Abstract
Objectives
Guided by the theory of stress proliferation, our study examined whether loneliness, citizenship status, and English proficiency were associated with psychological distress among older adults, and if citizenship status and English proficiency moderated these relationships.
Methods
Using the older adult subsample (65+ years) of the 2019–2020 California Health Interview Survey (N = 15,210), we assessed cross-sectional associations between loneliness, citizenship status, and English proficiency on psychological distress by conducting multivariable linear regression models. Interaction terms were included in subsequent models to determine if citizenship status and English proficiency moderated the relationship between loneliness and psychological distress.
Results
In unadjusted models, greater loneliness was associated with higher distress. Both naturalized citizens and noncitizens, and those with limited English proficiency (LEP) exhibited greater distress than US born citizens and those who speak English only (EO). After adjusting for sociodemographic and health covariables, loneliness remained significant for distress although the relationships between citizenship status and English proficiency became attenuated. With the inclusion of interactions, the magnitude of the relationship between loneliness and distress was stronger for naturalized citizens and those with LEP than native-born citizens and those who speak EO, respectively.
Discussion
Loneliness was the most consistent stressor affecting multiple life domains. However, our findings demonstrate that stress proliferation is occurring among older immigrant adults and the interplay between loneliness, citizenship status, and English proficiency is contributing to heightened distress. Further attention is needed in understanding the role of multiple stressors influencing mental health among immigrant older adults.
Keywords: Citizenship status, Immigration, Loneliness, Psychological distress, Stress proliferation, Stressors
A robust body of literature has examined whether and how unique stressors tied to immigration shape mental health disparities among immigrants, including older immigrant populations in the United States (Kirmayer et al., 2011; Mui & Kang, 2006; Pumariega et al., 2005). Across age groups, new immigrants are often confronted with numerous challenges that adversely affect mental health, including language and other cultural differences, obtaining employment, changes to their social status and family structure, and difficulties accessing health care and social services (G. Kim et al., 2011; Kirmayer et al., 2011). As a result, immigration-related stressors have been associated with greater psychological distress and poorer mental health outcomes (Torres & Wallace, 2013; Yoo et al., 2009). While this body of literature provides important insights into the relationships between immigration-related stressors and mental health disparities among older immigrant populations, questions regarding how other immigration-related stressors shape health outcomes remain unanswered. For older immigrants, some of these challenges are further compounded with aging, including the loss of primary social relationships and leaving behind familiar places, potentially leading to greater loneliness (Fokkema & Ciobanu, 2021).
Research demonstrates that loneliness, citizenship status, and English proficiency uniquely shape mental health among older immigrants (Fokkema & Ciobanu, 2021; Jang & Tang, 2022; G. Kim et al., 2011). Empirical scholarship on older immigrants is still in novel stages and has yet to determine how loneliness shapes relationships between unique immigration-related stressors (citizenship status, English proficiency) and psychological distress. The aims of our study are: (a) to examine how each of these stressors (loneliness, citizenship status, and English proficiency) affect psychological distress, and (b) to determine if the effects of loneliness on psychological distress are further amplified by citizenship status and English proficiency among older adults in California. California is an ideal setting for the current study as it has the largest population of older adults 65 years or older (5.9 million) in the United States (Kilduff, 2021). Additionally, one-fourth of Californians are foreign-born, with a sizeable population of Latinx and Asian immigrants, the two fastest growing immigrant groups in the United States (H. Johnson et al., 2021).
Stress and Health Framework
Researchers have outlined dynamic mechanisms of how stress contributes to health inequities (Pearlin et al., 2005; Thoits, 2010). One key development is the stress proliferation theory, which refers to a process by which a stressor may induce other stressors (Pearlin et al., 2005). Stressors that repeatedly emerge over time and major life events often have deleterious consequences for health because they disrupt an individual’s level of activities, quality of relationships, and social status. Stress proliferation is characterized by an initial stressor impacting other life domains and stressors (Thoits, 2010), further amplifying the effect of these stressors on health. Pearlin et al. (1997) posit that the stress proliferation process is not uniformly experienced across populations. In other words, the emergence and magnitude of stress proliferation are dependent on social and economic factors, such as citizenship status and English proficiency, and the ability to draw forth adequate resources (e.g., support) in navigating these challenges.
Many older migrants arrive in the United States to reunite with family members who migrated earlier (Carr & Tienda, 2013). Though they may be living with family members, these relations may not necessarily translate into sources of social support (Treas & Mazumdar, 2002). We posit that older immigrants may be more vulnerable to experiencing loneliness as they are often required to re-establish social networks and leave behind friends and family (Fokkema & Ciobanu, 2021). Moreover, the effects of loneliness on psychological distress may be further amplified among older noncitizens and those with a limited command of English, as detailed in following sections.
Loneliness Among Immigrants
Loneliness is a distressing and unpleasant feeling. It occurs when an individual is dissatisfied with the quality, frequency of contact, and/or closeness of the relationships they maintain with members of their social network (National Academies of Sciences, Engineering, and Medicine, 2020). Older adults experiencing greater loneliness are more likely to have worse physical and mental health and earlier mortality (National Academies of Sciences, Engineering, and Medicine, 2020). Loneliness is a critical factor to examine among older immigrants given they frequently report greater loneliness compared with older nonmigrants (Ali et al., 2021; Fokkema & Ciobanu, 2021), and because the migration process itself may exacerbate the influence of loneliness on mental health.
Loneliness among older immigrants may not only stem from the stress associated with the migration process but also during the process of adjusting to living in a new country and establishing new networks. Specifically, this includes missing relatives and friends back home, learning a new language, experiencing difficulties securing employment or housing, navigating new health and social systems, as well as experiencing racism, and xenophobia (Ali et al., 2021; Fokkema & Ciobanu, 2021). These integration processes can be viewed as chronic stressors among older immigrants, which is critical to understand given that chronic stress has been associated with greater loneliness among older adults (Hawkley et al., 2008).
Immigration Stressors and Health
Citizenship Status
Citizenship status is considered an idealized social status for immigrants. Becoming a naturalized U.S. citizen signifies becoming an “American” and has been linked to increased feelings of “belonging” (Van Hook et al., 2006). Moreover, Gee et al. (2016) found that noncitizens report lower subjective social status and greater levels of distress than citizens. Citizenship confers further advantages in becoming more integrated in society through formalized membership into a nation state via exclusive political, social, and civil rights (Bloemraad et al., 2008). This enables citizens to engage in the democratic process and have access to federal resources although noncitizens including temporary visa status holders and undocumented immigrants are excluded from these rights and resources.
An individual’s socioeconomic position is associated with opportunities that may place individuals at further disadvantage or advantage contributing to differential exposures to stress (Pearlin et al., 2005). For example, the eligibility criteria for applying for federal assistance and many employment opportunities require the applicant to either be a U.S. citizen or permanent resident (Fix & Passel, 2002). After the enactment of the Personal Responsibility and Work Opportunity Reconciliation Act in 1996, temporary visa and undocumented immigrants were no longer eligible for federal assistance including food stamps and social security (Fix & Passel, 2002). Citizenship status is increasingly recognized as a form of social stratification shaping immigrants’ socioeconomic position and impacting their health (Viruell-Fuentes et al., 2012). Specifically, noncitizens are more likely to live in poverty, have limited access to employment, and are less likely to have health insurance and to be diagnosed with chronic health conditions when compared with U.S. citizens (Sanchez et al., 2017; Semega et al., 2019; Tsuchiya & Demmer, 2021). The transition into becoming a U.S. citizen is a critical shift in identity with profound implications for immigrant health across the age range, including older immigrants. Further, older noncitizens who are lonely may be unaware of or unable to leverage critical health resources and financial support to address the challenges they face. Our study thus conceptualizes citizenship status as a stressor that may interact with other stressors, and in turn, affect health. Most studies focused on citizenship status have examined these relationships among young children or adults, with this area being severely underdeveloped among older adults.
English Proficiency
Previous research has identified stressors that are unique to the immigrant integration experience, or acculturative stress, that emerge during the process of transitioning to a new culture and place of residence (Caplan, 2007). Stressors also include language and communication challenges, which in turn, have implications for mental health outcomes (Chung & Epstein, 2014; Leong et al., 2013). Language barriers, or having a limited command of English, maybe a critical and persistent stressor in combination with other stressors among older immigrants, which may impact their ability to further develop their English language skills (G. Kim et al., 2011; Koehn et al., 2022). Those with limited English proficiency (LEP) experience challenges in navigating health care access and physician visits, being able to actively participate in their community, and re-establishing their social networks (G. Kim et al., 2011; Koehn et al., 2022; Treas & Mazumdar, 2002). Furthermore, older immigrants may have limited social relationships outside their families due to LEP (Koehn et al., 2022); therefore, older immigrants who are lonely (and with limited support) may not know who to confide in or to seek support to address these issues (in tandem with navigating new contexts), which may give rise to greater distress. Older immigrants with LEP frequently have poorer health and greater levels of distress alongside receiving poorer quality of care and fewer health care visits (G. Kim et al., 2011). Hence, LEP is a critical stressor for older immigrants for their integration and social mobility in U.S. society.
