Abstract
Objective:
The purpose of this study was to use a dual-process decision-making model to examine the longitudinal associations between alcohol-induced blackouts (blackouts) and alcohol use disorder (AUD) risk symptoms among college student drinkers.
Method:
Undergraduate drinkers (N = 2,024; 56% female; 87% White; 5% Hispanic) at a large northeastern university completed online surveys each semester during their first (Time [T] 1, T2), second (T3, T4), third (T5, T6), and fourth (T7, T8) years of college (87% retention across the study). Path analyses were examined testing the longitudinal associations between T1 willingness to experience a blackout, T1 intentions to avoid a blackout, T2–T8 drinking, T2–T8 blackouts, and T8 AUD risk symptoms. Hypotheses 1 and 2 tested the associations between T1 willingness, T1 intentions, T2–T8 drinking, and T2–T8 blackouts. Hypothesis 3 tested the associations between T2–T8 drinking, T2–T8 blackouts, and T8 AUD risk symptoms.
Results:
Students experienced an average of 8 (SD = 8) blackouts during college. Approximately 1,514 (88.8%) participants reported experiencing 1 of 8 AUD risk symptoms. T1 willingness was positively associated with T2–T8 blackouts. T2–T8 drinking and T2–T8 blackouts were positively associated with T8 AUD risk symptoms. T1 willingness significantly indirectly affected T8 AUD risk symptoms through its association with T2–T8 blackouts.
Conclusions:
Results estimated that, on average, college student drinkers experienced eight blackouts across 4 years of college, and 88% of participants reported experiencing at least one symptom of AUD in the last semester of college. Willingness to experience a blackout influenced students' AUD risk symptoms through the number of blackouts they experienced throughout college.
Alcohol-induced blackouts (blackouts) occur when an individual has an absence of memory for all or part of a drinking episode (Wetherill & Fromme et al., 2016; White, 2003). Approximately 4 out of 5 college student drinkers will experience a blackout at some point during college (Glenn et al., 2022). Blackouts are associated with a variety of severe consequences such as getting in trouble with the police, experiencing an alcohol-related injury, alcohol overdoses (Hingson et al., 2016), sexual assault (Voloshyna et al., 2018), sexual coercion victimization (Wilhite et al., 2018), driving under the influence (Robertson et al., 2019), and alcohol use disorder (AUD) symptoms (Studer et al., 2019). Heavy alcohol use is necessary but not always sufficient for experiencing a blackout (Wilhite & Fromme, 2015). Factors outside of drinking also influence blackout risk. These include family history of alcohol problems (LaBrie et al., 2011; Marino & Fromme, 2015), playing drinking games (Miller et al., 2018b; Ray et al., 2014), drinking motives (Merrill et al., 2016; Miller et al., 2020), peer norms (Merrill et al., 2016, 2022), and age at drinking onset (Gruber et al., 1996; Jennison & Johnson, 1994; Marino & Fromme, 2016; White et al., 2002). Despite extensive research documenting risk factors and harms associated with blackouts, there has been limited research examining psychosocial predictors influencing blackouts and subsequent AUD risk symptoms among college student drinkers.
Blackouts and AUD risk symptoms
Early research by Jellinek (1952) suggested that blackouts were one of the earlier signs of AUD. These findings have been replicated in studies among young adults (Studer et al., 2019; Yuen et al., 2021). Studer and colleagues (2019) examined Swiss male drinkers assessing blackouts, AUD, and alcohol use and found that those who reported blackouts at age 20 were significantly more likely to report AUD symptoms by age 25. Yuen and colleagues (2021) conducted a longitudinal study on Australian individuals ages 13 to 20 years and found that earlier age at onset of drinking and blackouts were associated with AUD symptoms. The current study extends findings from these studies to examine psychosocial factors influencing blackouts and AUD risk symptoms among a sample of college student drinkers.
Prototype Willingness Model
The current study used the Prototype Willingness Model (PWM) to examine willingness to experience blackouts, intentions to avoid blackouts, drinking, total blackouts experienced in college, and AUD risk symptoms among college student drinkers. The PWM is a dual-process model designed to capture and explain risk behaviors (Gerrard et al., 2008; Gibbons et al., 1998; Litt et al., 2014). The model suggests two specific paths that lead to risk-taking behaviors: the social reaction pathway (willingness) and the reasoned pathway (intentions; Gerrard et al., 2008; Gibbons et al., 1998, 2009; Pomery et al., 2009). Willingness reflects an individual's openness to opportunity, whereas intentions reflect what individuals plan to do or plan to avoid (Gerrard et al., 2008; Gibbons, 2020; Gibbons et al., 1998, 2009). When assessing health behaviors that concern health risk (e.g., experiencing a blackout), Gibbons (2020) suggests examining willingness to engage in the behavior and intentions to not engage in the behavior. Studies have observed willingness and intentions to be associated with a variety of risk-taking behaviors associated with alcohol use and related consequences (Glenn et al., 2022; Hultgren et al., 2018; Litt et al., 2014; Mallett et al., 2015; Scaglione et al., 2015). However, some research suggests that willingness may be a stronger predictor of risk behaviors than intentions (Gibbons, 2020; Litt et al., 2014; Merrill et al., 2022; Pomery et al., 2009). For example, Litt and colleagues (2014) conducted a study to evaluate the importance of willingness versus intentions in the context of spring break drinking behaviors among college students. They found that willingness was a stronger predictor than intentions when assessing high-risk drinking (e.g., getting drunk enough to black out or pass out). Merrill and colleagues (2022) conducted a qualitative study to understand the phenomenology of blackouts among college student drinkers. They found that willingness was more relevant than intentions when assessing blackouts. They also found that intentions to experience a blackout may reflect an intention to get drunk. Together, these studies are suggestive of the utility of examining the longitudinal associations using constructs from the PWM to assess blackouts and subsequent AUD risk symptoms among college student drinkers.
Current study
The aims of the current study were twofold: (a) assess descriptive statistics describing blackouts and AUD risk symptoms experienced in a sample of college student drinkers; and (b) examine a longitudinal path model testing the associations between first semester willingness to experience a blackout, first semester intentions to avoid experiencing a blackout, drinking, total blackouts experienced throughout college, and last semester AUD risk symptoms among college student drinkers. The theoretical model guiding the associations is provided in Figure 1. First, based on previous studies examining the PWM constructs (Litt et al, 2014; Merrill et al., 2022), it was hypothesized (H1) that first semester willingness to experience a blackout would be positively associated with average drinking throughout college (e.g., Semesters 2–8) and the total number of blackouts experienced throughout college (e.g., semesters 2–8). Based on Merrill and colleagues (2022), it was also hypothesized (H2) that first semester intentions to avoid a blackout would be negatively associated with average drinking throughout college and would have no association with the total number of blackouts experienced throughout college. Previous research suggests that students’ willingness and intentions from the first year of college are associated with future behaviors such as drinking and alcohol-related consequences (Glenn et al., 2022; Mallett et al., 2015; Trager et al., 2019). Examining first semester willingness and intentions provides a target for future prevention efforts focused on first-year student drinkers. Third, based on Studer et al. (2019) and Yuen et al. (2021), it was hypothesized (H3) that average drinking throughout college and total blackouts would be positively associated with last semester AUD risk symptoms. Finally, indirect effects were tested to assess the impact willingness and intentions have on AUD risk symptoms through their associations with drinking and blackouts.
