Abstract
OBJECTIVE:
To explore the effect of electroacupuncture on skeletal muscle pain in Parkinson's disease (PD).
METHODS:
A single-center randomized controlled trial was conducted with sixty patients with Parkinson's disease with skeletal muscle pain were randomly divided into electroacupuncture group and sham acupuncture control group with 30 patients each. The electric acupuncture group was treated with electric acupuncture, while the control group was treated with Park needle pseudoacupuncture. Both groups were treated 5 times a week for a total of 4 weeks, and both groups completed 20 treatments. King's Parkinson's Pain Scale (KPPS) and visual analog scale (VAS) were used before and after treatment to evaluate the pain degree of patients. Real-time shear wave elastography (SWE) and modified Ashworth score (MAS) were used to evaluate the changes of muscle tone. Parkinson's comprehensive Score Scale (MDS-UPDRS, including UPDRSⅡ and UPDRS Ⅲ) was used to evaluate exercise ability. Hamilton Depression Scale (HAMD) score was used to evaluate the emotional changes of patients. Spearman correlation analysis was used to explore the correlation between pain degree and muscle tone, exercise ability and emotion.
RESULTS:
During the study, one case fell off in the control group, and 30 cases were eventually included in the analysis and treatment group and 29 cases in the control group. After treatment, Young's modulus of biceps and quadriceps and shear wave velocity of biceps were decreased in electroacupuncture group compared with before treatment, while KPPS score, VAS score, UPDRSⅡ, UPDRS Ⅲ and modified Ashworth score were decreased, with statistical significance (P < 0.05). There was no statistical significance in control group (P > 0.05). After treatment, KPPS score, VAS score, UPDRSⅡ and UPDRS Ⅲ, MAS, HAMD score, Young's modulus of biceps and shear wave velocity in electroacupuncture group were significantly lower than those in control group (P < 0.05). Spearman correlation analysis showed that KPPS score was positively correlated with UPDRS Ⅲ (r = 0.414, P < 0.05). KPPS score was positively correlated with HAMD score (r = 0.576, P < 0.01).
CONCLUSION:
Electroacupuncture therapy can effectively improve skeletal muscle pain in patients with Parkinson's disease, reduce the muscle hardness of patients, improve patients' daily life ability, and improve patients' emotional disorders. The degree of skeletal muscle pain in PD patients is correlated with motor ability and emotional disorders, but there is no significant correlation between the degree of skeletal muscle pain and the muscle tone of PD patients.
Keywords: Parkinson disease; muscle, skeletal, pain; electroacupuncture; muscle tention; mood disorders; randomized controlled trial
1. INTRODUCTION
Parkinson's disease (PD) is a common chronic progressive neurological disease in middle-aged and elderly people, accompanied by a variety of motor and non-motor symptoms. As one of the common non-motor symptoms of Parkinson's disease, pain usually appears in the early stage of PD and may exist several years before clinical diagnosis,1 which seriously affects the quality of life of PD patients.2 According to the clinical characteristics of PD pain, it can be divided into five categories: musculoskeletal pain, nerve root or neuropathic pain, dystonia related pain, non-obstructive discomfort, and primary or central Parkinson's pain,3 among which skeletal muscle pain has the highest incidence, accounting for 66% of all pain.4 Skeletal muscle pain is nociceptive pain limited to different areas of the body,5 often occurring in the neck, shoulder, hip, knee and lower back of patients with Parkinson's disease.6 The origin of skeletal muscle pain is still unclear. Some studies believe that it is related to increased skeletal muscle tone of patients,7 while others believe that pain involves many factors, including sensory, biomechanical and psychological factors.8 Since it is not significantly regulated by dopaminergic treatment,9 dopaminergic treatment is ineffective for most skeletal muscle pain symptoms in PD patients. In recent years, acupuncture therapy has gradually become an important research direction for PD patients to intervene in non-motor symptoms, and previous studies have also confirmed the effectiveness of acupuncture therapy in treating non-motor symptoms of PD.10,⇓-12 Our early research observed that the treatment of PD accompanied pain by soft tendons and analgesic acupuncture has certain clinical efficacy, and has better effect on improving the pain caused by Parkinson's disease skeletal muscle pain, inability to sit still or restlessness.13 In this study, on the basis of previous studies, electroacupuncture therapy was used to treat PD skeletal muscle pain patients, observe its clinical efficacy, and at the same time, the patients' daily living ability and emotional disorders were evaluated, and at the same time, on the basis of confirming the efficacy, the correlation between PD skeletal muscle pain and patients' muscle tension and anxiety was evaluated.
