Abstract
近年来,在没有静脉参与的情况下,拉长、扩张、重叠和扭曲甚至呈螺旋环状的动脉被定义为纯动脉畸形(pure arterial malformation,PAM)。PAM十分罕见,其病因和治疗方法尚未完全阐明。本文报告2例PAM伴动脉瘤破裂蛛网膜下腔出血患者。患者均以剧烈头痛为首发症状,CT示蛛网膜下腔出血,CT血管造影(computed tomography angiography,CTA)示动脉瘤破裂伴蛛网膜下腔出血,进一步的数字减影血管造影(digital subtraction angiography,DSA)发现PAM合并动脉瘤。鉴于出血的分布和动脉瘤的位置,动脉瘤破裂出血的可能性最大。考虑到责任动脉参与远端血供,术中仅予以动脉瘤夹闭。以往一般认为对于PAM保守治疗是安全的。此2例患者的情况与所谓的“良性自然史”说法不相符。PAM可进展形成动脉瘤,并可能进一步发展为动脉瘤破裂出血,因此对PAM患者的长期随访是相当重要的。PAM伴动脉瘤形成的患者的手术指征有待进一步明确。对PAM伴动脉瘤破裂出血患者的处理同动脉瘤破裂出血患者,但是否同时处理单纯动脉畸形团仍有待对该疾病的进一步多中心、随机对照研究加以阐明。
Keywords: 纯动脉畸形, 动脉瘤, 蛛网膜下腔出血
Abstract
In recent years, in the absence of venous component, dilated, overlapping, and tortuous arteries forming a mass of arterial loops with a coil-like appearance have been defined as pure arterial malformation (PAM). It is extremely rare, and its etiology and treatment have not yet been fully elucidated. Here, we reported 2 cases of PAM with associated aneurysmal subarachnoid hemorrhage in this paper. Both patients had severe headache as the first symptom. Subarachnoid hemorrhage was found by CT and computed tomography angiography (CTA) and PAM with associated aneurysm was found by digital subtraction angiography (DSA). In view of the distribution of blood and the location of aneurysms, the aneurysm rupture was the most likely to be considered. Based on the involvement of the lesion in the distal blood supply, only the aneurysm was clamped during the operation. It used to be consider that PAM is safety, because of the presentation and natural history of previously reported cases. Through the cases we reported, we have doubted about “the benign natural history” and discussed its treatment. PAM can promote the formation of aneurysms and should be reviewed regularly. The surgical indications for PAM patients with aneurysm formation need to be further clarified. Management of PAM patients with ruptured aneurysm is the same as that of ruptured aneurysm. Whether there are indications needed to treat simple arterial malformations remains to be further elucidated with the multicenter, randomized controlled studies on this disease.
Keywords: pure arterial malformation, aneurysm, subarachnoid hemorrhage
近年来,在没有静脉引流的情况下,单纯拉长、扩张、重叠或扭曲的动脉被定义为纯动脉畸形(pure arterial malformation,PAM)[1]。PAM十分罕见,PAM伴动脉瘤形成则更少见。PAM的病因目前并未阐明,主要倾向于认为是先天因素导致PAM。对PAM是否应该采用手术治疗仍然存在争议。既往研究[2]认为保守治疗对于PAM是安全的,但最近一些研究在对PAM患者随访中观察到动脉瘤的形成及生长[3-4]。现报告中南大学湘雅医院(以下简称我院)神经外科收治的2例以广泛蛛网膜下腔出血导致剧烈头痛起病,且术中确诊为PAM动脉瘤破裂的病例。
1. 病例资料
患者1,男,51岁,2018年12月14日中午在家修理机械时突发剧烈头痛,休息后未见明显缓解。发作时患者神志清楚,无其他症状及神经功能障碍;发病前无明显特异性症状。患者头部CT示基底池及两侧大脑外侧裂有弥漫性蛛网膜下腔出血;CT血管造影(computed tomography angiography,CTA)示颅内动脉瘤,但动脉瘤形态及动脉瘤与载瘤动脉关系欠清,进一步完善数字减影血管造影(digital subtraction angiography,DSA)。DSA示:小脑后下动脉扩张、迂曲、缠绕,于反折处见一动脉瘤(图1)。患者因要求手术治疗而转入我院,入院后急诊行开颅探查+颅内动脉瘤夹闭术。通过枕下正中右拐入路,沿右侧椎动脉入颅段,探查见右侧小脑后下动脉于距离起始部不远处分叉形成两支,相互缠绕。一支远端动脉拉长,迂曲成环,另一支相互缠绕,近端形成囊状动脉瘤,指向下内方,大小约4 mm×3 mm×3 mm。分离周围粘连,用1枚动脉瘤夹完整夹闭瘤颈,于小脑后下动脉远端、脑干前方探查见2个串珠样小动脉瘤(图2),用1枚动脉瘤夹夹闭,探查小脑后下动脉通畅。考虑到责任动脉参与小脑供血,术中未对PAM进行处理。术后3个月复查CTA,未见动脉瘤显影。8个月后复查DSA,结果显示:小脑后下动脉重叠、迂曲、缠绕及环状回路同术前,动脉瘤夹闭完全(图3)。术后随访9个月,患者恢复良好,未见新发神经功能缺损。
图1.
