Abstract
Introduction
Providing hemodialysis to patients with kidney failure (KF) in conflict-affected areas poses a significant challenge. Achieving and sustaining reasonable quality hemodialysis operations in such regions necessitates a comprehensive approach.
Methods
In the conflict area of Northwest (NW) Syria, a 3-phase project was initiated to address the quality of hemodialysis operations. The assessment phase involved the examination of infection prevention and control (IPC) protocols, staff training, medical protocols, individualized hemodialysis prescriptions, and laboratory testing capabilities. The second phase involved activities toward capacity building and implementing an action plan based on feasibility and sustainability.
Results
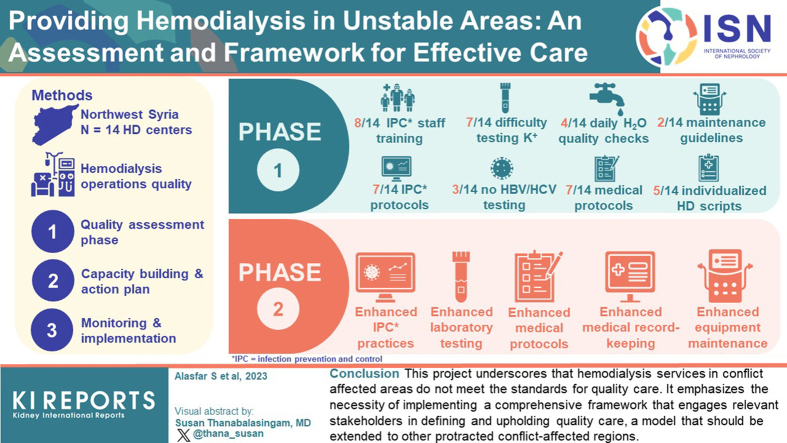
The assessment phase revealed that only 7 of 14 centers had IPC protocols, and 8 centers provided IPC training for their staff. Furthermore, only 7 centers had medical protocols, and 5 used individualized hemodialysis prescriptions. Difficulties in testing for potassium was reported in 7 centers and the inability to perform hepatitis B and C serologies was reported in 3 centers. Only 2 centers adhered to machine and water treatment system maintenance guidelines, and 4 conducted daily water quality checks. Recommendations were formulated, and an action plan was developed for implementation in the second phase. The plan encompassed enhancements in IPC practices, medical protocols, record-keeping, laboratory testing, and equipment maintenance.
Conclusion
This project underscores that hemodialysis services in conflict-affected areas do not meet the standards for quality care. It emphasizes the necessity of implementing a comprehensive framework that engages relevant stakeholders in defining and upholding quality care, a model that should be extended to other protracted conflict-affected regions.
Keywords: conflict, hemodialysis, kidney failure, wars
Graphical abstract
Managing KF with kidney replacement therapies requires complex infrastructure that is vulnerable to disruption during disasters, including armed conflicts.1,2 Patients undergoing dialysis for KF require regular access to dialysis facilities, machines, laboratory testing, medications, trained staff, and monitoring to maintain their health. However, continued access to these is often limited or disrupted in regions of conflict, leading to poor quality dialysis services and life-threatening complications. The vulnerability of infrastructure presents a unique set of challenges for humanitarian agencies and organizations working in the health sector to manage dialysis patients in areas affected by protracted conflict.
Despite the global increase in armed conflicts and the typically high prevalence of kidney disease in affected low and middle-income regions, humanitarian aid efforts have not adequately considered or addressed the management of KF in protracted armed conflict zones.3 This is partly because of patients with KF not being prioritized by humanitarian agencies, as well as the perceived and real challenges and complexity of administering dialysis, and the costs and logistics of maintaining its services. In addition, the need for dialysis services increases in these circumstances due to crush injuries, while the systems responsible for providing these services are deteriorating. In areas where some dialysis services have been maintained or resumed, the recent literature has revealed significant deficiencies and poor outcomes for patients with KF living in these areas.4, 5, 6, 7
Approximately 800 individuals with KF reside in NW Syria, which has been experiencing ongoing armed conflict since 2011.3 This area has a population of 4.5 million, of whom 2.8 million are internally displaced people. Furthermore, 3.3 million individuals are food insecure and have numerous comorbidities.8,9 Non-governmental organizations (NGOs), both international and local, have taken over the management of dialysis centers in the area. Reports indicating deficiencies in dialysis operations and of an increasing prevalence of hepatitis among patients on dialysis prompted the initiation of the "Improving Hemodialysis Services in Northwest Syria" quality improvement project.3,7 The project is a collaborative effort between the hemodialysis taskforce of the health cluster hub in Gaziantep, Turkey, led by the World Health Organization and Johns Hopkins University.3,8 In our recent call to action paper, we highlighted the preliminary findings about deficits in the standards of care at dialysis centers. These findings led to the development of an action plan aimed at improving the provision of care to meet minimum patient care standards.3
In this article, we present the detailed outcomes from the first phase of the project, where various aspects of baseline hemodialysis quality were evaluated. We then describe the second phase, which centered on devising an action plan to address the deficiencies and gaps identified in the initial phase. In addition, we outline a conceptual framework that we have developed to tackle these challenges, which holds potential for future use in other regions affected by protracted conflicts.
