Highlights
-
•
Testing rates were not commensurate with infection rates across race/ethnicity.
-
•
Wait times at testing sites are the most frequently reported barrier to testing.
-
•
Racial/ethnic minorities and low income persons experience more barriers to testing.
-
•
Restrictions on time off work while awaiting test results may effect disparities.
-
•
Structural barriers contribute to disparities in testing and infection rates.
Keywords: COVID-19, Testing, Access, Health disparity, Racial and ethnic disparity
Abstract
COVID-19 has disparately impacted low-income persons and racial and ethnic minorities–primarily Black and Hispanic populations. Our objective is to quantify disparities in access to COVID-19 testing and identify barriers to testing during the winter 2020–2021 surge in COVID-19 infections in Los Angeles County. An online survey was administered between December 2020 and January 2021 through which respondents were asked about their use of COVID testing and the barriers to testing they experienced. Our sample of 1,984 was reweighted to match the demographics of Los Angeles County. Despite similar testing rates to White residents, Hispanic residents were more likely to report testing positive. Persons with an annual income of $20,000 or less were less likely to receive a test than those with an income of $100,000 or more. Barriers to testing were more prevalent among racial/ethnic minorities and low-income persons. White respondents and high-income persons were more likely to report the ability to take time off work to await test results. Rates of testing were not commensurate with the rates of infection across racial/ethnic groups, which may be explained by higher rates of reported barriers to testing among Black and Hispanic residents. These findings may inform policies that address structural barriers to testing that disproportionately impact racial/ethnic minorities and low-income populations.
1. Introduction
COVID-19 has had a disparate impact on low-income persons and racial and ethnic minorities. Black, Hispanic and lower-income Americans are more likely to contract COVID-19 and to suffer negative consequences of the disease including hospitalization and death (Egede et al., 2020, Vahidy et al., 2020, Figueroa et al., 2021, Tan et al., 2021). As was the case in many other parts of the country, in Los Angeles County, Black and Hispanic residents and those living in the poorest neighborhoods have experienced disproportionately higher death rates from COVID-19 (Report on LA County COVID-19 Data Disaggregated by Race/Ethnicity and Socioeconomic Status, 2020, Munoz and Manthey, 2020, Lin, 2021.
Access to and utilization of COVID-19 testing is essential to curbing the spread of COVID-19, reducing deaths, and resuming economic activity (National Institute on Aging, 2021, Liang et al., 2020). Although higher rates of COVID testing have been found in communities with a greater proportion of White residents, communities with a greater proportion of Black and Latino residents have had higher rates of COVID cases and deaths (Figueroa et al., 2021, Liang et al., 2020, Lieberman-Cribbin et al., September 2020). Los Angeles was the first major city in the United States to offer free testing regardless of the presence of COVID symptoms. Numerous free testing sites were set up throughout the County including at health care providers, community hospitals and health centers, and in free standing sites such as parks and recreation centers (Los Angeles is now the first major US city to offer free coronavirus testing for all residents, 2020). Despite this effort, disparities in COVID testing rates persist (Reitsma et al., 2021, Munoz and Manthey, 2020). There is a negative correlation between case rate and testing rate among Latino residents of Los Angeles County (Reitsma et al., 2021). Furthermore, data collected on May 31, 2020 from LA County showed testing rates were lower in low-income neighborhoods and communities of color, (Report on LA County COVID-19 Data Disaggregated by Race/Ethnicity and Socioeconomic Status, 2020, Munoz and Manthey, 2020) though a high degree of missing demographic data makes it difficult to measure socioeconomic disparities in testing.
Although racial/ethnic inequities in COVID testing are well documented, the sources of those disparities are poorly understood. Perceived access to COVID testing is positively correlated with male sex, higher income, and possession of health insurance (Ali et al., 2021). In an online survey of Florida, Illinois, and Maryland residents conducted in September and October of 2020, the most commonly reported barriers to testing among those who wanted/needed a test but did not receive one were not knowing where to go and distance/waiting time (Clipman et al., 2020). Black participants were more likely to want/need a test but not receive one, though it is unclear if these barriers disproportionately affected Black residents (Clipman et al., 2020). Furthermore, a study of access to COVID testing in Massachusetts described shorter average drive times to COVID testing sites for Black, Hispanic, and Asian residents compared to White residents (Hu et al., 2020). Despite their closer proximity to testing sites, communities in Massachusetts with greater proportions of racial/ethnic minorities experienced disproportionately low testing rates with respect to the number of positive cases in those communities (Dryden-Peterson et al., 2020).
This is the first study to examine barriers to COVID-19 testing in a place where COVID-19 testing was widely available and free. Our objective was to understand disparities in access to and use of testing for COVID-19 during the winter 2020–2021 surge in COVID-19 infections. At this point in the pandemic, testing capacity was not constrained, and vaccines were not yet widely available, making testing one of the most important tools available to control the spread of the disease. At-home COVID testing kits were not widely available, and polymerase chain reaction (PCR) testing– a new public resource– was the gold standard for COVID surveillance and diagnosis. Through an online survey of nearly 2000 Los Angeles County residents administered in December 2020 through January 2021, we examined access and barriers to COVID-19 testing services.
2. Methods
We surveyed adults living in Los Angeles County between December 5, 2020 and January 10, 2021. Our online cross-sectional survey sampled from a Qualtrics market research panel of volunteers who were invited via email to participate in a Spanish or English survey on COVID-19 in exchange for voucher incentives. Our sampling included quotas for race/ethnicity, sex and income, and responses were reweighted using the 2019 American Community Survey to match the demographics of Los Angeles County. Our study utilizes anonymous survey data and is therefore exempt from Institutional Review Board approval.
