Abstract
Major research breakthroughs over the past 30 years in the field of substance use prevention have served to: (1) enhance understanding of pharmacological effects on the central and peripheral nervous systems and the health and social consequences of use of psychoactive substances, particularly for children and adolescents; (2) delineate the processes that increase vulnerability to or protect from initiation of substance use and progression to substance use disorders (SUDs) and, based on this understanding, (3) develop effective strategies and practices to prevent the initiation and escalation of substance use. The challenge we now face as a field is to “normalize” what we have learned from this research so that it is incorporated into the work of those involved in supporting, planning, and delivering prevention programming to populations around the world, is integrated into health and social service systems, and helps to shape public policies. But we wish to go further, to incorporate these effective prevention practices into everyday life and the mind-sets of the public, particularly parents and educators. This paper reviews the advances that have been made in the field of prevention and presents a framework and recommendations to achieve these objectives generated during several meetings of prevention and implementation science researchers sponsored by the International Consortium of Universities for Drug Demand Reduction (ICUDDR) that guides a roadmap to achieve “normalization.”
Keywords: Substance use, Prevention, Effective strategies, Service system, Normalization, Vulnerability, Registries
Introduction
The accumulation of knowledge regarding causal pathways to initiation of psychoactive substance use1 and the progression from substance use to misuse and substance use disorders (SUDs) has implicated an interrelationship between individual personal characteristics (e.g., psychological factors, physical and cognitive development), genetics, and socioenvironmental factors (e.g., parenting, family and school bonding, community norms, and structural factors) (Logan-Greene et al., 2019; Rose et al., 2019). This understanding of how the interaction between the individual and the micro- and macro-level environments can result in vulnerability has led to the development of a number of interventions that are effective, not only for preventing substance use, but also other problem behaviors (Allen et al., 2016; Astor et al., 2019; Faggiano et al., 2014; MacArthur et al., 2018; Paschall & Grube, 2020; Paschall et al., 2009). Despite this progress, incorporating evidence-based interventions and practices into the work of prevention professionals and the relevant work of other health, education, and social service professionals has been a challenge. We have also yet to reach key influencers—such as policymakers and public officials, parents and educators—with the knowledge and practices amassed to date; thus, there is a lack of appreciation for their potential to improve outcomes for young people. Toward that end, we assert that an integrative framework that considers findings from etiological and applied prevention research, as well as what we have learned from implementation science and practice, has the potential to facilitate the normalization of effective prevention strategies and practices into service program protocols, educational, health and social systems and policies, and the mindsets of the general public so they are incorporated into daily practices. The goal of this paper is to set forth recommendations as to how to increase the accessibility and utility of this information for practitioners and socializing agents within families, schools, and communities. We build on the work of others who have addressed this need, recognizing that to “normalize” effective practices within each of the groups mentioned above will require different approaches to achieve this goal. Ultimately, increasing the scalability and sustainably of these prevention strategies through normalization will enable our children and young people to flourish.
To support the recommendations, it is first necessary to provide an overview of the accumulated knowledge regarding factors and processes that reinforce and build resilience in families and children to support and enhance positive, healthy, and productive communities. We subsequently focus on two aspects of normalizing prevention. First is the implementation and dissemination approach, which is fraught with challenges. Although the field has germinated numerous evidence-based preventive interventions and policies, systematically, sustainably and reliably delivering them in our communities has not met with widescale success. Doing so largely revolves around the need to familiarize prevention professionals (who work with children/adolescents and their families, schools, and care providers) with the science, knowledge, and practices generated to date. As it stands, the overall lack of awareness and access to information from prevention science has stalled its translation to practical and clinical settings. And because implementing programs and interventions will never achieve population-level impacts without the supportive systems and prevention-oriented mindsets in place, we devote the remaining sections to the second aspect of normalizing prevention, which involves the embedding of core components or active ingredients of interventions (e.g., teaching life skills, reducing stress) and other practices known to improve behavioral outcomes (e.g., warm parenting, economic provisions to parents) into our daily lives, from households to human service systems and public policies. Achieving this end requires that these core components be reliably identified and that we determine effective means of incorporating these activities into common practice. In essence, the goal is to foster a “culture of prevention” with the potential to yield wholesale and equitable benefits to all in our society.
The Current Status of Substance Use Prevention Research
Findings from longitudinal studies on adolescents initiated in the mid-1970s (e.g., Brook et al., 1989; Huba et al., 1981; Kandel & Logan, 1984) were summarized by David Hawkins and his colleagues (1992) at the University of Washington. This major paper outlined indicators of risk associated with the initiation of substance use, and, to a lesser extent, factors that exert a protective effect against use. These factors have been confirmed and expanded upon in subsequent research (Hopfer et al., 2003; Rhee et al., 2003; Stone et al., 2012) and now form the basis for common liability models that focus on interrelationships between genetic (e.g., susceptibility to novelty seeking), neurobiological (e.g., weak prefrontal to limbic system connectivity, cognitive deficits) psychosocial (e.g., aggressiveness, inattention), and environmental/contextual/structural factors (e.g., poverty, child maltreatment, inequities) (Sloboda et al., 2012; Sloboda, 2018, Fishbein et al., 2016). Liability based on these interactions manifests as the level of risk of initiating substance use, progressing to the use of other substances, and onto developing a substance use disorder (SUD) (e.g., Rose et al., 2019; Vanyukov et al., 2012). This ever-growing body of evidence identifying risk and protective factors and delineating their effects on behavior points to mechanisms that can be altered via an environmental change to improve outcomes. Accordingly, preventive interventions and policies have been designed to target and improve liability conditions and the mechanisms they impact, with the ultimate goal of creating the most positive and supportive environments. This line of work has been resoundingly successful, resulting in dozens of evidence-based preventive interventions (NASEM, 2019).
Despite this progress, there is a regrettable lack of awareness among prevention professionals about the foundations laid in prevention science for understanding risk and protective factors, their impacts on social, emotional and physical health, and the potential for well-targeted interventions to move the mechanistic needle and, in effect, improve outcomes (e.g., Brook et al., 1989; Fishbein & Dariotis, 2019; Huba et al., 1981; Kandel & Logan, 1984; Sloboda, 2018; Trucco & Hartmann, 2021). Moreover, many prevention professionals are unfamiliar with or have not accessed existing resources, such as standards and registries (e.g., Blueprints for Healthy Development (https://www.blueprintsprograms.org/), California Evidence-Based Clearinghouse (https://www.cebc4cw.org/topic/substance-abuse-prevention-child-adolescent-programs/), EMCDDA Xchange Prevention registry (https://www.emcdda.europa.eu/best-practice/xchange)) Burkhardt et al., 2015; Means et al., 2015) to obtain guidance. This lack of utility is in part due to the historical focus of registries on efficacy rather than effectiveness, the research-laden language and complex organization of registry platforms are not accessible to many end-users, and the challenges in implementation, adoption, and scaling up (Buckley et al., 2020).
Increased familiarity with these linkages and processes, as well as an awareness of existing resources, can guide professionals in the selection of appropriate evidence-based preventive interventions that map to individual and contextual influences at the family, school, community, and systems levels. And because multiple conditions and mechanisms are in play, multiple integrated or systems of prevention services are often needed for any defined population or problem. The International Standards on Drug Use Prevention published by the United Nations Office on Drugs and Crime (UNODC) and the World Health Organization (WHO) (2013, 2018) is a resource that can provide guidance to policy makers and practitioners regarding evidence-based preventive interventions and policies salient and acceptable to any given community, as well as their availability, executability, and scalability (Campello et al., 2014).