2. METHODS
2.1. Study design
This study has passed the examination of the Hospital Ethics Committee of Beijing Hospital of Traditional Chinese Medicine, and the ethical approval number is SL-2020BL02-072-02. After the patient was diagnosed, the researcher would introduce the purpose, specific steps, benefits and risks of the study, and inform the randomization method in detail. The patient would sign the informed consent after expressing understanding. This study has been registered with ISRCTN (ISRCTN24310308). The study was a single-center randomized controlled trial involving patients admitted to Beijing Hospital of Traditional Chinese Medicine, Capital Medical University. Sixty patients were recruited and randomly divided into treatment group and control group in a 1∶1 ratio. The control group was treated with Park needle and the treatment group was treated with electric acupuncture. Patients in both groups were treated once a day and 5 times from Monday to Friday for a total of 4 weeks. Patients received 20 times of treatment. Due to the limitations of intervention methods, only the patients receiving treatment were blinded, and the treating physicians were not blinded. Data management and analysis Outcomes were assessed and analyzed by evaluators who were not involved in study design or electroacupuncture before enrollment and 4 weeks after treatment.
2.2. Participants
The recruited patients met the diagnostic criteria for PD in the Diagnostic Criteria for Parkinson's Disease in China (2016 Edition) 14 and met the diagnostic criteria for skeletal muscle pain, which was diagnosed according to the diagnostic criteria for chronic primary and secondary musculoskeletal pain in the latest International Classification of Diseases (ICD-11) published by WHO in June 2018.15
2.2.1. Inclusion criteria
(a) Patients who meet the diagnostic criteria for PD and chronic skeletal muscle pain; (b) There is no limitation on gender; (c) Aged 40-80 years; (d) The patient agrees to participate in the study and signs an informed consent form.
2.2.2. Exclusion criteria
(a) Those with severe organ dysfunction such as heart, liver and kidney; (b) Patients with schizophrenia, malignant tumor, disorders of the blood system, immune system and metabolism; (c) People with other types of dementia (vascular dementia, frontotemporal dementia, Alzheimer's disease, etc.); (d) Persons with severe cognitive impairment and language impairment; (e) Physical pain due to other diseases.
2.2.3. Drop out and suspension criteria
(a) Those who cannot tolerate it after treatment has begun; (b) Those whose condition worsens and they cannot adhere to treatment; (c) Patients who do not cooperate with the scale score and efficacy assessment; (d) Those who are unable to follow the established study protocol for treatment; (e) Concurrent analgesic therapy.
2.3. Sample size calculation
According to the study of acupuncture combined with levodopa in the treatment of PD Pain, after 4 weeks of treatment, the score of King's Parkinson's Pain Scale (KPPS) in the treatment group was (18.57 ± 6.14). The KPPS score of the control group was (24.17 ± 2.96).16 PASS11.0 software was used to calculate the sample size, independent sample T test was used, α was 0.05, 1-β was 0.9, δ was 2, and the ratio of patients in the treatment group and control group was 1∶1. The number of subjects in each group was calculated to be 25, according to the requirement that the case loss rate of clinical trials should not exceed 20%. It is concluded that 30 cases are required in each group, and the total sample size required in this study is 60 cases.
2.4. Randomization
Random numbers were automatically generated by a random number generator (IBM Corp., Armonk, NY, USA), each grouping scheme was placed in a light-tight envelope with a code written on the outside, sealed and handed to the researchers. Patients who met the inclusion and exclusion criteria were numbered, then the corresponding numbered envelope was opened and the study protocol was followed. The treatment regimen that each subject received was determined by the generated random sequence.
2.5. Blinding
The treating physician did not blind the group assignment, but only the enrolled patients. Treating physicians were trained to ensure that everyone involved received the same treatment. Assessors, data managers, and statisticians were not involved in treatment and were unaware of the grouping assignment to reduce the risk of bias.
2.6. Interventions
In principle, the type of Western Medicine and dosage of Western Medicine should not be changed in the two groups. Detailed records should be made if medication adjustment is needed. Electroacupuncture is administered without adjustment of daily medication.
2.6.1. Intervention group
Electroacupuncture was used in the Intervention group, and the acupoints were selected as the PD experience point of the Chinese medical master HE Puren.17 Main acupoints: Baihui (GV20),18 Qihai (CV6),18 Lieque (LU7),18 Tinggong (SI19).18 Auxiliary point: Upper pain add Jianyu (LI15),18 Quchi (LI11),18 Lower pain add Xuehai (SP10),18 Zusanli (ST36).18 Park tube + millimeter needle (1.5 inches) was used to puncture 10-30 mm. After De Qi use electro-acupuncture of Jianyu (LI15), Quchi (LI11), Xuehai (SP10), Zusanli (ST36), the frequency was 2 Hz/100 Hz alternately, and the needle was kept for 30 min, once a day, 5 times a week. The course of treatment lasted for 4 weeks, and a total of 20 times of electro-acupuncture treatment were received. The locating standards of acupoints refer to the National Standard GB/T12346-2021 "Name and Location of Acupoints" of the People's Republic of China.18 Needle: Huacheng single sterile acupuncture needle 0.3 mm × 40 mm, electroacupuncture instrument: Huatuo SDZ-V electronic needle therapy instrument.
