselmeyer B.H., Corps K.N., McGavern D.B. In Vivo Dynamics of Innate Immune Sentinels in the CNS. Intravital. 2012;1:95–106. doi: 10.4161/intv.22823. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.Schain A.J., Melo-Carrillo A., Borsook D., Grutzendler J., Strassman A.M., Burstein R. Activation of Pial and Dural Macrophages and Dendritic Cells by Cortical Spreading Depression: Activation of Meningeal Immune Cells by CSD. Ann. Neurol. 2018;83:508–521. doi: 10.1002/ana.25169. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.McMenamin P.G., Wealthall R.J., Deverall M., Cooper S.J., Griffin B. Macrophages and Dendritic Cells in the Rat Meninges and Choroid Plexus: Three-Dimensional Localisation by Environmental Scanning Electron Microscopy and Confocal Microscopy. Cell Tissue Res. 2003;313:259–269. doi: 10.1007/s00441-003-0779-0. [DOI] [PubMed] [Google Scholar]
- 62.Ling E.-A., Kaur C., Lu J. Origin, Nature, and Some Functional Considerations of Intraventricular Macrophages, with Special Reference to the Epiplexus Cells. Microsc. Res. Tech. 1998;41:43–56. doi: 10.1002/(SICI)1097-0029(19980401)41:1<43::AID-JEMT5>3.0.CO;2-V. [DOI] [PubMed] [Google Scholar]
- 63.Barkauskas D.S., Evans T.A., Myers J., Petrosiute A., Silver J., Huang A.Y. Extravascular CX3CR1+ Cells Extend Intravascular Dendritic Processes into Intact Central Nervous System Vessel Lumen. Microsc. Microanal. Off. J. Microsc. Soc. Am. Microbeam Anal. Soc. Microsc. Soc. Can. 2013;19:778–790. doi: 10.1017/S1431927613000482. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.Russo M.V., Latour L.L., McGavern D.B. Distinct Myeloid Cell Subsets Promote Meningeal Remodeling and Vascular Repair after Mild Traumatic Brain Injury. Nat. Immunol. 2018;19:442–452. doi: 10.1038/s41590-018-0086-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65.Colonna M., Butovsky O. Microglia Function in the Central Nervous System During Health and Neurodegeneration. Annu. Rev. Immunol. 2017;35:441–468. doi: 10.1146/annurev-immunol-051116-052358. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66.Tremblay M.-È., Stevens B., Sierra A., Wake H., Bessis A., Nimmerjahn A. The Role of Microglia in the Healthy Brain. J. Neurosci. 2011;31:16064–16069. doi: 10.1523/JNEUROSCI.4158-11.2011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67.Butovsky O., Weiner H.L. Microglial Signatures and Their Role in Health and Disease. Nat. Rev. Neurosci. 2018;19:622–635. doi: 10.1038/s41583-018-0057-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Lenz K.M., Nelson L.H. Microglia and Beyond: Innate Immune Cells As Regulators of Brain Development and Behavioral Function. Front. Immunol. 2018;9:698. doi: 10.3389/fimmu.2018.00698. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Chen Z., Trapp B.D. Microglia and Neuroprotection. J. Neurochem. 2016;136((Suppl. 1)):10–17. doi: 10.1111/jnc.13062. [DOI] [PubMed] [Google Scholar]
- 70.Goddery E.N., Fain C.E., Lipovsky C.G., Ayasoufi K., Yokanovich L.T., Malo C.S., Khadka R.H., Tritz Z.P., Jin F., Hansen M.J., et al. Microglia and Perivascular Macrophages Act as Antigen Presenting Cells to Promote CD8 T Cell Infiltration of the Brain. Front. Immunol. 2021;12:726421. doi: 10.3389/fimmu.2021.726421. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 71.Fabriek B.O., Van Haastert E.S., Galea I., Polfliet M.M.J., Döpp E.D., Van Den Heuvel M.M., Van Den Berg T.K., De Groot C.J.A., Van Der Valk P., Dijkstra C.D. CD163-Positive Perivascular Macrophages in the Human CNS Express Molecules for Antigen Recognition and Presentation. Glia. 2005;51:297–305. doi: 10.1002/glia.20208. [DOI] [PubMed] [Google Scholar]
