Abstract
Objectives
Relatively little is known about the lived experiences of older adults during the COVID-19 pandemic. We systematically review the international literature to understand the lived experiences of older adult’s experiences during the pandemic.
Design and methodology
This study uses a meta-ethnographical approach to investigate the included studies. The analyses were undertaken with constructivist grounded theory.
Results
Thirty-two studies met the inclusion criteria and only five papers were of low quality. Most, but not all studies, were from the global north. We identified three themes: desired and challenged wellbeing; coping and adaptation; and discrimination and intersectionality.
Overall, the studies’ findings were varied and reflected different times during the pandemic. Studies reported the impact of mass media messaging and its mostly negative impact on older adults. Many studies highlighted the impact of the COVID-19 pandemic on participants' social connectivity and well-being including missing the proximity of loved ones and in consequence experienced an increase in anxiety, feeling of depression, or loneliness. However, many studies reported how participants adapted to the change of lifestyle including new ways of communication, and social distancing. Some studies focused on discrimination and the experiences of sexual and gender minority and ethnic minority participants. Studies found that the pandemic impacted the participants’ well-being including suicidal risk behaviour, friendship loss, and increased mental health issues.
Conclusion
The COVID-19 pandemic disrupted and impacted older adults’ well-being worldwide. Despite the cultural and socio-economic differences many commonalities were found. Studies described the impact of mass media reporting, social connectivity, impact of confinement on well-being, coping, and on discrimination. The authors suggest that these findings need to be acknowledged for future pandemic strategies. Additionally, policy-making processes need to include older adults to address their needs. PROSPERO record [CRD42022331714], (Derrer-Merk et al., Older adults’ lived experiences during the COVID-19 pandemic: a systematic review, 2022).
Keywords: Covid-19, Older adults, Risk communication, Social connectivity, Discrimination, Well-being, Coping
Introduction
In March 2020 the World Health Organisation declared a pandemic caused by the virus SARS-CoV2 (COVID-19) [1]. At this time 118,000 cases in 114 countries were identified and 4,291 people had already lost their lives [2]. By July 2022, there were over 5.7 million active cases and over 6.4 million deaths [2]. Despite the effort to combat and eliminate the virus globally, new variants of the virus are still a concern. At the start of the pandemic, little was known about who would be most at risk, but emerging data suggested that both people with underlying health conditions and older people had a higher risk of becoming seriously ill [3]. Thus, countries worldwide imposed health and safety measures aimed at reducing viral transmission and protecting people at higher risk of contracting the virus [4]. These measures included: national lockdowns with different lengths and frequencies; targeted shopping times for older people; hygiene procedures (wearing masks, washing hands regularly, disinfecting hands); restricting or prohibiting social gatherings; working from home, school closure, and home-schooling.
Research suggests that lockdowns and protective measures impacted on people’s lives, and had a particular impact on older people. They were at higher risk from COVID-19, with greater disease severity and higher mortality compared to younger people [5]. Older adults were identified as at higher risk as they are more likely to have pre-existing conditions including heart disease, diabetes, and severe respiratory conditions [5]. Additionally, recent research highlights that COVID-19 and its safety measures led to increased mental health problems, including increased feelings of depression, anxiety, social isolation, and loneliness, potentially cognitive decline [6–22]. Other studies reported the consequences of only age-based protective health measures including self-isolation for people older people (e.g. feeling old, losing out the time with family) [23–30].
Over the past decade, the World Health Organisation (WHO) has recognised the importance of risk communication within public health emergency preparedness and response, especially in the context of epidemics and pandemics. Risk communication is defined as “the real-time exchange of information, advice and opinions between experts or officials, and people who face a threat (hazard) to their survival, health or economic or social well-being” ([31], p5). This includes reporting the risk and health protection measurements through media and governmental bodies. Constructing awareness and building trust in society are essential components of risk communication [32]. In the context of the pandemic, the WHO noted that individual risk perception helped to prompt problem-solving activities (such as wearing face masks, social distancing, and self-isolation). However, the prolonged perception of pandemic-related uncertainty and risk could also lead to heightened feelings of distress and anxiety [31, 33], see also [34–37].
This new and unprecedented disease provided the ground for researchers worldwide to investigate the COVID-19 pandemic. To date (August 2022), approximately 8072 studies have been recorded on the U.S. National Library of Medicine ClinicalTrials.gov [38] and 12002 systematic reviews have been registered at PROSPERO, concerning COVID-19. However, to our knowledge, there is little known about qualitative research as a response to the COVID-19 pandemic and how it impacted older adults’ well-being [39]. In particular, little is known about how older people experienced the pandemic. Thus, our research question considers: How did older adults experience the COVID-19 pandemic worldwide?
We use a qualitative evidence synthesis (QES) recommended by Cochrane Qualitative and Implementation Methods Group to identify peer-reviewed articles [40]. This provides an overview of existing research, identifies potential research gaps, and develops new cumulative knowledge concerning the COVID-19 pandemic and older adults’ experiences. QES is a valuable method for its potential to contribute to research and policy [41]. Flemming and Noyes [40] argue that the evidence synthesis from qualitative research provides a richer interpretation compared to single primary research. They identified an increasing demand for qualitative evidence synthesis from a wide range of “health and social professionals, policymakers, guideline developers and educationalists” (p.1).
Methodology
A systematic literature review requires a specific approach compared to other reviews. Although there is no consensus on how it is conducted, recent systematic literature reviews have agreed the following reporting criteria are addressed [42, 43]: (a) a research question; (b) reporting database, and search strategy; (c) inclusion and exclusion criteria; (d) reporting selection methods; (e) critically appraisal tools; (f) data analysis and synthesis. We applied these criteria in our study and began by registering the research protocol with Prospero [44].
Protocol
The study is registered at Prospero [44]. This systematic literature review incorporates qualitative studies concerning older adults’ experiences during the COVID-19 pandemic.
Search strategy
The primary qualitative articles were identified via a systematic search as per the qualitative-specific SPIDER approach [45]. The SPIDER tool is designed to structure qualitative research questions, focusing less on interventions and more on study design, and ‘samples’ rather than populations, encompassing:
S-Sample. This includes all articles concerning older adults aged 60 + [1].
P-Phenomena of Interest. How did older adults experience the COVID-19 pandemic?
D-Design. We aim to investigate qualitative studies concerning the experiences of older adults during the COVID-19 pandemic.
E-Evaluation. The evaluation of studies will be evaluated with the amended Critical Appraisal Skills Programme CASP [46].
R-Research type Qualitative
Information source
The following databases were searched: PsychInfo, Medline, CINAHL, Web of Science, Annual Review, Annual Review of Gerontology, and Geriatrics. A hand search was conducted on Google Scholar and additional searches examined the reference lists of the included papers. The keyword search included the following terms: (older adults or elderly) AND (COVID-19 or SARS or pandemic) AND (experiences); (older adults) AND (experience) AND (covid-19) OR (coronavirus); (older adults) AND (experience) AND (covid-19 OR coronavirus) AND (Qualitative). Additional hand search terms included e.g. senior, senior citizen, or old age.
Inclusion and exclusion criteria
Articles were included when they met the following criteria: primary research using qualitative methods related to the lived experience of older adults aged 60 + (i.e. the experiences of individuals during the COVID-19 pandemic); peer-reviewed journal articles published in English; related to the COVID-19 pandemic; empirical research; published from 2020 till August 2022.
Articles were excluded when: papers discussed health professionals’ experiences; diagnostics; medical studies; interventions; day-care; home care; or carers; experiences with dementia; studies including hospitals; quantitative studies; mixed-method studies; single-case studies; people under the age of 60; grey literature; scoping reviews, and systematic reviews. We excluded clinical/care-related studies as we wanted to explore the everyday experiences of people aged 60 + . Mixed-method studies were excluded as we were interested in what was represented in solely qualitative studies. However, we acknowledge, that mixed-method studies are valuable for future systematic reviews.
Meta-ethnography
The qualitative synthesis was undertaken by using meta-ethnography. The authors have chosen meta-ethnography over other methodologies as it is an inductive and interpretive synthesis analysis and is uniquely “suited to developing new conceptual models and theories” ([47], p 2), see also [48]. Therefore, it combines well with constructivist grounded theory methodology. Meta-ethnography also examines and identifies areas of disagreements between studies [48].
This is of particular interest as the lived experiences of older adults during the COVID-19 pandemic were likely to be diverse. The method enables the researcher to synthesise the findings (e.g. themes, concepts) from primary studies, acknowledging primary data (quotes) by “using a unique translation synthesis method to transcend the findings of individual study accounts and create higher order” constructs ([47], p. 2). The following seven steps were applied:
Getting started (identify area of interest). We were interested in the lived experiences of older adults worldwide.
Deciding what was relevant to the initial interest (defining the focus, locating relevant studies, decision to include studies, quality appraisal). We decided on the inclusion and exclusion criteria and an appropriate quality appraisal.
Reading the studies. We used the screening process described below (title, abstract, full text)
Determining how the studies were related (extracting first-order constructs- participants’ quotes and second-order construct- primary author interpretation, clustering the themes from the studies into new categories (Table 3).
Translating the studies into one another (comparing and contrasting the studies, checking commonalities or differences of each article) to organise and develop higher-order constructs by using constant comparison (Table 3). Translating is the process of finding commonalities between studies [48].
Synthesising the translation (reciprocal and refutational synthesis, a lines of argument synthesis (interpretation of the relationship between the themes- leads to key themes and constructs of higher order; creating new meaning, Tables 2, 3),
Expressing the synthesis (writing up the findings) [47, 48].
Table 3.
From codes to categories and higher order constructs
| Higher order constructs |
Desired and challenged wellbeing [3, 9, 23, 62, 63, 65–70, 72, 75–85, 88–90] |
Coping and adaptation [63, 64, 68, 69, 72, 75, 79, 81, 85, 87–90] |
Discrimination – intersectionality (age and race/ gender identity [23, 62, 63, 67, 70, 76, 84, 88] |
|---|---|---|---|
| Categories |
Risk perception- communication Social connectivity Impact of confinement on well-being |
Emotional Behavioural |
Ageism Racism Heterosexism |
| Code examples |
Threat of the virus Financial threat Ageing and mortality Media, news perception Health Physical distancing Support- family- friends Personal networks Value Social isolation loneliness Unmet needs Physical activity Mood change |
Hygiene routines Use of technology New activities Change of daily routines- adhering to restrictions- slowing the pace Positive attitude Spirituality Hope -vaccine |
Marginalisation Risk factors Dual burden Homogeneous view Lost autonomy Loss of community Lack of services Immigration Racism Ageism Gender discrimination Equality |
Table 2.
