Abstract
Background
Many youth in the criminal justice system are affected by mental health and/or substance use (MHS) challenges, yet only a minority receive treatment. One way to increase access to MHS care is integrated youth services (IYS), a community-based model of service delivery where youth can access evidence-based treatment for their MHS problems and other wellbeing needs, in one location. However, it is unknown what IYS services justice-involved youth prioritize.
Objective
This study explored what components of IYS justice-involved youth deem to be the most important in meeting their MHS service needs, in comparison with non-justice-involved youth, by conducting a secondary analysis of data gathered from a larger Ontario-wide study.
Method
Using a conjoint analysis, n = 55 justice-involved youth, and n = 188 non-justice-involved youth, completed thirteen choice tasks representing different combinations of IYS.
Results
Both justice-involved and non-justice-involved youth exhibited preferences for a broad range of core health services, including mental health services, substance misuse counseling, medication management, and physical or sexual health services. They also preferred a broad range of additional support services, in addition to fast access to care in a community setting that specializes in mental health services, with the incorporation of e-health services. Justice-involved youth prioritized working with a trained peer support worker to learn life skills and help them with the services they need. The importance of youth playing a leadership role in making decisions within IYS organizations was also a distinguishing preference among justice-involved youth.
Conclusions
Tailoring IYS to meet the service preferences of justice-involved youth may enhance service utilization, potentially leading to better outcomes for justice-involved youth and their communities.
Key Words: justice-involved youth, caregiver, patient preferences, integrated care, mental health and substance use
Résumé
Contexte
Nombre de jeunes dans le système de justice pénale sont affectés de problèmes de santé mentale et/ou d’utilisation de substances (SMS), pourtant seule une minorité reçoit un traitement. Une façon d’élargir l’accès aux soins SMS consiste dans les services intégrés à la jeunesse (SIJ), un modèle communautaire de prestation de service dans lequel les jeunes peuvent avoir accès à un traitement fondé sur les données probantes pour leurs problèmes de SMS et autres besoins de bien-être en un seul lieu. Cependant, on ne sait pas à quels SIJ les jeunes impliqués dans la justice accordent la priorité.
Objectif
La présente étude a exploré quelles composantes des SIJ sont jugées les plus importantes par les jeunes impliqués dans la justice pour répondre à leurs besoins de service de SMS, en comparaison avec les jeunes non impliqués dans la justice, au moyen d’une analyse secondaire des données recueillies d’une étude plus vaste à l’échelle de l’Ontario.
Méthode
À l’aide d’une analyse conjointe, n = 55 jeunes impliqués dans la justice, et n = 188 jeunes non impliqués dans la justice ont répondu à treize tâches à choix représentant différentes combinaisons de SIJ.
Résultats
Tant les jeunes impliqués dans la justice que les jeunes non impliqués ont affiché des préférences pour une large gamme de services de santé de base, notamment les services de santé mentale, la consultation pour abus de substances, la gestion des médicaments, et les services de santé physique ou sexuelle. Ils préféraient également une large gamme de services de soutien additionnels, en plus d’un accès rapide aux soins dans un milieu communautaire qui se spécialise en services de santé mentale, avec l’incorporation de services de santé en ligne. Les jeunes impliqués dans la justice accordaient la priorité au travail avec un pair aidant formé pour apprendre les compétences de la vie et les aider dans les services dont ils ont besoin. L’importance pour les jeunes de jouer un rôle de leadership dans la prise de décisions au sein des organisations de SIJ était également une préférence distincte chez les jeunes impliqués dans la justice.
Conclusions
Adapter les SIJ pour répondre aux préférences de services des jeunes impliqués dans la justice peut améliorer l’utilisation des services, et mener potentiellement à de meilleurs résultats pour les jeunes impliqués dans la justice et leurs communautés.
Mots clés: jeunes impliqués dans la justice, soignant, préférences des patients, soins intégrés, santé mentale et utilisation de substances
Introduction
Approximately 25% of Canadian youth experience mental health and/or substance use (MHS) problems (1, 2). These problems are particularly notable in youth involved in the criminal justice system (3, 4). Meta-analytic data show that the prevalence rates of MHS problems in justice-involved youth are high across a range of common disorders (4). The associated challenges of untreated MHS challenges are pervasive, affecting social, academic, and occupational functioning (5, 6). Justice-involved youth are at a particularly high risk for impairment, given the higher prevalence and severity of MHS problems in this population (3, 4, 7, 8).
Effective early intervention can mitigate the effects of MHS challenges and optimize positive youth outcomes (9, 10, 11, 12). For justice-involved youth, MHS treatment can redirect them away from a criminal trajectory (10, 13, 14). Conversely, untreated MHS challenges, particularly substance abuse, increases the risk for criminality and recidivism (e.g., 15, 16). Unfortunately, only a minority of justice-involved youth with MHS problems access treatment (8, 17, 18). For example, a U.S. meta-analytical report showed that about 45% of incarcerated adolescents had received either mental health or substance use services at some point in their lives (18).
Integrated Youth Services
One way to increase access to youth MHS services is integrated youth services (IYS; e.g., 19, 20, 21). An integrated youth service is a community-based model of service delivery through which youth can access evidence-based treatment for their MHS problems and other wellbeing needs, such as physical health, housing, and education concerns, in one location (20). Youth may be more likely to attend treatment at agencies where integrated services are provided (22).
There is a growing evidence-base demonstrating that an integrated approach that addresses the biopsychosocial needs of justice-involved youth may be best practice in supporting this population (e.g., 23, 24, 25). Given that the IYS model hinges on addressing a spectrum of youth needs (26), IYS are an optimal avenue for implementing services targeting this marginalized group of youth. Furthermore, service utilization, treatment completion (27), and a decrease in recidivism (28), have been associated with justice-involved youth who receive integrated care.
Although IYS are recognized as an optimal strategy in deliving services to youth, determining which services youth want to receive within an IYS is in a nascent stage. Furthermore, despite the various differences in MHS prevalance, presentation, and treatment engagement, it is unknown in what ways justice-involved youth differ from their non-justice-involved counterparts in terms of what their service preferences might be. Use of a conjoint analysis (29) may help to answer this question.
Using Conjoint Analysis to Understand Service Preferences
The conjoint analysis methodology holds that a service can have multiple attributes, and that within each attribute exists multiple levels (29). The conjoint analysis combines different levels of different service attributes in unique service combinations and asks respondents to choose between the proposed service packages in complex decision scenarios. By imitating complex decision making in the real-world (30), an electronic conjoint analysis prompts participants to make choices about their preferences for various hypothetical service options (29).
The conjoint analysis, and analogous discrete choice experiment, are popular methodologies in psychology research (31). Recently, a DCE study by Henderson and colleagues (32), from which this study conducts a secondary analysis of data, made contributions to understanding what services Ontario youth prefer within IYS. Henderson and colleagues (32) found three latent classes among youth who have nuanced preferences. Specifically, a Focused Services class most preferred fast access to MHS services, a Holistic Services class prioritized a large range of MHS and social services, and the Responsive Services class preferred individually tailored IYS services (e.g., culturally sensitive services). Importantly, this study also found consensus among the three latent classes in that most youth preferred a wrap-around service approach that encompassed a range of physical health, mental health, and social services, in a specialized setting with low wait times and flexible hours.
Despite the findings from the Henderson and colleagues (32) study, it did not examine the preferences of justice-involved youth. Given the potential differences in the MHS prevalence, presentation, and treatment engagement between justice-involved youth and non-justice-involved youth, it is reasonable to expect that justice-involved youth may differ from their counterparts in their service preferences. Tailoring IYS to meet the service preferences of justice-involved youth may ultimately enhance service utilization, potentially leading to better outcomes for justice-involved youth with MHS challenges.