2.6.2. Control group
In the control group, Park needle19 was used, and the acupoint selection was the same as that of the Intervention group. Huacheng flat head needle was placed into the Park tube, and the needle reached the acupoint of the patient without being pierced into the skin. The electric needle was connected at the same position, and the electric needle switch was turned on to adjust the minimum current. A total of 20 times of sham electroacupuncture were received.
2.7. Primary outcome measures
2.7.1. Skeletal muscle pain assessment
KPPS score was used for evaluation.20 KPPS score mainly included 7 dimensions (skeletal muscle pain, chronic pain, pain related to symptom fluctuation, night pain, mouth and face pain, pain related to swelling, and neuralgia), with a total of 14 items. The score of each item includes pain severity (0-3 points) and pain frequency (0-4 points). The final score of a single item is the product of pain severity and pain frequency, and the final score of the scale is the total score of 14 items accumulated (0-168 points).
2.7.2. Muscle tention assessment
Real-time Shear wave ultrasonic elastography (SWE) technology was used to detect the long axial Young's modulus and Shear wave elastography of biceps and quadriceps. SWE is a new ultrasonic elastic imaging technology, which has the advantages of safety, non-invasive, good repeatability, fast and simple, can quantify the hardness of biological tissues (lesions), obtain the elastic modulus, and be applied to muscle, tendon, nerve block and other musculoskeletal tissue diseases.21 The shear wave velocity (m/s) of the patient was obtained, and Young's modulus (Kpa) was deduced. The value of Young's modulus can directly reflect the elastic hardness of the tissue. The larger the value of Young's modulus, the larger the hardness of the tissue. The longer the shear wave velocity, the higher the hardness of the tissue.
2.8. Secondary outcome measures
2.8.1. Visual analogue score (VAS)
Pain was represented by a 10 cm long scale marked with 0 and 10 at both ends. Patients marked the point that best represented their pain intensity on the scale, and the distance from 0 to the marked point was the pain intensity score (0-10 points).22
2.8.2. MDS unified-Parkinson disease rating (MDS-UPDRS)
PD severity was scored comprehensively and in detail, including four parts: non-motor symptoms of daily life, motor symptoms of daily life, motor function test and motor complications. The study mainly used parts Ⅱ and Ⅲ for evaluation, activities of daily living (UPDRSⅡ): to evaluate patients' basic ability to live, motor function examination (UPDRS Ⅲ): to evaluate bradykinesia, rigidity, postural balance disorder, gait abnormality and hand functional activity disorder, etc.23
2.8.3. Modified Ashworth score (MAS)
Level 0: no increase in muscle tone (0 points); Grade Ⅰ: slight increase in muscle tone (1 point), grade Ⅰ+: slight increase in muscle tone (2 points); Grade Ⅱ: muscle tension increased significantly (3 points); Grade Ⅲ: serious increase in muscle tone (4 points); Grade Ⅳ: the affected part was rigid and unable to complete the passive movement during passive flexion and extension (score 5).24
2.8.4. Hamilton depression scale (HAMD)
HAMD scale 17-item version was used to divide the degree,25 no depression: HAMD score < 7; Mild depression:7 points < HAMD score ≤ 17 points; Moderate depression: 17 points < HAMD score ≤ 24 points; Severe depression: HAMD score > 24.
2.8.5. Related factors of skeletal muscle pain analysis
KPPS score, MAS and SWE test results were used to determine the relationship between pain and muscle tone. The correlation between KPPS score, UPDRS score and HAMD score was used to determine the relationship between pain and emotion.
2.9. Safety evaluation
During the whole process of acupuncture treatment, adverse reactions should be observed and recorded, including acupuncture dizziness, delayed acupuncture, broken acupuncture, bleeding, hematoma, infection, allergy, etc., timely treatment should be given, and at the same time, it should be decided whether to terminate the experiment of the subject. For serious adverse events, the "serious adverse event Report Form" should be filled in while corresponding measures should be taken urgently, and timely reported to the Ethics Committee and clinical supervision and management department to decide whether to terminate the whole experiment.