Themes per author and country
| Author | Title | Country | Themes of each article | Subthemes | Categories | Higher order constructs |
|---|---|---|---|---|---|---|
| Akkus et al., 2021 [62] | Perceptions and experiences of older people regarding the COVID-19 pandemic process: A phenomenological study | Turkey | The Meaning of COVID-19 | Multifaceted Fear, Social Restriction, Biology/Fate Dilemma, | Meaning of Covid-19 | Meaning |
| COVID-19 Outcomes: Overall Decline in Health and Well-being | Physical, mental, social, and economic outcomes or effects | Health | Wellbeing | |||
| Need for Support and Resources: “We became self-sufficient.” | Economic, health care, informational, and emotional and spiritual support | Support | Wellbeing | |||
| Attitudes toward Vaccination: “Everyone says something different.” | Fear of the vaccine; The Vaccine Offers Hope | Uncertainty | Wellbeing | |||
| Banerjee & Rao, 2021 [63] | The Graying Minority": Lived Experiences and Psychosocial Challenges of Older Transgender Adults During the COVID-19 Pandemic in India | India | Marginalization | Second” priority, stigma, social disconnection, perceived loss of dignity | Marginalisation | Wellbeing |
| The dual burden of “age” and “gender” | Prominence of ageism | Dual burden | Discrimination- dual burden | |||
| Deprived psychosexual needs, cornered in their communities | ||||||
| Multi-faceted survival threats | Psychological, emotional, financial | Health | Wellbeing | |||
| Coping | Social rituals and pride celebrations | Coping | Coping | |||
| Acceptance of the discomfort of beloning to the third gender | ||||||
| Spiritulity, hope | Wellbeing | |||||
| Unmeet needs | Kowledge, attitude, practice (KAP) related to COVID-19 | Unmet needs | ||||
| Social inclusion | Social connectivity | Wellbeing | ||||
| Mental health care | Health | Wellbeing | ||||
| The audience for their voices | Value | Wellbeing | ||||
| Brooke, J., & Clark, M., 2020 [64] | Older people’s early experience of household isolation and social distancing during COVID-19 | UK/Irland | Handwashing; two-metre social distancing; disinfecting practices; and face masks | Adaptation | Adaptation | |
| Protective measures | Social media, weather and the garden, tasks to complete | Adaptation | Adaptation | |||
| Current and future plans; and | Blessed, lucky and fortunate; and life still to be lived | |||||
| Acceptance of a good life, but still a life to live | Coping | Coping | ||||
| Bundy et al., 2021 [65] | The Lived Experience of Already-Lonely Older Adults During COVID-19 | USA | Loneliness Did Not Necessarily Compound | Loneliness | Wellbeing | |
| Managing Loneliness and Enduring Social Isolation | Social isolation | Wellbeing | ||||
| Loneliness, Protective, and Responsible | loneliness | Wellbeing | ||||
| The Anxieties of COVID-19 | Anxiety | Wellbeing | ||||
| Chemen and Gopalla, 2021 [66] | Lived experiences of older adults living in the community during the COVID-19 lockdown—The case of mauritius | Mauritius | Fears of the virus and fear of deprivation | Health | Wellbeing | |
| Relieving and recreating bounds | Social connectivity | Wellbeing | ||||
| Active contribution to family life | Support | Wellbeing | ||||
| Being and feeling valued within the family | Value/family | Wellbeing | ||||
| Rediscovering family time and family moments | Value/family | Wellbeing | ||||
| Fear of going back to normal | Uncertainty | Adaptation | ||||
| Social isolation | Social Isolation | Wellbeing | ||||
| Derrer-Merk et al., 2022 [9] | Older people's family relationships in disequilibrium during the COVID-19 pandemic. What really matters? | UK | Pre-pandemic to March 2020 | Social connectedness | Social connectivity | Wellbeing |
| Methods of support | Support | Wellbeing | ||||
| Pandemic March to July 2020 | Social disconnectedness | Social connectivity | Wellbeing | |||
| Change of desired ad perceived support | support | Wellbeing | ||||
| Derrer-Merk et al., 2022 [23] | Is protecting older adults from COVID-19 ageism? A comparative cross-cultural constructive grounded theory from the United Kingdom and Colombia | UK/Colombia | Benevolent versus hostile ageism | Ageism | Discrimination | |
| Society's view on ageing as homogenous | Homogeneous view | Discrimination | ||||
| Lost autonomy | Lost autonomy | Wellbeing | ||||
| Differences between the UK and Colombia | ||||||
| Falvo et al., 2021 [67] | Lived experiences of older adults during the first COVID-19 lockdown: A qualitative study | Switzerland | Impact on the individual level: Between fear of going out and a feeling of reclusion | Fear of going out, reclusion | Uncertainty | Wellbeing |
| Impact on the micro-social level: The dual role of the other | Social connectivity | Wellbeing | ||||
| Impact on the meso-social level: Between protection and stigmatization | Protection/ stigmatization | Wellbeing | ||||
| Impact on the macro-social level: Gestation of a new world | New world | Adaptation | ||||
| Fiocco et al., 2021 [68] | Stress and Adjustment during the COVID-19 Pandemic: A Qualitative Study on the Lived Experience of Canadian Older Adults | Canada | Perceived threat and challenges associated with the pandemic | Threat of contracting the SARA-CoV2 Virus | Threat of contracting the virus | Wellbeing |
| Financial Threat | Financial threat | Coping | ||||
| Fear Messaging in the Media |
Risk communication Risk perception |
Wellbeing | ||||
| Living Arrangement Challenges | Adaptation | |||||
| The Challenge of Physical Distancing and Minimal Social Interactions | Social connectivity | Wellbeing | ||||
| The Challenge of Health Management and Health Services | Health management | Wellbeing | ||||
| Use of Technology: A New Necessity | Technology | Wellbeing | ||||
| Coping with the COVID-19 pandemic | Behavioural strategies | Coping | Coping | |||
| Emotioal-focused strategies | Coping | Coping | ||||
| Social support | Support | Wellbeing | ||||
| Fristedt et al., 2022 [69] | Changes in daily life and wellbeing in adults, 70 years and older, in the beginning of the COVID-19 pandemic | Sweden | Suddenly at risk- … but it could be worse | My world closed down | Threat of the virus | Wellbeing |
| Negogiations, adaptaions and prioritazations to manage staying at home | Coping/ adaptation | Adaptation | ||||
| Barriers and facilitators to sustain occupational participation | Participation | Wellbeing | ||||
| Considerations of my own and other’s health and wellbeing | Health/ wellbeing | Wellbeing | ||||
| Gazibara et al., 2022 [70] | Experiences and aftermath of the COVID-19 lockdown among community-dwelling older people in Serbia | Serbia | Perception of the curfew announcement; | Being calm | Wellbeing | Wellbeing |
| Feeling distressed | Mental health | Wellbeing | ||||
| Feeling angry | Distress | |||||
| Attitude towards the curfew; | Positive and compliant | Adaptation | ||||
| Negative and resistant | Coping | Coping | ||||
| Organization of daily living; | Shopping for groceries | Adaptation | Adaptation | |||
| Access to healthcare services | Health services | Adaptation | ||||
| Daytime activities | Adaptation | Adaptation | ||||
| Mood | Mood | Wellbeing | ||||
| Frustrations/Limitations | Lack of physical activity | Wellbeing | Wellbeing | |||
| Lack of social interactions | Social connectivity | Wellbeing | ||||
| Time allocated for walking outside and grocery shopping | Exercise | Wellbeing | ||||
| Making sense of the curfew 15 months after | Adaptation | Wellbeing | ||||
| Giebel et al., 2022 [71] | COVID-19 Public Health Restrictions and Older Adults' Well-being in Uganda: Psychological Impacts and Coping Mechanisms | Uganda | Impact on emotional well-being; | Frustration about situation and boredom | Wellbeing | Wellbeing |
| Upset about inability to see friends and family | Social connectivity | Wellbeing | ||||
| Fear | ||||||
| Implications on physical well-being; | Frailty | Wellbeing | Wellbeing | |||
| Lack of cognitive and social stimulation | Coping | Coping | ||||
| Coping mechanisms | Acceptance | Coping | Coping | |||
| Faith | Adaptation | Adaptation | ||||
| Goins et al., 2021 [72] | Older Adults in the United States and COVID-19: A Qualitative Study of Perceptions, Finances, Coping, and Emotions | USA | Risk Perception | Yes, due to underlying conditions | Risk perception | Wellbeing |
| Yes, because of age but with reluctance; yes without reluctance but only because of age; yes with elaboration; no, because they are healthy despite meeting age criteria; no without elaboration | Wellbeing | |||||
| Financial impact | Yes negatively; yes positvely; no impact; no, not currently | Impact | Wellbeing | |||
| Coping Problem-focused: | Reduce exposure | Coping | Coping | |||
| Reduce susceptibility | Adaptation | Adaptation | ||||
| Emotion-focused: | Creating daily structure | Coping | Coping | |||
| New/creative activities | ||||||
| Connecting with others in new ways | Social connectivity | Wellbeing | ||||
| Limiting news media exposure | Coping | Wellbeing | ||||
| Emotions | Not affected | Coping | ||||
| Anxiety, fear, and loneliness | Mental health | Wellbeing | ||||
| Disappointments | Frustration | Wellbeing | ||||
| Positive feelings | Optimism | Wellbeing | ||||
| Gomes et al., 2021 [73] | Elderly people's experience facing social isolation in the COVID-19 pandemic | Brazil | Longing for extra-houshold routine and family life | Adaptation | Adaptation | |
| Building new routine | Coping | Coping | ||||
| Fear of the death | Health | Wellbing | ||||
| Strategies for preventing COVID-19 | Adaptation | Adaptation | ||||
| Spirituality and pleasurable activities pre-pandemic | Coping | Coping | ||||
| Signs and symptoms experienced during SARS-COV2 infection | Health | Wellbeing | ||||
| Gonçalves et al., 2022 [74] | Perceptions, feelings, and the routine of older adults during the isolation period caused by the COVID-19 pandemic: a qualitative study in four countries | Brazil, USA,Italy, Portugal | Deprivation | Freedom/right to come and go | Deprivation | Wellbeing |
| Restriction from being with others | Social connectivity | Wellbeing | ||||
| Changes in leisure | Adaptation | Adaptation | ||||
| Restriction of actions of self-management and self-care | Health | Wellbeing | ||||
| Work | Purpose in live | Wellbeing | ||||
| Medical consultations | Health | Wellbeing | ||||
| Adaptation process | Domestic chores | Adaptation | Adaptation | |||
| Recreation/leisure activities | Activities | Wellbeing | ||||
| Technological resources | Coping | Coping | ||||
| Idleness | Health | Wellbeing | ||||
| Coping strategies | Belief, faith, and hope | Coping | Coping | |||
| Information/following recommendations | Health | Wellbeing | ||||
| Family | Social connectivity | Wellbeing | ||||
| Emotional instability | Negative feelings – Positive feelings | Wellbeing | Wellbeing | |||
| Understanding of COVID-19 | Definition | Adaptation | Adaptation | |||
| Transmission – Symptoms | Health | Wellbeing | ||||
| Protective measures | Health | Wellbeing | ||||
| Greenwood-Hickman et al., 2021 [75] | A Qualitative Investigation of Impacts and Coping Strategies During the COVID-19 Pandemic Among Older Adults | USA | General Impacts to Daily Life | Staying at Home | Practical daily impact | Impact |
| Travel | Coping | Wellbeing | ||||
| Work | Adaptation | Adaptation | ||||
| Finances | Coping | Coping | ||||
| Policy impacts to behaviour | Adaptation | Adaptation | ||||
| Health and Activity Impacts Mental Health, Energy, and Stress | Mental health, engergy, and stress | Health | Wellbeing | |||
| Nutrition | Health | Wellbeing | ||||
| Physical Activity | Health | Wellbeing | ||||
| Sedentary Time | Health | Wellbeing | ||||
| Sleep; sickness/infection with COVID-19 | Health | Wellbeing | ||||
| Social Impacts Changes to In-person Social Engagement | Family Events | Social impact | Wellbeing | |||
| Coping Strategies | Coping | |||||
| Social Connection | Virtual | Social connectivity | Wellbeing | |||
| In person | ||||||
| Activities | Hobbies | Adaptation | Adaptation | |||
| Exercise | Health | Wellbeing | ||||
| Following Public Health Guidance and Minimizing Risk | Health, | Wellbeing | ||||
| HART participation | Participation | Wellbeing | ||||
| Beliefs and Attitude | Positive attitude | Adaptation | Adaptation | |||
| Spirituality | Health | Adaptation | ||||
| Hafford-Letchfieldet al., 2022 [76] | Unheard voices: A qualitative study of LGBT + older people experiences during the first wave of the COVID-19 pandemic in the UK | UK | Risk factors for LGBT + older people and organisations, including specific findings on trans experiences; | Risk factors experienced by LGBT + older people | Risk factors for minorities,Risk perception/experience | Wellbeing |
| Specific risks for trans people | Risk factors | Wellbeing | ||||
| Risk factors for LGBT + organisations | ||||||
| Care practices in LGBT + lives; |
Secure relationship/ partnership; offering accommodation to partners; increased visibility of concealed relationships; active outreach to family/ friends; reconnecting/ relationships; fear of formal care/ increase in volunteers; Advocacy in transfer to formal car |
Support | Wellbeing | |||
| strengths and benefits of networking | Opportunities to connect with neighbours; Kinder communities; being aware of others needs/ increase take up of services online; role of anonymity | Support social connectivity | Wellbeing | |||
| Politicisation of ageing and their relevance to LGBT + communities | Loss of community advocacy and support; perceived ageism; invisibility; Lack of inclusive services, active outreach to family/friends; effect of rurality on networks/ reduction in campaigning; less visibility in local authorities; lack of information in health and social care; increased fragmentation of services; lack of inclusive services; exclusion from contingency planning; access to additional funding |
Impact Support Discrimination Social connectivity |
