Abstract
Background:
Waterpipe tobacco (hookah) use is common among reproductive age patients and is often perceived as safer than cigarette use. Prior studies have shown a decrease in nausea and vomiting symptoms among pregnant people who use cigarettes, but no studies to date have examined these symptoms in pregnant people who use waterpipe tobacco.
Objective:
To investigate the extent of symptoms of nausea and vomiting of pregnancy among participants who self-reported waterpipe tobacco (WPT) use during and prior to pregnancy.
Methods:
Participants (N=99) were recruited for a prospective cohort study examining waterpipe tobacco use during pregnancy. Participants self-reported nausea and vomiting symptoms throughout pregnancy using the Pregnancy Unique Quantification of Emesis (PUQE) during first and third trimester. Medical conditions (hypertension, gestational diabetes mellitus) were determined by medical record review. Participants were evaluated by sole WPT use versus dual/poly WPT use and frequency of WPT use.
Results:
All (n=99) participants completed the PUQE questionnaire during first trimester and 82 (82.8%) completed the PUQE during third trimester. Almost all (91.9%) of participants reported moderate nausea and vomiting symptoms at both assessments. There was no difference in frequency of WPT use in pregnancy or rates of dual/poly WPT use in participants with all levels of the PUQE questionnaire. There was also no difference in rates of WPT use or PUQE scores between sole WPT users and dual/poly users. When comparing low WPT use (1-8 times during pregnancy) and high use (9 or more times), those who were in the higher-frequency use group had higher waterpipe dependence scale scores (7.2 vs 5.3, p<0.02). With regards to maternal medical comorbidities, the only difference between groups was that sole WPT users were more likely to have a diagnosis of asthma than dual/poly users (36.8% vs 14.9% p<0.02).
Conclusion:
There were no differences in symptoms of nausea and vomiting of pregnancy or medical conditions in pregnant people who use WPT with any frequency during pregnancy. However, sole WPT users had higher rates of asthma than dual/poly WPT users.
Introduction
Despite recommendations from the Surgeon General of the United States, the American College of Obstetricians and Gynecologists (ACOG) and other governing bodies, worldwide tobacco use amongst pregnant people continues to be prevalent1. One under-studied but increasingly popular form of tobacco is waterpipe tobacco (WPT), or hookah. In order to use WPT, tobacco is heated using charcoal bricks (often alongside fruit, herbs and spices). The smoke is then filtered through water and inhaled through a long pipe-like mouthpiece. The results of a cross-sectional survey of pregnant patients in Lebanon reported that 6% of patients used WPT during pregnancy2. A study out of Iran revealed that 8% to 14% of pregnant people reported WPT use in pregnancy3, 4. Of the patients in Iran who reported prenatal WPT use, an average of 1.37 sessions a day was reported3. Prevalence of WPT use in the United States (US) during pregnancy is reported to be 2.5%, and it is the third most common form of tobacco use in pregnancy after cigarettes and e-cigarettes5. Nicotine levels for both e-cigarettes and WPT vary by brand. E-cigarettes can have nicotine levels ranging from close to 0 to as high as 87.2 mg/mL6, while nicotine in WPT ranged from 0.8 mg/g to 52.7 mg/g7. These levels are higher than those found in conventional cigarettes of 13 mg8. WPT is commonly used by adolescents and young adults because many perceive it as “safer” than cigarette tobacco use1.
Nausea and vomiting of pregnancy affects 50-80% of pregnant patients9. Smoking prior to and during pregnancy is known to decrease symptoms of nausea and vomiting of pregnancy10, 11, though is not recommended due to its many other negative effects on the pregnancy, such as growth restriction, fetal demise, and preterm birth11, 12. Previous research by our group found that 68-73% of pregnant people preferred menthol/mint WPT flavors during pregnancy13, 14. Peppermint is a commonly recommended complementary medicine treatment for nausea and vomiting of pregnancy, and therefore the menthol/mint preferences could be related to symptomatic management of nausea and vomiting of pregnancy10.