2.10. Statistical analyses
All data were recorded into electronic data form, and a database was established using Epidata and Excel 2019. Statistical software SPSS 26.0 (IBM Corp., Armonk, NY, USA) was used for analysis. Normal distribution test was conducted for measurement data first. If the data met the normal distribution, mean ± standard deviation ($\bar{x}±s$) was used to represent the data. Paired sample t test was used for intra-group comparison, and independent sample t test was used for inter-group comparison. The non-normal distribution was represented by the median (interquartile distance) [M (P25, P75)], and Kruskal-Wallis H test was used. Bilateral tests were adopted in all cases, and the test level was ɑ = 0.05. Spearman non-parametric correlation analysis was used for correlation analysis, and P < 0.05 indicated statistical significance.
3. OUTCOME
Thirty patients were enrolled in each group. During the treatment, 1 case fell off in the control group, and 30 cases in the Intervention group and 29 cases in the control group were eventually included in the analysis. All 59 patients were treated with electroacupuncture 20 times. Coincidence protocol set analysis (PP) was used to analyze the results of 30 patients in the treatment group and 29 patients in the control group. The test flow chart is shown in Figure 1.
Figure 1. Flow chart of a randomized controlled clinical study of electroacupuncture for skeletal muscle pain in Parkinson's disease.
3.1. Comparison of patients' basic data
The two groups had no differences in baseline scores (all P > 0.05). There were no significant differences in gender, mean age, mean course of disease, biceps Young's modulus, quadriceps Young's modulus, biceps shear wave velocity, quadriceps shear wave velocity, KPPS score, VAS score, MAS, UPDRSⅡ, UPDRS Ⅲ and HAMD score between the two groups (Table 1).
Table 1.
Baseline data of Parkinson's disease patients in the two groups
| Variable | Control group (n = 29) |
Intervention group (n = 30) |
P value |
|---|---|---|---|
| Sex (M/F) (n) | M: 14, F: 15 | M: 17, F: 13 | 0.242 |
| Age (years) | 64.30±7.99 | 64.30±9.76 | 0.516 |
| History of PD (years) | 5.33±2.77 | 5.07±2.99 | 0.539 |
| Young's modulus of the biceps (Kpa) | 48.81±2.95 | 58.12±5.42 | 0.143 |
| Young's modulus of the quadriceps muscle (Kpa) | 9.71±1.01 | 11.9±1.28 | 0.190 |
| SWE velocity of the biceps (m/s) | 3.92±0.15 | 5.16±0.95 | 0.254 |
| SWE velocity of the quadriceps muscle (m/s) | 2.23±0.32 | 2.35±0.23 | 0.406 |
| KPPS score (points) | 18.67±1.61 | 25.47±4.47 | 0.603 |
| VAS score (points) | 4.93±0.32 | 5.87±0.39 | 0.073 |
| MAS (points) | 2.20±0.20 | 2.60±0.19 | 0.177 |
| UPDRSⅡ (points) | 15.27±2.29 | 18.00±2.22 | 0.982 |
| UPDRS Ⅲ (points) | 25.00±2.22 | 38.67±4.01 | 0.056 |
| HAMD score (points) | 9.33±5.96 | 10.26±5.18 | 0.551 |
Notes: control group: Park tube + millimeter needle; Intervention group: Electroacupuncture. M: male, F: female; SWE: Shear wave ultrasonic elastography; KPPS: King's Parkinson's Pain Scale; VAS: Visual analogue score; MAS: modified Ashworth score; UPDRSⅡ: Unified-Parkinson Disease Rating for activities of daily living; UPDRS Ⅲ: Unified-Parkinson Disease Rating for motor function examination; HAMD: Hamilton depression scale.
3.2. Comparison of Skeletal muscle pain
After treatment 4 weeks, KPPS and VAS scores in the Intervention group were significantly lower than those before treatment, and significantly lower than those in the control group (P < 0.05) (Table 2). Indicating that electroacupuncture can improve patients' subjective pain experience.
Table 2.
Comparison of Skeletal muscle pain in the two groups of Parkinson's disease patients ($\bar{x}±s$)
| Group | Treatment timing | Sample | KPPS score (points) | VAS score (points) |
|---|---|---|---|---|
| Intervention group | 0 week | 30 | 25.47±4.47 | 5.87±0.39 |
| 4 weeks | 30 | 13.67±2.94ab | 3.73±0.23ab | |
| Control group | 0 week | 29 | 18.67±1.61 | 4.93±0.32 |
| 4 weeks | 29 | 19.00±1.64 | 4.87±0.29 |
Notes: control group: park tube + millimeter needle; intervention group: electroacupuncture. KPPS: King's Parkinson's Pain Scale; VAS: visual analogue score. Compared with the same group at 0 week, aP < 0.05; compared with the control group at same time, bP < 0.05.
