Abstract
Benign lymphoepithelial cyst (BLEC) of the salivary gland is a gradually increasing cystic lesion commonly associated with human immunodeficiency virus (HIV) infection. In rare instances, it can be seen in immunocompetent patients. Here, such a classic case of BLEC of the parotid gland in an elderly seronegative patient has been reported. Proper medical history, physical examination, radiology, and fine needle aspiration can fetch a preoperative diagnosis. However, histopathology helps to rule out other possibilities. Surgical excision is the best treatment modality with lower chances of recurrences.
Keywords: Benign, cyst, cytology, parotid
CASE REPORT
A 62-year-old hypertensive male presented with a gradually progressing left-sided preauricular swelling for 3 months. There was no associated pain, local rise of temperature, or any changes in the overlying skin. On examination, a firm, nontender, and compressible swelling was identified at the left parotid region measuring 4 cm × 2.5 cm, which was fixed to the underlying structure. The contract-enhanced computed tomography (CECT) scan revealed a cystic lesion in the superficial lobe of the left parotid gland without any solid area or associated cervical lymphadenopathy. The right parotid gland was normal [Figure 1a]. The baseline investigations including complete hemogram, liver function test, kidney function test, and blood sugar levels were within normal limit. The patient was nonreactive to human immunodeficiency virus (HIV), hepatitis B, and hepatitis C tests. Fine needle aspiration cytology (FNAC) yielded only straw-colored fluid, which on cytology showed singly scattered lymphoid cells along with occasional neutrophils and cystic macrophages in a proteinaceous background [Figure 1b and 1c]. No salivary gland component was identified. A provisional cytological diagnosis of a benign cystic lesion was made. The superficial parotidectomy was performed. The gross specimen showed a cystic lesion measuring 2.5 cm in diameter, filled with thick brownish mucoid material [Figure 2a]. On microscopy, cystic lesion was lined by attenuated squamous epithelium beneath which a thick band of lymphocytic aggregates along with occasional germinal center formations was noted. Cyst lumen contained keratin debris and cholesterol clefts. Adjacent areas of normal salivary parenchyma were also seen [Figure 2b-d]. In collaboration with clinical history, radiology, cytology, and histopathology findings, a final diagnosis of benign lymphoepithelial cyst (BLEC) was reported. No recurrences or complications were reported in the follow-up visit of one year.
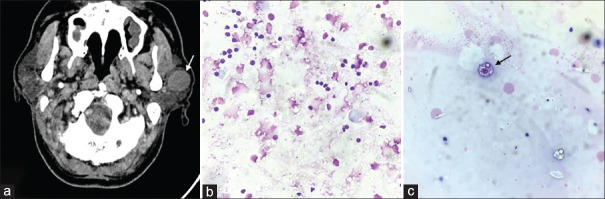
Figure 1.
(a) CECT scan showing cystic lesion in superficial lobe of left parotid, (b) and (c) Cytology smears show lymphoid cells along with occasional cystic macrophages (Giemsa, 400x)
Figure 2.
