Abstract
The Quality Payment Program (QPP) is a Medicare value-based payment program with 2 tracks: -Advanced Alternative Payment Models (A-APMs), including two-sided risk Accountable Care Organizations (ACOs), and Merit-based Incentive Payment System (MIPS). In 2020, A-APM eligible ACO clinicians received an additional 5% positive, and MIPS clinicians received up to 5% negative or 2% positive performance-based adjustments to their Medicare Part B medical services payments. It is unclear whether the different payment adjustments have differential impacts on total medical services payments for ACO and MIPS participants. We compare Medicare Part B medical services payments received by primary care clinicians participating in ACO and MIPS programs using Medicare Provider Utilization and Payment Public Use Files from 2014 to 2018 using difference-in-differences regressions. We have 254 395 observations from 50 879 unique clinicians (ACO = 37.86%; MIPS = 62.14%). Regression results suggest that ACO clinicians have significantly higher Medicare Part B medical services payments ($1003.88; 95% CI: [579.08, 1428.69]) when compared to MIPS clinicians. Our findings suggest that ACO clinicians had a greater increase in medical services payments when compared to MIPS clinicians following QPP participation. Increased payments for Medicare Part B medical services among ACO clinicians may be driven partly by higher payment adjustment rates for ACO clinicians for Part B medical services. However, increased Part B medical services payments could also reflect clinicians switching to increased outpatient services to prevent potentially costly inpatient services. Policymakers should examine both aspects when evaluating QPP effectiveness.
Keywords: accountable care organizations, merit-based incentive payment system, medicare part B payments, quality payment program, medicare, incentive
What do we already know about this topic?
Under the Quality Payment Program, clinicians receive different payment adjustment rates for Medicare Part B professional services based on whether they participate in the Advanced Alternative Payment Model (such as ACOs) or Merit-based Incentive Payment Systems; however, the impact of the different payment adjustments on Part B payments is unclear.
How does your research contribute to the field?
Compared to clinicians participating in MIPS, our study finds that ACO clinicians have higher Medicare Part B medical services payments following QPP implementation.
What are your research’s implications toward theory, practice, or policy?
Increased Part B medical services payments to ACO clinicians could be partly due to higher payment adjustments offered by QPP to ACO clinicians.
Policymakers should evaluate other possibilities for higher Part B payments to ACO clinicians including clinicians performing more outpatient services to prevent potentially costly inpatient services, when evaluating the effectiveness of QPP.
Introduction
Medicare pays for Part B services using the fee-for-service (FFS) payment model for beneficiaries enrolled in traditional Medicare (TM) plans. 1 Unadjusted FFS payment provides no explicit links to the quality of care.2,3 In recent years, Medicare payment policies have implemented value-based payment models that link clinicians’ payments with their performance in quality and cost of care.4 -7 The Centers for Medicare and Medicaid Services (CMS) created the Quality Payment Program (QPP) in 2017 to incorporate a value-based payment mechanism in the TM program. This payment reform links almost all TM clinicians’ payments to their performances.4 -8 The program’s objective is to reduce spending while improving the quality of care. QPP requires eligible clinicians to participate in either of 2 tracks - Advanced Alternative Payment Models (A-APMs) or Merit-based Incentive Payment System (MIPS).4 -8 Under the QPP, all eligible clinicians, which is almost all clinicians participating in the TM program, receive adjusted payments for their Medicare Part B professional services. This payment adjustment rate, however, differs for clinicians participating in either of the QPP tracks.8 -10 To encourage clinicians’ participation in APM programs, QPP offers higher positive payment adjustment rates to the A-APM track compared to the MIPS track. It is important to understand how this difference in payment adjustment rates between the 2 QPP tracks impacts clinicians’ total payments for Medicare Part B covered professional services. The difference in Part B payment adjustments between A-APM and MIPS clinicians could influence the use of relatively low-priced Part B services as alternatives to more expensive Part A services, affecting total Medicare expenditures.11 -17
Advanced APMs
A-APM is a voluntary track for eligible APMs such as Accountable Care Organizations (ACOs) who meet the criteria of qualifying participants (QPs), defined as clinicians whose Medicare beneficiaries assigned to an A-APM represent at least 20% of all their Medicare beneficiaries or those for whom 25% or more of their practice’s Medicare Part B payments come through eligible APMs. QPs receive a 5% positive adjustment to their Medicare Part B professional service payments.8,18 APM clinicians who do not meet QPs criteria can voluntarily participate in the MIPS. However, APMs not eligible for A-APM track, that is, not assuming financial risk, must participate in the MIPS program. These A-APM non-qualifying clinicians who voluntarily or mandatorily participate in the MIPS program receive MIPS-specific performance-based payment adjustments. 18
Accountable Care Organizations (ACOs) Under QPP
