Abstract
Background:
The level of maternal satisfaction with delivery services significantly affects health service utilization among women. Ethiopia’s healthcare system and health facilities’ quality have not much improved, which may contribute to women’s generally poor levels of satisfaction and there was a limited study about client satisfaction on delivery services in the study area. Thus, the purpose of this study was to assess level of maternal satisfaction with delivery service and its associated factors among women who gave birth in Tullo Woreda public health facilities, Eastern Ethiopia.
Methods:
A facility-based cross-sectional study was conducted from 1 to 30 September 2020 among 355 women who gave birth in Tullo Woreda public health facilities, Eastern Ethiopia Data were collected using a pretested structured questionnaire through a face-to-face interview and entered into Epidata version 3.1 and analyzed using statistical package for the social sciences (SPSS) version 25. The prevalence was reported using a 95% confidence interval and summary measures. Predictors were assessed using a multivariable logistic regression analysis model and reported using an adjusted odds ratio with 95% CI. Statistical significance was declared at a p-value of <0.05.
Results:
The overall satisfaction of mothers on delivery service was 33.5% (95% CI: 27.81, 39.13). Factors such as having no antenatal care (ANC) for the index pregnancy (AOR = 0.33; 95% CI: 0.19, 0.56), women who came to health centers on foot (AOR = 0.17; CI: 0.04, 0.74) and by auto-rickshaw (AOR = 0.16; 95 % CI: 0.04, 0.64), mothers who did not satisfied with toilet service at the delivery room (AOR = 0.49; 95% CI: 0.12, 0.86) and who were not satisfied with maternal drugs availability (AOR = 0.65; 95% CI: 0.11, 0.95) were predictors of maternal satisfaction.
Conclusions:
This study pointed out that only 33.5% of women were satisfied with delivery care services provided in public health facilities of the study area. Factors such as not having ANC, using foot and auto-rickshaw as means of transportation, availability of drugs, and toilets were predictor of maternal satisfactions. Awareness creation for the benefit of ANC follow-up and delivery in the health facilities and providing safe transportation during referral time may help mothers get a timely healthcare service, which may increase client satisfaction. The concerned entities must pay attention in timely availability of drugs and improving the toiles, which play a role in shaping and molding level of satisfaction of women.
Keywords: Delivery care service, quality service, pregnancy, health facility, Ethiopia
Introduction
Maternal satisfaction with delivery service is a crucial and frequently used metric for assessing the quality of healthcare services. 1 Women’s opinions of high-quality treatment have an impact on their level of satisfaction with childbirth, which is a multifaceted issue. However, it offers significant and affordable feedback for enhancing institutional childbirth care. 2
The level of maternal satisfaction with delivery services significantly affects health service utilization among women. According to a report in Ethiopia, the prevalence of institutional delivery among women was 48% in a health facility, which may be associated with the level of satisfaction. 3 This low prevalence of institutional delivery increases the maternal death rate, which occurs during labor and delivery and immediately postpartum as there is no care for the woman and child. 4 Maternal satisfaction with delivery services can also have a significant impact on women’s mental health. 5
Evidence showed that different factors significantly affect the level of maternal satisfaction with delivery services. Factors like mothers’ education level, occupational status, family income level, birth outcome, interpersonal interaction with care providers, privacy, and postpartum hospital stay all significantly affect women’s childbirth services satisfaction.2,6–8
The Federal Ministry of Health has increasingly focused on improving the quality of care over the past few years. This is evident in the Health Sector Development Plan IV, which discusses various elements of quality, including accelerating the speed of delivery, and identifies maternal and child health as five priority public health areas where the need is great. 9 Despite these efforts, Ethiopia’s healthcare system and health facilities’ quality have not much improved since the strategies of the health sector plan of Ethiopia, which may contribute to women’s generally poor levels of satisfaction.10,11
Despite different studies reporting the level of satisfaction, it is inconsistent and not at its expected level. The level of maternal satisfaction in Jimma, Ethiopia was 78.7%, 12 in eastern Ethiopia 80%, 8 in Addis Ababa, Ethiopia 63%, 6 and in west Shoa, Ethiopia 83.9%. 7 In addition, factors that affect women’s satisfaction with delivery care services are not consistent. Variable-like modes of delivery are inconsistent among different studies.7,8 Furthermore, maternal satisfaction is a crucial quality outcome indicator for healthcare providers and settings, particularly during labor and birth, as it significantly impacts the overall quality of care. 13
Moreover, evidence on mother satisfaction with service delivery aids in identifying other aspects of care that should be improved in Ethiopian contexts in order to meet long-term demand, generate notable modifications in the maternal care-seeking behavior, and pinpoint obstacles that ought to be eliminated. Therefore, this study aimed to assess the level of maternal satisfaction and its associated factors among delivered women in West Hararge Zone public health facilities.
Methods and materials
Study design, setting, and period
An institutional based cross-sectional study was conducted from 1 to 30 September 2020 among women gave birth at Tullo Woreda Public Health Facilities, Eastern Ethiopia. Tullo woreda is located in Oromia region, Eastern Ethiopia, at a distance of 375 km from Addis Ababa, Country’s capital city. According to the recent woreda health office report, the projected population size of the district was 205,572 and the district made up of three urban and 30 rural kebeles (smallest administrative units). There are 39 public health facilities (one primary hospital, eight health centers, and 30 Health Posts) available in the Woreda. Besides, private health institutions such as five rural drug venders, seven drug stores, 12 primary and two medium clinics, and two traditional healers were providing service at this woreda. Although a COVID-19 pandemic occurred during the course of this study, all facilities in the study area were required to provide services in accordance with guidelines and best practices for COVID-19 control and prevention. We used the Strengthening the Reporting of Observational Studies in Epidemiology cross-sectional checklist when writing our report. 14
Population and eligibility criteria
The source population of the study was all women who gave birth in public health facilities where as randomly selected women who gave birth in selected public health facilities were the study population. Women who gave birth in selected public health facilities during data collection time were included in the study, and women who were mentally or critically ill and unable to provide the necessary information were excluded from the study.