To our knowledge there is no research evaluating the degrees of nausea and vomiting symptoms in pregnant people who use WPT during pregnancy and no studies evaluating the of rates of maternal medical conditions in people who use WPT during pregnancy. This analysis seeks to evaluate the symptoms of nausea and vomiting in people who use WPT during pregnancy. In particular, we compared symptoms of nausea and vomiting and rates of medical conditions in pregnant people who used WPT only and those who used WPT in addition to other tobacco products. We also conducted comparisons based on frequency of WPT use in pregnancy. We hypothesized that pregnant people who were dual/poly users and those reporting more frequent WPT use would have lower rates of nausea/vomiting of pregnancy.
Methods
Study Design
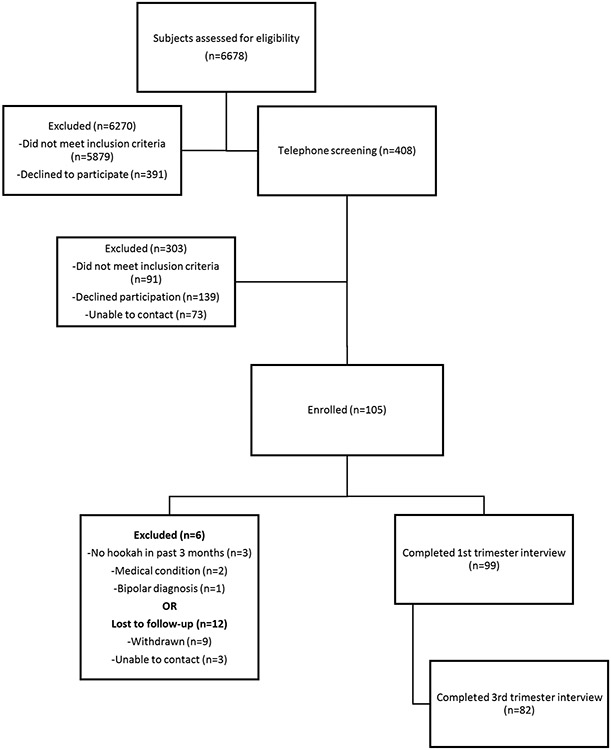
This is a secondary analysis of data from “Let’s Talk about Hookah,” a prospective cohort study of pregnant people who self-reported WPT use either during pregnancy and/or 3 months prior to conception13. Pregnant people were recruited via multiple methods (face-to-face contact, brochures, paper and electronic advertisements) from multiple obstetric offices and community sites in Rhode Island and Southern Massachusetts. If interested, participants were screened by telephone for inclusion. Inclusion criteria were English-speaking, age 18-40 years, WPT use at least once during pregnancy or in 3 months prior to conception, singleton gestation and no severe medical or psychiatric comorbidities. 408 women expressed interest initially, 139 were no longer interested when called, and 91 were ineligible. 25 did not attend their baseline interview and could not be rescheduled, leaving a total of 105 enrolled participants. 6 participants were excluded following the baseline interview due to either no WPT during preconception/pregnancy or a bipolar diagnosis (Figure 1).
Figure 1.
Subject Recruitment and Retention
Study Procedures and Measures
The initial surveys were completed during the baseline interview session during the late first or early second trimester (mean of 15 weeks’ gestation). Follow-up surveys were completed during third trimester at (mean of 30 weeks’ gestation). Interviews were conducted by research staff not involved in prenatal or clinical care. Questionnaires assessed demographic information, general health, pregnancy and tobacco history. Surveys were collected by trained research personnel. Medical conditions were assessed via self-report and through review of medical charts.
Timeline follow back (TLFB) Interview
The TLFB is a calendar-based assessment of daily substance use utilizing key dates (eg, holidays, personal events) to cue memory and increase accuracy of recall15-17. The TLFB was used to assess daily WPT use and other tobacco/nicotine product use (i.e. cigarettes, e-cigarettes, cigars/cigarillos/little cigars). The TLFB interview covered each day of pregnancy until the first interview as well as the 3 months prior to conception. Participants who reported use of any non-WPT tobacco product (ie, cigarettes, e-cigarettes, cigars/cigarillos/little cigars) during the three months prior to conception or pregnancy were categorized as dual/poly WPT users.
