Abstract
Background
Vitrectomy is an established treatment for the complications of proliferative diabetic retinopathy (PDR). However, a number of complications can occur during and after vitrectomy for PDR. These include bleeding and the creation of retinal holes during surgery, and bleeding, retinal detachment and scar tissue on the retina after surgery. These complications can limit vision, require further surgery and delay recovery. The use of anti‐vascular endothelial growth factor (anti‐VEGF) agents injected into the eye before surgery has been proposed to reduce the occurrence of these complications. Anti‐VEGF agents can reduce the amount and vascularity of abnormal new vessels associated with PDR, facilitating their dissection during surgery, reducing intra‐ and postoperative bleeding, and potentially improving outcomes.
Objectives
To assess the effects of perioperative anti‐VEGF use on the outcomes of vitrectomy for the treatment of complications for proliferative diabetic retinopathy (PDR).
Search methods
We searched the Cochrane Central Register of Controlled Trials (CENTRAL; which contains the Cochrane Eyes and Vision Trials Register; 2022, Issue 6); Ovid MEDLINE; Ovid Embase; the ISRCTN registry; ClinicalTrials.gov and the WHO ICTRP. The date of the search was 22 June 2022.
Selection criteria
We included randomised controlled trials (RCTs) that looked at the use of anti‐VEGFs and the incidence of complications in people undergoing vitrectomy for PDR.
Data collection and analysis
Two review authors independently assessed and extracted the data. We used the standard methodological procedures expected by Cochrane.
The critical outcomes of the review were the mean difference in best corrected visual acuity (BCVA) between study arms at six (± three) months after the primary vitrectomy, the incidence of early postoperative vitreous cavity haemorrhage (POVCH, within four weeks postoperatively), the incidence of late POVCH (occurring more than four weeks postoperatively), the incidence of revision surgery for POVCH within six months, the incidence of revision surgery for recurrent traction/macular pucker of any type and/or rhegmatogenous retinal detachment within six months and vision‐related quality of life (VRQOL) measures. Important outcomes included the proportion of people with a visual acuity of counting fingers (1.8 logMAR or worse), the number of operative retinal breaks reported and the frequency of silicone oil tamponade required at time of surgery.
Main results
The current review includes 28 RCTs that looked at the pre‐ or intraoperative use of intravitreal anti‐VEGFs to improve the outcomes of pars plana vitrectomy for complications of PDR. The studies were conducted in a variety of countries (11 from China, three from Iran, two from Italy, two from Mexico and the remaining studies from South Korea, the UK, Egypt, Brazil, Japan, Canada, the USA, Indonesia and Pakistan). The inclusion criteria for entry into the studies were the well‐recognised complications of proliferative retinopathy: non‐clearing vitreous haemorrhage, tractional retinal detachment involving the macula or combined tractional rhegmatogenous detachment. The included studies randomised a total of 1914 eyes.
We identified methodological issues in all of the included studies. Risk of bias was highest for masking of participants and investigators, and a number of studies were unclear when describing randomisation methods and sequence allocation.
Participants receiving intravitreal anti‐VEGF in addition to pars plana vitrectomy achieved better BCVA at six months compared to people undergoing vitrectomy alone (mean difference (MD) ‐0.25 logMAR, 95% confidence interval (CI) ‐0.39 to ‐0.11; 13 studies, 699 eyes; low‐certainty evidence).
Pre‐ or intraoperative anti‐VEGF reduced the incidence of early POVCH (12% versus 31%, risk ratio (RR) 0.44, 95% CI 0.34 to 0.58; 14 studies, 1038 eyes; moderate‐certainty evidence).
Perioperative anti‐VEGF use was also associated with a reduction in the incidence of late POVCH (10% versus 23%, RR 0.47, 95% CI 0.30 to 0.74; 11 studies, 579 eyes; high‐certainty evidence).
The need for revision surgery for POVCH occurred less frequently in the anti‐VEGF group compared with control, but the confidence intervals were wide and compatible with no effect (4% versus 13%, RR 0.44, 95% CI 0.15 to 1.28; 4 studies 207 eyes; moderate‐certainty evidence). Similar imprecisely measured effects were seen for revision surgery for rhegmatogenous retinal detachment (5% versus 11%, RR 0.50, 95% CI 0.15 to 1.66; 4 studies, 145 eyes; low‐certainty evidence).
Anti‐VEGFs reduce the incidence of intraoperative retinal breaks (12% versus 31%, RR 0.37, 95% CI 0.24 to 0.59; 12 studies, 915 eyes; high‐certainty evidence) and the need for silicone oil (19% versus 41%, RR 0.46, 95% CI 0.27 to 0.80; 10 studies, 591 eyes; very low‐certainty evidence).
No data were available on quality of life outcomes or the proportion of participants with visual acuity of counting fingers or worse.
Authors' conclusions
The perioperative use of anti‐VEGF reduces the risk of late POVCH, probably results in lower early POVCH risk and may improve visual outcomes. It also reduces the incidence of intraoperative retinal breaks. The evidence is very uncertain about its effect on the need for silicone oil tamponade. The reported complications from its use appear to be low. Agreement on variables included and outcome standardisation is required in trials studying vitrectomy for PDR.
Keywords: Humans, Diabetes Mellitus, Diabetic Retinopathy, Diabetic Retinopathy/complications, Diabetic Retinopathy/surgery, Endothelial Growth Factors, Postoperative Hemorrhage, Postoperative Hemorrhage/surgery, Retinal Detachment, Retinal Detachment/etiology, Retinal Detachment/surgery, Retinal Perforations, Retinal Perforations/complications, Silicone Oils, Vitrectomy, Vitrectomy/adverse effects
Plain language summary
Anti‐VEGF for prevention of complications after vitrectomy for proliferative diabetic retinopathy
Why is this question important?
Proliferative diabetic retinopathy (PDR) is the most advanced stage of diabetic retinopathy, which is a complication of diabetes. It is caused by abnormal new blood vessels that grow on the retina, the light sensitive layer at the back of the eye. Pars plana vitrectomy is an established surgical treatment for the complications of PDR. During this operation, the gel‐like substance that exists inside the eye, called the vitreous, is removed. The most common reason for performing vitrectomy is non‐clearing vitreous haemorrhage, where there is bleeding in the inner part of the eye called the vitreous cavity. When this occurs, vitreous loses transparency and the light cannot pass through it, causing vision loss. Anti‐vascular endothelial growth factor agents (anti‐VEGFs) are drugs that can stop these abnormal blood vessels growing and control the leaking blood, when they are injected inside the eye. The injection of anti‐VEGF agents before vitrectomy for the complications of PDR may make surgery easier, reduce intra‐ and postoperative bleeding and improve outcomes. However, there is no clear evidence about the different types of anti‐VEGF agents, the best time to use them or their effect on other outcomes. We reviewed published research to determine whether anti‐VEGF injections around the time of surgery have an effect on the outcomes of vitrectomy for the treatment of complications of PDR.
What did we want to find out?
We wanted to find out if the additional use of anti‐VEGF agents either before or during diabetic vitrectomy surgery was better than diabetic vitrectomy alone in terms of:
‐ visual outcomes; ‐ incidence of early and late POVCH; ‐ incidence of revision surgery for POVCH in the first six months postoperatively; ‐ incidence of revision surgery for recurrent traction/macular pucker (structural alteration in the macula, the part of the eye which is responsible for sharp, central vision, thus causing decline of visual function) in the first six months postoperatively; ‐ vision‐related quality of life measures; ‐ proportion of people with poor visual acuity (counting fingers or worse); ‐ number of intraoperative retinal breaks (tears in the light sensitive layer of the eye); ‐ frequency of silicone oil tamponade (a tamponade agent used to push the retina towards the eye wall and keep it stable).
What did we do?
We searched for studies that compared any anti‐VEGF combined with vitrectomy versus vitrectomy with no anti‐VEGF or with sham treatment or with any other anti‐VEGF in people undergoing vitrectomy for the complications of PDR. We compared and summarised the results of the studies and rated our confidence in the evidence, based on factors such as study methods and sizes.
What did we find?
We found 28 studies that involved 1914 eyes undergoing vitrectomy for complications of proliferative diabetic retinopathy. Sample sizes varied from 20 to 214 participants. The studies were from China (11), Iran (three), Italy (two) and Mexico (two), and the remaining studies were from South Korea, UK, Egypt, Brazil, Japan, Canada, USA, Indonesia and Pakistan. One study was multi‐centre, including 13 clinical sites from nine countries. Two studies declared receiving funding from the manufacturer of the anti‐VEGF drug studied.
Main results
The additional use of anti‐VEGFs in diabetic vitrectomy may improve visual outcomes at six months postoperatively. Their use also reduces the risk of late POVCH and probably reduces the risk of early POVCH. Anti‐VEGFs reduce intraoperative retinal breaks and may reduce the requirement for silicone oil tamponade.
Anti‐VEGF use probably results in a lower need for revision vitrectomy for POVCH, and may reduce the need for revision surgery for recurrent traction and/or retinal detachment.
We found no studies to help us answer our question about quality of life and the proportion of people with visual acuity of counting fingers or less.
What are the limitations of the evidence?
We are confident that anti‐VEGF injections reduce the incidence of late POVCH and intraoperative retinal breaks (high‐certainty evidence), fairly certain that they reduce the incidence of early POVCH and the need for revision surgery for POVCH (moderate‐certainty evidence) but less certain about the effects on visual outcomes, revision surgery for retinal detachment and silicone oil use (low‐certainty evidence).
How up‐to‐date is this evidence?
This review updates our previous review. The evidence is up‐to‐date to 22 June 2022.
Summary of findings
Summary of findings 1. Summary of findings.
| Anti‐vascular endothelial growth factors in combination with vitrectomy for complications of proliferative diabetic retinopathy | ||||||
|
Patient or population: people with proliferative diabetic retinopathy undergoing vitrectomy Settings: hospital Intervention: anti‐VEGF Comparison: no anti‐VEGF | ||||||
| Outcomes | Illustrative comparative risks* (95% CI) | Relative effect (95% CI) | No of participants (studies) | Certainty of the evidence (GRADE) | Comments | |
| Assumed risk | Corresponding risk | |||||
| Control | Anti‐VEGF | |||||
|
Mean BCVA (logMAR) 6 ± 3 months BCVA logMAR score of 0 corresponds to a Snellen score of 6/6. Negative logMAR scores correspond to BCVA better than Snellen 6/6, whereas higher positive logMAR scores correspond to BCVA worse than Snellen 6/6. |
The mean visual acuity ranged across control groups from 0.51 to 2.07 logMAR | The mean visual acuity ranged across anti‐VEGF groups from 0.29 to 1.10 logMAR | MD ‐0.25 (‐0.39 to ‐0.11) | 699 (13) | ⊕⊕⊝⊝ Low1 | Anti‐VEGF administration may result in an improvement in visual acuity postoperatively compared to control |
|
Early POVCH |
312 per 1000 |
137 per 1000 (106 to 181) | RR 0.44 (0.34 to 0.58) | 1038 (14) | ⊕⊕⊕⊝ Moderate2 |
Anti‐VEGF administration probably results in fewer cases of early POVCH compared to control |
|
Late POVCH |
231 per 1000 |
108 per 1000 (69 to 171) | RR 0.47 (0.30 to 0.74) | 579 (11) | ⊕⊕⊕⊕ High3 |
Anti‐VEGF administration results in fewer cases of late POVCH compared to control |
| Revision surgery for POVCH | 130 per 1000 | 57 per 1000 (20 to 166) | RR 0.44 (0.15 to 1.28) | 207 (4) | ⊕⊕⊕⊝ Moderate4 |
Anti‐VEGF administration probably results in fewer cases of revision surgery for POVCH compared to control |
| Revision surgery for recurrent traction and/or RRD |
114 per 1000 |
57 per 1000 (17 to 189) | RR 0.50 (0.15 to 1.66) | 145 (4) | ⊕⊕⊝⊝ Low5 |
Anti‐VEGF administration may result in fewer cases of revision surgery for recurrent traction and/or RRD compared to control |
| Intraoperative retinal breaks | 311 per 1000 | 115 per 1000 (75 to 183) | RR 0.37 (0.24 to 0.59) | 915 (12) | ⊕⊕⊕⊕ High6 |
Anti‐VEGF administration results in fewer cases of intraoperative retinal breaks compared with control |
| Silicone oil use | 412 per 1000 | 190 per 1000 (111 to 330) | RR 0.46 (0.27 to 0.80) | 591 (10) | ⊕⊝⊝⊝ Very low7 |
Anti‐VEGF administration may result in less use of silicone oil compared with control |
| *The basis for the assumed risk (e.g. the median control group risk across studies) is provided in footnotes. The corresponding risk (and its 95% confidence interval) is based on the assumed risk in the comparison group and the relative effect of the intervention (and its 95% CI). BCVA: best corrected visual acuity; CI: confidence interval; MD: mean difference; RR: risk ratio; POVCH: postoperative vitreous cavity haemorrhage; RRD: rhegmatogenous retinal detachment; TRD: tractional retinal detachment; VEGF: vascular endothelial growth factor | ||||||
| GRADE Working Group grades of evidence High certainty: Further research is very unlikely to change our confidence in the estimate of effect. Moderate‐certainty: Further research is likely to have an important impact on our confidence in the estimate of effect and may change the estimate. Low‐certainty: Further research is very likely to have an important impact on our confidence in the estimate of effect and is likely to change the estimate. Very low‐certainty: We are very uncertain about the estimate. | ||||||
1Downgraded one level for inconsistency (I2 = 75%) and one level for study limitations because most of the studies were graded as unclear/high risk of bias.
2Downgraded one level for possible publication bias (asymmetry in funnel plot). Many studies in this analysis suffer from poor masking, however this probably is not an issue for this particular outcome and thus we decided not to downgrade another level.
3Similarly, many studies in this analysis suffer from poor masking, however this probably is not an issue for this particular outcome and thus we decided not to downgrade for risk of bias.
4Downgraded one level for imprecision (confidence intervals include 1 ‐ no effect).
5Downgraded one level for imprecision (confidence intervals include 1 ‐ no effect) and downgraded one level because the majority of the included studies in the analysis suffer from serious risk of bias (selection and detection bias).
6A few studies in this analysis suffer from questionable masking. However, we do not feel that this might have affected this particular outcome (i.e. surgical performance/difficulty of surgery).
7Downgraded one level for inconsistency (minimal overlap of confidence intervals between studies), one level for possible publication bias (asymmetry in funnel plot) and one level for study limitation (questionable masking).
Background
Pars plana vitrectomy is an established and successful treatment for the complications of proliferative diabetic retinopathy (PDR) (Ho 1992; Jackson 2015; McLeod 1991). Overall, up to 10% of people presenting with PDR require vitrectomy within one year, depending on the study and the patients investigated (Kaiser 2000; Vaideanu 2014). The most common indication for surgery is non‐clearing vitreous haemorrhage (Ho 1992; McLeod 1991). Other common indications are macula‐involving or macula‐threatening tractional retinal detachment (TRD) or combined rhegmatogenous/tractional retinal detachment (Jackson 2015).
Description of the condition
The aim of vitrectomy is to maximise visual function in the short and long term. However, diabetic vitrectomy can be a complex surgical procedure, particularly if delamination and/or segmentation of the fibrovascular membranes is required and there is retinal detachment present (Hutton 1980; Jackson 2015). Surgery can be complicated by a range of intra‐ and postoperative problems that can affect the visual outcome and limit recovery. These can be summarised as follows:
Intra‐ and early postoperative bleeding causing early postoperative vitreous cavity haemorrhage (POVCH).
Retinal break formation during surgery and postoperative rhegmatogenous retinal detachment.
Persistent or recurrent traction causing postoperative macular traction or tractional retinal detachment requiring repeat vitrectomy.
Recurrent intraocular bleeding later following surgery causing late POVCH.
Retinal status at the end of surgery requiring the insertion of silicone oil as tamponade, which can be associated with a range of postoperative problems including visual loss.
Aetiology of complications
Postoperative vitreous cavity haemorrhage (POVCH)
POVCH can be a significant complication, occurring in approximately 20% to 30% of cases, although the reported range is large (5% to 80% of cases) (Benson 1988; Blankenship 1986; Liggett 1987; Nagbal 2017; Novak 1984; Tolentino 1989; Virata 2001; Yorston 2008).
Although there can be overlap, POVCH occurs in two main forms:
Early POVCH, being present from the first few postoperative days and delaying visual recovery by non‐clearance.
Late POVCH, occurring later during follow‐up, commonly at two to six months postoperatively, after a postoperative period during which the vitreous cavity was clear.
Persistent haemorrhage can result from operative and postoperative oozing of the remnants of new vessels or dissected tissue, or directly from the sclerostomies used to perform surgery. It can also occur from clot lysis in the first few postoperative days. Leaching of red blood cells can occur from retained old haemorrhages in residual anterior vitreous, causing apparent POVCH (McLeod 1991; Novak 1984; Tolentino 1989). Intraocular pressure at the end of vitrectomy has also been reported to have an effect on anatomical and visual recovery. Higher pressures were reported to result in better visual and anatomical outcomes (Zhou 2020). Consequently, ensuring waterproof sclerostomies at the end of surgery, even if that means suturing them when in doubt, can be beneficial in preventing postoperative hypotony.
Recurrent POVCH can occur from recurrent traction on residual new vessels, or indeed postoperative new vessel growth in the posterior retina. PDR is well known to be related to a range of angiogenic factors, such as vascular endothelial growth factor (VEGF), and these can remain raised postoperatively (Stefansson 2009), with postoperative new vessel growth in the posterior retina. Studies have also shown that a common cause of recurrent haemorrhage is new anterior vessel growth at the inner sclerostomy sites associated with fibrous traction (Bhende 2000; Hershberger 2004; Hotta 2000; Kreiger 1993; Sawa 2000; Steel 2008; West 2000). Termed 'entry site neovascularisation' (ESNV) (McLeod 2000), this is thought to be an aberrant wound‐healing response related to the presence of retinal and pars plana ischaemia (Kreiger 1993; Yeh 2005). The presence of ESNV is difficult to observe clinically because of the extreme anterior location but can be confirmed at the time of revision surgery with deep scleral indentation or endoscopic techniques (West 2000). It can also be localised, with anterior segment high‐resolution ultrasonography of the inner sclerostomy sites (Bhende 2000; Hershberger 2004; Hotta 2000; Steel 2008).
Retinal breaks and postoperative rhegmatogenous retinal detachment
Retinal breaks may exist at the time of vitrectomy in the case of combined rhegmatogenous tractional retinal detachment but can also be caused by surgery. They can occur in three main types:
Posterior breaks related to traction and membrane dissection.
Peripheral surgical entry site breaks partly related to instrument exchange at the pars plana entry ports. These have significantly reduced with the advent of cannulated transconjunctival vitrectomy systems (Issa 2011).
Retinal breaks created as a result of vitreous separation, an important part of surgery. Occasionally, they are associated with predisposing retinal lesions including lattice degeneration.
If inadequately treated or associated with persistent or recurrent traction, retinal breaks can result in retinal detachment.
Persistent or recurrent traction
Preretinal traction can be complex to completely remove and can be occult with the phenomenon of vitreoschisis, a splitting of the posterior vitreous cortex into multiple layers with adherence to the retina, as a consequence of diabetes (Kroll 2014; Sebag 1996). Epiretinal membrane is observed postoperatively after diabetic vitrectomy in 20% to 50% of cases; it can be associated with macular thickening and recurrent tractional detachment, can affect visual outcome and has been reported to require revision surgery in 7% to 22% of cases (Blankenship 1985; Gupta 2012; Mehta 2020; Oshima 2009; Schiff 2007; Yorston 2008). The exact cause of this is uncertain, although surgical and proteomic risk factors have been described (Hsu 2014; Yoshida 2017).
Consequences and management of complications after occurrence
POVCH
People with POVCH suffer a delay in their visual recovery which, in some cases, results in a worse level of visual acuity than preoperatively. Intraocular pressure can become raised from trabecular meshwork obstruction. If maculopathy is present, then additional laser treatment cannot be applied and intravitreal treatment may not be possible to continue, with the risk of worsening foveal function in the long term. Repeated clinic visits may be required to monitor POVCH, which may be a significant burden both for patients and health systems.
The initial treatment for POVCH is observation (Tolentino 1989). Spontaneous clearance occurs in some cases if no further bleeding occurs. This is because the red blood cells are no longer trapped in the gel structure of the vitreous and can circulate and clear more freely from the vitreous cavity. Clearance is related to the amount of haemorrhage, its recurrence and the degree of communication between anterior and posterior segments, allowing red blood cells to enter the anterior chamber and be cleared via the trabecular meshwork (McLeod 2000).
Non‐clearing POVCH necessitates revision surgery in approximately one‐third to one‐half of those who experience POVCH and approximately 10% to 20% of all patients undergoing surgery (Brown 1992; Han 1991; Martin 1992; Jackson 2015; Steel 2008; Yorston 2008). Non‐clearing POVCH is treated with surgery to remove haemorrhage and to treat any underlying cause that may have been identified. The timing of the surgery will depend on a variety of factors, including social situation, fellow‐eye status, maculopathy needing treatment, intraocular pressure, etc. Simple in‐office fluid‐air exchange has been proposed as an alternative to traditional revision surgery (Berrocal 2016).
In some patients, spontaneous clearing or revision surgery is followed by recurrent haemorrhage, which frustrates visual rehabilitation, especially if this occurs in the better eye.
Recently, intravitreal injection of anti‐VEGF agents has been used to promote resolution of POVCH (Antoszyk 2020; Chatziralli 2020).
Retinal breaks and rhegmatogenous retinal detachment
Retinal breaks are routinely successfully treated with laser or cryotherapy retinopexy; however, if undetected, obscured or in areas of unrelieved traction they can result in postoperative rhegmatogenous retinal detachment. Silicone oil is used in some cases to reduce the risk of postoperative rhegmatogenous retinal detachment. Silicone oil can be associated with peri‐retinal fibrosis, emulsification and a range of resultant complications, and can also be associated with unexplained visual loss (Chen 2021).
Epiretinal membrane (ERM) and recurrent traction
Persistent or recurrent traction can be associated with macular oedema and tractional detachment. These can affect vision and have been reported to require revision surgery in 7% to 22% of cases (Blankenship 1985; Gupta 2012; Oshima 2009; Schiff 2007; Yorston 2008).
Description of existing interventions to reduce the incidence of postoperative complications and how the interventions may work
At the time of the initial vitrectomy surgery, several surgical strategies have been used to prevent complications and avoid the need for repeat surgery. These strategies include the following:
-
Established surgical interventions that are generally regarded as standard clinical practice:
Ensuring adequate haemostasis at the time of vitrectomy with laser or intraocular bipolar coagulation or transient raised intraocular pressure, to maximise retinal view for adequate dissection and reduce postoperative oozing of dissected blood vessels.
Removal of peripheral haemorrhagic vitreous to reduce leaching of sequestered red blood cells postoperatively into the vitreous cavity.
Identification and removal of all posterior vitreoretinal traction. Vitreoschisis is known to occur in people with PDR, and identification of this and dissection in the true vitreoretinal plane are important to avoid recurrent traction and postoperative bleeding from neovascular tissue (Schwartz 1996).
Applying supplementary posterior panretinal photocoagulation to reduce neovascular tissue.
-
Other strategies to prevent POVCH that have been reported but not routinely adopted:
-
Surgical:
Applying additional retinal photocoagulation up to the ora serrata to ablate retro‐oral ischaemic retina and reduce production of postoperative neovascular growth factors (Liggett 1987; Mason 1978; Yeh 2005).
Direct treatment to the sclerostomy sites themselves with either cryotherapy or laser (Yeh 2005). This is thought to reduce the occurrence of entry site neovascularisation by inhibiting cellular migration through the sclerostomy wounds and causing focal atrophy of the ciliary epithelia.
Removal of Wieger’s ligament and thorough anterior vitrectomy, especially around the inner sclerostomy wounds (McLeod 2000; McLeod 2003). This may be effective by increasing the egress of red blood cells and growth factors from the posterior segment to the anterior segment for rapid clearance of any POVCH, reducing any concentration of growth factors around the sclerostomy sites themselves, and removing the vitreous scaffold along which anterior new vessels could grow.
Agents with physical actions thought to possibly reduce the rate of POVCH inserted into the eye during surgery, such as air (Joondeph 1989), gas (Koutsandrea 2001; Yang 2007), or viscoelastic substances (Packer 1989).
-
Pharmacologic:
Preoperative vascular endothelial growth factor (VEGF) inhibitor bevacizumab and alternative anti‐VEGF agents have been used in order to reduce vascular proliferation, permeability and vascularity of neovascular tissue (Romano 2009a; Romano 2009b; Yang 2008).
Intraoperative triamcinolone has been injected in order to reduce inflammation and vascular proliferation (Faghihi 2008).
Oral tranexamic acid, which inhibits fibrinolysis and hence clot dissolution, administered to the patient postoperatively (Laatikainen 1987; Ramezani 2005).
-
Description of the intervention
The use of anti‐VEGF agents injected into the vitreous cavity either before or at the time of surgery has been proposed to reduce the occurrence of a range of complications at the time of and after surgery.
How the intervention might work
Anti‐VEGF agents can reduce the amount and vascularity of abnormal retinal neovascularisation associated with PDR, facilitating surgical dissection, reducing intra‐ and postoperative bleeding and potentially improving outcomes. They may also reduce the occurrence of neovascularisation after surgery, reducing complications including bleeding. These effects may also reduce the need for silicone oil to be used, and reduce the need for re‐intervention for POVCH, recurrent traction or retinal detachment.
Why it is important to do this review
Diabetes mellitus is an increasing health problem. It is estimated that 7% (4.7 million) of the UK population are currently diabetic and that this will exceed 5.5 million by 2030. In the UK in 2010‐2011, 10% (GBP £10 billion) of the total NHS budget was spent treating the acute costs of diabetes and its complications, and this is predicted to increase to £17 billion by 2035 (Diabetes UK 2020). Diabetic retinopathy is one of the leading causes of blindness in the working age group in the UK, accounting for 14.4% of blind and partially sighted registrations (Liew 2014).
Within 20 years of diagnosis nearly all people with type 1 and almost two‐thirds of people with type 2 diabetes have some degree of retinopathy (Scanlon 2008); after 15 years, 30% and 10% of type 1 and type 2 diabetics, respectively, develop PDR (Klein 1984a; Klein 1984b). These patients are at risk of severe visual loss resulting from the complications of PDR. A study of patients at a large eye unit in the USA suggested that approximately 10% of patients presenting with PDR require vitrectomy surgery within one year (Kaiser 2000). Estimates based upon data from England suggest that approximately 4000 vitrectomies for the complications of PDR are currently performed annually in the UK (Vaideanu 2014). If 10% require revision surgery, this equates to 400 to 800 patients per annum in the UK. Repeat interventions expose the patient to further operative risk and anxiety and add to the overall cost of care.
The use of anti‐VEGF treatment is becoming increasingly common for many ophthalmic conditions and has significant revenue consequences. As well as reducing the vascularity of fibrovascular membranes they can increase fibrosis, resulting in new areas of tractional retinal detachment (El‐Sabagh 2011). A previous Cochrane Review has shown the benefit of pre‐ and intraoperative anti‐VEGF use in reducing the occurrence of early POVCH after diabetic vitrectomy (Smith 2015). However, the effectiveness of different types of anti‐VEGF agents, their optimum timing of use and their effect on other outcomes is unclear. An up‐to‐date review of the literature will aid in optimum patient management and in the design of future studies.
Objectives
To assess the effects of perioperative anti‐VEGF use on the outcomes of vitrectomy for the treatment of complications of proliferative diabetic retinopathy.
Methods
Criteria for considering studies for this review
Types of studies
This review included randomised controlled trials (RCTs). We imposed no language, publication status or date restrictions.
Types of participants
Participants in the trials were people with PDR undergoing vitrectomy for the complications of diabetic retinopathy for the first time. To provide an overall estimate of the effect of anti‐VEGF agents in a broad population, we applied no restrictions based on participants' residence, race, ethnicity, occupation, education or socio‐economic status in general.
Types of interventions
Intervention
Any anti‐VEGF combined with vitrectomy (within two weeks before or at time of vitrectomy). We considered any of the available anti‐VEGF treatments when given pre‐ or intraoperatively, including but not limited to:
bevacizumab 1.25 mg/0.05 mL;
ranibizumab 0.5 mg/0.05 mL;
pegaptanib 0.3 mg/0.05 mL;
aflibercept 2.0 mg/0.05 mL;
conbercept 0.5 mg/0.05 mL.
Comparator
Vitrectomy with no anti‐VEGF treatment or with sham treatment, or with any other anti‐VEGF.
Types of outcome measures
As the main aim of this review was to look at outcomes and complications following vitrectomy, we excluded studies that did not report any postoperative outcomes.
Critical
Mean difference in best corrected visual acuity (BCVA) between study arms at six (± three) months following the primary vitrectomy. BCVA values were collected regardless of the method that was used for assessment (e.g. Snellen, Early Treatment Diabetic Retinopathy Study (ETDRS) letters logMAR). We pooled data only if reported measurements could be converted to logMAR. According to the US Food and Drug Administration, a 15‐letter change (equating to 0.3 logMAR) in BCVA would be clinically significant (Csaky 2008).
The incidence of early POVCH after surgery. We defined early POVCH as haemorrhage present from the first postoperative day or within the first four weeks postoperatively, being at least grade 2 in severity as measured by the Diabetic Retinopathy Vitrectomy Study criteria (Anonymous 1985).
The incidence of late POVCH after surgery. We defined late POVCH as haemorrhage occurring more than four weeks postoperatively after a period during which the vitreous cavity was clear. The minimum length of follow‐up for this outcome was six months.
The incidence of revision surgery for POVCH in the first six months postoperatively.
The incidence of revision surgery for recurrent traction/macular pucker of any type and/or rhegmatogenous retinal detachment in the first six months postoperatively. Preoperative administration of intravitreal bevacizumab has been stated to reduce the revision vitrectomy rate in patients primarily operated for vitreous haemorrhage (VH) (17.4% versus 7.7%). However, in patients primarily operated for tractional retinal detachment (TRD), preoperative administration of intravitreal bevacizumab reportedly led to an increase in re‐vitrectomy rate (54.5% versus 78.6%) (Hu 2019b).
Vision‐related quality of life (VRQOL) measures using any validated quality of life questionnaire performed at least six months following vitrectomy. Many tools have been developed in order to assess VRQOL (de Boer 2004). The 25‐item National Eye Institute Visual Function Questionnaire (NEI VFQ‐25) has been validated in patients with diabetic retinopathy (Mangione 2001). A clinically significant gain of at least 15 letters in BCVA corresponds to a clinically significant gain of at least seven points in the overall composite score of the (NEI VFQ‐25 (Suñer 2017). However, we did not expect all studies to have used the same tool in order to assess VRQOL.
Important
Proportion of people with a visual acuity of counting fingers (1.8 logMAR or worse).
Number of operative retinal breaks reported.
Frequency of silicone oil tamponade required at time of surgery.
Follow‐up
Follow‐up for the included studies' outcome measures varied from one month to 12 months post vitrectomy. We looked at studies with any follow‐up period, using six (± three) month follow‐up data as a minimum for late POVCH, revision surgery and visual acuity. Follow‐up periods for the remaining outcomes varied and are described in the Characteristics of included studies section.
Search methods for identification of studies
Electronic searches
The Cochrane Eyes and Vision Information Specialist searched the following databases for randomised controlled trials and controlled clinical trials. There were no restrictions to language or year of publication. The date of the search was 22 June 2022.
Cochrane Central Register of Controlled Trials (CENTRAL 2022, Issue 6) (which contains the Cochrane Eyes and Vision Trials Register) in the Cochrane Library (searched 22 June 2022) (Appendix 1).
MEDLINE Ovid (1946 to 22 June 2022) (Appendix 2).
Embase Ovid (1980 to 22 June 2022) (Appendix 3).
LILACS (Latin American and Caribbean Health Science Information database (1982 to 22 June 2022) (Appendix 4).
ISRCTN registry (www.isrctn.com/editAdvancedSearch; searched 22 June 2022) (Appendix 5).
US National Institutes of Health Ongoing Trials Register ClinicalTrials.gov (www.clinicaltrials.gov; searched 22 June 2022) (Appendix 6).
World Health Organization (WHO) International Clinical Trials Registry Platform (ICTRP) (www.who.int/ictrp; searched 22 June 2022) (Appendix 7).
We ran the initial searches both with and without RCT search filters, as we wished to identify as much literature as possible. For subsequent updates, however, we will only run searches with RCT filters, as the review is focusing on evidence from RCTs only.
After editorial input, we decided to revise and broaden the search strategies for the review. The searches were constructed of terms for the following four components: diabetic retinopathy, vitrectomy, haemorrhage and anti‐VEGF drugs. The searches have now been amended whereby the terms for vitrectomy and for haemorrhage have been combined into one set of search terms. This has made the search broader and will help us to identify additional relevant studies.
Searching other resources
We manually searched the reference lists of the studies included in the review for additional trials. We did not specifically handsearch journals or conference proceedings for this review.
Data collection and analysis
Selection of studies
Two of the review authors independently assessed abstracts to ascertain which studies met the inclusion criteria for the review. We labelled the abstracts as included, unclear or excluded. We obtained full‐text copies of all included and unclear studies, and the two authors independently determined which studies met the inclusion criteria. We again labelled each study as included, unclear or excluded. We discussed any unclear articles and contacted the authors of the relevant article for further details when necessary. We also collected information on study design and setting, participant characteristics (including disease severity and age), study eligibility criteria, details of the intervention(s) given, the outcomes assessed, the source of study funding and any conflicts of interest stated by the investigators.
Data extraction and management
Two of the review authors independently extracted data using the standard methodological procedures recommended by Cochrane. We compared each data set and resolved any discrepancies by discussion. We independently entered data into RevMan Web and then rechecked the data (RevMan Web 2023).
We collected and recorded the following variables from the included studies:
Primary author
Title
Country where the study was conducted
Healthcare setting
Potential conflicts of interest
Eligibility criteria
RCT design
Randomisation timing
Randomisation method
Number of participants randomised
Number of eyes studied
Number of eyes studied per arm
Number of eyes analysed per arm
Number of participants lost with reasons
Baseline data provided
Baseline data differences
Type of intervention in each study arm
Follow‐up examination schedule
Outcomes with definitions
Outcome comparisons by group
Possible confounders
Quality of evidence for each outcome using the GRADE classification (GRADEpro GDT)
Potential sources of bias
Assessment of risk of bias in included studies
Two review authors structured the criteria for assessment of risk of bias using Cochrane's risk of bias tool (RoB 1) and assessed the risk of bias in each included study as per Chapter 8 of the Cochrane Handbook for Systematic Reviews of Interventions (Higgins 2017). We assessed each domain area, giving a judgement of 'low' risk of bias, 'high' risk of bias or 'unclear' risk of bias. A judgement of 'unclear' indicated that we were uncertain of the risk of bias. We looked specifically at the following domain areas:
Methods used to generate the study groups.
Methods used to conceal the allocation of the study groups.
Methods used to mask (blind) study participants and personnel.
Review of the study outcome data, looking specifically at the completeness of each study group outcome and selective outcome reporting.
Moreover, we performed assessment of reporting bias by testing for funnel plot asymmetry if there were at least 10 studies included in an analysis, as per Chapter 10 of the Cochrane Handbook for Systematic Reviews of Interventions (Higgins 2017). Asymmetry in the funnel plot may indicate small study effects and potential publication bias.
Measures of treatment effect
We presented dichotomous outcomes as a risk ratio with 95% confidence interval (CI) and continuous outcomes as mean difference with 95% CI.
The review's critical outcomes included dichotomous data on the incidence of persistent or early POVCH, the incidence of late POVCH following the primary surgery, the incidence of revision vitrectomy for POVCH, and also separately for recurrent traction/macular pucker/rhegmatogenous retinal detachment (RRD) up to six months postoperatively. We intended to analyse data regarding VRQOL as a critical outcome, whereas we analysed the mean difference in visual acuity at six (± three) months following the primary vitrectomy as continuous data. We also intended to analyse data on the proportion of people with visual acuity of counting fingers (CF) or worse as dichotomous data. We presented dichotomous data regarding the use of silicone oil tamponade at the time of primary surgery and continuous data regarding the number of intraoperative retinal breaks.
Unit of analysis issues
In the 2023 update, the eye receiving pars plana vitrectomy (PPV) for the complications of diabetic retinopathy was the unit of analysis. We included a few studies that included a small number of participants who had both eyes randomised (Ahn 2011; di Lauro 2009; Hu 2019; Manabe 2015; Ou 2021; Sohn 2012; Zhou 2017). Due to the number being small, we considered that the effect of interpersonal variance on the outcome would be negligible. Since the intervention given relates to the results of the specific eye being operated, risk of a confounding cross‐over effect is minimal.
Dealing with missing data
In clinical trials it is expected that reports will contain missing data (Dziura 2013). In our review, we tried to investigate the reasons for missing data because this might introduce bias into the study. Where data were missing in the included studies, we contacted the authors of the studies to request the missing data. In studies for which the authors could not provide missing data, we assessed whether the missing data would introduce 'low' or 'high' risk of bias, as per the Cochrane Handbook for Systematic Reviews of Interventions (Higgins 2017). We performed an intention‐to‐treat (ITT) analysis, using imputed data completed by the trial investigator. However, we did not impute missing data ourselves. When ITT analysis was not possible, we performed a complete case analysis, based on the assumption that data are missing randomly. We assessed this assumption for each included study separately based on factors like exclusion criteria and the proportion of participants that were lost to follow‐up.
Assessment of heterogeneity
We assessed clinical heterogeneity by review of the study manuscripts and presented a descriptive summary of the results. We assessed heterogeneity between studies included in the meta‐analysis using the I2 statistic. We took an I2 result of more than 50% as an indication of high study heterogeneity.
Assessment of reporting biases
To avoid the presence of reporting biases within the review, we searched trial registry databases, which allowed us to identify all registered trials, published and unpublished. We contacted the investigators of registered trials that were listed as having completed participant recruitment to ask for any unpublished data that may be relevant to the review outcomes.
Data synthesis
We performed analysis of data from the included RCTs for the critical and important outcomes where feasible. We used a random‐effects model in every comparison including at least three studies, otherwise we used a fixed‐effect model.
If we came across multi‐arm studies, we only included those outlined in our pre‐specified eligibility criteria. Using eligible studies, we planned to combine intervention groups to make a comparison in patients treated with anti‐VEGFs (within two weeks before or at the time of vitrectomy) versus vitrectomy with no anti‐VEGF treatment or with sham treatment, as described in the Cochrane Handbook for Systematic Reviews of Interventions (Higgins 2021).
Subgroup analysis and investigation of heterogeneity
Regarding the effect of different agents when administered at different time points peri‐operatively, we planned to perform pre‐specified subgroup analyses where possible, according to the Cochrane Handbook for Systematic Reviews of Interventions (Higgins 2021).
It is possible that the interval of preoperative anti‐VEGF injection may influence postoperative outcomes. An interval of at least five days, preoperatively has been reported to be more effective in terms of better visual outcomes and fewer postoperative complications (Castillo 2017).
Moreover, the indication for vitrectomy may affect the effectiveness of perioperative anti‐VEGF therapy based on surgical complexity and we therefore planned to assess for heterogeneity of response according to two broad indications, namely vitreous haemorrhage (VH) and traction retinal detachment (TRD), if possible.
We limited the number of subgroup analyses to avoid multiplicity issues. More specifically, we planned prespecified subgroup analyses for the following:
Mean difference in BCVA in all cases for anti‐VEGF administration < 5 days versus ≥ 5 days before surgery.
Incidence of early POVCH in all cases for anti‐VEGF administration < 5 days and ≥ 5 days before surgery.
Mean difference in BCVA in cases with main indication traction retinal detachment versus vitreous haemorrhage.
Mean difference in BCVA for bevacizumab (the most commonly used agent) versus all other agents.
Sensitivity analysis
Sensitivity analysis helps to assess the robustness of an analysis after the inclusion of studies graded as high risk of bias. In the original analysis we did not exclude any study on the basis of high risk of bias. However, to assess the strength of our findings, we performed additional sensitivity analyses to examine the effect of performance, detection and attrition bias by excluding studies at high risk in any one of these domains. Moreover, we performed a random‐effects meta‐analysis both with and without outlying studies as part of a sensitivity analysis when outliers were identified, according to the Cochrane Handbook for Systematic Reviews of Interventions (Higgins 2021).
Summary of findings and assessment of the certainty of the evidence
We prepared a summary of findings table presenting relative and absolute risks. We graded the overall quality (certainty) of the evidence for each outcome using the GRADE classification (GRADEpro GDT). We included the following outcomes in the summary of findings table.
Mean difference in visual acuity, logMAR (six ± three months)
Early POVCH (occurring within four weeks postoperatively)
Late POVCH (occurring more than four weeks postoperatively after a period during which the vitreous cavity was clear)
Incidence of revision vitrectomy for POVCH
Incidence of revision vitrectomy for recurrent traction/macular pucker (six months)
Number of intraoperative retinal breaks
Frequency of silicone oil tamponade required at time of surgery
Quality of life
Proportion of people with a visual acuity of counting fingers (1.8 logMAR or worse)
These outcomes were not defined a priori because the original protocol and first edition of this review were published before the summary of findings methodology was adopted by Cochrane Eyes and Vision.
Results
Description of studies
Results of the search
The electronic searches in the original review yielded a total of 472 titles and abstracts and six reports of ongoing studies (Smith 2011). After de‐duplication, the Information Specialist scanned 397 records and discarded 311 records that were not relevant to the scope of the review. We screened the titles and abstracts of the remaining 86 references. We rejected 70 abstracts as not eligible for inclusion in the review. We obtained and screened full‐text copies of 16 references, of which we included four studies and excluded 12 studies from the review.
The amended searches run in May 2015 retrieved a total of 1414 records (Figure 1). After removing duplicate records, we screened 1138 references and excluded 1110 records that were not relevant to the scope of the review. We assessed 28 full‐text reports of studies for potential inclusion in the review. In addition to the four previously included studies (Ahmadieh 2009; di Lauro 2009; Modarres 2009; Rizzo 2008), we have now included eight new studies (Ahn 2011; El Batarny 2008; Farahvash 2011; Hernández‐Da Mota 2010; Manabe 2015; Sohn 2012; Zaman 2013). We excluded 12 studies (Berk Ergun 2014; Bhavsar 2014; Demir 2013; Goncu 2014; Gupta 2008; Gupta 2012a; Gupta 2012b; Jirawison 2012; Li 2010; Pakzad‐Vaezi 2014; Sato 2013). We previously excluded da R Lucena 2009 and Yeh 2009 at the initial stage of screening abstracts. However, these two studies have been included in a meta‐analysis by Zhao 2011, so in the interests of transparency we have now added these studies to our list of excluded studies with reasons for exclusion.
1.
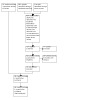
The updated electronic searches run in June 2022 yielded a total of 662 records (Figure 1). After removal of 208 duplicates, the Cochrane Information Specialist screened the remaining 454 records and removed 317 records that were not relevant to the scope of the review. We screened the remaining 137 records and after scanning for double and irrelevant records, we excluded outright 72 records. We obtained the full‐text reports of 65 records for further assessment and have included the following 16 new studies (Aleman 2019; Arevalo 2019; Comyn 2017; Cui 2018; Dong 2019; Ferraz 2013; Hu 2019; Jiang 2020; Li 2022; Ou 2021; Ren 2019; Su 2016; Wildan 2019; Yang 2016; Yu 2015; Zhou 2017). We excluded 49 new studies: see Characteristics of excluded studies for details.
In the previous version of this review there were 12 included studies (Smith 2015). In this 2023 update, Elwan 2013, which was previously an included study, has now been excluded as the study has been retracted. Pakzad Vaezi 2014, which was excluded in the previous version of the review, has now been included in the review because this study reports outcomes of interest.
Ongoing studies
On 11 September 2022, we checked the status of the eight ongoing trials previously listed in this review. Two trial reports have been moved to included and excluded studies within this review. Six reports remain as ongoing trials and we will assess them for potential inclusion when data become available (ISRCTN79120387; NCT00516464; NCT00931125; NCT01091896; NCT01151722; NCT01306981).
Included studies
We identified 28 completed studies from the electronic database searches that met our inclusion criteria; see the Characteristics of included studies table for details. All the data presented in the review were obtained from published literature.
Setting and participants
The included studies were conducted in a number of countries. Eleven were from China, three were from Iran, two were from Italy, two were from Mexico, and the remaining studies were from South Korea, the UK, Egypt, Brazil, Japan, Canada, the USA, Indonesia and Pakistan. One study was multi‐centre, including 13 clinical sites from nine countries. The included studies randomised a total of 1914 eyes. Sample size varied from 20 (Sohn 2012) to 214 (Arevalo 2019).
Intervention
The most frequently used anti‐VEGF regime was intravitreal bevacizumab (IVB) (1.25 mg/0.05 mL) within one week prior to pars plana vitrectomy. The studies with a different protocol were the following:
Ahn 2011 had an intervention group in which 1.25 mg IVB was given at the end of surgery (37 participants).
Aleman 2019 had an intervention group that received 1.25 mg Ziv‐aflibercept (IVZ) 1 to 10 days before vitrectomy (99 participants).
Comyn 2017 had an intervention group that received 0.5 mg ranibizumab (IVR) within one week of pars plana vitrectomy (15 participants).
Cui 2018 had an intervention group that received 0.5 mg conbercept (IVC) within one week of surgery (20 participants) and one group that received 0.5 mg IVR within one week of surgery (20 participants).
di Lauro 2009 had an intervention group that received 1.25 mg IVB three weeks before vitrectomy.
Hernández‐Da Mota 2010 gave 1.25 mg IVB 48 hours before surgery.
Hu 2019 had an intervention group that received 0.5 mg IVR one week before surgery (51 participants).
Jiang 2020 had an intervention group that received 0.5 mg IVC at the end of surgery (15 participants).
Li 2022 had an intervention group that received 0.5 mg IVR one day before surgery (16 participants) and another group that received 0.5 mg IVR three days before surgery (16 participants).
Manabe 2015 gave 0.16 mg (0.05 mL) IVB one day before surgery.
Modarres 2009 gave 2.5 mg IVB three to five days before surgery.
Ou 2021 had an intervention group that received 0.5 mg IVC five days before surgery (32 participants).
Pakzad Vaezi 2014 had an intervention group that received 0.5 mg IVR one week before surgery (15 participants).
Ren 2019 had an intervention group that received 0.5 mg IVC immediately after surgery (25 participants).
Su 2016 had an intervention group that received 0.5 mg IVC one week before surgery (18 participants).
Wildan 2019 had an intervention group that received 0.5 mg aflibercept (IVA) four to seven days before surgery (12 participants).
Yang 2016 had an intervention group that received 0.5 mg IVC three days before surgery (54 participants).
Yu 2015 had an intervention group that received 0.5 mg IVC two to six days before surgery (61 participants).
Zhou 2017 had an intervention group that received 0.5 mg IVC three to seven days before surgery (18 participants).
Outcomes
The main outcomes in the studies included best‐corrected visual acuity (BCVA), feasibility of surgery (operating time, intraoperative bleed and type of surgical steps required) and postoperative complications. The main postoperative complications were rate of POVCH, iris rubeosis and retinal detachment. Follow‐up varied significantly across the studies, ranging from one month (Ahmadieh 2009; Manabe 2015) to one year (Arevalo 2019; Jiang 2020). Li 2022 did not report clearly the exact follow‐up period. Most of the studies had a final follow‐up visit at six months.
A number of studies reporting the incidence of POVCH included participants who received silicone oil endotamponade, which has made interpretation of the study results difficult. The presence of silicone oil within the vitreous cavity precludes an accurate diagnosis of POVCH, as any blood would be localised to the far periphery of the posterior chamber. Grading of POVCH is not possible with silicone endotamponade present. In light of this, we have carried out sensitivity analyses on the incidence of POVCH excluding participants with silicone oil endotamponade. Two studies excluded participants who received silicone oil and gave an accurate grading system for POVCH (Ahmadieh 2009; Ahn 2011).
In addition, we identified nine ongoing RCTs and have provided details in the Characteristics of ongoing studies table. We cannot comment on whether these studies' characteristics meet the inclusion criteria until they are published and we can undertake a review of their methodology.
Excluded studies
We excluded 76 studies identified by the search that were either non‐randomised prospective studies or retrospective studies; see the Characteristics of excluded studies table. We excluded one study that did not collect data on POVCH (da R Lucena 2009).
Risk of bias in included studies
See also Figure 2.
2.