Accountable Care Organizations (ACOs) are one of the APMs eligible for the A-APM track. Since ACOs are one of the largest APM programs in Medicare19 -21 including those in the MIPS track,22,23 they are the choice of APMs for this study. ACOs are groups of clinicians who voluntarily take the responsibility of improving the quality of care and minimizing the cost of care for their attributed beneficiaries. ACO clinicians, in return, receive shared-saving bonuses based on their capacity to generate savings, assuming they meet the performance threshold.24 -26 Under QPP, ACO clinicians are eligible for one of the QPP tracks and related payment adjustments depending on their risk-sharing model and patient or payment volume. ACO clinicians under risk-sharing models who meet QPs criteria of the A-APM track receive a 5% positive adjustment to their Medicare Part B professional service payments. ACO clinicians under risk-sharing models who do not meet QPs criteria can voluntarily participate in the MIPS program to receive MIPS payment adjustment. ACO shared savings-only (no downside risk) clinicians are not eligible for the A-APM as they don’t bear financial risk and, therefore, must participate in the MIPS program and receive MIPS payment adjustments. 27
Merit-Based Incentive Payment System (MIPS)
The Merit-based Incentive Payment System (MIPS) is a modified FFS payment program that adjusts clinicians’ payments based on their performance in 4 categories—quality, improvement activities (IA), promoting interoperability (PI), and cost. It is a mandatory program for eligible TM clinicians meeting a low volume threshold (LVT), defined as payment of more than $30 000 and serving at least 100 patients in 2017 and $90 000 payment and 200 patients in 2018 under Medicare Part B program. Failure to participate and meet the program’s requirements results in a penalty. 8 MIPS-eligible clinicians must report several self-selected measures; at least 6 quality measures, 1 to 4 IA measures, and a full set of PI measures.28 -33 Performance on cost measures is assessed using Medicare claims data. Based on the performances of MIPS clinicians in these different performance categories, MIPS clinicians receive weighted aggregate scores that range from 0 to 100. This score is used to determine MIPS payment adjustment rates that ranged ±4% in 2017 and ±5% in 2018 with an additional 10% exceptional performance bonus for both years. However, MIPS is a budget-neutral program, thereby changing the MIPS adjustment rates from the stated yearly adjustment rates. The maximum positive payment adjustment with an exceptional performance bonus was 1.88% for the first performance year, 2017, and 1.68% for 2018.8,10,34
Payment Adjustment: ACO versus MIPS
Payment adjustment rates differ based on clinicians’ participation in the 2 QPP tracks. Under the A-APM track, an ACO risk-sharing clinician who meets QPs criteria receives a 5% positive adjustment to their professional service payments. Since A-APM has no performance reporting requirements and penalties, this fixed adjustment rate is guaranteed. MIPS payment adjustment rates, however, can be negative or positive and vary based on a clinician’s performance. Moreover, these rates are further subjected to a budget neutrality clause. All these provisions result in MIPS payment adjustment rates smaller than the stated 4% (2017) and 5% (2018). Within the MIPS program, there is a difference in payment adjustment rates between those who are part of APMs and those who are not. ACO clinicians who participate in the MIPS program (called ACO-MIPS henceforth in the manuscript) receive favorable scoring provisions making them more likely to receive better performance scores than non-ACO MIPS clinicians. These favorable scoring provisions include not being assessed on cost measures additionally under the MIPS program (costs drive shared savings in the ACO model), and comparatively higher weight on the quality score in the total score calculation. Early MIPS performance reports also showed that APMs participating in the MIPS track had higher performance scores.22,23 Since the adjustment rates are calculated based on these performance scores, ACO-MIPS clinicians with higher scores are likely to receive higher positive payment adjustment rates than non-ACO MIPS. Thus, ACO clinicians participating in either of the QPP tracks can receive higher payment adjustment rates than MIPS clinicians.
Conceptual Framework
Under QPP, ACO clinicians receive higher payment adjustment rates than MIPS clinicians. Since the payment adjustments apply to clinicians’ Medicare Part B professional services, clinicians might be motivated to increase their total Part B service payment by increasing the type and volume of Part B services they provide. For example—clinicians with a $100 000 unadjusted medical service payment and a 5% adjustment rate would receive a $105 000 adjusted payment, whereas clinicians with a $50 000 payment with a 5% adjustment rate would receive $52 500. The size of adjusted payments increases as the size of total unadjusted payments increases, given the adjustment rate is fixed. Thus, ACO clinicians have greater motivation to change their behavior in a direction that would increase their adjusted payment. More broadly, at the ACO and MIPS level, we hypothesize that ACO clinicians will have a higher increase in Medicare Part B medical services payments when compared to MIPS clinicians. The payment adjustment rate is comparatively greater for A-APM qualifying ACO risk-sharing clinicians than MIPS-ACO clinicians.27,35 This study hypothesizes that ACO risk-sharing clinicians will have a greater increase in Medicare Part B medical services payments than ACO-MIPS clinicians.
New Contribution
Prior studies have shown that ACO clinicians had higher Medicare Part B spending when compared to non-ACO Fee-for-Service (FFS) clinicians.11 -17 However, these studies were conducted before QPP was implemented in 2017 and compared the spending of ACO clinicians with that of non-ACO FFS clinicians. With the introduction of QPP in 2017, almost all FFS clinicians are exposed to QPP provisions; however, ACO and MIPS clinicians receive incentives that are different in size and nature. Moreover, prior studies have assessed the impact of ACO participation on spending at the ACO-beneficiary level. Since the QPP financial incentives are targeted at the provider level, it is important to evaluate the impact at the provider level by analyzing payments received by clinicians. To our knowledge, this is the first study to evaluate the differential impact of QPP incentives on Medicare Part B medical service payments received by ACO and MIPS clinicians.