The Present Study
A secondary analysis of data generated from an Ontario-wide conjoint analysis exploring the integrated youth services (IYS) preferences of youth, caregivers, and service provider groups (32, 33, 34) was conducted for this study. This study extended the larger conjoint analysis by contrasting the specific IYS component preferences of justice-involved youth when compared to non-justice-involved youth, in order to guide the design of services that align with justice-involved youths’ preferences. The following research question was addressed: What components of IYS do justice-involved youth deem to be the most important in meeting their MHS service needs, in comparison with non-justice-involved youth?
Method
Survey Development
Development of the study has been described in previous published literature by Hawke and colleagues (34). This study was part of a larger study examining integrated youth service preferences across general samples of service-seeking youth, caregivers, and service providers. The conjoint analysis survey tool was developed through collaboration among the lived experience engaged research team, including youth co-researchers. The items were developed pragmatically to include service options that currently exist or were recommended. It was then piloted in July 2019 among four youth at two youth-serving MHS organizations within Ontario.
Participants
A total sample of N = 243 youth (n = 55 justice-involved youth; n = 188 non-justice-involved youth) participated in the current study. In order to participate, youth had to be Ontario residents between the ages of 14 and 29 who self-selected for the study based on the advertised target of youth who have experienced MHS challenges. Previous MHS service use was not required. A total of 297 youth were recruited over a 5 month period from September 2019 to January 2020. Of this sample, 54 youth were excluded from the current study because they did not meet eligibility criteria (i.e., were not Ontario youth with MHS challenges). Of the remaining 243 youth, n = 55 endorsed justice-involvement (see below for assessment of justice-involvement). The proportion of justice-involved youth recruited in the current study is consistent with a previous Canadian study whose sample consisted of youth that presented at various clinical and non-clinical service sectors (i.e., 20% to 40%; 35).
Procedure
This study was approved by the Research Ethics Boards of the Centre for Addiction and Mental Health and Toronto Metropolitan University. Participants were recruited as part of the larger, Ontario-wide study by emailing a survey link to a database of over 600 MHS community agencies in Ontario (36). Prior to youth participation, informed consent was obtained through the survey link. Sawtooth Software, Version 9 (37) was used to administer the conjoint analysis. In addition to the conjoint analysis survey, participants also completed a questionnaire regarding sociodemographic information and service use, as well as a mental health screener. Median survey completion time was 17.52 minutes.
Measures
Justice Involvement
Justice involvement was assessed via the sociodemographic questionnaire. Youth were asked “Have you ever had legal system involvement?” Respondent choices were: “No, never”; “Yes, in the past 12 months”; or “Yes, more than a year ago.” Youth who endorsed having legal system involvement within the past year or more and also endorsed at least one of the following met inclusionary criteria for justice-involvement; “Do you have any legal charges?”; “Have you ever been arrested?”; “Are you currently on probation?”
Global Assessment for Individual Needs-Short Screener
The Global Assessment for Individual Needs-Short Screener (GAIN-SS; 38) was administered as a screener for mental health and substance use problems. The GAIN-SS is a 29-item questionnaire that asks youth to indicate if they have experienced problems associated with internalizing disorders, externalizing disorders, substance use disorders, and crime and violence problems. Responses were recorded using the following: 4 = past month, 3 = two to three months ago, 2 = four to 12 months, 1 = 1+ years ago, and 0 = never. This measure has demonstrated good internal consistency (α = .96), excellent validity (r = .84 to .94), sensitivity (90%), and specificity (92%; 38). Based on published guidelines, a clinical cut-off score for the Internalizing Scale was set at four (39), a clinical cut-off score for the Externalizing and Crime and Violence Scale was set at three (38), and a clinical cut-off score for the Substance Use Disorder Scale was set at two (40). Youth responses to the GAIN-SS were also used to cross-validate the study’s approach to defining justice-involvement (see Results, below).
Conjoint Analysis
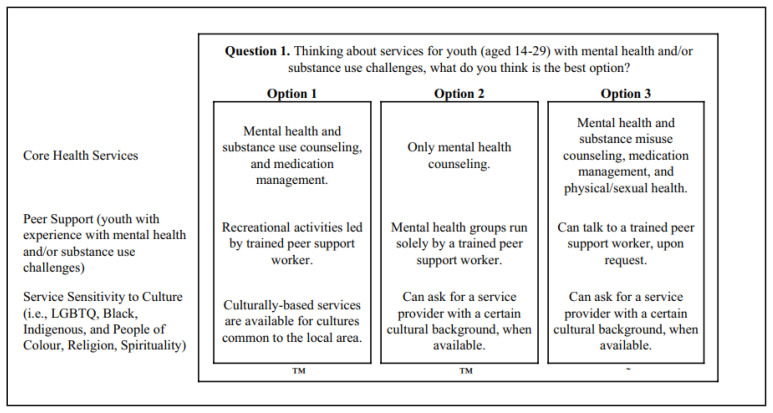
The conjoint analysis was composed of 12 attributes with four levels each. Sawtooth Software, Version 9 (37) randomly produced 999 versions of the survey and randomly assigned participants to complete one of the created versions. Thirteen choice tasks were shown to each participant, with three concepts per task, and three levels per concept (see Figure 1). One task was identical across all participants, in order to test for respondent reliability and validity (i.e., “hold-out” task).
Figure 1.
A sample choice task in the conjoint analysis
Data Analyses
Stage 1
A first-choice simulation was used to test the reliability of the conjoint analysis, with justice-involvement entered as a covariate. How well the model predicts participant responses was determined by comparing caregiver responses on the fixed-choice task (i.e., “hold-out” task) to predicted participant responses based on utility values generated by Hierarchical Bayes (HB) estimates.
Stage 2
A hierarchical Bayes (HB) analysis was conducted in Sawtooth Software Inc. (37) in order to determine Attribute Importance Scores (i.e., an indication of the relative importance of each attribute compared to the other attributes), with justice-involvement entered as a covariate. A MANOVA was performed, with justice-involvement as the independent variable and the Importance Scores for each attribute as the dependent variables to determine between-group differences in attribute preference. Where MANOVAs were significant, univariate ANOVAs with Bonferroni corrected p-values were run to determine whether attribute preferences were statistically different among groups.
Stage 3
Standardized, zero-centered individual utility values (which indicate the preference for each level within each attribute) generated by HB through Sawtooth Software (37) were used to analyze group differences in preferences among levels within each attribute. A series of MANOVAs was conducted in order to determine which levels distinguish participant groups, with justice-involvement as the independent variable and utility values for each level within an attribute as the dependent variables. Where MANOVAs were statistically significant, univariate ANOVAs with Bonferroni corrections were computed to identify the significant differences.
Stage 4
A randomized first choice simulation was run; this is a simulation analysis that predicts what percentage of justice-involved and non-justice-involved youth would prefer specified combinations (or scenarios) of IYS levels.
Results
Participant Characteristics
Justice-involved and non-justice-involved youth differed on most sociodemographic factors, with the exception of age and race/ethnicity. Justice-involved youth (Mage = 23.02, SD = 2.39) and non-justice-involved youth (Mage = 22.35, SD = 3.60) were similar in age, with no statistically significant difference between groups, t(132.26) = 1.62, p = .108, d = 0.22. There were also no statistically significant differences in race/ethnicity between groups, with the majority of justice-involved and non-justice-involved youth being White (83.6% and 65.4%, respectively). Sociodemographic information with Chi-square statistics, effect sizes, and Bonferroni-corrected post-hoc tests are displayed in Table 1.
Table 1.
