Abstract
目的
宫腔粘连是一种严重影响女性生育力的疾病,多继发于妊娠相关的清宫术或宫腔镜手术等宫腔内操作,因损伤子宫内膜基底层所致。宫腔镜宫腔粘连分离术是宫腔粘连治疗环节中最关键的一步,其最常见的并发症是子宫穿孔。一半以上的子宫穿孔发生在镜体或者探针/扩宫棒通过宫颈内口阶段。在这一阶段,不恰当的手术操作还可导致内膜损伤、粘连复发加重、宫颈裂伤及假道形成等手术并发症的发生。本研究旨在提出一种宫腔镜直视下通过镜体侧入后摆动或者镜下器械直接撑开来扩张宫颈内口及宫腔下段的方法,我们称之为镜下扩宫法,以提高宫颈内口和/或宫腔下段粘连患者扩宫的有效性及安全性。
方法
收集中南大学湘雅三医院2020年1月至2021年6月行宫腔镜宫腔粘连分离术的282例患者,年龄21~46(33.0±4.8)岁,根据美国生育协会(American Fertility Society,AFS)的宫腔粘连评分标准评为5~12分,其中有2例因外院传统扩宫分离粘连所致假道形成的患者。所有患者使用具有5Fr 器械通道、4.9 mm 外鞘直径的一体式宫腔镜行宫腔镜检查。采用镜下扩宫法扩张宫颈内口及宫腔下段。宫腔镜进入宫腔后,常规行宫腔粘连分离术及向宫腔内放置宫型节育环或者宫腔支架等。收集所有纳入病例的年龄、手术记录及手术视频资料,并统计其术中镜下扩宫的成功率和手术并发症发生率。
结果
所有患者均成功利用镜下扩宫法将宫腔镜置入宫腔,2例因外院扩宫导致假道形成的患者也在镜下扩宫的过程中及时识别并成功找到宫腔。无 1例在术中因宫颈内口和宫腔下段扩张失败而中转使用传统宫颈扩张棒扩宫。整个宫腔镜手术过程中,手术视野清晰,且无假道形成、子宫穿孔或宫颈撕裂等并发症的发生。术后1至3个月复查宫腔镜,所有患者均未见宫颈内口及宫腔下段明显的粘连狭窄。
结论
镜下扩宫法是在宫腔镜直视下对粘连的宫颈内口及宫腔进行“即诊即治”模式的解剖层次分离的方法。该方法在超声引导下,通过宫腔镜直视判断解剖层次,可降低解剖层次判断错误的概率;经验丰富的宫腔镜医师能及时发现既往手术所致的陈旧性假道并避免再次进入;通过镜下分离宫颈内口及宫腔下段粘连,避免强行插入宫腔镜体而损伤内膜,可有效降低假道形成、宫颈裂伤、子宫穿孔等手术并发症的发生;采用微型宫腔镜无需术前宫颈准备,可避免相关风险和不良影响,使得术前宫颈准备扩宫效果不佳的宫颈内口及宫腔下段粘连的患者得以有效扩宫,患者接受度高。镜下扩宫法对于宫腔镜技术娴熟的术者而言操作简单,值得临床推广。
Keywords: 宫腔粘连, 宫腔镜技术, 扩宫, 手术并发症, 不孕
Abstract
Objective
Intrauterine adhesion (IUA) is mainly caused by intrauterine operations such as pregnancy-related curettage and hysteroscopic surgery, resulting in the trauma to the basal layer of the endometrium. Hysteroscopic adhesiolysis is a crucial step in the comprehensive treatment of IUA, and the most common complication is uterine perforation. More than half of all uterine perforations occur during the hysteroscopy or probe/dilator pass through the internal os. Furthermore, inappropriate surgical procedures may lead to endometrial injury, recurrence or even aggravation of adhesions, and complications such as cervix laceration and false passage formation. This study aims to explore the usage of the hysteroscopic dilatation techniques to dilate the internal os and lower uterine segment, which is via hysteroscopy entering the internal os laterally and swinging, or by directly opening the forceps or scissors and bluntly spreading dissection under direct hysteroscopic vision. By using the hysteroscopic dilatation techniques, we intend to improve the effectiveness and safety of cervical dilation in patients with IUA in the internal os and/or lower uterine segment.
