Abstract
Migrants constitute a vulnerable segment of the population, particularly susceptible to various health challenges. Despite this, limited research has delved into the comparative health statuses of migrants and non-migrants in the rising elderly population. This study aims to bridge this gap by exploring health disparities between these two groups. Leveraging data from a nationally representative, large-scale Longitudinal Ageing Study in India (LASI) survey (n = 29002; 3103 Migrants and 25899 Non-migrants), this research focuses on four health indicators: self-rated health (SRH), depression, multimorbidity, and functional limitations. The study undertakes descriptive and bivariate analyses for migrant and non-migrant groups and employs propensity score matching techniques to fulfil its objectives. The findings reveal that for respective migrant and non-migrant populations, the prevalence of poor-SRH was 24.04 % and 16.29 %; depression was 12.32 % and 6.62 %; multimorbidity was 26.78 % and 15.71 %, and functional limitation was 28.35 % and 23.13 %. The study uncovers a 2.4 percentage point increase in poor self-rated health, a 1.0 percentage point rise in depression, and notably, a 4.2 and 1.0 percentage point elevation in multimorbidity and functional limitations among migrants relative to non-migrants. Evident from the outcomes is a stark health disparity, emphasising migrants' heightened vulnerability across multiple health dimensions. The implication of this research highlights the necessity for policy interventions aimed at eliminating health inequalities between migrant and non-migrant populations.
Keywords: Migration, Self-rated health, Depression, Multimorbidity, Functional limitation, India
Highlights
-
•
Revealing an essential, largely overlooked theme: health disparities among elderly migrants and non-migrants in India.
-
•
Migrants exhibit heightened vulnerability to poor-SRH, Depression, Multimorbidity and Functional limitations.
-
•
Health policies should be framed with targeted interventions to ensure that migrant populations are not left excluded.
1. Introduction
Increased longevity and declining fertility rates have led to the greying of the population worldwide. In 2019, there were 703 million older people in the world, and by 2050, that number is projected to have doubled (World Population Prospects, 2019). According to estimates, there will be 330 million senior citizens in India by 2050, which will account for 19.4 % of the country's total population (Sivaraju, Alam, & Verma, 2017). Likewise, there has been a significant surge in global international migration over the last twenty years, with the number of international migrants worldwide reaching over 281 million in 2020 from 173 million in 2000 (McAuliffe & Khadria, 1953). In India, there were around 319 million internal migrants in 2001, which increased to 450 million as of 2011; that number is expected to rise to a massive 600 million (Rajan & Bhagat, 2022a). However, despite being several times more substantial than international migration, internal migration has not gained as much attention (Wickramage, Vearey, Zwi, Robinson, & Knipper, 2018).
Migration can yield both positive and negative health consequences. On the positive end, migrants may discover better incomes, which may lead to better access to health care services in the destination places (Rajan, Bhagat, & Ram, 2022b; Rajan, 2022). On the contrary, migrants may be more susceptible to health issues due to various factors. These include psychological stress from the removal and resettlement procedure, alienation from their new environment, loss of social ties, a lower socioeconomic position, and language obstacles (Lu, 2010).
India is on the rise of chronic diseases (Singh, Chauhan, & Puri, 2023). The spectrum of chronic conditions extends beyond non-communicable diseases (NCDs) to encompass metabolic risk factors like obesity, hypertension, and high cholesterol, culminating in a surge of multimorbidity (MacKinnon et al., 2023; WHO, 2016). This burden is amplified in marginalised groups like migrants, accentuating health disparities (Sheikh et al., 2016). Additionally, migration engenders augmented functional health impediments due to socioeconomic discrepancies, cultural acclimatisation, constrained healthcare access, and psychosocial stressors, thereby compromising the wellbeing of migrants (Mandal, Pradhan, Mohanty, & Muhammad, 2023).
Empirical investigations on the health status of migrants, in contrast to that of non-migrant populations commonly reveal that, following their migration, migrants exhibit better health outcomes than the native populations despite having a comparatively disadvantaged socioeconomic status. This remains in the initial few years of migration, but with a longer stay, migrants lose this early health benefit (Juárez & Revuelta-Eugercios, 2016) Thus, the phenomenon is known as the Healthy Migrant Effect (HME); this phenomenon is quite evident among migrants in the developed and developing countries like Sweden (Helgesson, Johansson, Nordquist, Vingård, & Svartengren, 2019), Canada (McDonald & Kennedy, 2004), Netherlands, Belgium, and England (Reus-Pons, Kibele, & Janssen, 2017), South America (Cabieses, Tunstall, & Pickett, 2013), Australia (Anikeeva et al., 2012), Indonesia (Lu, 2008, 2010), China (Chen et al., 2022; Lu & Qin, 2014), Chile (Rada, Oyarte, & Cabieses, 2022). However, this also has some important contrast evidence worldwide; for example, a study in three European countries (Belgium, Netherlands, and England and Wales) found that non-migrants could be expected to live longer than migrants (Reus-Pons et al., 2017). Jatrana, Richardson, and Pasupuleti (2018) found mixed results in HME in the Australian context. They found that English-speaking migrants tend to report good health compared to native Australians; however, for all health outcomes, non-English-speaking migrants were at a disadvantage compared to native-born Australian people. (Dodd et al., 2017) examined HME in the Indian context, taking a relatively small sample in southern India, and found no significant difference in the health status of migrant and non-migrant persons.
Prior studies on migration and health in India primarily emphasised the adverse health impacts on migrants that result mainly from their participation in labour mobility (Dodd et al., 2017; Ravindranath & Mohan, 2022). Communicable disease among migrant workers was the major focus area, with a specific interest in HIV/AIDS (Saggurti et al., 2008, 2009) and malaria (Kumar et al., 2012). Additional studies have investigated health consequences linked to occupational health problems (Akram, 2014; Sarivaara, Uusiautti, & Määttä, 2013) and non-communicable diseases (Ebrahim et al., 2010; Sarivaara et al., 2013). Furthermore, very little literature suggests that migrants had an elevated risk of mental health problems than natives (Srivastava, Singh, Mishra, & Aditya, 2023). Ebrahim and colleagues found that rural-to-urban migrants had a higher risk of obesity and diabetes than their non-migrant urban counterparts (Ebrahim et al., 2010). Some Indian studies (Ebrahim et al., 2010; Mandal et al., 2023; Paul, Mandal, & Samanta, 2023; Srivastava et al., 2023) demonstrated that migrants are the vulnerable section of the population, exposed to various health issues. It remains inconclusive about the various exposures to health and how they act on migrant and non-migrant populations. No study attempted to investigate the difference in health status between migrants and non-migrants at later ages. Moreover, being a country with the second largest elderly population, more emphasis should be devoted to how these intersecting characteristics shape the ageing of migrant populations and find ways of addressing this within middle-aged and elderly-focused healthcare services (WHO, 2015). Hence, considering the limited research on migrant health disparities, this study recognises the nuanced health gap between migrant and non-migrant groups in India. Existing investigations into this disparity have predominantly focused on the global north. Nonetheless, the relevance of these findings to the global south, particularly within the Indian context, remains uncertain. To address this gap, the present pan-India study aims to elucidate the health disparity between migrants and non-migrants, contributing to a more comprehensive understanding of the issue.
2. Materials and methods
2.1. Data
The present study used the baseline survey of India's first nationally representative Longitudinal Ageing Study in India (LASI) conducted during 2017–2018. LASI is a national survey of health, social determinants, and wellbeing of middle-aged and older adults in India. This survey was conducted by the International Institute for Population Sciences (IIPS) in collaboration with the Harvard T.H. Chan School of Public Health and the University of Southern California (LASI, 2020). The LASI survey provides vital information on demographics, symptom-based health conditions, functional and mental health, family and social networks, household economic status, health insurance, healthcare utilisation, biomarkers, retirement, and life expectations across all of India's states and union territories (Bloom, Sekher, & Lee, 2021). This national survey adopted a multistage stratified area probability cluster sampling strategy, including a three-stage rural and four-stage urban sampling design. The initial step in each state/UT involved choosing the subdistricts (Tehsils/Talukas) or Primary Sampling Units (PSUs). The selection of wards in urban areas and villages in rural areas within the chosen PSUs took place in the second stage. In the third stage, households in rural areas were selected from sample villages. However, one Census Enumeration Block (CEB) was randomly chosen in each urban area during the third stage, and households were then chosen from this CEB during the fourth stage. Consequently, there was an additional stage of sampling in urban areas. Detailed information on the survey design, methodology and data collection was published in the LASI survey report and elsewhere (LASI, 2020; Perianayagam et al., 2022). Fig. 1 illustrates the sample selection procedure for the current study. The sample comprised 29002 participants, including 19319 males and 9683 females. The sex ratio for the whole sample was 502; for the migrant subgroup, it was 915. The mean age of the participants was 59.45 ± 10.61 SD, with a range of 45–116 years.
Fig. 1.
Flowchart of sample selection.
2.2. Treatment variable
The participants in our study were middle-aged and older individuals aged 45 and above who migrated to other places within 10 years from their place of last residence. As migration is the treatment variable, the migration information of the respondents was accessed in three steps. Those who responded “Since Birth" to the survey question “How many years have you been living (continuously) in this area?" were classified as non-migrant and others as migrant. However, among the migrants, those who reported their last residence was any country other than India to the survey question “Where were you living before coming to this place (place of last residence)" were excluded from the study as they were not considered internal migrants. Therefore, any respondents who did not respond to the survey question regarding their migration status and those who international migrants were also excluded from the study as the treatment sample was solely based on internal migrants. Furthermore, to get an explicit effect of migration on health outcomes, migrants who had resided in the destination areas for more than 10 years were excluded from the study. There was no overlapping between the treatment and control groups, as they were mutually exclusive.
2.3. Outcome variables
2.3.1. Poor-SRH
The following question was used in the LASI to measure participants' self-rated health status: “Overall, how is your health in general? Would you say it is very good, good, fair, poor, or very poor?" For the present study, the responses were dichotomised into “1″ for the response for poor-SRH (very poor and poor) and “0″ for the rest of the references as good-SRH (excellent, very good and good) (Mandal et al., 2023; Saha, Rahaman, Mandal, Biswas, & Govil, 2022).
2.3.2. Depression
The prevalence of major depression in older adults experiencing dysphoric symptoms was assessed using the Composite International Diagnostic Interview - Short Form (CIDI-SF) on a scale ranging from 0 to 10. This scale has been extensively used in population-based health surveys and estimates a probable psychiatric diagnosis of major depression. It has been verified in field settings. CIDI-SF has three screening (based on the presence of dysphoria and/or anhedonia for 2 or more weeks during the past 1 year) and seven symptom-based questions, and a positive response to three or more symptoms out of ten items are considered ‘depressed'. Depression was coded for the study as 0 for “not diagnosed with depression” and 1 for “diagnosed with depression” (Muhammad, Skariah, Kumar, & Srivastava, 2022).
2.3.3. Multimorbidity
Multimorbidity was assessed using the question, ‘Has any health professional ever diagnosed you with the following chronic conditions or diseases?' (High cholesterol, cancer or malignant tumour, diabetes, chronic heart disease, stroke, any kind of lung disease, bone or joint disease, neurological or mental disorders, and hypertension). When participants report having received a diagnosis from a medical professional for two or more chronic health conditions, this is known as multimorbidity. All chronic illnesses are totalled for this study, and one or no chronic illness is classified as “No Multimorbidity" (coded as 0), whereas multiple chronic illnesses are classified as “Multimorbidity" (coded as 1) (LASI, 2020; Srivastava et al., 2021, Srivastava et al., 2021).
2.3.4. Functional limitation
To assess Activities of Daily Living (ADL) limitations, LASI respondents were questioned if they were having any of the following limitations and they anticipated any of the following limitations to continue longer than three months: difficulty with dressing, walking across the room, bathing, eating, getting in or out of bed, or using the toilet (including getting up and down). In the LASI survey, Activities of Daily Living (IADL) were assessed by asking respondents if they were having any difficulties that were expected to last for at least 3 months, such as shopping for groceries, preparing a hot meal, making a telephone call, doing work around the house or garden, taking medications, managing money like paying bills and keeping track of expenses, and getting around or finding an address in unfamiliar places. In this study, we combined 1 + ADL and 1+IADL limitations for each individual and classified them as having a functional limitation (coded as 1) or not (coded as 0) (Mandal et al., 2023).
2.4. Matching covariates
In this study, a number of matching variables have been included on the basis of available literature (Barman, Saha, Dakua, & Roy, 2023; Ebrahim et al., 2010; Firdaus, 2017; MacKinnon et al., 2023; Mandal et al., 2023; Marques, Gama, Cheng, Osborne, & Dias, 2022; Saha, Mandal, Muhammad, Barman, & Ahmed, 2023; Saha, Muhammad, Mandal Id, Adhikary, & Barman, 2023; Samanta, Munda, Mandal, & Adhikary, 2023). The list of pre-intervention variables includes demographic, household, and health behaviours, includes age (45–59, 60–74, 75+ years), sex of the respondents (Male and female), educational attainment (no education, primary, secondary, and higher), marital status (married, widowed, and others), employment status (currently working, never worked, and retired), social participation (yes, and no), food insecurity status (no, mild, moderate, and severe), wealth quintile (poorest, poorer, middle, richer and richest), caste (scheduled caste, scheduled tribe, other backward classes and others) religion (Hindu, Muslim and others), physical activity (active and inactive), alcohol consumption (never, infrequent, frequent, and heavy), tobacco consumption (non-consumer, currently smoking, smokeless tobacco, and both smoking and smokeless) (refer to table A1 for more details).
