Abstract
A State-of-the Art lecture titled “Thrombo-Neuroinflammatory Disease” was presented at the International Society on Thrombosis and Haemostasis Congress in 2023. First, we would like to advocate for discrimination between immunothrombosis and thrombo-inflammation, as immunothrombosis describes an overshooting inflammatory reaction that results in detrimental thrombotic activity. In contrast, thrombo-inflammation describes the interplay of platelets and coagulation with the immunovascular system, resulting in the recruitment of immune cells and loss of barrier function (hence, hallmarks of inflammation). Both processes can be observed in the brain, with cerebral venous thrombosis being a prime example of immunothrombosis, while infarct progression in response to ischemic stroke is a paradigmatic example of thrombo-inflammation. Here, we review the pathomechanisms underlying cerebral venous thrombosis and ischemic stroke from a platelet-centric perspective and discuss translational implications. Finally, we summarize relevant new data on this topic presented during the 2023 International Society on Thrombosis and Haemostasis Congress.
Keywords: blood platelets, cerebral venous thrombosis, immunothrombosis, ischemic stroke, thrombo-inflammation
Graphical abstract
Essentials
-
•
Ischemic stroke and cerebral venous thrombosis are both leading causes of disability.
-
•
Both involve plasmatic coagulation, platelets, and immune cells, but pathomechanisms differ.
-
•
Stroke is a thrombo-inflammatory disease with immune cell recruitment and barrier breakdown.
-
•
Cerebral venous thrombosis is caused by thrombotic occlusion of cerebral veins and is a prime example of immunothrombosis.
1. Introduction
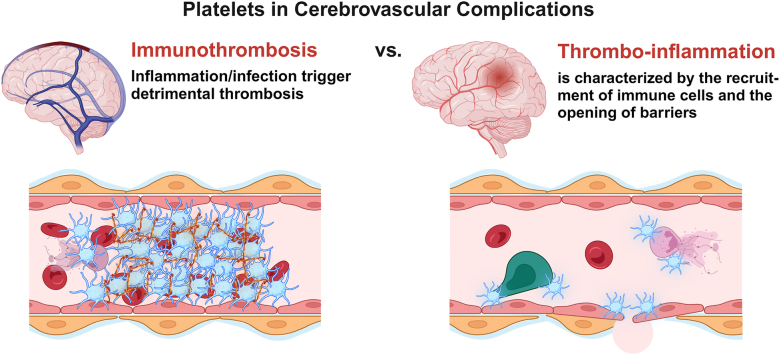
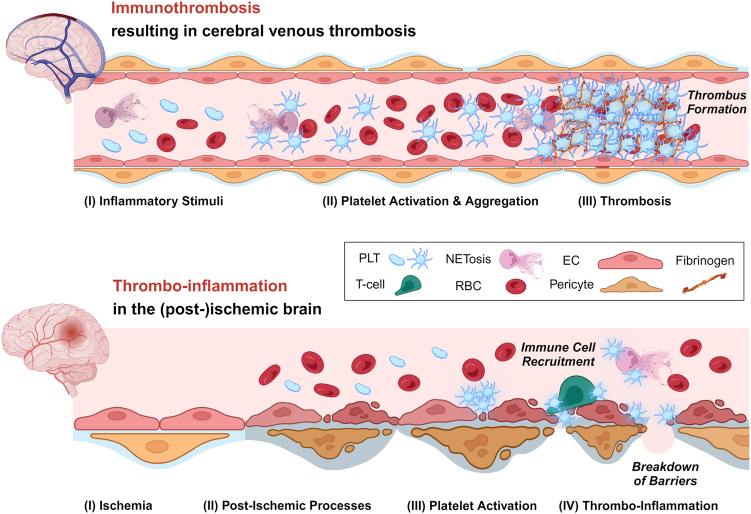
Platelets, which derive from megakaryocytes within the bone marrow, are best known for their role in hemostasis and thrombosis. However, during the last 15 years, it has become clear that they also act as effector cells in inflammation, immune responses, development, and maintenance of barrier integrity [[1], [2], [3], [4], [5], [6], [7], [8], [9]]. While thrombosis and inflammation were long considered separate (patho-)physiological processes, overwhelming experimental and clinical evidence has demonstrated that they are indeed closely intertwined. These interactions can occur in 2 fundamentally different manners: immunothrombosis or thrombo-inflammation.
The term immunothrombosis was introduced by Engelmann and Massberg [10] to describe immune-related thrombotic activity that prevents pathogen spreading. Meanwhile, the term immunothrombosis is used in a broader sense to describe infection or sterile inflammation-driven thrombotic events [11,12]. Importantly, the major pathological outcome is thrombosis, leading to insufficient supply of downstream tissue. Immunothrombosis should, however, not be confused with thrombo-inflammation, even though in both cases, an interplay between platelets and immune cells is observed (Figure 1). The term “thrombo-inflammation” was first proposed during studies of post-angioplasty restenosis due to platelet-leukocyte interactions [13]. Thrombo-inflammation was then recapitulated in studies involving platelet-eosinophil/neutrophil aggregation and platelet-promoted release of eosinophil/neutrophil oxidant products [14,15]. Subsequently, the Würzburg platelet group has used this term to describe the interplay of components of the thrombotic and inflammatory system driving ischemia/reperfusion (I/R) injury in acute ischemic stroke [1,[16], [17], [18], [19]]. In this process, initial platelet adhesion/activation pathways act in concert with key components of the contact pathway of plasmatic coagulation (factor [F]XII—kallikrein/kinin pathway) and immune cells to promote cerebral infarct growth [1]. Thus, the classical thromboembolic insult (brain artery occlusion) triggers a subsequent pathomechanism that again depends on platelets (and coagulation factors), which, however, in this context, use different signaling pathways and effector functions to orchestrate immune cell recruitment, edema formation, and eventually inflammatory tissue damage. Today, thrombo-inflammation is recognized as a major pathomechanism in a continuously growing number of arterial and venous disorders in different organs and disease states [2,20].
Figure 1.
Essential pathophysiological differences underlying immunothrombosis and thrombo-inflammation in the cerebral vasculature. Both entities involve platelets, the plasmatic coagulation cascade, and immune cells. However, the main difference is the primary outcome: in the case of immunothrombosis, the primary outcome is the occlusion of a blood vessel due to platelet-involved thrombotic activity in response to initial inflammatory stimuli. One example of an immunothrombotic disease is cerebral venous thrombosis. In the context of thrombo-inflammation, the hallmarks are the recruitment of immune cells and the disturbance of barrier functions. This is best exemplified in the context of ischemic stroke, where non-classical functions of platelets are activated during post-ischemic processes. These platelet functions beyond thrombosis then contribute to thrombo-inflammation. EC, endothelial cell; NET, neutrophil extracellular trap; PLT, platelet; RBC, red blood cell.
In the context of brain vasculature, typical immunothrombosis is seen in cerebral venous thrombosis (CVT), whereas thrombo-inflammation predominantly contributes to tissue damage/infarct progression following acute ischemic stroke. Thus, this review article will discuss more details about immunothrombosis and thrombo-inflammation based on these 2 prototypic diseases, respectively.
2. Cerebral Venous and Dural Sinus Thrombosis
Thrombosis takes place when an occlusive blood clot is developed in an artery or vein. Typical diseases caused by thrombosis include ischemic stroke, myocardial infarction, peripheral deep vein thrombosis, and its most dangerous complication, pulmonary embolism. The aftermath of thrombosis, in many cases, is fatal. Venous thrombosis harbors quite a few distinct features from arterial thrombosis, such as its growth at a low shear rate, frequent involvement of red blood cells, and a more prominent involvement of immune cells. Infections and inflammation are determined as risk factors for venous thrombosis, making the mechanisms of immunothrombosis a possible explanation for those “unprovoked” cases of venous thrombosis [21]. The emerging role of the hyperactivated immune system in venous thrombosis is represented by the involvement of neutrophil activation together with the formation and release of neutrophil extracellular traps (NETs) [22,23].
Cerebral venous and dural sinus thrombosis is a rare, atypical form of venous thrombosis that occurs either at a dural sinus (in particular, superior sagittal sinus), cortical vein, or the proximal jugular vein. Its occurrence in Western countries is estimated to be 4 per million in adults and 7 per million in neonates, with a mortality rate of 5% to 10% [24,25]. The risk factors of CVT can be genetic prothrombotic conditions, antiphospholipid syndrome, infections, head trauma, brain tumors, neurosurgery, anemia, and obesity, whereas the most significant risk factors are oral contraceptive use, pregnancy, and puerperium [26]. This indicates that hormonal changes contribute to the development of CVT and partly explains why women are more susceptible to CVT. CVT turns out to be the main cause of non-arterial stroke among young adults, accounting for 0.5% of all stroke cases. The symptoms of CVT can be highly heterogeneous, ranging from isolated headaches, visual/auditory disturbance, and hemiparesis to a comatose state, leaving the diagnosis of CVT a challenging task without the aid of medical imaging. Hydrocephalus, hemorrhage, intracranial hypertension, herniation, and seizure are common acute complications of CVT. Among several ongoing multicenter registries and clinical trials, the European guidelines on CVT diagnosis and management were updated in 2017 with recommendations made from an optimized level of evidence [27].
