Abstract
Objective:
There is substantial evidence linking anxiety sensitivity and distress intolerance to depressive symptoms, and further evidence linking depressive symptoms to alcohol and cannabis use. However, the prospective indirect associations of anxiety sensitivity and distress intolerance with alcohol and cannabis use through depressive symptoms remain uncertain. Thus, the current study examined whether depressive symptoms mediated the associations between anxiety sensitivity and distress intolerance with alcohol and cannabis use frequency, quantity, and problems in a longitudinal sample of veterans.
Method:
Participants (N = 361; 93% male; 80% White) were military veterans with lifetime cannabis use recruited from a Veterans Health Administration in the Northeastern United States. Eligible veterans completed three semi-annual assessments. Prospective mediation models were used to test for the effects of baseline anxiety sensitivity and distress intolerance on alcohol and cannabis use quantity, frequency and problems at 12 months via depressive symptoms at 6 months.
Results:
Baseline anxiety sensitivity was positively associated with 12-month alcohol problems. Baseline distress intolerance was positively associated with 12-month cannabis use frequency and quantity. Baseline anxiety sensitivity and distress intolerance significantly predicted increased alcohol problems and cannabis use frequency at 12 months through depressive symptoms at 6 months. There were no significant indirect effects of anxiety sensitivity and distress intolerance on alcohol use frequency or quantity, cannabis use quantity, or cannabis problems.
Conclusions:
Anxiety sensitivity and distress intolerance share a common pathway to alcohol problems and cannabis use frequency through depressive symptoms. Interventions focused on modulating negative affectivity may reduce cannabis use frequency and alcohol problems.
Co-occurring depression and substance use are common in Operation Enduring Freedom/Operation Iraqi Freedom (OEF/OIF) veterans (Blore et al., 2015; Liu et al., 2017; Metrik et al., 2016), with this comorbidity associated with poorer substance use disorder (SUD) treatment outcomes (Najt et al., 2011). Negative-reinforcement motivational models of addiction posit that negative affect promotes substance use to relieve distress (Baker et al., 2004; McCarthy et al., 2010), and negative emotional states commonly precede relapse (McCarthy et al., 2005). Emerging empirical work indicates that psychological vulnerability traits of sensitivity to unpleasant physiological and psychological states (anxiety sensitivity) and the inability to tolerate them (distress intolerance) are linked with depression (Lass & Winer, 2020; Short et al., 2020). Further, Gunn and colleagues (2020) demonstrated prospective associations between depression and alcohol use and cannabis use among veterans. A transdiagnostic vulnerability framework describes the mechanisms whereby emotional vulnerability factors, which give rise to depression, may increase risk for cigarette use because of substance-induced affect-modulating effects and maladaptive coping (Leventhal & Zvolensky, 2015). The purpose of the current study was to apply this framework to examine whether the transdiagnostic emotional vulnerability traits of anxiety sensitivity and distress intolerance are associated with alcohol use, cannabis use, and problems via depressive symptoms in veterans.
Anxiety sensitivity, distress intolerance, and substance use
Affect intolerance (i.e., emotional vulnerability), characterized by one's perceived sensitivity to and diminished ability to withstand uncomfortable emotional states, has been implicated as a transdiagnostic vulnerability (Bernstein et al., 2009; Zvolensky et al., 2007). Two lower-order facets of affect intolerance are anxiety sensitivity and distress intolerance. Anxiety sensitivity is characterized by fear of anxiety-related internal experiences and the tendency to catastrophize the meaning of these experiences (Reiss et al., 1986). Distress intolerance is the inability to endure aversive psychological (e.g., depression) or physiological (e.g., pain) states (Leyro et al., 2010).
Cross-sectional studies suggest that anxiety sensitivity is associated with a range of alcohol and cannabis involvement, including alcohol use quantity and frequency, alcohol problems, cannabis use frequency, and cannabis problems in the general population (Bonn-Miller et al., 2007; DeMartini & Carey, 2011; Guillot et al., 2018; Zvolensky et al., 2018) and in veterans (Lehman & Cheung, 2002; Stewart et al., 2019; Teeters et al., 2020). In contrast, distress intolerance is cross-sectionally linked with more severe patterns of substance use, such as alcohol problems, alcohol use disorder (AUD) symptoms, and cannabis problems in nonveterans (Bujarski et al., 2012; Dennhardt & Murphy, 2011; Gorka et al., 2012; Farris et al., 2016; Khan et al., 2018). However, in veterans, distress intolerance is cross-sectionally associated with indices of alcohol and cannabis use, including alcohol and cannabis use frequency in the context of a quit attempt (Brooks Holliday et al., 2016; Hasan et al., 2015).
Prospective work on the associations between affect sensitivity and alcohol and cannabis use is limited and is primarily concerned with general population. In young adults, baseline anxiety sensitivity was associated with the future development of AUD (Schmidt et al., 2007). Baseline anxiety sensitivity and distress intolerance have also been found to be associated with more frequent future substance use in young adults (Cho et al., 2021). Another nonveteran study examined the interactive effects of lower-order facets of anxiety sensitivity (physical concerns, mental incapacitation, social concerns) on subsequent cannabis use measured via ecological momentary assessment, finding that mental incapacitation and social concerns interacted with cannabis craving to prospectively predict cannabis use intentions (Buckner et al., 2011).
Anxiety sensitivity, distress intolerance, depressive symptoms, and substance use
Elevated anxiety sensitivity and distress intolerance may increase risk for and maintain internalizing disorders (Koch et al., 2016; Shaw et al., 2021; Zvolensky et al., 2010) and can be targeted in transdiagnostic treatment (Boswell et al., 2013; Bullis et al., 2019; Keough & Schmidt, 2012; Leventhal & Zvolensky et al., 2015; Norr et al., 2014). Cross-sectional studies have linked anxiety sensitivity and distress intolerance to depressive symptoms in veterans (Brooks Holliday et al., 2016; Mitchell et al., 2014) and nonveterans (Williams et al., 2013). Prospective data indicate that anxiety sensitivity and distress intolerance predicted depressive symptoms across the life span. In a longitudinal twin study, Zavos and colleagues (2012) found that anxiety sensitivity prospectively predicted elevated depressive symptoms. In adult female sexual assault survivors, heightened anxiety sensitivity 1 week after the sexual assault prospectively predicted depressive symptoms (Short et al., 2020). A recent review of the prospective effects of distress intolerance on depression describes similar patterns in adolescents and adults (Lass & Winer, 2020).
Depressive symptoms are cross-sectionally associated with alcohol use (Brooks Holliday et al., 2016), symptoms of AUD (Yoon et al., 2015), cannabis use frequency, and cannabis problems in veterans (Ashwal-Malka et al., 2022; Metrik et al., 2016) and nonveterans (Dierker et al., 2018). Prospective data suggest that depressive symptoms are linked with indices of alcohol or cannabis use and the development of problems. In veterans, depressive symptoms prospectively predicted alcohol use frequency (Gunn et al., 2020). In a prospective, population-based study of adolescents and young adults, depressive symptoms predicted the persistence of AUD diagnosis (Copeland et al., 2012). Prospective risk of AUD was also found to be associated with prior depression in a longitudinal, population-based twin study (Kuo et al., 2006). In women, depression at age 24 was associated with future AUD (McCarty et al., 2009). Baseline depression was associated with onset of cannabis use and cannabis use disorder (CUD) diagnosis over a 10-year period from adolescence to young adulthood (Wittchen et al., 2007).