Data collection methods
The data were collected by a pretested, structured questionnaire adapted from various literatures was used to collect data from the study participants.6,7,15–18 The data collection technique was interviewer-administered by trained data collectors. The data were collected by six BSc Nurse Health professionals who fluently speak Afaan Oromo (the local language). The questionnaire contains socio-demographic and economic characteristics, health service-related factors, and obstetric-related factors. Supervision was conducted by the principal investigator and two public health experts familiar with the study setting. Data collectors and supervisors were trained for 2 days on ethics, tool sampling, and data collection procedures. The data collection process was supervised on a daily basis, and timely feedback was communicated to the data collectors. Statistically, we performed Cronbach’s alpha, which is a measure used to assess the quality of our employed instruments. The result was 0.87, which was within acceptable ranges.
Variables and measurement
Satisfaction is defined as the fulfillment of a need or want. It was measured based on a five-point Likert scales, which are named very satisfied, satisfied, unsure, dissatisfied, and very dissatisfied. Clients were categorized as “not satisfied” if they scored below 75% of score calculated from the satisfaction measuring items and “satisfied” if their satisfaction was 75% or above from the satisfaction measuring items. The analysis of internal reliability was done using Cronbach’s α to check whether the items are internally consistent. If the result of Cronbach’s α is ⩾0.9 then the internal consistency is excellent, 0.8 ⩽ α < 0.9 as good, and 0.7 ⩽ α < 0.8 acceptable.
Satisfied: Just one’s expectation on delivery care provided. 19
Dissatisfied: Below women’s expectation of received delivery care. 20
Quality health care: A care which is safe, reliable, patient centered, efficient and provided to all in need in an equitable and timely manner. 21
Waiting time: Perceived time interval from arrival of the mother at the hospital/health center until first registered. The actual waiting time is less than 30 min. 12
Bias
There were a number of biases involved while conducting this research and researcher took explicit measure to avoid them. One of the bias was social desirability bias is when respondents responded satisfied with their appearance to healthcare providers or others, believing it made them appear good. To avoid this bias, the researchers paraphrases the questions in the way that was not socially desirable and allowing a participants to answer freely and openly without fear of judgment from another person. In addition, the data collectors were not employees of the selected facilities, and the exit interview was done away from the delivery unit.
Sample size determination and sampling procedures
Sample size was calculated using double population proportion using Epi-Info version 7 after considering significant factors such as ANC follow-up, 19 unwanted status of pregnancy, 22 and laboring time. 23 The sample size was calculated for each significant independent variable, considering the non-response rate, under the following statistical assumptions a power of 80% and a 95% confidence interval. Therefore, the maximum sample size calculated for the current study was 361.
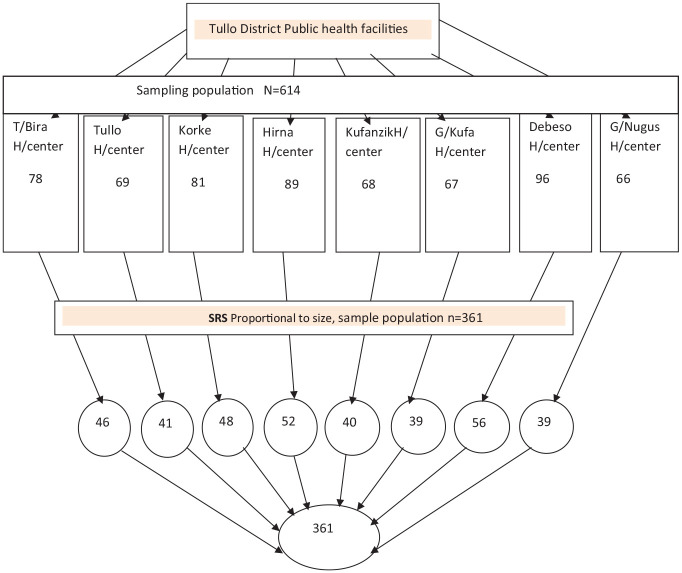
Initially, a simple random sampling method was used to select eight public health facilities providing delivery service in Tullo Woreda. The number of study units to be sampled from each health facility was determined using proportional allocation to size based on the number of client flows in the current year of 2020. The average 3-month caseload of each health facility was taken. Then, the systematic random sampling method was employed to select each study subject. The sampling fraction of the Kth interval was calculated as (N/n = 614/361 = 1.7–2). Based on the client’s card number, the starting woman was determined by using the lottery method, and every second delivered woman were included until the required sample was achieved (Figure 1).
Figure 1.
Schematic diagram showing maternal satisfaction and associated factors in the Tullo District Public health facilities, Eastern Ethiopia, 2020.
Data quality control
The questionnaire was initially prepared in English and then translated into the local languages by a bilingual expert (Afaan Oromo). Then, it was translated back into an English version to ensure its consistency. The data collectors and supervisor received training on the data collection tool and procedures. Before the actual study data collection, a pretest was conducted among 10% of the study participants in similar settings. The investigators and experienced research supervisors provided regular supervision.
Data processing and analysis
First, the collected data were checked for completeness and consistency. Then, they were cleaned, coded, and entered into EpiData version 3.1 for further analysis. The entered data were exported to SPSS version 25 for analysis. Descriptive and summary statistics were conducted and reported using frequency tables and figures. A binary logistic regression model was fitted to check for an association between independent variables and the outcome variable. The model’s fitness was checked by Hosmer–Lemeshow statistics and Omnibus tests. A multivariable analysis was performed to identify the true predictors of the outcome variables. A multi-collinearity test was carried out to check the presence of correlation between independent variables by using the standard error and co-linearity statistics, and no collinearity effects were detected. Thus, the value of the Variance Inflation Factor was 0.951. The direction and strength of the statistical association were measured by the odds ratio along with the 95% confidence interval (CI). A p-value of 0.05 was considered to be statistically significant in both bi-variable and multivariable analyses.