Methods
A total of 282 patients with adhesions in the internal os or lower uterine segment underwent HA in the Third Xiangya Hospital of Central South University from January 2020 to June 2021 were included, ranging from 21 to 46 (33.0±4.8) years old in age and 5 to 12 in the American Fertility Society score. Among them, there were 2 cases of false passage formation caused by traditional dilatation in other hospitals. All patients underwent hysteroscopy with integrated hysteroscopy with 5Fr instrument channel and 4.9 mm outer sheath diameter. The internal orifice of cervix and the lower segment of uterine cavity were dilated under the microscope. After the hysteroscopy entered the uterine cavity, the separation of uterine cavity adhesion and the placement of uterine contraceptive ring or uterine stent into the uterine cavity were performed routinely. Age, surgical records, and surgical videos of all included cases were collected. The success rate of dilation and the incidence of surgical complications were assessed.
Results
In all cases, the hysteroscopys successfully entered into the uterine cavity by using the hysteroscopic dilatation techniques without failure and switching to cervical dilators. In the 2 cases of false passage due to previous cervical dilation, the uterine cavity was identified and found successfully under direct hysteroscopic vision. During the whole surgery, the vision was clear, and no complications (such as cervix laceration, false passage formation, uterine perforation or water intoxication) occurred. One to 3 months postoperative hysteroscopy revealed no significant fibrotic stenosis in the internal os and lower uterine segment.
Conclusion
The hysteroscopic dilation techniques are a strategy for separation methods that is following structural hierarchy anatomy in the mode of “see and treat” for the adhesion in the internal os and uterine cavity under direct hysteroscopic vision. This method not only has ultrasound guidance, but also has the judgment of structural hierarchy anatomy under direct hysteroscopic vision, so there is less chance of anatomical level judgment error. This method makes full use of the hysteroscopic judgement of the experienced hysteroscopic surgeons, so that surgeons can timely find and avoid re-entering the old false passage caused by previous surgery. The adhesions in the internal os and lower uterine segment were separated by the hysteroscopic dilation techniques. In