Methods
Project Overview
Baseline information on dialysis operations and a situational analysis were collected in phase 1. In phase 2, the findings were utilized to establish agreed-upon minimal IPC and medical quality standards and build capacity to meet them. In phase 3, a monitoring and support supervision system will be implemented to track and sustain performance which meets these agreed-upon standards. During the first and second phases, an iterative process was undertaken through a combination of assessment instrument administration, small group meetings, and group workshops to conduct several activities simultaneously. Activities of the first 2 phases took place between October 2021 and June 2022. In accordance with ethical guidelines and regulations, this study has been approved by the Institutional Review Board of the Johns Hopkins University School of Public Health.
Assessment Instrument
In phase 1, a US-based Syrian American nephrologist led the development of an assessment instrument following accepted US hemodialysis standards, which was then modified with input from US-based and NW Syria-based dialysis experts (Supplementary Table S1). The assessment covered various areas related to hemodialysis, including current IPC practices, medical protocols, built environment, healthcare worker competencies, dialysis equipment maintenance, dialysis unit management and leadership, facility record keeping, and barriers to quality service delivery. The IPC assessment followed the World Health Organization IPC guidelines.10 A pilot of the assessment instrument was conducted, which helped refinement of the instrument for a full assessment based on the review of results. A data collection committee was created to gather data from dialysis units inside NW Syria, health authorities, and members of the hemodialysis taskforce of the health cluster. The taskforce is composed of organizations supporting hemodialysis in NW Syria. The final assessment instrument consisted of 346 questions and data were collected by the committee through in-person visits to dialysis centers, which involved observations, interviews with dialysis center managers and technicians, and data extracted from facility records.
Workshops and Small Group Interviews
During the first and second phases of the study, separate interviews were conducted with individual representatives of NGOs, senior dialysis technicians, and members of the hemodialysis taskforce. The interviews covered topics such as management at dialysis centers, their perception of quality, IPC practices and training, recent quality initiatives, and barriers to providing quality services. In addition, 4 workshops were held in the Turkish border city of Gaziantep during the first 2 phases. These workshops were attended by the Johns Hopkins team, representatives of NGOs administering dialysis, the hemodialysis taskforce, and health authorities from inside NW Syria.
Action Plan Development
After completing the initial phase and first 2 workshops, the project team analyzed the data collected and formulated recommendations to address the identified deficiencies in the management of KF in NW Syria. Based on these recommendations, a comprehensive work plan was developed for implementation during the second phase of the project. The action plan was designed to involve as many relevant stakeholders as possible, including healthcare providers, NGOs, and local policymakers. The work plan included several activities, such as training programs for healthcare providers, ensuring sustainable provision of essential medical supplies and equipment, and the development of a patient-centered approach to care.
Analysis
The assessment instrument was converted to a Kobo format for data collection and analysis. The dataset was checked for missing data and outliers. Continuous variables were presented as raw numbers, median, and interquartile range. Discrete variables were presented as percentages. Notes of the small-group interviews and workshops were reviewed for common themes to achieve understanding of participants’ perceptions. No unique patient identifiers were collected.
Results
Hemodialysis Centers
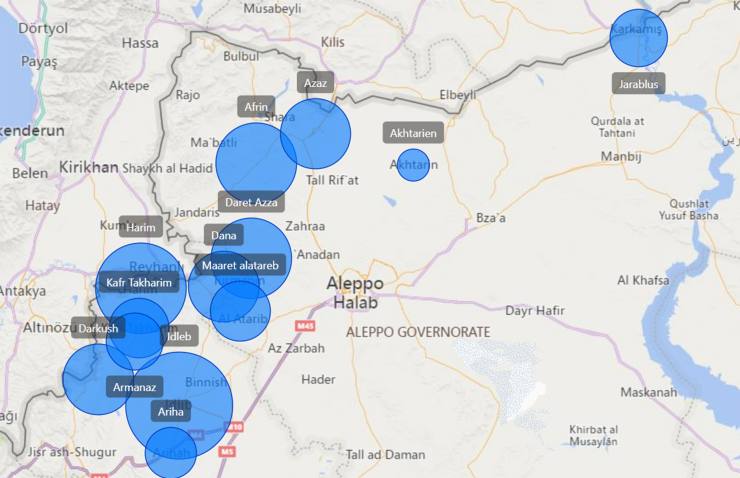
The geographic location of the 14 dialysis centers and their relative sizes are shown in Figure 1. Of the 14 dialysis centers, 3 were associated with hospitals, whereas the rest were standalone facilities. No center offered peritoneal dialysis. Dialysis centers reported 764 patients with KF at the time of survey; 59 patients appeared to be registered at more than 1 unit. The median number of new patients added per month for each center was 2 (interquartile range: 1–3). The median number of patients who discontinued dialysis or transferred per center per month was 2.5 (interquartile range: 1–4). Patient death records were available in 4 of the 14 dialysis centers. The median number of monthly hemodialysis sessions per center was 383 (74–474) and median number of patients with KF per center in the prior month was 45 (31–61) (Supplementary Figure S1).
