Version Changes
Revised. Amendments from Version 3
In this new version, we have added details about sample size, but mainly generalizability. We have also included information about confounding variables not considered in the manuscript (unmeasured confounders), and selection and measurement bias. We have also added comments regarding the clinical impact of our findings as well as the public health impact.
Abstract
Background
The long-term impact of elevated blood pressure on mortality outcomes has been recently revisited due to proposed changes in cut-offs for hypertension. This study aimed at assessing the association between high blood pressure levels and 10-year mortality using the Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC-7) and the American College of Cardiology and the American Heart Association (ACC/AHA) 2017 blood pressure guidelines.
Methods
Data analysis of the PERU MIGRANT Study, a prospective ongoing cohort, was used. The outcome of interest was 10-year all-cause mortality, and exposures were blood pressure categories according to the JNC-7 and ACC/AHA 2017 guidelines. Log-rank test, Kaplan-Meier and Cox regression models were used to assess the associations of interest controlling for confounders. Hazard ratios (HR) and 95% confidence intervals (95% CI) were estimated.
Results
A total of 976 records, mean age of 60.4 (SD: 11.4), 513 (52.6%) women, were analyzed. Hypertension prevalence at baseline almost doubled from 16.0% (95% CI 13.7%–18.4%) to 31.3% (95% CI 28.4%–34.3%), using the JNC-7 and ACC/AHA 2017 definitions, respectively. Sixty-three (6.4%) participants died during the 10-year follow-up, equating to a mortality rate of 3.6 (95% CI 2.4–4.7) per 1000 person-years. Using JNC-7, and compared to those with normal blood pressure, those with pre-hypertension and hypertension had 2.1-fold and 5.1-fold increased risk of death, respectively. Similar mortality effect sizes were estimated using ACC/AHA 2017 for stage-1 and stage-2 hypertension.
Conclusions
Blood pressure levels under two different definitions increased the risk of 10-year all-cause mortality. Hypertension prevalence doubled using ACC/AHA 2017 compared to JNC-7. The choice of blood pressure cut-offs to classify hypertension categories need to be balanced against the patients benefit and the capacities of the health system to adequately handle a large proportion of new patients.
Keywords: Hypertension, pre-hypertension, blood pressure, mortality
Introduction
Ischemic heart disease and cerebrovascular disease are the first and second cause of death globally. 1 , 2 Hypertension, as a cardiovascular risk factor, was the cause of 9.4 million deaths and is closely related to ischemic heart and cerebrovascular disease. 3 Worldwide, the number of adults living with hypertension has increased from 563 million in 1975 to 1.13 billion in 2015, and the prevalence of hypertension in 2015 was estimated to be 24.1% and 20.1% in men and women, respectively. 4
Levels of blood pressure before the development of hypertension are known as pre-hypertension according to the Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (known as JNC-7), 5 and those with pre-hypertension are more likely to develop hypertension and its consequences. In 2017, as part of the ongoing review process of full guidelines commissioned in about 6-year cycles, the American College of Cardiology and the American Heart Association (ACC/AHA 2017) changed the proposed cut-off points used for defining hypertension, and for instance, included part of the pre-hypertension cases as hypertension (known as stage 1 hypertension). 6 The adoption of the ACC/AHA 2017 guidelines may produce changes in the proportion of cases with hypertension as reported for the US general population by the Systolic Blood Pressure Intervention Trial (SPRINT) Study, where the prevalence of hypertension almost doubled from 49.7% using JNC-7 to 80.1% by ACC/AHA 2017. 7 Similar changes in hypertension prevalence have been described in different countries. 8 – 13
Different reports associate arterial mean and blood pressure levels with all-cause mortality and cardiovascular mortality. 14 – 16 Whilst the association between blood pressure levels, defined by JNC-7, and mortality has been well described, 17 the evidence of the impact of the new definitions of hypertension on all-cause mortality in resource-constrained settings remains limited. 15 , 18 Therefore, long-term studies involving populations from low- and middle-income countries (LMICs) are needed given that raised blood pressure is a major contributor to the global burden of disease. 19
This study aimed at assessing whether the levels of blood pressure, using two different guidelines, JNC-7 and ACC/AHA 2017, are associated with 10-year mortality using an ongoing Peruvian cohort study.
Methods
Study design
Data analysis of the PERU MIGRANT Study, a prospective ongoing cohort conducted enrolling three different population groups: rural, rural-to-urban migrants, and urban dwellers was carried out. 20 The baseline of the study was conducted in 2007–2008 and follow-ups were carried out in 2012–2013, 2015–2016, and 2018. 21 For this analysis, data from the baseline assessment and 2018 follow-up were used.
Settings and participants
Las Pampas de San Juan de Miraflores, a highly urbanized area in the city of Lima, was selected as the urban environment, whereas San Jose de Secce, a district of Ayacucho in the highlands, was selected as the rural site. Individuals who were ≥30 years of age and habitual residents in the selected study sites were invited to participate at baseline. Rural dwellers were enrolled in San Jose de Secce, while urban residents and rural-to-urban migrants were recruited from Las Pampas de San Juan de Miraflores in Lima. 20 Pregnant women or potential participants unable to understand procedures and consent were excluded.
