Introduction
Discoid lupus erythematosus (DLE) is the most common form of chronic cutaneous lupus erythematosus, an autoimmune skin disease that commonly involves photodistributed areas on the head and neck.1 Involvement of the nails has been reported previously but is extremely rare.2,3 We describe a case of DLE in the nail, which was ultimately treated with thalidomide after it was proven to be refractory to many therapies.
Case report
A 59-year-old woman with a 13-year history of systemic lupus erythematosus (SLE) with discoid and tumid lupus erythematosus of the face and scalp presented in October 2016 for an evaluation of recalcitrant onychodystrophy. A punch biopsy of the fifth fingernail of the left limb was performed earlier that month, which revealed basal layer squamatization, vacuolar interface change, basement membrane zone thickening, superficial and deep dermal perivascular mononuclear cell infiltrate, and diffuse hyalinized, hypocellular change with necrosis involving the reticular dermis, consistent with the connective tissue disease presumed to be DLE.
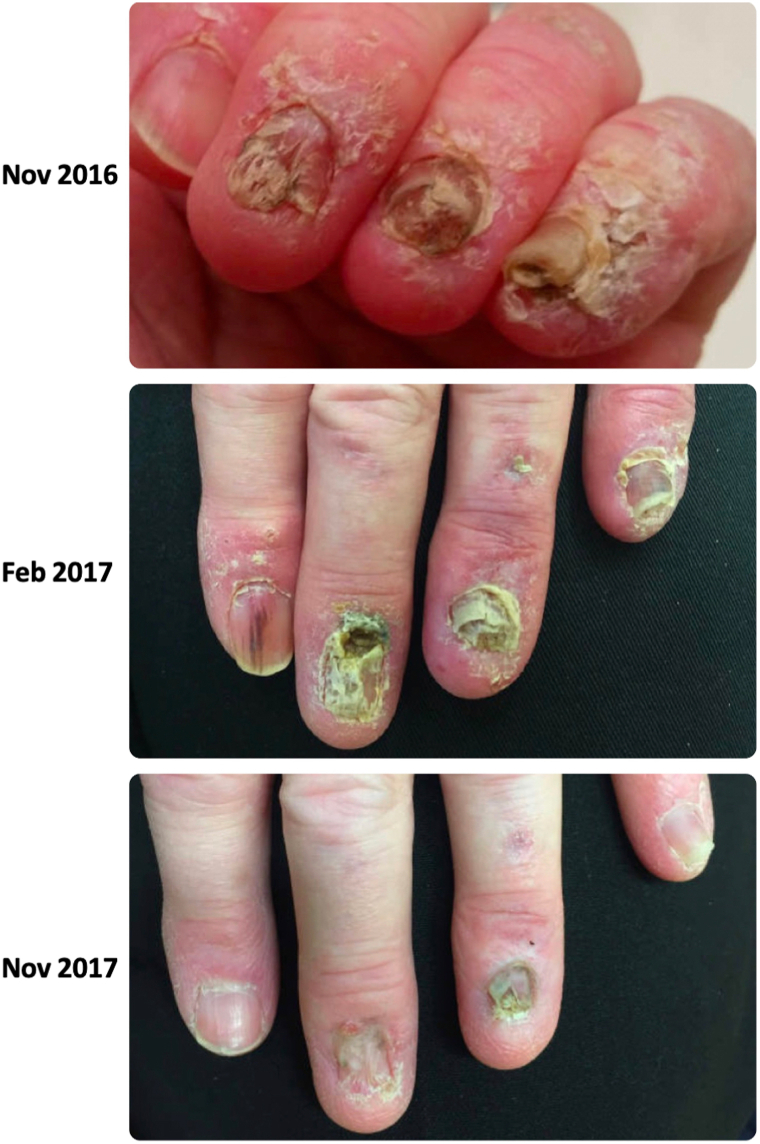
At the time of presentation, her systemic and cutaneous lupus were mostly controlled with hydroxychloroquine (200 mg twice daily), methotrexate (20 mg weekly), and aspirin (325 mg daily). However, the patient had a few newly developed erythematous plaques on the scalp (responsive to topical halobetasol 0.05% cream) and uncontrolled nail disease of the third, fourth, and fifth digits of the left hand. Dermatologic examination at the time of presentation revealed active DLE at the proximal nailfold with resultant onychodystrophy, subungual thickening, onychauxis, and atrophic scarring on the third, fourth, and fifth digits (Fig 1). The patient’s nail disease had previously failed to respond to multiple other medications, including mycophenolate mofetil, prednisone, azathioprine, and epratuzumab (SLE clinical trial).
Fig 1.
A 59-year-old woman with a 13-year history of systemic lupus erythematosus (SLE) with biopsy-proven discoid and tumid lupus erythematosus of the face and scalp with recalcitrant onychodystrophy. November 2016, Discoid lupus erythematosus at the proximal nailfold with resultant onychodystrophy, subungual thickening, onychauxis, and atrophic scarring on the third, fourth, and fifth digits of the left hand. February 2017, New nail involvement of the second digit after 5 months of treatment with thalidomide 50 mg 3 times weekly. November 2017, Index and small fingers with intact nail plates and minimal erythema with remarkable improvement in nail disease after increasing the dose of thalidomide to 50 mg 5 times weekly and using as-needed topical corticosteroids.