Pregnancy Unique Quantification of Emesis (PUQE) Scoring Index
Participants were evaluated twice over pregnancy, late first/early second trimester (mean = 15 weeks’ gestation) and third trimester (mean = 30 weeks’ gestation), for nausea and vomiting symptoms using the pregnancy unique quantification of emesis (PUQE) scoring index. The PUQE scoring index is a validated tool to assess the severity of nausea and vomiting of pregnancy18. This scoring index uses 3 questions to assess the frequency of nausea and vomiting symptoms. The sum of the responses to the questionnaire are classified into mild symptoms (score ≤6), moderate symptoms (7-12), and severe symptoms (≥13)18.
Lebanon Waterpipe Dependence Scale
Participants also completed the Lebanon Waterpipe Dependence Scale19. This is an 11-item questionnaire which assesses nicotine dependence among adult users of WPT which includes questions on frequency of usage, cost of usage and ability to stop using WPT19.
Statistical Analyses
WPT-only users (N=42) were compared to dual/poly WPT users (N=57) regarding nausea and vomiting of pregnancy and medical conditions. Additionally, nausea and vomiting symptoms and medical conditions were evaluated by frequency of WPT use: low WPT use (1-8 times) (N=58) and high WPT use (9 or more times) (N=34) during pregnancy.
Data were analyzed using STATA 15.0 (College Station, TX, USA). Continuous variables were compared using Wilcoxon rank-sum or Kruskal-Wallis tests, while categorical variables were analyzed using chi-squared tests. Significance was defined as p< 0.05.
Results
Participants Description
A total of 99 patients were included in final analyses. All 99 participants (100%) completed the PUQE during early 2nd trimester (mean = 15 weeks) and 82 (82.8%) completed the PUQE during 3rd trimester (mean = 30 weeks). The majority of participants had a moderate PUQE score (N=91, 91.9%), while 2 had a low score (2.0%) and 5 had a severe score (5.1%).
Sole versus dual/polysubstance WPT use
The total population was analyzed according to WPT use only (N=42) and dual WPT and tobacco use (N=57) (Table 1). The most common methods of tobacco consumption in the dual use group (in addition to WPT) were cigars/cigarillos/little cigars (33.3%) and cigarettes (19.3%). There were no baseline differences between pregnant persons who reported sole versus dual/polysubstance WPT use in terms of race; however, pregnant persons who used WPT only were more likely to self-identify as Latina/Hispanic. There were no significant differences between WPT groups in body mass index (BMI), gravidity, or parity. Additionally, no significant differences between groups in rates of gestational diabetes or hypertension were noted. Both groups had similar scores on the waterpipe dependence scale (6.0 vs 5.7, p=0.61). There were no significant differences between groups in the number of times WPT was used during pregnancy. There were also no significant differences between groups in PUQE score at time 1 (9.1 v 9.4, p=0.57) or time 2 (8.0 vs 8.2, p=0.60).
Table 1.
Characteristics and PUQE scores for sole versus dual/waterpipe tobacco use in the perinatal period
| WPT only N=42 |
Dual/Polysubstance use N=57 |
P-value | |
|---|---|---|---|
| Race | 0.301 | ||
| First Nations | 0 (0.0) | 1 (1.8) | |
| Asian | 0 (0.0) | 3 (5.3) | |
| Pacific Islander | 0 (0.0) | 0 (0.0) | |
| Black | 7 (l6.7) | 11 (19.3) | |
| White | 8 (19.0) | 15 (26.3) | |
| Other | 27 (64.3) | 27 (47.3) | |
| Ethnicity | 0.047 1 | ||
| Latina/Hispanic | 29 (69.0) | 28 (49.0) | |
| Not Latina/Hispanic | 13 (31.0) | 29 (51.0) | |
| Pre-pregnancy BMI | 29.6 (1.0) | 28.7 (1.0) | 0.372 |
| Parity | 1 (0-6) | 1 (0-4) | 0.592 |
| Hyperthyroidism | 1 (2.6) | 1 (2.1) | 1.00 |
| Hypothyroidism | 0 | 1 (2.1) | 1.00 |
| Asthma | 14 (36.8) | 7 (14.9) | 0.02 |
| Chronic HTN | 4 (9.5) | 4 (7.0) | 0.751 |
| GDM | 3 (7.1) | 6 (10.5) | 0.471 |