this way, the damage to the endometrium caused by forced insertion of the hysteroscopy can be avoided. Meticulous separation of adhesions and cervical dilation under direct hysteroscopic vision can effectively reduce the occurrence of surgical complications such as false passage formation, cervical laceration, and uterine perforation. The use of mini-hysteroscopy eliminates the need for preoperative cervical preparation, avoiding associated risks and side effects. Moreover, for patients with adhesions in the internal os and lower uterine segment, preoperative cervical preparation is not effective in cervical dilation, while the hysteroscopic dilation techniques are effective, with higher patient acceptance due to the absence of preoperative cervical preparation. For the skilled hysteroscopic surgeons, the hysteroscopic dilation technique is easy to operate and worthy of clinical application.
Keywords: intrauterine adhesions, hysteroscopic technique, cervical dilation, surgical complication, infertility
宫腔粘连是一种严重损伤女性生育能力的疾病,多由妊娠相关的清宫术[1]和宫腔镜手术[2]等宫腔内操作损伤子宫内膜基底层所致。子宫内膜在修复损伤过程中易形成粘连及疤痕组织,使宫腔异常。临床症状主要表现为月经量减少、闭经、复发性流产、不孕症、胎盘发育异常、胎盘粘连或植入等[3]。宫腔镜手术能在直视下分离粘连,重建患者宫腔形态,是宫腔粘连最有效的治疗方式。
宫腔镜下宫腔粘连分离术的手术难度与粘连的部位和严重程度密切相关。对于存在宫颈内口及宫腔下段粘连的患者,其手术难度主要在于如何将宫腔镜镜体通过明显狭窄甚至封闭的宫颈内口及宫腔下段,进而顺利进入宫腔中段和上段。若将镜体强行通过,不仅损伤宫颈内口黏膜及宫腔下段残存内膜,增加术后粘连复发的风险,而且可能导致宫颈裂伤、子宫肌层内假道形成,甚至发生子宫穿孔等医源性并发症。研究[4]表明子宫穿孔是宫腔粘连分离术中最常见的并发症,且一半以上发生在镜体或者探针/扩宫棒通过宫颈内口阶段。
目前临床上常在术前使用米索前列醇软化宫颈,或用宫颈扩张器扩张宫颈以降低镜体通过宫颈内口的阻力[5]。但米索前列醇的给药时机、剂量及途径尚不统一,使得宫颈软化效果不满意[6-7];金属扩宫棒易导致患者术中术后出现酸胀疼痛等不适,术者不易掌握扩宫力度和扩宫方向,容易出现宫颈裂伤、子宫穿孔及假道形成等并发症;亲水性扩张器则因材质有一定脆性,可能发生断裂而部分滞留宫腔[8]。以上宫颈准备对于由严重粘连导致的宫颈内口或宫腔下段狭窄扩张效果欠佳,更主要的是容易导致患者子宫内膜充血和出血,影响宫腔镜手术视野,进而延长手术时间和增加水中毒发生风险,此外,还存在发生恶心、呕吐等胃肠道不良反应和上行性感染等风险。另一个传统的方法是在超声引导下用探针或者扩宫棒探查和扩张宫颈内口和下段,但对于宫腔粘连内膜严重受损者,超声显示宫腔线往往困难,因而引起子宫穿孔或者不全穿孔的风险很大。
针对这一难题,本研究提出镜下扩宫法,即在宫腔镜直视下通过镜体侧入后摆动或撑开器械的方式扩张宫颈内口及宫腔下段,并对其有效性及安全性进行评估,以期提供一种安全有效的扩宫方法来替代传统的超声引导下的盲扩宫法。
1. 资料与方法
1.1. 一般资料
收集中南大学湘雅三医院(以下简称我院)2020年1月至2021年6月行宫腔镜宫腔粘连分离术的282例患者,年龄21~46(33.0±4.8)岁,根据美国生育协会(American Fertility Society,AFS)宫腔粘连评分标准评为5~12分,其中有2例因外院传统扩宫分离粘连所致假道形成的患者。所有患者均在宫腔镜手术前自愿签署手术知情同意书。本研究已获得中南大学湘雅三医院伦理委员会的批准(审批号:快I 22020)。
纳入标准:1)宫颈内口和/或宫腔下段粘连;2)术前未使用米索前列醇软化宫颈且未使用扩宫棒扩张宫颈;3)采用镜下扩宫法扩张宫颈内口及宫腔下段。排除标准:1)宫腔镜手术视频及病历资料不全者;2)未遵医嘱至我院完成宫腔镜复查者。
1.2. 手术方式及术后处理
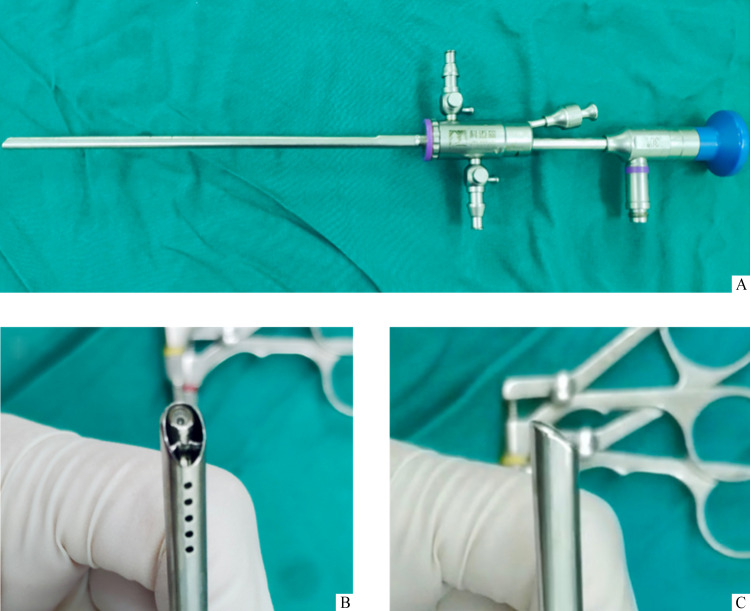
患者取膀胱截石位,常规消毒铺巾,静脉麻醉实施完毕后,双合诊明确子宫方位。然后使用具有5Fr器械通道、4.9 mm外鞘直径的一体式宫腔镜(图1)行宫腔镜检查。当镜体至近宫颈内口见宫颈内口及宫腔下段因粘连明显狭窄或者近乎封闭时,采用下述镜下扩宫法扩张宫颈内口及宫腔下段。
图1.
