Abstract
Introduction
Paederus dermatitis arises from inadvertent skin contact with insects of the genus Paederus, leading to irritant contact dermatitis. This study aims to highlight the diverse clinical presentations and the remarkable ability of the disease to mimic various dermatological conditions.
Methodology
A total of 15 patients diagnosed with Paederus dermatitis in a period of four months from August 2023 to November 2023 were included in this retrospective study. The demographic profile, detailed history, clinical presentation, and site of lesion distribution were documented.
Results
Out of 15 patients, nine were males, and eight were females. All patients exhibited a sudden onset of lesions accompanied by burning and pain, with an average duration of approximately 2.5 days. The most prevalent clinical presentation was the linear type, followed by kissing lesions, an erythematous patch with a central gray area, Nairobi eye, burnt appearance, and post-inflammatory pigmentation.
Conclusion
Paederus dermatitis is common in tropical areas like India but is prone to misdiagnosis due to its varied presentation. Increased awareness can lead to accurate diagnoses and simpler treatment plans, reducing patient confusion.
Keywords: burning sensation, blister beetle dermatitis, nairobi eye, vesiculobullous skin lesions, dermatitis linearis, kissing lesions, paederus dermatitis, irritant contact dermatitis (icd), rove beetles, blister beetle
Introduction
Paederus dermatitis is an irritant contact dermatitis caused by the accidental crushing of rove beetles, which releases a vesicant chemical, pederin. Contact of the skin with this potent blistering chemical through crushing results in the sudden onset of erythematous skin with vesicles and bullae with severe burning and stinging. The vesicant pederin is predominantly released at toxic doses by female rove beetles that bear endosymbiotic bacteria Pseudomonas species [1]. This beetle does not bite or sting, but accidental crushing or brushing against the skin causes the release of its hemolymph containing pederin that causes painful necrotic blisters [2-4].
Materials and methods
A retrospective case series analysis study was done in the Dermatology Department of Mahatma Gandhi Medical College and Research Institute located in Puducherry, India, for four months between August and November 2023. Approval for the said study was obtained from the Institutional Human Ethics Committee of Mahatma Gandhi Medical College and Research Institute (approval number: 314). All the patients who had attended the Dermatology Outpatient Department (OPD) during the study period with a clinical diagnosis of Paederus dermatitis made by the consultant were included. A total of 15 patients were included in the study, and all the clinical data was retrieved from the patient management system at the hospital. A detailed sociodemographic and clinical history included age, gender, patient's residential area, patient's awareness of any insect contact, sudden onset of lesions after waking up/travel, clinical morphology of the lesions, site of lesion, and associated symptoms such as burning, pain, blisters, or scarring. A case study proforma was made bearing all the relevant details. All these details were documented in the case study sheet. Data analysis was done using IBM SPSS Statistics for Windows, Version 22.0 (Released 2013; IBM Corp., Armonk, New York, United States), and results were expressed in frequency and percentage.
Results
In this case series study of 15 patients, the gender distribution was nine male and eight female patients. The clinicodemographic details of all the patients included in the study were recorded (Table 1). Thirteen patients recognized the onset of lesions post-sleep cycle, while two out of 15 patients did not correlate it with sleep or travel. Only two patients had prior knowledge of insect contact preceding the onset of lesions, and both of them noticed it during travel in a bus with the windshield open.
Table 1. Clinicodemographic details of the patients included in the study.
