During the last three and a half years (2020–2023), the coronavirus disease 2019 (COVID-19), caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), generated an international emergency, defined as a Public Health Emergency of International Concern (PHEIC) and was later declared a pandemic by the World Health Organization (WHO) [[1], [2], [3], [4]]. In May 2023, the Emergency Committee of the WHO met for the 15th time and recommended to the WHO Director-General Dr. Tedros Adhanom Ghebreyesus, that COVID-19 should no longer be categorized as a PHEIC. Although the recommendation was adopted, COVID-19 is still considered a global health threat [5]. COVID-19 has caused more than 767 million cases and 6.94 million deaths up to June 2023 (https://covid19.who.int/), and these numbers could be significantly higher, potentially even three to four times the excess mortality associated with this disease [[6], [7], [8], [9], [10]]. Moreover, early during this pandemic (2020) [[11], [12], [13], [14]], multiple studies began to recognize and understand that chronic consequences may occur in a significant proportion of patients [15,16], leading to various manifestations and affecting different systems and organs after the acute phase of the illness [17]. These chronic consequences have also been observed in other viral emerging and reemerging infectious diseases, such as chikungunya, Zika, Ebola, and even dengue [[18], [19], [20], [21], [22], [23], [24], [25], [26], [27], [28]].
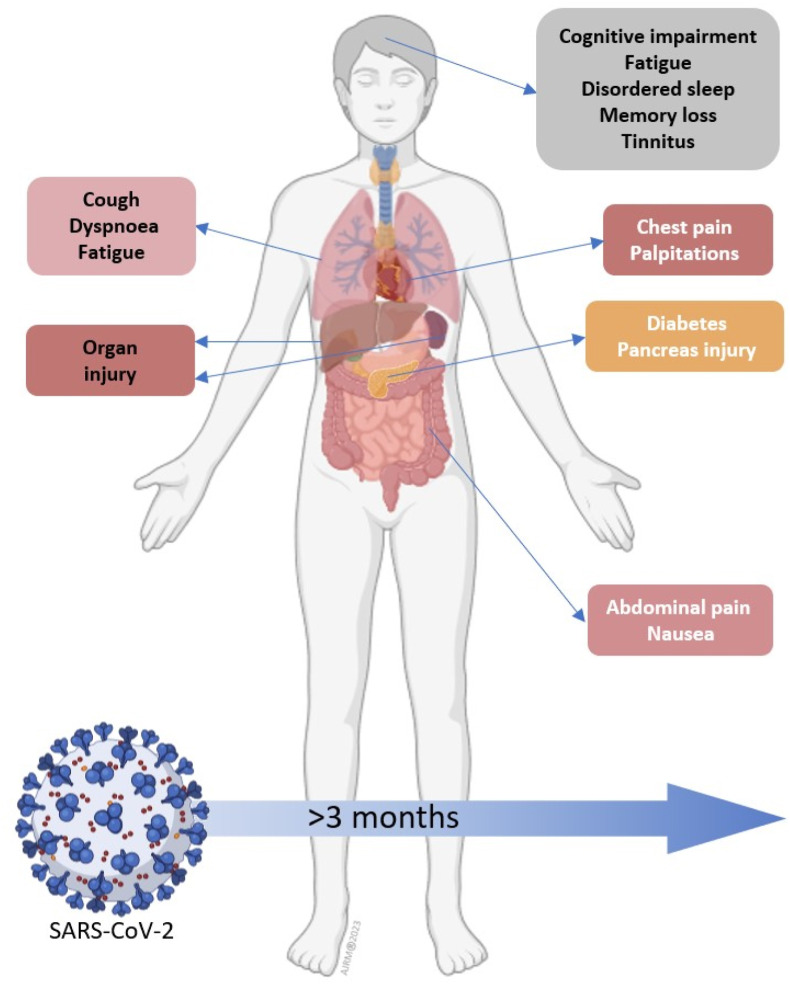
Long COVID-19, post-COVID-19 syndrome or post-acute sequelae of SARS-CoV-2 infection (PASC) [29] occur in individuals with a history of probable or confirmed SARS-CoV-2 infection [30], usually three months from the onset of COVID-19, presenting symptoms that last for at least two months and cannot be explained by an alternative diagnosis, as defined by the WHO [31,32]. The U.S. Centers for Disease Control and Prevention (CDC) uses the term “Post-COVID Conditions” (PCC) as an umbrella term for the wide range of health consequences that can be present four or more weeks after infection with SARS-CoV-2 (https://www.cdc.gov/coronavirus/2019-ncov/hcp/clinical-care/post-covid-conditions.html#print). Common clinical manifestations include fatigue, headache, attention disorder, dyspnea, cognitive dysfunction, and others (Fig. 1 ), which generally impact the patients’ daily functions [30]. The time frame of the symptoms in terms of onset and persistence is not the same for all presentations. Neurologic and cognitive symptoms tend to occur late and persist longer than gastrointestinal and respiratory symptoms [33,34].
Fig. 1.
Some of the clinical findings associated with long COVID-19, modified from Davis et al. [63].
