Abstract
Background
Palliative care performed a central role in responding to the systemic suffering incurred by the COVID-19 pandemic. Yet, few studies have elucidated the inpatient palliative care specialists’ experiences and perceptions.
Objective
Systematically review and synthesize the evolving roles and expectations of inpatient palliative care specialists in response to COVID-19.
Design
A systematic review and meta-synthesis informed by Thomas and Harden’s framework and Pozzar et al.’s approach was conducted in accordance with Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) guidelines.
Data Sources
MEDLINE, EMBASE, CINAHL, and PubMed were systematically searched for articles published between December 2019 and March 2023. We included all peer-reviewed qualitative and mixed-method literature studying the roles and expectations of inpatient palliative care specialists. A mixed-method appraisal tool was used for quality assessment.
Results
Of 3869 unique articles, 52 were included. Studies represented North American (n = 23), European (n = 16), South American (n = 4), Oceanic (n = 2), Asian (n = 2), West African (n = 1), Middle Eastern (n = 1), and inter-continental settings (n = 3). Most were reported in English (n = 50), conducted in 2020 (n = 28), and focused on the perspectives of inpatient palliative care clinicians (n = 28). Three descriptive themes captured the roles and expectations of inpatient palliative care specialists: shifting foundations, reorienting to relationships, and evolving identity. Two analytical themes were synthesized: palliative care propagates compassion through a healing presence, and palliative care enhances the systemic response to suffering through nimble leadership.
Conclusion
Inpatient palliative care specialists responded to the COVID-19 pandemic by establishing their healing presence and leading with their adaptability. To develop institutionally tailored and collaborative responses to future pandemics, future studies are needed to understand how inpatient palliative care clinicians are recognized and valued within their institutions.
Supplementary Information
The online version contains supplementary material available at 10.1007/s11606-023-08564-y.
KEY WORDS: palliative care, interprofessional care, collaboration, COVID-19, pandemic, meta-synthesis, roles, expectations
INTRODUCTION
The COVID-19 pandemic devastated the lives and livelihoods of millions of families globally.1 Beyond its immediate health impacts, COVID-19 tested healthcare providers and systems in their ability to deliver optimal care amidst unpredictable workloads, insufficient support, and exceptional uncertainty.2–4 Given that palliative care specialists are professionally trained in managing clinical uncertainty and providing individualized support in challenging emotional situations, palliative care may have been uniquely positioned to support patients, families, and interdisciplinary teams in the pandemic context.3–6
Emerging evidence investigating the effectiveness of inpatient palliative care during COVID-19 has demonstrated a multitude of positive outcomes. These benefits ranged from increased hospital efficiency to decreased uncertainty for patients and families during the end-of-life period.4,7–10 Moreover, core aspects of palliative care, including adequate symptom management, sensitive communication, and aid in complex decision-making, are now recognized as fundamental to healthcare provision more broadly.10 Despite acknowledgment of the importance of integrating palliative care into pandemic planning, very few studies have elucidated the roles and expectations of inpatient palliative care teams during a pandemic.2,3,7–9,11–13 Therefore, illuminating a holistic picture of inpatient palliative care’s role in a pandemic setting remains a priority.
This study aims to use a sociological lens to systematically review and synthesize how the roles and expectations of inpatient palliative care clinicians have evolved through the COVID-19 pandemic. By triangulating perspectives across individual, interpersonal, and institutional levels, we hope to better understand the impact of the pandemic on palliative care clinicians, characterize palliative care’s effectiveness amidst a pandemic, and facilitate palliative care integration into future pandemic responses.
METHODS
Registration
The study has been registered on PROSPERO, an international database of systematic reviews (CRD42022346213).