2.1. Measures
We modified or included survey questions that were based on validated questions from national surveys, the PhenX toolkit (Hamilton, 2011), as well as questions proposed by our research team (Supplemental Figure). The instrument was pre-tested in Spanish and English in a socio-economically diverse population and modified to improve comprehension and understandability. We asked participants if they had “ever been tested for COVID-19”, the type and number of tests, if they ever had to pay for a test and if they ever had a positive result. Participants reported where and when they had their most recent test and how long it took to get those test results. We asked all participants if they were ever prevented from getting tested, and participants could respond “yes” or “no” to a list of possible barriers or select a write-in option. We included potential barriers to testing described in the literature (Clipman et al., 2020) as well as barriers reported by survey pre-testers and experts in healthcare navigation. Barriers listed included but were not limited to not knowing where to get tested, long wait times to get tested, concern about paying for a test, and difficulty making an appointment. We also asked participants about their knowledge of LA County’s free COVID-19 testing policy and their confidence in getting a test in the next week on a scale of 1 to 4. Participants were asked if they would be able to take time off of work while waiting for test results and if that time off was paid or unpaid. Additionally, we provided participants a list of COVID testing sites including but not limited to work, free drive-through or walk-in sites, and schools from which they could select if they had used each site in the past. Participants provided demographic information, including their race/ethnicity and income and were asked about their health, risk factors for acquiring or having severe COVID-19, access to care, and comfort with doing things online. On 12/15/2020, an additional question was added to the survey that inquired if participants ever paid for a COVID test.
2.2. Analysis
We examined the weighted proportion of individuals who reported either ever having been tested for COVID-19 as well as various other indicators of use of testing across race/ethnicity and income groups. Responses were weighted by race/ethnicity (non-Hispanic White/Hispanic/Black/Asian), income (>$35,000/<$35,000), and sex (male/female) using the 2019 American Community Survey (ACS) for Los Angeles County. Groups for each of the 16 combinations of race, income, and sex, were created, and weights were created to weight the group up to the proportion represented in the ACS. Tests for differences across race/ethnicity and income were conducted using linear probability models, comparing each group to a reference group (Non-Hispanic White or Income > $100,000). Statistical analyses were performed in Stata 15 with α set at 0.05.
We also calculated adjusted odds ratios for each of these outcomes using multivariable logistic regressions which controlled for demographic characteristics (age, gender, income, and race), access to care, risk factors for COVID-19 as well as known predictors of vaccine hesitancy: US born, household size of 4 or more people, favorability of Donald Trump, health insurance type, having a regular doctor/clinic, self-rated health status, worked outside the home during the past week, intent to receive a flu vaccine, week survey was taken and the respondent’s geographic region in Los Angeles County (Service Planning Area). In the tables and figures, we chose to represent the weighted, un-adjusted odds ratios by performing univariate logistic regressions in order to measure existing disparities by race/ethnicity and income. Adjusting for other factors changes the meaning of the regression coefficients because it partials out other factors which may intersect with race (e.g. SES, structural factors, etc.) (VanderWeele and Robinson, 2014). Weighted and adjusted results available in the supplement (Supplemental Tables 1 and 2).
3. Results
2160 eligible respondents residing in Los Angeles County completed the survey. We excluded 103 respondents who had inconsistent responses, and 73 respondents who completed the survey too quickly (less than half of the median time that was established during the test phase). Our final analytical sample included 1,984 Los Angeles County residents. Table 1 displays the demographic composition of our survey sample, the weighted percentiles, and the comparative LA County demographics from the 2019 American Community Survey.
Table 1.
Survey Sample Demographics by Race/Ethnicity, Income, and Sex, Unweighted and Weighted with Respect to Los Angeles County Demographics: Los Angeles County, December 2020–January 2021.
| Frequencies |
||||
|---|---|---|---|---|
| Unweighted (% (N)) | Weighted (%) | LA County (%) | ||
| Race and Ethnicity | Black | 17.09 (339) | 11.02 | 7.62 |
| Hispanic | 46.47 (922) | 42.60 | 42.45 | |
| Non-Hispanic White | 19.96 (396) | 27.96 | 32.88 | |
| Asian | 15.02 (298) | 15.80 | 17.05 | |
| Other | 1.46 (29) | 2.60 | – | |
| Income | <$20,000 | 14.87 (295) | 15.45 | 13.43 |
| $20,000 - $50,000 | 22.93 (455) | 23.03 | 22.74 | |
| $50,000 to $100,000 | 34.38 (682) | 33.10 | 27.43 | |
| $100,000 + | 27.82 (552) | 28.42 | 36.40 | |
| Sex | Male | 45.87 (918) | 48.61 | 48.04 |
| Female | 54.13 (1074) | 51.39 | 51.96 | |
Note. LA County demographics for race/ethnicity, income, and sex are obtained from the 2019 American Community Survey, which did not include an “Other” category for Race and Ethnicity. Respondents were classified into the four ACS race/ethnicity categories by the survey provider. We reclassified individuals as “Other” only if they did not report being Hispanic ethnicity, or any of the other racial categories in our survey. Individuals reporting multiple races or ethnicities were classified into one of the ACS racial/ethnic categories.
Table 2 shows testing by race/ethnicity and income. Overall, 51 % of our weighted sample reported ever having been tested for COVID-19 and 6.4 % reported ever having tested positive. These rates differed by race/ethnicity. Compared to non-Hispanic White respondents, Asians were less likely to report ever having a COVID test (OR 0.70, 95CI 0.50–0.97). Despite having been tested at a similar rate to White respondents, Hispanic residents were more likely to report ever having tested positive for COVID-19 (OR 1.9, 95CI 1.1–3.3). We also found differences by income, with the lowest income group reporting the lowest utilization of testing and the lowest rate of testing positive. Overall 70 % of residents were aware testing was free at County sites, however residents making less than $20,000 per year were less likely to be aware of this policy than those in the highest income group (OR 0.66, 95CI 0.46–0.97).