2.5. Econometric analysis
2.5.1. Descriptive statistics
Bivariate and multivariate analysis have been performed to achieve study objectives. The prevalence of major health outcomes was presented as proportions for both migrant and non-migrant groups stratified by individual, household, and behavioural factors. The chi-squared test was used to check for differences in the prevalence of health outcomes between non-migrant and migrant populations. A multivariate logistic regression model was performed separately in both population groups to examine the adjusted effect of predictor variables on the probability of reporting major health outcomes.
2.5.2. Propensity score matching (PSM)
The PSM was used in the current study to evaluate the treatment effects of migration on four outcome variables, i.e., poor-SRH, depression, multimorbidity and functional limitation. PSM is a statistical method that helps assess the treatment effects for observational and cross-sectional data by minimising selection bias and modelling the experimental design with balanced baseline characteristics (Rosenbaum & Rubin, 1983). It creates a comparison group that can address the counterfactual (defined as what would be the outcome if the treatment did not occur). In PSM, different observed predictors are combined to provide a propensity score, representing each individual's likelihood of being assigned to the treatment group. A matched sample of participants in the treatment and control groups is created by utilising kernel matching based on this score. The propensity score is a balancing score of the observable predictors, indicating that the distribution of variables is similar in the treatment and comparison groups. Individuals who were migrant were assigned to the treatment group and matched with the control group using a one-to-one matching approach. The calculated propensity scores were based on various individual and household-level characteristics such as age, sex, educational status, marital status, working status, social participation, food insecurity, MPCE quintile, religion, caste, physical activity, alcohol, and tobacco consumption. A description of the method is given as follows:
In this study, PSM is the probability that migration determines the health outcome of a person with certain pre-specified characteristics and is written as
| (1) |
Where D = 0 if the person is non-migrant.
D = 1 if the person is a migrant.
And X is the vector of pre-intervention characteristics.
Defining the impact of migration on health outcomes; In PSM, three parameters are estimated. These are average treatment effect (ATE), average treatment effect on treated (ATT) and average treatment effect on untreated (ATU).
The ATE measures the mean impact of migration across the population. This parameter may be defined as
| (2) |
here is the mathematical expectation. is the average value of the potential health outcome for all the units in the migrant group; and is the average value of the potential health outcome for all the units in the non-migrant group.
In observational studies, most of the time, the parameter of interest is the average treatment effect on the treated (ATT), which is
| (3) |
| (4) |
where = (0, 1) refers to the control and treatment conditions. The term is a counterfactual mean which is not observable from the data. It shows the average outcome that the treated individuals would have obtained in the absence of migration, which is unobserved.
| (5) |
| (6) |
Where = (0, 1) refers to the control and treatment conditions. Where, is the observed mean, and it shows the average health outcome for the persons who were non-migrant. Where is the counterfactual mean outcome for non-migrants. It shows the average outcome that the controlled individuals would have obtained in the presence of migration, which is unobserved.
2.6. Background characteristics of the study population
Around 54.71 % of the migrant respondents and 49.62 % of the non-migrant respondents were Middle-aged (45–59). The share of the respondents aged between 60 and 74 was 32.23 % for migrants and 39.11 % for non-migrants. Around 13.06 % of migrants and 11.27 % of the non-migrants were aged 75+. Additionally, 42.82. % of non-migrant respondents had no formal education, 17.53 % of the non-migrants were widowed, and 59.88 % of the respondents were employed. Further, among migrant respondents, 39.71 % had no formal education, 25.38 % were widowed, and 35.75 % were employed. Notably, 6.60 % of non-migrant respondents and 6.24 % of migrant respondents faced severe food insecurity. However, 63.12 % of non-migrants and 60.26 % of migrants were physically active. Furthermore, 17.19 % and 29.28 % of the non-migrant and migrant respondents belonged to the lowest wealth quintile, respectively (see table A2 in Appendix).
3. Results
3.1. Prevalence of four different health outcome for migrant and non-migrant population
Non-migrants had a lower prevalence of Poor-SRH (16.28 % vs 18.95 %), depression (6.62 % vs 9.33 %), multimorbidity (15.70 % vs 20.25 %) and functional limitation (23.12 % vs 31.79 %) than their migrant counterparts. The stratified prevalence of the health outcomes can be found in Table 1 and Table 2. Fig. 2 displays the prevalence of poor self-rated health, depression, multimorbidity, and functional limitation among migrants stratified by the stream of migration.
Table 1.
Prevalence of poor-SRH and depression among migrant and non-migrant populations stratified by migration status.
| Background Characteristics | Poor-SRH |
Depression |
||||
|---|---|---|---|---|---|---|
| Migrant | Non-migrant | Difference (p-value) | Migrant | Non-migrant | Difference (p-value) | |
| Age | ||||||
| 45–59 | 11.78 | 9.72 | <0.001 | 14.37 | 6.19 | <0.001 |
| 60–74 | 23.56 | 18.16 | <0.001 | 9.56 | 6.66 | <0.001 |
| 75+ | 36.94 | 28.39 | <0.001 | 10.53 | 8.41 | <0.001 |
| Sex | ||||||
| Male | 25.4 | 15.21 | 0.038 | 16.09 | 6.76 | 0.027 |
| Female | 22.88 | 19.41 | <0.001 | 9.13 | 6.21 | <0.001 |
| Education | ||||||
| Higher | 8.28 | 7.31 | <0.001 | 3.85 | 4.90 | 0.192 |
| Secondary | 18.48 | 13.53 | <0.001 | 5.71 | 5.67 | 0.04 |
| Primary | 26.67 | 18.18 | <0.001 | 13.08 | 8.15 | <0.001 |
| Illiterate | 32.84 | 19.75 | <0.001 | 19.78 | 7.02 | <0.001 |
| Marital Status | ||||||
| Currently married | 23.87 | 14.50 | <0.001 | 13.18 | 6.25 | <0.001 |
| Widowed | 25.79 | 23.28 | 0.001 | 10.54 | 8.49 | <0.001 |
| Others | 14.19 | 21.58 | <0.001 | 7.62 | 5.81 | <0.001 |
| Employment status | ||||||
| Never worked | 22.24 | 20.52 | 0.007 | 9.74 | 6.41 | <0.001 |
| Retired | 38.45 | 26.73 | <0.001 | 20.14 | 8.46 | <0.001 |
| Currently Working | 11.42 | 10.56 | <0.001 | 6.78 | 5.81 | <0.001 |
| Social participation | ||||||
| Yes | 22.24 | 11.35 | <0.001 | 5.72 | 5.70 | <0.001 |
| No | 24.14 | 16.63 | <0.001 | 12.71 | 6.69 | <0.001 |
| Food insecurity status | ||||||
| No food insecurity | 22.63 | 13.48 | <0.001 | 12.68 | 5.25 | <0.001 |
| Mild food insecurity | 24.24 | 17.76 | <0.001 | 7.72 | 6.61 | 0.041 |
| Moderate food insecurity | 25.89 | 30.15 | 0.003 | 30.78 | 11.26 | <0.001 |
| Severe food insecurity | 34.95 | 28.59 | <0.001 | 25.92 | 17.12 | <0.001 |
| MPCE quintile | ||||||
| Richest | 22.18 | 16.67 | <0.001 | 7.24 | 6.10 | <0.001 |
| Richer | 20.22 | 16.59 | 0.001 | 9.42 | 5.31 | <0.001 |
| Middle | 18.29 | 15.68 | <0.001 | 8.24 | 6.67 | <0.001 |
| Poorer | 22.69 | 17.3 | <0.001 | 8.84 | 7.41 | 0.030 |
| Poorest | 31.95 | 15.00 | <0.001 | 21.55 | 8.09 | <0.001 |
| Caste | ||||||
| Others | 15.2 | 14.1 | <0.001 | 5.67 | 6.44 | 0.023 |
| OBC | 29.87 | 17.11 | <0.001 | 16.66 | 7.01 | <0.001 |
| SC/ST | 21.61 | 16.73 | <0.001 | 10.63 | 6.15 | <0.001 |
| Religion | ||||||
| Hindu | 20.13 | 16.56 | <0.001 | 8.00 | 6.72 | <0.001 |
| Muslim | 47.57 | 15.79 | 0.014 | 9.81 | 6.67 | <0.001 |
| Others | 23.35 | 13.42 | <0.001 | 8.89 | 5.28 | <0.001 |
| Physical activity | ||||||
| Active | 22.15 | 12.52 | <0.001 | 13.52 | 5.87 | <0.001 |
| Inactive | 26.90 | 22.73 | 0.001 | 10.49 | 7.92 | <0.001 |
| Alcohol consumption | ||||||
| Never consumed | 25.34 | 16.59 | <0.001 | 12.87 | 6.39 | 0.63 |
| Infrequent | 16.54 | 16.83 | 0.23 | 6.03 | 7.96 | 0.052 |
| frequent | 7.83 | 13.10 | 0.045 | 6.00 | 6.12 | 0.533 |
| heavy drinker | 20.84 | 12.85 | 0.115 | 8.43 | 7.27 | 0.641 |
| Tobacco consumption | ||||||
| Non consumer | 26.80 | 16.53 | <0.001 | 13.17 | 5.58 | <0.001 |
| Currently smoking | 13.81 | 17.93 | 0.001 | 7.63 | 7.16 | 0.12 |
| Smokeless tobacco | 18.91 | 14.12 | 0.002 | 11.39 | 7.58 | 0.574 |
| Both smoking and smokeless | 12.94 | 19.41 | 0.157 | 12.69 | 9.91 | <0.001 |
| Total | 24.04 | 16.29 | <0.001 | 12.32 | 6.62 | <0.001 |
Note: SC/ST: Schedule caste/Schedule tribe, OBC: Other backward caste, MPCE: Monthly per capita consumption expenditure, p-value is based on chi-square test when comparing the same category between migrant and non-migrant sample.
Table 2.
Prevalence of multimorbidity and functional limitation among migrant and non-migrant populations stratified by migration status.
| Background Characteristics | Multimorbidity |
Functional limitation |
||||
|---|---|---|---|---|---|---|
| Migrant | Non-migrant | Difference (p-value) | Migrant | Non-migrant | Difference (p-value) | |
| Age | ||||||
| 45–59 | 22.30 | 11.23 | <0.001 | 20.94 | 12.61 | <0.001 |
| 60–74 | 32.90 | 20.41 | <0.001 | 28.75 | 27.93 | <0.001 |
| 75+ | 30.47 | 19.10 | <0.001 | 58.45 | 52.76 | <0.001 |
| Sex | ||||||
| Male | 28.38 | 13.81 | <0.001 | 23.48 | 18.74 | 0.021 |
| Female | 25.43 | 21.22 | <0.001 | 32.47 | 35.86 | <0.001 |
| Education | ||||||
| Higher | 22.15 | 21.77 | <0.001 | 6.77 | 8.60 | 0.224 |
| Secondary | 30.39 | 18.45 | <0.001 | 13.27 | 16.03 | <0.001 |
| Primary | 27.12 | 14.21 | <0.001 | 26.04 | 21.20 | <0.001 |
| Illiterate | 26.04 | 12.95 | <0.001 | 48.10 | 32.52 | <0.001 |
| Marital Status | ||||||
| Married | 28.83 | 14.95 | <0.001 | 23.37 | 19.08 | <0.001 |
| Widowed | 22.33 | 20.50 | <0.001 | 43.11 | 41.38 | <0.001 |
| Others | 17.43 | 8.77 | <0.001 | 29.35 | 22.83 | <0.001 |
| Employment status | ||||||
| Never worked | 30.08 | 25.92 | <0.001 | 36.55 | 29.38 | 0.070 |
| Retired | 38.88 | 23.56 | <0.001 | 45.83 | 40.37 | <0.001 |
| Currently Working | 12.25 | 9.96 | <0.001 | 10.46 | 12.35 | <0.001 |
| Social participation | ||||||
| Yes | 29.05 | 14.79 | <0.001 | 10.37 | 16.74 | 0.040 |
| No | 26.65 | 15.77 | <0.001 | 29.42 | 23.57 | <0.001 |
| Food insecurity status | ||||||
| No food insecurity | 29.60 | 14.79 | <0.001 | 29.78 | 21.68 | <0.001 |
| Mild food insecurity | 21.47 | 15.93 | <0.001 | 24.23 | 22.57 | <0.001 |
| Moderate food insecurity | 20.03 | 18.56 | 0.705 | 37.60 | 33.63 | 0.0740 |
| Severe food insecurity | 32.95 | 21.59 | 0.041 | 33.72 | 35.36 | <0.001 |
| MPCE quintile | ||||||
| Richest | 17.27 | 10.05 | <0.001 | 26.70 | 26.10 | <0.001 |
| Richer | 14.33 | 12.48 | <0.001 | 23.70 | 13.19 | <0.001 |
| Middle | 15.90 | 13.88 | <0.001 | 24.60 | 22.29 | <0.001 |
| Poorer | 26.18 | 18.28 | <0.001 | 27.58 | 22.41 | <0.001 |
| Poorest | 46.17 | 26.48 | <0.001 | 33.24 | 21.00 | <0.001 |
| Caste | ||||||
| Others | 24.03 | 19.25 | <0.001 | 24.28 | 18.84 | <0.001 |
| OBC | 32.65 | 17.11 | <0.001 | 31.05 | 25.72 | <0.001 |
| SC/ST | 13.28 | 10.54 | <0.001 | 27.21 | 22.43 | <0.001 |
| Religion | ||||||
| Hindu | 22.64 | 14.60 | <0.001 | 24.66 | 23.12 | <0.001 |
| Muslim | 50.26 | 23.65 | <0.001 | 56.31 | 22.95 | <0.001 |
| Others | 28.76 | 16.55 | <0.001 | 17.53 | 23.50 | <0.001 |
| Physical activity | ||||||
| Active | 28.11 | 13.41 | <0.001 | 23.78 | 18.91 | <0.001 |
| Inactive | 24.77 | 19.64 | <0.001 | 35.29 | 30.34 | <0.001 |
| Alcohol consumption | ||||||
| Never consumed | 28.30 | 16.72 | <0.001 | 30.42 | 24.59 | <0.001 |
| Infrequent | 19.05 | 14.32 | <0.001 | 13.08 | 19.18 | 0.056 |
| frequent | 8.61 | 9.89 | 0.006 | 10.61 | 17.19 | 0.096 |
| heavy drinker | 10.24 | 7.05 | 0.391 | 9.92 | 15.69 | 0.805 |
| Tobacco consumption | ||||||
| Non consumer | 31.45 | 19.33 | <0.001 | 29.39 | 24.33 | <0.001 |
| Currently smoking | 10.74 | 11.71 | 0.010 | 26.50 | 19.18 | <0.001 |
| Smokeless tobacco | 16.58 | 11.69 | <0.001 | 24.32 | 23.78 | <0.001 |
| Both smoking and smokeless | 12.42 | 14.39 | 0.156 | 28.48 | 21.20 | 0.002 |
| Total | 26.78 | 15.71 | <0.001 | 28.35 | 23.13 | <0.001 |
Note: SC/ST: Schedule caste/Schedule tribe, OBC: Other backward caste, MPCE: Monthly per capita consumption expenditure, p-value is based on chi-square test when comparing the same category between migrant and non-migrant sample.
