Abstract
目的
不孕症的发病率呈逐年上升的趋势,其中30%以上与输卵管通畅性异常相关。四维超声子宫输卵管造影(4-dimensional hysterosalpingo-contrast sonography,4D HyCoSy)在诊断输卵管通畅性上既克服了三维成像的不足,特异性和准确性均较高,又避免了碘剂过敏、X线辐射等危害,接受度好且易掌握,在临床应用越来越广泛,但是目前尚无研究探讨4D HyCoSy与自然妊娠可能性相关的影像学标准。本研究对临床拟诊输卵管性不孕患者的临床资料及4D HyCoSy的影像特点进行分析,建立一种基于影像学特征的造影术后自然妊娠的预测模型。
方法
回顾性分析湖南省光琇医院2017年2月至2018年5月拟诊为输卵管性不孕症、具有完整4D HyCoSy影像学资料且显示至少一侧输卵管通畅的患者,收集患者的一般临床资料及影像数据,并随访患者造影术后3个月内的自然妊娠情况,将其分成自然妊娠组与非自然妊娠组。采用二元logistic回归分析各个变量与造影术后自然妊娠之间的相关性,将单因素logistic回归中差异有统计学意义(P<0.05)的变量纳入自然妊娠概率预测模型,并通过10倍交叉法验证预测模型的分类能力。
结果
收集到符合要求且遵医嘱试孕3个月的1 085名临床拟诊输卵管性不孕患者,其临床特征(年龄、不孕年限)及4D HyCoSy影像学特征(月经结束后3~7 d的内膜厚度、左侧输卵管显影情况、左侧卵巢周围造影剂弥散情况、右侧卵巢周围造影剂弥散情况)是术后3个月自然妊娠的独立预测因素。建立自然妊娠概率预测模型,10倍交叉法验证得出的曲线下面积(area under the curve,AUC)均大于0.75,最佳AUC为0.868。预测模型得出的Q值为自然妊娠概率,截断值是0.5,当Q值大于0.5时建议试孕3个月,小于0.5时建议采用辅助生殖技术助孕。
结论
基于输卵管性不孕患者的临床及4D HyCoSy的影像学特征成功建立了输卵管性不孕症女性造影术后自然妊娠的预测模型,此模型可有效辅助临床进行个体化决策。
Keywords: 四维超声子宫输卵管造影, 不孕症, 输卵管通畅性, 自然妊娠, 预测模型
Abstract
Objective
The incidence of infertility is increasing, more than 30% of them having related abnormal tubal patency. Four-dimensional (4D) hysterosalpingo-contrast sonography (HyCoSy) overcomes the shortcomings of 3D HyCoSy in the diagnosis of tubal patency, showing high specificity and accuracy. In addition, 4D HyCoSy discards iodine allergy and X-ray radiation and possesses easy-operating, contributing to good acceptance in clinical practice. However, there is no research to explore the imaging standards related to the possibility of natural pregnancy after 4D HyCoSy. If a predictive model of postoperative natural pregnancy was established using the analysis of clinical data combined with imaging characteristics of 4D HyCoSy of patients with tubal factor infertility, clinical decision-making can be wisely guided in the future. This study aims to establish a predictive model of natural pregnancy after 4D HyCoSy based on clinical data and imaging characteristics of patients with tubal factor in fertility.
Methods
A retrospective study was conducted for patients who were diagnosed with tubal factor infertility in Hunan Guangxiu Hospital from February 2017 to May 2018. The patients ought to possess complete 4D HyCoSy imaging data and at least one-side-unobstructed fallopian tube. General clinical data and imaging data were collected. Pregnancy outcome was followed up till 3 months after 4D HyCoSy. According to pregnancy outcome, patients were divided into a pregnancy group and a non‐pregnancy group. Binary logistic regression was used to analyze the correlation between various variables and natural pregnancy after 4D HyCoSy. The variables with significant difference (P<0.05) in single-factor logistic regression were included in the natural pregnancy probability prediction model. The classification accuracy was further verified with 10-fold cross-validation.
Results
A total of 1 085 patients with clinically suspected tubal factor infertility who met the requirements and followed the doctors’ prescription were collected. Clinical characteristics (age and duration of infertility) and 4D HyCoSy imaging characteristics (thickness of endometrium from the 3rd to the 7th day after the end of menstruation, visualization of the left fallopian tube, the diffusion of contrast agent around the left ovary, and the diffusion of contrast agent around the right ovary) were independent predictors for natural pregnancy 3 months after 4D HyCoSy. A natural pregnancy probability prediction model was established with the area under the curve (AUC) verified by the 10-fold cross-validation all greater than 0.75, and the best AUC was 0.868. The Q value obtained by the prediction model was the probability of natural pregnancy, and the cutoff value was 0.5. When the Q value was greater than 0.5, it was recommended to attempt natural pregnancy for 3 months, and when the Q value was less than 0.5, in vitro fertilization was adviced.
Conclusion
A predictive model for the evaluating probability of natural pregnancy in women with tubal factor infertility after 4D HyCoSy is successfully established based on the analysis for clinical data and imaging characteristics. This model shows a great potential in assisting clinical decision making.