Conventional perspectives hold that the contribution of platelets appears to be more fundamental in arterial thrombosis versus venous thrombosis [28]. Thus, arterial thrombosis is deemed a platelet-associated disease, and antiplatelet drugs have been greatly recommended for the primary and secondary prevention of arterial thrombotic diseases. Platelets in the venous thrombi are found proportionally low, so venous thrombosis is commonly regarded as a coagulation cascade-related disease that should be treated with anticoagulants. However, mounting evidence suggests that platelets also play critical roles in the growth of venous thrombi. Systemic platelet activation has been determined in patients with acute venous thromboembolism [29]. The absence of platelets dampens the formation of thrombi in experimental venous thrombosis [30]. Using antiplatelet drugs such as aspirin and clopidogrel in murine venous stasis models or for patients subjected to orthopedic surgery, the risks of venous thrombosis and recurrence are consistently reduced [31,32]. The bleeding risk was not appreciable.
When it selectively comes to CVT, however, current knowledge about the underlying pathomechanisms is limited, which is in part due to the limitations of current animal models [33]. It appears that CVT is an immunothrombotic disease as thrombi from patients with CVT are rich in NETs [34], and platelet-driven NET formation is a crucial factor for the formation of venous thrombi in deep vein thrombosis [35,36]. Further evidence comes from the fact that the COVID-19 pandemic resulted in rising numbers of CVT cases [37,38], with immunothrombosis being one of the pathomechanisms underlying COVID-19 [11].
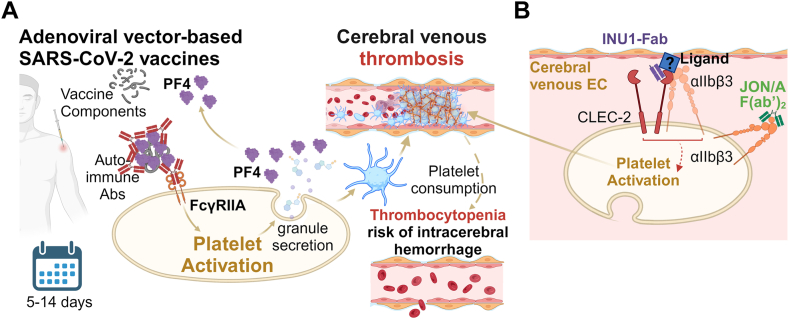
In response to the COVID-19 pandemic, vaccines were rapidly developed, and unprecedented numbers of people were vaccinated within short periods of time. This allowed that even very rare side effects of the vaccines were detectable. A small fraction of individuals who received AstraZeneca/Oxford and Johnson & Johnson recombinant adenovirus vector-based SARS-CoV-2 vaccines developed a vaccine-induced immune thrombotic thrombocytopenia (VITT). This term was coined to highlight the similarities between VITT and heparin-induced thrombocytopenia (HIT) [39], as highly pathogenic anti–platelet factor 4 (anti-PF4) autoantibodies with heparin-independent platelet-activating properties are present in those patients (Figure 2A). As these antibodies trigger platelet activation via the FcγRIIA receptor, patients are usually treated with intravenous (i.v.) immunoglobulin to block FcγRIIA and a non-heparin anticoagulant [39]. The most severe consequence of VITT is CVT [40], which is frequently followed by intracranial hemorrhage. Moreover, the first clinical data indicates that anti-PF4 antibodies from patients with VITT binding to certain epitopes on PF4 are more likely to be associated with CVT than others [41]. However, it is not clear whether a second hit is required for VITT-caused thrombi to develop within the cerebral vasculature.
Figure 2.
Cellular and molecular mechanisms regarding cerebral venous thrombosis (CVT) and vaccine-induced thrombotic thrombocytopenia (VITT). (A) One of the severe side effects of adenoviral vector-based SARS-CoV-2 vaccines is VITT. Briefly, the systemic inflammatory status due to vaccination can trigger a release of platelet factor 4 (PF4) from activated platelets. PF4 further forms a complex with vaccine components, which results in the engagement with anti-PF4 autoimmune antibodies (Abs). Once anti-PF4 antibodies are part of an immunocomplex, they are recognized by the FcγRIIA on the surface of platelets and neutrophils, leading to platelet activation and NETosis, ultimately resulting in thrombosis. As a severe complication of VITT, CVT occurs when the thrombi develop right in the brain venous system. The consumption of platelets further leads to secondary thrombocytopenia, which is particularly susceptible to intracerebral hemorrhage upon inflammatory conditions. (B) In an experimental CVT model, Fab-fragments of the anti-C-type lectin-like receptor-2 (CLEC-2) antibody INU1 apparently alter the conformation of CLEC-2. Consequently, CLEC-2 is able to interact with an unidentified ligand, which is enriched in cerebral veins. Then, cooperative signaling of CLEC-2 and αIIbβ3 triggers platelet activation, resulting in a rapidly progressing CVT. Blocking CLEC-2 signaling or αIIbβ3 (eg, using the anti-αIIbβ3 JON/A-F[ab’]2-fragments) prevents CVT, indicating that this might be a novel therapeutic strategy. EC, endothelial cell.
Recently, we revealed that the activation of C-type lectin-like receptor-2 (CLEC-2), whose signaling pathway is similar to that of FcγRIIA, can trigger CVT as well. Mice receiving a monovalent anti–CLEC-2 Fab-fragment (INU1) developed CVT within minutes after INU1-Fab i.v., which is accompanied by tonic-myoclonic seizures and thrombocytopenia [42]. Of note, thrombi were observed in various cerebral veins but not in other organs. The absence of CLEC-2 or inhibition of downstream signaling abolished all INU1-triggered effects, while heparin had only moderate effects. Interestingly, JON/A-F(ab’)2 fragments that block the fibrinogen binding site of αIIbβ3 not only prevent thrombus formation but also prevent platelet activation, which argues for cooperative signaling of the 2 platelet receptors [42]. As INU1-Fab does not activate platelets in vitro, we speculate that it alters CLEC-2’s conformation, enabling the receptor to interact with a yet-to-be-identified ligand in cerebral veins, which upon binding to CLEC-2, and in concert with αIIbβ3, causes CVT [42] (Figure 2B). Interestingly, we did not observe any signs of intracranial hemorrhage after αIIbβ3 blockade, indicating that this might be a potential therapeutic strategy for the treatment of CVT.
3. Ischemic Stroke
Stroke remains one of the leading causes of disability and death worldwide. Eighty percent to 90% of stroke cases are ischemic, meaning that they are caused by a thrombus that occludes a large vessel, resulting in insufficient supply of the downstream tissue. Consequently, restoration of blood flow is the main therapeutic goal, which can be achieved by thrombectomy or i.v. thrombolysis (using recombinant tissue-type plasminogen activator). However, only a small proportion of patients are eligible to receive these therapies [43]. Moreover, even upon successful removal of the large vessel occlusion, only a fraction of patients benefit [44], underscoring the need for new therapeutic regimens and, hence, a better understanding of underlying pathomechanisms.
Animal models of ischemic stroke have been and still are instrumental in enhancing our understanding of infarct progression following ischemic stroke. Among those, the rodent model of transient middle cerebral artery occlusion (tMCAO), where typically an hour of brain focal ischemia is induced using a commercialized intraluminal monofilament, followed by a 24-hour reperfusion, is widely used [45]. Using this model on Rag1−/− mice, which lack T and B cells, provided the first evidence that T cells contribute to infarct progression after ischemic stroke, as the adoptive transfer of T cells in Rag1−/− mice fully restored infarct volumes [46]. A follow-up study confirmed these results and revealed that the effect of T cells in ischemic stroke is independent of specific T-cell receptors or costimulatory molecules [47]. Interestingly, studies using the permanent middle cerebral artery occlusion (MCAO) model, in which the filament is not removed, revealed that T cells already contribute to neuronal damage under occlusion [48], indicating that the detrimental activity of T cells is not limited to classical I/R injury. In line with these data, a multicenter trial in mice demonstrated smaller infarcts after cortical infarctions in mice that received an antibody blocking the central T-cell integrin α4β1 [49]. The T-cell effect, however, is apparently linked to platelets, as Rag1−/− mice that receive T cells via an adoptive transfer after platelet depletion do not develop full-blown infarcts, indicating that platelets are orchestrating the detrimental effects of T cells [50]. One molecule linking the detrimental effects of platelets and T cells is the immune-receptor CD84, which is expressed on platelets and various immune cells, as mice lacking CD84 either on T cells or on platelets develop smaller infarcts following tMCAO [51].
Platelets have long been suspected of contributing to neuronal damage following ischemic stroke, as they accumulate at sites of cerebral infarctions [52] and are responsible for the initial insult (the occlusion of a large vessel). The common assumption has long been that platelets form aggregates within the microcirculation, preventing perfusion of the cerebral tissue. However, a seminal paper from Kleinschnitz et al. [16] has challenged this concept as it demonstrated that the blockade of αIIbβ3, the central platelet integrin essential for aggregation, has no beneficial effect but, in contrast, results in intracerebral hemorrhages. The detrimental effects of αIIbβ3 blockers in ischemic stroke were confirmed in clinical trials [53,54]. In line with these studies, we recently showed using light-sheet-fluorescence imaging that infarct progression precedes cerebral thrombosis [55], excluding thrombi as a central mechanism in ischemic stroke and underscoring that stroke is a thrombo-inflammatory disease (and not a thrombotic one). Remarkably, the difference in the efficacy of αIIbβ3 blockade is one of the key points that illustrate the differences between immunothrombosis and thrombo-inflammation. Since cerebrovascular thrombo-inflammation is featured by the disturbance of the blood–brain barrier (BBB), we hypothesize that the activity of αIIbβ3 is needed for the sealing of BBB breaches and the prevention of hemorrhagic transformation. In stark contrast, in the context of immunothrombotic CVT, blocking αIIbβ3 was beneficial in an experimental model and not associated with bleeding complications [42].