New onset symptoms may occur after the initial recovery from an acute COVID-19 infection, or may persist from the initial disease [32]. Symptoms may also fluctuate or relapse over time. Some studies have found that the quality of life of long COVID-19 patients is significantly affected compared to controls. In addition to the multiple clinical findings, some associated conditions, or diseases may also be triggered, including autoimmune diseases or diabetes mellitus. Other studies suggest the existence in long COVID-19 patients of clusters of symptoms associated with functional impairments. Different authors also propose that different clinical phenotypes may be related to distinct underlying pathophysiologic mechanisms of disease [35,36]. The COVID-Home study performed in the Netherlands, and recently presented at the 33rd European Congress of Clinical Microbiology and Infectious Diseases (ECCMID 2023), organized its patients into three distinct phenotypes. The first one comprised by younger, healthier patients that had little to no persistent symptoms, the second one comprised of obese morbid women that had the highest burden of long COVID symptoms but showed little biological abnormalities and finally a third group made of middle-aged males with few lasting symptoms but with marked laboratory anomalies. According to this study, once the symptoms of prolonged COVID are established, they tend to remain stable and without much variation over time, the same can be said of those people who do not develop the condition immediately [37].
Long COVID-19 may affect patients with comorbidities, pregnant women, the elderly, and children and adolescents [32]. In fact, a new definition for pediatric long COVID-19 was released on February 16, 2023 by the WHO [38]. With this important step, a better characterization of the disease in the pediatric age would be possible and awareness improved.
According to systematic reviews, long COVID-19 is estimated to occur in 43%–80% of patients that develop an acute infection [[39], [40], [41]]. According to the WHO, 10–20% of people infected by SARS-CoV-2 may go on to develop its symptoms (https://www.who.int/europe/news-room/fact-sheets/item/post-covid-19-condition). However, available studies of long COVID-19 syndrome are highly heterogeneous [42]. Thus, we would consider that between 325 and 606 million people would probably live with long COVID-19. Nevertheless, a key aspect is to assess the evolution and make the proper follow-up of such patients with long COVID-19. Therefore, studies assessing the trajectories of the evolution of post-COVID-19 conditions in the long term are widely needed [43]. A recent study assessing more than 2000 patients found that 91% of patients with post COVID-19 condition improved slowly over a two-year course, 5% improved rapidly, and 4% had a persistent condition [43].
Additionally, when patients have underlying chronic comorbidities, the outcomes would be worse. A recent large study of adult patients with chronic liver disease who were diagnosed with COVID-19 before May 2020, found that symptoms consistent with long-COVID-19 were present in 30% of patients with chronic liver disease [44]. Different studies have also demonstrated significant and long-lasting neurological manifestations [45,46]. It has been suggested that as many as 80% of patients who sustained COVID-19 will show one or several neurological symptoms that can last months after the acute infection. Neurological symptoms are most common in young adults, while encephalopathy is more common in older adults [45].
Multiple factors would affect such outcomes and were associated with reporting symptoms 12 weeks or more after infection [47]. Female sex, younger age, belonging to a an African-American, mixed ethnicity or another ethnic minority group, socioeconomic deprivation, smoking, high body mass index and the presence of a wide range of comorbidities were associated with increased risk of symptoms included in the WHO definition of long COVID-19, and they are statistically associated with SARS-CoV-2 infection reported 12 weeks or more after infection [48]. Several multi-organ symptoms have been described, and multiple adverse consequences have also been documented as new onset diseases including cardiovascular, thrombotic and cerebrovascular diseases, type 2 diabetes, myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) and dysautonomias such as postural orthostatic tachycardia syndrome (POTS) [33].
Health care workers, and local and national health authorities should recognize the importance of long COVID-19, including its proper diagnosis and management, as part of the health agenda to address it [49]. There is also an urgent need to develop evidence-based guidelines at national and international levels [50] dealing comprehensively with long COVID-19 [51]. As occurred with COVID-19 acute infection, many therapeutic approaches for long COVID-19 that have been already suggested, and even applied, are not well studied. Further, international studies are needed to establish the best practice to help the multitude of patients currently suffering this condition. Considering the involvement of multiple clinical areas and other healthcare professionals, the approach should be multidisciplinary, given not just the clinical but also the social and mental consequences of this long-term event [52]. We believe surveillance of long COVID-19 should be globally implemented; and it must considered a notifiable condition. To improve the documentation of long or post–COVID-19, a new International Classification of Diseases, Tenth Revision, Clinical Modification (ICD-10-CM) diagnosis code (U09.9 Post COVID-19 condition, unspecified) (https://www.who.int/standards/classifications/classification-of-diseases/emergency-use-icd-codes-for-covid-19-disease-outbreak) (Fig. 2 ) was introduced on October 1, 2021 [53,54]. In addition, global and local health authorities should begin to think about laws or policies related to total or partial disability as result of long COVID-19 [55,56].
Fig. 2.
ICD codes for COVID-19, according the WHO (https://www.who.int/standards/classifications/classification-of-diseases/emergency-use-icd-codes-for-covid-19-disease-outbreak).
Compared to the acute phase of COVID-19, where there is evidence that several pharmacologic interventions may reduce the severity of infections, lessen morbidity, and lower mortality [57], there is an absence of evidence-based treatments in the post-viral syndrome, which further fuels the frustration of affected patients and their clinicians [58]. Add to these problems the disparities in healthcare systems, especially in the most affected and vulnerable countries, which impose a significant disease burden on this complex and multifaceted disorder [59]. Long COVID-19 prevention is also an important area of practice and research. It is worth mentioning that vaccination against SARS-CoV-2 decreases the risk of long COVID-19 [60]. Also, in two cohort studies, nirmatrelvir and molnupiravir treatment reduced the risk of long COVID-19 when initiated early in patients at risk of severe disease progression [47,61].