Current Study
Older immigrants are more likely to experience loneliness compared with native-born older adults, which could have serious deleterious effects on their health and well-being. The association between loneliness and psychological distress may be magnified by citizenship status and English proficiency. Older adults who migrated in mid-life may experience challenges in drawing forth critical resources to navigate hardships due to difficulties in seeking support from family members (Pearlin et al., 1997) and in establishing networks that extend beyond family ties (Treas & Mazumdar, 2002). The complex interplay of loneliness, citizenship status, and English proficiency may contribute to heightened distress among older immigrants.
Prior literature has not equivocated how citizenship status or English proficiency may moderate the relationship between loneliness and psychological distress among older adults. In this study, we contend that citizenship status and English proficiency are stressors that constrain access to resources and impact the older immigrant’s integration process. These stressors may work in tandem to manifest worse health among immigrant older adults. The amalgamation of findings from previous studies provides support that the stress proliferation process is occurring among immigrants, which prompts further examination in understanding how loneliness may be amplified by the stressful transition in settling into a new country and impacting the mental health of older immigrants. We acknowledge the complex mechanisms of stress among immigrants with potentially both mediating and moderating pathways of stress on health; however, given our study is informed by the theory of stress proliferation, we will focus on the exacerbation (or moderation) of immigration-related stressors (citizenship status, English proficiency) for loneliness and psychological distress. The current study aims are described subsequently:
-
Aim 1: To determine whether loneliness, citizenship status, and English proficiency, as critical stressors, are associated with psychological distress.
Hypothesis 1: Older adults with greater levels of loneliness will report more psychological distress.
Hypothesis 2: Noncitizen older adults will exhibit greater psychological distress than native-born citizens.
Hypothesis 3: Older adults who report LEP will exhibit greater psychological distress compared to those who only speak English.
-
Aim 2: To test stress proliferation theory, we determine whether loneliness and distress is magnified by citizenship status and English proficiency.
Hypothesis 4: The relationship between loneliness and psychological distress will be stronger for noncitizens compared to native-born citizens.
Hypothesis 5: The relationship between loneliness and psychological distress will be stronger for those with LEP compared to English only speaking older adults.
Method
Sample
We utilized the 2019–2020 California Health Interview Survey (CHIS) Public Use File (PUF). CHIS is an annual, repeated cross-sectional statewide survey of California’s residential, noninstitutionalized population, and is the largest statewide health survey in the United States (California Health Interview Survey, 2021). Data are collected either online or by telephone on multiple issues, including physical and mental health, health behaviors, and health care access and utilization. CHIS began collecting data on loneliness among adults aged 65 years and older in 2019. The current study examined the older adult sample (65+ years) from 2019 to 2020 CHIS PUF. We only included older adults who identified as White, Hispanic/Latinx, and Asian. This is because there were very few noncitizens who identified as Black or other/Multiracial. With listwise deletion, the final sample consisted of 15,210 older adults.
Measures
The CHIS measured psychological distress using the Kessler-6 (K6) scale, which included a total of 6 items (α = 0.84). The K6 has been previously validated to measure and diagnose psychological distress among diverse populations, including older adults (Kessler et al., 2002; G. Kim et al., 2011). Respondents were asked about their symptoms of distress (in the past 30 days) including feeling “nervous,” “restless or fidgety,” and “worthless.” Responses ranged from none of the time = 0 to all of the time = 4. These items were summed, with higher scores indicative of greater distress. There were 10 respondents missing for this measure.
Loneliness was measured using the empirically validated UCLA 3-item loneliness scale (α = 0.82; Hughes et al., 2004). These items asked respondents how often do you feel that you either “lack companionship,” “are left out,” or “isolated from others,” with responses of (1) hardly ever, (2) some of the time, or (3) often. These items were summed, with higher scores representing greater loneliness. There were 99 respondents missing for this measure.
CHIS asks respondents if they are a citizen of the United States. Response categories included: (1) US born citizen (reference category), (2) naturalized citizen, or (3) noncitizen. Noncitizens included permanent residents, visa status holders, refugees/asylum, and undocumented residents. Previous studies have used similar measures to understand the relationship between citizenship and health (Gee et al., 2016; Tsuchiya & Demmer, 2021; Gubernskaya et al., 2013).
English proficiency is provided by the CHIS PUF and is measured by the following three categories: (1) speak English only (reference category), (2) speak English very well/well, and (3) speak English not well/not at all. Previous studies have used similar items to measure English proficiency, which has been associated with health (Gee & Ponce, 2010; G. Kim et al., 2011; Zhang et al., 2012). Two respondents had missing values for this measure.
Covariables
Sociodemographic, health, and survey year measures were included as factors associated with key variables in the study based on previous research (Gee et al., 2016; Jang & Tang, 2022; G. Kim et al., 2011). These measures were developed by CHIS investigators and included in the CHIS PUF data. Gender included two categories, (0) male as the reference category, or (1) female, respectively. Federal poverty level is a categorical measure (1) 0%–99% (reference category), (2) 100%–199%, (3) 200%–299%, and (4) 300+%. Age is categorized as (1) 65–74 (reference category), (2) 75–84, and (3) 85+. Marital status is categorized as (0) married/living with a partner (reference category) or (1) divorced/separated/widowed/never married. For educational attainment, respondents were asked about their highest grade of education completed, which included categories of (1) less than high school (reference category), (2) high school graduate, (3) some college, and (4) Bachelor’s degree or more.
CHIS collects race/ethnicity data asking respondents if they are of “Latino or Hispanic” descent. Those who self-identified as Hispanic/Latinx or Asian were asked what…“specific ethnic group are you...,” with further details of the design and methods reported on the CHIS website (healthpolicy.ucla.edu/chis). Race/ethnicity categories that were included were White, Hispanic/Latinx, African American, American Indian/Alaskan Native, Asian, and other/multiracial. For the current study, we included the following three racial/ethnic categories: “(1) non-Hispanic White (reference group),” “(2) Hispanic/Latinx,” and “(3) Asian.” We are unable to include respondents who self-identified as Black/African American (e.g., N = 2 for noncitizen Black immigrants), American Indian or Alaska Native, Native Hawaiian/Pacific Islander groups, or other/multiracial due to small sample sizes for these groups which would contribute to unreliable regression estimates. CHIS PUF does not include data by ethnicity/country of origin.
The employment status variable in the CHIS PUF included five categories: full-time employment, part-time employment, other employed, unemployed (looking for work), and unemployed (not looking for work). Respondents who were either unemployed (looking for work) or unemployed (not looking for work) were grouped together as (0) not employed (reference category). Those who were employed full-time, part-time, or other were combined into one category as (1) employed. Employment status was included as a covariate given 20% of Californians age 65 and older are still working (US Census, 2021), and because employment status has been associated with loneliness (Taylor, 2020) and well-being among immigrant older adults (B. J. Kim et al., 2017).
Health variables included self-rated health and Medicare status. Self-rated health was ascertained by asking respondents how they would rate their general health. Response categories included (4) excellent, (3) very good, (2) good, and (1) fair/poor (reference category). Fair (17.3%; N = 1,901) and poor (4.2%; N = 478) health were combined into a single category due to the smaller sample sizes for these responses. Medicare is a dichotomous variable indicating whether they had Medicare (no = 0 or referent category, yes = 1). Furthermore, self-rated health and Medicare (or insurance status) have been interlinked with critical variables of our study, specifically for psychological distress, English proficiency, citizenship, and other sociodemographic factors (Gee et al., 2016; Gubernskaya et al., 2013; G. Kim et al., 2011; Semega et al., 2019). Survey year is a binary measure, which included (0) 2019 (reference category) or (1) 2020 to account for the COVID-19 pandemic. During the pandemic, immigrants (including older immigrants) experienced greater vulnerabilities (S. Johnson et al., 2021).
Statistical Analyses
To provide sample characteristics, we compared sociodemographic and health characteristics by citizenship status and English proficiency through estimating bivariable relationships including χ2 tests with survey weights to compare differences (% weighted, unweighted n; Table 1). To investigate the two study aims, we used a series of nested multivariable linear regressions. Due to high correlations between citizenship status (Table 2) and English proficiency (Table 3) among older adults in this sample (further information provided upon request), we estimated separate multivariable models alongside loneliness on psychological distress. Model 1a examined citizenship status and loneliness together with psychological distress. Model 1b incorporated Model 1a and included sociodemographic covariables. Model 1c fully adjusted for all critical variables (sociodemographic, health) on psychological distress. Model 1d assessed the interaction effects of citizenship status and loneliness on distress. The same modeling methods were also conducted for English language proficiency (see Table 3, Models 2a–2d). All regression models were adjusted for survey year.