Wellbeing Discrimination |
|||
| Learning from communication and provision in a virtual world | Improved virtual services for trans; new peer networks/ increase in volunteers; and take up services online; costs and benefits of adapting services to virtual delivery; new peer networks | Adaptation | Adaptation | |||
| Huntley and Bratt, 2022 [77] | An interpretative phenomenological analysis of the lived experiences of older adults during the covid-19 pandemic in Sweden | Sweden | A life on hold | Adherence to restrictions | A life on hold | Wellbeing |
| Vaccines—a light at the end of the tunnel | Hope | |||||
| Caring for body and soul, and | Mood | Wellbeing | Wellbeing | |||
| Physical health | Health | Wellbeing | ||||
| Everyday meaningfulness | Meaningful live | Wellbeing | ||||
| Putting things into perspective | Longing and love | Meaningful live | Wellbeing | |||
| Privilege | Adaptation | Adaptation | ||||
| Nostalgia | Reflection | Adaptation | ||||
| Jiménez-Etxebarria et al., 2021 [78] | Impact of the COVID-19 Pandemic as perceived by Older People in Northern Spain | Spain | Confinement and Perceived Impact on Lifestyle, and Physical and Psychological Health | Activities carried out before the pandemic (volunteering, leisure, exercise, dependent care, learning | Impact health | Wellbeing |
| Impact of confinement on activities (interruption of activities, plans we cannot make, excitement due to cessation of activity, I do not know we will be able to return to the activities | Impact of confinement | Wellbeing | ||||
| Routine performed in confinement (Description of the routine, adaptive behaviour, | Adaptation | Adaptation | ||||
| Health | Impact of confinement on physical condition (I do not see any changes, neagive changes) | Health/wellbeing | Wellbeing | |||
| Impact of confinement in psychological state (same as always, notice changes, negative changes, positive emotions, ambigious or mixed emotions, uncertainty) | Emotional wellbeing | Wellbeing | ||||
| Social relationships during confinement | Search for contact maintenance (use of technology, | Social connectivity | Wellbeing | |||
| Contact assessment (satisfaction, this contact cannot be called a relationship, fear of physical contact) | Social connectivity | Wellbeing | ||||
| Changes in the form of relationship (contacts we cannot have, new forms of contact, remote family contact) | Social connectivity | Wellbeing | ||||
| Older people | Treatment of older people during the confinement (positive perception, negavite perception, nursing homes) | Perception | Wellbeing | |||
| State of confinement or pandemic | Attitudes (percieved negative aspects, notice positive aspects, manifest coping strategies) | Perception / adaptation | Wellbeing | |||
| Reflection on the future (how I value my personal situation, assess the social situation, | Reflection | Wellbeing | ||||
| Kremers et al., 2022 [79] | The psychosocial adaptability of independently living older adults to COVID-19 related social isolation in the Netherlands | Netherland | ‘Social behaviour during the COVID- 19 outbreak’, | Maintenance of contact | Social connectivity | Wellbeing |
| Adaptation | Adaptation | Adaptation | ||||
| Less contact | Social connectivity | Wellbeing | ||||
| ‘Emotional behaviour during the COVID- 19 outbreak’ | ||||||
| Motivation to expand the social network’ | Social connectivity | Wellbeing | ||||
| Kulmala et al., 2021 [80] | Personal Social Networks of Community-Dwelling Oldest Old During the Covid-19 Pandemic | Finland | The Size of the Personal Network Reduced Significantly | Avoiding all places with a lot of people; Fear (own or others) of the virus, Restricting contacts even with the closest family; Meetings outside impossible due to own of other person’s sickness or disability, A relative/friend is a caregiver for someone else and cannot leave home, Hobbies has been closed, Use of digital tools were perceived as difficult and were not applied, Relatives prohibited contacting other people | Social connectivity | Wellbeing |
| Personal Networks Remained the Same, but Modifications in Contacting Other People Were Done Based on Recommendations | Phone contacts increased; Relatives, friends and neighbors were met outside and with safety distances; Video, internet and WhatsApp contacts with the family started, Applying safer ways of greeting and meeting people, i.e., not shaking hands anymore, using face masks; Hobbies, i.e., physical activity groups, organized online | Social connectivity | Wellbeing | |||
| Personal Networks Increased During the Pandemic | Spending more time with partner; Contacting friends and relatives who had not been contacted for a long time; More frequent online contacts with children and grandchildren; Feeling socially more connected with the neighbors; Importance of pets increased | Social connectivity | Wellbeing | |||
| Significant or Unexpected Change in Personal Network Happened During the Pandemic | Death of a spouse;Death of a friend; Birth of great grandchildren | Social connectivity | Wellbeing | |||
| The Pandemic Did Not Influence Personal Networks at all | Phone contacts with relatives and friends were as common as previously; Friends and family visited regardless of restrictions or children live close or at the same house; Current personal social network was seen as fulfilling; Enjoying time alone and having no obligations to leave home | Social connectivity | Wellbeing | |||
| Mahapatra et al., 2021 [81] | Coping with COVID-19 pandemic: reflections of older couples living alone in urban Odisha, India | Indai | Theme 1: risk appraisal and feeling vulnerable | Risk perception | Wellbeing | |
| Theme 2: safeguarding against COVID-19 | Health | Wellbeing | ||||
| Theme 3: managing routine health care and emergency | Adaptation | Adaptation | ||||
| Theme 4: pursuing mental and psychological well-being | Wellbeing | Wellbeing | ||||
| McKinlay et al., 2021 [82] | A qualitative study about the mental health and wellbeing of older adults in the UK during the COVID-19 pandemic | UK | Potential Threats to Wellbeing | Concerns about end-of-life, ageing, and mortality; Thinking about end-of-life concerns, worries about ageing and frailty | Risk perception | Wellbeing |
| Grieving the loss of normality; Feeling life is on hold, craving normality, finding the state of the world upsetting | Wellbeing | Wellbeing | ||||
| Healthcare concerns;Fear of hospitalisation, fear of seeking help due to perceived lack of service availability, fear of leaving the house due to COVID | Health | Wellbeing | ||||
| Unable to engage with activities that protect wellbeing; Loss of leisure, lack of routine | Health | Wellbeing | ||||
| Protective Activities and Behaviours | Slowing the pace of life; More time for exercise and new hobbies, time for introspection, and organising affairs | Adaptation | Adaptation | |||
| Benefits of routine and social responsibility; Feeling “needed” and helping others, keeping busy with social obligations | Support / Adaptation | Adaptation | ||||
| Social interaction and support; Connecting with others, reciprocal offers of support | Support | Wellbeing | ||||
| Utilising skills, experience and resources to cope; Using past coping skills and experience, accustomed to isolation, accessing practical resources | Coping | Coping | ||||
| Pfabigan et al., 2022 [83] | Under reconstruction: the impact of COVID-19 policies on the lives and support networks of older people living alone. | Austria | Attitudes towards the pandemic situation and its threats | Attitudes | Adaptation | Adaptation |
| Dealing with restrictions and hygiene measures | Adaptation | Adaptation | ||||
| Managing everyday life and support | Adaptation/ support | Adaptation | ||||
| Shifts in support networks | ||||||
| Negotiating autonomy | Autonomy | Wellbeing | ||||
| Prigent et al., 2022 [84] | Intergenerational tension or cohesion during the covid-19 pandemic?: A letter-writing study with older new zealanders | New Zealand | Familial intergenerational interaction | Social connectivity | Wellbeing | |
| Neighborhood interactions | Social connectivity | Wellbeing | ||||
| Societal interactions | ||||||
| Sangrar et al., 2021 [85] | Exploring the Interpretation of COVID-19 Messaging on Older Adults' Experiences of Vulnerability | Canada | Theme 1: “Fact-Checking”: How Older Adults Interpret Early Information and Factors that Influence their Interpretation | a systematic approach to consuming COVID-19 messaging | Perception of news | Wellbeing |
| intrinsic factors of discourse consumption and interpretation | Risk perception | Wellbeing | ||||
| Extrinsic factors of discourse interpretation | ||||||
| Theme 2: “Just be Careful”: Manifestations of Vulnerability | Emotional responses to early messaging | Risk perception | Wellbeing | |||
| Personalizing pandemic messaging | Risk perception | Wellbeing | ||||
| Theme 3: “Changed the Lifestyle”: Impacts of COVID-19 Messaging on Everyday Living | Disrupted Routines | Impact of news risk perception | Wellbeing | |||
| Community engagement | Social connectivity | Wellbeing | ||||
| Theme 4: “NotBadin myLocale”: Contextual Considerations for Discourse Interpretation | Pandemic narrative | Impact of news | Wellbeing | |||
| Micro and macro contexts | Impact of news | Wellbeing | ||||
| Sattari and Billore, 2020 [86] | Bring it on Covid-19: being an older person in developing countries during a pandemic. Working with Older People | India/Iran | Perception of risk and fear | Risk perception | Wellbeing | |
| Change in lifestyle adaptation to the pandemic situation | Adaptation | Adaptation | ||||
| Verhage et al., 2021 [87] | Coping of Older Adults in Times of COVID-19: Considerations of Temporality Among Dutch Older Adults | Netherland | Situating the Crisis: Meaning in Life | Meaning | Wellbeing | |
| Coping Strategies During the Crisis | Self-enhancing comparisons (problem focused, emotional focused, meaning focused) | Coping | Coping | |||
| Gaining control by following measures | Adaptation | Adaptation | ||||
| Distraction | Adaptation | Adaptation | ||||
| Temporary acceptance | Adaptation | Adaptation | ||||
| Interpreting individual vulnerability | Risk perception | Risk perception | ||||
| Wang et al., 2021 [88] | Identities: experiences and impacts of the COVID-19 pandemic from the perspectives of older Chinese immigrants in Canada | Canada | Immigration | Minority experience | Discrimination | |
| Older age | Self perception | Wellbeing | ||||
| Racism towards people of Chinese descent? | Racism | Discrimination | ||||
| Family Roles as older parents and grandparents | Role | Identity | ||||
| Use of technology | Technology | Wellbeing | ||||
| Xie et al., 2021 [89] | Living Through the COVID-19 Pandemic: Community-Dwelling Older Adults’ Experiences | USA | Theme 1: positive experiences | Perception that the pandemic had not changed ones lifestyle | Impact on lifestyle | Wellbeing |
| Adjusting well—particularly with the aid of thechnology | Adaptation | Adaptation | ||||
| Being positive in perspective | ||||||
| The loner advantage | Loner advantage | Wellbeing | ||||
| Theme 2: mixed experiences | Doing well but unhappy about having to change lifestyle routines | Adaptation | Adaptation | |||
| Doing well but unhappy about not having in-person interactions | Social connectivity | Wellbeing | ||||
| Doing well but frustrated by others' behaviors | ||||||
| Maintaining physical health with fluctuations of isolation and symptoms of depression or anxiety |
Health Social connectivity |
Wellbeing | ||||
| Theme 3: negative experiences | Bitter about others( e.g. society, government) not caring for older adults | Impact Neglect | Wellbeing | |||
| Feeling isolated, bored, and powerless | Impact | Wellbeing | ||||
| Worsening as time goes by | ||||||
| Yang et al., 2021 [90] | The Experiences of Community-dwelling older adults during the COVID-19 Lockdown in Wuhan | China | Challenges posed by COVID- 19 | Tight medical resources | Limited resources Health | Wellbeing |
| Inconvenience in daily life | Inconvenience | Adaptation | ||||
| Negative emotions | Wellbeing | Wellbeing | ||||
| Support during the COVID- 19 epidemic | Social support | Support | Wellbeing | |||
| Technical support | ||||||
| Resilience amid challenges | coping in daily lives | Coping | Coping | |||
| Transcendence | ||||||
| Impact after the COVID- 19 epidemic | Mental burdens | Impact | Wellbeing | |||
| Sense of benefit from the lockdown | Benefit | Wellbeing | ||||
| Yıldırım, H., 2022 [91] | Psychosocial status of older adults aged 65 years and over during lockdown in Turkey and their perspectives on the outbreak | Turkey | Growing old is like a crime | Finding comfort | Wellbeing | Wellbeing |
| The inevitable course | Adaptation | Wellbeing | ||||
| The cost of lockdown at home | Coping well | Coping | Coping | |||
| The desire for equality | Equality | Equality | Discrimination | |||
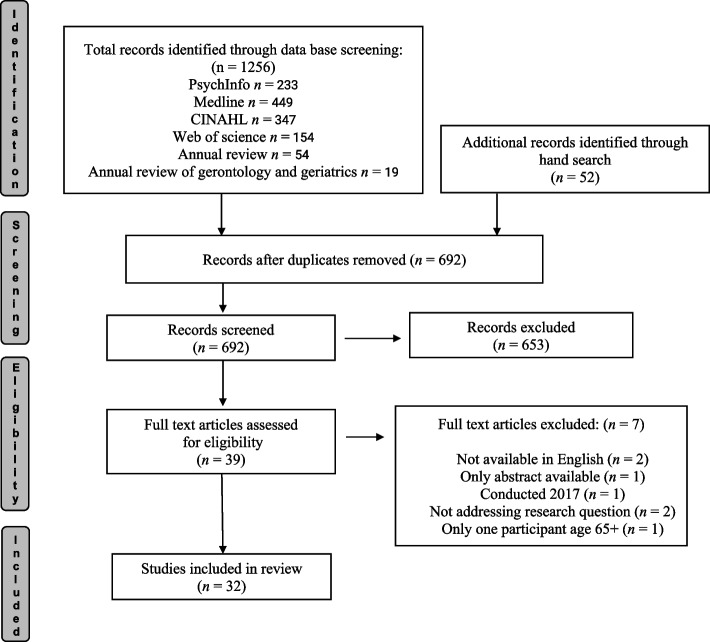
Screening and Study Selection
A 4-stage screening protocol was followed (Fig. 1 Prisma). First, all selected studies were screened for duplicates, which were deleted. Second, all remaining studies were screened for eligibility, and non-relevant studies were excluded at the preliminary stage. These screening steps were as follows: 1. title screening; 2. abstract screening, by the first and senior authors independently; and 3. full-text screening which was undertaken for almost all papers by the first author. However, 2 papers [9, 23] were assessed independently by LS, LR, and LMM to avoid a conflict of interest. The other co-authors also screened independently a portion of the papers each, to ensure that each paper had two independent screens to determine inclusion in the review [49]. This avoided bias and confirmed the eligibility of the included papers (Fig. 1). Endnote reference management was used to store the articles and aid the screening process.