Fig. 2.
Prevalence of health outcomes by streams of migration among the migrant population, India.
3.2. Determinants of different health outcomes among middle-aged and older migrant individuals
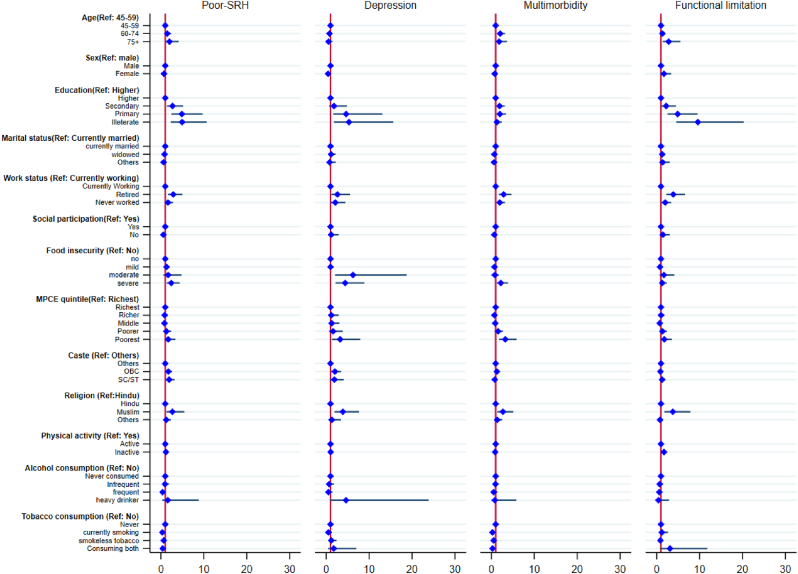
We utilised logistic regression estimates for poor-SRH, depression, multimorbidity, and functional limitation in the migrant population, adjusting for a distinct set of determinants (see Fig. 3). Among migrants, after adjusting for all selected covariates, respondents who had primary education [OR: 1.97; CI: 1.51, 3.40], or secondary education [OR: 1.90; CI: 1.17, 3.09] were more likely to report poor-SRH in comparison with their highly educated counterpart. Migrants who were retired from work were 2.84 times more likely to report poor-SRH than those who were currently working. In comparison with the middle-aged and older migrants without any food insecurity, those who had severe food insecurity were more likely to report poor-SRH [OR: 2.41; CI: 1.33, 4.36]. Female migrants were less likely to suffer from depression than male peers [OR:0.43; CI: 0.19, 0.99]. Migrants without any education [OR: 5.30; CI: 4.20, 6.40], primary education [OR: 4.63; CI: 2.33, 5.98], or secondary education [OR: 1.81; CI: 1.68, 2.11] likely to have elevated depression than highly educated migrants. Migrants with severe food insecurity were 4.41 times [OR: 4.41; CI: 2.19, 8.89] more likely to suffer from depression compared to those who did not have any food insecurity. Migrants from the poorest stata had a significant higher likelihood of having depression than the richest migrants [OR: 3.23; CI: 1.32, 5.91]. Old age migrants (60-74) were more likely to suffer from multimorbidity than their younger counterparts [OR: 2.05; CI: 1.34, 3.16]. In comparison with the highly educated respondents, migrants with primary education were more likely to suffer from multimorbidity [OR: 1.90; CI: 1.17, 3.09]. Middle and old aged migrants who never worked [OR: 1.95; CI: 1.21, 3.14] or retired [OR: 2.84; CI: 1.72, 4.69] were more likely to suffer from multimorbid conditions than their currently working counterparts. Middle-aged and older migrants from poorest were 3.24 times [OR: 3.24; CI: 1.78, 5.90] more likely to suffer from multimorbidity than their richest counterparts. Functional limitation was likely to be 2.79 times higher among the oldest old (70+) migrants than their middle-aged counterparts [OR 2.79; CI: 1.40, 5.55]. Migrants without any formal education were more likely to suffer from functional limitations than highly educated Migrants [OR: 6.61; CI: 4.55, 8.29]. The likelihood of suffering from functional limitation was 3.86 times higher in retired migrants than those who were currently working [OR: 3.86; CI: 2.25, 6.62]. Physically inactive migrants were more likely to suffer from physical limitation than physically active migrants [OR: 1.71; CI: 1.19, 2.45] (also see table A4 in Appendix).
Fig. 3.
Logistic regression estimates for four different health outcomes by their background characteristics among Middle-aged and older migrants.
3.3. Determinants of different health outcomes among middle-aged and older non-migrant individuals
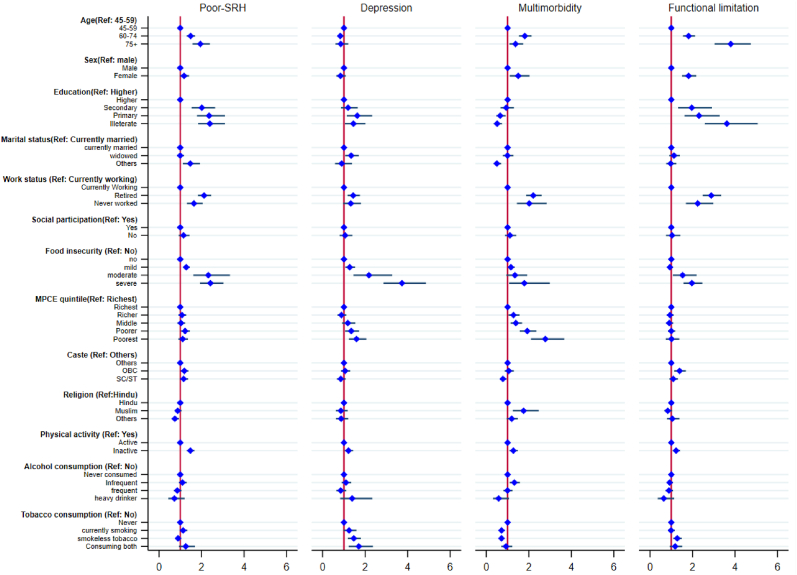
Fig. 4 provides the logistic regression estimates of four different health outcomes for non-migrant middle-aged and older adults in India. Increasing age was significantly associated with repositing of poor-SRH among the non-migrant respondents. A significant negative association has been identified between the level of educational attainment and reporting poor-SRH among non-migrants. Non-migrant individuals who were retied [OR: 2.12; CI: 1.83, 2.45] or never worked [OR: 1.64; CI: 1.32, 2.06] were more likely to report poor-SRH than currently working individuals. Respondents with severe food insecurity were 2.42 times significantly more likely to report poor-SRH than respondents without any food insecurity [OR: 2.42; CI: 1.93, 3.03]. Non-migrants who did not have any formal education and primary education were 1.44 times [OR: 1.45; CI: 1.04, 2.01] and 1.62 times [OR: 1.13; CI: 1.14, 2.33] more likely to suffer from depression than their higher-educated counterparts, respectively. Retired non-migrant individuals more likely to suffer from depression than their currently working peers [OR: 1.44; CI: 1.17, 1.75]. Non-migrants from poorest stata [OR: 1.59; CI: 1.23, 2.05] and having severe food insecurity [OR: 3.73; CI: 2.86, 4.86] were more likely to suffer from depression then their counterparts who were richest, and did not have any food insecurity, respectively. Non-migrants who were consuming both smoking and smokeless tobacco were more likely to develop depression than non-migrant who never consumed any tobacco [OR: 1.70; CI: 1.22, 2.36]. Retired non-migrants were highly likely to have multimorbidity than their counterparts who were currently working [OR: 2.21; CI: 1.87, 2.60]. Respondents from poorer [OR: 1.92; CI: 1.57, 2.35] and poorest [OR: 2.77; CI: 2.10, 3.66] stata were more likely to suffer from multimorbidity than richest non-migrants. Female respondents were more likely to suffer from multimorbidity than their male counterparts [OR: 1.81; CI: 1.54, 2.13]. This was also identical in the case of functional limitation in females [OR: 1.81; CI: 1.55, 2.12]. Compared with the highly educated non-migrants, respondents from lower educational backgrounds were more likely to suffer from functional limitations [OR: 3.61; CI: 2.57, 5.06]. Those who were never physically inactive were more likely to suffer from functional limitation than their counterparts who were physically active [OR: 1.23; CI: 1.06, 1.42].
Fig. 4.
Logistic regression estimates for four different health outcomes by their background characteristics among Middle-aged and older non-migrants.
3.4. Multivariate logistic regression estimates the effect of migration on health outcomes
The odds of reporting poor health for each health outcome, being a migrant (compared to non-migrant as reference), were calculated and progressively adjusted by each set of determinants (Table 3). The unadjusted analysis revealed, being a migrant was significantly associated with higher odds of experiencing poor-SRH, depression and multimorbidity except for functional limitations. After controlling for demographics, being a migrant was significantly associated with higher odds of suffering from poor-SRH, depression, multimorbidity and functional limitation. However, after adjusting by socioeconomic covariates and health behaviour factors, only the association with depression remained significant. Being a migrant was associated with 1.88 times [OR: 1.88; CI: 1.05, 3.34] higher odds of depression than non-migrant individuals.
Table 3.
Logistic regression estimates of different health outcomes for a migrant sequentially adjusted by demographic, socioeconomic and behavioural factors.
| Model 1: Crude OR |
Model 2: Adjusted OR by Model 1 + Demographics |
Model 3: Adjusted OR by Model 2 + SES |
Model 4: Adjusted OR by Model 3 + HB |
|
|---|---|---|---|---|
| OR [95 %CI] | OR [95 %CI] | OR [95 %CI] | OR [95 %CI] | |
| Poor-SRH | 1.63* [1.06, 2.49] | 1.69* [1.00, 2.85] | 1.46 [0.98, 2.18] | 1.45 [0.96, 2.18] |
| Depression | 1.98* [0.92, 4.27] | 2.20* [0.94, 5.15] | 1.82* [1.02, 3.25] | 1.88* [1.05, 3.34] |
| Multi- morbidity | 1.96*** [1.32, 2.93] | 1.68 [0.96, 2.94] | 1.31 [0.91, 1.88] | 1.28 [0.90, 1.81] |
| Functional limitation | 1.32 [0.91, 1.90] | 1.17 [0.67, 2.03] | 0.98 [0.65, 1.46] | 0.99 [0.66, 1.48] |
Note: OR represents odds ratio, CI represents confidence interval, Demographics includes age, sex, education status, marital status; Socioeconomic variables (SES) Includes employment status, social participation, food insecurity status, MPCE quintile, caste, religion; Health Behavioural variables (HB) includes physical activity, alcohol consumption and tobacco consumption, ***p ≤ 0.001, **p ≤ 0.01 and * p ≤ 0.05.