Table 2.
COVID Testing by Race/Ethnicity and Income: Los Angeles County, December 2020–January 2021.
| Race/Ethnicity (OR (N)) |
Income (OR (N)) |
|||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Total (N) | Non-Hispanic White | Hispanic | Black | Asian | Other | <$20,000 | $20,000–$50,000 | $50,000–$100,000 | $100,000 + | |
| Ever had a COVID test | 1010 | ref | 1.1 (0.81–1.4) | 0.85 (0.61–1.2) | 0.70a (0.50–0.97) | 0.74 (0.30–1.8) | 0.51a (0.36–0.71) | 0.79 (0.59–1.0) | 0.72a (0.28–0.95) | ref |
| Tested positive for COVID | 128 | ref | 1.9a (1.1–3.3) | 1.2 (0.56–2.4) | 0.84 (0.36–1.9) | 1 (N = 0) | 0.51a (0.28–0.95) | 0.91 (0.54–1.5) | 0.57a (0.35–0.91) | ref |
| Tested positive for COVID - among Tested | 128 | ref | 1.9a (1.1–3.4) | 1.3 (0.64–2.7) | 1.01 (0.43–2.4) | 1 (N = 0) | 0.73 (0.38–1.4) | 1.0 (0.59–1.7) | 0.65 (040–1.1) | ref |
| Number of COVID tests | – | ref | 1.1 (0.97–1.3) | 1.1 (0.86–1.3) | 0.96 (0.76–1.2) | 0.8 (0.45–1.4) | 0.61a (0.49–0.77) | 0.87 (0.73–1.0) | 0.80a (0.68–0.92) | ref |
| Time since most recent COVID test | – | ref | 0.89 (0.76–1.0) | 0.89 (0.73–1.1) | 0.86 (0.67–1.1) | 0.67 (0.37–1.2) | 0.87 (0.71–1.1) | 0.83 (0.69–1.0) | 0.76a (0.66–0.87) | ref |
| Ever had a blood test | 240 | ref | 0.52a (0.37–0.73) | 0.51a (0.32–0.81) | 0.22a (0.12–0.39) | 0.10a (0.01–0.79) | 0.37a (0.22–0.63) | 0.59a (0.38–0.92) | 0.50a (0.36–0.70) | ref |
| Got results same day or next day - among Tested | 409 | ref | 0.81 (0.57–1.1) | 0.59a(0.37–0.92) | 0.46a(0.27–0.76) | 1.5 (0.41–5.4) | 0.68 (0.42–1.1) | 0.63a (0.43–0.94) | 0.81 (0.59–1.1) | ref |
| Paid for a testaa (n = 650) | 113 | ref | 0.94 (0.56–1.5) | 0.28a(0.13–0.59) | 0.31a (0.15–0.65) | 1.1 (0.13–8.8) | 0.19a (0.07–0.55) | 0.31a (0.14–0.68) | 0.48a (0.30–0.78) | ref |
| Knowledge of free testing site policy | 1414 | ref | 0.96 (0.72–1.3) | 0.88 (0.62–1.3) | 1.1 (0.79–1.7) | 0.61 (0.24–1.6) | 0.66a (0.46–0.97) | 0.83 (0.61–1.1) | 1.1 (0.84–1.4) | ref |
| Confident of getting a test in the next week (very or somewhat) | 1426 | ref | 0.89 (0.66–1.2) | 0.89 (0.61–1.3) | 0.75 (0.51–1.1) | 0.54 (0.21–1.4) | 0.54a (0.37–0.80) | 0.56a (0.41–0.77) | 0.70a (0.54–0.92) | ref |
Note. Weighted by race/ethnicity, income, and sex. Total responses are reported as N where N is the number of “yes” survey responses. Results by race/ethnicity and income are reported as “OR (95CI)” where OR is Odds Ratio and 95CI is 95 % Confidence Interval. Rows labeled with a * display results as IRRs (Incidence Rate Ratio) in place of ORR. 95CI could not be calculated for outcomes for which N = 0.
aStatistically different (p value < 0.05) from reference group (Non-Hispanic white for differences in race/ethnicity, $100,000+ for difference across income groups).
aaSurvey question became available for respondents who took survey on or after 12/15/2020.
There were also statistically significant differences in the types of testing used. White and high income respondents were significantly more likely to report ever having used a serum antibody test (“a blood test” in the survey) compared to all other groups. White respondents also reported the highest rates of getting their results back the same or the next day. This difference was statistically significant compared to Black and to Asian respondents. Finally, Black and Asian respondents as well as all income groups below $100,000 per year were less likely to report paying for a test compared to White respondents and those making more than $100,000 per year, respectively.
Table 3 displays commonly reported barriers to testing. The most widely reported barrier to testing was worry about wait times at the testing site (30 %), followed by worry about getting the results back in time for it to matter (23 %), and worry about being able to get an appointment promptly (22 %). Compared to Whites, Hispanic respondents were significantly more likely to report two or more barriers to get tested (OR 1.5, 95CI 1.1–1.9). Specifically, they were more likely to report not knowing where to get tested (OR 1.5, 95CI 1.1–2.2), worrying about having to pay for testing (OR 1.7, 95CI 1.1–2.4), worrying about giving out personal information (OR 1.6, 95CI 1.1–2.3), worrying about wait times at the test site (OR 1.4, 95CI 1.0–1.9), and worrying about the staff not speaking their language (OR 1.9, 95CI 1.2–3.0).
Table 3.