患者1 术前影像资料
Figure 1 Preoperative images of case 1
A, B: Preoperative CT axial scan shows extensive subarachnoid hemorrhage. C: Preoperative CTA image. D, E, F: Preoperative DSA three-dimensional reconstruction image. Aneurysm is located in the middle of the malformative artery. Posterior inferior cerebellar artery is tortuous and intertwined, forming spiral coiled structure.
图2.
患者1 术中所见
Figure 2 Intraoperative findings in case 1
A: An aneurysm is exposed on the lateral part of the medulla oblongata. B: At the distal end of the artery, two beaded aneurysms are found at anterior reflexes in front of medulla oblongata, one of which has a breach. C: Blood flow is unobstructed after clipped the 2 aneurysms. D: Indocyanine green angiographyshows that the blood flow of posterior inferior cerebellar artery is unobstructed.
图3.
患者1 术后复查
Figure 3 Postoperative images of case 1
A: CTA; B, C: DSA. The feeding artery preserves well, and the tortuous, winding, and lengthy trace still exists.
患者2,男,49岁,2019年5月20日晚饭后休息时突发剧烈头痛伴视物模糊。患者发病前无明显特异性症状。患者头部CT示蛛网膜下腔出血;完善CTA检查时发现动脉瘤,且载瘤动脉形态异常。进一步行DSA,结果显示:右侧椎动脉入颅后发出第一支动脉,迂曲于颈髓前方向下走行至颈1~2椎体交界处向上反折,于反折处见一动脉瘤,大小约 3 mm×3 mm×3 mm(图4)。患者因要求手术治疗而转入我院,入院后急诊行开颅探查+颅内动脉瘤夹闭术。取枕部向右“7”字形切口开颅,术中见右侧椎动脉入颅后发出第一支动脉,迂曲于颈髓前方向下走行至颈1~2椎体交界处向上反折,于反折处见一动脉瘤,大小约3 mm×3 mm×3 mm,周围有陈旧性出血及假性包裹(图5)。分离显露瘤颈后用1枚迷你动脉瘤夹夹闭并切下瘤体送病理检查。未见迂曲动脉向上反折后形成明显的畸形血管团及引流静脉。考虑为PAM,且相关血管可能参与其他组织血供,故不予处理。术后次日复查CTA,未见动脉瘤显影。3个月后复查DSA,结果显示:动脉瘤夹闭完好,载瘤动脉通畅,单纯动脉畸形团同术前(图6)。共随访3个月,患者恢复可,未见新发神经功能缺损。
图4.
患者2 术前影像资料
Figure 4 Preoperative images of case 2
A, B: CT scan after the onset shows extensive subarachnoid hemorrhage and intraventricular hematocele. C: Three-dimensional image reconstructed by CTA shows a “gourd” in the reflexes of artery. D, E, F: Three-dimensional DSA images show that the aneurysm is located in the middle of the malformed artery. The responsible artery is tortuous and intertwined, forming spiral coiled structure.
图5.
患者2 术中所见
Figure 5 Intraoperative findings in case 2
A: Aneurysm at the reflexes of the malformed arteries; B: Shape of aneurysm with some pseudocomponents; C: Internal shape of aneurysm; D: Completely clipped aneurysm.
