Abstract
Immunoglobulin A (Chan in J Allergy Clin Immunol 134:1394–14014e4, 2014), the second most abundant immunoglobulin in serum, plays an important role in mucosal homeostasis. In human serum, there are two subclasses of IgA, IgA1 (≅ 90%) and IgA2 (≅ 10%), transcribed from two distinct heavy chain constant regions. This study evaluated the serum concentrations of total IgA, IgA1, and IgA2, and total IgG, IgG1, IgG2, IgG3, and IgG4 in T2-high asthmatics compared to healthy controls and the presence of gender-related variations of immunoglobulins. Total IgA levels were increased in asthmatics compared to controls. Even more marked was the increase in total IgA in male asthmatics compared to healthy male donors. IgA1 were increased only in male, but not in female asthmatics, compared to controls. Concentrations of IgG2, but not IgG1, IgG3, and IgG4, were reduced in asthmatics compared to controls. IgG4 levels were reduced in female compared to male asthmatics. In female asthmatics, IgA and IgA1 levels were increased in postmenopause compared to premenopause. IgA concentrations were augmented in mild, but not severe asthmatics. A positive correlation was found between IgA levels and the age of patients and an inverse correlation between serum concentrations of IgA2 and IgE in asthmatics. A positive correlation between total IgA or IgA2 and IgG2 was found in asthmatics. These results highlight a gender dimorphism in IgA subclasses in male and female T2-high asthmatics. More adequate consideration of immunological gender disparity in asthma may open new opportunities in personalized medicine by optimizing diagnosis and targeted therapy.
Supplementary Information
The online version contains supplementary material available at 10.1007/s10238-022-00828-x.
Keywords: Asthma, Gender dimorphism, IgA, IgA1, IgA2, Immunoglobulins
Introduction
Accumulating evidence indicates that gender has an impact on gene expression in various inflammatory diseases [2–6]. Males and females differ in their immunological responses to antigens and show distinctions in innate and adaptive immune responses [7]. Certain immunological sex differences are present throughout life, whereas others are only apparent before puberty and after menopause, suggesting that both genes and hormones are involved. It is important to acknowledge gender differences when considering the prevalence of various diseases between males in females. Under the Severe Asthma Research Program (SARP), the gender difference in asthma incidence, prevalence, and severity was assessed [8]. Between the age of 4 and 14 years, asthma was more prevalent in boys compared to girls. However, after puberty, asthma became more prevalent and severe in women [9]. Interestingly, after menopause, asthma becomes more severe in males [10]. Moreover, female patients experience more symptoms when compared to males, resulting in a poorer quality of life [9]. Even though gender-related differences in asthma prevalence and clinical features have been described, the mechanisms underlying this phenomenon have been incompletely elucidated.
Besides gender, aging profoundly influences the immune system [11–14]. In humans, the serum concentrations of IgG and IgA generally tend to increase slightly with age [15]. In postmenopausal women, changes in the immune system have been attributed to estrogen deprivation [16]. Sex hormones modulate both humoral and cell-mediated immune responses [17].
Immunoglobulin A [1] is the most produced antibody class in the body (≅ 60 mg/kg/day) and the predominant antibody in mucosal surfaces, where it plays an important role in mucosal homeostasis [18–20]. At mucosal surfaces, a joining (J) chain is added to IgA when it is synthesized forming primarily dimers [21]. The dimers bind to the poly-Ig receptor (pIgR) expressed at the basolateral side of mucosal epithelial cells before being transported to the apical side of the cells where it is released into the lumen by proteolytic cleavage [22]. Unlike IgA produced at mucosal surfaces, serum IgA is predominantly monomeric and not joined to the J chain or the secretory component [23]. In humans, IgA represents the second most prevalent immunoglobulin in the serum [24, 25]. There are two subclasses of human IgA, IgA1 and IgA2, transcribed from two distinct heavy chain constant regions, with the first one dominating in serum and most tissues and the second mainly secreted at the mucosal surfaces [26, 27]. Human IgA1 and IgA2 are encoded by different genes, α1 and α2, respectively, located on chromosome 14 [24, 28]. The two IgA subclasses have different stability and effector functions due to highly significant differences in the hinge region and glycosylation patterns [29, 30]. In human serum, the predominant IgA form is monomeric with a subclass distribution of about 90% IgA1 and 10% IgA2 [27, 29]. It has become clear that serum IgA1 has specific immunological functions independent from the role of secretory IgA [29]. Although the pathogenic role of IgE in asthma is well-established [31–33], the complex interplay of IgE, IgG, and IgA subclasses in allergic diseases has been recently reviewed [34].
Asthma is a heterogeneous group of inflammatory respiratory disorders characterized by distinct phenotypes (T2-high and T2-low) and variable clinical course [35–38]. The majority of asthmatic patients fall into the T2-high phenotype characterized by increased IgE and FeNO, hypereosinophilia, and overexpression of Th2 cytokines [35, 37]. T2-low asthma is presumably a heterogeneous condition incompletely understood [36, 38, 39].
To the best of our knowledge, the serum concentrations of IgG1 and IgA2 subclasses in asthma have not been reported so far. The aim of the study was twofold: first, to evaluate the serum concentrations of IgA (IgA1, IgA2) and IgG (IgG1, IgG2, IgG3, IgG4) subclasses in adult T2-high asthmatics compared to age-matched healthy controls; second, to investigate the presence or absence of gender-related variations of serum levels of IgA and IgG subclasses between male and female asthmatics and controls.
Materials and methods
Patients and methods
This case-control study was carried out at the Center for Basic and Clinical Immunology Research (CISI) of the Department of Translational Medical Sciences, University of Naples Federico II (Naples, Italy), from September 2020 to October 2021. Forty-three Caucasian asthmatic patients (mean age 46.7 ± 15.8 years) were recruited in the outpatient clinic of the Division of Allergy and Clinical Immunology. Fifty-five volunteers were enrolled as healthy matched controls (mean age 43.8 ± 9.5 years). The study was approved by the Ethics Committee of the University of Naples Federico II, School of Medicine (Prot. 198/18), and informed consent was obtained from all participants prior to collection of blood according to recommendations from the Declaration of Helsinki. All participants were enrolled if adherent to stringent exclusion and inclusion criteria and provided written informed consent to participate in the study. Patients were eligible for enrollment in the study if they were aged 18–70 years and had a clinical diagnosis of asthma according to Global Initiative for Asthma [GINA] 2021 criteria [40]. Key exclusion criteria for both healthy controls and asthmatics were acute and chronic infections, bronchiectasis, primary and secondary immunodeficiencies, autoimmune diseases, malignancies, cystic fibrosis, patient-reported smoking history or the onset of respiratory symptoms after the age of 40 years in current or previous smokers with a smoking history of at least 10 pack-years. None of the asthmatic patients has been or was treated with allergen-specific immunotherapy [41] or monoclonal antibodies anti-IgE, anti-IL-5/IL-5Rα, or anti-IL-4Rα [42–44]. Forty out of 43 patients were treated with daily low-dose of inhaled glucocorticoids (ICS) therapy [fluticasone propionate (FP), 100–200 μg or equivalent] plus two additional controllers (e.g., a long-acting β2-agonist and/or leukotriene receptor antagonist and/or long-acting muscarinic agonist); 3/43 of patients were treated with daily medium-dose of ICS (FP, 250–500 μg or equivalent); 6/43 of patients were on oral glucocorticoids (mean daily prednisone intake 11.6 mg/die). Table 1 shows the demographic and clinical characteristics of the patients and healthy volunteers included in the study. The following parameters were evaluated: the on-treatment forced expiratory volume in 1 s (FEV1, in liters), the score on the Asthma Control Test (ACT) [45], serum IgE, total IgA and subclasses (IgA1 and IgA2), and total IgG and subclasses (IgG1, IgG2, IgG3, IgG4). Pulmonary function test (Quark PTF, COSMED, Pavona di Albano, Italy) was performed according to the American Thoracic Society/European Respiratory Society (ATS/ERS) guidelines [36]. FEV1, Forced Vital Capacity (FVC), and FEV1/FVC were measured, and the best of three forced maneuvers was recorded. Results were expressed both as absolute values and as a percentage of the predicted values referred to European Respiratory Society (ERS) reference values [35]. The Body Mass Index (BMI) was calculated as body weight [46]/height2 (m2) [46]. Peripheral blood leukocyte counts were measured using an automated hematology analyzer [47].