The current study builds and extends on previous work by testing depressive symptoms as a prospective mediator of the effects of anxiety sensitivity and distress intolerance on alcohol and cannabis use indices in a longitudinal sample of veterans. We seek to expand prior research on emotional vulnerability risk factors among veterans in several ways. First, insufficient evidence exists to discern the temporal relationships between emotional vulnerability risk factors, depression, and substance use in veterans. Second, the transdiagnostic vulnerability framework, which postulates paths from emotional vulnerability factors (e.g., anxiety sensitivity, distress intolerance) to depression and cigarette smoking (Leventhal & Zvolensky, 2015), has not been tested with alcohol use and cannabis use. A wealth of research has tested coping motives as a mediator of the associations between distal vulnerability factors (i.e., anxiety sensitivity, distress intolerance) and substance use (Bonn-Miller et al., 2014; Bujarski et al., 2012; Farris et al., 2016; Johnson et al., 2010; Metrik et al., 2016; Wahesh et al., 2020). Yet, far fewer studies to date have tested the possible mediational role of depressive symptoms in the association between transdiagnostic vulnerabilities of anxiety sensitivity and distress intolerance with substance use behaviors, and these studies are cross-sectional in nature (Lechner et al., 2014). Longitudinal designs are well suited to address how vulnerability factors affect the course of substance use and related problems. In addition, prospective data provide an opportunity to test a potential mechanism by which transdiagnostic emotional vulnerability factors influence alcohol and cannabis use. To accomplish this goal, this study examined the prospective associations of baseline anxiety sensitivity and distress intolerance on alcohol and cannabis use quantity, frequency, and problems reported 12 months after baseline, with depressive symptoms 6 months after baseline as a mediator of these relationships in a large, clinically relevant sample of veterans returning from deployments to Iraq and Afghanistan. Based on prior work, we expected that baseline anxiety sensitivity and distress intolerance would significantly predict depressive symptoms 6 months after baseline. We also expected significant associations between baseline anxiety sensitivity and distress intolerance with 12-month alcohol problems, cannabis use indices, and cannabis problems to be mediated by 6-month depressive symptoms. We expect significant effects of distress intolerance, and not anxiety sensitivity, on alcohol use quantity and frequency to be mediated by depressive symptoms.
Method
Sample and procedure
Participants (N = 361) were post–9/11/2001 OEF/OIF/OND (Operation New Dawn) veterans recruited from a Veterans Health Administration (VHA) medical center in the Northeastern United States (Metrik et al., 2022). Participants met the following eligibility criteria: (a) ≥18 years old, (b) OEF/IEF/OND veteran, and (c) lifetime cannabis use. Participants were excluded for suicide risk in the past 2 weeks, psychotic symptoms in the past month, a score of 23 or less on the Mini-Mental Status Exam (Folstein et al., 1975), or active duty at baseline assessment (see Metrik et al., 2016, for full eligibility criteria and recruitment methods). Eligible veterans were invited for a baseline session to sign informed consent and complete an interview and self-report measures. Follow-up visits with a similar interview and self-report assessments completed by all participants occurred at 6 months (n = 312; 86.4%) and 12 months (n = 310; 85.9%). All study procedures were approved by Brown University and Providence VHA Institutional Review Boards. Participants were compensated $50 per visit and received a $50 bonus for completing all three sessions.
Measures
Demographics. Demographic information (e.g., age, sex, race/ethnicity) was verified in the VHA Computerized Patient Record System.
Anxiety sensitivity. Anxiety sensitivity was measured with the Anxiety Sensitivity Index–3 (ASI-3; Taylor et al., 2007), an 18-item self-report measure of the tendency to fear anxiety-related bodily sensations. The ASI-3 assesses three domains of anxiety sensitivity: physical (e.g., It scares me when my heart beats rapidly), cognitive (e.g., When my thoughts seem to speed up, I worry that I might be going crazy), and social concerns (e.g., When I tremble in the presence of others, I fear what people might think of me). Responders are asked to rate their agreement with each item based on their experiences with response options on a 5-point Likert scale ranging from 0 (very little) to 4 (very much), summed to create a total score with a possible range of 0–72. The total ASI-3 score was used in analyses. Internal consistency at baseline was excellent (α = .91).
Distress intolerance. Distress intolerance was measured with the Distress Tolerance Scale (DTS; Simons & Gaher, 2005), a 15-item scale assessing respondents’ perceived ability to experience and endure negative emotional states. The DTS assesses four domains of distress intolerance: Tolerance (e.g., Feeling distressed or upset is unbearable to me), Appraisal (e.g., My feelings of distress or feeling upset are not acceptable), Absorption (e.g., My feelings of distress are so intense that they completely take over), and Regulation (e.g., I’ll do anything to avoid feeling distressed or upset). Responders rate their agreement with each item based on their beliefs about feeling distressed using a 5-point Likert scale ranging from 1 (strongly agree) to 5 (strongly disagree). The total DTS score was used in analyses. Scores on this measure were recoded, such that higher scores indicate higher distress intolerance (lower distress tolerance) to mirror the direction of effects for anxiety sensitivity. Internal consistency at baseline was excellent (α = .92).
Depressive symptoms. Depressive symptoms were measured with the Inventory of Depression and Anxiety Symptoms–General Depression (IDAS-GD; Watson et al., 2008). The IDAS-GD includes 20 items rated on a 5-point Likert scale ranging from 1 (not at all) to 5 (extremely). These items assess symptoms experienced in the past 2 weeks, including specific depression symptoms (e.g., dysphoria, suicidality; “I felt depressed”) as well as symptoms of several anxiety disorders (e.g., panic, social anxiety; “I found myself worrying all the time”). Higher scores indicate more severe depressive symptoms. This scale demonstrates strong convergent validity in predicting major depressive disorder diagnosis as well as anxiety diagnoses (Stasik-O’Brien et al., 2019). Internal consistency was excellent at 6 months (α = .93).
Alcohol and cannabis use. The Timeline Followback Interview (TLFB; Dennis et al., 2004; Sobell & Sobell, 1992) is a calendar-assisted structured interview used to derive percentage of alcohol use and cannabis use days. The TLFB was administered at each visit (baseline, 6 months, and 12 months) and covered the 180 days preceding the visit. TLFB has high test–retest reliability and stability over periods of 180 days (Carey, 1997). The TLFB was also used to derive a measure of alcohol use quantity (i.e., drinks per day). Past-30-day cannabis use quantity was assessed with the following question: “In the past month, on average, how much marijuana per week do you think you used in ounces?” Responses ranged on a 12-point scale in common 1/16th to 1/8th increments from never used regularly to more than 1 ounce.
Alcohol problems. Alcohol problems were measured with the Short Index of Problems (SIP; Miller et al., 1995), a 15-item measure assessing past-month consequences related to alcohol use (e.g., When drinking, I have done impulsive things that I regretted later). Items are rated on a 4-point scale, ranging from 1 (never) to 4 (daily or almost daily). Higher scores indicate more alcohol problems. Internal consistency was excellent at 12 months (α = .90).
Cannabis problems. Cannabis problems were measured with the Marijuana Problems Scale (MPS; Stephens et al., 2000), a 19-item self-report questionnaire assessing problems experienced in the past 90 days because of cannabis use (e.g., problems between you and your partner). Three additional problems were assessed (to drink a lot more than you normally would have; to take risks, like driving a car while under the influence; to take risks, like riding in car with a driver who is under the influence), resulting in the assessment of 22 total problems. Response options included 0 (no problem), 1 (minor problem), and 2 (serious problem). A sum of the total numbers of problems endorsed was used as an outcome variable. Internal consistency was excellent at 12 months (α = .90).
Substance use disorder diagnosis. Symptoms of AUD and CUD were assessed using the Structured Clinical Interview for DSM-5 Non-Patient Edition (SCID-NP; First et al., 2015).
Analytic strategy
Preliminary descriptive analyses and bivariate correlations were conducted for all variables in IBM SPSS Statistics for Windows, Version 27 (IBM Corp., Armonk, NY). Primary analyses were conducted in Mplus Version 7 (Muthén & Muthén, 1998). All models were conducted using the full sample of 361 participants. Path modeling was used to examine the effects of anxiety sensitivity and distress intolerance on outcome variables at 12 months (alcohol use, alcohol problems, cannabis use, cannabis problems). The zero-inflated negative binomial (ZINB) distribution was used for 12-month cannabis problems, the only count variable. ZINB models simultaneously evaluate two different distributions of data. The logistic portion of the model estimates a binary outcome (likelihood of being an excess zero, i.e., not experiencing cannabis problems). The count portion of the model estimates a count/continuous outcome (number of cannabis problems), including only the proportion of zeros that would be expected in a negative binomial distribution with the given sample mean and variance (Wagner et al., 2015). All other outcomes were modeled as continuous.
