Abstract
Study design
Systematic review.
Objective
Erector spinae plane block (ESPB) is growing in popularity over the recent past as an adjuvant modality in multimodal analgesic management following lumbar spine surgery (LSS). The current updated meta-analysis was performed to analyze the efficacy of ESPB for postoperative analgesia in patients undergoing LSS.
Methods
We conducted independent and duplicate electronic database searches including PubMed, Embase and Cochrane Library till June 2023 for randomized controlled trials (RCTs) analyzing the efficacy of bilateral ESPB for postoperative pain relief in lumbar spine surgeries. Post-operative pain scores, total analgesic consumption, first analgesic requirement time, length of stay and complications were the outcomes evaluated. Statistical analysis was performed using STATA 17 software.
Results
32 RCTs including 1464 patients (ESPB/Control = 1077/1069) were included in the analysis. There was a significant pain relief in ESPB group, as compared to placebo across all timelines such as during immediate post-operative period (p < 0.001), 4 h (p < 0.001), 8 h (p < 0.001), 12 h (p < 0.001), 24 h (p = 0.001) post-surgery. Similarly, ESPB group showed a significant reduction in analgesic requirement at 8 h (p < 0.001), 12 h (p = 0.001), and 24 h (p < 0.001). However, no difference was noted in the first analgesic requirement time, time to ambulate or total length of stay in the hospital. ESPB demonstrated significantly improved overall satisfaction score for the analgesic management (p < 0.001), reduced intensive care stay (p < 0.05) with significantly reduced post-operative nausea and vomiting (p < 0.001) compared to controls.
Conclusion
ESPB offers prolonged post-operative pain relief compared to controls, thereby reducing the need for opioid consumption and its related complications.
Keywords: Erector spinae plane block, Lumbar spine surgery, Systematic review, Postoperative pain, Regional anaesthesia
1. Introduction
Spine surgeries are usually associated with severe post-operative pain; and a recent large-scale, multi-centered study ranked single- or two-level spinal fusion and long-segment thoracic fusion as the second- and third-most painful surgical procedures among 179 reviewed surgical interventions.1,2 Failure to achieve the good pain relief may result in various deleterious complications like delayed ambulation, thromboembolic complications and prolonged hospital stays, which not only add to the suffering of the patient but also to the cost of the procedure.3 In this context, an approach involving multimodal analgesic (MMA) therapy has been encouraged, so as to meliorate post-operative pain relief and facilitate early rehabilitation.4
The use of non-opioid and non-pharmacological alternatives in such multimodal therapies has gradually mitigated the requirement of prolonged opioid therapies during the post-operative period.5 In addition, diverse routes of administration of local anesthetic (LA) agents have been studied including local wound infiltration, and regional blocks such as spinal, epidural and paravertebral injections.6 Since dorsal rami innervate all the pain generators following lumbar spine surgery (LSS), regional anesthetic techniques like Thoraco Lumbar Interfascial Plane (TLIP) Block, Quadratus Lumborum (QL) block, Mid‐point Transverse process to Pleura (MTP) block, and Erector Spinae Plane Block (ESPB) have been developed to target them locally.7, 8, 9, 10 Among these regional blocks, lumbar ESPB has been widely studied.11 Despite such extensive research on this subject, there are significant lacunae in the existing literature such as inconsistent reporting of clinical efficacy, unpredictable injectate spread, different surgical procedures for which the block was administered, different regions of block (thoracic versus lumbar), inconsistencies in the MMA administration, different “Enhanced Recovery After Surgery” (ERAS) protocols, short-term pain assessment with paucity of data on chronic pain or quality of life; and relative deficiency of high-quality randomised controlled trials on this subject.11 Hence, the need for a systematic review/meta-analysis of the available prospective studies to provide conclusive evidence on the role and practice recommendations on EPSB in spine surgery can not be understated.
In this context, the current metaanalysis was performed to comprehensively evaluate the evidence in the existing literature regarding the efficacy of bilateral ESPB for postoperative analgesia in LSS. To the best of our knowledge, this is the largest meta-analysis published on this topic heretofore.
2. Materials & methods
This meta-analysis was performed in compliance with the recommendations of the Back Review Group of Cochrane Collaboration4 and presented in adherence to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement.12 Being a systematic review, patient consent or institutional review board approval was not sought for the conduction of the study.
2.1. Search strategy
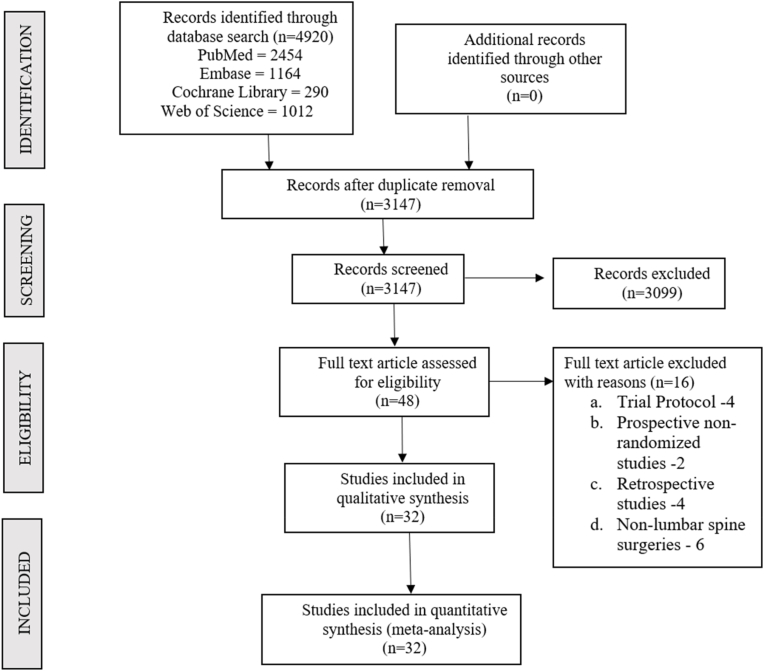
Two reviewers were involved in making an independent electronic literature search for RCTs evaluating the efficacy of bilateral ESPB for spine surgeries. The following databases were searched to identify the relevant studies: PubMed, Embase and the Cochrane Library up to June 2023. We did not apply any date or language restrictions to the search query. We used the following keywords in the database search: “Erector Spinae Plane Block”, “ESP Block”, “Erector Spinae block”. We also went through the references of the articles shortlisted from preliminary screening to identify studies missed in the preliminary search. According to the inclusion and exclusion criteria, studies were selected to be included for meta-analysis. In case of discrepancy in selecting the articles between the authors, it was settled by discussion until a consensus was reached. The sequence of selecting the studies for the analysis was given by the PRISMA flow diagram given in Fig. 1.
Fig. 1.
PRISMA flow diagram of the included studies.
2.2. Inclusion criteria
We included studies for analysis if they satisfied the following PICOS criteria:
Population: Patients undergoing surgery for lumbar spinal disease.
Intervention: ESPB.
Comparator: Placebo, other regional blocks.
Outcomes: Post-operative pain scores, number of patients requiring rescue analgesics, total analgesic consumption, complication rate.
Study Design: Randomized controlled trials (RCTs).
2.3. Exclusion criteria
Studies were excluded from selection if they had the following characteristics:
-
1.
Studies involving patients with acute spinal trauma
-
2.
Studies involving patients with a history of chronic pain and opioid dependence
-
3.
Studies involving erector spinae block for procedures other than lumbar spine surgeries
-
4.
Anatomical and cadaveric studies involving erector spinae block
-
5.
Studies without a comparator group such as case series and case reports
2.4. Data extraction
Two reviewers retrieved independently relevant data from articles included for analysis. Following data were extracted:
1Study characteristics: Year of publication, authors, country, number of patients enrolled
-
2.
Baseline characteristics: Mean age, gender proportions, body mass index, American Society of Anaesthesiologist (ASA) Grading, duration of surgery
-
3.
Primary Outcomes: Post-operative pain scores, total analgesic consumption
-
4.
Secondary Outcomes: First analgesic requirement time, time to ambulate, intensive care period, length of stay in the hospital
-
5.
Other Outcomes: Satisfaction score, complications
If any data was found missing from the included study, we contacted the corresponding authors of the study.
2.5. Risk of bias and quality assessment
Two reviewers independently assessed the methodological quality of the included studies with the help of Cochrane Collaboration's RoB 2 tool for RCTs, with five domains of bias assessment included in them.13
2.6. Statistical analysis
We performed the meta-analysis of the pooled data in Stata (17, Stata Corp LLC). In case of dichotomous variables, we utilised odds ratio (OR) with 95% Confidence Interval (CI); and for continuous variables, weighted mean difference (WMD) with 95% CI was utilised. We evaluated the heterogeneity of the pooled data using I2 statistics.14 If I2<50% and p > 0.1, fixed-effects model was employed in meta-analysis; and if I2>50% and p < 0.1, random-effects model was utilised. Publication bias was evaluated with funnel plots and egger regression test. Heterogeneity was explored with galbraith plot. Further, subgroup and sensitivity analyses were performed to explore into the cause heterogeneity. A p-value less than 0.05 was considered significant.