- 72.Mato M., Ookawara S., Sakamoto A., Aikawa E., Ogawa T., Mitsuhashi U., Masuzawa T., Suzuki H., Honda M., Yazaki Y., et al. Involvement of Specific Macrophage-Lineage Cells Surrounding Arterioles in Barrier and Scavenger Function in Brain Cortex. Proc. Natl. Acad. Sci. USA. 1996;93:3269–3274. doi: 10.1073/pnas.93.8.3269. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73.Lim H.Y., Lim S.Y., Tan C.K., Thiam C.H., Goh C.C., Carbajo D., Chew S.H.S., See P., Chakarov S., Wang X.N., et al. Hyaluronan Receptor LYVE-1-Expressing Macrophages Maintain Arterial Tone through Hyaluronan-Mediated Regulation of Smooth Muscle Cell Collagen. Immunity. 2018;49:326–341.e7. doi: 10.1016/j.immuni.2018.06.008. [DOI] [PubMed] [Google Scholar]
- 74.He H., Mack J.J., Güç E., Warren C.M., Squadrito M.L., Kilarski W.W., Baer C., Freshman R.D., McDonald A.I., Ziyad S., et al. Perivascular Macrophages Limit Permeability. Arterioscler. Thromb. Vasc. Biol. 2016;36:2203–2212. doi: 10.1161/ATVBAHA.116.307592. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 75.Galanternik M.V., Castranova D., Gore A.V., Blewett N.H., Jung H.M., Stratman A.N., Kirby M.R., Iben J., Miller M.F., Kawakami K., et al. A Novel Perivascular Cell Population in the Zebrafish Brain. eLife. 2017;6:e24369. doi: 10.7554/eLife.24369. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Liu C., Wu C., Yang Q., Gao J., Li L., Yang D., Luo L. Macrophages Mediate the Repair of Brain Vascular Rupture through Direct Physical Adhesion and Mechanical Traction. Immunity. 2016;44:1162–1176. doi: 10.1016/j.immuni.2016.03.008. [DOI] [PubMed] [Google Scholar]
- 77.Jais A., Solas M., Backes H., Chaurasia B., Kleinridders A., Theurich S., Mauer J., Steculorum S.M., Hampel B., Goldau J., et al. Myeloid-Cell-Derived VEGF Maintains Brain Glucose Uptake and Limits Cognitive Impairment in Obesity. Cell. 2016;165:882–895. doi: 10.1016/j.cell.2016.03.033. [DOI] [PubMed] [Google Scholar]
- 78.Mato M., Ookawara S., Sano M., Fukuda S. Uptake of Fat by Fluorescent Granular Perithelial Cells in Cerebral Cortex after Administration of Fat Rich Chow. Experientia. 1982;38:1496–1498. doi: 10.1007/BF01955791. [DOI] [PubMed] [Google Scholar]
- 79.Zhang Z., Li Z., Ma Z., Deng M., Xing M., Wu J., Jiang S., Wang Q., Guo Q., Zou W. Annexin A3 as a Marker Protein for Microglia in the Central Nervous System of Rats. Neural Plast. 2021;2021:e5575090. doi: 10.1155/2021/5575090. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80.Konishi H., Kobayashi M., Kunisawa T., Imai K., Sayo A., Malissen B., Crocker P.R., Sato K., Kiyama H. Siglec-H Is a Microglia-Specific Marker That Discriminates Microglia from CNS-Associated Macrophages and CNS-Infiltrating Monocytes. Glia. 2017;65:1927–1943. doi: 10.1002/glia.23204. [DOI] [PubMed] [Google Scholar]
- 81.Buttgereit A., Lelios I., Yu X., Vrohlings M., Krakoski N.R., Gautier E.L., Nishinakamura R., Becher B., Greter M. Sall1 Is a Transcriptional Regulator Defining Microglia Identity and Function. Nat. Immunol. 2016;17:1397–1406. doi: 10.1038/ni.3585. [DOI] [PubMed] [Google Scholar]
- 82.Kim W.-K., Alvarez X., Fisher J., Bronfin B., Westmoreland S., McLaurin J., Williams K. CD163 Identifies Perivascular Macrophages in Normal and Viral Encephalitic Brains and Potential Precursors to Perivascular Macrophages in Blood. Am. J. Pathol. 2006;168:822–834. doi: 10.2353/ajpath.2006.050215. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 83.Faraco G., Sugiyama Y., Lane D., Garcia-Bonilla L., Chang H., Santisteban M.M., Racchumi G., Murphy M., Van Rooijen N., Anrather J., et al. Perivascular Macrophages Mediate the Neurovascular and Cognitive Dysfunction Associated with Hypertension. J. Clin. Investig. 2016;126:4674–4689. doi: 10.1172/JCI86950. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 84.Zeisel A., Muñoz-Manchado A.B., Codeluppi S., Lönnerberg P., La Manno G., Juréus A., Marques S., Munguba H., He L., Betsholtz C., et al. Cell Types in the Mouse Cortex and Hippocampus Revealed by Single-Cell RNA-Seq. Science. 2015;347:1138–1142. doi: 10.1126/science.aaa1934. [DOI] [PubMed] [Google Scholar]