Keywords: four-dimensional hysterosalpingo-contrast sonography, infertility, tubal patency, natural pregnancy, predictive model
不孕症是指夫妻有正常性生活,未避孕1年仍未孕的情况[1]。近年来,不孕症的发病率呈逐年上升的趋势。输卵管疾病是导致女性不孕的首要病因,占女性不孕的25%~40%[2-3]。目前临床上常用的了解输卵管通畅性的方法较多,但是有其局限性,比如:子宫输卵管通液术不够准确,子宫输卵管碘油造影有X线辐射危害,碘油在输卵管和盆腔难以被吸收患者可能对碘剂过敏,腹腔镜下输卵管美蓝通液术(包括联合宫腔镜输卵管插管术)相对创伤大、费用高、需要全身麻醉等[4-6]。
随着超声造影技术的迅速发展,经阴道子宫输卵管超声造影(hysterosalpingo-contrast sonography,HyCoSy)具有无创、操作简便、无辐射、费用低和可满足多切面及多角度观察等优点,其在宫腔疾病和输卵管通畅性等方面的诊断价值已获得广泛认可[7]。经阴道HyCoSy主要是通过导管将超声微泡造影剂注入宫腔内并进入输卵管和盆腔,在微泡造影剂的帮助下,使宫腔的形态与输卵管的走形立体直观地显现,并通过卵巢周围有无造影剂包绕和盆腔造影剂弥散情况,判定输卵管是否通畅,观察子宫畸形、宫腔疾病、卵巢及盆腔粘连等情况[8]。近年来随着超声技术的发展,成像模式也不断更新,从二维(2-dimensional,2D)平面成像到三维(3-dimensional,3D)立体成像,再到实时3D动态(即四维超声输卵管造影,4D HyCoSy)。目前临床多应用2D HyCoSy及3D HyCoSy技术评价输卵管通畅性,但是2D HyCoSy不能在同一平面同时显示两条输卵管,且3D HyCoSy成像是静态图像,对于子宫肌层静脉逆流明显的患者很难从图像中辨别输卵管的形态。4D HyCoSy是实时3D图像,可以实时显示造影剂自导管进入宫腔至输卵管显影的全过程,显像清晰真实、动态直观,存储图像可进行多平面、多角度后处理,避免宫旁及肌层逆流干扰。
研究[5, 9-10]证实4D HyCoSy在诊断输卵管通畅性上既克服了3D成像的不足,特异性和准确性均较高,又避免了碘剂致敏、X线辐射等危害,经济且易掌握,在临床应用越来越广泛。但是临床上缺乏一个预测造影术后(非双侧输卵管均不通者)是否可以自然妊娠的标准,本研究拟建立一种基于4D HyCoSy影像学特征的造影术后自然妊娠的预测模型,为每个患者预测术后自然妊娠的概率和为临床医师制订个体化的诊疗方案提供依据。
1. 对象与方法
1.1. 对象
回顾性分析2017年2月22日至2018年5月31日于湖南省光琇医院妇产科拟诊为输卵管性不孕症,行4D HyCoSy且拥有完整影像学资料的1 433例患者。纳入标准:年龄在20~45岁,有正常性生活,未避孕,1年内未怀孕者,男方精液检查正常;高度怀疑输卵管性不孕;月经正常,且体温在37.5 ℃以下,黄体功能检测连续3个月显示功能良好;生殖医生建议可试孕并进行试孕至少3个月。排除标准:患者存在超声造影禁忌证,如妊娠及可疑妊娠、生殖道恶性肿瘤、生殖道感染及急性盆腔炎;患者合并其他可能导致不孕的因素,如生殖道先天发育异常、排卵障碍、子宫内膜异位症、子宫肌瘤、宫腔粘连、染色体异常、内分泌及免疫性因素等;合并有一侧或双侧输卵管切除病史;合并严重药物过敏、全身严重疾病及精神病史。
1.2. 检查方法
采用美国GE公司多功能彩色多普勒超声诊断仪(型号Voluson E8),探头频率:5.0~7.5 MHz。造影剂选用1%人血白蛋白包裹全氟丙烷的白蛋白微球。患者于月经结束后3~7 d行4D HyCoSy,且3 d内无性生活,检查时排空膀胱,采用截石位常规消毒铺巾,宫腔放置12Fr Foley管,气囊内注入生理盐水1.5~2.0 mL,调整气囊位置堵塞宫颈内口。采用常规腔内超声(transvaginal ultrasonography,TVS)检查观察子宫和卵巢的位置、内部回声、移动度,有无子宫直肠陷窝积液、盆腔粘连带、钙化灶等。将超声仪处于Contrast造影状态,开启4D扫描模式,取造影剂 20 mL,通过造影管推入宫腔内,实时追踪观察双侧输卵管近端、中段、远伞端,清晰显示宫腔和输卵管各段在盆腔内的走形,动态观察其与卵巢的关系、造影剂在卵巢周边的流动和溢出情况。推注造影剂的同时保存动态图像,4D成像后再利用3D成像对4D下不满意部分或重点部分进行补充观察与成像。若宫腔、盆腔存在病变,取注射用生理盐水10~20 mL,通过造影管向宫腔内缓慢推入,使宫腔充盈,行TVS检查,查看宫腔有无占位性病变、粘连,观察输卵管走形,伞端造影剂溢出情况,卵巢周围、肠管间造影剂弥散及肌层有无逆流。术后利用MagicCUT对图像进行修剪,留下清晰的宫腔及输卵管图像存储于仪器内,并利用动态图像进行分析,判断输卵管通畅程度。随访造影术后3个月自然妊娠情况。
1.3. 评价变量
评价变量包括月经结束后3~7 d的内膜厚度、卵巢与子宫位置关系、卵巢活动度、水囊量、水囊长径;宫腔显影形态;输卵管显影情况、输卵管管壁是否光整;输卵管走形/形态;输卵管伞端造影剂溢出情况;卵巢周围造影剂弥散、盆腔造影剂弥散、子宫肌层内造影剂渗入情况;造影剂推注阻力、阴道反流、造影管反流情况。
1.4. 统计学处理
采用SAS 9.4软件对所有研究变量进行统计学描述,连续变量以均数±标准差( ±s)描述,分类变量以各类别发生例数和百分比及缺失数描述。对基线变量与妊娠结局进行相关性分析。连续变量采用t检验,分类变量采用χ2检验;逐步回归采用向前向后法。模型预测表采用多因素logistic 回归,纳入模型的变量均为单因素分析中差异有统计学意义的变量。通过10倍交叉验证(10-fold cross-validation)法和受试者特征曲线的曲线下面积(area under the curve,AUC)来确定模型的分类能力,得出预测模型Q值,即自然妊娠概率。P<0.05为差异有统计学意义。
2. 结 果
2.1. 一般情况
在1 433例不孕症患者中,14例临床资料不全,246例失访,73例不符合纳入标准,15例患者4D HyCoSy显示双侧均不通,术后建议试管婴儿。最终纳入1 085例。术后3个月自然妊娠者301例(27.74%),未孕者784例。
2.2. 4D HyCoSy术后3个月自然妊娠的单因素分析
依据妊娠结局将纳入患者分为自然妊娠与非自然妊娠组,2组年龄(P<0.001),未避孕未孕时长(P<0.001),月经结束后3~7 d的内膜厚度(P=0.001),卵巢活动度(P<0.001),输卵管显影情况(P<0.01),输卵管管壁是否光整(P<0.05),输卵管走形/形态(P<0.01),输卵管伞端造影剂溢出情况(P<0.001),卵巢周围造影剂弥散情况(P<0.001),造影剂推注阻力情况(P<0.01)及造影剂反流情况差异均有统计学意义。其余变量差异均无统计学意义(均P>0.05,附表1,https://doi.org/10.11817/j.issn.1672-7347.2022.220179T1)。
表1.