Figure 1.
Geographic location and relative size of the hemodialysis centers in NW Syria.
IPC Practices and Medical Service Quality
In Table 1 and Supplementary Table S2, we present the responses to selected IPC practice questions. Seven of the 14 hemodialysis centers (50%) reported having an IPC protocol in place. Eight centers conducted general IPC training for staff. Medical service quality indicators are shown in Table 2 and Supplementary Table S3. Hemodialysis is administered twice weekly for all patients because of shortage in dialysis kits and a lack of knowledge among the staff regarding dialysis standards of care. None of the centers performed dialysis adequacy measures routinely. Seven centers (50%) had established medical protocols in place. Five of 14 centers (36%) lacked individualized patient hemodialysis prescriptions, and 9 of 14 (64%) had comprehensive care plans by a nephrologist. Two of 14 (14%) centers followed a manufacturer’s hemodialysis machine maintenance checklist, 4 of 14 centers (29%) performed daily checks for chlorine or chloramine levels before the first treatment. There was limited access to laboratory testing for potassium (7/14 centers, 50%), calcium and phosphorus (2/14, 14%), and hepatitis B and C serology (3/14, 21%).
Table 1.
Selected responses related to infection prevention and control
| Item | Result | |
|---|---|---|
| Presence of IPC protocol | ||
| IPC protocol present | 7/14 (50%) | |
| Source of IPC Protocol | National guidelines | 1/7 (14%) |
| Organization guidelines | 4/7 (57%) | |
| Local physician/nurse | 2/7 (29%) | |
| Presence of IPC advisor | 5/14 (36%) | |
| Key components of IPC | ||
| Written guidance on hepatitis B and C testing | 6/7 (85%) | |
| Effective cleaning & disinfection of equipment | 6/7 (85%) | |
| IPC training | ||
| IPC training in the last 12 months | 8/14 (43%) | |
| Training on accessing dialysis access and dialysis access infection | 6/8 (75%) | |
| IPC surveillance | ||
| Process to review surveillance results | 4/7 (57%) | |
| Frequency of screening for hepatitis B and C | Every 3 months | 2/14 (14%) |
| Every 6 months | 11/14 (79%) | |
| Screening staff for hepatitis B and C | 10/14 (71%) | |
| IPC implementation | ||
| Hepatitis B patients undergo hemodialysis in isolation | 8/14 (57%) | |
| Staff who are not vaccinated for hepatitis B are allowed to administer dialysis to patients with hepatitis B | 2/14 (14%) | |
| Staff caring for patients with hepatitis B are allowed to care for patients without hepatitis B at the same time | 12/14 (86%) | |
| IPC monitoring | ||
| Regular assessment of prevalence of infections | 8/14 (57%) | |
| Written procedures to examine infection control practice as soon as a patient is found to have hepatitis B or C or if there in an infection outbreak | 2/14 (14%) | |
| Built environment and supplies | ||
| The design of the unit follows a national or international guideline for dialysis units | 3/14 (21%) | |
| IPC records | ||
| IPC training Records | Yes | 4/14 (29%) |
| No | 4/14 (29%) | |
| No training received | 6/14 (43%) | |
| Records of patients’ hepatitis B vaccination | 3/14 (21%) | |
| Records of patients’ COVID-19 vaccination | 1/14 (7%) | |
IPC, infection prevention and control.
Table 2.
