Summary
Emerging adulthood, the period between ages 18 and 25, is distinct from older and younger populations in terms of both physiology and social circumstances. As a critical developmental window with long-lasting repercussions, emerging adulthood presents a key opportunity for prevention of cardiovascular disease. Despite significant advances in diabetes and cardiovascular disease prevention for other age groups, 18–25 year-olds remain underrepresented in research. Using diabetes prevention as an example, we analyzed the cited evidence behind four major guidelines that influence US clinical practice on screening and management of prediabetes in children and adults, revealing that the majority of these studies in both the pediatric and adult literature do not include emerging adults in their study populations. This gap between the pediatric and adult diabetes prevention literature creates a missing link connecting childhood risks to adult chronic disease. In this article, we draw attention to this often overlooked age group, and provide tangible recommendations as a path forward for both pediatric and adult researchers to increase the representation of emerging adults in diabetes prevention and other cardiovascular disease prevention studies.
Keywords: Emerging adulthood, Cardiovascular disease prevention, Diabetes prevention, Adolescent and young adult, Research design, Age representation in research
Emerging adulthood, the period between adolescence and adulthood conservatively defined as ages 18–25, presents a key opportunity for prevention of chronic disease. Despite significant advances in diabetes prevention, and more broadly cardiovascular disease (CVD) prevention for other age groups, 18–25 year-olds remain underrepresented in research. This gap between the paediatric and adult diabetes prevention literature creates a missing link connecting childhood risks to adult chronic disease.
A critical few years
While emerging adulthood spans less than a decade, findings from epidemiology and psychology demonstrate that this brief window is developmentally distinct and unusually impactful for future health.1 This period is defined by a beginning age of 18, as this age is accepted as delineating the end of childhood according to governmental and other societal definitions. The age at which a person exits emerging adulthood and moves on to adulthood is a matter of debate in the developmental literature, with some definitions extending to age 29 and others capping the period at 25.2, 3, 4 We have opted to use the more conservative definition of ages 18–25, as these ages are broadly accepted to comprise at least part of emerging adulthood, reflecting the core population within the developmental window.
During these years, exposures may have a particularly long-lasting impact on future health behaviours, socioeconomic achievement, and adult health trajectory.1,5 Intuitively, the launch into independent adulthood may be thought of as akin to early childhood, a “blank slate” opportunity (albeit influenced by childhood experience) on which new adults establish new habits, behaviours, and communities that they will carry forward throughout their adult lives. Corroborating this theory, studies demonstrate that emerging adults experience rapid weight gain that is sustained into later adulthood, lasting declines in physical activity, and sustained reductions in dietary quality.6
These years stand apart from other ages on physical and social dimensions. Physiologically, emerging adults have completed puberty but will not reach developmental maturity until closer to age 30. Well-known examples of this include peak bone mass and brain maturation that extend into the late 20s. Emerging adults experience unique social, psychological, environmental and commercial exposures. For example, emerging adults have some of the highest levels of social instability (e.g., highest rates of unemployment, frequent changes in household composition and geography).7 Their high prevalence of mental health disorders and not-yet-fully-developed executive function capacity mean emerging adults’ coping is different from that of general adults, and health impacts mediated by psychosocial stress may be experienced more strongly.8 Emerging adults also have among the lowest rates of health care access, and face age-based eligibility gaps in Medicaid.7 Pertinent to diabetes prevention, the heightened insulin resistance of puberty seems to regress during this period, though whether this is temporary or permanent remains understudied.9,10
Despite an increasing recognition of the life course development of diabetes and CVD,11 and specific calls for increased CVD prevention efforts targeted to young adults,12,13 wide gaps in the prevention literature remain. Existing prevention for emerging adults focuses primarily on age-group specific risk factors such as sexual health, mental health, substance use, and safety, rather than life-long diabetes and CVD prevention.14 Rare bright spots include the EARLY consortium of clinical trials for weight loss interventions in emerging adults,5,15 and the RISE consortium of trials on interventions for beta cell preservation which includes paediatric and adult arms for comparative analysis,16 yet these examples remain the exception.