3.3. Comparison of Muscle tention
After treatment 4 weeks, Young's modulus and SWE velocity of the biceps, SWE velocity of quadriceps muscle and MAS in Intervention group were significantly lower than those before treatment (P < 0.05); Young's modulus, SWE velocity of the biceps and MAS significantly lower than those in the control group (P < 0.05). There was no statistical significance in control group post and pre-treatment (P > 0.05) (Table 3).
Table 3.
Comparison of Muscle tention in the two groups of Parkinson's disease patients ($\bar{x}±s$)
| Group | Treatment Timing |
Sample | Biceps | Quadriceps muscle | MAS (points) | |||
|---|---|---|---|---|---|---|---|---|
| Young's modulus (Kpa) | SWE velocity (m/s) | Young's modulus (Kpa) | SWE velocity (m/s) | |||||
| Intervention | 0 week | 30 | 58.12±5.42 | 5.16±0.95 | 11.90±1.28 | 2.35±0.23 | 2.60±0.19 | |
| 4 weeks | 30 | 39.14±3.72ab | 3.48±0.15ab | 9.19±1.09 | 1.64±0.07a | 1.87±0.17ab | ||
| Control | 0 week | 29 | 48.81±2.95 | 3.92±0.15 | 9.71±1.01 | 2.23±0.32 | 2.20±0.20 | |
| 4 weeks | 29 | 49.87±3.06 | 4.02±0.14 | 11.09±1.19 | 1.64±0.07 | 2.00±0.22 | ||
Notes: control group: park tube + millimeter needle; intervention group: electroacupuncture. SWE: Shear wave ultrasonic elastography; MAS: modified Ashworth score. Compared with the same group at 0 week, aP < 0.05; compared with the control group at same time, bP < 0.05.
3.4. Comparison of UPDRSⅡ, UPDRSⅢ, HAMD score
After treatment 4 weeks, UPDRSⅡ, UPDRSⅢ, HAMD score in the intervention group were significantly lower than those before treatment, and significantly lower than those in the control group (P < 0.05). There was no statistical significance in control group post and pre-treatment (P > 0.05) (Table 4).
Table 4.
Comparison of UPDRSⅡ, UPDRSⅢ, HAMD score in the two groups of Parkinson's disease patients ($\bar{x}±s$)
| Group | Treatment timing | Sample | UPDRSⅡ (point) | UPDRSⅢ (points) | HAMD score (points) |
|---|---|---|---|---|---|
| Intervention | 0 week | 30 | 18.00±2.22 | 38.67±4.01 | 10.26±5.18 |
| 4 weeks | 30 | 9.47±1.18ab | 22.27±2.60ab | 7.26±4.62ab | |
| Control | 0 week | 29 | 15.27±2.29 | 25.00±2.22 | 9.33±5.96 |
| 4 weeks | 29 | 15.73±2.10 | 25.13±2.28 | 9.33±5.90 |
Notes: control group: park tube + millimeter needle; intervention group: electroacupuncture. UPDRSⅡ: Unified-Parkinson Disease Rating for activities of daily living; UPDRS Ⅲ: Unified-Parkinson Disease Rating for motor function examination; HAMD: Hamilton depression scale. Compared with the same group at 0 week, aP < 0.05; compared with the control group at same time, bP < 0.05.
3.5. Correlation analysis
3.5.1. Correlation between pain and muscle tension
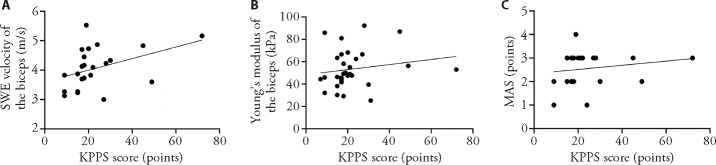
There was no correlation between KPPS score and SWE velocity of the biceps (r = 0.229, P > 0.05) (Figure 2A). There was no correlation between KPPS score and Young's modulus of the biceps (r = 0.049, P > 0.05) (Figure 2B). There was no correlation between KPPS score and MAS (r = 0.229, P > 0.05) (Figure 2C). Based on the results, there was no clear correlation between patients' pain experience and muscle tention.
Figure 2. Correlation between KPPS score and SWE velocity of the biceps, Young's modulus of the biceps, MAS.
A: correlation between KPPS score and SWE velocity of the biceps; B: correlation between KPPS score and Young's modulus of the biceps; C: correlation between KPPS score and MAS. KPPS: King's Parkinson's Pain Scale; SWE: Shear wave ultrasonic elastography; MAS: modified Ashworth score.
3.5.2. Correlation between pain and motor function and emotion
KPPS score was positively correlated with UPDRS Ⅲ score (r = 0.414, P < 0.05) (Figure 3A), and KPPS score was positively correlated with HAMD score (r = 0.576, P < 0.01) (Figure 3B), suggesting that patients' pain experience was closely related to motor function and emotion.