Ethical consideration
Ethical approval was obtained from the Institutional Health Research Ethics Review Committee (IHRERC) of Haramaya University, College of Health and Medical Sciences (IHRERC/174/2020). Supporting letter that explains the objective of the study was written to the Tullo Woreda Health Office. Before data collection, written informed consent was obtained from each study participant and their legally authorized representatives for minors. The consent was verbally explained for participants who were unable to read the consent, and the data collectors noted their consent. Their confidentiality was maintained, and the information obtained from each participant was generalized to the whole population.
Results
Sociodemographic characteristics of women
A total of 361 study participants were involved and yielding a response rate of 98.3%. The mean (±SD) age of the study participants were 27.78 (±6.738). One hundred forty-three (40.3%) and 163 (45.9%) of the respondents were between the ages of 15–25 and 26–35, respectively. Three hundred twenty-seven (92.1%) of the respondents were married, and 37 (10.4%) and 123 (34.6%) had a formal education and a certificate, respectively. In terms of respondents’ occupations, 103 (29%) of them were merchants, and 179 (50.4%) were housewives. The majority of participants, 267 (75.2%) were Muslims. Two hundred ninety-one (82%) of them were Oromo, and 302 (85.1%) of them came from rural areas, whereas only 53 (13.9%) of them were from urban areas (Table 1).
Table 1.
Sociodemographic characteristics of mothers gave birth in public health facilities, Tullo Woreda, Oromia, eastern Ethiopia, 2020 (n = 355).
| Characteristics | Variable category | Frequency | Percentage (%) |
|---|---|---|---|
| Residence | Urban | 53 | 14.9 |
| Rural | 302 | 85.3 | |
| Age of respondents | <25 | 143 | 40.3 |
| 25–35 | 163 | 45.9 | |
| ⩾36 | 49 | 13.8 | |
| Marital status | Married | 327 | 92.1 |
| Others * | 28 | 7.9 | |
| Educational level | No formal education | 123 | 34.6 |
| Grade 1–6 | 120 | 33.8 | |
| Grade 7–12 | 75 | 21.1 | |
| Certificate and above | 37 | 10.4 | |
| Occupation | Government employee | 41 | 11.5 |
| Merchant | 103 | 29 | |
| Housewife | 179 | 50.4 | |
| Others ** | 31 | 8.7 | |
| Religion | Orthodox | 76 | 21.4 |
| Muslim | 267 | 75.2 | |
| Others # | 12 | 3.4 | |
| Ethnicity | Oromo | 291 | 82 |
| Amhara | 45 | 12.7 | |
| Others ## | 18 | 5.3 |
Single, widowed, divorced and cohabit.
Private employees, students, and daily laborer.
Waqefata, catholic.
Gurage, Somali.
Health service-related factors
Regarding travel time taken to reach at health facilities, only 21 (5.9%) of women responded that they would travel more than 2 h to get to a health institution, whereas 142 (or 40%) took less than 30 min. The majority, 69.6% of them, arrived at the health facility on foot to give birth, and 292 (82.3%) of the respondents had to wait less than 10 min for the delivery service. Male healthcare providers attended more than half (60.3%), whereas female healthcare providers attended the remaining 39.7% delivery. Almost all respondents 332 (93.5%) seek to use the delivery service in the future, and 323 (91.0%) of them said they would advise others to use the delivery service (Table 2).
Table 2.
Health service-related factors of mothers who gave birth in public health facilities, Tullo Woreda, Oromia, eastern Ethiopia, 2020 (n = 355).
| Characteristics | Variable category | Frequency | Percentage (%) |
|---|---|---|---|
| Time taken to reach a health facility | 30 min | 142 | 40 |
| 1 h | 132 | 37.2 | |
| 2 h | 60 | 16.9 | |
| More than 2 h | 21 | 5.9 | |
| Mode of arrival | Ambulance | 78 | 22 |
| On foot | 287 | 69.6 | |
| Auto-rickshaw | 14 | 3.9 | |
| Other* | 16 | 4.5 | |
| Waiting time | Less than 10 min | 292 | 82.3 |
| 10–30 min | 57 | 16.1 | |
| More than 30 min | 6 | 1.7 | |
| ANC-antenatal care provider | Male | 220 | 62 |
| Female | 135 | 38 | |
| Delivery service care provider | Male | 214 | 60.3 |
| Female | 141 | 39.7 | |
| Seeking service in future | Yes | 332 | 93.5 |
| No | 23 | 6.5 | |
| Recommending service for friends and relatives | Yes | 323 | 91 |
| No | 32 | 9 |
By human, other public transportation.
Obstetric-related factors of respondents
Two hundred twenty (62%) of respondents were multipara, whereas 135 (38%) of them were primipara. Regarding their mode of delivery, 230 (64.8%) of women gave birth by spontaneous vaginal delivery and 125 (35.2%) of them gave birth by assisted vaginal delivery. Among women who participated in this study, many of them 329 (92.7%) had normal outcomes of delivery and the remaining 26 (7.3%) of them had complications. Like this, the majority 85.9% of fetal outcome was normal, whereas 44 (12.4%) of them were complicated (stillbirth, neonatal death, and distress). Regarding the status of pregnancies, 276 (77.7%) of pregnancies were wanted, whereas the remaining 79 (22.3%) were unwanted. Two hundred forty-seven (69.6%) of respondents had ANC follow-up during the current pregnancy, and almost all 93.5% of them know their blood pressure status during ANC service (Table 3).
