Abstract
Myoepitheliomas are uncommon neoplasms of major and minor salivary glands. These tumours are encapsulated and slow growing in nature and are benign in majority of the cases. The mean age of presentation is 40 years and this entity is rarely reported in younger age groups. Here, we seek to report a rare case of a 10-year-old patient who presented with a swelling below the right ear. Clinical and radiological evaluation revealed a mass in the parotid gland. This patient was treated with a superficial parotidectomy and subsequent histopathological examination revealed it to be a myoepithelioma.
Keywords: Myoepithelioma, Benign, Parotid, Neoplasm
Introduction
Myoepitheliomas are tumours of salivary gland origin composed of myoepithelial cells. Among all salivary gland tumours, these are uncommon and comprise only 1 to 1.5% [1]. The bulk of myoepitheliomas recognized in literature have been found to be benign, but malignant variants (myoepithelial carcinoma) have been described recently [2]. The former is an encapsulated, slow-growing lesion, and is nearly always asymptomatic. They affect a significant range of patients, with the mean age being 40 years. The incidences in parotid, submandibular and minor salivary glands are 48%, 10% and 42%, respectively [3, 4]. In 1943, Sheldon identified these lesions and characterized them as myoepithelioma. Since then, less than 100 cases have been reported in literature. The rate of recurrence of this type of tumour is fairly low after a complete excision. Conversely, malignant myoepithelioma (or myoepithelial carcinoma), is a medium-to-high grade malignancy seen principally in the parotid gland (65%). Histologically, it consists of myoepithelial cells with cellular atypia and neural infiltration seen along with infiltration of neighbouring structures. There may be distant metastasis and there is a tendency to recur in 60% of cases. Here, we present an uncommon case of a benign myoepithelioma of the parotid in a male child, one of the few reports in a younger age group.
Case Report
A 10-year old boy presented to our outpatient department with complaints of a swelling below the right ear since the last six months. The swelling was painless and slowly progressed in size. On examination, there was a 3 × 3 cm swelling in the territory of the right parotid gland. It was well-demarcated, was firm in consistency, not-tender, was not fixed to the surrounding structures. No concomitant facial weakness or cervical lymphadenopathy was present (Fig. 1). An ultrasonography scan showed a 3 × 3.5 cm lesion in the right parotid with regular borders. The mass showed a solid component with internal echoes. Furthermore, a computed tomography scan showed the presence of a solid mass lesion occupying the superficial lobe of the right parotid gland with homogenous enhancement and no infiltration of surrounding structures. Fine needle aspiration cytology was indicative of a pleomorphic adenoma. The patient underwent superficial parotidectomy; intraoperatively the tumour was found to be solid and well circumscribed (Figs. 2, 3 and 4). Subsequent to the surgery, histopathological examination revealed a hypercellular specimen with spindle shaped cells and clusters of epithelioid cells, suggestive of a myoepithelioma. The subtype was deemed to be of the mixed variety, including both the spindle cell and clear cell variants (Fig. 5A and B).
Fig. 1.
Patient at presentation
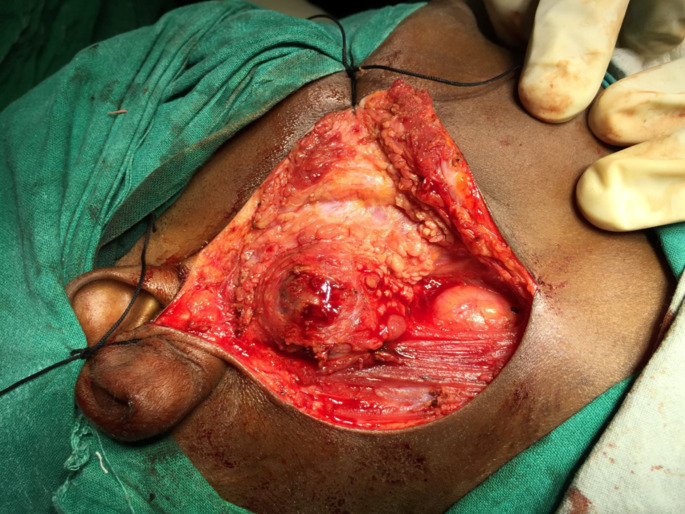
Fig. 2.