Sociodemographic and clinical characteristics of justice-involved (YJ) and non-justice-involved (non-YJ) participants, with significance tests and effect sizes
| Group | YJ (n = 55) % (n) | Non-YJ (n = 188) % (n) | χ2 (df) | p | Φ |
|---|---|---|---|---|---|
| Gender | 47.30 (2) | < .001 | .4421 | ||
| Woman | 22.2 (12)* | 64.9 (122)* | 46.24 (1) | < .001 | |
| Man | 77.8 (42)* | 26.6 (50)* | 31.36 (1) | < .001 | |
| Transgender/non-binary | 0 (0) | 8.5 (16) | 4.84 (1) | .028 | |
| Race/Ethnicity | 8.46 (4) | .076 | .1871 | ||
| White | 83.6 (46) | 65.4 (123) | |||
| Other | 7.3 (4) | 11.7 (22) | |||
| Asian | 1.8 (1) | 12.8 (24) | |||
| Black | 5.5 (3) | 5.9 (11) | |||
| Indigenous | 1.8 (1) | 4.3 (8) | |||
| Socioeconomic Status | 25.03 (3) | < .001 | .3221 | ||
| Live comfortably | 14.8 (8) | 30.3 (57) | 5.29 (1) | .022 | |
| Meets needs with a little left | 77.8 (42)* | 41.0 (77)* | 23.04 (1) | < .001 | |
| Just meet basic expenses | 3.7 (2)* | 25.5 (48)* | 12.25 (1) | < .001 | |
| Does not meet basic expenses | 3.7 (2) | 3.2 (6) | .040 (1) | .842 | |
| Region of Residence | 26.29 (2) | < .001 | .333 | ||
| Rural to Small Population | 49.1 (27) * | 18.1 (33)* | 21.16 (1) | < .001 | |
| Medium Population | 27.3 (15) | 23.6 (43) | .36 (1) | .549 | |
| Large Urban Population | 23.6 (13)* | 58.2 (106)* | 20.25 (1) | < .001 | |
| Physical Health | 11.56 (1) | .001 | .218 | ||
| Good to excellent | 94.5 (52) | 72.9 (137) | |||
| Fair to poor | 5.5 (3) | 27.1 (51) | |||
| Mental Health | 15.43 (1) | < .001 | .252 | ||
| Good to excellent | 83.6 (46) | 54.3 (102) | |||
| Fair to poor | 16.4 (9) | 45.7 (86) | |||
| Student Status | 4.19 (1) | .041 | .132 | ||
| Part- or full-time enrollment | 70.4 (38) | 54.8 (103) | |||
| Not enrolled | 29.6 (16) | 45.2 (85) | |||
| Education Level | 6.69 (2) | .035 | .167 | ||
| High school or less | 20.0 (11) | 27.6 (51) | 1.21 (1) | .271 | |
| Some college/university | 54.5 (30) | 35.1 (65() | 6.76 (1) | .009 | |
| Graduated college/university | 25.5 (14) | 37.3 (69) | 2.56 (1) | .110 | |
| Employment Status | 12.36 (3) | .006 | .226 | ||
| Full-time | 22.6 (12) | 33.5 (63) | 2.25 (1) | .134 | |
| Part-time | 52.8 (28)* | 28.2 (53)* | 11.56 (1) | < .001 | |
| Unemployed | 11.3 (6) | 24.5 (46) | 4.41 (1) | .036 | |
| Other | 13.2 (7) | 13.8 (26) | .010 (1) | .920 | |
| Housing | 32.83 (4) | < .001 | .3681 | ||
| Lives independently | 3.7 (2) | 11.7 (22) | 2.89 (1) | .089 | |
| With a partner | 59.4 (32)* | 19.7 (37)* | 32.49 (1) | < .001 | |
| With family | 27.8 (15)* | 52.7 (99)* | 10.24 (1) | < .001 | |
| With friends | 5.6 (3) | 11.7 (22) | 1.69 (1) | .194 | |
| GAIN-SS** | |||||
| Internalizing Disorder | 96.1 (49) | 78.9 (146) | 8.2 (1) | .004 | .186 |
| Externalizing Disorder | 96.4 (53) | 66.5 (121) | 19.32 (1) | < .001 | .286 |
| Substance Use Disorder | 90.9 (50) | 43.1 (81) | 39.17 (1) | < .001 | .401 |
| Crime and Violence Problems | 78.2 (43) | 14.9 (28) | 82.41 (1) | < .001 | .582 |
Statistically significant after Bonferroni-corrected post-hoc test
Proportion meeting the cutoff with scores suggesting a high likelihood of meeting diagnostic criteria or needing support in that domain.
Cramer’s V (Vε) was used as a measure of effect size due to small cell sizes.
Conjoint Analysis
Stage 1
A first-choice simulation accurately predicted participant responses at a rate of 71.2%, which is substantially higher than chance (i.e., 33.3%), suggesting reliability of the HB model’s estimates.
Stage 2
The relative importance of each attribute by group is presented in Table 2. The top three attributes for justice-involved youth, in order from most to least important, were: (1) Core Health Services, (2) Other Services, and (3) Wait Time. The least important attributes for justice-involved youth were (1) aregiver Involvement, (2) Engagement, and (3) Age Range. For non-justice-involved youth, the top three attributes were: (1) Core Health Services, (2) E-Health Services, and (3) Other Services, with the least important attributes being (1) Age Range, (2) Engagement, and (3) Peer Support.
Table 2.
The relative importance of each IYS attribute for justice-involved and non-justice-involved youth, and between-group MANOVA Pillai’s Trace statistic
| Attribute | Justice-Involved n = 55 | Non-Justice-Involved n = 188 | F (df) | p | ηp2 | ||
|---|---|---|---|---|---|---|---|
|
|
|
||||||
| M | SD | M | SD | ||||
| 1. Core Health Services | 10.10% | 3.48 | 10.86% | 3.05 | 2.53 (1) | .113 | .010 |
| 2. Other Services | 10.03% | 3.42 | 9.69% | 2.66 | .628 (1) | .429 | .003 |
| 3. Caregiver Involvement | 7.27% | 2.64 | 8.44% | 2.53 | 8.88 (1) | .003* | .036 |
| 4. Peer Support | 9.08% | 2.59 | 4.87% | 2.04 | 159.60 (1)a | <.001* | .398 |
| 5. Cultural Sensitivity | 8.22% | 3.49 | 8.82% | 2.71 | 1.83 (1)a | .178 | .008 |
| 6. E-Health Services | 8.49% | 2.98 | 10.19% | 2.90 | 14.51 (1) | <.001* | .057 |
| 7. Age Range | 6.36% | 2.40 | 6.67% | 2.29 | .792 (1) | .375 | .003 |
| 8. Time of Appointments | 8.32% | 3.52 | 8.23% | 5.53 | .044 (1)a | .835 | .000 |
| 9. Wait Time | 9.62% | 3.89 | 9.06% | 2.46 | 1.66 (1)a | .199 | .007 |
| 10. Location | 7.86% | 2.46 | 8.77% | 2.30 | 6.38 (1) | .012 | .026 |
| 11. Engagement | 7.21% | 3.32 | 5.67% | 2.77 | 11.90 (1) | .001* | .047 |
| 12. Information Sharing | 7.46% | 3.07 | 8.74% | 2.88 | 8.18 (1) | .005 | .033 |
| Total | 100% | 100% | |||||
Levene’s test of equality of error variance statistically significant
Statistically significant at the Bonferroni corrected p-value of .0042
Pillai’s Trace test was significant, V = .481, F(11, 231) = 19.42, p < .001, ηp2 = .481, indicating statistically significant group differences in the relative importance of attributes. Univariate ANOVAs with Bonferroni corrected p-values demonstrated statistically significant between-group differences in the importance of the following attributes: Caregiver Involvement (small effect), Peer Support (large effect), E-Health Services (small to medium effect), and Engagement (small to medium effect). Caregiver Involvement and E-Health Services attributes were significantly less important to justice-involved youth when compared to non-justice involved youth; in contrast, Peer Support and Engagement attributes were given higher importance among justice-involved youth compared to non-justice involved youth.