3. Results
3.1. Search results
Our search on electronic database yielded 4920 articles, from which 3147 articles were retrieved after initial screening and removal of duplicates. Screening of the titles and abstracts were then performed, resulting in the exclusion of 3099 manuscripts. Among the remaining 48 articles, 16 were excluded after full-text review. Finally, 32 RCTs11,15, 16, 17, 18, 19, 20, 21, 22, 23, 24, 25, 26, 27, 28, 29, 30, 31, 32, 33, 34, 35, 36, 37, 38, 39, 40, 41, 42, 43, 44, 45 involving a total of 2146 patients (ESPB group/Control group = 1077/1069) were included in our meta-analysis. PRISMA flow diagram of the study selection is presented in Fig. 1. The general characteristics of the RCTs included in our analysis are presented in Table 1; and the ESPB protocols of the included studies are depicted in Table 2. The control group included placebo treatment with either sham injection with saline or no treatment.
Table 1.
General characteristics of the included studies.
| Study No |
Author |
Year |
Design |
Total Cases |
Total Controls |
Age |
Age |
M/F |
M/F |
BMI |
BMI |
ASA I/II/III |
Duration of Surgery |
||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Case | Control | Case | Control | Case | Control | Case | Control | Case | Control | ||||||
| 1 | AM Yayik15 | 2019 | RCT | 30 | 30 | 50.53 ± 8.5 | 54.30 ± 8.56 | 17/13 | 19/11 | 30.11 ± 1.6 | 29.41 ± 1.2 | 12/10/8 | 13/12/5 | 91.5 ± 32.3 | 88.83 ± 19.9 |
| 2 | S Singh16 | 2019 | RCT | 20 | 20 | 35.40 ± 8.3 | 34.90 ± 10.1 | 17/3 | 18/2 | 25.1 ± 1.8 | 24.7 ± 1.6 | 12/5/3 | 10/5/5 | 149.3 ± 6.3 | 145.2 ± 8 |
| 3 | Ghamry17 | 2019 | RCT | 30 | 30 | 43.9 ± 9.8 | 42.8 ± 10.7 | 17/13 | 16/14 | NA | NA | 15/15/0 | 17/13/0 | 175.5 ± 13.6 | 179.4 ± 16.8 |
| 4 | Eskin 18 | 2020 | RCT | 40 | 40 | 58.0 ± 5.2 | 57.8 ± 5.2 | 16/24 | 17/23 | 25.6 ± 3.1 | 25.5 ± 2.2 | 5/28/7 | 3/30/7 | NA | NA |
| 5 | Zhang19 | 2020 | RCT | 30 | 30 | 64 ± 9.4 | 64 ± 10.3 | 13/17 | 8/22 | NA | NA | 6/22/2 | 7/19/4 | NA | NA |
| 6 | Siam20 | 2020 | RCT | 15 | 15 | 40.2 ± 10 | 42 ± 11.09 | 11/4 | 9/6 | 26.73 ± 1.91 | 26.97 ± 1.53 | NA | NA | NA | NA |
| 7 | Ciftci21 | 2020 | RCT | 30 | 30 | 46.1 ± 10.1 | 44.1 ± 8.3 | 16/14 | 15/15 | NA | NA | 17/13/0 | 18/12/0 | 71.7 ± 16.7 | 76.8 ± 20.3 |
| 8 | Wang22 | 2021 | RCT | 102 | 102 | 53.78 ± 10.16 | 55.69 ± 12.01 | 44/58 | 51/51 | 24 ± 2.71 | 24.28 ± 11.26 | 21/81/0 | 11/90/1 | 127.29 ± 30.45 | 130.92 ± 26.91 |
| 9 | Abd Ellatif23 | 2021 | RCT | 25 | 25 | 44.7 ± 11.2 | 44.1 ± 9.8 | 17/8 | 17/8 | 24.9 ± 2.38 | 24.2 ± 2.03 | 0/19/6 | 0/15/10 | 142.8 ± 6.7 | 140.8 ± 10.5 |
| 10 | Zhang24 | 2021 | RCT | 30 | 30 | 60.0 ± 9.6 | 59.5 ± 11.5 | 6/24 | 9/21 | 25.4 ± 3.2 | 24.7 ± 2.9 | 7/23/0 | 8/22/0 | 152.6 ± 38.7 | 143.5 ± 33.3 |
| 11 | Finnerty25 | 2021 | RCT | 30 | 30 | 59.2 ± 16.5 | 59.8 ± 15.5 | 12/18 | 17/13 | 27.2 ± 4.1 | 28.4 ± 5.4 | 5/23/2 | 7/22/1 | NA | NA |
| 12 | Goel26 | 2021 | RCT | 51 | 50 | 52.42 ± 13.05 | 52.16 ± 12.05 | 21/30 | 21/29 | 25.69 ± 3.99 | 26.33 ± 2.78 | 24/27/0 | 20/30/0 | 131.27 ± 11.26 | 132.92 ± 12.10 |
| 13 | Yu27 | 2021 | RCT | 40 | 40 | 55.50 ± 11.45 | 57.13 ± 10.62 | 19/21 | 17/23 | 21 ± 3 | 22 ± 2 | 15/25/0 | 14/26/0 | 1.37 ± 0.30 | 1.41 ± 0.30 |
| 14 | Zhu28 | 2021 | RCT | 20 | 20 | 59 ± 2 | 60 ± 2 | 7/13 | 8/12 | 25.3 ± 0.7 | 24.4 ± 0.5 | 4/16/0 | 3/17/0 | 128 ± 6 | 123 ± 5 |
| 15 | Yesiltas29 | 2021 | RCT | 28 | 28 | 61.0 ± 9.4 | 60.1 ± 11.7 | 11/17 | 7/21 | 28.1 ± 4.35 | 28.7 ± 3.6 | NA | NA | 262.6 ± 80.9 | 245.0 ± 97 |
| 16 | Jin 30 | 2021 | RCT | 35 | 35 | 56.73 ± 8.69 | 56.09 ± 11.37 | 12/18 | 15/17 | 23.88 ± 5.27 | 24.31 ± 4.86 | 6/19/5 | 9/13/10 | 211.50 ± 51.14 | 215.97 ± 59.629 |
| 17 | Wahdan31 | 2021 | RCT | 70 | 70 | 48.34 ± 11.19 | 46.4 ± 9.11 | 36/34 | 38/32 | NA | NA | NA | NA | 177.9 ± 56.43 | 184.5 ± 47.8 |
| 18 | Zhang32 | 2021 | RCT | 30 | 30 | 61 ± 12 | 64 ± 10 | 13/17 | 8/21 | NA | NA | 11/16/3 | 6/17/6 | NA | NA |
| 19 | Asar33 | 2022 | RCT | 35 | 35 | 61.86 ± 9.46 | 58.49 ± 8.77 | 6/29 | 11/24 | 31.25 ± 5.74 | 31.02 ± 5.07 | 5/22/8 | 6/19/10 | 213.00 ± 32.90 | 231.43 ± 32.78 |
| 20 | Lin 34 | 2022 | RCT | 42 | 41 | 65 ± 9.4 | 65 ± 7.2 | 12/30 | 18/23 | 23.4 ± 2.3 | 24.2 ± 1.9 | 1/23/18 | 2/27/12/ | 168 ± 21.2 | 175 ± 15.3 |
| 21 | Yörükoğlu35 | 2021 | RCT | 28 | 26 | 49 ± 11.3 | 47.6 ± 10.8 | NA | NA | NA | NA | 13/15/0 | 9/17/0 | 140.3 ± 31 | 135.3 ± 30.3 |
| 22 | Avis11 | 2022 | RCT | 25 | 24 | 67 ± 4.3 | 67 ± 4.1 | 19/6 | 18/6 | 28 ± 2.3 | 26 ± 2.3 | 4/18/3 | 3/18/3 | 112 ± 23.2 | 124 ± 31.2 |
| 23 | Vergari36 | 2022 | RCT | 30 | 30 | 57 ± 11 | 58 ± 10 | 17/13 | 14/16 | 24.7 ± 2.9 | 25.5 ± 3.6 | NA | NA | 216 ± 63 | 221 ± 47 |
| 24 | Abdelhamid37 | 2022 | RCT | 34 | 33 | 36.59 ± 11.92 | 37.06 ± 11.59 | 12/22 | 15/18 | 28.21 ± 2.85 | 27.29 ± 2.67 | NA | NA | 124.56 ± 12.57 | 120.00 ± 12.93 |
| 25 | Tantri38 | 2023 | RCT | 20 | 20 | 42.05 ± 15.75 | 47.90 ± 13.4 | 12/8 | 11/9 | 23.70 ± 4.12 | 23.0 ± 2.60 | 1/11/8 | 1/9/10 | 145 | 180 |
| 26 | Wittayapairoj39 | 2023 | RCT | 31 | 31 | 56.6 ± 11.8 | 54.7 ± 13.2 | 11/20 | 13/18 | 25.7 ± 3.5 | 25.9 ± 3.6 | 7/24/0 | 9/21/1 | 145.5 ± 71.2 | 132.6 ± 71.3 |
| 27 | Holas40 | 2023 | RCT | 28 | 28 | 52.68 ± 10.31 | 54.68 ± 13.56 | 17/11 | 16/12 | 26.48 ± 4.62 | 26.52 ± 4.41 | NA | NA | NA | NA |
| 28 | Jie41 | 2023 | RCT | 32 | 30 | 68.4 ± 5.6 | 69.4 ± 5.6 | 18/14 | 14/16 | 26.4 ± 1.8 | 25.7 ± 2.2 | 20/12/0 | 19/11/0 | 190 ± 23 | 192 ± 19 |
| 29 | Mohamoud42 | 2023 | RCT | 41 | 41 | 40.8 ± 12 | 45.1 ± 8.4 | 22/19 | 21/20 | 24.4 ± 2.7 | 25.2 ± 2.9 | 26/15 | 30/11 | 129.3 ± 9.1 | 129 ± 26 |
| 30 | Bellantonio43 | 2023 | RCT | 15 | 15 | 54.6 ± 16.8 | 60.4 ± 11.4 | 7/8 | 8/7 | 26.4 ± 5.7 | 27.5 ± 3.7 | 2/9/4 | 1/7/7 | NA | NA |
| 31 | Taşkaldıran44 | 2023 | RCT | 30 | 30 | 51.4 ± 13.05 | 53.3 ± 9.9 | 15/15 | 16/14 | 25.9 ± 2.64 | 25.4 ± 1.84 | NA | NA | 64.6 ± 15.75 | 69.8 ± 12.69 |
| 32 | Kumar45 | 2023 | RCT | 30 | 30 | 43.4 ± 15.1 | 39.1 ± 14.4 | 15/15 | 14/16 | 20.4 ± 1.9 | 20.2 ± 1.9 | 20/10 | 18/12 | 170.3 ± 42 | 190.8 ± 45 |
ASA Grading – American Society of Anaesthesiologist Grading; BMI – Body Mass Index; NA - Not Available; RCT- Randomised Controlled Trial.