| Patient | Sex | Age (years) | Locality | Knowledge of contact with insect | Proximity to field or terrestrial areas | Onset of lesions after sleep/travel |
| 1 | Male | 60 | Rural | No | Yes | Yes |
| 2 | Male | 43 | Rural | No | Yes | Yes |
| 3 | Male | 10 | Rural | No | Yes | Yes |
| 4 | Female | 35 | Rural | No | Yes | No |
| 5 | Female | 42 | Urban | Yes | No | Yes |
| 6 | Male | 28 | Urban | No | Yes | No |
| 7 | Male | 36 | Rural | No | Yes | Yes |
| 8 | Female | 12 | Rural | No | Yes | Yes |
| 9 | Male | 29 | Urban | No | Yes | Yes |
| 10 | Male | 33 | Rural | No | Yes | No |
| 11 | Female | 45 | Rural | No | Yes | Yes |
| 12 | Male | 52 | Rural | No | Yes | Yes |
| 13 | Female | 50 | Rural | No | Yes | Yes |
| 14 | Female | 47 | Rural | No | Yes | Yes |
| 15 | Male | 46 | Rural | Yes | No | Yes |
Regarding symptom presentation, burning was uniformly reported in 14 out of 15 patients (93.3%) with active lesions, redness in 14 out of 15 patients (93.3%), and blistering in 10 out of 15 patients (66.6%), and pain was observed in 12 out of 15 patients (80%). Only one patient presented late after the healing of the acute dermatitis with no symptoms. Additionally, severe