Stage 3
Results for the utility values are presented in Table 3. Statistically significant, mainly large, effects were found within all 12 attributes, with the exception of the attribute Other Services, where no statistically significant group differences were found. Results for each of the 12 attributes are presented below.
Table 3.
Utility values of IYS levels for justice-involved and non-justice-involved youth, and between-group MANOVA Pillai’s Trace statistic on attributes with follow-up ANOVA results on levels
| Attribute Levels | Justice-Involved n = 55 | Non-Justice-Involved n = 188 | V | F (df) | p | ηp2 | ||
|---|---|---|---|---|---|---|---|---|
|
|
|
|||||||
| M | SD | M | SD | |||||
| 1. Core Health Services | .043 | 3.59 (3,239) | .014 | .043 | ||||
| Only mental health counseling. | −42.57 | 43.78 | −60.95 | 35.69 | 10.12 (1)a | .002* | .040 | |
| Mental health and substance misuse counseling. | −10.34 | 26.79 | −9.55 | 22.17 | .049 (1) | .826 | .000 | |
| Mental health and substance misuse counseling, and medication management. | 20.58 | 31.26 | 24.66 | 20.41 | 1.30 (1)a | .255 | .005 | |
| Mental health and substance misuse counseling, medication management, and physical/sexual health. | 32.32 | 48.90 | 45.84 | 42.37 | 4.03 (1)a | .046 | .016 | |
|
| ||||||||
| 2. Other Services | .019 | 1.58 (3,239) | .195 | .019 | ||||
| Education and employment services. | −11.87 | 28.31 | −14.25 | 23.96 | ||||
| Housing, shelter and income support services. | 18.63 | 26.66 | 12.34 | 24.57 | ||||
| Legal support services. | −48.53 | 37.70 | −45.86 | 32.13 | ||||
| Choice of education, employment, housing, income support, and legal support services. | 41.76 | 42.26 | 47.77 | 36.79 | ||||
|
| ||||||||
| 3. Caregiver Involvement | .426 | 59.18 (3,239) | <.001 | .426 | ||||
| No caregiver involvement. | 2.12 | 29.20 | −47.24 | 23.16 | 170.70 (1)a | <.001* | .415 | |
| Caregivers receive own counseling. | 2.35 | 35.40 | 15.08 | 32.96 | 6.14 (1) | .014 | .025 | |
| Caregivers involved in family counseling with youth, with youth consent. | 19.27 | 30.75 | 29.18 | 27.31 | 5.28 (1) | .022 | .021 | |
| Caregivers involved in decisions regarding youth counseling, with youth consent. | −23.74 | 36.50 | 2.97 | 30.70 | 29.49 (1) | <.001* | .109 | |
|
| ||||||||
| 4. Peer Support | .401 | 53.24 (3,239) | <.001 | .401 | ||||
| Recreational activities led by trained peer support worker. | −46.20 | 25.28 | −13.74 | 21.09 | 91.83 (1) | <.001* | .276 | |
| Can talk to a trained peer support worker, upon request. | −2.74 | 24.61 | −10.22 | 19.23 | 5.63 (1)a | .018 | .023 | |
| Mental health groups run solely by a trained peer support worker. | −1.09 | 29.30 | 2.07 | 21.02 | .79 (1)a | .375 | .003 | |
| Youth can be matched to an ongoing trained peer support worker to learn life skills and help them with services they need. | 50.03 | 28.66 | 21.90 | 19.48 | 70.37 (1)a | <.001* | .226 | |
|
| ||||||||
| 5. Cultural Sensitivity | .185 | 18.09 (3,239) | <.001 | .185 | ||||
| Cultural background is not considered when picking a service or service provider. | 7.06 | 43.68 | −38.69 | 44.14 | 45.94 (1) | <.001* | .160 | |
| Can ask for a service provider with a certain cultural background, when available. | 9.19 | 35.83 | 10.33 | 24.49 | .073 (1)a | .787 | .000 | |
| Services are culturally sensitive and trauma-informed. | −20.08 | |||||||
| Culturally-based services are available for cultures common in the local area. | 48.88 | 24.78 | 41.84 | 45.23 (1)a | <.001* | .158 | ||
|
| ||||||||
| 6. E-Health Services | .194 | 19.13 (3,239) | <.001 | .194 | ||||
| No e-health or electronic services. | −29.17 | 33.40 | −53.51 | 27.82 | 29.64 (1)a | <.001* | .110 | |
| Can schedule or reschedule appointments via email, text or online. | 28.90 | 29.58 | 21.69 | 27.09 | 2.89 (1) | .091 | .012 | |
| E-health services are offered 24/7 alongside in-person services during office hours. | 17.44 | 45.21 | 52.87 | 34.72 | 38.35 (1)a | <.001* | .137 | |
| All services are delivered only through a website, e-mail, text, or phone app. | −17.17 | 33.83 | −21.06 | 25.50 | .845 (1)a | .359 | .003 | |
|
| ||||||||
| 7. Age Range | .302 | 34.42 (3,239) | <.001 | .302 | ||||
| Services for ages 12–24, in a youth-only setting. | −16.03 | 31.44 | −22.73 | 23.64 | 2.91 (1)a | .089 | .012 | |
| Services for ages 12–29, in a youth-only setting. | −10.50 | 24.99 | 17.70 | 20.11 | 74.57 (1)a | <.001* | .236 | |
| Services for ages 12–24, in a setting that also has services for children 0–12. | 10.22 | 32.54 | −20.93 | 28.32 | 48.04 (1)a | <.001* | .166 | |
| Services for ages 12–29, in a setting that also has services for adults 29+. | 16.31 | 25.39 | 25.95 | 24.77 | 6.37 (1) | .012* | .026 | |
|
| ||||||||
| 8. Time of Appointments | .525 | 88.15 (3,239) | <.001 | .525 | ||||
| Monday to Friday, 9AM–5PM. | 22.50 | 36.13 | −37.21 | 25.55 | 189.85 (1)a | <.001* | .441 | |
| Monday to Friday, 9AM–9PM. | 3.55 | 31.89 | −6.04 | 25.17 | 5.43 (1)a | .021* | .022 | |
| Monday to Friday, 9AM–9PM, and Saturday, 9AM–5PM. | −3.90 | 24.37 | 29.80 | 21.01 | 101.64 (1) | <.001* | .297 | |
| 24/7. | −22.15 | 57.66 | 13.45 | 47.45 | 21.64 (1)a | <.001* | .082 | |
|
| ||||||||
| 9. Wait Time | .466 | 69.49 (3,239) | <.001 | .466 | ||||
| See a counselor for the first time immediately, during office hours. | 14.46 | 32.42 | 46.23 | 26.70 | 54.46 (1)a | <.001* | .184 | |
| See a counselor for the first time after about 72 hours. | 32.11 | 37.65 | 18.48 | 33.40 | 6.68 (1) | .010* | .027 | |
| See a counselor for the first time after about 1 month. | −56.15 | 37.27 | −24.53 | 30.81 | 40.59 (1)a | <.001* | .144 | |
| See a counselor for the first time after more than 1 month. | 9.57 | 32.15 | −40.18 | 26.95 | 132.46 (1)a | <.001* | .355 | |
|
| ||||||||
| 10. Location | .199 | 19.78 (3,239) | <.001 | .199 | ||||
| Building or office in the community that specializes in mental health services. | 24.92 | 31.82 | 39.42 | 23.42 | 13.71 (1)a | <.001* | .054 | |
| Youth cafe and recreation centre. | 5.32 | 35.63 | 23.40 | 30.13 | 14.08 (1)a | <.001* | .055 | |
| Hospital or doctor’s office. | −1.59 | 35.05 | −34.07 | 33.87 | 38.53 (1) | <.001* | .138 | |
| School setting. | −28.65 | 31.14 | −28.75 | 26.16 | .001 (1)a | .981 | .000 | |
|
| ||||||||
| 11. Engagement | .151 | 14.14 (3,239) | <.001 | .151 | ||||
| Youth and caregivers give feedback, e.g., anonymous surveys. | −27.64 | 40.31 | −1.34 | 35.14 | 22.26 (1) | <.001* | .085 | |
| Youth and caregivers are on staff at the organization. | 0.12 | 24.15 | −20.38 | 22.19 | 34.87 (1) | <.001* | .126 | |
| Youth and caregivers are on an advisory group that gives feedback on services and evaluation. | −1.48 | 21.73 | 7.11 | 16.54 | 9.87 (1)a | .002* | .039 | |
| Youth and caregivers play a leadership role in making decisions for the organization. | 29.01 | 31.07 | 14.62 | 27.09 | 11.21 (1) | <.001* | .044 | |
|
| ||||||||
| 12. Information Sharing | .285 | 31.83 (3,239) | <.001 | .285 | ||||
| No sharing of personal information with caregivers. | −27.31 | 34.56 | −31.72 | 28.74 | .909 (1)a | .341 | .004 | |
| All personal information is available to caregivers, with youth consent. | 19.20 | 31.99 | −20.11 | 28.68 | 75.77 (1) | <.001* | .239 | |
| Service provider decides what information to share with caregivers, with youth consent. | 2.01 | 29.74 | 1.62 | 23.72 | .010 (1) | .919 | .000 | |
| Youth and service provider work together to decide what personal information to share with caregivers and how that can be helpful. | 6.11 | 38.17 | 50.21 | 33.96 | 67.77 (1) | <.001* | .219 | |
Levene’s test of equality of error variance statistically significant
Statistically significant at the Bonferroni corrected p-value of .0125
Core Health Services. Both groups most preferred “Mental health and substance misuse counseling, medication management, and physical/sexual health” over all other combinations of core health service options, with no significant differences in preference between groups.