Methods
Data Source and Study Participants
We obtained information on Medicare Part B payments received and the characteristics of patients served by clinicians from the Medicare Provider Utilization and Payment Data-Physician and Other Supplier Public Use File (MPUPD-POS PUF) for years 2014 to 2018. 36 We obtained information on clinicians’ participation in ACOs and sub-tracks for 2017 and 2018 using the Alternative Payment Model Provider-level Research Identifiable File (RIF). We identified MIPS-eligible clinicians using the QPP Eligibility Provider-level RIF for 2017-2018. We collected information on clinicians’ participation in the Medicare Shared Savings Program (MSSP) from 2012 to 2016 using the MSSP ACO Provider-level RIF. All RIF datasets were obtained from the Centers for Medicare and Medicaid Services (CMS). Information on county characteristics was obtained from the Area Health Resource File and the CMS Multiple Chronic Conditions datasets.37,38
Our study sample included primary care clinicians who participated either in ACOs (treatment group) or non-ACO MIPS (comparison group) programs during the intervention period (2017-2018). Since ACO clinicians (both ACO risk-sharing and shared savings-only models) receive higher and fixed incentives when compared to MIPS clinicians, ACO clinicians were considered the treatment group, and MIPS clinicians were considered the comparison group in our analyses. ACOs in our study included clinicians participating in ACO risk-sharing (downside) and/or shared savings-only (upside-only) models. MIPS group included clinicians eligible for the MIPS program but not participating in any ACOs or any other types of APMs. We restricted the study sample to primary care clinicians in our study because they are the majority participants in both MIPS and ACO programs.22,23,39,40 Primary care clinicians included physicians, physician assistants, and nurse practitioners. Since the Medicare Shared Savings Program began before 2017, and ACOs were established before 2017, we restricted our sample to clinicians who did not participate in the MSSP before 2017. ACO programs assess clinician’s performance based on total spending per beneficiary served by ACO clinicians. Prior participation in ACO programs might affect clinicians’ behaviors, especially regarding their focus on payments for different types of services. Therefore, excluding prior MSSP participants from the study sample provides a cleaner ACO study sample for this study.
In a separate classification, we identified clinicians participating in ACO risk-sharing/downside models as A-APM eligible ACOs, clinicians under the ACO shared-savings only models (as they are required to participate in MIPS) as ACO-MIPS, and non-ACO MIPS eligible clinicians as non-ACO MIPS clinicians. Our main study sample is a balanced panel sample and included clinicians that had information on dependent and independent variables for all 5 years (2014-2018). To avoid the influence of extreme observations, we exclude clinicians below the first and above 99th percentiles in Part B medical services payments.
Main Measures
We used standardized payments received by clinicians for Medicare Part B medical services because these are the services used for payment adjustments. We used the Consumer Price Index to adjust payment to 2018 dollars.
Covariates
We adjusted for factors that can affect healthcare spending; age, Hierarchical Condition Categories (HCC) risk score, percentage of female beneficiaries, and percentage of white beneficiaries. Prior studies have shown that demographic characteristics like age, gender, and race of patients served by clinicians affect spending and clinicians’ participation in ACO programs.14 -17,41 We accounted for the HCC risk score which helps in predicting expected spending for a patient compared to the average Medicare population. A higher risk score denotes that the patient is sicker and has a relatively higher expected healthcare cost. 42 We also controlled for county characteristics including Health Professional Shortage Area (HPSA) designation, Core-Based Statistical Area (CBSA) classification (1 for metropolitan statistical area and 0 for non-metropolitan (including micropolitan statistical area)), unemployment rate, median household income, and percentage of the TM beneficiaries with multiple chronic conditions.14 -17 Total payments depend on different clinician-level characteristics like number of beneficiaries and volume of services. Therefore, we controlled for the total number of beneficiaries and the total number of services in our study.
Study Design
Standard difference-in-differences designs have 2 groups and 2 time periods that allow us to estimate causal effects under the parallel trend assumption. When there are multiple treatment groups and time periods, researchers often use a common variant of the DID model using unit and time fixed effects.43,44 More specifically, we use two-way (provider and year) fixed effects linear regressions to analyze medical services payments for clinicians. The regression equation for the analysis is:
The dependent variable is standardized payment for a clinician “i” during time “t.” ACO is a dummy variable based on whether clinicians are participating in either an ACO or MIPS during the 2017 to 2018 (intervention) period. The estimate of interest is which is the effect of QPP participation on the Medicare Part B payments for ACO clinicians compared to MIPS clinicians. is provider fixed effect that accounts for time-invariant clinician characteristics. indicates time fixed effect to account for common time trends. X represents covariates—clinician, patient, and county-level characteristics. We used robust standard errors clustered at the clinician level. We utilized an event study design to analyze pre-intervention trends to examine the differences in payments between ACO and MIPS clinicians before the implementation of QPP.
Subgroup Analyses
We conducted several subgroup analyses to understand the source of the impact and the differential impact of payment adjustment rates on different ACO sub-tracks. ACOs under different sub-tracks have different payment adjustment rates based on their participation in either of the 2 QPP tracks. We conducted subgroup analyses to compare payments between clinicians eligible for the A-APM track (ACO risk-sharing clinicians) and clinicians participating in the MIPS track (ACO shared savings-only and non-ACO clinicians in the MIPS program). This comparison is expected to identify the source of the impact and tease out the effect of QPP payment adjustment rates. Additionally, we compared the payment of ACO clinicians who participated in one-sided shared savings-only and two-sided risk-sharing models, and ACO clinicians in either of the sub-tracks with MIPS clinicians.