Table 3.
Obstetric-related factors of mothers gave birth in public health facilities, Tullo Woreda, Oromia, eastern Ethiopia, 2020 (n = 355).
| Characteristics | Variables category | Frequency | Percentage (%) |
|---|---|---|---|
| Number of pregnancies or parity | Primipara | 135 | 38 |
| Multipara | 220 | 62 | |
| The current mode of delivery | Spontaneous vaginal delivery | 230 | 64.8 |
| Assisted vaginal | 125 | 35.2 | |
| Outcome of delivery | Normal | 329 | 92.7 |
| Complicated | 26 | 7.3 | |
| Fetal outcome | Normal | 305 | 85.9 |
| Complicated | 50 | 14.1 | |
| Status of pregnancy | Wanted | 276 | 77.7 |
| Unwanted | 79 | 22.3 | |
| ANC follow-up | Yes | 247 | 69.6 |
| No | 108 | 30.4 | |
| Blood pressure measured during giving service | Yes | 332 | 93.5 |
| No | 23 | 6.5 |
Maternal services satisfaction
A majority 232 (65.3%) and 222 (62.5%) of mothers were not satisfied with the availability of maternal service drugs and water availability at the period of giving birth in the facility. Again 282 (70.4%), 272 (76.6%), 266 (74.9%), 244 (68.7%), 289 (81.4%), 265 (74.6%), and 275 (77.5%) mothers were not satisfied with cleanliness of delivery room, health professional gender who give delivery service, blood pressure measurement services, keep confidentiality of information, respectful delivery care service, privacy maintaining during delivery, and advice given about institution delivery and postnatal care (PNC), respectively. But almost half 186 (52.4%), 184 (51.8%), and 210 (59.2%) mothers were satisfied with the services of toilet, adequacy of the waiting area, and freedom of delivery position, respectively (Table 4).
Table 4.
Maternal satisfaction level with each service of mothers who gave birth in public health facilities, Tullo Woreda, Oromia, eastern Ethiopia, 2020 (n = 355).
| Maternal service area | Satisfied | Frequency | Percentage (%) |
|---|---|---|---|
| Drug availability | Yes | 123 | 34.7 |
| No | 232 | 65.3 | |
| Water service availability | Yes | 133 | 37.5 |
| No | 222 | 62.5 | |
| Cleanliness of delivery room | Yes | 73 | 20.6 |
| No | 282 | 70.4 | |
| Adequacy of the waiting area | Yes | 186 | 52.4 |
| No | 169 | 47.6 | |
| Toilet service | Yes | 184 | 51.8 |
| No | 171 | 44.5 | |
| Health professional gender | Yes | 83 | 23.4 |
| No | 272 | 76.6 | |
| Blood pressure measurement | Yes | 89 | 25.1 |
| No | 266 | 74.9 | |
| Freedom of delivery position | Yes | 210 | 59.2 |
| No | 145 | 40.8 | |
| Confidentiality of information | Yes | 111 | 31.3 |
| No | 244 | 68.7 | |
| Respectful delivery care service | Yes | 66 | 18.6 |
| No | 289 | 81.4 | |
| Privacy maintains during delivery | Yes | 90 | 25.4 |
| No | 265 | 74.6 | |
| Advice about institution delivery and PNC | Yes | 80 | 22.5 |
| No | 275 | 77.5 |
Level of maternal satisfaction with delivery service
In this study, 119 (33.5%; 95% CI: 27.81, 39.13) mothers reported being satisfied with the overall delivery service given when giving birth in health facilities (Figure 2).
Figure 2.
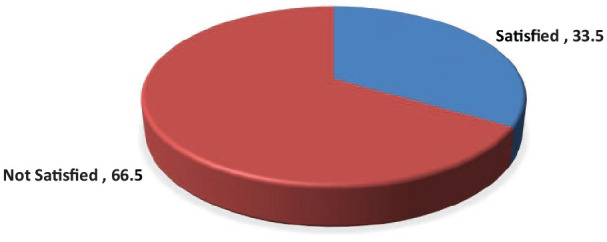
Overall maternal satisfaction of mothers gave birth in public health facilities, Tullo Woreda, Oromia, eastern Ethiopia, 2020 (n = 355).
Factors associated with maternal satisfaction
All respondent-related characteristics such as Socio-demographic characteristics of mothers, Obstetric-related factors of mothers, and specific service satisfaction-related factors were assessed for possible association with overall maternal service satisfaction among mothers using a bi-variable logistic regression model. Accordingly, sociodemographic variables (residence, educational level of mother, and occupation of mothers), obstetric and health service-related variables (ANC follow-up for the past pregnancy, history of pregnancy, delivery outcome, and mode of transportation to reach health facilities), and specific maternal health service-related satisfaction (toilet availability, maternal care drugs availability, Maintaining mothers privacy during delivery, and respectful maternal care service) were variables found to be associated at p < 0.25 with overall maternal service satisfaction among mothers on bivariate analysis and a candidate for final multivariable logistic regression analysis.
In this study, mothers who reached health facilities on their own feet 83% (AOR = 0.17; 95% CI: 0.04, 0.74) and by auto-rickshaw 84 % (AOR = 0.16; 95% CI: 0.04, 0.64) times less likely to be satisfied with overall delivery service compared to those who reached health facilities by ambulance transportation. Additionally, mothers who are not satisfied with toilet service at the delivery room were 51% times less likely to be satisfied with overall delivery services (AOR = 0.49; 95% CI: 0.12, 0.86) than their counterparts and also mothers who are not satisfied with maternal drugs availability during delivery service use were 35% times less likely to be satisfied with overall delivery services (AOR = 0.65; 95% CI: 0.11, 0.95) than their counterparts. Finally, this study revealed that mothers who do not have a history of ANC follow-up were 67% times less likely to be satisfied with overall delivery services (AOR = 0.33; 95% CI: 0.19, 0.56) than mothers who had a history of ANC follow-up during their pregnancy (Table 5).