Figure 1.
Theoretical model. DDQ = Daily Drinking Questionnaire; AUD = alcohol use disorder.
Method
Procedures and participants
To obtain our longitudinal college student drinking sample, we used the following inclusion criteria: first-year student between ages 18 and 19 years old at baseline and reported drinking in the month before baseline. During their first fall semester on campus, 4,000 students at a large, public university in the northeastern United States were randomly selected from the university registrar's database. Participants were sent a pre-notification letter and an email invitation describing the study and inviting their participation with up to seven reminder emails. Recruitment materials included a URL and a PIN to access the survey. Informed consent was presented to students upon logging into the baseline survey. A total of 2,690 (67.3%) students responded to the email invitation and completed the baseline survey (Time [T] 1) at the end of the fall semester. Of the 2,690 students who completed baseline, 2,024 (75%) met the study inclusion criteria and were invited to complete surveys at the end of the spring semester during their first year (T2), and at the end of each fall and spring semester during their second (T3, T4), third (T5, T6), and fourth (T7, T8) years of college. Data collection at each timepoint was scheduled to avoid overlap with exam periods and spring break to reflect typical drinking patterns. The baseline survey occurred in the fall of 2012 and the final T8 survey occurred in the spring of 2016. Students received $25 for completing surveys in Year 1, $30 for Year 2, $35 for Year 3, and $40 for Year 4. Students received an additional $5 for each survey they completed within 5 days of receiving the email invitation. All study procedures were reviewed and approved by the university's institutional review board.
Measures
Measures were assessed at the student level and collected via online self-report surveys. All measures were assessed and adjusted for outliers (skewness values beyond +/-2 and kurtosis values +/- 5; Tabachnick & Fidell, 2013). T1 drinking was adjusted for outliers. Measures adjusted for outliers were recoded to equal a value of 3.3 times the standard deviation beyond the mean.
Willingness (T1). Students responded to a single item asking, “In the next few months, I am willing to not be able to remember large stretches of time as a result of drinking” (as used by Glenn et al., 2022; Mallett et al., 2015). Response options were on a 7-point scale ranging from -3 (strongly disagree) to 3 (strongly agree). Higher scores indicated that the participant was more willing to not remember large stretches of time in the next few months.
Intentions (T1). Students responded to a single item asking, “In the next few months, I intend to avoid not being able to remember large stretches of time as a result of drinking.” Based off recommendations from Gibbons (2020), the intention item reflects wording recommended for behaviors that concern health risk and therefore uses the terminology “intend to avoid” instead of “intend to experience.” Response options were on a 7-point scale ranging from -3 (strongly disagree) to 3 (strongly agree). Higher scores indicated that the participant intended to avoid not being able to remember large stretches of time as a result of drinking.
Drinking (T1, T2–T8). Student drinking was assessed using the Daily Drinking Questionnaire (DDQ; Collins et al., 1985). The DDQ captured how much alcohol students drank in a typical week during the current semester. Responses for each of the 7 days were summed to create a measure of typical weekly drinking (T1). We created a composite drinking measure capturing typical weekly drinking throughout college (T2–T8: α = .94).
Alcohol-induced blackouts (T1, T2–T8). Blackouts were assessed using a single item adapted from the Young Adult Alcohol Consequences Questionnaire (YAACQ; Read et al., 2006). Participants were asked to indicate the number of times they could not remember large stretches of time while drinking during the current semester. Responses were measured on a 9-point scale where 0 = never experienced consequence, 1 = 1 time, 2 = 2 times, 3 = 3 times, 4 = 4–6 times, 5 = 7–11 times, 6 = 12–20 times, 7 = 21–39 times, and 8 = 40 or more times. When we examined the frequencies for each consequence, responses were rarely at 5 or more. This observation led us to truncate the measure and recode responses where 0 = never experienced consequence, 1 = 1 time, 2 = 2 times, 3 = 3 times, and 4 = 4 or more times. This recoding has been used in prior studies (see Glenn et al., 2022). We then summed across each semester to achieve an estimate of the total number of blackouts students experienced throughout college (T2–T8 Cronbach's α = .89).
AUD risk symptoms (T1, T8). AUD risk symptoms were assessed in the final semester of college using 15 items adapted from the YAACQ (Read et al., 2006), 1 item from the Young Adult Alcohol Problems Screening Test (YAAPST; Hurlbut & Sher, 1992), and 3 items adapted from the YAACQ and YAAPST (Cleveland et al., 2018, Glenn et al., 2022, Mallett et al., 2015, Reavy et al., 2016). The 19 items were selected to map onto 8 of the 11 current symptoms listed in the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5; American Psychiatric Association, 2013), AUD criteria (National Institute on Alcohol Abuse and Alcoholism, 2021). Table 1 provides a full description of the 19 items. Participants were asked to indicate the number of times they experienced (specific consequence) during the current semester. Responses were measured on a 9-point scale where 0 = never experienced consequence, 1 = 1 time, 2 = 2 times, 3 = 3 times, 4 = 4–6 times, 5 = 7–11 times, 6 = 12–20 times, 7 = 21–39 times, and 8 = 40 or more times. First, responses to the 19 items were recoded to a binary scale where 0 = symptom not present and 1 = symptom present. Following the recoding of the response scales for all 19 items, on DSM-5 criteria symptoms where there were multiple items mapped to the symptom (e.g., Spent a lot of time drinking? Or being sick or getting over other aftereffects?) the items were summed and recoded to indicate 0 = symptom not present and 1 = symptom present. On items where the DSM-5 criteria required symptoms to be present more than once (e.g., More than once wanted to cut down or stop drinking, or tried to, but couldn't), items mapped to that symptom were summed and recoded to a binary scale where 0 = symptom present 1 or fewer times and 1 = symptom present at least 2 times. For example, if a participant reported experiencing trying to quit drinking 1 time and thinking about stopping or cutting down from drinking 1 time, they were coded as having the DSM-5 symptom of, “More than once wanted to cut down or stop drinking, or tried to, but couldn't?”. This resulted in 8 DSM-5 items that were coded as 0 = symptom not present and 1 = symptom present. Finally, the 8 DSM-5 items were summed to achieve an estimate of the total number of AUD risk symptoms students experienced in their last semester of college (T8—19 items, α = .88, T8—8 AUD symptoms, α = .79). Only 11 of the 20 items were measured at baseline. The covariate for baseline AUD risk symptoms assesses 5 of the study's 8 AUD risk symptoms (T1: 11 items, α = .76; T1: 5 AUD symptoms, α = .67).
Table 1.