一体式宫腔镜
Figure 1 Integrated hysteroscopy
A: Integrated hysteroscopy with a 4.9 mm diameter outer sheath and a 5Fr working channel; B: Front view of the anterior-oriented hysteroscopy bevel; C: Lateral view of the anterior-oriented hysteroscopy bevel.
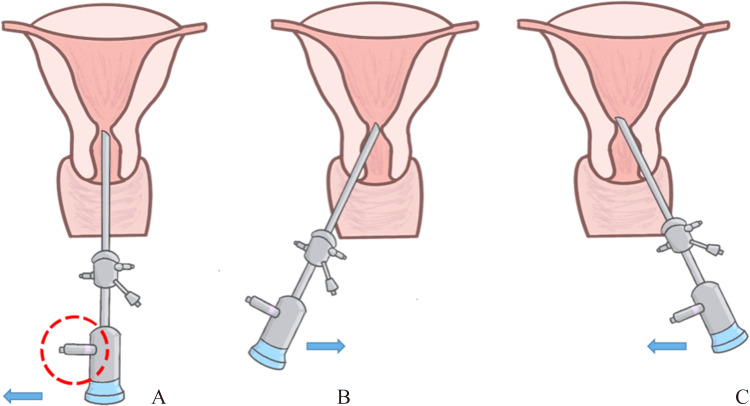
1)摆动法:调整宫腔镜光缆至患者右侧水平位,此时宫腔镜镜体前端的斜面朝向患者宫颈内口左侧壁(图2A),镜体向左上方且镜体头端斜面向左侧壁推进2~3 mm(图2B),使镜头尖端进入狭窄的粘连内的腔隙,随后将镜体头端摆向患者右侧(图2C),利用摆动向右侧钝性推开粘连。重复以上操作,直至达到钝性分离粘连,扩张宫颈内口及宫腔下段的目的。注意在摆动镜体的过程中需保持宫腔镜光缆水平方向且原位摆动镜头,否则容易使镜头铲起宫颈内口和宫腔下段的内膜。
图2.
摆动法示意图
Figure 2 Diagram of the horizontal swinging separation technique
A: Put the light post at the right horizontal position and the anterior-oriented hysteroscopy bevel faces the left cervical wall. B: Hysteroscope body is to the upper left and the hysteroscopy bevel is pushed to the left side wall to enter 2-3 mm. C: Swing the hysteroscopy head to the right of the patient, and use the swing to bluntly push the adhesion to the right. Red dotted circle indicates the light post, and the blue arrows indicate the direction to move the hysteroscopy.
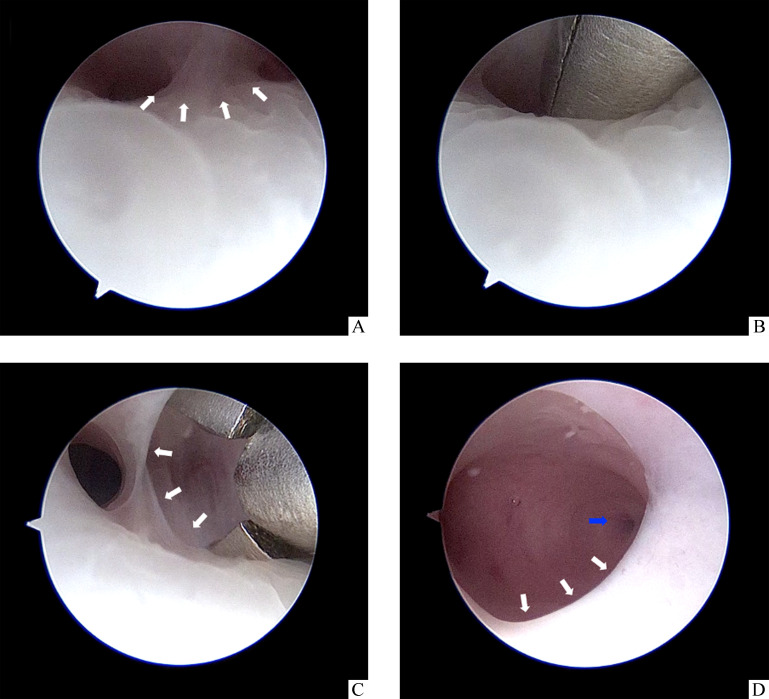
2)撑开法:在宫腔镜直视下将5Fr双关节勺型钳或单关节剪刀反复向子宫前后壁方向张开(图3A~3C),也可辅以向左右方向张开,以钝性分离宫颈内口及宫腔下段处的纤维性粘连。注意撑开的部位应尽量靠近肌壁以达到充分的扩宫效果。5Fr双关节勺型钳或单关节剪前端张开最大直径均可达到8 mm,经充分扩张后,外鞘直径为4.9 mm的宫腔镜镜体可顺利通过。
图3.