Fig. 1.
Prisma flow diagram adapted from Page et al. [50]. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ, 372, n71. https://doi.org/10.1136/bmj.n71)
Data extraction
After title and abstract screening, 39 papers were selected for reading the full article. 7 papers were excluded after the full-text assessment (1 study was conducted in 2017, but published in 2021; 2 papers were not fully available in English, 2 papers did not address the research question, 1 article was based on a conference abstract only, 1 article had only one participant age 65 +).
The full-text screening included 32 studies. All the included studies, alongside the CASP template, data extraction table, the draft of this article, and translation for synthesising the findings [47, 48] were available and accessible on google drive for all co-authors. All authors discussed the findings in regular meetings.
Quality appraisal
A critical appraisal tool assesses a study for its trustworthiness, methodological rigor, and biases and ensures “transparency in the assessment of primary research” ([51], p. 5); see also [48–53]. There is currently no gold standard for assessing primary qualitative studies, but different authors agreed that the amended CASPS checklist was appropriate to assess qualitative studies [46, 54]. Thus, we use the amended CASP appraisal tool [42]. The amended CASP appraisal tool aims to improve qualitative evidence synthesis by assessing ontology and epistemology (Table 1 CASP appraisal tool).
Table 1.
Amended CASP critical appraisal tool [46]
| 1. Was there a clear statement of the aims? | 2. Is a qualitative method appropriate? | 3. Was the research design appropriate to address the aims? | 4. Was the recruitment strategy appropriate to the aims of the study? | 5. Was the data collected in a way that addressed the research issue | 6. Has the relationship between researcher and participants been adequately considered? | 7. Have ethical issues been taken into account? | 8. Was the data analysis sufficiently rigorous? | 9. Is there a clear statement of findings? | 10. How valuable is the research (High, middle, low) |
11. Ontology/epistemology/ Are the study’s theoretical underpinnings clear, consistent and conceptually correct? |
A numerical score was assigned to each question to indicate whether the criteria had been met (= 2), partially met (= 1), or not met (= 0) [54]; see also [55]. The score 16 – 22 are considered to be moderate and high-quality studies. The studies scored 15 and below were identified as low-quality papers. Although we focus on higher-quality papers, we did not exclude papers to avoid the exclusion of insightful and meaningful data [42, 48, 52–57]. The quality of the paper was considered in developing the evidence synthesis.
We followed the appraisal questions applied for each included study and answered the criteria either ‘Yes’, ‘Cannot tell’, or ‘No’. (Table 1 CASP appraisal criteria). The tenth question asking the value of the article was answered with ‘high’ of importance, ‘middle’, or low of importance. The new eleventh question in the CASP tool concerning ontology and epistemology was answered with yes, no, or partly (Table 1).
Data synthesis
The data synthesis followed the seven steps of Meta-Ethnography developed by Noblit & Hare [58], starting the data synthesis at step 3, described in detail by [47]. This encompasses: reading the studies; determining how the studies are related; translating the studies into one another; synthesis the translations; and expressing synthesis. This review provides a synthesis of the findings from studies related to the experiences of older adults during the COVID-19 pandemic. The qualitative analyses are based on constructivist grounded theory [59] to identify the experiences of older adults during the COVID-19 pandemic (non-clinical) populations. The analysis is inductive and iterative, uses constant comparison, and aims to develop a theory. The qualitative synthesis encompasses all text labelled as ‘results’ or ‘findings’ and uses this as raw data. The raw data includes participant’s quotes; thus, the synthesis is grounded in the participant's experience [47, 48, 60, 61]. The initial coding was undertaken for each eligible article line by line. Please see Table 2 Themes per author and country. Focused coding was applied using constant comparison, which is a widely used approach in grounded theory [61]. In particular, common and recurring as well as contradicting concepts within the studies were identified, clustered into categories, and overarching higher order constructs were developed [47, 48, 60] (Tables 2, 3, 4).
Table 4.
Characteristics of studies and participants and presence of analytical themes. (aHigher order constructs: Risk perception and risk communication; coping and adaptation; Discrimination- intersectionality)
| Author | Research aims | Country | Recruitment strategy | Participants’ age | Number of participants | Methodology | CASP score | Higher order constructsa | ||
|---|---|---|---|---|---|---|---|---|---|---|
| 1 | 2 | 3 | ||||||||
| Akkus et al., 2021 [62] | To examine thoroughly the perceptions and experiences of older people regarding the COVID-19 outbreak | Turkey | Purposeful snowball sampling | 10 women, 6 men, age range 65 -80 | 16 | Content analysis | 18 | X | ||
| Banerjee & Rao, 2021 [63] | To explore the lived experiences and psychosocial challenges of older transgender adults during the COVID-19 pandemic in India | India | Purposeful snowball sampling from LGBTQ community, Index participant was known | Age range 64- 71, mean age 66.4 | 10 | Hasse’s adaptation of Colaizzi’s phenomenological | 19 | X | X | X |
| Brooke & Clark, 2020 [64] | To explore older people's initial experience of household isolation, social distancing and shielding, and the plans they constructed to support them through the COVID-19 pandemic | UK, Rep Ireland | Snowball and mouth to word | Age range 70—89 mean age 77 (5.77 SD) 4 Cabirian, 1 European, 13 English | 19 | Inductive phenomenology | 21 | X | ||
| Bundy et al., 2021 [65] | To understand how already-lonely older individuals navigated and endured the social isolation of the pandemic | USA | Conducted with patients of a large health care system during assessment | 65 + + age range 65–92 average 73, 7 women, 5 men | 12 | Constant comparative method | 21 | X | ||
| Chemen & Gopalla, 2021 [66] | To explored the lived experiences of older adults living in the community during the COVID-19 sanitary lockdown in the small island state of Mauritius | Mauritius | Convenience snowball sampling | 3 men, 12 women, mean age 69.6 (SD 6.88) no age range available | 15 | Thematic analysis | 22 | X | ||
| Derrer-Merk et al., 2022b [9] | To explores how older people in the United Kingdom experienced changes in inter- and intragenerational support during the COVID-19 pandemic | UK | COVID-19 psychological research consortium | 65 + age range 65- 83 mean 71, SD 5; 18 women, 15 men, 18 living alone 15 not | 33 | Constructivist grounded theory | 21 | X | ||
| Derrer-Merk, et al., 2022c [23] | To explore consequence of COVID-19 measures established new form of ageism in the United Kingdom and Colombia | UK/Colombia | COVID-19 psychological research consortium and snowball sampling | 65/60; UK 65 + age range 65- 83 mean 71, SD 5; 18 women, 15 men, 18 living alone 15 not? CO 32 age range 63–95, mean 69 SD 9, 16 men, 16 women, each 8 living alone or not | 65 | Constructivist grounded theory | 21 | X | X | |
| Falvo et al., 2021 [67] | To explore the lived experiences of individuals aged 64 or older during the first COVID-19 lockdown | Ticino/ Switzerland | Available database from the local source population | 64 + age range 64–85, 12 women, 7 men, average age 75, SD 6,04 | 19 | Inductive thematic analysis | 19 | X | ||
| Fiocco et al., 2021 [68] | To understand the lived experience of community dwelling older adults during the first six months of the pandemic in Ontario, Canada | Canada | Snowball sampling within Stress and Healthy Aging Research Lab and community partners | 65 + , age range 65–81, 13 women, 9 men, average 72.33, SD 4.25, | 22 | Inductive thematic analysis | 18 | X | X | |
| Fristedt et al., 2022 [69] | To explore how adults 70 + experienced and managed changes in everyday life due to the COVID-19 pandemic and how those changes affected wellbeing at the beginning of the virus outbreak | Sweden | Part of the ‘At Risk Study’, a qualitative longitudinal project | 70 + 11 women, 6 men, mean age 76, age range 71–87 | 17 | Qualitative context analysis | 18 | X | X | |
| Gazibara et al., 2022 [70] | To examine the experiences and perceptions of curfew for older people in Serbia 15 months after the curfew had ended | Serbia | Snowball sampling | 65 + , 15 women, 8 men, age range 66–90, mean age 72.4, SD 6.2 | 23 | Descriptive information, using naturalistic theoretical orientation. Qualitative content analysis | 18 | X | X | |
| Giebel et al., 2022 [71] | To explore the psychological effects of COVID-19 public health measures on older adults in Uganda and their coping mechanisms | Uganda | Purpose sampling, Snowball sampling | 60 + , 23 women, 7 men, no other information | 30 | Deductive thematic analysis | 14 | X | X | |
| Goins et al., 2021 [72] | To understand COVID-related perceptions and behaviours of older adults residing in the United States | USA | Master students recruited each 2 participants, convenience sampling | 65 + mean age 72.4 SD 6.7 age range 65–92, 24 women, 19 men | 43 | Low-inference qualitative descriptive design | 18 | X | X | |
| Gomes et al., 2021 [73] | To unveil the experience of the elderly with social isolation in the pandemic of COVID-19 | Brazil | Not mentioned | 60 + age range 60–79 | 14 | Inductive classification of words IRAMUTEC and multivariate analysis | 14 | X | ||
| Gonçalves et al., 2022 [74] | To evaluate the knowledge, routine, and perception of older adults from four countries about dealing with COVID-19 in the social isolation period | Brazil, United States, Italy, and Portugal | Snowball technique | Mean age varied from 65.8 to 72.4 Brazil 69.5 (SD 6.2), USA 68.4 (SD 10.6), Portugal 72.4 (SD 7.6), Italy 65.8 (SD 3.7) total male 6, women 19 | 25 | Content analysis based on thematic units | 13 | X | X | |
| Greenwood-Hickman et al., 2021 [75] | To explore the physical, mental, and social health impacts of the pandemic on older adults and their coping techniques | USA | HART randomized controlled trial'- recruited from Kaiser Permanente Washington membership panels in King County, WA | 16 women, 8 men, 1 non-binary, mean age 68, range 60–77 no SD | 25 | Inductive thematic approach assisted by Atlas | 20 | X | X | |
| Hafford-Letchfield et al., 2022 [76] | To report immediate impact of social distancing measures on the lives (LGBT +) | UK | Nothing mentioned | 60 + age from the professional is not known, 60–74, LGBT, 12 women, 5 men | 17 LGBT older adults + 6 professionals from the LGBT community centre | Content analysis, from audio and memos, no transcripts | 16 | X | X | X |
| Huntley & Bratt, 2022 [77] | To explore the lived experiences of eight older adults in Sweden, of living during a pandemic | Sweden | Convenience sampling snowball sampling | 70 + age range 71–82 four men, four women | 8 | Interpretative phenomenological analysis (IPA) using diaries across a 14-day period, followed by interviews | 21 | X | ||
| Jiménez-Etxebarria et al., 2021 [78] | To explore the perspective, perception, attitudes, treatment, and changes of people over 67 | Spain | Convenience sampling, snowball technique | 67 age range 68–81, 6 men, 20 women, (no mean or SD) | 26 | Inductive approach | 21 | X | X | |