Figure 3. Correlation between KPPS score and UPDRS Ⅲ, HAMD score.

A: correlation between KPPS score and UPDRS Ⅲ score; B: correlation between KPPS score and HAMD score. KPPS: King's Parkinson's Pain Scale; UPDRS Ⅲ: Unified-Parkinson Disease Rating for motor function examination; HAMD: Hamilton depression scale.
3.6. Safety evaluation
A small amount of bleeding and subcutaneous hematoma were observed at the acupuncture site in some patients in the electroacupuncture treatment group, which was pressed and disinfected with cotton swabs. Most of the hematoma could be relieved by itself, and no discomfort cases were observed in the electroacupuncture group and the control group during the follow-up, indicating that this research method had good safety.
4. DISCUSSION
As a common degenerative neurological disease in the elderly, PD mainly presents motor symptoms and non-motor symptoms clinically. In the non-motor symptoms, pain is relatively common and disturbs elderly patients to a large extent, causing different obstacles in their daily life and exercise ability. In China the research on PD pain has lagged behind relatively foreign countries, and in recent years, more and more experts in our country began to pay attention to this symptom.26 Studies have shown that 40% of PD patients find it difficult to accurately describe their pain feelings when seeing a doctor,12 so the pain symptoms of PD are often ignored in the diagnosis and treatment. Therefore, it is necessary to pay high attention to the pain symptoms of patients in the treatment of PD, and timely intervention to improve the quality of life of patients. We selected PD patients with pain as research objects to explore the clinical effect of electroacupuncture in improving the skeletal muscle pain of PD patients, providing reference for the treatment of this disease. It is also suggested that non-motor symptoms of PD may be a new direction for acupuncture to improve the daily living ability of PD patients.
In this study, acupuncture point selection is based on the experience of Professor He Puren, a Chinese medical master in our department.17 Baihui (GV20), Qihai (CV6), Lique (LU7), listening palace (SI19) mainly. Upper limb pain plus Jianyu (LI15) and Quchi (LI11), lower limb pain plus Xuehai (SP10) and Zusanli (ST36). Baihui will be the acupoint of the Du meridian, has the therapeutic effect of awakening the spirit, Qihai is the acupoint of the Ren meridian, can supplement the Qi and kidney, and the use of two points can adjust the governor, Qi and brain. Liyue deficiency for the hand Taiyin lung meridian of the collaterals, through the Ren meridian, there is a lung and wind, through the meridian activating collaterals. Listening Palace point is the hand sun small intestine meridian point, is the hand, foot Shaoyang and hand sun three meridian meeting, is Professor Hepuren's experience point in the treatment of Parkinson's disease, has the role of hearing ear opening, calming god and determination. With shoulder Jianyu, Quchi point of the upper limb, Xuehai and Zusanli of the lower limb, it can jointly play the effect of opening and benefiting the brain, stopping fibrillation and clearing collaterally.
This study found that electroacupuncture therapy can effectively improve skeletal muscle pain in patients with Parkinson's disease, reduce the muscle tention of patients, improve patients' daily living ability and improve mood disorders. Correlation studies have found that the degree of skeletal muscle pain in patients with Parkinson's disease is correlated with exercise ability and emotional disorders, while the degree of skeletal muscle pain is not significantly correlated with the muscle tention of patients.
Firstly, KPPS score and VAS score were used to evaluate skeletal muscle pain before and after treatment. KPPS score evaluated both pain severity and pain frequency, which could better explain the effect of pain improvement. The results showed that after treatment, KPPS and VAS scores in the treatment group were significantly lower than before treatment, and significantly lower than after treatment in the control group, while there was no statistically significant difference in KPPS and VAS scores in the control group before and after treatment, indicating that electroacupuncture can effectively improve skeletal muscle pain in patients with Parkinson's disease, and the efficacy is positive, while pseudoacupuncture showed no analgesic effect. Secondly, we evaluated the efficacy of electroacupuncture therapy on the primary disease PD by using UPDRSⅡ and UPDRSⅢ scores in the Parkinson's comprehensive score scale. The results showed that the UPDRSⅡ and UPDRSⅢ scores in the electro-acupuncture group were lower after treatment than before treatment, while there was no difference in the control group before and after treatment. These results indicate that electroacupuncture therapy can not only improve skeletal muscle pain, but also significantly improve PD patients' activities of daily living and motor function, and may also be effective for PD motor symptoms. Third, we used the subjective index of modified Ashworth score and the SWE technique to detect the long axis Young's modulus of biceps and quadriceps muscle and the objective index of shear wave elastography to evaluate the muscle tension of patients. The results showed that the biceps Young modulus, shear wave velocity, quadriceps shear wave velocity and Ashworth score of the electroacupuncture group were all lower than before treatment, but there was no difference before and after treatment in the control group, suggesting that electroacupuncture can significantly reduce the muscle tension of the upper and lower limbs of PD patients, which may be one of the mechanisms of improving the motor function of PD patients. When the skeletal muscle pain of PD patients is significant, the motor function is lost, and the quality of life is decreased, the patients are prone to bad emotions. Studies have shown that depression can occur at any stage of PD, with up to 40% of PD patients experiencing depression at the onset of the disease and up to 70% of PD patients experiencing depressive symptoms at advanced stages.27 Therefore, HAMD score was used for evaluation before and after treatment in this study, and it was found that HAMD score was significantly reduced after electroacupuncture treatment, indicating that depression status was also significantly improved, which may be related to reducing patients' pain perception and improving exercise ability.