Table 1.
Characteristics of Older Adults by Citizenship Status and English Proficiency, 2019–2020 California Health Interview Survey
| Variables | Citizenship status | English proficiency | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Full sample (N = 15,309) | US born citizen (n = 12,861) | Naturalized citizen (n = 2,200) | Noncitizen (n = 248) | p-value | English only (n = 12,825) | Very well/well (n = 1,972) | Not well/not at all (n = 510) | p-value | |
| M (SD) or % (N) | |||||||||
| Psychological distress (0–24) | 2.71 (4.64) | 2.57 (4.65) | 3.05 (4.23) | 3.03 (2.78) | ** | 2.55 (4.74) | 2.57 (3.53) | 4.01 (3.61) | *** |
| Loneliness (3–9) | 3.87 (1.86) | 3.88 (2.00) | 3.88 (1.50) | 3.68 (0.86) | n.s. | 3.88 (2.04) | 3.81 (1.43) | 3.93 (1.12) | n.s. |
| Citizenship status | *** | ||||||||
| US born citizen (ref.) | 71.11% (12,861) | –– | –– | –– | 91.73% (12,043) | 34.14% (796) |
2.35% (21) |
||
| Naturalized citizen | 24.58% (2,200) | –– | –– | –– | 7.17% (695) |
60.55% (1,098) |
73.81% (406) |
||
| Noncitizen | 4.32% (248) |
–– | –– | –– | 1.10% (87) |
5.31% (78) |
23.84% (83) |
||
| English proficiency | *** | ||||||||
| English only (ref.) | 70.03% (12,825) | 90.34% (12,043) | 20.44% (695) | 17.76% (87) |
–– | –– | –– | ||
| Very well/well | 19.39% (1,972) | 9.31% (796) |
47.77% (1,098) | 23.82% (78) |
–– | –– | –– | ||
| Not well/not at all | 10.59% (510) | 0.35% (21) |
31.80% (406) | 58.43% (83) |
–– | –– | –– | ||
| Gender | n.s. | ** | |||||||
| Male (ref.) | 45.62% (7,318) | 44.69% (6,058) | 47.93% (1,135) | 47.81% (125) | 45.07% (6,040) | 50.42% (1,047) |
40.40% (229) |
||
| Female | 54.38% (7,991) | 55.31% (6,803) | 52.07% (1,065) | 52.19% (123) | 54.93% (6,785) | 49.58% (925) |
59.60% (281) |
||
| Race | *** | *** | |||||||
| Non-Hispanic White (ref.) | 64.70% (12,499) | 82.30% (11,628) | 21.50% (766) | 20.64% (105) | 86.00% (11,768) | 20.75% (698) |
4.33% (33) |
||
| Hispanic/Latinx | 23.35% (1,495) | 15.04% (890) |
40.90% (522) | 60.27% (83) |
10.15% (605) |
50.22% (644) |
61.50% (226) |
||
| Asian | 11.95% (1,315) | 2.65% (343) |
37.60% (912) | 19.09% (60) |
3.85% (452) |
29.03% (610) |
34.17% (251) |
||
| Poverty level | *** | *** | |||||||
| 0%–99% (ref.) | 10.84% (938) | 6.80% (627) |
17.27% (258) | 40.60% (53) |
6.03% (610) |
12.56% (169) |
39.50% (159) |
||
| 100%–199% | 16.72% (1,887) | 12.87% (1,407) | 26.88% (426) | 22.36% (54) |
12.72% (1,383) | 20.71% (320) |
35.89% (184) |
||
| 200%–299% | 13.88% (2,069) | 14.78% (1,777) | 12.37% (263) | 7.79% (30) |
14.64% (1,758) | 14.12% (257) |
8.40% (53) |
||
| 300%+ FPL | 58.56% (10,415) | 65.55% (9,050) | 43.48% (1,254) | 29.25% (111) | 66.61% (9,074) | 52.61% (1,226) |
16.22% (114) |
||
| Age | n.s. | * | |||||||
| 65–74 (ref.) | 56.85% (9,313) | 55.63% (7,800) | 60.48% (1,350) | 56.28% (163) | 55.32% (7,745) | 62.58% (1,260) |
56.48% (307) |
||
| 75–84 | 31.90% (4,606) | 32.55% (3,881) | 29.71% (659) | 33.74% (66) |
32.83% (3,894) | 29.18% (558) |
30.78% (154) |
||
| 85+ | 11.25% (1,390) | 11.82% (1,180) | 9.80% (191) |
9.99% (19) |
11.85% (1,186) | 8.24% (154) |
12.74% (49) |
||
| Marital status | ** | ** | |||||||
| Married/partnered (ref.) | 61.35% (8,482) | 59.19% (6,945) | 67.19% (1,391) | 63.51% (146) | 59.55% (6,939) | 66.79% (1,231) |
63.27% (311) |
||
| Widowed/divorced/separated/unmarried | 38.65% (6,827) | 40.81% (5,916) | 32.81% (809) | 36.49% (102) | 40.45% (5,886) | 33.21% (741) |
36.73% (199) |
||
| Educational attainment | *** | *** | |||||||
| Less than high school (ref.) | 18.36% (556) | 8.12% (233) |
38.99% (253) | 69.53% (70) |
8.05% (225) |
24.93% (116) |
74.54% (215) |
||
| High school graduate | 23.53% (2,005) | 27.04% (1,726) | 15.95% (255) | 8.82% (24) |
26.63% (1,691) | 17.60% (217) |
13.87% (97) |
||
| Some college | 21.06% (4,670) | 24.17% (4,055) | 14.57% (565) | 6.82% (50) |
23.92% (4,041) | 19.36% (547) |
5.22% (80) |
||
| Bachelor’s degree or higher | 37.05% (8,078) | 40.67% (6,847) | 30.49% (1,127) | 14.82% (104) | 41.40% (6,868) | 38.12% (1,092) |
6.37% (118) |
||
| Employment status | n.s. | *** | |||||||
| No (ref.) | 79.53% (11,980) | 79.68% (10,095) | 79.34% (1,699) | 78.20% (186) | 79.46% (10,090) | 76.20% (1,463) |
86.15% (426) |
||
| Yes | 20.47% (3,329) | 20.32% (2,766) | 20.66% (501) | 21.80% (62) |
20.54% (2,735) | 23.80% (509) |
13.85% (84) |
||
| Self-rated health | *** | *** | |||||||
| Fair/poor (ref.) | 21.45% (2,379) | 17.61% (1,811) | 28.67% (493) |
43.47% (75) |
16.46% (1,784) | 22.56% (345) |
52.40% (250) |
||
| Good | 33.63% (4,751) | 32.49% (3,890) | 36.36% (779) | 36.91% (82) |
32.61% (3,874) | 37.10% (693) |
33.99% (183) |
||
| Very good | 32.69% (5,824) | 35.75% (5,073) | 27.15% (684) | 13.91% (67) |
36.48% (5,086) | 30.14% (671) |
12.29% (66) |
||
| Excellent | 12.23% (2,355) | 14.15% (2,087) | 7.83% (244) |
5.71% (24) |
14.45% (2,081) | 10.20% (263) |
1.31% (11) |
||
| Medicare coverage | *** | *** | |||||||
| No (ref.) | 6.86% (776) |
4.97% (600) |
8.92% (136) |
26.19% (40) |
5.00% (595) |
10.01% (137) |
13.42% (44) |
||
| Yes | 93.14% (14,533) | 95.03% (12,261) | 91.08% (2,064) | 73.81% (208) | 95.00% (12,230) | 89.99% (1,835) |
86.58% (466) |
||
| Year | n.s. | n.s. | |||||||
| 2019 (ref.) | 49.24% (8,040) | 50.07% (6,784) | 46.50% (1,140) | 51.29% (116) | 50.62% (6,790) | 46.26% (1,008) |
45.55% (240) |
||
| 2020 | 50.76% (7,269) | 49.93% (6,077) | 53.50% (1,060) | 48.71% (132) | 49.38% (6,035) | 53.74% (964) |
54.45% (270) |
||
Notes: Survey weights were applied to all percentages, means, and standard deviations (SD). The frequencies are unweighted. Percentages and n are presented for categorical variables, and n, means, and standard deviations are presented for continuous variables.
*Indicates statistical significance at the .05 level.
**Indicates statistical significance at the .01 level.
***Indicates statistical significance at the .001 level. Not significant p values are denoted with n.s.
Table 2.
