Abstract
Urothelial cell carcinomas represent the vast majority of urinary bladder tumors.
However, many inflammatory and non-neoplastic conditions can mimic a urinary bladder malignancy. In that matter, diverticulitis can progress into colovesical fistula formation with a bladder wall abscess that can mimic a pseudo mass. Nonetheless, the presence of a bladder wall mass, usually requires pathologic examination. We report the case of a 60 year old woman with recurrent urinary infections due to a focal bladder mass revealing a colovesical fistula as a complication of sigmoid diverticulitis.
1. Introduction
Diverticulosis is a very common condition, most likely to occur in the sigmoïd. Diverticulitis represents a complication that ranges from inflammation, perforation to infection. Urothelial cell carcinomas on the other hand, represent the vast majority of urinary bladder tumors. However, many inflammatory and non-neoplastic conditions can mimic a urinary bladder malignancy among which diverticulitis represents a very specific subset.
2. Case presentation
We report the case of a 60 year old woman, with no past medical history presenting with recurrent urinary infections, and an episode of hematuria. The patient was febrile with abdominal tenderness on physical examination, laboratory results on the other hand showed elevated white blood cell count 16,940/mm3 and urinary analysis found evidence of infection and isolated Escherichia Coli. Initial abdominal ultrasound found no signs of hydronephrosis or obstruction, however a large dome bladder mass was found bulging in the bladder lumen. Therefore, a CT work up was performed, suggesting the presence of a urinary bladder tumor for which the patient underwent a trans urethral resection. Cystoscopy found a polypoid pediculated mass of the urinary dome with no extension to the trigone. Histopathological analysis came back negative for any malignant lesion. It revealed a chronic non-specific cystitis with inflammatory changes and no evidence of carcinoma in situ.
The patient reported persistent hematuria later complicated with pyuria, fever and signs of sepsis. Subsequently, an abdomino pelvic CT was performed at our institution.
It showed a diffuse thickening of the urinary bladder wall with a focal, ill-defined mass of the left aspect of the dome, protruding into the bladder lumen. This mass showed soft tissue density, a central low attenuation component with an air-fluid level and surrounding fat stranding (Fig. 1). It presented a close contact with the adjacent sigmoid colon.
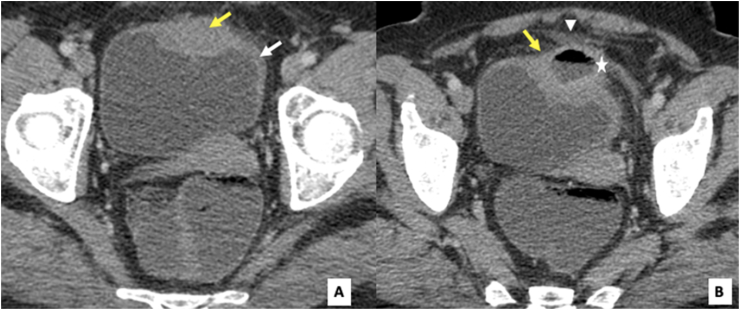
Fig. 1.
Axial CT images (A & B) at the portal phase showing diffuse bladder wall thickening (white arrow) with focal ill-defined mass (yellow arrow) of the left aspect of the dome, protruding into the bladder lumen. This mass is of soft tissue density, with a central low attenuation component and an air-fluid level (white asterisk) and surrounding fat stranding (white arrow head). (For interpretation of the references to colour in this figure legend, the reader is referred to the Web version of this article.)
The sigmoid colon presented diffuse circumferential wall thickening with many diverticuli in this segment, along with major paracolic fat stranding (Fig. 2). This fat stranding was extending to the bladder where the intervening fat plane between the bladder dome mass and colon was absent. Both the air-fluid level within the mass and the presence of a gas locule in the inflamed tissue between the colon and bladder were in keeping with a fistula. Gas was also noted in the bladder, although no contrast was seen in the sigmoid colon at the excretory phase and after the patient was put in a prone position(Fig. 3, Fig. 4).
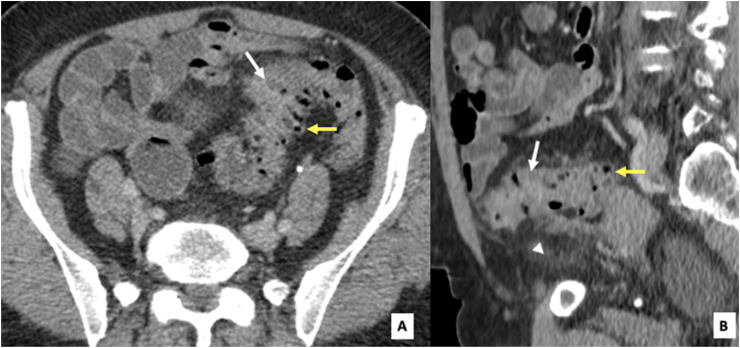
Fig. 2.