Selected Responses regarding medical quality indicators
| Item | Result | |
|---|---|---|
| Medical protocols | ||
| Medical protocols present | 7/14 (50%) | |
| Individualized dialysis prescription | 9/14 (64%) | |
| Comprehensive assessments by a nephrologist | 5/14 (36%) all monthly | |
| Medical records for each dialysis visit | 12/14 (86%) | |
| Record of patients’ death | 3/14 (21%) | |
| Equipment and maintenance | ||
| Frequency of dialysis machines maintenance per year | 0 | 2/12 (16%) |
| 1 | 3/12 (25%) | |
| 2 | 4/12 (33%) | |
| 3 | 4/12 (33%) | |
| 4 | 1/12 (8%) | |
| Dialysis maintenance follows the manufacturer check list | 2/12 (16%) | |
| Regular maintenance for water treatment system | 2/14 (14%) | |
| Water quality assessment done in the last 12 months | 5/14 (36%) | |
| Access to laboratory testing | ||||
|---|---|---|---|---|
| How easy is it to get laboratory testing? | Easy | Moderate | Difficult | Not possible |
| Hemoglobin/Hematocrit | 12 (86%) | 2 (14%) | 0 (0%) | 0 (0%) |
| Calcium and phosphorus | 7 (50%) | 5 (36%) | 1 (7%) | 1 (7%) |
| Potassium | 4 (29%) | 3 (21%) | 2 (14%) | 5 (36%) |
| PTH | 4 (29%) | 1 (7%) | 1 (7%) | 8 (57%) |
| Iron studies | 7 (50%) | 1 (7%) | 1 (7%) | 5 (36%) |
| Hepatitis B serology | 10 (71%) | 1 (7%) | 1 (7%) | 2 (14%) |
| Hepatitis C serology | 10 (71%) | 1 (7%) | 1 (7%) | 2 (14%) |
| Blood culture | 0 (0%) | 0 (0%) | 3 (21%) | 11 (79%) |
PTH, parathyroid hormone.
Workshops
Each workshop commenced with an introductory session highlighting the project's objectives. This was followed by an update on the project's advancement. Subsequently, participants were divided into groups, each assigned to address the workshop objectives as identified below. The workshops concluded with a comprehensive summary and a forward-looking discussion on the upcoming stages.
The workshops were guided by the Johns Hopkins University team, comprising a professor in public health who is specialized in planning programs to address humanitarian health challenges during disasters, and a US-based nephrologist fluent in Arabic. The attendee roster encompassed the leader of the World Health Organization Health Cluster hemodialysis taskforce, a Syrian physician, and public health practitioner. Accompanying them were other members from the taskforce, which included a practicing nephrologist and program manager, both operating within NW Syria. Furthermore, representatives from NGOs responsible for executing dialysis initiatives were in attendance. These participants had a diverse background, ranging from physicians and nurses to public health practitioners, all involved in the management of dialysis programs in their NGO. A representative from the health directorate in NW Syria was also present. The overall attendance fluctuated within the range of 15 to 20 participants per workshop.
In the first workshop, participants used an Ishikawa fishbone diagram to identify and categorize problems into 6 categories, which include protocols and procedures, medicines and supply chain, healthcare worker skills, equipment and their maintenance, built environment, and patients’ understanding and compliance.11 In Supplementary Table S4, we summarize these problems and solutions suggested by participants. The second workshop focused on mapping the changes needed to reach the desired solution using the Theory of Change model, with participants working in separate teams on IPC, medical quality and protocols, equipment and supplies, laboratory support, and record keeping.12 The workshop resulted in recommendations and a vision of action utilizing available resources. The third workshop involved developing minimum standards of performance for IPC and medical quality, taking into consideration the low resource environment of NW Syria, with a set of quality indicators selected for monitoring during the third phase activities. Finally, the fourth workshop established the basic outline for the future project third phase of monitoring and support supervision.
Developing and Implementation of the Action Plan
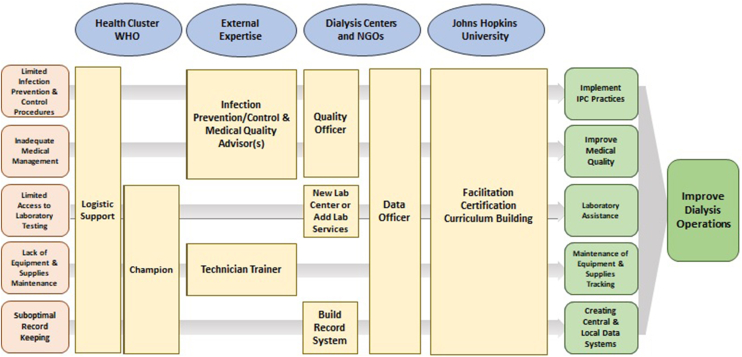
An action plan was developed to improve IPC practices, medical quality services, record keeping, laboratory testing, and equipment maintenance, which were identified as high priority categories during the second workshop. A range of stakeholders were engaged in various aspects of the action plan, with external advisors in dialysis medical quality and IPC practices providing support. In the second phase, available curricula and protocols addressing IPC and medical quality were reviewed and modified. On-site and online, a 4-day training program was conducted for dialysis nurses and technicians. This comprehensive course was led by both Syrian and international nephrologists in accordance with the developed curriculum. Standard forms for record keeping were developed and distributed to dialysis facilities; and standardized protocols for laboratory testing were created. Building a central laboratory site was deemed unfeasible because of transportation difficulties in the conflict-affected area of NW Syria. Dialysis machine and water treatment system maintenance was identified as a high priority. Two weeks of training for biotechnicians is planned as soon as suitable candidates are selected. Because of the scarcity of nephrologists in the area, with only 2 actively practicing, 1 dialysis technician per center has been appointed as a quality officer for the upcoming support supervision phase. The action items and stakeholders involved in implementing the action plan are illustrated in Figure 2.