| Kremers et al., 2022 [79] | To explore independently living older adults’ perceptions of social and emotional well- being during the COVID- 19- related self- isolation, and their motivation to expand their social network in the future | Netherland | Snowball sampling Local newspaper and website advertisement, ‘Netwerk 100’, and the personal network of the researchers | 56 + age range 56–87, mean age 72, (SD 7.5) 11 women, 9 men | 20 | Open coding process, grounded theory approach | 19 | X | X | |
| Kulmala et al., 2021 [80] | To investigated changes in personal networks among community-dwelling oldest-old individuals (persons aged 80 and over) during the first and second waves of the COVID-19 pandemic in Finland | Finland | Cardiovascular Risk Factors, Aging, and Dementia (CAIDE85 +) study | 80 + age mean, 84.8 Sd 7.3, 10 women, 5 men, | 15 | Directed content analyses | 16 | X | ||
| Mahapatra, et al., 2021 [81] | To explore the ‘coping reflections’ of elderly couples living alone (without any other family members) during the COVID-19 pandemic in urban Odisha, India | India | Our study was nested within a larger community-based study | 65 + couples living alone, 11 couples = 22 participants | 11 | Interpretive thematic analysis | 20 | X | X | |
| McKinlay et al., 2021 [82] | To examine factors that threatened and protected the wellbeing of older adults living in the UK during social distancing restrictions due to the COVID-19 pandemic | UK | Purposive, snowball sampling | 70 + 9 women, 11 men, average 79 age range 70 s -90 s | 20 | Reflexive thematic analysis | 21 | X | X | |
| Pfabigan et al., 2022 [83] | To explore how the COVID-19 containment policies affected older people living alone | Austria | The sub-study is part of the OPLA study | Age range79-94 mean 85; 1 mn, 6 women | 7 | Framework method | 20 | X | X | |
| Prigent et al., 2022 [84] | To explore experiences of intergenerational interaction during the first COVID-19 lockdown in Aotearoa, New Zealand (NZ) | New Zealand | Nationwide Snowball sampling | 70 + / 13 younger as s70 age range 60–94, 67% women, 29 men, 3 no gender | 412 letters | Reflexive thematic analysis | 20 | X | ||
| Sangrar et al., 2021 [85] | To examined perspectives on COVID-19 messaging | Canada | Purposive sampling | 65 + 67- 91 age range, average 75.4, SD 7.0, 14 women, 4 men | 18 | Inductive thematic analysis | 20 | X | ||
| Sattari & Billore, 2020 [86] | To explore the respective risk perception toward the Covid-19 pandemic among the elderly in two developing countries | India and Iran | Not described | 60–85, age range 65–83, 12 men, 10 women, | 22 | Not described | 9 | X | X | |
| Verhage et al., 2021 [87] | To explore how Dutch older adult’s view this crisis and cope with measures | Netherland | Snowball sampling | 54–95. age range 54–95, mean age 75.5, 34 women, 25 men | 59 | Constant comparison | 22 | X | X | |
| Wang et al., 2021 [88] | To understand the unique experiences of older Chinese adults in Canada in the early stages of the COVID-19 pandemic | Canada | Criterion sampling, purposive sampling | 65 + , age range 65–83, average 73, 8 women, 7 men | 15 | Thematic analysis | 21 | X | X | |
| Xie et al., 2021 [89] | To address the gap of COVID-19 pandemic’s impact of community-dwelling older adults’ lived experiences during this historical period | USA, Texas | Snowball sampling through local organizations (e.g., senior centers, Meals on Wheels) | 65–92. mean age 73.6, SD 6.33, 138 women 62 men, | 200 | Inductive thematic analysis | 17 | X | X | |
| Yang et al., 2021 [90] | To explore the experiences of community- dwelling older adults in Wuhan during the coronavirus disease 2019 lockdown | China | Purposive and snowball sampling | 65 + women 10, men 8, mean age 72, SD 5.53 | 18 | Colaizzi's phenomenological approach | 19 | X | X | |
| Yildirim, 2022 [91] | To identify the psychosocial status, attitudes, and experiences of individuals aged 65 and over who were in- home lockdown during the COVID- 19 outbreak in Turkey | Turkey | Snowball sampling method | 65 + , mean age 71.33 SD 5.26, age range 65–91, women 23, men 28 | 51 | Thematic analysis | 13 | X | X | X |
aTheme 1: Risk perception and risk communication
Theme 2: Coping and adaptation
Theme 3: Discrimination- intersectionality
Findings
We identified twenty-seven out of thirty-two studies as moderate-high quality; they met most of the criteria (scoring 16/22 or above on the CASP; [54]. Only five papers were identified as low qualitative papers scoring 15 and below [71, 73, 74, 86, 91]. Please see the scores provided for each paper in Table 4. The low-quality papers did not provide sufficient details regarding the researcher’s relationship with the participants, sampling and recruitment, data collection, rigor in the analysis, or epistemological or ontological reasoning. For example, Yildirim [91] used verbatim notes as data without recording or transcribing them. This article described the analytical process briefly but was missing a discussion of the applied reflexivity of using verbatim notes and its limitations [92].
This systematic review found that many studies did not mention the relationship between the authors and the participant. The CASP critical appraisal tool asks: Has the relationship between the researcher and participants been adequately considered? (reflecting on own role, potential bias). Many studies reported that the recruitment was drawn from larger studies and that the qualitative study was a sub-study. Others reported that participants contacted the researcher after advertising the study. One study Goins et al., [72] reported that students recruited family members, but did not discuss how this potential bias impacted the results.
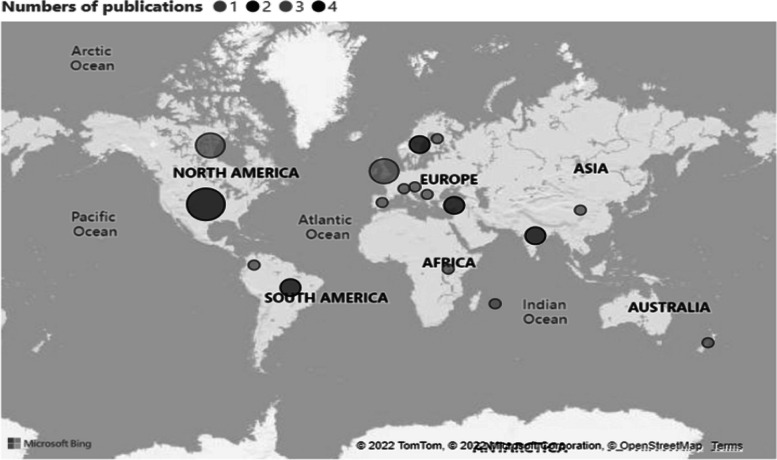
Our review brings new insights into older adults’ experiences during the pandemic worldwide. The studies were conducted on almost all continents. The majority of the articles were written in Europe followed by North America and Canada (4: USA; 3: Canada, UK; 2: Brazil, India, Netherlands, Sweden, Turkey 2; 1: Austria, China, Finland, India/Iran, Mauritius, New Zealand, Serbia, Spain, Switzerland, Uganda, UK/Ireland, UK/Colombia) (see Fig. 2). Note, as the review focuses on English language publications, we are unable to comment on qualitative research conducted in other languages see [72].
Fig. 2.
Numbers of publications by country
The characteristics of the included studies and the presence of analytical themes can be found in Table 4. We used the following characteristics: Author and year of publication, research aims, the country conducted, Participant’s age, number of participants, analytical methodology, CASP score, and themes.
We identified three themes: desired and challenged wellbeing; coping and adaptation; discrimination and intersectionality. We will discuss the themes in turn.
Desired and challenged wellbeing
Most of the studies reported the impact of the COVID-19 pandemic on the well-being of older adults. Factors which influenced wellbeing included: risk communication and risk perception; social connectivity; confinement (at home); and means of coping and adapting. In this context, well-being refers to the evidence reported about participants' physical and mental health, and social connectivity.
Risk perception and risk communication
Politicians and media transmitted messages about the response to the pandemic to the public worldwide. These included mortality and morbidity reports, and details of health and safety regulations like social distancing, shielding- self-isolation, or wearing masks [34–37]. As this risk communication is crucial to combat the spread of the virus, it is also important to understand how people perceived the reporting during the pandemic.
Seven studies reported on how the mass media impacted participants' well-being [23, 67, 68, 70, 72, 81, 85]. Sangrar et al. [68] investigated how older adults responded to COVID-19 messaging: “My reaction was to try to make sure that I listen to everything and [I] made sure I was aware of all the suggestions and the precautions that were being expressed by various agencies …”. (p. 4). Other studies reported the negative impact on participants' well-being of constant messaging and as a consequence stopped watching the news to maintain emotional well-being [3, 67, 68, 70, 72, 81, 85]. Derrer-Merk et al. [23] reported one participant said that “At first, watching the news every day is depressing and getting more and more depressing by the day, so I’ve had to stop watching it for my own peace of mind” (p. 13). In addition, news reporting impacted participants’ risk perception. For example, “Sometimes we are scared to hear the huge coverage of COVID-19 news, in particular the repeated message ‘older is risky’, although the message is useful.” ([81], p5).
Social connectivity
Social connectivity and support from family and community were found in fourteen of the studies as important themes [9, 62, 66–68, 75–80, 83, 84, 90].
The impact of COVID-19 on social networks highlighted the diverse experiences of participants. Some participants reported that the size of social contact was reduced: “We have been quite isolated during this corona time” ?([80], p. 3). Whilst other participants reported that the network was stable except that the method of contact was different: “These friends and relatives, they visited and called as often as before, but of course, we needed to use the telephone when it was not possible to meet” ([77], p. 5). Many participants in this study did not want to expand their social network see also [9, 77–79]. Hafford-Letchfield et al. [76] reported that established social networks and relationships were beneficial for the participants: “Covid has affected our relationship (with partner), we spend some really positive close time together and support each other a lot” (p. 7).
On the other hand, other studies reported decreases of, and gaps in, social connectedness: “I couldn’t do a lot of things that I’ve been doing for years. That was playing competitive badminton three times a week, I couldn’t do that. I couldn’t get up early and go volunteer in Seattle” [9, 67, 75]. A loss of social connection with children and grandchildren was often mentioned: “We cannot see our grandchildren up close and personal because, well because they [the parents] don’t want us, they don’t want to risk our being with the kids … it’s been an emotional loss exacerbated by the COVID thing” ([68] p.10); see also [9, 67, 78]. On the contrary, Chemen & Gopalla [66] note that those older adults who were living with other family members reported that they were more valued: “Last night my daughter-in-law thanked me for helping with my granddaughter” (p.4).
Despite reports of social disconnectedness, some studies highlighted the importance of support from family members and how support changed during the COVID-19 pandemic [9, 62, 81, 83, 90]. Yang et al. [90] argued that social support was essential during the Lockdown in China: “N6 said: ‘I asked my son-in-law to take me to the hospital” (p. 4810). Mahapatra et al. [81] found, in an Indian study, that the complex interplay of support on different levels (individual, family, and community) helped participants to adapt to the new situation. For example, this participant reported that: “The local police are very helpful. When I rang them for something and asked them to find out about it, they responded immediately” (p. 5).