Table 5.
Bi-variable and multivariable logistic regression analysis of factors associated with overall maternal satisfaction among mothers attending the public health facilities in Tullo Woreda, Oromia, eastern Ethiopia, 2020 (n = 355).
| Variables (n = 355) | Overall maternal satisfied | COR (95% CI) | AOR (95% CI) | p-Value | |
|---|---|---|---|---|---|
| Yes(No.& %) | No(No.& %) | ||||
| Residence | |||||
| Urban | 21 (5.9%) | 32 (9%) | 1 | 1 | |
| Rural | 161 (45.4%) | 141 (39.7%) | 0.55 (0.21, 1.48) | 2.168 (0.97, 4.87) | 0.061 |
| Educational status of mothers | |||||
| No formal education | 67 (18.87%) | 56 (15.77%) | 1 | 1 | |
| Grade 1-6 | 60 (16.9%) | 60 (16.9%) | 1.44 (0.73, 2.83) | 0.27 (0.06, 1.18) | 0.081 |
| Grade 7-12 | 42 (11.8%) | 33 (9.29%) | 0.93 (0.41, 2.11) | 0.45 (0.10, 1.99) | 0.295 |
| Certificate & above | 13 (3.67%) | 24 (6.76%) | 2.51 (0.46, 13.80) | 0.30 (0.08, 1.20) | 0.088 |
| Occupational status of mothers | |||||
| Government employee | 16 (4.5%) | 25 (7%) | 1 | 1 | |
| Private employee | 6 (1.7%) | 5 (1.4%) | 0.85 (0.11, 2.83) | 1.52 (0.27, 8.51) | 0.631 |
| Merchant | 59 (16.6%) | 44 (12.4%) | 0.93 (0.20, 4.40) | 0.77 (0.10, 5.76) | 0.799 |
| Housewife | 90 (25.4%) | 89 (25%) | 1.35 (0.03, 6.01) | 1.45 (0.46, 4.6) | 0.532 |
| Other | 10 (2.8%) | 11 (3.1%) | 0.23 (0.03, 2.02) | 2.01 (0.66, 6.17) | 0.225 |
| Transportation means to reach at HF | |||||
| Ambulance | 35 (9.86%) | 43 (12.11%) | 1 | 1 | |
| On foot | 138 (38.87%) | 109 (30.7%) | 1.03 (0.49, 2.17) | 0.17 (0.04, 0.74) | 0.018* |
| Auto- rickshaw | 6 (1.69%) | 8 (2.25%) | 1.69 (0.33, 8.63) | 0.16 (0.04, 0.64) | 0.010* |
| Other | 3 (0.85%) | 13 (3.66%) | 4.75 (0.96, 23.41) | 0.17 (0.02, 1.21) | 0.077 |
| Satisfaction to the available to toilet | |||||
| Yes | 57 (33.7%) | 112 (66.3%) | 1 | 1 | |
| No | 62 (33.3%) | 124 (66.7%) | 1.97 (0.90, 4.29) | 0.49 (0.12, 0.86) | 0.023* |
| Drugs availability satisfaction | |||||
| Yes | 41 (24.3%) | 82 (75.7%) | 1 | 1 | |
| No | 78 (33.6%) | 154 (66.4%) | 1.73 (1.14, 2.63) | 0.65 (0.11, 0.95) | 0.043* |
| Privacy maintained during delivery | |||||
| Yes | 31 (18.3%) | 59 (81.7%) | 1 | 1 | |
| No | 88 (33.2%) | 177 (66.8%) | 1.73 (1.14, 2.63) | 0.95 (0.51, 1.75) | 0.862 |
| Respectful maternal care during delivery | |||||
| Yes | 22 (13.0%) | 38 (87.0%) | 1 | 1 | |
| No | 97 (33.5%) | 198 (68.5%) | 1.91 (0.99, 3.66) | 0.62 (0.28, 1.36) | 0.237 |
| History of antenatal care follow-up | |||||
| Yes | 146 (41.1%) | 101 (28.5%) | 1 | 1 | |
| No | 36 (10.1%) | 72 (20%) | 3.09 (1.67, 5.74) | 0.33 (0.19, 0.56) | 0.000* |
| History of pregnancy | |||||
| Wanted | 154 (43.38%) | 122 (34.36%) | 1 | 1 | |
| Unwanted | 28 (7.88%) | 51 (14.36%) | 1.68 (0.82, 3.43) | 0.54 (0.298, 1.02) | 0.056 |
| Outcome of delivery | |||||
| Normal | 175 (49.3%) | 154 (43.38%) | 1 | 1 | |
| Complicated | 7 (1.97%) | 19 (5.35%) | 2.42 (0.74, 7.90) | 0.39 (0.14, 1.12) | 0.080 |
Statistically significant.
Discussion
This study assessed the prevalence and determinants of maternal satisfaction among mothers attending the public health facilities in Tullo Woreda, Eastern Ethiopia. The study pointed out that overall maternal satisfaction was 33.5% (95% CI: 27.81, 39.13). Thus, it revealed that only one in every three women who gave birth in the aforementioned health facilities were satisfied with delivery services. Factors, such as ANC follow-up, means of transportation, the availability of toilets, and drugs, were identified as a predictor of maternal satisfactions.