Sensitivity Analyses
We conducted several sensitivity analyses to examine the validity of our results. Although we excluded payment outliers, we used logged versions of payments as outcomes in one of the sensitivity analyses. The payment adjustment bonus is calculated based on the clinician’s payments for Medicare Part B medical services but does not consider total and drug services payments in calculating the bonus amount. Therefore, we conducted analyses to examine the impact of the program on total and drug services payments under Medicare Part B. We conducted a sensitivity analysis that included the unbalanced panel sample to check whether excluding clinicians without all 5 years’ data affected our main results. Additionally, we conducted a separate analysis to examine the impact on clinicians who started their ACO participation in 2018. Since we excluded clinicians who dropped out of ACO programs in 2018 after participating in 2017, we also analyzed the impact on these clinicians separately.
Results
Our primary study sample included 254 395 observations from 50 879 unique primary care clinicians (ACO = 37.86% and MIPS = 62.14%). ACO and MIPS clinicians at baseline had largely similar beneficiaries in terms of HCC risk score, percentage of female, and white beneficiaries. Similarly, ACO and MIPS clinicians were in counties with similar unemployment rates, and household income (Table 1).
Table 1.
Baseline Characteristics (Years 2014-2016).
| Baseline sample (N = 152 637); Unique clinicians = 50,879 | ||||
|---|---|---|---|---|
| ACO clinicians | MIPS clinicians (N = 94 845; 62.14%) | |||
| Overall (N = 57 792; 37.86%) | #ACO risk-sharing (N = 22 464; 38.87%) | #ACO shared-saving only (N = 35 328; 61.13%) | ||
| Beneficiary characteristics | ||||
| HCC risk score (mean) | 1.58 | 1.61 | 1.56 | 1.61 |
| Age of beneficiaries (mean) | 71.83 | 71.76 | 71.87 | 71.51 |
| Female beneficiaries | 58.73 | 58.40 | 58.94 | 58.12 |
| White beneficiaries | 79.24 | 78.44 | 79.75 | 77.21 |
| County characteristics | ||||
| Unemployment rate | 5.36 | 5.23 | 5.45 | 5.55 |
| Median household income (in thousands) | 58.96 | 61.46 | 57.36 | 58.44 |
| Prevalence of multiple chronic conditions (>1 CC) | 67.62 | 66.42% | 68.38 | 67.35 |
| HPSA: 1 = designated as a shortage area (whole or partial county) | 91.48 | 94.6 | 89.47 | 91.86 |
| CBSA:1 = metropolitan statistical area | 91.56 | 95.19 | 89.25 | 89.36 |
| Clinicians’ characteristics (mean) | ||||
| Total number of beneficiaries | 363 | 331 | 384 | 363 |
| Total number of services | 2236 | 1959 | 2412 | 2495 |
| Total number of beneficiaries with medical services | 363 | 331 | 383 | 363 |
| Total number of medical services | 1610 | 1395 | 1746 | 1694 |
| Total number of beneficiaries with drug services | 69 | 60 | 76 | 67 |
| Total number of drug services | 626 | 564 | 666 | 801 |
| Standardized payment (mean) | ||||
| Total payment | 88 335.72 | 79 197.75 | 94 146.27 | 95 567.41 |
| Total medical services payment | 81 663.81 | 73 161.37 | 87 070.25 | 88 714.16 |
| Total drug payment | 6671.90 | 6036.37 | 7076.02 | 6853.26 |
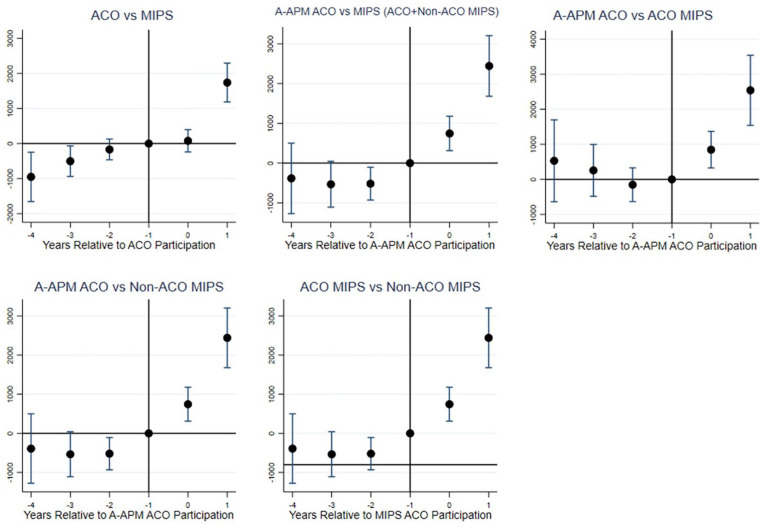
Two-way fixed effects regression results suggest that ACO clinicians had significantly higher medical service payments ($738.69; 95% CI: [343.40, 1133.99]) when compared to MIPS clinicians (Table 2). ACOs eligible for the A-APM track had higher medical services payments ($1533.80; 95% CI: [1003.59, 2064.00]) than ACO and non-ACO MIPS clinicians. Our subgroup analyses showed that ACO clinicians’ higher payments for medical services were driven by clinicians participating in ACO risk-sharing models ($1534.64; 95% CI: [1004.11, 2065.17]). Clinicians under ACO risk-sharing tracks had higher payments for medical services ($1106.71; 95% CI:[446.79, 1766.62]) as compared to those under ACO shared savings-only tracks. However, we did not find a statistically significant difference between ACO (shared savings-only track) and non-ACO MIPS clinicians (Table 2). Event-study analyses suggest no issues of violation of parallel trends assumption in most comparisons (Figure 1). The results from our sensitivity analyses were consistent with our main results (Appendix 1).