多元logistic回归分析结果
Table 1 Results of multiviriate logistic regression analysis
| 变量 | β | SE | Z | OR(95% CI) | P |
|---|---|---|---|---|---|
| 年龄 | 0.049 4 | 0.017 0 | 2.898 9 | 1.05(1.02, 1.08) | 0.001 |
| 未避孕 | 0.086 8 | 0.032 7 | 2.654 2 | 1.08(1.02, 1.15) | 0.001 |
| 内膜厚度 | 0.116 1 | 0.039 2 | 2.959 0 | 1.11(1.04, 1.19) | 0.001 |
| 变量 | β | SE | Z | OR(95% CI) | P |
|---|---|---|---|---|---|
| 左侧输卵管显影 | |||||
| 全程显影 | Reference | 1.00 | |||
| 间断显影 | 0.418 3 | 0.301 3 | 1.388 5 | 1.32(0.79, 2.2) | 0.297 |
| 全程未显影 | 3.312 6 | 1.011 0 | 3.276 5 | 7.52(2.05, 27.55) | 0.001 |
| 双侧输卵管显影情况 | |||||
| 良好 | Reference | 1.00 | |||
| 一般 | -1.741 2 | 0.647 4 | -2.689 6 | 0.42(0.19, 0.92) | 0.005 |
| 欠佳 | -2.614 9 | 1.785 4 | -1.464 6 | 0.28(0.06, 1.29) | 0.102 |
| 左侧卵巢周围造影剂弥散状态 | |||||
| 环状 | Reference | 1.00 | |||
| 半环状 | 0.678 7 | 0.257 3 | 2.638 1 | 1.57(1.16, 2.13) | 0.001 |
| 未见弥散 | 1.913 8 | 0.999 8 | 1.914 1 | 1.14(0.67, 1.93) | 0.629 |
| 右侧卵巢周围造影剂弥散状态 | |||||
| 环状 | Reference | 1.00 | |||
| 半环状 | 0.715 2 | 0.282 9 | 2.528 2 | 1.65(1.23, 2.23) | 0.001 |
| 未见弥散 | 3.400 8 | 1.106 3 | 3.074 1 | 4.52(2.28, 8.95) | 0.001 |
2.3. 4D HyCoSy术后3个月自然妊娠的单因素回归分析
单因素回归分析结果显示:年龄(OR=1.05,95% CI:1.02~1.09,P<0.01);未避孕未孕时长(OR=1.09,95% CI:1.02~1.16,P<0.01);内膜厚度(OR=1.12,95% CI:1.04~1.21,P<0.01);左侧输卵管显影情况(OR=27.46,95% CI:3.78~199.17,P<0.01);左侧卵巢周围造影剂弥散情况(OR=1.97,95% CI:1.19~3.26,P<0.01);右侧卵巢周围造影剂弥散情况(半环形弥散:OR=2.04,95% CI:1.17~3.56,P<0.01;未见弥散:OR=29.99,95% CI:3.43~262.18,P<0.01)差异具有统计学意义(附表2,https://doi.org/10.11817/j.issn.1672-7347.2022.220179T2)。
2.4. 4D HyCoSy术后3个月自然妊娠的多因素logistic回归分析
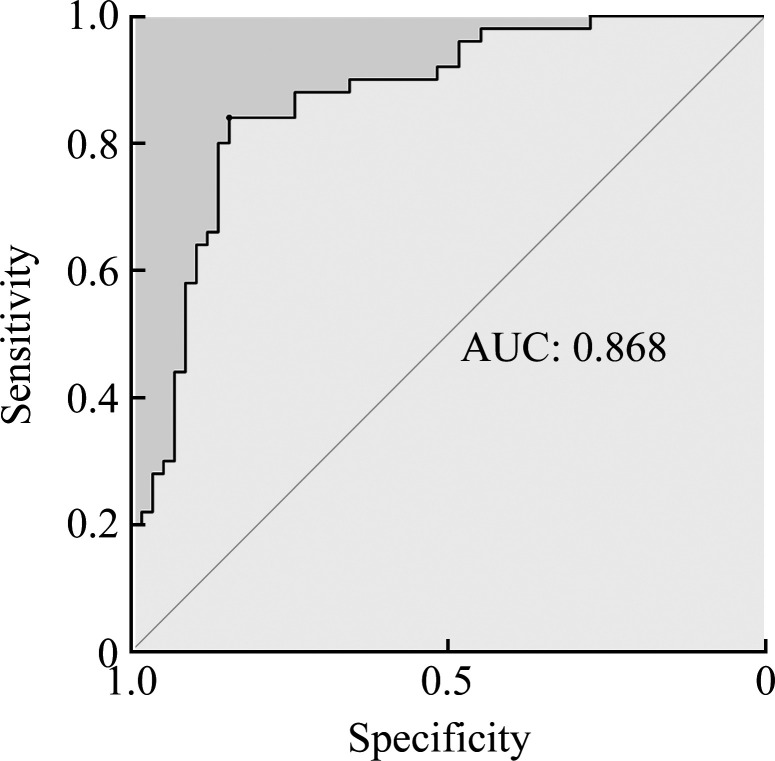
将单因素分析中差异有统计学意义的变量(年龄、未避孕未孕时长、内膜厚度、左侧输卵管显影、左侧输卵管显影、左侧卵巢周围造影剂弥散情况、右侧卵巢周围造影剂造影剂弥散情况)纳入模型(表1),通过10倍交叉验证法和受试者特征曲线的AUC来确定模型的分类能力,10倍交叉验证预测的AUC值均大于0.75,最佳AUC为0.868(图1)。预测模型得出的Q值为自然妊娠概率,截断值为0.5,当Q值大于0.5建议自然怀孕1年,小于0.5建议采用辅助生殖技术。
图1.
基于四维超声子宫输卵管造影影像学特征的造影术后自然妊娠预测模型的曲线下面积为0.868
Figure 1 Area under the curve of the model established for predicting natural pregnancy possibility based on the imaging characteristics of 4-dimensional hysterosalpingo-contrast sonography is 0.868
3. 讨 论
输卵管是女性生殖系统的重要组成部分,具有拾卵、输送精子、提供受精场所、营养受精卵和输送胚胎等功能,被形象地称为“生命的管道”[11]。女性不孕与输卵管生理解剖结构具有密切相关性[5, 12]。输卵管通畅程度、蠕动情况、拾卵功能和盆腔内环境是影响输卵管生殖状态的主要因素。
近年来,超声诊断仪不断推陈出新,超声医学进入了快速发展期,二维、多普勒超声、超声造影技术在妇科中的应用越来越广泛。诊断不孕症用到的一项非常关键的技术就是HyCoSy。该技术目前已经成为检测输卵管是否通畅的重要手段之一。4D HyCoSy是继2D、3D之后的一种新型超声造影技术,其集成超声造影技术及3D成像的优点,立体直观地将输卵管全段显现出来,尤其对位置特殊,形状盘曲或扭曲的输卵管有较好的显现效果。另外,4D HyCoSy还可以观察子宫、卵巢及盆腔情况,能获得宫腔及输卵管腔的3D立体容积成像[13-14],在对不孕症相关的宫腔病变如宫腔粘连、黏膜下肌瘤、子宫内膜息肉等的辨别中较为敏感,且诊断符合率高,与腹腔镜检查结果有较高的一致性[15-16]。4D HyCoSy用大扇角进行扫查,重建输卵管的走形,更形象、直观地显示输卵管的阻塞部位及走形细微的变化,并根据输卵管的具体情况加大推注压力,对输卵管有一定的疏通治疗作用,有助于提高输卵管阻塞性不孕症患者的受孕率。分析其原因有以下几方面:1)流动的造影剂对输卵管有机械的冲洗和扩张作用;2)造影剂的流动可对周围组织产生牵拉,可分离轻度的粘连;3)造影剂进入宫颈管内改变了局部黏液环境,使精子更容易通过且存活时间更长,还可以减少精子被单核细胞吞噬[17];4)造影剂直径较小,溶于血液,可通过呼吸排出,安全无辐射[18],术后不需要避孕[19]。Shalve等[20]的研究则显示:用4D HyCoSy检测出输卵管双侧均通畅的不孕症患者,给予人工授精,在2个人工授精的周期内,患者累计怀孕率约28.90%。Wang等[21]研究发现用4D HyCoSy检测出输卵管有一侧通畅的患者也有较高的妊娠率。本研究中不孕患者4D HyCoSy后随访3个月,自然妊娠率为27.74%。