wincing pain upon touch was noted in 14 out of 15 patients, corresponding to approximately 93.3% of the study group. The video demonstrating the pain on touching the lesion is given below (Video 1).
Video 1. Video demonstrating severe wincing pain on touching the lesion in Paederus dermatitis.
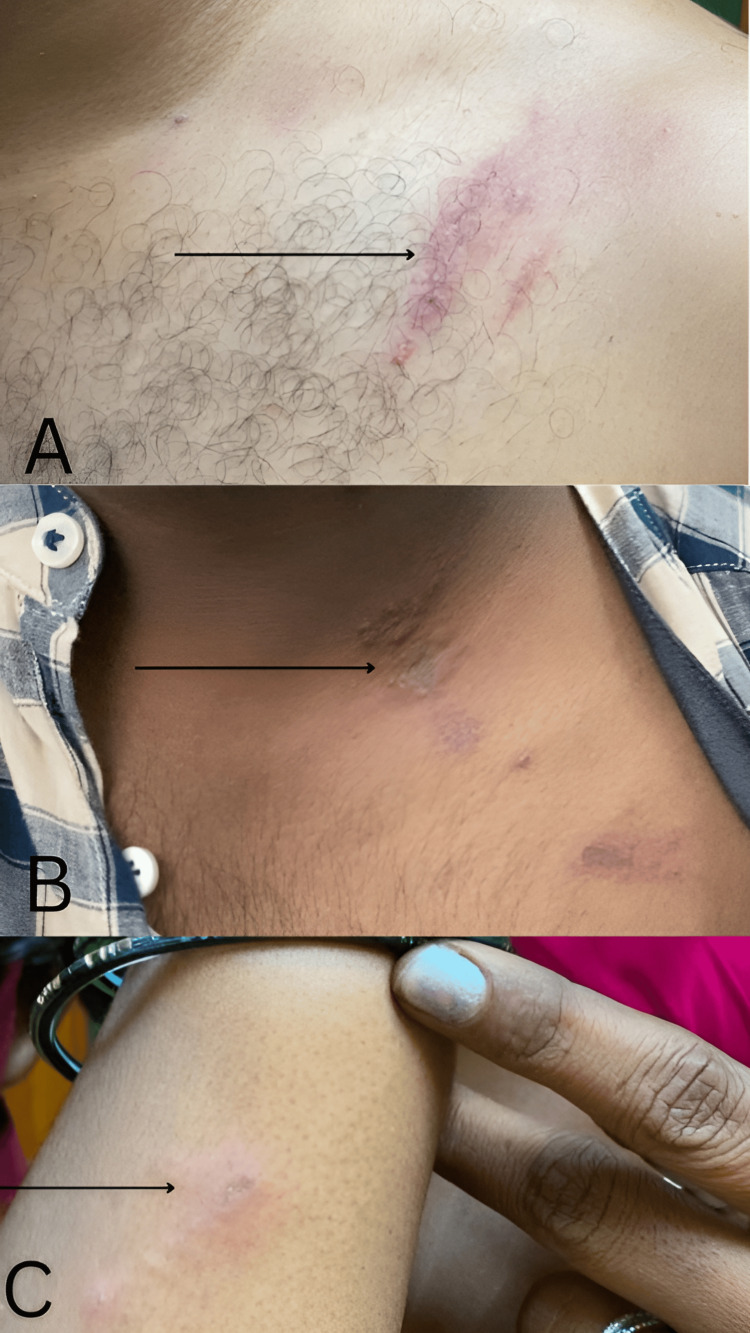
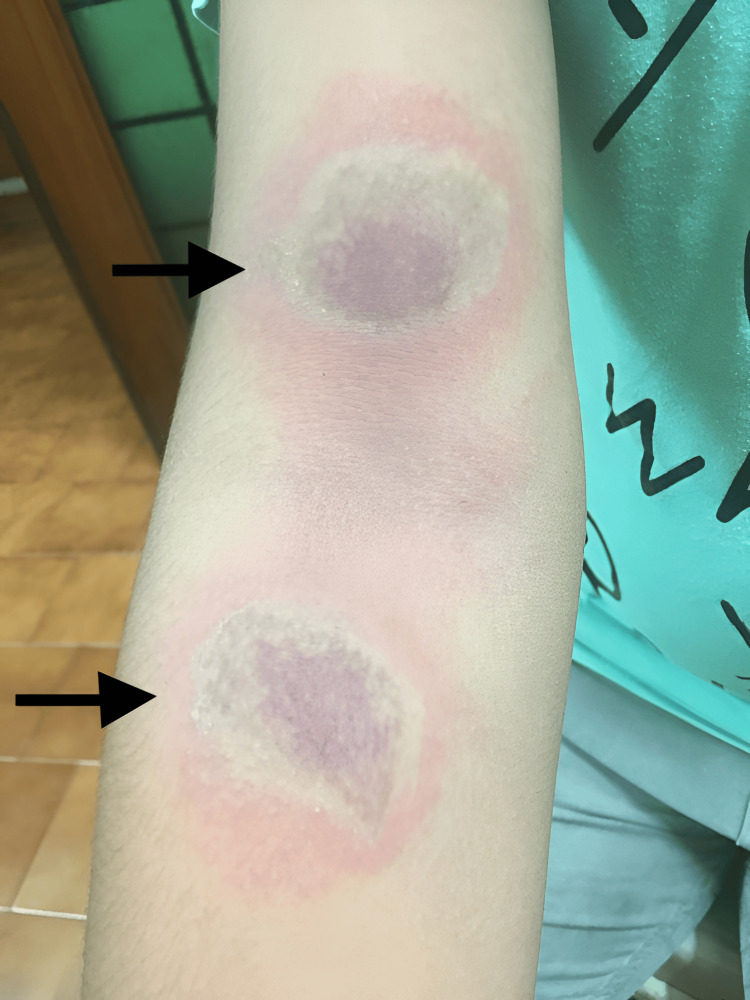
Among the various morphological patterns observed, the predominant pattern was a linear erythematous plaque with vesicles (Figures 1A-1C). This linear pattern of presentation was identified in seven out of 15 patients (46.6%). This was followed by the next common pattern in our study which was erythematous lesions with a central gray area (Figure 2) which was observed in three patients contributing to 20% and kissing lesions (Figure 3) seen in two patients contributing to 13.3% of the study.
Figure 1. Linear presentation of blister beetle dermatitis over the left shoulder (A), left side of the neck (B), and right forearm (C).
Figure 2. Erythematous lesion with central gray area and peripheral vesicles over the right shoulder and lateral chest wall.
Figure 3. Kissing lesion over the right cubital flexural area.