Table 2.
ESPB protocols of included studies.
| Study No | Author | Local Anaesthetic | Concentration | Volume | Control Intervention |
|---|---|---|---|---|---|
| 1 | AM Yayik15 | Bupivacaine | 0.25% | 20 ml | No intervention |
| 2 | S Singh16 | Bupivacaine | 0.50% | 20 ml | No intervention |
| 3 | Ghamry17 | Bupivacaine | 0.25% | 20 ml | No intervention |
| 4 | Eskin 18 | Bupivacaine | 0.25% | 20 ml | MTP block with 20 ml of 0.25% Bupivacaine |
| 5 | Zhang19 | Ropivacaine | 0.30% | 25 ml | No intervention |
| 6 | Siam20 | Bupivacaine | 0.25% | 20 ml | MMA(ketorolac 0.75 mg/kg and paracetamol 10 mg/kg) |
| 7 | Ciftci21 | Bupivacaine | 0.25% | 20 ml | Modified TLIP block with 40 ml of 0.25% Bupivacaine |
| 8 | Wang22 | Ropivacaine | 0.38% | 30 ml | TLIP block with 30 ml of 0.375% Ropivacaine |
| 9 | Abd Ellatif23 | Bupivacaine | 0.25% | 0.3–0.4 ml/kg | QLB with 0.3–0.4 ml/kg of 0.25% Bupivacaine |
| 10 | Zhang24 | Ropivacaine | 0.40% | 20 ml | Sham block with 1% lidocaine |
| 11 | Finnerty25 | Levobupivacaine | 0.25% | 20 ml | No intervention |
| 12 | Goel26 | Bupivacaine | 0.25% | 20 ml | No intervention |
| 13 | Yu27 | Bupivacaine | 0.25% | 30 ml | No intervention |
| 14 | Zhu28 | Ropivacaine | 0.38% | 30 ml | No intervention |
| 15 | Yesiltas29 | Bupivacaine & Lidocaine | 0.25% | Bupicavaine & Lidocaine | Placebo with Normal saline |
| 16 | Jin 30 | Ropivacaine | 0.38% | 20 ml | No intervention |
| 17 | Wahdan31 | Levobupivacaine | 0.25% | 20 ml | Placebo with Normal saline |
| 18 | Zhang32 | Ropivacaine | 0.30% | 25 ml | Placebo with Normal saline |
| 19 | Asar33 | Bupivacaine & Lidocaine | 0.5% bupivacaine & 2% lidocaine | 10 ml Bupicavaine & 5 ml Lidocaine | No Intervention |
| 20 | Lin34 | Ropivacaine | 0.38% | 20 ml | No Intervention |
| 21 | Yörükoğlu35 | Bupivacaine | 0.25% | 20 ml | Placebo with normal saline |
| 22 | Avis11 | Ropivacaine | 3.75 mg/ml | 40 ml | Placebo with normal saline |
| 23 | Vergari36 | Ropivacaine | 0.38% | 20 ml | Wound infiltration with 40 ml 0.375% ropivacaine at the end of surgery |
| 24 | Abdelhamid37 | Bupivacaine | 0.25% | 40 ml | Epidural with 20 ml 0.25% bupivacaine |
| 25 | Tantri38 | Bupivacaine | 0.25% | 20 ml | TLIP block with 20 ml 0.25% bupivacaine |
| 26 | Wittayapairoj39 | Bupivacaine | 0.38% | 20 ml | No intervention |
| 27 | Holas40 | Levobupivacaine | 0.25% | 20 ml | Placebo with Normal saline |
| 38 | Jie41 | Ropivacaine | 0.40% | 20 ml | Placebo with Normal saline |
| 39 | Mohamoud42 | Bupivacaine | 0.25% | 20 ml | Intrathecal morphine |
| 30 | Bellantonio43 | Ropivacaine | 0.40% | 20 ml | No intervention |
| 31 | Taşkaldıran44 | Bupivacaine | 0.25% | 20 ml | No intervention |
| 32 | Kumar45 | Ropivacaine | 0.20% | 20 ml | Modified TLIP block with 20 ml of 0.2% ropivacaine |
MMA – Multimodal analgesia; MTP - Mid-point Transverse process to Pleura; QL – Quadratus Lumborum; TLIP – Thoraco-Lumbar Interfascial Plane.
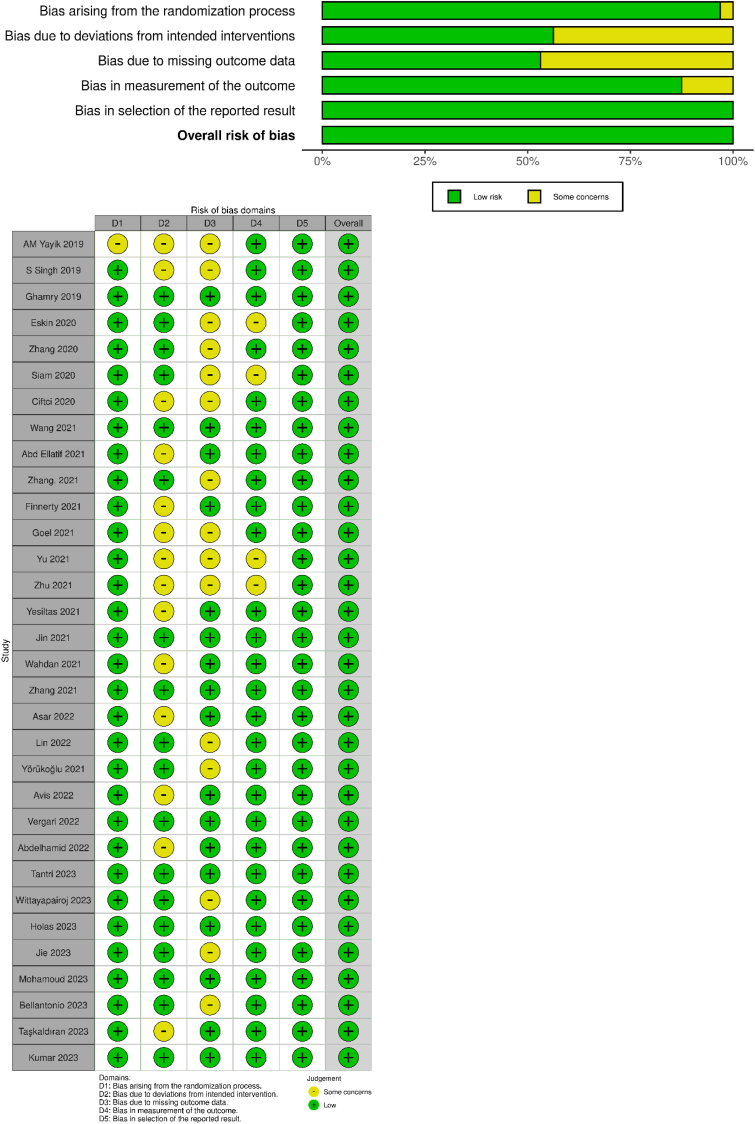
3.2. Quality assessment
The methodological quality assessment of the included studies is shown in Fig. 2. None of the studies had to be excluded from the analysis due to high risk of bias from the available data.
Fig. 2.