Multivariable Regression Models Examining Loneliness, Citizenship Status, and Psychological Distress among Older Adults, 2019–2020 California Health Interview Survey (N = 15,210)
| Variables | Model 1a | Model 1b | Model 1c | Model 1d |
|---|---|---|---|---|
| b 95% CI |
b 95% CI |
b 95% CI |
b 95% CI |
|
| Loneliness | 1.33*** [1.24, 1.43] |
1.32*** [1.23, 1.42] |
1.23*** [1.13, 1.32] |
1.08*** [0.98, 1.18] |
| Citizenship status | ||||
| US born citizen (ref.) | — | — | — | — |
| Naturalized citizen | 0.48*** [0.23, 0.74] |
0.11 [−0.25, 0.48] |
0.11 [−0.24, 0.45] |
−1.75*** [−2.62, −0.88] |
| Noncitizen | 0.60* [0.00, 1.20] |
0.06 [−0.54, 0.66] |
−0.18 [−0.79, 0.42] |
−2.17 [−4.68, 0.34] |
| Loneliness × citizenship status | ||||
| Loneliness × native-born citizen (ref.) | — | — | — | — |
| Loneliness naturalized citizen | — | — | — | 0.48*** [0.26, 0.70] |
| Loneliness × noncitizen | — | — | — | 0.53 [−0.17. 1.24] |
| Gender | ||||
| Male (ref.) | — | — | — | — |
| Female | — | 0.40*** [0.21, 0.59] |
0.45*** [0.26, 0.64] |
0.44*** [0.25, 0.63] |
| Race | ||||
| Non-Hispanic White (ref.) | — | — | — | — |
| Hispanic/Latinx | — | −0.07 [−0.43, 0.28] |
−0.24 [−0.57, 0.09] |
−0.22 [−0.57, 0.12] |
| Asian | — | 0.23 [−0.18, 0.65] |
0.01 [−0.38, 0.40] |
0.01 [−0.39, 0.41] |
| Poverty level | ||||
| 0%–99% (ref.) | — | — | — | — |
| 100%–199% | — | 0.00 [−0.49, 0.50] |
0.04 [−0.46, 0.54] |
0.03 [−0.47, 0.53] |
| 200%–299% | — | −0.56** [−0.96, −0.16] |
−0.39 [−0.79, 0.01] |
−0.35 [−0.76, 0.05] |
| 300%+ FPL | — | −0.72*** [−1.10, −0.35] |
−0.48* [−0.86, −0.09] |
−0.47* [−0.85, −0.08] |
| Age | ||||
| 65–74 (ref.) | — | — | — | — |
| 75–84 | — | −0.10 [−0.29, 0.09] |
−0.13 [−0.32, 0.06] |
−0.15 [−0.34, 0.03] |
| 85+ | — | −0.10 [−0.43, 0.23] |
−0.29 [−0.61, 0.04] |
−0.31 [−0.63, 0.00] |
| Marital status | ||||
| Married or partnered (ref.) | — | — | — | — |
| Widowed/divorced/separated/unmarried | — | −0.42*** [−0.61, −0.23] |
−0.42*** [−0.61, −0.23] |
−0.41*** [−0.60, −0.22] |
| Educational attainment | ||||
| Less than high school (ref.) | — | — | — | — |
| High school graduate | — | −0.22 [−0.64, 0.20] |
−0.05 [−0.45, 0.35] |
−0.04 [−0.44, 0.36] |
| Some college | — | −0.35 [−0.74, 0.04] |
−0.08 [−0.44, 0.28] |
−0.05 [−0.42, 0.31] |
| Bachelor’s degree or higher | — | −0.49* [−0.87, −0.11] |
−0.14 [−0.48, 0.20] |
−0.11 [−0.46, 0.24] |
| Employment status | ||||
| No (ref.) | — | — | — | — |
| Yes | — | 0.15 [−0.05, 0.35] |
0.33** [0.12, 0.53] |
0.30** [0.10, 0.50] |
| Self-rated health | ||||
| Fair/poor (ref.) | — | — | — | — |
| Good | — | — | −1.51*** [−1.82, −1.19] |
−1.51*** [−1.82. −1.19] |
| Very good | — | — | −1.93*** [−2.26, −1.60] |
−1.95*** [−2.28, −1.62] |
| Excellent | — | — | −2.19*** [−2.53, −1.84] |
−2.23*** [−2.57, −1.88] |
| Medicare coverage | ||||
| No (ref.) | — | — | — | — |
| Yes | — | — | −0.36* [−0.71, 0.00] |
−0.34* [−0.68, 0.00] |
| Year | ||||
| 2019 (ref.) | — | — | — | — |
| 2020 | 0.01 [−0.17. 0.19] |
0.00 [−0.18. 0.18] |
−0.02 [−0.19, 0.14] |
0.01 [−0.15, 0.17] |
| Constant | −2.59*** [−2.93, −2.26] |
−1.70*** [−2.19, −1.20] |
0.07 [−0.61, 0.75] |
0.60 [−0.04, 1.25] |
| R 2 | 0.29 | 0.30 | 0.35 | 0.35 |
Notes: For all models, regression coefficients and standard errors (SE) are presented, with SEs being in parentheses. Model 1a examines the association among key variables only, including citizenship status and loneliness. Model 1b examines key variables and sociodemographic factors only. Model 1c examines the key variables, sociodemographic and health factors on psychological distress. Model 1d contains all the previous variables and the moderation effect of loneliness by citizenship status. Model 1a: F(4,156) = 195.92***, R2 = 0.29. Model 1b: F(17,143) = 52.90***, R2 = 0.30. Model 1c: F(21, 139) = 59.73***, R2 = 0.35. Model 1d: F(23,137) = 56.60***, R2 = 0.35. FPL = federal poverty level.
*Indicates statistical significance at the .05 level.
**Indicates statistical significance at the .01 level.
***Indicates statistical significance at the.001 level.
Table 3.
Multivariable Regression Models Examining Loneliness, English Proficiency and Psychological Distress Among Older Adults, 2019–2020 California Health Interview Survey (N = 15,210)
| Variables | Model 2a | Model 2b | Model 2c | Model 2d |
|---|---|---|---|---|
| b 95% CI |
b 95% CI |
b 95% CI |
b 95% CI |
|
| Loneliness | 1.33*** [1.23, 1.42] |
1.32*** [1.23, 1.42] |
1.23*** [1.14, 1.33] |
1.10*** [1.00, 1.21] |
| English proficiency | ||||
| English only (ref.) | — | — | — | — |
| Very well/well | 0.12 [−0.11, 0.34] |
0.05 [−0.28, 0.38] |
−0.01 [−0.33, 0.31] |
−0.52 [−1.30, 0.27] |
| Not well/not at all | 1.35*** [0.87, 1.83] |
0.97** [0.29, 1.64] |
0.57 [−0.08, 1.22] |
−2.81*** [−4.31, −1.30] |
| Loneliness × English proficiency | ||||
| Loneliness × English only (ref.) | — | — | — | – |
| Loneliness × very well/well | — | — | — | 0.13 [−0.08, 0.34] |
| Loneliness × not well/not at all | — | — | — | 0.85*** [0.50, 1.20] |
| Gender | ||||
| Male (ref.) | — | — | — | — |
| Female | — | 0.39*** [0.20, 0.57] |
0.44*** [0.25, 0.63] |
0.43*** [0.23, 0.62] |
| Race | ||||
| Non-Hispanic White (ref.) | — | — | — | — |
| Hispanic/Latinx | — | −0.17 [−0.58, 0.24] |
−0.28 [−0.66, 0.11] |
−0.25 [−0.66, 0.15] |
| Asian | — | 0.07 [−0.34, 0.48] |
−0.05 [−0.44, 0.34] |
−0.12 [−0.53, 0.28] |
| Poverty level | ||||
| 0%–99% (ref.) | — | — | — | — |
| 100%–199% | — | 0.10 [−0.42, 0.62] |
0.12 [−0.40, 0.64] |
0.07 [−0.45, 0.59] |
| 200%–299% | — | −0.40 [−0.82, 0.03] |
−0.28 [−0.70, 0.15] |
−0.32 [−0.74, 0.11] |
| 300%+ FPL | — | −0.55** [−0.95, −0.15] |
−0.36 [−0.76, 0.04] |
−0.42* [−0.83, −0.02] |
| Age | ||||
| 65–74 (ref.) | — | — | — | — |
| 75–84 | — | −0.10 [−0.29, 0.09] |
−0.13 [−0.32, 0.06] |
−0.16 [−0.35, 0.03] |
| 85+ | — | −0.11 [−0.44, 0.22] |
−0.29 [−0.61, 0.04] |
−0.28 [−0.61, 0.04] |
| Marital status | ||||
| Married or partnered (ref.) | — | — | — | — |
| Widowed/divorced/separated/unmarried | — | −0.39*** [−0.57, −0.20] |
−0.40*** [−0.59, −0.22] |
−0.39*** [−0.58, −0.20] |
| Educational attainment | ||||
| Less than high school (ref.) | — | — | — | — |
| High school graduate | — | 0.00 [−0.39, 0.40] |
0.09 [−0.29, 0.48] |
0.04 [−0.34, 0.43] |
| Some college | — | −0.11 [−0.47, 0.26] |
0.07 [−0.28, 0.42] |
0.05 [−0.30, 0.41] |
| Bachelor’s degree or higher | — | −0.25 [−0.60, 0.10] |
0.01 [−0.32, 0.34] |
−0.01 [−0.35, 0.33] |