Nevertheless, platelets are central contributors to infarct progression following ischemic stroke, as many platelet receptors and signaling pathways are involved in stroke development (Table 1 [16,48,51,53,54,[56], [57], [58], [59], [60], [61], [62], [63], [64], [65], [66], [67], [68], [69], [70], [71], [7]; Figure 3). As the final common pathway of platelet activation, integrin activation is of minor importance that raises the question: What platelet effector functions are of relevance instead (Table 2 [[76], [77], [78], [79], [80], [81], [82], [83]]; Figure 3)? Platelet degranulation is clearly a factor, as mice with ablated dense granule secretion (Unc13d−/−) develop smaller infarcts [77], potentially due to reduced platelet activation in the absence of adenosine diphosphate release. Likewise, Nbeal2-/- mice, whose platelets lack α-granules, develop smaller infarcts [76], indicating that among the plethora of factors stored in these granules, some contribute to infarct progression. One critical component has been identified as high-mobility group box 1, which is elevated in patients with stroke, and mice lacking this protein in platelets develop smaller infarcts [84]. High-mobility group box 1 contributes to cerebral damage by promoting the formation of NETs [84]. Likewise, inhibition of NETs by neonatal NET-inhibitory factor [84] or DNase [85] reduces infarct volumes after tMCAO. Interestingly, platelets not only stimulate NET formation but also recruit neutrophils by exposing the neutrophil PSGL-1 ligand P-selectin and by exposing phosphatidylserine (PS) [86]. In a recent study [79], mice with cyclophilin D deficient platelets were investigated. These animals had less neutrophil infiltration and smaller infarct sizes following tMCAO (but not permanent MCAO), which was attributed to the abolished PS exposure in CypD−/− platelets. Of note, however, the lack of the scramblase TMEM16F also abolished platelet PS exposure, but Tmem16f-/- mice displayed unaltered infarct volumes following tMCAO [80]. On the other hand, blocking PS by annexin A1 [81] or lactadherin [82] reduced infarct volumes in experimental stroke models, supporting the role of PS in infarct progression. Besides secretion or PS exposure, receptor shedding is another mode of platelets to modulate inflammation, as CD84 shedding fosters T-cell recruitment into the ischemic brain [51]. A simplified model of platelets as orchestrators of thrombo-inflammation is depicted in Figure 3.
Table 1.
Overview of platelet receptors involved in the pathogenesis of ischemic stroke.
| Receptor/ligand | Model | Intervention | Outcome | Reference |
|---|---|---|---|---|
| αIIbβ3 | tMCAO (M) | Blockade | Unaltered infarct sizes, intracerebral hemorrhages | [16] |
| αIIbβ3 | H | Blockade | No benefits of treatment, higher rate of intracranial hemorrhages | [53,54] |
| β1-integrin | tMCAO (M/R) | Blockade | Bigger infarct volumes and worsened outcome with less angiogenesis and vascular remodeling | [56,57] |
| CD84 | tMCAO (M) | Genetic deficiency | Smaller infarct sizes, better neurologic outcome with less immunocyte extravasation | [51] |
| GPIbα | tMCAO (M/R) | Blockade | Smaller infarct sizes, reduced apoptosis, reduced neuroinflammation, better neurologic outcome without inducing intracerebral hemorrhage | [16,58] |
| GPIbα | tMCAO (M) | Genetic deficiency | Smaller infarct sizes, better neurologic outcome in the absence of the GPIbα ectodomain or in case of defective signaling (phospholipase D1 ablation) | [59,60] |
| GPIbα | pMCAO (M) | Blockade | Smaller infarct sizes, reduced apoptosis, less immunocyte extravasation | [48] |
| GPV | tMCAO (M) | Recombinant protein | Smaller infarct sizes, better neurologic outcome | [61] |
| GPVI | tMCAO (M) | Receptor depletion | Smaller infarct sizes, better neurologic outcome—similar results upon blockade/deficiency of the downstream kinase Syk | [16,62] |
| GPVI | tMCAO (M) | Recombinant protein (competitive inhibition) | Smaller infarct sizes, better neurologic outcome without inducing intracerebral bleeding | [63] |
| GPVI | pMCAO (M) | Receptor depletion | Smaller infarct sizes with reduced immunocyte extravasation | [64] |
| PAR1 | pMCAO (M) tMCAO (R) |
Genetic deficiency RNA silencing |
Smaller infarct sizes associated with decreased plasmin and thrombin activities, better functional outcome | [65,66] |
| PAR4 | tMCAO (M) | Genetic deficiency | Smaller infarct sizes, better neurologic outcome with less platelet/endothelial and leukocyte/endothelial interactions and less BBB leakage | [67] |
| PAR4 | tMCAO (M) | Blockade | Smaller infarct sizes, outcome negatively associated with the platelet-neutrophil aggregate formation | [68] |
| P2Y1 | tMCAO (M/R) | Genetic deficiency Blockade |
Improvement in post-ischemia cognitive impairment with diminished neuroinflammation | [69] |
| P2Y12 | tMCAO (M) | Blockade | Smaller infarct sizes, better neurologic outcome with a better cerebral blood flow | [70] |
| P2Y12 | H | Blockade | Safe and effective for acute stenting upon acute ischemic stroke | [71] |
| VWF | Guinea pig | Blockade | Smaller infarct sizes with better cerebral blood flow, void of intracerebral hemorrhage | [72] |
| VWF | tMCAO (M) | Genetic deficiency | Smaller infarct sizes, better neurologic outcome | [73,74] |
| VWF | tMCAO (M) | Smaller multimers due to rhADAMTS-13 | Smaller infarct sizes, better neurologic outcome without inducing intracranial hemorrhage conversion | [75] |
BBB, blood–brain barrier; GP, glycoprotein; H, human/clinical study; M, mouse; pMCAO, permanent middle cerebral occlusion; R, rat; Syk, spleen tyrosine kinase; tMCAO, transient middle cerebral artery occlusion; VWF, von Willebrand factor.
Figure 3.
A simplified model of platelets as orchestrators of thrombo-inflammation (as seen in acute ischemic stroke). The (post-)ischemic endothelium exposes von Willebrand factor (VWF), allowing platelets to interact with VWF via glycoprotein (GP) Ibα, which is critical for infarct progression. Subsequently, platelets become activated via various signaling pathways, including GPVI, PARs, and ADP receptors, among others. Upon activation, platelets shed CD84, thereby recruiting T cells, expose P-selectin (a ligand for PSGL-1 on neutrophils) or phosphatidylserine (PS) (which promotes not only plasmatic coagulation but also supports NETosis), and activate their integrin receptors. On the one hand, plasmatic coagulation results in more thrombin generation, further activating platelets. On the other hand, thrombin cleaves GPV, and soluble GPV dampens fibrin generation. Activated platelets also secrete their granule content, resulting in the release of second-wave mediators such as ADP (from dense granules) as well as protein factors such as high-mobility group box 1 (HMGB1) (from α-granules) that contribute to the recruitment of neutrophils and trigger NETosis. Ultimately, this all converges in the recruitment of immune cells and the disruption of the blood–brain barrier (BBB), demonstrating that ischemic stroke is a thrombo-inflammatory disease. Corresponding strategies of potential intervention and aftermaths are indicated by thumbs up or down (depending on the outcome in experimental models) for future therapeutic developments. ADP, adenosine diphosphate; EC, endothelial cell; NETosis, NET activation and release; PAR, protease-activated receptor; PLD1, phospholipase D1; Syk, spleen tyrosine kinase.
Table 2.
Overview of platelet effector functions involved in the pathogenesis of ischemic stroke.
| Effector function | Model | Intervention | Outcome | Reference |
|---|---|---|---|---|
| α-granule secretion | tMCAO (M) | Nbeal2−/− | Smaller infarct sizes, better neurologic outcome | [76] |
| δ-granule secretion | tMCAO (M) | Unc13d−/− | Smaller infarct sizes, better neurologic outcome without signs of ICH | [77] |
| Granule secretion | tMCAO (M) | Nbeal2−/−/Unc13d-/- | Smaller infarct sizes, however, more frequent ICH resulting in higher mortality | [78] |
| PS exposure | tMCAO (M) | CypD−/− | Smaller infarct sizes, better neurologic outcome with reduced platelet-neutrophil aggregates and neutrophil recruitment | [79] |
| PS exposure | tMCAO (M) | Tmem16f−/− | Unaltered infarct volumes and neurologic outcome | [80] |
| PS exposure | tMCAO (M) | Blockade with annexin A1 | Smaller infarct sizes, better neurologic outcome with less platelet activation/aggregation and less thrombosis | [81] |
| PS exposure | dMCAO (M) | Blockade with lactadherin | Smaller infarct sizes, better neurologic outcome with preserved vascular and BBB integrity, less neurodegeneration, and less neuroinflammation | [82] |
| Serotonin | tMCAO (M) | 5Htt−/− | Reduced platelet serotonin content did not affect stroke outcomes | [83] |
BBB, blood–brain barrier; dMCAO, distal middle cerebral occlusion; ICH, intracranial hemorrhage; M, mouse; PS, phosphatidylserine; tMCAO, transient middle cerebral artery occlusion.