Figure 2.
Action plan for second phase including stakeholders and their roles. NGO, Non-governmental organization; WHO, World Health Organization.
Discussion
There is limited literature that describes the impact of protracted armed conflict on patients with KF and hemodialysis operations.3,13 The findings of the first phase of the Improving Hemodialysis Services in NW Syria project highlight the critical gaps in dialysis management in protracted conflict zones. Crucial aspects of dialysis quality were inconsistently implemented. In addition, maintenance of dialysis machines and water quality checks were inadequate. The presence of essential personnel such as nephrologists and machine biotechnicians was variable.
To provide an understanding of the context, it is important to note that before the outbreak of the conflict, Syria faced significant health challenges common to many areas in low and middle-income countries. There is limited literature on the management of patients with KF in Syria before the war; however, the available publications reveal that the existing infrastructure before the war was already strained, and the frequency of dialysis treatments provided were below the recommended level. A report from the Syrian Ministry of Health, which was published 6 years before the conflict, estimated there were about 10,000 patients with KF and pointed out that existing units performed 150,000 dialysis sessions per year.6 Based on these numbers, Sekkarie et al.6 calculated the dialysis frequency to be 2 sessions/patient/week. Under the original system, patients received dialysis in government-owned hospital-based facilities for free or at discounted rates, or at private clinics for a fee.6 A cross-sectional study conducted in 2006 in Aleppo City suggests that the incidence rate of dialysis was relatively low because of the high cost associated with treatment. The study found that 550 patients were undergoing hemodialysis for end-stage renal disease in Aleppo City during 2006, with 145 new patients during the same period. Accordingly, the hemodialysis incidence rate was 60 per million population per year and the prevalence rate was 226 per million population, in comparison to the global incidence range of 85 to 378 per million population per year and a prevalence of 759 per million.14,15 There was no peritoneal dialysis in Syria before the war.6
During conflict, in addition to insecurity and the disruption of civil infrastructure that is necessary for dialysis such as water, electricity, and secure built environment; there is disruption in transportation and delivery of aid, and the targeting of healthcare facilities.1,4,7,16, 17, 18 The skilled workforce is often targeted for assassination, or they may migrate to seek better living conditions.19 Moreover, organizations providing dialysis care in conflict zones often face funding challenges. This leaves facilities struggling to secure new sources of funding and decide which aspects of the dialysis operation to prioritize with the limited resources. Although some consider it an ethical concern to prioritize hemodialysis for a small number of patients (with a high and disproportionate requirement for resources) when there are other pressing needs, the needs of this highly vulnerable group of patients cannot be simply ignored, especially when conflicts become chronic and a degree of “normality”. In addition, NGOs trying to implement dialysis in conflict zones without the requisite expertise may contribute to the deficiencies observed.3 The independent nature of these implementing organizations has often been a challenge for coordination of methods, resources, information, and duplication of efforts.20, 21, 22 Compounding these challenges is the frequent absence of minimal standards for dialysis in such settings, which lead to a degree of therapeutic nihilism, given that international standards may not be achievable. Importantly, conflict and natural disasters can give rise to their own causes of KF, such as crush injuries, infections, and exposure to toxins. These events can also worsen existing health issues in patients on chronic dialysis, all further stretching the fragile dialysis capacities. This was evident during the earthquake in February 2023 that impacted the same area in NW Syria and pushed the capacity of dialysis facilities to the extreme.13