| Employment status | ||||
| No (ref.) | — | — | — | — |
| Yes | — | 0.15 [−0.05, 0.35] |
0.32** [0.12, 0.53] |
0.31** [0.11, 0.52] |
| Self-rated health | ||||
| Fair/poor (ref.) | — | — | — | — |
| Good | — | — | -1.46*** [−1.77, −1.15] |
−1.46*** [−1.77, −1.14] |
| Very good | — | — | −1.87*** [−2.19, −1.55] |
−1.90*** [−2.22, −1.57] |
| Excellent | — | — | −2.13*** [−2.47, −1.79] |
−2.19*** [−2.53, −1.85] |
| Medicare coverage | ||||
| No (ref.) | — | — | — | — |
| Yes | — | — | −0.30 [−0.66, 0.05] |
−0.32 [−0.67, 0.02] |
| Year | ||||
| 2019 (ref.) | – | – | – | – |
| 2020 | 0.00 [−0.18, 0.18] |
−0.01 [−0.18, 0.17] |
−0.02 [−0.19, 0.14] |
0.05 [−0.11, 0.21] |
| Constant | −2.59*** [−2.92, −2.25] |
−2.07*** [−2.58, −1.55] |
−0.28 [−0.99, 0.42] |
0.32 [–0.36, 1.00] |
| R 2 | 0.30 | 0.31 | 0.35 | 0.36 |
Notes: For all models, regression coefficients and standard errors (SE) are presented, with SEs in parentheses. Model 2a examines the association among key variables only, including English proficiency and loneliness. Model 2b examines key variables and sociodemographic factors only. Model 2c examines the key variables, sociodemographic and health factors on psychological distress. Model 2d contains all the previous variables and the moderation effect of loneliness by English proficiency. Model 2a: F(4,156) = 210.21***, R2 = 0.30. Model 2b: F(17, 143) = 56.06***, R2 = 0.31. Model 2c: F(21, 139) = 61.18***, R2 = 0.35. Model 2d: F(23, 137) = 56.81***, R2 = 0.36. FPL = federal poverty level.
*Indicates statistical significance at the .05 level.
**Indicates statistical significance at the .01 level.
***Indicates statistical significance at the .001 level.
We conducted supplemental analyses to examine if the effects of loneliness, citizenship status, and English proficiency on psychological distress differed by race/ethnicity. Previous research has demonstrated disparities in loneliness and psychological distress by race/ethnicity (Taylor & Nguyen, 2020; Watkins & Johnson, 2018), which may reflect variations due to cultural factors among immigrant populations (Hossen, 2012; Treas & Mazumdar, 2002). We examined race/ethnicity stratified multivariable linear regression models for White, Hispanic/Latinx, and Asian older adults (see Supplemental Tables A and B). However, due to limited samples of noncitizens, these results may be hampered by precision and unstable standard error estimates, and hence, we invite future exploration in this area.
We applied complex survey weights for all analyses to account for sampling probabilities to obtain estimates representative of the older population in California using Stata version 17.0 (StataCorp, College Station, TX). CHIS has low missing data as the data are imputed for almost every variable. Further information regarding imputation can be found elsewhere (see CHIS Methodology Report). In the current analysis, 99 respondents had missing data across all study variables. Due to the minimal missing data (<1%), we excluded respondents with missing observations, with a final analytic sample of 15,210 older adults.
Results
Descriptive Statistics
In 2019–2020 (Table 1), the mean psychological distress score was 2.71 (SD = 4.64). Most were either US born citizens (71.1%) or naturalized citizens (24.6%) and spoke English only (70.0%) or very well/well (19.4%). On average, respondents reported loneliness scores of 3.87 (SD = 1.86). Most were female (54.4%), self-identified as non-Hispanic White (64.7%) or Hispanic/Latinx (23.4%), lived 300% above the federal poverty level (58.6%; FPL), were 65–74 years old (56.9%), and were married or partnered (61.4%). More than half had either some college (21.1%) or a bachelor’s degree or more (37.1%) and were not employed (79.5%). The majority reported either very good (32.7%) or good (33.6%) health and had Medicare (93.1%). Overall, there was an even split across the survey cycles.
Regarding differences in citizenship status, naturalized citizens (M = 3.05, SD = 4.23) and noncitizens (M = 3.03, SD = 2.78) exhibited higher levels of distress than US born citizens. Noncitizens were more likely to report LEP (speak English not well/not at all). Both noncitizens and those with LEP were more likely to self-identify as Hispanic/Latinx or Asian, live in poverty (0%–99% FPL), have less than a high school education, report fair/poor health, and were less likely to have Medicare than US born citizens or those who speak English only.
Multivariable Models
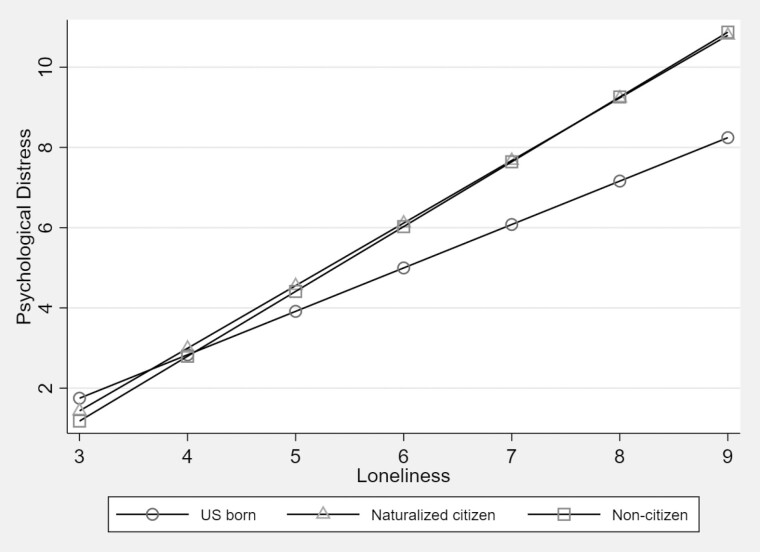
Table 2 displays the results of the multivariable models between citizenship and loneliness on distress. In the unadjusted model (Model 1a), greater loneliness (b = 1.33, p < .001) is associated with higher psychological distress. Both naturalized (b = 0.48, p < .001) and noncitizens (b = 0.60, p < .05) exhibit greater distress than US born citizens. However, in Model 1b, after adjustment of sociodemographic factors, loneliness remained significant on distress (b = 1.23, p < .001), although citizenship status was no longer significant. After the inclusion of self-rated health and Medicare coverage (Model 1c), loneliness remained significant although citizenship remained nonsignificant. Model 1d shows a significant interaction between citizenship and loneliness in that the effect of loneliness on distress was greater for naturalized citizens than US born citizens (Figure 1).
Figure 1.
Citizenship status as a moderator in the relationship between loneliness and psychological distress among older Californians, 2019–2020 California Health Interview Survey (N = 15,210)
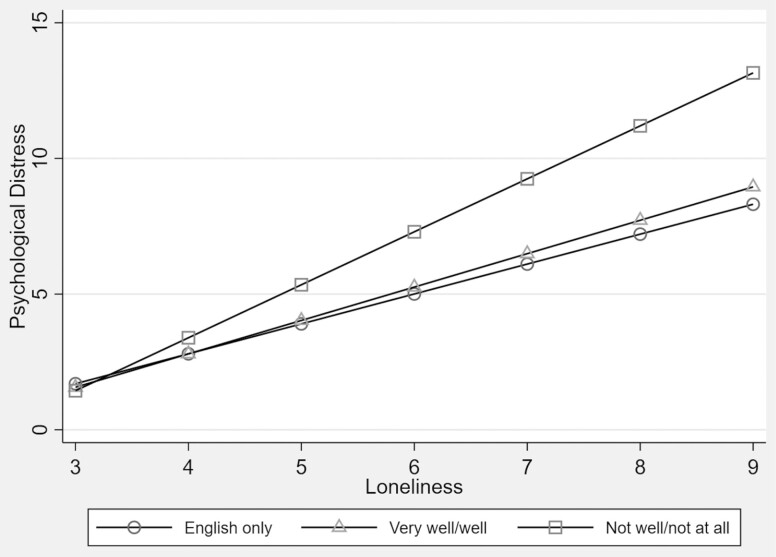
Table 3 displays the multivariable results for English proficiency, loneliness, and distress. Model 2a shows the unadjusted analyses, loneliness was associated with higher distress (b = 1.33, p < .001). Those with LEP have higher levels of distress (b = 1.35, p < .001) than those who speak English only. These associations remained significant after adjusting for sociodemographic factors (Model 2b). After the inclusion of self-rated health and Medicare, loneliness remained significant (b = 1.23, p < .001) although English proficiency was no longer associated with distress. The interaction between loneliness and English proficiency was significant (Model 2d) in that the effect of loneliness was stronger for those with LEP than those who speak English only (Figure 2).