5Fr双关节勺型钳分离粘连
Figure 3 Blunt spreading dissection with a 5Fr double-action forceps
A: Adhesions at the internal os. B: Put the 5Fr double-action forceps at the adhesions site. C: Open a 5Fr double-action forceps toward the anterior and posterior intrauterine walls. D: After separating the cervical adhesion, the adhesion is observed in the lower segment. The white arrows indicate adhesion, and the blue arrows indicate the fallopian tubal ostium.
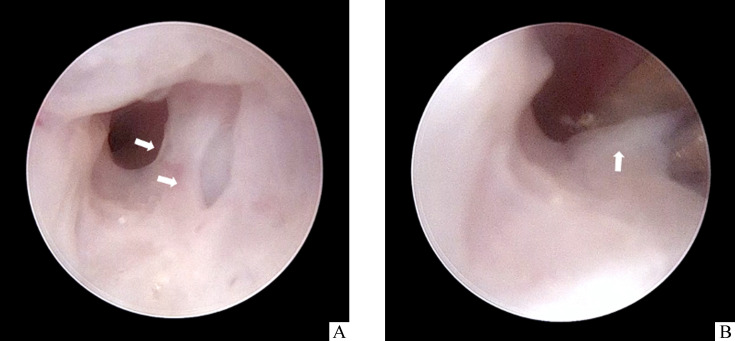
如宫颈内口处完全粘连封闭,可利用宫腔镜的放大作用,仔细辨认子宫腔前后壁之间的层次后,再沿粘连部位较薄弱处逐步撑开分离粘连部位。对于难以撑开的致密肌性粘连组织,则可采用单关节剪刀犁断粘连后再行上述撑开法(图4)。
图4.
单关节剪刀分离粘连
Figure 4 Dissection of adhesions with a single-action scissors
A: Put the single-action forceps at the adhesions site. B: Dissect the adhesion with the scissors. The white arrows indicate adhesions.
宫腔镜进入宫腔后,常规行宫腔粘连分离术及向宫腔内放置宫型节育环或者宫腔支架等。根据宫颈内口及宫腔下段狭窄程度留置宫腔气囊管1~3周[9]或者带尾部的宫腔支架(图5)。所有患者均于术后1至3个月至我院复查宫腔镜,以了解宫颈内口及宫腔下段是否再次狭窄或粘连。
图5.