Surgical exposure of tumour
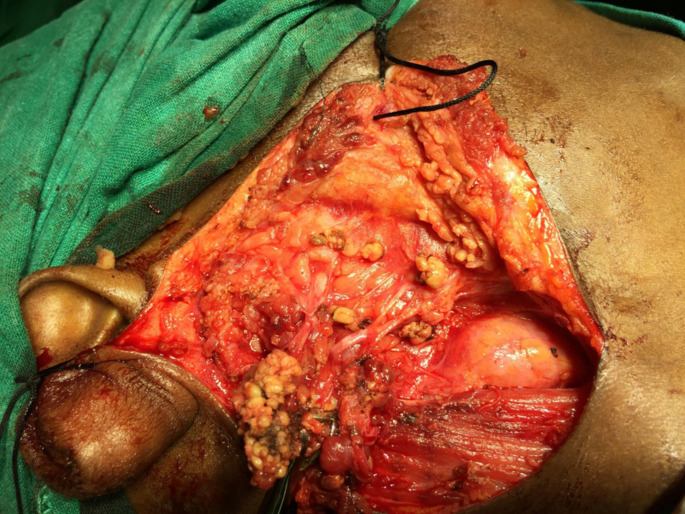
Fig. 3.
Surgical picture after excision of tumour along with adequate surgical margins
Fig. 4.
Surgical specimen
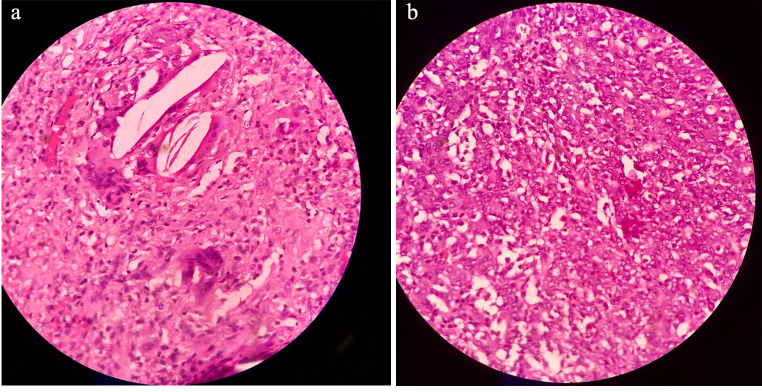
Fig. 5.
A & B: Histopathological slide showing hypercellular specimen with spindle shaped cells and clusters of epithelioid cells (Staining Method: H & E)
Discussion
Myoepithelial cells are contractile cells originating from ectoderm, which can normally be found in tissues having a secretory function (for example: both major and minor salivary glands, lacrimal glands, sweat glands, prostate, and breast). Salivary gland tumours which are usually found to contain myoepithelial cells comprise adenoid cystic carcinoma, pleomorphic adenoma and epithelial-myoepithelial carcinoma arising from intercalated ducts [5–7]. Tumours solely containing myoepithelial cells are scarce, making up less than 1% of all salivary gland tumours. Histologically, benign myoepithelioma is composed of myoepithelial cells where up to 5% ductal epithelial cells can be present, while a large number of ductal formations points towards the diagnosis of a mixed tumour. The majority of these tumours are seen in the parotid, but also occur in the submandibular or accessory glands of the oral cavity (cheek, tongue, lips, mouth floor, hard palate, soft palate, gingiva, retromolar trigone) [4, 8]. Occasionally, they also arise from the respiratory tract glands (nasal cavity, nasopharyngeal, laryngeal, lung). Myoepitheliomas are rare, solid, capsulated tumours of the salivary gland found with equivalent incidence in both sexes [5]. Though these tumours have been reported in ages ranging from 6 to 81, the mean age is around 40 years. Five cellular patterns can be distinguished in benign myoepitheliomas: (1) spindle cells, (2) plasmacytoid cells, (3) reticular pattern, (4) clear cells, and (5) combination of various types of cells. The spindle cell variety is the most common overall and is typical of parotid myoepitheliomas. Differential diagnoses may comprise mucoepidermoid carcinoma, pleomorphic adenoma, adenocystic carcinoma, clear cell adenocarcinoma or acinic cell adenocarcinoma. In contrast to pleomorphic adenoma, these tumours do not have any differentiation of the ductal epithelium, and may present with minimal stromal elements. Gene studies, especially cytogenetic/molecular, done mainly for pleomorphic adenomas have shown recurrent specific chromosomal alterations at the 8q 12 and 12q 13 – q 15 regions. Nevertheless, the cell origin of these alterations remains unclear. Cytogenetic analysis of the myoepithelioma on the other hand, shows 12q 12 involved in a translocation with a previously unknown component (1 q), and non-random del (9) (q 22.1q 22.3) and del (13) (q 12q 22). The chromosomal abnormalities originate from the myoepithelial cell. Moreover, myoepitheliomas have shown 12 q alterations which have also been reported in a subset of pleomorphic adenomas as well [9]. The proteins S 100 and vimentin are not usually present in normal myoepithelial cells; they are quite sensitive but non- specific markers of neoplastic myoepithelial cells. Biologically, myoepithelial tumours are usually benign, but the malignant variants are locally invasive and can also produce metastases. The latter variants demonstrate aggressive growths which infiltrate, as well as regions of necrosis, cytologic atypia, elevated mitotic rate and cellular pleomorphism [8]. Numerous studies have demonstrated that assessing cellular proliferative activity are beneficial in the differentiating between the benign and the malignant myoepithelial tumours; further, a Ki-67 labelling index higher than 10% is diagnostic of myoepithelial carcinoma [9]. The primary treatment of myoepithelial carcinomas remains surgical. Due to the elevated recurrence rate, the surgery should be radical with ample tissue margins. Adjuvant treatment (chemotherapy +/- radiotherapy) are not useful for treating myoepithelial carcinomas. The treatment approach for benign myoepitheliomas, on the other hand, is analogous to that of mixed tumours: comprehensive surgical excision with sufficient tissue margins. The majority of myoepitheliomas have a benign progression with low recurrence chances, with these rates reported as being similar to that of pleomorphic adenomas [10].