Description of DSM-5 measure and items
| DSM-5 AUD symptom | Description of item(s) used for symptom |
|---|---|
| 1). Had times when you ended up drinking more, or longer, than you intended? | 1a). I drank more than I originally had planned.a,e 1b). I have ended up drinking on nights when I had planned not to drink.a,e |
| 2). More than once wanted to cut down or stop drinking, or tried to, but couldn’t? | 2a). I have tried to quit drinking because I thought I was drinking too much.a,e 2b). I have thought about needing to cut down or stop drinking.a,e |
| 3). Spent a lot of time drinking? Or being sick or getting over other aftereffects? | 3a). I have felt very sick to my stomach or thrown up after drinking.a,d,e 3b). I have spent too much time drinking.a,e |
| 4). Found that drinking—or being sick from drinking—often interfered with taking care of your home or family? Or caused job troubles? Or school problems? | 4a). I have not gone to work or have missed class because of drinking, a hangover, or other illness caused by drinking.a,d,e 4b). The quality of my work or schoolwork has suffered because of drinking.a,d,e 4c). My drinking has created problems between myself and my boyfriend/girlfriend/spouse/parents, or other near relatives.a,d,e |
| 5). Continued to drink even though it was causing trouble with your family or friends? | 5a). I have neglected my obligations to family, work, or school because of drinking.a,e |
| 6). More than once gotten into situations while or after drinking that increased your chances of getting hurt (such as driving, swimming, using machinery, walking in a dangerous area, or having unsafe sex)? | 6a). I have been injured or my physical appearance has been harmed by my drinking.c,d,e 6b). I have been pressured or forced to have sex with someone because I was too drunk to prevent it.b,d,e 6c). I have started a serious argument or fight with someone while drinking.c,d,e 6d). I have made inappropriate sexual advances toward someone after drinking.c,d,e 6e). I have driven a car when I knew I had too much to drink to drive.a,d,e |
| 7). Had to drink much more than you once did to get the effect you want? Or found that your usual number of drinks had much less effect than before? | 7a). I have found that I needed larger amounts of alcohol to feel any effect, or that I could no longer get high/drunk on the amount that used to get me high or drunk.a,d,e |
| 8). Found that when the effects of alcohol were wearing off, you had withdrawal symptoms, such as trouble sleeping, shakiness, restlessness, nausea, sweating, a racing heart, or a seizure? Or sensed things that were not there? | 8a). I have had a hangover (headache, sick stomach) the morning after drinking.a,d,e 8b). I have had “the shakes” after stopping or cutting down on drinking (e.g., hands shake so that coffee cup rattles in the saucer or have trouble lighting a cigarette).a,e 8c). I have felt anxious, agitated, or restless after stopping or cutting down on drinking.a,e |
Notes: DSM-5 = Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition; AUD = alcohol use disorder; YAACQ = Young Adult Alcohol Consequences Questionnaire; YAAPST = Young Adult Alcohol Problems Screening Test.
Item from YAACQ;
item from YAAPST;
item adapted from YAACQ or YAAPST;
item asked at T1;
item asked at T8.
Control variables.
High school drinking (T1): High school drinking was assessed using items adapted from the DDQ (Collins et al., 1985). The DDQ asked students to consider a week during their senior year of high school. It captured how much alcohol students drank in a typical week during their senior year. Responses for each of the 7 days were summed to create a measure of typical weekly drinking during participants’ senior year of high school.
High school blackouts (T1): High school blackouts were measured using a single item adapted from the YAACQ (Read et al., 2006). Participants were asked to think back to their senior year of high school and indicate whether they had ever drunk to the point where they could not remember large stretches of time while drinking. Responses were on a dichotomous scale with yes (1) and no (0).
Age at onset of drinking (T1): Age at onset of drinking was measured by asking participants, “How old were you the first time you drank alcohol (that is, more than a few sips)?”. Response options included I have never drunk alcohol, Age 10 or younger, 11, 12, 13, 14, 15, 16, 17, 18, or 19. This scale has been used in multiple studies (e.g., Hingson et al., 2006; Mallett et al., 2010). Because of low responses in younger age categories, responses were recoded to 0 (age 13 or younger), 1 (14), 2 (15), 3 (16), 4 (17), and 5 (18–19).
Family history of AUD (T1): Students responded to 5 items indicating if they believed any of their biological relatives experienced problems with alcohol or had been alcoholics. The relatives included biological mother, biological father, one or more of your biological siblings, grandparents (biological mother's side), and grandparents (biological father's side). Response options were on a 3-point scale with no (0), yes (1), and not applicable (9). Not applicable items were recoded to a score of 0. Responses for all 5 items were summed. Scores ranging from 1 to 5 were recoded to 1 to indicate family history of AUD.
Analytic plan
Descriptive statistics were conducted using IBM SPSS Statistics for Windows, Version 29 (IBM Corp., Armonk, NY) to examine the total number of blackouts across each year of college and by sex and to provide frequencies for blackouts and AUD risk symptoms. Zero-order correlations were used to assess the associations between the constructs and outcomes. To test H1 to H3, a path model was examined using MPlus 8 (Muthén & Muthén, 2017). The theoretical model (Figure 1) included covariates for high school drinking, high school blackouts, T1 drinking, T1 blackouts, 5 of 8 AUD risk symptoms, age at onset drinking, family history of AUD, and sex. Missing values were analyzed using full-information maximum likelihood. The model was estimated using bootstrapped samples (N = 2,000) to account for non-normality in drinking, blackouts, and AUD risk outcomes. Significant direct associations were derived by examining 95% asymmetrical confidence intervals (CIs) surrounding the parameter estimates of the unstandardized paths. Significant indirect effects were derived by examining bootstrapped asymmetrical 95% CIs surrounding the parameter estimates of the product of the paths reflecting the effect (e.g., the product of the path between T1 willingness, T2–T8 blackouts, and T8 AUD risk symptoms).
Results
Participants
At the baseline survey, the average age of the participants was 18.2 (SD = 0.4) years. The majority of participants identified as female (56%) and White (87.3%). A minority of participants identified as Hispanic (5.1%), Asian (4.7%), Black (3.3%), and multiracial (2.9%). Retention from each survey (e.g., T1 to T2, T1 to T3, etc.,) ranged from 86% to 90%. Final retention from T1 to T8 was 87%. There were no significant differences on sex, race, ethnicity, or our main outcomes of interest for those who participated in the research versus those who did not.
Descriptive statistics
Participants reported an average willingness to experience a blackout score of -1.90 (SD = 1.52) and an average intention to avoid experiencing a blackout score of 1.93 (SD = 1.60). Between T2 and T8, participants reported drinking on average 12.48 (SD = 8.79) drinks in a typical week of college. During the first semester (T1), the average number of drinks during a typical week of college was 10.84 (SD = 8.66). Table 2 provides descriptive statistics examining blackouts by year and sex and describes frequencies of blackouts and AUD risk symptoms reported by college student drinkers. During 4 years of college (T1–T8), students experienced an estimated number of 8.16 blackouts (SD = 8.08). Between T2 and T8 (the total blackout variable used in the statistical model), the average number of blackouts was 7.25 (SD = 7.27). During the first semester of college, the average number of blackouts was 0.99 (SD = 1.37). Students also experienced approximately 2 blackouts during each year of college (e.g., T1–T2, T3–T4). Men experienced significantly more total blackouts (T1–T8) during college than women (t = 2.35, p = .02). Approximately 88% of the sample indicated that they experienced at least 1 of the 8 AUD risk symptoms at T8.