Table 1.
Demographic and clinical characteristics of healthy controls and asthma patients
| Characteristics | Healthy controls | Asthma patients | p-value |
|---|---|---|---|
| Subjects, n° | 55 | 43 | NA |
| Age (years) | 43.8 ± 9.5 | 46.7 ± 15.8 | 0.54 |
| Sex, male/female | 32/23 | 11/32 | NA |
| BMI (Kg/m2) | 25.79 ± 3.24 | 26.01 ± 4.46 | 0.82 |
| Smokers, n°(%) | None | None | NA |
| Age of asthma diagnosis | NA | 28.4 ± 18.8 | NA |
| Annualized Asthma Exacerbation Rate (AAER) | NA | 0.53 ± 1 | NA |
| ACT (score) | NA | 16.3 ± 5.2 | NA |
| Allergic Rhinitis, n° (%) | None | 37 (86.1) | NA |
| CRSsNP, n° (%) | None | 13 (30.02) | NA |
| CRSwNP, n° (% | None | 7 (16.3) | NA |
| FEV1 (L/s) | 3.72 ± 0.88 | 2.44 ± 0.82 | **** |
| FEV1 (%) | 106.3 ± 11.74 | 78.85 ± 21.05 | **** |
| FEV1/FCV ratio (%) | 100 ± 9.44 | 93.26 ± 13.38 | NS |
| FEF25–75 (%) | 110 ± 18.5 | 75.47 ± 36.23 | **** |
| ICS use (%) | None | 83.7 | NA |
| LABA use (%) | None | 74.4 | NA |
| LTRA use (%) | None | 44.2 | NA |
| LAMA use (%) | None | 4.7 | NA |
| OCS use, n (%) | None | 6 (14.0) | NA |
| Dose of OCS (mg/d), PRED equivalent | None | 11.6 ± 10.3 | NA |
CRSsNP chronic sinusitis without nasal polyps, CRSwNP chronic sinusitis withnasal polyps, FEV1 Forced expiratory volume in the 1st second; FVC Forced vital capacity; FEV1/FCV ratio (%) actual ratio of the two parameters; FEF25−75 forced expiratory flow between 25 and 75% of FVC; ICS Inhaled glucocorticoids; OCS Oral glucocorticoids; LABA Long-acting ß-2 agonist; LTRA Leukotriene-receptor antagonist; LAMA Long-acting muscarinic agonist; ACT asthma control test; BMI Body mass index. PRED prednisone; NA not applicable; *p < 0.05; **p < 0.01; ***p < 0.0005; ****p < 0.0001
Measurement of serum immunoglobulins
Serum samples from venous blood were stored in aliquots at − 80 °C until tested. Total IgE, IgG and subclasses (IgG1, IgG2, IgG3, IgG4), and IgA were measured by nephelometry using Behring BN™ II System (Siemens Healthcare Diagnostics Ltd, Erlangen, Germany). Calibration was performed using N protein standard SL (OQIM), according to Sanguin nephelometric standard M1590 (based on WHO67/97 reference serum) [48]. The precision evaluation (coefficient of variation: CV) for the measurement of IgG and IgG subclasses was done according to the Clinical and Laboratory Standards Institute (CLSI) EP05-A3 guidelines [49]. The intra-assay CVs ranged from 1.8 to 3.6%. The linearity for the measurement of IgG and IgG subclasses (coefficient of determination: R2) was assessed according to the CLSI EP06-A guidelines [50]. The R2 values ranged from 0.97 to 0.99. IgA1 and IgA2 subclasses were assessed by using the Binding Site SPAPLUS® turbidimetric analyzer (The Binding Site, Birmingham, UK). The CVs were 1.4% (IgA1) and 1.7% (IgA2). The correlation coefficients were 0.99 (IgA1) and 0.99 (IgA2). IgE were measured by chemiluminescent immunoassay using Immunolite 2000 (Siemens Healthcare Diagnostics Ltd, Erlangen, Germany). The CV was 2.9%, and the coefficient of correlation was 0.99.
Statistical analysis
Statistical analysis was performed by using GraphPad Prism 8 software (GraphPad Software, La Jolla, CA, USA). Data are expressed as mean ± standard deviation (SD) of the indicated number of experiments. Values from groups were compared by Student’s t test or Mann–Whitney U test based on the parametric or nonparametric distribution of the continuous variables. One-way analysis of variance (ANOVA) followed by Tukey’s post hoc was used for multiple comparisons. For the correlation analyses, Pearson’s correlation method was used. P values less than 0.05 were considered significant.
Results
Demographic and clinical characteristics of asthma patients and healthy controls
The demographic and clinical characteristics of healthy donors and asthma patients are given in Table 1. The median age was 46.7 ± 15.8 years for asthmatics and 43.8 ± 9.5 years for healthy controls. Thirty-two patients (74.4%) were female and 11 (25.6%) were male. None of healthy controls and asthma patients were smokers. All patients had a T2-high phenotype based on skin test positivity and/or specific IgE (65.2%), hypereosinophilia (34.8%), and increased FeNO levels. Asthmatic patients had an annualized asthma exacerbations rate (AAER) of 0.53 and an ACT score of 16.3 ± 5.2. Allergic rhinitis (86.1%) and chronic rhinosinusitis without nasal polyps (30.2%) and with nasal polyps (CRSwNP) (16.3%) were comorbidities of asthmatics. FEV1 in asthmatics was lower in healthy controls (2.44 ± 0.82 L/s vs. 3.72 ± 0.88 L/s; p < 0.0001).
Serum concentrations of IgE, IgA1, and IgA2 subclasses in asthma patients and healthy controls
The serum concentrations of IgE, total IgA, IgA1, and IgA2 subclasses in controls and asthmatics are given in Table 2, which also reports the concentrations of these immunoglobulin classes and subclasses in male and female subjects. As expected, serum IgE concentrations were significantly increased (p < 0.0001) in all asthmatic subjects irrespectively of gender (Table 2). Total serum IgA levels were also increased (p < 0.05) in asthmatics compared to controls (Fig. 1A). Even more marked (p < 0.01) was the increase in total serum IgA in male asthmatics when compared to healthy male donors (Fig. 1B). By contrast, the serum concentrations of IgA were not different between female asthmatics and controls (Table 2).
Table 2.
Serum concentrations of IgE, IgA, IgA1, and IgA2 subclasses in healthy controls and asthma patients
| Laboratory data | Healthy controls | Asthma patients | p-value |
|---|---|---|---|
| Serum total IgE (Log 10) | |||
| Total | 1713 | 2563 | **** |
| Male | 1613 | 2565 | **** |
| Female | 1694 | 2453 | **** |
| Serum IgA (g/L) | |||
| Total | 1.95 ± 0.70 | 2.39 ± 0.94 | * |
| Male | 1.96 ± 0.62 | 3.142 ± 1.05 | ** |
| Female | 1.94 ± 0.79 | 2.105 ± 0.83 | NS |
| Serum IgA1 (g/L) | |||
| Total | 1.530 ± 0.57 | 1.708 ± 0.74 | NS |
| Male | 1.568 ± 0.57 | 2.223 ± 0.91 | * |
| Female | 1.486 ± 0.57 | 1.526 ± 0.59 | NS |
| Serum IgA2 (g/L) | |||
| Total | 0.437 ± 0.25 | 0.369 ± 0.18 | NS |
| Male | 0.462 ± 0.29 | 0.408 ± 0.21 | NS |
| Female | 0.398 ± 0.19 | 0.356 ± 0.17 | NS |
NA not applicable; NS not significant. *p < 0.05; **p < 0.01; ****p < 0.0001
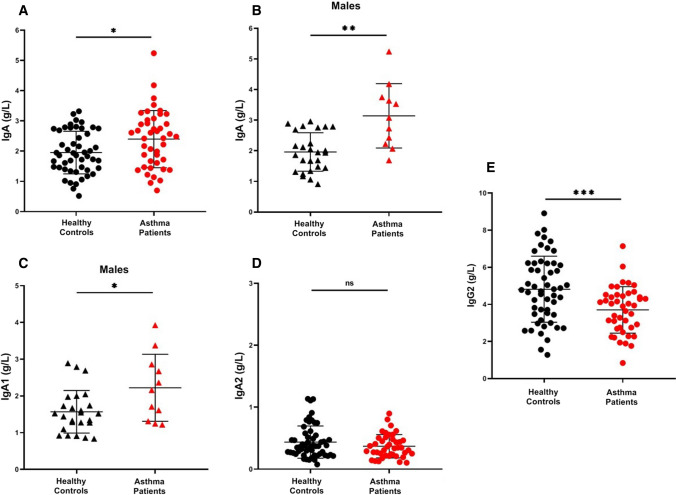
Fig. 1.