The evidence gap for emerging adults: example of the diabetes prevention guidelines
As an example of this missing link in the prevention literature, we reviewed the age ranges of study populations in the cited evidence behind four major guidelines that influence US clinical practice on screening and management of prediabetes in children and adults: American Diabetes Association Standards of Care in Diabetes,17 US Preventive Services Taskforce (USPSTF) guidelines on screening for prediabetes in adults and children,18,19 and American Academy of Pediatrics (AAP) guidelines on obesity.20
Search methods
From each guideline's associated evidence review, we compiled all articles on which the guidelines were based. This included: for USPSTF, all articles in tables; for AAP, all articles in the tables in the “Glucose Metabolism” sections; ADA all citations in the review, excluding those that were not studies of a sample population (such as systematic reviews, guidelines, narratives and commentaries), as this review did not include tables specifying which articles were the basis of the guidelines.
We de-duplicated across and within sources, including de-duplication of exact references, and of trial name, such that if multiple articles described the same trial we included only one article (with the exception of large nationally representative samples, e.g., NHANES, given that different articles drew upon different sample subsets).
For each article, we recorded the youngest and oldest age of participants. If the article did not report participant ages in the body of the text but provided a separate reference or appendix for detailed recruitment methodology, we followed that reference to look for participant age range. If both inclusion criteria and an actual age range were reported, we listed the actual age range. Finally, if the reported age range included any ages within 18–25, we then reviewed the article to determine whether an age breakdown was included in the text, tables, or figures.
The gap in diabetes prevention guidelines
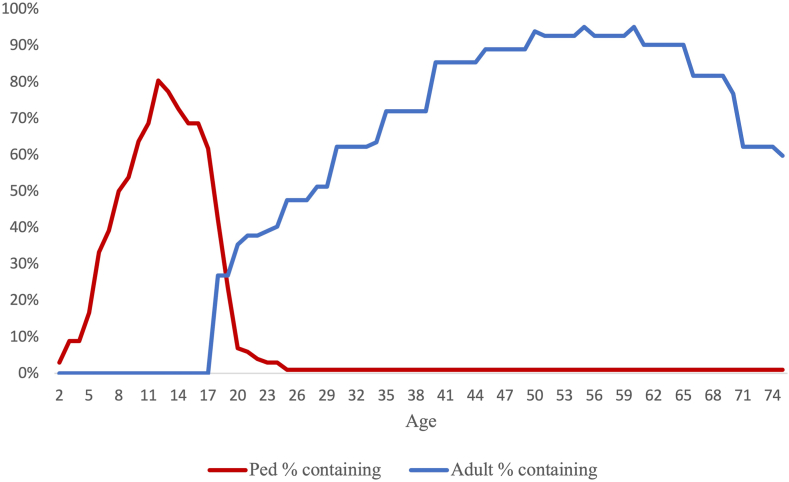
Of the 209 studies cited in the guidelines’ evidence reviews, 11% (n = 22) included the entire 18–25 age range (Fig. 1). Most paediatric studies had an upper age at or below 18, and adult studies had a lower age above 18.
Fig. 1.
Percentage of pediatric and adult studies cited in major diabetes prevention guidelines containing each age within their study population. Overall sample of 209 articles included n = 94 adult and n = 115 pediatric studies. Figure excludes articles not reporting age range of study population (12%, n = 25).
This gap is problematic in determining screening and treatment recommendations for the nearly quarter of emerging adults who have prediabetes.21 For example, it is unclear whether metformin may be effective in preventing diabetes for emerging adults. A recent review of adult prediabetes trials found metformin most effective for diabetes prevention in those under 60,22 while a similar review of paediatric trials found metformin ineffective at diabetes prevention in youth.23 The youngest age of participants in the cited adult trials was 25, and the oldest participants in the youth trials were 19, with none of the cited trials including 19–25 year-olds.
Importantly, the studies included in our analysis form the basis of clinical practice guidelines and therefore primarily represent clinical trials. Observational data may offer insights about populations underrepresented in clinical trials, and indeed there are examples of this across the CVD prevention literature.24,25 However, this is not a substitute for inclusion in clinical trials, both because clinical trial results are themselves unreliable if they rely on non-representative samples, and because conclusions drawn from observational studies are more prone to error.26 Marginalized populations such as emerging adults should benefit from the strength of clinical trial data.
Multiple factors likely contribute to the emerging adulthood gap. These include real and perceived limitations, such as the convention that paediatrics ends at 18, that young adults may be earlier in the natural history of chronic disease processes and therefore less likely to develop measurable outcomes within the study period, difficulty with recruitment and retention of emerging adults, differing IRB requirements for participants above and below 18, and sample size constraints that are powered only for more homogenous age groups. These downsides may be outweighed by theoretical benefits of including the emerging adult population in prediabetes screening and management—such as earlier intervention to delay progression longer, and maintaining the gains from preventive interventions in childhood. These benefits may be particularly strong for populations with earlier onset and/or higher prevalence of diabetes and CVD, including marginalised racial and ethnic groups in the US and people in low and middle-income countries such as in Central and Latin America.27,28 Without dedicated study the extent of these potential limitations and strength of potential benefits remain untested.
