Abstract
Lymphoproliferative disorders comprise of a group of heterogenous diseases characterised by uncontrolled production of lymphocytes.Castleman disease (CD) is one such disease and comprises of a group of rare disorders that involve enlarged lymph nodes and a broad range of inflammatory symptoms and laboratory abnormalities [1]. We came across young girl who presented to us in the out patient department with this disease After ruling out other pathologies and confirming the diagnosis by doing a tissue biopsy the girl was treated surgically and is disease free till date.
Keywords: Paediatric Castleman disease, Unicentric CD, Neck mass
Introduction
Lymphoproliferative disorders comprise of a group of heterogenous diseases characterised by uncontrolled production of lymphocytes .One rare form of this disorder is Castlemans disease.Castleman disease (CD) describes a group of at least 4 disorders that share a spectrum of characteristic histopathological features but have a wide range of aetiologies, presentations, treatments, and outcomes. CD was first described in the 1950s by Benjamin Castleman as localized mediastinal lymph node enlargement characterized by increased numbers of lymphoid follicles with germinal centre involution and marked capillary proliferation, including follicular and interfollicular endothelial hyperplasia [2]. According to the clinical presentation and disease course, CD is divided into unicentric CD (UCD), a localized and reversible disease involving a single lymph node [4], and multicentric CD (MCD), a systemic, progressive and often fatal disease with lymphadenopathy in multiple nodes [5]. More recently, an intermediate subtype referred to as ‘oligocentric CD’ or ‘regional CD’ has been described [6], which affects a few lymph nodes and is generally considered to have a clinical course similar to that of UCD [6].
Case Report
A 12 year female child came to the ENT OPD with presentation of left side painless neck swelling since 2 years. On physical examination, a large, discrete, mobile, non-tender mass of 4 × 5 cm in dimension was found in the left upper cervical lymph node level. The clinical findings prompted a diagnosis of Chronic cervical lymphadenopathy. Fine needle aspiration cytology of the left cervical mass was performed. The cytology report came out to be reactive cervical lymphadenopathy. Marked proliferation of non neoplastic polyclonal Lymphocytes forming follicles with an active germinal centre were consistent with the histopathological diagnosis.Ultrasonological diagnosis came out to be Chronic Cervical lymphadenopathy. Patient was given a week of antibiotic course of amoxicillin and clavulinic acid combination and was asked to review after 10 days. Since the swelling did not regress after the medical management, patient was taken up for incisional biopsy under general anaesthesia. Wedge biopsy was taken from level III lymph node of left side and sent for histopathology department for diagnosis. The HPR diagnosis came out to be suspicious of castlemans disease.
We did an MRI of the chest and abdomen to look for any other enlarged lymph nodes.,In the absence of any other lymphadenopathy a final diagnosis of Unicentric Castlemans disease was made .Our physicians advised to observe the patient but the swelling gradually increased.After 1 month interval, patient was taken up for complete excision of the lymph node.
The HPR diagnosis was reported as Castle man disease(Unicentric).On Post operative follow up the patient did well and there is no sign of recurrence till date(one year).
Image 1.

Section from lymph node showing involution of germinal centres and onion skin appearance of mantle zone.
Image 2.
CT Scan (plain) Of neck showing Cervical lymph node enlargement
Image 3.
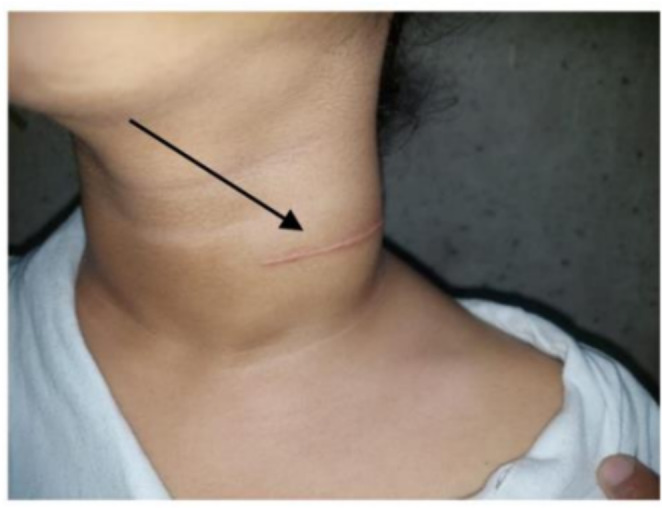
Photographic image of neck showing the lymph nodal enlargement and scar of open biopsy
Image 4.