Fig. 5 shows the covariate balance plot. Considering both raw and matched samples, the balance plot shows kernel density plots for the variables across treatment levels. In order to evaluate the accuracy of the overlap assumption, the reported estimated densities represent the probabilities associated with each treatment. As shown in Fig. 5, the calculated densities show significant volume in the overlapped region, providing strong support for the overlap assumption. This finding highlights the substantial overlap between the two density distributions. Notably, the density map for the matched sample shows a significant amount of overlap, demonstrating that matching based on estimated propensity scores successfully balanced the confounders. With both assumptions satisfied in the study, it is clear that the treatment assignment is substantially ignorable, ensuring the unbiasedness of the calculated treatment effects.
Fig. 5.
Balance diagnostic before and after matching using Kernel density.
Table 4 presents the average values of individual matching variables before and after matching for both the treated and control groups. It illustrates the reduction in percentage bias subsequent to matching, along with the standardised difference assessing distinctions among the matched pairs. Notably, the mean differences became statistically insignificant across all covariates after matching, signifying a sufficient balance achieved among the covariates.
Table 4.
Covariate Balance of baseline characteristics across Treatment and Comparison Groups before and after Matching.
| Characteristics | Before matching |
After matching |
||||
|---|---|---|---|---|---|---|
| Mean Treated | Mean Comparison | StdDif | Mean Treated | Mean Comparison | StdDif | |
| Age- 45-59 | 0.588 | 0.523 | 0.131* | 0.581 | 0.587 | −0.012 |
| Age- 60-74 | 0.325 | 0.375 | −0.104* | 0.332 | 0.327 | 0.012 |
| Age- 75+ | 0.086 | 0.102 | −0.053 | 0.087 | 0.087 | 0.001 |
| Sex-male | 0.449 | 0.692 | −0.507* | 0.466 | 0.473 | −0.013 |
| Sex-female | 0.551 | 0.308 | 0.507* | 0.534 | 0.527 | 0.013 |
| Education- illiterate | 0.316 | 0.432 | −0.242* | 0.328 | 0.321 | 0.016 |
| Education- primary | 0.180 | 0.193 | −0.032 | 0.181 | 0.182 | −0.002 |
| Education- secondary | 0.312 | 0.264 | 0.105* | 0.309 | 0.303 | 0.013 |
| Education- higher | 0.192 | 0.111 | 0.227* | 0.181 | 0.194 | −0.035 |
| Marital status- married | 0.722 | 0.786 | −0.149* | 0.726 | 0.732 | −0.016 |
| Marital status- widowed | 0.229 | 0.172 | 0.143* | 0.224 | 0.216 | 0.020 |
| Marital Status- others | 0.049 | 0.042 | 0.034 | 0.050 | 0.051 | −0.007 |
| Work- never worked | 0.321 | 0.158 | 0.390* | 0.305 | 0.303 | 0.006 |
| Work- retired | 0.274 | 0.263 | 0.024 | 0.276 | 0.268 | 0.017 |
| Work- currently working | 0.405 | 0.579 | −0.354* | 0.419 | 0.429 | −0.020 |
| Food insecurity- none | 0.533 | 0.566 | −0.067 | 0.538 | 0.538 | 0.000 |
| Food insecurity- mild | 0.390 | 0.368 | 0.046 | 0.389 | 0.387 | 0.006 |
| Food insecurity- moderate | 0.024 | 0.018 | 0.039 | 0.022 | 0.022 | −0.001 |
| Food insecurity- severe | 0.053 | 0.048 | 0.024 | 0.051 | 0.053 | −0.011 |
| Social participation- no | 0.906 | 0.912 | −0.023 | 0.905 | 0.902 | 0.012 |
| Social participation- yes | 0.094 | 0.088 | 0.023 | 0.095 | 0.098 | −0.012 |
| MPCE- Poorest | 0.132 | 0.216 | −0.223* | 0.136 | 0.135 | 0.003 |
| MPCE- Poorer | 0.169 | 0.209 | −0.102* | 0.174 | 0.179 | −0.012 |
| MPCE- Middle | 0.196 | 0.201 | −0.013 | 0.198 | 0.199 | −0.001 |
| MPCE- Richer | 0.212 | 0.193 | 0.046 | 0.212 | 0.207 | 0.011 |
| MPCE- richest | 0.291 | 0.181 | 0.262* | 0.280 | 0.280 | −0.001 |
| Caste- SC/ST | 0.276 | 0.386 | −0.236* | 0.284 | 0.284 | −0.001 |
| Caste- others | 0.385 | 0.393 | −0.016 | 0.391 | 0.391 | 0.001 |
| Caste- OBC | 0.339 | 0.221 | 0.265* | 0.325 | 0.325 | 0.001 |
| Religion- muslin | 0.722 | 0.717 | 0.011 | 0.720 | 0.735 | −0.032 |
| Religion- others | 0.110 | 0.113 | −0.007 | 0.113 | 0.111 | 0.004 |
| Religion- Hindu | 0.168 | 0.170 | −0.007 | 0.167 | 0.154 | 0.035 |
| Physical activity- active | 0.567 | 0.624 | −0.117* | 0.574 | 0.576 | −0.004 |
| Physical activity- inactive | 0.433 | 0.376 | 0.117* | 0.426 | 0.424 | 0.004 |
| Alcohol consumption- never | 0.855 | 0.745 | 0.278* | 0.850 | 0.850 | 0.000 |
| Alcohol consumption- frequent | 0.052 | 0.099 | −0.178* | 0.054 | 0.055 | −0.002 |
| Alcohol consumption- heavy | 0.008 | 0.013 | −0.043 | 0.009 | 0.009 | −0.001 |
| Tobacco consumption – never | 0.723 | 0.547 | 0.372* | 0.713 | 0.715 | −0.003 |
| Tobacco consumption – smoker | 0.106 | 0.166 | −0.175* | 0.111 | 0.112 | −0.003 |
| Tobacco consumption – smokeless | 0.143 | 0.232 | −0.228* | 0.148 | 0.147 | 0.004 |
| Tobacco consumption- both | 0.027 | 0.055 | −0.142* | 0.028 | 0.027 | 0.004 |
Note: *Absolute value of mean standardised difference above 10 %; StdDif: Standardised difference (%); SC/ST: Schedule caste/Schedule Tribe; OBC: Other backward class.
3.5. Propensity matching score estimates the effect of migration on health outcomes
Table 5 illustrates the propensity matching score results to understand the impact of migration on self-rated health, depression, multimorbidity and functional limitation. The unmatched sample estimates revealed that the migrants in India had reported 3.0 percentage points higher poor-SRH than non-migrants. The ATT findings revealed that within the treatment group, individuals who underwent migration experienced an average increase of 2.4 percentage points in reporting poor-SRH compared to those respondents who had not migrated. The ATT results indicate that depression was typically 1.0 percentage points higher among migrant groups than non-migrant groups. Middle-aged and older adults who were migrants, on average, suffered 4.2 % more multimorbid conditions than their non-migrant counterparts. The difference between treated and control values in ATT and ATE concerning functional limitations was noted at 2.3 % and 1.9 %, indicating that middle-aged and older adults who migrated were more prone to experiencing functional limitations. The findings from the Average Treatment Effect on the Untreated (ATU) analysis revealed that for individuals who did not migrate, migration would have led to an average rise of 1.7 % in reported poor-SRH, 0.2 % in depression, 4.0 % in multimorbidity, and 0.6 % in functional limitations.
Table 5.
Propensity Score Matching estimates the impact of migration status on the Health Outcomes.
| Variable | Sample | Treated | Controls | Difference | SE. | T-stat |
|---|---|---|---|---|---|---|
| Self-rated Health | Unmatched | 0.178 | 0.148 | 0.030 | 0.007 | 4.410 |
| ATT | 0.178 | 0.154 | 0.024 | 0.007 | 3.190 | |
| ATU | 0.148 | 0.165 | 0.017 | |||
| ATE | 0.017 | |||||
| Depression | Unmatched | 0.064 | 0.054 | 0.010 | 0.004 | 2.310 |
| ATT | 0.064 | 0.054 | 0.010 | 0.005 | 2.100 | |
| ATU | 0.054 | 0.056 | 0.002 | |||
| ATE | 0.003 | |||||
| Multimorbidity | Unmatched | 0.237 | 0.154 | 0.083 | 0.007 | 11.820 |
| ATT | 0.237 | 0.195 | 0.042 | 0.008 | 5.120 | |
| ATU | 0.154 | 0.194 | 0.040 | |||
| ATE | 0.040 | |||||
| Functional limitation | Unmatched | 0.212 | 0.201 | 0.011 | 0.008 | 1.430 |
| ATT | 0.212 | 0.203 | 0.010 | 0.008 | 1.180 | |
| ATU | 0.201 | 0.195 | 0.006 | |||
| ATE | 0.005 |
Note-ATE: Average Treatment Effect; ATT: Average Treatment Effect on the Treated; ATU: Average Treatment Effect on the Untreated; SE: standard error.
4. Discussion
This study is based on large-scale, nationally representative secondary data on middle-aged and older adults in India. This research delves into health disparities between migrant and non-migrant groups, focusing on four outcome variables: poor self-rated health, depression, multimorbidity, and functional limitations. It analyses associations with demographics, socioeconomics, and health behaviours. Employing propensity score matching on middle-aged and older individuals, the study provides insights into the intricate relationship between migration and health impairments. This study found that migrants were more likely to suffer from poor-SRH, depression, multimorbidity and functional limitation than non-migrants. Migrants' self-rated health is influenced by multifaceted social determinants, including socioeconomic inequalities, restricted healthcare access, language barriers, discrimination, and migration-related stressors (Srivastava, Chauhan, & Patel, 2021; Tsoh et al., 2016). We found migrants likely to report 2.4 percentage points higher poor-SRH, which was in line with the other studies (Lanari & Bussini, 2012; Mandal et al., 2023; Reus-Pons, Mulder, Kibele, & Janssen, 2018). In fact, an elevated risk of depression and chronic morbidity can be seen among the migrant population, which also aligns with the previous literature (Marin et al., 2022). The impact of migration on an individual's mental health and wellbeing is well established in existing literature (Banal et al., 2010; Jurado et al., 2017). Our results are also in line with the existing studies, which suggest that various risk factors are associated with an increased risk of depression in migrants; these include socioeconomic status, encompassing low income and limited education, which shapes vulnerability (Chen et al., 2022; Essayagh et al., 2023; Foo et al., 2018; Gkiouleka et al., 2018; Jang & Tang, 2021; R. Patel, Kumar, & Chauhan, 2022). In addition to that, a combination of inadequate social support, discrimination, and stigma also contributes to depression (Allen, Kunicki, & Greaney, 2023; García-Cid, Gómez-Jacinto, Hombrados-Mendieta, Millán-Franco, & Moscato, 2020; Wang, Li, Stanton, & Fang, 2010). Additionally, in a new environment, cultural aspects such as acculturation play a pivotal role in shaping the mental health of migrants, especially during the initial years of migration (Jang & Tang, 2021; Jurado et al., 2017; Marin et al., 2022). We found migrants have an elevated prevalence of multimorbidity than non-migrants. The elevated multimorbidity among migrants may be attributed to limited access to a nutritious diet, lifestyle changes in a new environment, limited healthcare access, and low health literacy (Ansari, Anand, Singh, & Hossain, 2023; P. Patel, Muhammad, & Sahoo, 2023; Sinha, Kerketta, Ghosal, Kanungo, & Pati, 2022). Additionally, occupational hazards in ‘3D′ work and elevated psychological stress compound the issue of multimorbidity among migrants (Babu, Swain, Mishra, & Kar, 2010; Kreps & Sparks, 2008). With regard to theoretical considerations of the development of health disparities, the findings of this study can be interpreted through the lens of the cumulative disadvantage theory, which posits that the health of migrants is impacted negatively over the course of their lives due to their persistent low socioeconomic status (Dannefer, 2003; O'Rand, 1996). The descriptive analysis showed some relevant socioeconomic and health behavioural differences that might lead to the health disparity between the migrant- and non-migrant populations. Migrants reported higher food insecurity, lower educational attainment, and less physical activity than their non-migrants; in addition, non-migrants were socially more active and currently working. Prior studies indicate that migrants experience adverse health effects due to factors such as material deprivation, poor working and living conditions, cultural and language barriers, social isolation, and limited healthcare access (Borhade Anjali, 2016; María & Arias Uriona, 2020; Nitika, Nongkynrih, & Gupta, 2014).