Other Services. Both groups most preferred a “Choice of education, employment, housing, income support, and legal support services” within this level, with no significant differences in preference between groups.
Caregiver Involvement. Both groups showed the greatest preference for the level “Caregivers involved in family counseling with youth, with youth consent,” with no statistically significant differences in preference between groups.
Peer Support. Both groups most preferred that “Youth can be matched to an ongoing trained peer support worker to learn life skills and help them with services they need.” However, justice-involved youth found this level significantly more desirable than non-justice-involved youth, representing a large effect.
Cultural Sensitivity. Justice-involved youth demonstrated the strongest preference for the level “Can ask for a service provider with a certain cultural background, when available.” Non-justice-involved youth demonstrated the strongest preference for the level “Services are culturally sensitive and trauma-informed,” in contrast, justice-involved youth preferred this level least, with differences between groups reaching statistical significance and a large effect size.
E-Health Services. Non-justice-involved deemed “E-health services are offered 24/7 alongside in-person services during office hours” as most preferable, however, justice-involved youth found it significantly less preferable, giving most preference to the level “Can schedule or reschedule appointments via email, text or online.” Notably, “E-health services are offered 24/7 alongside in-person services during office hours” was the most preferred level among all 48 levels for non-justice-involved youth.
Age Range. Both groups most preferred “Services for ages 12–29, in a setting that also has services for adults 29+.” However, non-justice-involved youth preferred this age range significantly more than justice-involved youth.
Time of Appointments. Statistically significant group differences were found across all four levels within this attribute, with small to large effect sizes. Justice-involved youth showed preference for appointment times Monday to Friday, 9AM–5PM. In contrast, non-justice-involved youth showed preference for Monday to Friday, 9AM–9PM.
Wait Time. Statistically significant group differences were found across all four levels within this attribute, with predominantly large effect sizes. Justice-involved youth most preferred to “See a counselor for the first time after about 72 hours.” In contrast, non-justice-involved youth most preferred seeing a counselor immediately, with longer wait times given increasingly less preference across the levels.
Location. Both groups most preferred that the location of services be offered in a “Building or office in the community that specializes in mental health services,” however, non-justice involved youth preferred this significantly more than justice-involved youth.
Engagement. Statistically significant group differences were found across all four levels within this attribute, with small to large effect sizes. Both groups most preferred that “Youth and caregivers play a leadership role in making decisions for the organization,” with justice-involved youth preferring this significantly more than non-justice-involved youth. Notably, this preference to play a leadership role was among justice-involved youth’s top five most preferred levels.
Information Sharing. Justice-involved you preferred that “All personal information is available to caregivers, with youth consent” most, while non-justice involved youth found this significantly less preferable, representing a large effect. Rather, non-justice-involved youth preferred that “Youth and service provider work together to decide what personal information to share with caregivers and how that can be helpful,” while justice-involved youth found this significantly less preferable, also representing a large effect.
Stage 4
Results from the simulation are presented in Table 4. The randomized first choice simulation demonstrated that when justice-involved youths’ top preferred level within each of the 12 attributes is included in a hypothetical IYS scenario (i.e., Scenario 1), 71.3% of justice-involved youth preferred the model, compared to a mere 6.4% of non-justice-involved youth. When non-justice-involved youths top preferred level within each of the 12 attributes was included in a hypothetical IYS scenario (i.e., Scenario 2), preference for the model increased substantially among non-justice-involved youth, to 93.6%. In contrast, preference for the model decreased among non-justice-involved youth, to 28.7%.
Table 4.
Randomized first choice simulation results of each group’s ideal IYS scenario, with standard errors and 95% confidence intervals
| Non-Justice-Involved Youth n = 55 | Justice-Involved Youth n = 188 | |||||
|---|---|---|---|---|---|---|
|
|
|
|||||
| Shares of Preference | SE | 95% CI | Shares of Preference | SE | 95% CI | |
| Scenario 1 | 71.3% | 5.2% | 61.2%–81.4% | 6.4% | 1.4% | 3.6%–9.1% |
| Scenario 2 | 28.7% | 5.2% | 18.6%–38.8% | 93.6% | 1.4% | 90.9%–96.4% |
SE = Standard Error
CI = 95% Confidence Interval
Scenario 1 refers to when the most preferred level of justice-involved youth is implemented across all 12 attributes
Scenario 2 refers to when the most preferred level of non-justice-involved youth is implemented across all 12 attributes
Discussion
This study used a conjoint analysis to examine the IYS preferences of justice-involved youth, contrasting their preferences to those of non-justice-involved youth. The ultimate goal of this study was to understand what service aspects may promote access to care in justice-involved youth, in order to inform IYS design in Ontario.
This study revealed consensus on a variety of top IYS preferences among justice-involved and non-justice involved youth, which can inform IYS models in Ontario. It is clear that justice-involved and non-justice-involved youth alike wish to see an array of core health services that includes mental health and substance misuse counseling, medication management, and physical/sexual health. This is consistent with findings from the larger Ontario-wide study (32), from which this study’s data are drawn, as well as other literature exploring the service preferences of youth (22). Furthermore, all youth are unanimous in their preference for a broad range of additional IYS services, namely, education, employment, housing, income support, and legal support services. Because continued disengagement in these domains may exacerbate MHS difficulties (41), connecting both justice-involved and non-justice-involved youth with support in these areas is paramount. In the context of strained resources and service limitations, these results highlight areas for service prioritization to best respond to the service preferences of justice-involved youth.
Findings from this study also demonstrate that fast access to care is a priority among both justice-involved and non-justice-involved youth, which reflects literature to date (32, 42, 43). Incorporation of e-health services was also a high preference among justice-involved and non-justice-involved youth, consistent with other research exploring service preferences of youth across justice-involved and non-justice-involved populations (44). Finally, both youth groups preferred that the location of services be offered in a community setting that specializes in mental health services, in comparison with school, medical, and community settings. This is consistent with Henderson and colleagues (32) findings that youth across latent classes prefer community-based care, as well as other IYS models that use community-based settings to increase accessibility to MHS care (20, 45).