With the incidence of kidney disease on the rise in low and middle-income countries where many persons are displaced by protracted conflict, it is crucial for dialysis implementing agencies such as NGOs to have access to expertise in dialysis administration and resources to build quality dialysis units that meet minimum standards.23 A comprehensive training program for local NGOs by the international nephrology community could help bridge the knowledge gap and improve the quality of dialysis care in conflict zones utilizing the available resources such as the International Society of Nephrology framework on administering dialysis in low-resources environment.24 Postgraduate medical education to train new nephrologists exists in NW Syria but it is not sufficient.17,25 To coordinate dialysis care among numerous agencies operating in an affected area, local leadership bodies are essential. The Sphere standards developed in 1997 and the United Nations humanitarian reforms with the cluster system in 2005 have significantly improved the quality of healthcare as well as coordination within the humanitarian health sector in areas affected by conflict, and these clusters can assume this role.26 International and regional nephrology organizations that have experience in such settings, such as the Renal Disaster Preparedness Working Group from the International Society of Nephrology and the Renal Disaster Relief Task Force of the European Renal Association can work with the health clusters to incorporate awareness and develop comprehensive guidance to meet the complex needs of persons with KF in humanitarian emergencies. Other initiatives such as the Syrian National Kidney Foundation, can contribute their expertise in program planning in areas of protracted disasters or conflict. The health cluster is frequently activated in areas affected by disaster or conflict, with 26 currently being activated.27
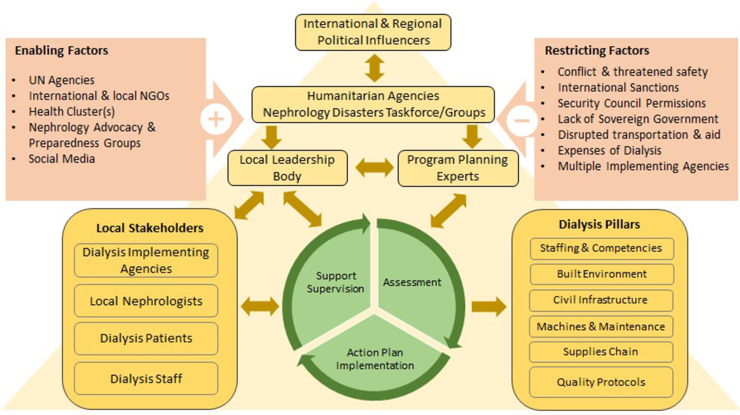
The "Improving Hemodialysis Services in Northwest Syria" project provides a framework for these local leadership bodies and an action plan for stakeholders to collaborate in improving the quality of dialysis services (Figure 3) and establishing achievable standards. The framework's strength lies in its iterative process, allowing for continuous refinement of the plan to accommodate evolving needs in conflict settings. The framework is centered around a quality improvement initiative that starts with an assessment phase. To perform this assessment, a combination of methods such as assessment instruments, small group meetings, and workshops are necessary to identify the best solutions that fit low-resource environments in conflict settings and continuously modify the priorities as needed. The second step after the assessment was to create an action plan, considering limited resources and utilizing available expertise from both outside and local sources while increasing coordination between implementing NGOs. Establishing a governance or leadership body is crucial to ensure coordinated implementation of the action plan. In this case, the health cluster hub in Turkey, which coordinates more than 50 health organizations and provides cross-border assistance into NW Syria, played this role. The quality improvement project also includes a supportive supervision phase to ensure the long-term sustainability of quality dialysis services and refine plans as circumstances dictate. Agreeing on minimal standards, and a data collection system and dashboard to monitor quality indicators should be part of the action plan to launch the next phase of support supervision. This will help identify areas of improvement and ensure that quality care is being provided to patients.
Figure 3.
Framework for assessment and improving dialysis services in areas affected by protracted armed conflict. NGO, Non-governmental organization
As the action plan is being developed within this framework, it is essential to engage different stakeholders in these distinct phases, including agencies implementing dialysis such as NGOs, dialysis staff, local nephrologists and physicians, local leadership bodies, experts in program planning in areas affected by conflict, and most importantly, patients. The action plan should target multiple levels. The first level is dialysis staff and equipment, which is the foundation of dialysis. This can be achieved by creating a tailored dialysis training curriculum and implementing protocols to empower the staff and build necessary capacities. In addition, providing support and enforcing these protocols by the implementing NGOs is essential. At the next level, it is crucial to empower the local leadership body and establish trust between them, implementing NGOs, and dialysis staff. Providing the local leadership body with the necessary expertise in dialysis and resources is essential for effective collaboration and management. For NW Syria, the World Health Organization health cluster played this role by establishing the hemodialysis task force. Furthermore, advocacy at the international level and to regional political influencers through political channels and social media is necessary to increase awareness of the struggles of patients with KF and ensure the continuous delivery of supplies and support to the implementing agencies.