Methodological quality and risk of bias assessment of all the included studies.
3.3. Primary outcomes
3.3.1. Post-operative pain scores
Post-operative pain scores were compared between the groups at multiple time points in the included studies. In order to standardize the comparison, we included the post-operative pain scores at immediate post-op, 4-, 8-, 12- and 24-h time points for our analysis.
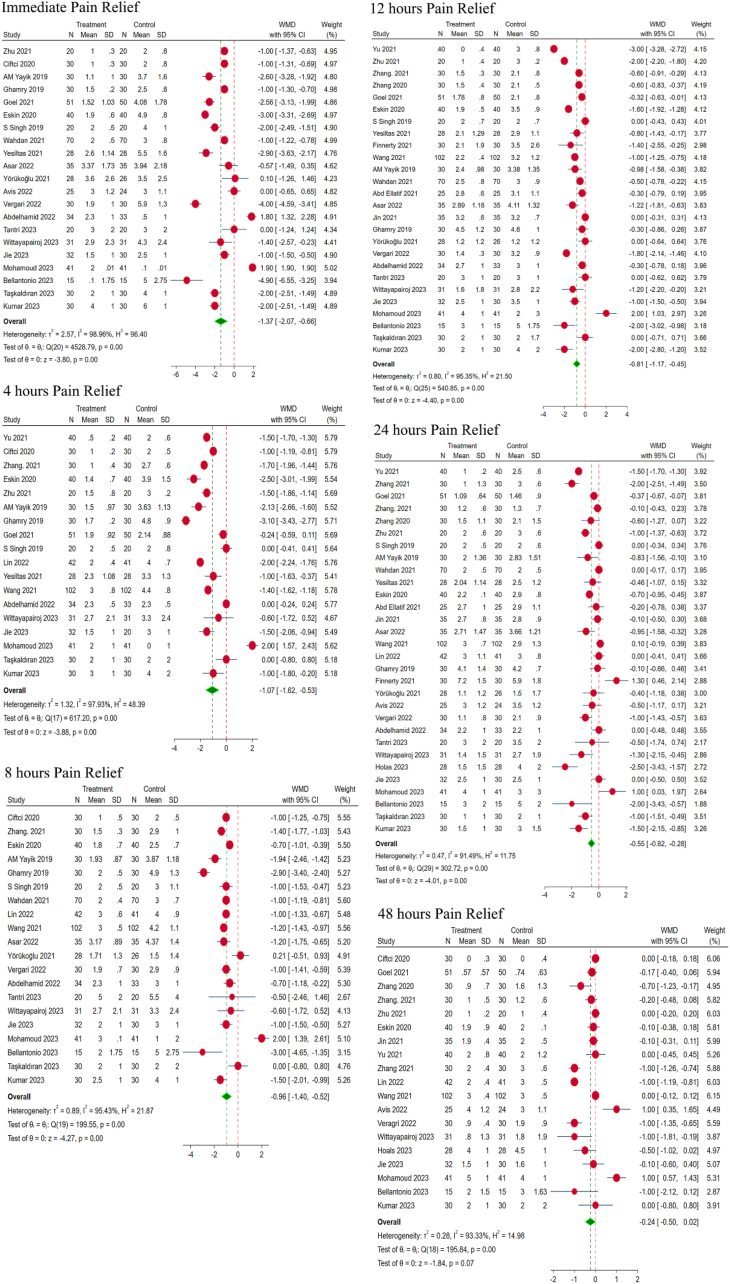
With regard to the immediate post-operative pain scores, significant heterogeneity existed between the included studies; and therefore, random-effects model was used. The ESPB group showed a significant pain relief, as compared to control (WMD = −1.37, 95% CI [−2.07, −0.66], p < 0.001; I2 = 98.96%, p < 0.001), as shown in Fig. 3. At 4-h post-operative time point, ESPB continued to demonstrate a significant difference in pain relief, in comparison with the control population. In view of significant heterogeneity, random-effects model was used for the analysis (WMD = −1.07, 95% CI [−1.62, −0.53], p < 0.001; I2 = 97.93%, p < 0.001; as shown in Fig. 3).
Fig. 3.
Forest plot of the included studies comparing post-operative pain scores at various time points.
Similarly, at the 8-, 12-, and 24-h time points too, the ESPB group remained superior to the control group {with significant heterogeneity, as given by WMD = −0.96, 95% CI [−1.40, −0.52], p < 0.001; I2 = 95.43%, p < 0.001; WMD = −0.81, 95% CI [−1.17, −0.45], p < 0.001; I2 = 95.35%, p < 0.001; WMD = −0.55, 95% CI [−0.82, −0.28], p < 0.001; I2 = 91.49%, p < 0.001; Fig. 3}. However, at 48 h, although the ESPB group demonstrated considerable pain relief in comparison with control population, a significant difference could not be made out (WMD = −0.24, 95% CI [−0.50, 0.02], p = 0.07; I2 = 93.33%, p < 0.001; as shown in Fig. 3).
3.3.2. Total analgesic consumption
Among the multiple time points evaluated in the included studies, we analysed the post-operative analgesia consumption reported at the 8-, 12- and 24-h time points for our analysis. We could clearly observe that there was no uniformity in the usage of the analgesic drugs across the reviewed studies. For example, while parenteral morphine was employed in one of the studies; parenteral tramadol was utilised as the rescue analgesic during the post-operative period in another.
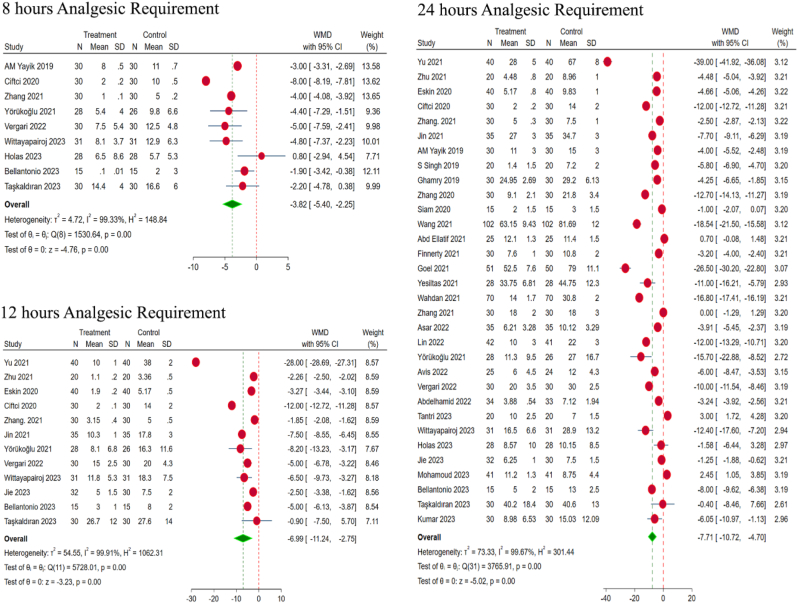
Therefore, in order to standardize the analgesic usage among the included studies for analysis, we utilized the equivalent conversion recommendation by Palliate Care Formulary between the analgesics.14 All the reported analgesic usage were converted into morphine equivalents. In compared with the controls, the ESPB group showed significantly reduced total rescue analgesic consumption {with significant heterogeneity at 8-, 12- and 24-h time points; as given by (WMD = −3.82, 95% CI [−5.40, −2.25], p < 0.001; I2 = 99.33%, p < 0.001), (WMD = −6.99, 95% CI [−11.24, −2.75], p < 0.001; I2 = 99.91%, p < 0.001), and (WMD = −7.71, 95% CI [−10.72, −4.70], p < 0.001; I2 = 99.67%, p < 0.001), respectively (Fig. 4).
Fig. 4.
Forest plot of the included studies comparing total analgesic consumption at various time points.
3.4. Secondary Outcomes
3.4.1. First analgesic requirement time
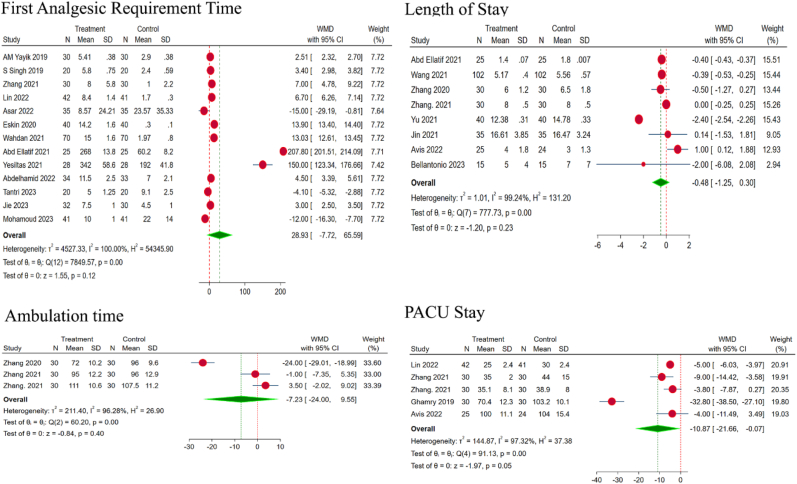
We also analyzed the time required by both the groups for the first analgesic administration post-operatively. On analysis, although the ESPB group showed longer time for first analgesic requirement; it was not statistically significant (WMD = 28.93, 95% CI [−7.72, 65.59], p = 0.120; I2 = 100%, p < 0.001) as shown in Fig. 5.