Risk of bias summary: review authors' judgements about each risk of bias item for each included study.
Allocation
Eleven studies clearly stated how the random sequence generation was performed and we graded the methods as 'low' risk for randomisation and allocation (Ahmadieh 2009; Ahn 2011; Aleman 2019; Arevalo 2019; Comyn 2017; Hu 2019; Jiang 2020; Ou 2021; Pakzad Vaezi 2014; Ren 2019; Rizzo 2008).
Ten studies stated that participants were randomly assigned into the groups, but provided no description on how the randomisation or sequence allocation was performed (Cui 2018; di Lauro 2009; Dong 2019; Ferraz 2013; Su 2016; Wildan 2019; Yang 2016; Yu 2015; Zaman 2013; Zhou 2017). Six studies did not provide any details about the randomisation methods (El Batarny 2008; Farahvash 2011; Hernández‐Da Mota 2010; Li 2022; Modarres 2009; Sohn 2012). We graded the methods used for randomisation in these studies as 'unclear'.
We assessed five studies at 'low' risk of selection bias, as a clear description of how this process was performed was provided (Ahmadieh 2009; Ahn 2011; Arevalo 2019; Comyn 2017; Manabe 2015).
We graded the remaining studies as unclear, because they did not comment on the allocation procedure.
Blinding
We assessed seven studies as at 'low' risk of bias for masking (blinding), as a clear description of how this process was performed was provided (Ahmadieh 2009; Arevalo 2019; Comyn 2017; di Lauro 2009; Manabe 2015, Pakzad Vaezi 2014; Sohn 2012). We graded Aleman 2019 as low risk for performance bias since both participants and personnel were masked, but as high risk for detection bias since unmasked personnel provided postoperative examinations. We graded Cui 2018 as high risk for performance bias since participants were not masked and as low risk for detection bias since surgeries were performed by masked surgeons. We graded seven studies that had an open‐label design as 'high' risk (Ahn 2011; El Batarny 2008; Farahvash 2011; Hernández‐Da Mota 2010; Hu 2019; Su 2016; Zaman 2013). We graded Jiang 2020 and Li 2022 as high risk for performance bias since participants were not masked and low risk for detection bias since all the assessors were masked to the group. We graded nine studies that did not comment on the masking of participants or investigators as 'unclear' (Dong 2019; Ferraz 2013; Modarres 2009; Ou 2021; Rizzo 2008; Wildan 2019; Yang 2016; Yu 2015; Zhou 2017). Ren 2019 reported that all the surgeries were performed by the same masked surgeon, however it is not clarified who performed the postoperative examinations. As a result we graded this study as having an unclear risk of bias.
Incomplete outcome data
Ahmadieh 2009, Ahn 2011, Farahvash 2011 and Sohn 2012 clearly accounted for each participant who failed to complete the study protocol. Moreover, attrition rates and loss to follow‐up rates were similar between arms in these studies. It should be noted that in Ahmadieh 2009, less than half of the participants (16 of 35) within the treatment group failed to complete the protocol, and 18 of 35 participants within the control group completed the protocol. Manabe 2015 reported participant flow and all participants were followed up to one month. Li 2022 did not clearly report the exact follow‐up period, thus rendering the study at high risk of bias. Although the remaining included studies did not comment directly on the attrition rate, it is clear from the results that all participants completed follow‐up.
Selective reporting
Ferraz 2013 did not report the incidence of late POVCH. Li 2022 did not provide a list of prespecified outcome measures. For this reason we graded these studies as high risk. Ahmadieh 2009, Ahn 2011, Aleman 2019, Arevalo 2019, Comyn 2017, di Lauro 2009, Jiang 2020, Manabe 2015, Pakzad Vaezi 2014, Ren 2019 and Sohn 2012 reported all the outcomes stated in the original trial register and we graded them as low risk. The remaining studies did not provide information about a study protocol or trial register in order to confirm whether all prespecified outcome measures were reported (Cui 2018; Dong 2019; El Batarny 2008; Farahvash 2011; Hernández‐Da Mota 2010; Hu 2019; Modarres 2009; Ou 2021; Rizzo 2008; Su 2016; Wildan 2019; Yang 2016; Yu 2015; Zaman 2013; Zhou 2017). As a result, we have graded these studies as at unclear risk of bias.
Other potential sources of bias
Ahmadieh 2009 recorded a high number of participants who failed to complete the trial in both the control and treatment groups: 15 of 35 in the control group and 19 of 35 in the treatment group. The main reasons for failing to complete follow‐up were vitreous haemorrhage reabsorption, silicone oil endotamponade, gas tamponade and loss to follow‐up.
Ahn 2011 included 107 eyes of 91 participants. The 16 bilateral participants were included in the data analysis; no comment was made as to whether adjustment for within‐person correlation was performed during statistical analysis.
In Comyn 2017 and Pakzad Vaezi 2014, the authors declared receiving funding from the manufacturer of the anti‐VEGF studied.
In the intravitreal bevacizumab (IVB) group of Manabe 2015, participants with bilateral proliferative diabetic retinopathy (PDR) received IVB in one eye only, and the other eye was excluded from the study. The authors considered that IVB injected in one eye may have an effect on the contralateral eye. In the control group, both eyes of bilateral cases were included in the study.
Effects of interventions
See: Table 1
We have described the effect of each intervention in order of outcome type.
Critical outcomes
1. Visual acuity at six (± three) months following the primary vitrectomy
Analysis 1.1 includes all studies that compared any anti‐vascular endothelial growth factor (VEGF) given preoperatively to control. Thirteen studies including 699 participants (392 in the anti‐VEGF arm and 307 in the control arm) were included in the analysis. The use of anti‐VEGF preoperatively was shown to improve visual acuity (mean difference (MD) ‐0.25 logMAR, 95% confidence interval (CI) ‐0.39 to ‐0.11). The studies Ahn 2011 and Hernández‐Da Mota 2010 appear to be outliers. After excluding these two outlying studies, anti‐VEGF administration was associated with a significant improvement in postoperative best corrected visual acuity (BCVA) (MD ‐0.23 logMAR, 95% CI ‐0.32 to ‐0.14). These results were robust to all further sensitivity analyses. There were a few studies that reported visual outcomes, however they did not contribute data that could be included in the analysis. Ahmadieh 2009 and Yang 2016 reported a significant improvement in BCVA in the anti‐VEGF arm versus the control, however they only measured visual acuity at one month postoperatively. Similarly, Arevalo 2019 reported better outcomes at 12 months with preoperative anti‐VEGF compared to pars plana vitrectomy (PPV) alone. Ferraz 2013 only graphically presented the visual outcomes, however they did not establish a statistically significant benefit of anti‐VEGF. Manabe 2015 and Su 2016 only reported the change in BCVA during the first month postoperatively, without a statistically significant difference between the groups. Rizzo 2008 did not report standard deviations. However, the improvement in BCVA was slightly significant in the anti‐VEGF group, while in the control group it was not. Su 2016 reported better visual outcomes for the anti‐VEGF group at six weeks compared to the control group. When investigating possible publication bias, the funnel plot seemed to be symmetrical (Figure 3).
1.1. Analysis.