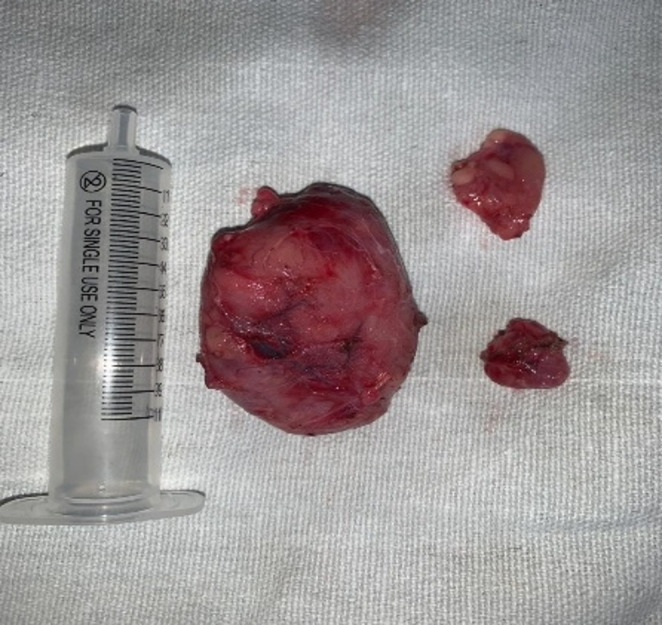
Showing specimen
Discussion
CD is a rare lymphoproliferative disorder, described for the first time by Castleman et al. [2, 3] in 1954 in a single case then in 1956 in a group of 13 patients with localized benign lymphadenopathy. This rare disease is also termed as localized nodal hyperplasia, angiomatous lymphoid hamartoma, or giant lymph node hyperplasia. Williams and Kaude both reported that lymph nodes in the mediastinum were the most common presentation (70%) and that the neck and abdomen were the least common (15%) sites for CD [7].
CD is first classified based on the number of regions of enlarged lymph nodes that demonstrate histopathologic features consistent with CD. Unicentric CD (UCD) involves a single enlarged lymph node or region of lymph nodes, whereas multicentric CD (MCD) involves multiple regions of enlarged lymph nodes [8].
MCD is further divided based on Kaposi sarcoma-associated herpesvirus (KSHV)/human herpesvirus-8 (HHV-8) infection status. POEMS is a paraneoplastic syndrome that often co-occurs with MCD (POEMS-associated MCD) [9].
UCD being able to be eliminated with surgical resection has a good prognosis. However, since multiple systemic disorders involve MCD and sometimes concomitant diseases like HIV and HHV-8 can also be present, specific chemotherapy regimens have not been assigned, and better treatment methods still need to be explored. Moreover, along with the deficient treatment options, nonspecific clinical features that often go unnoticed with limited diagnostic measures also lead to delayed confirmation of its diagnosis. Its prognosis is, therefore, abysmal [11].
Both UCD and MCD can sometimes progress to non-Hodgkin lymphoma (NHL) [12].
In our case, Ct scan showed a solitary well-defined lymph node that was clear and separable from other surroundings. Fine needle aspiration cytology (FNAC) findings may not always be conclusive. CT and MRI are usually of great value in the case prognosis.
Surgical resection is considered the cornerstone of radical treatment for unicentric CD and is the most widely accepted therapy in the literature therefore the upfront excision decision was taken in our case for diagnostic and radical concerns. A systematic review by Talat et al. [13] of 278 unicentric patients found that surgical resection resulted in 95% disease-free survival at 3 years. In case the surgical resection was not applicable, or the lymph node is not accessible, radiation therapy could be an effective way to destroy the affected tissue. Radiation doses of ranges 30–45 Gy appear to be effective, although tumor responses have been documented at lower doses [14]. Multicentric CD however tends to have a variable prognosis with no documented treatment consensus. A variety of combination treatments have been tried with surgical excision, chemotherapy and steroids [13]. In patients with associated Kaposi’s sarcoma monthly polychemotherapy (e.g.: cyclophosphamide, vincristine, doxorubicin and prednisone) has been tried with limited success [15]. Anti-IL 6 antibodies have shown success with systemic symptoms, as have steroids. Most treatment modalities immunosuppression, increasing the chances of opportunistic infections [13]. Recent suggestions are that treatment with the anti-herpes virus drug ganciclovir or the anti-CD20 B cell monoclonal antibody, rituximab, may markedly improve outcome [15].