In addition to increasing the availability of and capacity to implement evidence-based interventions and policies, prevention researchers have developed tools to screen those at risk to determine both the sources and extent of liability and vulnerability, such as the Drug Use Screening Inventory (https://www.einsight.net/solutions/dusi/), and the Problem Oriented Screening Instrument for Teenagers (https://www.emcdda.europa.eu/html.cfm/index4439EN.html) that identify problem behaviors and risk status of adolescents, or the Youth Risk Index (personalytics.rti.org/) that provides measures of propensity or risk for problem health behaviors and addresses the needs of younger children aged 9 to 13 (Ridenour et al., 2015). These tools—when used by trained school staff, health and prevention professionals, and others who counsel children and adolescents—provide guidance for “next steps” to address any imminent behavioral or substance use problem. Survey tools based on the experiences of national surveys are also available to examine the epidemiology of substance use across any given population. Examples of these research tools include the U.S. Youth Risk Behavioral Survey from the Centers for Disease Control (https://www.cdc.gov/healthyyouth/data/yrbs/index.htm), Monitoring the Future (https://monitoringthefuture.org/), National Survey on Drug Use and Health (https://www.samhsa.gov/data/data-we-collect/nsduh-national-survey-drug-use-and-health), and, in Europe, the European School Survey Project on Alcohol and Other Drugs (http://espad.org/).
In summary, over the past 40 years, there has been an incremental building of information and products to enhance prevention efforts at multiple levels. We have yet to sort out how best to enhance awareness about prevention generally and increase the utility of existing tools and interventions specifically to increase their uptake and ensure they are implemented with fidelity by end-users. The only available studies on the adoption of research-based or evidence-based preventive interventions were conducted by Hallfors and Godette (2002) and Ringwalt and colleagues (2002, 2008, 2009, 2011) in the USA. These researchers conducted surveys with administrators of a representative sample of schools in the USA and found that even when the delivery of research-based prevention programming was mandated, and at times funded, the adoption of these programs occurred in less than half of middle schools and less than 20% of high schools. There remains a large divide between research and practice.
Facilitating Research-to-Practice Efforts
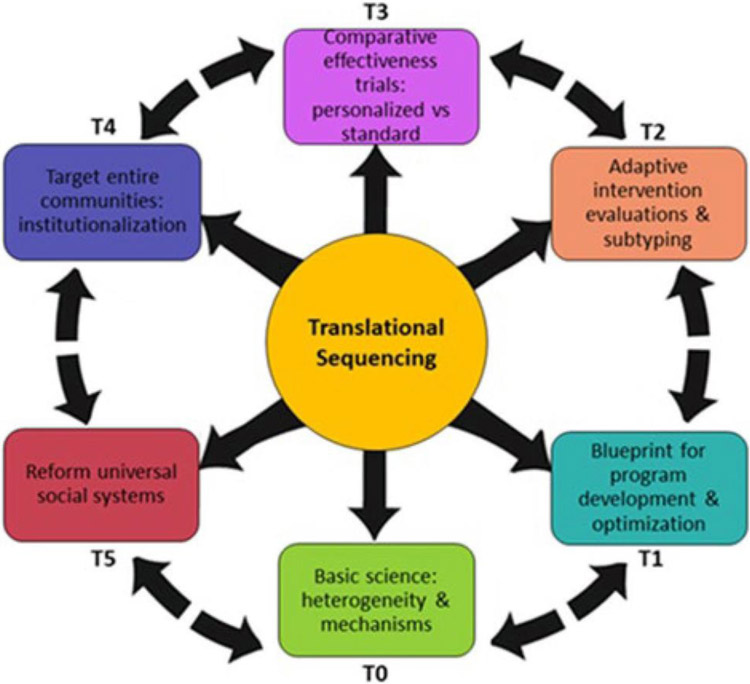
Thus, it is incumbent upon researchers and practitioners working in concert to determine how to effectively transfer this knowledge to improve the lives of children, young people, families, and communities. This “challenge” has prompted a number of efforts including the concept of translational sequencing (Fishbein et al., 2016) and implementation science (Fixsen & Blase, 2008) which includes the exploration, adoption/preparation, implementation, sustainment (EPIS) framework (Moullin et al., 2019; May & Finch, 2009). Fishbein and colleagues (2016) have laid out a spectrum of prevention research phases to facilitate the process of translating the existing knowledge and practices generated by prevention science into real-world changes in community practice, societal systems and government policies. The spectrum begins with incentivizing basic researchers to address the question of “what works best for whom, why and under what circumstances.” Thus, basic science findings can more directly contribute to the design of program components that target underlying mechanisms in the phenomena we wish to prevent. The next step is to subject resultant programs to efficacy and effectiveness trials that determine the best fit for different subgroups. Once verified, programs can be implemented in “real world” settings, with ongoing evaluation and refinement to determine what will work best in different communities and cultural settings. The process continues with a scaling up of those programs with established benefits and resonance with communities and then legislative and agency-level policy reforms to sustainably transform social systems (see Fig. 1). The bi- and multi-directional arrows suggest interactions among basic and prevention researchers, policy makers, and practitioners. Although not addressed specifically, the approach also suggests that there is a coordinating body(ies) to mobilize these efforts.
Fig. 1.
Spectrum of translational phases
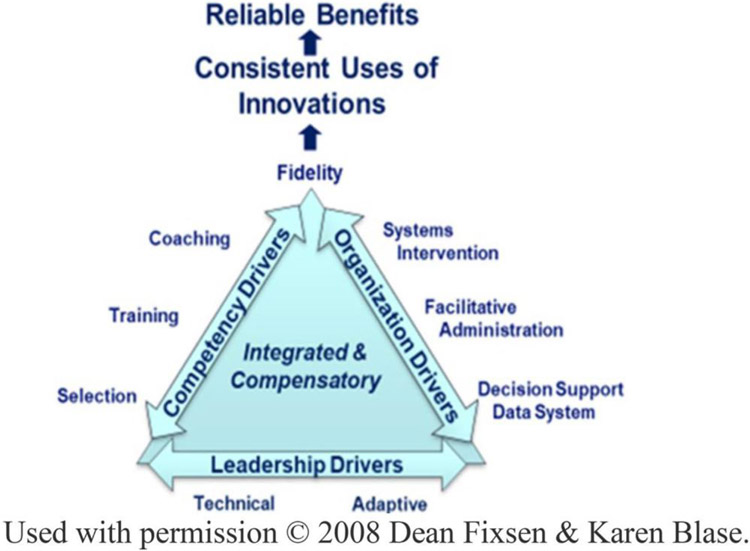
One of the most successful approaches to implementation and sustainability was developed by Fixsen and Blase (2008), summarized in Fig. 2. In this model, implementation drivers are the “drivers of change.” The three depicted here: competency drivers, organizational drivers, and leadership drivers have been demonstrated to be associated with the adoption of an “innovation” and the extent to which the adoption is implemented and sustained over time.
Fig. 2.
Drivers of change
Examples of these successes include motivational interviewing (e.g., Miller et al., 2004; Martino et al., 2008); positive behavioral interventions and supports (McIntosh et al., 2016); and behavioral health care practices (Margolies et al., 2017). All three disseminate information to support: (1) the use of the intervention itself and (2) the use of implementation best practices for training, coaching, fidelity assessment, organization/management, leadership, and system support. Users with intervention expertise become the best trainers, coaches, fidelity assessors, and so forth, with the additional support for learning implementation skills (e.g., Ogden et al., 2005). They already know the intervention (e.g., met fidelity criteria multiple times) and “only” need to learn, for example, coaching skills or fidelity assessment skills. While this approach has been successful, the resources and time that have been required to normalize their practice have been immense and issues of fidelity remain (Hall et al., 2016).
Furthermore, May and colleagues (2015, 2022) suggest 4 domains for normalization: coherence, cognitive participation, collective action, and reflexive monitoring. This team, the normalization process group, also has designed a tool kit that can be used to implement an innovative strategy and can identify barriers to implementation and suggests ways to overcome them (https://normalization-process-theory.northumbria.ac.uk/about-us/).
While there is still much to learn, a great deal of knowledge is available, yet unused. By merging prevention science with dissemination and implementation science, we can identify the next steps to further reduce substance use and its negative impacts on children, families, communities, and society at large. In the next section, we identify three populations that would benefit most from what has been learned from prevention science and describe how to best transfer this knowledge for implementation.