Table 2.
Effect of QPP on Medicare Part B Medical Services Payments.
| Regression estimates (95% CI) | Pre-intervention joint test estimate | |
|---|---|---|
| ACO vs MIPS | ||
| Medical services payment (N = 254 395) | 738.69 *** (343.40-1133.99) | 2.51 |
| A-APM eligible ACO vs MIPS [includes both ACO-MIPS and non-ACO MIPS] | ||
| Medical Services Payment (N = 225 955) | 1533.80 *** (1003.59-2064.00) | 2.06 |
| ACO risk sharing vs ACO shared savings-only | ||
| Medical services payment (N = 67 880) | 1106.71 ** (446.79-1766.62) | 1.06 |
| ACO Risk Sharing vs non-ACO MIPS | ||
| Medical services payment (N = 225 890) | 1534.64 *** (1004.11-2065.17) | 2.07 |
| ACO shared savings-only vs non-ACO MIPS | ||
| Medical services payment (N = 225 905) | 203.48 (−295.60 to 702.56) | 2.07 |
Note. We used provider fixed-effect linear regression. Covariates include age of beneficiaries, percentage of white and female beneficiaries, HCC risk score, unemployment rate, median household income (in 1000s), HPSA status, CBSA status, prevalence of multiple chronic conditions, and number of beneficiaries with total, medical, and drug services.
P < .05. **P < .01. ***P < .001; 95% CI in parentheses.
Figure 1.
Yearly medical services payment estimates of ACO versus MIPS clinicians.
Discussion
Our study compared Medicare Part B medical services payments between ACO clinicians in different tracks and MIPS clinicians under the QPP. Findings from this study suggest that ACO clinicians have comparatively higher Medicare Part B medical services payments than MIPS clinicians. Although an increase in Medicare Part B payments of $1534 for ACO clinicians appears relatively small, it constitutes 1.9% of overall baseline Part B medical services payments. It is possible that these higher medical service payments among ACO clinicians could be partly influenced by the higher positive payment adjustment rates offered to these clinicians when compared to MIPS clinicians. However, it must be noted that the practice patterns of ACO clinicians might be influenced by other factors, such as ACO-specific shared savings bonuses. Prior evidence has reported such influence; ACO clinicians received higher payments for physician services for their attributed beneficiaries when compared to non-ACO clinicians.11 -17
We conducted a few subgroup analyses to understand the sources of the payment differences for medical services. ACO sub-tracks are assessed similarly on cost and quality of care. ACO shared savings bonuses are not directly linked to their medical services payments, as these bonuses are calculated based on the total savings they generate.45,46 Our findings of higher medical services payments among ACO risk-sharing clinicians when compared to ACO shared savings-only clinicians may indicate the differential effect of QPP payment adjustments on the medical services payments. Since ACO risk-sharing clinicians receive higher adjustment rates under QPP, it might have played a role in the receipt of higher medical service payment among ACO risk-sharing clinicians when compared to ACO-shared savings-only clinicians. Moreover, a similar indicative effect was reported by another subgroup analysis that compared medical services payments between ACO risk-sharing clinicians and MIPS clinicians (ACO and non-ACO clinicians under the MIPS track). Early performance reports have shown that ACO MIPS clinicians scored better than non-ACO clinicians under the MIPS program in 2017 and 2018.22,23 However, our study did not find a significant difference in medical services payment between ACO and non-ACO MIPS clinicians. This suggests that performance score difference may not translate into a difference in medical services payment due to smaller (<2%) MIPS payment adjustment rates.22,23
This study has an important policy implication. We find that ACO clinicians increased medical services payments relative to MIPS clinicians following QPP. These increased payments may be due to higher payment adjustment rates offered to these ACO clinicians or due to ACOs changing their practice patterns to increase outpatient care with the hope of preventing potentially expensive inpatient care. Policymakers should examine both issues to evaluate QPP’s effectiveness in reducing total spending. Increased use of relatively low-priced services can be crucial in reducing total spending. Earlier studies have shown that ACO clinicians could reduce total spending by substituting relatively expensive inpatient services with inexpensive physician and outpatient services.11 -17 The higher medical services payments observed among ACO primary care clinicians could be such a substitution, thereby potentially slowing Medicare spending growth. QPP provides higher payment adjustment rates to the A-APM participants to encourage clinicians to participate in the APMs, including two-sided risk ACOs. 8 If more clinicians are attracted to ACO risk-sharing models because of higher payments, and if ACOs succeed in generating savings, the increase in physician services payment may play a role in reducing total healthcare costs. Since Medicare pays fixed predetermined fees to clinicians for their services, a possible way to increase payments could be by changing the number and types of services that would increase their Part B payments. Assuming a parallel decrease in more expensive treatments of the conditions, overall spending may decline, generating savings in total Medicare expenditures. Our study was not designed to evaluate total Medicare expenditures, but a future study should examine whether increased medical services payments are offset by a reduction in inpatient expenditures. If there are no corresponding reductions in inpatient expenditures, it is possible that an overuse of Part B medical services leads to increased total expenditures. Clinicians under ACO and MIPS programs are assessed on their performance on the total cost, which might counterbalance such possibility. However, any possibility of such overuse requires continuous attention.