Axial (A) and sagittal (B) CT images diffuse circumferential wall thickening (white arrow) of the sigmoid colon with many diverticuli (yellow arrow), along with major paracolic fat stranding (white arrow). (For interpretation of the references to colour in this figure legend, the reader is referred to the Web version of this article.)
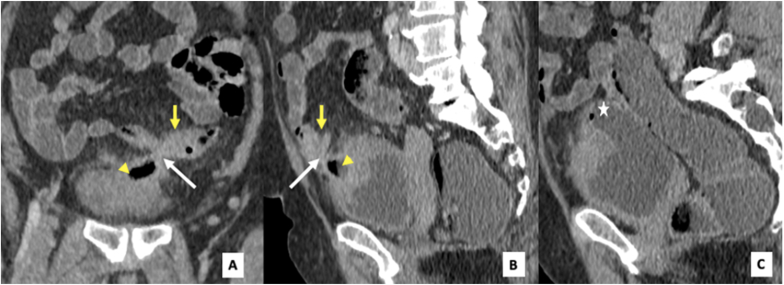
Fig. 3.
Coronal (A), sagittal (B & C), showing fat stranding with a gas locule in the inflamed tissue between the colon (yellow arrow) and bladder where the intervening fat plane between the bladder dome mass (yellow arrow head) and colon is absent (white arrow). Note the gas in the bladder (white asterisk). (For interpretation of the references to colour in this figure legend, the reader is referred to the Web version of this article.)
Fig. 4.
Axial (A) and sagittal (B) CT images showing no contrast the sigmoid colon at the excretory phase and after the patient was put in a prone position.
The diagnosis of a sigmoid diverticulitis with a colo-vesical fistula and abscess formation was made. The patient then had a sigmoid colon resection and a bladder repair.
Histopathological analysis of both the sigmoid colon and vesical sample unsured there was no underlying malignancy.
3. Discussion
The vast majority of urinary bladder tumors are commonly urothelial cell carcinomas.1
However many conditions can cause a focal wall thickening or a bladder mass mimicking a malignancy. These inflammatory pseudo tumors or non-neoplastic wall masses are important to recognize to avoid misdiagnosis and treatment delays.2 Although imaging features can overlap with malignant bladder lesions, a systematic approach and analysis of possible extra vesical findings allow the diagnosis to be readily made. Extrinsic inflammatory changes associated with diverticulitis can cause fistula formation to the bladder or focal wall bladder abnormalities.3
Regarding colonic diverticula formation, it is thought to involve a bowel wall abnormality and increased intra luminal pressure.4 The most common site of colonic diverticula development is the sigmoid colon. Diverticulitis is caused by obstruction of the neck of the diverticulum resulting in inflammation, possible perforation and infection. Local inflammatory changes may progress into abscess formation or fistulas typically on the left wall of the bladder.
Clinical presentation can be non-specific with abdominal unremitting pain and tenderness, fever and possible changes in bowel movement. In most instances the diagnosis of a colo-vesical fistula can be suspected given the presence of pneumaturia, faecaluria and recurrent urinary tract infections.5
Imaging and particularly computed tomography, is the most sensitive imaging modality to make a confident diagnosis.6
It features imaging findings of both diverticulitis and colo-vesical fistula. Colonic diverticulosis most frequently involving the sigmoid or left colon, with segmental wall circumferential wall thickening containing diverticula associated with peri colonic fat stranding. CT demonstrates bladder thickening or mass typically on the left wall. The mass can be of soft tissue density which can be misdiagnosed as a primary bladder tumor. Imaging findings also include bladder wall thickening adjacent to the colonic segment and paracolic fat stranding.2,6
The presence of gas in the bladder lumen and within the bladder mass help clinch the diagnosis. Like in our case the mass had a central low density attenuation with an air fluid level. Less frequently the tract itself can be directly visualized. In that matter, oral contrast administration can be helpful to confirm the diagnosis with opacification of the bladder.7,8
Other disorders can be among the differential of a non-neoplastic bladder mass such as inflammatory pseudo tumors, endometriosis and Crohn's disease. In these cases, clinical presentation, patient's history and specific radiologic appearance especially extra vesical findings make it easy to diagnose.2
Surgical resection of the fistulous tract and the abnormal bowel segment is the treatment of choice.9 Further colonoscopy is advised to ensure there is no underlying malignancy.