Normalizing Evidence-Based Prevention Practices, Messages, and Policies
Relative to the second aspect of normalization—the embedding of prevention principles and practices into daily life, there are three end-user groups to whom these efforts might be aimed. The first two are the prevention workforce which includes those who are (1) officially designated as prevention professionals/specialists and (2) delivering prevention services even if not self-identifying as prevention professionals, such as social workers, family service providers, educators, and health professionals. These groupings should also consider students who may enroll in the ever-growing graduate programs in prevention science or in related fields (e.g., social work, sociology, psychology, public health) that are essentially prevention-oriented (Pavlovská et al., 2019). The third includes individuals who socialize human beings from birth to death by shaping belief systems, attitudes, and behaviors relevant to our social, emotional, and physical health. These socialization agents are found in our micro-level environments and include parents and family, educators, members of faith-based communities, peers, and colleagues at work. In our macro-level environments, socialization occurs via rules, regulations, and laws at all governmental levels, as well as our physical and socio-economic-cultural milieus.
The literature lays out three primary challenges in incorporating into practice what we know works from research. The first is developing a “culture” that supports a nurturing society (Biglan & Embry, 2013; Biglan et al., 2017; Crowley & Jones, 2017; Wilson et al., 2014). The second is identifying what should be translated. Embry and Biglan (2008) have identified core components or “kernels,” such as verbal praise or time outs at the individual level and taxation at the policy level, which can be integrated into everyday life. The third is communicating these ideas via credible messaging that supports the ability to improve the lives of children and adults, to demonstrate when and how to incorporate them into practice, and to supply “behavioral” indicators of successful implementation (Biglan et al., 2020).
These challenges are not unique for substance use prevention (e.g., Garcia & Calantone, 2002; Sloboda et al., 2014). Over the past 2 decades, there has been a focus in the social and health services arenas, including the prevention field in general, on the delivery of evidence-based interventions (EBIs) grounded in rigorous evaluations and research. This push to promote the dissemination and diffusion of EBIs as rapidly as possible has given rise to a new field of study called implementation science (Madon et al., 2007). Eccles and colleagues (2009) define implementation research as “the scientific study of methods to promote the systematic uptake of clinical research findings and other evidence-based practices into routine practice, and hence to improve the quality (effectiveness, reliability, safety, appropriateness, equity, efficiency) of health care. It includes the study of influences on healthcare professional and organizational behavior.” Implementation science integrates and extends a number of disciplines, including operations research, health services research, industrial engineering, and management science (Schackman, 2010), but it also draws from a range of other related disciplines, including decision science, epidemiology, statistics, ethics, sociology, anthropology, and economics (Sloboda et al., 2014). Implementation science includes a number of constructs that are relevant such as the normalization process theory and approaches that build on Rogers’ diffusion of innovation theory (Rogers, 1995). These efforts attempt to identify factors that enhance or deter the adoption and implementation of innovations, particularly those that involve the uptake of evidence-based preventive interventions and policies.
The processes of implementation are illustrated in the Consolidated Framework for Implementation Research (Damschroder et al., 2009; Kirk et al., 2015) which assumes that, in any complex intervention, there are core components that are essential and others that can be adapted to the individuals involved within the setting (both societal and organizational) they inhabit. The process of implementation takes into context the environment, the practice, and the dissemination and implementation support activities that are necessary to bring evidence to widescale use.
Meta-analyses have been conducted around several diffusion and dissemination processes, such as the use of printed educational materials (Farmer et al., 2008), professional guidelines (Grimshaw et al., 2006), educational outreach visits (O’Brien et al., 2007), continuing education meetings and workshops (Forsetlund et al., 2009), and audit and feedback procedures (Ivers et al., 2012). All of these reviews found small effects of the strategy employed and recommended employing combinations of these strategies (Grimshaw et al., 2006). Although no formal evaluations of these systems have been conducted, studies of the adoption of recommended interventions indicate that only a small percentage of the targeted providers actually incorporate them into practice (e.g., Brownson et al., 2007; Hallfors et al., 2007; Ringwalt et al., 2002, 2008).
The prevention field has developed several complex systems approaches that have demonstrated success in the implementation of evidence-based prevention strategies, including the Getting to Outcomes (Chinman et al., 2008), Communities That Care (Fagan et al., 2011), and Promoting School-Community-University Partnerships to Enhance Resilience (PROSPER)(Crowley et al., 2012). The research of Palinkas and colleagues (2020) supports the importance of collaborations as important elements of sustainability. These systems approaches provide both guidance and tools necessary to identify and define the problem of concern and provide interventions that have the potential to ameliorate the targeted problem. However, these programs also face obstacles, not only in the availability of resources needed to integrate evidence-based strategies into ongoing programming, but also the acceptance and embrace of new content or delivery strategies. Minor changes in already existing delivery processes for instance will generally be better received than major changes requiring in-depth training. The intervention itself is not only important in the dissemination phase of the implementation process, but has implications at all phases (Chambers et al., 2013).
Innovation, whether within a service delivery system or a factory, must address two aspects of the process: the product, which in our case, is the intervention, and the delivery of the product or service (Cooper, 1998; Sloboda et al., 2014). Recognition of this dichotomy suggests that some evidence-based prevention approaches may be more readily accepted and implemented than others. It also suggests that the introduction of any new prevention approach must address these two aspects and use methodologies and techniques appropriate for the group involved. In the next section, we describe potential target populations and suggest approaches that could be used to “normalize” prevention principles and practices.
Target Populations for Normalizing Prevention Principles and Practices
The primary targets for this information are wide-ranging: prevention professionals, other health and social service professionals and educators who deliver prevention programming, and the general population, including parents, policy makers, law enforcement agencies, and other entities that influence the lives of our young people.
Prevention Professionals
The term prevention professionals encompasses those who are responsible for implementing preventive interventions or enforcing prevention policies. Prevention professionals do not all share the same training, either in terms of the level of education (high school, college, or graduate school) or in the discipline (e.g., sociology, psychology, public health, health education, social work). There has been an effort to address this problem with the Substance Abuse and Mental Health Services Administration (SAMHSA) developing the Substance Use Prevention Framework to provide a guide for prevention planning processes and the Prevention Core Competencies (SAMHSA, 2021). The framework provides a learning health system model that incorporates local data into an assessment of needs and resources that inform the selection of evidence-based interventions that are targeted to local need. It outlines implementation strategies and issues and informs implementers on how to use data to apply continuous assessment to improve outcomes. The core competencies outline the expected knowledge, skills and attitudes for people who identify as prevention professionals. They are built around the domains of systems thinking, assessment, capacity building, planning, implementation science, and evaluation which match onto the elements of the prevention framework.
There has not been a universal movement to train prevention practitioners or students in professional schools in the field of prevention science. New efforts include the Universal Prevention Curriculum delivered through the International Society of Substance Use Professionals (https://www.issup.net/training/universal-prevention-curriculum), the European Monitoring Centre on Drugs and Drug Addiction (https://www.emcdda.europa.eu/emcdda-home-page_en) and the non-profit organization, Applied Prevention Science International (https://www.apsintl.org). A growing number of universities have established degree programs based on prevention science (Pavlovská et al., 2019). However, these remain primarily in the USA, and the content of these programs varies. In the USA, the Prevention Technology Transfer Centers, established and funded by SAMHSA (https://pttcnetwork.org/) have initiated webinar series and self-paced courses around specific topics and are in the process of training trainers across regional centers to provide a basic course in prevention science and its application to practice with a focus on SAMHSA’s Core Competencies.