The pathophysiology of long COVID-19 remains elusive partly because of the multiple possible signs, symptoms, and organ systems involved. A lack of understanding of long COVID-19 inevitably complicates care [59]. Then, more comprehensive and multidisciplinary research on these consequences is of utmost importance [62,63]. Even viral persistence beyond three months has also been reported, as well as identification of RNA or isolation of the virus itself from different organs and systems [64,65]. In a 2022 study, the expression of SARS-CoV-2 RNA in the gut mucosa ∼7 months after mild acute COVID-19 was observed in 32 of 46 patients with inflammatory bowel disease [66]. Viral nucleocapsid protein persisted in 24 of 46 patients in gut epithelium and CD8+ T cells. Expression of SARS-CoV-2 antigens was not detectable in stool, and viral antigen persistence was unrelated to the severity of acute COVID-19, immunosuppressive therapy, or gut inflammation. Authors could not culture SARS-CoV-2 from the gut tissue of patients with viral antigen persistence [66]. Post-acute sequelae of COVID-19 were reported from most patients with viral antigen persistence but not from patients without viral antigen persistence [66]. Different long-term gastrointestinal consequences of COVID-19 have been reported, including motility disorders, acid-related disorders (dyspepsia, gastroesophageal reflux disease, peptic ulcer disease), functional intestinal disorders, acute pancreatitis, hepatic and biliary disease [67]. Even more, long detection of SARS-CoV-2 in other organs and tissues has been reported in different publications [68], in some reaching up to more than a year post-infection [[69], [70], [71], [72]], mainly in immunocompromised patients. Most studies focus on the clinical consequences of long COVID-19, but few assess viral persistence in different organs and tissues and the immunological profile of such conditions [[73], [74], [75], [76]]. In the acute infection, studies have associated COVID-19 clinical evolution with the microbiome [77]. A recent study among recovered COVID-19 patients, found that the relative abundance of some specific primarily opportunistic pathogens, such as bacteria and fungi, was decreased in recovered patients, while the abundance of butyrate-producing organisms was increased in these patients. Moreover, these differences were still present for some organisms at 12 months after recovery, indicating the need for long-term monitoring of COVID-19 patients after virus clearance [78].
Immune system dysregulation [79,80] with or without reactivation of latent pathogens such as Epstein-Barr virus (EBV) and human herpesvirus 6 (HHV-6) [81,82] has also been described. Other authors have explored the effects of SARS-CoV-2 on the microbiota, including the virome [83]. Other possible factors include autoimmunity [84,85], immune system dysfunction through molecular mimicry [86], microvascular blood clotting with endothelial dysfunction [87,88], and dysfunctional signaling in the brainstem or vagus nerve [86,89].
As occurred after COVID-19 cases rose in 2020, when healthcare and academic centers prepared to attend population with this emerging disease [[90], [91], [92], [93], [94], [95]]; it is prime time to have a rapid response to this threatening growing long COVID-19 pandemic. Institutions need to be prepared for the long COVID-19 consequences and to provide evidence-based health care to those thousands or millions affected by this sequela of the pandemic. At the same time, at the community level, the population needs to be educated and understand the potential long impact of COVID-19 and the situation regarding the status of knowledge on the problem, including the evolving approaches to diagnosis and management of its clinical consequences [96].
In countries where health authorities manage targeted resources and create control programs, these should integrally include long COVID-19 [97], with the idea to incorporate this into the regular surveillance and management at the population level to mitigate and decrease the long-term impacts of the post-COVID-19 syndrome [63].
As of today, the most effective preventive strategy to prevent post-COVID syndromes, long COVID, and associated long-term impact, is vaccination of adults and children [[98], [99], [100]]. It is crucial to decrease sequelae, societal costs, and economic impact of long COVID-19 to healthcare systems and societies. In the era of vaccine hesitancy, motivating vaccination of individuals is essential to prevent these problems, particularly in children who remain at much lower vaccination rates than adults. The consequences of reinfection of patients with different SARS-CoV2 variants and the impact of vaccination in preventing long COVID-19, remains unknown and should be subject to continuous monitoring and research. Finally, we consider that the creation of research networks should be encouraged to guide future long COVID-19 policies, including the impact of vaccination, long-term clinical impact, and burden on health systems, among others.
Declaration of competing interest
None.
References