4. International Society on Thrombosis and Haemostasis 2023 Congress Report
Among advances in fundamental, translational, population, and clinical studies relevant to society, the International Society on Thrombosis and Haemostasis (ISTH) has highlighted the most recent advances regarding CVT- or VITT-relevant immunothrombosis during its 2023 Congress. In addition, several presentations provided new insights into pathomechanisms underlying ischemic stroke, which is a paradigmatic thrombo-inflammatory disease. Here, we highlight selected presentations of the ISTH 2023 Congress regarding cerebral immunothrombosis and thrombo-neuroinflammation.
4.1. ISTH 2023—advances regarding CVT and VITT
CVT represents a considerable fraction of venous thrombotic events in pediatric patients, which have been associated with poor outcomes. Manco-Johnson et al. [87] assessed the current outcomes of CVT in pediatric thrombosis centers. They found that mortality and thromboembolism recurrence have become scarce in pediatric cases of CVT. By contrast, long-term neurologic deficits prevail in these cohorts, including epilepsy, motor disorders, speech, and learning difficulties [87].
As elucidated above, VITT is a very rare but life-threatening adverse complication of adenoviral vector-related vaccines against the SARS-CoV-2 virus, characterized by thrombocytopenia and, in some cases, CVT. Anti-PF4 antibody immunocomplexes are the main trigger of platelet activation in not only VITT but also classical HIT. Wang et al. [88] have generated recombinant anti-PF4 antibodies derived from the sera of patients with VITT and presented their initial characterization at the congress. The recombinant human VITT anti-PF4 immunoglobulin G (IgG) will serve as a pivotal research tool for understanding the pathophysiology of VITT.
The laboratory-based differential diagnosis between VITT and HIT appears to be a challenging task. HIT anti-PF4 antibodies generally last 50 to 80 days after heparin exposure, while VITT anti-PF4 antibodies turn out to be detectable for longer periods of time [89]. Rollin et al. [90] established a competitive enzyme immunoassay with a monoclonal anti-PF4 F(ab’)2 fragment to discriminate between HIT and VITT antibodies in patient samples. Along the same lines, Schönborn et al. [91,92] have developed a set of novel assay prototypes to distinguish the anti-PF4 IgG of patients with VITT from those of patients with HIT. The identification of VITT-specific anti-PF4 IgG further benefits the prospective diagnosis of an overlooked cohort developing anti-PF4 IgG and severe immunothrombosis without the preceding exposure to heparin or vaccination because the type of anti-PF4 IgG in these patients turns out to be predominantly VITT-specific. Moreover, Nazy et al. [93] correlated the susceptibility of cerebral venous sinus thrombosis among patients with VITT with a special subset of anti-PF4 IgG, which binds to specific epitopes on the PF4 tetramer, enabling them to trigger platelet activation in the absence of exogenous PF4.
Nocella et al. [94,95] performed a series of studies using direct samples from patients with VITT. They determined that the appreciable thrombosis in these patients is preceded by PAD4-mediated NET formation and massive leukocyte-platelet interactions [94,95], which underscores that VITT and CVT are immunothrombotic diseases. In accordance with these findings, Wang et al. [96] assessed inflammatory and thrombotic parameters in patients with VITT and observed a correlation between disease severity and hyperinflammation, NETosis, and extensive cell death resulting in lymphocyte loss. Martins-Gonçalves et al. [97] suggested a positive association of NLRP3-driven inflammasome activation in patients with VITT, indicating an inflammatory process that underlies this disorder of immunothrombosis. Lombardi et al. [98] and Pallucci et al. [99] compared the effect of adenovirus-based and messenger RNA–based SARS-CoV-2 vaccines on platelet immune cell interactions and observed more sustained interactions upon messenger RNA–based vaccination, while adenovirus-based vaccines triggered antiviral-like responses resulting in platelet clearance. The authors speculate that more sustained platelet-B cell interactions might result in more efficient vaccination responses. Meanwhile, Keragala et al. [100] performed a pioneering investigation on the fibrinolytic system in patients with VITT. They found that VITT is associated with a remarkable hyperfibrinolytic state in addition to its well-established characteristic thrombosis, thrombocytopenia, and the generation of anti-PF4 IgG, which they attribute to a yet-to-be-identified plasma factor capable of reinforcing tissue-type plasminogen activator–associated plasminogen activation [100].
It has been repeatedly reported by a host of studies that anti-PF4 antibodies are also detectable and tangibly elevated in the plasma among non-VITT cohorts vaccinated by an adenovirus-based vaccine (represented by Guerra et al. [101]). The clinical significance of non-pathogenic anti-PF4 IgG remains obscure. It is speculated that anti-PF4 antibodies are not the only culprit for VITT. This hypothesis is supported by another study presented during the ISTH Congress. Rauova et al. [102] have developed an experimental mouse model based on vaccination with adenovirus-based vaccines to recapitulate the major clinical and pathologic features of VITT. Notably, mice developing VITT-like symptoms had only slightly elevated levels of anti-PF4 antibodies, while a more pronounced increase of circulating antibodies directed against the platelet-derived chemokine NAP2 was observed. The authors speculated that anti-NAP2 antibodies might contribute to the development of VITT.
Zlamal et al. [103] assessed inhibitors of the spleen tyrosine kinase (Syk), which mediates tyrosine phosphorylation downstream of (hem)ITAM receptors like FcγRIIa, with regard to their effect on VITT antibody-mediated platelet activation. In fact, 2 of the 3 tested Syk inhibitors dampened platelet activation [103]. Consequently, the authors suggest Syk inhibition as a potential therapeutic approach, which is in line with studies using a mouse model of CVT [42].
4.2. ISTH 2023—advances regarding pathomechanisms underlying ischemic stroke
In an experimental study, the effects of ambient light and red light exposure were investigated. The authors reported that red light exposure correlates with reduced platelet aggregation, activation, and particularly reduced platelet-dependent NET formation, culminating in a reduction of post-ischemia brain tissue damage [104]. However, we would kindly remind our readers that many of the studies mentioned in the ISTH Congress Report have not been peer-reviewed. In thrombo-inflammatory disease settings, platelets orchestrate immune cell recruitment (eg, neutrophil recruitment) and regulate vascular functions. Mechanistically, new processes of how platelets can regulate thrombo-inflammation were presented during the ISTH 2023 Congress. A new platelet-derived membrane structure called platelet-derived integrin and tetraspanin-enriched tethers (PITTs) was presented [105], which was detected on lung endothelium following pulmonary inflammation and neutrophils interacted with PITTs, indicating a potential role in immune cell recruitment. Of note, fewer PITTs were observed in von Willebrand factor (VWF)–deficient animals. Albeit the authors did not assess the role of PITTs in experimental stroke, it is tempting to speculate that PITTs might be involved in VWF-dependent immune cell recruitment following ischemic stroke, as post-ischemic endothelial cells expose VWF[106], and previous studies have shown that platelet αIIbβ3 can modulate neutrophil activities [107,108].
Another mechanism for how platelets recruit neutrophils could be the secretion of the lipid mediator leukotriene B4 (LTB4, [109]). Hackenbroch et al. [109] presented data from mice lacking the hydrolase Lta4h that is responsible for the last step of LTB4 biosynthesis and reported no alteration in hemostasis or classical platelet assays but reduced neutrophil recruitment in inflammatory disease models with mice lacking platelet-derived LTB4.
The interplay of platelets and neutrophils in the context of ischemic stroke is a focus of Denorme’s research [68,84], who presented his latest study at the ISTH Congress [68,110]. Previous studies revealed that a dimorphism within the major thrombin receptor, protease-activated receptor 4 (PAR4), on platelets accounts for differences in platelet reactivity between races as Black people carry more frequently the more reactive variant PAR4Thr120, while in White individuals, the PAR4Ala120 variant is dominant [111]. In line with the elevated platelet reactivity of the Thr120-variant, this variant was associated with a higher incidence of ischemic stroke and a worsened outcome [68,110]. To explore the underlying mechanisms, the authors capitalized on humanized mice expressing either hPAR4Thr120 or hPAR4Ala120. The hPAR4Thr120 mice show worsened post-stroke outcomes, where significant thrombo-inflammation metrics are engaged, including platelet-neutrophil interactions and NETs. Notably, these post-stroke phenotypes seen in hPAR4Thr120 mice are unresponsive to the mainstay antiplatelet drugs such as ticagrelor (P2Y12 antagonist) and aspirin (TxA2 synthesis inhibitor). Instead, post-stroke outcomes in hPAR4Thr120 mice are considerably improved following the therapeutic strategy of blocking platelet-neutrophil interactions with an anti-P-selection antibody. These novel experimental findings highlight the fundamental role of thrombo-inflammation in the pathophysiology of cerebral I/R injuries and point toward novel therapeutic avenues.
As elucidated above, we favor a model in which the early events of hemostasis (ie, platelet adhesion and activation) are key players mediating proinflammatory signaling pathways following ischemic stroke. In contrast, classical platelet aggregation is not involved in these thrombo-inflammatory processes but may instead help prevent inflammatory hemorrhagic conversion. In line with this concept, Janus-Bell et al. [112] presented a study using platelet-specific deficiency (using the PF4-Cre system) of either β1- and/or β3-integrins. Interestingly, only mice whose platelets lacked all integrins displayed brain hemorrhages 6 hours after transient MCAO, indicating that the 2 β1- and β3-integrins can, in part, compensate for one another in maintaining vascular integrity following experimental stroke.