Barriers to COVID Testing by Race/Ethnicity and Income: Los Angeles County, December 2020 - January 2021.
| Race/Ethnicity (OR (N)) |
Income (OR (N)) |
|||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Total (N) | Non-Hispanic White | Hispanic | Black | Asian | Other | <$20,000 | $20,000 - $50,000 | $50,000 to $100,000 | $100,000+ | |
| Didn't know where to go for testing | 393 | ref | 1.5a (1.1–2.2) | 1.2 (0.80–1.9) | 0.92 (0.58–1.5) | 1.2 (0.34–4.1) | 1.2 (0.82–1.9) | 1.3 (0.95–1.9) | 0.85 (0.63–1.1) | ref |
| Didn't have transportation to or from the testing site | 280 | ref | 1.1 (0.73–1.6) | 1.2 (0.76–2.0) | 0.56 (0.31–1.0) | 2.0 (0.60–6.6) | 2.1a (1.4–3.3) | 1.6a (1.1–2.4) | 0.9 (0.47–1.0) | ref |
| Worried about not being able to pay for a test | 416 | ref | 1.7a (1.1–2.4) | 1.4 (0.83–1.9) | 0.98 (0.77–1.8) | 3.0 (0.91–7.7) | 1.6a (1.1–2.4) | 1.8a (1.3–2.5) | 1.2 (0.89–1.7) | ref |
| Didn't have someone to watch my children/other people in my care while I went to get tested | 261 | ref | 1.5 (0.99–2.2) | 1.4 (0.87–2.3) | 0.98 (0.57–1.7) | 2.3 (0.90–9.8) | 0.89 (0.54–1.5) | 1.1 (0.72–1.6) | 0.79 (0.56–1.1) | ref |
| Couldn't take time off from work to get tested | 280 | ref | 1.4 (0.92–2.0) | 1.5 (0.91–2.3) | 1.1 (0.66–1.8) | 0.90 (0.17–4.7) | 1.0 (0.63–1.6) | 1.1 (0.74–1.7) | 0.98 (0.70–1.4) | ref |
| Couldn't get an appointment for a test in time | 433 | ref | 1.4 (0.99–1.9) | 0.87 (0.57–1.3) | 1.2 (0.77–1.7) | 1.1 (0.31–3.7) | 0.84 (0.56–1.3) | 1.1 (0.81–1.6) | 1.0 (0.77–1.4) | ref |
| Worried about giving my personal information to the staff at the test site | 311 | ref | 1.6a (1.1–2.3) | 1.3 (0.83–2.1) | 1.0 (0.61–1.6) | 0.85 (0.16–4.5) | 1.1 (0.70–1.6) | 1.1 (0.75–1.6) | 0.84 (0.61–1.2) | ref |
| Worried wait times for testing would be too long | 586 | ref | 1.4a (1.0–1.9) | 1.1 (0.74–1.5) | 1.3 (0.88–1.8) | 1.7 (0.63–4.5) | 0.90 (0.62–1.3) | 0.77 (0.57–1.0) | 0.82 (0.64–1.1) | ref |
| Didn't think I would get my test results back in time for it to matter | 434 | ref | 0.93 (0.68–1.3) | 0.73 (0.49–1.1) | 0.81 (0.54–1.2) | 0.92 (0.29–2.9) | 1.2 (0.76–1.8) | 1.1 (0.81–1.6) | 0.93 (0.70–1.2) | ref |
| Worried that testing site staff wouldn't speak my language | 180 | ref | 1.9a (1.2–3.0) | 1.3 (0.73–2.4) | 0.32a (0.13–0.81) | 1.5 (0.27–8.4) | 1.2 (0.69–2.0) | 0.70 (0.44–1.1) | 0.59a (0.39–0.90) | ref |
| Some other reason | 172 | ref | 0.88 (0.55–1.4) | 1.2 (0.69–2.0) | 0.56 (0.30–1.1) | 1 (N = 0) | 0.95 (0.52–1.7) | 0.73 (0.44–1.2) | 0.60a (0.40–0.90) | ref |
| Two or more barriers | 778 | ref | 1.5a (1.1–1.9) | 1.2 (0.88–1.7) | 0.99 (0.70–1.4) | 1.1 (0.40–2.9) | 1.3 (0.94–1.9) | 1.3 (0.99–1.8) | 0.97 (0.76–1.2) | ref |
Note. Weighted by race/ethnicity, income, and sex. Total responses are reported as N where N is the number of “yes” survey responses for a given barrier. Results by race/ethnicity and income are reported as “OR (95CI)” where OR is Odds Ratio and 95CI is 95 % Confidence Interval. 95CI could not be calculated for outcomes for which N = 0.
aStatistically different (p value < 0.05) from reference group (Non-Hispanic white for differences in race/ethnicity, $100,000+ for difference across income groups).
There were several notable differences in barriers to testing among respondents who never got tested for COVID-19 (Supplemental Table 3). Black and Hispanic respondents and those in the lowest two income groups were more likely to experience two or more barriers to testing compared to White respondents and those in the highest income group. Respondents with lower incomes (under $50,000) were significantly more likely to not know where to go for testing, not have transportation to get to testing sites and be worried about paying for a test. Compared to Whites, Black, Hispanic and Asian respondents were significantly more likely to report they couldn’t get a testing appointment in time and were worried about giving their personal information to staff at the test site. Hispanic respondents experienced significantly higher rates of many barriers including that they did not know where to get tested, did not have someone to watch their family members while getting tested or were unable to take time off work for testing, were more likely to worry about paying for a test, wait times at test sites and staff at testing sites not speaking their language.