Fig. 5.
Forest plot of the included studies comparing the outcome measures like first analgesic requirement time, ambulation time, intensive care period, and length of stay complication rate.
3.4.2. Ambulation time
The time required by the two groups to ambulate following surgery was also compared. On analysis, although ESPB group showed a trend towards earlier ambulation; the difference was not statistically significant (WMD = −7.23, 95% CI [−24.00, 9.55], p = 0.45; I2 = 96.28%, p < 0.001), as shown in Fig. 5.
3.4.3. Intensive care stay
We also analyzed the time spent by the two groups in the post-anaesthesia care unit (PACU) following surgery. On analysis, the ESPB group showed significantly shorter stay in PACU, as compared with the control group (WMD = −10.87, 95% CI [−25.66, −0.07], p = 0.05; I2 = 97.32%, p < 0.001; as shown in Fig. 5).
3.4.4. Length of stay
The total length of stay was compared between the two groups following surgery. Upon analysis, although the ESPB group showed shorter length of stay in comparison with the control group; the difference was not statistically significant (WMD = −0.48, 95% CI [−1.25, 0.30], p = 0.23; I2 = 99.24%, p < 0.001; as shown in Fig. 5).
3.5. Other Outcomes
3.5.1. Satisfaction score
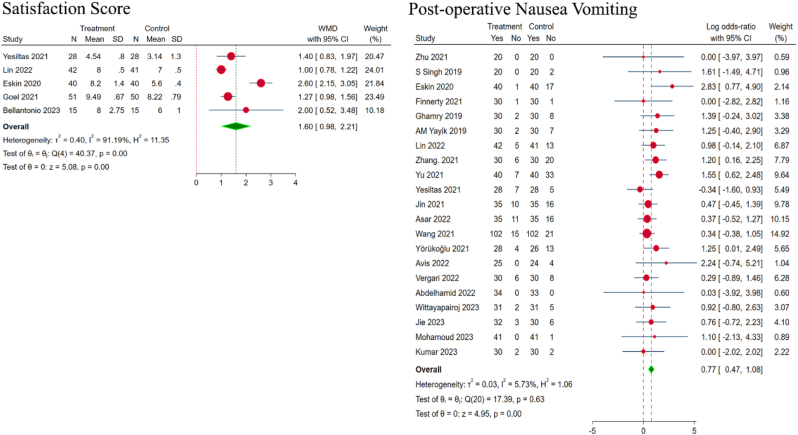
We also analyzed the satisfaction scores of the patients regarding the analgesic management in the two groups; and observed that the ESPB group demonstrated significantly higher satisfaction score, in comparison with the control group (WMD = 1.60, 95% CI [0.98, 2.21], p < 0.001; I2 = 91.19%, p < 0.001), as shown in Fig. 6.
Fig. 6.
Forest plot of the included studies comparing the outcome measures like satisfaction score and complication such as post-operative nausea vomitting.
3.5.2. Complications
Among the various complications studied between the groups, the ESPB group showed significantly fewer events of post-operative nausea and vomiting (PONV), as compared to the placebo group. There was no significant heterogeneity (RR = 0.77, 95% CI [0.47, 1.08], p < 0.001; I2 = 5.73%, p = 0.63), as shown in Fig. 6.
3.5.3. Publication bias analysis
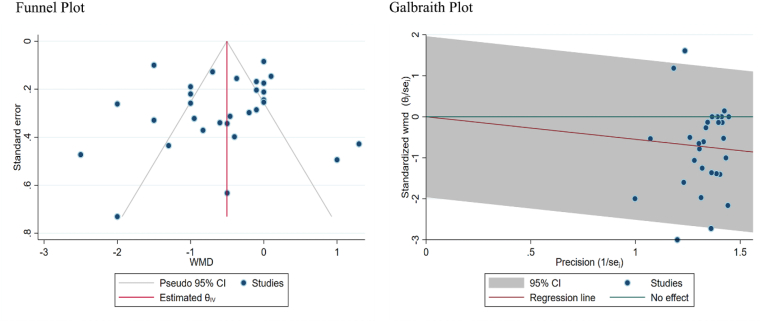
Funnel plot was generated to assess the publication bias in the primary outcomes (total analgesic requirement and magnitude of pain relief). We did not note any asymmetry as shown in Fig. 7. Further Egger's regression test did not show significant publication bias (p = 0.074).
Fig. 7.
Funnel plot and galbraith plot for total analgesic consumption in the included studies assessing the publication bias and heterogeneity in the included studies.
3.5.4. Subgroup analysis
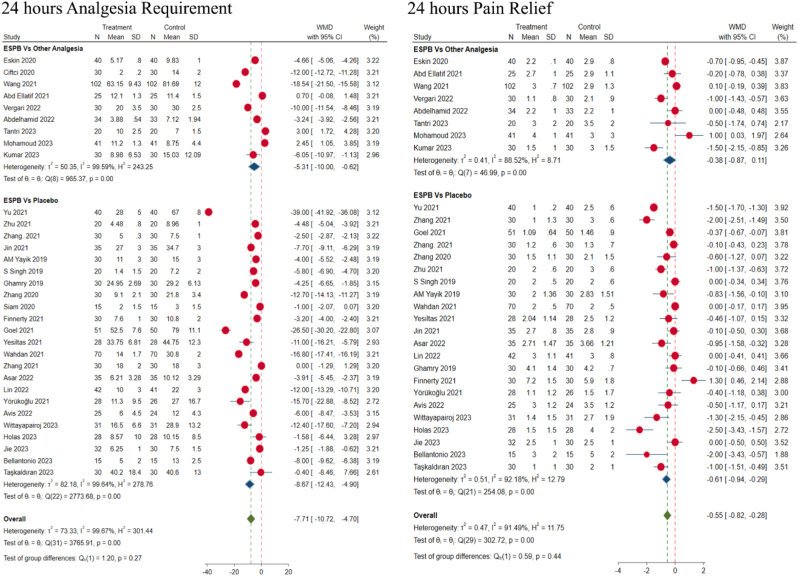
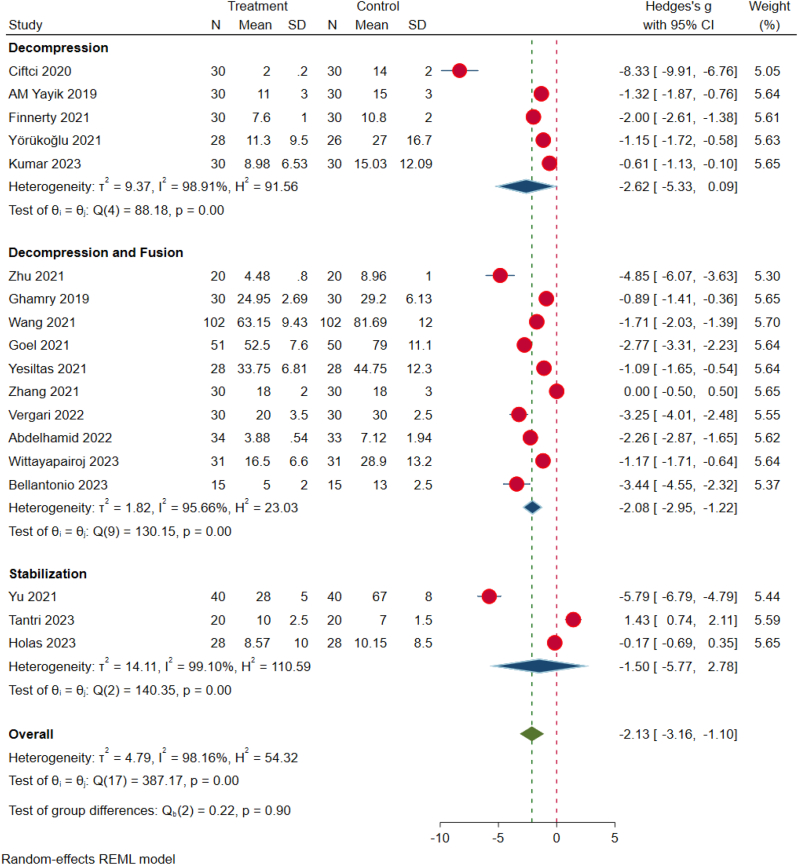
We stratified the results based on the control groups of the reviewed studies. We subgrouped the studies, based on their primary outcomes into those which utilised placebo versus those which evaluated alternate analgesic agents. We noted that the ESPB administration outperformed the placebo and other analgesic modalities (like TLIP, MTP, QL blocks) with regard to the overall analgesic requirements (p < 0.05). With regard to pain relief, although ESPB group demonstrated improved pain relief compared to other methods employed statistical significance was not achieved (p = 0.06) as shown in Fig. 8. Further, we tried to categorize the studies based on the surgeries involved. With regard to overall analgesic requirement, ESPB demonstrated significant benefit in fusion surgeries (p < 0.001) whereas the benefit of the treatment effect with ESPB was not significant in trauma stabilization and decompression surgeries of lumbar spine as shown in Fig. 9.