Participants were randomly selected using an age- (30–39, 40–49, 50–59, and 60+) and sex- stratified sampling approach, using the most up-to-date census in the study area. San Jose de Secce (Ayacucho) was the area chosen for the selection of rural dwellers. Migrants were those born in Ayacucho but living in Las Pampas de San Juan de Miraflores (Lima) at the time of the study enrolment. Finally, urban dwellers were those permanently living in the same area. 20
Power estimations were based on major risk factors in Huaraz (highlands) and Lima. The baseline study aimed at recruiting 1000 participants (200 in rural and urban groups, and 600 in the migrant group). Comparing Lima and highlands groups, the study had 84% power to detect a difference in the prevalence of hypertension (33% vs. 19.5%) enrolling 200 subjects in each group. Such power was 81% in the case of type 2 diabetes (7.6% versus 1.3%). 20
Definition of variables
Outcome The outcome of interest was the time until an event, defined as the time, in years, lapsed from the baseline assessment (2007–2008) to death or censorship during follow-up. Information about vital status and date of death (or censoring) was obtained via assessment of the National Record of Identification and Civil Status (RENIEC (Spanish acronym)) conducted in 2018.
Exposure The exposure variable was hypertension-related categories using measurements of systolic blood pressure (SBP) and diastolic blood pressure (DBP) under two different definitions, JNC-7 and ACC/AHA 2017. Under the JNC-7 definition, 5 individuals were split into three categories: normal (SBP < 120 mm Hg and DBP <80 mm Hg without using specific medication), pre-hypertension (SBP 120–139 mm Hg and DBP 80–89 mm Hg without anti-hypertensive therapy), and hypertension (SBP ≥ 140 mm Hg or DBP ≥ 90 mm Hg, or those reporting previous diagnosis done by a physician or current anti-hypertensive treatment). On the other hand, under the ACC/AHA 2017 definition, 6 participants were split into four categories: normal (same as those in JNC-7), elevated blood pressure (SBP 120–129 mm Hg and DBP < 80 mm Hg, without medication), stage 1 hypertension (SBP 130–139 mm Hg and DBP 80–89 mm Hg without treatment), and stage 2 hypertension (same as those with hypertension in the JNC-7).
Covariates Other variables included as potential confounders in the analysis were: age (30–39, 40–49, 50–59, and 60+ years), sex (men vs. women), education level (less than seven vs. more than seven years), socioeconomic status, defined by using an assets index and then split in tertiles (low, middle, high), and population group (rural, rural-to-urban migrant, and urban). In addition, behavioural variables were also included: daily smoking, self-reported, based on the consumption of at least one cigarette per day; alcohol use, defined according to the self-reported consumption of six or more beers (or equivalent) on the same occasion at least once a month (low vs. high); and physical activity level, based on the short version of the International Physical Activity Questionnaire (IPAQ) and split into low and moderate/high ( www.ipaq.ki.se). Finally, total cholesterol (< 200 mg/dL and ≥ 200 mg/dL) and type 2 diabetes, defined as fasting glucose ≥ 126 mg/dL or previous diagnosis made by a physician, were also included.
Procedures
Recruitment of participants was conducted by community health workers utilizing standardized tools. Questionnaires were based on the World Health Organization (WHO) STEPwise approach to surveillance (STEPs), validated in a pilot study and previously published. 20 Fieldworker’s training included application of informed consent and questionnaires, and the attainment of clinical measurements using appropriate and calibrated methods. Blood pressure was measured in seated position after a resting period of five minutes. Measures were done by triplicate using an automated device (OMRON HEM-780) and the average of the second and third measurements was used to define hypertension. Laboratory assessments were performed on venous samples taken in the morning after a minimum of eight hours (maximum 12 hours) of fasting. Total cholesterol was measured in serum, and fasting glucose was measured in plasma using a Cobas ® 6000 Modular Platform automated analyser and reagents supplied by Roche Diagnostics.
Statistical analysis
STATA 16 for Windows (Stata Corp, College Station TX, US; RRID:SCR_012763) was used for statistical analysis. An open-access alternative that can provide an equivalent function is the R stats package (R Project for Statistical Computing, RRID:SCR_001905). Sociodemographic, lifestyle behavioural and anthropometric variables were described according to each definition of blood pressure levels (JNC-7 and ACC/AHA 2017) using the Chi-squared test. Variables were also described according to vital status using the Log-rank test. A plot of the Kaplan-Meier estimator was used to evaluate the assumption of proportional hazards graphically, whereas such assessment was done in post-hoc analysis using the Schoenfeld residuals. Crude and adjusted Cox regression models were used to estimate the strength of the association between variables of interest (i.e., blood pressure and all-cause mortality), reporting hazard ratios (HR) and 95% confidence intervals (95% CI). Potential confounders were selected under epidemiological criteria, based on literature and available in the dataset. Since the selection of participant's sample was stratified by age (i.e., 30-39, 40-49, 50-59, 60+), such variable was included in that form in adjusted models. Using full-adjusted models, Akaike and Bayesian information criteria (AIC and BIC).