Through the International Certification and Reciprocity Consortium’s (IC&RC) Prevention Think Tank, the field now has a code of ethics that is comparable to other professional groups. Still lacking for the field to be fully professionalized is a self-governing body of practitioners with the authority to define the issues prevention professionals address and how best to address them and to sanction professionals who do not abide by the procedures and code of ethics. Forty-two states in the USA, the US Army and Navy, and the Indian Health Service have certifying and licensing boards requiring passing the IC&RC prevention specialist examination (https://internationalcredentialing.org/). In addition, six other countries offer certification and licensing in prevention based on the IC&RC examination.
However, there remain systemic, structural, and cultural issues that have yet to be addressed that could remain barriers to the support of prevention programming (Sumnall, 2019). Studies of the prevention workforce in the USA underscore some of the system and structural issues. High turnover rates and limited opportunities for advancement are consistent impediments for building the capacity of the prevention workforce (Center for Applied Research Solutions, 2013; Eby et al., 2010; Prevention Sub-Committee on the South Carolina Department of Alcohol and Other Drug Abuse Services, 2007; Spurlock et al., 2021). The lack of a formalized substance use prevention service delivery system with consistent funding and recognition makes prevention invisible in communities.
Next Steps for Prevention Professionals
Normalizing the delivery of evidence-based prevention interventions and policies in communities represents a national service delivery system that recognizes and establishes the field of prevention as a profession and supports the implementation and monitoring of a program of comprehensive prevention services to meet the needs of the community being served. As mentioned above, several components of such a system are in place. These include established professional standards, supported by a credentialing process that includes testing, experience and continuing education requirements, and an education pathway to achieve the credentialing standards. Normalization requires at least three additional steps. First, expanding the prevention workforce would involve their acceptance and recognition as members of public health and school-based health teams addressing youth behavioral problems. Second, clarifying guidance is needed regarding the range of duties for prevention professionals and whether they should maintain a focus on primary prevention or include secondary and tertiary prevention. For example, there has been recent controversy as prevention professionals have been asked to assume tertiary prevention roles in preventing death due to overdose. Extension of their roles has occurred without changes to the system design and will require adjustments to education, credentialing and training standards, as well as an increase in the workforce so that adequate attention can be maintained on primary prevention activities. And third, funding support should be continuous for the implementation of prevention programming. By addressing these three issues, we move from a system design to a functional system. Furthermore, as described earlier, addressing the dichotomy of innovations is critical—the innovation itself is the evidence-based prevention program, while the delivery of that program as designed requires another level of innovation with the appropriate oversight, technical assistance and guidance for adaptation where needed. Our discussion primarily focuses on the adoption of the evidence-based prevention program and its component parts, with the goal to institutionalize the systematic delivery of those programs and the embedding of its principles and practices in the daily actions of individuals and the systems that serve them.
Other Service Professionals Who Deliver Prevention Programming
There has been a growing literature that integrates the implementation of evidence-based prevention programming into existing policies that address behavioral health and education issues (Aarons et al., 2011; Bethell et al., 2017; Fagan et al., 2019; Matson et al., 2022; Sims et al., 2019). Indeed the State of Ohio has supported the Pax Good Behavior Game (https://www.goodbehaviorgame.org/pax-good-behavior-game) and the State of Colorado supports Communities That Care (https://www.chi-colorado.org/prevention/ctc/). Another approach suggested by Biglan and Cody (2013) is the development of coalitions of behavioral researchers and organizations to support the concept of “nurturing communities” that incorporate these programs. The literature on introducing innovative practices within the health, education, and social service professional communities has highlighted the challenges facing these groups around highly relevant practices (e.g., Aarons & Sommerfeld, 2012; Hearld et al., 2019; Meyers, 2020; Morago, 2010; Murad, 2017; Saunders et al., 2019). For instance, a review of articles listed on PubMed on these issues for clinical and social work practices revealed the following for the period 2000–2021. The terms “innovative” and “evidence-based” are fairly new to the social services field compared to clinical practice in general. In addition, there is some overlap across the search terms “dissemination,” “implementation,” and “adoption.” We see that over 4000 articles on innovative clinical practice mention “implementation” compared to almost 8000 articles on evidence-based clinical practices whereas for the social services, only 44 articles on innovative social services mentioned “implementation” and 76 for articles focused on evidence-based social services. Clearly there is a need for clarifying terms and definitions across service and disciplinary areas.
Given that many health and social service practitioners and educators who may be implementing preventive interventions do not identify themselves as prevention professionals, a different dissemination approach from those who do identify themselves as prevention professionals may be required. Preventive interventions that are determined to be EBIs are complex and may prove challenging to implement in settings that may not be receptive institutionally or structurally. The complexity arises from the theoretical foundations of these programs that guide the development of program content, structure, and delivery or instructional strategy. Although mediational analyses and multivariate modeling have helped to identify the constructs/variables that explain much of the variation in the outcomes of interest, there remain questions regarding the prevention process involved to achieve these effects. Furthermore, as these programs are based on learning processes it may be that no one variable or construct alone explains the intervention outcome which is dependent on multiple variables and processes (Hansen et al., 2007; O’Rourke & MacKinnon, 2019). The initiation of the Collaboratory by the National Institutes of Health (NIH Collaboratory Rethinking Clinical Trials—The Living Textbook—Rethinking Clinical Trials) may serve as the most recent and promising effort in this area (e.g., Melnick et al., 2022). Other efforts by the National Institutes of Health include the support of “pragmatic trials” to further examine factors related to the implementation and sustainability of evidence-based practices in health care systems (Scheuer et al., 2022).
Next Steps for Other Professionals
For the workforce that is not specialized in prevention but who work with children and families, normalization requires concrete, simple interventions and activities whenever possible. Funded research needs to shift from the development of complex, multi-component interventions to understanding the key drivers of intervention success; research should focus on disaggregation and assessment of the interaction of components of evidence-based prevention interventions and policies to determine what processes explain positive outcomes. The NIH Collaboratory has the potential to inform this process. In addition, newer study designs such as Multiphase Optimization Strategy (MOST) (Collins et al., 2007) or fractional factorial (Bose, 1947; Gunst & Mason, 2009) will help identify the key drivers of success in existing interventions and could lead to a better understanding of change pathways.
Health care and education professionals need simple risk screening tools and clear protocols for addressing risk. These can be developed from existing knowledge and refined and simplified based on disaggregation research. Even as this research proceeds, protocols can be developed with prevention expert workgroups in conjunction with health and education professionals using existing prevention strategy core concepts. This activity could occur at the national level, facilitated by SAMHSA, NIH or the National Academy of Sciences, or at the international level facilitated by WHO and UNODC. Again, as in the case of the prevention professional, in addition to these efforts, systems are needed to assure that the services are delivered as designed.
General Population (Parents, Educators, Policy Makers, Law Enforcement, and Others Who Influence the Lives of Young People)
Translation of evidence-based preventive interventions and policies for the general population will involve a variety of communication and messaging strategies to reinforce positive attitudes, beliefs, norms, and behaviors and to change them when they are neutral or negative. The translational process will also require behavioral and environmental interventions such as training education professionals on changing school climate to create positive and safe places for children to thrive (e.g., positive interventions and behavioral supports- https://www.pbis.org/; Prinz et al., 2016). It will also involve policy changes at various levels from the national to the community. In their article on scaling up evidence-based interventions, Fagan and colleagues (2019) enumerated three recommendations: “(1) provide more public policies and funding to support the creation, testing, and scaling up of EBIs; (2) develop and evaluate specific frameworks that address systems level barriers impeding EBI scale-up; and (3) promote public support for EBIs, community capacity to implement EBIs at scale, and partnerships between community stakeholders, policy makers, practitioners, and scientists within and across systems” (p 1162). In addition, the National Prevention Science Coalition for Healthy Lives (https://www.npscoalition.org) prepares briefs for policy makers at all levels. Lastly, the lessons learned from efforts to reduce smoking as detailed in the Institute of Medicine’s report, Ending the Tobacco Problem (2007) provide some guidance as to how to develop a strategic plan to reinforce community norms to support the prevention of substance use in general and a culture of prevention specifically.