Serum concentrations of IgA in healthy controls and asthma patients (a) Serum concentrations of IgA in healthy male controls and asthma patients (b) Serum concentration of IgA1 in healthy male controls and asthma patients (c) Serum concentrations of IgA2 in healthy controls and asthma patients (d) Serum concentrations of IgG2 in healthy controls and asthma patients (e) Data are presented as scatter plots with mean ± SD. Significance was tested with two sided Student’s t test. *p < 0.05; **p < 0.01; ***p < 0.001
In human serum, IgA1 represents the major (≅ 90%) IgA subclass [27]. Therefore, we measured serum IgA1 and IgA2 subclasses in asthmatics and controls. Serum IgA1 did not differ between these two groups. However, when subjects were analyzed by gender, we found that serum IgA1 levels were significantly increased (p < 0.05) in male asthmatics compared to controls (Fig. 1C), but not in females (Table 2). IgA2 represents approximately 10% of serum IgA [27]. The serum concentrations of IgA2 did not differ between asthmatics and controls in both males and females (Table 2).
Serum concentrations of total IgG and subclasses in asthma patients and healthy controls
Serum concentrations of total IgG did not differ between asthmatics and controls in both males and females (Table 3). Similarly, IgG1, IgG3, and IgG4 subclasses did not differ between asthmatics and healthy donors in both males and females (Table 3). By contrast, concentrations of IgG2 were lower in asthmatics when compared to controls (p < 0.001) (Fig. 1E). The latter difference was particularly evident in males (p < 0.0001) but not in females (Table 3).
Table 3.
Serum concentrations of IgG and IgG subclasses in healthy controls and asthma patients
| Laboratory data | Healthy controls | Asthma patients | p-value |
|---|---|---|---|
| Serum IgG (g/L) | |||
| Total | 10.71 ± 2.1 | 10.38 ± 2.4 | NS |
| Male | 11.50 ± 1.7 | 10.04 ± 2.1 | NS |
| Female | 9.78 ± 2 | 10.49 ± 2.5 | NS |
| Serum IgG1 (g/L) | |||
| Total | 7.15 ± 1.4 | 7.52 ± 2.2 | NS |
| Male | 7.44 ± 1.2 | 7.06 ± 2.7 | NS |
| Female | 6.86 ± 1.6 | 7.67 ± 2.1 | NS |
| Serum IgG2 (g/L) | |||
| Total | 4.81 ± 1.7 | 3.70 ± 1.2 | *** |
| Male | 5.51 ± 1.5 | 3.92 ± 0.9 | **** |
| Female | 3.86 ± 1.5 | 3.62 ± 1.3 | NS |
| Serum IgG3 (g/L) | |||
| Total | 0.31 ± 0.3 | 0.34 ± 0.2 | NS |
| Male | 0.33 ± 0.3 | 0.31 ± 0.1 | NS |
| Female | 0.27 ± 0.1 | 0.34 ± 0.2 | NS |
| Serum IgG4 (g/L) | |||
| Total | 0.89 ± 0.6 | 0.86 ± 0.9 | NS |
| Male | 0.99 ± 0.4 | 1.5 ± 1.3 | NS |
| Female | 0.74 ± 0.7 | 0.63 ± 0.6 | NS |
NS not significant. *p < 0.05. ****p < 0.0001
Gender-specific differences of serum immunoglobulins in asthma patients
The previous results highlighted unexpected gender-specific differences in total IgA and IgA1 (Table 2). Therefore, we systematically compared gender-specific differences of all serum immunoglobulins examined (IgE, total IgA, IgA1, IgA2, total IgG, IgG1, IgG2, IgG3, and IgG4) in asthma patients (Table 4).
Table 4.
Gender-specific differences in asthma patients
| Laboratory data | Asthmatic males | Asthmatic females | p-value |
|---|---|---|---|
| Serum total IgE (Log 10) | 2565 | 2453 | NS |
| Serum IgA (g/L) | 3.142 ± 1.05 | 2.105 ± 0.83 | *** |
| Serum IgA1 (g/L) | 2.223 ± 0.91 | 1.526 ± 0.59 | * |
| Serum IgA2 (g/L) | 0.408 ± 0.21 | 0.356 ± 0.17 | NS |
| Serum IgG (g/L) | 10.04 ± 2.1 | 10.49 ± 2.5 | NS |
| Serum IgG1(g/L) | 7.06 ± 2.7 | 7.67 ± 2.1 | NS |
| Serum IgG2(g/L) | 3.92 ± 0.9 | 3.62 ± 1.3 | NS |
| Serum IgG3 (g/L) | 0.31 ± 0.1 | 0.34 ± 0.2 | NS |
| Serum IgG4 (g/L) | 1.5 ± 1.3 | 0.63 ± 0.6 | * |
NS not significant. *p < 0.05; ***p < 0.001
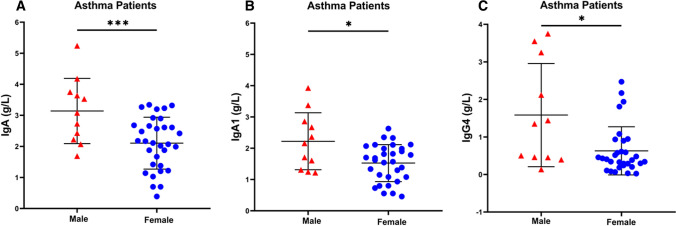
Figure 2A shows that serum concentrations of total IgA were markedly increased (p < 0.001) in males when compared to female asthmatics. Examining serum concentrations of IgA1, we found that asthmatic males had higher values than females (p < 0.05) (Fig. 2B). Interestingly, also the concentrations of IgG4 were increased (p < 0.05) in male asthmatics compared to females (Fig. 2C). Concentrations of other IgA and IgG subclasses did not differ between male and female asthmatics (Table 4).
Fig. 2.
Serum concentration of IgA (a), IgA1 (b) and IgG4 (c) in male and female asthma patients. Data are presented as scatter plots with mean ± SD. Significance was tested with two-sided Student’s t test. *p < 0.05; ***p < 0.001
Serum concentrations of IgA pre- and postmenopause in female asthma patients
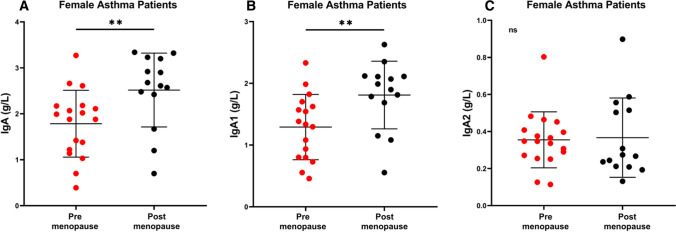
Gender differences in asthma incidence, prevalence, and severity have been started to be appreciated [8]. Moreover, menopause can affect asthma severity [10]. Besides gender, aging profoundly influences the innate and adaptive immune system [11–14]. When we evaluated the effects of menopause on total IgA and IgA subclasses in asthmatics, we found that serum concentrations of total IgA were significantly increased (p < 0.01) after menopause (Fig. 3A). Similarly, the serum levels of IgA1 were increased (p < 0.01) after menopause (Fig. 3B). The specificity of this observation was supported by the finding that serum concentrations of IgA2 were not affected by menopause in female asthma subjects (Fig. 3C). Similarly, serum levels of IgG and their subclasses and IgE did not differ in controls and asthmatics between pre- and postmenopause (data not shown).
Fig. 3.