Ethics
The original PERU MIGRANT Study was approved by Institutional Review Boards (IRB) at Universidad Peruana Cayetano Heredia (approval codes: 51103, 60014 and 64094) in Peru and London School of Hygiene and Tropical Medicine (approval code: 5115) in the UK. Follow-up was approved by the IRB at the UPCH only. Written informed consent was given by study participants prior to starting research activities. Permission was obtained to use personal identifiers to link participant’s information with vital status records; and only deidentified and anonymized data was used for publication. 22 The protocol for this secondary data analysis was approved by the ethics committee at Universidad Peruana de Ciencias Aplicadas (approval code: PI178-17) in Lima, Peru.
Results
Characteristics of the study population at baseline
A total of 989 participants were enrolled at baseline, but 13 (1.3%) were excluded as no mortality information was available at the end of the study. Thus, only 976 were included in further analyses. Of them, 196 (20.1%) were rural, 582 (59.6%) migrants, and 198 (20.3%) were urban dwellers, have a mean age of 60.4 (SD: 11.4), and 513 (52.6%) were women.
Hypertension prevalence at baseline almost doubled from 16.0% (95% CI 13.7%–18.4%) to 31.3% (95% CI 28.4%–34.3%) using the JNC-7 and ACC/AHA 2017 guidelines, respectively. In both definitions, high blood pressure levels were more frequent among males, older subjects, migrant and urban dwellers, as well as those with obesity and those with type 2 diabetes mellitus ( Table 1 and Table 2).
Table 1. Characteristics of the study population by blood pressure levels according to the Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC-7).
| Blood pressure level | |||
|---|---|---|---|
| Normal | Pre-hypertension | Hypertension | |
| (n = 508) | (n = 312) | (n = 156) | |
| Sex | |||
| Men | 181 (35.6%) | 206 (66.0%) | 76 (48.7%) |
| Age | |||
| 30–39 years | 194 (38.2%) | 74 (23.7%) | 13 (8.3%) |
| 40–49 years | 158 (31.1%) | 90 (28.9%) | 30 (19.2%) |
| 50–59 years | 119 (23.4%) | 99 (31.7%) | 52 (33.4%) |
| 60+ years | 37 (7.3%) | 49 (15.7%) | 61 (39.1%) |
| Education level | |||
| <7 years | 237 (46.7%) | 148 (47.6%) | 86 (55.1%) |
| 7+ years | 270 (53.3%) | 163 (52.4%) | 70 (44.9%) |
| Socioeconomic status | |||
| Low | 226 (44.5%) | 134 (43.0%) | 64 (41.0%) |
| Middle | 113 (22.2%) | 79 (25.3%) | 45 (28.9%) |
| High | 169 (33.3%) | 99 (31.7%) | 47 (30.1%) |
| Population group | |||
| Rural | 105 (20.7%) | 68 (21.8%) | 23 (14.7%) |
| Rural-to-urban migrant | 316 (62.2%) | 192 (61.5%) | 74 (47.4%) |
| Urban | 87 (17.1%) | 52 (16.7%) | 59 (37.8%) |
| Daily smoking | |||
| Yes | 14 (2.8%) | 9 (2.9%) | 10 (6.4%) |
| Alcohol use | |||
| High consumption | 38 (7.5%) | 33 (10.6%) | 15 (9.6%) |
| Physical activity | |||
| Low levels | 132 (26.2%) | 72 (23.2%) | 48 (31.2%) |
| Obesity | |||
| BMI ≥ 30 kg/m 2 | 90 (17.7%) | 57 (18.3%) | 49 (31.4%) |
| Total cholesterol | |||
| ≥200 mg/dL | 124 (24.4%) | 117 (37.6%) | 63 (40.4%) |
| Type 2 diabetes | |||
| Yes | 11 (2.2%) | 15 (4.8%) | 13 (8.4%) |
Table 2. Characteristics of the study population by blood pressure levels according to the American College of Cardiology and the American Heart Association (ACC/AHA) 2017.