Once the BBB is disturbed, platelets could leave the vasculature, reach the parenchyma, and interact with cells of the neurovascular interface they would usually not encounter. Bourne et al. [113] reported that platelets can be found interacting with microglia following photothrombosis-induced stroke. As platelets modulate the inflammatory profile of microglia in vitro, the authors speculate that these interactions modulate post-stroke neuroinflammation, albeit it remains to be determined how frequently these interactions occur.
5. Future Directions
The last decade has revealed that platelets orchestrate far more than hemostasis and thrombosis; they are versatile effectors cells in a wide variety of (patho-)physiological processes. While thrombosis and inflammation were long considered 2 separate (patho-)physiological processes, the concept of thrombo-inflammation recognizes that they are not only closely intertwined but often also interdependent. Platelets have a key role in this concept as central orchestrators of immune cell trafficking and activation, vascular barrier function, and organ integrity. Correct concepts of disease progression and knowledge of the detrimental factors will be essential, as it appears likely that molecules critically involved in thrombo-inflammation may be less relevant in immunothrombosis and vice versa. The advent of advanced imaging techniques and the prevalence of high-throughput data science will certainly uncover further roles of platelets and deepen our understanding of the underlying mechanisms providing new targets for therapeutic interventions.
Acknowledgments
We thank Dr Vanessa Göb for proofreading this review.
Funding
The authors’ research was supported by the Collaborative Research Center/Transregio 240 (CRC/TR 240, project number 374031971) and the CRC 1525 (project number 453989101) of the Deutsche Forschungsgemeinschaft (German Research Foundation) and the Rudolf Virchow Center.
Author contributions
L.L. and D.S. performed the literature review and wrote and revised the manuscript.
Relationship disclosure
There are no competing interests to disclose.
Footnotes
Handling Editor: Dr Neil Zakai
References
- 1.Stoll G., Nieswandt B. Thrombo-inflammation in acute ischaemic stroke – implications for treatment. Nat Rev Neurol. 2019;15:473–481. doi: 10.1038/s41582-019-0221-1. [DOI] [PubMed] [Google Scholar]
- 2.Guo L., Rondina M.T. The era of thromboinflammation: platelets are dynamic sensors and effector cells during infectious diseases. Front Immunol. 2019;10:2204. doi: 10.3389/fimmu.2019.02204. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.van der Meijden P.E.J., Heemskerk J.W.M. Platelet biology and functions: new concepts and clinical perspectives. Nat Rev Cardiol. 2019;16:166–179. doi: 10.1038/s41569-018-0110-0. [DOI] [PubMed] [Google Scholar]
- 4.Uhrin P., Zaujec J., Breuss J.M., Olcaydu D., Chrenek P., Stockinger H., et al. Novel function for blood platelets and podoplanin in developmental separation of blood and lymphatic circulation. Blood. 2010;115:3997–4005. doi: 10.1182/blood-2009-04-216069. [DOI] [PubMed] [Google Scholar]
- 5.Margraf A., Nussbaum C., Sperandio M. Ontogeny of platelet function. Blood Adv. 2019;3:692–703. doi: 10.1182/bloodadvances.2018024372. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Hoover C., Kondo Y., Shao B., McDaniel M.J., Lee R., McGee S., et al. Heightened activation of embryonic megakaryocytes causes aneurysms in the developing brain of mice lacking podoplanin. Blood. 2021;137:2756–2769. doi: 10.1182/blood.2020010310. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Gupta S., Konradt C., Corken A., Ware J., Nieswandt B., Di Paola J., et al. Hemostasis vs. homeostasis: platelets are essential for preserving vascular barrier function in the absence of injury or inflammation. Proc Natl Acad Sci U S A. 2020;117:24316–24325. doi: 10.1073/pnas.2007642117. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Ho-Tin-Noé B., Boulaftali Y., Camerer E. Platelets and vascular integrity: how platelets prevent bleeding in inflammation. Blood. 2018;131:277–288. doi: 10.1182/blood-2017-06-742676. [DOI] [PubMed] [Google Scholar]
- 9.Chaudhary P.K., Kim S., Kim S. An insight into recent advances on platelet function in health and disease. Int J Mol Sci. 2022;23:6022. doi: 10.3390/ijms23116022. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Engelmann B., Massberg S. Thrombosis as an intravascular effector of innate immunity. Nat Rev Immunol. 2013;13:34–45. doi: 10.1038/nri3345. [DOI] [PubMed] [Google Scholar]
- 11.Bonaventura A., Vecchié A., Dagna L., Martinod K., Dixon D.L., Van Tassell B.W., et al. Endothelial dysfunction and immunothrombosis as key pathogenic mechanisms in COVID-19. Nat Rev Immunol. 2021;21:319–329. doi: 10.1038/s41577-021-00536-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Zhang H., Goswami J., Varley P., van der Windt D.J., Ren J., Loughran P., et al. Hepatic surgical stress promotes systemic immunothrombosis that results in distant organ injury. Front Immunol. 2020;11:987. doi: 10.3389/fimmu.2020.00987. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Tanguay J.F., Geoffroy P., Sirois M.G., Libersan D., Kumar A., Schaub R.G., et al. Prevention of in-stent restenosis via reduction of thrombo-inflammatory reactions with recombinant P-selectin glycoprotein ligand-1. Thromb Haemost. 2004;91:1186–1193. doi: 10.1160/TH03-11-0701. [DOI] [PubMed] [Google Scholar]
- 14.Wang J.S., Yen H.L., Yang C.M. Warm-up exercise suppresses platelet-eosinophil/neutrophil aggregation and platelet-promoted release of eosinophil/neutrophil oxidant products enhanced by severe exercise in men. Thromb Haemost. 2006;95:490–498. doi: 10.1160/TH05-09-0646. [DOI] [PubMed] [Google Scholar]
- 15.Wang J.S., Lin H.Y., Cheng M.L., Wong M.K. Chronic intermittent hypoxia modulates eosinophil- and neutrophil-platelet aggregation and inflammatory cytokine secretion caused by strenuous exercise in men. J Appl Physiol (1985) 2007;103:305–314. doi: 10.1152/japplphysiol.00226.2007. [DOI] [PubMed] [Google Scholar]
- 16.Kleinschnitz C., Pozgajova M., Pham M., Bendszus M., Nieswandt B., Stoll G. Targeting platelets in acute experimental stroke: impact of glycoprotein Ib, VI, and IIb/IIIa blockade on infarct size, functional outcome, and intracranial bleeding. Circulation. 2007;115:2323–2330. doi: 10.1161/CIRCULATIONAHA.107.691279. [DOI] [PubMed] [Google Scholar]
- 17.Kleinschnitz C., Stoll G., Bendszus M., Schuh K., Pauer H.U., Burfeind P., et al. Targeting coagulation factor XII provides protection from pathological thrombosis in cerebral ischemia without interfering with hemostasis. J Exp Med. 2006;203:513–518. doi: 10.1084/jem.20052458. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Nieswandt B., Kleinschnitz C., Stoll G. Ischaemic stroke: a thrombo-inflammatory disease? J Physiol. 2011;589:4115–4123. doi: 10.1113/jphysiol.2011.212886. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Renné T., Pozgajová M., Grüner S., Schuh K., Pauer H.U., Burfeind P., et al. Defective thrombus formation in mice lacking coagulation factor XII. J Exp Med. 2005;202:271–281. doi: 10.1084/jem.20050664. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Jackson S.P., Darbousset R., Schoenwaelder S.M. Thromboinflammation: challenges of therapeutically targeting coagulation and other host defense mechanisms. Blood. 2019;133:906–918. doi: 10.1182/blood-2018-11-882993. [DOI] [PubMed] [Google Scholar]
- 21.Vazquez-Garza E., Jerjes-Sanchez C., Navarrete A., Joya-Harrison J., Rodriguez D. Venous thromboembolism: thrombosis, inflammation, and immunothrombosis for clinicians. J Thromb Thrombolysis. 2017;44:377–385. doi: 10.1007/s11239-017-1528-7. [DOI] [PubMed] [Google Scholar]
- 22.Kimball A.S., Obi A.T., Diaz J.A., Henke P.K. The emerging role of NETs in venous thrombosis and immunothrombosis. Front Immunol. 2016;7:236. doi: 10.3389/fimmu.2016.00236. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Nayak L., Sweet D.R., Thomas A., Lapping S.D., Kalikasingh K., Madera A., et al. A targetable pathway in neutrophils mitigates both arterial and venous thrombosis. Sci Transl Med. 2022;14 doi: 10.1126/scitranslmed.abj7465. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Martinelli I., Passamonti S.M., Rossi E., De Stefano V. Cerebral sinus-venous thrombosis. Intern Emerg Med. 2012;7(Suppl 3):S221–S225. doi: 10.1007/s11739-012-0806-9. [DOI] [PubMed] [Google Scholar]