Serum concentrations of IgA (a), IgA1 (b), and IgA2 (c) in pre- (mean age 33.6 ± 10 years) and postmenopause (mean age 60.3 ± 5.1 years) female asthmatic patients. Data are presented as scatter plots with mean ± SD. Significance was tested with two-sided Student’s t test. **p < 0.01
Correlations between asthma severity and serum concentration of IgA
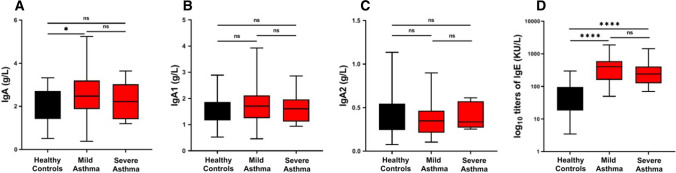
The alterations of serum concentrations of total IgA and IgA1 in asthmatics prompted us to investigate the possible correlations between asthma severity and the concentrations of these immunoglobulins. Figure 4A shows that serum levels of total IgA were increased in mild, but not in severe asthmatics compared to controls. Serum concentrations of IgA1 in mild and severe asthmatics did not differ from controls (Fig. 4B), whereas IgA2 levels were reduced in both mild and severe asthma patients vs. controls (Fig. 4C). As expected, IgE levels were significantly increased (p < 0.0001) in both mild and severe asthmatics (Fig. 4D).
Fig. 4.
Serum concentrations of IgA (a), IgA1 (b), IgA2 (c) and IgE (d) in healthy controls, mild, and severe asthmatics. Data are presented as box plots with medians and interquartile ranges plus whiskers ranging from min to max. Significance was tested using one-way ANOVA followed by Tukey’s post hoc. *p < 0.05; ****p < 0.0001
Correlations between serum concentrations of IgA and age of asthmatics and controls
Serum levels of IgG and IgA tend to increase slightly with age [15]. In adult healthy subjects, there was no correlation between serum concentrations of IgA, IgA1, and IgA2 and the age of donors (data not shown). By contrast, we found a positive correlation (r = 0.36; p < 0.05) between serum levels of total IgA and the age of asthmatics (Supplementary Fig. 1). No significant correlations were found between the age of asthmatics and serum concentrations of both IgA1 and IgA2 (data not shown).
Correlations between serum concentrations of IgE and IgA subclasses in asthmatics and controls
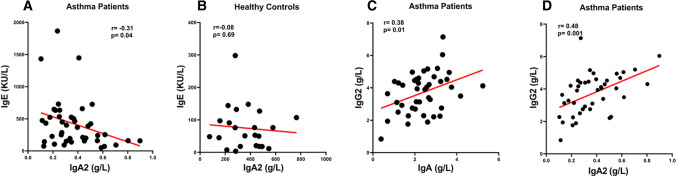
The pathogenic role of IgE in asthma and allergic disorders is well-established [31–33]. The role of IgA subclasses in asthma has been recently emphasized [34]. We found an inverse correlation (r = −0.31; p < 0.05) between serum concentrations of IgA2 and IgE in asthmatics (Fig. 5A) but not in controls (Fig. 5B). No correlations were found between serum IgE and total IgA and IgA1 in both normal donors and asthmatics (data not shown).
Fig. 5.
Correlations between serum concentrations of IgA2 and IgE in asthma patients (a) and healthy controls (b). Correlations between serum concentrations of IgA (c) or IgA2 (d) and IgG2 in asthma patients. Significance was tested with Pearson’s correlation method. *p < 0.05; ***p < 0.001
Correlations between serum concentrations of IgA and IgG subclasses in asthmatics and controls
We investigated possible correlations between serum concentrations of IgA and IgG subclasses in asthmatics and controls. There was no correlation between total IgA and IgG in both controls and asthmatics (data not shown). Similarly, there was no correlation between total IgA and IgG1, IgG2, IgG3, and IgG4 in healthy subjects (data not shown). In asthmatics, there was a correlation between serum concentrations of total IgA and IgG2 (r = 0.38; p < 0.01) (Fig. 5C). Similarly, there was a correlation (r = 0.48; p < 0.001) between serum concentrations of IgA2 and IgG2 (Fig. 5D). As expected, we found close correlations between serum levels of total IgG and IgG1 (r = 0.84; p < 0.0001), IgG2 (r = 0.40; p < 0.001), IgG3 (r = 0.32; p < 0.05), but not IgG4 (r = 0.09; NS) in asthmatics (Supplementary Fig. 2A, B, C, D). By contrast, we found a positive correlation between total IgG and only IgG1 in the control group (r = 0.68; p < 0.0001) (Supplementary Fig. 3A, B, C, D).
Discussion
In this study, we found that serum concentrations of IgE and total IgA were significantly increased in adult patients with T2-high asthma compared to healthy controls. IgA levels were increased in males but not in female asthmatics. Similarly, IgA1 were increased only in males, but not in female asthmatics, compared to controls. IgG2, but not IgG1, IgG3, and IgG4, was lower in asthmatics compared to healthy donors. This difference was significant in male but not in female asthmatics. In addition, IgG4 concentrations were reduced in females compared to male asthmatics. Considering the blocking activity of IgG4, the latter findings might explain why asthma tends to be more severe in women [9]. Total IgA and IgA1 were increased after menopause in female asthmatics. Serum concentrations of total IgA were increased in mild, but not severe asthmatics compared to controls, whereas IgE levels were increased in both groups of asthmatics. An inverse correlation between serum levels of IgA2 and IgE was found in asthmatics but not in controls. A positive correlation was found between IgG2 and both total IgA and IgA2 in asthmatics. Collectively, our results highlight a gender dimorphism in IgA subclasses in asthmatic patients.
Previous studies have examined the serum concentrations of total IgA in children [51–55] and adults with asthma [56–58]. Unfortunately, these studies have not evaluated the serum concentrations of IgA1 and IgA2 in both healthy controls and asthmatics. Moreover, these old studies did not examine the phenotype of asthmatic patients. In addition, serum concentrations of IgA increase with age [58, 59] and, therefore, results in children cannot be compared to those in adults. In a previous study on 15 normal subjects, 9 mild and 22 adults with severe asthma, serum IgA and IgG were decreased only in severe asthmatics compared to healthy controls [56]. These results apparently differ from our study in which we found that mild, but not severe T2-high asthmatics, had increased serum total IgA levels. In a population-based study, history of asthma was more prevalent in adults with selective IgA deficiency [57]. In a large population-based study of 1,136 adult patients with asthma, serum IgA increased with age and positively correlated to IgE [58]. To the best of our knowledge, our study is the first to evaluate the serum concentrations of total IgA, IgA1 and IgA2 in adult patients with T2-high asthma compared to age-matched healthy subjects. We found that serum levels of total IgA are increased in asthmatic subjects compared to controls, total IgA are lower in female asthmatics compared to males, and IgA1 subclass is increased in male asthmatics compared to controls. Steffen and collaborators have also demonstrated that serum IgA and IgA1, but not IgA2 are increased in healthy men compared to women [29].
Human IgG subclasses are similar in structure but differ in binding to receptors and accessory molecules, altering their functionality [60]. In this study, we found that serum levels of IgG2 were lower in asthmatics compared to controls. Moreover, IgG4 concentrations were decreased in females compared to male asthmatics. In a small number of asthmatics and healthy subjects, serum IgG in severe asthmatics were decreased when compared to controls [56]. By contrast, in a large study, allergic subjects had significantly higher IgG4 levels than controls and this difference was more pronounced for men than women [61].
IgG4 coexist as two isomers differing from other immunoglobulin subclasses in the disulfide bonding of hinge cysteines [34, 60]. In vivo, half-molecules of IgG4 recombine randomly with other half-molecules of IgG4, combining specificities of two molecules, resulting in monovalent-bispecific antibodies [62]. The resulting IgG antibody has low affinity for the activating Fc receptor for IgG (FcγR), while retaining high affinity for the inhibiting FcγRIIb. IgG, by interacting with FcγRIIb inhibits downstream signaling through FcεRI, thus preventing the release of proinflammatory mediators from basophils and mast cells [63]. IgG4 has therefore been characterized as “blocking antibody” in the context of allergic disorders [34]. The clinical relevance of lower concentrations of IgG4 in female compared to male asthmatics requires additional investigations.