Figure 2.
English proficiency as a moderator in the relationship between loneliness and psychological distress among older Californians, 2019–2020 California Health Interview Survey (N = 15,210)
Sensitivity Analyses
Additional analyses were conducted to assess whether the relationship between loneliness, citizenship, and English proficiency differed by race/ethnicity for psychological distress. Greater loneliness was significantly associated with distress across all groups, non-Hispanic White, Hispanic/Latinx, and Asian older adults, after adjusting for either citizenship status (Supplementary Table A) or English proficiency (Supplementary Table B). Citizenship status (Supplementary Table A) was only significant for distress among White older adults, where noncitizen White older adults had lower levels of distress than US born Whites. English proficiency (Supplementary Table A) was not significant in any of the models by race/ethnicity.
Discussion
The current study provides evidence of multiple stressors experienced by marginalized older immigrants. For the first study aim, we examined whether each of the stressors—loneliness, citizenship status, and English proficiency—were significantly associated with distress. Findings from the multivariate analysis support our first hypothesis, in that loneliness was associated with distress. Our second and third hypotheses were not supported, given the relationships between citizenship status and English proficiency on distress were attenuated in subsequent models. The loneliness-distress relationship was robust and significant even after adjusting for sociodemographic and health factors. Sensitivity analyses also revealed loneliness was significantly associated with distress across all racial older adults.
Across all three stressors, the robust findings for the loneliness–distress relationship (given loneliness was most consistently associated with distress) may be explained by the fact that loneliness may stem from many different causes and can consistently and negatively affect multiple life domains (Hawkley et al., 2008). Additionally, older immigrants often arrive to the United States for family reunification purposes; however, this does not necessarily lead to greater social support. Instead, Treas and Mazumdar (2002) found reunification led to greater feelings of loneliness. The integration experience for immigrant families may lead to changes and shifts in interpersonal dynamics that may not necessarily be reflective of the cultural practices of their country of origin (Hossen, 2012). Thus, this may translate to differences in values and lifestyles between parents and their children leading to conflicts and strained relationships among families, contributing to greater loneliness. These strained relationships are reflected in older adults’ subjective reflection of the quality of relationships with family and friends, and hence, directly linked with their mental health, which is consistent with the findings of our study. Typically, support networks may provide access to financial resources and health care, however, for older immigrants this may not be the case due to having a smaller network size, which may also explain the robust relationship between loneliness and distress in our study.
Conversely, we did not observe any significant relationships for both citizenship status and English proficiency on distress after adjusting for sociodemographic and health factors, as these stressors may affect access to resources or social determinants. Citizenship status is reflective of immigration policies which contribute to social exclusion based on their legal status through various eligibility criteria to access federal benefits, health insurance, employment opportunities (Fix & Passel, 2002), and ultimately, contributing to precarity. Citizenship was initially significant for distress; however, after controlling for sociodemographic factors, this relationship was attenuated. Due to legal and residency restrictions, noncitizens may not have equitable access to resources and opportunities that are beneficial to their health and hence, experience constraints in income, job opportunities, or access to health insurance/Medicare (Sanchez et al., 2017; Semega et al., 2019). Indeed, in our sample we find that older noncitizens were more likely to have lower education and to live in poverty and were less likely to have Medicare insurance. Citizenship may be a critical determinant of health through access to social resources (Viruell-Fuentes et al., 2012). Researchers have elucidated that stress may result from hierarchical effects of social stratification (Pearlin et al., 2005). These results provide support for how citizenship streams access to resources through social stratification, where those without citizenship experience multiple constraints. In other words, citizenship and health may be mediated by social determinant factors. However, more research is needed to further assess these pathways among older immigrants and by documentation status.
Along the same lines, in initial models, respondents who reported LEP had higher levels of distress than those who only speak English. However, English proficiency was no longer associated with distress after adjusting for health covariables. English proficiency has implications for communication and in turn, contributes to challenges and difficulties in navigating systems and resources (e.g., health care). Hence, LEP exerts influence through relational and transactional mechanisms, including access to health care and establishing social relationships in their communities, which directly translates into greater distress (G. Kim et al., 2011; Koehn et al., 2022; Treas & Mazumdar, 2002). Older immigrants in our sample who reported LEP are more likely to have higher levels of distress and are less likely to have Medicare. The process of obtaining Medicare may be even more challenging for those with LEP due to navigating the complex enrollment and eligibility processes as they may require further assistance (Centers for Medicare & Medicaid Services, 2017). These stressors may affect one’s life in specific situations and/or time points, with the magnitude of the proliferation of these stressors to be influenced by access to resources or in this case, citizenship status and English proficiency.
Hurh and Kim (1990) found immigrants may experience two points of vulnerability, the initial stage occurring upon arrival as they experience challenges in integration (e.g., language and communication challenges, constrained job opportunities) and the later stage when they have experienced social exclusion further impacting their process of integration. For older adults, these two stages of vulnerability may be occurring and overlapping at the same time, and hence, affecting them on a situational basis (e.g., when accessing health care or other critical resources). Taken together, loneliness, citizenship status, and English proficiency each are stressors that affect distress, with loneliness exerting stronger effects on distress.
Stress Proliferation
For our second study aim, we tested the theory of stress proliferation by examining whether stressors linked to the immigrant integration process, either citizenship status or English proficiency, contribute to enhanced effects for loneliness and distress. We hypothesized the relationship between loneliness and psychological distress would be stronger for noncitizens in comparison to US born citizens; however, we found that this relationship was stronger for naturalized citizens, and hence, did not support our initial hypothesis for noncitizens (hypothesis 4). We also found the relationship between loneliness and distress was stronger for those with LEP compared with those who only speak English, which supported our fifth hypothesis. Overall, these results show that one stressor combined with another stressor has amplified and deleterious effects on health, supporting the stress proliferation theory.
Interestingly, the relationship between loneliness and distress was amplified among naturalized citizens and not for noncitizens, which we did not anticipate; however, this may be explained due to the fact that the timing of critical transitions may constrain opportunities and impact other stressors (Pearlin et al., 2005). Naturalized citizens may have access to greater benefits compared with noncitizens; however, this shift in identity may not immediately translate to better circumstances for newly naturalized older citizens. If they are experiencing challenges in learning and navigating new systems without adequate support, despite changes to their citizenship status, they are nevertheless stuck in limbo (Koehn et al., 2022). Further, the specific timing of when they migrated and obtained citizenship may have considerable implications for health. Indeed, Gubernskaya et al. (2013) found differences in health by citizenship status among older immigrants based on age of migration. Specifically, naturalized citizens who migrated in the United States during their childhood or youth had fewer functional limitations compared with noncitizens, although those who had arrived during adulthood (middle age or older) reported greater functional limitations compared with noncitizens. Others have also found that older immigrants who arrived in the United States in midlife or older exhibited worse health (Jang & Tang, 2022; Wu & Penning, 2015). However, due to data constraints and limited samples of older noncitizens in CHIS, we were unable to explore these relationships in greater detail, which may have also contributed to nonsignificant findings for noncitizen older adults. We invite further exploration in this area.
Immigrants who are experiencing greater loneliness also report LEP had greater levels of distress. The creation of strong relationships outside of the family unit for older immigrants may already be challenging, in tandem as they navigate language/communication barriers, which can further amplify their stress levels and contribute to distress. These findings align with previous research in that prior stress exposures may induce other stressors during the integration process (Li, 2016; Tsuchiya et al., 2021). For older immigrants, the process of integration may be much slower and more challenging due to the aging process and navigating new systems with fewer resources and constrained English abilities, enhancing the effect of stressors on health. In sum, our findings demonstrate that the combination of the aforementioned stressors leads to greater levels of distress among immigrant older adults.