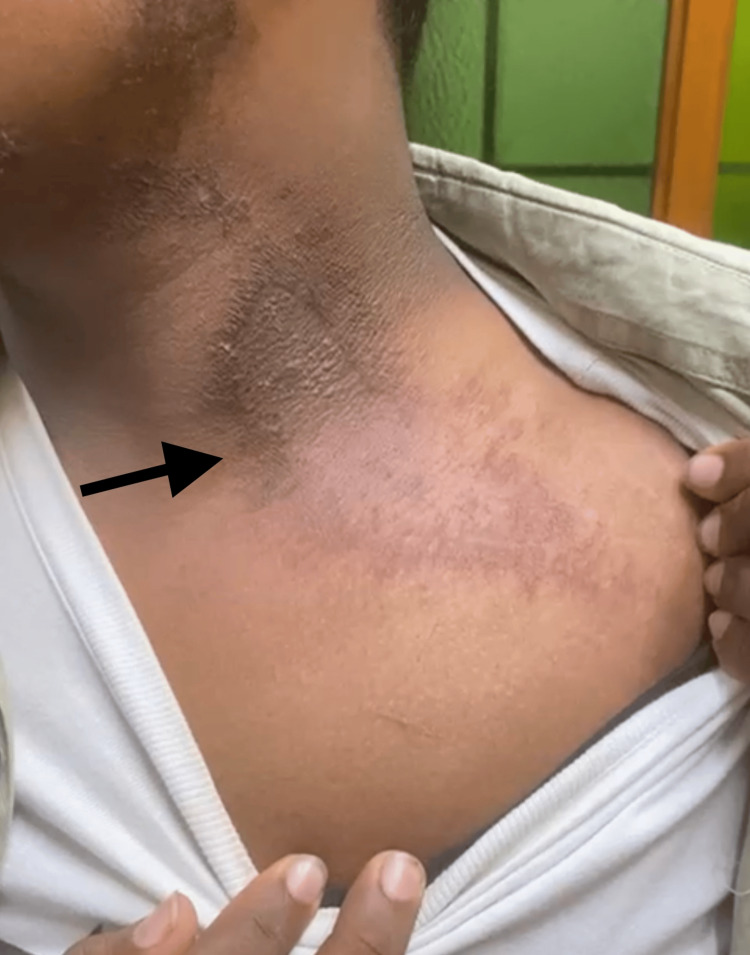
A burnt appearance of the skin (Figure 4) was noted in one patient contributing to 6.6% of the study. Other patterns noted were Nairobi eye appearance (1% in one patient) and post-inflammatory hyperpigmentation (6.6% in one patient), respectively. All the patterns of clinical presentation and associated symptoms at presentation are summarized in Table 2.
Table 2. Symptom presentation and morphological patterns of Paederus dermatitis.
| Variables | Number | Percent |
| Symptoms | ||
| Pain | 12 | 80% |
| Redness | 14 | 81% |
| Blistering | 10 | 66.6% |
| Burning | 14 | 93.3% |
| Severe pain on touch | 14 | 93.3% |
| Morphology | ||
| Linear lesion | 7 | 46.6% |
| Kissing lesion | 2 | 13.3% |
| Erythematous lesion with gray area | 3 | 20% |
| Burnt appearance | 1 | 6.6% |
| Nairobi eye | 1 | 6.6% |
| Post-inflammatory hyperpigmentation | 1 | 6.6% |
Figure 4. Burnt appearance over the left side of the neck .
The average duration of the lesion lasted from two to 10 days in all patients. All lesions were present only on the exposed area of the body with the face and neck as the commonest sites in nine of 15 patients, followed by the trunk and upper limbs in three patients each.
Discussion
Paederus dermatitis, also known as "dermatitis linearis," "rove beetle dermatitis," and "Staphylinidae dermatitis," is caused by beetles of the order Coleoptera, genus Paederus, under subfamilies Meloidae, Oedemeridae, and Staphylinidae. Paederus dermatitis is known to be an entomological model of irritant contact dermatitis [2-5]. Sometimes, Paederus dermatitis is referred to as blister beetle dermatitis. But it should be noted that Paederus dermatitis is caused by beetles of the Staphylinidae family of the order Coleoptera and blister beetle dermatitis is caused by the beetles of Meloidae and Oedemeridae families of the order Coleoptera. Pederin, the toxin responsible for Paederus dermatitis, is produced by endosymbiotic Pseudomonas bacteria within Paederus beetles. Blister beetle dermatitis also known as cantharidin dermatitis is caused by the toxin cantharidin. Non-inflammatory vesicles and bullae characterized it. Cantharidin has a different chemical structure from pederin and induces a less cutaneous violent reaction that occurs within a few hours of exposure [6,7].
Reaction to pederin has a delayed onset, typically occurring 12-48 hours post exposure. Scarring and hyperpigmentation are commonly observed after Paederus dermatitis, whereas dermatitis from cantharidin rarely results in scarring. Paederus dermatitis is characterized by vesicles, bullae, and pustules arising on intensely inflamed skin. Acute dermatitis caused by pederin occurs corresponding to the shape and dimension of the area over which the vesicant chemical was released. Paederus dermatitis is a self-healing condition [6,8-11].