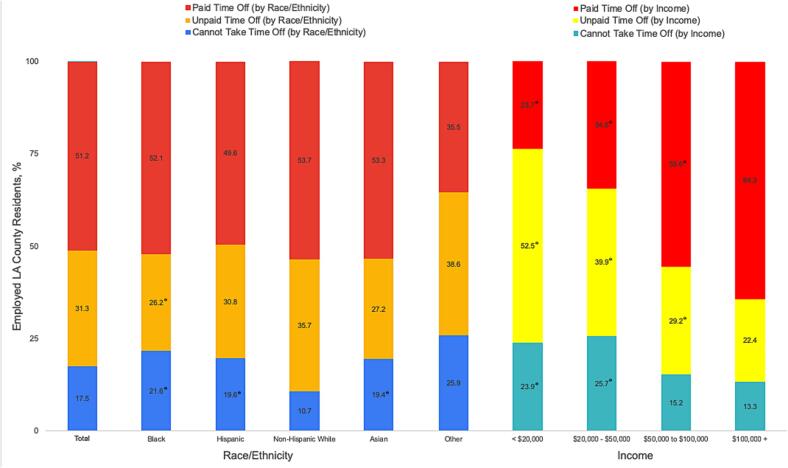
Fig. 1 shows differences in the ability to take time off from work while waiting for test results among employed respondents. White employed respondents, and employed respondents in the highest income group were the most likely to report being able to take time off from work while waiting for test results. One in four employed respondents in the lowest income group could not take any time off work while their test results were pending.
Fig. 1.
Ability to Take Time Off Work While Waiting for Test Results by Race/Ethnicity and Income: Los Angeles County, December 2020 - January 2021. Note. Weighted by race/ethnicity, income, and sex. Survey results were excluded due to unemployment, not working, and retirement. *Statistically different (p value < 0.05) from reference group (Non-Hispanic white for differences in race/ethnicity, $100,000+ for difference across income groups).
There were significant differences in types of testing sites used by race/ethnicity and income (Table 4). Hispanic and Asian residents were significantly less likely to get tested at a doctor’s office or clinic compared to White residents (OR 0.69 and 0.36, 95CI 0.41–0.86 and 0.20–0.63 respectively) and more likely to get tested at a free drive-through test site (OR 1.7 and 2.8, 95CI 1.2–2.5 and 1.6–4.1 respectively). Black and Asian residents were more likely than White residents to get tested at a college or university (OR 3.6 and 11.4, 95CI 1.3–10.0 and 1.5–12.3 respectively). Residents in the lowest income group (incomes below $20,000 per year) were more likely to get tested at a college or university (OR 3.8, 95CI 1.6–9.4) and less likely to get tested at work compared to those in the highest income group (OR 0.35, 95CI 0.18–0.70). The most common testing site for White residents and those in the highest income group were doctor's offices or clinics while free drive-through testing sites were most commonly used by all other groups.
Table 4.
COVID Testing Sites by Race/Ethnicity and Income: Los Angeles County, December 2020–January 2021.
| Race/Ethnicity (OR) |
Income (OR) |
|||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Total (%) | Non-Hispanic White | Hispanic | Black | Asian | Other | <$20,000 | $20,000 - $50,000 | $50,000 to $100,000 | $100,000 + | |
| Work | 21.3 % | ref | 1.1 (0.75–1.7) | 1.2 (0.70–2.0) | 0.62 (0.33–1.2) | 0.72 (0.18–2.9) | 0.35a (0.18–0.70) | 0.48a (0.30–0.78) | 0.69 (0.47–1.0) | ref |
| Doctor's Office or Clinic | 26.4 % | ref | 0.59a (0.41–0.86) | 0.70 (0.43–1.1) | 0.36a (0.20–0.63) | 0.22 (0.04–1.0) | 0.58 (0.32–1.0) | 0.56a (0.36–0.89) | 0.67a (0.47–0.95) | ref |
| Hospital or Emergency room | 16.8 % | ref | 0.57a (0.36–0.90) | 0.62 (0.34–1.1) | 0.54 (0.29–1.0) | 1.0 (0.17–6.0) | 0.61 (0.30–1.2) | 1.0 (0.58–1.7) | 0.71 (0.47–1.1) | ref |
| Free Drive-through Site | 35.1 % | ref | 1.7a (1.2–2.5) | 1.3 (0.81–2.1) | 2.5a (1.6–4.1) | 0.73 (0.21–2.6) | 1.5 (0.97–2.5) | 1.4 (0.97–2.1) | 1.3 (0.91–1.8) | ref |
| Free Walk-in Site | 13.2 % | ref | 1.3 (0.77–2.2) | 1.5 (0.73–2.9) | 1.3 (0.66–2.6) | 1.5 (0.35–6.0) | 1.2 (0.64–2.3) | 0.92 (0.49–1.7) | 1.6 (0.98–2.5) | ref |
| Pharmacy | 6.2 % | ref | 0.99 (0.51–2.0) | 1.1 (0.44–2.6) | 1.6 (0.74–3.6) | 1 (N = 0) | 1.1 (0.48–2.4) | 0.41 (0.17–1.0) | 1.3 (0.71–2.4) | ref |
| School, College or University | 5.7 % | ref | 1.7 (0.69–4.4) | 3.6a (1.3–10.0) | 4.3a (1.5–12.3) | 11.4a (1.7–75.0) | 3.8a (1.6–9.4) | 1.5 (0.53–4.3) | 2.0 (0.91–4.2) | ref |
| Other | 3.9 % | ref | 0.91 (0.39–2.1) | 0.95 (0.32–2.8) | 1.5 (0.53–4.0) | 3.0 (0.56–16.4) | 0.51 (0.18–1.5) | 0.27a (0.09–0.76) | 0.57 (0.26–1.2) | ref |
Note. Weighted by race/ethnicity, income, and sex. Total results are reported as % of those responding “yes,” and results by race/ethnicity and income group are reported as ORs (Odds Ratios) with 95CI (95 % Confidence Interval). 95CI could not be calculated for outcomes for which N = 0.
aStatistically different (p value < 0.05) from reference group (Non-Hispanic white for differences in race/ethnicity, $100,000+ for difference across income groups).