- 1.Dhama K., Khan S., Tiwari R., Sircar S., Bhat S., Malik Y.S., et al. Coronavirus disease 2019-COVID-19. Clin Microbiol Rev. 2020:33. doi: 10.1128/CMR.00028-20. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Rodriguez-Morales A.J., Cardona-Ospina J.A., Gutiérrez-Ocampo E., Villamizar-Peña R., Holguin-Rivera Y., Escalera-Antezana J.P., et al. Clinical, laboratory and imaging features of COVID-19: a systematic review and meta-analysis. Trav Med Infect Dis. 2020;34 doi: 10.1016/j.tmaid.2020.101623. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Farahat R.A., Abdelaal A., Umar T.P., El-Sakka A.A., Benmelouka A.Y., Albakri K., et al. The emergence of SARS-CoV-2 Omicron subvariants: current situation and future trends. Inf Med. 2022;30:480–494. doi: 10.53854/liim-3004-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Marcolino M.S., Ziegelmann P.K., Souza-Silva M.V.R., Nascimento I.J.B., Oliveira L.M., Monteiro L.S., et al. Clinical characteristics and outcomes of patients hospitalized with COVID-19 in Brazil: results from the Brazilian COVID-19 registry. Int J Infect Dis. 2021;107:300–310. doi: 10.1016/j.ijid.2021.01.019. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.de Araújo G.R., de Castro P., Ávila I.R., Bezerra J.M.T., Barbosa D.S. Effects of public health emergencies of international concern on disease control: a systematic review. Rev Panam Salud Públic. 2023;47:e74. doi: 10.26633/RPSP.2023.74. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Rodriguez-Morales A.J., Gallego V., Escalera-Antezana J.P., Méndez C.A., Zambrano L.I., Franco-Paredes C., et al. COVID-19 in Latin America: the implications of the first confirmed case in Brazil. Trav Med Infect Dis. 2020;35 doi: 10.1016/j.tmaid.2020.101613. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Cimerman S., Chebabo A., Cunha C.A.D., Rodríguez-Morales A.J. Deep impact of COVID-19 in the healthcare of Latin America: the case of Brazil. Braz J Infect Dis. 2020;24:93–95. doi: 10.1016/j.bjid.2020.04.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Cimerman S., Chebabo A., Cunha C.A.D., Rodríguez-Morales A.J. One year after the arrival of COVID-19 in Latin America: what have we learned in Brazil and other countries? Braz J Infect Dis. 2021;25 doi: 10.1016/j.bjid.2021.101571. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Tazerji S.S., Shahabinejad F., Tokasi M., Rad M.A., Khan M.S., Safdar M., et al. Global data analysis and risk factors associated with morbidity and mortality of COVID-19. Gene reports. 2022;26 doi: 10.1016/j.genrep.2022.101505. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Estimating excess mortality due to the COVID-19 pandemic: a systematic analysis of COVID-19-related mortality, 2020-21. Lancet (London, England) 2022;399:1513–1536. doi: 10.1016/S0140-6736(21)02796-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Barker-Davies R.M., O'Sullivan O., Senaratne K.P.P., Baker P., Cranley M., Dharm-Datta S., et al. The Stanford Hall consensus statement for post-COVID-19 rehabilitation. Br J Sports Med. 2020;54:949–959. doi: 10.1136/bjsports-2020-102596. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Karzai F., Madan R.A., Dahut W.L. The world of clinical trial development post COVID-19: lessons learned from a global pandemic. Clin Cancer Res. 2020;26:4198–4200. doi: 10.1158/1078-0432.CCR-20-1914. [DOI] [PubMed] [Google Scholar]
- 13.Davido B., Seang S., Tubiana R., de Truchis P. Post-COVID-19 chronic symptoms: a postinfectious entity? Clin Microbiol Infect. 2020;26:1448–1449. doi: 10.1016/j.cmi.2020.07.028. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Klok F.A., Boon G., Barco S., Endres M., Geelhoed J.J.M., Knauss S., et al. The Post-COVID-19 Functional Status scale: a tool to measure functional status over time after COVID-19. Eur Respir J. 2020;56 doi: 10.1183/13993003.01494-2020. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Salamanna F., Veronesi F., Martini L., Landini M.P., Fini M. Post-COVID-19 syndrome: the persistent symptoms at the post-viral stage of the disease. A systematic review of the current data. Front Med. 2021;8 doi: 10.3389/fmed.2021.653516. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Renaud-Charest O., Lui L.M.W., Eskander S., Ceban F., Ho R., Di Vincenzo J.D., et al. Onset and frequency of depression in post-COVID-19 syndrome: a systematic review. J Psychiatr Res. 2021;144:129–137. doi: 10.1016/j.jpsychires.2021.09.054. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Al-Aly Z., Xie Y., Bowe B. High-dimensional characterization of post-acute sequelae of COVID-19. Nature. 2021;594:259–264. doi: 10.1038/s41586-021-03553-9. [DOI] [PubMed] [Google Scholar]
- 18.Rodríguez-Morales A.J., Simon F. Chronic chikungunya, still to be fully understood. Int J Infect Dis. 2019;86:133–134. doi: 10.1016/j.ijid.2019.07.024. [DOI] [PubMed] [Google Scholar]
- 19.Amaral J.K., Bingham C.O., 3rd, Taylor P.C., Vilá L.M., Weinblatt M.E., Schoen R.T. Pathogenesis of chronic chikungunya arthritis: resemblances and links with rheumatoid arthritis. Trav Med Infect Dis. 2023;52 doi: 10.1016/j.tmaid.2022.102534. [DOI] [PubMed] [Google Scholar]
- 20.Cardona-Ospina J.A., Rodríguez-Morales A.J., Teixeira M.G., Gérardin P. vol. 70. Arthritis & rheumatology; Hoboken, NJ): 2018. p. 1891. (Need for Accurate and Consistent Definition of Chronic Chikungunya Arthritis: comment on the Article by Chang et al). [DOI] [PubMed] [Google Scholar]