Fig. 8.
Subgroup analysis showing the forest plot of the included RCTs comparing the outcome measures like pain scores, total analgesic consumption.
Fig. 9.
Subgroup analysis showing the forest plot of the included RCTs comparing the total analgesic consumption across different surgery types.
3.5.5. Sensitivity analysis
We also assessed the heterogeneity among the primary outcomes with galbraith plot, as shown in Fig. 7; and the included studies were within the 95% confidence interval range. We also performed sensitivity analysis for all the outcomes; as well as the heterogeneity among the reviewed studies. None of the studies could be excluded, on the basis of any disproportionate influence over the overall outcome.
4. Discussion
The overall number of spine surgeries performed worldwide annually has tremendously increased over the past two decades. A majority of the patients undergoing these spinal procedures are afflicted by chronic mechanical disability, neuropathic pain syndrome and psychological difficulties.46 In addition, spinal surgeries (lumbar spinal procedures, in particular) have been demonstrated to inflict severe post-operative pain in a majority of patients.2 With this background, the need for post-operative MMA following spinal surgeries has been progressively acknowledged world-wide.4 Over the past decade, ESPB has been described as a simple, ultrasound-guided, regional modality for providing axial pain relief.10 It was initially described in 2010 as a local, analgesic option in pain following rib fractures[E10]. In 2016, it was further described by Forero et al10 for the treatment of thoracic, neuropathic pain; and has henceforth, been utilised by anesthesiologists for acute and chronic pain management.10,47 It has been employed as an adjuvant analgesic modality in the treatment of thoracic, abdominal wall and breast surgeries.48,49 Over the past few years, it has been increasing recognised as a simple component of peri-operative MMA in patients undergoing spinal surgery.40 Over the recent years, although multiple prospective trials have been published; the availability of systematic reviews or meta-analysis on this subject is fairly limited. The current meta-analysis was thus planned to comprehensively analyse the present literature; and put forth the best available evidence regarding bilateral ESPB as a pre-emptive analgesic modality in patients undergoing spinal surgery.
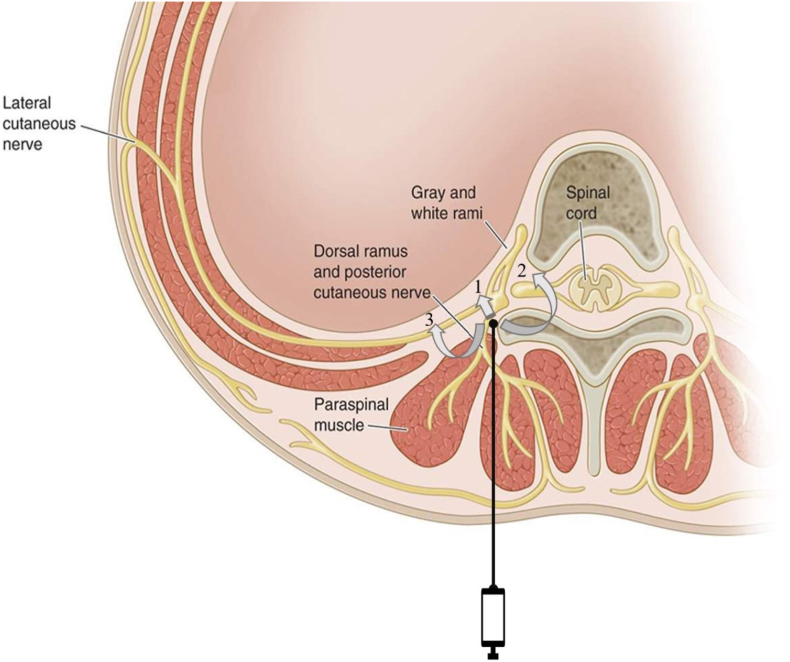
Based on our meta-analysis, we could observe that ESPB substantially mitigated the severity of post-operative pain at all the time points of evaluation during the initial 24 h; although the difference at 48 h was not statistically significant. The post-operative pain following posterior spinal surgeries has been attributed to the mechanical insults during dissection, intra-operative retraction, partial devascularisation of soft tissues, denervation of bony tissues, ligaments, muscular tissues; as well as injuries sustained by the intervertebral discs and facetal articulations. Additionally, neuropathic pain may also develop secondary to the intra-operative insults sustained by the nerve roots leaving the spinal canal or by the spinal cord itself.31,40 ESPB involves injection of LA agent between the deep fascia of erector spinae musculature and transverse process of the vertebra.37 Being an interfascial plane block, ESPB leads to proximo-distal migration of the LA, thereby resulting in the blockade of medial and lateral branches of the dorsal rami of lumbar nerve roots.45 In addition, the drug is distributed anteriorly and laterally too, thereby enabling its spread to the paravertebral, epidural and intercostal regions as shown in Fig. 10. In the clinical scenario, it has been purported that the type of opioid utilised during the intra-operative (remifentanil/fentanyl/sufentanil) as well as the opioid administered post-operatively (fentanyl/morphine/pethidine/sufentanil) can potentially impact the efficacy of ESPB.50 Although there is substantial evidence supporting ESPB in the context of immediate post-operative pain relief, there is insufficient data regarding its role in the intermediate- or long-term follow-up.45
Fig. 10.
Illustration on the localization of ESPB needle and spaces of distribution of drug apart from cranio-caudal spread including epidural (1), and paravertebral (2) spaces anteriorly and intercoastal space (3) laterally with ESPB.
We could also clearly observe that the administration of ESPB substantially mitigated the need for opioid analgesia during the early post-operative period (at the 8-, 12- and 24-h post-operative time points), as observed by the reduction in morphine equivalents. This has been postulated to be one of the most crucial benefits of the regional blocks, which have become an integral part of the multimodal pain-control regimen during the post-operative period.11 Such additional pain relief offered by ESPB can potentially obviate the adverse effects associated with opioid usage including nausea, vomiting, hypotension, excessive sedation, gastrointestinal disturbances, post-operative urinary retention, delayed rehabilitation or ambulation, long-term physical or psychological dependence; and respiratory complications including respiratory depression or aspiration pneumonitis.36,41,44 Taskaldiran et al44 demonstrated that the use of ESPB mitigated the need for opioids during the intra-operative and 1st-post-operative hour. It is well-recognised that administration of high doses of opioids (especially remifentanil) intraoperatively, can result in “hyperalgesia” during the immediate post-operative period; which may be obviated by ESPB.44 In our analysis, we did not observe any significant difference in the time required for first analgesic dose administration (which has been described in the literature as a measure of the effective duration of analgesia following the regional block) following ESPB.
Two of the most important reasons for the growing popularity of ESPB are its procedural simplicity and the ease of identifying the landmarks using an ultrasound or fluoroscopically.36 Diverse variations in the ESPB techniques have been described heretofore, with respect to the timing of administration, patient positioning (prone versus lateral), direction of drug administration (lateromedial vs craniocaudal), level of administration (incisional vs thoracic vs lumbar), approaches (in-plane vs out-of-plane); as well as the types, volumes or concentrations of LA utilised.50 However, it is a recently introduced block; and the technique is constantly evolving with time.
Based on our analysis, we could observe that the use of ESPB significantly reduced the length of patient stay in the PACU following spine surgery. The other secondary outcome parameters employed in the studies were ambulation time and the overall length of hospital stay. Although we could clearly observe a trend towards early ambulation and shorter length of hospital stay in the ESPB group; the overall difference was not statistically different. The “Enhanced Recovery After Surgery” (ERAS) protocol has been described as multidisciplinary strategies involving pre-operative patient counselling, systematic prehabilitation and optimisation of patients’ health with the collective goal of mitigating the overall healthcare costs, reducing adverse events or complications, as well as facilitating early discharge and meliorated outcomes.51,52 With the exponential growth in the number of spine surgeries and the huge increase in the related expenditure; there has been global shift toward ERAS protocol during the post-operative period.53 In this context, ESPB is growingly acknowledged as an effective strategy in patients undergoing spine surgeries. Similar to the observations in a previous meta-analysis by Oh et al,50 our analysis also demonstrated a significantly higher patient satisfaction scores following the administration of ESPB.
With regard to the safety profile, ESPB has not be correlated with any major complications like toxicity of LA agents, neurological deteriorations, pleural injury or pneumothorax. However, there have been some minor adverse events reported in some studies like priapism and transient motor weakness.36,50,51 In the study by Taskaldiran et al,44 the use of bupivacaine in ESPB resulted in higher cardiovascular risk, since the drug bio-availability was higher as compared to other paraspinal blocks. This relative safety of the technique has been attributed to the relative remoteness of approach to vulnerable vital structures like spinal cord, nerve roots, vascular tissues and pleura.44 Previous studies have acknowledged the need for larger, prospective studies to clearly establish the long-term safety profile of the procedure.36,44,50,51 Based on our meta-analysis, we could observe a statistically significant reduction of post-operative nausea and vomiting (PONV) in patients undergoing ESPB.35,39 This finding may be correlated with the reduced need for intra- and early post-operative opioid analgesia. Previous studies have correlated lower PONV rates with substantially improved satisfaction score and shorter hospital stay.