Prospective mediation was tested using bootstrapped joint significance tests for indirect effects (MacKinnon et al., 2004). Mediation analysis involves examining associations between the independent variables and mediator (a-path); the mediator and outcomes, controlling for the independent variables (b-path); the independent variables and outcomes (c-path); and the independent variables and outcomes, controlling for the mediator (ć-path; Figure 1). We examined the indirect effect of baseline distress intolerance and anxiety sensitivity on 12-month alcohol use, alcohol problems, cannabis use, and cannabis problems through 6-month depressive symptoms in one model. We did not require a significant direct effect and instead tested the indirect effects of the baseline variables on all outcomes (Hayes, 2009; Hayes & Rockwood, 2017; Rucker et al., 2011). Analyses controlled for sex, race/ethnicity (non-Hispanic White vs. other race/ ethnicities), and baseline past-6-month alcohol and cannabis use. All significant direct and indirect effects reported were robust to these covariates.
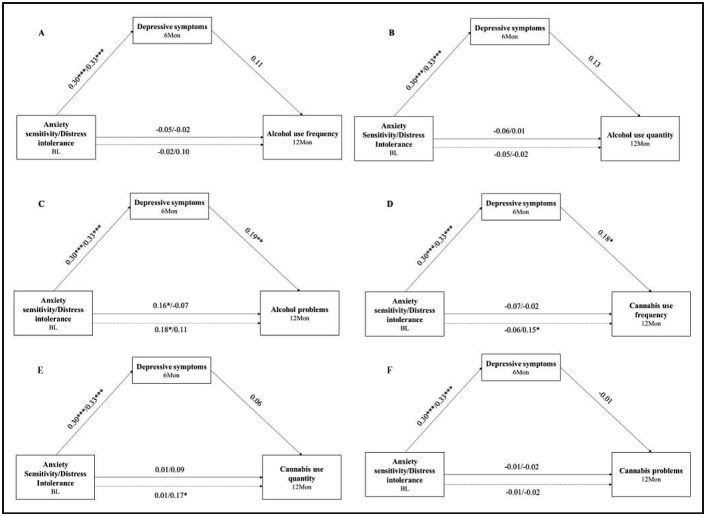
Figure 1.
Prospective mediation models. Mediation of the relation between anxiety sensitivity/distress intolerance and alcohol use frequency (Panel A), alcohol problems (Panel B), cannabis use frequency (Panel C), number of cannabis problems (Panel D), alcohol use quantity (Panel E), and cannabis use quantity (Panel F). a-path = arrow from anxiety sensitivity/distress intolerance to depressive symptoms; b-path = arrow from depressive symptoms to substance use outcome (e.g., alcohol problems); c-path = dotted line from anxiety sensitivity/distress intolerance to substance use outcome;ć-path = arrow from anxiety sensitivity/distress intolerance to substance use outcome. All models included baseline alcohol and cannabis use as covariates. BL = baseline; Mon. = months. *p < .05; **p < .01; ***p < .001.
Results
Descriptive statistics
Demographics are in Table 1. At baseline, 90% of the sample reported at least one instance of alcohol use in the past 6 months, and 38.2% of the sample reported at least one instance of cannabis use. The average alcohol use and cannabis use rates in the overall sample were approximately 25% and 16%, respectively, of days in the 6 months before baseline. Among those endorsing alcohol use, the average rate was 29.9% days. Among those endorsing cannabis use, the average rate was 42.5% days. As previously reported, 15% of the sample met diagnosis of past-month major depressive disorder according to the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5; American Psychiatric Association, 2013; Gunn et al., 2020), and 13% met diagnosis of past-month posttraumatic stress disorder according to the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV; American Psychiatric Association, 1994; Metrik et al., 2022). Regarding SUDs, 31.3% of the sample met DSM-5 criteria for AUD in the past year, and 14.7% of the sample met criteria for CUD in the past year at baseline.
Table 1.
Sample demographics and baseline characteristics (N = 361)

| Variable | n | % |
|---|---|---|
| Sex | ||
| Male | 337 | 93 |
| Race | ||
| White | 289 | 80 |
| Black/African American | 16 | 4 |
| Asian | 6 | 2 |
| Native Hawaiian/Pacific Islander | 2 | 1 |
| American Indian/Alaska Native | 2 | 1 |
| Multiracial | 17 | 4 |
| Other | 29 | 8 |
| Ethnicity | ||
| Hispanic/Latino(a) | 43 | 27 |
| Marital status | ||
| Single/never married | 116 | 32 |
| Married/living with partner | 173 | 48 |
| Divorced/separated | 72 | 20 |
| Employment status | ||
| Employed | 283 | 78 |
| Unemployed/homemaker | 67 | 19 |
| Student | 87 | 24 |
| Military service | 101 | 28 |
| Military operation(s) served in | ||
| Operation Enduring Freedom (OEF) | 269 | 75 |
| Operation Iraqi Freedom (OIF) | 191 | 53 |
| Operation New Dawn (OND) | 71 | 20 |
| Prescribed any medication | 219 | 61 |
| M | SD | |
| Age | 33.56 | 9.44 |
| Years of education completed | 13.73 | 2.11 |
| Number of deployments post-9/11/2001 | 1.88 | 1.15 |
| Years since last deployment | 3.95 | 2.79 |
| Baseline % alcohol use days (past 6 months) | 25.13 | 28.83 |
| Baseline % cannabis use days (past 6 months) | 16.23 | 32.85 |
| Number of alcohol problems at 12 months | 1.84 | 3.17 |
| Number of cannabis problems at 12 months | 0.93 | 2.44 |
| Baseline % other drug use | ||
| (nonalcohol/cannabis, past 6 months) | 4.07 | 15.02 |
Table 2 presents bivariate correlations among study variables. Baseline anxiety sensitivity and distress intolerance variables were positively associated. Anxiety sensitivity and distress intolerance were positively associated with depressive symptoms and cannabis use frequency and quantity. Anxiety sensitivity was positively associated with alcohol problems. Distress intolerance was positively associated with cannabis problems. Depressive symptoms were positively associated with alcohol problems, cannabis use frequency, cannabis use quantity, and cannabis problems.
Table 2.
Bivariate correlations
| 1. | 2. | 3. | 4. | 5. | 6. | 7. | 8. | M (SD) | |
|---|---|---|---|---|---|---|---|---|---|
| 1. BL Anxiety sensitivity (ASI-3) | 16.22(12.51) | ||||||||
| 2. BL Distress intolerance (DTS) | 61*** | 2.49 (0.84) | |||||||
| 3. M6 Depressive symptoms (IDAS-GD) | 49*** | .50*** | 41.99(13.03) | ||||||
| 4. YR Alcohol use frequency | -.02 | -.05 | .06 | 25.85 (30.04) | |||||
| 5. YR Alcohol use quantity | .11 | .09 | .08 | .15* | 1.23 (2.07) | ||||
| 6. YR Alcohol problems (SIP) | .21*** | .10 | .22*** | .34*** | .30** | 16.81 (3.63) | |||
| 7. YR Cannabis use frequency | .14* | .22*** | .24*** | -.09 | .12* | -.03 | 16.58 (32.93) | ||
| 8. YR Cannabis use quantity | .18** | .25*** | .23*** | -.10 | .14* | .05 | .82*** | 0.97 (2.14) | |
| 9. YR Cannabis problems (MPS) | .11 | .13* | .12* | -.07 | .07 | .04 | .39*** | .41*** | 0.93 (2.45) |
Notes: Correlations are Pearson correlations. BL = baseline; ASI-3 = Anxiety Sensitivity Index–3; DTS = Distress Tolerance Scale; M6 = 6 months after baseline; IDAS-GD = Inventory of Depression and Anxiety Symptoms–General Depression; YR = 12 months after baseline; SIP = Short Index of Problems; MPS = Marijuana Problems Scale.
p < .05;
p < .01;
p < .001.
Prospective mediation
Alcohol-related outcomes. Results are presented in Table 3, and prospective mediation models are depicted in Figure 1. Baseline anxiety sensitivity (c-path; b = 0.18, SE = 0.07, p = .01) had a significant effect on 12-month alcohol problems but not alcohol use frequency or quantity. Depressive symptoms at 6 months (b-path; b = 0.19, SE = 0.07, p = .008) had a significant effect on 12-month alcohol problems but not alcohol use frequency or quantity. There was no indirect effect of anxiety sensitivity on alcohol use frequency or quantity via depressive symptoms (Figures 1a and 1b). The indirect effect of baseline anxiety sensitivity on 12-month alcohol problems through 6-month depressive symptoms was significant (b = 0.06, SE = 0.02, p = .01), suggesting that 6-month depressive symptoms mediated the relation between baseline anxiety sensitivity and 12-month alcohol problems (Figure 1c).