| Blood pressure level | ||||
|---|---|---|---|---|
| Normal | Elevated | Stage 1 hypertension | Stage 2 hypertension | |
| (n = 508) | (n = 163) | (n = 149) | (n = 156) | |
| Sex | ||||
| Men | 181 (35.6%) | 104 (63.8%) | 102 (68.4%) | 76 (48.7%) |
| Age | ||||
| 30–39 years | 194 (38.2%) | 41 (25.1%) | 33 (22.1%) | 13 (8.3%) |
| 40–49 years | 158 (31.1%) | 39 (23.9%) | 51 (34.2%) | 30 (19.2%) |
| 50–59 years | 119 (23.4%) | 56 (34.4%) | 43 (28.9%) | 52 (33.4%) |
| 60+ years | 37 (7.3%) | 27 (16.6%) | 22 (14.8%) | 61 (39.1%) |
| Education level | ||||
| <7 years | 237 (46.7%) | 80 (49.4%) | 68 (45.6%) | 86 (55.1%) |
| 7+ years | 270 (53.3%) | 82 (50.6%) | 81 (54.4%) | 70 (44.9%) |
| Socioeconomic status | ||||
| Low | 226 (44.5%) | 73 (44.8%) | 61 (41.0%) | 64 (41.0%) |
| Middle | 113 (22.2%) | 35 (21.5%) | 44 (29.5%) | 45 (28.9%) |
| High | 169 (33.3%) | 55 (33.7%) | 44 (29.5%) | 47 (30.1%) |
| Population group | ||||
| Rural | 105 (20.7%) | 37 (22.7%) | 31 (20.8%) | 23 (14.7%) |
| Rural-to-urban migrant | 316 (62.2%) | 104 (63.8%) | 88 (59.1%) | 74 (47.4%) |
| Urban | 87 (17.1%) | 22 (13.5%) | 30 (20.1%) | 59 (37.8%) |
| Daily smoking | ||||
| Yes | 14 (2.8%) | 3 (1.8%) | 6 (4.1%) | 10 (6.4%) |
| Alcohol use | ||||
| High consumption | 38 (7.5%) | 18 (11.0%) | 15 (10.1%) | 15 (9.6%) |
| Physical activity | ||||
| Low levels | 132 (26.2%) | 39 (24.2%) | 33 (22.2%) | 48 (31.2%) |
| Obesity | ||||
| BMI ≥ 30 kg/m 2 | 90 (17.7%) | 31 (19.0%) | 26 (17.5%) | 49 (31.4%) |
| Total cholesterol | ||||
| ≥200 mg/dL | 124 (24.4%) | 61 (37.7%) | 56 (37.6%) | 63 (40.4%) |
| Type 2 diabetes | ||||
| Yes | 11 (2.2%) | 5 (3.1%) | 10 (6.7%) | 13 (8.4%) |
Mortality and associated factors
A total of 63 (6.4%) participants died during the 10-year follow-up with 9992.6 person-years of follow-up and a mortality rate of 3.6 (95% CI 2.4–4.7) per 1000 person-years. Men, older individuals, those with lower education, those with lower socioeconomic status, and having type 2 diabetes mellitus had an increased risk of 10-year mortality ( Table 3).
Table 3. Characteristics of the study population by vital status.
| Vital status | ||
|---|---|---|
| Alive (n = 913) | Dead (n = 63) | |
| Sex | ||
| Women | 491 (95.7%) | 22 (4.3%) |
| Men | 422 (91.1%) | 41 (8.9%) |
| Age | ||
| 30–39 years | 279 (99.3%) | 2 (0.7%) |
| 40–49 years | 272 (97.8%) | 6 (2.2%) |
| 50–59 years | 254 (94.1%) | 16 (5.9%) |
| 60+ years | 108 (74.5%) | 39 (26.5%) |
| Education level | ||
| <7 years | 428 (90.9%) | 43 (9.1%) |
| 7+ years | 483 (96.0%) | 20 (4.0%) |
| Socioeconomic status | ||
| Low | 386 (91.0%) | 38 (9.0%) |
| Middle | 229 (96.6%) | 8 (3.4%) |
| High | 298 (94.6%) | 17 (5.4%) |
| Population group | ||
| Rural | 178 (90.8%) | 18 (9.2%) |
| Rural-to-urban migrant | 550 (94.5%) | 32 (5.5%) |
| Urban | 185 (93.4%) | 13 (6.6%) |
| Daily smoking | ||
| No | 880 (93.5%) | 61 (6.5%) |
| Yes | 31 (93.9%) | 2 (6.1%) |
| Alcohol use | ||
| Low consumption | 834 (93.7%) | 56 (6.3%) |
| High consumption | 79 (91.9%) | 7 (8.1%) |
| Physical activity | ||
| High/moderate levels | 667 (93.2%) | 49 (6.8%) |
| Low levels | 239 (94.8%) | 13 (5.2%) |
| Obesity | ||
| BMI < 30 kg/m 2 | 727 (93.2%) | 53 (6.8%) |
| BMI ≥ 30 kg/m 2 | 186 (94.9%) | 10 (5.1%) |
| Total cholesterol | ||
| <200 mg/dL | 623 (92.9%) | 48 (7.1%) |
| ≥200 mg/dL | 290 (95.4%) | 14 (4.6%) |
| Type 2 diabetes | ||
| No | 879 (93.9%) | 57 (6.1%) |
| Yes | 33 (84.6%) | 6 (15.4%) |
Blood pressure levels and 10-year mortality
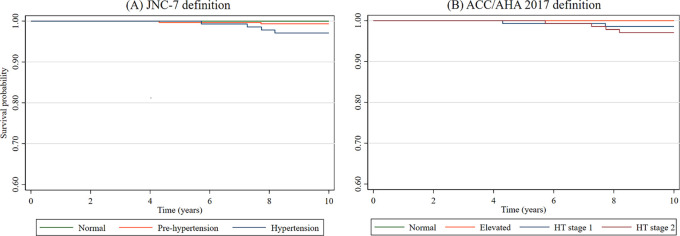
Kaplan-Meier plots were created using the exposures of interest ( Figure 1). There was evidence of an association between hypertension-related categories and all-cause mortality ( Table 4). Using the JNC-7 guideline and compared to those with normal blood pressure, those with pre-hypertension and hypertension had 2-fold and 3.4-fold increased hazard of death, respectively. On the other hand, using the ACC/AHA 2017 definition and compared to those with normal blood pressure, stage 1 and stage 2 hypertension were associated with a 2.5- and 3.5-fold increase in the hazard of mortality. There was no evidence of an association between the ACC/AHA 2017’s elevated blood pressure category and mortality.