- 85.Ajami B., Samusik N., Wieghofer P., Ho P.P., Crotti A., Bjornson Z., Prinz M., Fantl W.J., Nolan G.P., Steinman L. Single-Cell Mass Cytometry Reveals Distinct Populations of Brain Myeloid Cells in Mouse Neuroinflammation and Neurodegeneration Models. Nat. Neurosci. 2018;21:541–551. doi: 10.1038/s41593-018-0100-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 86.Cummings J. Alzheimer’s Disease Diagnostic Criteria: Practical Applications. Alzheimers Res. Ther. 2012;4:35. doi: 10.1186/alzrt138. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 87.Tiwari S., Atluri V., Kaushik A., Yndart A., Nair M. Alzheimer’s Disease: Pathogenesis, Diagnostics, and Therapeutics. Int. J. Nanomed. 2019;14:5541–5554. doi: 10.2147/IJN.S200490. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 88.Muralidar S., Ambi S.V., Sekaran S., Thirumalai D., Palaniappan B. Role of Tau Protein in Alzheimer’s Disease: The Prime Pathological Player. Int. J. Biol. Macromol. 2020;163:1599–1617. doi: 10.1016/j.ijbiomac.2020.07.327. [DOI] [PubMed] [Google Scholar]
- 89.Weber S.A., Patel R.K., Lutsep H.L. Cerebral Amyloid Angiopathy: Diagnosis and Potential Therapies. Expert Rev. Neurother. 2018;18:503–513. doi: 10.1080/14737175.2018.1480938. [DOI] [PubMed] [Google Scholar]
- 90.Hawkes C.A., McLaurin J. Selective Targeting of Perivascular Macrophages for Clearance of Beta-Amyloid in Cerebral Amyloid Angiopathy. Proc. Natl. Acad. Sci. USA. 2009;106:1261–1266. doi: 10.1073/pnas.0805453106. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 91.Park L., Uekawa K., Garcia-Bonilla L., Koizumi K., Murphy M., Pistik R., Younkin L., Younkin S., Zhou P., Carlson G., et al. Brain Perivascular Macrophages Initiate the Neurovascular Dysfunction of Alzheimer Aβ Peptides. Circ. Res. 2017;121:258–269. doi: 10.1161/CIRCRESAHA.117.311054. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 92.Simon D.K., Tanner C.M., Brundin P. Parkinson Disease Epidemiology, Pathology, Genetics, and Pathophysiology. Clin. Geriatr. Med. 2020;36:1–12. doi: 10.1016/j.cger.2019.08.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 93.Lee J.-W., Chun W., Lee H.J., Kim S.-M., Min J.-H., Kim D.-Y., Kim M.-O., Ryu H.W., Lee S.U. The Role of Microglia in the Development of Neurodegenerative Diseases. Biomedicines. 2021;9:1449. doi: 10.3390/biomedicines9101449. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 94.Gómez-Benito M., Granado N., García-Sanz P., Michel A., Dumoulin M., Moratalla R. Modeling Parkinson’s Disease with the Alpha-Synuclein Protein. Front. Pharmacol. 2020;11:356. doi: 10.3389/fphar.2020.00356. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 95.Guo M., Wang J., Zhao Y., Feng Y., Han S., Dong Q., Cui M., Tieu K. Microglial Exosomes Facilitate α-Synuclein Transmission in Parkinson’s Disease. Brain J. Neurol. 2020;143:1476–1497. doi: 10.1093/brain/awaa090. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 96.Schonhoff A., Figge D., Williams G., Jurkuvenaite A., Gallups N., Childers G., Webster J., Standaert D., Goldman J., Harms A. Border-Associated Macrophages Mediate the Neuroinflammatory Response in an Alpha-Synuclein Model of Parkinson Disease. bioRxiv. :2022. doi: 10.1101/2022.10.12.511960. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 97.Qin H., Buckley J.A., Li X., Liu Y., Fox T.H., Meares G.P., Yu H., Yan Z., Harms A.S., Li Y., et al. Inhibition of the JAK/STAT Pathway Protects Against α-Synuclein-Induced Neuroinflammation and Dopaminergic Neurodegeneration. J. Neurosci. 2016;36:5144–5159. doi: 10.1523/JNEUROSCI.4658-15.2016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 98.Walton C., King R., Rechtman L., Kaye W., Leray E., Marrie R.A., Robertson N., La Rocca N., Uitdehaag B., van der Mei I., et al. Rising Prevalence of Multiple Sclerosis Worldwide: Insights from the Atlas of MS, Third Edition. Mult. Scler. J. 2020;26:1816–1821. doi: 10.1177/1352458520970841. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 99.Mirmosayyeb O., Brand S., Barzegar M., Afshari-Safavi A., Nehzat N., Shaygannejad V., Sadeghi Bahmani D. Clinical Characteristics and Disability Progression of Early- and Late-Onset Multiple Sclerosis Compared to Adult-Onset Multiple Sclerosis. J. Clin. Med. 2020;9:1326. doi: 10.3390/jcm9051326. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 100.Polman C.H., Reingold S.C., Banwell B., Clanet M., Cohen J.A., Filippi M., Fujihara K., Havrdova E., Hutchinson M., Kappos L., et al. Diagnostic Criteria for Multiple Sclerosis: 2010 Revisions to the McDonald Criteria. Ann. Neurol. 2011;69:292–302. doi: 10.1002/ana.22366. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 101.Alcina A., Fedetz M., Vidal-Cobo I., Andrés-León E., García-Sánchez M.-I., Barroso-del-Jesus A., Eichau S., Gil-Varea E., Villar L.-M., Saiz A., et al. Identification of the Genetic Mechanism That Associates L3MBTL3 to Multiple Sclerosis. Hum. Mol. Genet. 2022;31:2155–2163. doi: 10.1093/hmg/ddac009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 102.Jandric D., Lipp I., Paling D., Rog D., Castellazzi G., Haroon H., Parkes L., Parker G.J.M., Tomassini V., Muhlert N. Mechanisms of Network Changes in Cognitive Impairment in Multiple Sclerosis. Neurology. 2021;97:e1886–e1897. doi: 10.1212/WNL.0000000000012834. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 103.Correale J., Marrodan M., Ysrraelit M.C. Mechanisms of Neurodegeneration and Axonal Dysfunction in Progressive Multiple Sclerosis. Biomedicines. 2019;7:14. doi: 10.3390/biomedicines7010014. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 104.Jäckle K., Zeis T., Schaeren-Wiemers N., Junker A., van der Meer F., Kramann N., Stadelmann C., Brück W. Molecular Signature of Slowly Expanding Lesions in Progressive Multiple Sclerosis. Brain. 2020;143:2073–2088. doi: 10.1093/brain/awaa158. [DOI] [PubMed] [Google Scholar]
- 105.Kamma E., Lasisi W., Libner C., Ng H.S., Plemel J.R. Central Nervous System Macrophages in Progressive Multiple Sclerosis: Relationship to Neurodegeneration and Therapeutics. J. Neuroinflamm. 2022;19:45. doi: 10.1186/s12974-022-02408-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 106.Miedema A., Gerrits E., Brouwer N., Jiang Q., Kracht L., Meijer M., Nutma E., Peferoen-Baert R., Pijnacker A.T.E., Wesseling E.M., et al. Brain Macrophages Acquire Distinct Transcriptomes in Multiple Sclerosis Lesions and Normal Appearing White Matter. Acta Neuropathol. Commun. 2022;10:8. doi: 10.1186/s40478-021-01306-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 107.Locatelli G., Theodorou D., Kendirli A., Jordão M.J.C., Staszewski O., Phulphagar K., Cantuti-Castelvetri L., Dagkalis A., Bessis A., Simons M., et al. Mononuclear Phagocytes Locally Specify and Adapt Their Phenotype in a Multiple Sclerosis Model. Nat. Neurosci. 2018;21:1196–1208. doi: 10.1038/s41593-018-0212-3. [DOI] [PubMed] [Google Scholar]