Table 3.
Indirect effects of anxiety sensitivity and distress intolerance on alcohol outcomes via depressive symptoms
| Variable | Alcohol use frequency | Alcohol use quantity | Alcohol problems | |||
|---|---|---|---|---|---|---|
| Anxiety sensitivity β (SE) [95% CI] | Distress intolerance β (SE) [95% CI] | Anxiety sensitivity β (SE) [95% CI] | Distress intolerance β (SE) [95% CI] | Anxiety sensitivity β (SE) [95% CI] | Distress intolerance β (SE) [95% CI] | |
| b-path | .11 (.07) | .13 (.6) | .19**(.07) | |||
| c-path | -.02 (.08) | .10 (.08) | -.05 (.08) | -.02 (.07) | .18 (.07)* | .11 (.08) |
| [-.19, .14] | [-.25, .05] | [-.04, .02] | [-.40, .28] | [.04, .31] | [-.25, .04] | |
| c’-path | -.05 (.05) | -.02 (.05) | -.06 (.09) | .01 (.07) | .16 (.07)* | -.07 (.07) |
| [-.15, .05] | [-.12, .09] | [-.23, .11] | [-.13, .15] | [.02, .29] | [-.21, .07] | |
| Indirect | .02 (.02) | .03 (.02) | .04 (.02) | .04 (.02) | .06 (.02)* | .06 (.03)* |
| [-.01, .05] | [-.01, .06] | [-.01, .08] | [-.01, .08] | [.01, .10] | [.01, .10] | |
Notes: Parameters are standardized. Mediation models also included covariates (sex, race/ethnicity, baseline alcohol and cannabis use) not presented.
p < .05;
p < .01.
Baseline distress intolerance had no significant effects on alcohol-related outcomes (c-paths). There was no indirect effect of distress intolerance on alcohol use frequency or quantity via depressive symptoms (Figures 1a and 1b). The indirect effect of baseline distress intolerance on 12-month alcohol problems through 6-month depressive symptoms was significant (b = 0.07, SE = 0.03, p = .01; Figure 1c).
Cannabis-related outcomes. There were no significant effects of baseline anxiety sensitivity on cannabis use quantity, frequency, and problems (c-paths). Depressive symptoms at 6 months had a significant effect on cannabis use frequency at 12 months (b-path; Table 4; b = 0.18, SE = 0.06, p = .004). The indirect effect of baseline anxiety sensitivity on 12-month cannabis use frequency was significant (b = 0.05, SE = 0.02, p = .03; Figure 1d). There were no significant indirect effects of anxiety sensitivity on cannabis use quantity or problems (Figures 1e & 1f).
Table 4.
Indirect effects of anxiety sensitivity and distress intolerance on cannabis outcomes via depressive symptoms
| Variable | Cannabis use frequency | Cannabis use quantity | Cannabis problems (number) | Cannabis problems (zero-inflated) | ||||
|---|---|---|---|---|---|---|---|---|
| Anxiety sensitivity β (SE) [95% CI] | Distress intolerance β (SE) [95% CI] | Anxiety sensitivity β (SE) [95% CI] | Distress intolerance β (SE) [95% CI] | Anxiety sensitivity β (SE) [95% CI] | Distress intolerance β (SE) [95% CI] | Anxiety sensitivity β (SE) [95% CI] | Distress intolerance β (SE) [95% CI] | |
| b-path | .18* (.06) | .06 (.07) | -.01 (.03) | .07 (.01) | ||||
| c-path | -.06 (.07) | .15 (.07)* | .01 (.07) | .17 (.07)* | -.01 (.04) | -.02 (.03) | -.006 (.003) | .003 (.004) |
| [-.21, .08] | [.01, .30] | [-.03, .03] | [.08, .79] | [-.09, .07] | [-.08, .04] | [-.01, .00] | [-.00, .01] | |
| c’-path | -.07 (.04) | -.02 (.04) | .01 (.07) | .09 (.06) | -.01 (.04) | -.02 (.03) | -.01 (.003) | .009 (.004) |
| [-.15, .02] | [-.10, .07] | [-.13, .15] | [-.03, .2] | [-.09, .07] | [-.08, .04] | [-.01, .00] | [-.00, .01] | |
| Indirect | .03 (.01)* | .03 (.01)* | .02 (.02) | .02 (.02) | .000 (.000) | -.001 (.003) | -.002 (.002) | .02 (.03) |
| [.003, .05] | [.003, .06] | [-.02, .04] | [-.03, .04] | [.00, .00] | [-.01, .004] | [-.01, .00] | [-.03, .06] | |
Notes: Parameters are standardized. Mediation models also included covariates (sex, race/ethnicity, baseline alcohol and cannabis use) not presented.
p < .05.
Baseline distress intolerance had a significant effect on 12-month cannabis use frequency (c-path; b = 0.15, SE = 0.07, p = .04) and cannabis use quantity (c-path; b = 0.17, SE = 0.07, p = .03). The indirect effect of baseline distress intolerance on cannabis use frequency through 6-month depressive symptoms was significant (b = 0.06, SE = 0.02, p = .02; Figure 1d). There were no significant indirect effects of distress intolerance on cannabis use quantity or problems (Figures 1e & 1f). Using the problem severity score of the MPS did not alter these results (Hodgins & Stea, 2018).
Discussion
The current study aimed to examine whether depressive symptoms mediated the prospective associations between anxiety sensitivity and distress intolerance and indices of alcohol use and cannabis use in veterans. The results suggest that anxiety sensitivity and distress intolerance may demonstrate the same indirect effects on alcohol problems and cannabis use frequency through depressive symptoms. Previous studies have suggested that individuals high in anxiety sensitivity may be at risk for alcohol problems, particularly if they endorse drinking to cope with negative affect (Novak et al., 2003). Our hypothesis that depressive symptoms would mediate the association between anxiety sensitivity and alcohol problems was supported. As expected, the relationship between distress intolerance and alcohol problems was also mediated by depressive symptoms. Individuals experiencing depressive symptoms likely drink, at least partially, to relieve negative affect. This drinking pattern is more likely to result in higher-risk alcohol use (Jacobson et al., 2008). In contrast, the results of the current study do not support a significant role for anxiety sensitivity and distress intolerance in alcohol use frequency or quantity. Alcohol is legal and easily accessible, and drinking motives vary substantially. The results of this study may be explained by literature suggesting that drinking to cope with negative affect is related to alcohol problems (Cooper et al., 2016). The results of our study are consistent with work demonstrating that anxiety sensitivity tends to be cross-sectionally associated with alcohol problems but not alcohol use consumption and suggest that distress intolerance may demonstrate a similar pattern (Chavarria et al., 2015; Kelly et al., 2020).
The hypothesis that anxiety sensitivity and distress intolerance are related to cannabis use frequency through depressive symptoms was also supported. As expected, there was no significant association between anxiety sensitivity or distress intolerance and cannabis use quantity.At the time of data collection, recreational cannabis use was not regionally legal or decriminalized. Although all veterans resided in states with medical cannabis laws, access to cannabis was significantly lower than to alcohol, as participants were obtaining cannabis illicitly or with a medical marijuana card. In prior work on cannabis use motives among individuals using cannabis medicinally in this sample, anxiety/stress, posttraumatic stress disorder, pain, and depression were among the most frequently endorsed conditions for cannabis use (Metrik et al., 2018). Thus, veterans with heightened anxiety sensitivity or distress intolerance may be more likely to seek cannabis to alleviate these negative psychological/physical experiences, potentially resulting in more frequent cannabis use.
Despite sharing common associations with alcohol problems and cannabis use frequency, anxiety sensitivity and distress intolerance may have differential direct effects. In this study, anxiety sensitivity had a direct effect on alcohol problems, whereas distress intolerance had direct effects on cannabis use frequency and quantity. Consistent with Leventhal and Zvolensky's (2015) transdiagnostic vulnerability framework, the results of our study suggest that this pattern of alcohol use may develop because of depressive symptoms. In contrast, distress intolerance appears to relate to indices of cannabis use but not problems, such that higher distress intolerance leads one to use greater quantities of cannabis more frequently without endorsement of negative consequences. Such a pattern suggests that individuals high in distress intolerance may use cannabis with greater frequency to relieve depressive symptoms and may associate cannabis with therapeutic benefits instead of problems (Metrik et al., 2018). Future studies should consider other possible mechanisms by which anxiety sensitivity and distress intolerance prospectively influence substance use.