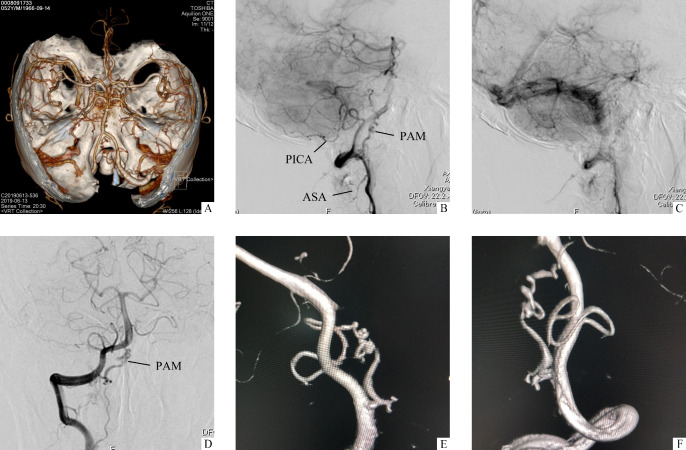
图6.
患者2 术后复查
Figure 6 Postoperative images of case 2
A: CTA; B, C, D: DSA shows that there is no obvious change in simple artery malformation. Aneurysm is completely clipped. The diseased artery is dysplastic vessel, located above the anterior spinal artery aneurysm and below the posterior inferior cerebellar artery, without obvious drainage vein. E, F: Three-dimensional DSA images show that aneurysm is completely clipped, the blood flow of the parent artery is unobstructed after operation, and the simple artery malformation is the same as that before operation. PAM: Pure arterial malformation; PICA: Posterior inferior cerebellar artery; ASA: Anterior spinal artery.
2. 讨 论
PAM极易与动静脉畸形或动静脉瘘相混淆。动静脉畸形和动静脉瘘均为动脉和静脉之间的异常连接导致脑血流动力学异常[5-6]。由于本文报告的2例患者影像学检查并未发现病灶有静脉成分参与,且通过手术得到进一步证实,因此本研究的2例患者并非后颅窝及髓周动静脉畸形或动静脉瘘。此外,本研究中的2病例与扩张性动脉病(多裂畸形)也不同。扩张性动脉病以动脉明显伸长、变宽和弯曲为主要特征,在颅内首先累及椎动脉和基底动脉[7]。而在此次报告的病例中,病变血管重叠、扩张、扭曲合并动脉瘤生成,累及的血管是冗长多余的,呈螺旋或线圈状卷曲成环。
2017年Brinjikji等[2]报道的12例PAM患者中无1例出现颅内出血或脑梗死,除1例头痛明显患者接受手术治疗,其他患者均选择保守治疗,部分患者在长达30年的随访中病变无明显进展。因此,人们认为PAM为良性病变,保守治疗是安全的。本文报告2例以广泛蛛网膜下腔出血导致剧烈头痛起病的PAM伴动脉瘤患者,并于术中确诊为PAM合并动脉瘤破裂出血。笔者查阅文献,未见有确诊为PAM伴动脉瘤破裂出血的报道。本文报告的病例再次扩展了人们对于PAM的认识。其实,早在2014年,Feliciano等[8]就报道1例右侧大脑中动脉动脉畸形伴基底节脑出血的病例,当时就考虑为PAM伴中小动脉瘤破裂出血。2018年12月Munich等[4]展示了1例基底动脉穿支PAM伴动脉瘤破裂患者的动脉瘤夹闭术。而2019年华中科技大学同济医院Yue等[3]对1例PAM患者连续随访3年,观察到该患者PAM病灶末端动脉瘤从无到有的动态发展过程,考虑到动脉瘤破裂风险,患者最终接受了手术治疗。
在PubMed中使用关键词“pure arterial malformation”检索文献,共获得4篇文献[1-4],这4篇文献报道了9例患者PAM中含有动脉瘤成分,其中2例疑似PAM中动脉瘤破裂出血。共有3名患者接受了手术治疗,其中1例患者接受介入手术治疗,2例患者接受开颅手术治疗。值得一提的是,Yue等[3]的手术处理并非夹闭动脉瘤瘤颈,而是直接夹闭载瘤动脉的上游,一并阻断了畸形动脉团的血供。除1例未在文中描述预后外,其余报道的病例随访期间均预后良好(表1)。
表1.