Next Steps for the General Population
Achieving the next steps for prevention professionals and professionals that work with children and families will move the needle on normalizing substance use prevention for the general public. An adequate well-trained workforce embedded in public health and education, knowledge and protocols designed for healthcare and non-specialist education professionals increase the probability that parents and communities know what is necessary and have access to resources that address their specific needs.
Using the science of dissemination and implementation can further extend the ability of the general public to address substance use issues. History points to the successful tobacco campaign that involved policy changes carefully timed with public health messaging and to the early impaired driving campaign that also used policy change and public health messaging to achieve the goals of reducing the percent of fatalities related to driving under the influence of alcohol (McCartt et al., 2010). To some extent, the general public interacting with the service professionals mentioned above will be exposed to and trained in effective prevention practices, such as effective parenting skills, emotion regulatory strategies, and practices in the classroom environment to enhance family and school bonding. Although reaching the broader public is more challenging, it is possible, as demonstrated by Sanders and his colleagues (Pickering & Sanders, 2013; Sanders et al., 2008).
Conclusions
Prevention science and its application to prevention practice have evolved providing the field of prevention with evidence-based interventions and policies. It is time for the results of these decades of accumulated knowledge to be fully transferred to the general population to improve the physical, emotional, and social health of communities. The challenge, as presented in this paper, is five-fold. First, how can this information be disseminated to prevention and health and social service professionals to integrate and sustain in their ongoing services? Second, how can this knowledge base and skills be incorporated into the education and training of these prevention, health, and social service professionals? Third, how can these practices be integrated into everyday life to the extent that they become part of the community fabric? Fourth, to what extent do these practices “fit” into relevant cultural groups? Fifth, how do we develop an ongoing research agenda to address these challenges? We offer “next steps” that logically follow from where we are now and what dissemination and implementation science would suggest are the appropriate processes to address these challenges. How to move forward depends greatly on the efforts not only of prevention professionals everywhere but also key institutions and organizations with a focus on prevention to develop a comprehensive strategy to normalize those prevention practices that will have the greatest impact on the health of our communities. We summarize several efforts that have been made to facilitate and expedite the translational process from research to practice. However, a more systematic approach is needed that brings together representatives from various sectors to develop an action plan addressing each of the groups outlined in this paper. Suggested leadership for this effort in the USA could be the Society for Prevention Research along with the National Institutes of Health and the National Academy of Medicine and internationally, the European Union Society of Prevention Research with the United Nations Office on Drugs and Crime and the International Consortium of Universities for Drug Demand Reduction, the sponsor of this paper.
Funding
Funding for this project was provided by the Bureau of International Narcotics and Law Enforcement Affairs grant #SINLEC19CA0381.
Footnotes
Conflict of Interest The authors declare co competing interests.
Psychoactive substances when taken in or administered into one’s system, affect mental processes, e.g., perception, consciousness, cognition or mood and emotions and include alcohol, nicotine, caffeine, cannabis, opiates, cocaine, etc.
References
- Aarons GA, Hurlburt M, & Horwitz SM (2011). Advancing a conceptual model of evidence-based implementation in public service sectors. Administration and Policy in Mental Health and Mental Health Services Research, 38, 4–23. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Aarons GA, & Sommerfeld DH (2012). Leadership, innovation climate, and attitudes toward evidence-based practice during a statewide implementation. Journal of the American Academy of Children and Adolescent Psychiatry, 51(4), 423–431. 10.1016/j.jaac.2012.01.018 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Allen ML, Garcia-Huidobro D, Porta C, Curran D, Patel R, Miller J, & Borowsky I (2016). Effective parenting interventions to reduce youth substance use: A systematic review. Pediatrics, 138(2), e20154425. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Astor RL, Urman R, Barrington-Trimis JL, Berhane K, Steinberg J, Cousineau M, Leventhal AM, Unger JB, Cruz T, Pentz MA, Samet JM, & McConnell R (2019). Tobacco retail licensing and youth product use. Pediatrics, 143(2), e20173536. 10.1542/peds.2017-3536. Epub 2019 Jan 7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bethell CD, Solloway MR, Guinosso S, Hassink S, Srivastav A, Ford D, & Simpson LA (2017). Prioritizing possibilities for child and family health: An agenda to address adverse childhood experiences and foster the social and emotional roots of well-being in pediatrics. Academic Pediatrics, 17, S36–S50. [DOI] [PubMed] [Google Scholar]
- Biglan A, & Cody C (2013). Integrating the human sciences to evolve effective policies. Journal of Economic and Behavioral Organizations, 90(Suppl), S152–S162. 10.1016/j.jebo.2012.12.018 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Biglan A, & Embry DD (2013). A framework for intentional cultural change. Journal of Contextual Behavioral Science, 2, 3–4. 10.1016/j.jcbs.2013.06.001 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Biglan A, Elfner K, Garbacz SA, Komro K, Prinz RJ, Weist MD, Wilson DK, & Zarling A (2020). A strategic plan for strengthening America’s families: A brief from the coalition of behavioral science organizations. Clinical Child and Family Psychological Review, 23(2), 153–175. 10.1007/s10567-020-00318-0 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Biglan A, Van Ryzin MJ, & Hawkins JD (2017). Evolving a more nurturing society to prevent adverse childhood experiences. Academic Pediatrics, 17(7 Supplement), S150–S157. 10.1016/j.acap.2017.04.002 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bose RC (1947). Mathematical theory of the symmetrical factorial design. Sankhyā: The Indian Journal of Statistics, 107–166. [Google Scholar]
- Brook JS, Whiteman M, Gordon AS, & Cohen P (1989). Changes in drug involvement: A longitudinal study of childhood and adolescent determinants. Psychological Reports, 65(3 Pt 1), 707–726. 10.2466/pr0.1989.65.3.707 [DOI] [PubMed] [Google Scholar]
- Brownson RC, Ballew P, Dieffenderfer B, Haire-Joshu D, Heath GW, Kreuter MW, & Myers BA (2007). Evidence-based interventions to promote physical activity: What contributes to dissemination by state health departments. American Journal of Preventive Medicine, 33(1 Suppl), S66–73. 10.1016/j.amepre.2007.03.011.. [DOI] [PubMed] [Google Scholar]
- Buckley PR, Fagan AA, Pampel FC, & Hill KG (2020). Making evidence-based interventions relevant for users: A comparison of requirements for dissemination readiness across program registries. Evaluation Review, 44(1), 51–83. 10.1177/0193841X20933776 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Burkhardt JT, Schröter DC, Magura S, Means SN, & Coryn CL (2015). An overview of evidence-based program registers (EBPRs) for behavioral health. Evaluation and Program Planning, 48, 92–99. 10.1016/j.evalprogplan.2014.09.006 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Campello G, Sloboda Z, Heikkil H, & Brotherhood A (2014). International standards on drug use prevention: the future of drug use prevention world-wide. International Journal of Prevention and Treatment of Substance Use Disorders, 1, 6–27. [Google Scholar]