The breakout in the number of cases has been often noticed to occur during or after rainy seasons [3,11-18]. Adults of a few Paederus species are at times very abundant, especially in tropical countries [15]. Paederus beetles, notably Paederus melampus, are associated with dermatitis outbreaks in countries like Sri Lanka and India, with high prevalence in regions of India such as Odisha, West Bengal, Punjab, Rajasthan, and Tamil Nadu and Karnataka. These beetles, typically measuring 7-10 mm in length, inhabit moist environments, feeding on small insects and plant debris. Various species of the genus Paederus, found globally, are primarily nocturnal and are strongly attracted to light. In our study, 14 out of 15 patients reported noticing lesions immediately upon waking from sleep, aligning with the nocturnal activity of the beetle. While they typically do not bite or sting, their hemolymph, when crushed on contact, acts as a potent irritant, causing irritant contact dermatitis [3]. If the beetles are found on the skin, brushing them off, rather than crushing them, avoids producing dermatitis [17].
The predominant symptoms reported were pain, itching, redness, and tenderness in exposed parts of the body. This finding is similar to the other findings reported in other studies, by Kellner and Dettner [10] and Gyeltshen et al. [11]. The majority of the lesions presented were linear erythematous followed by erythematous lesions with gray centers. The mean duration of the skin rash from onset until recovery was 13 days. Our study findings were similar to studies done by Gyeltshen et al. [11].
Most people are unaware of contact with the insect as it usually occurs at night during sleep when the insects are crushed reflexly. Dermatitis caused by Paederus affects individuals of any gender, age, race, or social background, depending on their activities and the presence of insects. The condition is more commonly observed in exposed areas of the skin. The incidence of cases tends to be higher in the last quarter of the year, following the rainy season [3,17]. Symptoms manifest within 24-48 hours after contact and may take a week or more to resolve. Mostly exposed areas of the body are affected. The characteristic linear appearance of this lesion is due to the crushing of the insect and the subsequent smearing of the toxin on the skin. A drip mark is occasionally seen when the toxin has run down the skin producing whiplash dermatitis [12]. These findings in a study by Karthikeyan and Kumar were similar to our study [6].
The lesions are characterized by erythema and edema, often appearing linear and resembling a whiplash. Vesicles typically emerge towards the center of the affected area, frequently progressing to pustules [5,8]. Complications of Paederus dermatitis encompass post-inflammatory hyperpigmentation, secondary infections, and severe exfoliating and ulcerating dermatitis that may necessitate hospitalization [5]. Additionally, conjunctivitis caused by pederin exposure is sometimes mistaken for preseptal cellulitis, an ocular infection [18-22].
Clinical presentations vary based on morphological types. Dermatitis linearis is the most common pattern and occurs in any exposed site. The characteristic presentation is erythematous vesicles and pustules with edema arranged in a linear pattern resembling a whiplash [6]. The localized pustular dermatosis pattern mimics irritant contact dermatitis, displaying grouped pustules at the insect-crushed site [6,14,16]. The other clinical pattern is an erythematous patch with an irregular border, which develops an increasingly gray, necrotic center, appearing similar to a burn. The pathognomonic lesions of Paederus dermatitis are kissing lesion patterns. This develops when damaged skin surfaces come into contact with previously unaffected skin, such as in the flexures of the elbow or adjacent surfaces of the thighs [6,14,17]. The uncommon but still reported variants of Paederus dermatitis include (a) extensive skin involvement with systemic symptoms like fever and vomiting, (b) genital lesions that arise from passive toxin transfer from other exposed areas of the skin, (c) Nairobi eye variant which is associated with ocular toxin involvement which may present as unilateral periorbital dermatitis with keratoconjunctivitis and the name originating from Zaire in 1915, (d) atypical presentation of Paederus dermatitis which presents as diffuse erythematous and desquamative lesions primarily on the upper body and face, (e) erythrodermic presentation involving more than 90% of body surface area with erythema and scaling, and (f) systemic involvement of the lung. Lymph nodes can also be seen very rarely in Paederus dermatitis [6,14,16,17,22-28]. The atypicality in clinical presentation can be attributed to the following factors: contact with specific Paederus species, repeated exposure in endemic areas, underlying immune disorders like atopy, immunological phenomena, and impact of infested water sources [29]. Systemic involvements requiring admissions are also reported in a study by Padhi et al. Vasculitis-like Paederus presentation, erythema multiforme-like presentation, and lung involvement have also been documented [2-4,30].