Previous studies indicate that serum IgA levels increase with age [58, 59]. We found that serum concentrations of IgA are significantly correlated with the age of asthmatic patients. This observation prompted us to analyze total IgA, IgA1, and IgA2 in female asthmatics and controls before and after menopause. Interestingly, we found that total IgA and IgA1 are increased in postmenopausal asthmatic women. We cannot exclude the possibility that the alterations in total IgA and IgA1 levels found in post-menopausal asthmatic women are associated with the age of donors. However, the specificity of our observation is supported by the finding that serum IgA2 are not affected by menopause in female patients. This novel observation is not surprising because it is well-established that menopause has a distinct impact on the female immune system. For instance, several hormones (e.g., estradiol, testosterone, FH, FSH) can affect the immune responses [7, 64, 65]. At menopause, estradiol production in the ovaries ceases. Thereafter, only basal levels of progesterone are being synthesized by the adrenal glands. In aged women, dehydroepiandrosterone (DHEA) and testosterone levels decrease, yet follicle-stimulating hormone (FSH) and luteinizing hormone (LH) levels rise from the fourth decade onward [66]. In men, there is a slower yet steady decline in testosterone levels displaying no clear turning point [67]. For instance, female hormones can modulate IgA production in experimental models [68–70].
IgE is central to type I immediate allergic responses [31–33]. Allergen-specific IgA2 and polymeric IgA2 have been shown to be elevated following allergen immunotherapy [34, 71]. A positive correlation between serum IgA and IgE has been reported in adult asthmatics [58]. Our present study for the first time demonstrates an inverse correlation between serum IgE and IgA2 in asthmatics. Moreover, we found a positive correlation between IgG2 and both total IgA and IgA2 only in asthmatic patients. The latter observation is interesting because the types of antigens that could elicit IgG2 and IgA appear to be similar, as the majority of environmental antigens that induce IgA are glycosylated. Moreover, both IgA2 [27, 72] and IgG2 can form dimers [60]. Collectively, our results reveal a series of complex correlations between serum IgA2 and both IgE and IgG2 in asthmatics that require additional investigations.
Gender differences in serum IgA and IgA1 and to a lesser extent in IgG4 between male and female asthmatics could be explained by genetic, epigenetic and non-genetic factors (e.g., microbiota, lifestyle). At first sight, the findings that IgA, IgA1, and IgG4 are increased in male asthmatics versus females were surprising because nine genes corresponding to nine isotypes of heavy chains (i.e., μ, δ, γ1, γ2, γ3, γ4, α2 and ε) are located on chromosome 14 [73]. However, we cannot rule out the possibility that some of the ≅ 50 X-linked genes involved in the modulation of immunity [74] also dictate sex differences in immunoglobulin synthesis.
Epigenetic studies could help to address the molecular basis of disparities of serum IgA, IgA1, and IgG4 in male and female asthmatics. The possibility exists that sex hormones influence epigenetic factors (e.g., DNA methylation, chromatin conformation) [75, 76] that control immunoglobulin synthesis, thus playing a role in gender-dependent IgA, IgA1, and IgG4 disparities in male and female asthmatics.
Sex hormones, in particular androgens, seem critical in shaping the gut microbiota composition [77, 78]. There is growing evidence for gender dimorphism of gut microbiota in humans and other species [79–81], which may contribute to divergent development of the host immune system [82, 83]. Asthma development has been increasingly associated with gut and lung microbiome alterations [84, 85]. An aberrant IgA response to the gut microbiota precedes asthma development [86]. IgA regulates the composition and function of the gut microbiota and modulates its interaction with the host [20, 87]. Future studies should investigate the possible interactions between gut and lung microbiota, sex hormones and serum IgA subclasses in male and female asthmatics.
In adults, asthma is more prevalent and severe in women [9]. In addition, female patients experience more symptoms when compared to males [9]. Sex disparities in asthma remain poorly understood and could be influenced by lifestyle-associated allergy risk factors (e.g., exposure to cigarette smoke, diesel exhaust, detergents) [88]. It is difficult to control lifestyle in patient cohorts; however, the existence of lifestyle-dependent sex differences in IgA and IgG subclasses could be investigated by using appropriate experimental models of lung inflammation [27].
This study has several limitations that should be pointed out. The sample size of the asthma patient and healthy control cohorts investigated in the present study is limited. Further studies on larger cohorts of both healthy controls and asthmatics could better highlight the significance of gender dimorphism in IgA and IgG subclasses in these patients. For instance, we anticipate that it would be necessary to examine at least one order of magnitude larger cohorts to correlate alterations of serum IgA and IgG subclasses to lung function in asthmatic patients. Asthma is a heterogeneous group of inflammatory disorders characterized by distinct subtypes and variable clinical courses [35–38]. The patients included in this study were adults with a T2-high asthma phenotype of different severity (mild and severe). The limited sample size of patients did not allow to correlate the serum concentrations of IgA and IgG subclasses to T2-low or T2-high asthma [39, 89]. Finally, results might be confounded by glucocorticoid treatment [90], especially because the majority of the asthmatic participants were using high-dose ICS and some systemic glucocorticoids. The effects of high-dose ICS and systemic glucocorticoids on serum levels of IgA and IgG subclasses in asthmatics are not known.
Conclusions
Our study showing different levels of gender dimorphism in IgA subclasses in asthmatic patients might have translational relevance in clinical manifestations of asthma. First, we found that IgA and IgA1 were markedly increased in males, but not female asthmatics compared to controls. Similarly, IgG4 were augmented in male compared to female asthmatics. Second, within the female asthma population, IgA and IgA1 were increased after menopause compared to premenopause. IgA antibodies play important roles in protecting subjects from bacterial and viral infections at mucosal surfaces, including in the airways [91–93]. In this study, we found that females have lower levels of IgA, IgA1, and IgG4 compared to male asthmatics. It is tempting to speculate that lower serum concentrations of these antibodies in female asthmatics could contribute to the increased prevalence and severity of asthma in adult women [9]. Interestingly, after menopause, asthma becomes more severe in males [10] and serum levels of IgA/IgA1 are higher in postmenopause compared to premenopause in female asthmatics.
The impact of gender on disease biology and treatment outcomes is well-appreciated in medical disciplines, such as cardiology [94, 95] and oncology [96–98], whereas its relevance in allergy was thus far underestimated in both clinical and preclinical studies. More adequate consideration of the immunological basis of gender disparity in asthma may open new opportunities in personalized medicine by optimizing diagnosis and targeted therapy.
Supplementary Information
Below is the link to the electronic supplementary material.
Acknowledgements
The authors thank Dr. Gjada Criscuolo for her excellent managerial assistance in preparing this manuscript and the administrative staff (Dr. Roberto Bifulco, Dr. Anna Ferraro and Dr. Maria Cristina Fucci), without whom it would not be possible to work as a team. The authors apologize to the many researchers who have contributed importantly to the field and whose work was not cited due to space constraints.
Abbreviations
- ACT
Asthma control test
- BMI
Body max index
- ERS
European respiratory society
- DHEA
Dehydroepiandrosterone
- FcγR
Fc receptor for IgG
- FSH
Follicle-stimulating hormone
- FEV1
Forced expiratory volume in the 1st second
- FEF25–75
Forced expiratory flow between 25 and 75% of FVC
- FVC
Forced vital capacity
- GCP
Good clinical practice
- ICS
Inhaled glucocorticoids
- Ig
Immunoglobulin
- LABA
Long-acting ß-2 agonist
- LAMA
Long-acting muscarinic agonist
- LH
Luteinizing hormone
- LTRA
Leukotriene-receptor antagonist
- OCS
Oral glucocorticoids
- pIgR
Poly-Ig receptor
- PRED
Prednisone
- SARP
Severe asthma research program
Authors’ contribution
GV, RP, BC, GDS, MRG, GM, LP and GS designed and conducted laboratory studies, designed and performed data analysis, interpreted data, and drafted the manuscript. GV, RP, and LP interpreted data and edited the manuscript. All authors reviewed and approved the contents of the manuscript.
Funding
Open access funding provided by Università degli Studi di Napoli Federico II within the CRUI-CARE Agreement. This work was supported in part by grants from the CISI-Lab Project (University of Naples Federico II), TIMING Project and Campania Bioscience (Regione Campania), MIUR-PRIN 2017M8YMR8_005, AIRC (25123).
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Declarations
Conflict of interest
All authors declared they have no conflict of interest.
Consent for publication
Patients signed informed consent regarding publishing their data.
Ethics approval
The study was approved by the Ethics Committee of the University of Naples Federico II, School of Medicine (Prot. 198/18), and informed consent was obtained from all participants prior to collection of blood according to recommendations from the Declaration of Helsinki.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Footnotes
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Gilda Varricchi and Remo Poto Co-first authors.
Change history
7/24/2022
Missing Open Access funding information has been added in the Funding Note
Contributor Information
Gilda Varricchi, Email: gildanet@gmail.com.