- Center for Applied Research Solutions. (2013). California’s substance abuse prevention workforce development—survey report. http://www.ca-cpi.org/docs/Resources/SAP_Workforce_Development/CPI-SAP-Workforce-Survey-Report.pdf [Google Scholar]
- Chambers DA, Glasgow RE, & Stange KC (2013). The dynamic sustainability framework: Addressing the paradox of sustainment amid ongoing change. Implementation Science, 8, 117. 10.1186/1748-5908-8-117 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Chinman M, Hunter SB, Ebener P, Paddock SM, Stillman L, Imm P, & Wandersman A (2008). The getting to outcomes demonstration and evaluation: An illustration of the prevention support system. American Journal of Community Psychology, 41(3–4), 206–224. 10.1007/s10464-008-9163-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Collins LM, Murphy SA, & Strecher V (2007). The multiphase optimization strategy (MOST) and the sequential multiple assignment randomized trial (SMART): New methods for more potent eHealth interventions. American Journal of Preventive Medicine, 32(5), S112–S118. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cooper JR (1998). A multidimensional approach to the adoption of innovation. Management Decision, 36(8), 493–502. [Google Scholar]
- Crowley M, & Jones D (2017). A framework for valuing investments in a nurturing society: Opportunities for prevention research. Clinical Child and Family Psychological Review, 20(1), 87–103. 10.1007/s10567-017-0228-3 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Crowley DM, Greenberg MT, Feinberg ME, Spoth RL, & Redmond CR (2012). The effect of the PROSPER partnership model on cultivating local stakeholder knowledge of evidence-based programs: A five-year longitudinal study of 28 communities. Prevention Science, 13(1), 96–105. 10.1007/s11121-011-0250-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Damschroder LJ, Aron DC, Keith RE, Kirsh SR, Alexander JA, & Lowery JC (2009). Fostering implementation of health services research findings into practice: A consolidated framework for advancing implementation science. Implementation Science, 4(1), 1–15. 10.1186/1748-5908-4-50 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Eby LT, Burk H, & Maher CP (2010). How serious of a problem is staff turnover in substance abuse treatment? A longitudinal study of actual turnover. Journal of Substance Abuse Treatment, 39(3), 264–271, ISSN 0740–5472. 10.1016/j.jsat.2010.06.009 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Eccles MP, Armstrong D, Baker R, Cleary K, Davies H, Davies S, Glasziou P, Ilott I, Kinmonth AL, Leng G, Logan S, Marteau T, Michie S, Rogers H, Rycroft-Malone J, & Sibbald B (2009). An implementation research agenda. Implementation Science, 4, 18. 10.1186/1748-5908-4-18. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Embry DD, & Biglan A (2008). Evidence-based kernels: Fundamental units of behavioral influence. Clinical Child and Family Psychological Review, 3, 75–113. 10.1007/s10567-008-0036-x [DOI] [PMC free article] [PubMed] [Google Scholar]
- Fagan AA, Arthur MW, Hanson K, Briney JS, & Hawkins JD (2011). Effects of communities that care on the adoption and implementation fidelity of evidence-based prevention programs in communities: Results from a randomized controlled trial. Prevention Science, 12(3), 223–234. 10.1007/s11121-011-0226-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Fagan AA, Bumbarger BK, Barth RP, Bradshaw CP, Cooper BR, Supplee LH, & Walker DK (2019). Scaling up evidence-based interventions in us public systems to prevent behavioral health problems: Challenges and opportunities. Prevention Science, 20(8), 1147–1168. 10.1007/s11121-019-01048-8 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Faggiano F, Allara E, Giannotta F, Molinar R, Sumnall H, et al. (2014). Europe needs a central, transparent, and evidence-based approval process for behavioural preventive interventions. PLOS Medicine, 11(10):e1001740. 10.1371/journal.pmed.1001740 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Farmer AP, Légaré F, Turcot L, Grimshaw J, Harvey E, McGowan JL, & Wolf F (2008). Printed educational materials: Effects on professional practice and health care outcomes. The Cochrane Database of Systematic Reviews, (3):CD004398. 10.1002/14651858.CD004398.pub2. Update in: The Cochrane Database of Systematic Reviews, 2012;10:CD004398. [DOI] [PubMed] [Google Scholar]
- Fishbein DH, & Dariotis JK (2019). Personalizing and optimizing preventive intervention models via a translational neuroscience framework. Prevention Science, 20(1), 10–20. 10.1007/s11121-017-0851-8 [DOI] [PubMed] [Google Scholar]
- Fishbein DH, Ridenour TA, Stahl M, & Sussman S (2016). The full translational spectrum of prevention science: Facilitating the transfer of knowledge to practices and policies that prevent behavioral health problems. Translational Behavioral Medicine, 6(1), 5–16. 10.1007/s13142-015-0376-2 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Fixsen DL, & Blase KA (2008). Effective applications of innovations. Paper presented at the OASAS Meetings, New York State. [Google Scholar]
- Forsetlund L, Bjørndal A, Rashidian A, Jamtvedt G, O'Brien MA, Wolf F, Davis D, Odgaard-Jensen J, & Oxman AD (2009). Continuing education meetings and workshops: Effects on professional practice and health care outcomes. Cochrane Database of Systematic Reviews, (2):CD003030. 10.1002/14651858.CD003030.pub2. Update in: Cochrane Database Syst Rev. 2021 Sep 15;9:CD003030. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Garcia R, & Calantone R (2002). A critical look at technological innovation typology and innovativeness terminology: A literature review. The Journal of Product Innovation Management, 19, 110–132. [Google Scholar]
- Grimshaw J, Eccles M, Thomas R, MacLennan G, Ramsay C, Fraser C, & Vale L (2006). Toward evidence-based quality improvement. Evidence (and its limitations) of the effectiveness of guideline dissemination and implementation strategies 1966–1998. Journal of General Internal Medicine, 21 Suppl 2(Suppl 2), S14–20. 10.1111/j.1525-1497.2006.00357.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gunst RF, & Mason RL (2009). Fractional factorial design. Wiley Interdisciplinary Reviews: Computational Statistics, 1(2), 234–244. [Google Scholar]
- Hall K, Staiger PK, Simpson A, Best D, & Lubman DI (2016). After 30 years of dissemination, have we achieved sustained practice change in motivational interviewing? Addiction, 111(7), 1144–1150. 10.1111/add.13014 [DOI] [PubMed] [Google Scholar]
- Hallfors D, & Godette D (2002). Will the ‘principles of effectiveness’ improve prevention practice? Early findings from a diffusion study. Health Education Research, 17(4), 461–470. 10.1093/her/17.4.461 [DOI] [PubMed] [Google Scholar]
- Hallfors DD, Pankratz M, & Hartman S (2007). Does federal policy support the use of scientific evidence in school-based prevention programs? Prevention Science, 8(1), 75–81. [DOI] [PubMed] [Google Scholar]
- Hansen WB, Dusenbury L, Bishop D, & Derzon JH (2007). Substance abuse prevention program content: Systematizing the classification of what programs target for change. Health Education Research, 22(3), 351–360. 10.1093/her/cyl091 [DOI] [PubMed] [Google Scholar]
- Hawkins JD, Catalano RF, & Miller JY (1992). Risk and protective factors for alcohol and other drug problems in adolescence and early adulthood: Implications for substance abuse prevention. Psychological Bulletin, 112, 64–105. 10.1037/0033-2909.112.1.64 [DOI] [PubMed] [Google Scholar]
- Hearld L, Alexander JA, Wolf LJ, & Shi Y (2019). Dissemination of quality improvement innovations by multisector health care alliances. Journal of Health Organization Management, 33(4), 511–528. 10.1108/JHOM-08-2017-0195 [DOI] [PubMed] [Google Scholar]