Table 2.
Descriptive statistics on blackouts and alcohol use disorder (AUD) risk symptoms

| Variable | n | M | SD | Range |
|---|---|---|---|---|
| Blackouts by year | ||||
| Year 1 (T1–T2) | 2,024 | 1.9 | 2.3 | 0–8 |
| Year 2 (T3–T4) | 1,871 | 2.1 | 2.4 | 0–8 |
| Year 3 (T5–T6) | 1,817 | 2.2 | 2.5 | 0–8 |
| Year 4 (T7–T8) | 1,815 | 2.0 | 2.3 | 0–8 |
| Total (T1–T8) | 1,387 | 8.2 | 8.1 | 0–32 |
| Total blackouts (T1–T8) by sex* | ||||
| Male | 552 | 8.8 | 8.4 | 0–32 |
| Female | 835 | 7.7 | 7.8 | 0–32 |
| n | % | Range | ||
|---|---|---|---|---|
| Proportion of total blackouts (T1–T8) | ||||
| 0 | 257 | 18.5% | 0–32 | |
| 1–4 | 362 | 26.2% | ||
| 5–8 | 230 | 16.6% | ||
| 9–12 | 172 | 12.3% | ||
| 13 or more | 366 | 26.4% | ||
| AUD risk symptoms (T8) | ||||
| 0 | 206 | 12% | 0–8 | |
| 1 | 123 | 7.2% | ||
| 2 | 201 | 11.7% | ||
| 3 | 364 | 21.2% | ||
| 4 | 307 | 17.8% | ||
| 5 | 213 | 12.4% | ||
| 6 | 171 | 9.9% | ||
| 7 | 78 | 4.5% | ||
| 8 | 57 | 3.3% |
Notes: Independent sample t test revealed significant differences in total blackouts (T1–T8) by sex (*p = .02). The total n for blackouts by year, proportion of total blackouts, and AUD risk symptoms may not add up to 2,024 participants because of missing data; only participants with complete data for each timepoint are included in this number.
During participants’ senior year of high school, students reported on average 5.46 drinks during a typical week (SD = 6.61) and 489 (24.2%) reported experiencing a blackout. A total of 123 students (6.1%) started drinking at age 13 or younger, 232 (11.5%) at age 14, 355 (17.5%) at age 15, 562 (27.8%) at age 16, 429 (21.2%) at age 17, and 319 (15.8%) at ages 18 or 19. Approximately 1,403 (69.3%) of the sample reported no family history of AUD and 618 (30.5%) reported a family history of AUD.
Path model statistics and results
Table 3 includes the correlation matrix of the observed variables of interest. Almost all correlations were significant at the .01 level with small (e.g., .05) to large (e.g., ≥.7) effect sizes. The statistical path model examined indicated good model fit (root mean square error of approximation = .05, 90% CI [.04, .06], p = .64; comparative fit index = .99; Tucker–Lewis index = .94; standardized root mean squared residual = .03). The unstandardized path coefficients are shown in Figure 2.
Table 3.
Correlation matrix of observed variables of interest
| Variable | 1. | 2. | 3. | 4. | 5. | 6. | 7. | 8. | 9. | 10. | 11. | 12. | 13. |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1. Willingness (T1) | – | ||||||||||||
| 2. Intentions (T1) | -.48** | – | |||||||||||
| 3. Drinking (T2–T8) | .33** | -.25** | – | ||||||||||
| 4. Blackouts (T2–T8) | .43** | -.30** | .68** | – | |||||||||
| 5. AUD (T8) | .20** | -.13** | .46** | .50** | – | ||||||||
| 6. H.S. drinking (T1) | .38** | -.26** | .50** | .41** | .19** | – | |||||||
| 7. H.S. blackouts (T1) | .42** | -.26** | .31** | .43** | .17** | .44** | – | ||||||
| 8. Drinking (T1) | .44** | -.29** | .65** | .52** | .28** | .69** | .40** | – | |||||
| 9. Blackouts (T1) | .53** | -.34** | .41** | .56** | .24** | .43** | .55** | .57** | – | ||||
| 10. AUD (T1) | .37** | -.24** | .42** | .48** | .34** | .40** | .35** | .58** | .59** | – | |||
| 11. Age at onset (T1) | -.25** | .19** | -.32** | -.35** | -.15** | -.49** | -.35** | -.41** | -.33** | -.33** | – | ||
| 12. Family history (T1) | .02 | .02 | -.02 | .01 | .04 | .04 | .07** | .03 | .04 | .04* | -.10** | – | |
| 13. Sex (T1) | -.20** | .16** | -.30** | -.07* | .01 | -.23** | -.07** | -.24** | -.05* | -.02 | .02 | .05* | – |
Notes: H.S. = high school. (*p < .05; **p < .01). Correlations at or above .25 are bolded because they are equal to or greater than an effect size (using r2) of .05.
Figure 2.
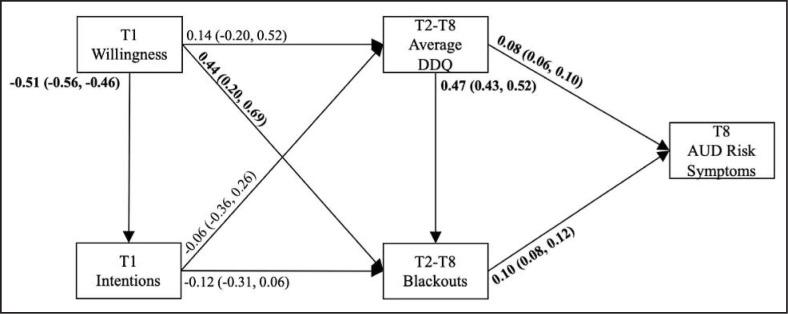
Path model. DDQ = Daily Drinking Questionnaire; AUD = alcohol use disorder. Unstandardized beta values and asymmetrical 95% confidence intervals reported. Bold values are significant.
Direct effects. Table 4 includes all model path statistics for significant direct effects. T1 willingness was negatively associated with T1 intentions (b = -0.51, 95% CI [-0.56, -0.46]). T1 willingness was positively associated with T2–T8 total blackouts (b = 0.44, 95% CI [0.20, 0.69]). T2–T8 drinking was positively associated with T2–T8 blackouts (b = 0.47, 95% CI [0.43, 0.52]). T2–T8 drinking (b = 0.08, 95% CI [0.06, 0.10]) and T2–T8 total blackouts (b = 0.10, 95% CI [0.08, 0.12]) were positively associated with T8 AUD risk symptoms. No other significant direct paths were observed.
Table 4.