Figure 1. Kaplan-Meier function using (A) JNC-7 and (B) ACC/AHA definitions.
HT = Hypertension.
Table 4. Association between blood pressure levels by Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC-7) and American College of Cardiology and the American Heart Association (ACC/AHA) 2017 definition and 10-year mortality: crude and adjusted Cox models.
| Blood pressure definition | Vital status | ||||
|---|---|---|---|---|---|
| Alive | Dead | Crude model | Adjusted model 1 * | Adjusted model 2 ** | |
| (n = 913) | (n = 63) | HR (95% CI) | HR (95% CI) | HR (95% CI) | |
| JNC-7 | |||||
| Normal | 497 (97.8%) | 11 (2.2%) | 1 (Reference) | 1 (Reference) | 1 (Reference) |
| Pre-hypertension | 289 (92.6%) | 23 (7.4%) | 3.50 (1.71–7.19) | 2.04 (1.02–4.25) | 2.00 (1.01–4.18) |
| Hypertension | 127 (81.4%) | 29 (18.6%) | 9.4 (4.71–18.89) | 3.52 (1.68–7.36) | 3.45 (1.62–7.33) |
| ACC/AHA 2017 | |||||
| Normal | 497 (97.8%) | 11 (2.2%) | 1 (Reference) | 1 (Reference) | 1 (Reference) |
| Elevated blood pressure | 153 (93.9%) | 10 (6.1%) | 2.87 (1.21–6.75) | 1.64 (0.69–3.91) | 1.55 (0.63–3.81) |
| Stage 1 hypertension | 136 (91.3%) | 13 (8.7%) | 4.22 (1.89–9.42) | 2.54 (1.11–5.84) | 2.47 (1.07–5.74) |
| Stage 2 hypertension | 127 (81.4%) | 29 (18.6%) | 9.44 (4.71–18.89) | 3.55 (1.69–7.42) | 3.48 (1.64–7.39) |
Bold estimates are significant at p < 0.05 level.
Adjusted model 1 was controlled by age, sex, population group, education level, and socioeconomic status.
Adjusted model 2 was controlled by age, sex, population group, education level, socioeconomic status, daily smoking, alcohol use, physical activity, obesity status, total cholesterol, and type 2 diabetes mellitus.
When comparing adjusted models, AIC and BIC were very similar (AIC was 741.3 for JNC-7 vs. 742.2 for ACC/AHA 2017, whereas BIC was 824.1 for JNC-7 vs. 829.9 for ACC/AHA 2017), highlighting no difference between models.
Discussion
Main findings
According to our findings, high blood pressure levels increased the risk of 10-year all-cause mortality, and our estimates showed similar long-term effect sizes across blood pressure categories using two different guidelines. As countries move into better universal health coverage, primary prevention and access to medications should be secured to reduce the health burden of raised blood pressure. However, how countries prepare and secure resources to successfully meet the challenges of hypertension will depend on how this is defined. There was a remarkable difference on hypertension prevalence depending on whether the JNC-7 or the ACC/AHA 2017 definition was followed, but the latter definition would avoid approximately 20% more deaths than the JNC-7 guideline. This carries relevant implications and repercussions for patients and health systems. Should the ACC/AHA 2017 definition be adopted because this will require securing treatment for a substantial larger population with the costs and challenges it entails.
Comparison with previous studies
In the US, the SPRINT Study, conducted in 2010, reported that the ACC/AHA 2017 definition significantly increased the prevalence of patients with hypertension and identified more patients who will experience adverse cardiovascular events. 7 However, it can be argued that information came from a clinical trial, which may have included more high-risk patients than in the general population; also, participants in the SPRINT Study were followed-up for 3.3 years. Conversely, we conducted a population-based 10-year follow-up study, advancing the evidence for the general population.
Because of data availability, we could not assess cardiovascular mortality; nonetheless, it is likely that we would have seen a similar – or even larger – effect as the one herein reported for all-cause mortality. In a pooled analysis of prospective cohorts conducted in China, starting from 1996 to 2010, 15 the ACC/AHA 2017 stage 1 hypertension was associated with an increased risk of cardiovascular disease mortality; notably, another cohort study with participants recruited from 1997 to 1999, and with 20 years of follow-up, did not find such association in rural dwellers in the same country. 18 The difference could be explained by different risk factor profiles in rural areas, or presumably lower levels of risk factors over twenty years ago. Using the National Health and Nutrition Examination Surveys between 2003 and 2014, a study found that the ACC/AHA 2017 guidelines would increase the proportion of stroke survivors in the US compared to the JNC-7 definition. 23 Thus, there is a potential benefit of applying the ACC/AHA 2017 guidelines, although this needs to be verified in different population groups.