- 21.Paniz-Mondolfi A.E., Rodriguez-Morales A.J., Blohm G., Marquez M., Villamil-Gomez W.E. ChikDenMaZika Syndrome: the challenge of diagnosing arboviral infections in the midst of concurrent epidemics. Ann Clin Microbiol Antimicrob. 2016;15:42. doi: 10.1186/s12941-016-0157-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Rodriguez-Morales A.J., Gil-Restrepo A.F., Ramirez-Jaramillo V., Montoya-Arias C.P., Acevedo-Mendoza W.F., Bedoya-Arias J.E., et al. vol. 5. 2016. p. 360. (Post-chikungunya chronic inflammatory rheumatism: results from a retrospective follow-up study of 283 adult and child cases in La Virginia, Risaralda, Colombia). F1000Res. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Rodriguez-Morales A.J., Restrepo-Posada V.M., Acevedo-Escalante N., Rodriguez-Munoz E.D., Valencia-Marin M., Castrillon-Spitia J.D., et al. Impaired quality of life after chikungunya virus infection: a 12-month follow-up study of its chronic inflammatory rheumatism in La Virginia, Risaralda, Colombia. Rheumatol Int. 2017;37:1757–1758. doi: 10.1007/s00296-017-3795-1. [DOI] [PubMed] [Google Scholar]
- 24.Cardona-Ospina J.A., Zapata M.F., Grajales M., Arias M.A., Grajales J., Bedoya-Rendón H.D., et al. Physical growth and neurodevelopment of a cohort of children after 3.5 Years of follow-up from mothers with Zika infection during pregnancy-third report of the ZIKERNCOL study. J Trop Pediatr. 2021;67 doi: 10.1093/tropej/fmab032. [DOI] [PubMed] [Google Scholar]
- 25.Rodríguez-Morales A.J., Bonilla-Aldana D.K., Bonilla-Aldana J.L., Arteaga-Livias K., Pecho-Silva S., Escalera-Antezana J.P. Role of Zika virus infection in cases and outbreaks of Guillain-Barré syndrome in Latin America: pooling the prevalence of studies. Trav Med Infect Dis. 2021;39 doi: 10.1016/j.tmaid.2020.101905. [DOI] [PubMed] [Google Scholar]
- 26.Forrester J.V. Ebola virus and persistent chronic infection: when does replication cease? Ann Transl Med. 2018;6:S39. doi: 10.21037/atm.2018.09.60. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Keita M., Diallo B., Mesfin S., Marega A., Nebie K.Y., Magassouba N., et al. Subsequent mortality in survivors of Ebola virus disease in Guinea: a nationwide retrospective cohort study. Lancet Infect Dis. 2019;19:1202–1208. doi: 10.1016/S1473-3099(19)30313-5. [DOI] [PubMed] [Google Scholar]
- 28.Zambrano L.I., Fuentes-Barahona I.C., Portillo-Pineda R., Aguilar-Ponce M., Murillo-Padilla J.C., Suazo-Menocal M., et al. Assessment of post-dengue rheumatic symptoms using the WOMAC and DAS-28 questionnaires in a Honduran population after a four-month follow-up. Trop. Med. Infect. Dis. 2022;7 doi: 10.3390/tropicalmed7120394. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Thaweethai T., Jolley S.E., Karlson E.W., Levitan E.B., Levy B., McComsey G.A., et al. Development of a definition of postacute sequelae of SARS-CoV-2 infection. JAMA. 2023 doi: 10.1001/jama.2023.8823. in press. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Lopez-Leon S., Wegman-Ostrosky T., Perelman C., Sepulveda R., Rebolledo P.A., Cuapio A., et al. More than 50 long-term effects of COVID-19: a systematic review and meta-analysis. Sci Rep. 2021;11 doi: 10.1038/s41598-021-95565-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Morrow A.K., Malone L.A., Kokorelis C., Petracek L.S., Eastin E.F., Lobner K.L., et al. Long-term COVID 19 sequelae in adolescents: the overlap with orthostatic intolerance and ME/CFS. Curr. Pediatr. Rep. 2022;10:31–44. doi: 10.1007/s40124-022-00261-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Soriano J.B., Murthy S., Marshall J.C., Relan P., Diaz J.V. A clinical case definition of post-COVID-19 condition by a Delphi consensus. Lancet Infect Dis. 2022;22:e102–e107. doi: 10.1016/S1473-3099(21)00703-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Davis H.E., Assaf G.S., McCorkell L., Wei H., Low R.J., Re'em Y., et al. Characterizing long COVID in an international cohort: 7 months of symptoms and their impact. EClinicalMed. 2021;38 doi: 10.1016/j.eclinm.2021.101019. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Jason L.A., Islam M., Conroy K., Cotler J., Torres C., Johnson M., et al. COVID-19 symptoms over time: comparing long-haulers to ME/CFS. Fatigue : Biomed. Health. Behav. 2021;9:59–68. doi: 10.1080/21641846.2021.1922140. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Kenny G., McCann K., O'Brien C., Savinelli S., Tinago W., Yousif O., et al. Identification of distinct long COVID clinical phenotypes through cluster analysis of self-reported symptoms. Open Forum Infect Dis. 2022;9 doi: 10.1093/ofid/ofac060. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Tami A., van der Gun B.T.F., Wold K.I., Vincenti-González M.F., Veloo A.C.M., Knoester M., et al. The COVID HOME study research protocol: prospective cohort study of non-hospitalised COVID-19 patients. PLoS One. 2022;17 doi: 10.1371/journal.pone.0273599. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Barboza A.P., Luna-Muschi A., Leal F., Mendes E., Manuli E., Ghilardi F., et al. 2023. Long COVID in Brazil: a multicentre study 12. COVID-19 epidemiology - local, regional, national, global. Abstract. 33rd European congress of clinical Microbiology and infectious diseases (ECCMID 2023) Copenhaguen, Denmark, April 15-18, 2023. [Google Scholar]
- 38.WHO . 2023. A clinical case definition for post COVID-19 condition in children and adolescents by expert consensus.https://www.who.int/publications/i/item/WHO-2019-nCoV-Post-COVID-19-condition-CA-Clinical-case-definition-2023-1. 2023 [Google Scholar]