Giuseppe Spadaro, Email: spadaro@unina.it.
References
- 1.Chan YC, Ramadani F, Santos AF, et al. Auto-anti-IgE: naturally occurring IgG anti-IgE antibodies may inhibit allergen-induced basophil activation. J Allergy Clin Immunol. 2014;134(6):1394–14014e4. doi: 10.1016/j.jaci.2014.06.029. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Oliva M, Munoz-Aguirre M, Kim-Hellmuth S et al., The impact of sex on gene expression across human tissues. Science 2020;369(6509). [DOI] [PMC free article] [PubMed]
- 3.van Eijk LT, Dorresteijn MJ, Smits P, et al. Gender differences in the innate immune response and vascular reactivity following the administration of endotoxin to human volunteers. Crit Care Med. 2007;35(6):1464–1469. doi: 10.1097/01.CCM.0000266534.14262.E8. [DOI] [PubMed] [Google Scholar]
- 4.Fish EN. The X-files in immunity: sex-based differences predispose immune responses. Nat Rev Immunol. 2008;8(9):737–744. doi: 10.1038/nri2394. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Faner R, Gonzalez N, Cruz T, Kalko SG, Agusti A. Systemic inflammatory response to smoking in chronic obstructive pulmonary disease: evidence of a gender effect. PLoS ONE. 2014;9(5):e97491. doi: 10.1371/journal.pone.0097491. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Han MK. Chronic obstructive pulmonary disease in women: a biologically focused review with a systematic search strategy. Int J Chron Obstruct Pulmon Dis. 2020;15:711–721. doi: 10.2147/COPD.S237228. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Klein SL, Flanagan KL. Sex differences in immune responses. Nat Rev Immunol. 2016;16(10):626–638. doi: 10.1038/nri.2016.90. [DOI] [PubMed] [Google Scholar]
- 8.Jarjour NN, Erzurum SC, Bleecker ER, et al. Severe asthma: lessons learned from the national heart, lung, and blood institute severe asthma research program. Am J Respir Crit Care Med. 2012;185(4):356–362. doi: 10.1164/rccm.201107-1317PP. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.NHIS, Center for disease control and prevention 2012.
- 10.Zein JG, Dweik RA, Comhair SA, et al. Asthma Is More Severe in Older Adults. PLoS ONE. 2015;10(7):e0133490. doi: 10.1371/journal.pone.0133490. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Gustafson CE, Kim C, Weyand CM, Goronzy JJ. Influence of immune aging on vaccine responses. J Allergy Clin Immunol. 2020;145(5):1309–1321. doi: 10.1016/j.jaci.2020.03.017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Busse PJ, Birmingham JM, Calatroni A, et al. Effect of aging on sputum inflammation and asthma control. J Allergy Clin Immunol. 2017;139(6):1808–1818. doi: 10.1016/j.jaci.2016.09.015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Mittelbrunn M, Kroemer G. Hallmarks of T cell aging. Nat Immunol. 2021;22(6):687–698. doi: 10.1038/s41590-021-00927-z. [DOI] [PubMed] [Google Scholar]
- 14.Varricchi G, Bencivenga L, Poto R, et al. The emerging role of T follicular helper (TFH) cells in aging: Influence on the immune frailty. Ageing Res Rev. 2020;61:101071. doi: 10.1016/j.arr.2020.101071. [DOI] [PubMed] [Google Scholar]
- 15.Suzuki K, Hirokawa K, Hatakeyama S. Age-related change of distribution of immunoglobulin containing cells in human bone marrow. Changes in patients with benign monoclonal gammopathy and multiple myeloma. Virchows Arch A Pathol Anat Histopathol. 1984;404(3):243–251. doi: 10.1007/BF00694890. [DOI] [PubMed] [Google Scholar]
- 16.Gameiro C, Romao F. Changes in the immune system during menopause and aging. Front Biosci (Elite Ed) 2010;2:1299–1303. doi: 10.2741/e190. [DOI] [PubMed] [Google Scholar]
- 17.Lahita RG. Sex steroids and the rheumatic diseases. Arthritis Rheum. 1985;28(2):121–126. doi: 10.1002/art.1780280202. [DOI] [PubMed] [Google Scholar]
- 18.Fagarasan S, Honjo T. Intestinal IgA synthesis: regulation of front-line body defences. Nat Rev Immunol. 2003;3(1):63–72. doi: 10.1038/nri982. [DOI] [PubMed] [Google Scholar]
- 19.Aleyd E, Heineke MH, van Egmond M. The era of the immunoglobulin A Fc receptor FcalphaRI; its function and potential as target in disease. Immunol Rev. 2015;268(1):123–138. doi: 10.1111/imr.12337. [DOI] [PubMed] [Google Scholar]
- 20.Rollenske T, Burkhalter S, Muerner L, et al. Parallelism of intestinal secretory IgA shapes functional microbial fitness. Nature. 2021;598(7882):657–661. doi: 10.1038/s41586-021-03973-7. [DOI] [PubMed] [Google Scholar]
- 21.Mestecky J, Zikan J, Butler WT. Immunoglobulin M and secretory immunoglobulin A: presence of a common polypeptide chain different from light chains. Science. 1971;171(3976):1163–1165. doi: 10.1126/science.171.3976.1163. [DOI] [PubMed] [Google Scholar]
- 22.Brandtzaeg P. Mucosal and glandular distribution of immunoglobulin components: differential localization of free and bound SC in secretory epithelial cells. J Immunol. 1974;112(4):1553–1559. [PubMed] [Google Scholar]
- 23.Leong KW, Ding JL. The unexplored roles of human serum IgA. DNA Cell Biol. 2014;33(12):823–829. doi: 10.1089/dna.2014.2639. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Kerr MA. The structure and function of human IgA. Biochem J. 1990;271(2):285–296. doi: 10.1042/bj2710285. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Mestecky J, Russell MW, Jackson S, Brown TA. The human IgA system: a reassessment. Clin Immunol Immunopathol. 1986;40(1):105–114. doi: 10.1016/0090-1229(86)90073-5. [DOI] [PubMed] [Google Scholar]
- 26.Brandtzaeg P, Johansen FE. Mucosal B cells: phenotypic characteristics, transcriptional regulation, and homing properties. Immunol Rev. 2005;206:32–63. doi: 10.1111/j.0105-2896.2005.00283.x. [DOI] [PubMed] [Google Scholar]
- 27.de Sousa-Pereira P, Woof JM, IgA: structure, function, and developability. Antibodies (Basel), 2019;8(4). [DOI] [PMC free article] [PubMed]
- 28.Woof JM, Kerr MA. The function of immunoglobulin A in immunity. J Pathol. 2006;208(2):270–282. doi: 10.1002/path.1877. [DOI] [PubMed] [Google Scholar]
- 29.Steffen U, Koeleman CA, Sokolova MV, et al. IgA subclasses have different effector functions associated with distinct glycosylation profiles. Nat Commun. 2020;11(1):120. doi: 10.1038/s41467-019-13992-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Kilian M, Reinholdt J, Lomholt H, Poulsen K, Frandsen EV. Biological significance of IgA1 proteases in bacterial colonization and pathogenesis: critical evaluation of experimental evidence. APMIS. 1996;104(5):321–338. doi: 10.1111/j.1699-0463.1996.tb00724.x. [DOI] [PubMed] [Google Scholar]
- 31.Gould HJ, Sutton BJ, Beavil AJ, et al. The biology of IGE and the basis of allergic disease. Annu Rev Immunol. 2003;21:579–628. doi: 10.1146/annurev.immunol.21.120601.141103. [DOI] [PubMed] [Google Scholar]
- 32.Ishizaka K, Ishizaka T, Hornbrook MM. Physico-chemical properties of human reaginic antibody. IV. Presence of a unique immunoglobulin as a carrier of reaginic activity. J Immunol. 1966;97(1):75–85. [PubMed] [Google Scholar]
- 33.Johansson SG, Bennich H. Immunological studies of an atypical (myeloma) immunoglobulin. Immunology. 1967;13(4):381–394. [PMC free article] [PubMed] [Google Scholar]
- 34.Shamji MH, Valenta R, Jardetzky T, et al. The role of allergen-specific IgE, IgG and IgA in allergic disease. Allergy. 2021;76:3627. [DOI] [PMC free article] [PubMed]
- 35.Fahy JV. Type 2 inflammation in asthma–present in most, absent in many. Nat Rev Immunol. 2015;15(1):57–65. doi: 10.1038/nri3786. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Kalchiem-Dekel O, Yao X, Levine SJ. Meeting the challenge of identifying new treatments for type 2-low neutrophilic asthma. Chest. 2020;157(1):26–33. doi: 10.1016/j.chest.2019.08.2192. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Peters MC, Wenzel SE. Intersection of biology and therapeutics: type 2 targeted therapeutics for adult asthma. Lancet. 2020;395(10221):371–383. doi: 10.1016/S0140-6736(19)33005-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Sze E, Bhalla A, Nair P. Mechanisms and therapeutic strategies for non-T2 asthma. Allergy. 2020;75(2):311–325. doi: 10.1111/all.13985. [DOI] [PubMed] [Google Scholar]
- 39.Fitzpatrick AM, Chipps BE, Holguin F, Woodruff PG. T2-"Low" asthma: overview and management strategies. J Allergy Clin Immunol Pract. 2020;8(2):452–463. doi: 10.1016/j.jaip.2019.11.006. [DOI] [PubMed] [Google Scholar]
- 40.Global Initiative for Asthma (GINA), Global strategy for asthma management and prevention. 2021.