4D HyCoSy可实时动态地观察造影剂流入宫腔及输卵管,并从输卵管伞端弥散入盆腔的情况。造影过程中重点观察输卵管柔软度、黏膜结构、通畅度、造影剂在盆腔内的弥散情况。输卵管柔软提示输卵管肌细胞功能正常,当炎症及子宫内膜异位症等病变使输卵管肌层受累时,可导致疤痕形成,从而使输卵管柔软度异常。研究[22]发现输卵管柔软度可作为反映输卵管病变程度的一项重要指标,对于输卵管欠柔软或僵硬的患者,建议放弃疏通或整形术而直接行体外受精-胚胎移植(in vitro fertilization and embryo transfer,IVF-ET)。Kudaiberdieva等[23]发现妊娠结局与输卵管伞端变形程度和输卵管黏膜受损程度有关,本研究证实了这一观点。本研究单因素和多因素logistic回归分析得出输卵管显影、卵巢周围造影剂弥散情况与造影术后妊娠结局显著相关。当管腔内存在粘连导致管腔狭窄时,盆腔内仅少量造影剂弥散,甚至需加压后盆腔内方可见造影剂从伞端缓慢流出,管壁僵硬、毛糙,可见憩室或龛影,管腔扭曲,粘连严重者甚至卷曲成团状,出现积水,说明肌层严重受损,管壁弹性差,蠕动功能及收缩功能减低;管腔稍扭曲、粗细不均,表示输卵管周围有粘连,复查时盆腔内可见造影剂弥散欠均匀,局部可呈斑片状,说明盆腔内可能存在粘连;输卵管走行区可见管腔内造影剂残留,说明黏膜受损,纤毛细胞功能异常,不能及时将造影剂排空(典型病例的4D HyCoSy图详见附图1,https://doi.org/10.11817/j.issn.1672-7347.2022.220179F1)。炎症会引起输卵管内膜肿胀,分泌物增多,黏膜上皮坏死脱落,导致管腔狭窄或阻塞[24]。当炎症破坏整个管壁时,纤毛运动及平滑肌舒缩功能异常,形成瘢痕后可使管壁僵硬、形态扭曲,粘连严重时甚至改变输卵管与卵巢原有的位置关系,导致不孕、异位妊娠、盆腔炎[25]。
子宫内膜厚度作为一个重要的临床指标与妊娠结局密切相关。受精卵经输卵管到达子宫,以囊胚的形式种植于营养丰富的子宫内膜内,良好的子宫内膜是胚胎着床的必要条件,而内膜的转化是一个动态过程[26]。有学者[27]认为:胚胎着床期子宫内膜过薄(<8 mm),不利于胚胎种植,临床妊娠率极低;子宫内膜厚度>16 mm,临床妊娠率也降低。Liu等[28]研究发现:在月经早期子宫内膜过厚(>7 mm)的冻胚移植患者妊娠率明显低于内膜≤7 mm的患者。在本研究中,妊娠组月经早期子宫内膜厚度为(6.69 ±1.86) mm,未妊娠组内膜为(7.17±2.08) mm,提示月经早期子宫内膜过厚的冻胚移植患者妊娠率降低。这与上述报道一致。
本组研究对象年龄为20~40岁,卵巢功能均正常,妊娠组与非妊娠组的年龄差异具有统计学意义,提示年龄与输卵管通畅程度相关,分析原因为年龄小的患者生殖系统受感染的机会要比年龄大有过妊娠史的小。本研究中4D HyCoSy后妊娠结局和患者不孕年限呈负相关,提示不孕年限越长,输卵管损害恢复越差,妊娠预后越差。随着不孕时间的延长,盆腔内粘连的程度会逐渐加重[29]。此外,不孕症容易引发患者焦虑、抑郁等负面情绪,也会影响正常受孕,二者相互促进和制约[30]。因此,应该及早发现并积极治疗输卵管阻塞性不孕,从而减少输卵管的损伤,提高妊娠率。
4D HyCoSy在诊断输卵管通畅性中特异性和准确性均较高,但是临床上缺乏一个预测造影术后是否可以自然妊娠的影像学标准。本研究将单因素分析中差异有统计学意义的变量(年龄、未避孕、内膜厚度、左侧输卵管显影、右侧输卵管显影、左侧卵巢周围造影剂弥散情况、右侧卵巢周围造影剂弥散情况)纳入4D HyCoSy术后妊娠结局预测模型,通过10倍交叉验证法得出的AUC均大于0.75,提示本研究的预测模型可较准确预测4D HyCoSy术后自然受孕的妊娠结局。对于输卵管情况好或轻度损伤,自然妊娠概率大的患者,可试孕或适当给予药物保守治疗。对于输卵管损伤严重,自然妊娠概率小,年龄大,有急切的生育要求、不孕年限长等的患者,可考虑直接行IVF-ET,以免反复治疗效果不佳而增加患者心理、生理及经济上的负担。
综上所述,本研究基于输卵管性不孕患者的临床及4D HyCoSy的影像表现建立自然妊娠的预测模型,能有效预测造影术后是否可以自然妊娠,有利于临床医生为患者制订最佳的诊疗方案,具有一定的指导意义。
附录.
附表1.
2组一般资料比较
| 指标 | 自然怀孕/人工授精(n=301) | 试管/未孕(n=784) | P |
|---|---|---|---|
| 年龄/岁 | 30.18±4.20 | 31.62±5.01 | <0.001 |
| 水囊长径/cm | 12.64±1.79 | 12.70±4.31 | 0.811 |
| 造影剂量/mL | 18.73(4.86) | 18.43(6.26) | 0.448 |
| 未避孕/年 | 2.68(2.17) | 3.43(3.05) | <0.001 |
| 内膜厚度/mm | 6.69(1.86) | 7.17(2.08) | 0.001 |
| 水囊量/mL | 0.92(0.41) | 0.92(0.48) | 0.958 |
| 反流量/mL | 2.39(4.55) | 2.81(4.72) | 0.189 |
| 子宫畸形/[例(%)] | 0.129 | ||
| 无 | 278(92.3) | 698(89.0) | |
| 有 | 23(7.7) | 86(11.0) | |
| 输卵管手术史/[例(%)] | 0.266 | ||
| 无 | 293(97.3) | 750(95.7) | |
| 有 | 8(2.7) | 34(4.3) | |
| 左侧卵巢与子宫/[例(%)] | 0.398 | ||
| 邻近 | 223(74.1) | 560(71.3) | |
| 远离 | 78(25.9) | 224(28.7) | |
| 右侧卵巢与子宫/[例(%)] | 0.304 | ||
| 邻近 | 172(57.1) | 477(60.8) | |
| 远离 | 129(42.9) | 307(39.2) | |
| 卵巢远离子宫的个数/[例(%)] | 0.648 | ||
| 0 | 131(43.5) | 335(42.8) | |
| 1 | 133(44.2) | 365(46.6) | |
| 2 | 37(12.3) | 83(10.6) | |
| 左侧卵巢活动度/[例(%)] | <0.001 | ||
| 好 | 146(48.5) | 286(36.2) | |
| 欠佳 | 155(51.5) | 498(63.8) | |
| 右侧卵巢活动度/[例(%)] | <0.001 | ||
| 好 | 191(63.5) | 372(47.4) | |
| 欠佳 | 110(36.5) | 412(52.6) | |
| 卵巢活动度欠佳的个数/[例(%)] | <0.001 | ||
| 0 | 122(40.5) | 190(24.3) | |
| 1 | 93(30.9) | 276(35.2) | |
| 2 | 86(28.6) | 317(40.5) | |
| 左侧输卵管显影/[例(%)] | <0.01 | ||
| 全程显影 | 263(87.4) | 625(80.0) | |
| 间断显影 | 33(11.0) | 103(13.2) | |
| 全程未显影 | 5(1.7) | 53(6.8) | |
| 右侧输卵管显影/[例(%)] | <0.05 | ||
| 全程显影 | 265(88.3) | 634(82.1) | |
| 间断显影 | 27(9.0) | 97(12.6) | |
| 全程未显影 | 8(2.7) | 41(5.3) |
Supplementary Table 1 Comparison of clinical data between the 2 groups
附表1.
