Abstract
Introduction
Ultrasound-guided quadratus lumborum block and erector spinae plane block are widely used for postoperative analgesia in adult patients undergoing abdominal surgeries. This protocol aims to compare the analgesic effects between ultrasound-guided quadratus lumborum block and erector spinae plane block on postoperative pain in abdominal surgeries.
Methods and analysis
Four databases, including PubMed, EMBASE, Web of Science and the Cochrane Central Register of Controlled Trials (CENTRAL), will be searched. Randomised controlled trials that compared the analgesic effects between ultrasound-guided quadratus lumborum block and erector spinae plane block on postoperative pain in adult patients will be identified. The primary outcomes are time to the first analgesic request and postoperative analgesic consumption over 24 hours. Secondary outcomes will include postoperative pain scores and the incidence of side effects. RevMan V.5.3 software will be used for data processing and statistical analysis. The Grading of Recommendation, Assessment, Development and Evaluation approach will be used to assess the evidence quality of outcomes.
Ethics and dissemination
Ethical approval is not required for this study. Results of this present study will be submitted to a peer-reviewed journal.
PROSPERO registration number
CRD42023445802.
Keywords: Meta-Analysis, Adult anaesthesia, Pain management
STRENGTHS AND LIMITATIONS OF THIS STUDY.
High clinical heterogeneity might exist among studies due to the surgery type, the length and location of the incision, anaesthesia type, local anaesthetic and adjuvants.
We will explore the source of heterogeneity by subgroup analysis and meta-regression, which may also identify the preferred nerve block type for specific surgery types.
The Grading of Recommendation, Assessment, Development and Evaluation approach will assess the quality of evidence and provide guidance for the clinical application of ultrasound-guided quadratus lumborum block and erector spinae plane block.
Introduction
Regional anaesthesia contributes to an important component of the multimodal analgesia strategy by reducing postoperative pain intensity and opioid consumption.1–4 With advancements in ultrasound techniques, various peripheral nerve blocks have been widely used for many surgery types. Ultrasound-guided quadratus lumborum block, first reported in 2007, is effective in providing postoperative analgesia for abdominal surgeries by spreading the local anaesthetic across the quadratus lumborum muscle to block the intermuscular nerves.5 The ultrasound-guided erector spinae plane block was first reported in 20166 and can block both somatic and visceral pain by delivering the local anaesthetic to the paravertebral space and blocking the ventral and dorsal rami of spinal nerves.7 Currently, an increasing number of randomised controlled trials (RCTs) have compared the analgesic effects between ultrasound-guided quadratus lumborum block and erector spinae plane block on postoperative pain in abdominal surgeries,8–13 but the results were not consistent. Therefore, it is worthwhile to perform a systematic review and meta-analysis to determine whether ultrasound-guided erector spinae plane block is superior to ultrasound-guided quadratus lumborum block in postoperative analgesia for patients undergoing abdominal surgeries.
Methods and analysis
Study registration
This protocol was registered in the International Prospective Register of Systematic Reviews (ID: CRD42023445802). This protocol is conducted in line with the Preferred Reporting Items for Systematic Review and Meta-Analysis Protocols. Ethical approval is not applicable.
Search strategy
Four databases, including PubMed, EMBASE, Web of Science and the Cochrane Central Register of Controlled Trials (CENTRAL), will be searched from their inception to 16 January 2024. English language will be restricted. Search terms will include “quadratus lumborum block”, “erector spinae plane block” and “randomized controlled trials”. The strategy for the PubMed search is described in table 1.
Table 1.
Search strategy for PubMed
| No | Search terms |
| #1 | Quadratus lumborum block(Title/Abstract) |
| #2 | Erector spinae plane block(Title/Abstract) |
| #3 | #1 AND #2 |
| #4 | Randomized controlled trial(Title/Abstract) |
| #5 | Clinical trial randomized(Title/Abstract) |
| #6 | Controlled clinical trial(Title/Abstract) |
| #7 | Clinical trial(Title/Abstract) |
| #8 | Randomized(Title/Abstract) |
| #9 | Trial(Title/Abstract) |
| #10 | #4 OR #5 OR #6 OR #7 OR #8 OR #9 |
| #11 | #3 AND #10 |
Inclusion and exclusion criteria
Inclusion criteria will be the followings: (1) Study design: RCTs; (2) Participants: adult patients (>18 years) undergoing abdominal surgeries; (3) Comparisons: quadratus lumborum block versus erector spinae plane block and (4) Primary outcomes: time to the first analgesic request and postoperative analgesic consumption over 24 hours; secondary outcomes: pain scores at 2 hours, 4 hours, 8 hours, 12 hours and 24 hours postoperatively, and the incidence of side effects. Non-RCTs, such as retrospective studies, reviews, meta-analyses, case reports and paediatric studies, will be excluded.