- 25.Silvis S.M., de Sousa D.A., Ferro J.M., Coutinho J.M. Cerebral venous thrombosis. Nat Rev Neurol. 2017;13:555–565. doi: 10.1038/nrneurol.2017.104. [DOI] [PubMed] [Google Scholar]
- 26.Ferro J.M., Canhão P., Aguiar de Sousa D. Cerebral venous thrombosis. Presse Med. 2016;45:e429–e450. doi: 10.1016/j.lpm.2016.10.007. [DOI] [PubMed] [Google Scholar]
- 27.Ferro J.M., Bousser M.G., Canhão P., Coutinho J.M., Crassard I., Dentali F., et al. European Stroke Organization guideline for the diagnosis and treatment of cerebral venous thrombosis - endorsed by the European Academy of Neurology. Eur J Neurol. 2017;24:1203–1213. doi: 10.1111/ene.13381. [DOI] [PubMed] [Google Scholar]
- 28.Yeung J., Li W., Holinstat M. Platelet signaling and disease: targeted therapy for thrombosis and other related diseases. Pharmacol Rev. 2018;70:526–548. doi: 10.1124/pr.117.014530. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Chirinos J.A., Heresi G.A., Velasquez H., Jy W., Jimenez J.J., Ahn E., et al. Elevation of endothelial microparticles, platelets, and leukocyte activation in patients with venous thromboembolism. J Am Coll Cardiol. 2005;45:1467–1471. doi: 10.1016/j.jacc.2004.12.075. [DOI] [PubMed] [Google Scholar]
- 30.Heestermans M., Poenou G., Duchez A.C., Hamzeh-Cognasse H., Bertoletti L., Cognasse F. Immunothrombosis and the role of platelets in venous thromboembolic diseases. Int J Mol Sci. 2022;23 doi: 10.3390/ijms232113176. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Tarantino E., Amadio P., Squellerio I., Porro B., Sandrini L., Turnu L., et al. Role of thromboxane-dependent platelet activation in venous thrombosis: aspirin effects in mouse model. Pharmacol Res. 2016;107:415–425. doi: 10.1016/j.phrs.2016.04.001. [DOI] [PubMed] [Google Scholar]
- 32.Mistry D.A., Chandratreya A., Lee P.Y.F. A systematic review on the use of aspirin in the prevention of deep vein thrombosis in major elective lower limb orthopedic surgery: an update from the past 3 years. Surg J (N Y) 2017;3:e191–e196. doi: 10.1055/s-0037-1615817. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Bourrienne M.C., Gay J., Mazighi M., Ajzenberg N. State of the art in cerebral venous sinus thrombosis animal models. J Thromb Haemost. 2022;20:2187–2196. doi: 10.1111/jth.15816. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Jin J., Qiao S., Liu J., Li W., Wang F., Gao X., et al. Neutrophil extracellular traps promote thrombogenicity in cerebral venous sinus thrombosis. Cell Biosci. 2022;12:114. doi: 10.1186/s13578-022-00845-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Brill A., Fuchs T.A., Savchenko A.S., Thomas G.M., Martinod K., De Meyer S.F., et al. Neutrophil extracellular traps promote deep vein thrombosis in mice. J Thromb Haemost. 2012;10:136–144. doi: 10.1111/j.1538-7836.2011.04544.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.von Brühl M.L., Stark K., Steinhart A., Chandraratne S., Konrad I., Lorenz M., et al. Monocytes, neutrophils, and platelets cooperate to initiate and propagate venous thrombosis in mice in vivo. J Exp Med. 2012;209:819–835. doi: 10.1084/jem.20112322. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Siegler J.E., Cardona P., Arenillas J.F., Talavera B., Guillen A.N., Chavarría-Miranda A., et al. Cerebrovascular events and outcomes in hospitalized patients with COVID-19: the SVIN COVID-19 multinational registry. Int J Stroke. 2021;16:437–447. doi: 10.1177/1747493020959216. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Ostovan V.R., Foroughi R., Rostami M., Almasi-Dooghaee M., Esmaili M., Bidaki A.A., et al. Cerebral venous sinus thrombosis associated with COVID-19: a case series and literature review. J Neurol. 2021;268:3549–3560. doi: 10.1007/s00415-021-10450-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Cines D.B., Greinacher A. Vaccine-induced immune thrombotic thrombocytopenia. Blood. 2023;141:1659–1665. doi: 10.1182/blood.2022017696. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Wittstock M., Walter U., Volmer E., Storch A., Weber M.A., Großmann A. Cerebral venous sinus thrombosis after adenovirus-vectored COVID-19 vaccination: review of the neurological-neuroradiological procedure. Neuroradiology. 2022;64:865–874. doi: 10.1007/s00234-022-02914-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Huynh A., Arnold D.M., Ivetic N., Clare R., Hadzi-Tosev M., Liu Y., et al. Antibodies against platelet factor 4 and the risk of cerebral venous sinus thrombosis in patients with vaccine-induced immune thrombotic thrombocytopenia. J Thromb Haemost. 2023;21:2833–2843. doi: 10.1016/j.jtha.2023.06.026. [DOI] [PubMed] [Google Scholar]
- 42.Stegner D., Göb V., Krenzlin V., Beck S., Hemmen K., Schuhmann M.K., et al. Foudroyant cerebral venous (sinus) thrombosis triggered through CLEC-2 and GPIIb/IIIa dependent platelet activation. Nat Cardiovasc Res. 2022;1:132–141. doi: 10.1038/s44161-021-00017-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Saini V., Guada L., Yavagal D.R. Global epidemiology of stroke and access to acute ischemic stroke interventions. Neurology. 2021;97(Suppl 2):S6–S16. doi: 10.1212/WNL.0000000000012781. [DOI] [PubMed] [Google Scholar]
- 44.Church E.W., Gundersen A., Glantz M.J., Simon S.D. Number needed to treat for stroke thrombectomy based on a systematic review and meta-analysis. Clin Neurol Neurosurg. 2017;156:83–88. doi: 10.1016/j.clineuro.2017.03.005. [DOI] [PubMed] [Google Scholar]
- 45.Braeuninger S., Kleinschnitz C., Nieswandt B., Stoll G. Focal cerebral ischemia. Methods Mol Biol. 2012;788:29–42. doi: 10.1007/978-1-61779-307-3_3. [DOI] [PubMed] [Google Scholar]
- 46.Yilmaz G., Arumugam T.V., Stokes K.Y., Granger D.N. Role of T lymphocytes and interferon-gamma in ischemic stroke. Circulation. 2006;113:2105–2112. doi: 10.1161/CIRCULATIONAHA.105.593046. [DOI] [PubMed] [Google Scholar]
- 47.Kleinschnitz C., Schwab N., Kraft P., Hagedorn I., Dreykluft A., Schwarz T., et al. Early detrimental T-cell effects in experimental cerebral ischemia are neither related to adaptive immunity nor thrombus formation. Blood. 2010;115:3835–3842. doi: 10.1182/blood-2009-10-249078. [DOI] [PubMed] [Google Scholar]
- 48.Schuhmann M.K., Bieber M., Franke M., Kollikowski A.M., Stegner D., Heinze K.G., et al. Platelets and lymphocytes drive progressive penumbral tissue loss during middle cerebral artery occlusion in mice. J Neuroinflammation. 2021;18:46. doi: 10.1186/s12974-021-02095-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Llovera G., Hofmann K., Roth S., Salas-Pérdomo A., Ferrer-Ferrer M., Perego C., et al. Results of a preclinical randomized controlled multicenter trial (pRCT): anti-CD49d treatment for acute brain ischemia. Sci Transl Med. 2015;7 doi: 10.1126/scitranslmed.aaa9853. [DOI] [PubMed] [Google Scholar]
- 50.Kleinschnitz C., Kraft P., Dreykluft A., Hagedorn I., Göbel K., Schuhmann M.K., et al. Regulatory T cells are strong promoters of acute ischemic stroke in mice by inducing dysfunction of the cerebral microvasculature. Blood. 2013;121:679–691. doi: 10.1182/blood-2012-04-426734. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Schuhmann M.K., Stoll G., Bieber M., Vögtle T., Hofmann S., Klaus V., et al. CD84 links T cell and platelet activity in cerebral thrombo-inflammation in acute stroke. Circ Res. 2020;127:1023–1035. doi: 10.1161/CIRCRESAHA.120.316655. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Del Zoppo G.J., Copeland B.R., Harker L.A., Waltz T.A., Zyroff J., Hanson S.R., et al. Experimental acute thrombotic stroke in baboons. Stroke. 1986;17:1254–1265. doi: 10.1161/01.str.17.6.1254. [DOI] [PubMed] [Google Scholar]
- 53.Adams H.P., Jr., Effron M.B., Torner J., Dávalos A., Frayne J., Teal P., et al. Emergency administration of abciximab for treatment of patients with acute ischemic stroke: results of an international phase III trial: abciximab in Emergency Treatment of Stroke Trial (AbESTT-II) Stroke. 2008;39:87–99. doi: 10.1161/STROKEAHA.106.476648. [DOI] [PubMed] [Google Scholar]
- 54.Kellert L., Hametner C., Rohde S., Bendszus M., Hacke W., Ringleb P., et al. Endovascular stroke therapy: tirofiban is associated with risk of fatal intracerebral hemorrhage and poor outcome. Stroke. 2013;44:1453–1455. doi: 10.1161/STROKEAHA.111.000502. [DOI] [PubMed] [Google Scholar]