Public health relevance
The ACC/AHA 2017 guidelines radically proposed to change definitions of blood pressure levels, with pre-hypertension split into two categories: elevated blood pressure and stage 1 hypertension. Multiple authors have questioned this change, and pinpointed that hypertension prevalence would increase, pharmacotherapy of hypertension will start at a lower blood pressure level, and the threshold for hypertension control will decrease. 10 , 24 Thus, cases of stage 1 hypertension, previously classified as pre-hypertension in JNC-7, will start treatment with an initial anti-hypertensive drug if estimated 10-year cardiovascular risk is ≥ 10%, 6 but CV risk scores have showed poor concordance in Latin America populations 25 ; whereas those in stage 2 hypertension would start with two anti-hypertensive drugs. 26 – 28 In support of these concerns, a study showed that hypertension prevalence would increase by 40% in the US. 10 Similarly in Peru, using information from a population-based survey, the prevalence of hypertension would increase from 14% to 32%. 12 Peru is a middle-income country with a fragile and fragmented healthcare system, with poor response to the challenges of chronic conditions. Increasing the number of people with hypertension may benefit those with blood pressure levels in the range 130–139/80–89 mm Hg, but would represent a major investment (i.e., human resources, budget and time) so that these patients can receive adequate treatment, management, and follow-up. Treatment must be guaranteed for hypertension (using JNC-7) and stage 2 hypertension (ACC/AHA 2017) to reduce mortality risk. If this effect can be seen in pre-hypertension (JNC-7) and stage 1 hypertension (ACC/AHA 2017) should be further assessed. Thus, a thoroughly planned and balanced policy would be needed to provide care to those who most needed it. From the clinical perspective, a tailored follow-up of those individuals with pre-hypertension (or stage 1 hypertension) may be required to decide appropriate treatment, even high-risk stratification may be considered. In addition to that, a combination of population-wide interventions may be also needed. 29
As the risk of coronary artery disease and stroke rise progressively increases as blood pressure increases above 115/75 mm Hg, 30 the beginning of antihypertensive therapy will certainly have advantages, especially the reduction of patient’s complications and mortality. 31 However, there will be an increase of primary care costs, which can be more deleterious in resource-constrained settings. A recent study conducted in the US has estimated that reaching the goals of the ACC/AHA 2017 guidelines will reduce 610,000 cardiovascular events and avoid 334,000 total deaths per year among adults 40 years and older. 32 Nevertheless, the potential increase of adverse events related to the use of anti-hypertensive drugs should be also considered 33 as well as a substantial number of hypertension cases giving up or taking medication irregularly. Thus, although the adoption of ACC/AHA 2017 guidelines may seem pertinent in term of complications and mortality reduction, Peru as well as other low- and middle-income countries, may not be prepared for this scenario.
Strengths and limitations
This study takes advantage of an ongoing population-based cohort study conducted in a resource-constrained setting with three different population groups to evaluate the impact of two definitions of high blood pressure levels and 10-year mortality. However, this study has some limitations that should be highlighted. First, due to data availability, this study analysed all-cause mortality as outcome instead of assessing cardiovascular mortality. Since blood pressure increases the risk of cardiovascular events and mortality, we can speculate that the association of interest will be stronger and probably did not vary between hypertension definitions as in our analysis. Second, some variables, relevant to understand the relationship between hypertension and all-cause mortality, were not available (e.g., diet patterns, salt consumption, among others). Third, although left truncation can be present as subjects <30 years were excluded, the potential effect of such limitation may be negligible as the prevalence of hypertension is low in that age group. Fourth, selection bias can be an issue as studied population groups were selected in specific sites and may not be totally representative of the general population. In addition, measurement bias may be present. However, standard procedures were used to assess blood pressure levels. Finally, we did not assess the potential effect of anti-hypertensive drugs on mortality due to limited sample size.
Conclusions
Blood pressures levels under two different definitions increased the risk of 10-year all-cause mortality. Hypertension prevalence doubled using the ACC/AHA 2017 compared to the JNC-7 definition. The choice of blood pressure cut-offs to classify hypertension categories need to be balanced against the patient’s benefit and the capacities of the health system to adequately handle a large proportion of new patients. Cardiovascular disease prevention, and, in particular, the prevention of blood pressure-related mortality, will benefit from the estimates reported in this study to adequately inform local decision making, which in addition to disease burden should recognize balance benefits and risks within existing capacities to secure and guarantee adequate and effective treatment for all the new patients with raised blood pressure.
Data availability
Underlying data
Figshare: Underlying data for ‘Blood pressure and 10-year all-cause mortality: Findings from the PERU MIGRANT Study’, ‘PERU MIGRANT Study’, https://doi.org/10.6084/m9.figshare.16811350.v3. 22
This project includes the following underlying data:
-
-
PERU MIGRANT Dataset (mortality).csv
-
-
Dictionary.txt
Data are available under the terms of the Creative Commons Attribution 4.0 International license (CC-BY 4.0).
Author contributions
Aida Hidalgo-Benites: conceptualization, data curation, formal analysis, investigation, methodology, writing original draft, and writing review and editing.
Valeria Senosain-Leon: conceptualization, data curation, formal analysis, investigation, methodology, writing original draft, and writing review and editing.
Rodrigo M. Carrillo-Larco: data curation, formal analysis, investigation, methodology, validation, and writing review and editing.
Andrea Ruiz-Alejos: data curation, formal analysis, funding acquisition, investigation, methodology, and writing review and editing.
Robert H. Gilman: funding acquisition, investigation, methodology, supervision, validation, and writing review and editing.