In this study, the overall client satisfaction with delivery service was 33.5%. This finding was in line with the study conducted in Mizan Aman town in Southern nation and nationalities of Ethiopia which was 30.4% and higher than the finding of study conducted at Gandhi Memorial Hospital which ranges between 2.4% and 21%.17,24 However, the current finding was lower than the results of studies conducted in Jimma, Ethiopia 78.7%, 12 West Arsi, Ethiopia 74.6%, 16 and Addis Ababa, Ethiopia 82% and studies conducted in other countries such Ghana 94%, 9 Egypt 78.5%, 25 and India 67.8%. 2 The discrepancy between this study and others may be due to differences in socio-cultural, demographic, time of the study, study setting (health center vs hospital), real quality of services, and operational definition of the study variable. It also may be due to expectations of women or less quality of provided services. The other possible justification for low women’s satisfaction in our study may be due to work overload on providers, especially at Hirna Health Center due to the closure of Hirna Hospital since it was selected as a COVID-19 treatment center during the data collection period. Regardless of their low level of satisfaction, the majority of them suggested seeking service and recommending centers for others. This may be due to clients’ awareness of complications related to home delivery. More importantly, the current finding may imply that low satisfaction decreases institutional delivery service utilization or leads to maternal complications and death as a result of home delivery. 26 This may hinder our country from reaching the 2030 sustainable development goal (SDG) target of a 70/100,000 maternal mortality ratio. 27 As explained in World Health organization recommendation guidelines, to achieve a positive childbirth experience for women and their babies, competent and motivated healthcare professionals working where essential physical resources are available are required. 28
According to this study, ANC follow-up has a statistically significant association with maternal satisfactions of delivery service. Thus, women who did not have ANC follow-up are 67% less likely to be satisfied than their counterparts. This was in agreement with the studies conducted in the Somali region, Eastern Ethiopia, 18 West Shewa Zone, Ethiopia, 29 Wolaita Sodo University Hospital, Ethiopia 30 Jimma Zone, Ethiopia, 22 and Gondar Teaching and Referral Hospital, Northwest Ethiopia. 31 This might be a result of mothers receiving antenatal care becoming more aware of institutional delivery services and other fundamental maternal health services. This study suggests that local and national programs should give careful consideration to increasing mothers’ awareness of the advantages of ANC follow-up through advocacy and health education. Moreover, access to prenatal counseling about the advantages of institutional delivery may lead to the development of a cordial relationship in which caregivers and mothers become friends during the delivery care process. In general, the quality of ANC services positively influences women’s healthcare-seeking behavior and good practices of mothers and family members. 32
In the final model of multivariable analysis, the means of transportations was found to be associated with the maternal satisfactions of delivery services. Accordingly, women who came with their foot and took an auto-rickshaw as means of transportation were 83% and 84% less likely to be satisfied with delivery services than those who received ambulance service to arrive at health facilities, respectively. This is supported by the study conducted in Central Ethiopia, in which mothers receiving ambulance service to arrive at health facilities were more likely to be satisfied. 15 One of the possible justifications could be those who obtained ambulance service reach health facility quickly and can get services quickly, but women who did not receive ambulances promptly may give birth on the way to health facilities which in turn hugely and immensely affect their satisfactions. Furthermore, this may be due to the geographic problem, which was time-consuming and difficult even for non-pregnant and healthy people.
The current study also revealed that mothers who are not satisfied with toilet service at the delivery room were 51% less likely to be satisfied with overall delivery services compared to their counterparts which was comparable with the study done in West Shoa Zone, Oromia Region, Ethiopia 7 and Wollega Zone, Oromia Regional State, Western Ethiopia. 33 It is known that toilet service is one of the important components of maternal service in the delivery room. In addition, mothers may perceive as their privacy did not maintain when they were dissatisfied with toilet service. Hence, a mother’s dissatisfaction with a specific service obviously affects the overall maternal satisfaction with the delivery service. Another possible justification for this finding might be that it can be related to the study settings since the current study was conducted in health centers in which there was a low presence and quality of toilets in the delivery room. Therefore, this implies that the administrative body of health facilities should pay attention to solving the problem related to the lack of toilets and sanitation to ensure that mothers receive adequate and quality services.
Furthermore, the current study revealed that mothers who were not satisfied with free maternal drugs availability during delivery service use were 35% less likely to be satisfied with overall delivery services than their counterparts. This finding of the study was supported by the study done in Northwest Ethiopia 31 and Gamo Gofa Zone, Southwest Ethiopia. 34 This may be related to the study settings and period. The current study was conducted during the emergency of COVID-19 and it impacted the overall service delivery system worldwide. This implies that accessibility of cost-free service may increase institutional delivery and level of satisfaction as well. However, this can have a negative effect on maternal satisfaction and their institutional delivery perception and expectation of mothers. In addition, the pandemic of COVID-19 may have catastrophic direct and indirect negative effect on overall maternal services, and threatening the significant advancements achieved over the previous few decades. 35
Strength and limitation of the study
In this study, due to the nature of the cross-sectional study design, it would be impossible to determine the causal relationship between the variable and the outcome in the analysis. Since the data was collected at discharge time from the ward after delivery, recall bias may be reduced. However, the study respondents may be afraid to express their feelings to data collectors because they are in an institution where they receive a health care service.
Conclusions
This study pointed out that only one in every three women are satisfied with delivery care services provided in public health facilities of the study area. This low level of maternal satisfaction suggests that facilities management and healthcare providers need to work hard to raise the satisfaction of delivery services. Factors such as not having ANC, using foot and auto-rickshaw as means of transportation, availability of drugs and toilets were predictor of maternal satisfactions. Awareness creation for the benefit of ANC follow-up and delivery in the health facilities, and providing safe transportation during referral time may help mothers get a timely healthcare service, which may increase client satisfaction. The concerned entities must pay attention in timely availability of drugs and improving the toiles, which play a role in shaping and molding level of satisfaction of women. Furthermore, additional comparative studies might be required at different levels of health facilities to provide a variation in the degree of maternal satisfaction with delivery services.