Limitations
Several limitations should be noted for our study. This study used a cross-sectional design to assess relationships and thus, causation cannot be inferred. Psychological distress may be a critical driver for loneliness; nonetheless, due to the study limitations we were not able to test the temporality of this relationship. Empirical research demonstrates that loneliness is a stressor and contributes to distress among immigrant older adults and older adults generally (Jang & Tang, 2022; Taylor et al., 2018). Prior research has shown that loneliness and mental health were amplified among those with more negative family strain (Jang & Tang, 2022); however, we were unable to assess the role of social support and quality of family relationships in this study. Further investigation is needed to examine these relationships alongside measures of support and family relations to determine protective factors for these stressors among immigrant older adults. Due to sensitivity of information and respondent confidentiality, CHIS does not collect data on when a noncitizen immigrant became a naturalized citizen and the CHIS PUF does not provide data for when immigrants arrived in the United States or by country of origin and documentation status. It would be beneficial for future research to disentangle the timing of when the immigrant came to the United States and by country of origin, as well as legal status transitions alongside other stressors in elucidating the changes in health particularly for immigrant older adults. We also recognize the importance of understanding differences in loneliness and distress to be driven by the interplay between race/ethnicity, citizenship status, and English proficiency for loneliness and distress. However, with limited sample sizes for noncitizen immigrants and by race/ethnicity for older immigrants, we invite future studies to explore these intersectional identities as well as consider using advanced methods (e.g., propensity score, longitudinal) to empirically test disparities and changes to health among immigrants over time. There may also be potential mediating mechanisms of social determinant factors for citizenship status, English proficiency, and distress. The primary focus of our study was to examine how these stressors may proliferate (or moderate) as they reflect access to resources. We invite future research to examine these pathways among immigrant older adults. Our data were based on a population sample of older adults in California. The impact of these stressors on distress may vary by locale within and outside of California. Yet, a notable strength of our study is the recency of our data. Our findings are timely and of important relevance in understanding critical stressors among immigrant older adults.
Conclusion
As one of the first studies to examine citizenship status, English proficiency, and loneliness on psychological distress, the current study contributes to the literature in understanding the stress process and how stressors may proliferate across other stressors to shape the health of immigrant older adults. With increasing projections of immigrant older adults by 2060 (Camarota & Zeigler, 2019), it is vital to understand what contributes to greater vulnerability and adverse health for immigrant older adults. Practitioners could consider ways to address loneliness among older adults through tailored programming and the development of supportive relationships outside their family to ameliorate the burden of stressors they are experiencing. These results point us toward future research in understanding critical stressors and needs of immigrant older adults and their health.
Supplementary Material
Contributor Information
Kazumi Tsuchiya, Dalla Lana School of Public Health, University of Toronto, Toronto, Ontario, Canada.
Harry Owen Taylor, Factor-Inwentash Faculty of Social Work, University of Toronto, Toronto, Ontario, Canada.
Adrian Matias Bacong, Center for Asian Health Research and Education, Stanford University, Stanford, California, USA.
Michael David Niño, Department of Sociology and Criminology, University of Arkansas, Fayetteville, Arizona, USA.
Funding
For the preparation of this article, H.O.T. was supported by funding from the National Institute on Aging (1 P30 AG 059298).
Conflict of Interest
None declared.
Author Contributions
K. Tsuchiya planned and conceptualized the study, supervised the data analysis, and wrote the paper. H. O. Taylor assisted in the conceptualization of the study, performed all statistical analyses, wrote sections of the paper, and contributed to the revising and editing of the paper. A. M. Bacong contributed to the editing of the paper. M. D. Niño assisted in the conceptualization, writing, editing, and revising of the paper.
References
- Ali, S. H., Islam, T., Pillai, S., Kalasapudi, L., Mammen, S., Inala, S., Kalasapudi, V., Islam, N. S., & Gunness, H. (2021). Loneliness and mental health outcomes among South Asian older adult immigrants in the United States: A cross-sectional study. International Journal of Geriatric Psychiatry, 36(9), 1423–1435. doi: 10.1002/gps.5549 [DOI] [PubMed] [Google Scholar]
- Bloemraad, I., Korteweg, A., & Yurdakul, G. (2008). Citizenship and immigration: Multiculturalism, assimilation, and challenges to the Nation-State. Annual Review of Sociology, 34(1), 153–179. doi: 10.1146/annurev.soc.34.040507.134608 [DOI] [Google Scholar]
- California Health Interview Survey. (2021). CHIS 2019–2020 methodology report series: Report 1—Sample design. UCLA Center for Health Policy Research. [Google Scholar]
- Camarota, S. A., & Zeigler, K. (2019). Projecting the impact of immigration on the U.S. population. Center for Immigration Studies Backgrounder. Accessed January 3, 2023. https://cis.org/Report/Projecting-Impact-Immigration-US-Population [Google Scholar]
- Caplan, S. (2007). Latinos, acculturation, and acculturative stress: A dimensional concept analysis. Policy, Politics, & Nursing Practice, 8(2), 93–106. doi: 10.1177/1527154407301751 [DOI] [PubMed] [Google Scholar]
- Carr, S., & Tienda, M. (2013). Family sponsorship and late-age immigration in aging America: Revised and expanded estimates of chained migration. Population Research and Policy Review, 32(6), 825–849. doi: 10.1007/s11113-013-9300-y [DOI] [PMC free article] [PubMed] [Google Scholar]
- Centers for Medicare & Medicaid Services. (2017, April). Understanding communication and language needs of Medicare beneficiaries. Accessed March 27, 2023. https://www.cms.gov/About-CMS/Agency-Information/OMH/Downloads/Issue-Briefs-Understanding-Communication-and-Language-Needs-of-Medicare-Beneficiaries.pdf
- Chung, H., & Epstein, N. B. (2014). Perceived racial discrimination, acculturative stress, and psychological distress among Asian immigrants: The moderating effects of support and interpersonal strain from a partner. International Journal of Intercultural Relations, 42, 129–139. doi: 10.1016/j.ijintrel.2014.04.003 [DOI] [Google Scholar]
- Fix, M., & Passel, J. (2002). The Scope and Impact of Welfare Reform’s Immigrant Provisions. Discussion Papers. Assessing the New Federalism: An Urban Institute Program To Assess Changing Social Policies. Accessed March 20, 2023. https://eric.ed.gov/?id=ED462496.