| Gestational hypertension | 2 (5.3) | 4 (8.5) | 0.69 |
| Preeclampsia | 2 (5.3) | 3 (6.4) | 1.00 |
| Waterpipe dependence scale | 6.0 (0.5) | 5.7 (0.4) | 0.612 |
| Mode of tobacco consumption (dual users only) | - | ||
| WPT and Cigarettes | - | 11 (19.3) | |
| WPT and ECigs | - | 5 (8.8) | |
| WPT and Cigars/Cigarillos/Little Cigars | - | 19 (33.3) | |
| WPT and Cigarettes and Ecigs | - | 1 (1.8) | |
| WPT and Cigarettes, and Cigars/Cigarillos/Little | - | 7 (12.3) | |
| Cigars | - | 5 (8.8) | |
| WPT and Ecigs, and Cigars/Cigarillos/Little Cigars | - | 9 (15.8) | |
| WPT and Cigarettes, ECigs, and | |||
| Cigars/Cigarillos/Little Cigars | |||
| Average WPT use in pregnancy | 12.3 (3.3) | 8.5 (1.9) | 0.352 |
| Number of times WPT used in pregnancy | 0.651 | ||
| Not used during pregnancy | 9 (21.4) | 7 (12.3) | |
| 1-2 times during pregnancy | 13 (31.0) | 24 (42.1) | |
| 3-9 times during pregnancy | 10 (23.8) | 11(19.3) | |
| >9 times during pregnancy | 10 (23.8) | 15 (26.3) | |
| PUQE score at 1st trimester | 9.1 (0.3) | 9.4 (0.2) | 0.572 |
| PUQE score at 3nd trimester | 8.0 (0.2) | 8.2 (0.2) | 0.602 |
Fisher’s exact
Wilcoxon rank-sum
Data are reported as mean (standard deviation) for continuous variables, median (range) for ordinal variables and n (percent). Bold signifies statistical significance.
Dual users refers to participants who used both WPT and cigarettes, while solo use refers to WPT use alone
Abbreviations: WPT = waterpipe tobacco, PUQE =pregnancy unique quantification of emesis, BMI = body mass index (kg/m2), GDM = gestational diabetes mellitus, HTN = hypertension, Ecigs = electronic cigarettes
Frequency of WPT use
The data was also analyzed by low WPT use (N=58) versus high WPT use (N=34) during pregnancy (Table 2). Participants who reported high WPT use were significantly more likely to identify as Latina/Hispanic ethnicity than low WPT users (73.5% vs. 48.3%, respectively; p<0.02). There were no significant baseline differences between groups in reported race. There were no other demographic differences in terms of pre-pregnancy BMI, gravidity, parity, rates of gestational diabetes (GDM) or hypertension based on WPT usage. Pregnant people who reported high WPT use had significantly higher scores on the waterpipe dependence scale (7.2) in comparison to low users (5.3) p<0.02. There were no significant differences in the PUQE score in either the 1st or the 3rd trimester for participants who reported high versus low WPT use.
Table 2.
Demographics and PUQE score by High and Low Frequency of WPT Use
| Low use (1-8 times) N=58 |
High use (9+ times) N=34 |
P-value | |
|---|---|---|---|
| Race | 0.301 | ||
| First Nations | 1 (1.7) | 0 (0.0) | |
| Asian | 3 (5.2) | 0 (0.0) | |
| Pacific Islander | 0 (0.0) | 0 (0.0) | |
| Black | 13 (22.4) | 4 (11.8) | |
| White | 12 (43.1) | 7 (20.6) | |
| Other | 29 (50.0) | 23 (67.6) | |
| Ethnicity | 0.02 1 | ||
| Latina/Hispanic | 28 (48.3) | 25 (73.5) | |
| Not Latina/Hispanic | 30 (51.7) | 9 (26.5) | |
| Pre-pregnancy BMI | 28.74 (0.9) | 29.18(1.2) | 0.732 |
| Parity | 1 (0-4) | 1 (0-3) | 0.252 |
| Hyperthyroidism | 1 (2.1) | 3 (9.7) | 0.291 |
| Hypothyroidism | 0 | 1 (3.2) | 0.391 |
| Asthma | 12 (25.0) | 5 (16.1) | 0.411 |
| Chronic hypertension | 3 (6.3) | 4 (12.9) | 0.311 |
| Gestational diabetes | 4 (8.3) | 4 (12.9) | 0.511 |
| Gestational hypertension | 3 (6.3) | 3 (9.7) | 0.671 |
| Preeclampsia | 1 (2.1) | 3 (9.7) | 0.291 |
| Dual/Poly Users | 36 (62.1) | 18 (52.9) | 0.391 |
| Waterpipe dependence scale | 5.3 (0.4) | 7.2 (0.6) | 0.02 2 |
| PUQE score at 1st trimester | 9.3 (0.3) | 9.1 (0.3) | 0.642 |
| PUQE score at 3rd trimester | 7.9 (0.2) | 8.3 (0.4) | 0.442 |
Fisher’s exact
Wilcoxon rank-sum
Data are reported as mean (standard deviation) for continuous variables, median (range) for ordinal variables and n (percent). Bold signifies statistical significance.