While this is an example of diabetes prevention, we suspect that corollary examples exist in other areas of CVD prevention, such as screening and preventive measures for hypertension, hyperlipidaemia, and lifestyle risk factors. This is because there is no theoretical reason why the diabetes literature in particular would exclude young adults but other fields would be more inclusive, especially since type 2 diabetes is recognised to occur at all ages, including during adolescence and young adulthood. However, future efforts could conduct similar analyses of other aspects of CVD prevention beyond diabetes.
Recommendations
Given the unique aspects that set it apart from other age groups, emerging adulthood merits both dedicated study and improved representation in diabetes prevention research and likely broader CVD prevention research. There is precedent to calling upon general researchers to improve age representation, namely the NIH's Inclusion Across the Lifespan policy, which is intended to ensure children and older adults are included in research.29 The following strategies for paediatric and adult investigators would help alleviate the emerging adulthood blind spot to improve prevention across the life course.
Increase prevention research dedicated to emerging adults
Prevention researchers should consider developing dedicated studies for this underserved age group. A small number of recent young adult prevention studies have kicked off this effort, but these studies are often overlooked in guidelines.17, 18, 19, 20 This reflects a need for increased visibility and rigor, with larger, more robust studies of prevention in this age range.
-
•
Conduct studies specifically focused on diabetes and CVD prevention in young adults that include 18–25 year-olds.
Avoid arbitrary age cutoffs in exclusion criteria
Our review of adult studies showed that 74% set a lower age limit above 18. This is a missed opportunity to learn about emerging adults.
Similarly, our review of paediatric studies showed that 75% used an upper age cutoff of 18 or younger. There is strong precedent to include at least up to 21 or even older in paediatric studies (e.g., the AAP considers the clinical “age of paediatrics” to extend to 21; parental insurance covers to age 26). Paediatric investigators already use strategies to reach adolescents, so reaching the emerging adult group is especially feasible.
-
•
Adult studies should include the entire adult population, with a lower age limit of 18 (or younger).
-
•
Paediatric studies should include the entire age of paediatrics, with an upper age limit of 21 (or older).
-
•
These limits should apply to all adult and paediatric studies, except in cases where more restrictive cutoffs may be theoretically justified (e.g. studies dedicated to early childhood or older adults).
Deploy tailored strategies for improved recruitment and retention of emerging adults
Expanding inclusion criteria is just the first step. In five articles reporting inclusion criteria ≥18, the youngest ages of actual participants ranged from 23 to 35 years. To recruit for proportionate representation, investigators can draw upon existing strategies that have been shown to improve emerging adult research participation, including digital recruitment, flexible scheduling, and opportunities for participatory design.30
-
•
Use emerging adult friendly strategies in recruitment efforts.
Increase attention to age representation
Investigators can publish age breakdowns in descriptions of population samples. While most studies publish mean age in descriptive tables, age breakdowns allow for more accurate assessment of generalizability. Only 8% (n = 7) of the studies we reviewed that had inclusion criteria for at least some ages within 18–25 reported an age breakdown. When reported, many of these age bands were wide, grounded in numbers of participants (e.g. age 18–45) rather than by theory.
-
•
Show breakdowns of age groups (not just mean age) in descriptions of study populations.
-
•
Age bands should be grounded in theory (e.g. groups expected to have similar physiology and/or life circumstances, as it pertains to the study question) rather than by numbers of participants.
-
•
Age bands should be sufficiently narrow to draw inferences about generalizability (e.g. 18–25, rather than 18–45).
Include emerging adults in studies in proportion to their population representation
Finally, investigators should strive for at least proportionate age inclusion (if not overrepresentation) to achieve a representative sample. The few age breakdowns included in existing publications reflected an underrepresentation of young adults, e.g. less than 3% of study participants in a US based study, while 19–25 year-olds comprise 11% of the US population.
-
•
The proportion of the study population that is 18–25 years old should be equivalent to, or greater than, the population-wide proportion of people in this age group.