This study has limitations. We excluded specialists from our study to construct appropriate comparison groups. This exclusion should not bias our results because primary care clinicians are the dominant participants in both MIPS track,22,23 and ACO programs.47 -49 However, this exclusion of specialists will limit the generalizability of our study findings to primary care clinicians. Furthermore, we excluded clinicians with extremely low and high payments to minimize the extreme effect of outliers on the results. We excluded clinicians who did not have information on all dependent and independent variables for all 5 years from our primary study sample. Moreover, we excluded clinicians who participated in an ACO in 2017 but dropped out in 2018 from our study population. However, we conducted sensitivity analyses by including those clinicians and found consistent results. We were unable to differentiate QPs and partial QPs from our datasets, therefore, we treated both types of ACO risk-sharing clinicians as A-APM eligible clinicians. QPP experience reports showed that the number of partial QPs was less than 100 in both the 2017 and 2018 performance years.22,23 Thus, the inclusion of partial QPs as A-APM eligible clinicians may have no significant effect on our findings. To isolate the effect of QPP on ACOs and MIPS clinicians, we restricted our sample to clinicians without prior participation in the MSSP. However, there is a likelihood that clinicians in our study sample might have participated in other value-based programs. Due to data limitations, we could not account for participation in other value-based programs. Finally, our study could not assess total healthcare costs due to data limitations. QPP incentives are tied to Part B payments, but total healthcare costs depend on many other factors, including patient-level factors. Such patient-level information is not available in the dataset used for this study.
Conclusion
Our study findings suggest ACO clinicians received higher Medicare Part B medical services payments than MIPS clinicians. These higher payments may be partly due to higher payment adjustment rates offered to these ACO clinicians by QPP and partly due to the change in their practice patterns from their participation in the ACO program. This higher payment was observed more among clinicians participating under ACO risk-sharing models. Our findings provide an early report showing changes in payments for Medicare Part B medical services between ACO and MIPS clinicians following QPP implementation. Payment change requires time to show effect, and future studies should investigate long-term effects. Moreover, payment adjustment rates and performance thresholds for receiving bonuses are scheduled to increase for MIPS clinicians with each passing year. It is, therefore, necessary to continue studying the impact of these increasing bonuses on Medicare Part B medical services payments. One of the main objectives of QPP is to minimize the total cost of care. Since the payment adjustment rates are applied to Medicare Part B professional services payments, the focus of this study was to analyze the impact on Part B payments. Future research could be conducted to analyze the impact of QPP on the total cost of care by analyzing combined payments for Medicare Part A and B services.
Supplemental Material
Supplemental material, sj-docx-1-inq-10.1177_00469580241240177 for ACO Clinicians Have Higher Medicare Part B Medical Services Payments Than MIPS Clinicians Under the Quality Payment Program by Mina Shrestha, Hari Sharma and Keith J. Mueller in INQUIRY: The Journal of Health Care Organization, Provision, and Financing
Footnotes
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding: The author(s) received no financial support for the research, authorship, and/or publication of this article.
Research Ethics and Patient Consent: Not applicable.
ORCID iD: Mina Shrestha  https://orcid.org/0000-0002-8497-8051
https://orcid.org/0000-0002-8497-8051
Supplemental Material: Supplemental material for this article is available online.