At the time of presentation, 0.1 cc of intralesional triamcinolone (5 mg/cc) was injected into the third, fourth, and fifth digits of the left hand. In place of hydroxychloroquine (200 mg twice daily), the patient was given chloroquine (250 mg daily) owing to its increased bioavailability.4 One month later, upon re-evaluation, little improvement was seen and systemic therapy was adjusted to include thalidomide (50 mg 3 times per week) in place of methotrexate (20 mg weekly). Thalidomide was chosen as it has been shown to be effective in recalcitrant discoid lupus that has failed other treatments.5
After 5 months of treatment with thalidomide (50 mg 3 times weekly), new nail involvement of the second digit developed. The thalidomide dose was subsequently increased and adjusted over the next year based on the patient’s tolerance. The only dose-limiting side effect of thalidomide for this patient was a mild tremor. Topical corticosteroids were prescribed for as-needed use, although the patient used them sparingly due to personal preference. Regarding the patient’s most recent visit in April 2023, her nail disease has markedly improved with intact nail plates and minimal erythema of the index and small fingers. She is currently stable and receiving thalidomide 50 mg 5 times weekly, with no noted adverse effects (Fig 1).
Discussion
DLE is the most common (73%-85%) and refractory (30%-40%) form of cutaneous lupus erythematosus.1,6 It typically presents as persistent scaly, disk-like plaques with a chronic course, as seen in this patient. Although 25% of cases of SLE present with nail disease, nail involvement in DLE is very rare and has only been reported in a handful of patients.2,3 It has been posited that nail dystrophy in DLE may indicate severe disease conditions demonstrated by increased capillaroscopic abnormalities and high damage indices, such as elevated endothelial cell activation markers and autoantibodies.2 This case was confirmed by biopsy as connective tissue disease, presumed to be DLE, although the differential of DLE-related nail dystrophy should include onychomycosis, psoriasis, lichen planus, Darier disease, and nail trauma.7
First-line therapies for DLE include antimalarial agents, topical steroids, and sun protection.6 However, refractory cases often require a combination of antimalarial and other immunosuppressant therapies. The few reported cases of DLE involving the nail required a combination of systemic corticosteroids, retinoids, and antimalarials to achieve nail improvement2,3 Although thalidomide is known to be an effective therapy for treating DLE, to our knowledge, this is the first report of the use of thalidomide to control DLE-related nail disease.6
Thalidomide has been shown to be effective against multiple chronic refractory inflammatory dermatologic conditions, including refractory DLE, with doses up to 400 mg/day.6,8 Its mechanism in DLE is thought to be due to cytokine inhibition, inhibition of macrophage activation, Treg response regulation, inhibition of angiogenesis, T-cell modulation, and promotion of NK-cell-mediated cytotoxicity.6 Side effects of high-dose thalidomide limit its use to refractory cases. However, low-doses at 50 mg every day or every other day have been shown to be sufficient to maintain the remission of DLE without adverse drug effects.6 As shown by our patient’s marked improvement, thalidomide may be particularly useful in the treatment of DLE-associated nail dystrophy.
Conflicts of interest
JFM is a consultant and/or investigator for Merck, Abbvie, Dermavant, Eli, Lilly, Novartis, Janssen, UCB, Celgene, Sanofi, Regeneron, Arena, Sun Pharma, Biogen, Pfizer, EMD Sorono, Avotres, and Leo Pharma.
Footnotes
Funding sources: None.
IRB approval status: Not applicable.
Patient consent: All patients gave consent for their photographs and medical information to be published in print and online and with the understanding that this information may be publicly available.
References
- 1.Durosaro O., Davis M.D.P., Reed K.B., et al. Incidence of cutaneous lupus erythematosus, 1965–2005: a population-based study. Arch Dermatol. 2009;145(3):249–253. doi: 10.1001/archdermatol.2009.21. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Navarro-Triviño F.J., Ruiz-Villaverde R. Chronic Discoid Lupus: An uncommon cause of nail atrophy. Sultan Qaboos Univ Med J. 2018;18(3):e411–e412. doi: 10.18295/squmj.2018.18.03.029. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Richert B., André J., Bourguignon R., De La Brassinne M. Hyperkeratotic nail discoid lupus erythematosus evolving towards systemic lupus erythematosus: therapeutic difficulties. J Eur Acad Dermatol Venereol. 2004;18(6):728–730. doi: 10.1111/j.1468-3083.2004.01068.x. [DOI] [PubMed] [Google Scholar]
- 4.Furst D.E. Pharmacokinetics of hydroxychloroquine and chloroquine during treatment of rheumatic diseases. Lupus. 1996;5(suppl 1):S11–S15. [PubMed] [Google Scholar]
- 5.Cortés-Hernández J., Torres-Salido M., Castro-Marrero J., et al. Thalidomide in the treatment of refractory cutaneous lupus erythematosus: prognostic factors of clinical outcome. Br J Dermatol. 2012;166(3):616–623. doi: 10.1111/j.1365-2133.2011.10693.x. [DOI] [PubMed] [Google Scholar]
- 6.Domingo S., Solé C., Moliné T., Ferrer B., Ordi-Ros J., Cortés-Hernández J. Efficacy of thalidomide in discoid lupus erythematosus: insights into the molecular mechanisms. Dermatology. 2020;236(5):467–476. doi: 10.1159/000508672. [DOI] [PubMed] [Google Scholar]
- 7.Tully A.S., Clinic C. Evaluation of Nail Abnormalities. Am Fam Physician. 2012;85(8):779–787. [PubMed] [Google Scholar]
- 8.Ordi-Ros J., Cortés F., Cucurull E., et al. Thalidomide in the treatment of cutaneous lupus refractory to conventional therapy. J Rheumatol. 2000;27(6):1429–1433. [PubMed] [Google Scholar]