Comparison 1: Anti‐VEGF versus control, Outcome 1: Mean BCVA
3.

We carried out subgroup analyses to compare the effect on visual acuity of any anti‐VEGF given less than five days preoperatively to at least five days postoperatively (Analysis 2.1). Analysis 2.1.1, consisting of seven studies with 396 participants (209 in the anti‐VEGF arm and 187 in the control arm), showed that administration of anti‐VEGF less than five days preoperatively leads to an improvement in visual acuity (MD ‐0.30 logMAR, 95% CI ‐0.53 to ‐0.07). Analysis 2.1.2 consists of four studies with 207 participants (116 in the anti‐VEGF group and 91 in the control group) and shows that administration of anti‐VEGF more than five days preoperatively (range 5 to 21 days) also leads to an improvement in visual acuity (MD ‐0.13 logMAR, 95% CI ‐0.20 to ‐0.06). These results were robust to all further sensitivity analyses. The test for subgroup differences showed no statistically significant results (P = 0.20).
2.1. Analysis.

Comparison 2: Anti‐VEGF versus control: subgroup analysis ‐ time of administration of anti‐VEGF, Outcome 1: Mean BCVA
Only one study included participants that were listed for surgery solely due to tractional retinal detachment. Hernández‐Da Mota 2010 compared 20 participants that received bevacizumab 48 hours prior to vitrectomy to controls. The authors concluded that preoperative bevacizumab leads to an increase in visual acuity (MD ‐1.31 logMAR, 95% CI ‐1.76 to 0.86), however this was not statistically significant. Analysis 3.1 includes studies with participants listed for surgery solely due to vitreous haemorrhage. Three studies with 137 participants (77 in the anti‐VEGF group and 60 in the control group) were included. The analysis shows that preoperative anti‐VEGF leads to a lower but statistically significant increase in visual acuity compared to tractional retinal detachment cases (MD ‐0.25 logMAR, 95% CI ‐0.37 to ‐0.13). The test for subgroup differences showed statistically significant results (P < 0.01). These results were robust to all further sensitivity analyses.
3.1. Analysis.

Comparison 3: Anti‐VEGF versus control: subgroup analysis ‐ main indication for vitrectomy, Outcome 1: Mean BCVA
We carried out subgroup analyses to compare bevacizumab, the most commonly used agent, to control and all other anti‐VEGFs to control, respectively (Analysis 4.1). Analysis 4.1.1 includes six studies with 307 participants and shows that preoperative bevacizumab leads to an increase in visual acuity that was not statistically significant (MD ‐0.35 logMAR, 95% CI ‐0.79 to 0.08). However, two out of six studies presented considerable heterogeneity, with a mean difference in BCVA ranging from 1.31 logMAR better vision in the anti‐VEGF group (Hernández‐Da Mota 2010) to 0.14 logMAR better vision in the control group (Ahn 2011). As a result, a pooled estimate of effect for this comparison may not be informative. On the other hand, Analysis 4.1.2 includes six studies with 272 participants and it shows that all other anti‐VEGF agents combined, when given preoperatively, lead to a statistically significant increase in visual acuity (MD ‐0.19 logMAR, 95% CI ‐0.28 to ‐0.10). These results were robust to all further sensitivity analyses. No statistically significant difference was shown when testing for subgroup differences (P = 0.48).
4.1. Analysis.

Comparison 4: Anti‐VEGF versus control: subgroup analysis ‐ bevacizumab versus other anti‐VEGF, Outcome 1: Mean BCVA
2. The incidence of early postoperative vitreous cavity haemorrhage (POVCH) after surgery
Fourteen studies with 544 participants receiving preoperative anti‐VEGF and 494 control group participants were included in Analysis 1.2. This shows that preoperative administration of anti‐VEGF significantly reduces the risk of early (less than four weeks postoperatively) POVCH (risk ratio (RR) 0.44, 95% CI 0.34 to 0.58). These results were robust to all further sensitivity analyses. A funnel plot showed asymmetry, thus implying possible publication bias and heterogeneity due to differences in the size of each study (Figure 4).
1.2. Analysis.

Comparison 1: Anti‐VEGF versus control, Outcome 2: Early POVCH
4.

We additionally carried out subgroup analyses that divided the studies according to when the anti‐VEGF agent was administered (Analysis 2.2). Analysis 2.2.1 includes studies that administered any anti‐VEGF less than five days preoperatively. It includes eight studies with 618 participants and shows that anti‐VEGF administration leads to a statistically significant decrease in the risk of early POVCH (RR 0.44, 95% 0.29 to 0.66). Similarly, Analysis 2.2.2 includes five studies that examined the use of any anti‐VEGF at least five days prior to surgery (range 5 to 21 days). This shows that anti‐VEGF leads to a comparable decrease in the risk of early POVCH (RR 0.26, 95% 0.14 to 0.51). These results were robust to all further sensitivity analyses.
2.2. Analysis.

Comparison 2: Anti‐VEGF versus control: subgroup analysis ‐ time of administration of anti‐VEGF, Outcome 2: Early POVCH
3. The incidence of late POVCH after surgery
Eleven studies with 579 participants were included in Analysis 1.3. This shows that administration of anti‐VEGF leads to a reduction in the risk of late (at least four weeks postoperatively) POVCH (RR 0.47, 95% CI 0.30 to 0.74). These results were robust to all further sensitivity analyses and a funnel plot did not reveal any asymmetry (Figure 5).
1.3. Analysis.

Comparison 1: Anti‐VEGF versus control, Outcome 3: Late POVCH
5.

4. The incidence of revision surgery for POVCH at six months
Four studies with 207 participants (115 treated preoperatively with anti‐VEGF and 92 in the control group) were included in Analysis 1.4. Anti‐VEGF administration was associated with a non‐statistically significant decrease in the incidence of revision surgery after six months (RR 0.44, 95% CI 0.15 to 1.28). When we performed a sensitivity analysis by excluding studies with a high risk of performance bias from the analysis, anti‐VEGF administration was associated with a statistically significant reduction in the incidence of revision surgery after six months (RR 0.18, 95% CI 0.04 to 0.85).
1.4. Analysis.

Comparison 1: Anti‐VEGF versus control, Outcome 4: Revision surgery for POVCH
5. The incidence of revision surgery for recurrent traction/macular pucker of any type and/or rhegmatogenous retinal detachment at six months
Four studies with 145 participants (75 treated with anti‐VEGF and 70 in the control group) were included in Analysis 1.5. Anti‐VEGF administration reduced the rates of revision surgery for these indications, however the confidence intervals were wide and compatible with no effect (RR 0.50, 95% CI 0.15 to 1.66).
1.5. Analysis.

Comparison 1: Anti‐VEGF versus control, Outcome 5: Revision surgery for recurrent traction and/or RRD
6. Quality of life measures performed at least six months following vitrectomy
There are currently no studies that report on this outcome.
Important outcomes
1. Proportion of people with visual acuity of counting fingers (1.8 logMAR or worse)
No studies reported visual outcomes in a way that could be used for extracting the proportion of people with this visual acuity.
2. Number of intraoperative retinal breaks
We synthesised 12 studies with 915 participants (468 receiving anti‐VEGF and 447 receiving control) for this outcome. Analysis 1.6 shows that anti‐VEGF administration leads to a statistically significant reduction in the risk of intraoperative retinal breaks (RR 0.37, 95% CI 0.24 to 0.59). These results were robust to all further sensitivity analyses. A funnel plot was symmetrical (Figure 6).
1.6. Analysis.

Comparison 1: Anti‐VEGF versus control, Outcome 6: Intraoperative retinal breaks
6.

3. Frequency of silicone oil tamponade required at the time of surgery
Ten studies with 591 participants were included in the analysis, which shows that preoperative use of anti‐VEGF leads to a decrease in the need for silicone oil tamponade (RR 0.46, 95% CI 0.27 to 0.80) (Analysis 1.7). Of note, when performing sensitivity analysis by excluding studies with high risk of performance bias, this decrease is not statistically significant (RR 0.58, 95% CI 0.28 to 1.19). When examining for possible publication bias and differences in the size of effect, a funnel plot showed asymmetry (Figure 7).
1.7. Analysis.

Comparison 1: Anti‐VEGF versus control, Outcome 7: Silicone oil use
7.