Study selection
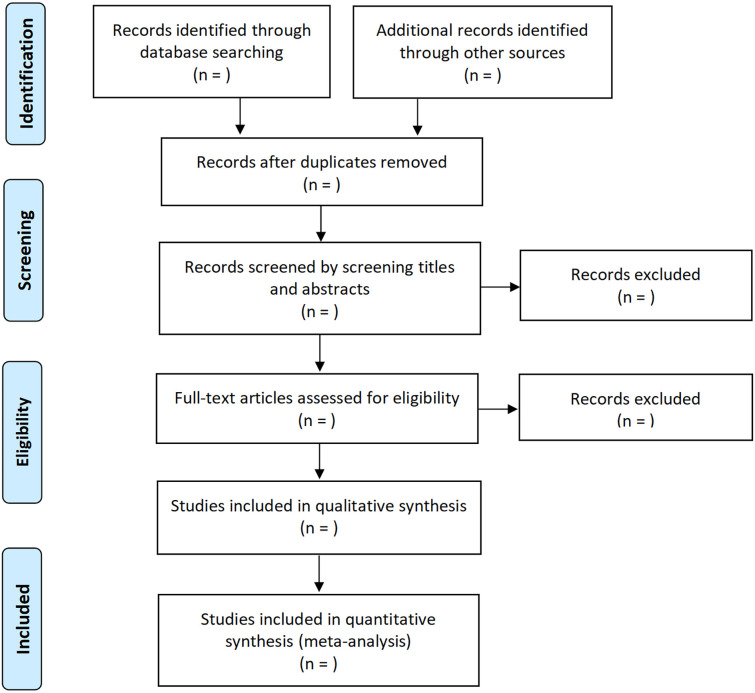
The titles and abstracts of initially identified studies will first be screened by two authors (XZ and DZ). Then, the full texts of potentially relevant studies will be reviewed. Disagreements will be discussed with another author (XW). The flow chart of study selection is shown in figure 1.
Figure 1.
The flow chart of study selection.
Data extraction
The following information will be extracted from the included studies by two independent authors (XZ and DZ): authors and published year, settings, sample size, characteristics of participants, surgery type, the approach of quadratus lumborum block, type of anaesthesia, comparisons, outcomes and analgesic strategy for perioperative pain.
Risk of bias assessment
The risk of bias will be assessed using the Cochrane Collaboration’s tool, which includes: (1) random sequence generation and allocation concealment (selection bias); (2) blinding of participants and personnel (performance bias); (3) blinding of outcome assessment (detection bias); (4) incomplete outcome data (attrition bias) and (5) selective reporting (reporting bias). Each estimation will be reported as ‘low’, ‘high’ or ‘unclear’. Disagreements will be resolved by discussion with a third author (XW).
Statistical analysis
RevMan V.5.3 software (The Nordic Cochrane Centre, The Cochrane Collaboration, 2014) will be used for statistical analysis. Continuous data will be presented as the mean differences with 95% CIs, while dichotomous data will be calculated by risk ratios (RR) with 95% CI. The I2 test will reflect the statistical heterogeneity. Data will be synthesised either by a fixed-effect model (I2<50%, low heterogeneity) or by a random-effect model (I2>50%, high heterogeneity), and subgroup analysis and meta-regression will be conducted to explore the source of heterogeneity. Sensitivity analyses will further assess whether the results are robust and reliable. A p<0.05 indicates statistical significance. The Grading of Recommendation, Assessment, Development and Evaluation (GRADE) approach will be used to evaluate the quality of evidence for outcomes.
Patient and public involvement
Not applicable.
Ethics and dissemination
The ethical approval is not required for this study. The results will be submitted to a peer-reviewed journal.
Discussion
Currently, ultrasound-guided quadratus lumborum block and erector spinae plane block are commonly used for postoperative analgesia in various abdominal surgeries, such as laparoscopic cholecystectomy, laparoscopic sleeve gastrectomy, caesarean section, hysterectomy and open nephrectomy. In this protocol, we will not specify the type of abdominal surgeries, so we can perform subgroup analysis according to the surgery types, which may recommend preferred nerve block type for specific surgery type. Therefore, this protocol will include RCTs regardless of the types of abdominal surgeries.
The quadratus lumborum block usually can be achieved through four approaches, including lateral, posterior, anterior and intramuscular quadratus lumborum block. In this protocol, we will include RCTs regardless of the quadratus lumborum block approaches, and we aim to perform subgroup analysis according to these different approaches, which may recommend a preferred approach of quadratus lumborum block for specific surgery.
In terms of the outcomes, it should be noticed that the design methodologies of the included RCTs will influence the pooled results of each outcome, thus making it difficult to designate one of these outcomes as a gold standard for all included studies. Moreover, the outcome of total postoperative analgesic consumption may be susceptible to the nonlinear interactions between the study drug and the rescue medication. It should also be considered that high clinical heterogeneity might exist among studies due to the surgery type, the length and location of the incision, the anaesthesia type, the local anaesthetic and adjuvants. Therefore, it is necessary to explore the source of heterogeneity by subgroup analysis and meta-regression. Finally, the GRADE approach will assess the quality of evidence and provide guidance for the clinical application of ultrasound-guided quadratus lumborum block and erector spinae plane block.