In order to further analyze the correlation between pain and muscle tension, exercise ability and emotion, this study was verified by Spearman non-parametric correlation analysis. The results showed that there was no correlation between KPPS score and Ashworth score, biceps Young modulus and biceps shear wave velocity, suggesting that there was no clear correlation between skeletal muscle pain and muscle tension. However, some studies have suggested that the degree of skeletal muscle pain in PD patients may be related to the increase in muscle tone,7 but no such correlation was found in this study, and the analysis may be related to the small sample size. KPPS score is positively correlated with UPDRS Ⅲ score and HAMD score, indicating that skeletal muscle pain in PD patients can affect their exercise ability and lead to emotional disorders, which is the same as previous research results.28 The improvement of skeletal muscle pain after electroacupuncture is helpful to improve patients' exercise ability and mood, but the mechanism of electroacupuncture to improve skeletal muscle pain in PD patients needs further research, and the efficacy of acupuncture therapy on PD non-motor symptoms also needs more research to be clarified.
Although this study found some valuable results, it still has some limitations: we were not able to conduct a large multi-center trial due to the limited number of patients enrolled in Parkinson's disease, which may affect the final results; because the results were assessed on a clinical scale, there may be bias. In addition, longer follow-up is needed to verify the continued clinical effectiveness of the intervention.
Contributor Information
Jingqing SUN, Email: sunjingqing@bjzhongyi.com.
Yingxue CUI, Email: yingxuecui@163.com.
REFERENCES
- 1. Antonini A, Tinazzi M. . Targeting pain in Parkinson’s disease. Lancet Neurol 2015; 14: 1144-5. [DOI] [PubMed] [Google Scholar]
- 2. Silverdale MA, Kobylecki C, Kass-Iliyya L, et al. . A detailed clinical study of pain in 1957 participants with early/moderate Parkinson’s disease. Parkinsonism Relat Disord 2018; 56: 27-32. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3. Ernst M, Folkerts AK, Gollan R, et al. . Physical exercise for people with Parkinson's disease: a systematic review and network Meta-analysis. Cochrane Database Syst Rev 2023; 1: CD013856. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4. Kim YE, Kim HJ, Yun JY, et al. . Musculoskeletal problems affect the quality of life of patients with Parkinson’s disease. J Movem Disord 2018; 11: 133-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5. Tueth LE, Duncan RP. . Musculoskeletal pain in Parkinson’s disease: a narrative review. Neurodegener Dis Manag 2021; 11: 373-85. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6. Kim YE, Lee WW, Yun JY, Yang HJ, Kim HJ, Jeon BS. . Musculoskeletal problems in Parkinson’s disease: neglected issues. Parkinsonism Relat Disord 2013; 19: 666-9. [DOI] [PubMed] [Google Scholar]
- 7. Chaudhuri KR, Rizos A, Trenkwalder C, et al. . King’s Parkinson’s disease pain scale, the first scale for pain in PD: an international validation. Mov Disord 2015; 30: 1623-31. [DOI] [PubMed] [Google Scholar]
- 8. Butera KA, Roff SR, Buford TW, Cruz-Almeida Y. . The impact of multisite pain on functional outcomes in older adults: biopsychosocial considerations. Pain Res 2019; 12: 1115-25. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9. Wasner G, Deuschl G. . Pains in Parkinson disease-many syndromes under one umbrella. Nat Rev Neurol 2012; 8: 284-94. [DOI] [PubMed] [Google Scholar]
- 10. Deuel LM, Seeberger LC. . Complementary therapies in Parkinson disease: a review of acupuncture, Taichi, Qigong, Yoga, and Cannabis. Neurotherapeutics 2020, 17: 1434-55. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11. Jang JH, Yeom MJ, Ahn S. . Acupuncture inhibits neuroinflammation and gut microbial dysbiosis in a mouse model of Parkinson's disease. Brain Behav Immun 2020; 89: 641-55. [DOI] [PubMed] [Google Scholar]