Paederus dermatitis is often confused with many dermatological diseases owing to the clinical similarities like herpes zoster and herpes simplex, bullous impetigo, pustular psoriasis, Sneddon-Wilkinson disease, fungal infections, and allergic reactions [12,16,22].
Considering the analysis of our case study and review of the literature on various Paederus dermatitis cases, we can clearly understand that the diagnosis of this dermatitis is strongly based on complete history-taking and careful clinical examination of the lesions. We have proposed a diagnostic aid system to confirm the diagnosis of Paederus dermatitis. The following data from history which includes (i) history of contact with any insect, (ii) onset of lesions noticed after sleep or travel, (iii) patient's locality, especially if surrounding a field or from an endemic region of Paederus dermatitis, (iv) objective criteria for diagnosis, (v) sudden onset of lesions, and (vi) presence of severe pain and burning sensation can be elicited to make a diagnosis. The presence of any of the morphological patterns like the most commonly seen linear or streaky pattern of dermatitis with or without kissing lesions and erythematous patches with central gray necrotic burn-like lesions can be noted. The correlation of data from history and clinical findings will lead to a most probable diagnosis of Paederus dermatitis. Since any dermatoses with vesiculobullous lesions can be put as a differential to Paederus dermatitis, a diagnostic checklist system as mentioned in our study can be useful in the appropriate diagnosis of the same.
Limitations of the study
The smaller sample size was the limitation of the study.
Conclusions
Paederus dermatitis is an acute condition caused by beetles mostly in tropical areas. Learning to recognize Paederus beetles and avoiding handling or crushing by blowing off these insects from the skin will help decrease these eruptions. Closing the doors and windows and turning off the light sources in sleeping areas can be practiced to help reduce contact with these insects. Clinical knowledge of various morphological patterns of Paederus dermatitis and correlating the salient points from the patient's history will enable the physician to flinch the correct diagnosis, not only improving the patient's treatment outcome but also preventing misdiagnosis.
The authors have declared that no competing interests exist.
Author Contributions
Concept and design: Bhanupriya Tamilselvan, Srikanth Shanmugam, Pragasam Shakthi
Acquisition, analysis, or interpretation of data: Bhanupriya Tamilselvan, Srikanth Shanmugam, Pragasam Shakthi
Drafting of the manuscript: Bhanupriya Tamilselvan, Srikanth Shanmugam, Pragasam Shakthi
Critical review of the manuscript for important intellectual content: Bhanupriya Tamilselvan, Srikanth Shanmugam, Pragasam Shakthi
Supervision: Bhanupriya Tamilselvan, Srikanth Shanmugam, Pragasam Shakthi
Human Ethics
Consent was obtained or waived by all participants in this study. Institutional Human Ethics Committee of Mahatma Gandhi Medical College and Research Institute issued approval 314
Animal Ethics
Animal subjects: All authors have confirmed that this study did not involve animal subjects or tissue.