(续)
| 指标 | 自然怀孕/人工授精(n=301) | 试管/未孕(n=784) | P |
|---|---|---|---|
| 双侧输卵管显影情况/[例(%)] | <0.05 | ||
| 良好 | 279(92.7) | 680(86.7) | |
| 一般 | 18(6.0) | 72(9.2) | |
| 欠佳 | 4(1.3) | 32(4.1) | |
| 左侧输卵管管壁/[例(%)] | 0.172 | ||
| 光整 | 273(90.7) | 686(87.5) | |
| 不光整 | 28(9.3) | 98(12.5) | |
| 右侧输卵管管壁/[例(%)] | <0.05 | ||
| 光整 | 276(91.7) | 680(86.7) | |
| 不光整 | 25(8.3) | 104(13.3) | |
| 输卵管管壁/[例(%)] | <0.05 | ||
| 双侧光整 | 258(85.7) | 618(78.8) | |
| 一侧光整 | 33(11.0) | 130(16.6) | |
| 双侧均不光整 | 10(3.3) | 36(4.6) | |
| 左侧输卵管走形/形态/[例(%)] | 0.532 | ||
| 柔顺 | 57(16.2) | 198(18.0) | |
| 不柔顺 | 244(83.8) | 586(82.0) | |
| 右侧输卵管走形/形态/[例(%)] | <0.01 | ||
| 柔顺 | 114(36.0) | 256(26.5) | |
| 不柔顺 | 187(64.0) | 528(73.5) | |
| 输卵管走形/形态/[例(%)] | 0.715 | ||
| 双侧均柔顺 | 24(8.0) | 66(8.6) | |
| 一侧柔顺 | 119(39.8) | 284(37.2) | |
| 双侧均不柔顺 | 156(52.2) | 415(54.2) | |
| 左侧输卵管伞端造影剂溢出情况/[例(%)] | <0.01 | ||
| 大量溢出 | 212(70.4) | 484(62.0) | |
| 少量溢出 | 53(17.6) | 135(17.3) | |
| 未见溢出 | 36(12.0) | 162(20.7) | |
| 右侧输卵管伞端造影剂溢出情况/[例(%)] | <0.001 | ||
| 大量溢出 | 240(80.0) | 522(66.8) | |
| 少量溢出 | 39(13.0) | 121(15.5) | |
| 未见溢出 | 21(7.0) | 139(17.8) | |
| 左侧卵巢周围造影剂弥散状态/[例(%)] | <0.001 | ||
| 环状 | 135(44.9) | 228(29.1) | |
| 半环状 | 129(42.9) | 394(50.3) | |
| 未见弥散 | 37(12.2) | 162(20.6) | |
| 右侧卵巢周围造影剂弥散状态/[例(%)] | <0.001 | ||
| 环状 | 169(56.2) | 289(36.9) | |
| 半环状 | 112(37.2) | 353(45.1) | |
| 未见弥散 | 20(6.6) | 141(18.0) | |
| 子宫肌层内造影剂渗入情况/[例(%)] | 0.575 | ||
| 未见渗入 | 246(81.7) | 627(79.9) | |
| 见渗入 | 55(18.3) | 157(20.1) |
附表1.
(续)
| 指标 | 自然怀孕/人工授精(n=301) | 试管/未孕(n=784) | P |
|---|---|---|---|
| 阻力情况/[例(%)] | <0.01 | ||
| 全程无阻力 | 96(32.4) | 171(22.0) | |
| 前有后无 | 11(3.7) | 33(4.2) | |
| 前无后有 | 33(11.2) | 103(13.3) | |
| 全程有阻力 | 156(52.7) | 470(60.5) | |
| 诊断/[例(%)] | 0.229 | ||
| 原发性不孕 | 120(39.9) | 356(44.1) | |
| 继发性不孕 | 181(60.1) | 438(55.9) | |
| 妇科手术史/[例(%)] | 0.603 | ||
| 无 | 133(44.2) | 352(46.2) | |
| 有 | 168(55.8) | 422(53.8) | |
| 月经持续天数/[例(%)] | 0.080 | ||
| 正常 | 278(92.4) | 694(88.5) | |
| 异常 | 23(7.6) | 90(11.5) | |
| 月经量/[例(%)] | 0.125 | ||
| 适量 | 210(69.8) | 503(64.4) | |
| 量少 | 65(21.6) | 216(27.7) | |
| 量多 | 26(8.6) | 62(7.9) | |
| 有无痛经/[例(%)] | 0.318 | ||
| 无 | 161(53.5) | 393(49.9) | |
| 有 | 140(46.5) | 391(50.1) | |
| 月经周期/[例(%)] | 0.541 | ||
| 正常 | 276(91.6) | 718(90.2) | |
| 异常 | 25(8.4) | 76(9.8) | |
| 宫腔形态/[例(%)] | 0.081 | ||
| 正常 | 261(86.7) | 644(82.1) | |
| 异常 | 40(13.3) | 140(17.9) | |
| 反流情况/[例(%)] | <0.05 | ||
| 无 | 167(55.5) | 378(48.2) | |
| 有 | 134(44.5) | 406(51.8) |
附表2.