- 108.Theotokis P., Lourbopoulos A., Touloumi O., Lagoudaki R., Kofidou E., Nousiopoulou E., Poulatsidou K.-N., Kesidou E., Tascos N., Spandou E., et al. Time Course and Spatial Profile of Nogo-A Expression in Experimental Autoimmune Encephalomyelitis in C57BL/6 Mice. J. Neuropathol. Exp. Neurol. 2012;71:907–920. doi: 10.1097/NEN.0b013e31826caebe. [DOI] [PubMed] [Google Scholar]
- 109.Theotokis P., Touloumi O., Lagoudaki R., Nousiopoulou E., Kesidou E., Siafis S., Tselios T., Lourbopoulos A., Karacostas D., Grigoriadis N., et al. Nogo Receptor Complex Expression Dynamics in the Inflammatory Foci of Central Nervous System Experimental Autoimmune Demyelination. J. Neuroinflamm. 2016;13:265. doi: 10.1186/s12974-016-0730-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 110.Montilla A., Zabala A., Er-Lukowiak M., Rissiek B., Magnus T., Rodriguez-Iglesias N., Sierra A., Matute C., Domercq M. Microglia and Meningeal Macrophages Depletion Delays the Onset of Experimental Autoimmune Encephalomyelitis. Cell Death Dis. 2023;14:16. doi: 10.1038/s41419-023-05551-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 111.McCarthy D.P., Richards M.H., Miller S.D. Mouse Models of Multiple Sclerosis: Experimental Autoimmune Encephalomyelitis and Theiler’s Virus-Induced Demyelinating Disease. Methods Mol. Biol. 2012;900:381–401. doi: 10.1007/978-1-60761-720-4_19. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 112.Donninelli G., Saraf-Sinik I., Mazziotti V., Capone A., Grasso M.G., Battistini L., Reynolds R., Magliozzi R., Volpe E. Interleukin-9 Regulates Macrophage Activation in the Progressive Multiple Sclerosis Brain. J. Neuroinflamm. 2020;17:149. doi: 10.1186/s12974-020-01770-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 113.Roczkowsky A., Doan M.A.L., Hlavay B., Mamik M.K., Branton W.G., McKenzie B.A., Saito L.B., Schmitt L., Eitzen G., Di Cara F., et al. Peroxisome Injury in Multiple Sclerosis: Protective Effects of 4-Phenylbutyrate in CNS-Associated Macrophages. J. Neurosci. Off. J. Soc. Neurosci. 2022;42:7152–7165. doi: 10.1523/JNEUROSCI.0312-22.2022. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 114.Grajchen E., Hendriks J.J.A., Bogie J.F.J. The Physiology of Foamy Phagocytes in Multiple Sclerosis. Acta Neuropathol. Commun. 2018;6:124. doi: 10.1186/s40478-018-0628-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 115.Haidar M., Loix M., Vanherle S., Dierckx T., Vangansewinkel T., Gervois P., Wolfs E., Lambrichts I., Bogie J.F.J., Hendriks J.J.A. Targeting Lipophagy in Macrophages Improves Repair in Multiple Sclerosis. Autophagy. 2022;18:2697–2710. doi: 10.1080/15548627.2022.2047343. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 116.Pedragosa J., Salas-Perdomo A., Gallizioli M., Cugota R., Miró-Mur F., Briansó F., Justicia C., Pérez-Asensio F., Marquez-Kisinousky L., Urra X., et al. CNS-Border Associated Macrophages Respond to Acute Ischemic Stroke Attracting Granulocytes and Promoting Vascular Leakage. Acta Neuropathol. Commun. 2018;6:76. doi: 10.1186/s40478-018-0581-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 117.Wan H., Brathwaite S., Ai J., Hynynen K., Macdonald R.L. Role of Perivascular and Meningeal Macrophages in Outcome following Experimental Subarachnoid Hemorrhage. J. Cereb. Blood Flow Metab. 2021;41:1842–1857. doi: 10.1177/0271678X20980296. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 118.Kolosowska N., Keuters M.H., Wojciechowski S., Keksa-Goldsteine V., Laine M., Malm T., Goldsteins G., Koistinaho J., Dhungana H. Peripheral Administration of IL-13 Induces Anti-Inflammatory Microglial/Macrophage Responses and Provides Neuroprotection in Ischemic Stroke. Neurotherapeutics. 2019;16:1304–1319. doi: 10.1007/s13311-019-00761-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
Not applicable.