References
- 1.Blister beetles and the ten plagues. Norton SA, Lyons C. Lancet. 2002;359:1950. doi: 10.1016/S0140-6736(02)08759-7. [DOI] [PubMed] [Google Scholar]
- 2.Paederus dermatitis: an outbreak, increasing incidence or changing seasonal pattern? Coondoo A, Nandy J. Indian J Dermatol. 2013;58:410. doi: 10.4103/0019-5154.117357. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Clinicoepidemiological profile of 590 cases of beetle dermatitis in western Orissa. Padhi T, Mohanty P, Jena S, Sirka CS, Mishra S. Indian J Dermatol Venereol Leprol. 2007;73:333–335. doi: 10.4103/0378-6323.35735. [DOI] [PubMed] [Google Scholar]
- 4.Erythema multiforme associated with blister beetle dermatitis. Inanir I. Contact Dermatitis. 2002;46:175. doi: 10.1034/j.1600-0536.2002.460310.x. [DOI] [PubMed] [Google Scholar]
- 5.Comparison of the efficacy of fluocinolone cream, triclocarban soap and betamethasone lotion with placebo in the treatment of Paederus dermatitis. Davoudi SM, Rostami P, Emadi SN, Sadr B, Khabiri E. https://www.iranjd.ir/article_101164.html Iran J Dermatol. 2006;9:217–220. [Google Scholar]
- 6.Paederus dermatitis. Karthikeyan K, Kumar A. Indian J Dermatol Venereol Leprol. 2017;83:424–431. doi: 10.4103/0378-6323.198441. [DOI] [PubMed] [Google Scholar]
- 7.Treatment outcome of Paederus dermatitis due to rove beetles (Coleoptera: Staphylinidae) on guinea pigs. Fakoorziba MR, Eghbal F, Azizi K, Moemenbellah-Fard MD. https://pubmed.ncbi.nlm.nih.gov/22041764/ Trop Biomed. 2011;28:418–424. [PubMed] [Google Scholar]
- 8.Paederus dermatitis: a case series. Srihari S, Kombettu AP, Rudrappa KG, Betkerur J. Indian Dermatol Online J. 2017;8:361–364. doi: 10.4103/idoj.IDOJ_238_16. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Outbreak of dermatitis linearis caused by Paederus ilsae and Paederus iliensis (Coleoptera: Staphylinidae) at a military base in Iraq. Davidson SA, Norton SA, Carder MC, Debboun M. https://pubmed.ncbi.nlm.nih.gov/20084733/ US Army Med Dep J. 2009:6–15. [PubMed] [Google Scholar]
- 10.Allocation of pederin during lifetime of Paederus rove beetles (Coleoptera: Staphylinidae): evidence for polymorphism of hemolymph toxin. Kellner RL, Dettner K. J Chem Ecol. 1995;21:1719–1733. doi: 10.1007/BF02033672. [DOI] [PubMed] [Google Scholar]
- 11.Clinical description and treatment outcomes of Paederus dermatitis in Phuentsholing, Bhutan in 2021: a cross-sectional study. Gyeltshen K, Sangye N, Tenzin KC, Dorji T. Skin Health Dis. 2023;3:0. doi: 10.1002/ski2.223. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Paederus dermatitis--a mimic. George AO. Contact Dermatitis. 1993;29:212–213. doi: 10.1111/j.1600-0536.1993.tb03543.x. [DOI] [PubMed] [Google Scholar]
- 13.Literature review of the causes, treatment, and prevention of dermatitis linearis. Beaulieu BA, Irish SR. J Travel Med. 2016;23:0. doi: 10.1093/jtm/taw032. [DOI] [PubMed] [Google Scholar]
- 14.Evacuation of an Aboriginal community in response to an outbreak of blistering dermatitis induced by a beetle (Paederus australis) Todd RE, Guthridge SL, Montgomery BL. Med J Aust. 1996;164:238–240. doi: 10.5694/j.1326-5377.1996.tb94150.x. [DOI] [PubMed] [Google Scholar]
- 15.Dermatitis linearis: vesicating dermatosis caused by Paederus species (Coleoptera: Staphylinidae). Case series and review. Cressey BD, Paniz-Mondolfi AE, Rodríguez-Morales AJ, Ayala JM, De Ascenção Da Silva AA. Wilderness Environ Med. 2013;24:124–131. doi: 10.1016/j.wem.2012.11.005. [DOI] [PubMed] [Google Scholar]