Supplemental Material
Supplemental material, sj-docx-1-smo-10.1177_20503121241233214 for Two out of every three pregnant women who gave birth in public health facilities of Tullo Woreda were dissatisfied with deliveries services, Eastern Ethiopia by Shasho Debelle, Mulugeta Gamachu, Alemayehu Deressa, Adera Debella, Addis Eyeberu, Galana Mamo Ayana, Abdi Birhanu, Hamdi Fekredin Zakaria, Fenan Reshid, Nega Assefa and Ibsa Mussa in SAGE Open Medicine
Supplemental material, sj-docx-2-smo-10.1177_20503121241233214 for Two out of every three pregnant women who gave birth in public health facilities of Tullo Woreda were dissatisfied with deliveries services, Eastern Ethiopia by Shasho Debelle, Mulugeta Gamachu, Alemayehu Deressa, Adera Debella, Addis Eyeberu, Galana Mamo Ayana, Abdi Birhanu, Hamdi Fekredin Zakaria, Fenan Reshid, Nega Assefa and Ibsa Mussa in SAGE Open Medicine
Acknowledgments
The authors extend their deepest thanks to Haramaya University and individuals who participated in the study: data collectors, supervisors, and administrative officials for providing their constructive support during data collection.
Footnotes
Authors contributions: Shasho Debelle conceived the idea and played key roles in data review, drafting, and writing the final product. Data analysis, drafting, and manuscript preparation were all done by all co-authors. Finally, all authors read and approved the final version of the manuscript for publication, and they all agreed on all aspects of this work.
Availability of data and materials: All data used to analyze this study is available from the corresponding author upon reasonable request.
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding: The authors received no financial support for the research, authorship, and/or publication of this article.
Consent to the publication: Not applicable.
Trial registration: Not applicable.
ORCID iDs: Mulugeta Gamachu  https://orcid.org/0000-0003-3890-5203
https://orcid.org/0000-0003-3890-5203
Alemayehu Deressa  https://orcid.org/0000-0001-9751-868X
https://orcid.org/0000-0001-9751-868X
Adera Debella  https://orcid.org/0000-0002-8060-0027
https://orcid.org/0000-0002-8060-0027
Addis Eyeberu  https://orcid.org/0000-0002-3147-3770
https://orcid.org/0000-0002-3147-3770
Galana Mamo Ayana  https://orcid.org/0000-0001-6082-0172
https://orcid.org/0000-0001-6082-0172
Abdi Birhanu  https://orcid.org/0000-0003-1312-0637
https://orcid.org/0000-0003-1312-0637
Nega Assefa  https://orcid.org/0000-0003-0341-2329
https://orcid.org/0000-0003-0341-2329
Ibsa Mussa  https://orcid.org/0000-0002-6318-4092
https://orcid.org/0000-0002-6318-4092
Supplemental material: Supplemental material for this article is available online.
References
- 1. Prakash B. Patient satisfaction. J Cutan Aesthet Surg 2010; 3(3): 151–155. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2. Jha P, Larsson M, Christensson K, et al. Satisfaction with childbirth services provided in public health facilities: results from a crosssectional survey among postnatal women in Chhattisgarh, India. Global Health Action 2017; 10(1): 1386932. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3. FMoH. Mini demographic and health survey, https://dhsprogram.com/pubs/pdf/FR363/FR363.pdf (2019, accessed 25 August 2020).
- 4. WHO. WHO recommendations Intrapartum care for a positive childbirth experience Transforming care of women and babies for improved health and well-being, www.who.int/reproductivehealth (2018, accessed 25 August 2020). [DOI] [PMC free article] [PubMed]
- 5. Sandin-Bojö A-K, Kvist LJ. Care in labor: a Swedish survey using the Bologna Score. Birth 2008; 35(4): 321–328. [DOI] [PubMed] [Google Scholar]
- 6. Eziawdres D, Worku W, Taye M. Maternal satisfaction with delivery services and its associated factors among mothers who gave birth at public health centers in Yeka Sub City, Addis Ababa, Ethiopia. Health Serv Insights 2021; 14: 11786329211050722. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7. Gejea T, Abadiga M, Hasen T. Maternal satisfaction with delivery services of government hospitals in Ambo town, West Shoa zone, Oromia region, Ethiopia, 2020. Patient Prefer Adherence 2020; 14: 1225–1235. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8. Kidane A, Getachew T, Mesfin F, et al. Maternal satisfaction on delivery care services and associated factors at public hospitals in eastern Ethiopia. Int Health 2023; 15(2): 189–197. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9. Adjei KK, Kikuchi K, Owusu-Agyei S, et al. Women’s overall satisfaction with health facility delivery services in Ghana: a mixed-methods study. Trop Med Health 2019; 47: 41. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10. Fisseha G, Berhane Y, Worku A, et al. Quality of the delivery services in health facilities in Northern Ethiopia. BMC Health Serv Res 2017; 17: 187. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11. Tayelgn A, Zegeye DT, Kebede Y. Mothers’ satisfaction with referral hospital delivery service in Amhara Region, Ethiopia. BMC Pregnancy Childbirth 2011; 11: 78. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12. Gonie A, Tebeje B, Sinaga M. Satisfaction towards skilled delivery services and associated factors among mothers who gave birth at government health facilities, Jimma Town, Ethiopia. Clin Mother Child Health 2018; 15: 1000302. [Google Scholar]
- 13. Debono D, Travaglia J. Complaints and patient satisfaction: a comprehensive review of the literature. Australia: University of New South Wales, Centre for Clinical Governance Research in Health, 2009. [Google Scholar]
- 14. von Elm E, Altman DG, Egger M, et al. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) Statement: guidelines for reporting observational studies. BMJ 2007; 335(7624): 806–808. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15. Debela AB, Mekuria M, Kolola T, et al. Maternal satisfaction and factors associated with institutional delivery care in Central Ethiopia: a mixed study. Patient Prefer Adherence 2021; 15: 387–398. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16. Edaso AU, Teshome GS. Mothers’ satisfaction with delivery services and associated factors at health institutions in west Arsi, Oromia regional state, Ethiopia. MOJ Womens Health 2019; 8(1): 110–119. [Google Scholar]
- 17. Melese T, Gebrehiwot Y, Bisetegne D, et al. Assessment of client satisfaction in labor and delivery services at a maternity referral hospital in Ethiopia. Pan Afr Med J 2014; 17: 76. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18. Shiferaw Z, Mahad A, Haile S. Maternal satisfaction and associated factors towards institutional delivery service at public hospitals in the Somali region, Eastern Ethiopia. PLoS One 2022; 17(11): e0277224. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19. Amdemichael R, Tafa M, Fekadu H. Maternal satisfaction with the delivery services in Assela Hospital, Arsi Zone, Oromia Region. Gynecol Obstet 2014; 4(12): 1000257. [Google Scholar]
- 20. Temamo AA, Abebe A. Mothers’ satisfaction with institutional delivery service and associated factors among women attending hospitals in Wolaita Zone Administration, SNNPR, Ethiopia. J Nutr Diet Pract 2018; 2: 1–12. [Google Scholar]
- 21. FMoH. Health sector transformation plan, https://www.cmpethiopia.org/content/download/2268/9612/file/HSTP%20Final%202015-10-19.pdf (2015, accessed 20 August 2020).