Final model statistics for direct effects

| Paths | b | SE | [95% CI] |
|---|---|---|---|
| Outcome | |||
| AUD (T8) | |||
| Predictors | |||
| Drinking (T2–T8) | 0.08 | 0.01 | [0.06, 0.10] |
| Blackouts (T2–T8) | 0.10 | 0.01 | [0.08, 0.12] |
| Covariates | |||
| H.S. drinking (T1) | -0.02 | 0.01 | [-0.04, 0.01] |
| H.S. blackouts (T1) | -0.08 | 0.14 | [-0.34, 0.20] |
| Drinking (T1) | -0.02 | 0.01 | [-0.04, -0.01] |
| Blackouts (T1) | -0.17 | 0.05 | [-0.27, -0.08] |
| DSM (T1) | 0.25 | 0.04 | [0.17, 0.32] |
| Age at onset (T1) | 0.06 | 0.04 | [-0.01, 0.14] |
| Family history (T1) | 0.19 | 0.09 | [0.01, 0.36] |
| Sex (T1) | 0.43 | 0.10 | [0.25, 0.62] |
| Outcome | |||
| Drinking (T2–T8) | |||
| Predictors | |||
| Willingness (T1) | 0.14 | 0.18 | [-0.20, 0.52] |
| Intentions (T1) | -0.06 | 0.16 | [-0.36, 0.26] |
| Covariates | |||
| H.S. drinking (T1) | 0.09 | 0.06 | [-0.02, 0.22] |
| H.S. blackouts (T1) | 0.33 | 0.55 | [-0.76, 1.40] |
| Drinking (T1) | 0.51 | 0.05 | [0.41, 0.62] |
| Blackouts (T1) | 0.27 | 0.22 | [-0.16, 0.70] |
| DSM (T1) | 0.49 | 0.17 | [0.17, 0.82] |
| Age at onset (T1) | -0.30 | 0.16 | [-0.61, 0.03] |
| Family history (T1) | -0.58 | 0.37 | [-1.28, 0.12] |
| Sex (T1) | -3.01 | 0.38 | [-3.71, -2.24] |
| Outcome | |||
| Blackouts (T2–T8) | |||
| Predictors | |||
| Drinking (T2–T8) | 0.47 | 0.02 | [0.43, 0.52] |
| Willingness (T1) | 0.44 | 0.12 | [0.20, 0.69] |
| Intentions (T1) | -0.12 | 0.09 | [-0.31, 0.06] |
| Covariates | |||
| H.S. drinking (T1) | -0.01 | 0.03 | [-0.08, 0.06] |
| H.S. blackouts (T1) | 1.94 | 0.41 | [1.12, 2.74] |
| Drinking (T1) | -0.08 | 0.03 | [-0.14, -0.01] |
| Blackouts (T1) | 1.14 | 0.17 | [0.81, 1.46] |
| DSM (T1) | 0.42 | 0.12 | [0.19, 0.65] |
| Age at onset (T1) | -0.21 | 0.11 | [-0.41, 0.01] |
| Family history (T1) | -0.09 | 0.26 | [-0.56, 0.47] |
| Sex (T1) | 1.83 | 0.27 | [1.31, 2.34] |
| Outcome | |||
| Intentions (T1) | |||
| Predictor | |||
| Willingness (T1) | -0.51 | 0.02 | [-0.56, -0.46] |
Notes: CI = confidence interval; AUD = alcohol use disorder; H.S. = high school; DSM = Diagnostic and Statistical Manual of Mental Disorders. Beta values unstandardized. Bolded b values indicate significant 95% asymmetrical CIs.
Indirect effects. Table 5 includes all model path statistics for indirect effects. T1 willingness significantly indirectly affected T8 AUD risk symptoms through its association with T2–T8 blackouts (b = 0.05, 95% CI [0.02, 0.07]). No other significant indirect paths were observed.
Table 5.
Final model statistics for indirect effects
| Paths (Predictor) → Mediator → Outcome | b | SE | [95% CI] |
|---|---|---|---|
| Willingness (T1) → Drinking (T2–T8) → AUD Risk Symptoms (T8) | 0.01 | 0.01 | [-0.02, 0.04] |
| Intentions (T1) → Drinking (T2–T8) → AUD Risk Symptoms (T8) | 0.00 | 0.01 | [-0.03, 0.02] |
| Willingness (T1) → Blackouts (T2–T8) → AUD Risk Symptoms (T8) | 0.05 | 0.01 | [0.02, 0.07] |
| Intentions (T1) → Blackouts (T2–T8) → AUD Risk Symptoms (T8) | -0.01 | 0.01 | [-0.03, 0.01] |
Notes: CI = confidence interval; AUD = alcohol use disorder. Beta values unstandardized. Bolded b values indicate significant 95% asymmetrical CIs.
Discussion
The first aim of the current study estimated that college student drinkers experienced an estimated number of 8 blackouts throughout college and approximately 2 blackouts during each year of college. Men experienced significantly (e.g., 8.8) more blackouts than women (e.g., 7.7). This finding builds on past research (Chartier et al., 2011) suggesting that male students experience significantly more blackouts throughout college than female students. A small portion of the sample (18.5%) reported never experiencing a blackout during college. Approximately 1,514 (88%) students reported experiencing at least 1 of 8 AUD risk symptoms in the final semester of college.
The second aim of the study was to use a dual-process decision-making model to examine the longitudinal associations between willingness to experience a blackout, intentions to avoid a blackout, drinking, blackouts, and AUD risk symptoms. Partial support was observed for H1 proposing that willingness to experience a blackout would be positively associated with drinking and blackouts. Willingness was positively associated with blackouts. These findings are consistent with past research, which has found associations between willingness, blackouts, and other alcohol-related consequences among college student drinkers (Glenn et al., 2022; Litt et al., 2014; Trager et al., 2019). Willingness was not associated with drinking. These findings are not consistent with past research, which has found positive associations between willingness and alcohol use (Glenn et al., 2022; Mallett et al., 2011). One explanation for the difference in these findings is that past studies have examined willingness to experience multiple consequences and not the single blackout item. These findings suggest that willingness to experience a blackout is not a proxy for willingness to drink.
Partial support was observed for H2 proposing that intentions to avoid a blackout would be negatively associated with drinking and would have no association with blackouts. Merrill and colleagues (2022) suggested that intentions to experience a blackout may be students expressing their intention to get drunk. According to this idea, we expected that students who intended to avoid a blackout would drink less and students who did not intend to avoid a blackout would drink more. Our findings were not consistent with this idea as we did not find a significant association between intentions and drinking. However, our results are consistent with past research, which suggested that intentions to avoid multiple consequences had no association with future drinking behaviors (Mallett et al., 2015). Intentions were not associated with blackouts. Past studies have suggested that willingness is a stronger predictor than intentions when assessing high-risk drinking behaviors like blackouts (Litt et al., 2014; Merrill et al., 2022). Our findings confirm previous research by suggesting that willingness, but not intentions, is associated with experiencing more blackouts throughout college.