- 55.Göb V., Voll M.G., Zimmermann L., Hemmen K., Stoll G., Nieswandt B., et al. Infarct growth precedes cerebral thrombosis following experimental stroke in mice. Sci Rep. 2021;11 doi: 10.1038/s41598-021-02360-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56.Lathia J.D., Chigurupati S., Thundyil J., Selvaraj P.K., Mughal M.R., Woodruff T.M., et al. Pivotal role for beta-1 integrin in neurovascular remodelling after ischemic stroke. Exp Neurol. 2010;221:107–114. doi: 10.1016/j.expneurol.2009.10.007. [DOI] [PubMed] [Google Scholar]
- 57.Li X.L., Guo Y., Zhang Y.S., Zhao Y., Zhang L. Effects of integrin β1 on behavior and neurovascular regeneration in rats with cerebral ischemia-reperfusion injury. Eur Rev Med Pharmacol Sci. 2019;23:3487–3494. doi: 10.26355/eurrev_201904_17714. [DOI] [PubMed] [Google Scholar]
- 58.Luo S.Y., Li R., Le Z.Y., Li Q.L., Chen Z.W. Anfibatide protects against rat cerebral ischemia/reperfusion injury via TLR4/JNK/caspase-3 pathway. Eur J Pharmacol. 2017;807:127–137. doi: 10.1016/j.ejphar.2017.04.002. [DOI] [PubMed] [Google Scholar]
- 59.De Meyer S.F., Schwarz T., Schatzberg D., Wagner D.D. Platelet glycoprotein Ibα is an important mediator of ischemic stroke in mice. Exp Transl Stroke Med. 2011;3:9. doi: 10.1186/2040-7378-3-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.Elvers M., Stegner D., Hagedorn I., Kleinschnitz C., Braun A., Kuijpers M.E., et al. Impaired alpha(IIb)beta(3) integrin activation and shear-dependent thrombus formation in mice lacking phospholipase D1. Sci Signal. 2010;3:ra1. doi: 10.1126/scisignal.2000551. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Beck S., Öftering P., Li R., Hemmen K., Nagy M., Wang Y., et al. Platelet glycoprotein V spatio-temporally controls fibrin formation. Nat Cardiovasc Res. 2023;2:368–382. doi: 10.1038/s44161-023-00254-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.van Eeuwijk J.M., Stegner D., Lamb D.J., Kraft P., Beck S., Thielmann I., et al. The novel oral Syk inhibitor, Bl1002494, protects mice from arterial thrombosis and thromboinflammatory brain infarction. Arterioscler Thromb Vasc Biol. 2016;36:1247–1253. doi: 10.1161/ATVBAHA.115.306883. [DOI] [PubMed] [Google Scholar]
- 63.Goebel S., Li Z., Vogelmann J., Holthoff H.P., Degen H., Hermann D.M., et al. The GPVI-Fc fusion protein Revacept improves cerebral infarct volume and functional outcome in stroke. PloS One. 2013;8 doi: 10.1371/journal.pone.0066960. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.Bieber M., Schuhmann M.K., Kollikowski A.M., Stegner D., Nieswandt B., Pham M., et al. Targeting platelet glycoprotein VI attenuates progressive ischemic brain damage before recanalization during middle cerebral artery occlusion in mice. Exp Neurol. 2021;344 doi: 10.1016/j.expneurol.2021.113804. [DOI] [PubMed] [Google Scholar]
- 65.Shavit-Stein E., Mindel E., Gofrit S.G., Chapman J., Maggio N. Ischemic stroke in PAR1 KO mice: decreased brain plasmin and thrombin activity along with decreased infarct volume. PloS One. 2021;16 doi: 10.1371/journal.pone.0248431. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66.Rajput P.S., Lyden P.D., Chen B., Lamb J.A., Pereira B., Lamb A., et al. Protease activated receptor-1 mediates cytotoxicity during ischemia using in vivo and in vitro models. Neuroscience. 2014;281:229–240. doi: 10.1016/j.neuroscience.2014.09.038. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67.Mao Y., Zhang M., Tuma R.F., Kunapuli S.P. Deficiency of PAR4 attenuates cerebral ischemia/reperfusion injury in mice. J Cereb Blood Flow Metab. 2010;30:1044–1052. doi: 10.1038/jcbfm.2009.283. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Denorme F., Armstrong N.D., Stoller M.L., Portier I., Tugolukova E.A., Tanner R.M., et al. The predominant PAR4 variant in individuals of African ancestry worsens murine and human stroke outcomes. J Clin Invest. 2023;133 doi: 10.1172/JCI169608. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Chin Y., Kishi M., Sekino M., Nakajo F., Abe Y., Terazono Y., et al. Involvement of glial P2Y₁ receptors in cognitive deficit after focal cerebral stroke in a rodent model. J Neuroinflammation. 2013;10:95. doi: 10.1186/1742-2094-10-95. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Yamauchi K., Imai T., Shimazawa M., Iwama T., Hara H. Effects of ticagrelor in a mouse model of ischemic stroke. Sci Rep. 2017;7 doi: 10.1038/s41598-017-12205-w. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 71.Elhorany M., Lenck S., Degos V., Sourour N.A., Frasca Polara G., Shotar E., et al. Cangrelor and stenting in acute ischemic stroke: monocentric case series. Clin Neuroradiol. 2021;31:439–448. doi: 10.1007/s00062-020-00907-0. [DOI] [PubMed] [Google Scholar]
- 72.Momi S., Tantucci M., Van Roy M., Ulrichts H., Ricci G., Gresele P. Reperfusion of cerebral artery thrombosis by the GPIb-VWF blockade with the Nanobody ALX-0081 reduces brain infarct size in guinea pigs. Blood. 2013;121:5088–5097. doi: 10.1182/blood-2012-11-464545. [DOI] [PubMed] [Google Scholar]
- 73.Kleinschnitz C., De Meyer S.F., Schwarz T., Austinat M., Vanhoorelbeke K., Nieswandt B., et al. Deficiency of von Willebrand factor protects mice from ischemic stroke. Blood. 2009;113:3600–3603. doi: 10.1182/blood-2008-09-180695. [DOI] [PubMed] [Google Scholar]
- 74.Verhenne S., Denorme F., Libbrecht S., Vandenbulcke A., Pareyn I., Deckmyn H., et al. Platelet-derived VWF is not essential for normal thrombosis and hemostasis but fosters ischemic stroke injury in mice. Blood. 2015;126:1715–1722. doi: 10.1182/blood-2015-03-632901. [DOI] [PubMed] [Google Scholar]
- 75.Zhao B.Q., Chauhan A.K., Canault M., Patten I.S., Yang J.J., Dockal M., et al. von Willebrand factor-cleaving protease ADAMTS13 reduces ischemic brain injury in experimental stroke. Blood. 2009;114:3329–3334. doi: 10.1182/blood-2009-03-213264. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Deppermann C., Cherpokova D., Nurden P., Schulz J.N., Thielmann I., Kraft P., et al. Gray platelet syndrome and defective thrombo-inflammation in Nbeal2-deficient mice. J Clin Invest. 2013;123:3331–3342. doi: 10.1172/JCI69210. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77.Stegner D., Deppermann C., Kraft P., Morowski M., Kleinschnitz C., Stoll G., et al. Munc13-4-mediated secretion is essential for infarct progression but not intracranial hemostasis in acute stroke. J Thromb Haemost. 2013;11:1430–1433. doi: 10.1111/jth.12293. [DOI] [PubMed] [Google Scholar]
- 78.Deppermann C., Kraft P., Volz J., Schuhmann M.K., Beck S., Wolf K., et al. Platelet secretion is crucial to prevent bleeding in the ischemic brain but not in the inflamed skin or lung in mice. Blood. 2017;129:1702–1706. doi: 10.1182/blood-2016-12-750711. [DOI] [PubMed] [Google Scholar]
- 79.Denorme F., Manne B.K., Portier I., Eustes A.S., Kosaka Y., Kile B.T., et al. Platelet necrosis mediates ischemic stroke outcome in mice. Blood. 2020;135:429–440. doi: 10.1182/blood.2019002124. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80.Baig A.A., Haining E.J., Geuss E., Beck S., Swieringa F., Wanitchakool P., et al. TMEM16F-mediated platelet membrane phospholipid scrambling is critical for hemostasis and thrombosis but not thromboinflammation in mice-brief report. Arterioscler Thromb Vasc Biol. 2016;36:2152–2157. doi: 10.1161/ATVBAHA.116.307727. [DOI] [PubMed] [Google Scholar]