(a) Cut surface showing a cystic lesion filled with mucoid brownish material, (b) and (c) Microscopy showing cyst wall containing dense lymphoid tissue underneath the squamous epithelium with the focal germinal center formation in (d) (Hematoxylin and Eosin, 400x)
DISCUSSION
BLEC of salivary gland is a rare, slow-growing lesion that predominantly involves the parotid gland. It can be unilateral or bilateral and uniloculated or multiloculated. BLEC is typically present as a clinical symptom in immunocompromised adults, ideally those who are HIV infected. Nonetheless, HIV-negative people can also be involved infrequently. Clinically, BLEC manifests as a gradual, painless swelling, which may grow into a large mass, causing cosmetic disfiguration.[1]
The pathogenesis remains unknown; however, a few theories are hypothesized in HIV-infected patients. The first theory is HIV-induced lymphoproliferation of intraparotid lymph nodes entrapped during embryogenesis. In this process, epithelial remnants in lymphoid tissue undergo cystic enlargement. The second theory is obstructive etiology, in which HIV-infected cells migrate into the parotid and induce lymphoid hyperplasia and salivary ductal metaplasia. Eventually, cystic lesion develops due to ductal obstruction. The cyst content has higher concentrations of HIV-1 p24 antigen and RNA copies.[2] In immunocompetent patients, similar lymphoproliferation pathogenesis due to other viral infections or lymphatic obstruction due to any chronic inflammation has been postulated.[3]
Radiology, FNAC, and histopathology are mandatory for proper diagnosis and management. Imaging studies characteristically detect intraparotid thin-walled cysts with or without cervical lymphadenopathy. The extent of the lesion can also be assessed through radiology.[2] On cytology, BLEC characteristically shows polymorphous population of lymphoid cells, cystic macrophages, and epithelial cells in a proteinaceous background. However, there are several differential diagnosis of parotid gland cystic lesions on cytology, as depicted on a flow chart [Figure 3].[4]
Figure 3.

Flow chart illustrating cystic lesions of parotid and their characteristic cytological features (Abbreviations: ACC-Acinic cell carcinoma; BLEC-Benign lymphoepithelial cyst; LGMEC-Low grade mucoepidermoid carcinoma; PA-Pleomorphic adenoma; PDP-Polycystic disease of parotid; SC-Secretory carcinoma; SCC-Squamous cell carcinoma; WT-Warthin tumor)
Histopathology is always confirmatory by revealing epithelial cysts lined by squamous, columnar, cuboidal, or mucin-secreting epithelium and abundant lymphoid tissue with germinal center formations underneath. BLEC can neither recur nor metastasize; hence, a definite histological diagnosis aids in the exclusion of malignant lesions, especially low-grade mucoepidermoid carcinoma and metastatic squamous cell carcinoma.[1,4]
The gold standard treatment is superficial parotidectomy. Enucleation of the cyst may be associated with recurrences. Other conservative treatment modalities including repeat aspiration, sclerotherapy, radiotherapy, and highly active antiretroviral therapy are reserved for immunocompromised patients. Close follow-up is advised in immunocompromised patients for rare incidences of recurrences.[3,5]
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
REFERENCES
- 1.Joshi J, Shah S, Agarwal D, Khasgiwal A. Benign lymphoepithelial cyst of parotid gland: Review and case report. J Oral Maxillofac Pathol. 2018;22(Suppl 1):S91–7. doi: 10.4103/jomfp.JOMFP_252_17. doi:10.4103/jomfp. JOMFP_252_17. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Sekikawa Y, Hongo I. HIV-associated benign lymphoepithelial cysts of the parotid glands confirmed by HIV-1 p24 antigen immunostaining. BMJ Case Rep. 2017;2017:bcr2017221869. doi: 10.1136/bcr-2017-221869. doi:10.1136/bcr-2017-221869. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Thong HK, Athar PPSH, Mustaffa WMW. Benign lymphoepithelial cyst: An unusual cause of parotid swelling in two immunocompetent patients. Open Access Maced J Med Sci. 2019;7:2142–5. doi: 10.3889/oamjms.2019.577. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Pantanowitz L, Thompson LDR, Rossi ED. Diagnostic approach to fine needle aspirations of cystic lesions of the salivary gland. Head Neck Pathol. 2018;12:548–61. doi: 10.1007/s12105-018-0904-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Wu G, Yousaf A, Kessler E, Seitelman E, Datta R. Recurrent lymphoepithelial cysts after parotidectomy in an undiagnosed HIV-positive patient. J Surg Case Rep. 2020;2020:rjaa300. doi: 10.1093/jscr/rjaa300. doi:10.1093/jscr/rjaa300. [DOI] [PMC free article] [PubMed] [Google Scholar]