Full support was observed for H3, which proposed that drinking and blackouts would be positively associated with AUD risk symptoms. Students who consumed more alcohol and experienced a higher number of blackouts throughout college experienced more AUD risk symptoms in their last semester of college. This finding is consistent with past studies suggesting that higher levels of drinking in young adulthood are associated with future AUD risk symptoms (Benjet et al., 2022; Tavolacci et al., 2019). These findings also extend previous research suggesting that blackouts are uniquely associated with future AUD risk symptoms among young adults independent of drinking (Studer et al., 2019; Yuen et al., 2021).
Finally, results from hypotheses H1 and H3 suggest that willingness to experience a blackout indirectly affected last semester AUD risk symptoms through its associations with the total number of blackouts experienced throughout college. Students who were more willing to experience a blackout in the first semester of college experienced more blackouts throughout college and subsequently experienced more AUD risk symptoms in the last semester of college.
Implications
Findings from the current study have several important implications for interventions. First, these findings underscore the importance of changing students’ willingness toward experiencing a blackout and reducing student drinking. Changing students’ willingness to experience a blackout is a crucial factor to reduce future blackouts and AUD risk symptoms. Students may not perceive blackouts as an aversive experience and subsequently downplay their severity (Mallett et al., 2008). Second, many college student drinking interventions are delivered to students before starting college and/or during the first semester of college (e.g., see Hultgren et al., 2019; Riordan et al., 2015). Results from the current study suggest that students who are drinking at higher levels and experiencing more blackouts reported throughout college experienced more AUD risk symptoms in the final semester of college. These students may benefit from additional interventions delivered during the final year of college. These interventions should focus on reducing students’ drinking and the number of blackouts they experience. Further, screenings for blackouts and AUD risk symptoms (e.g., during visits to health services; ScreenU for alcohol; https://screenu.org) may be a useful way to identify students experiencing symptoms of AUD and offer an opportunity to provide intervention or resources for treatment services.
Limitations
The current study is not without limitations. First, participants in this study were recruited from a single large public university where the majority of students identified as White. This recruitment method is common to longitudinal studies published on college drinking (e.g., Marino & Fromme, 2016; Merrill et al., 2016). Although drinking rates at the university students were recruited from are similar to those at other large universities with respect to national drinking norms (Johnston et al., 2019), these findings may not be generalizable to all college students, such as those attending community college and to non–college-attending young adults. Second, blackouts were assessed using a single item adapted from the YAACQ (Read et al., 2006). However, there are two types of blackouts often categorized as an absence of memory for all (en bloc) or part (fragmentary) of a drinking episode (Goodwin et al., 1969; Hingson et al., 2016; Miller et al., 2018a). The current study was not able to distinguish between the two types of blackouts. The question used to assess blackouts in the current study (i.e., unable to remember large stretches of time) closely matches an en bloc blackout (Boness et al., 2022). Future work should examine the associations between fragmentary blackouts, en bloc blackouts, and AUD risk symptoms among college student drinkers. Third, this study relies on self-report measurement of blackouts, a topic characterized by memory loss. Future research should address blackouts using ambulatory assessment methods. Fourth, our estimate for the total number of blackouts experienced during college (T1–T8 descriptive item and T2–T8 analytic item) was calculated only for individuals with complete data at these timepoints. Individuals with incomplete data at any timepoint were coded as missing. This decision was made in an effort to avoid underestimating the total number of blackouts students experienced during college. Although individuals with missing data at any timepoint reported on average more blackouts during each semester (e.g., T1, T2, etc.), the mean differences were very small. For example, at T4 students with missing data at any timepoint reported on average 1.37 blackouts and students with no missing data reported on average 1.15 blackouts. Fifth, the DSM-5 lists criteria for evaluating the severity of AUD symptoms (e.g., mild, moderate, severe). The current study only examined 8 of the 11 DSM-5 symptoms for AUD at T8. Our findings are not meant to diagnose individuals with AUD but to identify those who are experiencing AUD risk symptoms. Since we did not evaluate all 11 DSM-5 symptoms, we chose to not examine our findings by the severity of symptoms. Future studies using the full DSM-5 AUD symptoms should explore the associations between blackouts and severity of AUD. Sixth, because of the need to collect a lot of background and screening information at baseline, we reduced respondent burden by only asking students to report on 11 of the 19 AUD risk items at baseline. Therefore, we were unable to control for all AUD risk symptoms participants could have experienced at baseline. Finally, our analytic approach examining our associations using a path model does not disaggregate between- and within-person associations in the exact way alternative analytic approaches (e.g., multilevel models) do. However, our model includes T1 measures of our outcomes (drinking, blackouts, and AUD risk). Therefore, associations can be interpreted as predictions of within-person change in outcomes because controlling for baseline levels allows prediction of the residualized change (see, e.g., Castro-Schilo & Grimm, 2018). Future research may benefit from using other analytic approaches such as multilevel models to fully disaggregate between- and within-person associations.
Conclusions
Results from the current study estimated that college student drinkers experienced 8 blackouts during college. Approximately 88% of the sample indicated that they experienced at least 1 of 8 AUD risk symptoms in the last semester of college. Evidence from this study also suggests that students’ willingness to experience a blackout influenced AUD risk symptoms through students’ total blackouts experienced throughout college.