Recent work has identified anxiety sensitivity, distress intolerance, depressive symptoms, and substance use as treatment targets that may be related. Norr and colleagues (2014) found that the effects of intervention on internalizing symptoms were mediated by improvements in anxiety sensitivity and distress intolerance. In addition, distress intolerance may improve following SUD treatment (Reese et al., 2019). Improvements in anxiety sensitivity have also been linked to reductions in alcohol use (Wolitzky-Taylor et al., 2018). Mood management treatment has been associated with improvements in negative affect and lower rates of cannabis use among individuals with CUD and high anxiety sensitivity or distress intolerance (Wolitzky-Taylor et al., 2022). Recent work in veterans suggests that anxiety sensitivity and distress intolerance may be appropriate treatment targets for reducing alcohol and other drug use (Vujanovic et al., 2022). There are well-established interventions for alcohol use, cannabis use, and co-occurring depressive symptoms (Kay-Lambkin et al., 2009). In addition, integrated treatment focused on depressive symptoms and substance use may be more effective than treatment with a singular focus (Baker et al., 2010). Consistent with this literature, our results suggest that anxiety sensitivity, distress intolerance, and depressive symptoms may all serve as treatment targets for alcohol problems and reduction in cannabis use. Future work could also examine whether the lower-order facets of anxiety sensitivity and distress intolerance also exhibit similar associations with substance use outcomes.
To our knowledge, this is the first study to examine the potential effects of anxiety sensitivity and distress intolerance on a range of indices of alcohol and cannabis involvement in a longitudinal veteran sample. The longitudinal nature of the study allowed for the examination of a clinically relevant mechanism by which these factors influence alcohol and cannabis involvement. This study serves as a conservative examination of pathways to alcohol use and cannabis use in a sample with diverse patterns of substance use.
The results of this study should be considered in the context of a few limitations. First, this sample consisted of disproportionately male, White veterans, limiting the generalizability of these results to other demographic groups. A recent study suggested that distress intolerance is associated with alcohol use in women but not in men, highlighting the potential importance of accounting for sex (Gilmore et al., 2018). Similarly, literature suggests that distress intolerance was associated with alcohol problems in African American but not European American college students (Dennhardt & Murphy, 2011). Racial discrimination may also influence problems that individuals may experience when using alcohol or cannabis. The measure of depressive symptoms in this study assessed symptoms over the past 2 weeks, which may not provide an accurate representation of symptoms experienced in a 6-month period. Last, although the current study design provides important information on the prospective associations between anxiety sensitivity and distress intolerance with substance use outcomes among veterans, interpretation of findings may be limited by using covariates of baseline cannabis use and alcohol use but not all indices of substance use.
Footnotes
This work was supported by National Institute on DrugAbuse Grants R01 DA033425 (Jane Metrik and Brian Borsari) and T32 DA016184 (principal investigator: Damaris J. Rohsenow) and National Institute on Alcohol Abuse and Alcoholism Grant K08 AA027551 (principal investigator: Rachel L. Gunn). The authors have no conflicts of interest to declare.
References
- American Psychiatric Association. (4th ed.). Washington, DC: Author; 1994. Diagnostic and statistical manual of mental disorders. [Google Scholar]
- American Psychiatric Association. (5th ed.). Arlington, VA: Author; 2013. Diagnostic and statistical manual of mental disorders. [Google Scholar]
- Ashwal-Malka A., Tal-Kishner K., Feingold D. Moral injury and cannabis use disorder among Israeli combat veterans: The role of depression and perceived social support. Addictive Behaviors. 2022;124:107114. doi: 10.1016/j.addbeh.2021.107114. doi:10.1016/j.addbeh.2021.107114. [DOI] [PubMed] [Google Scholar]
- Baker A. L., Kavanagh D. J., Kay-Lambkin F. J., Hunt S. A., Lewin T. J., Carr V. J., Connolly J. Randomized controlled trial of cognitive-behavioural therapy for coexisting depression and alcohol problems: Short-term outcome. Addiction. 2010;105:87–99. doi: 10.1111/j.1360-0443.2009.02757.x. doi:10.1111/j.1360-0443.2009.02757.x. [DOI] [PubMed] [Google Scholar]
- Baker T. B., Piper M. E., McCarthy D. E., Majeskie M. R., Fiore M. C. Addiction motivation reformulated: An affective processing model of negative reinforcement. Psychological Review. 2004;111:33–51. doi: 10.1037/0033-295X.111.1.33. doi:10.1037/0033-295X.111.1.33. [DOI] [PubMed] [Google Scholar]
- Bernstein A., Zvolensky M. J., Vujanovic A. A., Moos R. Integrating anxiety sensitivity, distress tolerance, and discomfort intolerance: A hierarchical model of affect sensitivity and tolerance. Behavior Therapy. 2009;40:291–301. doi: 10.1016/j.beth.2008.08.001. doi:10.1016/j.beth.2008.08.001. [DOI] [PubMed] [Google Scholar]
- Blore J. D., Sim M. R., Forbes A. B., Creamer M. C., Kelsall H. L. Depression in Gulf War veterans: A systematic review and meta-analysis. Psychological Medicine. 2015;45:1565–1580. doi: 10.1017/S0033291714001913. doi:10.1017/S0033291714001913. [DOI] [PubMed] [Google Scholar]
- Bonn-Miller M. O., Boden M. T., Bucossi M. M., Babson K. A. Self-reported cannabis use characteristics, patterns and helpfulness among medical cannabis users. American Journal of Drug and Alcohol Abuse. 2014;40:23–30. doi: 10.3109/00952990.2013.821477. doi:10.3109/00952990.2013.821477. [DOI] [PubMed] [Google Scholar]
- Bonn-Miller M. O., Zvolensky M. J., Bernstein A. Marijuana use motives: Concurrent relations to frequency of past 30-day use and anxiety sensitivity among young adult marijuana smokers. Addictive Behaviors. 2007;32:49–62. doi: 10.1016/j.addbeh.2006.03.018. doi:10.1016/j.addbeh.2006.03.018. [DOI] [PubMed] [Google Scholar]
- Boswell J. F., Farchione T. J., Sauer-Zavala S., Murray H. W., Fortune M. R., Barlow D. H. Anxiety sensitivity and interoceptive exposure: A transdiagnostic construct and change strategy. Behavior Therapy. 2013;44:417–431. doi: 10.1016/j.beth.2013.03.006. doi:10.1016/j.beth.2013.03.006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Brooks Holliday S., Pedersen E. R., Leventhal A. M. Depression, posttraumatic stress, and alcohol misuse in young adult veterans: The transdiagnostic role of distress tolerance. Drug and Alcohol Dependence. 2016;161:348–355. doi: 10.1016/j.drugalcdep.2016.02.030. doi:10.1016/j.drugalcdep.2016.02.030. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Buckner J. D., Keough M. E., Schmidt N. B. Problematic alcohol and cannabis use among young adults: The roles of depression and discomfort and distress tolerance. Addictive Behaviors. 2007;32:1957–1963. doi: 10.1016/j.addbeh.2006.12.019. doi:10.1016/j.addbeh.2006.12.019. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Buckner J. D., Zvolensky M. J., Smits J. A. J., Norton P. J., Crosby R. D., Wonderlich S. A., Schmidt N. B. Anxiety sensitivity and marijuana use: An analysis from ecological momentary assessment. Depression and Anxiety. 2011;28:420–426. doi: 10.1002/da.20816. doi:10.1002/da.20816. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bujarski S. J., Norberg M. M., Copeland J. The association between distress tolerance and cannabis use-related problems: The mediating and moderating roles of coping motives and gender. Addictive Behaviors. 2012;37:1181–1184. doi: 10.1016/j.addbeh.2012.05.014. doi:10.1016/j.addbeh.2012.05.014. [DOI] [PubMed] [Google Scholar]