- 39.Cabrera Martimbianco A.L., Pacheco R.L., Bagattini A.M., Riera R. Frequency, signs and symptoms, and criteria adopted for long COVID-19: a systematic review. Int J Clin Pract. 2021;75 doi: 10.1111/ijcp.14357. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Chen C., Haupert S.R., Zimmermann L., Shi X., Fritsche L.G., Mukherjee B. Global prevalence of post-coronavirus disease 2019 (COVID-19) condition or long COVID: a meta-analysis and systematic review. J Infect Dis. 2022;226:1593–1607. doi: 10.1093/infdis/jiac136. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Natarajan A., Shetty A., Delanerolle G., Zeng Y., Zhang Y., Raymont V., et al. A systematic review and meta-analysis of long COVID symptoms. Syst Rev. 2023;12:88. doi: 10.1186/s13643-023-02250-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Lampl B.M.J., Leitzmann M.F., Salzberger B. Prevalence of post-COVID-19 conditions depends on the method of assessment. J Infect Dis. 2023;227:306. doi: 10.1093/infdis/jiac467. [DOI] [PubMed] [Google Scholar]
- 43.Servier C., Porcher R., Pane I., Ravaud P., Tran V.-T. Trajectories of the evolution of post COVID-19 condition, up to two years after symptoms onset. Int J Infect Dis. 2023 doi: 10.1016/j.ijid.2023.05.007. in press. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Aby E.S., Moafa G., Latt N., Sultan M.T., Cacioppo P.A., Kumar S., et al. Long-term clinical outcomes of patients with COVID-19 and chronic liver disease: US multicenter COLD study. Hepatol. Commun. 2023;7 doi: 10.1097/01.HC9.0000897224.68874.de. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Granholm A.C. Long-term effects of SARS-CoV-2 in the brain: clinical consequences and molecular mechanisms. J Clin Med. 2023:12. doi: 10.3390/jcm12093190. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Xu E., Xie Y., Al-Aly Z. Long-term neurologic outcomes of COVID-19. Nat Med. 2022;28:2406–2415. doi: 10.1038/s41591-022-02001-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Tsampasian V., Elghazaly H., Chattopadhyay R., Debski M., TKP Naing, Garg P., et al. Risk factors associated with post-COVID-19 condition: a systematic review and meta-analysis. JAMA Intern Med. 2023 doi: 10.1001/jamainternmed.2023.0750. in press. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Subramanian A., Nirantharakumar K., Hughes S., Myles P., Williams T., Gokhale K.M., et al. Symptoms and risk factors for long COVID in non-hospitalized adults. Nat Med. 2022;28:1706–1714. doi: 10.1038/s41591-022-01909-w. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Garout M.A., Saleh S.A.K., Adly H.M., Abdulkhaliq A.A., Khafagy A.A., Abdeltawab M.R., et al. Post-COVID-19 syndrome: assessment of short- and long-term post-recovery symptoms in recovered cases in Saudi Arabia. Infection. 2022;50:1431–1439. doi: 10.1007/s15010-022-01788-w. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Saaavedra-Trujillo C.H., et al. Consenso colombiano de atención, diagnóstico y manejo de la infección por SARS-COV-2/COVID-19 en establecimientos de atención de la salud - recomendaciones basadas en consenso de expertos e informadas en la evidencia. Infectio. 2020;24:1–102. [Google Scholar]
- 51.Franke C., Berlit P., Prüss H. Neurological manifestations of post-COVID-19 syndrome S1-guideline of the German society of neurology. Neurol. Res. Pract. 2022;4:28. doi: 10.1186/s42466-022-00191-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Ngeow W.C., Tang L., Ho J.Y., Tay H.W., Wong R.C.W., Ahmad M.S., et al. The provision of dental care to COVID-19 survivors: a concise review. Int Dent J. 2022;72:421–435. doi: 10.1016/j.identj.2022.05.009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.McGrath L.J., Scott A.M., Surinach A., Chambers R., Benigno M., Malhotra D. Use of the postacute sequelae of COVID-19 diagnosis code in routine clinical practice in the US. JAMA Netw Open. 2022;5 doi: 10.1001/jamanetworkopen.2022.35089. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.O'Hare A.M., Vig E.K., Iwashyna T.J., Fox A., Taylor J.S., Viglianti E.M., et al. Complexity and challenges of the clinical diagnosis and management of long COVID. JAMA Netw Open. 2022;5 doi: 10.1001/jamanetworkopen.2022.40332. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Dorfman D., Berger Z. Approving workplace accommodations for patients with long covid - advice for clinicians. N Engl J Med. 2023 doi: 10.1056/NEJMp2302676. in press. [DOI] [PubMed] [Google Scholar]
- 56.Gallegos M., Morgan M.L., Burgos-Videla C., Caycho-Rodríguez T., Martino P., Cervigni M. The impact of long Covid on people’s capacity to work. Ann. Work Expos. Health. 2023 doi: 10.1093/annweh/wxad029. in press. [DOI] [PubMed] [Google Scholar]
- 57.Update to living WHO guideline on drugs to prevent covid-19. BMJ. 2023;380:692. doi: 10.1136/bmj.p692. [DOI] [PubMed] [Google Scholar]
- 58.Rudofker E.W., Parker H., Cornwell W.K., 3rd An exercise prescription as a novel management strategy for treatment of long COVID. JACC Case Rep. 2022;4:1344–1347. doi: 10.1016/j.jaccas.2022.06.026. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Nikolich J., Rosen C.J. Toward comprehensive care for long covid. N Engl J Med 2023. in press. [DOI] [PubMed]
- 60.Manu P. Therapeutic vaccination is the most promising intervention for long COVID. Am J Therapeut. 2023 doi: 10.1097/MJT.0000000000001641. in press. [DOI] [PubMed] [Google Scholar]