Discussion
Summary of main results
The aim of this review was to establish whether the use of anti‐vascular endothelial growth factors (VEGFs) as an adjunct to pars plana vitrectomy, either pre‐ or intraoperatively, is of benefit. Currently the review includes 28 randomised controlled trials (RCTs), which look at the use of bevacizumab, ranibizumab, aflibercept, Ziv‐aflibercept and conbercept. The critical outcomes were the effect of anti‐VEGF on best corrected visual acuity (BCVA), early and late postoperative vitreous cavity haemorrhage (POVCH), revision surgery for POVCH, revision surgery for recurrent traction/macular pucker of any type and/or rhegmatogenous retinal detachment and vision‐related quality of life (VRQOL). We summarised the effect of anti‐VEGFs by outcome type.
Participants receiving intravitreal anti‐VEGF in addition to pars plana vitrectomy achieved better BCVA at six months compared to people undergoing vitrectomy alone (mean difference (MD) ‐0.25 logMAR, 95% confidence interval (CI) ‐0.39 to ‐0.11; 13 studies, 699 eyes; low‐certainty evidence). Subgroup analyses showed that perioperative anti‐VEGF might be more beneficial in terms of visual outcomes when administered less than five days preoperatively (MD ‐0.30 logMAR, 95% CI ‐0.53 to ‐0.07; 7 studies, 396 eyes) compared to ≥ 5 days preoperatively (MD ‐0.13 logMAR, 95% CI ‐0.20 to ‐0.06; 4 studies, 207 eyes), although the test for subgroup effect was not statistically significant. Clinically significant regression of neovascularisation has been reported to happen during the first week following treatment with anti‐VEGF in proliferative diabetic retinopathy (PDR) patients. Moreover, the half‐life of bevacizumab in a non‐vitrectomised eye has been reported to be 6.7 days. The occurrence of increased traction following anti‐VEGF injections prior to vitrectomy has also been widely reported and related to the time period between injection and surgery, with longer periods increasing the risk of visually significant macular traction (Russo 2019). As a result, administration of anti‐VEGF closer to the surgery date might still facilitate the surgery, minimise the risk of macular traction and provide better visual outcomes (Jorge 2006; Zhang 2013; Zhu 2008).
Pre‐ or intraoperative anti‐VEGF reduced the incidence of early POVCH (12% versus 31%, risk ratio (RR) 0.44, 95% CI 0.34 to 0.58; 14 studies, 1038 eyes; moderate‐certainty evidence). Both administration < 5 days preoperatively (15% versus 35%, RR 0.44, 95% CI 0.29 to 0.66; 8 studies, 618 eyes) and ≥ 5 days preoperatively (6% versus 30%, RR 0.26, 95% CI 0.14 to 0.51; 5 studies, 259 eyes) reduced the incidence of early POVCH.
Perioperative anti‐VEGF use was also associated with a reduction in the incidence of late POVCH (10% versus 23%, RR 0.47, 95% CI 0.30 to 0.74; 11 studies, 579 eyes; high‐certainty evidence).
The need for revision surgery for POVCH occurred less frequently in the anti‐VEGF group compared with the control group but the confidence intervals were wide and compatible with no effect (4% versus 13%, RR 0.44, 95% CI 0.15 to 1.28; 4 studies 207 eyes; moderate‐certainty evidence). Similar imprecisely measured effects were seen for revision surgery for rhegmatogenous retinal detachment (5% versus 11%, RR 0.50, 95% CI 0.15 to 1.66; 4 studies, 145 eyes; low‐certainty evidence). Anti‐VEGF facilitated the surgery by reducing the incidence of intraoperative retinal breaks (12% versus 31%, RR 0.37, 95% CI 0.24 to 0.59; 12 studies, 915 eyes; high‐certainty evidence). The evidence is very uncertain about the effect of perioperative anti‐VEGF on the need for silicone oil (19% versus 41%, RR 0.46, 95% CI 0.27 to 0.80; 10 studies, 591 eyes; very low‐certainty evidence).
No data were available on quality of life outcomes or the proportion of participants with visual acuity of counting fingers (CF) (1.8 logMAR or worse).
Overall completeness and applicability of evidence
This review includes 28 studies conducted in Europe, North America, Africa and Asia. The results of these studies are likely to be applicable to standard clinical practice. The studies consistently showed that intravitreal anti‐VEGF applied around the time of vitrectomy to reduce the occurrence of complications of proliferative diabetic retinopathy decreases the risk of both early and late POVCH. Anti‐VEGF use was also associated with statistically significant better postoperative BCVA. However, the evidence was less complete and could not be analysed with respect to other outcomes: the effect of anti‐VEGF on VRQOL and the proportion of patients with a low postoperative BCVA (less than counting fingers).
The included studies used a variety of regimens, including bevacizumab, ranibizumab, aflibercept, Ziv‐aflibercept and conbercept. Most studies used a similar dose of bevacizumab (1.25 mg), but a variety of regimens were used in terms of the time of administration. No data were available on other anti‐VEGF agents.
Quality of the evidence
The design of RCTs to look at the effect of adjunctive use of anti‐VEGF in diabetic vitrectomy is difficult. There are a number of indications for vitrectomy in proliferative retinopathy. These vary from non‐clearing vitreous haemorrhage in older patients with previously treated inactive proliferative diabetic retinopathy, through to younger patients with active untreated proliferative diabetic retinopathy and severe tractional changes. Many of the included RCTs had a heterogenous group of participants, as above, and the effect of anti‐VEGF on POVCH and BCVA may differ depending on the patient type.
Ten of the included studies appear to be at high risk of performance bias due to the personnel and participants not being masked. This is a significant proportion and may limit confidence in the estimate of the treatment effect of anti‐VEGF.
Potential biases in the review process
We followed our pre‐specified review protocol and documented the rationale for any changes from protocol.
Agreements and disagreements with other studies or reviews
Zhao 2011 is a systematic review looking at the potential benefits of preoperative intravitreal bevacizumab on both intraoperative outcomes (including intraoperative bleeding, endodiathermy, iatrogenic retinal tears and mean surgical time) and postoperative outcomes (including BCVA, recurrent vitreous haemorrhage, reabsorption time of blood and other complications).
Data analysis of included studies within the Zhao 2011 review, which looked at the incidence of early POVCH, showed an almost statistically significant result in favour of the treatment group (odds ratio (OR) 5.48, 95% CI 0.97 to 31.02; P = 0.05). This result is in agreement with the data analysis in this review. However, it should be noted that many of the included studies within the Zhao 2011 data analysis contained participants who received silicone oil endotamponade, which may be a significant source of bias. Also, the authors of Zhao 2011 commented that due to varying definitions of POVCH, study heterogeneity within the data analysis was high (I2 = 93.6%), so the results should be interpreted with caution.
Zhang 2013 reported similar outcomes in a meta‐analysis of the reported data on preoperative intravitreal bevacizumab use in vitrectomy for proliferative diabetic retinopathy. The study reported a beneficial effect of intravitreal bevacizumab on the rate of early POVCH (OR 0.35, 95% CI 0.21 to 0.58) and no effect on the rate of late POVCH (OR 0.55, 95% Cl 0.25 to 1.21).
Veliz 2014 summarised the results of a previously published version of this review. Zhang 2013, Zhao 2011 and Veliz 2014 concluded that bevacizumab probably decreases intraoperative bleeding, but its effect on visual acuity is uncertain. They concluded that it might increase the risk of cardiovascular events, but this was based on a RR of 2.2 with a 95% CI from 0.11 to 44.3, so there is considerable uncertainty in this estimate as well.
In a RCT, Castillo 2017 reported better outcomes when administering bevacizumab 5 to 10 days before vitrectomy as compared with a shorter interval. In our review, although both comparisons showed a statistically significant reduction in the incidence of early POVCH, this was greater when anti‐VEGF was administered < 5 days preoperatively rather than ≥ 5 days preoperatively.
In a recent meta‐analysis, Dervenis 2021 reported similar outcomes in terms of the effect of intravitreal bevacizumab on iatrogenic retinal breaks, POVCH and visual outcomes.
Authors' conclusions
Implications for practice.
This review provides support for the use of perioperative anti‐vascular endothelial growth factor (VEGF) to improve visual outcomes, reduce the risk of POVCH after vitrectomy for proliferative diabetic retinopathy and facilitate surgery. The current analysis suggests that pre‐ or intraoperative anti‐VEGF use may improve best corrected visual acuity (BCVA), likely reduces the risk of early postoperative vitreous cavity haemorrhage (POVCH) and it reduces the risk of late POVCH, and minimises the incidence of intraoperative retinal breaks. The evidence is very uncertain about the effect of anti‐VEGF on the need for silicone oil tamponade.
Implications for research.
Further randomised studies looking at the effect of anti‐VEGF agents on vision‐related quality of life (VRQOL) are needed. Furthermore, the spontaneous clearance of vitreous haemorrhage or clearance following the injection of an anti‐VEGF should be reported clearly in future studies. A minimum follow‐up period of at least six months is important to ensure that the long‐term effect of anti‐VEGF use is documented. Visual acuity should be analysed at defined time points and measured before and after further surgery to remove POVCH. We recommend grading of POVCH using the criteria within the Diabetic Retinopathy Vitrectomy Study, making the outcome of randomised controlled trials (RCTs) more comparable and easier to subject to further analysis. There is a need for agreement on variable and outcome reporting standardisation in trials with patients undergoing vitrectomy for proliferative diabetic retinopathy (PDR). Finally, more studies looking at surgical time and choice of final tamponade are needed. With a trend towards shorter tamponade agents, we need more studies looking at the effect that these agents may have on the outcomes of diabetic vitrectomy (Dervenis 2022; Govers 2022; Rush 2022).
What's new
| Date | Event | Description |
|---|---|---|
| 31 May 2023 | New citation required but conclusions have not changed | The title has been changed from 'Anti‐vascular endothelial growth factor for prevention of postoperative vitreous cavity haemorrhage after vitrectomy for proliferative diabetic retinopathy'. The PICO was also amended. |
| 31 May 2023 | New search has been performed | New trials have been included that met the inclusion criteria. |
History
Protocol first published: Issue 1, 2010 Review first published: Issue 5, 2011
| Date | Event | Description |
|---|---|---|
| 22 October 2014 | New citation required and conclusions have changed | Issue 8, 2015: Eight new RCTs were identified that met the inclusion criteria (Ahn 2011; El Batarny 2008; Elwan 2013; Farahvash 2011; Hernández‐Da Mota 2010; Manabe 2015; Sohn 2012; Zaman 2013). |
| 22 September 2014 | New search has been performed | Issue 8, 2015: Electronic searches were updated. |
Acknowledgements
The electronic searches were developed and executed by the Cochrane Eyes and Vision (CEV) editorial team.
We thank the following peer reviewers for the 2023 update:
Jayanth Sridhar MD, Bascom Palmer Eye Institute;
James Bainbridge, NIHR Moorfields Biomedical Research Centre; and
Leslie Choi, Evidence Synthesis Development Editor (Cochrane Central Executive Team).
We thank the following staff at CEV:
Jennifer Evans, for her assistance on the review;
Anupa Shah, for her help throughout the review process; and
Iris Gordon for her help on the literature search.
We thank Hsin‐Wen Wu for translating the included studies published in the International Eye Science journal.
CEV Co‐ordinating Editors Jennifer Evans and Gianni Virgili signed off the review for publication.
Appendices
Appendix 1. CENTRAL search strategy
#1 MeSH descriptor: [Diabetic Retinopathy] explode all trees #2 (diabet* or proliferative or non‐proliferative) near/4 retinopath* #3 DR near/3 (eye* or vision or visual* or sight) #4 #1 or #2 or #3 #5 MeSH descriptor: [Vitrectomy] explode all trees #6 vitrectom* #7 PPV* #8 #5 or #6 or #7 #9 MeSH descriptor: [Angiogenesis Inhibitors] explode all trees #10 MeSH descriptor: [Angiogenesis Inducing Agents] this term only #11 MeSH descriptor: [Endothelial Growth Factors] this term only #12 MeSH descriptor: [Vascular Endothelial Growth Factors] explode all trees #13 macugen or pegaptanib or lucentis or rhufab or ranibizumab or bevacizumab or avastin or aflibercept or conbercept or OPT 302 or Opthea or RTH258 or faricimab or brolucizumab or leizumabor or abicipar pegol #14 anti near/2 VEGF* #15 anti near/1 angiogen* #16 endothelial near/2 growth near/2 factor* #17 VEGF TRAP* #18 #9 or #10 or #11 or #12 or #13 or #14 or #15 or #16 or #17 #19 #4 and #8 and #18
Appendix 2. MEDLINE Ovid search strategy
1. randomized controlled trial.pt. 2. (randomized or randomised).ab,ti. 3. placebo.ab,ti. 4. dt.fs. 5. randomly.ab,ti. 6. trial.ab,ti. 7. groups.ab,ti. 8. or/1‐7 9. exp animals/ 10. exp humans/ 11. 9 not (9 and 10) 12. 8 not 11 13. diabetic retinopathy/ 14. ((diabet$ or proliferative or non‐proliferative) adj4 retinopath$).tw. 15. diabetic retinopathy.kw. 16. (DR adj3 (eye$ or vision or visual$ or sight$)).tw. 17. or/13‐16 18. exp vitrectomy/ 19. vitrectom$.tw. 20. PPV$.tw. 21. or/18‐20 22. exp angiogenesis inhibitors/ 23. angiogenesis inducing agents/ 24. endothelial growth factors/ 25. exp vascular endothelial growth factors/ 26. (macugen$ or pegaptanib$ or lucentis$ or rhufab$ or ranibizumab$ or bevacizumab$ or avastin$ or aflibercept$ or conbercept$ or OPT 302 or Opthea$ or RTH258 or faricimab or brolucizumab or leizumabor or abicipar pegol).tw. 27. (anti adj2 VEGF$).tw. 28. (anti adj1 angiogen$).tw. 29. (endothelial adj2 growth adj2 factor$).tw. 30. VEGF TRAP$.tw. 31. or/22‐30 32. 12 and 17 and 21 and 31
The search filter for trials at the beginning of the MEDLINE strategy is from the published paper by Glanville 2006.
Appendix 3. EMBASE Ovid search strategy
1. exp randomized controlled trial/ 2. exp randomization/ 3. exp double blind procedure/ 4. exp single blind procedure/ 5. random$.tw. 6. or/1‐5 7. (animal or animal experiment).sh. 8. human.sh. 9. 7 and 8 10. 7 not 9 11. 6 not 10 12. exp clinical trial/ 13. (clin$ adj3 trial$).tw. 14. ((singl$ or doubl$ or trebl$ or tripl$) adj3 (blind$ or mask$)).tw. 15. exp placebo/ 16. placebo$.tw. 17. random$.tw. 18. exp experimental design/ 19. exp crossover procedure/ 20. exp control group/ 21. exp latin square design/ 22. or/12‐21 23. 22 not 10 24. 23 not 11 25. exp comparative study/ 26. exp evaluation/ 27. exp prospective study/ 28. (control$ or prospectiv$ or volunteer$).tw. 29. or/25‐28 30. 29 not 10 31. 30 not (11 or 23) 32. 11 or 24 or 31 33. exp diabetic retinopathy/ 34. ((diabet$ or proliferative or non‐proliferative) adj4 retinopath$).tw. 35. (proliferat$ adj3 retinopath$).tw. 36. (DR adj3 (eye$ or vision or visual$ or sight$)).tw. 37. or/33‐36 38. exp vitrectomy/ 39. vitrectom$.tw. 40. PPV$.tw. 41. or/38‐40 42. angiogenesis/ 43. angiogenesis inhibitors/ 44. angiogenesis factor/ 45. monoclonal antibody/ 46. exp endothelial cell growth factor/ 47. vasculotropin/ 48. (macugen$ or pegaptanib$ or lucentis$ or rhufab$ or ranibizumab$ or bevacizumab$ or avastin$ or aflibercept$ or conbercept$ or OPT 302 or Opthea$ or RTH258 or faricimab or brolucizumab or leizumabor or abicipar pegol).tw. 49. (anti adj2 VEGF$).tw. 50. (endothelial adj2 growth adj2 factor$).tw. 51. (anti adj1 angiogen$).tw. 52. VEGF TRAP$.tw. 53. or/42‐52 54. 37 and 41 and 53 55. 32 and 54
Appendix 4. LILACS search strategy
diabetic retinopathy [Words] and vitrectom$ or PPV$ [Words] and ranibizumab or bevacizumab or avastin or aflibercept or conbercept or OPT 302 or Opthea or RTH258 or faricimab or brolucizumab or leizumabor or abicipar pegol [Words]
Appendix 5. ISRCTN search strategy
(Diabetic Retinopathy) AND (vitretomy OR PPV) AND (Ranibizumab OR Bevacizumab OR Avastin OR Aflibercept OR Conbercept OR faricimab OR brolucizumab OR leizumabor)
Appendix 6. ClinicalTrials.gov search strategy
(Ranibizumab OR Bevacizumab OR Avastin OR Aflibercept OR Conbercept OR OPT 302 OR Opthea OR RTH258 OR faricimab OR brolucizumab OR leizumabor OR abicipar pegol ) AND (Diabetic Retinopathy) AND (vitretomy OR PPV)
Appendix 7. WHO ICTRP search strategy
Diabetic Retinopathy = condition AND Ranibizumab OR Bevacizumab OR Avastin OR Aflibercept OR Conbercept OR OPT 302 OR Opthea OR RTH258 OR faricimab OR brolucizumab OR leizumabor OR abicipar pegol = intervention
Data and analyses
Comparison 1. Anti‐VEGF versus control.
| Outcome or subgroup title | No. of studies | No. of participants | Statistical method | Effect size |
|---|---|---|---|---|
| 1.1 Mean BCVA | 13 | 699 | Mean Difference (IV, Random, 95% CI) | ‐0.25 [‐0.39, ‐0.11] |
| 1.2 Early POVCH | 14 | 1038 | Risk Ratio (M‐H, Random, 95% CI) | 0.44 [0.34, 0.58] |
| 1.3 Late POVCH | 11 | 579 | Risk Ratio (M‐H, Random, 95% CI) | 0.47 [0.30, 0.74] |
| 1.4 Revision surgery for POVCH | 4 | 207 | Risk Ratio (M‐H, Random, 95% CI) | 0.44 [0.15, 1.28] |
| 1.5 Revision surgery for recurrent traction and/or RRD | 4 | 145 | Risk Ratio (M‐H, Random, 95% CI) | 0.50 [0.15, 1.66] |
| 1.6 Intraoperative retinal breaks | 12 | 915 | Risk Ratio (M‐H, Random, 95% CI) | 0.37 [0.24, 0.59] |
| 1.7 Silicone oil use | 10 | 591 | Risk Ratio (M‐H, Random, 95% CI) | 0.46 [0.27, 0.80] |
Comparison 2. Anti‐VEGF versus control: subgroup analysis ‐ time of administration of anti‐VEGF.
| Outcome or subgroup title | No. of studies | No. of participants | Statistical method | Effect size |
|---|---|---|---|---|
| 2.1 Mean BCVA | 11 | 603 | Mean Difference (IV, Random, 95% CI) | ‐0.26 [‐0.41, ‐0.10] |
| 2.1.1 Anti‐VEGF administered < 5 days preoperatively | 7 | 396 | Mean Difference (IV, Random, 95% CI) | ‐0.30 [‐0.53, ‐0.07] |
| 2.1.2 Anti‐VEGF administered ≥ 5 days preoperatively | 4 | 207 | Mean Difference (IV, Random, 95% CI) | ‐0.13 [‐0.20, ‐0.06] |
| 2.2 Early POVCH | 13 | 877 | Risk Ratio (M‐H, Random, 95% CI) | 0.39 [0.28, 0.55] |
| 2.2.1 Anti‐VEGF administered < 5 days preoperatively | 8 | 618 | Risk Ratio (M‐H, Random, 95% CI) | 0.44 [0.29, 0.66] |
| 2.2.2 Anti‐VEGF administered ≥ 5 days preoperatively | 5 | 259 | Risk Ratio (M‐H, Random, 95% CI) | 0.26 [0.14, 0.51] |
Comparison 3. Anti‐VEGF versus control: subgroup analysis ‐ main indication for vitrectomy.
| Outcome or subgroup title | No. of studies | No. of participants | Statistical method | Effect size |
|---|---|---|---|---|
| 3.1 Mean BCVA | 4 | 177 | Mean Difference (IV, Random, 95% CI) | ‐0.42 [‐0.72, ‐0.13] |
| 3.1.1 Main indication for surgery: vitreous haemorrhage | 3 | 137 | Mean Difference (IV, Random, 95% CI) | ‐0.25 [‐0.37, ‐0.13] |
| 3.1.2 Main indication for surgery: tractional retinal detachment | 1 | 40 | Mean Difference (IV, Random, 95% CI) | ‐1.31 [‐1.76, ‐0.86] |
Comparison 4. Anti‐VEGF versus control: subgroup analysis ‐ bevacizumab versus other anti‐VEGF.
| Outcome or subgroup title | No. of studies | No. of participants | Statistical method | Effect size |
|---|---|---|---|---|
| 4.1 Mean BCVA | 12 | 579 | Mean Difference (IV, Random, 95% CI) | ‐0.22 [‐0.36, ‐0.08] |
| 4.1.1 Bevacizumab versus control | 6 | 307 | Mean Difference (IV, Random, 95% CI) | ‐0.35 [‐0.79, 0.08] |
| 4.1.2 All other anti‐VEGFs versus control | 6 | 272 | Mean Difference (IV, Random, 95% CI) | ‐0.19 [‐0.28, ‐0.10] |
Characteristics of studies
Characteristics of included studies [ordered by study ID]
Ahmadieh 2009.
| Study characteristics | ||
| Methods | Prospective, randomised, double‐masked clinical trial Country: Iran | |
| Participants | Number: 68 eyes of 68 participants undergoing PPV Age: mean (± SD) age was 55.2 ± 11.1 years (range 21 to 76 years) Sex: 34 (50%) males; 34 (50%) females Inclusion criteria:
Exclusion criteria:
|
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Primary outcome measure:
Secondary outcome measures:
Follow‐up: 1 day, 1 week and 1 month after surgery |
|
| Notes | Trial registration number: NCT00524875 Date study conducted: January 2007 to December 2007 Funding: not reported Conflict of interest: reported that there were none |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | Randomisation was performed by random block permutation according to a computer‐generated randomisation list. |
| Allocation concealment (selection bias) | Low risk | Details of the allocation were unknown to the investigators. |
| Blinding of participants and personnel (performance bias) All outcomes | Low risk | Participants and personnel were masked to the treatment method. |
| Blinding of outcome assessment (detection bias) All outcomes | Low risk | Visual acuity was measured by an optometrist who was masked to the groups. All pre‐ and postoperative examinations were performed by one of the authors (NS), who was also masked to the study group identification. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | A flow chart included within the results section accounted for all participants who failed to complete the study protocol. |
| Selective reporting (reporting bias) | Low risk | All primary and secondary outcomes were reported, based on both the intention‐to‐treat analysis and per‐protocol analysis. |
Ahn 2011.
| Study characteristics | ||
| Methods | Prospective, randomised, open‐label trial Country: South Korea |
|
| Participants | Number: 107 Age: mean age (± SD). Preoperative IVB group 51.0 (± 9.5), intraoperative IVB group 55.6 (± 10.6), and control 55.0 (± 11.4) Sex: (male/female): preoperative IVB group 23/13, intraoperative IVB group 21/16 and control 16/18 Inclusion criteria:
Exclusion criteria:
|
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Primary outcome measures:
Secondary outcome measures:
Follow‐up: 1 day, 1 week, 1, 3 and 6 months after surgery if there were no postoperative events |
|
| Notes | A total of 107 eyes of 91 participants, of which there were 16 bilateral participants, were included for analysis Trial registration number: NTC00745498 Date study conducted: June 2008 to October 2010 (from trials registry entry) Funding: not reported Conflict of interest: reported that there were none |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | Randomisation was carried out using a permuted block analysis. |
| Allocation concealment (selection bias) | Low risk | Allocation was performed by a biostatistician. |
| Blinding of participants and personnel (performance bias) All outcomes | High risk | The study was open‐label. |
| Blinding of outcome assessment (detection bias) All outcomes | High risk | The study was open‐label. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | The distribution and attrition rate of study participants was clearly described in a flow chart. |
| Selective reporting (reporting bias) | Low risk | All outcomes were reported. |
Aleman 2019.
| Study characteristics | ||
| Methods | Prospective, randomised, double‐masked clinical trial Country: Mexico |
|
| Participants | Number: 206 Age: mean age was 58.0 years (range 56.0 to 60.1 years) in IVZ group and 55.8 (range 53.9 to 57.8 years) in IVB group Sex: (male/female): preoperative IVZ group 44/38, preoperative IVB group 47/44 Inclusion criteria:
Exclusion criteria:
|
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Primary outcome measure:
Secondary outcome measures:
Follow‐up: 15 ± 5 days, 40 ± 10 days, 185 ± 15 days (6 months) |
|
| Notes | 206 participants randomised and 173 participants completed follow‐up Trial registration number: NCT02590094 Date study conducted: October 2016 to August 2018 Funding: none Conflict of Interest: none declared |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | Randomisation was carried out using a simulated coin toss programme. |
| Allocation concealment (selection bias) | Unclear risk | Not reported. |
| Blinding of participants and personnel (performance bias) All outcomes | Low risk | Both participants and personnel were masked to the treatment method. |
| Blinding of outcome assessment (detection bias) All outcomes | High risk | Unmasked vitreoretinal department faculty and fellows rendered the preoperative and postoperative care. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | The distribution and attrition rate of study participants was clearly described in a flow chart. |
| Selective reporting (reporting bias) | Low risk | All primary and secondary outcomes were analysed and reported. |
Arevalo 2019.
| Study characteristics | ||
| Methods | Prospective, randomised, double‐masked, multi‐centre clinical trial Countries: multi‐centre (13 clinical sites from 9 countries) – PACORES (Pan‐American collaborative retina study group) |
|
| Participants | Number: 214 Age: mean age (± SD) was 59.5 ± 11.0 years in IVB group and 61.3 ± 10 in sham group Sex: (Male %): preoperative IVB group 62%, preoperative sham group 54% Inclusion criteria:
Exclusion criteria: Ocular:
Systemic:
|
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Primary outcome measure:
Secondary outcome measures:
Follow‐up: 12 months |
|
| Notes | Trial registration number: NCT01976923 Date study conducted: November 2013 to July 2015 Funding: none reported Conflict of Interest: none declared |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | Randomisation was performed using an Internet‐based randomisation generator using the method of randomly permuted blocks. |
| Allocation concealment (selection bias) | Low risk | Allocation was performed by a retina specialist not involved in patient treatment or follow‐up. |
| Blinding of participants and personnel (performance bias) All outcomes | Low risk | All follow‐up examinations were performed by personnel masked to the type of treatment. Patients were masked too. |