4. Discussion
We found that by December 2020 and January 2021, approximately half of adults in Los Angeles County had been tested for COVID-19. Despite similar rates of testing across different race and ethnic groups, the rates of COVID testing were not commensurate with the rates of infection across groups. In particular, Hispanic participants who received a COVID-19 test were significantly more likely to test positive. This pattern of disparities is consistent with data reported by the Los Angeles County Department of Public Health representing high rates of COVID cases among Hispanic residents despite testing rates comparable to that of White residents (Los Angeles County Department of Public Health, 2021). Testing disparities were also prevalent across income groups. Respondents making >$100 K had the highest rate of testing but also the highest rate of testing positive for COVID-19. Although the county began providing COVID-19 tests for free in April of 2020, when surveyed in December, only 70.0 % of LA County adult residents were aware that testing was free. Respondents in the lowest income group were the least likely to be aware of the free testing policy. Confidence in being able to get a test within the next week also declined as income declined.
Barriers to testing were more prevalent among racial/ethnic minorities and low income persons. Such barriers may explain lower rates of testing in these groups despite likely having a higher need for testing (Lieberman-Cribbin et al., September 2020, Dryden-Peterson et al., 2020). Hispanic participants were more likely to report multiple different barriers to COVID testing. While some barriers may have been related to a lack of clear information about testing –such as not knowing where to get tested or having to pay for a test– many were related to broader structural barriers including a lack of childcare, transportation and an inability to take time off work. These barriers have previously been shown to limit access to health care for racial/ethnic minorities and low-income persons (Ahmed et al., 2001, Miller et al., 2019). Barriers such as not being able to get an appointment in time, wait times at testing sites, and results taking too long were also more problematic in these groups. Such delays may create a perception that testing is futile and discourage individuals from seeking COVID tests (McElfish et al.,March, 2021). One possible explanation for the disparities we observed is that when free, publicly run testing sites were strained, particularly during the surges of COVID cases, higher-income and White residents had an easier time getting tested through health systems compared to other groups. This is supported by our survey in that racial/ethnic minorities and lower-income groups were most likely to use free drive through testing sites and those in the highest income group and White residents were more likely to use clinics or doctor’s offices. Long wait times and a lack of appointments at free, public testing sites may also have encouraged individuals to seek COVID tests at other locations. However, private health insurance and group coverage plans were not required to provide non-medically necessary COVID tests, which includes screening tests conducted prior to January 15, 2022 (Healey, 2022, Keith, 2022). This results in out-of-pocket costs for COVID testing, which poses a greater barrier to low-income groups as they were significantly more likely to report concern about being able to pay for a COVID test. As seen during the surge of the Omicron COVID-19 variant in January 2022, a high demand for testing has resulted in price gouging for at-home testing kits, which may be resold for a much higher price than their retail value (Butler, 2022).
Restrictions on taking time off work while waiting for test results may have contributed to higher rates of COVID-19 transmission and infection in racial/ethnic minority and low-income communities. Although there is no statistically significant difference across race/ethnicity and income in reporting inability to take time off of work as a barrier to COVID testing, Fig. 1 shows statistically significant differences among employed respondents in their ability to time off of work is masked when failing to account for employment status. Working Black, Hispanic and Asian residents and lower-income residents were less likely to be offered any time off work while their COVID-19 tests were pending. Given that the pandemic coincided with increased economic hardship in these same groups, who also are more likely to work outside the home, (Selden and Berdahl, 2020) having to make the choice between losing income or a job and returning to work despite concerns about having COVID-19 may have contributed to differences in COVID-19 infection rates across groups.
Our study had several limitations. As an internet-based survey, our data collection method is susceptible to self-selection bias (Wright, 2005) and may exclude those without internet access, such as older adults and lower-income individuals (NW, 1615 L. St, Suite 800 Washington, 2021). Sampling quotas on sex, income, race, and ethnicity were included, and our survey was available in both English and Spanish, but we were unable to sufficiently sample individuals who speak Spanish as their primary language. Responses were also weighted by sex, income, race, and ethnicity, but we chose not to adjust for other demographic characteristics in order to represent the true burden of barriers to COVID-19 testing. Additionally, our survey did not ask respondents if they experienced difficulties signing up for a COVID test online– a well-documented barrier that inhibited seniors from signing up for COVID vaccine appointments (Browning, 2021). Because the survey sample was geographically restricted to residents of Los Angeles County, generalizability of its findings may be limited. Finally, many statistical tests were performed which may result in potential spurious associations.
While Los Angeles County undertook an unprecedented effort to test residents during this pandemic there were several factors that may have contributed to undertesting in groups that ultimately were most vulnerable to COVID-19. First, testing strategies that could circumvent broader structural barriers to accessing test sites, such as transportation, childcare and time off work, were necessary. Second, ensuring that enough resources were available for free, publicly accessible testing–which were most commonly used by lower income groups and racial/ethnic minorities–was critically important during the surge. This included adequate appointment time slots, after work hour appointments and increased capacity to rapidly process tests. Delayed receipt of test results, which disproportionately affected some marginalized groups we surveyed, could have led to increased transmission. Lastly, developing and enforcing policies that protect workers from repercussions of testing, including paid time off for both getting tested and waiting for test results. While California offers some protections for employees in the case that testing is required for their job, more explicit protections and clearer enforcement may be needed.