Liam Smeeth: funding acquisition, investigation, methodology, supervision, validation, and writing review and editing.
J. Jaime Miranda: conceptualization, funding acquisition, investigation, methodology, supervision, validation, and writing review and editing.
Antonio Bernabe-Ortiz: conceptualization, data curation, formal analysis, funding acquisition, investigation, methodology, supervision, and writing review and editing.
Funding Statement
RMC-L is supported by a Wellcome Trust International Training Fellowship, London, UK (214185/Z/18/Z). AB-O (103994/Z/14/Z) and JJM (074833/Z/04/Z, 20517/Z/16/Z) were supported by the Wellcome Trust, London, UK.
The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
[version 4; peer review: 2 approved]
References
- 1. GBD 2015 DALUs and HALE Collaborators: Global, regional, and national disability-adjusted life-years (DALYs) for 315 diseases and injuries and healthy life expectancy (HALE), 1990-2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet. 2016;388(10053):1603–1658. 10.1016/S0140-6736(16)31460-X [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2. World Health Organization: Global Status Report on Noncommunicable Diseases 2014. Geneva, Switzerland: WHO;2014. [Google Scholar]
- 3. Lim SS, Vos T, Flaxman AD, et al. : A comparative risk assessment of burden of disease and injury attributable to 67 risk factors and risk factor clusters in 21 regions, 1990–2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet. 2012;380(9859):2224–2260. 10.1016/S0140-6736(12)61766-8 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4. NCD Risk Factor Collaboration (NCD-RisC): Worldwide trends in blood pressure from 1975 to 2015: a pooled analysis of 1479 population-based measurement studies with 19.1 million participants. Lancet. 2017;389(10064):37–55. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5. Chobanian AV, Bakris GL, Black HR, et al. : Seventh report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. Hypertension. 2003;42(6):1206–1252. 10.1161/01.HYP.0000107251.49515.c2 [DOI] [PubMed] [Google Scholar]
- 6. Whelton PK, Carey RM, Aronow WS, et al. : 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults: Executive Summary: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation. 2018;138(17):e426–e483. 10.1161/CIR.0000000000000597 [DOI] [PubMed] [Google Scholar]
- 7. Vaduganathan M, Pareek M, Qamar A, et al. : Baseline Blood Pressure, the 2017 ACC/AHA High Blood Pressure Guidelines, and Long-Term Cardiovascular Risk in SPRINT. Am. J. Med. 2018;131(8):956–960. 10.1016/j.amjmed.2017.12.049 [DOI] [PubMed] [Google Scholar]
- 8. Aronow WS: Implications of the new 2017 American College of Cardiology/American Aeart Association Guidelines for Hypertension. Minerva Cardioangiol. 2019;67(5):399–410. 10.23736/S0026-4725.19.04965-X [DOI] [PubMed] [Google Scholar]
- 9. Asgari S, Khaloo P, Khalili D, et al. : Status of Hypertension in Tehran: Potential impact of the ACC/AHA 2017 and JNC7 Guidelines, 2012–2015. Sci. Rep. 2019;9(1):6382. 10.1038/s41598-019-42809-3 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10. Muntner P, Carey RM, Gidding S, et al. : Potential US Population Impact of the 2017 ACC/AHA High Blood Pressure Guideline. Circulation. 2018;137(2):109–118. 10.1161/CIRCULATIONAHA.117.032582 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11. Nakagawa N, Hasebe N: Impact of the 2017 American College of Cardiology/American Heart Association Blood Pressure Guidelines on the Next Blood Pressure Guidelines in Asia. Curr. Hypertens. Rep. 2019;21(1):2. 10.1007/s11906-019-0906-2 [DOI] [PubMed] [Google Scholar]
- 12. Hernandez-Vasquez A, Rojas-Roque C, Santero M, et al. : Changes in the prevalence of hypertension in Peru using the new guideline of the American College of Cardiology. Rev. Med. Chil. 2019;147(5):545–556. 10.4067/S0034-98872019000500545 [DOI] [PubMed] [Google Scholar]
- 13. Hernández-Vásquez A, Santero M: New 2017 ACC/AHA hypertension guideline: Implications for a Latin American country like Peru. Eur. J. Prev. Cardiol. 2019;26(6):668–670. 10.1177/2047487318799489 [DOI] [PubMed] [Google Scholar]
- 14. Mosley WJ, 2nd, Greenland P, Garside DB, et al. : Predictive utility of pulse pressure and other blood pressure measures for cardiovascular outcomes. Hypertension. 2007;49(6):1256–1264. 10.1161/HYPERTENSIONAHA.106.083592 [DOI] [PubMed] [Google Scholar]