- Bullis J. R., Boettcher H., Sauer Zavala S., Farchione T. J., Barlow D. H.2019What is an emotional disorder? A transdiagnostic mechanistic definition with implications for assessment, treatment, and prevention Clinical Psychology: Science and Practice 26, Article e12278doi:10.1037/h0101755 [Google Scholar]
- Carey K. B. Reliability and validity of the Time-Line Follow-Back interview among psychiatric outpatients: A preliminary report. Psychology of Addictive Behaviors. 1997;11:26–33. doi:10.1037/0893-164X.11.1.26. [Google Scholar]
- Chavarria J., Allan N. P., Boffa J. W., Albanese B. J., Schmidt N. B., Zvolensky M. J. Decomposing the relationship between anxiety sensitivity and alcohol use. Journal of Studies on Alcohol and Drugs. 2015;76:957–961. doi: 10.15288/jsad.2015.76.957. doi:10.15288/jsad.2015.76.957. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cho J., Bello M. S., Christie N. C., Monterosso J. R., Leventhal A. M. Adolescent emotional disorder symptoms and transdiagnostic vulnerabilities as predictors of young adult substance use during the COVID-19 pandemic: Mediation by substance-related coping behaviors. Cognitive Behaviour Therapy. 2021;50:276–294. doi: 10.1080/16506073.2021.1882552. doi:10.1080/16506073.2021.1882552. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cooper M. L., Kuntsche E., Levitt A., Barber L. L., Wolf S.2016Motivational models of substance use: A review of theory and research on motives for using alcohol, marijuana, and tobaccoIn Sher K. J. (Ed.), The Oxford handbook of substance use and substance use disorderspp. 375–421.New York, NY: Oxford University Press; doi:10.1093/oxfordhb/9780199381678.013.017 [Google Scholar]
- Copeland W. E., Angold A., Shanahan L., Dreyfuss J., Dlamini I., Costello E. J. Predicting persistent alcohol problems: A prospective analysis from the Great Smoky Mountain Study. Psychological Medicine. 2012;42:1925–1935. doi: 10.1017/S0033291711002790. doi:10.1017/S0033291711002790. [DOI] [PMC free article] [PubMed] [Google Scholar]
- DeMartini K. S., Carey K. B. The role of anxiety sensitivity and drinking motives in predicting alcohol use: A critical review. Clinical Psychology Review. 2011;31:169–177. doi: 10.1016/j.cpr.2010.10.001. doi:10.1016/j.cpr.2010.10.001. [DOI] [PubMed] [Google Scholar]
- Dennhardt A. A., Murphy J. G. Associations between depression, distress tolerance, delay discounting, and alcohol-related problems in European American and African American college students. Psychology of Addictive Behaviors. 2011;25:595–604. doi: 10.1037/a0025807. doi:10.1037/a0025807. [DOI] [PubMed] [Google Scholar]
- Dennis M. L., Funk R., Godley S. H., Godley M. D., Waldron H. Cross-validation of the alcohol and cannabis use measures in the Global Appraisal of Individual Needs (GAIN) and Timeline Followback (TLFB; Form 90) among adolescents in substance abuse treatment. Addiction. 2004;99:120–128. doi: 10.1111/j.1360-0443.2004.00859.x. doi:/10.1111/j.13600443.2004.00859.x. [DOI] [PubMed] [Google Scholar]
- Dierker L., Selya A., Lanza S., Li R., Rose J. Depression and marijuana use disorder symptoms among current marijuana users. Addictive Behaviors. 2018;76:161–168. doi: 10.1016/j.addbeh.2017.08.013. doi:10.1016/j.addbeh.2017.08.013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Farris S. G., Metrik J., Bonn-Miller M. O., Kahler C. W., Zvolensky M. J. Anxiety sensitivity and distress intolerance as predictors of cannabis dependence symptoms, problems, and craving: The mediating role of coping motives. Journal of Studies on Alcohol and Drugs. 2016;77:889–897. doi: 10.15288/jsad.2016.77.889. doi:10.15288/jsad.2016.77.889. [DOI] [PMC free article] [PubMed] [Google Scholar]
- First M. B., Williams J. B. W., Karg R. S., Spitzer R. L. research version; SCID-5 RV) Arlington, VA: American Psychiatric Association; 2015. Structured clinical interview for DSM-5 – research version (SCID-5 for DSM-5. [Google Scholar]
- Folstein M. F., Folstein S. E., McHugh P. R. “Mini-mental state”: A practical method for grading the cognitive state of patients for the clinician. Journal of Psychiatric Research. 1975;12:189–198. doi: 10.1016/0022-3956(75)90026-6. doi:10.1016/0022-3956(75)90026-6. [DOI] [PubMed] [Google Scholar]
- Gilmore A. K., Jones J. L., Moreland A. D., Hahn C. K., Brady K. T., Back S. E. Gender moderates the association between distress tolerance and alcohol use among individuals with opioid use disorder. Drug and Alcohol Dependence. 2018;190:9–12. doi: 10.1016/j.drugalcdep.2018.05.016. doi:10.1016/j.drugalcdep.2018.05.016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gorka S. M., Ali B., Daughters S. B. The role of distress tolerance in the relationship between depressive symptoms and problematic alcohol use. Psychology of Addictive Behaviors. 2012;26:621–626. doi: 10.1037/a0026386. doi:10.1037/a0026386. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Guillot C. R., Blumenthal H., Zvolensky M. J., Schmidt N. B. Anxiety sensitivity components in relation to alcohol and cannabis use, motives, and problems in treatment seeking cigarette smokers. Addictive Behaviors. 2018;82:166–173. doi: 10.1016/j.addbeh.2018.03.008. doi:10.1016/j.addbeh.2018.03.008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gunn R. L., Stevens A. K., Micalizzi L., Jackson K. M., Borsari B., Metrik J. Longitudinal associations between negative urgency, symptoms of depression, cannabis and alcohol use in veterans. Experimental and Clinical Psychopharmacology. 2020;28:426–437. doi: 10.1037/pha0000357. doi:10.1037/pha0000357. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hasan N. S., Babson K. A., Banducci A. N., Bonn-Miller M. O. The prospective effects of perceived and laboratory indices of distress tolerance on cannabis use following a self-guided quit attempt. Psychology of Addictive Behaviors. 2015;29:933–940. doi: 10.1037/adb0000132. doi:10.1037/adb0000132. [DOI] [PubMed] [Google Scholar]
- Hayes A. F. Beyond Baron and Kenny: Statistical mediation analysis in the new millennium. Communication Monographs. 2009;76:408–420. doi:10.1080/03637750903310360. [Google Scholar]
- Hayes A. F., Rockwood N. J. Regression-based statistical mediation and moderation analysis in clinical research: Observations, recommendations, and implementation. Behaviour Research and Therapy. 2017;98:39–57. doi: 10.1016/j.brat.2016.11.001. doi:10.1016/j.brat.2016.11.001. [DOI] [PubMed] [Google Scholar]
- Hodgins D. C., Stea J. N. Psychometric evaluation of a lifetime version of the marijuana problems scale. Addictive Behaviors Reports. 2018;8:21–24. doi: 10.1016/j.abrep.2018.05.001. doi:10.1016/j.abrep.2018.05.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Jacobson I. G., Ryan M. A. K., Hooper T. I., Smith T. C., Amoroso P. J., Boyko E. J., Bell N. C. Alcohol use and alcohol-related problems before and after military combat deployment. JAMA. 2008;300:663–675. doi: 10.1001/jama.300.6.663. doi:10.1001/jama.300.6.663. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Johnson K., Mullin J. L., Marshall E. C., Bonn-Miller M. O., Zvolensky M. Exploring the mediational role of coping motives for marijuana use in terms of the relation between anxiety sensitivity and marijuana dependence. American Journal on Addictions. 2010;19:277–282. doi: 10.1111/j.1521-0391.2010.00041.x. doi:10.1111/j.1521-0391.2010.00041.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kay Lambkin F. J., Baker A. L., Lewin T. J., Carr V. J.2009Computer based psychological treatment for comorbid depression and problematic alcohol and/or cannabis use: A randomized controlled trial of clinical efficacy Addiction 104378–388.doi:10.1111/j.1360-0443.2008.02444.x [DOI] [PubMed] [Google Scholar]