Conclusion
This case report is presented for the purpose of its rare incidence. A unicentric Castleman disease presents as a single lymph node swelling anywhere in the body most commonly seen in mediastinum in 70% of the cases and head And neck region in another 30% of the patient. These swellings can commonly be confused for cervical tubercular lymphadenitis, nodal secondaries, and lymphoma. Surgical resection of localised unicentric CD is the treatment of choice for therapeutic and diagnostic purposes. Patient should be kept on regular follow up to rule out any incidence of recurrence or further progress of disease.
Funding
No funding was obtained.
Declarations
Consent
Written informed consent was taken from the patient for publication of this case.
Conflict of interest
No conflict of interest between authors.
Footnotes
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.https://cdcn.org/castleman-disease/overview/
- 2.Castleman B, Iverson L, Menendez,VP. Localized mediastinal lymphnode hyperplasia resembling thymoma. Cancer. 1956;9(4):822-830. [DOI] [PubMed]
- 3.Castleman, B. & Towne, V. W. Case records of the Massachusetts General Hospital: Case No. 40231. N. Engl. J. Med 250, 1001–1005 (1954). [DOI] [PubMed]
- 4.Keller, A. R., Hochholzer, L. & Castleman, B. Hyaline-vascular and plasma-cell types of giant lymph node hyperplasia of the mediastinum and other locations. Cancer 29, 670–683 (1972). [DOI] [PubMed]
- 5.Kessler, E. Multicentric giant lymph node hyperplasia. A report of seven cases. Cancer 56, 2446–2451 (1985). [DOI] [PubMed]
- 6.van Rhee, F. et al. International evidence-based consensus diagnostic and treatment guidelines for unicentric Castleman disease. Blood Adv 4, 6039–6050 (2020). [DOI] [PMC free article] [PubMed]
- 7.Williams D.S. Castleman’s disease. J. Insur. Med. N. Y. N. 2013;43(4):256–258. [PubMed] [Google Scholar] [PubMed] [Google Scholar] . [PubMed]
- 8.https://www.hemonc.theclinics.com/article/S0889-8588(17)30142-9/fulltext
- 9.POEMS syndrome and Castleman’s disease. in: Zimmerman T.M. Kumar S.K. Biology and management of unusual plasma cell dyscrasias. Springer, New York2017: 41-69
- 10.Clinicopathologic analysis of TAFRO syndrome demonstrates a distinct subtype of HHV-8-negative multicentric Castleman disease. Am J Hematol 2016; 91: 220-226 [DOI] [PubMed]
- 11.Wang J, Liang LJ, Wang YM, Mei ZY, Liu YZ, Liu LN, Fang BJ, Song YP. [Analysis of the clinicopathologic features as well as diagnosis and treatment of 59 patients with Castleman disease]. Zhonghua Xue Ye Xue Za Zhi. 2020 Aug 14;41(8):666–670. [PMC free article] [PubMed] [Reference list] [DOI] [PMC free article] [PubMed]
- 12.van Rhee F, Greenway A, Stone K. Treatment of Idiopathic Castleman Disease. Hematol Oncol Clin North Am. 2018 Feb;32(1):89–106. [PubMed] [Reference list] [DOI] [PubMed]
- 13.Talat N., Schulte K.M. Castleman’s disease: systematic analysis of 416 patients from the literature. Oncologist. 2011;16(9):1316–1324. [PMC free article] [PubMed] [Google Scholar] [PMC free article] [PubMed] [Google Scholar] [DOI] [PMC free article] [PubMed]
- 14.Chronowski G.M., Ha C.S., Wilder R.B., Cabanillas F., Manning J., Cox J.D. Treatment of unicentric and multicentric Castleman disease and the role of radiotherapy. Cancer. 2001;92(3):670–676. [PubMed] [Google Scholar] [DOI] [PubMed]
- 15.Iyer S., Bhatti M.I., Halliday M. Castleman’s disease-a case report. Int. J. Surg. Case Rep. 2010;1(3):25–26. [PMC free article] [PubMed] [Google Scholar] [PMC free article] [PubMed] [Google Scholar] [DOI] [PMC free article] [PubMed]