References
- 1. Muhlestein D, Burton N, Winfield L. The changing payment landscape of current CMS payment models foreshadows future plans. Health Affairs Blog. 2017. [Google Scholar]
- 2. Guterman S. Wielding the carrot and the stick: how to move the U.S. health care system away from fee-for-service payment. The Commonwealth Fund Blog; 2013. Accessed December 10, 2023. https://www.commonwealthfund.org/blog/2013/wielding-carrot-and-stick-how-move-us-health-care-system-away-fee-service-payment. [Google Scholar]
- 3. Findlay S. Medicare’s New Physician Payment System. Health Affairs Health Policy Brief. 2016. [Google Scholar]
- 4. Blumenthal D, Davis K, Guterman S. Medicare at 50–origins and evolution. New Engl J Med. 2015;372(5):479-486. [DOI] [PubMed] [Google Scholar]
- 5. Anderson G, Davis K, Guterman S. Medicare payment reform: aligning incentives for better care. Issue Brief. 2015;20:1-12. [PubMed] [Google Scholar]
- 6. Novikov D, Cizmic Z, Feng JE, Iorio R, Meftah M. The historical development of value-based care: how we got here. J Bone Joint Surg Am. 2018;100(22):e144. [DOI] [PubMed] [Google Scholar]
- 7. Altman D, Frist WH. Medicare and medicaid at 50 years: perspectives of beneficiaries, health care professionals and institutions, and policy makers. JAMA. 2015;314(4):384-395. [DOI] [PubMed] [Google Scholar]
- 8. Department of Health and Human Services, Centers for Medicare and Medicaid Services. Quality payment program. 2016. Accessed July 31, 2023. https://www.federalregister.gov/d/2016-25240
- 9. Burwell SM. Setting value-based payment goals–HHS efforts to improve U.S. health care. New Engl J Med. 2015;372(10):897-899. [DOI] [PubMed] [Google Scholar]
- 10. Rosenkrantz AB, Nicola GN, Allen B, Jr, Hughes DR, Hirsch JA. Macra, MIPS, and the new medicare quality payment program: an update for radiologists. J Am Coll Radiol. 2017;14(3):316-323. [DOI] [PubMed] [Google Scholar]
- 11. McWilliams JM, Gilstrap LG, Stevenson DG, et al. Changes in postacute care in the medicare shared savings program. JAMA Intern Med. 2017;177(4):518-526. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12. Abrams M, Nuzum R, Zezza M, et al. The affordable care act’s payment and delivery system reforms: a progress report at five years. Issue Brief. 2015;12:1-16. [PubMed] [Google Scholar]
- 13. Centers for Medicare and Medicaid Services. Medicare accountable care organizations 2015 performance year quality and financial results. Centers for Medicare and Medicaid Services; 2016. Accessed April 2020. [Google Scholar]
- 14. McWilliams JM, Chernew ME, Landon BE, Schwartz AL. Performance differences in year 1 of pioneer accountable care organizations. New Engl J Med. 2015;372(20):1927-1936. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15. McWilliams JM, Hatfield LA, Chernew ME, Landon BE, Schwartz AL. Early performance of accountable care organizations in medicare. New Engl J Med. 2016;374(24):2357-2366. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16. Kury FSP, Baik SH, McDonald CJ. Analysis of healthcare cost and utilization in the first two years of the Medicare shared savings program using Big Data from the CMS enclave. AMIA Annu Symp Proc. 2016;2016:724-733. [PMC free article] [PubMed] [Google Scholar]
- 17. McWilliams JM. Changes in medicare shared savings program savings from 2013 to 2014. JAMA. 2016;316(16):1711-1713. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18. Quality Payment Program. Advanced alternative payment models (APMs). Quality Payment Program; 2017. Accessed December 12, 2021. https://qpp.cms.gov/apms/advanced-apms?py=2018 [Google Scholar]
- 19. Muhlestein D, Bleser W, Saunders R, et al. Spread of ACOs and value-based payment models in 2019: gauging the impact of pathways to success. Health Affairs Blog. 2019. [Google Scholar]
- 20. Muhlestein D, Saunders R, Richards R, McClellan M. Recent progress in the value journey: growth of ACOs and value-based payment models in 2018. Health Affairs Blog. 2018. [Google Scholar]
- 21. Muhlestein D, Saunders R, McClellan M. Growth of ACOs and alternative payment models in 2017. Health Affairs Blog. 2017. [Google Scholar]
- 22. Quality Payment Program. 2017 Quality payment program experience report. Quality Payment Program, Centers for Medicare and Medicaid Services; 2019. Accessed June 20, 2022. https://qpp-cm-prod-content.s3.amazonaws.com/uploads/491/2017%20QPP%20Experience%20Report.pdf [Google Scholar]
- 23. Quality Payment Program. 2018 Quality payment program experience report. Centers for Medicare and Medicaid Services; 2020. Accessed April 7, 2022. https://qpp-cm-prod-content.s3.amazonaws.com/uploads/1091/2018%20QPP%20Experience%20Report.pdf [Google Scholar]
- 24. Nyweide DJ, Lee W, Cuerdon TT, et al. Association of pioneer accountable care organizations vs traditional medicare fee for service with spending, utilization, and patient experience. JAMA. 2015;313(21):2152-2161. [DOI] [PubMed] [Google Scholar]
- 25. Kaufman BG, Spivack BS, Stearns SC, Song PH, O'Brien EC. Impact of accountable care organizations on utilization, care, and outcomes: a systematic review. Med Care Res Rev. 2019;76(3):255-290. [DOI] [PubMed] [Google Scholar]
- 26. McWilliams JM, Hatfield LA, Landon BE, Hamed P, Chernew ME. Medicare spending after 3 years of the medicare shared savings program. New Engl J Med. 2018;379(12):1139-1149. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27. National Association of ACOs. The ACO Guide to MACRA. National association of ACOs. 2018. Accessed January 24, 2022. https://naacos.memberclicks.net/assets/docs/pdf/macra/TheACOGuidetoMACRA_2018EditionFullReport080118.pdf