- 15. Liu N, Yang JJ, Meng R, et al. : Associations of blood pressure categories defined by 2017 ACC/AHA guidelines with mortality in China: Pooled results from three prospective cohorts. Eur. J. Prev. Cardiol. 2020;27(4):345–354. 10.1177/2047487319862066 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16. Zhao L, Song Y, Dong P, et al. : Brachial pulse pressure and cardiovascular or all-cause mortality in the general population: a meta-analysis of prospective observational studies. J. Clin. Hypertens. (Greenwich). 2014;16(9):678–685. 10.1111/jch.12375 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17. Bundy JD, Li C, Stuchlik P, et al. : Systolic Blood Pressure Reduction and Risk of Cardiovascular Disease and Mortality: A Systematic Review and Network Meta-analysis. JAMA Cardiol. 2017;2(7):775–781. 10.1001/jamacardio.2017.1421 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18. Wang M, Wu T, Yu C, et al. : Association between blood pressure levels and cardiovascular deaths: a 20-year follow-up study in rural China. BMJ Open. 2020;10(2):e035190. 10.1136/bmjopen-2019-035190 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19. NCD Risk Factor Collaboration (NCD-RisC) - Americas Working Group: Trends in cardiometabolic risk factors in the Americas between 1980 and 2014: a pooled analysis of population-based surveys. Lancet Glob. Health. 2020;8(1):e123–e133. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20. Miranda JJ, Gilman RH, Garcia HH, et al. : The effect on cardiovascular risk factors of migration from rural to urban areas in Peru: PERU MIGRANT Study. BMC Cardiovasc. Disord. 2009;9:23. 10.1186/1471-2261-9-23 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21. Carrillo-Larco RM, Ruiz-Alejos A, Bernabe-Ortiz A, et al. : Cohort Profile: The PERU MIGRANT Study-A prospective cohort study of rural dwellers, urban dwellers and rural-to-urban migrants in Peru. Int. J. Epidemiol. 2017;46(6):1752-f. 10.1093/ije/dyx116 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22. Miranda JJ, Bernabe-Ortiz A, Carrillo-Larco RM: PERU MIGRANT Study. Figshare. Dataset. 2021. 10.6084/m9.figshare.16811350.v3 [DOI]
- 23. Lekoubou A, Bishu KG, Ovbiagele B: Nationwide Impact of the 2017 American College of Cardiology/American Heart Association Blood Pressure Guidelines on Stroke Survivors. J. Am. Heart Assoc. 2018;7(12). 10.1161/JAHA.118.008548 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24. Wang TD: Our Stance towards the 2017 ACC/AHA High Blood Pressure Clinical Practice Guideline: Has the Pendulum Swung Too Far?. Acta Cardiol. Sin. 2018;34(1):1–3. 10.6515/ACS.201801_34(1).20171218A [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25. Bazo-Alvarez JC, Quispe R, Peralta F, et al. : Agreement Between Cardiovascular Disease Risk Scores in Resource-Limited Settings: Evidence from 5 Peruvian Sites. Crit. Pathw. Cardiol. 2015;14(2):74–80. 10.1097/HPC.0000000000000045 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26. Blonsky R, Pohl M, Nally JV, et al. : 2017 ACC/AHA hypertension guidelines: Toward tighter control. Cleve. Clin. J. Med. 2018;85(10):771–778. 10.3949/ccjm.85a.18028 [DOI] [PubMed] [Google Scholar]
- 27. Brook RD, Rajagopalan S: 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults. A report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J. Am. Soc. Hypertens. 2018;12(3):238. 10.1016/j.jash.2018.01.004 [DOI] [PubMed] [Google Scholar]
- 28. Colantonio LD, Booth JN, 3rd, Bress AP, et al. : 2017 ACC/AHA Blood Pressure Treatment Guideline Recommendations and Cardiovascular Risk. J. Am. Coll. Cardiol. 2018;72(11):1187–1197. 10.1016/j.jacc.2018.05.074 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29. Bernabe-Ortiz A, Sal y Rosas VG, Ponce-Lucero V, et al. : Effect of salt substitution on community-wide blood pressure and hypertension incidence. Nat. Med. 2020;26(3):374–378. 10.1038/s41591-020-0754-2 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30. James PA, Oparil S, Carter BL, et al. : 2014 evidence-based guideline for the management of high blood pressure in adults: report from the panel members appointed to the Eighth Joint National Committee (JNC 8). JAMA. 2014;311(5):507–520. 10.1001/jama.2013.284427 [DOI] [PubMed] [Google Scholar]
- 31. Jaeger BC, Anstey DE, Bress AP, et al. : Cardiovascular Disease and Mortality in Adults Aged >/=60 Years According to Recommendations by the American College of Cardiology/American Heart Association and American College of Physicians/American Academy of Family Physicians. Hypertension. 2019;73(2):327–334. 10.1161/HYPERTENSIONAHA.118.12291 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32. Bundy JD, Mills KT, Chen J, et al. : Estimating the Association of the 2017 and 2014 Hypertension Guidelines With Cardiovascular Events and Deaths in US Adults: An Analysis of National DataAssociation of the 2014 and 2017 Hypertension Guidelines With Cardiovascular Events and Deaths in US AdultsAssociation of the 2014 and 2017 Hypertension Guidelines With Cardiovascular Events and Deaths in US Adults. JAMA Cardiol. 2018;3(7):572–581. 10.1001/jamacardio.2018.1240 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33. Olowofela AO, Isah AO: A profile of adverse effects of antihypertensive medicines in a tertiary care clinic in Nigeria. Ann. Afr. Med. 2017;16(3):114–119. 10.4103/aam.aam_6_17 [DOI] [PMC free article] [PubMed] [Google Scholar]