- 61.Tran V.T., Perrodeau E., Saldanha J., Pane I., Ravaud P. Efficacy of first dose of covid-19 vaccine versus no vaccination on symptoms of patients with long covid: target trial emulation based on ComPaRe e-cohort. BMJ Med. 2023;2 doi: 10.1136/bmjmed-2022-000229. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Bonilla-Aldana D.K., Quintero-Rada K., Montoya-Posada J.P., Ramirez-Ocampo S., Paniz-Mondolfi A., Rabaan A.A., et al. SARS-CoV, MERS-CoV and now the 2019-novel CoV: have we investigated enough about coronaviruses? - a bibliometric analysis. Trav Med Infect Dis. 2020;33 doi: 10.1016/j.tmaid.2020.101566. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63.Davis H.E., McCorkell L., Vogel J.M., Topol E.J. Long COVID: major findings, mechanisms and recommendations. Nat Rev Microbiol. 2023;21:133–146. doi: 10.1038/s41579-022-00846-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.O'Donnell J.S., Chappell K.J. Chronic SARS-CoV-2, a cause of post-acute COVID-19 sequelae (Long-COVID)? Front Microbiol. 2021;12 doi: 10.3389/fmicb.2021.724654. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65.Vojdani A., Vojdani E., Saidara E., Maes M. Persistent SARS-CoV-2 infection, EBV, HHV-6 and other factors may contribute to inflammation and autoimmunity in long COVID. Viruses. 2023;15 doi: 10.3390/v15020400. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66.Zollner A., Koch R., Jukic A., Pfister A., Meyer M., Rössler A., et al. Postacute COVID-19 is characterized by gut viral antigen persistence in inflammatory bowel diseases. Gastroenterology. 2022;163:495–506.e8. doi: 10.1053/j.gastro.2022.04.037. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67.Xu E., Xie Y., Al-Aly Z. Long-term gastrointestinal outcomes of COVID-19. Nat Commun. 2023;14:983. doi: 10.1038/s41467-023-36223-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Chen B., Julg B., Mohandas S., Bradfute S.B. Viral persistence, reactivation, and mechanisms of long COVID. Elife. 2023;12 doi: 10.7554/eLife.86015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Stokel-Walker C. How long does SARS-CoV-2 stay in the body? BMJ. 2022;377:o1555. doi: 10.1136/bmj.o1555. [DOI] [PubMed] [Google Scholar]
- 70.Nussenblatt V., Roder A.E., Das S., de Wit E., Youn J.H., Banakis S., et al. Yearlong COVID-19 infection reveals within-host evolution of SARS-CoV-2 in a patient with B-cell depletion. J Infect Dis. 2022;225:1118–1123. doi: 10.1093/infdis/jiab622. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 71.Li L., Li S., Pan Y., Qin L., Yang S., Tan D., et al. An immunocompetent patient with high neutralizing antibody titers who shed COVID-19 virus for 169 days - China, 2020. China CDC weekly. 2021;3:688–691. doi: 10.46234/ccdcw2021.163. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 72.Pérez-Lago L., Aldámiz-Echevarría T., García-Martínez R., Pérez-Latorre L., Herranz M., Sola-Campoy P.J., et al. Different within-host viral evolution dynamics in severely immunosuppressed cases with persistent SARS-CoV-2. Biomedicines. 2021;9 doi: 10.3390/biomedicines9070808. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73.Scharf R.E., Anaya J.M. Post-COVID syndrome in adults-an overview. Viruses. 2023;15 doi: 10.3390/v15030675. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 74.Rojas M., Rodriguez Y., Acosta-Ampudia Y., Monsalve D.M., Zhu C., Li Q.Z., et al. Autoimmunity is a hallmark of post-COVID syndrome. J Transl Med. 2022;20:129. doi: 10.1186/s12967-022-03328-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 75.Anaya J.M., Herran M., Beltran S., Rojas M. Is post-COVID syndrome an autoimmune disease? Expet Rev Clin Immunol. 2022;18:653–666. doi: 10.1080/1744666X.2022.2085561. [DOI] [PubMed] [Google Scholar]
- 76.Anaya J.M., Rojas M., Salinas M.L., Rodriguez Y., Roa G., Lozano M., et al. Post-COVID syndrome. A case series and comprehensive review. Autoimmun Rev. 2021;20 doi: 10.1016/j.autrev.2021.102947. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77.Yamamoto S., Saito M., Tamura A., Prawisuda D., Mizutani T., Yotsuyanagi H. The human microbiome and COVID-19: a systematic review. PLoS One. 2021;16 doi: 10.1371/journal.pone.0253293. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 78.Wei N., Zhu G., Zhao T., Wang Y., Lou H., Li H., et al. Characterization of oral bacterial and fungal microbiome in recovered COVID-19 patients. BMC Microbiol. 2023;23:123. doi: 10.1186/s12866-023-02872-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 79.Glynne P., Tahmasebi N., Gant V., Gupta R. Long COVID following mild SARS-CoV-2 infection: characteristic T cell alterations and response to antihistamines. J Invest Med. 2022;70:61–67. doi: 10.1136/jim-2021-002051. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80.Phetsouphanh C., Darley D.R., Wilson D.B., Howe A., Munier C.M.L., Patel S.K., et al. Immunological dysfunction persists for 8 months following initial mild-to-moderate SARS-CoV-2 infection. Nat Immunol. 2022;23:210–216. doi: 10.1038/s41590-021-01113-x. [DOI] [PubMed] [Google Scholar]