While support for the above foundational aspects to IYS care was found, so were preferences that clearly distinguish justice-involved youth from their non-justice-involved counterparts. Among the most important of these distinctions were justice-involved youth prioritization of peer support, and engagement in IYS by playing a leadership role. Indeed, justice-involved youth strongly preferred ongoing support from a trained peer support worker. This parallels research that demonstrates the importance of peer support at this developmental stage (46), and the preference of many youth to speak with peers rather than psychologists or psychiatrists in mental health services (47), which appear to be particularly strong among justice involved youth. Notably, positive peer mentorship, often provided by an older youth with former involvement in the criminal justice system (48, 49), may serve to reduce MHS stigma, a major barrier to treatment among justice-involved youth. Furthermore, the limited research conducted in this area suggests that peer mentorship of justice-involved youth may improve protective factors and reduce recidivism (48).
Engagement in an IYS leadership role was also a preference among justice-involved youth. This preference is distinct from non-justice-involved youth, in which engagement in any form was among the lowest preferred service characteristics. Engaging justice-involved youth in an IYS leadership role could have substantial benefits, including skill acquisition, empowerment, and social engagement (50, 51). Engagement may also impact positive development through the mentorship of prosocial adults, which in turn can foster a sense of connectedness to community and increase social trust (52, 53). Youth engagement in the design and delivery of IYS services may also make services more relevant to other youth (54), potentially enhancing the effectiveness and efficiency of services.
Model Simulation
Findings from model simulation support the need for flexible options that would enhance engagement among justice-involved youth. For example, an IYS that includes the option to work with an ongoing trained peer support worker would be attractive to nearly three-quarters of justice-involved youth, suggesting that services that incorporate this feature may increase the likelihood of engaging justice-involved youth and hence, the outcomes they achieve. However, an IYS model based on justice-involved youth preferences would be far less acceptable to non-justice-involved youth. Conversely, an IYS model based on non-justice-involved youth preferences would be acceptable to only 28.7% of justice-involved youth based on the simulation. This highlights the potential drawbacks in approaching Ontario IYS models as a “one-size-fits-all” service, and the benefit of creating flexible options for justice-involved and non-justice-involved youth in one location.
The need for flexible integrated services is consistent with Henderson and colleagues (32) call for a multitude of diverse services to meet the IYS preferences of Ontario youth. This finding also parallels literature regarding the importance of youth accessing fundamental elements of IYS (e.g., fast access to MHS services), as well as the incorporation of specific services based on youth need and local feasibility (e.g., peer support; 20). Fortunately, justice-involved and non-justice-involved youth have consensus on many of their top priorities, therefore the incorporation of flexible options would be relatively minor. For example, in addition to options for peer support and engagement, e-health services may be used for appointment scheduling (a preferences of justice-involved youth), or to supplement in-person services (a preference of non-justice-involved youth). Constellations of effective services that align with the preferences of justice-involved youth hold the potential to attract a greater proportion of youth to access services, to encourage them to stay in services longer, and to produce more favorable outcomes.
Limitations
A limitation to this study is that justice-involved youth participants were not representative of the general justice-involved youth population in Ontario (55, 56). Most justice-involved youth in the present sample were White, reported a somewhat high SES, lived in rural to small population centres, and were engaged in employment and education, which is not consistent with Canadian statistics (56). These sociodemographic irregularities may be a sampling issue. For example, recruitment flyers for these studies were circulated among community agencies that serve youth with MHS needs. If justice-involved youth are not engaging in these agencies, recruitment efforts would not have reached them. Furthermore, it is also possible that fewer black, Indigenous, and people of colour (BIPOC) who are justice-involved youth do not identify as having MHS challenges (57). Not identifying as having MHS challenges may result in self-selection out of the study. It is imperative that future research continue to develop strategies to engage justice-involved youth, specifically BIPOC youth samples, in order to give marginalized populations a voice and increase the ecological validity of findings (51).
A further limitation to these studies is that a small sample size and low statistical power prohibited participants from being matched on sociodemographic factors such as gender, where there was a large unequal representation between justice-involved and non-justice involved youth groups. Similarly, moderator analyses could not be conducted to analyze within-group differences in various sociodemographic variables. Although the study was piloted with youth and appeared to be understood, it is possible that the formulation of the question introduced a confound by querying the participants about their preferences for youth in general rather than specifically for themselves. It should also be noted conjoint analysis findings should not be the sole source of information to design services, as local engagement and other sources of evidence are also paramount. Future research may wish to address these limitations in order to answer research questions with more precision.
Data for this study were collected prior to the COVID-19 pandemic. Impacts of the pandemic on youth mental health and substance use (58), as well as changes to service delivery models in general (57, 58, 59), could have an impact on the future MHS service preferences of youth and caregivers. As such, a replication of this study in post-pandemic times is warranted.
Conclusion
This was the first known study to examinee the specific IYS component preferences of justice-involved youth. Like their non-justice-involved counterparts, justice-involved youth exhibited preferences for fast access to a broad range core health and additional services in a community setting, that incorporates e-health services. These service characteristics should form the foundation of IYS care in Ontario. In addition, the option to work with a trained peer support worker, and to play a leadership role in making decisions for IYS organizations, may be important to engage justice-involved youth in a trauma-informed manner that enables them to contribute safely. An IYS model that is designed to include these elements, in addition to flexible options in peer support and engagement, has the potential to enhance service utilization in justice-involved youth, a notoriously underserved population.
Footnotes
Conflict of Interest
This research was funded by the Canadian Institutes of Health Research, the Rx and D Health Research Fund, and the Ontario Centre of Excellence for Child and Youth Mental Health. Dr. J.L. Henderson is the Executive Director of Youth Wellness Hubs Ontario. The authors have no financial relationships or other ties to disclose.