Impact of confinement on well being
Most articles highlighted the impact of confinement on older adults’ well-being [9, 62, 63, 65, 67, 69, 70, 72, 75, 77–79, 81–83, 85, 89, 90].
Some studies found that participants maintained emotional well-being during the pandemic and it did not change their lifestyle [79, 80, 82, 83, 89, 92]: “Actually, I used this crisis period to clean my house. Bookcases are completely cleaned and I discarded old books. Well, we have actually been very busy with those kind of jobs. So, we were not bored at all” ([79], p. 5). In McKinlay et al. [82]’s study, nearly half of the participants found that having a sense of purpose helped to maintain their well-being: “You have to have a purpose you see. I think mental resilience is all about having a sense of purpose” (p. 6).
However, at the same time, the majority of the articles (12 out of 18) highlighted the negative impact of confinement and social distancing. Participants talked of increased depressive feelings and anxiety. For example, one of Akkus et al.’s [62] participants said: “... I am depressed; people died. Terrible disease does not give up, it always kills, I am afraid of it …” (p. 549). Similarly, one of Falvo et al.’s [67] participants remarked: “I am locked inside my house and I am afraid to go out” (p. 7).
Many of the studies reported the negative impact of loneliness as a result of confinement on participants’ well-being including [69, 70, 72, 78, 79, 90, 93]. Falvo et al. [67] reported that many participants experienced loneliness: “What sense does it make when you are not even able to see a family member? I mean, it is the saddest thing not to have the comfort of having your family next to you, to be really alone” (p. 8).
Not all studies found a negative impact on loneliness. For example, a “loner advantage” was found by Xie et al. ([82], p. 386). In this study participants found benefits in already being alone “It’s just a part of who I am, and I think that helps—if you can be alone, it really is an asset when you have to be alone” ([82], p. 386).
Bundy et al. [80] investigated loneliness from already lonely older adults and found that many participants did not attribute the loneliness to the pandemic: “It’s not been a whole lot, because I was already sitting around the house a whole lot anyway ( …). It’s basically the same, pretty well … I’d pretty well be like this anyway with COVID or without COVID” (p. 873) (see also [83]).
A study from Serbia investigated how the curfew was perceived 15 months afterward. Some participants were calm: “I realized that … well … it was simply necessary. For that reason, we accepted it as a measure that is for the common good” ([70], p.634). Others were shocked: “Above all, it was a huge surprise and sort of a shock, a complete shock because I have never, ever seen it in my life and I felt horrible, because I thought that something even worse is coming, that I even could not fathom” ([70], p. 634).
The lockdowns brought not only mental health issues to the fore but impacted the physical health of participants. Some reported they were fearful of the COVID-19 pandemic: “... For a little while I was afraid to leave, to go outside. I didn’t know if you got it from the air” ([75]. p. 6). Another study reported: “It’s been important for me to walk heartily so that I get a bit sweaty and that I breathe properly so that I fill my lungs—so that I can be prepared—and be as strong as possible, in case I should catch that coronavirus” ([77], p. 9); see also [70, 78, 82, 85].
Coping and adaptation
Many studies mentioned older adults’ processes of coping and adaptation during the pandemic [63, 64, 68, 69, 72, 75, 79, 81, 85, 87–90].
A variety of coping processes were reported including: acceptance; behavioural adaptation; emotional regulation; creating new routines; or using new technology. Kremers et al. [79] reported: “We are very realistic about the situation and we all have to go through it. Better days will come” (p. e71). Behavioural adaptation was reported: “Because I’m asthmatic, I was wearing the disposable masks, I really had trouble breathing. But I was determined to find a mask I could wear” ([68], p. 14). New routines with protective hygiene helped some participants at the beginning of the pandemic to cope with the health threat: “I am washing my hands all the time, my hands are raw from washing them all the time, I don't think I need to wash them as much as I do but I do it just in case, I don’t have anybody coming in, so there is nobody contaminating me, but I keep washing” ([69], p. 4391); see also [72]. Verhage et al. [87] reported strategies of coping including self-enhancing comparisons, distraction, and temporary acceptance: “There are so many people in worse circumstances …” (p. e294). Other studies reported how participants used a new technology: “I have recently learned to use WhatsApp, where I can make video phone calls.” ([88], p. 163); see also [89].
Discrimination -intersectionality (age and race/gender identity)
Seven studies reported ageism, racism, and gender discrimination experienced by older adults during the pandemic [23, 63, 67, 70, 76, 84, 88].
Prigent et al. [84], conducted in a New Zealand study, found that ageism was reciprocal. Younger people spoke against older adults: “why don’t you do everyone a favour and drop dead you f******g b**** it’s all because of ones like you that people are losing jobs” (p. 11). On the other hand, older adults spoke against the younger generation: “Shame to see the much younger generations often flout the rules and generally risk the gains made by the team. Sheer arrogance on their part and no sanctions applied” (p.11). Although one study reported benevolent ageism [23] most studies found hostile ageism [23, 63, 67, 70, 76, 84]. One study from Canada exploring 15 older adult’s Chinese immigrants’ experiences reported racism as people around them thought they would bring the virus into the country. The negative impact on existing friendships was told by a Chinese man aged 69 “I can tell some people are blatantly despising us. I can feel it. When I talked with my Caucasian friends verbally, they would indirectly blame us for the problem. Eventually, many of our friendships ended because of this issue” ([88], p161). In addition, this study reported ageism when participants in nursing homes felt neglected by the Canadian government.
Two papers reported experiences of sexual and gender minorities (SGM) (e.g. transgender, queer, lesbian or gay) and found additional burdens during the pandemic [63, 76]. People experienced marginalisation, stereotypes, and discrimination, as well as financial crisis: “I have faced this throughout life. Now people look at me in a way as if I am responsible for the virus.” ([63], p. 6). The consequence of marginalisation and ignorance of people with different gender identities was also noted by Hafford- Letchfield et al. [76]: “People have been moved out of their accommodation into hotels with people they don't know …. a gay man committed suicide, community members know of several that have attempted suicide. They are feeling pretty marginalised and vulnerable and you see what people are writing on the chat pages” (p.4). The intersection of ageism, racism, and heterosexism and its negative impact on people’s well-being during the pandemic reflects additional burden and stressors for older adults.
Discussion
This systematic literature review is important as it provides new insights into the lived experiences of older adults during the COVID-19 pandemic, worldwide. Our study highlights that the COVID-19 pandemic brought an increase in English-written qualitative articles to the fore. We found that 32 articles met the inclusion criteria but 5 were low quality. A lack of transparency reduces the trustworthiness of the study for the reader and the scientific community. This is particularly relevant as qualitative research is often criticised for its bias or lack of rigor [94]. However, their findings are additional evidence for our study.
Our aim was to explore, in a systematic literature review, the lived experiences of older adults during the COVID-19 pandemic worldwide. The evidence highlights the themes of desired and challenged wellbeing, coping and adaptation, and discrimination and intersectionality, on wellbeing.
Perceived risk communication was experienced by many participants as overwhelming and anxiety-provoking. This finding supports Anwar et al.’s [37] study from the beginning of the pandemic which found, in addition to circulating information, that mass media influenced the public's behaviour and in consequence the spread of disease. The impact can be positive but has also been revealed to be negative as well. They suggest evaluating the role of the mass media in relation to what and how it has been conveyed and perceived. The disrupted social connectivity found in our review supports earlier studies that reported the negative impact of people’s well-being [6–28] at the beginning of the pandemic. This finding is important for future health crisis management, as the protective health measures such as confinement or self-isolation had a negative impact on many of the participants’ emotional wellbeing including increased anxiety, feelings of depression, and loneliness during the lockdowns. As a result of our review, future protective health measures should support people’s desire to maintain proximity with their loved ones and friends. However, we want to stress that our findings are mixed.
The ability of older adults to adapt and cope with the health crisis is important: many of the reported studies noted the diverse strategies used by older people to adapt to new circumstances. These included learning new technologies or changing daily routines. Politicians and the media and politicians should recognise both older adults' risk of disease and its consequences, but also their adaptability in the face of fast-changing health measures. This analysis supports studies conducted over the past decades on lifespan development, which found that people learn and adapt livelong to changing circumstances [95–97].
We found that discrimination against age, race, and gender identity was reported in some studies, in particular exploring participants’ experiences with immigration backgrounds and sexual and gender minorities. These studies highlighted the intersection of age and gender or race and were additional stressors for older adults and support the findings from Ramirez et al. [98] This review suggests that more research should be conducted to investigate the experiences of minority groups to develop relevant policies for future health crises.
Our review was undertaken two years after the pandemic started. At the cut-off point of our search strategy, no longitudinal studies had been found. However, in December 2022 a longitudinal study conducted in the USA explored older adult’s advice given to others [99]. They found that fostering and maintaining well-being, having a positive life perspective, and being connected to others were coping strategies during the pandemic [100]. This study supports the results of the higher order constructs of coping and adaptation in this study. Thus, more longitudinal studies are needed to enhance our understanding of the long-term consequences of the COVID-19 pandemic. The impact of the COVID-19 restrictions on older adults’ lives is evident. We suggest that future strategies and policies, which aim to protect older adults, should not only focus on the physical health threat but also acknowledge older adults' needs including psychological support, social connectedness, and instrumental support. The policies regarding older adult’s protections changed quickly but little is known about older adults’ involvement in decision making [100]. We suggest including older adults as consultants in policymaking decisions to ensure that their own self-determinism and independence are taken into consideration.
There are some limitations to this study. It did not include the lived experiences of older adults in care facilities or hospitals. The studies were undertaken during the COVID-19 pandemic and therefore data collection was not generally undertaken face-to-face. Thus, many studies included participants who had access to a phone, internet, or email, others could not be contacted. Additionally, we did not include published papers after August 2022. Even after capturing the most commonly used terms and performing additional hand searches, the search terms used might not be comprehensive. The authors found the quality of the papers to be variable, and their credibility was in question. We acknowledge that more qualitative studies might have been published in other languages than English and were not considered in this analysis.
To conclude, this systematic literature review found many similarities in the experiences of older adults during the Covid-19 pandemic despite cultural and socio-economic differences. However, we stress to acknowledge the heterogeneity of the experiences. This study highlights that the interplay of mass media reports of the COVID-19 pandemic and the policies to protect older adults had a direct impact on older adults’ well-being. The intersection of ‘isms’ (ageism, racism, and heterosexism) brought an additional burden for some older adults [98]. These results and knowledge about the drawbacks of health-protecting measures need to be included in future policies to maintain older adults’ well-being during a health crisis.
Acknowledgements
Not applicable
Authors’ contributions
Elfriede Derrer-Merk contributed to the design, analysis, and writing the draft. Maria-Fernanda Rodriguez-Reyes contributed to the analysis, revised the draft, and approved the submission. Laura K. Soulsby contributed to the analysis, revised the draft, and approved the submission. Louise Roper contributed to the analysis, revised the draft, and approved the submission. Kate M. Bennett contributed to the design, analysis, writing the draft, and approved the submission.
Funding
Not applicable.
Availability of data and materials
The systematic literature review is based on already published articles. And all data analysed during this study are included in this manuscript. No additional data was used.
Declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Footnotes
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.World Health Organisation (WHO): WHO Director-General’s opening remarks at the media briefing on COVID-19 - 11 March 2020. 2020. Retrieved from https://www.who.int/director-general/speeches/detail/who-director-general-s-opening-remarks-at-the-media-briefing-on-covid-19---11-march-2020.
- 2.WorldOMeter: Coronavirus toll update: Cases & deaths by country. 2022. Worldometers. https://www.worldometers.info/coronavirus/.
- 3.World Health Organisation (WHO): Coronavirus disease. 2022. https://www.who.int/health-topics/coronavirus#tab=tab. Aaccessed 5 Oct 2022.