5. Conclusion
Structural barriers to COVID testing contributed to lower testing rates among racial/ethnic minorities and low-income persons despite greater positive test rates. Allocating additional resources to free, public testing sites may have mitigated lack of available appointments, long wait times, and delayed test results disparately experienced by racial/ethnic minorities and low-income persons during the COVID-19 pandemic. Better resourced testing sites in communities with a greater proportion of non-White, low-income residents should be prioritized in future responses to communicable diseases and other public health needs. Furthermore, policies that grant paid time off for employees to be tested for COVID and wait for their test results may have reduced disparities in COVID infections and outcomes experienced by racial/ethnic minorities and low-income persons. In future infectious outbreaks, work-place protections may reduce the disparate burden of transmission among employed racial/ethnic minorities and lower-income persons.
6. Disclosures
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper. This study was funded by the WM Keck Foundation.
CRediT authorship contribution statement
Zain Khalifeh: Writing – original draft, Writing – review & editing, Investigation, Formal analysis, Visualization. Sonali Saluja: Writing – original draft, Supervision, Project administration, Methodology, Investigation, Funding acquisition, Conceptualization. Chun Nok Lam: Formal analysis. Cameron Kaplan: Writing – review & editing, Writing – original draft, Supervision, Project administration, Methodology, Investigation, Funding acquisition, Formal analysis, Conceptualization.
Declaration of competing interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Footnotes
Supplementary data to this article can be found online at https://doi.org/10.1016/j.pmedr.2023.102567.
Appendix A. Supplementary data
The following are the Supplementary data to this article:
Data availability
Data will be made available on request.
References
- Ahmed S.M., Lemkau J.P., Nealeigh N., Mann B. Barriers to healthcare access in a non-elderly urban poor American population. Health Soc. Care Community. 2001;9(6):445–453. doi: 10.1046/j.1365-2524.2001.00318.x. [DOI] [PubMed] [Google Scholar]
- Ali S.H., Tozan Y., Jones A.M., Foreman J., Capasso A., DiClemente R.J. Regional and socioeconomic predictors of perceived ability to access coronavirus testing in the united states: results from a nationwide online COVID-19 survey. Ann. Epidemiol. June 2021;58:7–14. doi: 10.1016/j.annepidem.2021.03.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Browning, Kellen. “Seniors Seeking Vaccines Have a Problem: They Can’t Use the Internet.” The New York Times, February 28, 2021, sec. Technology. https://www.nytimes.com/2021/02/28/technology/seniors-vaccines-technology.html.
- Butler, Kelsey. “Rapid COVID Tests Are Reselling for Triple the Retail Price - Los Angeles Times.” New York Times. Accessed January 16, 2022. https://www.latimes.com/business/story/2022-01-05/rapid-covid-tests-are-reselling-for-triple-the-retail-price.
- Clipman, Steven J., Amy Wesolowski, Shruti H. Mehta, Smisha Agarwal, Sarah E. Cobey, Derek A.T. Cummings, Dustin G. Gibson, Alain B. Labrique, Gregory D. Kirk, and Sunil S. Solomon. “SARS-CoV-2 Testing in Florida, Illinois, and Maryland: Access and Barriers.” Preprint. medRXIV. Epidemiology, December 24, 2020. 10.1101/2020.12.23.20248789. https://www.medrxiv.org/content/10.1101/2020.12.23.20248789v1. [DOI]
- Dryden-Peterson, Scott, Gustavo E. Velásquez, Thomas J. Stopka, Sonya Davey, Shahin Lockman, and Bisola Ojikutu. “SARS-CoV-2 Testing Disparities in Massachusetts.” MedRxiv, November 4, 2020, 2020.11.02.20224469. 10.1101/2020.11.02.20224469. [DOI] [PMC free article] [PubMed]
- Egede, Leonard E., Rebekah J. Walker, Emma Garacci, and John R. Raymond. “Racial/Ethnic Differences In COVID-19 Screening, Hospitalization, And Mortality In Southeast Wisconsin: Study Examines Racial/Ethnic Differences in COVID-19 Screening, Symptom Presentation, Hospitalization, and Mortality among 31,549 Adults Tested for COVID-19 in Wisconsin.” Health Affairs 39, no. 11 (November 1, 2020): 1926–34. 10.1377/hlthaff.2020.01081. [DOI] [PMC free article] [PubMed]
- Figueroa, Jose F., Rishi K. Wadhera, Winta T. Mehtsun, Kristen Riley, Jessica Phelan, and Ashish K. Jha. “Association of Race, Ethnicity, and Community-Level Factors with COVID-19 Cases and Deaths across U.S. Counties.” Healthcare 9, no. 1 (March 1, 2021): 100495. 10.1016/j.hjdsi.2020.100495. [DOI] [PMC free article] [PubMed]
- Hamilton,, et al. The PhenX Toolkit: Get the Most From Your Measures. Am. J. Epidemiol. 2011;174(3):253–260. doi: 10.1093/aje/kwr193. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Healey, John. “More Free Rapid COVID Tests Are Coming. Here’s What We Know so Far.” Los Angeles Times, January 13, 2022. https://www.latimes.com/california/story/2022-01-13/how-to-get-your-free-at-home-covid-test.
- Hu, Tao, Han Yue, Changzhen Wang, Bing She, Xinyue Ye, Regina Liu, Xinyan Zhu, Weihe Wendy Guan, and Shuming Bao. “Racial Segregation, Testing Site Access, and COVID-19 Incidence Rate in Massachusetts, USA.” International Journal of Environmental Research and Public Health 17, no. 24 (January 2020): 9528. 10.3390/ijerph17249528. [DOI] [PMC free article] [PubMed]
- Keith, Katie. “Insurers And Plans Must Cover At-Home Tests For COVID-19 | Health Affairs Forefront.” Health Affairs. Accessed January 16, 2022. https://www.healthaffairs.org/do/10.1377/forefront.20220111.960247/full/.