Conclusion
Emerging adulthood is a critical link connecting childhood risks to adult chronic disease. However, 18–25 year-olds have been left out of diabetes prevention research within both the paediatric and adult literature, as demonstrated by our review of the evidence informing guidelines for prediabetes screening and management. All researchers can take steps to make their work more inclusive of this underserved age group. With increased awareness and inclusion of this important age group, researchers can make lasting impacts to prevent diabetes and cardiovascular disease over the life course.
Contributors
AA contributed to conceptualisation, conducted the literature search, analysis, and initial drafting of the manuscript. HKS contributed to conceptualisation, writing, review and editing of the manuscript.
Declaration of interests
HKS is the recipient of multiple grants and holds leadership roles related to obesity and diabetes, all through non-profit, government and academic entities. AA has no conflicts of interest to disclose.
Acknowledgements
AA is supported by the Health Resources and Services Administration (HRSA) of the US Department of Health and Human Services (HHS) through grant number T32HP19025. HKS is supported by the National Institute of Diabetes and Digestive and Kidney Diseases under award number P30DK092924. The contents are those of the author(s) and do not necessarily represent the official views of, nor an endorsement, by HRSA, HHS or the US Government.
References
- 1.Arnett J.J. Emerging adulthood: what is it, and what is it good for? Child Dev Perspect. 2007;1(2):68–73. [Google Scholar]
- 2.Nelson L.J. The theory of emerging adulthood 20 years later: a look at where it has taken us, what we know now, and where we need to go. Emerg Adulthood. 2021;9(3):179–188. [Google Scholar]
- 3.Nice M.L., Joseph M. The features of emerging adulthood and individuation: relations and differences by college-going status, age, and living situation. Emerg Adulthood. 2023;11(2):271–287. [Google Scholar]
- 4.Arnett J.J., Mitra D. Are the features of emerging adulthood developmentally distinctive? A comparison of ages 18–60 in the United States. Emerg Adulthood. 2020;8(5):412–419. [Google Scholar]
- 5.Lanoye A., Brown K.L., LaRose J.G. The transition into young adulthood: a critical period for weight control. Curr Diabetes Rep. 2017;17:1–14. doi: 10.1007/s11892-017-0938-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Nelson M.C., Story M., Larson N.I., Neumark-Sztainer D., Lytle L.A. Emerging adulthood and college-aged youth: an overlooked age for weight-related behavior change. Obesity. 2008;16(10):2205. doi: 10.1038/oby.2008.365. [DOI] [PubMed] [Google Scholar]
- 7.Adams G., Hahn H., Coffey A. Urban Institute; Washington, DC: 2021. Stabilizing young people transitioning to adulthood: opportunities and challenges with key safety net programs. [Google Scholar]
- 8.Huang Y., Heflin C.M., Validova A. Material hardship, perceived stress, and health in early adulthood. Ann Epidemiol. 2021;53:69–75. doi: 10.1016/j.annepidem.2020.08.017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Kelsey M.M., Zeitler P.S. Insulin resistance of puberty. Curr Diabetes Rep. 2016;16:1–6. doi: 10.1007/s11892-016-0751-5. [DOI] [PubMed] [Google Scholar]
- 10.Love-Osborne K.A., Sheeder J.L., Nadeau K.J., Zeitler P. Longitudinal follow up of dysglycemia in overweight and obese pediatric patients. Pediatr Diabetes. 2018;19(2):199–204. doi: 10.1111/pedi.12570. [DOI] [PubMed] [Google Scholar]
- 11.Lloyd-Jones D.M., Allen N.B., Anderson C.A.M., et al. Life's essential 8: updating and enhancing the American heart association's construct of cardiovascular health: a presidential advisory from the American heart association. Circulation. 2022;146(5):e18–e43. doi: 10.1161/CIR.0000000000001078. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Gooding H.C., Gidding S.S., Moran A.E., et al. Challenges and opportunities for the prevention and treatment of cardiovascular disease among young adults: report from a national heart, lung, and blood institute working group. J Am Heart Assoc. 2020;9(19) doi: 10.1161/JAHA.120.016115. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Allen N., Wilkins J.T. The urgent need to refocus cardiovascular disease prevention efforts on young adults. JAMA. 2023;329(11):886–887. doi: 10.1001/jama.2023.2308. [DOI] [PubMed] [Google Scholar]