Abbreviations: WPT = waterpipe tobacco, PUQE =pregnancy unique quantification of emesis, BMI = body mass index (kg/m2), GDM = gestational diabetes mellitus, HTN = hypertension
Comment:
Principal findings:
In this secondary analysis of a prospective cohort study of pregnant people who self-reported WPT use in pregnancy, most participants reported moderate severity of their nausea and vomiting symptoms. However, the severity of nausea and vomiting symptoms did not differ by WPT use group (WPT-only vs. dual/poly WPT use) or frequency of use (high vs. low)..
Results:
This study evaluated the symptoms of nausea and vomiting of pregnancy and medical conditions among participants who reported use of WPT in pregnancy. The majority of participants who used WPT reported moderate nausea and vomiting symptoms of pregnancy. No differences in nausea and vomiting symptoms among participants who only used WPT and those who used both WPT and other tobacco products were identified. Similarly, there was also no difference in symptoms of nausea or vomiting among those with low and high frequency of WPT use.
Additionally, we evaluated the rates of medical comorbidities among this cohort including medical complications of pregnancy such as GDM and preeclampsia and did not find any significant differences between groups when assessing by frequency of WPT use or sole vs dual/poly WPT use. Rates of thyroid disease, hypertensive disease and diabetes also did not differ between groups. Rates of asthma were higher among sole WPT users as compared to dual/poly WPT users.
Clinical Implications
Prior data has shown that cigarette smokers have less nausea and vomiting of pregnancy than nonsmokers20. We therefore expected lower PUQE scores in pregnant people who used WPT tobacco more frequently; however, our results were not consistent with this hypothesis. One reason for this may be that people who use solely WPT are likely to be sporadic users, as compared to those who use cigarettes, which tend to be used daily. Alternatively, this may be due to the fact that participants with more severe nausea and vomiting symptoms did not elect to participate in the research due to the seriousness of their symptoms, leaving only those with mild to moderate symptoms who felt well enough to engage.
Despite patient knowledge that tobacco is harmful to the developing fetus 21, 22, 2.5% of pregnant people continue to report use of WPT in pregnancy in the United States5. Studies from Iran and Jordan have demonstrated adverse pregnancy outcomes with WPT use in pregnancy including lower birth weights.3, 23, 24 This highlights the importance of continued research and need for patient education on the use of WPT during pregnancy.
Future research
Prior research from our group has evaluated tobacco flavor preferences for pregnant people of reproductive age and found that sweet flavors were preferred outside of pregnancy, while pregnant patients prefer menthol/mint and fruit flavors13, 25. As ginger and peppermint flavored teas and lozenges are often used as nonmedical treatment of nausea in early pregnancy9, this may be why patients prefer these flavors. Future research into why pregnant participants have these preferences, could assist in more public health effort to limit the sale and advertisement of these products. Additionally, providers should continue to advocate for legislation which addresses the sale of flavored tobacco products as this may be an area for intervention in order to decrease use amongst pregnant individuals.