| Blinding of outcome assessment (detection bias) All outcomes | Low risk | Personnel performing follow‐up examinations were masked to the type of treatment. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | No comment was made. However, it is clear from the results that all participants completed follow‐up. |
| Selective reporting (reporting bias) | Low risk | All outcomes were reported. |
Comyn 2017.
| Study characteristics | ||
| Methods | Pilot, prospective, randomised, double‐masked, single‐centre clinical trial Country: United Kingdom |
|
| Participants | Number: 30 Age: mean age (± SD) was 48.7 ± 18 years in IVR group and 57.1 ± 14 in preoperative saline group Sex: (male/female): preoperative IVR group 6/9 and preoperative saline group 3/12 Inclusion criteria:
Exclusion criteria:
|
|
| Interventions | Interventions:
|
|
| Outcomes | Primary outcome measure:
Secondary outcome measures:
Follow‐up: 12 weeks |
|
| Notes | Trial registration number: NCT01306981 Date study conducted: March 2011 to March 2013 (from ClinicalTrials.gov) Funding: by an unrestricted research grant from Novartis Pharmaceuticals UK Ltd; the National Institute for Health Research Biomedical Research Centre at Moorfields Eye Hospital National Health Service Foundation Trust and University College London Institute of Ophthalmology; and a multi‐user equipment grant from The Wellcome Trust Conflict of Interest: OC has received travel support from Novartis. None declared from the remaining authors. |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | Randomisation was performed using random permuted blocks of varying sizes. |
| Allocation concealment (selection bias) | Low risk | The allocation was held by the trial statistician. |
| Blinding of participants and personnel (performance bias) All outcomes | Low risk | Both participants and personnel performing assessments were masked to the interventions. |
| Blinding of outcome assessment (detection bias) All outcomes | Low risk | Masked assessing investigators performed all postoperative assessments. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | All patients completed follow‐up. |
| Selective reporting (reporting bias) | Low risk | All outcomes were reported. |
Cui 2018.
| Study characteristics | ||
| Methods | Prospective, randomised clinical trial Country: China |
|
| Participants | Number: 60 Age: mean age (± SD) was 60.74 ± 2.63 years in IVC group, 55.28 ± 5.16 in the IVR group and 57.49 ± 4.22 in IVTA group Sex: (male/female): preoperative IVC group 9/8, preoperative IVR group 13/6 and preoperative IVTA group 10/5 Inclusion criteria:
Exclusion criteria:
|
|
| Interventions | Interventions:
|
|
| Outcomes | Primary outcome measure:
Secondary outcome measures:
Follow‐up: 6 months |
|
| Notes | 60 patients randomised and 58 patients completed the follow‐up Date study conducted: January 2015 to December 2015 Funding: from the First Hospital of Qiqihar City, Heilongjiang, China, the National Natural Science Foundation of China, the US Department of Veterans Affairs and the Veterans Administration Medical Center at Memphis, TN Conflict of Interest: none declared |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Unclear risk | “Patients were randomly divided…” |
| Allocation concealment (selection bias) | Unclear risk | Not stated in the report. |
| Blinding of participants and personnel (performance bias) All outcomes | High risk | Participants were not masked to their study group. |
| Blinding of outcome assessment (detection bias) All outcomes | Low risk | The surgeries were performed by two masked surgeons. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | The distribution and attrition rates of the participants are clearly presented in a flow chart. |
| Selective reporting (reporting bias) | Unclear risk | All outcomes were reported. |
di Lauro 2009.
| Study characteristics | ||
| Methods | Prospective, interventional randomised controlled trial Country: Italy | |
| Participants | Number: 72 eyes of 68 participants Age: not given Sex: not given Inclusion criteria:
Exclusion criteria:
|
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Primary outcome measures:
Secondary outcome measures:
Follow‐up: 1, 6, 12 and 24 weeks after surgery, and ultrasonography was performed before and 24 weeks after the injection |
|
| Notes | Trial registration number: NCT01025934 Date study conducted: October 2005 to May 2007 Funding: not reported Conflict of interest: reported that there were none |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Unclear risk | "We randomly assigned eligible patients... " and "The patients were randomly divided into three treatment groups (A, B, C)". |
| Allocation concealment (selection bias) | Unclear risk | Not stated in the report. |
| Blinding of participants and personnel (performance bias) All outcomes | Low risk | A sham injection was used in the control group. |
| Blinding of outcome assessment (detection bias) All outcomes | Low risk | A sham injection was used in the control group. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | Not stated in the report, however clear from the results that all participants completed follow‐up. |
| Selective reporting (reporting bias) | Low risk | Data for all main outcomes were analysed and presented. |
Dong 2019.
| Study characteristics | ||
| Methods | Prospective, randomised clinical trial Country: China |
|
| Participants | Number: 120 eyes of 120 participants undergoing PPV Age: mean (± SD) age was 56.61 ± 5.32 years (range 20 to 82 years) in the vitrectomy alone group and 57.31 ± 5.62 years (range 21 to 84) in the IVR group Sex: male/female: 33/27 in the vitrectomy alone group and 35/25 in the IVR group Inclusion criteria:
Exclusion criteria:
|
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes |
Follow‐up: 6 months |
|
| Notes | Date study conducted: October 2014 to November 2017 Funding: not reported Conflict of interest: not reported |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Unclear risk | “120 eyes of 120 patients were randomly divided into two groups…” |
| Allocation concealment (selection bias) | Unclear risk | Not reported. |
| Blinding of participants and personnel (performance bias) All outcomes | Unclear risk | Not reported. |
| Blinding of outcome assessment (detection bias) All outcomes | Unclear risk | Not reported. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | Not stated in the report, however clear from the results that all participants completed follow‐up. |
| Selective reporting (reporting bias) | Unclear risk | All primary and secondary outcomes were reported. |
El Batarny 2008.
| Study characteristics | ||
| Methods | Prospective, randomised, open‐label, controlled trial Country: Egypt |
|
| Participants | Number: 30 Age: mean (± SD). Control group 46 (± 12) and intervention group 44 (± 11) Sex: not given Inclusion criteria:
Exclusion criteria not stated |
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Primary outcomes:
Follow‐up: 1 day, 7 days, 2 weeks, 1 month and then monthly until end of study (all participants completed a minimum of 6 months) |
|
| Notes | Trial registration number: not reported Date study conducted: not reported Funding: not reported Conflict of interest: reported that there were none |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Unclear risk | Participants were randomised by diagnosis. Not clear statement on randomisation sequence. |
| Allocation concealment (selection bias) | Unclear risk | Not stated. |
| Blinding of participants and personnel (performance bias) All outcomes | High risk | Participants were not masked to their study group. |
| Blinding of outcome assessment (detection bias) All outcomes | High risk | Not mentioned, and treatment groups were different. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | All participants completed follow‐up. |
| Selective reporting (reporting bias) | Unclear risk | All outcomes were reported. |
Farahvash 2011.
| Study characteristics | ||
| Methods | Randomised, single‐masked (surgeon), controlled trial Country: Iran |
|
| Participants | Number: 35 Age: mean (range) 58.5 (37 to 73) Sex: (male/female): 18/17 Inclusion criteria:
Exclusion criteria:
|
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Primary outcomes:
Secondary outcomes
Follow‐up: 1 day, 1 week, every 3 months (minimum follow‐up 3 months) |
|
| Notes | We contacted the authors to further discuss the severity of POVCH in each arm of the study. Although no formal grading scale was used to assess the POVCH, the authors described the clinical findings as follows: "We had two cases of early vitreous cavity haemorrhage (within 4 weeks of surgery), both in non injection group. The haemorrhage was dense and fundus obscuring, but resolved spontaneously during follow up. Both of them have been undergone vitrectomy for vitreous haemorrhage without TRD, with no air, SF6 or silicone as a tamponade. We had five cases of late vitreous cavity haemorrhage before writing of paper (occurring after more than 4 weeks), two in non injection group and three in injection group. Only in one participant in injection group, vitreous cavity haemorrhage was dense and fundus obscuring. In other participants, it presented as recurrent bouts of non fundus obscuring vitreous cavity haemorrhage". Trial registration number: not reported Date study conducted: January 2008 to January 2009 Funding: not reported Conflict of interest: reported that there were none |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Unclear risk | "Participants were randomly assigned..." Not enough information on random sequence generation. |
| Allocation concealment (selection bias) | Unclear risk | Not stated. |
| Blinding of participants and personnel (performance bias) All outcomes | High risk | Study participants were not masked to which group they had been randomised to. |
| Blinding of outcome assessment (detection bias) All outcomes | Unclear risk | All surgeons were masked regarding treatment group, but it was unclear if the outcome assessors were masked. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | Participants who failed to complete the study follow‐up are clearly accounted for in the results. |
| Selective reporting (reporting bias) | Unclear risk | All outcomes were reported. |
Ferraz 2013.
| Study characteristics | ||
| Methods | Prospective, interventional consecutive, randomised, clinical trial Country: Brazil |
|
| Participants | Number: 27 eyes of 27 participants undergoing PPV Age: mean (± SD) age was 52.2 ± 13.9 years Sex: 17 males; 10 females Inclusion criteria:
Exclusion criteria:
|
|
| Interventions | Interventions:
|
|
| Outcomes | Primary outcome measures:
Follow‐up: 1 week, 1 month and 6 months after surgery |
|
| Notes | Trial registration number: not reported Date study conducted: not reported Funding: not reported Conflict of interest: reported that there were none |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Unclear risk | “The patients were randomized in order to assign…” |
| Allocation concealment (selection bias) | Unclear risk | Not reported. |
| Blinding of participants and personnel (performance bias) All outcomes | Unclear risk | Not reported. |
| Blinding of outcome assessment (detection bias) All outcomes | Unclear risk | Not reported. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | Not stated in the report, however clear from the results that all participants completed follow‐up. |
| Selective reporting (reporting bias) | High risk | The incidence of late (> 4 weeks) postoperative VH is not reported, although it is mentioned in the methods section of the report as one of the primary outcomes. |
Hernández‐Da Mota 2010.
| Study characteristics | ||
| Methods | Prospective, randomised, open‐label study Country: Mexico |
|
| Participants | Number: 40 Age: mean 55.7 (both groups) Sex: not given Inclusion criteria:
Exclusion criteria:
|
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Primary outcomes:
Follow‐up: 1 week, 3 and 6 months |
|
| Notes | No response from authors to correspondence asking for clarification of POVCH definitions Trial registration number: not reported Date study conducted: not reported Funding: reported none Conflict of interest: reported that there were none |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Unclear risk | "Patients were randomly assigned into two groups", |
| Allocation concealment (selection bias) | Unclear risk | Not stated, |
| Blinding of participants and personnel (performance bias) All outcomes | High risk | Participants were not masked to treatment group, |
| Blinding of outcome assessment (detection bias) All outcomes | High risk | "For all patients, visual acuity and intraocular pressure were measured and recorded before PPV in a standardized, masked manner" However, not clearly stated whether outcome assessment was always masked and whether other outcomes, such as intraocular bleeding, were masked, |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | Although not directly stated, it is clear from the results that all participants completed the stated follow‐up, |
| Selective reporting (reporting bias) | Unclear risk | All outcomes were reported, |
Hu 2019.
| Study characteristics | ||
| Methods | Prospective, randomised clinical trial Country: China |
|
| Participants | Number: 106 eyes of 84 participants undergoing PPV Age: mean (± SD) age was 62.5 ± 5.4 years for the IVR group and 63.0 ± 4.6 years for the control group Sex: male/female: 22/20 in the IVR group and 25/17 in the control group Inclusion criteria:
Exclusion criteria:
|
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Outcome measures:
Follow‐up: 3 months |
|
| Notes | Trial registration number: not reported Date study conducted: January 2016 to January 2018 Funding: Yancheng Medical Science and Technology Development Program (No.YK2014016) Conflict of interest: not reported |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | Randomisation was performed by random number table method. |
| Allocation concealment (selection bias) | Unclear risk | Not reported. |
| Blinding of participants and personnel (performance bias) All outcomes | High risk | Participants were not masked to their study group. |
| Blinding of outcome assessment (detection bias) All outcomes | High risk | Surgeons were not masked to the intervention. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | It is not reported, however from the results it is clear that all participants completed follow‐up. |
| Selective reporting (reporting bias) | Unclear risk | All outcomes were reported. |
Jiang 2020.
| Study characteristics | ||
| Methods | Prospective, randomised pilot study Country: China |
|
| Participants | Number: 60 Age: mean age (± SD) was 55.54 ± 9.94 years in intraoperative IVC group and 53.5 ± 9.59 in control group Sex: male/female: intraoperative IVC group 6/9, control group 10/5 Inclusion criteria:
Exclusion criteria:
|
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Primary outcome measure:
Secondary outcome measures:
Follow‐up: 1 day, 1 week, 1 month, 3 months, 6 months and 12 months |
|
| Notes | 60 patients were randomised and 30 completed the 12‐months follow‐up Trial registration number: ChiCTR1800015751 Date study conducted: not reported Funding: National Natural Science Foundation of China (Grant No. 81870670 and Grant No.81500734), the Shanghai health bureau project (20184Y0215) and Shanghai science and technology commission project (Grant No. 18411965100). The funder had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript. Conflict of interest: none declared |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | Randomisation according to randomised table. |
| Allocation concealment (selection bias) | Unclear risk | Not reported. |
| Blinding of participants and personnel (performance bias) All outcomes | High risk | Participants were not masked to the group. |
| Blinding of outcome assessment (detection bias) All outcomes | Low risk | Assessors were masked to the group. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | The distribution and attrition rates of the participants are clearly presented in a flow chart. |
| Selective reporting (reporting bias) | Low risk | All outcomes were reported. |
Li 2022.
| Study characteristics | ||
| Methods | Pilot, randomised clinical trial Country: China |
|
| Participants | Number: 48 eyes of 48 participants undergoing PPV Age: mean (± SD) age was 49.9 ± 9.8 years Sex: 27 (56.3%) males; 21 (43.7%) females Inclusion criteria:
Exclusion criteria:
|
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes |
Follow‐up: not clearly reported |
|
| Notes | Trial registration number: ChiCTR‐ONC‐16009520 Date study conducted: November 2016 to July 2018 Funding: National Natural Science Foundation of Hunan Province and the Innovation and Development Project of Hunan Development and Reform Commission Conflict of interest: reported that there were none |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Unclear risk | Not reported. |
| Allocation concealment (selection bias) | Unclear risk | Not reported. |
| Blinding of participants and personnel (performance bias) All outcomes | High risk | Participants were not masked to the intervention. |
| Blinding of outcome assessment (detection bias) All outcomes | Low risk | All assessments were performed by one of the authors (JZ), who was masked to the study group identification. |
| Incomplete outcome data (attrition bias) All outcomes | High risk | The exact follow‐up period is not clearly stated. |
| Selective reporting (reporting bias) | High risk | There is no clear list of prespecified outcome measures for this study. |
Manabe 2015.
| Study characteristics | ||
| Methods | Prospective, double‐masked randomised controlled trial Country: Japan |
|
| Participants | Number: 62 people (66 eyes) Age: average 60 years (range 20 to 82) Sex: 82% male Inclusion criteria:
Exclusion criteria:
|
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Primary outcome:
Secondary outcome measures:
|
|
| Notes | Trial registration number: NCT01854593 Date study conducted: June 2012 to August 2013 Funding: not reported Conflict of interest: reported "none" |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Unclear risk | Not reported. |
| Allocation concealment (selection bias) | Low risk | "...were randomised using the envelop method" "Both the investigators and patients were masked to the treatment assignment". |
| Blinding of participants and personnel (performance bias) All outcomes | Low risk | "Both the investigators and patients were masked to the treatment assignment". |
| Blinding of outcome assessment (detection bias) All outcomes | Low risk | "All postoperative examinations were performed by three vitreoretinal surgeons (H.S., T.H., H.N.) who also were masked to the study group allocation". |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | All randomised participants were followed up for 1 month. |
| Selective reporting (reporting bias) | Low risk | All outcomes on trial registry entry reported. |
Modarres 2009.
| Study characteristics | ||
| Methods | Prospective, single‐masked (surgeon), randomised clinical trial Country: Iran | |
| Participants | Number: 40 Age: mean (± SD). Intervention group 55.8 (± 11.3) and control group 53.2 (± 11.7) Sex: not given Inclusion criteria:
Exclusion criteria:
Follow‐up: mean follow‐up 7 ± 3.6 months |
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Primary outcome measure:
Secondary outcome measure:
Follow‐up: mean follow‐up 7 ± 3.6 months |
|
| Notes | Trial registration number: not reported Date study conducted: not reported Funding: not reported Conflict of interest: reported that there were none |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Unclear risk | "40 eyes of 40 diabetic participants who were candidates for vitrectomy were randomly assigned to receive ..." |
| Allocation concealment (selection bias) | Unclear risk | Not stated in report. |
| Blinding of participants and personnel (performance bias) All outcomes | Unclear risk | Not stated in report. |
| Blinding of outcome assessment (detection bias) All outcomes | Unclear risk | "The surgeons were masked as to the injection", but not clear if the outcome assessors were masked. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | Not stated in report, however clear from the results that all participants completed follow‐up. |
| Selective reporting (reporting bias) | Unclear risk | All data discussed within the primary outcome for facilitation of surgery were analysed. |
Ou 2021.
| Study characteristics | ||
| Methods | Prospective, randomised control trial Country: China |
|
| Participants | Number: 75 eyes of 64 patients Age: mean (± SD) age: preoperative IVC group 56.71 (± 12.65), only vitrectomy group 57.35 (± 10.98) Sex: male/female: preoperative IVC group 15/17, vitrectomy only group 14/18 Inclusion criteria:
Exclusion criteria: not reported |
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Outcome measures:
Follow‐up: 3 months |
|
| Notes | Trial registration number: not reported Date study conducted: January 2016 to October 2019 Funding: not reported Conflict of interest: not reported |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | Randomisation was carried out using a random number table method. |
| Allocation concealment (selection bias) | Unclear risk | Not stated in the report. |
| Blinding of participants and personnel (performance bias) All outcomes | Unclear risk | Not stated in the report. |
| Blinding of outcome assessment (detection bias) All outcomes | Unclear risk | Not clear if the outcome assessors were blinded. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | It is not clearly stated in the text, however from the results it is obvious that all patients completed follow‐up. |
| Selective reporting (reporting bias) | Unclear risk | All outcomes were reported. |
Pakzad Vaezi 2014.
| Study characteristics | ||
| Methods | Prospective, randomised, double‐masked pilot study Country: Canada |
|
| Participants | Number: 29 Age: mean (± SD) age: preoperative IVR group 51.6 (± 12.3), preoperative IVB group 52.8 (± 10.5) Sex: male/female: preoperative IVR group 6/15 and preoperative IVB group 11/14 Inclusion criteria:
Exclusion criteria:
|
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Outcome measures:
|
|
| Notes | Trial registration number: NCT01760746 Date study conducted: July 2012 to April 2015 (from trial registry) Funding: not reported Conflict of interest: Drs. Albiani, Kirker, Merkur, Kertes, Eng, and Forooghian receive honoraria from Novartis. Drs. Pakzad‐Vaezi, Albiani, Kirker, Merkur, Kertes, Eng, and Forooghian receive research funding from Novartis. Dr. Fallah has no financial or proprietary interest in the materials presented herein. |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | A stratified randomisation algorithm was used. |
| Allocation concealment (selection bias) | Unclear risk | It is not stated who performed the allocation and whether they were masked or not. |
| Blinding of participants and personnel (performance bias) All outcomes | Low risk | Both investigators and participants were masked to the identity of the study drug. |
| Blinding of outcome assessment (detection bias) All outcomes | Low risk | Both investigators and participants were masked to the identity of the study drug. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | Although it is not clearly stated, it is obvious from the results that all patients completed follow‐up. |
| Selective reporting (reporting bias) | Low risk | All outcomes on trial registry entry reported. |
Ren 2019.
| Study characteristics | ||
| Methods | Prospective, randomised, controlled trial Country: China |
|
| Participants | Number: 50 Age: mean (range). Preoperative IVC group 57 (28 to 69) and control group 62 (46 to 80) Sex: male/female: preoperative IVC group 16/9 and control group 14/11 Inclusion criteria:
Exclusion criteria:
|
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Outcome measures:
|
|
| Notes | Trial registration number: NCT03426540 Date study conducted: January 2017 to March 2018 Funding: this article is supported by National Natural Science Foundation of China (81600723) Conflict of interest: none declared |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | Patients were randomly allocated according to randomised table. |
| Allocation concealment (selection bias) | Unclear risk | It is not stated who performed the allocation and whether they were masked or not. |
| Blinding of participants and personnel (performance bias) All outcomes | Low risk | The surgeon performing the operations was masked. It is not stated whether the participants were masked. |
| Blinding of outcome assessment (detection bias) All outcomes | Unclear risk | The surgeon performing the operations was masked. However, it is not clearly stated who performed the postoperative examinations. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | Although it is not clearly stated, it is obvious from the results that all patients completed follow‐up. |
| Selective reporting (reporting bias) | Low risk | All outcomes on trial registry entry reported. |
Rizzo 2008.
| Study characteristics | ||
| Methods | Interventional, consecutive, randomised, prospective study Country: Italy | |
| Participants | Number: 22 Age: mean (range). 52 years (24 to 63) Sex: not given Inclusion criteria:
Exclusion criteria:
|
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Primary outcome measure:
Secondary outcome measure:
Follow‐up: up to 6 months |
|
| Notes | Trial registration number: not reported Date study conducted: not reported Funding: not reported Conflict of interest: reported that there were none |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Low risk | "We used a table of random numbers in order to assign each study participant to group 1 or 2". |
| Allocation concealment (selection bias) | Unclear risk | Not stated in report. |
| Blinding of participants and personnel (performance bias) All outcomes | Unclear risk | Not stated in report. |
| Blinding of outcome assessment (detection bias) All outcomes | Unclear risk | Not stated in report. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | Not stated in report, however it is clear from the results that all participants completed follow‐up. |