- 41.Karacs J, Reithofer M, Kitzmuller C et al., Adjuvants and vaccines used in allergen-specific immunotherapy induce neutrophil extracellular traps. Vaccines (Basel), 2021;9(4). [DOI] [PMC free article] [PubMed]
- 42.Canonica GW, Senna G, Mitchell PD, et al. Therapeutic interventions in severe asthma. World Allergy Organ J. 2016;9(1):40. doi: 10.1186/s40413-016-0130-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Detoraki A, Di Capua L, Varricchi G, et al. Omalizumab in patients with eosinophilic granulomatosis with polyangiitis: a 36-month follow-up study. J Asthma. 2016;53(2):201–206. doi: 10.3109/02770903.2015.1081700. [DOI] [PubMed] [Google Scholar]
- 44.Bagnasco D, Ferrando M, Varricchi G, et al. Anti-Interleukin 5 (IL-5) and IL-5Ra biological drugs: efficacy, safety, and future perspectives in severe eosinophilic asthma. Front Med (Lausanne) 2017;4:135. doi: 10.3389/fmed.2017.00135. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Schatz M, Sorkness CA, Li JT, et al. Asthma Control Test: reliability, validity, and responsiveness in patients not previously followed by asthma specialists. J Allergy Clin Immunol. 2006;117(3):549–556. doi: 10.1016/j.jaci.2006.01.011. [DOI] [PubMed] [Google Scholar]
- 46.Vural P, Akgul C, Canbaz M. Effects of hormone replacement therapy on plasma pro-inflammatory and anti-inflammatory cytokines and some bone turnover markers in postmenopausal women. Pharmacol Res. 2006;54(4):298–302. doi: 10.1016/j.phrs.2006.06.006. [DOI] [PubMed] [Google Scholar]
- 47.Varricchi G, Modestino L, Poto R, et al. Neutrophil extracellular traps and neutrophil-derived mediators as possible biomarkers in bronchial asthma. Clin Exp Med. 2021 doi: 10.1007/s10238-021-00750-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Klein F, Skvaril F, Vermeeren R, Vlug A, Duimel WJ. The quantification of human IgG subclasses in reference preparations. Clin Chim Acta. 1985;150(2):119–127. doi: 10.1016/0009-8981(85)90262-1. [DOI] [PubMed] [Google Scholar]
- 49.Institute CLS, Evaluation of precision of quantitative measurement procedures: approved guideline-Third Edition. CLSI Document EP05-A3. Wayne, PA, 2014.
- 50.Institute CLS, Evaluation of the linearity of quantitative measurement procedures: a statistical approach; Approved guideline. CLSI Document EP06-A. Wayne, PA, 2003.
- 51.Ludviksson BR, Eiriksson TH, Ardal B, Sigfusson A, Valdimarsson H. Correlation between serum immunoglobulin A concentrations and allergic manifestations in infants. J Pediatr. 1992;121(1):23–27. doi: 10.1016/s0022-3476(05)82535-1. [DOI] [PubMed] [Google Scholar]
- 52.Ostergaard PA. IgA levels, bacterial carrier rate, and the development of bronchial asthma in children. Acta Pathol Microbiol Scand C. 1977;85(3):187–195. [PubMed] [Google Scholar]
- 53.Ostergaard PA, Eriksen J. Association between HLA-A1, B8 in children with extrinsic asthma and IgA deficiency. Eur J Pediatr. 1979;131(4):263–270. doi: 10.1007/BF00444347. [DOI] [PubMed] [Google Scholar]
- 54.Taylor B, Fergusson DM, Mahoney GN, Hartley WA, Abbott J. Specific IgA and IgE in childhood asthma, eczema and food allergy. Clin Allergy. 1982;12(5):499–505. doi: 10.1111/j.1365-2222.1982.tb01648.x. [DOI] [PubMed] [Google Scholar]
- 55.Siegler DI, Citron KM. Serum and parotid salivary IgA in chronic bronchitis and asthma. Thorax. 1974;29(3):313–316. doi: 10.1136/thx.29.3.313. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56.Balzar S, Strand M, Nakano T, Wenzel SE. Subtle immunodeficiency in severe asthma: IgA and IgG2 correlate with lung function and symptoms. Int Arch Allergy Immunol. 2006;140(2):96–102. doi: 10.1159/000092252. [DOI] [PubMed] [Google Scholar]
- 57.Urm SH, Yun HD, Fenta YA, et al. Asthma and risk of selective IgA deficiency or common variable immunodeficiency: a population-based case-control study. Mayo Clin Proc. 2013;88(8):813–821. doi: 10.1016/j.mayocp.2013.05.021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.Kim WJ, Choi IS, Kim CS, Lee JH, Kang HW. Relationship between serum IgA level and allergy/asthma. Korean J Intern Med. 2017;32(1):137–145. doi: 10.3904/kjim.2014.160. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Weber-Mzell D, Kotanko P, Hauer AC, et al. Gender, age and seasonal effects on IgA deficiency: a study of 7293 Caucasians. Eur J Clin Invest. 2004;34(3):224–228. doi: 10.1111/j.1365-2362.2004.01311.x. [DOI] [PubMed] [Google Scholar]
- 60.Vidarsson G, Dekkers G, Rispens T. IgG subclasses and allotypes: from structure to effector functions. Front Immunol. 2014;5:520. doi: 10.3389/fimmu.2014.00520. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Magnusson CG, Cesbron JY, Djurup R, Capron A, Johansson SG. Raised serum IgG4 levels in patients with atopy and filariasis: application of an automated particle-counting immunoassay using monoclonal antibody. Int Arch Allergy Appl Immunol. 1986;81(3):238–244. doi: 10.1159/000234141. [DOI] [PubMed] [Google Scholar]
- 62.van der Neut Kolfschoten M, Schuurman J, Losen M, et al. Anti-inflammatory activity of human IgG4 antibodies by dynamic Fab arm exchange. Science. 2007;317(5844):1554–1557. doi: 10.1126/science.1144603. [DOI] [PubMed] [Google Scholar]
- 63.Bruhns P, Fremont S, Daeron M. Regulation of allergy by Fc receptors. Curr Opin Immunol. 2005;17(6):662–669. doi: 10.1016/j.coi.2005.09.012. [DOI] [PubMed] [Google Scholar]
- 64.Giefing-Kroll C, Berger P, Lepperdinger G, Grubeck-Loebenstein B. How sex and age affect immune responses, susceptibility to infections, and response to vaccination. Aging Cell. 2015;14(3):309–321. doi: 10.1111/acel.12326. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65.Marquez EJ, Chung CH, Marches R, et al. Sexual-dimorphism in human immune system aging. Nat Commun. 2020;11(1):751. doi: 10.1038/s41467-020-14396-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66.Al-Azzawi F, Palacios S. Hormonal changes during menopause. Maturitas. 2009;63(2):135–137. doi: 10.1016/j.maturitas.2009.03.009. [DOI] [PubMed] [Google Scholar]
- 67.Bhasin S, Pencina M, Jasuja GK, et al. Reference ranges for testosterone in men generated using liquid chromatography tandem mass spectrometry in a community-based sample of healthy nonobese young men in the Framingham Heart Study and applied to three geographically distinct cohorts. J Clin Endocrinol Metab. 2011;96(8):2430–2439. doi: 10.1210/jc.2010-3012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Fink AL, Engle K, Ursin RL, Tang WY, Klein SL. Biological sex affects vaccine efficacy and protection against influenza in mice. Proc Natl Acad Sci U S A. 2018;115(49):12477–12512. doi: 10.1073/pnas.1805268115. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Christoforidou Z, Mora Ortiz M, Poveda C, et al. Sexual dimorphism in immune development and in response to nutritional intervention in neonatal piglets. Front Immunol. 2019;10:2705. doi: 10.3389/fimmu.2019.02705. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Wira CR, Sullivan DA. Estradiol and progesterone regulation of immunoglobulin A and G and secretory component in cervicovaginal secretions of the rat. Biol Reprod. 1985;32(1):90–95. doi: 10.1095/biolreprod32.1.90. [DOI] [PubMed] [Google Scholar]