In what follows, our study indicated that a few crucial factors contributed to the disparity in health between migrants and non-migrants. In developing countries like India, migrants frequently move to other locations to pursue employment opportunities, accepting positions in the “3D" category (dirty, dangerous and demeaning) jobs (Bhagat, Sahoo, Roy, & Govil, 2020; Hirudayaraj, Barhate, & McLean, 2023; Jayaram & Varma, 2020). As a result, occupational elements such as industry, working conditions, working hours, and workplace discrimination may negatively impact the health of these migrants substantially, with these health disadvantages accumulating over time and affecting the health of migrants in their later ages (Jayaram & Varma, 2020; Srinivasan & Ilango, 2013). Extant empirical literature showed that low education levels were positively associated with health disparities (Kimbrough, 2012; Oshio, 2018; Zajacova & Lawrence, 2018), lower levels of education among the migrants resulted in limited health literacy, making it more difficult for them to understand and manage their health conditions. They may also be less likely to engage in preventive health behaviours, such as getting regular check-ups and screenings, are more likely to engage in health-risk behaviours (Lee & Seon, 2019; Margolis, 2013). Limited health literacy results in poor health care utilisation (Groot & Maassen Van Den Brink, 2006; Marques et al., 2022; Raghupathi & Raghupathi, 2020; Srinivasan & Ilango, 2013). Internal migration is frequently employed as a livelihood strategy to combat food insecurity in numerous developing countries, including India, which has the world's largest population of undernourished individuals (McGuire, 2015). The relationship between food-insecurity and migration operates bidirectionally, serving both as a catalyst and a result. Recognising the profound impact of insufficient food security, it has been acknowledged that it can negatively affect chronic, mental, and physical health in various ways (Jones, 2017; Nagata et al., 2019; Seligman, Bindman, Vittinghoff, Kanaya, & Kushel, 2007). Inadequate access to nutritious food can lead to increased vulnerability to chronic diseases, compromised mental wellbeing, and heightened risks for physical health issues (Chung et al., 2023; Fang, Thomsen, & Nayga, 2021; Seligman, Laraia, & Kushel, 2010). In older adults, it is correlated with an elevated risk of diet-related chronic illnesses, sarcopenia, appetite decline, poor psychological status, social isolation, poor health, and poor quality (Choithani, 2017; McGuire, 2015; Orjuela-Grimm et al., 2022; R. Patel et al., 2022). It is also important to recognise that while ageing factors are similar across populations, migration-led risk factors can also affect the health and quality of life in old age. These factors include exposure to adverse events, low acculturation, and lack of social support (Allen et al., 2023; García-Cid et al., 2020). Existing research illustrated that the absence of social support negatively affects the health of migrants (Salinero-Fort et al., 2011; Záleská, Brabcová, & Vacková, 2014). Migration often involves leaving behind family and keens, leading to social isolation, and potentially negatively impacting mental wellbeing and life satisfaction in the new environment (Firdaus, 2017; Hombrados-Mendieta et al., 2019; Marin et al., 2022). Our findings shed light on the influence that socioeconomic, demographic, and behavioural health factors have significant implications on the health status of migrants; this new evidence highlights plausible underlying mechanisms contributing to health disparities between migrant and non-migrant populations. This study is unique in many ways and has several strengths; first, this study examines the migrant and non-migrant heath disparity at a national level, making it a valuable contribution to the field. Second, the study is also unique in its focus on the health of middle-aged and older adults, a population that has not been well studied in the context of migration. Third, this study utilises a large-scale, nationally representative dataset, which allows for reliable results. Fourth, this work employs a robust and advanced methodology, ensuring the generation of reliable and sound estimates. Additionally, the chosen approach is designed to yield dependable outcomes, enhancing the credibility of the findings. Finally, to fully understand the health disparity, the study also considers four outcome variables, which provide a more nuanced understanding of the phenomenon and sets it apart from other existing studies that have relied on single outcome indicators.
The findings of this study should be interpreted considering a few limitations. Estimations in the study are based on self-reported data; therefore, the results may be subject to recall and reporting biases. The study lacked additional migratory variables, such as reasons for migration, which was not available in the dataset. This implies that the study could not comprehensively grasp the various contexts and mechanisms by which migration occurred and its effects on health outcomes. Finally, the study did not explore sex-specific health consequences of migration, as it focused on the Indian context, where almost every female migrates to her husband's home. This may limit the understanding of sex-specific health outcomes in the context of later-life migration.
5. Conclusion
The present study is a pioneering effort to examine and explain the disparities in overall, physical, and psychological health differences between middle-aged and older migrants and non-migrants in the Indian context. The study results indicate a significant disparity in health status between migrant and non-migrant populations. Migrants are found to be in a vulnerable situation across all health indicators. These findings underscore the necessity for improved management of the overall health status of middle- and old-aged migrants in India. This research advocates the necessity of understanding the gender-specific differences in health and health transitions among older migrants and non-migrants. India has no structural health policy or programme separately for the migrant population. Our study suggests that being the home of one of the largest internal migrants, a structural and heterogenous policy and program should be framed, which specifically targets migrant's health issues, especially for old-age migrants. In addition, existing health policies should be modified with targeted interventions to ensure that migrant populations are not left excluded. The specific needs of elderly migrants should be included in the National Policy for Senior Citizens (NPSC), regardless of their place of origin. Finally, this study also recommends intervention strategies to address the social security of old-age migrants and to provide them with the necessary support for healthy ageing. It is essential to implement these policy interventions to ensure that middle and old-aged migrant populations in India receive adequate healthcare services, and can age with dignity, and to do that; it is recommended that greater resources should be allocated towards public health interventions so that India can achieve its goal of “leaving no one behind" in terms of health protection.
Ethical statement
The data is available to the public for free (https://lasi-india.org/) Survey agencies that conducted the field survey for the data collection have collected prior informed written consent from the respondent before data collection. No information could lead the identification of the respondents. We received ethical approvals from these organizations: Indian Council of Medical Research (ICMR) in Delhi, International Institute for Population Sciences (IIPS) in Mumbai, Harvard T.H. Chan School of Public Health (HSPH) in Boston, University of Southern California (USC) in Los Angeles, ICMR-National AIDS Research Institute (NARI) in Pune, and Regional Geriatric Centres (RGCs) under the Ministry of Health and Family Welfare, Government of India. Our study followed the guidelines for protecting human subjects outlined in the Declaration of Helsinki.
CRediT authorship contribution statement
Bittu Mandal: Writing – review & editing, Writing – original draft, Visualization, Resources, Methodology, Formal analysis, Data curation, Conceptualization. Kalandi Charan Pradhan: Supervision, Validation, Conceptualization.
Declarations of competing interest
None.
Appendix.
Table A1.
Description of the covariates
| Variables | Categories | Description of the category | |
|---|---|---|---|
| Age | 45-59; 60–74;≥75 | ||
| Sex | Male; Female | ||
| Religion | Hindu; Muslim; Christian; Others | ||
| Caste | Scheduled castes (SC)/scheduled tribe (ST); Other backward classes (OBC); Others | ||
| Education | No education; up to primary; up to secondary; higher | ||
| Marital Status | Currently married; widowed; others | ||
| Wealth | Poorest; poorer, middle; richer; richest | ||
| Employment Status | Never worked; retired; currently working | ||
| Social Participation | Yes; no | ||
| Food Insecurity | Mild | if the respondent reduced the size of your meals or skipped meals | |
| because there was not enough food at its household | |||
| If the respondent did not eat enough food of his/her choice (excluding fasting/food-related restrictions due to religious or health-related reason | |||
| Moderate | if the respondent reduced the size of your meals or skipped meals | ||
| because there was not enough food in the household | |||
| Severe | if the respondent ‘was hungry but did not eat or ‘did not eat for a whole | ||
| day' because there was not enough food in its household (excluding fasting/food-related restrictions due to religious or health-related reasons | |||
| Physical Activity | Active | Those who were either engaged in moderate physical activity (at least 150 min throughout the week) or, vigorous physical activity (at least 75 min throughout the week) or an equivalent combination of both | |
| Inactive | Those who are not engaged in any type of moderate or vigorous physical activity for a given time throughout the week. | ||
| Never | Those who have never been involved in any physical activities | ||
| Consumption of tobacco | Never consumed tobacco | Never consumed tobacco, neither smoking nor smokeless tobacco. | |
| Currently smoking | Currently smoking but not smokeless tobacco. | ||
| Currently consumed smokeless tobacco | Consumers of smokeless tobacco only | ||
| Consumed both smoking and smokeless tobacco | Using both smoking and smokeless tobacco | ||
| Consumption of alcohol | Never consumed alcohol | Never consumed alcohol | |
| Frequently consumed but not heavy drinker | Those who consumed 1–3 days/month | ||
| Infrequently consumed but not heavy drinker | Those who consumed 1–4 days/week but not more than 5 drinks on any occasion | ||
| Heavy drinker | Those who consumed more than 5 drinks on any occasion in past 30 days |
Table A2.
Socio-demographic profile of respondents stratified by migration status
| Background characteristics | Migrant |
Non-migrant |
||
|---|---|---|---|---|
| Sample | Percentage | Sample | Percentage | |
| Age | ||||
| 45–59 | 1825 | 54.71 | 13549 | 49.62 |
| 60–74 | 1010 | 32.23 | 9712 | 39.11 |
| 75+ | 268 | 13.06 | 2638 | 11.27 |
| Sex | ||||
| Male | 1393 | 45.8 | 17926 | 74.36 |
| Female | 1710 | 54.2 | 7973 | 25.64 |
| Education | ||||
| Higher | 596 | 15.75 | 2879 | 12.76 |
| Secondary | 967 | 26.72 | 6838 | 25.32 |
| Primary | 560 | 17.82 | 4996 | 19.11 |
| Illiterate | 980 | 39.71 | 11186 | 42.82 |
| Marital Status | ||||
| Married | 2239 | 71.06 | 20345 | 78.92 |
| Widowed | 711 | 25.58 | 4459 | 17.53 |
| Others | 153 | 3.37 | 1095 | 3.55 |
| Employment status | ||||
| Never worked | 996 | 29.3 | 4082 | 12.22 |
| Retired | 849 | 34.95 | 6809 | 27.9 |
| Currently Working | 1258 | 35.75 | 15008 | 59.88 |
| Social participation | ||||
| Yes | 293 | 5.61 | 2272 | 6.47 |
| No | 2810 | 94.39 | 23627 | 93.53 |
| Food insecurity status | ||||
| No food insecurity | 1653 | 57.03 | 14656 | 56.9 |
| Mild food insecurity | 1210 | 33.99 | 9522 | 34.52 |
| Moderate food insecurity | 74 | 2.74 | 471 | 1.98 |
| Severe food insecurity | 166 | 6.24 | 1250 | 6.6 |
| MPCE quintile | ||||
| Richest | 409 | 13.71 | 5590 | 21.99 |
| Richer | 525 | 16.62 | 5413 | 22.28 |
| Middle | 607 | 20.05 | 5198 | 19.92 |
| Poorer | 658 | 20.34 | 5008 | 18.63 |
| Poorest | 904 | 29.28 | 4690 | 17.19 |
| Caste | ||||
| Others | 1051 | 30.28 | 5718 | 23.74 |
| OBC | 1196 | 52.9 | 10182 | 47.2 |
| SC/ST | 856 | 16.82 | 9999 | 29.07 |
| Religion | ||||
| Hindu | 2241 | 79.26 | 18,576 | 82.99 |
| Muslim | 342 | 13.37 | 2914 | 10.92 |
| Others | 520 | 7.36 | 4409 | 6.09 |
| Physical activity | ||||
| Active | 1759 | 60.26 | 16161 | 63.12 |
| Inactive | 1344 | 39.74 | 9738 | 36.88 |
| Alcohol consumption | ||||
| Never consumed | 2652 | 88.81 | 19283 | 76.77 |
| Infrequent | 263 | 6.43 | 3718 | 13.67 |
| frequent | 162 | 4 | 2568 | 8.36 |
| heavy drinker | 26 | 0.75 | 330 | 1.19 |
| Tobacco consumption | ||||
| Non consumer | 245 | 73.34 | 14173 | 50.65 |
| Currently smoking | 330 | 10.7 | 4301 | 17.23 |
| Smokeless tobacco | 445 | 14.03 | 6009 | 26.68 |
| Both smoking and smokeless | 83 | 1.94 | 1416 | 5.44 |
| Total | 3103 | 10.7 | 25899 | 89.3 |
SC/ST: Schedule caste/Schedule tribe, OBC: Other backward caste, MPCE: Monthly per capita consumption expenditure.
Table A3.
Matching statistics
| Treatment assignment | Off support | On support | Total |
|---|---|---|---|
| Untreated | 22,796 | 3103 | 25,899 |
| Treated | 0 | 3103 | 3103 |
| Total | 22,796 | 6206 | 29,002 |
Table A4.