- Kelly M. E., Guillot C. R., Quinn E. N., Lucke H. R., Bello M. S., Pang R. D., Leventhal A. M. Anxiety sensitivity in relation to cigarette smoking and other substance use in African American smokers. Psychology of Addictive Behaviors. 2020;34:669–679. doi: 10.1037/adb0000573. doi:10.1037/adb0000573. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Keough M. E., Schmidt N. B. Refinement of a brief anxiety sensitivity reduction intervention. Journal of Consulting and Clinical Psychology. 2012;80:766–772. doi: 10.1037/a0027961. doi:10.1037/a0027961. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Khan A. J., Pedrelli P., Shapero B. G., Fisher L., Nyer M., Farabaugh A. I., MacPherson L. The association between distress tolerance and alcohol related problems: The pathway of drinking to cope. Substance Use & Misuse. 2018;53:2199–2209. doi: 10.1080/10826084.2018.1464027. doi:10.1080/10826084.201 8.1464027. [DOI] [PubMed] [Google Scholar]
- Koch E. I., Eye B. D., Ellison G., Gourley B.2016Targeting anxiety sensitivity to prevent the development of psychopathologyIn Israelashvili M., Romano J.L. (Eds.), The Cambridge handbook of international prevention sciencepp. 457–477.New York, NY: Cambridge University Press [Google Scholar]
- Kuo P.-H., Gardner C. O., Kendler K. S., Prescott C. A. The temporal relationship of the onsets of alcohol dependence and major depression: Using a genetically informative study design. Psychological Medicine. 2006;36:1153–1162. doi: 10.1017/S0033291706007860. doi:10.1017/S0033291706007860. [DOI] [PubMed] [Google Scholar]
- Lass A. N. S., Winer E. S. Distress tolerance and symptoms of depression: A review and integration of literatures. Clinical Psychology: Science and Practice. 2020;27 Article e12336. doi:10.1037/h0101778. [Google Scholar]
- Lechner W. V., Shadur J. M., Banducci A. N., Grant D. M., Morse M., Lejuez C. W. The mediating role of depression in the relationship between anxiety sensitivity and alcohol dependence. Addictive Behaviors. 2014;39:1243–1248. doi: 10.1016/j.addbeh.2014.04.002. doi:10.1016/j.addbeh.2014.04.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lehman C. L., Cheung R. C. Depression, anxiety, post-traumatic stress, and alcohol related problems among veterans with chronic hepatitis C. American Journal of Gastroenterology. 2002;97:2640–2646. doi: 10.1111/j.1572-0241.2002.06042.x. doi:10.1016/S0002-9270(02)04400-3. [DOI] [PubMed] [Google Scholar]
- Leventhal A. M., Zvolensky M. J. Anxiety, depression, and cigarette smoking: A transdiagnostic vulnerability framework to understanding emotion–smoking comorbidity. Psychological Bulletin. 2015;141:176–212. doi: 10.1037/bul0000003. doi:10.1037/bul0000003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Leyro T. M., Zvolensky M. J., Bernstein A. Distress tolerance and psychopathological symptoms and disorders: A review of the empirical literature among adults. Psychological Bulletin. 2010;136:576–600. doi: 10.1037/a0019712. doi:10.1037/a0019712. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Liu Y., Sayam S., Shao X., Wang K., Zheng S., Li Y., Wang L. Prevalence of and trends in diabetes among veterans, United States, 2005–2014. Preventing Chronic Disease. 2017;14:170230. doi: 10.5888/pcd14.170230. doi:10.5888/pcd14.170230. [DOI] [PMC free article] [PubMed] [Google Scholar]
- MacKinnon D. P., Lockwood C. M., Williams J. Confidence limits for the indirect effect: Distribution of the product and resampling methods. Multivariate Behavioral Research. 2004;39:99–128. doi: 10.1207/s15327906mbr3901_4. doi:10.1207/s15327906mbr3901_4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McCarthy D. E., Curtin J. J., Piper M. E., Baker T. B.2010Negative reinforcement: Possible clinical implications of an integrative modelIn Kassel J. D. (Ed.), Substance abuse and emotionpp. 15–42.American Psychological Association; doi:10.1037/12067-001 [Google Scholar]
- McCarthy D. M., Tomlinson K. L., Anderson K. G., Marlatt G. A., Brown S. A. Relapse in alcohol- and drug-disordered adolescents with comorbid psychopathology: Changes in psychiatric symptoms. Psychology of Addictive Behaviors. 2005;19:28–34. doi: 10.1037/0893-164X.19.1.28. doi:10.1037/0893-164X.19.1.28. [DOI] [PubMed] [Google Scholar]
- McCarty C. A., Kosterman R., Mason W. A., McCauley E., Hawkins J. D., Herrenkohl T. I., Lengua L. J. Longitudinal associations among depression, obesity and alcohol use disorders in young adulthood. General Hospital Psychiatry. 2009;31:442–450. doi: 10.1016/j.genhosppsych.2009.05.013. doi:10.1016/j.genhosppsych.2009.05.013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Metrik J., Bassett S. S., Aston E. R., Jackson K. M., Borsari B. Medicinal versus recreational cannabis use among returning veterans. Translational Issues in Psychological Science. 2018;4:6–20. doi: 10.1037/tps0000133. doi:10.1037%2Ftps0000133. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Metrik J., Jackson K., Bassett S. S., Zvolensky M. J., Seal K., Borsari B. The mediating roles of coping, sleep, and anxiety motives in cannabis use and problems among returning veterans with PTSD and MDD. Psychology of Addictive Behaviors. 2016;30:743–754. doi: 10.1037/adb0000210. doi:10.1037/adb0000210. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Metrik J., Stevens A. K., Gunn R. L., Borsari B., Jackson K. M. Cannabis use and posttraumatic stress disorder: Prospective evidence from a longitudinal study of veterans. Psychological Medicine. 2022;52:446–456. doi: 10.1017/S003329172000197X. doi:10.1017/S003329172000197X. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Miller W. R. (No. 95) Bethesda, MD: National Institute on Alcohol Abuse and Alcoholism; 1995. The Drinker Inventory of Consequences (DrInC): An instrument for assessing adverse consequences of alcohol abuse: Test manual. [Google Scholar]
- Mitchell M. A., Capron D. W., Raines A. M., Schmidt N. B. Reduction of cognitive concerns of anxiety sensitivity is uniquely associated with reduction of PTSD and depressive symptoms: A comparison of civilians and veterans. Journal of Psychiatric Research. 2014;48:25–31. doi: 10.1016/j.jpsychires.2013.10.013. doi:10.1016/j.jpsychires.2013.10.013. [DOI] [PubMed] [Google Scholar]
- Muthén L. K., Muthén B. O. (7th ed.). Los Angeles, CA: Author; 1998–2012. Mplus user's guide. [Google Scholar]
- Najt P., Fusar-Poli P., Brambilla P. Co-occurring mental and substance abuse disorders: A review on the potential predictors and clinical outcomes. Psychiatry Research. 2011;186:159–164. doi: 10.1016/j.psychres.2010.07.042. doi:10.1016/j.psychres.2010.07.042. [DOI] [PubMed] [Google Scholar]
- Norr A. M., Allan N. P., Macatee R. J., Keough M. E., Schmidt N. B. The effects of an anxiety sensitivity intervention on anxiety, depression, and worry: Mediation through affect tolerances. Behaviour Research and Therapy. 2014;59:12–19. doi: 10.1016/j.brat.2014.05.011. doi:10.1016/j.brat.2014.05.011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Novak A., Burgess E. S., Clark M., Zvolensky M. J., Brown R. A. Anxiety sensitivity, self-reported motives for alcohol and nicotine use, and level of consumption. Journal of Anxiety Disorders. 2003;17:165–180. doi: 10.1016/s0887-6185(02)00175-5. doi:10.1016/S0887-6185(02)00175-5. [DOI] [PubMed] [Google Scholar]