Footnotes
This work was supported by National Institute on Alcohol Abuse and Alcoholism Grant R01AA021117 (principal investigator: Kimberly A. Mallett) and National Institute on Drug Abuse Grant T32DA017629 (multiple principal investigators: Jennifer Maggs and Stephanie Lanza). The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
References
- American Psychiatric Association. Diagnostic and statistical manual of mental disorders. 5th ed. Arlington, VA: Author; 2013. [Google Scholar]
- Benjet C., Mortier P., Kiekens G., Ebert D. D., Auerbach R. P., Kessler R. C., Cuijpers P., Green J. G., Nock M. K., Demyttenaere K., Albor Y., Bruffaerts R. A risk algorithm that predicts alcohol use disorders among college students. European Child & Adolescent Psychiatry. 2022;31(7):1–11. doi: 10.1007/s00787-020-01712-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Boness C. L., Gatten N., Treece M. K., Miller M. B. A mixed-methods approach to improve the measurement of alcohol-induced blackouts: ABOM-2. Alcoholism: Clinical and Experimental Research. 2022;46(8):1497–1514. doi: 10.1111/acer.14882. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Castro-Schilo L., Grimm K. J. Using residualized change versus difference scores for longitudinal research. Journal of Social and Personal Relationships. 2018;35(1):32–58. doi: 10.1177/0265407517718387. [DOI] [Google Scholar]
- Chartier K. G., Hesselbrock M. N., Hesselbrock V. M. Alcohol problems in young adults transitioning from adolescence to adulthood: The association with race and gender. Addictive Behaviors. 2011;36(3):167–174. doi: 10.1016/j.addbeh.2010.10.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cleveland M. J., Mallett K. A., Turrisi R., Sell N. M., Reavy R., Trager B. Using latent transition analysis to compare effects of residency status on alcohol-related consequences during the first two years of college. Addictive Behaviors. 2018;87:276–282. doi: 10.1016/j.addbeh.2018.06.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Collins L., Graham J. W., Hansen W. B., Johnson C. A. Agreement between retrospective accounts of substance use and earlier reported substance use. Applied Psychological Measurement. 1985;9(3):301–309. doi: 10.1177/014662168500900308. [DOI] [Google Scholar]
- Gerrard M., Gibbons F. X., Houlihan A. E., Stock M. L., Pomery E. A. A dual-process approach to health risk decision making: The prototype willingness model. Developmental Review. 2008;28(1):29–61. doi: 10.1016/j.dr.2007.10.001. [DOI] [Google Scholar]
- Glenn S. D., Turrisi J., Waldron K. A., Mallett K. A., Russell M. A., Reavy R. R. Examining the longitudinal associations between what early college experiences influence individuals’ experiencing more total consequences. Addictive Behaviors. 2022;132:107357. doi: 10.1016/j.addbeh.2022.107357. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gibbons F. X.Intention, expectation, and willingness. 2020. https://cancercontrol.cancer.gov/brp/research/constructs/intention-expectation-willingness
- Gibbons F. X., Gerrard M., Blanton H., Russell D. W. Reasoned action and social reaction: Willingness and intention as independent predictors of health risk. Journal of Personality and Social Psychology. 1998;74(5):1164–1180. doi: 10.1037/0022-3514.74.5.1164. [DOI] [PubMed] [Google Scholar]
- Gibbons F. X., Houlihan A. E., Gerrard M. Reason and reaction: The utility of a dual-focus, dual-processing perspective on promotion and prevention of adolescent health risk behaviour. British Journal of Health Psychology. 2009;14(Pt 2):231–248. doi: 10.1348/135910708X376640. [DOI] [PubMed] [Google Scholar]
- Goodwin D. W., Crane J. B., Guze S. B. Alcoholic “blackouts”: A review and clinical study of 100 alcoholics. American Journal of Psychiatry. 1969;126(2):191–198. doi: 10.1176/ajp.126.2.191. [DOI] [PubMed] [Google Scholar]
- Gruber E., DiClemente R. J., Anderson M. M., Lodico M. Early drinking onset and its association with alcohol use and problem behavior in late adolescence. Preventive Medicine. 1996;25(3):293–300. doi: 10.1006/pmed.1996.0059. [DOI] [PubMed] [Google Scholar]
- Hingson R., Zha W., Simons-Morton B., White A. Alcohol induced blackouts as predictors of other drinking related harms among emerging young adults. Alcoholism: Clinical and Experimental Research. 2016;40(4):776–784. doi: 10.1111/acer.13010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hingson R. W., Heeren T., Winter M. R. Age at drinking onset and alcohol dependence: Age at onset, duration, and severity. Archives of Pediatrics & Adolescent Medicine. 2006;160(7):739–746. doi: 10.1001/archpedi.160.7.739. [DOI] [PubMed] [Google Scholar]
- Hultgren B. A., Turrisi R., Cleveland M. J., Mallett K. A., Reavy R., Larimer M. E., Geisner I. M., Hospital M. M. Transitions in drinking behaviors across the college years: A latent transition analysis. Addictive Behaviors. 2019;92:108–114. doi: 10.1016/j.addbeh.2018.12.021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hultgren B. A., Turrisi R., Mallett K. A., Ackerman S., Larimer M. E., McCarthy D., Romano E. A longitudinal examination of decisions to ride and decline rides with drinking drivers. Alcoholism: Clinical and Experimental Research. 2018;42(9):1748–1755. doi: 10.1111/acer.13818. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hurlbut S. C., Sher K. J. Assessing alcohol problems in college students. Journal of American College Health. 1992;41(2):49–58. doi: 10.1080/07448481.1992.10392818. [DOI] [PubMed] [Google Scholar]
- Jellinek E. M. Phases of alcohol addiction. Quarterly Journal of Studies on Alcohol. 1952;13(4):673–684. doi: 10.15288/qjsa.1952.13.673. [DOI] [PubMed] [Google Scholar]
- Jennison K. M., Johnson K. A. Drinking-induced blackouts among young adults: Results from a national longitudinal study. International Journal of the Addictions. 1994;29(1):23–51. doi: 10.3109/10826089409047367. [DOI] [PubMed] [Google Scholar]
- Johnston L. D., Miech R. A., O’Mally P. M., Bachman J. G., Schulenberg J. E., Patrick M. E. Monitoring the Future National Survey Results on Drug Use 1975–2018: Overview, Key Findings on Adolescent Drug Use. Institute for Social Research, The University of Michigan; 2019. http://monitoringthefuture.org/pubs.html#monographs [Google Scholar]
- LaBrie J. W., Hummer J., Kenney S., Lac A., Pedersen E. Identifying factors that increase the likelihood for alcohol-induced blackouts in the prepartying context. Substance Use & Misuse. 2011;46(8):992–1002. doi: 10.3109/10826084.2010.542229. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Litt D. M., Lewis M. A., Patrick M. E., Rodriguez L., Neighbors C., Kaysen D. L. Spring break versus spring broken: Predictive utility of spring break alcohol intentions and willingness at varying levels of extremity. Prevention Science. 2014;15(1):85–93. doi: 10.1007/s11121-012-0355-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Mallett K. A., Bachrach R. L., Turrisi R. Are all negative consequences truly negative? Assessing variations among college students’ perceptions of alcohol related consequences. Addictive Behaviors. 2008;33(10):1375–1381. doi: 10.1016/j.addbeh.2008.06.014. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Mallett K. A., Ray A. E., Turrisi R., Belden C., Bachrach R. L., Larimer M. E. Age of drinking onset as a moderator of the efficacy of parent-based, brief motivational, and combined intervention approaches to reduce drinking and consequences among college students. Alcoholism: Clinical and Experimental Research. 2010;34(7):1154–1161. doi: 10.1111/j.1530-0277.2010.01192.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Mallett K. A., Turrisi R., Cleveland M. J., Scaglione N. M., Reavy R., Sell N. M., Varvil-Weld L. A dual-process examination of alcohol-related consequences among first-year college students. Journal of Studies on Alcohol and Drugs. 2015;76(6):862–871. doi: 10.15288/jsad.2015.76.862. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Mallett K. A., Varvil-Weld L., Turrisi R., Read A. An examination of college students’ willingness to experience consequences as a unique predictor of alcohol problems. Psychology of Addictive Behaviors. 