Supplementary Material
Footnotes
Contributors: Conceptualisation: XZ and DZ. Data curation: XZ and YW. Formal analysis: XZ and YW. Methodology: XZ and XW. Validation: XZ and XW. Writing–original draft: XZ and DZ. Writing–review and editing: YW and XW.
Funding: This work was supported by grant no. 2022NSFSC1399 (To DZ) from the Natural Science Foundation of Sichuan Province.
Competing interests: None declared.
Patient and public involvement: Patients and/or the public were not involved in the design, or conduct, or reporting, or dissemination plans of this research.
Provenance and peer review: Not commissioned; externally peer reviewed.
Ethics statements
Patient consent for publication
Not applicable.
References
- 1. Finnerty O, Carney J, McDonnell JG. Trunk blocks for abdominal surgery. Anaesthesia 2010;65 Suppl 1:76–83. 10.1111/j.1365-2044.2009.06203.x [DOI] [PubMed] [Google Scholar]
- 2. Guerra-Londono CE, Privorotskiy A, Cozowicz C, et al. Assessment of Intercostal nerve block analgesia for thoracic surgery: a systematic review and meta-analysis. JAMA Netw Open 2021;4:e2133394. 10.1001/jamanetworkopen.2021.33394 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3. Grape S, Kirkham KR, Akiki L, et al. Transversus abdominis plane block versus local anesthetic wound infiltration for optimal analgesia after laparoscopic cholecystectomy: a systematic review and meta-analysis with trial sequential analysis. J Clin Anesth 2021;75:110450. 10.1016/j.jclinane.2021.110450 [DOI] [PubMed] [Google Scholar]
- 4. Ní Eochagáin A, Singleton BN, Moorthy A, et al. Regional and neuraxial anaesthesia techniques for spinal surgery: a scoping review. Br J Anaesth 2022;129:598–611. 10.1016/j.bja.2022.05.028 [DOI] [PubMed] [Google Scholar]
- 5. Kang W, Lu D, Yang X, et al. Postoperative analgesic effects of various quadratus lumborum block approaches following cesarean section: a randomized controlled trial. J Pain Res 2019;12:2305–12. 10.2147/JPR.S202772 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6. Forero M, Adhikary SD, Lopez H, et al. The erector spinae plane block: a novel analgesic technique in thoracic neuropathic pain. Reg Anesth Pain Med 2016;41:621–7. 10.1097/AAP.0000000000000451 [DOI] [PubMed] [Google Scholar]
- 7. Tulgar S, Ahiskalioglu A, De Cassai A, et al. Efficacy of bilateral erector spinae plane block in the management of pain: current insights. J Pain Res 2019;12:2597–613. 10.2147/JPR.S182128 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8. Hassanein A, Abdel-Haleem M, Mohamed SR. Regional analgesia for laparoscopic cholecystectomy using ultrasound-guided quadratus lumborum block or erector spinae block: a randomized controlled trial. Pain Physician 2023;26:E133–41. [PubMed] [Google Scholar]
- 9. Ashoor TM, Jalal AS, Said AM, et al. Ultrasound-guided techniques for postoperative analgesia in patients undergoing laparoscopic sleeve gastrectomy: erector spinae plane block vs. Pain Physician 2023;26:245–56. [PubMed] [Google Scholar]
- 10. Priya TK, Singla D, Talawar P, et al. Comparative efficacy of quadratus lumborum type-II and erector spinae plane block in patients undergoing caesarean section under spinal anaesthesia: a randomised controlled trial. Int J Obstet Anesth 2023;53:103614. 10.1016/j.ijoa.2022.103614 [DOI] [PubMed] [Google Scholar]
- 11. Onay M, Erdoğan Kayhan G, Özen A, et al. Comparison of ultrasound-guided quadratus lumborum block and erector spinae plane block in terms of their effects on postoperative pain in open nephrectomy. Minerva Anestesiol 2023;89:32–9. 10.23736/S0375-9393.22.16635-6 [DOI] [PubMed] [Google Scholar]
- 12. Aygun H, Kavrut Ozturk N, Pamukcu AS, et al. Comparison of ultrasound guided erector spinae plane block and quadratus lumborum block for postoperative analgesia in laparoscopic cholecystectomy patients; a prospective randomized study. J Clin Anesth 2020;62:109696. 10.1016/j.jclinane.2019.109696 [DOI] [PubMed] [Google Scholar]
- 13. Aksu C, Şen MC, Akay MA, et al. Erector Spinae plane block vs quadratus lumborum block for pediatric lower abdominal surgery: a double blinded, prospective, and randomized trial. Journal of Clinical Anesthesia 2019;57:24–8. 10.1016/j.jclinane.2019.03.006 [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.