- 22. Tadesse BH, Bayou GT, Tsega G, et al. Mothers’ satisfaction with institutional delivery service in public health facilities of Omo Nada District, Jimma Zone. Clin Med Res 2017; 6: 23–30. [Google Scholar]
- 23. Bitew K, Ayichiluhm M, Yimam K. Maternal satisfaction on delivery service and its associated factors among mothers who gave birth in public health facilities of Debre Markos Town, Northwest Ethiopia. J Biomed Biotechnol 2015; 2015: 460767. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24. Yarinbab TE, Adraro W, Tariku R, et al. Level of maternal satisfaction and its determinants at health facilities in Mizan-Aman Town, Ethiopia: cross sectional study. Int J Womens Health Wellness 2019; 5(1): 88. [Google Scholar]
- 25. Sayed W, Abd El, Aal DEM, Mohammed HS, et al. Maternal satisfaction with delivery services at tertiary university hospital in upper Egypt, is it actually satisfying? Int J Reprod Contracep Obstet Gynecol 2018; 7(7): 2547. [Google Scholar]
- 26. Nigusie A, Azale T, Yitayal M. Institutional delivery service utilization and associated factors in Ethiopia: a systematic review and META-analysis. BMC Pregnancy Childbirth 2020; 20(1): 364. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27. SDG. SDG health and health-related targets, https://www.who.int/data/gho/data/themes/topics/topic-details/GHO/sdgtarget3-1-reduce-maternal-mortality (2016, accessed 20 August 2020).
- 28. World Health Organization. WHO recommendations Intrapartum care for a positive childbirth experience. Geneva, Switzerland: World Health Organization, 2018. [PubMed] [Google Scholar]
- 29. Argawu AS, Erana MM. Maternal satisfaction on delivery service and its associated factors in public health facilities at West Shewa Zone, Ethiopia. Ethiop J Health Sci 2023; 33(2): 301–310. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30. Wolka S, Assegid S, Tantu T, et al. Determinants of maternal satisfaction with existing delivery care at Wolaita Sodo University teaching and referral hospital, Ethiopia. BioMed Res Int 2020; 2020: 6403123. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31. Gashaye KT, Tsegaye AT, Shiferaw G, et al. Client satisfaction with existing labor and delivery care and associated factors among mothers who gave birth in university of Gondar teaching hospital; Northwest Ethiopia: Institution based cross-sectional study. PLoS One 2019; 14(2): e0210693. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32. Sychareun V, Somphet V, Chaleunvong K, et al. Perceptions and understandings of pregnancy, antenatal care and postpartum care among rural Lao women and their families. BMC Pregnancy Childbirth 2016; 16(1): 245. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33. Gejea T, Abadiga M, Hasen T. Maternal satisfaction with delivery services of Government Hospitals in Ambo Town, West Shoa Zone, Oromia Region, Ethiopia, 2020. Patient Prefer Adherence 2020; 14: 1225–1235. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34. Tesfaye R, Worku A, Godana W, et al. Client satisfaction with delivery care service and associated factors in the public health facilities of Gamo Gofa Zone, Southwest Ethiopia: in a resource limited setting. Obstet Gynecol Int 2016; 2016: 5798068. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35. Desta AA, Woldearegay TW, Gebremeskel E, et al. Impacts of COVID-19 on essential health services in Tigray, Northern Ethiopia: a pre-post study. PLoS One 2021; 16(8): e0256330. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Supplemental material, sj-docx-1-smo-10.1177_20503121241233214 for Two out of every three pregnant women who gave birth in public health facilities of Tullo Woreda were dissatisfied with deliveries services, Eastern Ethiopia by Shasho Debelle, Mulugeta Gamachu, Alemayehu Deressa, Adera Debella, Addis Eyeberu, Galana Mamo Ayana, Abdi Birhanu, Hamdi Fekredin Zakaria, Fenan Reshid, Nega Assefa and Ibsa Mussa in SAGE Open Medicine
Supplemental material, sj-docx-2-smo-10.1177_20503121241233214 for Two out of every three pregnant women who gave birth in public health facilities of Tullo Woreda were dissatisfied with deliveries services, Eastern Ethiopia by Shasho Debelle, Mulugeta Gamachu, Alemayehu Deressa, Adera Debella, Addis Eyeberu, Galana Mamo Ayana, Abdi Birhanu, Hamdi Fekredin Zakaria, Fenan Reshid, Nega Assefa and Ibsa Mussa in SAGE Open Medicine