Logistic regression estimates of Poor-self-rated health and Depression stratified by migration status
| Poor-SRH |
Depression |
|||||||
|---|---|---|---|---|---|---|---|---|
| Migrant |
Non-Migrant |
Migrant |
Non-Migrant |
|||||
| OR | 95 %CI | OR | 95 %CI | OR | 95 %CI | OR | 95 %CI | |
| Age | ||||||||
| 45–59 | Ref | Ref | Ref | Ref | ||||
| 60–74 | 1.48 | [0.93, 2.35] | 1.49*** | [1.30, 1.70] | 0.76 | [0.42, 1.39] | 0.83 | [0.70, 0.99] |
| 75+ | 1.99 | [0.95, 4.16] | 1.95*** | [1.58, 2.40] | 0.54 | [0.20, 1.48] | 0.85 | [0.60, 1.21] |
| Sex | ||||||||
| Male | Ref | Ref | Ref | Ref | ||||
| Female | 0.71 | [0.37, 1.35] | 1.18 | [0.99, 1.41] | 0.43* | [0.19, 0.99] | 0.84 | [0.65, 1.09] |
| Education | ||||||||
| Higher | Ref | Ref | Ref | Ref | ||||
| Secondary | 2.70*** | [1.41, 5.15] | 2.01*** | [1.53, 2.63] | 1.81*** | [1.68, 2.11] | 1.19*** | [0.86, 1.65] |
| Primary | 4.87*** | [2.44, 9.71] | 2.36*** | [1.78, 3.10] | 4.63*** | [2.33, 5.98] | 1.62*** | [1.13, 2.33] |
| Illiterate | 4.93*** | [2.28, 10.65] | 2.39*** | [1.84, 3.10] | 5.30*** | [1.80, 15.62] | 1.44*** | [1.04, 2.01] |
| Marital Status | ||||||||
| Married | Ref | Ref | Ref | Ref | ||||
| Widowed | 0.83 | [0.52, 1.33] | 1.00 | [0.84, 1.18] | 1.14 | [0.59, 2.19] | 1.34* | [1.06, 1.70] |
| Others | 0.62 | [0.29, 1.33] | 1.47** | [1.12, 1.93] | 0.79 | [0.28, 2.22] | 0.90 | [0.58, 1.38] |
| Employment status | ||||||||
| Currently working | Ref | Ref | Ref | Ref | ||||
| Never worked | 1.65 | [0.96, 2.84] | 1.64*** | [1.32, 2.06] | 2.11* | [1.00, 4.46] | 1.32 | [0.97, 1.80] |
| Retired | 2.87*** | [1.65, 5.01] | 2.12*** | [1.83, 2.45] | 2.61* | [1.23, 5.55] | 1.44*** | [1.17, 1.75] |
| Social participation | ||||||||
| Yes | Ref | Ref | Ref | Ref | ||||
| No | 0.57 | [0.27, 1.2] | 1.15 | [0.93, 1.44] | 1.15 | [0.46, 2.9] | 1.06 | [0.80, 1.40] |
| Food insecurity status | ||||||||
| No food insecurity | Ref | Ref | Ref | Ref | ||||
| Mild food insecurity | 1.31 | [0.86, 2.00] | 1.28*** | [1.14, 1.45] | 1.01 | [0.60, 1.72] | 1.27 | [1.06, 1.53] |
| Moderate food insecurity | 1.68 | [0.59, 4.79] | 2.32*** | [1.62, 3.34] | 6.25*** | [2.09, 18.74] | 2.18*** | [1.45, 3.27] |
| Severe food insecurity | 2.41*** | [1.33, 4.36] | 2.42*** | [1.93, 3.03] | 4.41*** | [2.19, 8.89] | 3.73*** | [2.86, 4.86] |
| MPCE quintile | ||||||||
| Richest | Ref | Ref | Ref | Ref | ||||
| Richer | 0.86 | [0.47, 1.57] | 1.08 | [0.91, 1.28] | 1.18 | [0.48, 2.89] | 0.88 | [0.69, 1.11] |
| Middle | 0.81 | [0.44, 1.50] | 1.04 | [0.86, 1.23] | 1.28 | [0.53, 3.09] | 1.18 | [0.91, 1.53] |
| Poorer | 1.28 | [0.69, 2.36] | 1.23* | [1.03, 1.45] | 1.61 | [0.67, 3.86] | 1.34 | [1.05, 1.71] |
| Poorest | 1.69 | [0.84, 3.36] | 1.11 | [0.91, 1.36] | 3.23* | [1.32, 5.91] | 1.59* | [1.23, 2.05] |
| Caste | ||||||||
| Others | Ref | Ref | Ref | Ref | ||||
| OBC | 0.52*** | [0.32, 0.87] | 0.86 | [0.73, 1.02] | 0.53 | [0.25, 1.14] | 1.17 | [0.93, 1.49] |
| SC/ST | 0.90 | [0.58, 1.39] | 1.03 | [0.90, 1.18] | 1.07 | [0.55, 2.06] | 1.24 | [1.02, 1.50] |
| Religion | ||||||||
| Hindu | Ref | Ref | Ref | Ref | ||||
| Muslim | 2.67*** | [1.31, 5.41] | 0.88 | [0.73, 1.06] | 3.87*** | [1.96, 7.65] | 0.85 | [0.62, 1.18] |
| Others | 1.25 | [0.68, 2.29] | 0.75** | [0.60, 0.94] | 1.33 | [0.51, 3.43] | 0.87 | [0.62, 1.21] |
| Physical activity | ||||||||
| Active | Ref | Ref | Ref | Ref | ||||
| Inactive | 1.17 | [0.8, 1.70] | 1.47*** | [1.31, 1.67] | 1.04 | [0.64, 1.68] | 1.21* | [1.03, 1.43] |
| Alcohol consumption | ||||||||
| Never consumed | Ref | Ref | Ref | Ref | ||||
| Infrequent | 0.94 | [0.47, 1.90] | 1.11 | [0.94, 1.3] | 0.68 | [0.25, 1.85] | 1.09 | [0.89, 1.35] |
| frequent | 0.39* | [0.18, 0.87] | 0.86 | [0.70, 1.06] | 0.52 | [0.19, 1.46] | 0.85 | [0.65, 1.11] |
| heavy drinker | 1.60 | [0.29, 8.81] | 0.73 | [0.44, 1.21] | 4.62 | [0.89, 23.87] | 1.39 | [0.82, 2.34] |
| Tobacco consumption | ||||||||
| Non consumer | Ref | Ref | Ref | Ref | ||||
| Currently smoking | 0.33* | [0.13, 0.85] | 1.14 | [0.96, 1.34] | 0.52 | [0.2, 1.31] | 1.25 | [0.98, 1.58] |
| Smokeless tobacco | 0.66 | [0.39, 1.12] | 0.90 | [0.78, 1.04] | 1.19 | [0.6, 2.37] | 1.46*** | [1.19, 1.80] |
| Both smoking and smokeless | 0.42 | [0.14, 1.22] | 1.26 | [0.94, 1.69] | 1.76 | [0.44, 7.05] | 1.70*** | [1.22, 2.36] |
| Pseudo R2 | 0.1694 | 0.0844 | 0.2544 | 0.0827 | ||||
Note: Ref: Reference, OR: Odds ratio, CI: Confidence Interval, SC/ST: Schedule caste/Schedule tribe, OBC: Other backward caste, MPCE: Monthly per capita consumption expenditure, ***p ≤ 0.001, **p < 0.01 and * p ≤ 0.05.
Table A5Logistic regression estimates of Multimorbidity, and functional limitation stratified by migration status
| Multimorbidity |
Functional limitation |
|||||||
|---|---|---|---|---|---|---|---|---|
| Migrant |
Non-Migrant |
Migrant |
Non-Migrant |
|||||
| OR | 95 %CI | OR | 95 %CI | OR | 95 %CI | OR | 95 %CI | |
| Age | ||||||||
| 45–59 | Ref | Ref | Ref | |||||
| 60–74 | 2.05*** | [1.34, 3.16] | 1.81*** | [1.54, 2.13] | 1.33 | [0.88, 2.02] | 1.81*** | [1.55, 2.12] |
| 75+ | 1.81 | [0.90, 3.62] | 1.37** | [1.09, 1.73] | 2.79*** | [1.40, 5.55] | 3.80*** | [3.04, 4.75] |
| Sex | ||||||||
| Male | Ref | Ref | Ref | Ref | ||||
| Female | 0.78 | [0.46, 1.34] | 1.50* | [1.10, 2.03] | 1.70 | [0.86, 3.36] | 1.81*** | [1.51, 2.18] |
| Education | ||||||||
| Higher | Ref | Ref | Ref | Ref | ||||
| Secondary | 1.90** | [1.17, 3.09] | 1.97*** | [1.36, 2.86] | 2.21*** | [0.05, 0.22] | 1.96** | [1.32, 2.91] |
| Primary | 1.97* | [1.51, 3.40] | 1.84*** | [1.43, 2.36] | 4.89*** | [0.12, 0.43] | 2.30*** | [1.62, 3.27] |
| Illiterate | 1.29 | [0.69, 2.41] | 1.28* | [1.07, 1.54] | 9.61*** | [4.55, 20.29] | 3.61*** | [2.57, 5.06] |
| Marital Status | ||||||||
| Married | Ref | Ref | Ref | Ref | ||||
| Widowed | 0.70 | [0.46, 1.08] | 0.99 | [0.77, 1.28] | 1.29 | [0.84, 1.98] | 1.13 | [0.91, 1.40] |
| Others | 0.62 | [0.29, 1.30] | 0.49*** | [0.35, 0.70] | 1.40 | [0.64, 3.05] | 0.97 | [0.76, 1.23] |
| Employment status | ||||||||
| Currently working | Ref | Ref | Ref | Ref | ||||
| Never worked | 1.95** | [1.21, 3.14] | 2.02*** | [1.44, 2.83] | 2.00** | [1.19, 3.36] | 2.25*** | [1.69, 2.98] |
| Retired | 2.84*** | [1.72, 4.69] | 2.21*** | [1.87, 2.60] | 3.86*** | [2.25, 6.62] | 2.88*** | [2.48, 3.35] |
| Social participation | ||||||||
| Yes | Ref | Ref | Ref | Ref | ||||
| No | 0.68 | [0.37, 1.23] | 1.11 | [0.88, 1.41] | 1.46 | [0.70, 3.05] | 1.04 | [0.75, 1.43] |
| Food insecurity status | ||||||||
| No food insecurity | Ref | Ref | Ref | Ref | ||||
| Mild food insecurity | 0.72 | [0.49, 1.06] | 1.16* | [1.00, 1.33] | 0.77 | [0.50, 1.18] | 0.94 | [0.82, 1.07] |
| Moderate food insecurity | 0.80 | [0.37, 1.72] | 1.34 | [0.94, 1.92] | 1.68 | [0.69, 4.11] | 1.53 | [1.07, 2.19] |
| Severe food insecurity | 2.21 | [1.24, 3.93] | 1.79** | [1.07, 2.98] | 1.29 | [0.70, 2.38] | 1.97*** | [1.58, 2.46] |
| MPCE quintile | ||||||||
| Richest | Ref | Ref | Ref | Ref | ||||
| Richer | 0.70 | [0.40, 1.23] | 1.27 | [1.04, 1.56] | 1.02 | [0.57, 1.80] | 0.93 | [0.78, 1.11] |
| Middle | 0.88 | [0.51, 1.52] | 1.38* | [1.14, 1.68] | 0.71 | [0.39.1.27] | 0.90 | [0.75, 1.09] |
| Poorer | 1.56 | [0.90, 2.69] | 1.92*** | [1.57, 2.35] | 1.35 | [0.76, 2.39] | 1.00 | [0.83, 1.18] |
| Poorest | 3.24*** | [1.78, 5.90] | 2.77*** | [2.10, 3.66] | 1.78 | [0.89, 3.54] | 1.01 | [0.74, 1.37] |
| Caste | ||||||||
| Others | Ref | Ref | Ref | Ref | ||||
| OBC | 1.25 | [0.79, 1.97] | 1.28* | [1.05, 1.56] | 0.79 | [0.49, 1.27] | 0.91 | [0.76, 1.1] |
| SC/ST | 1.63** | [1.06, 2.50] | 1.35*** | [1.15, 1.59] | 0.68 | [0.44, 1.05] | 1.27*** | [1.1, 1.47] |
| Religion | ||||||||
| Hindu | Ref | Ref | Ref | Ref | ||||
| Muslim | 2.68** | [1.41, 5.13] | 1.75*** | [1.25, 2.46] | 3.77*** | [1.80, 7.87] | 0.83 | [0.67, 1.04] |
| Others | 1.36 | [0.74, 2.50] | 1.19 | [0.96, 1.48] | 0.77 | [0.44, 1.35] | 1.05 | [0.80, 1.38] |
| Physical activity | ||||||||
| Active | Ref | Ref | Ref | Ref | ||||
| Inactive | 0.88 | [0.63, 1.22] | 1.27*** | [1.09, 1.48] | 1.71*** | [1.19, 2.45] | 1.23** | [1.06, 1.42] |
| Alcohol consumption | ||||||||
| Never consumed | Ref | Ref | Ref | Ref | ||||
| Infrequent | 0.94 | [0.51, 1.72] | 1.32*** | [1.10, 1.58] | 0.69 | [0.32, 1.52] | 0.92 | [0.78, 1.08] |
| frequent | 0.54 | [0.21, 1.36] | 1.00 | [0.81, 1.23] | 0.61 | [0.28, 1.32] | 0.89 | [0.73, 1.08] |
| heavy drinker | 0.80 | [0.11, 5.81] | 0.58 | [0.31, 1.07] | 0.42 | [0.06, 2.88] | 0.65 | [0.37, 1.14] |
| Tobacco consumption | ||||||||
| Non consumer | Ref | Ref | Ref | Ref | ||||
| Currently smoking | 0.26** | [0.12, 0.56] | 0.72*** | [0.59, 0.87] | 1.21 | [0.55, 2.63] | 0.99 | [0.84, 1.17] |
| Smokeless tobacco | 0.54** | [0.34, 0.85] | 0.71*** | [0.61, 0.84] | 0.87 | [0.52, 1.44] | 1.28*** | [1.1, 1.49] |
| Both smoking and smokeless | 0.27** | [0.09, 0.83] | 0.92 | [0.70, 1.21] | 3.10 | [0.81, 11.83] | 1.18 | [0.92, 1.52] |
| Pseudo R2 | 0.1955 | 0.1042 | 0.2685 | 0.1693 | ||||
Note: Ref: Reference, OR: Odds ratio, CI: Confidence Interval, SC/ST: Schedule caste/Schedule tribe, OBC: Other backward caste, MPCE: Monthly per capita consumption expenditure, ***p ≤ 0.001, **p < 0.01 and * p ≤ 0.05.