Strengths and Limitations
To our knowledge this is one of the first analyses of the association of WPT use and nausea/vomiting of pregnancy. This study adds a moderate size cohort to the paucity of data from the United States as related to evaluation of symptoms of nausea and vomiting among pregnant patients who used WPT. Additionally, this study includes high quality data that was prospectively collected by trained research personnel with validated instruments.
As with any survey study, there is recall and response bias. Additionally, data was not collected on the use of antinausea/antiemetic medications in the treatment of nausea and vomiting symptoms, need for hospitalization, weight gain or weight loss or diagnosis of hyperemesis gravidarum which could further help to delineate symptom severity. Also, as this study focused on participants who reported WPT use and we did not have a group of participants without any WPT use to serve as a control group.
Conclusions
The majority of pregnant people who used WPT during pregnancy reported moderate nausea and vomiting symptoms which did not vary by frequency of WPT use or dual use of WPT and other tobacco products. Further research to characterize motivation and factors for WPT use in pregnancy are necessary.
Acknowledgments
Funding for this study and manuscript preparation was supported by the National Institute on Drug Abuse (NIDA) of the National Institutes of Health and the Center for Tobacco Products of the U.S. Food and Drug Administration (FDA) under grant 5R01 DA042484 to Laura R. Stroud, PhD, and Lori A.J. Scott-Sheldon, PhD. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health or the Food and Drug Administration. NIDA, CTP, and FDA had no role in the study design, collection, analysis or interpretation of the data, writing the manuscript, or the decision to submit the paper for publication.
Footnotes
Declaration: The authors do not have any conflicts of interest to report.
References:
- 1.Tobacco and Nicotine Cessation During Pregnancy: ACOG Committee Opinion, Number 807. Obstet Gynecol. May 2020;135(5):e221–e229. doi: 10.1097/AOG.0000000000003822 [DOI] [PubMed] [Google Scholar]
- 2.Chaaya M, Awwad J, Campbell OM, Sibai A, Kaddour A. Demographic and psychosocial profile of smoking among pregnant women in Lebanon: public health implications. Matern Child Health J. Sep 2003;7(3):179–86. doi: 10.1023/a:1025136421230 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Nematollahi S, Mansournia MA, Foroushani AR, et al. The effects of water-pipe smoking on birth weight: a population-based prospective cohort study in southern Iran. Epidemiol Health. 2018;40:e2018008. doi: 10.4178/epih.e2018008 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Mirahmadizadeh A, Nakhaee N. Prevalence of waterpipe smoking among rural pregnant women in Southern Iran. Med Princ Pract. 2008;17(6):435–9. doi: 10.1159/000151563 [DOI] [PubMed] [Google Scholar]
- 5.Kurti AN, Redner R, Lopez AA, et al. Tobacco and nicotine delivery product use in a national sample of pregnant women. Prev Med. Nov 2017;104:50–56. doi: 10.1016/j.ypmed.2017.07.030 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.In: Eaton DL, Kwan LY, Stratton K, eds. Public Health Consequences of E-Cigarettes. 2018. [PubMed] [Google Scholar]
- 7.Mahboub B, Mohammad AB, Nahle A, Vats M, Al Assaf O, Al-Zarooni H. Analytical Determination of Nicotine and Tar Levels in Various Dokha and Shisha Tobacco Products. J Anal Toxicol. Sep 1 2018;42(7):496–502. doi: 10.1093/jat/bky029 [DOI] [PubMed] [Google Scholar]
- 8.Malson JL, Sims K, Murty R, Pickworth WB. Comparison of the nicotine content of tobacco used in bidis and conventional cigarettes. Tob Control. Jun 2001;10(2):181–3. doi: 10.1136/tc.10.2.181 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Committee on Practice B-O. ACOG Practice Bulletin No. 189: Nausea And Vomiting Of Pregnancy. Obstet Gynecol. Jan 2018;131(1):e15–e30. doi: 10.1097/AOG.0000000000002456 [DOI] [PubMed] [Google Scholar]