- 71.Shamji MH, Kappen JH, Akdis M, et al. Biomarkers for monitoring clinical efficacy of allergen immunotherapy for allergic rhinoconjunctivitis and allergic asthma: an EAACI Position Paper. Allergy. 2017;72(8):1156–1173. doi: 10.1111/all.13138. [DOI] [PubMed] [Google Scholar]
- 72.Breedveld A, van Egmond M. IgA and FcalphaRI: pathological roles and therapeutic opportunities. Front Immunol. 2019;10:553. doi: 10.3389/fimmu.2019.00553. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73.Lefranc MP, Lefranc G, Immunoglobulins or Antibodies: IMGT((R)) bridging genes, structures and functions. Biomedicines, 2020; 8(9). [DOI] [PMC free article] [PubMed]
- 74.Meester I, Manilla-Munoz E, Leon-Cachon RBR, et al. SeXY chromosomes and the immune system: reflections after a comparative study. Biol Sex Differ. 2020;11(1):3. doi: 10.1186/s13293-019-0278-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 75.Nugent BM, Wright CL, Shetty AC, et al. Brain feminization requires active repression of masculinization via DNA methylation. Nat Neurosci. 2015;18(5):690–697. doi: 10.1038/nn.3988. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Fullwood MJ, Liu MH, Pan YF, et al. An oestrogen-receptor-alpha-bound human chromatin interactome. Nature. 2009;462(7269):58–64. doi: 10.1038/nature08497. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77.Markle JG, Frank DN, Mortin-Toth S, et al. Sex differences in the gut microbiome drive hormone-dependent regulation of autoimmunity. Science. 2013;339(6123):1084–1088. doi: 10.1126/science.1233521. [DOI] [PubMed] [Google Scholar]
- 78.Kim YS, Unno T, Kim BY, Park MS. Sex differences in gut microbiota. World J Mens Health. 2020;38(1):48–60. doi: 10.5534/wjmh.190009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 79.Org E, Mehrabian M, Parks BW, et al. Sex differences and hormonal effects on gut microbiota composition in mice. Gut Microbes. 2016;7(4):313–322. doi: 10.1080/19490976.2016.1203502. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80.Xiao L, Estelle J, Kiilerich P, et al. A reference gene catalogue of the pig gut microbiome. Nat Microbiol. 2016;1:16161. doi: 10.1038/nmicrobiol.2016.161. [DOI] [PubMed] [Google Scholar]
- 81.Sheng L, Jena PK, Liu HX, et al. Gender differences in bile acids and microbiota in relationship with gender dissimilarity in steatosis induced by diet and FXR inactivation. Sci Rep. 2017;7(1):1748. doi: 10.1038/s41598-017-01576-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 82.Cebra JJ. Influences of microbiota on intestinal immune system development. Am J Clin Nutr. 1999;69(5):1046S–S1051. doi: 10.1093/ajcn/69.5.1046s. [DOI] [PubMed] [Google Scholar]
- 83.Kabat AM, Srinivasan N, Maloy KJ. Modulation of immune development and function by intestinal microbiota. Trends Immunol. 2014;35(11):507–517. doi: 10.1016/j.it.2014.07.010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 84.Chung KF. Airway microbial dysbiosis in asthmatic patients: a target for prevention and treatment? J Allergy Clin Immunol. 2017;139(4):1071–1081. doi: 10.1016/j.jaci.2017.02.004. [DOI] [PubMed] [Google Scholar]
- 85.Lehtimaki J, Thorsen J, Rasmussen MA, et al. Urbanized microbiota in infants, immune constitution, and later risk of atopic diseases. J Allergy Clin Immunol. 2021;148(1):234–243. doi: 10.1016/j.jaci.2020.12.621. [DOI] [PubMed] [Google Scholar]
- 86.Dzidic M, Abrahamsson TR, Artacho A, et al. Aberrant IgA responses to the gut microbiota during infancy precede asthma and allergy development. J Allergy Clin Immunol. 2017;139(3):1017–1025 e14. doi: 10.1016/j.jaci.2016.06.047. [DOI] [PubMed] [Google Scholar]
- 87.Pabst O, Izcue A. Secretory IgA: controlling the gut microbiota. Nat Rev Gastroenterol Hepatol. 2022;19:149. [DOI] [PubMed]
- 88.Akdis CA. Does the epithelial barrier hypothesis explain the increase in allergy, autoimmunity and other chronic conditions? Nat Rev Immunol. 2021;21(11):739–751. doi: 10.1038/s41577-021-00538-7. [DOI] [PubMed] [Google Scholar]
- 89.Peters MC, Ringel L, Dyjack N, et al. A transcriptomic method to determine airway immune dysfunction in T2-High and T2-low asthma. Am J Respir Crit Care Med. 2019;199(4):465–477. doi: 10.1164/rccm.201807-1291OC. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 90.Klaustermeyer WB, Wong SC, Schoettler JJ, Gianos ME, Heiner DC. Quantitative immunoglobulins and IgG subclasses in patients with corticosteroid-dependent reversible airway obstruction. Ann Allergy. 1989;63(4):327–330. [PubMed] [Google Scholar]
- 91.Mazanec MB, Kaetzel CS, Lamm ME, Fletcher D, Nedrud JG. Intracellular neutralization of virus by immunoglobulin A antibodies. Proc Natl Acad Sci U S A. 1992;89(15):6901–6905. doi: 10.1073/pnas.89.15.6901. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 92.Kulkarni V, Ruprecht RM. Mucosal IgA responses: damaged in established HIV infection-yet, effective weapon against HIV transmission. Front Immunol. 2017;8:1581. doi: 10.3389/fimmu.2017.01581. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 93.Maurer MA, Meyer L, Bianchi M, et al. Glycosylation of human IgA directly inhibits influenza A and other sialic-acid-binding viruses. Cell Rep. 2018;23(1):90–99. doi: 10.1016/j.celrep.2018.03.027. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 94.Tamargo J, Rosano G, Walther T, et al. Gender differences in the effects of cardiovascular drugs. Eur Heart J Cardiovasc Pharmacother. 2017;3(3):163–182. doi: 10.1093/ehjcvp/pvw042. [DOI] [PubMed] [Google Scholar]
- 95.Regitz-Zagrosek V, Oertelt-Prigione S, Prescott E, et al. Gender in cardiovascular diseases: impact on clinical manifestations, management, and outcomes. Eur Heart J. 2016;37(1):24–34. doi: 10.1093/eurheartj/ehv598. [DOI] [PubMed] [Google Scholar]
- 96.Wagner AD, Oertelt-Prigione S, Adjei A, et al. Gender medicine and oncology: report and consensus of an ESMO workshop. Ann Oncol. 2019;30(12):1914–1924. doi: 10.1093/annonc/mdz414. [DOI] [PubMed] [Google Scholar]
- 97.Ozdemir BC, Csajka C, Dotto GP, Wagner AD. Sex differences in efficacy and toxicity of systemic treatments: an undervalued issue in the era of precision oncology. J Clin Oncol. 2018;36(26):2680–2683. doi: 10.1200/JCO.2018.78.3290. [DOI] [PubMed] [Google Scholar]
- 98.Clocchiatti A, Cora E, Zhang Y, Dotto GP. Sexual dimorphism in cancer. Nat Rev Cancer. 2016;16(5):330–339. doi: 10.1038/nrc.2016.30. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Data Availability Statement
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.