In 2022, Oh et al50 published a meta-analysis on the adjuvant role of ESPB in multimodal analgesia following spinal surgery. Similar to our observations, they also concluded that ESPB was associated with reduced opioid consumption in the initial 24 h, mitigated pain severity in the first 48 h, and improved patient satisfaction. Since the previous meta-analysis, multiple prospective studies have been published. Therefore, we performed the current meta-analysis to update the evidence in the literature to provide the most recent practice recommendations.
4.1. Limitations
There is substantial heterogeneity in the reviewed studies regarding the techniques of ESPB administration, drug dosage, intra- and peri-operative analgesic protocols employed, types of lumbar surgeries, and outcome measurements. There is still substantial paucity of data regarding the ideal approach, timing, dosage, type of LA used in ESPB, duration of its efficacy, ideal level of block delivery, and intermediate- or long-term outcome. These are potential topics for future, large-scale, randomised controlled studies on this subject. Despite these limitations, our study is the largest meta-analysis performed hitherto; and substantially adds to the previously published reviews on ESPB.
5. Conclusion
ESPB offers prolonged post-operative pain relief compared to controls, thereby reducing the need for opioid consumption and its related complications. The utilisation of ESPB significantly improves the patient satisfaction rate.
Funding
No funding was utilised for the conduction of this study.
CRediT authorship contribution statement
Sathish Muthu: Writing – review & editing, Writing – original draft, Visualization, Validation, Supervision, Software, Resources, Project administration, Methodology, Investigation, Formal analysis, Data curation, Conceptualization. Vibhu Krishnan Viswanathan: Writing – review & editing, Writing – original draft, Validation, Supervision, Formal analysis, Data curation, Conceptualization. Saravanan Annamalai: Writing – review & editing, Supervision, Project administration, Formal analysis. Mohammed Thabrez: Writing – review & editing, Investigation, Formal analysis, Data curation.
Declaration of competing interest
On behalf of all authors, corresponding author declare no conflict of interest.
References
- 1.Bianconi M., Ferraro L., Ricci R., et al. The pharmacokinetics and efficacy of ropivacaine continuous wound instillation after spine fusion surgery. Anesth Analg. 2004;98:166. doi: 10.1213/01.ANE.0000093310.47375.44. [DOI] [PubMed] [Google Scholar]
- 2.Gerbershagen H.J., Aduckathil S., van Wijck A.J.M., et al. Pain intensity on the first day after surgery: a prospective cohort study comparing 179 surgical procedures. Anesthesiology. 2013;118:934–944. doi: 10.1097/ALN.0b013e31828866b3. [DOI] [PubMed] [Google Scholar]
- 3.Bajwa S.J.S., Haldar R. Pain management following spinal surgeries: an appraisal of the available options. J Craniovertebral Junction Spine. 2015;6:105–110. doi: 10.4103/0974-8237.161589. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Bae S., Alboog A., Esquivel K.S., et al. Efficacy of perioperative pharmacological and regional pain interventions in adult spine surgery: a network meta-analysis and systematic review of randomised controlled trials. Br J Anaesth. 2022;128:98–117. doi: 10.1016/j.bja.2021.08.034. [DOI] [PubMed] [Google Scholar]
- 5.Soffin E.M., Beckman J.D., Tseng A., et al. Enhanced recovery after lumbar spine fusion: a randomized controlled trial to assess the quality of patient recovery. Anesthesiology. 2020;133:350–363. doi: 10.1097/ALN.0000000000003346. [DOI] [PubMed] [Google Scholar]
- 6.Samagh N., Pai R.K., Mathews T.K., et al. Pre-emptive caudal epidural analgesia with ropivacaine for lumbosacral spine surgery: a randomized case control study. J Anaesthesiol Clin Pharmacol. 2018;34:237–241. doi: 10.4103/joacp.JOACP_72_17. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Long G., Liu C., Liang T., Zhan X. The efficacy of thoracolumbar interfascial plane block for lumbar spinal surgeries: a systematic review and meta-analysis. J Orthop Surg Res. 2023;18:318. doi: 10.1186/s13018-023-03798-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Costache I., de Neumann L., Ramnanan C.J., et al. The mid-point transverse process to pleura (MTP) block: a new end-point for thoracic paravertebral block. Anaesthesia. 2017;72:1230–1236. doi: 10.1111/anae.14004. [DOI] [PubMed] [Google Scholar]
- 9.Dhanjal S., Tonder S. StatPearls. StatPearls Publishing, Treasure Island (FL) 2023. Quadratus lumborum block. [PubMed] [Google Scholar]
- 10.Forero M., Adhikary S.D., Lopez H., et al. The erector spinae plane block: a novel analgesic technique in thoracic neuropathic pain. Reg Anesth Pain Med. 2016;41:621–627. doi: 10.1097/AAP.0000000000000451. [DOI] [PubMed] [Google Scholar]
- 11.Avis G., Gricourt Y., Vialatte P.B., et al. Analgesic efficacy of erector spinae plane blocks for lumbar spine surgery: a randomized double-blind controlled clinical trial. Reg Anesth Pain Med rapm-2022-103737. 2022 doi: 10.1136/rapm-2022-103737. [DOI] [PubMed] [Google Scholar]
- 12.Page M.J., McKenzie J.E., Bossuyt P.M., et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71. doi: 10.1136/bmj.n71. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Sterne J.A.C., Savović J., Page M.J., et al. RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ. 2019;366:l4898. doi: 10.1136/bmj.l4898. [DOI] [PubMed] [Google Scholar]
- 14.Higgins J.P.T., Thompson S.G., Deeks J.J., Altman D.G. Measuring inconsistency in meta-analyses. BMJ. 2003;327:557–560. doi: 10.1136/bmj.327.7414.557. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Yayik A.M., Cesur S., Ozturk F., et al. Postoperative analgesic efficacy of the ultrasound-guided erector spinae plane block in patients undergoing lumbar spinal decompression surgery: a randomized controlled study. World Neurosurg. 2019;126:e779–e785. doi: 10.1016/j.wneu.2019.02.149. [DOI] [PubMed] [Google Scholar]
- 16.Singh S., Choudhary N.K., Lalin D., Verma V.K. Bilateral ultrasound-guided erector spinae plane block for postoperative analgesia in lumbar spine surgery: a randomized control trial. J Neurosurg Anesthesiol. 2020;32:330–334. doi: 10.1097/ANA.0000000000000603. [DOI] [PubMed] [Google Scholar]
- 17.Ghamry M., Elgebaly A., Anwar A., Shaddad M. Ultrasound-guided erector spinae plane block for acute pain management in patients undergoing posterior lumbar interbody fusion under general anaesthesia. South Afr J Anaesth Analg. 2019;25:26–31. doi: 10.36303/SAJAA.2019.25.6.A4. [DOI] [Google Scholar]
- 18.Eskin M.B., Ceylan A., Özhan M.Ö., Atik B. Ultrasound-guided erector spinae block versus mid-transverse process to pleura block for postoperative analgesia in lumbar spinal surgery. Anaesthesist. 2020;69:742–750. doi: 10.1007/s00101-020-00848-w. [DOI] [PubMed] [Google Scholar]
- 19.Zhang T.-J., Zhang J.-J., Qu Z.-Y., et al. Bilateral erector spinae plane blocks for open posterior lumbar surgery. J Pain Res. 2020;13:709–717. doi: 10.2147/JPR.S248171. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Siam E.M., Abo Aliaa D.M., Elmedany S., Abdelaa M.E. Erector spinae plane block combined with general anaesthesia versus conventional general anaesthesia in lumbar spine surgery. Egypt J Anaesth. 2020;36:201–226. doi: 10.1080/11101849.2020.1821501. [DOI] [Google Scholar]
- 21.Ciftci B., Ekinci M., Celik E.C., et al. Ultrasound-guided erector spinae plane block versus modified-thoracolumbar interfascial plane block for lumbar discectomy surgery: a randomized, controlled study. World Neurosurg. 2020;144:e849–e855. doi: 10.1016/j.wneu.2020.09.077. [DOI] [PubMed] [Google Scholar]
- 22.Wang L., Wu Y., Dou L., et al. Comparison of two ultrasound-guided plane blocks for pain and postoperative opioid requirement in lumbar spine fusion surgery: a prospective, randomized, and controlled clinical trial. Pain Ther. 2021;10:1331–1341. doi: 10.1007/s40122-021-00295-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Abd Ellatif S.E., Abdelnaby S.M. Ultrasound guided erector spinae plane block versus quadratus lumborum block for postoperative analgesia in patient undergoing open nephrectomy: a randomized controlled study. Egypt J Anaesth. 2021;37:123–134. doi: 10.1080/11101849.2021.1894661. [DOI] [Google Scholar]