- Fokkema, T., & Ciobanu, R. O. (2021). Older migrants and loneliness: Scanning the field and looking forward. European Journal of Ageing, 18(3), 291–297. doi: 10.1007/s10433-021-00646-2 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gee, G. C., Morey, B. N., Walsemann, K. M., Ro, A., & Takeuchi, D. T. (2016). Citizenship as privilege and social identity: Implications for psychological distress. American Behavioral Scientist, 60(5–6), 680–704. doi: 10.1177/0002764216632834 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gee, G. C., & Ponce, N. (2010). Associations between racial discrimination, limited English proficiency, and health-related quality of life among 6 Asian Ethnic Groups in California. American Journal of Public Health, 100(5), 888–895. doi: 10.2105/AJPH.2009.178012 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gubernskaya, Z., Bean, F. D., & Van Hook, J. (2013). (Un)Healthy immigrant citizens: Naturalization and activity limitations in older age. Journal of Health and Social Behavior, 54(4), 427–443. doi: 10.1177/0022146513504760 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hawkley, L. C., Hughes, M. E., Waite, L. J., Masi, C. M., Thisted, R. A., & Cacioppo, J. T. (2008). From social structural factors to perceptions of relationship quality and loneliness: the Chicago Health, Aging, and Social Relations Study. The Journals of Gerontology, Series B: Psychological Sciences and Social Sciences, 63(6), S375–S384. doi: 10.1093/geronb/63.6.S375 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hossen, A. (2012). Social isolation and loneliness among elderly immigrants: The case of South Asian elderly living in Canada. Journal of International Social Issues, 1(1), 1–10. [Google Scholar]
- Hughes, M. E., Waite, L. J., Hawkley, L. C., & Cacioppo, J. T. (2004). A short scale for measuring loneliness in large surveys: Results from two population-based studies. Research on Aging, 26(6), 655–672. doi: 10.1177/0164027504268574 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hurh, W. M., & Kim, K. C. (1990). Adaptation stages and mental health of Korean male immigrants in the United States. International Migration Review, 24(3), 456–479. doi: 10.2307/2546369 [DOI] [Google Scholar]
- Jang, H., & Tang, F. (2022). Loneliness, age at immigration, family relationships, and depression among older immigrants: A moderated relationship. Journal of Social and Personal Relationships, 39(6), 1602–1622. doi: 10.1177/02654075211061279 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Johnson, H., Perez, C. A., & Mejia, M. C. (2021). Immigrants in California. Public Policy Institute of California. https://www.ppic.org/publication/immigrants-in-california/ [Google Scholar]
- Johnson, S., Bacsu, J., McIntosh, T., Jeffery, B., & Novik, N. (2021). Competing challenges for immigrant seniors: Social isolation and the pandemic. Healthcare Management Forum, 34(5), 266–271. doi: 10.1177/08404704211009233 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kessler, R. C., Andrews, G., Colpe, L. J., Hiripi, E., Mroczek, D. K., Normand, S.-L. T., Walters, E. E., & Zaslavsky, A. M. (2002). Short screening scales to monitor population prevalences and trends in non-specific psychological distress. Psychological Medicine, 32(6), 959–976. doi: 10.1017/S0033291702006074 [DOI] [PubMed] [Google Scholar]
- Kilduff, L. (2021, December). Which U.S. States have the oldest populations? Population Reference Bureau. Accessed January 9, 2023. https://www.prb.org/resources/which-us-states-are-the-oldest/ [Google Scholar]
- Kim, B. J., Jun, H., Lee, J., Linton, K., Kim, M., & Browne, C. (2017). Subjective well-being in older Chinese and Korean immigrants in the United States: Effects of self-rated health and employment status. Social Work in Public Health, 32(8), 510–520. doi: 10.1080/19371918.2017.1373719 [DOI] [PubMed] [Google Scholar]
- Kim, G., Worley, C. B., Allen, R. S., Vinson, L., Crowther, M. R., Parmelee, P., & Chiriboga, D. A. (2011). Vulnerability of older Latino and Asian immigrants with limited English proficiency. Journal of the American Geriatrics Society, 59(7), 1246–1252. doi: 10.1111/j.1532-5415.2011.03483.x [DOI] [PubMed] [Google Scholar]
- Kirmayer, L. J., Narasiah, L., Munoz, M., Rashid, M., Ryder, A. G., Guzder, J., Hassan, G., Rousseau, C., Pottie, K.; & Canadian Collaboration for Immigrant and Refugee Health (CCIRH). (2011). Common mental health problems in immigrants and refugees: General approach in primary care. Canadian Medical Association Journal, 183(12), E959–E967. doi: 10.1503/cmaj.090292 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Koehn, S., Ferrer, I., & Brotman, S. (2022). Between loneliness and belonging: Narratives of social isolation among immigrant older adults in Canada. Ageing & Society, 42(5), 1117–1137. doi: 10.1017/S0144686X20001348 [DOI] [Google Scholar]
- Leong, F., Park, Y. S., & Kalibatseva, Z. (2013). Disentangling immigrant status in mental health: Psychological protective and risk factors among Latino and Asian American immigrants. American Journal of Orthopsychiatry, 83(2pt3), 361–371. doi: 10.1111/ajop.12020 [DOI] [PubMed] [Google Scholar]
- Li, M. (2016). Pre-migration trauma and post-migration stressors for Asian and Latino American immigrants: Transnational stress proliferation. Social Indicators Research, 129(1), 47–59. doi: 10.1007/s11205-015-1090-7 [DOI] [Google Scholar]
- Mui, A. C., & Kang, S.-Y. (2006). Acculturation stress and depression among Asian immigrant elders. Social Work, 51(3), 243–255. doi: 10.1093/sw/51.3.243 [DOI] [PubMed] [Google Scholar]
- National Academies of Sciences, Engineering, and Medicine. (2020). Social isolation and loneliness in older adults: Opportunities for the health care system. National Academies Press. [PubMed] [Google Scholar]
- Pearlin, L. I., Aneshensel, C. S., & LeBlanc, A. J. (1997). The forms and mechanisms of stress proliferation: The case of AIDS caregivers. Journal of Health and Social Behavior, 223–236. doi: 10.2307/2955368 [DOI] [PubMed] [Google Scholar]
- Pearlin, L. I., Schieman, S., Fazio, E. M., & Meersman, S. C. (2005). Stress, health, and the life course: Some conceptual perspectives. Journal of Health and Social Behavior, 46(2), 205–219. doi: 10.1177/002214650504600206 [DOI] [PubMed] [Google Scholar]
- Pumariega, A. J., Rothe, E., & Pumariega, J. B. (2005). Mental health of immigrants and refugees. Community Mental Health Journal, 41(5), 581–597. doi: 10.1007/s10597-005-6363-1 [DOI] [PubMed] [Google Scholar]
- Sanchez, G. R., Vargas, E. D., Juarez, M. D., Gomez-Aguinaga, B., & Pedraza, F. I. (2017). Nativity and citizenship status affect Latinos’ health insurance coverage under the ACA. Journal of Ethnic and Migration Studies, 43(12), 2037–2054. doi: 10.1080/1369183x.2017.1323450 [DOI] [Google Scholar]
- Semega, J., Kollar, M., Creamer, J., & Mohanty, A. (2019). Income and poverty in the United States: 2018 (p. 88) [Current Population Reports]. U.S. Census Bureau. [Google Scholar]
- Taylor, H. O. (2020). Social isolation’s influence on loneliness among older adults. Clinical Social Work Journal, 48(1), 140–151. doi: 10.1007/s10615-019-00737-9 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Taylor, H. O., & Nguyen, A. W. (2020). Depressive symptoms and loneliness among black and white older adults: The moderating effects of race. Innovation in Aging, 4(5), igaa048. doi: 10.1093/geroni/igaa048 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Taylor, H. O., Taylor, R. J., Nguyen, A. W., & Chatters, L. (2018). Social isolation, depression, and psychological distress among older adults. Journal of Aging and Health, 30(2), 229–246. doi: 10.1177/0898264316673511 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Thoits, P. A. (2010). Stress and health: Major findings and policy implications. Journal of Health and Social Behavior, 51(1_suppl), S41–53. doi: 10.1177/0022146510383499 [DOI] [PubMed] [Google Scholar]
- Torres, J. M., & Wallace, S. P. (2013). Migration circumstances, psychological distress, and self-rated physical health for Latino immigrants in the United States. American Journal of Public Health, 103(9), 1619–1627. doi: 10.2105/AJPH.2012.301195 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Treas, J., & Mazumdar, S. (2002). Older people in America’s immigrant families: Dilemmas of dependence, integration, and isolation. Journal of Aging Studies, 16(3), 243–258. doi: 10.1016/s0890-4065(02)00048-8 [DOI] [Google Scholar]
- Tsuchiya, K., & Demmer, R. T. (2021). Citizenship status and prevalence of diagnosed and undiagnosed hypertension and diabetes among adults in the U.S., 2011–2016. Diabetes Care, 44(3), e38–e39. doi: 10.2337/dc20-2453 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Tsuchiya, K., Toles, O., Levesque, C., Horner, K., Ryu, E., Chan, L., & DeWaard, J. (2021). Perceived structural vulnerabilities among detained noncitizen immigrants in Minnesota. PLoS One, 16(6), e0252232. doi: 10.1371/journal.pone.0252232 [DOI] [PMC free article] [PubMed] [Google Scholar]
- US Census. (2021). Work status in the past 12 months by employment status for the civilian population 65 years and over. Accessed January 9, 2023.https://data.census.gov/table?q=California+Employment&t=Older+Population&tid=ACSDT1Y2021.C23004&tp=false
- Van Hook, J., Brown, S. K., & Bean, F. D. (2006). For love or money? Welfare reform and immigrant maturalization. Social Forces, 85(2), 643–666. doi: 10.1353/sof.2007.0029 [DOI] [Google Scholar]
- Viruell-Fuentes, E. A., Miranda, P. Y., & Abdulrahim, S. (2012). More than culture: Structural racism, intersectionality theory, and immigrant health. Social Science & Medicine, 75(12), 2099–2106. doi: 10.1016/j.socscimed.2011.12.037 [DOI] [PubMed] [Google Scholar]
- Watkins, D. C., & Johnson, N. C. (2018). Age and gender differences in psychological distress among African Americans and Whites: Findings from the 2016 National Health Interview Survey. Healthcare, 6(1), Article 1. doi: 10.3390/healthcare6010006 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wu, Z., & Penning, M. (2015). Immigration and loneliness in later life. Ageing & Society, 35, 64–95. doi: 10.1017/S0144686X13000470 [DOI] [Google Scholar]
- Yoo, H. C., Gee, G. C., & Takeuchi, D. (2009). Discrimination and health among Asian American immigrants: Disentangling racial from language discrimination. Social Science & Medicine, 68(4), 726–732. doi: 10.1016/j.socscimed.2008.11.013 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zhang, W., Hong, S., Takeuchi, D. T., & Mossakowski, K. N. (2012). Limited English proficiency and psychological distress among Latinos and Asian Americans. Social Science & Medicine, 75(6), 1006–1014. doi: 10.1016/j.socscimed.2012.05.012 [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.