Conclusions
Myoepitheliomas are salivary gland neoplasms composed of myoepithelial cells. These tumours are uncommon, and rarely reported in younger age groups. The most widely accepted management of myoepithelioma is surgical excision with ample margins of surrounding tissue. A recurrence rate of 15–18% has been observed, mostly in cases with incomplete resection. Prognosis for this benign tumour is favourable and the patient should be followed up regularly to detect any recurrence, should it occur.
Acknowledgements
Nil.
Declarations
Ethical Approval
All procedures used in this research were approved by the Ethical Committee of Kasturba Medical College, Mangalore, Manipal Academy of Higher Education.
Conflict of Interest
The authors declare no conflicts of interest associated with this manuscript.
Ethical Committee clearance
Ethical Committee clearance taken from institutional ethical committee.
Footnotes
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.Kawashima Y, Kobayashi D, Ishikawa N, Kishimoto S. A case of myoepithelioma arising in an accessory parotid gland. J LaryngolOtol. 2002;116:474–476. doi: 10.1258/0022215021911112. [DOI] [PubMed] [Google Scholar]
- 2.Savera AT, Sloman A, Huvos AG, Klimstra DS. Myoepithelialcarcinoma of salivary glands: a clinicopathologic study of 25 patients. Am J Surg Pathol. 2000;24(6):761–774. doi: 10.1097/00000478-200006000-00001. [DOI] [PubMed] [Google Scholar]
- 3.Batsakis JG, EL-NaggarAK,Luna MA (1992) Pathology consultation: epithelial- myoepithelial carcinoma of salivary glands. Ann OtolRhinolLaryngol :101:540 [DOI] [PubMed]
- 4.Ferri E, Pavon I, Armato E, Cavaleri S, Capuzzo P, Ianniello F Myoepithelioma of a minor salivary gland of the cheek: case report. ActaOtorhinolaryngolItal 26(1):43–46 [PMC free article] [PubMed]
- 5.Hamperl H. The myothelia (myoepithelial cells).Normal state; regressive changes; hyperplasia; tumours. Curr Top Pathol. 1970;53:161–220. doi: 10.1007/978-3-662-30514-0_3. [DOI] [PubMed] [Google Scholar]
- 6.Thompson SH, Bender S, Richards A. Plasmacytoidmyoepithelioma of a minor salivary glands. J Oral MaxillofacSurg. 1985;43:285–288. doi: 10.1016/0278-2391(85)90289-7. [DOI] [PubMed] [Google Scholar]
- 7.Taylor J, Tighe JV. A minor salivar gland tumour presenting with dysphagia. J LaryngolOtol. 1999;113:569–572. doi: 10.1017/S0022215100144512. [DOI] [PubMed] [Google Scholar]
- 8.Suba Z, Nemeth Z, Gyulai-Gaal S, Ujpal M, Szende B, Szabo G (2003) Malignant myoepithelioma Clinicopathological and immunohistochemical characteristics. Int J Oral Maxillofac;32:339 – 41 [DOI] [PubMed]
- 9.Nagao T, Sugano I, Ishida Y. Salivary gland malignant myoepithelioma. A clinicopathologic and immunohistochemical study of ten cases. Cancer. 1988;83:1292–1299. doi: 10.1002/(SICI)1097-0142(19981001)83:7<1292::AID-CNCR4>3.0.CO;2-L. [DOI] [PubMed] [Google Scholar]
- 10.De Stefani A, Lerda W, Bussi M, Valente G, Cortesina G (1999) Tumors of the parapharyngeal space: Case report of clear cell myoepithelioma of the parotid gland. 19:276–282 [PubMed]