| Selective reporting (reporting bias) | Unclear risk | Results for the feasibility of surgery were stated, but no analysis was performed. |
Sohn 2012.
| Study characteristics | ||
| Methods | Prospective, double‐masked, interventional study Country: USA |
|
| Participants | Number: 20 eyes of 19 participants Age: median 52 years Sex: male/female: 12/7 Inclusion criteria:
Exclusion criteria:
|
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Clinical outcomes:
Follow‐up: up to 3 months |
|
| Notes | — | |
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Unclear risk | Not stated in report. |
| Allocation concealment (selection bias) | Unclear risk | Not stated in report. |
| Blinding of participants and personnel (performance bias) All outcomes | Low risk | Participants in the control group underwent a sham injection. |
| Blinding of outcome assessment (detection bias) All outcomes | Low risk | Participants in the control group underwent a sham injection. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | The number of participants lost to follow‐up was clearly stated. |
| Selective reporting (reporting bias) | Low risk | All outcomes were reported. |
Su 2016.
| Study characteristics | ||
| Methods | Randomised controlled trial Country: China |
|
| Participants | Number: 36 eyes of 36 participants Age: not reported Sex: not reported Inclusion criteria:
Exclusion criteria:
|
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Primary outcomes:
Secondary outcomes:
|
|
| Notes | Trial registration number: not reported Date study conducted: not reported Funding: not reported Conflict of interest: none reported |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Unclear risk | “Patients were randomly assigned…” |
| Allocation concealment (selection bias) | Unclear risk | Not stated in the report. |
| Blinding of participants and personnel (performance bias) All outcomes | High risk | The surgeon was masked to the intervention. However, participants were not blinded. |
| Blinding of outcome assessment (detection bias) All outcomes | Unclear risk | Not reported. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | Although not clearly stated, it is obvious from the results that all patients completed follow‐up. |
| Selective reporting (reporting bias) | Unclear risk | All outcomes were reported. |
Wildan 2019.
| Study characteristics | ||
| Methods | Randomised controlled trial Country: Indonesia |
|
| Participants | Number: 24 Age: mean (± SD). IVA group 51 (± 12) and IVB group 53.50 (± 9). Sex: not reported Inclusion criteria:
Exclusion criteria:
|
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Clinical outcomes:
|
|
| Notes | Trial registration number: not reported Date study conducted: January 2015 to July 2016 Funding: not reported Conflict of interest: not reported |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Unclear risk | “Subjects who met the inclusion criteria were then randomized.” |
| Allocation concealment (selection bias) | Unclear risk | Not stated in the report. |
| Blinding of participants and personnel (performance bias) All outcomes | Unclear risk | The surgeon was masked to the intervention. However, there is no report about the participants. |
| Blinding of outcome assessment (detection bias) All outcomes | Unclear risk | Not reported. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | Although not clearly stated, it is obvious from the results that all patients completed follow‐up. |
| Selective reporting (reporting bias) | Unclear risk | All outcomes were reported. |
Yang 2016.
| Study characteristics | ||
| Methods | Prospective, single‐centre, single‐dose, randomised, controlled clinical trial Country: China |
|
| Participants | Number: 107 Age: mean (± SD). IVC group 48.63 (± 8.24) and control group 49.64 (± 8.71) Sex: male/female: IVC group 27/27 and control group 24/29 Inclusion criteria:
Exclusion criteria:
|
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Clinical outcomes:
|
|
| Notes | Trial registration number: not reported Date study conducted: March 2014 to January 2015 Funding: supported by Yunnan Applied Basic Research Projects Items (no. 2014FB093), Science and Technology for People‐Benefit Projects of Yunnan Province (no. 2014RA070), and Special‐Purpose Fund of Wang Longde Academician Workstation Conflict of interest: none reported |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Unclear risk | “Patients were randomised into two categories.” |
| Allocation concealment (selection bias) | Unclear risk | Not stated in the report. |
| Blinding of participants and personnel (performance bias) All outcomes | Unclear risk | The surgeons were masked to the intervention. However, there is no report about the participants. |
| Blinding of outcome assessment (detection bias) All outcomes | Low risk | Assessors were masked to treatment group. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | Participant flow is clearly presented in a flow chart. |
| Selective reporting (reporting bias) | Unclear risk | All outcomes were reported. |
Yu 2015.
| Study characteristics | ||
| Methods | Randomised controlled trial Country: China |
|
| Participants | Number: 125 Age: mean (range) 47.27 (27 to 77) Sex: 59 males and 66 females Inclusion criteria:
Exclusion criteria: not reported |
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Primary outcomes:
|
|
| Notes | Trial registration number: not reported Date study conducted: January 2011 to December 2014 Funding: not reported Conflict of interest: none reported |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Unclear risk | It is stated in the manuscript that patients were randomly assigned to treatment groups. |
| Allocation concealment (selection bias) | Unclear risk | Not reported. |
| Blinding of participants and personnel (performance bias) All outcomes | Unclear risk | Not reported. |
| Blinding of outcome assessment (detection bias) All outcomes | Unclear risk | Not reported. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | Although not clearly stated, it is obvious from the results that all patients completed follow‐up. |
| Selective reporting (reporting bias) | Unclear risk | All outcomes were reported. |
Zaman 2013.
| Study characteristics | ||
| Methods | Randomised, open‐label, controlled trial Country: Pakistan |
|
| Participants | Number: 54 Age: mean (± SD) 52.07 (± 5.54); range 39 to 67 Sex: male/female: 32/22 Inclusion criteria:
Exclusion criteria: not stated |
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Primary outcome measures:
Follow‐up: days 1, 7, 14 and then monthly for up to 6 months |
|
| Notes | We attempted to contact the corresponding author to clarify details in the methodology and results, but have received no response Trial registration number: not reported Date study conducted: September 2010 to August 2011 Funding: not reported Conflict of interest: not reported |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Unclear risk | "Patients were randomised into two categories". No further details provided. |
| Allocation concealment (selection bias) | Unclear risk | Not commented on within the article. |
| Blinding of participants and personnel (performance bias) All outcomes | High risk | Although no specific comment was made, the study appears to be open‐label. |
| Blinding of outcome assessment (detection bias) All outcomes | High risk | Although no specific comment was made, the study appears to be open‐label. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | All participants completed the study protocol. |
| Selective reporting (reporting bias) | Unclear risk | All stated outcomes were presented in the results. |
Zhou 2017.
| Study characteristics | ||
| Methods | Randomised, controlled trial Country: China |
|
| Participants | Number: 42 eyes from 35 patients Age: mean. IVC group 72.46 and no IVC group 52.07 Sex: male/female: IVC group 8/10 and no IVC group 8/9 Inclusion criteria:
Exclusion criteria: not reported |
|
| Interventions | Intervention:
Comparator:
|
|
| Outcomes | Outcome measures:
Follow‐up: 6 months |
|
| Notes | Trial registration number: not reported Date study conducted: October 2014 to August 2016 Funding: not reported Conflict of interest: not reported |
|
| Risk of bias | ||
| Bias | Authors' judgement | Support for judgement |
| Random sequence generation (selection bias) | Unclear risk | It is stated in the manuscript that patients were randomly assigned to treatment groups. |
| Allocation concealment (selection bias) | Unclear risk | Not commented on within the article. |
| Blinding of participants and personnel (performance bias) All outcomes | Unclear risk | Not commented on within the article. |
| Blinding of outcome assessment (detection bias) All outcomes | Unclear risk | Not commented on within the article. |
| Incomplete outcome data (attrition bias) All outcomes | Low risk | From the results it is obvious that all participants completed the study protocol. |
| Selective reporting (reporting bias) | Unclear risk | All stated outcomes were presented in the results. |
ARMD: age‐related macular degeneration BCVA: best‐corrected visual acuity bFGF: basic fibroblast growth factor CMT: central macular thickness CRT: central retinal thickness CTGF: connective tissue growth factor DMO: diabetic macular oedema DR: diabetic retinopathy FAZ: foveal avascular zone GAS6: growth arrest‐specific protein 6 IOP: intraocular pressure IVB: intravitreal bevacizumab IVC: intravitreal conbercept IVR: intravitreal ranibizumab IVTA: intravitreal triamcinolone acetonide IVZ: intravitreal Ziv‐aflibercept NVG: neovascular glaucoma PDR: proliferative diabetic retinopathy PIGF: placental growth factor POVCH: postoperative vitreous cavity haemorrhage PPV: pars plana vitrectomy PRP: panretinal photocoagulation RAO: retinal artery occlusion RD: retinal detachment RRD: rhegmatogenous retinal detachment RVO: retinal vein occlusion SD: standard deviation SDF‐1: stromal cell‐derived factor 1 T1DM/T2DM: type I/type II diabetes mellitus TIA: transient ischaemic attack TRD: tractional retinal detachment VA: visual acuity VEGF: vascular endothelial growth factor VH: vitreous haemorrhage
Characteristics of excluded studies [ordered by study ID]
| Study | Reason for exclusion |
|---|---|
| Abd 2020 | Study group did not receive vitrectomy, it received panretinal photocoagulation |
| Abdelhakim 2011 | This prospective case series included 20 eyes and found the following results:
The study was excluded as it was non‐randomised |
| Albuquerque 2014 | Anti‐VEGF agent was administered again 6 weeks postoperatively |
| Antoszyk 2020 | Study arm did not receive vitrectomy |
| Antoszyk 2021 | Study arm did not receive vitrectomy |
| Berk Ergun 2014 | This study was excluded as it is retrospective |
| Bhavsar 2014 | Vitrectomy was an outcome rather than an intervention |
| Castillo 2017 | No control arm; all arms received the same anti‐VEGF |
| Castillo 2018 | No control arm; all arms received the same anti‐VEGF |
| Chakraborty 2021 | Retrospective design |
| Chatziralli 2020 | Study arm did not receive vitrectomy after ranibizumab |
| Cheema 2010 | This study was excluded as it is retrospective |
| Chelala 2018 | No vitrectomy performed |
| Chen 2020 | Non‐randomised study |
| Comyn 2019 | No outcomes of interest reported |
| da R Lucena 2009 | Did not assess POVCH |
| Demir 2013 | This study was excluded as it is retrospective |
| Dirani 2014 | Vitrectomy was an outcome rather than an intervention; initially none of the groups received vitrectomy |
| Doganay 2010 | This prospective case‐controlled study was excluded due to lack of randomisation. Participants were divided into 2 groups: Group 1 (n = 32) received 1.25 mg of IVB 1 week before surgery; Group 2 (n = 50) did not. Results:
|
| Elwan 2013 | Study has been retracted |
| Feng 2018 | Control arm included eyes with non‐diabetic ocular disease |
| Forooghian 2016 | No outcomes of interest reported |
| Gao 2020 | All arms received anti‐VEGF injection |
| Goncu 2014 | Excluded as not randomised |
| Gupta 2008 | Excluded as not randomised |
| Gupta 2012a | This study was excluded due to its retrospective design |
| Gupta 2012b | Excluded as this is a retrospective observational study |
| Haseeb 2019 | Not randomised |
| Hu 2021 | Retrospective design |
| Hu 2022 | No outcomes of interest reported |
| Ishikawa 2009 | This study was excluded because of small numbers and no control group; also no comment made on POVCH |
| Jiao 2014 | No outcomes of interest reported |
| Jin‐An 2014 | No outcomes of interest reported |
| Jirawison 2012 | Excluded as this is a retrospective observational study |
| Jorge 2021 | Both groups received the same anti‐VEGF; one group did not receive vitrectomy |
| Karimov 2021 | Retrospective design |
| Kasetty 2021 | Both study arms received aflibercept; no control group |
| Kawano 2013 | Not randomised |
| Leonard 2014 | All patients received the same anti‐VEGF preoperatively |
| Li 2010 | This study was excluded due to its retrospective design |
| Li 2015 | Study group included macular hole patients as well as patients with proliferative diabetic retinopathy |
| Li 2016 | Retrospective design |
| Li 2020 | Control group included non diabetic patients |
| Liu 2019 | All study arms received anti‐VEGF injection; outcomes of interest not reported |
| Lo 2009 | This study was excluded due to its retrospective design |
| Ma 2016 | Non randomised study |
| Marcus 2017 | All study arms received the same anti‐VEGF; no control group |
| Meng 2016 | Vitrectomy was an outcome rather than an intervention; initially no treatment group was supposed to receive vitrectomy |
| NCT01589718 | Withdrawn prior to enrolment |
| Oshima 2009 | This study was excluded because of the retrospective enrolment of participants, the absence of randomisation and the different study periods of the two groups |
| Ozer 2022 | No control group ‐ everyone received the same anti‐VEGF; no outcomes of interest reported |
| Papavasileiou 2017 | Retrospective design |
| Park 2010 | This study was excluded due to its retrospective design |
| Park 2021 | Vitrectomy was an outcome rather an intervention; initially no patient was supposed to have vitrectomy |
| Pokroy 2011 | This study was excluded due to its retrospective design |
| Romano 2009a | Found the following results:
This prospective study was excluded due to the lack of a control group. Participants also received an additional dose of bevacizumab at the end of surgery, which makes interpretation of the effect of the preoperative bevacizumab on POVCH difficult. |
| Romano 2009b | Found the following results:
This prospective study was excluded due to the lack of a control group |
| Sato 2013 | This study was excluded due to its retrospective design |
| Shi 2020 | No control group; all arms received anti‐VEGF injection |
| Starnes 2019 | All study arms received the same anti‐VEGF agent; no control group |
| Sun 2017 | No outcomes of interest reported |
| Sun 2022 | Did not report any outcomes of interest (it only measures levels of cytokines) |
| Tsubota 2019 | Non randomised study; no outcomes of interest reported |
| Turkseven Kumral 2021 | Retrospective study |
| Victor 2014 | No outcomes of interest reported |
| Vidinova 2020 | Non randomised study |
| Wang 2019 | No outcomes of interest were reported |
| Wang 2020 | No outcomes of interest reported |
| Yang 2008 | Found the following results:
This study was excluded due to the small numbers and lack of randomisation (participants in the control group were selected retrospectively). Also C3F8 was used in addition to preoperative anti‐VEGF in all participants in the treatment group. |
| Yeh 2009 | Excluded as participants allocated by alternation |
| Yeoh 2008 | Found the following results:
This study was excluded due to the lack of a control group. |
| Yeung 2010 | This study was excluded as it is retrospective |
| Yin 2017 | Not randomised |
| Zeng 2017 | Non‐randomised study |
| Zhou 2018a | Control group included eyes without diabetic pathology |
| Zhou 2018b | Non‐randomised |
BCVA: best‐corrected visual acuity IVB: intravitreal bevacizumab logMAR: logarithm of minimal angle of resolution POVCH: postoperative vitreous cavity haemorrhage SD: standard deviation VEGF: vascular endothelial growth factor
Characteristics of ongoing studies [ordered by study ID]
ISRCTN79120387.
| Study name | A randomised, single‐masked, phase IV pilot study of the efficacy and safety of adjunctive intravitreal Avastin® (bevacizumab) in the prevention of early postoperative vitreous haemorrhage following diabetic vitrectomy |
| Methods | Randomised, single‐masked, controlled trial |
| Participants | 30 |
| Interventions | Avastin® will be administered intravitreally in a single‐ or dual‐dose regimen of 1.25 mg (in 0.05 mL) 2 weeks prior to vitrectomy and at the end of vitrectomy if internal tamponade (oil, air or gas) was not used. No sham intravitreal injections will be given before or after vitrectomy if participant is randomised to the usual treatment group. |
| Outcomes | Primary: Postoperative vitreous haemorrhage based on 2 masked clinical assessments at 6 weeks and 6 months Secondary:
|
| Starting date | 2007 |
| Contact information | Mr Lyndon da Cruz Moorfields Eye Hospital, 162 City Road, London |
| Notes | No reply from lead investigator |
NCT00516464.
| Study name | Evaluation of ranibizumab on the ease of procedure and complication rate in proliferative diabetic retinopathy (PDR) requiring vitrectomy |
| Methods | Randomised, single‐masked, controlled trial |
| Participants | 40 |
| Interventions | 40 participants will be enrolled and randomised 3:1 to ranibizumab or vitrectomy alone. 30 consented, enrolled participants will receive 3 intravitreal injections of 0.5 mg ranibizumab administered 1 to 3 weeks pre‐procedure, intraoperatively, and 1 month post‐vitrectomy |
| Outcomes | To evaluate the effect of ranibizumab on vitrectomy complications such as recurrent vitreous haemorrhage, postoperative retinal detachment rates, and development of intraoperative retinal breaks (time frame: 6 months) |
| Starting date | August 2007 |
| Contact information | Retina Associates, PA. Shawnee Mission, Kansas, United States, 66204 Contact: Lexie Manning 913‐831‐7400 lmanning@kcretina.com [mailto:lmanning%40kcretina.com?subject=NCT00516464, FVF4295, Evaluation of Ranibizumab in Proliferative Diabetic Retinopathy (PDR) Requiring Vitrectomy] |
| Notes | Principal Investigator: Gregory M Fox, MD. Contacted: Lead author clarified that they are unlikely to have any data relevant to this review and will probably not go on to publish data from this trial |
NCT00931125.
| Study name | Randomized, double blinded, controlled, two‐center study assessing the safety and efficacy of intravitreal ranibizumab as a preoperative adjunct treatment before vitrectomy surgery in proliferative diabetic retinopathy (PDR) compared to vitrectomy alone |
| Methods | Randomised, double‐masked, controlled trial |
| Participants | Active, not recruiting Estimate 70 |
| Interventions | This is a randomised, double‐masked, controlled, 2‐centre study assessing the feasibility, efficacy and safety of intravitreal ranibizumab injection applied as a preoperative adjunct treatment before vitrectomy surgery in severe PDR. Comparator arm consists of participants receiving standard vitrectomy alone with sham intravitreal injection preoperatively. |
| Outcomes | Primary outcome measures:
Secondary outcome measures:
|
| Starting date | March 2009 Estimated study completion date: December 2013 |
| Contact information | University of Debrecen, Medical and Health Science Center, Faculty of Medicine, Department of Ophthalmology |
| Notes | Debrecen, Hungary, H‐4012 |
NCT01091896.
| Study name | Adjuvant intravitreal bevacizumab in pars plana vitrectomy for vitreous hemorrhage secondary to diabetic retinopathy |
| Methods | Randomised, single‐masked, controlled trial |
| Participants | Not stated |
| Interventions | No intervention: 1 ‐ no bevacizumab. Participants will neither receive bevacizumab before nor during vitrectomy Experimental: 2 ‐ bevacizumab before vitrectomy. Participants will receive intravitreal injection of 1.25 mg of bevacizumab (0.05 mL) 7 days before vitrectomy Experimental: 3 ‐ bevacizumab after vitrectomy. Participants will receive intravitreal injection of 1.25 mg of bevacizumab (0.05 mL) at the end of vitrectomy |
| Outcomes | Primary outcome measure: recurrent vitreous haemorrhage incidence after vitrectomy Secondary outcome measure: visual outcome |
| Starting date | 2010 Estimated study completion date: March 2011 |
| Contact information | felipeppalmeida@yahoo.com.br [mailto:felipeppalmeida%40yahoo.com.br?subject=NCT01091896, IBEViH, Adjuvant Intravitreal Bevacizumab in Pars Plana Vitrectomy for Vitreous Hemorrhage] |
| Notes | Principal Investigator: Felipe Almeida |
NCT01151722.
| Study name | Adjuvant intravitreal bevacizumab in pars plana vitrectomy for diabetic vitreous hemorrhage (ABeVi) |
| Methods | Randomised, single‐masked, controlled trial |
| Participants | Not stated |
| Interventions | No intervention: no injection, no bevacizumab Experimental 2: bevacizumab before vitrectomy Experimental 3: bevacizumab after vitrectomy |
| Outcomes | Primary outcome measure: vitreous haemorrhage recurrence (time frame: 3 months) |
| Starting date | 2009 Estimated study completion date: December 2009 |
| Contact information | felipeppalmeida@yahoo.com.br [mailto:felipeppalmeida%40yahoo.com.br?subject=NCT01151722, HCRP22, Adjuvant Intravitreal Bevacizumab in Pars Plana Vitrectomy for Diabetic Vitreous Hemorrhage] |
| Notes | Principal Investigator: Felipe Almeida, MD |
NCT01306981.
| Study name | A prospective, randomised controlled trial of ranibizumab pre‐treatment in diabetic vitrectomy ‐ a pilot study |
| Methods | Randomised, double‐masked, controlled study |
| Participants | Not stated |
| Interventions | Participants will be randomised 1:1 to receive either ranibizumab intravitreal injection (0.5 mg in 0.05 mL) or saline subconjunctival injection at the time of surgery |
| Outcomes | Primary outcome measures: BCVA (time frame: 12 weeks postoperative) Secondary outcome measures:
|
| Starting date | 2011 Estimated study completion date: March 2013 |
| Contact information | Moorfields Eye Hospital NHS Foundation Trust |
| Notes | Principal Investigator: Mr James W Bainbridge MA, PhD, FRCOphth. Contacted: Currently the study is in the write‐up stages. Unpublished data on the rate of POVCH are as follows: Vitreous cavity haemorrhage occurred in 4/15 in the ranibizumab (Lucentis®) arm and 6/15 in the control arm At 12‐weeks postoperative persistent vitreous cavity haemorrhage was observed in 0/15 in the ranibizumab arm and 2/15 in the control arm |
BCVA: best‐corrected visual acuity ETDRS: Early Treatment Diabetic Retinopathy Study PDR: proliferative diabetic retinopathy TRD: tractional retinal detachment VEGF: vascular endothelial growth factor
Differences between protocol and review
Due to the importance of postoperative retinal detachment, we included an additional analysis to enable patients and surgeons to make a more informed choice when deciding to use intravitreal bevacizumab as an adjunct to vitrectomy.
Our protocol specified that we would exclude participants who received silicone oil endotamponade in the review analysis. Peer review comments on our review questioned whether this would give rise to bias, so we presented analyses of all participants and sensitivity analyses excluding silicone oil cases. These additional analyses were not originally planned within the protocol.
Our protocol specified that we would present odds ratios or risk ratios. We have chosen to present risk ratios as they are easier to interpret.
For the 2023 update, in response to a request from the Cochrane Eyes and Vision (CEV) editorial base, we changed the title of the review from "Anti‐vascular endothelial growth factor for prevention of postoperative vitreous cavity haemorrhage after vitrectomy for proliferative diabetic retinopathy" to "Anti‐vascular endothelial growth factor in combination with vitrectomy for the treatment of complications of proliferative diabetic retinopathy". The CEV editors had noted overlap between the current review and another CEV review "Anti‐vascular endothelial growth factor for proliferative diabetic retinopathy". After discussion with the review author teams of both reviews, it was agreed to modify the PICO framework for each updated review to ensure that relevant indications and outcomes were covered, but with no overlap between the two reviews. We also updated the outcomes following updated guidance from the Cochrane Handbook for Systematic Reviews of Interventions (Higgins 2021).
Contributions of authors
For the 2023 update:
JS, ND, PD, DS
Co‐ordinating the review
Screening search results
Data management
Screening retrieved papers against inclusion criteria
Appraising quality of papers
Abstracting data from papers
Analysis of data
Interpretation of data
Entering data into RevMan
Writing the review
Updating the review
Sources of support
Internal sources
No sources of support provided
External sources
-
Public Health Agency, UK
This review update was supported by the HSC Research and Development (R&D) Division of the Public Health Agency, which funds the Cochrane Eyes and Vision editorial base at Queen's University Belfast.
Declarations of interest
For the 2021 update (taken from CoI forms completed on 24 March 2021):
JS: No conflicts to declare ND: No conflicts to declare PD: No conflicts to declare DS: No conflicts to declare
New search for studies and content updated (no change to conclusions)
References
References to studies included in this review
Ahmadieh 2009 {published data only}
- Ahmadieh H, Shoeibi N, Entezari M, Monshizadeh R. Intravitreal bevacizumab for prevention of early postvitrectomy hemorrhage in diabetic patients: a randomized clinical trial. Ophthalmology 2009;116(10):1943-8. [DOI] [PubMed] [Google Scholar]
Ahn 2011 {published data only}