纯动脉畸形伴动脉动脉瘤患者的临床资料
Table 1 Clinical data of PAM with aneurysm
| 序号 | 作者及文献 | 年份 | 年龄/岁 | 性别 | 诊断方式 | 病灶位置 | 症状 | 影像学表现 | 治疗方式 | 随访时间 | 预后 |
|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | McLaughlin等[1] | 2013 | 8 | 女 | DSA | 左侧床突上段ICA,M1段近端 | 无 | 血管紧密缠绕、扩张,局灶性动脉瘤 | 保守治疗 | 未描述 | 未描述 |
| 2 | McLaughlin等[1] | 2013 | 24 | 女 | DSA | 左侧PCoA、P2段囊状动脉瘤 | 频繁头痛、头晕 | 血管紧密缠绕、中度扩张,局灶性囊状动脉瘤 | 保守治疗 | 30年 | 良好 |
| 3 | Feliciano等[8] | 2014 | 42 | 男 | DSA | 右侧MCA | 头痛 | M1段远端明显扩张伴动脉瘤簇,基底节出血,疑似中小动脉瘤破裂 | 保守治疗 | 12个月 | 良好 |
| 4 | Brinjikji等[2] | 2018 | 10 | 女 | DSA | 左侧ICA、PCoA、PCA | 患侧剧烈头痛 |
床突上段ICA多发假性动脉瘤,部分钙化,PCoA、PCA呈螺旋状 弯曲和扩张 |
介入治疗 | 72个月 | 良好 |
| 5 | Brinjikji等[2] | 2018 | 19 | 女 | DSA | 左侧MCA | 无 | M1段远端和豆纹动脉呈螺旋状弯曲,伴叠加的多叶动脉瘤,轻度狭窄 | 保守治疗 | 36个月 | 良好 |
| 6 | Brinjikji等[2] | 2018 | 25 | 女 | DSA | 左侧ICA床突上段、M1段 | 头痛 |
床突上段颈内动脉曲张、呈螺旋状外观,M1段 3个局灶性动脉瘤,伴 钙化 |
保守治疗 | 60个月 | 良好 |
| 7 | Brinjikji等[2] | 2018 | 35 | 女 | DSA | 左侧PCoA、PCA | 头痛 | 动脉扭曲伴局灶性动脉瘤扩张,伴钙化 | 保守治疗 | 84个月 | 良好 |
| 序号 | 作者及文献 | 年份 | 年龄/岁 | 性别 | 诊断方式 | 病灶位置 | 症状 | 影像学表现 | 治疗方式 | 随访时间 | 预后 |
|---|---|---|---|---|---|---|---|---|---|---|---|
| 8 | Munich等[4] | 2018 | 37 | 女 | 手术 | BA分支动脉瘤 | 剧烈头痛,视物模糊 |
基底尖以上血管异常缠结,疑似动脉瘤破裂 出血,伴钙化 |
开颅手术 | 1个月 | 良好 |
| 9 | Yue等[3] | 2019 | 42 | 男 | 手术 | 右A1段,病灶末端巨大的动脉瘤并伴有血栓形成 | 频繁头痛 | A1段紧密卷曲,在PAM内动脉瘤样结构 | 开颅手术 | 3个月 | 良好 |
ICA:颈内动脉;MCA:大脑中动脉;PCoA:后交通动脉;PCA:大脑后动脉;PICA:小脑后下动脉;VA:椎动脉;BA:基底动脉;A1段:大脑前动脉水平段;M1段:大脑中动脉水平段;P2段:大脑后动脉环池段。
已有证据[9]表明:血流动力学应激、血管危险因素(包括高血压、脂质积聚、动脉硬化、吸烟)等以及遗传易感性均参与动脉瘤的形成。相比于基底动脉环中常见的动脉瘤,当前一般认为血管走形对血流动力学的改变是脑动静脉畸形中动脉瘤形成的主要病理生理机制[10],PAM中动脉瘤成分与动静脉畸形中的动脉瘤可能有着相似的形成原理。在本文报告的2例患者的手术过程中可见动脉瘤位于畸形动脉的反折处。因此,PAM中畸形动脉血管迂曲、缠绕、甚至反折导致的血流动力学不稳定可能是PAM中动脉瘤形成的主要病理生理机制。
PAM有可能进展为动脉瘤形成、甚至动脉瘤破裂。对于PAM,保守治疗真的安全吗?PAM中动脉瘤成分未破裂的患者是否有手术指征,目前只能参考颅内未破裂动脉瘤的治疗原则[11]。在手术过程中,是否有必要牺牲远端血供,直接阻断PAM血供?是夹闭动脉瘤,不处理PAM;还是对PAM进行血管重建?不含动脉瘤成分的PAM在某些情况下是否也需要手术治疗?回答以上问题需研究更多的PAM合并动脉瘤病例。
综上,笔者认为PAM可进展形成动脉瘤,甚至可能发生动脉瘤破裂出血,因此对于PAM患者的长期随访是相当重要的。PAM伴动脉瘤形成患者的手术指征有待进一步明确。对PAM伴动脉瘤破裂出血患者的处理同动脉瘤破裂出血患者,但是否一并处理单纯动脉畸形团仍有待对该疾病的进一步多中心、随机对照研究来阐明。
利益冲突声明
作者声称无任何利益冲突。
原文网址
http://xbyxb.csu.edu.cn/xbwk/fileup/PDF/202102200.pdf
参考文献