- 81.Durstenfeld M.S., Peluso M.J., Peyser N.D., Lin F., Knight S.J., Djibo A., et al. Factors associated with long covid symptoms in an online cohort study. medRxiv. 2022 doi: 10.1093/ofid/ofad047. preprint. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 82.Zubchenko S., Kril I., Nadizhko O., Matsyura O., Chopyak V. Herpesvirus infections and post-COVID-19 manifestations: a pilot observational study. Rheumatol Int. 2022;42:1523–1530. doi: 10.1007/s00296-022-05146-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 83.Liu Q., Mak J.W.Y., Su Q., Yeoh Y.K., Lui G.C., Ng S.S.S., et al. Gut microbiota dynamics in a prospective cohort of patients with post-acute COVID-19 syndrome. Gut. 2022;71:544–552. doi: 10.1136/gutjnl-2021-325989. [DOI] [PubMed] [Google Scholar]
- 84.Arthur J.M., Forrest J.C., Boehme K.W., Kennedy J.L., Owens S., Herzog C., et al. Development of ACE2 autoantibodies after SARS-CoV-2 infection. PLoS One. 2021;16 doi: 10.1371/journal.pone.0257016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 85.Wallukat G., Hohberger B., Wenzel K., Furst J., Schulze-Rothe S., Wallukat A., et al. Functional autoantibodies against G-protein coupled receptors in patients with persistent Long-COVID-19 symptoms. J Transl Autoimmun. 2021;4 doi: 10.1016/j.jtauto.2021.100100. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 86.Proal A.D., VanElzakker M.B. Long COVID or post-acute sequelae of COVID-19 (PASC): an overview of biological factors that may contribute to persistent symptoms. Front Microbiol. 2021;12 doi: 10.3389/fmicb.2021.698169. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 87.Charfeddine S., Ibn Hadj Amor H., Jdidi J., Torjmen S., Kraiem S., Hammami R., et al. Long COVID 19 syndrome: is it related to microcirculation and endothelial dysfunction? Insights from TUN-EndCOV study. Front Cardiovasc Med. 2021;8 doi: 10.3389/fcvm.2021.745758. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 88.Pretorius E., Venter C., Laubscher G.J., Kotze M.J., Oladejo S.O., Watson L.R., et al. Prevalence of symptoms, comorbidities, fibrin amyloid microclots and platelet pathology in individuals with Long COVID/Post-Acute Sequelae of COVID-19 (PASC) Cardiovasc Diabetol. 2022;21:148. doi: 10.1186/s12933-022-01579-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 89.Spudich S., Nath A. Nervous system consequences of COVID-19. Science. 2022;375:267–269. doi: 10.1126/science.abm2052. [DOI] [PubMed] [Google Scholar]
- 90.Díaz-Guio D.A., Villamil-Gómez W.E., Dajud L., Pérez-Díaz C.E., Bonilla-Aldana D.K., Mondragon-Cardona A., et al. Will the Colombian intensive care units collapse due to the COVID-19 pandemic? Trav Med Infect Dis. 2020;38 doi: 10.1016/j.tmaid.2020.101746. [DOI] [PubMed] [Google Scholar]
- 91.Edgar M., Selvaraj S.A., Lee K.E., Caraballo-Arias Y., Harrell M., Rodriguez-Morales A.J. Healthcare workers, epidemic biological risks - recommendations based on the experience with COVID-19 and Ebolavirus. Inf Med. 2022;30:168–179. doi: 10.53854/liim-3002-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 92.Sánchez-Duque J.A., Arce-Villalobos L.R., Rodríguez-Morales A.J. [Coronavirus disease 2019 (COVID-19) in Latin America: role of primary care in preparedness and response] Atención Primaria. 2020;52:369–372. doi: 10.1016/j.aprim.2020.04.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 93.Ortiz-Martínez Y., Garcia-Robledo J.E., Vásquez-Castañeda D.L., Bonilla-Aldana D.K., Rodriguez-Morales A.J. Can Google® trends predict COVID-19 incidence and help preparedness? The situation in Colombia. Trav Med Infect Dis. 2020;37 doi: 10.1016/j.tmaid.2020.101703. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 94.Escalera-Antezana J.P., Lizon-Ferrufino N.F., Maldonado-Alanoca A., Alarcón-De-la-Vega G., Alvarado-Arnez L.E., Balderrama-Saavedra M.A., et al. Clinical features of the first cases and a cluster of Coronavirus Disease 2019 (COVID-19) in Bolivia imported from Italy and Spain. Trav Med Infect Dis. 2020;35 doi: 10.1016/j.tmaid.2020.101653. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 95.Rodriguez-Morales A.J., Paniz-Mondolfi A.E., Faccini-Martínez Á A., Henao-Martínez A.F., Ruiz-Saenz J., Martinez-Gutierrez M., et al. The constant threat of zoonotic and vector-borne emerging tropical diseases: living on the edge. Front Trop Dis. 2021;2 doi: 10.3389/fitd.2021.676905. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 96.Müller L.S., Reiners S., Becker J., Hertel G. Long-term effects of COVID-19 on work routines and organizational culture - a case study within higher education's administration. J Bus Res. 2023;163 doi: 10.1016/j.jbusres.2023.113927. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 97.Landhuis E.W. How primary care physicians can recognize and treat long COVID. JAMA. 2023;329:1727–1729. doi: 10.1001/jama.2023.6604. [DOI] [PubMed] [Google Scholar]
- 98.Rodriguez-Morales A.J., León-Figueroa D.A., Romaní L., McHugh T.D., Leblebicioglu H. Vaccination of children against COVID-19: the experience in Latin America. Ann Clin Microbiol Antimicrob. 2022;21:14. doi: 10.1186/s12941-022-00505-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 99.Solante R., Alvarez-Moreno C., Burhan E., Chariyalertsak S., Chiu N.C., Chuenkitmongkol S., et al. Expert review of global real-world data on COVID-19 vaccine booster effectiveness and safety during the omicron-dominant phase of the pandemic. Expet Rev Vaccine. 2023;22:1–16. doi: 10.1080/14760584.2023.2143347. [DOI] [PubMed] [Google Scholar]
- 100.SLIPE Guía sobre Vacunación para COVID en Niños. https://slipe.org/web/wp-content/uploads/2023/04/Publicacion-vacunas-covid-ninios.pdf. 2023