- 4.Ayouni I, Maatoug J, Dhouib W, Zammit N, Fredj SB, Ghammam R, Ghannem H. Effective public health measures to mitigate the spread of COVID-19: a systematic review. BMC Public Health. 2021;21(1):1015. doi: 10.1186/s12889-021-11111-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Cerasoli B. The frail future of geriatrics. Lancet Healthy Longev. 2020;1(1):e11. doi: 10.1016/S2666-7568(20)30005-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Allen K-A, Arslan G, Craig H, Arefi S, Yaghoobzadeh A, Sharif Nia H. The psychometric evaluation of the sense of belonging instrument (SOBI) with Iranian older adults. BMC Geriatr. 2021;21(1):211. doi: 10.1186/s12877-021-02115-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Bailey L, Ward M, DiCosimo A, Baunta S, Cunningham C, Romero-Ortuno R, Kenny RA, Purcell R, Lannon R, McCarroll K, et al. Physical and mental health of older people while cocooning during the COVID-19 pandemic. QJM. 2021;114(9):648–653. doi: 10.1093/qjmed/hcab015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Dahlberg L. Loneliness during the COVID-19 pandemic. Aging Ment Health. 2021;25(7):1161–1164. doi: 10.1080/13607863.2021.1875195. [DOI] [PubMed] [Google Scholar]
- 9.Derrer-Merk E, Ferson S, Mannis A, Bentall R, Bennett KM. Older people's family relationships in disequilibrium during the COVID-19 pandemic. What really matters? Ageing Soc. 2022:1–18.
- 10.Derrer-Merk E, Ferson S, Mannis A, Bentall RP, Bennett KM. Belongingness challenged: Exploring the impact on older adults during the COVID-19 pandemic. PLoS ONE. 2022;17(10):e0276561. doi: 10.1371/journal.pone.0276561. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Heidinger T, Richter L. The effect of COVID-19 on loneliness in the elderly. An empirical comparison of pre-and peri-pandemic loneliness in community-dwelling elderly. Front Psychol. 2020;11:(585308). [DOI] [PMC free article] [PubMed]
- 12.Richter L, Heidinger T. Hitting close to home: the effect of COVID-19 illness in the social environment on psychological burden in older adults. Front Psychol. 2021;12:(737787). [DOI] [PMC free article] [PubMed]
- 13.Krendl AC, Perry BL. The impact of sheltering in place during the COVID-19 pandemic on older adults' social and mental well-being. J Gerontol B Psychol Sci Soc Sci. 2021;76(2):e53–e58. doi: 10.1093/geronb/gbaa110. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Litwin, H., & Levinsky, M. Social networks and mental health change in older adults after the Covid-19 outbreak. Aging Ment Health. 2021:1–6. 10.1080/13607863.2021.1902468. [DOI] [PubMed]
- 15.De Pue S, Gillebert C, Dierckx E, Vanderhasselt MA, De Raedt R, Van den Bussche E. The impact of the COVID-19 pandemic on wellbeing and cognitive functioning of older adults. Sci Rep. 2021;11(1):4636. doi: 10.1038/s41598-021-84127-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Shahid Z, Kalayanamitra R, McClafferty B, Kepko D, Ramgobin D, Patel R, Aggarwal CS, Vunnam R, Sahu N, Bhatt D, et al. COVID-19 and older adults: what we know. J Am Geriatr Soc. 2020;68(5):926–929. doi: 10.1111/jgs.16472. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Smith M, Steinman L, Casey E. Combatting social isolation among older adults in a time of physical distancing: the COVID-19 social connectivity paradox. Front Public Health. 2020;8:403. doi: 10.3389/fpubh.2020.00403. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Cohn-Schwartz E, Finlay JM, Kobayashi LC. Perceptions of societal ageism and declines in subjective memory during the COVID-19 pandemic: longitudinal evidence from US adults aged ≥55 years. J Soc Issues. 2022;78(4):924–38. [DOI] [PMC free article] [PubMed]
- 19.Tsoukalis-Chaikalis N, Demsia S, Stamatopoulou A, Chaniotis D, Tel Nu. Systematic Mapping Study of Covid-19 Psychological Impact. 2021;15(3):820.
- 20.van Gerwen M, Alsen M, Little C, Barlow J, Genden E, Naymagon L, Tremblay D. Risk factors and outcomes of COVID-19 in New York City; a retrospective cohort study. J Med Virol. 2021;93(2):907–915. doi: 10.1002/jmv.26337. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Victor CR, Rippon I, Barreto M, Hammond C, Qualter P. Older adults’ experiences of loneliness over the lifecourse: an exploratory study using the BBC loneliness experiment. Arch Gerontol Geriatr. 2022;102:104740. doi: 10.1016/j.archger.2022.104740. [DOI] [PubMed] [Google Scholar]
- 22.Vrach IT, Tomar R. Mental health impacts of social isolation in older people during COVID pandemic. Prog Neurol Psychiatry. 2020;24(4):25–29. [Google Scholar]
- 23.Derrer-Merk E, Reyes-Rodriguez M-F, Salazar A-M, Guevara M, Rodríguez G, Fonseca A-M, Camacho N, Ferson S, Mannis A, Bentall RP, et al. Is protecting older adults from COVID-19 Ageism? A comparative cross-cultural constructive grounded theory from the United Kingdom and Colombia. J Soc Issues. 2022;78(4):900–23. [DOI] [PMC free article] [PubMed]
- 24.Lytle A, Levy SR. Reducing ageism toward older adults and highlighting older adults as contributors during the COVID-19 pandemic. J Soc Issues. 2022;78(4):1066–84. [DOI] [PMC free article] [PubMed]
- 25.McDarby M, Ju CH, Picchiello MC, Carpenter BD. Older adults’ perceptions and experiences of ageism during the COVID-19 pandemic. J Soc Issues. 2022;78(4):939–64. [DOI] [PMC free article] [PubMed]
- 26.Drury L, Abrams D, Swift HJ. Intergenerational contact during and beyond COVID-19. J Soc Issues. 2022;78(4):860–82. [DOI] [PMC free article] [PubMed]
- 27.Kanık B, Uluğ ÖM, Solak N, Chayinska M. “Let the strongest survive”: Ageism and social Darwinism as barriers to supporting policies to benefit older individuals. J Soc Issues. 2022;00:1–25. [Google Scholar]
- 28.Spaccatini F, Giovannelli I, Pacilli MG. “You are stealing our present”: Younger people's ageism towards older people predicts attitude towards age-based COVID-19 restriction measures. J Soc Issues. 2022;78(4):769–89. [DOI] [PMC free article] [PubMed]
- 29.Sutter A, Vaswani M, Denice P, Choi KH, Bouchard H, Esses VM. Ageism toward older adults during the COVID-19 pandemic: Intergenerational conflict and support. J Soc Issues. 2022;78(4):815–41. [DOI] [PMC free article] [PubMed]
- 30.Swift H, Chasteen A. Ageism in the time of COVID-19. Group Process Intergroup Relat. 2021;24:246–252. doi: 10.1177/1368430220983452. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.World Health Organisation (WHO): Risk Communication in times of an epidemic or pandemic. Asset paper series Epidemics and Pandemics: 2017. https://www.who.int/emergencies/risk-communicationsWHORCaCERaoSAo.
- 32.Bailey A, Harris MA, Bogle D, Jama A, Muir SA, Miller S, Walters CA, Govia I. Coping with COVID-19: health risk communication and vulnerable groups. Disaster Med Public Health Prep. 2021;17:e22. doi: 10.1017/dmp.2021.225. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Li X, Lyu H. Epidemic risk perception PS, and mental health during COVID-19 pandemic: a moderated mediating model. Front Psychol. 2021;11:563741. doi: 10.3389/fpsyg.2020.563741. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Sandman P M & American Industrial Hygiene Association: Responding to community outrage: strategies for effective risk communication. American Industrial Hygiene Association. 2003.
- 35.Sandman, P M. Introduction and orientation index. https://www.psandman.com/index-intro.htm. Retrieved 13 October 2022.
- 36.Anderson M, Pitchforth E, Asaria M, Brayne C, Casadei B, Charlesworth A, Coulter A, Franklin BD, Donaldson C, Drummond M, et al. LSE-Lancet Commission on the future of the NHS: re-laying the foundations for an equitable and efficient health and care service after COVID-19. Lancet. 2021;397(10288):1915–1978. doi: 10.1016/S0140-6736(21)00232-4. [DOI] [PubMed] [Google Scholar]
- 37.Anwar A, Malik M, Raees V, Anwar A. Role of mass media and public health communications in the COVID-19 pandemic. Cureus. 2020;12(9):e10453. doi: 10.7759/cureus.10453. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.U.S. National Library of Medicine: COVID-19 - Search Details - ClinicalTrials.gov: Clinicaltrials.gov 2022. Retrieved October 13, 2022, from https://clinicaltrials.gov/ct2/results/details?cond=COVID-19.
- 39.Tremblay S, Castiglione S, Audet L-A, Desmarais M, Horace M, Peláez S. Conducting qualitative research to respond to COVID-19 challenges: reflections for the present and beyond. Int J Qual Methods. 2021;20:16094069211009679. [Google Scholar]
- 40.Flemming K, Noyes J. Qualitative evidence synthesis: where are we at? Int J Qual Methods. 2021;20:1609406921993276. [Google Scholar]
- 41.Booth A. Searching for qualitative research for inclusion in systematic reviews: a structured methodological review. Syst Rev. 2016;5(1):74. doi: 10.1186/s13643-016-0249-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Krnic Martinic M, Pieper D, Glatt A, Puljak L. Definition of a systematic review used in overviews of systematic reviews, meta-epidemiological studies and textbooks. BMC Med Res Methodol. 2019;19(1):203. doi: 10.1186/s12874-019-0855-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Phillips V, Barker E. Systematic reviews: structure, form and content. J Perioper Pract. 2021;31(9):349–353. doi: 10.1177/1750458921994693. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Derrer-Merk E, Soulsby L, Reyes Rodriguez M, Ferson S, Mannis A, Bennett KM. Older adults' lived experiences during the COVID-19 pandemic: a systematic review. 2022. PROSPERO 2022 CRD42022331714. Available from: https://www.crd.york.ac.uk/prospero/display_record.php?ID=CRD42022331714.