- Ahn J, Woo SJ, Chung H, Park KH. The effect of adjunctive intravitreal bevacizumab for preventing postvitrectomy hemorrhage in proliferative diabetic retinopathy. Ophthalmology 2011;118(11):2218-26. [DOI] [PubMed] [Google Scholar]
Aleman 2019 {published data only}
- Aleman I, Castillo Velazquez J, Rush SW, Rush RB. Ziv-aflibercept versus bevacizumab administration prior to diabetic vitrectomy: a randomised and controlled trial. British Journal of Ophthalmology 2019;103(12):1740-6. [DOI] [PubMed] [Google Scholar]
Arevalo 2019 {published data only}
- Arevalo JF, Lasave AF, Kozak I, Al Rashaed S, Al Kahtani E, Maia M, et al. Preoperative bevacizumab for tractional retinal detachment in proliferative diabetic retinopathy: a prospective randomized clinical trial. American Journal of Ophthalmology 2019;207:279-87. [DOI] [PubMed] [Google Scholar]
Comyn 2017 {published data only}
- Comyn O, Wickham L, Charteris DG, Sullivan PM, Ezra E, Gregor Z, et al. Ranibizumab pretreatment in diabetic vitrectomy: a pilot randomised controlled trial (the RaDiVit study). Eye 2017;31:1253-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
Cui 2018 {published data only}
- Cui J, Chen H, Lu H, Dong F, Wei D, Jiao Y, e al. Efficacy and safety of intravitreal conbercept, ranibizumab, and triamcinolone on 23-gauge vitrectomy for patients with proliferative diabetic retinopathy. Journal of Ophthalmology 2018;2018:4927259. [DOI: 10.1155/2018/4927259] [DOI] [PMC free article] [PubMed] [Google Scholar]
di Lauro 2009 {published data only}
- di Lauro R, De Ruggiero P, di Lauro R, di Lauro MT, Romano MR. Intravitreal bevacizumab for the surgical treatment of severe proliferative retinopathy. Graefes Archive for Clinical and Experimental Ophthalmology 2010;248(6):785-91. [DOI] [PubMed] [Google Scholar]
Dong 2019 {published data only}
- Dong X. Effect of ranibizumab on the efficacy of vitrectomy in patients with PDR. International Eye Science 2019;19(5):809-12. [Google Scholar]
El Batarny 2008 {published data only}
- El Batarny AM. Intravitreal bevacizumab as an adjunctive therapy before diabetic vitrectomy. Clinical Ophthalmology 2008;2(4):709-16. [PMC free article] [PubMed] [Google Scholar]
Farahvash 2011 {published data only}
- Farahvash MS, Majidi AR, Roohipoor R, Ghassemi F. Preoperative injection of intravitreal bevacizumab in dense diabetic vitreous hemorrhage. Retina 2011;31(7):1254-60. [DOI] [PubMed] [Google Scholar]
Ferraz 2013 {published data only}
- Ferraz AJ, Morita C, Preti RC, Nascimento VP, Maia Junior OO, Carvalho de Barros A, et al. Use of intravitreal bevacizumab or triamcinolone acetonide as a preoperative adjunct to vitrectomy for vitreous haemorrhage in diabetics. Revista Brasileira de Oftalmologia 2013;72(1):12-6. [Google Scholar]
Hernández‐Da Mota 2010 {published data only}
- Hernández-Da Mota SE, Nuñez-Solorio SM. Experience with intravitreal bevacizumab as a preoperative adjunct in 23-G vitrectomy for advanced proliferative diabetic retinopathy. European Journal of Ophthalmology 2010;20(6):1047-52. [DOI] [PubMed] [Google Scholar]
Hu 2019 {published data only}
- Hu HT, Sun T, Wang H, Wu HX, Hao LX. Effect of ranibizumab injection on the surgical outcome and complications of PDR patients before PPV. International Eye Science 2019;19(5):817-20. [Google Scholar]
Jiang 2020 {published data only}
- Jiang T, Gu J, Zhang P, Chen W, Chang Q. The effect of adjunctive intravitreal conbercept at the end of diabetic vitrectomy for the prevention of post-vitrectomy hemorrhage in patients with severe proliferative diabetic retinopathy: a prospective, randomized pilot study. BMC Ophthalmology 2020;20(1):43. [DOI] [PMC free article] [PubMed] [Google Scholar]
Li 2022 {published data only}
- Li S, Yang Y, Zou J, Zeng J, Ding C. The efficacy and safety of intravitreal injection of Ranibizumab as pre‑treatment for vitrectomy in proliferative diabetic retinopathy with vitreous hemorrhage. BMC Ophthalmology 2022;22(1):63. [DOI] [PMC free article] [PubMed] [Google Scholar]
Manabe 2015 {published data only}
- Manabe A, Shimada H, Hattori T, Nakashizuka H, Yuzawa M. Randomized controlled study of intravitreal bevacizumab 0.16 mg injected one day before surgery for proliferative diabetic retinopathy. Retina 2015;35(9):1800-7. [DOI] [PubMed] [Google Scholar]
Modarres 2009 {published data only}
- Modarres M, Nazari H, Falavarjani KG, Naseripour M, Hashemi M, Parvaresh MM. Intravitreal injection of bevacizumab before vitrectomy for proliferative diabetic retinopathy. European Journal of Ophthalmology 2009;19(5):848-52. [DOI] [PubMed] [Google Scholar]
Ou 2021 {published data only}
- Ou Z, Wang Q, Jiang J, Liu X. Intravitreal injection of Conbercept combined with PPV in the treatment of proliferative diabetic retinopathy. International Eye Science 2021;21(6):986-90. [Google Scholar]
Pakzad Vaezi 2014 {published data only}
- Pakzad-Vaezi K, Albiani DA, Kirker AW, Merkur AB, Kertes PJ, Eng KT, et al. A randomized study comparing the efficacy of bevacizumab and ranibizumab as pre-treatment for pars plana vitrectomy in proliferative diabetic retinopathy. Ophthalmic Surgery, Lasers and Imaging Retina 2014;45(6):521-4. [DOI] [PubMed] [Google Scholar]
Ren 2019 {published data only}
- Ren X, Bu S, Zhang X, Jiang Y, Tan L, Zhang H, et al. Safety and efficacy of intravitreal conbercept injection after vitrectomy for the treatment of proliferative diabetic retinopathy. Eye 2019;33(7):1177-83. [DOI] [PMC free article] [PubMed] [Google Scholar]
Rizzo 2008 {published data only}
- Rizzo S, Genovesi-Ebert F, Di Bartolo E, Vento A, Miniaci S, Williams G. Injection of intravitreal bevacizumab (Avastin) as a preoperative adjunct before vitrectomy surgery in the treatment of severe proliferative diabetic retinopathy (PDR). Graefe's Archive for Clinical and Experimental Ophthalmology 2008;246(6):837-42. [DOI] [PubMed] [Google Scholar]
Sohn 2012 {published data only}
- Sohn EH, He S, Kim LA, Salehi-Had H, Javaheri M, Spee C, et al. Angiofibrotic response to vascular endothelial growth factor inhibition in diabetic retinal detachment: report no. 1. Archives of Ophthalmology 2012;130(9):1127-34. [DOI] [PMC free article] [PubMed] [Google Scholar]
Su 2016 {published data only}
- Su L, Ren X, Wei H, Zhao L, Zhang X, Liu J, et al. Intravitreal conbercept (KH902) for surgical treatment of severe proliferative diabetic retinopathy. Retina 2016;36(5):938-43. [DOI] [PubMed] [Google Scholar]
Wildan 2019 {published data only}
- Wildan A, Winarto, Kristina TN. Aflibercept and bevacizumab injection effects on visual acuity of post vitrectomy diabetic retinopathy. Pakistan Journal of Medical and Health Sciences 2019;13(4):1214-8. [Google Scholar]
Yang 2016 {published data only}
- Yang X, Xu J, Wang R, Mei Y, Lei H, Liu J, et al. A randomized controlled trial of conbercept pretreatment before vitrectomy in proliferative diabetic retinopathy. Journal of Ophthalmology 2016;2016:2473234. [DOI: 10.1155/2016/2473234] [DOI] [PMC free article] [PubMed] [Google Scholar]
Yu 2015 {published data only}
- Yu XQ, Cao GP, Tang MX. Effect of vitrectomy combined medication hyperplastic on patients with diabetic retinopathy. International Eye Science 2015;15(8):1402-4. [Google Scholar]
Zaman 2013 {published data only}
- Zaman Y, Rehman A, Memon AF. Intravitreal Avastin as an adjunct in patients with proliferative diabetic retinopathy undergoing pars plana vitrectomy. Pakistan Journal of Medical Science 2013;29(2):590-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
Zhou 2017 {published data only}
- Zhou YM, Lu YL, Huang JH. Clinical effect of 25G+ vitrectomy combined with intravitreal injection of conbercept in the treatment of severe proliferative diabetic retinopathy. International Eye Science 2017;17(12):2321-4. [Google Scholar]
References to studies excluded from this review
Abd 2020 {published data only}
- Abd Elhamid AH, Mohamed AAEA, Khattab AM. Intravitreal aflibercept injection with panretinal photocoagulation versus early vitrectomy for diabetic vitreous hemorrhage: randomized clinical trial. BMC Ophthalmology 2020;20(1):130. [DOI] [PMC free article] [PubMed] [Google Scholar]
Abdelhakim 2011 {published data only}
- Abdelhakim MA, Macky TA, Mansour KA, Mortada HA. Bevacizumab (Avastin) as an adjunct to vitrectomy in the management of severe proliferative diabetic retinopathy: a prospective case series. Ophthalmic Research 2011;45(1):23-30. [DOI] [PubMed] [Google Scholar]
Albuquerque 2014 {published data only}
- Albuquerque TL, Pierozzi GS, Araujo AC, Neto NH, Carregal TB, Martins MC. Comparative, randomized, double blinded study of the use of anti-VEGF in patients with vitreous hemorrhage or tractional retinal detachment secondary to diabetic retinopathy. Investigative Ophthalmology and Visual Science 2014;55(13):ARVO E-abstract 4391. [Google Scholar]
Antoszyk 2020 {published data only}
- Antoszyk AN, Glassman AR, Beaulieu WT, Jampol LM, Jhaveri CD, Punjabi OS, et al. Effect of intravitreous aflibercept vs vitrectomy with panretinal photocoagulation on visual acuity in patients with vitreous hemorrhage from proliferative diabetic retinopathy: a randomized clinical trial. JAMA 2020;324(23):2383-95. [DOI] [PMC free article] [PubMed] [Google Scholar]
Antoszyk 2021 {published data only}
- Antoszyk AN. Initial aflibercept versus vitrectomy with panretinal photocoagulation for vitreous hemorrhage (VH) from proliferative diabetic retinopathy (PDR): a DRCR retina network randomized clinical trial. Investigative Ophthalmology and Visual Science 2021;62(8):ARVO E-abstract 1113. [Google Scholar]
Berk Ergun 2014 {published data only}
- Berk Ergun S, Toklu Y, Cakmak HB, Raza S, Simsek S. The effect of intravitreal bevacizumab as a pretreatment of vitrectomy for diabetic vitreous hemorrhage on recurrent hemorrhage. Seminars in Ophthalmology 2015;30(3):177-80. [DOI] [PubMed] [Google Scholar]
Bhavsar 2014 {published data only}
- Bhavsar AR, Torres K, Glassman AR, Jampol LM, Kinyoun JL, Diabetic Retinopathy Clinical Research Network. Evaluation of results 1 year following short-term use of ranibizumab for vitreous hemorrhage due to proliferative diabetic retinopathy. JAMA Ophthalmology 2014;132(7):889-90. [DOI] [PMC free article] [PubMed] [Google Scholar]
Castillo 2017 {published data only}
- Castillo J, Aleman I, Rush SW, Rush RB. Preoperative bevacizumab administration in proliferative diabetic retinopathy patients undergoing vitrectomy: a randomized and controlled trial comparing interval variation. American Journal of Ophthalmology 2017;183:1-10. [DOI] [PubMed] [Google Scholar]
Castillo 2018 {published data only}
- Castillo Velazquez J, Aleman I, Rush SW, Rush RB. Bevacizumab before diabetic vitrectomy: a clinical trial assessing 3 dosing amounts. Ophthalmology Retina 2018;2(10):1010-20. [DOI] [PubMed] [Google Scholar]
Chakraborty 2021 {published data only}
- Chakraborty D, Maiti A, Kelkar A, Sengupta S, Roy S, Bolisetty M, et al. Outcomes of preoperative bevacizumab in diabetics with nonclearing vitreous hemorrhage without tractional detachment - a quasi-randomized retrospective study. Indian Journal of Ophthalmology 2021;69(11):3283-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
Chatziralli 2020 {published data only}
- Chatziralli I, Dimitriou E, Theodossiadis G, Bourouki E, Bagli E, Kitsos G, et al. Intravitreal ranibizumab versus vitrectomy for recurrent vitreous haemorrhage after pars plana vitrectomy for proliferative diabetic retinopathy: a prospective study. International Ophthalmology 2020;40(4):841-7. [DOI] [PubMed] [Google Scholar]
Cheema 2010 {published data only}
- Cheema RA, Mushtaq J, Al-Khars W, Al-Askar E, Cheema MA. Role of intravitreal bevacizumab (Avastin) injected at the end of diabetic vitrectomy in preventing postoperative recurrent vitreous hemorrhage. Retina 2010;30(10):1646-50. [DOI] [PubMed] [Google Scholar]
Chelala 2018 {published data only}
- Chelala E, Nehme J, El Rami H, Aoun R, Dirani A, Fadlallah A, et al. Efficacy of intravitreal ranibizumab injections in the treatment of vitreous hemorrhage related to proliferative diabetic retinopathy. Retina 2018;38(6):1127-33. [DOI] [PubMed] [Google Scholar]
Chen 2020 {published data only}
- Chen HJ, Wang CG, Dou HL, Feng XF, Xu YM, Ma ZZ. Effect of intravitreal ranibizumab pretreatment on vitrectomy in young patients with proliferative diabetic retinopathy. Annals of Palliative Medicine 2020;9(1):82-9. [DOI] [PubMed] [Google Scholar]
Comyn 2019 {published data only}
- Comyn O, Lange C, Bainbridge JW. Vitreous and plasma cytokine levels in subjects with advanced proliferative diabetic retinopathy in the Ranibizumab in Diabetic Vitrectomy (RaDiVit) Study. Investigative Ophthalmology and Visual Science 2019;60(9):ARVO E-abstract 5362. [Google Scholar]
da R Lucena 2009 {published data only}
- da R Lucena D, Ribeiro JA, Costa RA, Barbosa JC, Scott IU, Figueiredo-Pontes LL, et al. Intraoperative bleeding during vitrectomy for diabetic tractional retinal detachment with versus without preoperative intravitreal bevacizumab (IBeTra study). British Journal of Ophthalmology 2009;93(5):688-91. [DOI] [PubMed] [Google Scholar]
Demir 2013 {published data only}
- Demir M, Oba E, Can E, Kara O, Cinar S. Effect of bevacizumab injection before vitrectomy on intravitreal hemorrhage in pseudophakic patients with proliferative diabetic retinopathy. Ophthalmology and Eye Diseases 2013;5:11-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
Dirani 2014 {published data only}
- Dirani A, Fadlallah A, Azar G, Chelala E, Nehme J, Alameddine R, et al. Intravitreal ranibizumab for vitreous hemorrhage in proliferative diabetic retinopathy. Investigative Ophthalmology and Visual Science 2014;55(13):ARVO E-abstract 4395. [Google Scholar]
Doganay 2010 {published data only}
- Doganay S, Koc B, Cankaya C, Duz C, Bilak S. The effect on surgical success of intravitreal bevacizumab given before pars plana vitrectomy in diabetic patients [Diyabetik olgularda pars plana vitrektomiden once uygulanan intravitreal bevacizumabın cerrahi başarıya etkisi]. Retina-Vitreus 2010;18(4):310-3. [Google Scholar]
Elwan 2013 {published data only}
Feng 2018 {published data only}
- Feng J, Li B, Wen J, Jiang Y. Preoperative timing of intravitreal bevacizumab injection for proliferative diabetic retinopathy patients. Ophthalmic Research 2018;60(4):250-7. [DOI] [PubMed] [Google Scholar]
Forooghian 2016 {published data only}
- Forooghian F, Kertes PJ, Eng KT, Albiani DA, Kirker AW, Merkur AB, et al. Alterations in intraocular cytokine levels following intravitreal ranibizumab. Canadian Journal of Ophthalmology 2016;51(2):87-90. [DOI] [PubMed] [Google Scholar]
Gao 2020 {published data only}
- Gao S, Lin Z, Chen Y, Xu J, Zhang Q, Chen J, et al. Intravitreal conbercept injection as an adjuvant in vitrectomy with silicone oil infusion for severe proliferative diabetic retinopathy. Journal of Ocular Pharmacology and Therapeutics 2020;36(5):304-10. [DOI] [PubMed] [Google Scholar]
Goncu 2014 {published data only}
- Goncu T, Ozdek S, Unlu M. The role of intraoperative bevacizumab for prevention of postoperative vitreous hemorrhage in diabetic vitreous hemorrhage. European Journal of Ophthalmology 2014;24(1):88-93. [DOI] [PubMed] [Google Scholar]
Gupta 2008 {published data only}
- Gupta A, Gupta V, Gupta P, Dogra M. Preoperative intravitreal bevacizumab improves visual outcome in diabetic vitreous surgery. American Academy of Ophthalmology 2008:252. [Google Scholar]
Gupta 2012a {published data only}
- Gupta B, Sivaprasad S, Wong R, Laidlaw A, Jackson TL, McHugh D, et al. Visual and anatomical outcomes following vitrectomy for complications of diabetic retinopathy: the DRIVE UK study. Eye 2012;26(4):510-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
Gupta 2012b {published data only}
- Gupta A, Bansal R, Gupta V, Dogra MR. Six-month visual outcome after pars plana vitrectomy in proliferative diabetic retinopathy with or without a single preoperative injection of intravitreal bevacizumab. International Ophthalmology 2012;32(2):135-44. [DOI] [PubMed] [Google Scholar]
Haseeb 2019 {published data only}
- Haseeb U, Aziz-Ur-Rehman, Haseeb M. Visual outcomes of pars plana vitrectomy alone or with intravitreal bevacizumab in patients of diabetic vitreous haemorrhage. Journal of the College of Physicians and Surgeons - Pakistan 2019;29(8):728-31. [DOI] [PubMed] [Google Scholar]
Hu 2021 {published data only}
- Hu L, Chen Q, Du Z, Wang W, Zhao G. Evaluation of vitrectomy combined preoperative intravitreal ranibizumab and postoperative intravitreal triamcinolone acetonide for proliferative diabetic retinopathy. International Ophthalmology 2021;41(5):1635-42. [DOI] [PubMed] [Google Scholar]
Hu 2022 {published data only}
- Hu Z, Cao X, Chen L, Su Y, Ji J, Yuan S, et al. Monitoring intraocular proangiogenic and profibrotic cytokines within 7 days after adjunctive anti-vascular endothelial growth factor therapy for proliferative diabetic retinopathy. Acta Ophthalmologica 2022;100(3):e726-36. [DOI] [PubMed] [Google Scholar]
Ishikawa 2009 {published data only}
- Ishikawa K, Honda S, Tsukahara Y, Negi A. Preferable use of intravitreal bevacizumab as a pretreatment of vitrectomy for severe proliferative diabetic retinopathy. Eye 2009;23(1):108-11. [DOI] [PubMed] [Google Scholar]
Jiao 2014 {published data only}
- Jiao C, Spee C, He S, Mullins R, Eliott D, Hinton DR, et al. Angiofibrotic response to bevacizumab on fibrovascular membranes in proliferative diabetic retinopathy. Investigative Ophthalmology and Visual Science 2014;55(13):ARVO E-abstract 5821. [Google Scholar]
Jin‐An 2014 {published data only}
- Jin-An X, Qing-Yu B, An-Ming X. Changes of cytokines in the aqueous humor following avastin intravitreous injection. Chinese Journal of Tissue Engineering Research 2014;18(42):6805-10. [Google Scholar]
Jirawison 2012 {published data only}
- Jirawison C, Ittipunkul N. Intravitreal bevacizumab at the end of diabetic vitrectomy for prevention of postoperative vitreous hemorrhage: a comparative study. Journal of the Medical Association of Thailand 2012;95(Suppl 4):S136-42. [PubMed] [Google Scholar]
Jorge 2021 {published data only}
- Jorge DM, Tavares Neto JEDS, Poli-Neto OB, Scott IU, Jorge R. Intravitreal bevacizumab (IVB) versus IVB in combination with pars plana vitrectomy for vitreous hemorrhage secondary to proliferative diabetic retinopathy: a randomized clinical trial. International Journal of Retina and Vitreous 2021;7(1):35. [DOI] [PMC free article] [PubMed] [Google Scholar]
Karimov 2021 {published data only}
- Karimov M, Akhundova L. Anti-vascular endothelial growth factor therapy as an adjunct to diabetic vitrectomy. Open Ophthalmology Journal 2021;15(1):137-43. [Google Scholar]
Kasetty 2021 {published data only}
- Kasetty VM, Marcus DM, Singh H, Frazier H, Starnes D. Complications, compliance and 3-year outcomes after endolaserless vitrectomy with aflibercept monotherapy for PDR-related vitreous hemorrhage. Investigative Ophthalmology and Visual Science 2021;62(8):ARVO E-abstract 1119. [Google Scholar]
Kawano 2013 {published data only}
- Kawano S, Yamashita T, Sonoda Y, Yamakiri K, Sakamoto T. Post-operative hemorrhage after vitrectomy for proliferative diabetic retinopathy with or without pre-surgical intravitreal bevacizumab. Investigative Ophthalmology and Visual Science 2013;54(15):ARVO E-abstract 216. [Google Scholar]
Leonard 2014 {published data only}
- Leonard RE, Shah VA. Intravitreal aflibercept as a surgical adjuvant in severe proliferative diabetic retinopathy. Investigative Ophthalmology and Visual Science 2014;55(13):ARVO E-abstract 4401. [Google Scholar]
Li 2010 {published data only}
- Li CR, Sun SG, Hong W. Effect of intravitreal bevacizumab injection before vitrectomy on proliferative diabetic retinopathy. International Journal of Ophthalmology 2010;3(3):261-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
Li 2015 {published data only}
- Li JK, Wei F, Jin XH, Dai YM, Cui HS, Li YM. Changes in vitreous VEGF, bFGF and fibrosis in proliferative diabetic retinopathy after intravitreal bevacizumab. International Journal of Ophthalmology 2015;8(6):1202-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
Li 2016 {published data only}
- Li S, Yang Y, Zou J, Zeng J, Ding C. Effect of ranibizumab intravitreal injection before 23G-vitrectomy surgery in the treatment of patients with proliferative diabetic retinopathy. International Eye Science 2016;16(10):1959-61. [Google Scholar]
Li 2020 {published data only}
- Li B, Li MD, Ye JJ, Chen Z, Guo ZJ, Di Y. Vascular endothelial growth factor concentration in vitreous humor of patients with severe proliferative diabetic retinopathy after intravitreal injection of conbercept as an adjunctive therapy for vitrectomy. Chinese Medical Journal 2020;133(6):664-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
Liu 2019 {published data only}
- Liu Q, Xie P, Yuan S, Hu Z. Day regimes of CONbercept on cytokinEs of PDR patients undergoing vitrectomy trial (CONCEPT): effects of preoperative intravitreal conbercept on cytokines in the vitreous with proliferative diabetic retinopathy. Investigative Ophthalmology and Visual Science 2019;60(9):ARVO E-abstract 5372. [Google Scholar]
Lo 2009 {published data only}
- Lo WR, Kim SJ, Aaberg TM Sr, Bergstrom C, Srivastava SK, Yan J, et al. Visual outcomes and incidence of recurrent vitreous hemorrhage after vitrectomy in diabetic eyes pretreated with bevacizumab (Avastin). Retina 2009;29(7):926-31. [DOI] [PMC free article] [PubMed] [Google Scholar]
Ma 2016 {published data only}
- Ma YC, Luo XQ, Ding RX. Clinical effect of intravitreal injection of ranibizumab for severe proliferative diabetic retinopathy. International Eye Science 2016;16(1):111-3. [Google Scholar]
Marcus 2017 {published data only}
- Marcus DM, Singh H, Farooq A, Starnes D, Walia H. Endolaserless vitrectomy with intravitreal aflibercept injection (IAI) for proliferative diabetic retinopathy (PDR)-related vitreous hemorrhage (LASER LESS TRIAL). Investigative Ophthalmology and Visual Science 2017;58(8):ARVO E-abstract 5036. [Google Scholar]
Meng 2016 {published data only}
- Meng N, Ren BC. Effect of intravitreal injection of bevacizumab for vitreous hemorrhage in patients with proliferative diabetic retinopathy. International Eye Science 2016;16(5):972-4. [Google Scholar]
NCT01589718 {unpublished data only}
- NCT01589718. A phase III randomized 1:1, masked, study of the safety, tolerability, and efficacy of intravitreal pre-op 0.3mg pegaptanib sodium versus sham, for adjuvant management of TRD and vit hem associated with PDR. clinicaltrials.gov/show/NCT01589718 (first received 2 May 2012).
Oshima 2009 {published data only}
- Oshima Y, Shima C, Wakabayashi T, Kusaka S, Shiraga F, Ohji M, et al. Microincision vitrectomy surgery and intravitreal bevacizumab as a surgical adjunct to treat diabetic traction retinal detachment. Ophthalmology 2009;116(5):927-38. [DOI] [PubMed] [Google Scholar]
Ozer 2022 {published data only}
- Ozer F, Tokuc EO, Albayrak MG, Akpinar G, Kasap M, Karabas VL. Comparison of before versus after intravitreal bevacizumab injection, growth factor levels and fibrotic markers in vitreous samples from patients with proliferative diabetic retinopathy. Graefes Archive for Clinical and Experimental Ophthalmology 2022;260(6):1899-906. [DOI] [PubMed] [Google Scholar]
Papavasileiou 2017 {published data only}
- Papavasileiou E, Vasalaki M, Garnavou-Xirou C, Velissaris S, Zygoura V, McHugh D, et al. Vitrectomy with fibrovascular membrane delamination for proliferative diabetic retinopathy with or without preoperative Avastin. Hellenic Journal of Nuclear Medicine 2017;20(Suppl):161. [DOI: 10.1111/j.1755-3768.2017.02313] [DOI] [PubMed] [Google Scholar]
Park 2010 {published data only}
- Park DH, Shin JP, Kim SY. Intravitreal injection of bevacizumab and triamcinolone acetonide at the end of vitrectomy for diabetic vitreous hemorrhage: a comparative study. Graefes Archive for Clinical and Experimental Ophthalmology 2010;248(5):641-50. [DOI] [PubMed] [Google Scholar]
Park 2021 {published data only}
- Park YJ, Ahn J, Kim TW, Park SJ, Joo K, Park KH, et al. Efficacy of bevacizumab for vitreous haemorrhage in proliferative diabetic retinopathy with prior complete panretinal photocoagulation. Eye 2021;35(11):3056-63. [DOI] [PMC free article] [PubMed] [Google Scholar]
Pokroy 2011 {published data only}
- Pokroy R, Desai UR, Du E, Li Y, Edwards P. Bevacizumab prior to vitrectomy for diabetic traction retinal detachment. Eye 2011;28(8):989-97. [DOI] [PMC free article] [PubMed] [Google Scholar]
Romano 2009a {published data only}
- Romano MR, Gibran SK, Marticorena J, Wong D, Heimann H. Can a preoperative bevacizumab injection prevent recurrent postvitrectomy diabetic vitreous haemorrhage? Eye 2009;23(8):1698-701. [DOI] [PubMed] [Google Scholar]
Romano 2009b {published data only}
- Romano MR, Gibran SK, Marticorena J, Wong D. Can an intraoperative bevacizumab injection prevent recurrent postvitrectomy diabetic vitreous hemorrhage? European Journal of Ophthalmology 2009;19(4):618-21. [DOI] [PubMed] [Google Scholar]
Sato 2013 {published data only}
- Sato T, Morita S, Bando H, Sato S, Ikeda T, Emi K. Early vitreous hemorrhage after vitrectomy with preoperative intravitreal bevacizumab for proliferative diabetic retinopathy. Middle East African Journal of Ophthalmology 2013;20(1):51-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
Shi 2020 {published data only}
- Shi SH, Xu F, Li M. Clinical study of conbercept in patients with proliferative diabetic retinopathy undergoing vitrectomy. International Eye Science 2020;20(5):852-5. [Google Scholar]
Starnes 2019 {published data only}
- Starnes DC, Lalane R, Walia H, Farooq A, Frazier H, Marcus W, et al. Endolaserless vitrectomy with intravitreal aflibercept injection (IAI) for proliferative diabetic retinopathy (PDR)-related vitreous hemorrhage: LASER LESS TRIAL 1-year results. Investigative Ophthalmology and Visual Science 2019;60(9):ARVO E-abstract 6559. [Google Scholar]
Sun 2017 {published data only}
- Sun L, Tao Y. Effects of Bevacizumab on CTGF and PEDF in proliferative membrane in patients with PDR. International Eye Science 2017;17(6):1051-4. [Google Scholar]
Sun 2022 {published data only}