单因素logistic回归结果
| 指标 | β | SE | z | Pr(>|z|) | OR(95% CI) |
|---|---|---|---|---|---|
| 年龄 | 0.069 | 0.015 | 4.361 | <0.001 | 1.07(1.04, 1.10) |
| 水囊长径 | 0.005 | 0.019 | 0.239 | 0.811 | 1.00(0.97, 1.04) |
| 造影剂量 | -0.009 | 0.011 | -0.760 | 0.448 | 0.99(0.97, 1.01) |
| 未避孕 | 0.110 | 0.029 | 3.829 | <0.001 | 1.12(1.06, 1.18) |
| 内膜厚度 | 0.121 | 0.035 | 3.454 | <0.001 | 1.13(1.05, 1.21) |
| 水囊量 | 0.008 | 0.147 | 0.052 | 0.958 | 1.01(0.76, 1.34) |
| 反流量 | 0.021 | 0.016 | 1.309 | 0.191 | 1.02(0.99, 1.05) |
| 子宫畸形 | |||||
| 无 | Reference | ||||
| 有 | 0.398 | 0.245 | 1.623 | 0.105 | 1.49(0.92, 2.41) |
| 输卵管手术史 | |||||
| 无 | Reference | ||||
| 有 | 0.508 | 0.399 | 1.274 | 0.203 | 1.66(0.76, 3.63) |
| 左侧卵巢与子宫 | |||||
| 邻近 | Reference | ||||
| 远离 | 0.141 | 0.154 | 0.921 | 0.357 | 1.15(0.85, 1.56) |
| 右侧卵巢与子宫 | |||||
| 邻近 | Reference | ||||
| 远离 | -0.151 | 0.138 | -1.097 | 0.273 | 0.86(0.66, 1.13) |
| 卵巢远离子宫的个数 | |||||
| 0 | Reference | ||||
| 1 | 0.071 | 0.145 | 0.489 | 0.625 | 1.07(0.81, 1.42) |
| 2 | -0.131 | 0.223 | -0.588 | 0.557 | 0.88(0.57, 1.36) |
| 左侧卵巢活动度 | |||||
| 好 | Reference | ||||
| 欠佳 | 0.509 | 0.137 | 3.706 | <0.001 | 1.66(1.27, 2.18) |
| 右侧卵巢活动度 | |||||
| 好 | Reference | ||||
| 欠佳 | 0.657 | 0.140 | 4.708 | <0.001 | 1.93(1.47, 2.53) |
| 卵巢活动度欠佳的个数 | |||||
| 0 | Reference | ||||
| 1 | 0.645 | 0.167 | 3.865 | <0.001 | 1.91(1.37, 2.64) |
| 2 | 0.862 | 0.168 | 5.127 | <0.001 | 2.37(1.70, 3.29) |
| 左侧输卵管显影 | |||||
| 全程显影 | Reference | ||||
| 间断显影 | 0.273 | 0.213 | 1.279 | 0.201 | 1.31(0.86, 1.99) |
| 全程未显影 | 1.495 | 0.473 | 3.158 | <0.001 | 4.46(1.76, 11.28) |
| 右侧输卵管显影 | |||||
| 全程显影 | Reference | ||||
| 间断显影 | 0.407 | 0.230 | 1.771 | 0.077 | 1.5(0.96, 2.35) |
| 全程未显影 | 0.762 | 0.393 | 1.937 | 0.053 | 2.14(0.99, 4.63) |
Supplementary Table 2 Results of univariate logistic regression
附表2.
(续)
| 指标 | β | SE | z | Pr(>|z|) | OR(95% CI) |
|---|---|---|---|---|---|
| 双侧输卵管显影情况 | |||||
| 良好 | Reference | ||||
| 一般 | 0.495 | 0.273 | 1.815 | 0.069 | 1.64(0.96, 2.80) |
| 欠佳 | 1.189 | 0.535 | 2.221 | <0.05 | 3.28(1.15, 9.37) |
| 左侧输卵管管壁 | |||||
| 光整 | Reference | ||||
| 不光整 | 0.331 | 0.226 | 1.467 | 0.143 | 1.39(0.89, 2.17) |
| 右侧输卵管管壁 | |||||
| 光整 | Reference | ||||
| 不光整 | 0.524 | 0.234 | 2.240 | <0.05 | 1.69(1.07, 2.67) |
| 输卵管管壁 | |||||
| 双侧光整 | Reference | ||||
| 一侧光整 | 0.498 | 0.209 | 2.386 | <0.05 | 1.64(1.09, 2.47) |
| 双侧均不光整 | 0.407 | 0.365 | 1.116 | 0.264 | 1.5(0.73, 3.07) |
| 左侧输卵管走形/形态 | |||||
| 柔顺 | Reference | ||||
| 不柔顺 | -0.134 | 0.187 | -0.715 | 0.474 | 0.88(0.61, 1.26) |
| 右侧输卵管走形/形态 | |||||
| 柔顺 | Reference | ||||
| 不柔顺 | 0.445 | 0.148 | 2.998 | <0.01 | 1.56(1.17, 2.09) |
| 输卵管走形/形态 | |||||
| 双侧均柔顺 | Reference | ||||
| 一侧柔顺 | -0.142 | 0.262 | -0.541 | 0.589 | 0.87(0.52, 1.45) |
| 双侧均不柔顺 | -0.033 | 0.256 | -0.130 | 0.897 | 0.97(0.59, 1.60) |
| 左侧输卵管伞端造影剂溢出情况 | |||||
| 大量溢出 | Reference | ||||
| 少量溢出 | 0.111 | 0.182 | 0.602 | 0.547 | 1.12(0.78, 1.59) |
| 未见溢出 | 0.679 | 0.202 | 3.362 | <0.001 | 1.97(1.33, 2.93) |
| 右侧输卵管伞端造影剂溢出情况 | |||||
| 大量溢出 | Reference | ||||
| 少量溢出 | 0.355 | 0.200 | 1.776 | 0.076 | 1.43(0.96, 2.11) |
| 未见溢出 | 1.113 | 0.247 | 4.510 | <0.001 | 3.04(1.88, 4.94) |
| 左侧卵巢周围造影剂弥散状态 | |||||
| 环状 | Reference | ||||
| 半环状 | 0.593 | 0.149 | 3.987 | <0.001 | 1.81(1.35, 2.42) |
| 未见弥散 | 0.953 | 0.212 | 4.491 | <0.001 | 2.59(1.71, 3.93) |
| 右侧卵巢周围造影剂弥散状态 | |||||
| 环状 | Reference | ||||
| 半环状 | 0.611 | 0.145 | 4.206 | <0.001 | 1.84(1.39, 2.45) |
| 未见弥散 | 1.417 | 0.258 | 5.494 | <0.001 | 4.12(2.49, 6.83) |
| 子宫肌层内造影剂渗入情况 | |||||
| 未见渗入 | Reference | ||||
| 见渗入 | 0.112 | 0.174 | 0.647 | 0.518 | 1.12(0.80, 1.57) |
附表2.