带尾部的宫腔支架
Figure 5 Intrauterine stent with tail
1.3. 有效性及安全性评价
记录并评估282例患者首诊及复查的手术视频,从扩宫成功率及手术并发症的发生率两个方面评价镜下扩宫法的有效性及安全性。其中,扩宫成功率指宫腔镜术中未改用传统的超声引导下探针探宫及宫颈扩张棒扩张宫颈内口和宫腔下段,而仅使用镜下扩宫法扩张宫颈内口及宫腔下段,使得镜体顺利进入宫腔的患者比例。手术并发症发生率指术中发生宫颈裂伤、子宫肌层假道形成或子宫穿孔等并发症的患者比例。
另外,本研究还从宫腔镜手术视野清晰度、术后宫颈内口和宫腔下段再粘连两个方面评价镜下扩宫法的优劣。
2. 结 果
282例患者利用镜下扩宫法均成功将宫腔镜置入宫腔,无1例术中因扩宫失败而转为传统宫颈扩张棒扩宫,扩宫成功率100%。在整个宫腔镜手术过程中,手术视野清晰,且无假道形成、子宫穿孔或宫颈撕裂等并发症发生(视频1,http://xbyxb.csu.edu.cn/videoDetails?columnId=32333389&type=&lang=zh),手术并发症发生率为0%。术后1至3个月复查宫腔镜示宫颈及宫腔下段无明显粘连狭窄。
3. 讨 论
宫腔镜宫腔粘连分离术是宫腔粘连综合治疗方案中至关重要的环节。临床上,中重度粘连常导致宫颈内口及宫腔下段狭窄甚至完全封闭,使宫腔镜进入宫腔的难度增加。在本组病例中,有2例因宫颈管粘连狭窄,在外院行宫腔镜宫腔粘连分离术时应用传统扩宫法导致假道形成,在我院首诊时仍可见宫腔下段狭窄。
本研究所使用的镜下扩宫法是在宫腔镜直视下,通过宫腔镜镜头尖端侧入后镜体摆动的钝性力量、双关节勺型钳或单关节剪刀撑开的方式,在分离粘连的同时扩张宫颈内口及宫腔下段。使用该方法,所有病例均成功置入宫腔镜,无1例因镜下扩宫失败而中转使用宫颈扩张棒。在宫腔镜手术过程中,手术视野清晰,无假道形成、子宫穿孔或宫颈撕裂等并发症发生。术后1至3个月复查宫腔镜示宫颈及宫腔下段无明显粘连狭窄,表明该方法避免了内膜损伤、粘连狭窄复发加重以及手术并发症的形成,而这些并发症在以往对宫颈内口或宫腔下段粘连狭窄的宫腔镜宫腔粘连分离术中、术后极易出现。
其原因在于:1)本研究使用带有5Fr操作通道的微型宫腔镜,能够在直视下以镜下扩宫法进行“即诊即治”一体化(see and treat with the same hysteroscopy)操作,能及时发现并避免再次进入既往手术所致的陈旧性假道。2)摆动法是将宫腔镜前端斜面贴近宫颈壁,避免了镜头尖端在进镜过程中铲到宫颈内口及宫腔下段的内膜,减轻了宫颈及宫腔下段内膜的损伤,在一定程度上预防了此处粘连狭窄的复发。3)摆动法利用镜体外鞘为无创设计的特点,将镜头尖端置入粘连缝隙,利用镜体摆动的力量钝性分离粘连;撑开法则是利用宫腔镜的放大作用辨认子宫前后壁之间的层次,再沿粘连薄弱处钝性分离粘连,对于无法撑开的致密肌性粘连,也可结合单关节剪刀犁断粘连、松解狭窄环。二者均能在宫腔镜直视下仔细识别粘连的部位、性质及程度,并对宫颈内口和宫腔下段的粘连进行有效分离。同时因术中犁断了狭窄环,也可减少粘连狭窄的再次形成。4)应用该方法无需进行术前宫颈准备。更重要的是,当患者存在宫颈内口及宫腔下段粘连时,术前宫颈准备往往难以达到满意的扩宫效果,但镜下扩宫法可以有效扩宫,并且避免了药物相关的不良反应,适用人群更广;避免了术前侵袭性操作给患者带来的不适,患者接受度更高,花费更少,同时规避了反复多次扩宫带来的宫颈撕裂、子宫穿孔或假道形成等潜在风险;减少了因扩张导致的子宫内膜充血和/或出血,有利于手术视野的暴露,降低了手术难度,安全系数高。
综上所述,镜下扩宫法是在宫腔镜直视下进行的“即诊即治”一体化治疗,相比传统超声引导下的探宫和扩宫操作,本方法不仅有超声引导,更有宫腔镜直视下的解剖层次的判断,因此发生解剖层次判断错误的概率更小。对于经验丰富的宫腔镜医师而言,镜下扩宫法可充分利用宫腔镜医师的镜下判断经验,及时发现并避免再次进入既往手术所致的陈旧性假道;通过镜体侧入后摆动或者镜下器械直接撑开法分离宫颈内口及宫腔下段粘连,可避免强行插入宫腔镜体而造成此处内膜损伤的加重和粘连狭窄的复发;经宫腔镜直视下细致分离粘连并扩宫,有效降低了假道形成、宫颈裂伤、子宫穿孔等手术并发症的发生;无需宫颈术前准备,可避免药物相关的不良反应、术前侵袭性操作给患者带来的不适及因扩张治疗导致的子宫内膜充血和/或出血;宫颈术前准备对存在宫颈内口及宫腔下段粘连的患者,扩宫效果不佳,而镜下扩宫法则能有效扩宫,患者接受度高,且适用人群广。对于宫腔镜技术娴熟的术者来说,该方法操作简单,值得临床推广。
基金资助
湖南省临床医疗技术创新引导项目(2020SK53605);湖南省自然科学基金 (2021JJ40953)。
This work was supported by the Hunan Provincial Clinical Medical Technology Innovation Guiding Plan (2020SK53605) and the Natural Science Foundation of Hunan Province (2021JJ40953), China.