- 14.Harris S.K., Aalsma M.C., Weitzman E.R., et al. Research on clinical preventive services for adolescents and young adults: where are we and where do we need to go? J Adolesc Health. 2017;60(3):249–260. doi: 10.1016/j.jadohealth.2016.10.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Johnson K.C., Thomas F., Richey P., et al. The primary results of the treating adult smokers at risk for weight gain with interactive technology (TARGIT) study. Obesity. 2017;25(10):1691–1698. doi: 10.1002/oby.21968. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Rise C. Restoring Insulin Secretion (RISE): design of studies of β-cell preservation in prediabetes and early type 2 diabetes across the life span. Diabetes Care. 2014;37(3):780–788. doi: 10.2337/dc13-1879. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.ElSayed N.A., Aleppo G., Aroda V.R., et al. 3. Prevention or delay of type 2 diabetes and associated comorbidities: standards of care in diabetes—2023. Diabetes Care. 2023;46(Supplement_1):S41–S48. doi: 10.2337/dc23-S003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Jonas D.E., Vander Schaaf E.B., Riley S., et al. Screening for prediabetes and type 2 diabetes in children and adolescents: evidence report and systematic review for the US preventive services task force. JAMA. 2022;328(10):968–979. doi: 10.1001/jama.2022.7957. [DOI] [PubMed] [Google Scholar]
- 19.Jonas D.E., Crotty K., Yun J.D.Y., et al. Screening for prediabetes and type 2 diabetes: updated evidence report and systematic review for the US preventive services task force. JAMA. 2021;326(8):744–760. doi: 10.1001/jama.2021.10403. [DOI] [PubMed] [Google Scholar]
- 20.Skinner A.C., Staiano A.E., Armstrong S.C., et al. Appraisal of clinical care practices for child obesity treatment. Part II: comorbidities. Pediatrics. 2023;151 doi: 10.1542/peds.2022-060643. [DOI] [PubMed] [Google Scholar]
- 21.Andes L.J., Cheng Y.J., Rolka D.B., Gregg E.W., Imperatore G. Prevalence of prediabetes among adolescents and young adults in the United States, 2005-2016. JAMA Pediatr. 2020;174(2):e194498. doi: 10.1001/jamapediatrics.2019.4498. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Echouffo-Tcheugui J.B., Perreault L., Ji L., Dagogo-Jack S. Diagnosis and management of prediabetes: a review. JAMA. 2023;329(14):1206–1216. doi: 10.1001/jama.2023.4063. [DOI] [PubMed] [Google Scholar]
- 23.Magge S.N., Silverstein J., Elder D., Nadeau K., Hannon T.S. Evaluation and treatment of prediabetes in youth. J Pediatr. 2020;219:11–22. doi: 10.1016/j.jpeds.2019.12.061. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Nadal J.F., Cases M.M., Puente D.M. Epidemiology and clinical management of type 2 diabetes mellitus and associated comorbidities in Spain (e-Management study) Med Clín. 2016;147:1–7. doi: 10.1016/S0025-7753(17)30618-8. [DOI] [PubMed] [Google Scholar]
- 25.Kautzky-Willer A., Leutner M., Harreiter J. Sex differences in type 2 diabetes. Diabetologia. 2023;66(6):986–1002. doi: 10.1007/s00125-023-05891-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Liu F., Panagiotakos D. Real-world data: a brief review of the methods, applications, challenges and opportunities. BMC Med Res Methodol. 2022;22(1):287. doi: 10.1186/s12874-022-01768-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Pool L.R., Ning H., Lloyd-Jones D.M., Allen N.B. Trends in racial/ethnic disparities in cardiovascular health among US adults from 1999–2012. J Am Heart Assoc. 2017;6(9) doi: 10.1161/JAHA.117.006027. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Okwuosa I.S., Lewsey S.C., Adesiyun T., Blumenthal R.S., Yancy C.W. Worldwide disparities in cardiovascular disease: challenges and solutions. Int J Cardiol. 2016;202:433–440. doi: 10.1016/j.ijcard.2015.08.172. [DOI] [PubMed] [Google Scholar]
- 29.NIH . 2023. Inclusion across the lifespan.https://grants.nih.gov/policy/inclusion/lifespan.htm [Google Scholar]
- 30.LaRose J.G., Reading J.M., Lanoye A., Brown K.L. Recruitment and retention of emerging adults in lifestyle interventions: findings from the REACH trial. Contemp Clin Trials. 2022;121 doi: 10.1016/j.cct.2022.106904. [DOI] [PMC free article] [PubMed] [Google Scholar]