- 16.Clinical and epidemiological study of Paederus dermatitis in Manipal, India. Taneja A, Nayak UK S, Shenoi SD. http:////www.jpad.com.pk/index.php/jpad/article/view/295 J Pak Assoc Dermatol. 2016;23:133–138. [Google Scholar]
- 17.Nairobi fly (Paederus) dermatitis in South Sudan: a case report. Iserson KV, Walton EK. Wilderness Environ Med. 2012;23:251–254. doi: 10.1016/j.wem.2012.03.005. [DOI] [PubMed] [Google Scholar]
- 18.Capinera JL. Encyclopedia of Entomology. Florida, USA: Springer Science and Business Media. Florida (USA): Springer Science and Business Media; 2008. Encyclopedia of entomology. [Google Scholar]
- 19.Paederus dermatitis. Singh G, Yousuf Ali S. Indian J Dermatol Venereol Leprol. 2007;73:13–15. doi: 10.4103/0378-6323.30644. [DOI] [PubMed] [Google Scholar]
- 20.Whiplash rove beetle dermatitis in central Queensland. Banney LA, Wood DJ, Francis GD. Australas J Dermatol. 2000;41:162–167. doi: 10.1046/j.1440-0960.2000.00421.x. [DOI] [PubMed] [Google Scholar]
- 21.A contribution to the rove beetles (Coleoptera: Staphylinoidea: Staphylinidae) of Iranian rice fields and surrounding grasslands. Ghahari H, Anlaş S, Sakenin H, Ostovan H, Tabari M. https://www.google.com/url?sa=t&rct=j&q=&esrc=s&source=web&cd=&ved=2ahUKEwiRp4ORz6eEAxVYk1YBHWGaC40QFnoECB4QAQ&url=https%3A%2F%2Fwww.zobodat.at%2Fpdf%2FLBB_0041_2_1959-1968.pdf&usg=AOvVaw3we69I_tuxOSeZ1jJGQCuO&opi=89978449 Linzer Biol Beitr. 2009;41:1959–1968. [Google Scholar]
- 22.Blister beetle periorbital dermatitis and keratoconjunctivitis in Tanzania. Poole TR. Eye (Lond) 1998;12:883–885. doi: 10.1038/eye.1998.223. [DOI] [PubMed] [Google Scholar]
- 23.Paederus dermatitis in Egypt: a clinicopathological and ultrastructural study. Assaf M, Nofal E, Nofal A, Assar O, Azmy A. J Eur Acad Dermatol Venereol. 2010;24:1197–1201. doi: 10.1111/j.1468-3083.2010.03621.x. [DOI] [PubMed] [Google Scholar]
- 24.Staphylinid blister beetle dermatitis. Brazzelli V, Martinoli S, Prestinari F, Rosso R, Borroni G. Contact Dermatitis. 2002;46:183–184. doi: 10.1034/j.1600-0536.2002.460315.x. [DOI] [PubMed] [Google Scholar]
- 25.Paederus dermatitis: an easy diagnosable but misdiagnosed eruption. Gelmetti C, Grimalt R. Eur J Pediatr. 1993;152:6–8. doi: 10.1007/BF02072506. [DOI] [PubMed] [Google Scholar]
- 26.Periocular Paederus dermatitis mimicking preseptal cellulitis. Canan H, Altan-Yaycioglu R, Durdu M. Can J Ophthalmol. 2013;48:121–125. doi: 10.1016/j.jcjo.2012.10.004. [DOI] [PubMed] [Google Scholar]
- 27.Dermatitis due to Paederus colombinus: report of an epidemic outbreak of 68 cases in the province of Darien, Panama. Cáceres L, Suarez JA, Jackman C, et al. Cureus. 2017;9:0. doi: 10.7759/cureus.1158. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Paederus dermatitis in northern Iran: a report of 156 cases. Zargari O, Kimyai-Asadi A, Fathalikhani F, Panahi M. Int J Dermatol. 2003;42:608–612. doi: 10.1046/j.1365-4362.2003.01771.x. [DOI] [PubMed] [Google Scholar]
- 29.Paederus dermatitis in Sierra Leone. Qadir SN, Raza N, Rahman SB. https://pubmed.ncbi.nlm.nih.gov/17459295/ Dermatol Online J. 2006;12:9. [PubMed] [Google Scholar]
- 30.Quantitative characterization of cantharidin in the false blister beetle, Oedemera podagrariae ventralis, of the southern slopes of Mount Elborz, Iran. Abtahi SM, Nikbakhtzadeh MR, Vatandoost H, Mehdinia A, Rahimi-Foroshani A, Shayeghi M. J Insect Sci. 2012;12:152. doi: 10.1673/031.012.15201. [DOI] [PMC free article] [PubMed] [Google Scholar]