2011;25(1):41–47. doi: 10.1037/a0021494. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Marino E. N., Fromme K. Alcohol-induced blackouts and maternal family history of problematic alcohol use. Addictive Behaviors. 2015;45:201–206. doi: 10.1016/j.addbeh.2015.01.043. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Marino E. N., Fromme K. Early onset drinking predicts greater level but not growth of alcohol-induced blackouts beyond the effect of binge drinking during emerging adulthood. Alcoholism: Clinical and Experimental Research. 2016;40(3):599–605. doi: 10.1111/acer.12981. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Merrill J. E., Boyle H. K., López G., Riordan B. C., Marie Ward, R., Rosen R. K., Carey K. B. Recent alcohol-induced blackouts among heavy drinking college students: A qualitative examination of intentions, willingness, and social context. Experimental and Clinical Psychopharmacology. 2022;30(6):831–840. doi: 10.1037/pha0000513. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Merrill J. E., Treloar H., Fernandez A. C., Monnig M. A., Jackson K. M., Barnett N. P. Latent growth classes of alcohol-related blackouts over the first 2 years of college. Psychology of Addictive Behaviors. 2016;30(8):827–837. doi: 10.1037/adb0000214. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Miller M. B., Davis C. N., Merrill J. E., DiBello A. M., Carey K. B. Intentions and motives to experience alcohol-induced blackout among young adults in college. Psychology of Addictive Behaviors. 2020;34(6):690–698. doi: 10.1037/adb0000572. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Miller M. B., Merrill J. E., DiBello A. M., Carey K. B. Distinctions in alcohol-induced memory impairment: A mixed methods study of en bloc versus fragmentary blackouts. Alcoholism: Clinical and Experimental Research. 2018a;42(10):2000–2010. doi: 10.1111/acer.13850. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Miller M. B., Merrill J. E., Singh S., DiBello A. M., Carey K. B. College student knowledge of blackouts and implications for alcohol intervention: A qualitative analysis. Psychology of Addictive Behaviors. 2018b;32(8):933–943. doi: 10.1037/adb0000419. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Muthén L. K., Muthén B. O. Mplus: Statistical analysis with latent variables: User’s guide (Version 8) Authors; 2017. [Google Scholar]
- National Institute on Alcohol Abuse and Alcoholism. Alcohol use disorder: A comparison between DSM-IV and DSM-5. 2021. https://www.niaaa.nih.gov/publications/brochures-and-fact-sheets/alcohol-use-disorder-comparison-between-dsm
- Pomery E. A., Gibbons F. X., Reis-Bergan M., Gerrard M. From willingness to intention: Experience moderates the shift from reactive to reasoned behavior. Personality and Social Psychology Bulletin. 2009;35(7):894–908. doi: 10.1177/0146167209335166. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ray A. E., Stapleton J. L., Turrisi R., Mun E.-Y. Drinking game play among first-year college student drinkers: An event-specific analysis of the risk for alcohol use and problems. American Journal of Drug and Alcohol Abuse. 2014;40(5):353–358. doi: 10.3109/00952990.2014.930151. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Read J. P., Kahler C. W., Strong D. R., Colder C. R. Development and preliminary validation of the young adult alcohol consequences questionnaire. Journal of Studies on Alcohol. 2006;67(1):169–177. doi: 10.15288/jsa.2006.67.169. [DOI] [PubMed] [Google Scholar]
- Reavy R., Cleveland M. J., Mallett K. A., Scaglione N. M., Sell N. M., Turrisi R. An examination of the relationship between consequence-specific normative belief patterns and alcohol-related consequences among college students. Alcoholism: Clinical and Experimental Research. 2016;40(12):2631–2638. doi: 10.1111/acer.13242. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Riordan B. C., Conner T. S., Flett J. A. M., Scarf D. A brief orientation week ecological momentary intervention to reduce university student alcohol consumption. Journal of Studies on Alcohol and Drugs. 2015;76(4):525–529. doi: 10.15288/jsad.2015.76.525. [DOI] [PubMed] [Google Scholar]
- Robertson A. A., Zhou Q. M., Tatch A., Walsh M. Gender-specific predictors of recidivism among DUI offenders. Journal of Studies on Alcohol and Drugs. 2019;80(6):641–650. doi: 10.15288/jsad.2019.80.641. [DOI] [PubMed] [Google Scholar]
- Scaglione N. M., Hultgren B. A., Reavy R., Mallett K. A., Turrisi R., Cleveland M. J., Sell N. M. Do students use contextual protective behaviors to reduce alcohol-related sexual risk? Examination of a dual-process decision-making model. Psychology of Addictive Behaviors. 2015;29(3):733–743. doi: 10.1037/adb0000113. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Studer J., Gmel G., Bertholet N., Marmet S., Daeppen J. B. Alcohol-induced blackouts at age 20 predict the incidence, maintenance and severity of alcohol dependence at age 25: A prospective study in a sample of young Swiss men. Addiction. 2019;114(9):1556–1566. doi: 10.1111/add.14647. [DOI] [PubMed] [Google Scholar]
- Tabachnick B. G., Fidell L. S. Using Multivariate Statistics 6. Allyn and Bacon; 2013. [Google Scholar]
- Tavolacci M. P., Berthon Q., Cerasuolo D., Dechelotte P., Ladner J., Baguet A. Does binge drinking between the age of 18 and 25 years predict alcohol dependence in adulthood? A retrospective case-control study in France. BMJ. 2019;9(5):e026375. doi: 10.1136/bmjopen-2018-026375. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Trager B. M., Mallett K. A., Turrisi R., Sell N. M., Hultgren B. A. Willingness as a mediator of the effects of personality on alcohol-related consequences between the first and second years of college: A longitudinal prospective study. Addictive Behaviors. 2019;89:172–177. doi: 10.1016/j.addbeh.2018.10.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Voloshyna D. M., Bonar E. E., Cunningham R. M., Ilgen M. A., Blow F. C., Walton M. A. Blackouts among male and female youth seeking emergency department care. American Journal of Drug and Alcohol Abuse. 2018;44(1):129–139. doi: 10.1080/00952990.2016.1265975. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wetherill R. R., Fromme K. Alcohol-induced blackouts: A review of recent clinical research with practical implications and recommendations for future studies. Alcoholism: Clinical and Experimental Research. 2016;40(5):922–935. doi: 10.1111/acer.13051. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wilhite E. R., Fromme K. Alcohol-induced blackouts and other negative outcomes during the transition out of college. Journal of Studies on Alcohol and Drugs. 2015;76(4):516–524. doi: 10.15288/jsad.2015.76.516. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wilhite E. R., Mallard T., Fromme K. A longitudinal event-level investigation of alcohol intoxication, alcohol-related blackouts, childhood sexual abuse, and sexual victimization among college students. Psychology of Addictive Behaviors. 2018;32(3):289–300. doi: 10.1037/adb0000353. [DOI] [PMC free article] [PubMed] [Google Scholar]
- White A. M. What happened? Alcohol, memory blackouts, and the brain. Alcohol Research & Health. 2003;27(2):186–196. [PMC free article] [PubMed] [Google Scholar]
- White A. M., Jamieson-Drake D. W., Swartzwelder H. S. Prevalence and correlates of alcohol-induced blackouts among college students: Results of an e-mail survey. Journal of American College Health. 2002;51(3):117–131. doi: 10.1080/07448480209596339. [DOI] [PubMed] [Google Scholar]
- Yuen W. S., Chan G., Bruno R., Clare P. J., Aiken A., Mattick R., Farrell M., Kypri K., Slade T., Hutchinson D., McBride N., McCambridge J., Boland V., Peacock A. Trajectories of alcohol-induced blackouts in adolescence: Early risk factors and alcohol use disorder outcomes in early adulthood. Addiction. 2021;116(8):2039–2048. doi: 10.1111/add.15415. [DOI] [PubMed] [Google Scholar]