References
- 1.Georgiades K, Duncan L, Wang L, Comeau J, Boyle MH. Six-month prevalence of mental disorders and service contacts among children and youth in Ontario: evidence from the 2014 Ontario child health study. The Canadian Journal of Psychiatry. 2019;64(4):246–255. doi: 10.1177/0706743719830024. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Pearson C, Janz T, Ali J. Statistics Canada. Ottawa: Statistics Canada; 2013. Mental and Substance Use Disorders in Canada. Available from: https://www150.statcan.gc.ca/n1/pub/82-624-x/2013001/article/11855-eng.htm. [Google Scholar]
- 3.Borschmann R, Janca E, Carter A, Willoughby M, Hughes N, Snow K, et al. The health of adolescents in detention: a global scoping review. The Lancet Public Health. 2020;5(2):e114–e126. doi: 10.1016/S2468-2667(19)30217-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Livanou M, Furtado V, Winsper C, Silvester A, Singh SP. Prevalence of mental disorders and symptoms among incarcerated youth: a meta-analysis of 30 studies. International Journal of Forensic Mental Health. 2019;18(4):400–414. doi: 10.1080/14999013.2019.1619636. [DOI] [Google Scholar]
- 5.Auerbach RP, Alonso J, Axinn WG, Cuijpers P, Ebert DD, Green JG, et al. Mental disorders among college students in the world health organization world mental health surveys. Psychological Medicine. 2016;46(14):2955–2970. doi: 10.1017/S0033291716001665. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Brown A, Lubman DI, Paxton SJ. Reducing sexually-transmitted infection risk in young people with first-episode psychosis. International Journal of Mental Health Nursing. 2011;20(1):12–20. doi: 10.1111/j.1447-0349.2010.00700.x. [DOI] [PubMed] [Google Scholar]
- 7.Rosenberg HJ, Vance JE, Rosenberg SD, Wolford GL, Ashley SW, Howard ML. Trauma exposure, psychiatric disorders, and resiliency in juvenile-justice-involved youth. Psychological Trauma: Theory, Research, Practice, and Policy. 2014;6(4):430–437. doi: 10.1037/a0033199. [DOI] [Google Scholar]
- 8.Yonek JC, Dauria EF, Kemp K, Koinis-Mitchell D, Marshall BDL, Tolou-Shams M. Factors associated with use of mental health and substance use treatment services by justice-involved youths. Psychiatric Services. 2019;70(7):586–595. doi: 10.1176/appi.ps.201800322. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Cosgrave EM, Yung AR, Killackey E, Buckby JA, Godfrey KA, Stanford CA, et al. Met and unmet need in youth mental health. Journal of Mental Health. 2008;17(6):618–628. doi: 10.1080/09638230701506267. [DOI] [Google Scholar]
- 10.Hoeve M, McReynolds LS, Wasserman GA. Service referral for juvenile justice youths: associations with psychiatric disorder and recidivism. Administration and Policy in Mental Health and Mental Health Services Research. 2013;41(3):379–389. doi: 10.1007/s10488-013-0472-x. [DOI] [PubMed] [Google Scholar]
- 11.Kessler RC, Berglund P, Demler O, Jin R, Merikangas KR, Walters EE. Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the national comorbidity survey replication. Archives of General Psychiatry. 2005;62(6):593. doi: 10.1001/archpsyc.62.6.593. [DOI] [PubMed] [Google Scholar]
- 12.Kuehn BM. Mental illness takes heavy toll on youth. JAMA. 2005;294(3):293. doi: 10.1001/jama.294.3.293. [DOI] [PubMed] [Google Scholar]
- 13.Cuellar AE, McReynolds LS, Wasserman GA. A cure for crime: can mental health treatment diversion reduce crime among youth? Journal of Policy Analysis and Management. 2005;25(1):197–214. doi: 10.1002/pam.20162. [DOI] [PubMed] [Google Scholar]
- 14.Liebenberg L, Ungar MA. A comparison of service use among youth involved with juvenile justice and mental health. Children and Youth Services Review. 2014;39:117–122. doi: 10.1016/j.childyouth.2014.02.007. [DOI] [Google Scholar]
- 15.Farrington DP, Gaffney H, Ttofi MM. Systematic reviews of explanatory risk factors for violence, offending, and delinquency. Aggression and Violent Behavior. 2017;33:24–36. doi: 10.1016/j.avb.2016.11.004. [DOI] [Google Scholar]
- 16.Scott T, Brown SL. Risks, strengths, gender, and recidivism among justice-involved youth: a meta-analysis. Journal of Consulting and Clinical Psychology. 2018;86(11):931–945. doi: 10.1037/ccp0000343. [DOI] [PubMed] [Google Scholar]
- 17.Teplin LA, Abram KM, McClelland GM, Washburn JJ, Pikus AK. Detecting mental disorder in juvenile detainees: who receives services. American Journal of Public Health. 2005;95(10):1773–1780. doi: 10.2105/AJPH.2005.067819. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.White LM, Aalsma MC, Salyers MP, Hershberger AR, Anderson VR, Schwartz K, et al. Behavioral health service utilization among detained adolescents: a meta-analysis of prevalence and potential moderators. Journal of Adolescent Health. 2019;64(6):700–708. doi: 10.1016/j.jadohealth.2019.02.010. [DOI] [PubMed] [Google Scholar]
- 19.Henderson JL, Cheung A, Cleverley K, Chaim G, Moretti ME, de Oliveira C, et al. Integrated collaborative care teams to enhance service delivery to youth with mental health and substance use challenges: protocol for a pragmatic randomised controlled trial. BMJ Open. 2017;7(2):e014080. doi: 10.1136/bmjopen-2016-014080. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.McGorry PD, Mei C, Chanen A, Hodges C, Alvarez-Jimenez M, Killackey E. Designing and scaling up integrated youth mental health care. World Psychiatry. 2022;21(1):61–76. doi: 10.1002/wps.20938. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Settipani C, Hawke LD, Cleverley K, Chaim G, Cheung A, Mehra K, et al. Key attributes of integrated community-based youth service hubs for mental health: a scoping review. International Journal of Mental Health Systems. 2019;13(1) doi: 10.1186/s13033-019-0306-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Kozloff N, Cheung AH, Ross LE, Winer H, Ierfino D, Bullock H, et al. Factors influencing service use among homeless youths with co-occurring disorders. Psychiatric Services. 2013;64(9):925–928. doi: 10.1176/appi.ps.201200257. [DOI] [PubMed] [Google Scholar]
- 23.Åström T, Bergström M, Håkansson K, Jonsson AK, Munthe C, Wirtberg I, et al. Treatment foster care oregon for delinquent adolescents: a systematic review and meta-analysis. Research on Social Work Practice. 2019;30(4):355–367. doi: 10.1177/1049731519890394. [DOI] [Google Scholar]
- 24.Owen MC, Wallace SB, Alderman EM, Chung R, Grubb L, Lee J, et al. Advocacy and collaborative health care for justice-involved youth. Pediatrics. 2020;146(1) doi: 10.1542/peds.2020-1755. [DOI] [PubMed] [Google Scholar]
- 25.Littell JH, Pigott TD, Nilsen KH, Green SJ, Montgomery OLK. Multisystemic Therapy® for social, emotional, and behavioural problems in youth age 10 to 17: an updated systematic review and meta-analysis. Campbell Systematic Reviews. 2021;17(4) doi: 10.1002/cl2.1158. [DOI] [Google Scholar]
- 26.Halsall T, Manion I, Iyer SN, Mathias S, Purcell R, Henderson J. Trends in mental health system transformation: integrating youth services within the Canadian context. Healthcare Management Forum. 2019;32(2):51–55. doi: 10.1177/0840470418808815. [DOI] [PubMed] [Google Scholar]
- 27.Stathis SL, Letters P, Doolan I, Whittingham D. Developing an integrated substance use and mental health service in the specialised setting of a youth detention centre. Drug and Alcohol Review. 2006;25(2):149–155. doi: 10.1080/09595230500537613. [DOI] [PubMed] [Google Scholar]
- 28.Barrett JG, Janopaul-Naylor E. Description of a collaborative community approach to impacting juvenile arrests. Psychological Services. 2016;13(2):133–139. doi: 10.1037/ser0000066. [DOI] [PubMed] [Google Scholar]
- 29.Orme BK. Getting Started with Conjoint Analysis: Strategies for Product Design and Pricing Research. New York: Research Publisher; 2014. [Google Scholar]