Data availability
Data is publicly available on request from -https://iipsindia.ac.in/sites/default/files/LASI_DataRequestForm_0.pdf
References
- Akram M. Occupational disease and public health concerns of migrant construction workers: A social epidemiological study in western Uttar Pradesh. Social Change. 2014;44(1):97–117. doi: 10.1177/0049085713514828. [DOI] [Google Scholar]
- Allen J.D., Kunicki Z.J., Greaney M.L. Mental health of Brazilian immigrant women: The role of discrimination, social support, and community strengths. Journal of Immigrant and Minority Health. 2023;25(5):1016–1024. doi: 10.1007/S10903-023-01485-2/TABLES/2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Anikeeva O., Bi P., Hiller J.E., Ryan P., Roder D., Han G.S. Trends in cancer mortality rates among migrants in Australia: 1981–2007. Cancer Epidemiology. 2012;36(2):e74–e82. doi: 10.1016/J.CANEP.2011.10.011. [DOI] [PubMed] [Google Scholar]
- Anjali B. 2016. Migrant's (Denied) access to health care in India. 2016. [Google Scholar]
- Ansari S., Anand A., Singh S., Hossain B. Exploring food insecurity and multimorbidity in Indian socially disadvantaged people: Cross-sectional findings from LASI, 2017–18. BMC Public Health. 2023;23(1):1–13. doi: 10.1186/S12889-023-16132-6/TABLES/6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Babu B.v., Swain B.K., Mishra S., Kar S.K. Primary healthcare services among a migrant indigenous population living in an eastern Indian city. Journal of Immigrant and Minority Health. 2010;12(1):53–59. doi: 10.1007/S10903-008-9181-Z/TABLES/1. [DOI] [PubMed] [Google Scholar]
- Banal R., Thappa J., Shah H.U., Hussain A., Chowhan A., Kaur H., et al. Psychiatric morbidity in adult Kashmiri migrants living in a migrant camp at Jammu. Indian Journal of Psychiatry. 2010;52(2):154–158. doi: 10.4103/0019-5545.64597. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Barman P., Saha A., Dakua M., Roy A. Does the intensity of religiosity and spirituality in later life improve mental well-being? Evidence from India. Journal of Religion, Spirituality and Aging. 2023;35(4):455–475. doi: 10.1080/15528030.2022.2100560. [DOI] [Google Scholar]
- Bhagat R., Sahoo H., Roy A.K., Govil D. Vol. 17. 2020. pp. 705–718. (The COVID-19, migration and livelihood in India: Challenges and policy issues). 5. [DOI] [Google Scholar]
- Bloom D.E., Sekher T.V., Lee J. Longitudinal aging study in India (LASI): New data resources for addressing aging in India. Nature Aging. 2021;1(12):1070–1072. doi: 10.1038/s43587-021-00155-y. 2021 1:12. [DOI] [PubMed] [Google Scholar]
- Cabieses B., Tunstall H., Pickett K. Testing the latino paradox in Latin America: A population-based study of intra-regional immigrants in Chile. Revista Medica de Chile. 2013;141(10):1255–1265. doi: 10.4067/S0034-98872013001000004. [DOI] [PubMed] [Google Scholar]
- Chen F., Zheng M., Xu J., Hall B.J., Pan Y., Ling L., et al. Impact of migration status on incidence of depression in the middle-aged and elderly population in China: Exploring healthy migrant and salmon bias hypotheses from a mental health perspective. Journal of Affective Disorders. 2022;315:182–189. doi: 10.1016/j.jad.2022.07.048. [DOI] [PubMed] [Google Scholar]
- Choithani C. Understanding the linkages between migration and household food security in India. Geographical Research. 2017;55(2):192–205. doi: 10.1111/1745-5871.12223. [DOI] [Google Scholar]
- Chung Y.-N., Ka G., Chung K., Ahmed D., Benavente P., Diaz E. Food insecurity among international migrants during the COVID-19 pandemic: A scoping review. International Journal of Environmental Research and Public Health. 2023;20(7):5273. doi: 10.3390/IJERPH20075273. 2023, Vol. 20, Page 5273. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Dannefer D. Cumulative advantage/disadvantage and the life course: Cross-fertilizing age and social science theory. The Journals of Gerontology: Serie Bibliographique. 2003;58(6):S327–S337. doi: 10.1093/GERONB/58.6.S327. [DOI] [PubMed] [Google Scholar]
- Dodd W., Humphries S., Patel K., Majowicz S., Little M., Dewey C. Determinants of internal migrant health and the healthy migrant effect in south India: A mixed methods study. BMC International Health and Human Rights. 2017;17(1):1–12. doi: 10.1186/S12914-017-0132-4/TABLES/2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ebrahim S., Kinra S., Bowen L., Andersen E., Ben-Shlomo Y., Lyngdoh T., et al. The effect of rural-to-urban migration on obesity and diabetes in India: A cross-sectional study. PLoS Medicine. 2010;7(4) doi: 10.1371/JOURNAL.PMED.1000268. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Essayagh F., Essayagh M., Essayagh S., Marc I., Bukassa G., El otmani I., et al. The prevalence and risk factors for anxiety and depression symptoms among migrants in Morocco. Scientific Reports. 2023;13(1):1–10. doi: 10.1038/s41598-023-30715-8. 2023 13:1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Fang D., Thomsen M.R., Nayga R.M. The association between food insecurity and mental health during the COVID-19 pandemic. BMC Public Health. 2021;21(1):1–8. doi: 10.1186/S12889-021-10631-0/FIGURES/1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Firdaus G. Mental well-being of migrants in urban center of India: Analyzing the role of social environment. Indian Journal of Psychiatry. 2017;59(2):164–169. doi: 10.4103/PSYCHIATRY.INDIANJPSYCHIATRY_272_15. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Foo S.Q., Tam W.W., Ho C.S., Tran B.X., Nguyen L.H., McIntyre R.S., et al. Prevalence of depression among migrants: A systematic review and meta-analysis. International Journal of Environmental Research and Public Health. 2018;15(9):1986. doi: 10.3390/IJERPH15091986. 2018, Vol. 15, Page 1986. [DOI] [PMC free article] [PubMed] [Google Scholar]
- García-Cid A., Gómez-Jacinto L., Hombrados-Mendieta I., Millán-Franco M., Moscato G. Discrimination and psychosocial well-being of migrants in Spain: The moderating role of sense of community. Frontiers in Psychology. 2020;11 doi: 10.3389/FPSYG.2020.02235/BIBTEX. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gkiouleka A., Avrami L., Kostaki A., Huijts T., Eikemo T.A., Stathopoulou T. Depressive symptoms among migrants and non-migrants in europe: Documenting and explaining inequalities in times of socio-economic instability. The European Journal of Public Health. 2018;28(suppl_5):54–60. doi: 10.1093/EURPUB/CKY202. [DOI] [PubMed] [Google Scholar]
- Groot W., Maassen Van Den Brink H. 2006. 4.A. What does education do to our health?https://www.oecd.org/education/innovation-education/37425763.pdf [Google Scholar]
- Helgesson M., Johansson B., Nordquist T., Vingård E., Svartengren M. Healthy migrant effect in the Swedish context: A register-based, longitudinal cohort study. BMJ Open. 2019;9(3) doi: 10.1136/BMJOPEN-2018-026972. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hirudayaraj M., Barhate B., McLean G.N. Work conditions of interstate migrant workers in India: A critical realist exploration. Human Resource Development Quarterly. 2023 doi: 10.1002/HRDQ.21515. [DOI] [Google Scholar]
- Hombrados-Mendieta I., Millán-Franco M., Gómez-Jacinto L., Gonzalez-Castro F., Martos-Méndez M.J., García-Cid A. Positive influences of social support on sense of community, life satisfaction and the health of immigrants in Spain. Frontiers in Psychology. 2019;10:2555. doi: 10.3389/FPSYG.2019.02555/BIBTEX. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Jang H., Tang F. Loneliness, age at immigration, family relationships, and depression among older immigrants: A moderated relationship. Journal of Social and Personal Relationships. 2021;39(6):1602–1622. doi: 10.1177/02654075211061279. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Jatrana S., Richardson K., Pasupuleti S.S.R. Investigating the dynamics of migration and health in Australia: A longitudinal study. European Journal of Population. 2018;34(4):519–565. doi: 10.1007/S10680-017-9439-Z/TABLES/9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Jayaram N., Varma D. Examining the ‘labour’ in labour migration: Migrant workers' informal work arrangements and access to labour rights in urban sectors. Indian Journal of Labour Economics. 2020;63(4):999–1019. doi: 10.1007/S41027-020-00288-5/METRICS. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Jones A.D. Food insecurity and mental health status: A global analysis of 149 countries. American Journal of Preventive Medicine. 2017;53(2):264–273. doi: 10.1016/J.AMEPRE.2017.04.008. [DOI] [PubMed] [Google Scholar]
- Juárez S.P., Revuelta-Eugercios Exploring the ’healthy migrant paradox’ in Sweden. A cross sectional study focused on perinatal outcomes. Journal of Immigrant and Minority Health. 2016;18:42–50. doi: 10.1007/s10903-015-0157-5. [DOI] [PubMed] [Google Scholar]
- Jurado D., Alarcón R.D., Martínez-Ortega J.M., Mendieta-Marichal Y., Gutiérrez-Rojas L., Gurpegui M. Factors associated with psychological distress or common mental disorders in migrant populations across the world. Revista de Psiquiatía y Salud Mental. 2017;10(1):45–58. doi: 10.1016/J.RPSMEN.2017.02.004. [DOI] [PubMed] [Google Scholar]
- Kimbrough J. Health literacy as a contributor to immigrant health disparities. Journal of Health Disparities Research and Practice. 2012;1(2) https://digitalscholarship.unlv.edu/jhdrp/vol1/iss2/6 [Google Scholar]
- Kreps G.L., Sparks L. Meeting the health literacy needs of immigrant populations. Patient Education and Counseling. 2008;71(3):328–332. doi: 10.1016/J.PEC.2008.03.001. [DOI] [PubMed] [Google Scholar]
- Kumar A., Chery L., Biswas C., Dubhashi N., Dutta P., Dua V.K., et al. Malaria in south asia: Prevalence and control. Acta Tropica. 2012;121(3):246–255. doi: 10.1016/j.actatropica.2012.01.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lanari D., Bussini O. International migration and health inequalities in later life. Ageing and Society. 2012;32(6):935–962. doi: 10.1017/S0144686X11000730. [DOI] [Google Scholar]
- LASI International Institute for Population Sciences (IIPS), NPHCE, MoHFW, et al. Longitudinal Ageing Study in India (LASI) Wave 1. 2020. https://lasi.hsph.harvard.edu/files/lasi/files/lasi_india_report_2020.pdf?m=1610054498 Mumbai, India.