- 81.Senchenkova E.Y., Ansari J., Becker F., Vital S.A., Al-Yafeai Z., Sparkenbaugh E.M., et al. Novel role for the AnxA1-Fpr2/ALX signaling axis as a key regulator of platelet function to promote resolution of inflammation. Circulation. 2019;140:319–335. doi: 10.1161/CIRCULATIONAHA.118.039345. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 82.Chen Z., Chopp M., Zacharek A., Li W., Venkat P., Wang F., et al. Brain-derived microparticles (BDMPs) contribute to neuroinflammation and lactadherin reduces BDMP induced neuroinflammation and improves outcome after stroke. Front Immunol. 2019;10:2747. doi: 10.3389/fimmu.2019.02747. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 83.Wolf K., Braun A., Haining E.J., Tseng Y.L., Kraft P., Schuhmann M.K., et al. Partially defective store operated calcium entry and Hem(ITAM) signaling in platelets of serotonin transporter deficient mice. PLoS One. 2016;11 doi: 10.1371/journal.pone.0147664. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 84.Denorme F., Portier I., Rustad J.L., Cody M.J., de Araujo C.V., Hoki C., et al. Neutrophil extracellular traps regulate ischemic stroke brain injury. J Clin Invest. 2022;132 doi: 10.1172/JCI154225. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 85.De Meyer S.F., Stoll G., Wagner D.D., Kleinschnitz C. von Willebrand factor: an emerging target in stroke therapy. Stroke. 2012;43:599–606. doi: 10.1161/STROKEAHA.111.628867. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 86.Denorme F., Rustad J.L., Campbell R.A. Brothers in arms: platelets and neutrophils in ischemic stroke. Curr Opin Hematol. 2021;28:301–307. doi: 10.1097/MOH.0000000000000665. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 87.Manco-Johnson M., Thompson V., Thornhill D., Nederveld C., Smith J., Smith T., et al. Outcomes of cerebrosinovenous thrombosis in infants and children [abstract] Res Pract Thromb Haemost. 2023;7 [Google Scholar]
- 88.Wang J., van der Neut Kolfschoten M., Rutten L., Hill B., Tan C., Bos R., et al. Recombinant human anti-PF4 IgGs regenerated from VITT sera activate platelets and endothelial cells [abstract] Res Pract Thromb Haemost. 2023;7 [Google Scholar]
- 89.Hack M., Zhang Y., Clare R., Ivetic N., Bhakta H., Lucier K., et al. Longitudinal study on the persistence of anti-platelet factor 4 antibodies in vaccine-induced immune thrombotic thrombocytopenia after 14 months [abstract] Res Pract Thromb Haemost. 2023;7 [Google Scholar]
- 90.Rollin J., Vayne C., Clare R., Atsouawe M., Cordonnier C., Lemoine S., et al. Usefulness of 1E12, a monoclonal anti-platelet factor 4 antibody to improve diagnosis of vaccine-induced immune thrombotic thrombocytopenia [abstract] Res Pract Thromb Haemost. 2023;7 doi: 10.1016/j.jtha.2024.05.005. [DOI] [PubMed] [Google Scholar]
- 91.Schönborn L., Esteban O., Wesche J., Dobosz P., Broto M., Puig S.R., et al. Heparin- and vaccine-independent anti-platelet factor 4 immunothrombosis. SSRN. 2023 doi: 10.2139/ssrn.4519530. [DOI] [Google Scholar]
- 92.Schönborn L., Esteban O., Wesche J., Dobosz P., Broto M., Rovira S., et al. Anti-platelet factor 4 induced immunothrombosis independent of heparin or vaccination [abstract] Res Pract Thromb Haemost. 2023;7 [Google Scholar]
- 93.Nazy I., Huynh A., Arnold D. Distinct antibody groups in patients with vaccine-induced immune thrombotic thrombocytopenia (VITT) and their clinical implications [abstract] Res Pract Thromb Haemost. 2023;7 [Google Scholar]
- 94.Carnevale R., Leopizzi M., Dominici M., d'Amati G., Bartimoccia S., Nocella C., et al. PAD4-Induced NETosis via cathepsin G-mediated platelet-neutrophil interaction in ChAdOx1 vaccine-induced thrombosis—brief report. Arterioscler Thromb Vasc Biol. 2023;43:e396–e403. doi: 10.1161/ATVBAHA.123.319522. [DOI] [PubMed] [Google Scholar]
- 95.Nocella C., Carnevale R., Leopizzi M., Dominici M., d'Amati G., Bartimoccia S., et al. PAD4-mediated NETosis in ChAdOx1 vaccine-induced thrombosis [abstract] Res Pract Thromb Haemost. 2023;7 doi: 10.1161/ATVBAHA.123.319522. [DOI] [PubMed] [Google Scholar]
- 96.Wang G., Abrams S., Shaw R., Toh C., Nicolson P., Montague S., et al. Hyperinflammation and extensive cell death occurred in VITT and indicate severity and poor outcomes [abstract] Res Pract Thromb Haemost. 2023;7 [Google Scholar]
- 97.Martins-Gonçalves R., Mendes-De-Almeida D.P., Sacramento C.Q., Vicente Rozini S., Bokel J., Vitiello Teixeira G., et al. Inflammasome activation in vaccine-induced thrombotic thrombocytopenia (VITT) after immunization with adenovirus-based SARS-CoV-2 vaccines [abstract] Res Pract Thromb Haemost. 2023;7 [Google Scholar]
- 98.Lombardi L., Maiorca F., Marrapodi R., Sabetta A., Scafa N., Pallucci D., et al. Distinct platelet crosstalk with adaptive and innate immune cells after adenoviral and mRNA vaccination against SARS-CoV-2. J Thromb Haemost. 2023;21:1636–1649. doi: 10.1016/j.jtha.2023.03.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 99.Pallucci D., Lombardi L., Maiorca F., Marrapodi R., Sabetta A., Scafa N., et al. Platelet-B cell interactions modulate the antibody response to adenoviral and mRNA vaccines against SARS-CoV-2 [abstract] Res Pract Thromb Haemost. 2023;7 [Google Scholar]
- 100.Keragala C., McFadyen J., Ho H., McCutcheon F., Liu Z., Stevens H., et al. Vaccine-induced immune thrombotic thrombocytopenia produces a marked hyperfibrinolytic state and generates a plasma cofactor that potentiates tPA-mediated plasminogen activation [abstract] Res Pract Thromb Haemost. 2023;7 [Google Scholar]
- 101.Guerra J., Penteado R., De Campos Guerra J., de Aranda V., Rocco Villarinho A., Oliveira dos Santos A., et al. Change in the pattern of HIT(LIA)-negative patients after immunization with AstraZeneca vaccine in a Brazilian population [abstract] Res Pract Thromb Haemost. 2023;7 [Google Scholar]
- 102.Rauova L., Oberg J., Field C., Levine N., Gollomp K., Arepally G., et al. Chadox1 exposure-induced neutrophil-activating peptide 2 (NAP2) antibodies: murine-based insights into the pathogenesis of thrombosis with thrombocytopenia syndrome (TTS) [abstract] Res Pract Thromb Haemost. 2023;7 [Google Scholar]
- 103.Zlamal J., Singh A., Uzun G., Weich K., Althaus K., Bakchoul T. Impact of spleen tyrosine kinase inhibition on vaccine-induced thrombotic thrombocytopenia antibody-induced procoagulant platelet and thrombus formation [abstract] Res Pract Thromb Haemost. 2023;7 [Google Scholar]
- 104.Andraska E., Denorme F., Kalenmeier C., Arivudainambi A., Dyer M., Rosengart M., et al. The spectrum of light exposure modulates platelet function [abstract] Res Pract Thromb Haemost. 2023;7 [Google Scholar]
- 105.Johnson D., Kusch C., Burkard P., Meub M., Nurden P., Gross C., et al. Platelet-derived integrin and tetraspanin-enriched tethers (pitts) orchestrate neutrophil recruitment and drive pulmonary thrombo-inflammation [abstract] Res Pract Thromb Haemost. 2023;7 [Google Scholar]
- 106.Pinsky D.J., Naka Y., Liao H., Oz M.C., Wagner D.D., Mayadas T.N., et al. Hypoxia-induced exocytosis of endothelial cell Weibel-Palade bodies. A mechanism for rapid neutrophil recruitment after cardiac preservation. J Clin Invest. 1996;97:493–500. doi: 10.1172/JCI118440. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 107.Constantinescu-Bercu A., Grassi L., Frontini M., Salles-Crawley, Woollard K., Crawley J.T. Activated αIIbβ3 on platelets mediates flow-dependent NETosis via SLC44A2. Elife. 2020;9 doi: 10.7554/eLife.53353. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 108.Schönichen C., Montague S.J., Brouns S.L.N., Burston J.J., Cosemans J.M.E.M., Jurk K., et al. Antagonistic roles of human platelet integrin αIIbβ3 and chemokines in regulating neutrophil activation and fate on arterial thrombi under flow. Arterioscler Thromb Vasc Biol. 2023;43:1700–1712. doi: 10.1161/ATVBAHA.122.318767. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 109.Hackenbroch C., Gross C., Cimen T., Rubenzucker S., Beck S., Girbl T., et al. Platelet-derived LTB4 mediates neutrophil recruitment [abstract] Res Pract Thromb Haemost. 2023;7 [Google Scholar]
- 110.Denorme F., Armstrong N., Stoller M., Portier I., Rustad J., Cody M., et al. A Common, racially diverse protease activated receptor 4 functional variant impacts ischemic stroke outcomes: evidence for a pharmacogenetic effect [abstract] Res Pract Thromb Haemost. 2023;7 [Google Scholar]
- 111.Edelstein L.C., Simon L.M., Montoya R.T., Holinstat M., Chen E.S., Bergeron A., et al. Racial difference in human platelet PAR4 reactivity reflects expression of PCTP and miR-376c. Nat Med. 2013;19:1609–1616. doi: 10.1038/nm.3385. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 112.Janus-Bell E., Receveur N., Mercier L., Mouriaux C., Hechler B., Reiser J., et al. Cooperation between platelet β1 and β3 integrins in the arrest of bleeding under inflammatory conditions in mice [abstract] Res Pract Thromb Haemost. 2023;7 doi: 10.1161/ATVBAHA.124.321104. [DOI] [PubMed] [Google Scholar]
- 113.Bourne J., Suthya A., Wilson J., Wanrooy B., Hickey M., Wong C. Modulating platelet-microglial complexes to limit neuroinflammation post-ischemic stroke [abstract] Res Pract Thromb Haemost. 2023;7 [Google Scholar]