- 30.Phillips KA, Johnson FR, Maddala T. Measuring what people value: a comparison of “attitude” and “preference” surveys. Health Services Research. 2002;37(6):1659–1679. doi: 10.1111/14756773.01116. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.McGrady ME, Pai ALH, Prosser LA. Using discrete choice experiments to develop and Deliver patient-centered psychological interventions: a systematic review. Health Psychology Review. 2020;15(2):314–332. doi: 10.1080/17437199.2020.1715813. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Henderson J, Hawke LD, Iyer SN, Hayes E, Darnay K, Mathias S, et al. Youth perspectives on integrated youth services: a discrete choice conjoint experiment. The Canadian Journal of Psychiatry. 2021;67(7):524–533. doi: 10.1177/07067437211044717. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Hawke LD, Thabane L, Iyer SN, Jaouich A, Reaume-Zimmer P, Henderson J. Service providers endorse integrated services model for youth with mental health and substance use challenges: findings from a discrete choice experiment. BMC Health Services Research. 2021;21(1) doi: 10.1186/s12913-021-07038-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Hawke LD, Thabane L, Wilkins L, Mathias S, Iyer SN, Henderson J. Don’t forget the caregivers! a discrete choice experiment examining caregiver views of integrated youth services. The Patient: Patient-Centered Outcomes Research. 2021;14(6):791–802. doi: 10.1007/s40271021-00510-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Henderson Jl, Chaim G, Hawke Ld. Screening for substance use and mental health problems in a cross-sectoral sample of Canadian youth. International Journal of Mental Health Systems. 2017;11(1) doi: 10.1186/s13033-017-0128-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Watson P, Mehra K, Hawke LD, Henderson J. Service provision for depressed children and youth: a survey of the scope and nature of services in Ontario. BMC Health Services Research. 2019;19(1) doi: 10.1186/s12913-019-4784-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Sawtooth Software Inc. Lighthouse Studio, Version 9.6: Software for Web Interviewing and Conjoint Analysis. Provo: Author; 2018. [Google Scholar]
- 38.Dennis M, Chan Y, Funk R. Development and validation of the GAIN short screener (GSS) for internalizing, externalizing and substance use disorders and crime/violence problems among adolescents and adults. American Journal on Addictions. 2006;15(s1):80–91. doi: 10.1080/10550490601006055. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Khanano R, Barbic S, Henderson J, Mathias S, Richardson CG. Reliability and concurrent validity of the GAIN short screener among youth utilizing integrated health services. Journal of the Canadian Academy of Child and Adolescent Psychiatry. 2021;30(2):82–91. [PMC free article] [PubMed] [Google Scholar]
- 40.Smith T, Hawke LD, Chaim G, Henderson J. Housing instability and concurrent substance use and mental health concerns: an examination of Canadian youth. Journal of the Canadian Academy of Child and Adolescent Psychiatry. 2017;26(3):214–223. [PMC free article] [PubMed] [Google Scholar]
- 41.Goldman-Mellor S, Caspi A, Arseneault L, Ajala N, Ambler A, Danese A, et al. Committed to work but vulnerable: self-perceptions and mental health in NEET 18-year olds from a contemporary British cohort. Journal of Child Psychology and Psychiatry. 2015;57(2):196–203. doi: 10.1111/jcpp.12459. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Becker MPE, Christensen BK, Cunningham CE, Furimsky I, Rimas H, Wilson F, et al. Preferences for early intervention mental health services: a discrete-choice conjoint experiment. Psychiatric Services. 2016;67(2):184–191. doi: 10.1176/appi.ps.201400306. [DOI] [PubMed] [Google Scholar]
- 43.Becker MPE, Cunningham CE, Christensen BK, Furimsky I, Rimas H, Wilson F, et al. Investigating service features to sustain engagement in early intervention mental health services. Early Intervention in Psychiatry. 2017;13(2):241–250. doi: 10.1111/eip.12470. [DOI] [PubMed] [Google Scholar]
- 44.Munson MR, Lox JA. Clinical social work practice with former system youth with mental health needs: perspective of those in need. Clinical Social Work Journal. 2012;40(2):255–260. doi: 10.1007/s10615-012-0381-6. [DOI] [Google Scholar]
- 45.Wang A, Tobon JI, Bieling P, Jeffs L, Colvin E, Zipursky RB. Rethinking service design for youth with mental health needs: the development of the youth wellness centre, St. Joseph’s Healthcare Hamilton. Early Intervention in Psychiatry. 2019;14(3):365–372. doi: 10.1111/eip.12904. [DOI] [PubMed] [Google Scholar]
- 46.Martin CE, Houston AM, Mmari KN, Decker MR. Urban teens and young adults describe drama, disrespect, dating violence and help-seeking preferences. Maternal and Child Health Journal. 2011;16(5):957–966. doi: 10.1007/s10995-011-0819-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Cunningham CE, Zipursky RB, Christensen BK, Bieling PJ, Madsen V, Rimas H, et al. Modeling the mental health service utilization decisions of university undergraduates: a discrete choice conjoint experiment. Journal of American College Health. 2017;65(6):389–399. doi: 10.1080/07448481.2017.1322090. [DOI] [PubMed] [Google Scholar]
- 48.Buck G. Peer Mentoring in Criminal Justice. London: Routledge; 2020. [DOI] [Google Scholar]
- 49.Lopez-Humphreys M, Teater B. Peer mentoring justice-involved youth: a training model to promote secondary desistance and restorative justice among mentors. The International Journal of Restorative Justice. 2018;1(2):187–209. doi: 10.5553/IJRJ/258908912018001002002. [DOI] [Google Scholar]
- 50.Checkoway B, Richards-Schuster K. Youth participation in community evaluation research. The American Journal of Evaluation. 2003;24(1):21–33. doi: 10.1016/S1098-2140(02)00268-0. [DOI] [Google Scholar]
- 51.Powers JL, Tiffany JS. Engaging youth in participatory research and evaluation. Journal of Public Health Management and Practice. 2006;12:S79–S87. doi: 10.1097/00124784-200611001-00015. [DOI] [PubMed] [Google Scholar]
- 52.Suleiman AB, Soleimanpour S, London J. Youth action for health through youth-led research. Journal of Community Practice. 2006;14(1–2):125–145. doi: 10.1300/J125v14n01_08. [DOI] [Google Scholar]
- 53.Zeldin S, Christens BD, Powers JL. The psychology and practice of youth-adult partnership: bridging generations for youth development and community change. American Journal of Community Psychology. 2012;51(3–4):385–397. doi: 10.1007/s10464-012-9558-y. [DOI] [PubMed] [Google Scholar]
- 54.Hawke LD, Mehra K, Settipani C, Relihan J, Darnay K, Chaim G, et al. What makes mental health and substance use services youth friendly? A scoping review of literature. BMC Health Services Research. 2019;19(1) doi: 10.1186/s12913-019-4066-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Henderson J, Hawke LD, Chaim G. Not in employment, education or training: mental health, substance use, and disengagement in a multi-sectoral sample of service-seeking Canadian youth. Children and Youth Services Review. 2017;75:138–145. doi: 10.1016/j.childyouth.2017.02.024. [DOI] [Google Scholar]
- 56.Public Safety Canada. A statistical snapshot of youth at risk and youth offending in Canada. Ottawa: National Crime Prevention Centre; 2012. Available from: https://www.publicsafety.gc.ca/cnt/rsrcs/pblctns/ststclsnpsht-yth/ssyr-eng.pdf. [Google Scholar]
- 57.Samuel IA. Utilization of mental health services among African-American male adolescents released from juvenile detention: examining reasons for within-group disparities in help-seeking behaviors. Child and Adolescent Social Work Journal. 2014;32(1):33–43. doi: 10.1007/s10560-014-0357-1. [DOI] [Google Scholar]
- 58.Hawke LD, Barbic SP, Voineskos A, Szatmari P, Cleverley K, Hayes E, et al. Impacts of COVID-19 on youth mental health, substance use, and well-being: a rapid survey of clinical and community samples: Répercussions de la COVID-19 sur la santé mentale, l’utilisation de substances et le bien-être des adolescents: un sondage rapide d’échantillons cliniques et communautaires. The Canadian Journal of Psychiatry. 2020;65(10):701–709. doi: 10.1177/0706743720940562. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Hawke LD, Sheikhan NY, MacCon K, Henderson J. Going virtual: youth attitudes toward and experiences of virtual mental health and substance use services during the COVID-19 pandemic. BMC Health Services Research. 2021;21(1) doi: 10.1186/s12913-021-06321-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.Marcelin LH, Cela T, Dembo R, Jean-Gilles M, Page B, Demezier D, et al. Remote delivery of a therapeutic intervention to court-mandated youths of Haitian descent during COVID-19. Journal of Community Psychology. 2021;49(7):2938–2958. doi: 10.1002/jcop.22559. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Nicholas J, Bell IH, Thompson A, Valentine L, Simsir P, Sheppard H, et al. Implementation lessons from the transition to telehealth during COVID-19: a survey of clinicians and young people from youth mental health services. Psychiatry Research. 2021;299:113848. doi: 10.1016/j.psychres.2021.113848. [DOI] [PMC free article] [PubMed] [Google Scholar]