- 12. Fan JQ, Lu WJ, Tan WQ. . Acupuncture for Parkinson's disease: from theory to practice. Biomed Pharmacother 2022; 149: 112907. [DOI] [PubMed] [Google Scholar]
- 13. Wang S, Guo J, Feng Q, et al. . Effectivenss of “Rou Jin Zhi Tong” needling on the treatment of patients with Parkinson's disease accompanied by different types of pain. Zhong Yi Za Zhi 2021; 62: 609-14. [Google Scholar]
- 14. Parkinson's disease and movement disorders group, Chinese society of neurology; Chinese medical doctor association, branch of neurology, Parkinson's disease and movement disorders. . Diagnostic criteria of Parkinson's disease in China (2016 edition). Zhong Hua Shen Jing Ke Za Zhi 2016; 49: 268-71. [Google Scholar]
- 15. Lyu Y, Cheng J, Fan B, et al. . ICD-11 classification of chronic pain Chinese compiled version. Zhong Guo Teng Tong Yi Xue Za Zhi 2018; 24: 801-5. [Google Scholar]
- 16. Li J, Zhu B, Gu Z, et al. . Musculoskeletal pain in Parkinson’s disease. Front Neurol 2022; 12: 756538. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17. He P. . Clinical application of acupuncture and moxibustion “He Shi San Tong” Method (TCM master He Puren's acupuncture and moxibustion heart method series). Beijing: People's Medical Publishing House, 2014: 77- 8. [Google Scholar]
- 18. Institute of acupuncture and moxibustion, China academy of Chinese medical sciences. . Name and location of meridian points. Beijing: State Administration for Market Regulation, Standardization Administration, 2021: 8, 10, 19, 14, 15, 37, 38. [Google Scholar]
- 19. Feng S, Li B, Zhang H, et al. . Placebo control and methodological problems in acupuncture clinical trials. Zhong Guo Zhen Jiu 2021, 42: 437-41. [DOI] [PubMed] [Google Scholar]
- 20. Martinez-Martin P, Rizos AM, Wetmore J, et al. . First comprehensive tool for screening pain in Parkinson’s disease: the King's Parkinson's disease pain questionnaire. Eur J Neurol 2018; 25: 1255-61. [DOI] [PubMed] [Google Scholar]
- 21. Li Q. . Technical progress of ultrasonic shear wave elastography. Zhong Guo Yi Liao She Bei 2017; 32: 101-5. [Google Scholar]
- 22. Feng Y. . Clinical anesthesia series:pain volume. Beijing: Peking University Medical Press, 2010: 24- 5. [Google Scholar]
- 23. Goetz CG, Stebbins GT, Chmura TA, Fahn S, Poewe W, Tanner CM. . Teaching program for the movement disorder society‐sponsored revision of the unified Parkinson's disease rating scale: (MDS‐UPDRS). Movem Disord 2010; 25: 1190-4. [DOI] [PubMed] [Google Scholar]
- 24. Rw B, Smith M. . Interrater reliability of a modified ashworth scale of muscle spasticity. Phys Ther 1987; 67: 206-7. [DOI] [PubMed] [Google Scholar]
- 25. Beck AT, Ward CH, Mendelson M, Mock J, Erbaugh J. . An inventory for measuring depression. Arch Gener Psychiat 1961; 4: 561-71. [DOI] [PubMed] [Google Scholar]
- 26. Antonini A, Barone P, Marconi R, et al. . The progression of non-motor symptoms in Parkinson’s disease and their contribution to motor disability and quality of life. J Neurol 2012; 259: 2621-31. [DOI] [PubMed] [Google Scholar]
- 27. Aarsland D, Brønnick K, Alves G, et al. . The spectrum of neuropsychiatric symptoms in patients with early untreated Parkinson's disease. J Neurol Neurosurg Psychiatry 2009; 80: 928-30. [DOI] [PubMed] [Google Scholar]
- 28. Cai L. . Clinical assessment of pain symptoms and associated factor analysis. In: Neurology Professional Committee of Jiangxi Society of Integrated Traditional Chinese and Western Medicine, editors. Compilation of papers of the eighth Academic Exchange meeting of Neurology Professional Committee of Jiangxi Society of Integrated Traditional Chinese and Western Medicine; 2019 May 31; Jiangxi, China. Nanchang: Neurology Professional Committee of Jiangxi Society of Integrated Traditional Chinese and Western Medicine, 2019: 4- 5. [Google Scholar]