- Sun H, Zou W, Zhang Z, Huang D, Zhao J, Qin B, et al. Vitreous inflammatory cytokines and chemokines, not altered after preoperative adjunctive conbercept injection, but associated with early postoperative macular edema in patients with proliferative diabetic retinopathy. Frontiers in Physiology 2022;13:846003. [DOI] [PMC free article] [PubMed] [Google Scholar]
Tsubota 2019 {published data only}
- Tsubota K, Usui Y, Wakabayashi Y, Suzuki J, Ueda S, Goto H. Effectiveness of prophylactic intravitreal bevacizumab injection to proliferative diabetic retinopathy patients with elevated preoperative intraocular VEGF in preventing complications after vitrectomy. Clinical Ophthalmology 2019;13:1063-70. [DOI] [PMC free article] [PubMed] [Google Scholar]
Turkseven Kumral 2021 {published data only}
- Turkseven Kumral E, Ercalik NY. Intravitreal ranibizumab versus aflibercept for diabetic macular edema in vitrectomized eyes: 12 month results. Seminars in Ophthalmology 2021;36(8):723-7. [DOI] [PubMed] [Google Scholar]
Victor 2014 {published data only}
- Victor AA, Gondhowiardjo TD, Waspadji S, Wanandi SI, Bachtiar A, Suyatna FD, et al. Effect of laser photocoagulation and bevacizumab intravitreal in proliferative diabetic retinopathy: review on biomarkers of oxidative stress. Medical Journal of Indonesia 2014;23(2):79-86. [Google Scholar]
Vidinova 2020 {published data only}
- Vidinova CN, Gouguchkova PT, Dimitrov T, Vidinov KN, Nocheva H. Comparative clinical and ultrastructural analysis of the results from ranibizumab and aflibercept in patients with PDR [Ultrastruktureller und klinischer Vergleich des Ergebnisses bei PDR-Patienten, behandelt mit Ranibizumab oder Aflibercept – von Grundlagenforschungen zu den klinischen Therapien]. Klinische Monatsblatter fur Augenheilkunde 2020;237(1):79-84. [DOI] [PubMed] [Google Scholar]
Wang 2019 {published data only}
- Wang J, Gao X, Liu J, Wang J, Zhang Y, Zhang T, et al. Effect of intravitreal conbercept treatment on the expression of long noncoding RNAs and mRNAs in proliferative diabetic retinopathy patients. Acta Opthalmologica 2019;97(6):e902-12. [DOI] [PubMed] [Google Scholar]
Wang 2020 {published data only}
- Wang XT, Li SY, Fan W, Li J, Feng RF, Zhang ZP, et al. Changes of vitreous cytokine levels in eyes with PDR after intravitreal injection of ranibizumab or triamcinolone acetonide. International Eye Science 2020;20(7):1158-63. [Google Scholar]
Yang 2008 {published data only}
- Yang CM, Yeh PT, Yang CH, Chen MS. Bevacizumab pretreatment and long-acting gas infusion on vitreous clear-up after diabetic vitrectomy. American Journal of Ophthalmology 2008;146(2):211-7. [DOI] [PubMed] [Google Scholar]
Yeh 2009 {published data only}
- Yeh PT, Yang CM, Lin YC, Chen MS, Yang CH. Bevacizumab pretreatment in vitrectomy with silicone oil for severe diabetic retinopathy. Retina 2009;29(6):768-74. [DOI] [PubMed] [Google Scholar]
Yeoh 2008 {published data only}
- Yeoh J, Williams C, Allen P, Buttery R, Chiu D, Clark B. Avastin as an adjunct to vitrectomy in the management of severe proliferative diabetic retinopathy: a prospective case series. Clinical and Experimental Ophthalmology 2008;36(5):449-54. [PubMed] [Google Scholar]
Yeung 2010 {published data only}
- Yeung L, Liu L, Wu WC, Kuo YH, Chao AN, Chen KJ, et al. Reducing the incidence of early postoperative vitreous haemorrhage by preoperative intravitreal bevacizumab in vitrectomy for diabetic tractional retinal detachment. Acta Opthalmologica 2010;88(6):635-40. [DOI] [PubMed] [Google Scholar]
Yin 2017 {published data only}
- Yin N, Zhao S, Zhu HN. Efficacy comparison of conbercept and ranibizumab as pre-treatment for pars plana vitrectomy in proliferative diabetic retinopathy. International Eye Science 2017;17(7):1300-2. [Google Scholar]
Zeng 2017 {published data only}
- Zeng G, Li P, Ye Y. Effects of intravitreal injection of conbercept on vitrectomy for proliferative diabetic retinopathy. Chinese Journal of Experimental Ophthalmology 2017;35(10):920-3. [Google Scholar]
Zhou 2018a {published data only}
- Zhou J, Liu Z, Chen M, Luo ZH, Li YQ, Qi GY, et al. Concentrations of VEGF and PlGF decrease in eyes after intravitreal conbercept injection. Diabetes Therapy 2018;9(6):2393-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
Zhou 2018b {published data only}
- Zhou HS, Ma HZ, Liang WL, Yan SG. Effects of vitrectomy with preoperative intravitreal conbercept for proliferative diabetic retinopathy. International Eye Science 2018;18(2):363-6. [Google Scholar]
References to ongoing studies
ISRCTN79120387 {unpublished data only}79120387
- ISRCTN79120387. A randomised, single-masked, phase IV pilot study of the efficacy and safety of adjunctive intravitreal Avastin® (bevacizumab) in the prevention of early postoperative vitreous haemorrhage following diabetic vitrectomy. www.controlled-trials.com/ISRCTN79120387 (first received 18 September 2007).
NCT00516464 {unpublished data only}
- NCT00516464. Evaluation of ranibizumab in proliferative diabetic retinopathy (PDR) requiring vitrectomy. clinicaltrials.gov/ct2/show/NCT00516464 (first received 15 August 2007).
NCT00931125 {unpublished data only}
- NCT00931125. Randomized, double blinded, controlled, two-center study assessing the safety and efficacy of intravitreal ranibizumab as a preoperative adjunct treatment before vitrectomy surgery in proliferative diabetic retinopathy (PDR) compared to vitrectomy alone. clinicaltrials.gov/show/NCT00931125 (first received 2 July 2009).
NCT01091896 {unpublished data only}
- NCT01091896. Adjuvant intravitreal bevacizumab in pars plana vitrectomy for vitreous hemorrhage secondary to diabetic retinopathy. clinicaltrials.gov/show/NCT01091896 (first received 24 March 2010).
NCT01151722 {unpublished data only}
- NCT01151722. Adjuvant intravitreal bevacizumab in pars plana vitrectomy for diabetic vitreous hemorrhage. clinicaltrials.gov/show/NCT01151722 (first received 28 June 2010).
NCT01306981 {unpublished data only}
- NCT01306981. A prospective, randomised controlled trial of ranibizumab pre-treatment in diabetic vitrectomy - a pilot study. clinicaltrials.gov/show/NCT01306981 (first received 2 March 2011).
Additional references
Anonymous 1985
- Anonymous. Two-year course of visual acuity in severe proliferative diabetic retinopathy with conventional management. Diabetic Retinopathy Vitrectomy Study (DRVS) report #1. Ophthalmology 1985;92(4):492-502. [DOI] [PubMed] [Google Scholar]
Benson 1988
- Benson WE, Brown GC, Tasman W, McNamara JA. Complications of vitrectomy for non-clearing vitreous hemorrhage in diabetic patients. Ophthalmic Surgery 1988;19(12):862-4. [PubMed] [Google Scholar]
Berrocal 2016
- Berrocal MH, Acaba LA, Acaba A. Surgery for diabetic eye complications. Current Diabetes Reports 2016;16:1-7. [DOI] [PubMed] [Google Scholar]
Bhende 2000
- Bhende M, Agraharam SG, Gopal L, Sumasri K, Sukumar B, George J, et al. Ultrasound biomicroscopy of sclerotomy sites after pars plana vitrectomy for diabetic vitreous hemorrhage. Ophthalmology 2000;107(9):1729-36. [DOI] [PubMed] [Google Scholar]
Blankenship 1985
- Blankenship GW, Machemer R. Long-term diabetic vitrectomy results. Report of 10 year follow-up. Ophthalmology 1985;92(4):503-6. [DOI] [PubMed] [Google Scholar]
Blankenship 1986
- Blankenship GW. Management of vitreous cavity hemorrhage following pars plana vitrectomy for diabetic retinopathy. Ophthalmology 1986;93(1):39-44. [DOI] [PubMed] [Google Scholar]
Brown 1992
- Brown GC, Tasman WS, Benson WE, McNamara JA, Eagle RC Jr. Reoperation following diabetic vitrectomy. Archives of Ophthalmology 1992;110(4):506-10. [DOI] [PubMed] [Google Scholar]
Chen 2021
- Chen Y, Kearns VR, Zhou L, Sandinha T, Lam WC, Steel DH, et al. Silicone oil in vitreoretinal surgery: indications, complications, new developments and alternative long-term tamponade agents. Acta Ophthalmologica 2021;99(3):240-50. [DOI] [PubMed] [Google Scholar]
Csaky 2008
- Csaky KG, Richman EA, Ferris FL. Report from the NEI/FDA Ophthalmic Clinical Trial Design and Endpoints Symposium. Investigative Ophthalmology & Visual Science 2008;49:479-89. [DOI] [PubMed] [Google Scholar]
de Boer 2004
- Boer MR, Moll AC, Vet HC, Terwee CB, Völker-Dieben HJ, Rens GH. Psychometric properties of vision-related quality of life questionnaires: a systematic review. Ophthalmic & Physiological Optics 2004;24(4):257-73. [DOI: 10.1111/j.1475-1313.2004.00187.x] [DOI] [PubMed] [Google Scholar]
Dervenis 2021
- Dervenis P, Dervenis N, Steel D, Sandinha T, Tranos P, Vasilakis P, et al. Intravitreal bevacizumab prior to vitrectomy for proliferative diabetic retinopathy: a systematic review. Therapeutic Advances in Ophthalmology 2021;13:25158414211059256. [DOI] [PMC free article] [PubMed] [Google Scholar]
Dervenis 2022
- Dervenis N, Dervenis P, Sandinha T, Murphy DC, Steel DH. Intraocular tamponade choice with vitrectomy and internal limiting membrane peeling for idiopathic macular hole: a systematic review and meta-analysis. Ophthalmology. Retina 2022;6(6):457-68. [DOI: 10.1016/j.oret.2022.01.023] [DOI] [PubMed] [Google Scholar]
Diabetes UK 2020
- Diabetes UK. Diabetes: facts and stats. www.diabetes.org.uk/professionals/position-statements-reports/statistics/diabetes-prevalence-2019 (accessed 6 June 2021).
Dziura 2013
- Dziura JD, Post LA, Zhao Q, Fu Z, Peduzzi P. Strategies for dealing with missing data in clinical trials: from design to analysis. Yale Journal of Biology and Medicine 2013;86(3):343-58. [PMID: ] [PMC free article] [PubMed] [Google Scholar]
El‐Sabagh 2011
- El-Sabagh HA, Abdelghaffar W, Labib AM, Mateo C, Hashem TM, Al-Tamimi DM, et al. Preoperative intravitreal bevacizumab use as an adjuvant to diabetic vitrectomy: histopathologic findings and clinical implications. Ophthalmology 2011;118(4):636-41. [DOI] [PubMed] [Google Scholar]
Faghihi 2008
- Faghihi H, Taheri A, Farahvash MS, Esfahani MR, Rajabi MT. Intravitreal triamcinolone acetonide injection at the end of vitrectomy for diabetic vitreous hemorrhage: a randomized, clinical trial. Retina 2008;28(9):1241-6. [DOI] [PubMed] [Google Scholar]
Glanville 2006
- Glanville JM, Lefebvre C, Miles JN, Camosso-Stefinovic J. How to identify randomized controlled trials in MEDLINE: ten years on. Journal of the Medical Library Association 2006;94(2):130-6. [PMC free article] [PubMed] [Google Scholar]
Govers 2022
- Govers BM, Lamers MPM, Klevering BJ, Keijser S. Air versus fluorinated gas tamponades in pars plana vitrectomy treatment for primary rhegmatogenous retinal detachment. Acta Ophthalmologica 2022;100(8):e1600-5. [DOI: 10.1111/aos.15144] [DOI] [PMC free article] [PubMed] [Google Scholar]
GRADEpro GDT [Computer program]
- GRADEpro GDT. Hamilton (ON): McMaster University (developed by Evidence Prime), accessed 1 September 2022. Available from gradepro.org.
Gupta 2012
- Gupta B, Sivaprasad S, Wong R, Laidlaw A, Jackson TL, McHugh D, et al. Visual and anatomical outcomes following vitrectomy for complications of diabetic retinopathy: the DRIVE UK study. Eye 2012;26(4):510-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
Han 1991
- Han DP, Murphy ML, Mieler WF, Abrams GW. Outpatient fluid-air exchange for severe postvitrectomy diabetic vitreous hemorrhage. Long-term results and complications. Retina 1991;11(3):309-14. [DOI] [PubMed] [Google Scholar]
Hershberger 2004
- Hershberger VS, Augsburger JJ, Hutchins RK, Raymond LA, Krug S. Fibrovascular ingrowth at sclerotomy sites in vitrectomized diabetic eyes with recurrent vitreous hemorrhage: ultrasound biomicroscopy findings. Ophthalmology 2004;111(6):1215-21. [DOI] [PubMed] [Google Scholar]
Higgins 2017
- Higgins JPT, Altman DG, Sterne JAC (editors). Chapter 8: Assessing risk of bias in included studies. In: Higgins JPT, Churchill R, Chandler J, Cumpston MS (editors), Cochrane Handbook for Systematic Reviews of Interventions version 5.2.0 (updated June 2017), Cochrane, 2017. Available from www.training.cochrane.org/handbook.
Higgins 2021
- Higgins JP, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA, editor(s). Cochrane Handbook for Systematic Reviews of Interventions Version 6.2 (updated February 2021). Cochrane, 2021. Available from training.cochrane.org/handbook. [DOI] [PMC free article] [PubMed]
Ho 1992
- Ho T, Smiddy WE, Flynn HW Jr. Vitrectomy in the management of diabetic eye disease. Survey of Ophthalmology 1992;37(3):190-202. [DOI] [PubMed] [Google Scholar]
Hotta 2000
- Hotta K, Hirakata A, Ohi Y, Yamamoto R, Shinoda K, Oshitari K, et al. Ultrasound biomicroscopy for examination of the sclerotomy site in eyes with proliferative diabetic retinopathy after vitrectomy. Retina 2000;20(1):52-8. [DOI] [PubMed] [Google Scholar]
Hsu 2014
- Hsu YR, Yang CM, Yeh PT. Clinical and histological features of epiretinal membrane after diabetic vitrectomy. Graefe's Archive for Clinical and Experimental Ophthalmology 2014;252(3):401-10. [DOI] [PubMed] [Google Scholar]
Hu 2019b
- Hu X, Pan Q, Zheng J, Song Z, Zhang Z. Reoperation following vitrectomy for diabetic vitreous hemorrhage with versus without preoperative intravitreal bevacizumab. BMC Ophthalmology 2019;19:200. [DOI] [PMC free article] [PubMed] [Google Scholar]
Hutton 1980
- Hutton WL, Bernstein I, Fuller D. Diabetic traction retinal detachment. Factors influencing final visual acuity. Ophthalmology 1980;87:1071-7. [DOI] [PubMed] [Google Scholar]
Issa 2011
- Issa SA, Connor A, Habib M, Steel DH. Comparison of retinal breaks observed during 23 gauge transconjunctival vitrectomy versus conventional 20 gauge surgery for proliferative diabetic retinopathy. Clinical Ophthalmology 2011;2011(5):109-14. [DOI] [PMC free article] [PubMed] [Google Scholar]
Jackson 2015
- Jackson TL, Johnston RL, Donachie PHJ, Williamson TJ, Sparrow JM, Steel DH. The Royal College of Ophthalmologists' national ophthalmology database study of vitreoretinal surgery: report 6, diabetic vitrectomy. JAMA Ophthalmology 2016;134(1):79-85. [DOI] [PubMed] [Google Scholar]
Joondeph 1989
- Joondeph BC, Blankenship GW. Hemostatic effects of air versus fluid in diabetic vitrectomy. Ophthalmology 1989;96(12):1701-6. [DOI] [PubMed] [Google Scholar]
Jorge 2006
- Jorge R, Costa RA, Calucci D, Cintra LP, Scott IU. Intravitreal bevacizumab (Avastin) for persistent new vessels in diabetic retinopathy (IBEPE study). Retina 2006;26(9):1006-13. [DOI: 10.1097/01.iae.0000246884.76018.63] [DOI] [PubMed] [Google Scholar]
Kaiser 2000
- Kaiser RS, Maguire MG, Grunwald JE, Lieb D, Jani B, Brucker AJ, et al. One-year outcomes of panretinal photocoagulation in proliferative diabetic retinopathy. American Journal of Ophthalmology 2000;129(2):178-85. [DOI] [PubMed] [Google Scholar]
Klein 1984a
- Klein R, Klein BE, Moss SE, Davis MD, DeMets DL. The Wisconsin epidemiologic study of diabetic retinopathy. II. Prevalence and risk of diabetic retinopathy when age at diagnosis is less than 30 years. Archives of Ophthalmology 1984;102(4):520-6. [DOI] [PubMed] [Google Scholar]
Klein 1984b
- Klein R, Klein BE, Moss SE, Davis MD, DeMets DL. The Wisconsin epidemiologic study of diabetic retinopathy. III. Prevalence and risk of diabetic retinopathy when age at diagnosis is 30 or more years. Archives of Ophthalmology 1984;102(4):527-32. [DOI] [PubMed] [Google Scholar]
Koutsandrea 2001
- Koutsandrea CN, Apostolopoulos MN, Chatzoulis DZ, Parikakis EA, Theodossiadis GP. Hemostatic effects of SF6 after diabetic vitrectomy for vitreous hemorrhage. Acta Ophthalmologica Scandinavica 2001;79(1):34-8. [DOI] [PubMed] [Google Scholar]
Kreiger 1993
- Kreiger AE. Wound complications in pars plana vitrectomy. Retina 1993;13(4):335-44. [DOI] [PubMed] [Google Scholar]
Kroll 2014
- Kroll P, Rodrigues EB, Meyer CH. Vitreous. New York, NY: Springer, 2014. [Google Scholar]
Laatikainen 1987
- Laatikainen L, Summanen P, Immonen I. Effect of tranexamic acid on postvitrectomy haemorrhage in diabetic patients. International Ophthalmology 1987;10(3):153-5. [DOI] [PubMed] [Google Scholar]
Liew 2014
- Liew G, Michaelides M, Bunce C. A comparison of the causes of blindness certifications in England and Wales in working age adults (16-64 years), 1999-2000 with 2009-2010. BMJ Open 2014;12(4):2. [DOI] [PMC free article] [PubMed] [Google Scholar]
Liggett 1987
- Liggett PE, Lean JS, Barlow WE, Ryan SJ. Intraoperative argon endophotocoagulation for recurrent vitreous hemorrhage after vitrectomy for diabetic retinopathy. American Journal of Ophthalmology 1987;103(2):146-9. [DOI] [PubMed] [Google Scholar]
Mangione 2001
- Mangione CM, Lee PP, Gutierrez PR, Spritzer K, Berry S, Hays RD, National Eye Institute Visual Function Questionnaire Field Test Investigators. Development of the 25-item National Eye Institute Visual Function Questionnaire. Archives of Ophthalmology 2001;119(7):1050-8. [DOI: 10.1001/archopht.119.7.1050] [DOI] [PubMed] [Google Scholar]
Martin 1992
- Martin DF, McCuen BW 2nd. Efficacy of fluid-air exchange for postvitrectomy diabetic vitreous hemorrhage. American Journal of Ophthalmology 1992;114(4):457-63. [DOI] [PubMed] [Google Scholar]
Mason 1978
- Mason G, Peyman GA. The role of vitrectomy in diabetic retinopathy. International Ophthalmology Clinics 1978;18(4):133-64. [PubMed] [Google Scholar]
McLeod 1991
- McLeod D. Microsurgical management of neovascularisation secondary to posterior segment ischaemia. Eye 1991;5(Pt 2):252-9. [DOI] [PubMed] [Google Scholar]
McLeod 2000
- McLeod D. Entry site neovascularisation after diabetic vitrectomy. British Journal of Ophthalmology 2000;84(8):810-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
McLeod 2003
- McLeod D. Wieger's ligament [republished in Ophthalmology. 2003 Jun;110(6):1265]. Ophthalmology 2003;110(4):628. [DOI] [PubMed] [Google Scholar]
Mehta 2020
- Mehta A, Rana-Rahman R, Klaassen I, Rees J, Steel DH. The effect of internal limiting membrane cleaning on epiretinal membrane formation after vitrectomy for proliferative diabetic retinopathy. Ophthalmologica 2020;243(6):426-35. [DOI] [PubMed] [Google Scholar]
Nagbal 2017
- Nagbal M, Mehrotra N, Vishnoi A. The role of perioperative anti-VEGF during vitrectomy for vitreous hemorrhage in relation to postoperative nonclearing vitreous hemorrhage and cystoid macular edema. Journal of VitreoRetinal Diseases 2017;1(6):379-84. [Google Scholar]
Novak 1984
- Novak MA, Rice TA, Michels RG, Auer C. Vitreous hemorrhage after vitrectomy for diabetic retinopathy. Ophthalmology 1984;91(12):1485-9. [DOI] [PubMed] [Google Scholar]
Packer 1989
- Packer AJ, McCuen BW 2nd, Hutton WL, Ramsay RC. Procoagulant effects of intraocular sodium hyaluronate (Healon) after phakic diabetic vitrectomy. A prospective, randomized study. Ophthalmology 1989;96(10):1491-4. [DOI] [PubMed] [Google Scholar]
Ramezani 2005
- Ramezani AR, Ahmadieh H, Ghaseminejad AK, Yazdani S, Golestan B. Effect of tranexamic acid on early postvitrectomy diabetic haemorrhage; a randomised clinical trial. British Journal of Ophthalmology 2005;89(8):1041-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
RevMan Web 2023 [Computer program]
- Review Manager Web (RevMan Web). Version 4.26.0. The Cochrane Collaboration, 2023. Available at revman.cochrane.org.
Rush 2022
- Rush RB, Velazquez JC, Rosales CR, Rush SW. Gas tamponade for the prevention of postoperative vitreous hemorrhaging after diabetic vitrectomy: a randomized clinical trial. American Journal of Ophthalmology 2022;242:173-80. [DOI: 10.1016/j.ajo.2022.06.015] [DOI] [PubMed] [Google Scholar]
Russo 2019
- Russo A, Longo A, Avitabile T, Bonfiglio V, Fallico M, Boscia F, et al. Incidence and risk factors for tractional macular detachment after anti-vascular endothelial growth factor agent pretreatment before vitrectomy for complicated proliferative diabetic retinopathy. Journal of Clinical Medicine 2019;8(11):1960. [DOI: 10.3390/jcm8111960] [DOI] [PMC free article] [PubMed] [Google Scholar]
Sawa 2000
- Sawa H, Ikeda T, Matsumoto Y, Niiya A, Kinoshita S. Neovascularization from scleral wound as cause of vitreous rebleeding after vitrectomy for proliferative diabetic retinopathy. Japanese Journal of Ophthalmology 2000;44(2):154-60. [DOI] [PubMed] [Google Scholar]
Scanlon 2008
- Scanlon PH. The English national screening programme for sight threatening diabetic retinopathy. Journal of Medical Screening 2008;15(1):1-4. [DOI] [PubMed] [Google Scholar]
Schiff 2007
- Schiff WM, Barile GR, Hwang JC, Tseng JJ, Cekic O, Del Priore LV, et al. Diabetic vitrectomy: influence of lens status upon anatomic and visual outcomes. Ophthalmology 2007;114(3):544-50. [DOI] [PubMed] [Google Scholar]
Schwartz 1996
- Schwatz SD, Alexander R, Hiscott P, Gregor ZJ. Recognition of vitreoschisis in proliferative diabetic retinopathy. A useful landmark in vitrectomy for diabetic traction retinal detachment. Ophthalmology 1996;103(2):323-8. [DOI] [PubMed] [Google Scholar]
Sebag 1996
- Sebag J. Diabetic vitreopathy. Ophthalmology 1996;103(2):205-6. [DOI] [PubMed] [Google Scholar]
Steel 2008
- Steel DH, Habib MS, Park S, Hildreth AJ, Owen RI. Entry site neovascularization and vitreous cavity hemorrhage after diabetic vitrectomy. The predictive value of inner sclerostomy site ultrasonography. Ophthalmology 2008;115(3):525-32. [DOI] [PubMed] [Google Scholar]
Stefansson 2009
- Stefansson E. Physiology of vitreous surgery. Graefes Archives of Clinical and Experimental Ophthalmology 2009;247(2):147-63. [DOI] [PubMed] [Google Scholar]
Suñer 2017
- Suner IJ, Bressler NM, Varma R, Dolan CM, Ward J, Turpcu A. Responsiveness of the National Eye Institute Visual Function Questionnaire-25 to visual acuity gains in patients with diabetic macular edema: Evidence from the RIDE and RISE Trials. Retina 2017;37(6):1126-33. [DOI] [PMC free article] [PubMed] [Google Scholar]
Tolentino 1989
- Tolentino FI, Cajita VN, Gancayco T, Skates S. Vitreous hemorrhage after closed vitrectomy for proliferative diabetic retinopathy. Ophthalmology 1989;96(10):1495-500. [DOI] [PubMed] [Google Scholar]
Vaideanu 2014
- Vaideanu D, Sandhu SS, Ling J, Richardson J, Steel DH. Rate of diabetic vitrectomy in a defined geographical part of North East England. Ophthalmic Epidemiology 2014;21(3):178-83. [DOI] [PubMed] [Google Scholar]
Veliz 2014
- Veliz D, Rada G. Does preoperative intravitreal bevacizumab reduce complications of vitrectomy for proliferative diabetic retinopathy? [El uso preoperatorio de bevacizumab reduce lascomplicaciones en pacientes con retinopatía diabéticasometidos a vitrectomía?]. Medwave 2014;14(11):e6052. [DOI] [PubMed] [Google Scholar]
Virata 2001
- Virata SR, Kylstra JA. Postoperative complications following vitrectomy for proliferative diabetic retinopathy with sew-on and noncontact wide-angle viewing lenses. Ophthalmic Surgery and Lasers 2001;32(3):193-7. [PubMed] [Google Scholar]
West 2000
- West JF, Gregor ZJ. Fibrovascular ingrowth and recurrent haemorrhage following diabetic vitrectomy. British Journal of Ophthalmology 2000;84(8):822-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
Yang 2007
- Yang CM, Yeh PT, Yang CH. Intravitreal long-acting gas in the prevention of early postoperative vitreous hemorrhage in diabetic vitrectomy. Ophthalmology 2007;114(4):710-5. [DOI] [PubMed] [Google Scholar]
Yeh 2005
- Yeh PT, Yang CM, Yang CH, Huang JS. Cryotherapy of the anterior retina and sclerotomy sites in diabetic vitrectomy to prevent recurrent vitreous hemorrhage: an ultrasound biomicroscopy study. Ophthalmology 2005;112(12):2095-102. [DOI] [PubMed] [Google Scholar]
Yorston 2008
- Yorston D, Wickham L, Benson S, Bunce C, Sheard R, Charteris D. Predictive clinical features and outcomes of vitrectomy for proliferative diabetic retinopathy. British Journal of Ophthalmology 2008;92(3):365-8. [DOI] [PubMed] [Google Scholar]
Yoshida 2017
- Yoshida S, Kobayashi Y, Nakao S, Sassa Y, Hisatomi T, Ikeda Y, et al . Differential association of elevated inflammatory cytokines with postoperative fibrous proliferation and neovascularization after unsuccessful vitrectomy in eyes with proliferative diabetic retinopathy. Clinical Ophthalmology 2017;11:1697-705. [DOI] [PMC free article] [PubMed] [Google Scholar]
Zhang 2013
- Zhang ZH, Liu HY, Hernandez-Da Mota SE, Romano MR, Falavarjani KG, Ahmadieh H, et al. Vitrectomy with or without preoperative intravitreal bevacizumab for proliferative diabetic retinopathy: a meta-analysis of randomized controlled trials. American Journal of Ophthalmology 2013;156(1):106-15. [DOI] [PubMed] [Google Scholar]
Zhao 2011
- Zhao LQ, Zhu H, Zhao PQ, Hu YQ. A systematic review and meta-analysis of clinical outcomes of vitrectomy with or without intravitreal bevacizumab pretreatment for severe diabetic retinopathy. British Journal of Ophthalmology 2011;95(9):1216-22. [DOI] [PMC free article] [PubMed] [Google Scholar]
Zhou 2020
- Zhou C, Zhang Z, Luo D, Gu C, Lahm T, Draga D, Qiu Q. A relatively higher intraocular pressure set at the end of vitrectomy is associated with a more stable and rapid visual recovery for patients with vitreous haemorrhage. Acta Ophthalmologica 2020;98(4):e428-33. [DOI: 10.1111/aos.14293] [DOI] [PubMed] [Google Scholar]
Zhu 2008
- Zhu Q, Ziemssen F, Henke-Fahle S, Tatar O, Szurman P, Aisenbrey S, et al, Tübingen Bevacizumab Study Group, Grisanti S. Vitreous levels of bevacizumab and vascular endothelial growth factor-A in patients with choroidal neovascularization. Ophthalmology 2008;115(10):1750-5. [DOI: 10.1016/j.ophtha.2008.04.023] [DOI] [PubMed] [Google Scholar]
References to other published versions of this review
Smith 2011
- Smith JM, Steel DHW. Anti-vascular endothelial growth factor for prevention of postoperative vitreous cavity haemorrhage after vitrectomy for proliferative diabetic retinopathy. Cochrane Database of Systematic Reviews 2011, Issue 5. Art. No: CD008214. [DOI: 10.1002/14651858.CD008214.pub2] [DOI] [PubMed] [Google Scholar]
Smith 2015
- Smith JM, Steel DHW. Anti-vascular endothelial growth factor for prevention of postoperative vitreous cavity haemorrhage after vitrectomy for proliferative diabetic retinopathy. Cochrane Database of Systematic Reviews 2015, Issue 8. Art. No: CD008214. [DOI: 10.1002/14651858.CD008214.pub3] [DOI] [PMC free article] [PubMed] [Google Scholar]
Steel 2010
- Steel DHW, Smith JM. Anti-vascular endothelial growth factor for prevention of postoperative vitreous cavity haemorrhage after vitrectomy for proliferative diabetic retinopathy. Cochrane Database of Systematic Reviews 2010, Issue 1. Art. No: CD008214. [DOI: 10.1002/14651858.CD008214] [DOI] [Google Scholar]