(续)
| 指标 | β | SE | z | Pr(>|z|) | OR(95% CI) |
|---|---|---|---|---|---|
| 阻力情况 | |||||
| 全程无阻力 | Reference | ||||
| 前有后无 | 0.521 | 0.371 | 1.406 | 0.159 | 1.68(0.81, 3.48) |
| 前无后有 | 0.561 | 0.237 | 2.364 | <0.05 | 1.75(1.1, 2.79) |
| 全程有阻力 | 0.526 | 0.158 | 3.337 | <0.001 | 1.69(1.24, 2.3) |
| 诊断 | |||||
| 原发性不孕 | Reference | ||||
| 继发性不孕 | -0.175 | 0.138 | -1.270 | 0.204 | 0.84(0.64, 1.1) |
| 妇科手术史 | |||||
| 无 | Reference | ||||
| 有 | -0.080 | 0.136 | -0.588 | 0.556 | 0.92(0.71, 1.21) |
| 月经持续天数 | |||||
| 正常 | Reference | ||||
| 异常 | 0.451 | 0.244 | 1.847 | 0.065 | 1.57(0.97, 2.53) |
| 月经量 | |||||
| 适量 | Reference | ||||
| 量少 | 0.327 | 0.164 | 2.001 | <0.05 | 1.39(1.01, 1.91) |
| 量多 | -0.004 | 0.248 | -0.018 | 0.986 | 1(0.61, 1.62) |
| 有无痛经 | |||||
| 无 | Reference | ||||
| 有 | 0.145 | 0.136 | 1.066 | 0.287 | 1.16(0.89, 1.51) |
| 月经周期 | |||||
| 正常 | Reference | ||||
| 异常 | 0.175 | 0.241 | 0.727 | 0.468 | 1.19(0.74, 1.91) |
| 宫腔形态 | |||||
| 正常 | Reference | ||||
| 异常 | 0.354 | 0.194 | 1.829 | 0.068 | 1.43(0.97, 2.08) |
| 反流情况 | |||||
| 无 | Reference | ||||
| 有 | 0.292 | 0.136 | 2.141 | <0.05 | 1.34(1.02, 1.75) |
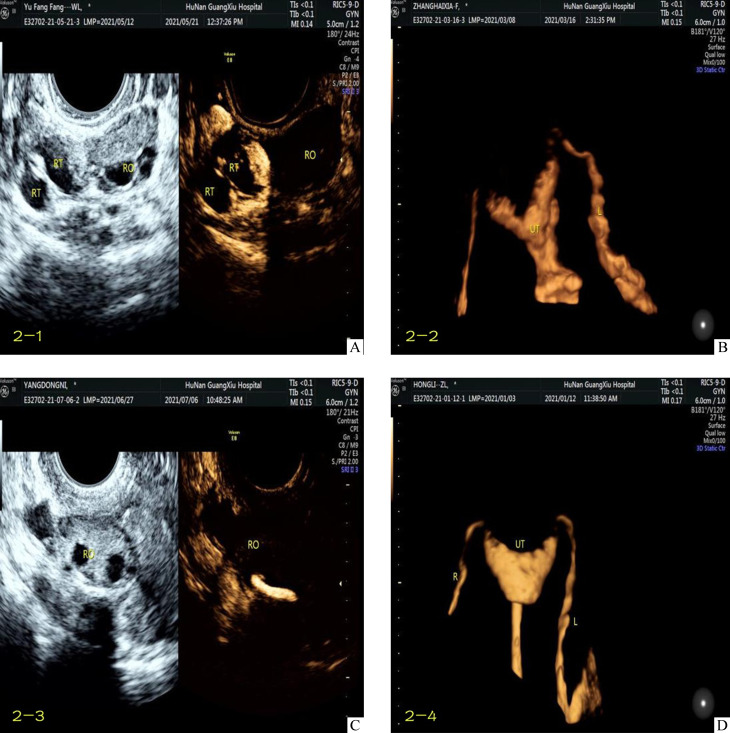
附图1. 典型病例的四维超声子宫输卵管造影图Supplementary Figure 1 Imaging of 4-dimensional hysterosalpingo-contrast sonography of typical patient .
A: Hydrosalpinx on the right side with accumulation of contrast media; B: Uneven left fallopian tube in nodule shape; C: Accumulation of contrast media in the right fallopian tube and no obvious contrast media around the right ovary; D: Stiff left fallopian tube and close to the serosal layer.
基金资助
国家重点研发项目(2018YFC1004800);湖南省科技计划项目(2021SK53704,2020SK53605)。
This study was supported by the National Key Research and Development Program (2018YFC1004800) and the Hunan Provincial Clinical Medical Technology Innovation Guiding Project (2021SK53704, 2020SK53605), China.
利益冲突声明
作者声称无任何利益冲突。
作者贡献
赵行平 数据分析;论文设计、撰写与修改;费玲燕,顾盼 数据采集;徐大宝 研究设计;张白云 论文指导;杨益民 论文指导及修改。全体作者阅读并同意最终的文本。
原文网址
http://xbyxb.csu.edu.cn/xbwk/fileup/PDF/2022111600.pdf
参考文献
- 1. Mandia L, Personeni C, Antonazzo P, et al. Ultrasound in infertility setting: optimal strategy to evaluate the assessment of tubal patency[J]. Biomed Res Int, 2017, 2017: 3205895. 10.1155/2017/3205895. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2. Feinberg EC. True, true, and unrelated: tubal patency, tubal architecture, and tubal function[J]. Fertil Steril, 2018, 110(4): 646-647. 10.1016/j.fertnstert.2018.06.007. [DOI] [PubMed] [Google Scholar]
- 3. Parry JP, Riche D, Rushing J, et al. Performing the Parryscope technique gently for office tubal patency assessment[J]. Fertil Steril, 2017, 108(4): 718. 10.1016/j.fertnstert.2017.07.1159. [DOI] [PubMed] [Google Scholar]
- 4. Promberger R, Simek IM, Nouri K, et al. Accuracy of tubal patency assessment in diagnostic hysteroscopy compared with laparoscopy in infertile women: a retrospective cohort study[J]. J Minim Invasive Gynecol, 2018, 25(5): 794-799. 10.1016/j.jmig.2017.11.020. [DOI] [PubMed] [Google Scholar]
- 5. He YN, Ma XH, Xu JJ, et al. Comparison of assessment methods for fallopian tubal patency and peritubal adhesion between transvaginal 4-dimensional hysterosalpingo-contrast sonography and laparoscopic chromopertubation[J]. J Ultrasound Med, 2017, 36(3): 547-556. 10.7863/ultra.15.11056. [DOI] [PubMed] [Google Scholar]
- 6. Ott J, Hager M, Nouri K, et al. Assessment of tubal patency: a prospective comparison of diagnostic hysteroscopy and laparoscopic chromopertubation[J]. J Minim Invasive Gynecol, 2020, 27(1): 135-140. 10.1016/j.jmig.2019.03.006. [DOI] [PubMed] [Google Scholar]
- 7. Exacoustos C, di Giovanni A, Szabolcs B, et al. Automated three-dimensional coded contrast imaging hysterosalpingo-contrast sonography: feasibility in office tubal patency testing[J]. Ultrasound Obstet Gynecol, 2013, 41(3): 328-335. 10.1002/uog.11200. [DOI] [PubMed] [Google Scholar]
- 8. Wang WQ, Zhou QL, Zhou XX, et al. Influence factors on contrast agent venous intravasation during transvaginal 4-dimensional hysterosalpingo-contrast sonography[J]. J Ultrasound Med, 2018, 37(10): 2379-2385. 10.1002/jum.14594. [DOI] [PubMed] [Google Scholar]
- 9. Lőrincz J, Jakab A, Török P. Comparison of current methods of tubal patency assessment[J]. Orv Hetil, 2017, 158(9): 324-330. 10.1556/650.2017.30653. [DOI] [PubMed] [Google Scholar]
- 10. Lawrie TA, Kulier R, Nardin JM. Techniques for the interruption of tubal patency for female sterilisation[J]. Cochrane Database Syst Rev, 2016(8): CD003034. 10.1002/14651858.CD003034.pub4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11. Raban O, Zilber H, Hadar E, et al. Isolated fallopian tube torsion: A unique ultrasound identity or a serial copycat? [J]. J Ultrasound Med, 2018, 37(10): 2387-2393. 10.1002/jum.14595. [DOI] [PubMed] [Google Scholar]