- Hopfer CJ, Crowley TJ, & Hewitt JK (2003). Review of twin and adoption studies of adolescent substance use. Journal of the American Academy of Child & Adolescent Psychiatry, 42(6), 710–719. [DOI] [PubMed] [Google Scholar]
- Huba GJ, Wingard JA, & Bentler PM (1981). Intentions to use drugs among adolescents: A longitudinal analysis. International Journal of the Addictions, 16(2), 331–339. 10.3109/10826088109038832 [DOI] [PubMed] [Google Scholar]
- Institute of Medicine. (2007). Ending the tobacco problem: A blueprint for the nation. Washington, DC: The National Academies Press. 10.17226/11795 [DOI] [Google Scholar]
- Ivers N, Jamtvedt G, Flottorp S, Young JM, Odgaard-Jensen J, French SD, O'Brien MA, Johansen M, Grimshaw J, and Oxman AD (2012). Audit and feedback: Effects on professional practice and healthcare outcomes. Cochrane Database of Systematic Reviews, (6), CD000259. 10.1002/14651858.CD000259.pu3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kandel DB, & Logan JA (1984). Patterns of drug use from adolescence to young adulthood: I. Periods of risk for initiation, continued use, and discontinuation. American Journal of Public Health, 74(7), 660–666. 10.2105/ajph.74.7.660 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kirk MA, Kelley C, Yankey N, Birken SA, Abadie B, & Damschroder L (2015). A systematic review of the use of the consolidated framework for implementation research. Implementation Science, 11, 72. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Logan-Greene P, Linn B, Hartinger-Saunders R, Nochajski T, Wieczorek WF, & Rittner B (2019). Understanding the ecological context of mental, emotional, and behavioral health problems: A person-centered approach. Journal of Community Psychology, 47(4), 833–855. 10.1002/jcop.22156. Epub 2019 Jan 17. [DOI] [PubMed] [Google Scholar]
- MacArthur G, Caldwell DM, Redmore J, Watkins SH, Kipping R, White J, Chittleborough C, Langford R, Er V, Lingam R, Pasch K, Gunnell D, Hickman M, & Campbell R (2018). Individual-, family-, and school-level interventions targeting multiple risk behaviours in young people. Cochrane Database of Systematic Reviews, Issue 10. Art. No.: CD009927. 10.1002/14651858.CD009927.pub2 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Madon T, Hofman KJ, Kupfer L, & Glass RI (2007). Public health. Implementation science. Science, 318(5857), 1728–1729. 10.1126/science.1150009. [DOI] [PubMed] [Google Scholar]
- Margolies PJ, Humensky JL, Chiang I-C, Covell NH, Broadway-Wilson K, Gregory R, Jewell TC, Scannevin G Jr., Baker S, & Dixon LB (2017). Is there a role for fidelity self-assessment in the individual placement and support model of supported employment? Psychiatric Services, 68(9), 975–978. 10.1176/appi.ps.201600264 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Martino S, Gallon S, Ball SA, & Carroll KM (2008). A step forward in teaching addiction counselors how to supervise motivational interviewing using a clinical trials training approach. Journal of Teaching in the Addictions, 6(2), 39–67. [Google Scholar]
- Matson PA, Ridenour T, Ialongo N, Spoth R, Prado G, Hammond CJ, Hawkins JD, & Hoover A Jr. (2022). State of the art in substance use prevention and early intervention: Applications to pediatric primary care settings. Prevention Science, 23, 204–211. [DOI] [PMC free article] [PubMed] [Google Scholar]
- May C, & Finch T (2009). Implementing, embedding, and integrating practices: An outline of normalization process theory. Sociology, 43(3), 535–554. [Google Scholar]
- May C, Rapley T, Mair FS, Treweek S, Murray E, Ballini L, Macfarlane A Girling M, & Finch TL (2015). Normalization Process Theory On-line Users’ Manual, Toolkit and Nomad Instrument. Available from: http://www.normalizationprocess.org [Google Scholar]
- May CR, Albers B, Bracher M, Finch TL, Gilbert A, Girling M, Greenwood K, MacFarlane A, Mair FS, May CM, Murray E, Potthoff S, & Rapley T (2022). Translational framework for implementation evaluation and research: A normalisation process theory coding manual for qualitative research and instrument development. Implementation Science, 17(1), 19. 10.1186/s13012-022-01191-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McCartt AT, Hellinga LA, & Kirley BB (2010). The effects of minimum legal drinking age 21 laws on alcohol-related driving in the United States. Journal of Safety Research, 41(2), 173–181. 10.1016/j.jsr.2010.01.002. Epub 2010 Mar 9. [DOI] [PubMed] [Google Scholar]
- McIntosh K, Mercer SH, Nese RNT, & Ghemraoui A (2016). Identifying and predicting distinct patterns of implementation in a school-wide behavior support framework. Prevention Science, 17(8), 992–1001. 10.1007/s11121-016-0700-1 [DOI] [PubMed] [Google Scholar]
- Means SN, Magura S, Burkhardt JT, Schröter DC, & Coryn CL (2015). Comparing rating paradigms for evidence-based program registers in behavioral health: Evidentiary criteria and implications for assessing programs. Evaluation and Program Planning, 48, 100–116. 10.1016/j.evalprogplan.2014.09.007 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Melnick ER, Nath B, Dziura JD, Casey MF, Jeffery MM, Paek H, Soares WE 3rd, Hoppe JA, Rajeevan H, Li F, Skains RM, Walter LA, Patel MD, Chari SV, Platts-Mills TF, Hess EP, & D'Onofrio G (2022). User centered clinical decision support to implement initiation of buprenorphine for opioid use disorder in the emergency department: EMBED pragmatic cluster randomized controlled trial. British Medical Journal, 377:e069271. 10.1136/bmj-2021-069271. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Meyers MO (2020). Innovations in surgical technique and translation to broad clinical practice. Journal of Clinical Oncology, 19, 2119–2121. 10.1200/JCO.20.00885 [DOI] [PubMed] [Google Scholar]
- Miller WR, Yahne CE, Moyers TB, Martinez J, & Pirritano M (2004). A randomized trial of methods to help clinicians learn motivational interviewing. Journal of Consulting and Clinical Psychology, 72(6), 1050. [DOI] [PubMed] [Google Scholar]
- Morago P (2010). Dissemination and implementation of evidence-based practice in the social services: A UK survey. Journal of Evidence Based Social Work, 7(5), 452–465. 10.1080/15433714.2010.494973 [DOI] [PubMed] [Google Scholar]
- Moullin JC, Dickson KS, Stadnick NA, Rabin B, & Aarons GA (2019). Systematic review of the Exploration, Preparation, Implementation, Sustainment (EPIS) framework. Implementation Science, 14, 1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Murad MH (2017). Clinical practice guidelines: A primer on development and dissemination. Mayo Clinic Proceedings, 92(3), 423–433. 10.1016/j.mayocp.2017.01.001 [DOI] [PubMed] [Google Scholar]
- National Academies of Sciences, Engineering, and Medicine. (2019). Fostering healthy mental, emotional, and behavioral development in children and youth: A national agenda. Washington, DC: The National Academies Press. [PubMed] [Google Scholar]
- O'Brien MA, Rogers S, Jamtvedt G, Oxman AD, Odgaard-Jensen J, Kristoffersen DT, Forsetlund L, Bainbridge D, Freemantle N, Davis D, Haynes RB, & Harvey E (2007). Educational outreach visits: Effects on professional practice and health care outcomes. Cochrane Database of Systematic Reviews, 4(4), CD000409. 10.1002/14651858.CD000409.pub2 [DOI] [PMC free article] [PubMed] [Google Scholar]
- O’Rourke HP, & MacKinnon DP (2019). The importance of mediation analysis in substance-use prevention. In Sloboda Z, Petras H, Robertson E & Hingson R (Eds.), Prevention of Substance Use. Advances in Prevention Science (pp. 233–246). New York: Springer. [Google Scholar]
- Ogden T, Forgatch MS, Askeland E, Patterson GR, & Bullock BM (2005). Large scale implementation of parent management training at the national level: The case of Norway. Journal of Social Work Practice, 19(3), 317–329. [Google Scholar]