- 28. Quality Payment Program. Quality Measures Requirements. 2018 Quality requirements. Centers for Medicare and Medicaid Services; 2018. Accessed June 9, 2022. https://qpp.cms.gov/mips/quality-requirements?py=2018 [Google Scholar]
- 29. Quality Payment Program. Quality Measures Requirements. 2017 Quality requirements. Centers for Medicare and Medicaid Services; 2017. Accessed June 28, 2022. https://qpp.cms.gov/mips/quality-requirements?py=2017 [Google Scholar]
- 30. Quality Payment Program. Promoting Interoperability Requirements. 2017 Promoting interoperability requirements. Centers for Medicare and Medicaid Services; 2017. Accessed June 9, 2022. https://qpp.cms.gov/mips/promoting-interoperability?py=2017 [Google Scholar]
- 31. Quality Payment Program. Promoting Interoperability Requirements. 2018 Promoting Interoperability Requirements. Centers for Medicare and Medicaid Services; 2018. Accessed June 9, 2022. https://qpp.cms.gov/mips/promoting-interoperability?py=2018 [Google Scholar]
- 32. Quality Payment Program. Improvement Activities Performance Category: Traditional MIPS requirements. 2017 Improvement activities requirements. Centers for Medicare and Medicaid Services; 2017. Accessed June 9, 2022. https://qpp.cms.gov/mips/improvement-activities?py=2017 [Google Scholar]
- 33. Quality Payment Program. Improvement Activities Performance Category: Traditional MIPS requirements. 2018 Improvement activities requirements. Centers for Medicare and Medicaid Services; 2018. Accessed June 9, 2022. https://qpp.cms.gov/mips/improvement-activities?py=2018 [Google Scholar]
- 34. Simons JP, Woo K, Rathbun JA, Johnson BL, Copeland TP. Quality measures in the merit-based Incentive Payment System. J Vasc Surg. 2018;68(3):931-932. [DOI] [PubMed] [Google Scholar]
- 35. National Association of ACOs. The ACO Guide to MACRA. National Association of ACOs. 2019. Accessed January 24, 2022. https://naacos.memberclicks.net/assets/docs/pdf/macra/TheACO_GuidetoMACRA_2019EditionFullReport022019v2.pdf
- 36. Centers for Medicare and Medicaid Services. Medicare physician & other practitioners - by provider and service. Centers for Medicare and Medicaid Services; 2021. Accessed June 25, 2022. https://data.cms.gov/provider-summary-by-type-of-service/medicare-physician-other-practitioners/medicare-physician-other-practitioners-by-provider-and-service [Google Scholar]
- 37. Health Resources and Services Administration. Area health resources files. Health Resources and Services Administation; 2022. Accessed June 22, 2022. https://data.hrsa.gov/topics/health-workforce/ahrf [Google Scholar]
- 38. Centers for Medicare and Medicaid Services. Multiple chronic conditions. Centers for Medicare and Medicaid Services. 2021. Accessed June 22, 2022. https://data.cms.gov/medicare-chronic-conditions/multiple-chronic-conditions [Google Scholar]
- 39. McWilliams JM. Accountable care organizations: a challenging opportunity for primary care to demonstrate its value. J Gen Intern Med. 2014;29(6):830-831. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40. American Medical Association. A majority of physicians now take part in an ACO. American Medical Association; 2019. Accessed June 12, 2022. https://www.ama-assn.org/practice-management/payment-delivery-models/majority-physicians-now-take-part-aco [Google Scholar]
- 41. Schwartz AL, Chernew ME, Landon BE, McWilliams JM. Changes in low-value services in year 1 of the medicare pioneer accountable care organization program. JAMA Intern Med. 2015;175(11):1815-1825. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42. Hoffman AF, Reiter KL, Randolph RK. Average Beneficiary CMS Hierarchical Condition Category (HCC) Risk Scores for Rural and Urban Providers. Sheps Center for Health Services Research; 2018. [Google Scholar]
- 43. Wing C, Simon K, Bello-Gomez RA. Designing difference in difference studies: best practices for public health policy research. Annu Rev Public Health. 2018;39(1):453-469. [DOI] [PubMed] [Google Scholar]
- 44. Harper S, Strumpf EC, Kaufman JS. Do medical Marijuana laws increase marijuana use? Replication study and extension. Ann Epidemiol. 2012;22(3):207-212. [DOI] [PubMed] [Google Scholar]
- 45. Centers for Medicare and Medicaid Services. SSP fact sheet. Centers for Medicare and Medicaid Services; 2017. Accessed January 24, 2022. https://www.cms.gov/Medicare/Medicare-Fee-for-Service-Payment/sharedsavingsprogram/Downloads/2017-MSSP-Fact-Sheet.pdf [Google Scholar]
- 46. Physician Advocacy Institute, Healthsperien. Medicare shared savings program (MSSP) accountable care organizations overview. Physician Advocacy Institute; 2022. Accessed June 12, 2022. http://www.physiciansadvocacyinstitute.org/Portals/0/assets/docs/Advanced-APM-Pathway/Medicare%20Shared%20Savings%20Program%20Overview.pdf [Google Scholar]
- 47. Muhlestein D, Tu T, Colla CH. Accountable care organizations are increasingly led by physician groups rather than hospital systems. Am J Manag Care. 2020;26(5):225-228. [DOI] [PubMed] [Google Scholar]
- 48. Mechanic RE. Aligning specialist physicians with accountable care organizations. The American Journal of Accountable Care. 2022;10:5-6. [Google Scholar]
- 49. Council of Accountable Physician Practices. Characteristics and performance of ACOs and accountable physician groups: what does the evidence tell us? 2021. Accessed December 12, 2023. https://www.institute4ac.org/wp-content/uploads/2021/09/capp_IAC_aco_paper.pdf
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Supplemental material, sj-docx-1-inq-10.1177_00469580241240177 for ACO Clinicians Have Higher Medicare Part B Medical Services Payments Than MIPS Clinicians Under the Quality Payment Program by Mina Shrestha, Hari Sharma and Keith J. Mueller in INQUIRY: The Journal of Health Care Organization, Provision, and Financing