- 45.Cooke A, Smith D, Booth A. Beyond PICO: the SPIDER tool for qualitative evidence synthesis. Qual Health Res. 2012;22:1435–1443. doi: 10.1177/1049732312452938. [DOI] [PubMed] [Google Scholar]
- 46.Long HA, French DP, Brooks JM. Optimising the value of the critical appraisal skills programme (CASP) tool for quality appraisal in qualitative evidence synthesis. Res Methods Med Health Sci. 2020;1(1):31–42. [Google Scholar]
- 47.Sattar R, Lawton R, Panagioti M, Johnson J. Meta-ethnography in healthcare research: a guide to using a meta-ethnographic approach for literature synthesis. BMC Health Serv Res. 2021;21(1):50. doi: 10.1186/s12913-020-06049-w. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Soundy A, Heneghan NR. Meta-ethnography. Int Rev Sport Exerc Psychol. 2022;15(1):266–286. [Google Scholar]
- 49.Fallon V, Groves R, Halford JCG, Bennett KM, Harrold JA. Postpartum anxiety and infant-feeding outcomes: a systematic review. J Hum Lact. 2016;32(4):740–758. doi: 10.1177/0890334416662241. [DOI] [PubMed] [Google Scholar]
- 50.Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, Shamseer L, Tetzlaff JM, Akl EA, Brennan SE, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. PLoS Med. 2021;18(3):e1003583. doi: 10.1371/journal.pmed.1003583. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Tod D, Booth A, Smith B. Critical appraisal. Int Rev Sport Exerc Psychol. 2022;15(1):52–72. [Google Scholar]
- 52.Morse J. Why the Qualitative Health Research (QHR) review process does not use checklists. Qual Health Res. 2021;31(5):819–821. doi: 10.1177/1049732321994114. [DOI] [PubMed] [Google Scholar]
- 53.Munthe-Kaas HM, Glenton C, Booth A, Noyes J, Lewin S. Systematic mapping of existing tools to appraise methodological strengths and limitations of qualitative research: first stage in the development of the CAMELOT tool. BMC Med Res Methodol. 2019;19(1):113. doi: 10.1186/s12874-019-0728-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Njau B, Covin C, Lisasi E, Damian D, Mushi D, Boulle A, Mathews C. A systematic review of qualitative evidence on factors enabling and deterring uptake of HIV self-testing in Africa. BMC Public Health. 2019;19(1):1289. doi: 10.1186/s12889-019-7685-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Butler A, Hall H, Copnell B. A guide to writing a qualitative systematic review protocol to enhance evidence-based practice in nursing and health care. Worldviews Evid Based Nurs. 2016;13(3):241–249. doi: 10.1111/wvn.12134. [DOI] [PubMed] [Google Scholar]
- 56.Soilemezi D, Linceviciute S. Synthesizing qualitative research: reflections and lessons learnt by two new reviewers. Int J Qual Methods. 2018;17(1):1609406918768014. [Google Scholar]
- 57.Booth A. Harnessing energies, resolving tensions: acknowledging a dual heritage for qualitative evidence synthesis. Qual Health Res. 2019;29(1):18–31. doi: 10.1177/1049732318808247. [DOI] [PubMed] [Google Scholar]
- 58.Carroll C, Booth A. Quality assessment of qualitative evidence for systematic review and synthesis: Is it meaningful, and if so, how should it be performed? Res Synth Methods. 2015;6(2):149–154. doi: 10.1002/jrsm.1128. [DOI] [PubMed] [Google Scholar]
- 59.Charmaz K. Constructing Grounded Theory. 2. London: Sage; 2014. [Google Scholar]
- 60.Toye F, Seers K, Allcock N, Briggs M, Carr E, Barker K. Meta-ethnography 25 years on: challenges and insights for synthesising a large number of qualitative studies. BMC Med Res Methodol. 2014;14(1):80. doi: 10.1186/1471-2288-14-80. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Noblit GW, Hare RD. Meta-ethnography: synthesizing qualitative studies. California: Sage Publications Ltd; 1988. [Google Scholar]
- 62.Akkus Y, Parlak A, Karacan Y, Karatay G. Perceptions and experiences of older people regarding the COVID-19 pandemic process: a phenomenological study. Turk Geriatri Dergisi. 2021;24:546–556. [Google Scholar]
- 63.Banerjee D, Rao TSS. “The Graying Minority”: lived experiences and psychosocial challenges of older transgender adults during the COVID-19 pandemic in India, A qualitative exploration. Front Psychiatry. 2021;11:604472. doi: 10.3389/fpsyt.2020.604472. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.Brooke J, Jackson D. Older people and COVID-19: Isolation, risk and ageism. J Clin Nurs. 2020;29(13-14):2044–6. [DOI] [PubMed]
- 65.Bundy H, Lee HM, Sturkey KN, Caprio AJ. The lived experience of already-lonely older adults during COVID-19. Gerontologist. 2021;61(6):870–877. doi: 10.1093/geront/gnab078. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66.Chemen S, Gopalla YN. Lived experiences of older adults living in the community during the COVID-19 lockdown - The case of mauritius. J Aging Stud. 2021;57:100932. doi: 10.1016/j.jaging.2021.100932. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67.Falvo I, Zufferey MC, Albanese E, Fadda M. Lived experiences of older adults during the first COVID-19 lockdown: a qualitative study. PLoS ONE. 2021;16(6):e0252101. doi: 10.1371/journal.pone.0252101. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Fiocco AJ, Gryspeerdt C, Franco G. Stress and adjustment during the COVID-19 pandemic: a qualitative study on the lived experience of Canadian older adults. Int J Environ Res Public Health. 2021;18(24):12922. doi: 10.3390/ijerph182412922. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Fristedt S, Carlsson G, Kylén M, Jonsson O, Granbom M. Changes in daily life and wellbeing in adults, 70 years and older, in the beginning of the COVID-19 pandemic. Scand J Occup Ther. 2022;29(6):511–521. doi: 10.1080/11038128.2021.1933171. [DOI] [PubMed] [Google Scholar]
- 70.Gazibara T, Maksimovic N, Dotlic J, Jeremic Stojkovic V, Cvjetkovic S, Milic M. Experiences and aftermath of the COVID-19 lockdown among community-dwelling older people in Serbia: a qualitative study. J Eval Clin Pract. 2022;28(4):631–640. doi: 10.1111/jep.13641. [DOI] [PubMed] [Google Scholar]
- 71.Giebel C, Ivan B, Ddumba I. COVID-19 public health restrictions and older adults’ well-being in Uganda: psychological impacts and coping mechanisms. Clin Gerontol. 2022;45(1):97–105. doi: 10.1080/07317115.2021.1910394. [DOI] [PubMed] [Google Scholar]
- 72.Goins RT, Anderson E, Minick H, Daniels H. Older adults in the United States and COVID-19: a qualitative study of perceptions, finances, coping, and emotions. Front Public Health. 2021;9:660536. doi: 10.3389/fpubh.2021.660536. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73.Gomes MACFC, Fontenele NAO, Galindo Neto NM, Barros LM, Frota NM. Elderly people’s experience facing social isolation in the COVID-19 pandemic. Rev Rene. 2021;22:e69236. doi: 10.15253/2175-6783.20212269236. [DOI] [Google Scholar]
- 74.Gonçalves AR, Barcelos JLM, Duarte AP, Lucchetti G, Gonçalves DR. Silva e Dutra FCM, Gonçalves JRL: Perceptions, feelings, and the routine of older adults during the isolation period caused by the COVID-19 pandemic: a qualitative study in four countries. Aging Ment Health. 2022;26(5):911–918. doi: 10.1080/13607863.2021.1891198. [DOI] [PubMed] [Google Scholar]
- 75.Greenwood-Hickman MA, Dahlquist J, Cooper J, Holden E, McClure JB, Mettert KD, Perry SR, Rosenberg DE. "They're Going to Zoom It": a qualitative investigation of impacts and coping strategies during the COVID-19 pandemic among older adults. Front Public Health. 2021;9:679976. doi: 10.3389/fpubh.2021.679976. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Hafford-Letchfield T, Toze M, Westwood S. Unheard voices: a qualitative study of LGBT+ older people experiences during the first wave of the COVID-19 pandemic in the UK. Health Soc Care Community. 2022;30(4):e1233–e1243. doi: 10.1111/hsc.13531. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77.Huntley R, Bratt AS. An interpretative phenomenological analysis of the lived experiences of older adults during the covid-19 pandemic in sweden. Nordic Psychol. 2022;75(1)3–19.
- 78.Jiménez-Etxebarria E, Bernaras Iturrioz E, Jaureguizar J. Impact of the COVID-19 pandemic as perceived by older people in Northern Spain. Psychol Res Behav Manag. 2021;14:1789–1803. doi: 10.2147/PRBM.S308537. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 79.Kremers EM, Janssen JHM, Nieuwboer MS, Olde Rikkert MGM, Peeters GMEE. The psychosocial adaptability of independently living older adults to COVID-19 related social isolation in the Netherlands: a qualitative study. Health Soc Care Community. 2022;30(1):e67–e74. doi: 10.1111/hsc.13436. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80.Kulmala J, Tiilikainen E, Lisko I, Ngandu T, Kivipelto M, Solomon A. Personal social networks of community-dwelling oldest old during the Covid-19 pandemic—A qualitative study. Front Public Health. 2021;9:1–10. [DOI] [PMC free article] [PubMed]
- 81.Mahapatra P, Sahoo KC, Desaraju S, Pati S. Coping with COVID-19 pandemic: reflections of older couples living alone in urban Odisha India. Prim Health Care Res Dev. 2021;22:e64. doi: 10.1017/S1463423621000207. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 82.McKinlay AR, Fancourt D, Burton A. A qualitative study about the mental health and wellbeing of older adults in the UK during the COVID-19 pandemic. BMC Geriatr. 2021;21(1):1–10. doi: 10.1186/s12877-021-02367-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 83.Pfabigan J, Wosko P, Pichler B, Reitinger E, Pleschberger S. Under reconstruction: the impact of COVID-19 policies on the lives and support networks of older people living alone. Int J Care Caring. 2022;6(1-2):211–28. [DOI] [PMC free article] [PubMed]
- 84.Prigent C, Morgan T, Wiles J, Morgan K, Williams L, Gott M. Intergenerational tension or cohesion during the covid-19 pandemic?: A letter-writing study with older new zealanders. J Intergenerational Relationsh. 2022;20(4):386–405.
- 85.Sangrar R, Porter MM, Chesser S. Exploring the interpretation of COVID-19 messaging on older adults. Experiences of vulnerability. Can J Aging Rev Can Vieil. 2021;40(4):533–542. [Google Scholar]
- 86.Sattari S, Billore S. Bring it on Covid-19: being an older person in developing countries during a pandemic. Working Older People. 2020;24(4):281–291. [Google Scholar]
- 87.Verhage M, Thielman L, Kock L, Lindenberg J. Coping of older adults in times of COVID-19: considerations of temporality among dutch older adults. J Gerontol B. 2021;76(7):e290–9. [DOI] [PMC free article] [PubMed]
- 88.Wang Q, Liu JKK, Walsh CA. Identities: experiences and impacts of the COVID-19 pandemic from the perspectives of older Chinese immigrants in Canada. China J Soc Work. 2021;14(2):153–171. [Google Scholar]
- 89.Xie B, Shiroma K, De Main AS, Davis NW, Fingerman K, Danesh V. Living through the COVID-19 pandemic: community-dwelling older adults’ experiences. J Aging Soc Policy. 2021;33(4–5):380–397. doi: 10.1080/08959420.2021.1962174. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 90.Yang Q, Wang Y, Tian C, Chen Y, Mao J. The Experiences of Community-dwelling older adults during the COVID-19 lockdown in Wuhan: a qualitative study. J Adv Nurs (John Wiley & Sons, Inc) 2021;77(12):4805–4814. doi: 10.1111/jan.14978. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 91.Yıldırım H. Psychosocial status of older adults aged 65 years and over during lockdown in Turkey and their perspectives on the outbreak. Health Soc Care Community. 2022;30(3):899–907. doi: 10.1111/hsc.13542. [DOI] [PubMed] [Google Scholar]
- 92.Hill Z, Tawiah-Agyemang C, Kirkwood B, Kendall C. Are verbatim transcripts necessary in applied qualitative research: experiences from two community-based intervention trials in Ghana. Emerg Themes Epidemiol. 2022;19(1):5. doi: 10.1186/s12982-022-00115-w. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 93.Giles D. Performed across Europe and written up in English: the double challenge for qualitative psychologists. Qual Res Psychol. 2019;16(3):503–507. [Google Scholar]
- 94.Anderson C. Presenting and evaluating qualitative research. Am J Pharm Educ. 2010;74(8):141. doi: 10.5688/aj7408141. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 95.Nikitin J, Freund A. The Adaptation Process of Aging. The Cambridge Handbook of Successful Aging. Chapter: 17. Cambridge University Press. 2019. p. 281–98.
- 96.Deimling GT, Kahana B, Bowman KF, Schaefer ML. Cancer survivorship and psychological distress in later life. Psychooncology. 2002;11(6):479–494. doi: 10.1002/pon.614. [DOI] [PubMed] [Google Scholar]
- 97.Baltes PB, Staudinger UM, Lindenberger U. Lifespan psychology: theory and application to intellectual functioning. Annu Rev Psychol. 1999;50:471–507. doi: 10.1146/annurev.psych.50.1.471. [DOI] [PubMed] [Google Scholar]
- 98.Ramirez L, Monahan C, Palacios-Espinosa X, Levy SR. Intersections of ageism toward older adults and other isms during the COVID-19 pandemic. J Soc Issues. 2022;78(4):965–990. doi: 10.1111/josi.12574. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 99.Van Vleet B, Fuller HR, Hofmann B, Huseth-Zosel A. Untapped insight: a longitudinal qualitative analysis of older adults’ advice during the COVID-19 pandemic. Innov Aging. 2022;6(7):igac071. doi: 10.1093/geroni/igac071. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 100.Gietel-Basten S, Matus K, Mori R. COVID-19 as a trigger for innovation in policy action for older persons? Evid Asia Policy Soc. 2022;41(1):168–186. [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
The systematic literature review is based on already published articles. And all data analysed during this study are included in this manuscript. No additional data was used.