- Palinkas LA, Spear SE, Mendon SJ, Villamar J, Reynolds C, Green CD, Olson C, Adade A, & Brown CH (2020). Conceptualizing and measuring sustainability of prevention programs, policies, and practices. Translational Behavioral Medicine, 10(1), 136–145. 10.1093/tbm/ibz170. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Paschall MJ, & Grube JW (2020). Recreational marijuana availability in Oregon and use among adolescents. American Journal of Preventive Medicine, 58(2), e63–e69. 10.1016/j.amepre.2019.09.020 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Paschall MJ, Grube JW, & Kypri K (2009). Alcohol control policies and alcohol consumption by youth: A multinational study. Addiction, 104(11), 1849–1855. 10.1111/j.1360-0443.2009.02698.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Pavlovská A, Peters RH, Gabrhelík R, Miovský M, Sloboda Z, & Babor TF (2019). Overview of the university-based addiction studies programmes in the United States. Journal of Substance Use, 24(1), 55–60. [Google Scholar]
- Pickering JA, & Sanders MR (2013) Enhancing communities through the design, development and dissemination of positive parenting interventions. Journal of Applied Research on Children: Informing Policy for Children at Risk, 4(2), Article 18. https://digitalcommons.library.tmc.edu/childrenatrisk/vol4/iss2/18 [Google Scholar]
- Prevention Sub-Committee of the South Carolina Department of Alcohol and Other Drug Abuse Services and Behavioral Health Services Association of South Carolina, Inc. (2007). South Carolina prevention workforce development plan. https://www.daodas.sc.gov/wp-content/uploads/2019/11/SC-Prevention-Workforce-Development-Plan.pdf [Google Scholar]
- Prinz RJ, Sanders MR, Shapiro CJ, Whitaker DJ, & Lutzker JR (2016). Addendum to “Population-based prevention of child maltreatment: The U.S. triple P system population trial”. Prevention Science, 17(3), 410–416. 10.1007/s11121-016-0631-x. [DOI] [PubMed] [Google Scholar]
- Rhee SH, Hewitt JK, Young SE, Corley RP, Crowley TJ, & Stallings MC (2003). Genetic and environmental influences on substance initiation, use, and problem use in adolescents. Archives of General Psychiatry, 60(12), 1256–1264. [DOI] [PubMed] [Google Scholar]
- Ridenour TA, Willis D, Bogen DL, Novak S, Scherer J, Reynolds MD, Zhai ZW, & Tarter RE (2015). Detecting initiation or risk for initiation of substance use before high school during pediatric well-child check-ups. Drug and Alcohol Dependence, 150, 54–62. 10.1016/j.drugalcdep.2015.02.013 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ringwalt C, Hanley S, Vincus AA, Ennett ST, Rohrbach LA, & Bowling JM (2008). The prevalence of effective substance use prevention curricula in the nation’s high schools. Journal of Primary Prevention, 29(6), 479–488. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ringwalt C, Vincus AA, Hanley S, Ennett ST, Bowling JM, & Haws S (2011). The prevalence of evidence-based drug use prevention curricula in U.S. middle schools in 2008. Prevention Science, 12(1), 63–69. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ringwalt CL, Ennett S, Vincus A, Thorne J, Rohrbach LA, & Simons-Rudolph A (2002). The prevalence of effective substance use prevention curricula in U.S. middle schools. Prevention Science, 3(4), 257–265. [DOI] [PubMed] [Google Scholar]
- Ringwalt C, Vincus AA, Hanley S, Ennett ST, Bowling JM, & Rohrbach LA (2009). The prevalence of evidence-based drug use prevention curricula in U.S. middle schools in 2005. Prevention Science, 10(1), 33–40. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Rogers EM (1995). Lessons for guidelines from the diffusion of innovations. Joint Commission Journal on Quality Improvement, 21(7), 324–328. 10.1016/s1070-3241(16)30155-9. [DOI] [PubMed] [Google Scholar]
- Rose EJ, Picci G, & Fishbein DH (2019). Neurocognitive precursors of substance misuse corresponding to risk, resistance, and resilience pathways: Implications for prevention science. Frontiers in Psychiatry, 10, 399. 10.3389/fpsyt.2019.00399 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sanders MR, Ralph A, Sofronoff K, Gardiner P, Thompson R, Dwyer S, & Bidwell K (2008). Every family: A population approach to reducing behavioral and emotional problems in children making the transition to school. Journal of Primary Prevention., 29(3), 197–222. 10.1007/s10935-008-0139-7. Erratum In: JPrimPrev. 2014 Dec;35(6):451. [DOI] [PubMed] [Google Scholar]
- Saunders H, Gallagher-Ford L, Kvist T, & Vehviläinen-Julkunen K (2019). Practicing healthcare professionals’ evidence-based practice competencies: An overview of systematic reviews. Worldviews Evidence Based Nursing, 16(3), 176–185. [DOI] [PubMed] [Google Scholar]
- Schackman BR (2010). Implementation science for the prevention and treatment of HIV/AIDS. Journal of Acquired Immune Deficiency Syndrome, 55. Supplement, 1, S27–S31. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Scheuer H, Kuklinski MR, Sterling SA, Catalano RF, Beck A, Braciszewski J, Boggs J, Hawkins JD, Loree AM, Weisner C, Carey S, Elsiss F, Morse E, Negusse R, Jessen A, Kline-Simon A, Oesterle S, Quesenberry C, Sofrygin O, & Yoon T (2022). Parent-focused prevention of adolescent health risk behavior: Study protocol for a multisite cluster-randomized trial implemented in pediatric primary care. Contemporary Clinical Trials, 106621. 10.1016/j.cct.2021.106621. Epub 2021 Nov 14. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sims BE, Armstead T, Niolon P, Meyer A, & Blachman-Demner D (2019). Commentary on scaling-up evidence-based interventions in us public systems to prevent behavioral health problems. Prevention Science, 20(8), 1173–1177. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sloboda Z (2018). School-based prevention-evolution of evidence-based strategies. In Leukefeld CG & Gullotta TP (Eds.), Adolescent Substance Abuse: Evidence-Based Approaches to Prevention and Treatment (pp. 191–212). Springer. [Google Scholar]
- Sloboda Z, Dusenbury L, & Petras H (2014). Implementation science and the effective delivery of evidence-based prevention. In Sloboda Z & Petras H (Eds.), Defining Prevention Science (pp. 293–314). Springer. [Google Scholar]
- Sloboda Z, Glantz MD, & Tarter RE (2012). Revisiting the concepts of risk and protective factors for understanding the etiology and development of substance use and substance use disorders: Implications for prevention. Substance Use and Misuse, 47(8–9), 944–962. [DOI] [PubMed] [Google Scholar]
- Spurlock S, Morse R, & Meharg H (2021). Rhode Island substance use prevention: Workforce Development-2020–2024. Department of Behavioral Health Care, Developmental Disabilities and Hospitals. [Google Scholar]
- Stone AL, Becker LG, Huber AM, & Catalano RF (2012). Review of risk and protective factors of substance use and problem use in emerging adulthood. Addictive Behaviors, 37(7), 747–775. [DOI] [PubMed] [Google Scholar]
- Substance Abuse and Mental Health Services Administration. (2021). Prevention Core Competencies. Publication No. PEP20–03–08–001. Rockville, MD: Substance Abuse and Mental Health Services Administration. [Google Scholar]
- Sumnall HR (2019). The substance use prevention workforce: An international perspective. In Sloboda Z, Petras H, Robertson E, & Hingson R (Eds.), Prevention of Substance Use (pp. 395–412). Springer. [Google Scholar]
- Trucco EM, & Hartmann SA (2021). Understanding the etiology of adolescent substance use through developmental perspectives. Child Development Perspectives, 15(4), 257–264. 10.1111/cdep.12426. Epub 2021 Aug 24. [DOI] [PMC free article] [PubMed] [Google Scholar]
- United Nations Office on Drugs and Crime. (2013, 2018). International standards on drug use prevention. Vienna: United Nations Office on Drugs and Crime. [Google Scholar]
- Vanyukov MM, Tarter RE, Kirillova GP, Kirisci L, Reynolds MD, Kreek MJ, Conway KP, Maher BS, Iacono WG, Bierut L, Neale MC, Clark DB, & Ridenour TA (2012). Common liability to addiction and “gateway hypothesis”: Theoretical, empirical and evolutionary perspective. Drug and Alcohol Dependence, 123(1), S3–S17. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wilson DS, Hayes SC, Biglan A, & Embry DD (2014). Evolving the future: Toward a science of intentional change. Behavioral and Brain Sciences, 37(4), 395–416. [DOI] [PMC free article] [PubMed] [Google Scholar]