- 12. Rodriguez AM, Kilic GS, Vu TP, et al. Analysis of tubal patency after essure placement[J]. J Minim Invasive Gynecol, 2013, 20(4): 468-472. 10.1016/j.jmig.2013.01.013. [DOI] [PubMed] [Google Scholar]
- 13. Hamilton J, Latarche E, Gillott C, et al. Intrauterine insemination results are not affected if hysterosalpingo contrast sonography is used as the sole test of tubal patency[J]. Fertil Steril, 2003, 80(1): 165-171. 10.1016/s0015-0282(03)00567-3. [DOI] [PubMed] [Google Scholar]
- 14. Jagadambe A, Oakeshott P, Ojha K, et al. Methods of assessing tubal patency[J]. Sex Transm Infect, 2012, 88(4): 249. 10.1136/sextrans-2012-050559. [DOI] [PubMed] [Google Scholar]
- 15. Kupesic S, Plavsic BM. 2D and 3D hysterosalpingo-contrast-sonography in the assessment of uterine cavity and tubal patency[J]. Eur J Obstet Gynecol Reprod Biol, 2007, 133(1): 64-69. 10.1016/j.ejogrb.2006.10.010. [DOI] [PubMed] [Google Scholar]
- 16. Kuzmin A, Linde V. Diagnostic and remedial capability of transcervical falloposcopy in conjunction with laparoscopy[J]. Gynecol Endocrinol, 2014, 30(Suppl 1): 17-19. 10.3109/09513590.2014.945771. [DOI] [PubMed] [Google Scholar]
- 17. Johnson NP, Hadden WE, Chamley LW. Fertility enhancement by hysterosalpingography with oil-soluble contrast media: reality not myth[J]. AJR Am J Roentgenol, 2005, 185(6): 1654;author reply1654-1654;author reply1657. 10.2214/AJR.05.5159. [DOI] [PubMed] [Google Scholar]
- 18. Ludwin I, Ludwin A, Wiechec M, et al. Accuracy of hysterosalpingo-foam sonography in comparison to hysterosalpingo-contrast sonography with air/saline and to laparoscopy with dye[J]. Hum Reprod, 2017, 32(4): 758-769. 10.1093/humrep/dex013. [DOI] [PubMed] [Google Scholar]
- 19. Exacoustos C, Pizzo A, Lazzeri L, et al. Three-dimensional hysterosalpingo contrast sonography with gel foam: methodology and feasibility to obtain 3-dimensional volumes of tubal shape[J]. J Minim Invasive Gynecol, 2017, 24(5): 827-832. 10.1016/j.jmig.2017.04.007. [DOI] [PubMed] [Google Scholar]
- 20. Shaleve J, Krissi H, Blankstein J, et al. Modified hysterosalpingography during infertility work-up: use of contrast medium and saline to investigate mechanical factors[J]. Fertil Steril, 2000, 74(2): 372-375. 10.1016/s0015-0282(00)00632-4. [DOI] [PubMed] [Google Scholar]
- 21. Wang R, van Welie N, van Rijswijk J, et al. Effectiveness on fertility outcome of tubal Flushing with different contrast media: systematic review and network meta-analysis[J]. Ultrasound Obstet Gynecol, 2019, 54(2): 172-181. 10.1002/uog.20238. [DOI] [PubMed] [Google Scholar]
- 22. Jurkovic D, Memtsa M, Sawyer E, et al. Single-dose systemic methotrexate vs expectant management for treatment of tubal ectopic pregnancy: a placebo-controlled randomized trial[J]. Ultrasound Obstet Gynecol, 2017, 49(2): 171-176. 10.1002/uog.17329. [DOI] [PubMed] [Google Scholar]
- 23. Kudaiberdieva A, Kangeldieva A. Prediction of laparoscopic surgery outcomes in tubal infertility[J]. Aust N Z J Obstet Gynaecol, 2005, 45(5): 460-463. 10.1111/j.1479-828X.2005.00463.x. [DOI] [PubMed] [Google Scholar]
- 24. Simpson WL, Beitia LG, Mester J. Hysterosalpingography: a reemerging study[J]. Radiographics, 2006, 26(2): 419-431. 10.1148/rg.262055109. [DOI] [PubMed] [Google Scholar]
- 25. Revzin MV, Mathur M, Dave HB, et al. Pelvic inflammatory disease: multimodality imaging approach with clinical-pathologic correlation[J]. Radiographics, 2016, 36(5): 1579-1596. 10.1148/rg.2016150202. [DOI] [PubMed] [Google Scholar]
- 26. Arya S, Kupesic Plavsic S. Preimplantation 3D ultrasound: current uses and challenges[J]. J Perinat Med, 2017, 45(6): 745-758. 10.1515/jpm-2016-0361. [DOI] [PubMed] [Google Scholar]
- 27. Jung YH, Kim YY, Kim MH, et al. Endometrial injury may promote implantation in patients with increased endometrial thickness on the day of hCG administration[J]. Fertil Steril, 2013, 100(3): S388. 10.1016/j.fertnstert.2013.07.703. [DOI] [Google Scholar]
- 28. Liu WJ, Nong YQ, Ruan JX, et al. Impact of endometrial thickness during menstruation and endometrial scratching on the pregnancy in frozen-thawed embryo transfer[J]. J Obstet Gynaecol Res, 2019, 45(3): 619-625. 10.1111/jog.13872. [DOI] [PubMed] [Google Scholar]
- 29. Reekie J, Donovan B, Guy R, et al. Risk of pelvic inflammatory disease in relation to Chlamydia and gonorrhea testing, repeat testing, and positivity: a population-based cohort study[J]. Clin Infect Dis, 2017, 66(3): 437-443. 10.1093/cid/cix769. [DOI] [PubMed] [Google Scholar]
- 30. Lawson AK, Klock SC, Pavone ME, et al. Prospective study of depression and anxiety in female fertility preservation and infertility patients[J]. Fertil Steril, 2014, 102(5): 1377-1384. 10.1016/j.fertnstert.2014.07.765. [DOI] [PMC free article] [PubMed] [Google Scholar]