- 1. McLaughlin N, Raychev R, Duckwiler G, et al. Pure arterial malformation of the posterior cerebral artery: Importance of its recognition[J].J Neurosurg, 2013, 119(3): 655-660. [DOI] [PubMed] [Google Scholar]
- 2. Brinjikji W, Cloft HJ, Flemming KD, et al. Pure arterial malformations[J].J Neurosurg, 2018, 129(1): 91-99. [DOI] [PubMed] [Google Scholar]
- 3. Yue H, Ling W, Hanmin C, et al. Progressive pure arterial malformations of the anterior cerebral artery[J].World Neurosurg, 2019, 131: e52-e64. [DOI] [PubMed] [Google Scholar]
- 4. Munich SA, Brunet MC, Starke RM, et al. Clipping of basilar perforator pure arterial malformation aneurysm: 2-dimensional operative video[J].Oper Neurosurg (Hagerstown), 2019, 17(2): E67. [DOI] [PubMed] [Google Scholar]
- 5. Lawton MT, Rutledge WC, Kim H, et al. Brain arteriovenous malformations[J].Nat Rev Dis Primers, 2015, 1: 15008. [DOI] [PubMed] [Google Scholar]
- 6. Reynolds MR, Lanzino G, Zipfel GJ. Intracranial dural arteriovenous fistulae[J].Stroke, 2017, 48(5): 1424-1431. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7. Lou M, Caplan LR. Vertebrobasilar dilatative arteriopathy (dolichoectasia)[J].Ann NY Acad Sci, 2010, 1184: 121-133. [DOI] [PubMed] [Google Scholar]
- 8. Feliciano CE, Pamias-Portalatin E, Mendoza-Torres J, et al. Color-coded digital subtraction angiography in the management of a rare case of middle cerebral artery pure arterial malformation a technical and case report[J].Interv Neuroradiol, 2014, 20(6): 715-721. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9. Etminan N, Rinkel GJ. Unruptured intracranial aneurysms: Development, rupture and preventive management[J].Nat Rev Neurol, 2017, 13(2): 126. [DOI] [PubMed] [Google Scholar]
- 10. Shakur SF, Amin-Hanjani S, Mostafa H, et al. Hemodynamic characteristics of cerebral arteriovenous malformation feeder vessels with and without aneurysms[J].Stroke, 2015, 46(7): 1997-1999. [DOI] [PubMed] [Google Scholar]
- 11. Thompson BG, Brown RD, Amin-Hanjani S, et al. Guidelines for the management of patients with unruptured intracranial aneurysms: A guideline for healthcare professionals from the american heart association/american stroke association[J].Stroke, 2015, 46(8): 2368-2400. [DOI] [PubMed] [Google Scholar]