- Reese E. D., Conway C. C., Anand D., Bauer D. J., Daughters S. B. Distress tolerance trajectories following substance use treatment. Journal of Consulting and Clinical Psychology. 2019;87:645–656. doi: 10.1037/ccp0000403. doi:10.1037/ccp0000403. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Reiss S., Peterson R. A., Gursky D. M., McNally R. J. Anxiety sensitivity, anxiety frequency and the prediction of fearfulness. Behaviour Research and Therapy. 1986;24:1–8. doi: 10.1016/0005-7967(86)90143-9. doi:10.1016/0005-7967(86)90143-9. [DOI] [PubMed] [Google Scholar]
- Rucker D. D., Preacher K. J., Tormala Z. L., Petty R. E. Mediation analysis in social psychology: Current practices and new recommendations. Social and Personality Psychology Compass. 2011;5:359–371. doi:10.1111/j.1751-9004.2011.00355.x. [Google Scholar]
- Schmidt N. B., Buckner J. D., Keough M. E. Anxiety sensitivity as a prospective predictor of alcohol use disorders. Behavior Modification. 2007;31:202–219. doi: 10.1177/0145445506297019. doi:10.1177/0145445506297019. [DOI] [PubMed] [Google Scholar]
- Shaw A.M., Halliday E.R., Tonarely N.A., Ehrenreich-May J. Relationship of affect intolerance with anxiety, depressive, and obsessive-compulsive symptoms in youth. Journal of Affective Disorders. 2021;280:34–44. doi: 10.1016/j.jad.2020.10.048. doi:10.1016/j.jad.2020.10.048. [DOI] [PubMed] [Google Scholar]
- Short N. A., Lechner M., Bell K., Black J., Buchanan J., Ho J., McLean S. A. Anxiety sensitivity prospectively predicts increased acute posttraumatic stress and related symptoms after sexual assault. Journal of Traumatic Stress. 2020;33:1111–1120. doi: 10.1002/jts.22613. doi:10.1002/jts.22613. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Simons J. S., Gaher R. M. The Distress Tolerance Scale: Development and validation of a self-report measure. Motivation and Emotion. 2005;29:83–102. doi:10.1007/s11031-005-7955-3. [Google Scholar]
- Sobell L. C., Sobell M. B.1992Timeline follow-back: A technique for assessing self-reported alcohol consumptionIn Litten R. Z., Allen J. P. (Eds.), Measuring alcohol consumption: Psychosocial and biological methodspp. 41–72.Humana Press; Retrieved from https://psycnet.apa.org/doi/10.1007/978-1-4612-0357-5_3 [Google Scholar]
- Stasik-O’Brien S. M., Brock R. L., Chmielewski M., Naragon-Gainey K., Koffel E., McDade Montez E., Watson D. Clinical utility of the Inventory of Depression and Anxiety Symptoms (IDAS) Assessment. 2019;26:944–960. doi: 10.1177/1073191118790036. doi:10.1177/1073191118790036. [DOI] [PubMed] [Google Scholar]
- Stephens R. S., Roffman R. A., Curtin L. Comparison of extended versus brief treatments for marijuana use. Journal of Consulting and Clinical Psychology. 2000;68:898–908. Doi:10.1037/0022-006X.68.5.898. [PubMed] [Google Scholar]
- Stewart K. L., Farris S. G., Jackson K. M., Borsari B., Metrik J. Cannabis use and anxiety sensitivity in relation to physical health and functioning in post-9/11 veterans. Cognitive Therapy and Research. 2019;43:45–54. doi: 10.1007/s10608-018-9950-5. doi:10.1007/s10608-0189950-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Taylor S., Zvolensky M. J., Cox B. J., Deacon B., Heimberg R. G., Ledley D. R., Cardenas S. J. Robust dimensions of anxiety sensitivity: Development and initial validation of the Anxiety Sensitivity Index-3. Psychological Assessment. 2007;19:176–188. doi: 10.1037/1040-3590.19.2.176. doi:10.1037/1040-3590.19.2.176. [DOI] [PubMed] [Google Scholar]
- Teeters J. B., Woodward M. J., Meshesha L. Z., Tripp J. C. Cannabis use in civilian college students and college student service members/veterans: The moderating effect of anxiety. American Journal of Drug and Alcohol Abuse. 2020;46:777–783. doi: 10.1080/00952990.2020.1753758. doi:10.1080/00952990.202 0.1753758. [DOI] [PubMed] [Google Scholar]
- Vujanovic A. A., McGrew S. J., Walton J. L., Raines A. M. Posttraumatic stress and substance use among military veterans: Associations with distress intolerance and anxiety sensitivity. Addictive Behaviors. 2022;126:107177. doi: 10.1016/j.addbeh.2021.107177. doi:10.1016/j.addbeh.2021.107177. [DOI] [PubMed] [Google Scholar]
- Wagner B., Riggs P., Mikulich-Gilbertson S. The importance of distribution-choice in modeling substance use data: A comparison of negative binomial, beta binomial, and zero-inflated distributions. American Journal of Drug and Alcohol Abuse. 2015;41:489–497. doi: 10.3109/00952990.2015.1056447. doi:10.3109/00952990.2015.1056447. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wahesh E., Moreton A., McKechnie M. The indirect effect of distress tolerance on young adult alcohol use behaviors via coping motives. Journal of Addictions & Offender Counseling. 2020;41:111–127. doi:10.1002/jaoc.12084. [Google Scholar]
- Watson D., O’Hara M. W., Chmielewski M., McDade-Montez E. A., Koffel E., Stuart S. Further validation of the IDAS: Evidence of convergent, discriminant, criterion, and incremental validity. Psychological Assessment. 2008;20:248–259. doi: 10.1037/a0012570. doi:10.1037/a0012570. [DOI] [PubMed] [Google Scholar]
- Williams A. D., Thompson J., Andrews G. The impact of psychological distress tolerance in the treatment of depression. Behaviour Research and Therapy. 2013;51:469–475. doi: 10.1016/j.brat.2013.05.005. doi:10.1016/j.brat.2013.05.005. [DOI] [PubMed] [Google Scholar]
- Wittchen H. U., Fröhlich C., Behrendt S., Günther A., Rehm J., Zimmermann P., Perkonigg A.2007Cannabis use and cannabis use disorders and their relationship to mental disorders: A 10-year prospective-longitudinal community study in adolescents Drug and Alcohol Dependence 88, Supplement 1S60–S70doi:10.1016/j.drugalcdep.2006.12.013 [DOI] [PubMed] [Google Scholar]
- Wolitzky-Taylor K., Drazdowski T. K., Niles A., Roy-Byrne P., Ries R., Rawson R., Craske M. G. Change in anxiety sensitivity and substance use coping motives as putative mediators of treatment efficacy among substance users. Behaviour Research and Therapy. 2018;107:34–41. doi: 10.1016/j.brat.2018.05.010. doi:10.1016/j.brat.2018.05.010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wolitzky-Taylor K., Glasner S., Tanner A., Ghahremani D. G., London E. D. Targeting maladaptive reactivity to negative affect in emerging adults with cannabis use disorder: A preliminary test and proof of concept. Behaviour Research and Therapy. 2022;150:104032. doi: 10.1016/j.brat.2022.104032. doi:10.1016/j.brat.2022.104032. [DOI] [PubMed] [Google Scholar]
- Yoon G., Petrakis I. L., Rosenheck R. A. Correlates of major depressive disorder with and without comorbid alcohol use disorder nationally in the Veterans Health Administration. American Journal on Addictions. 2015;24:419–426. doi: 10.1111/ajad.12219. doi:10.1111/ajad.12219. [DOI] [PubMed] [Google Scholar]
- Zavos H. M. S., Rijsdijk F. V., Eley T. C. A longitudinal, genetically informative, study of associations between anxiety sensitivity, anxiety and depression. Behavior Genetics. 2012;42:592–602. doi: 10.1007/s10519-012-9535-0. doi:10.1007/s10519-012-9535-0. [DOI] [PubMed] [Google Scholar]
- Zvolensky M. J., Mayorga N. A., Garey L. Worry, anxiety sensitivity, and electronic cigarettes among adults. Psychiatry Research. 2018;269:321–327. doi: 10.1016/j.psychres.2018.08.087. doi:10.1016/j.psychres.2018.08.087. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zvolensky M. J., Vujanovic A. A., Bernstein A., Bonn-Miller M. O., Marshall E. C., Leyro T. M. Marijuana use motives: A confirmatory test and evaluation among young adult marijuana users. Addictive Behaviors. 2007;32:3122–3130. doi: 10.1016/j.addbeh.2007.06.010. doi:10.1016/j.addbeh.2007.06.010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zvolensky M. J., Vujanovic A. A., Bernstein A., Leyro T. Distress tolerance: Theory, measurement, and relations to psychopathology. Current Directions in Psychological Science. 2010;19:406–410. doi: 10.1177/0963721410388642. doi:10.1177/0963721410388642. [DOI] [PMC free article] [PubMed] [Google Scholar]