利益冲突声明
作者声称无任何利益冲突。
作者贡献
周曾梓 数据分析,论文撰写与修改;赵美丹 数据采集,论文撰写;邹凌霄 数据采集与分析;伍美容 论文指导与审阅;徐大宝 研究设计、指导及修改。全体作者阅读并同意最终的文本。
原文网址
http://xbyxb.csu.edu.cn/xbwk/fileup/PDF/2022111586.pdf
参考文献
- 1. Deans R, Abbott J. Review of intrauterine adhesions[J]. J Minim Invasive Gynecol, 2010, 17(5): 555-569. https:// 10.1016/j.jmig.2010.04.016. [DOI] [PubMed] [Google Scholar]
- 2. Hooker AB, Lemmers M, Thurkow AL, et al. Systematic review and meta-analysis of intrauterine adhesions after miscarriage: prevalence, risk factors and long-term reproductive outcome[J]. Hum Reprod Update, 2014, 20(2): 262-278. https:// 10.1093/humupd/dmt045. [DOI] [PubMed] [Google Scholar]
- 3. Dreisler E, Kjer JJ. Asherman’s syndrome: current perspectives on diagnosis and management[J]. Int J Womens Health, 2019, 11: 191-198. 10.2147/IJWH.S165474. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4. Jansen FW, Vredevoogd CB, van Ulzen K, et al. Complications of hysteroscopy: a prospective, multicenter study[J]. Obstet Gynecol, 2000, 96(2): 266-270. 10.1016/s0029-7844(00)00865-6. [DOI] [PubMed] [Google Scholar]
- 5. Wood MA, Kerrigan KL, Burns MK, et al. Overcoming the challenging cervix: identification and techniques to access the uterine cavity[J]. Obstet Gynecol Surv, 2018, 73(11): 641-649. 10.1097/OGX.0000000000000614. [DOI] [PubMed] [Google Scholar]
- 6. Zhuo ZH, Yu HM, Gao L, et al. Effectiveness of misoprostol administration for cervical ripening in women before operative hysteroscopy: a randomized, double-blinded controlled trial[J]. Minim Invasive Ther Allied Technol, 2019, 28(6): 344-350. 10.1080/13645706.2018.1559195. [DOI] [PubMed] [Google Scholar]
- 7. Fernandez H, Alby JD, Tournoux C, et al. Vaginal misoprostol for cervical ripening before operative hysteroscopy in pre-menopausal women: a double-blind, placebo-controlled trial with three dose regimens[J]. Hum Reprod, 2004, 19(7): 1618-1621. 10.1093/humrep/deh302. [DOI] [PubMed] [Google Scholar]
- 8. Nilsson W, Mikhael S, Kaplan J. Chronic pelvic pain and infertility resulting from unrecognized retained Laminaria [J]. Case Rep Obstet Gynecol, 2017, 2017: 6345712. 10.1155/2017/6345712. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9. Salma U, Xue M, Md Sayed AS, et al. Efficacy of intrauterine device in the treatment of intrauterine adhesions[J]. Biomed Res Int, 2014, 2014: 589296. 10.1155/2014/589296. [DOI] [PMC free article] [PubMed] [Google Scholar]