Although our framework is comprehensive, there are some limitations to our project. One key limitation is the lack of patient engagement, which could have provided valuable insights into the patient’s experience of hemodialysis in conflict zones. In addition, although we collected data from dialysis unit administrators, technicians, and nurses, there is a concern that the information from administrators may not have captured all operational details. Furthermore, it is important to acknowledge that performance standards established in this project may not match practices in high-income countries; however, the goal is to achieve the optimal levels of performance, given the existing resources. By setting realistic performance levels, there is a greater chance of sustainability, which is critical for providing ongoing care to patients with KF in conflict zones.
In summary, prolonged conflict disrupts noncommunicable disease programs. Existing hemodialysis services are particularly sensitive to disruption, considering the sophisticated nature of services and the sensitivity of operations, which can easily lead to a reduction in the quality of care. Considering that dialysis care plays a critical role in supporting not only patients but also their households, it is crucial to address these challenges. This paper highlights the deficits in hemodialysis operations in these circumstances and proposes a conceptual framework for assessing and planning programs aimed at improving the quality of hemodialysis care for individuals with KF in unstable areas. The framework engages all stakeholders involved in the delivery of care. Although developed in response to the situation in Syria, the framework can be applied in similar contexts with minor adjustments. Dialysis operations without minimum standards pose a significant risk to patients and dialysis staff, and it is the responsibility of the nephrology community and humanitarian agencies to ensure that patients receive dialysis care with reasonable quality.
Disclosure
SA reports research/grant support from Shire and CareDx. VL is a member of the International Society of Nephrology’s Renal Disaster Preparedness Working Group and the Renal Disaster Relief Task Force of the European Renal Association. All the other authors declared no competing interests.
Acknowledgment
We acknowledge the following non-governmental organizations that are active in hemodialysis services in northwest Syria: Afaq, Al-Ameen, Bahar, Islamic Relief Worldwide, Hand In Hand For Aid and Development (HIHFAD), Shafakq, Syrian American Medical Association (SAMS), Syria Relief and Development (SRD), Union of Medical Care and Relief Organizations (UOSSM), Syrian Expatriate Medical Association (SEMA), and Physicians Across Continent (PAC). Source of support is the World Health Organization Assessment of Hemodialysis Service delivery Grant 2021/1128207-1.
Footnotes
Figure S1. Service volume of each dialysis center in Northwest Syria.
Table S1. Phase 1 assessment instrument.
Table S2. Answers to questions of phase 1 assessment instrument related to infection prevention and control.
Table S3. Answers to questions of phase 1 assessment instrument related to medical quality indicators.
Table S4. Problem identification and solution proposals as suggested by workshop participants.
Supplementary Material
Figure S1. Service volume of each dialysis center in Northwest Syria.
Table S1. Phase 1 assessment instrument.
Table S2. Answers to questions of phase 1 assessment instrument related to infection prevention and control.
Table S3. Answers to questions of phase 1 assessment instrument related to medical quality indicators.
Table S4. Problem identification and solution proposals as suggested by workshop participants.
References
- 1.Sekkarie M., Murad L., Al-Makki A., Al-Saghir F., Rifai O., Isreb M. End-stage kidney disease in areas of armed conflicts: challenges and solutions. Semin Nephrol. 2020;40:354–362. doi: 10.1016/j.semnephrol.2020.06.003. [DOI] [PubMed] [Google Scholar]
- 2.Berhe E., Ross W., Teka H., Abraha H.E., Wall L. Dialysis service in the embattled Tigray region of Ethiopia: a call to action. Int J Nephrol. 2022;2022 doi: 10.1155/2022/8141548. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Alasfar S., Alashavi H., Nasan K.H., et al. Improving and maintaining quality of hemodialysis in areas affected by war: a call to action. Kidney Int. 2023;103:817–820. doi: 10.1016/j.kint.2023.02.004. [DOI] [PubMed] [Google Scholar]
- 4.Alasfar S., Isreb M., Kaysi S., Hatahet K. Renal transplantation in areas of armed conflict. Semin Nephrol. 2020;40:386–392. doi: 10.1016/j.semnephrol.2020.06.006. [DOI] [PubMed] [Google Scholar]
- 5.Berhe E., Paltiel O., Teka H., et al. Ethiopia’s Tigray dialysis service cut due to dwindling supplies amid war. Kidney Int Rep. 2022;7:1136–1137. doi: 10.1016/j.ekir.2022.02.024. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Sekkarie M.A., Zanabli A.R., Rifai A.O., Murad L.B., Al-Makki A.A. The Syrian conflict: assessment of the ESRD system and response to hemodialysis needs during a humanitarian and medical crisis. Kidney Int. 2015;87:262–265. doi: 10.1038/ki.2014.336. [DOI] [PubMed] [Google Scholar]
- 7.Isreb M.A., Kaysi S., Rifai A.O., et al. The effect of war on Syrian refugees with end-stage renal disease. Kidney Int Rep. 2017;2:960–963. doi: 10.1016/j.ekir.2017.05.009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Burnham G.M., Alashavi H., Alasfar S. Quality improvement methods to strengthen hemodialysis in Northwest Syria. J Glob Health Sci. 2022;4:e16. doi: 10.35500/jghs.2022.4.e16. [DOI] [Google Scholar]
- 9.United Nations Office for the Coordination of Humanitarian Affairs NORTH-WEST SYRIA Situation Report. https://reports.unocha.org/en/country/syria/
- 10.World Health Organization Infection prevention and control assessment framework at the facility level. https://www.who.int/publications/i/item/WHO-HIS-SDS-2018.9 Published 2018.