- 10.Ozgoli G, Saei Ghare Naz M. Effects of Complementary Medicine on Nausea and Vomiting in Pregnancy: A Systematic Review. Int J Prev Med. 2018;9:75. doi: 10.4103/ijpvm.IJPVM_430_16 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Kallen B, Lundberg G, Aberg A. Relationship between vitamin use, smoking, and nausea and vomiting of pregnancy. Acta Obstet Gynecol Scand. Oct 2003;82(10):916–20. [PubMed] [Google Scholar]
- 12.El-Zaatari ZM, Chami HA, Zaatari GS. Health effects associated with waterpipe smoking. Tob Control. Mar 2015;24 Suppl 1:i31–i43. doi: 10.1136/tobaccocontrol-2014-051908 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Stroud L, Werner E, Matteson K, et al. Waterpipe (hookah) tobacco use in pregnancy: use, preferences and perceptions of flavours. Tob Control. Feb 2020;29(Suppl 2):s62–s71. doi: 10.1136/tobaccocontrol-2019-054984 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Stroud LR, Papandonatos GD, Sharma E, et al. Flavored waterpipe tobacco preferences, perceptions, and use in pregnant women: A latent factor mapping approach. Addict Behav. Mar 2022;126:107194. doi: 10.1016/j.addbeh.2021.107194 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Sobell LSaM. Timeline Followback: A technique for assessing self-reported alcohol consumption. In: Allen RLaJ, ed. Measuring alcohol consumption: psychosocial and biochemical methods. Humana Press; 1992. [Google Scholar]
- 16.Sobell LSaM. Alcohol Timeline Followback users' manual. Addiction Research Foundation; 1995. [Google Scholar]
- 17.Robinson SM, Sobell LC, Sobell MB, Leo GI. Reliability of the Timeline Followback for cocaine, cannabis, and cigarette use. Psychol Addict Behav. Mar 2014;28(1):154–62. doi: 10.1037/a0030992 [DOI] [PubMed] [Google Scholar]
- 18.Lacasse A, Rey E, Ferreira E, Morin C, Berard A. Validity of a modified Pregnancy-Unique Quantification of Emesis and Nausea (PUQE) scoring index to assess severity of nausea and vomiting of pregnancy. Am J Obstet Gynecol. Jan 2008;198(1):71 e1–7. doi: 10.1016/j.ajog.2007.05.051 [DOI] [PubMed] [Google Scholar]
- 19.Hallit S, Obeid S, Sacre H, Salameh P. Lebanese Waterpipe Dependence Scale (LWDS-11) validation in a sample of Lebanese adolescents. BMC Public Health. Sep 6 2021;21(1):1627. doi: 10.1186/s12889-021-11662-3 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Little RE, Hook EB. Maternal alcohol and tobacco consumption and their association with nausea and vomiting during pregnancy. Acta Obstet Gynecol Scand. 1979;58(1):15–7. doi: 10.3109/00016347909154905 [DOI] [PubMed] [Google Scholar]
- 21.Kahr MK, Padgett S, Shope CD, et al. A qualitative assessment of the perceived risks of electronic cigarette and hookah use in pregnancy. BMC Public Health. Dec 21 2015;15:1273. doi: 10.1186/s12889-015-2586-4 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Azab M, Khabour OF, Alzoubi KH, et al. Exposure of pregnant women to waterpipe and cigarette smoke. Nicotine Tob Res. Jan 2013;15(1):231–7. doi: 10.1093/ntr/nts119 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Al-Sheyab NA, Al-Fuqha RA, Kheirallah KA, Khabour OF, Alzoubi KH. Anthropometric measurements of newborns of women who smoke waterpipe during pregnancy: a comparative retrospective design. Inhal Toxicol. Nov 2016;28(13):629–635. doi: 10.1080/08958378.2016.1244227 [DOI] [PubMed] [Google Scholar]
- 24.Nuwayhid IA, Yamout B, Azar G, Kambris MA. Narghile (hubble-bubble) smoking, low birth weight, and other pregnancy outcomes. Am J Epidemiol. Aug 15 1998;148(4):375–83. doi: 10.1093/oxfordjournals.aje.a009656 [DOI] [PubMed] [Google Scholar]
- 25.Scott-Sheldon LAJ, Stroud LR. Preferences and Perceptions of Flavored Hookah Tobacco among US Women. Am J Health Behav. May 1 2018;42(3):37–46. doi: 10.5993/AJHB.42.3.4 [DOI] [PubMed] [Google Scholar]