- Lee J., Seon J. Educational attainment and health behaviors among young adult men: Racial/ethnic disparities. American Journal of Men's Health. 2019;13(6) doi: 10.1177/1557988319894488/ASSET/IMAGES/LARGE/10.1177_1557988319894488-FIG2.JPEG. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lu Y. Test of the ‘healthy migrant hypothesis’: A longitudinal analysis of health selectivity of internal migration in Indonesia. Social Science & Medicine. 2008;67(8):1331–1339. doi: 10.1016/J.SOCSCIMED.2008.06.017. [DOI] [PubMed] [Google Scholar]
- Lu Y. Rural-urban migration and health: Evidence from longitudinal data in Indonesia. Social Science & Medicine. 2010;70(3):412–419. doi: 10.1016/J.SOCSCIMED.2009.10.028. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lu Y., Qin L. Healthy migrant and salmon bias hypotheses: A study of health and internal migration in China. Social Science & Medicine. 2014;102:41–48. doi: 10.1016/J.SOCSCIMED.2013.11.040. [DOI] [PubMed] [Google Scholar]
- MacKinnon M.J., Picchio C.A., Nomah D.K., Segura A.R., van Selm L., Fernández E., et al. Chronic conditions and multimorbidity among West African migrants in greater Barcelona, Spain. Frontiers in Public Health. 2023;11 doi: 10.3389/FPUBH.2023.1142672/BIBTEX. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Mandal B., Pradhan K.C., Mohanty P., Muhammad T. Migration status, physical limitations and associated self-rated health: A study of older Indian adults. BMC Geriatrics. 2023;23(1):1–16. doi: 10.1186/S12877-023-04002-0/FIGURES/1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Margolis R. Educational differences in healthy behavior changes and adherence among middle-aged Americans. Journal of Health and Social Behavior. 2013;54(3):353–368. doi: 10.1177/0022146513489312/ASSET/IMAGES/LARGE/10.1177_0022146513489312-FIG2.JPEG. [DOI] [PMC free article] [PubMed] [Google Scholar]
- María A., Arias Uriona F. 2020. Dynamics of health and Welfare. [Google Scholar]
- Marin I.B., Fernández D., Ayuso-Mateos J.L., Leonardi M., Tobiasz-Adamczyk B., Koskinen S., et al. Healthy aging and late-life depression in Europe: Does migration matter? Frontiers of Medicine. 2022;9:3038. doi: 10.3389/FMED.2022.866524/BIBTEX. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Marques M., Gama A., Cheng C., Osborne R., Dias S. Addressing health literacy to reduce inequalities among migrants: Which profiles need our attention? The European Journal of Public Health. 2022;32(Supplement_3) doi: 10.1093/EURPUB/CKAC131.368. [DOI] [Google Scholar]
- McAuliffe M., Khadria B. 1953. International organization for migration. 2020). World migration report 2020. [Google Scholar]
- McDonald J.T., Kennedy S. Insights into the ‘healthy immigrant effect’: Health status and health service use of immigrants to Canada. Social Science & Medicine. 2004;59(8):1613–1627. doi: 10.1016/J.SOCSCIMED.2004.02.004. [DOI] [PubMed] [Google Scholar]
- McGuire S. FAO, IFAD, and WFP. The state of food insecurity in the world 2015: Meeting the 2015 international hunger targets: Taking stock of uneven progress. Rome: FAO, 2015. Advances in Nutrition. 2015;6(5):623–624. doi: 10.3945/AN.115.009936. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Muhammad T., Skariah A.E., Kumar M., Srivastava S. Socioeconomic and health-related inequalities in major depressive symptoms among older adults: A wagstaff's decomposition analysis of data from the LASI baseline survey, 2017–2018. BMJ Open. 2022;12(6) doi: 10.1136/BMJOPEN-2021-054730. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Nagata J.M., Palar K., Gooding H.C., Garber A.K., Bibbins-Domingo K., Weiser S.D. Food insecurity and chronic disease in US young adults: Findings from the national longitudinal study of adolescent to adult health. Journal of General Internal Medicine. 2019;34(12):2756–2762. doi: 10.1007/S11606-019-05317-8/TABLES/3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Nitika A.L., Nongkynrih B., Gupta S. Migrants to urban India: Need for public health action. Indian Journal of Community Medicine: Official Publication of Indian Association of Preventive & Social Medicine. 2014;39(2):73. doi: 10.4103/0970-0218.132718. [DOI] [PMC free article] [PubMed] [Google Scholar]
- O'Rand A.M. The precious and the precocious: Understanding cumulative disadvantage and cumulative advantage over the life course. The Gerontologist. 1996;36(2):230–238. doi: 10.1093/GERONT/36.2.230. [DOI] [PubMed] [Google Scholar]
- Orjuela-Grimm M., Deschak C., Aragon Gama C.A., Bhatt Carreño S., Hoyos L., Mundo V., et al. Migrants on the move and food (In)security: A call for research. Journal of Immigrant and Minority Health. 2022;24(5):1318–1327. doi: 10.1007/S10903-021-01276-7/TABLES/1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Oshio T. Widening disparities in health between educational levels and their determinants in later life: Evidence from a nine-year cohort study. BMC Public Health. 2018;18(1):1–10. doi: 10.1186/S12889-018-5181-7/TABLES/4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Patel R., Kumar S., Chauhan S. Exploring association between food insecurity and depression among older adults in India. Dialogues in Health. 2022;1 doi: 10.1016/J.DIALOG.2022.100042. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Patel P., Muhammad T., Sahoo H. The burden of disease-specific multimorbidity among older adults in India and its states: Evidence from LASI. BMC Geriatrics. 2023;23(1) doi: 10.1186/S12877-023-03728-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Paul M., Mandal S., Samanta R. Does early-life migration experience determine health and health-risk behavior in later life? Evidence from elderly returns migrants in Kerala, India. SSM - Population Health. 2023;23 doi: 10.1016/J.SSMPH.2023.101449. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Perianayagam A., Bloom D., Lee J., Parasuraman S., Sekher T.v., Mohanty S.K., et al. Cohort profile: The longitudinal ageing study in India (LASI) International Journal of Epidemiology. 2022;51(4):e167–e176. doi: 10.1093/IJE/DYAB266. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Rada I., Oyarte M., Cabieses B. A comparative analysis of health status of international migrants and local population in Chile: A population-based, cross-sectional analysis from a social determinants of health perspective. BMC Public Health. 2022;22(1):1–19. doi: 10.1186/S12889-022-13709-5/TABLES/9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Raghupathi V., Raghupathi W. The influence of education on health: An empirical assessment of OECD countries for the period 1995-2015. Archives of Public Health. 2020;78(1):1–18. doi: 10.1186/S13690-020-00402-5/FIGURES/17. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Rajan S.I. India migration report 2021 : Migrants and health (irudaya rajan sebastian. 1st ed., Vol. 1. Taylor & Francis Limited; 2022. [Google Scholar]
- Rajan S.I., Bhagat R.B. Internal migration and the covid-19 pandemic in India. IMISCOE Research Series. 2022:227–248. doi: 10.1007/978-3-030-81210-2_12. [DOI] [Google Scholar]
- Rajan S.I., Bhagat R.B., Ram B. In: Researching internal migration. 1st ed., Vol. 1. Irudaya Rajan S., Bhagat R.B., editors. 2022. [Google Scholar]
- Ravindranath D., Mohan P. Migration and health: Charting questions for future research. India Migration Report 2021. Migrants and Health. 2022:1–8. doi: 10.4324/9781003287667-1/MIGRATION-HEALTH-DIVYA-RAVINDRANATH-PAVITRA-MOHAN. [DOI] [Google Scholar]
- Reus-Pons M., Kibele E.U.B., Janssen F. Differences in healthy life expectancy between older migrants and non-migrants in three European countries over time. International Journal of Public Health. 2017;62(5):531–540. doi: 10.1007/S00038-017-0949-6/TABLES/5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Reus-Pons M., Mulder C.H., Kibele E.U.B., Janssen F. Differences in the health transition patterns of migrants and non-migrants aged 50 and older in southern and western Europe (2004–2015) BMC Medicine. 2018;16(1) doi: 10.1186/S12916-018-1044-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Rosenbaum P.R., Rubin D.B. The central role of the propensity score in observational studies for causal effects. Biometrika. 1983;70(1):41–55. doi: 10.1093/BIOMET/70.1.41. [DOI] [Google Scholar]
- Saggurti N., Schensul S.L., Verma R.K. Migration, mobility and sexual risk behavior in Mumbai, India: Mobile men with non-residential wife show increased risk. AIDS and Behavior. 2009;13(5):921–927. doi: 10.1007/s10461-009-9564-8. [DOI] [PubMed] [Google Scholar]
- Saggurti N., Verma R.K., Jain A., Ramarao S., Anil Kumar K., Subbiah A., et al. HIV risk behaviours among contracted and non-contracted male migrant workers in India: Potential role of labour contractors and contractual systems in HIV prevention. AIDS. 2008;22(SUPPL. 5):S127–S136. doi: 10.1097/01.aids.0000343771.75023.cc. [DOI] [PubMed] [Google Scholar]
- Saha A., Mandal B., Muhammad T., Barman P., Ahmed W. Gender-specific determinants of overweight and obesity among older adults in India: Evidence from a cross-sectional survey, 2017-18. BMC Public Health. 2023;23(1):1–15. doi: 10.1186/S12889-023-17156-8/TABLES/3. [DOI] [PMC free article] [PubMed] [Google Scholar] [Retracted]
- Saha A., Muhammad T., Mandal Id B., Adhikary M., Barman P. Socio-demographic and behavioral correlates of excess weight and its health consequences among older adults in India: Evidence from a cross-sectional study, 2017–18. PLoS One. 2023;18(10) doi: 10.1371/JOURNAL.PONE.0291920. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Saha A., Rahaman M., Mandal B., Biswas S., Govil D. Rural urban differences in self-rated health among older adults: Examining the role of marital status and living arrangements. BMC Public Health. 2022;22(1):1–15. doi: 10.1186/S12889-022-14569-9/TABLES/4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Salinero-Fort M.Á., Del Otero-Sanz L., Martín-Madrazo C., De Burgos-Lunar C., Chico-Moraleja R.M., Rodés-Soldevila B., et al. The relationship between social support and self-reported health status in immigrants: An adjusted analysis in the Madrid Cross Sectional Study. BMC Family Practice. 2011;12(1):1–9. doi: 10.1186/1471-2296-12-46/TABLES/3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Samanta R., Munda J., Mandal S., Adhikary M. Health-care utilisation among India's middle and older aged migrants: Scrutinizing the status and predictors using andersen's simplified healthcare utilisation framework. International Journal of Migration, Health and Social Care. 2023;19(2):142–156. doi: 10.1108/IJMHSC-07-2022-0068/FULL/XML. [DOI] [Google Scholar]
- Sarivaara E., Uusiautti S., Määttä K. Occupational health problems of women migrant workers in thogamalai, karur district, Tamil nadu, India. International Research Journal of Social Sciences. 2013;2(1):1–7. doi: 10.5296/ijssr.v2i1.4521. [DOI] [Google Scholar]
- Seligman H.K., Bindman A.B., Vittinghoff E., Kanaya A.M., Kushel M.B. Food insecurity is associated with diabetes mellitus: Results from the national health examination and nutrition examination survey (NHANES) 1999–2002. Journal of General Internal Medicine. 2007;22(7):1018–1023. doi: 10.1007/s11606-007-0192-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Seligman H.K., Laraia B.A., Kushel M.B. Food insecurity is associated with chronic disease among low-income NHANES participants. The Journal of Nutrition. 2010;140(2):304–310. doi: 10.3945/JN.109.112573. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Singh S.K., Chauhan K., Puri P. Chronic non-communicable disease burden among reproductive-age women in India: Evidence from recent demographic and health survey. BMC Women's Health. 2023;23(1):1–15. doi: 10.1186/S12905-023-02171-Z/TABLES/4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sinha A., Kerketta S., Ghosal S., Kanungo S., Pati S. Multimorbidity among urban poor in India: Findings from LASI, wave-1. Frontiers in Public Health. 2022;10 doi: 10.3389/FPUBH.2022.881967/BIBTEX. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sivaraju S., Alam M., Verma S. 2017. Caring for our elders: Early responses India ageing report-2017.https://india.unfpa.org/sites/default/files/pub-pdf/India%20Ageing%20Report%20-%202017%20%28Final%20Version%29.pdf [Google Scholar]
- Srinivasan S., Ilango P. SSRN Electronic Journal; 2013. Occupational health problems of women migrant workers in thogamalai, karur district, Tamil nadu, India. [DOI] [Google Scholar]
- Srivastava S., Chauhan S., Patel R. Socio-economic inequalities in the prevalence of poor self-rated health among older adults in India from 2004 to 2014: A decomposition analysis. Ageing International. 2021;46(2):182–199. doi: 10.1007/S12126-020-09385-8/TABLES/5. [DOI] [Google Scholar]
- Srivastava S., Joseph K.J.V., Dristhi D., Muhammad T. Interaction of physical activity on the association of obesity-related measures with multimorbidity among older adults: A population-based cross-sectional study in India. BMJ Open. 2021;11(5) doi: 10.1136/BMJOPEN-2021-050245. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Srivastava S., Singh R., Mishra P.S., Aditya A. Association of cognitive impairment with migrant status among older adults in India: A cross-sectional study. Handbook of Aging, Health and Public Policy. 2023;1–23 doi: 10.1007/978-981-16-1914-4_192-1. [DOI] [Google Scholar]
- Tsoh J.Y., Sentell T., Gildengorin G., Le G.M., Chan E., Fung L.C., et al. Healthcare communication barriers and self-rated health in older Chinese American immigrants. Journal of Community Health. 2016;41(4):741–752. doi: 10.1007/S10900-015-0148-4/TABLES/3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wang B., Li X., Stanton B., Fang X. The influence of social stigma and discriminatory experience on psychological distress and quality of life among rural-to-urban migrants in China. Social Science & Medicine. 2010;71(1):84–92. doi: 10.1016/J.SOCSCIMED.2010.03.021. [DOI] [PubMed] [Google Scholar]
- WHO Reprinted from: World report on ageing and health: Chapter 3: Health in older age. 2015. http://www.who.int/ageing/publications/world-report-2015/en/ WHO.
- WHO . 2016. Multimorbidity technical series on safer primary care multimorbidity: Technical series on safer primary care.http://apps.who.int/bookorders [Google Scholar]
- Wickramage K., Vearey J., Zwi A.B., Robinson C., Knipper M. Migration and health: A global public health research priority. BMC Public Health. 2018;18(1):1–9. doi: 10.1186/S12889-018-5932-5/TABLES/2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- World Population Prospects . World population prospects 2019. 2019. World population Prospects.https://www.un.org/development/desa/pd/sites/www.un.org.development.desa.pd/files/files/documents/2020/Jan/wpp2019_highlights.pdf [Google Scholar]
- Zajacova A., Lawrence E.M. Vol. 39. 2018. pp. 273–289. (The relationship between education and health: Reducing disparities through a contextual approach). 10.1146/Annurev-Publhealth-031816-044628. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Záleská V., Brabcová I., Vacková J. Migration and its impact on mental and physical health: Social support and its main functions. Kontakt. 2014;16(4):e236–e241. doi: 10.1016/J.KONTAKT.2014.05.007. [DOI] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
Data is publicly available on request from -https://iipsindia.ac.in/sites/default/files/LASI_DataRequestForm_0.pdf