- Liang, Li-Lin, Ching-Hung Tseng, Hsiu J. Ho, and Chun-Ying Wu. “Covid-19 Mortality Is Negatively Associated with Test Number and Government Effectiveness.” Scientific Reports 10, no. 1 (July 24, 2020): 12567. 10.1038/s41598-020-68862-x. [DOI] [PMC free article] [PubMed]
- Lieberman-Cribbin W., Tuminello S., Flores R.M., Taioli E. Disparities in COVID-19 testing and positivity in New York City. Am. J. Prev. Med. September 2020;59(3):326–332. doi: 10.1016/j.amepre.2020.06.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lin II, Rong-Gong, and Luke Money. “Deaths among Latinos in L.A. County from COVID-19 Rising at Astonishing Levels.” Los Angeles Times, January 14, 2021. https://www.latimes.com/california/story/2021-01-14/latino-black-and-poor-residents-suffer-dramatically-worsening-covid-death-rates.
- Los Angeles County Department of Public Health. “LA County COVID-19 Surveillance Dashboard.” Accessed June 18, 2021. http://dashboard.publichealth.lacounty.gov/covid19_surveillance_dashboard/.
- Los Angeles is now the first major US city to offer free coronavirus testing for all residents. CNN. Updated April 30, 2020. Accessed June 27, 2020. Available from: https://www.cnn.com/2020/04/30/us/los-angeles-free-coronavirus-test/index.html.
- McElfish P.A., Purvis R., James L.P., Willis D.E., Andersen J.A. Perceived Barriers to COVID-19 Testing. Int. J. Environ. Res. Public Health. March 2021;18(5):2278. doi: 10.3390/ijerph18052278. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Miller, Brittany C., Jennifer M. Bowers, Jackelyn B. Payne, and Anne Moyer. “Barriers to Mammography Screening among Racial and Ethnic Minority Women.” Social Science & Medicine 239 (October 1, 2019): 112494. 10.1016/j.socscimed.2019.112494. [DOI] [PubMed]
- Munoz, Anabel, and Grace Manthey. “Whiter, Richer Areas in LA Have More Access to COVID-19 Testing - but the Gap May Be Narrowing.” ABC7 Los Angeles, July 22, 2020. https://abc7.com/6329349/.
- National Institute on Aging. “Why COVID-19 Testing Is the Key to Getting Back to Normal.” Accessed March 28, 2021. http://www.nia.nih.gov/news/why-covid-19-testing-key-getting-back-normal.
- NW, 1615 L. St, Suite 800 Washington, and DC 20036 USA202-419-4300 | Main202-857-8562 | Fax202-419-4372 | Media Inquiries. “Demographics of Internet and Home Broadband Usage in the United States.” Pew Research Center: Internet, Science & Tech (blog). Accessed December 23, 2021. https://www.pewresearch.org/internet/fact-sheet/internet-broadband/.
- Reitsma, Marissa B., Anneke L. Claypool, Jason Vargo, Priya B. Shete, Ryan McCorvie, William H. Wheeler, David A. Rocha, et al. “Racial/Ethnic Disparities In COVID-19 Exposure Risk, Testing, And Cases At The Subcounty Level In California.” Health Affairs 40, no. 6 (June 2021): 870–78. 10.1377/hlthaff.2021.00098. [DOI] [PMC free article] [PubMed]
- Report on LA County COVID-19 Data Disaggregated by Race/Ethnicity and Socioeconomic Status. County of Los Angeles Department of Public Health. April 28, 2020. Accessed June 27, 2020. Available from: https://www.documentcloud.org/documents/6884202-LA-County-Racial-Ethnic- Socioeconomic-Data-COVID19.html#document/p6/a563075.
- Selden, Thomas M., and Terceira A. Berdahl. “COVID-19 And Racial/Ethnic Disparities In Health Risk, Employment, And Household Composition.” Health Affairs 39, no. 9 (September 1, 2020): 1624–32. 10.1377/hlthaff.2020.00897. [DOI] [PubMed]
- Tan A.X., Hinman J.A., Abdel Magid H.S., Nelson L.M., Odden M.C. Association between income inequality and county-level COVID-19 cases and deaths in the US. JAMA Netw Open. 2021;4(5):e218799. doi: 10.1001/jamanetworkopen.2021.8799. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Vahidy, Farhaan S., Juan Carlos Nicolas, Jennifer R. Meeks, Osman Khan, Alan Pan, Stephen L. Jones, Faisal Masud, et al. “Racial and Ethnic Disparities in SARS-CoV-2 Pandemic: Analysis of a COVID-19 Observational Registry for a Diverse US Metropolitan Population.” BMJ Open 10, no. 8 (August 1, 2020): e039849. 10.1136/bmjopen-2020-039849. [DOI] [PMC free article] [PubMed]
- VanderWeele T.J., Robinson W.R. On the causal interpretation of race in regressions adjusting for confounding and mediating variables. Epidemiology. 2014;25(4):473–484. doi: 10.1097/EDE.0000000000000105. PMID: 24887159; PMCID: PMC4125322. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wright, K.B. “Researching Internet-Based Populations: Advantages and Disadvantages of Online Survey Research, Online Questionnaire Authoring Software Packages, and Web Survey Services.” J. Comput.-Mediat. Commun. 10, no. 3 (April 1, 2005): JCMC1034. 10.1111/j.1083-6101.2005.tb00259.x. [DOI]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Data Availability Statement
Data will be made available on request.