Good knowledge of this particular non-neoplastic bladder tumor is important to recognize and every clinician and radiologist should be aware of this entity. Colo vesical fistulas as a complication of diverticulis is common, however, mass and abscess formation on the bladder wall can be misleading. Computed tomography is the modality of choice to diagnose diverticulitis and its complications. Therefore, imaging plays a pivotal role to avoid misdiagnosis and ensure prompt management and treatment.
4. Conclusion
This case highlights the imaging features of diverticulitis complicated with colovesical fistulas as a rare cause of non-neoplastic bladder tumors. It appears important for every clinician and radiologist to be aware of this entity. While common presentation of diverticulitis can be easier to recognize and biopsy of all bladder lesion is well-established, good knowledge of possible fistulisation and pseudo bladder mass formation, warrants early detection and avoids misdiagnosis to initiate appropriate treatment management.
Declaration of interest
None.
CRediT authorship contribution statement
Selma Khouchoua: Writing – review & editing, Writing – original draft, Validation, Supervision, Methodology, Investigation, Data curation, Conceptualization. Kaoutar Imrani: Writing – review & editing, Supervision. Sara Cherkaoui: Validation. Nabil Moatassim Billah: Supervision. Ittimade Nassar: Supervision.
References
- 1.Wong-You–Cheong J.J., Woodward P.J., ManningMA, Sesterhenn I.A. Neoplasms of the urinarybladder: radiologic-pathologic correlation. Radiographics. 2006;26:553–580. doi: 10.1148/rg.262055172. [DOI] [PubMed] [Google Scholar]
- 2.Wong-You-Cheong J.J., Woodward P.J., Manning M.A., Davis C.J. From the archives of the AFIP: inflammatory and nonneoplastic bladder masses: radiologic-pathologic correlation. Radiographics. 2006 Nov-Dec;26(6):1847–1868. doi: 10.1148/rg.266065126. PMID: 17102055. [DOI] [PubMed] [Google Scholar]
- 3.Destigter K.K., Keating D.P. Imaging update: acute colonic diverticulitis. Clin Colon Rectal Surg. 2009;22:147–155. doi: 10.1055/s-0029-1236158. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Mulhall A.M., Mahid S.S., Petras R.E., Galandiuk S. Diverticular disease associated with inflammatory bowel disease-like colitis: a systematic review. Dis Colon Rectum. 2009;52:1072–1079. doi: 10.1007/DCR.0b013e31819ef79a. [DOI] [PubMed] [Google Scholar]
- 5.Sakhalkar O.V., Goyal A., Abualruz A.R. Segmental colitis associated with diverticulosis. Cureus. 2023 May 8;15(5) doi: 10.7759/cureus.38724. PMID: 37292528; PMCID: PMC10246860. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Yu N.C., Raman S.S., Patel M., Barbaric Z. Fistulas of the genitourinary tract: a radiologic review. Radiographics. 2004;24:1331–1352. doi: 10.1148/rg.245035219. [DOI] [PubMed] [Google Scholar]
- 7.Sugi M.D., Sun D.C., Menias C.O., Prabhu V., Choi H.H. Acute diverticulitis: key features for guiding clinical management. Eur J Radiol. 2020 Jul;128 doi: 10.1016/j.ejrad.2020.109026. Epub 2020 Apr 30. PMID: 32422553. [DOI] [PubMed] [Google Scholar]
- 8.Kessner R., Barnes S., Halpern P., Makrin V., Blachar A. CT for acute nontraumatic abdominal pain-is oral contrast really required? Acad Radiol. 2017 Jul;24(7):840–845. doi: 10.1016/j.acra.2017.01.013. Epub 2017 Feb 23. PMID: 28237189. [DOI] [PubMed] [Google Scholar]
- 9.You H., Sweeny A., Cooper M.L., Von Papen M., Innes J. The management of diverticulitis: a review of the guidelines. Med J Aust. 2019 Nov;211(9):421–427. doi: 10.5694/mja2.50276. Epub 2019 Jul 28. PMID: 31352692. KEY WORDS: Urinary bladder, hematuria, fistula, diverticulosis, sigmoid, CT. [DOI] [PubMed] [Google Scholar]