- 24.Zhang Q., Wu Y., Ren F., et al. Bilateral ultrasound-guided erector spinae plane block in patients undergoing lumbar spinal fusion: a randomized controlled trial. J Clin Anesth. 2021;68 doi: 10.1016/j.jclinane.2020.110090. [DOI] [PubMed] [Google Scholar]
- 25.Finnerty D., Ní Eochagáin A., Ahmed M., et al. A randomised trial of bilateral erector spinae plane block vs. no block for thoracolumbar decompressive spinal surgery. Anaesthesia. 2021;76:1499–1503. doi: 10.1111/anae.15488. [DOI] [PubMed] [Google Scholar]
- 26.Goel V.K., Chandramohan M., Murugan C., et al. Clinical efficacy of ultrasound guided bilateral erector spinae block for single-level lumbar fusion surgery: a prospective, randomized, case-control study. Spine J. 2021;21:1873–1880. doi: 10.1016/j.spinee.2021.06.015. [DOI] [PubMed] [Google Scholar]
- 27.Yu Y., Wang M., Ying H., et al. The analgesic efficacy of erector spinae plane blocks in patients undergoing posterior lumbar spinal surgery for lumbar fracture. World Neurosurg. 2021;147:e1–e7. doi: 10.1016/j.wneu.2020.10.175. [DOI] [PubMed] [Google Scholar]
- 28.Zhu L., Wang M., Wang X., et al. Changes of opioid consumption after lumbar fusion using ultrasound-guided lumbar erector spinae plane block: a randomized controlled trial. Pain Physician. 2021;24:E161–E168. [PubMed] [Google Scholar]
- 29.Yeşiltaş S., Abdallah A., Uysal Ö., et al. The efficacy of intraoperative freehand erector spinae plane block in lumbar spondylolisthesis: a randomized controlled study. Spine. 2021;46:E902–E910. doi: 10.1097/BRS.0000000000003966. [DOI] [PubMed] [Google Scholar]
- 30.Jin Y., Zhao S., Cai J., et al. Erector spinae plane block for perioperative pain control and short-term outcomes in lumbar laminoplasty: a randomized clinical trial. J Pain Res. 2021;14:2717–2727. doi: 10.2147/JPR.S321514. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Wahdan A.S., Radwan T.A., Mohammed M.M., et al. Effect of bilateral ultrasound-guided erector spinae blocks on postoperative pain and opioid use after lumbar spine surgery: a prospective randomized controlled trial. Egypt J Anaesth. 2021;37:100–106. doi: 10.1080/11101849.2021.1893984. [DOI] [Google Scholar]
- 32.Zhang J.-J., Zhang T.-J., Qu Z.-Y., et al. Erector spinae plane block at lower thoracic level for analgesia in lumbar spine surgery: a randomized controlled trial. World J Clin Cases. 2021;9:5126–5134. doi: 10.12998/wjcc.v9.i19.5126. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Asar S., Sarı S., Altinpulluk E.Y., Turgut M. Efficacy of erector spinae plane block on postoperative pain in patients undergoing lumbar spine surgery. Eur Spine J. 2022;31:197–204. doi: 10.1007/s00586-021-07056-z. [DOI] [PubMed] [Google Scholar]
- 34.Lin H., Guan J., Luo S., et al. Bilateral erector spinae plane block for quality of recovery following posterior lumbar interbody fusion: a randomized controlled trial. Pain Ther. 2022;11:861–871. doi: 10.1007/s40122-022-00395-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Yörükoğlu H.U., İçli D., Aksu C., et al. Erector spinae block for postoperative pain management in lumbar disc hernia repair. J Anesth. 2021;35:420–425. doi: 10.1007/s00540-021-02920-0. [DOI] [PubMed] [Google Scholar]
- 36.Vergari A., Frassanito L., DI Muro M., et al. Bilateral lumbar ultrasound-guided erector spinae plane block versus local anesthetic infiltration for perioperative analgesia in lumbar spine surgery: a randomized controlled trial. Minerva Anestesiol. 2022;88:465–471. doi: 10.23736/S0375-9393.22.15950-X. [DOI] [PubMed] [Google Scholar]
- 37.Abdelhamid H.S., ElSabbagh H.A., Amin S.M., Abdelhakeem A.K. Erector spinae plane block vs. single shot epidural block for postoperative analgesia in lumbar spine surgery: a randomized controlled trial. Anaesth Pain Intensive Care. 2022;26:310–317. doi: 10.35975/apic.v26i3.1897. [DOI] [Google Scholar]
- 38.Tantri A.R., Rahmi R., Marsaban A.H.M., et al. Comparison of postoperative IL-6 and IL-10 levels following Erector Spinae Plane Block (ESPB) and classical Thoracolumbar Interfascial Plane (TLIP) block in a posterior lumbar decompression and stabilization procedure: a randomized controlled trial. BMC Anesthesiol. 2023;23:13. doi: 10.1186/s12871-023-01973-w. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Wittayapairoj A., Wittayapairoj K., Kulawong A., Huntula Y. Effect of intermediate dose dexamethasone on post-operative pain in lumbar spine surgery: a randomized, triple-blind, placebo-controlled trial. Asian journal of anesthesiology. 2017;55:73–77. doi: 10.1016/j.aja.2017.08.001. [DOI] [PubMed] [Google Scholar]
- 40.Holas M., Hlásny J., Gajdoš R., et al. Does erector spinae plane block decrease analgesia requirements after minimal-invasive posterior transpedicular stabilization in patients with vertebral body fracture? A prospective, randomized, double-blind controlled study. Global Spine J. 2023 doi: 10.1177/21925682231156558. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Jie P., Wenqi Z., Youping W., Yongyuan M. Effects of bilateral erector spinae plane block for posterior lumbar spine surgery in elderly patients. J Cent S Univ Med Sci. 2023;48 doi: 10.11817/j.issn.1672-7347.2023.220151. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Mahmoud A.M., Ragab S.G., Shawky M.A., et al. The efficacy of erector spinae plane block compared with intrathecal morphine in postoperative analgesia in patients undergoing lumbar spine surgery: a double-blind prospective comparative study. Pain Physician. 2023;26:149–159. [PubMed] [Google Scholar]
- 43.Bellantonio D., Bolondi G., Cultrera F., et al. Erector spinae plane block for perioperative pain management in neurosurgical lower-thoracic and lumbar spinal fusion: a single-centre prospective randomised controlled trial. BMC Anesthesiol. 2023;23:187. doi: 10.1186/s12871-023-02130-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Taşkaldıran Y. Is opioid-free anesthesia possible by using erector spinae plane block in spinal surgery? Cureus. 2021;13 doi: 10.7759/cureus.18666. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Kumar A., Sinha C., Kumar A., et al. Modified thoracolumbar interfascial plane block versus erector spinae plane block in patients undergoing spine surgeries: a randomized controlled trial. J Neurosurg Anesthesiol. 2023 doi: 10.1097/ANA.0000000000000900. [DOI] [PubMed] [Google Scholar]
- 46.McCarthy R.J., Adams A.M., Sremac A.C., et al. Trajectories of opioid consumption from day of surgery to 28 days postoperatively: a prospective cohort study in patients undergoing abdominal, joint, or spine surgery. Reg Anesth Pain Med. 2021;46:1067–1075. doi: 10.1136/rapm-2021-102910. [DOI] [PubMed] [Google Scholar]
- 47.Truitt M.S., Mooty R.C., Amos J., et al. Out with the old, in with the new: a novel approach to treating pain associated with rib fractures. World J Surg. 2010;34:2359–2362. doi: 10.1007/s00268-010-0651-9. [DOI] [PubMed] [Google Scholar]
- 48.Chin K.J., Malhas L., Perlas A. The erector spinae plane block provides visceral abdominal analgesia in bariatric surgery: a report of 3 cases. Reg Anesth Pain Med. 2017;42:372–376. doi: 10.1097/AAP.0000000000000581. [DOI] [PubMed] [Google Scholar]
- 49.Gürkan Y., Aksu C., Kuş A., et al. Ultrasound guided erector spinae plane block reduces postoperative opioid consumption following breast surgery: a randomized controlled study. J Clin Anesth. 2018;50:65–68. doi: 10.1016/j.jclinane.2018.06.033. [DOI] [PubMed] [Google Scholar]
- 50.Oh S.K., Lim B.G., Won Y.J., et al. Analgesic efficacy of erector spinae plane block in lumbar spine surgery: a systematic review and meta-analysis. J Clin Anesth. 2022;78 doi: 10.1016/j.jclinane.2022.110647. [DOI] [PubMed] [Google Scholar]
- 51.Liu H., Zhu J., Wen J., Fu Q. Ultrasound-guided erector spinae plane block for postoperative short-term outcomes in lumbar spine surgery: a meta-analysis and systematic review. Medicine (Baltim) 2023;102 doi: 10.1097/MD.0000000000032981. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Bansal T., Sharan A.D., Garg B. Enhanced recovery after surgery (ERAS) protocol in spine surgery. J Clin Orthop Trauma. 2022;31 doi: 10.1016/j.jcot.2022.101944. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.Tong Y., Fernandez L., Bendo J.A., Spivak J.M. Enhanced recovery after surgery trends in adult spine surgery: a systematic review. Internet J Spine Surg. 2020;14:623–640. doi: 10.14444/7083. [DOI] [PMC free article] [PubMed] [Google Scholar]