- 11.Ishikawa K., Loftus J.H. 3rd ed. 3A Corporation; 1990. Introduction to Quality Control. [Google Scholar]
- 12.Ajzen I. The theory of planned behavior. Organ Behav Hum Decis Processes. 1991;50:179–211. doi: 10.1016/0749-5978(91)90020-T. [DOI] [Google Scholar]
- 13.Alasfar S., Zakaria W., Nasan K.H., et al. Dealing with dramatic health care problems during times of natural disaster and armed conflict. Kidney Int. 2023;104:221–224. doi: 10.1016/j.kint.2023.05.003. [DOI] [PubMed] [Google Scholar]
- 14.Moukeh G., Yacoub R., Fahdi F., Rastam S., Albitar S. Epidemiology of hemodialysis patients in Aleppo city. Saudi J Kidney Dis Transplant. 2009;20:140–146. [PubMed] [Google Scholar]
- 15.Thurlow J.S., Joshi M., Yan G., et al. Global epidemiology of end-stage kidney disease and disparities in kidney replacement therapy. Am J Nephrol. 2021;52:98–107. doi: 10.1159/000514550. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Al-Makki A., Rifai A.O., Murad L., et al. The Syrian national kidney foundation: response for the need of kidney patients during the crisis. Avicenna J Med. 2014;4:54–57. doi: 10.4103/2231-0770.133331. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Koubar S.H., Hajj Nasan K., Sekkarie M.A.K. Nephrology workforce and education in conflict zones. Kidney Int Rep. 2022;7:129–132. doi: 10.1016/j.ekir.2021.11.024. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Alasfar S., Berhe E., Karam S., Luyckx V. Impact of persistent conflict and destabilizing events on dialysis care. Nat Rev Nephrol. 2023;19:688–689. doi: 10.1038/s41581-023-00759-0. [DOI] [PubMed] [Google Scholar]
- 19.Burnham G.M., Lafta R., Doocy S. Doctors leaving 12 tertiary hospitals in Iraq, 2004-2007. Soc Sci Med. 2009;69:172–177. doi: 10.1016/j.socscimed.2009.05.021. [DOI] [PubMed] [Google Scholar]
- 20.Fowler A. 1st ed. Routledge; 1997. Striking a Balance: a Guide to Enhancing the Effectiveness of Non-governmental Organisations in International Development. [DOI] [Google Scholar]
- 21.World Health Organization Everybody’s business--strengthening health systems to improve health outcomes: WHO’s framework for action. https://apps.who.int/iris/handle/10665/43918 Published 2007.
- 22.Pfeiffer J., Johnson W., Fort M., et al. Strengthening health systems in poor countries: a code of conduct for nongovernmental organizations. Am J Public Health. 2008;98:2134–2140. doi: 10.2105/AJPH.2007.125989. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.George C., Mogueo A., Okpechi I., Echouffo-Tcheugui J.B., Kengne A.P. Chronic kidney disease in low-income to middle-income countries: the case for increased screening. BMJ Glob Health. 2017;2 doi: 10.1136/bmjgh-2016-000256. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.International Society of Nephrology The ISN framework for developing dialysis programs in low-resource settings. www.theisn.orghttps://www.theisn.org/wp-content/uploads/2021/03/ISN-Framework-Dialysis-Report-HIRES.pdf Published 2021.
- 25.Bdaiwi Y., Alchalati S., Sabouni A., et al. Medical education system (re)building in a fragile setting: Northwest Syria as a case study. PLOS Glob Public Health. 2023;3 doi: 10.1371/journal.pgph.0001340. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.The Sphere Handbook: Humanitarian Charter and Minimum Standards in Humanitarian Response. 4th ed. Sphere Association; Sphere: 2018. www.spherestandards.org/handbook [Google Scholar]
- 27.The World Health Organization Health Cluster countries and regions. https://healthcluster.who.int/countries-and-regions
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.