Search Strategy
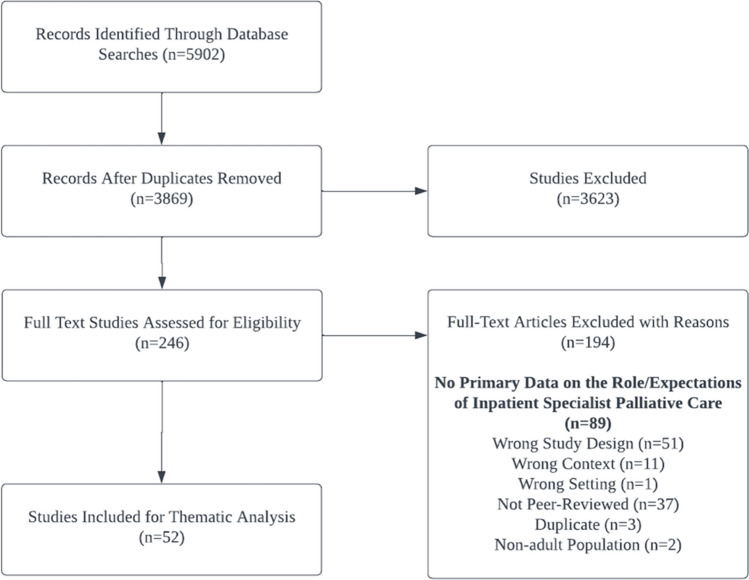
Informed by Thomas and Harden’s methods,14 we conducted a systematic review and thematic synthesis of articles published between December 2019 and March 2023 while following the Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) guidelines and the Enhancing Transparency in Reporting the Synthesis of Qualitative Research (ENTREQ) statement.15 We chose December 2019 as the index month in alignment with the index case of COVID-19. In collaboration with our institutional research librarian (CW), we searched MEDLINE, EMBASE, CINAHL, and PubMed for potentially eligible articles (Table 1). We conducted the original search in August 2022, and an updated search in March 2023. We included articles for review and synthesis if they (a) were original peer-reviewed manuscripts, (b) employed qualitative or mixed methods, and (c) had findings related to the experiences or perceptions of inpatient palliative care specialists (Table 2). Three authors (DWZ, SGR, ZJ) independently screened article titles and abstracts to identify potentially eligible articles, and then assessed full-text articles for relevant findings (Fig. 1).
Table 1.
Database Search Strategy and Results
| Database | search strategy | Records retrieved; August 2020 | Records retrieved; March 2023 |
|---|---|---|
|
MEDLINE 1 COVID-19/ or exp COVID-19 Testing/ or COVID-19 Vaccines/ or SARS-CoV2/ 2 (coronavirus/ or betacoronavirus/ or coronavirus infections/) and (disease outbreaks/ or epidemics/ or pandemics/) 3 (nCoV* or 2019nCoV or 19nCoV or COVID19* or COVID or SARS-COV-2 or SARSCOV-2 or SARS-COV2 or SARSCOV2 or SARS coronavirus 2 or Severe Acute Respiratory Syndrome Coronavirus 2 or Severe Acute Respiratory Syndrome Corona Virus 2).ti,ab,kf,nm,ot,ox,rx,px. 4 ((new or novel or "19" or "2019" or Wuhan or Hubei or China or Chinese) adj3 (coronavirus* or corona virus* or betacoronavirus* or CoV or HCoV)).ti,ab,kf,ot. 5 (longCOVID* or postCOVID* or postcoronavirus* or postSARS*).ti,ab,kf,ot. 6 ((coronavirus* or corona virus* or betacoronavirus*) adj3 (pandemic* or epidemic* or outbreak* or crisis)).ti,ab,kf,ot. 7 ((Wuhan or Hubei) adj5 pneumonia).ti,ab,kf,ot. 8 1 or 2 or 3 or 4 or 5 or 6 or 7 9 limit 8 to yr="2019 -Current" 10 (pandemic* or epidemic*).ti,ab. 11 Palliative Care/ or "Hospice and Palliative Care Nursing"/ or Palliative Medicine/ 12 (palliative* or hospice* or "end of life").ti,ab. 13 disease outbreaks/ or epidemics/ or pandemics/ 14 9 or 10 or 13 15 11 or 12 16 14 and 15 |
1534 | 590 |
|
EMBASE 1sars-related coronavirus/ 2(coronavirinae/ or betacoronavirus/ or coronavirus infection/) and (epidemic/ or pandemic/) 3(nCoV* or 2019nCoV or 19nCoV or COVID19* or COVID or SARS-COV-2 or SARSCOV-2 or SARS-COV2 or SARSCOV2 or SARS coronavirus 2 or Severe Acute Respiratory Syndrome Coronavirus 2 or Severe Acute Respiratory Syndrome Corona Virus 2).ti,ab,kw,hw,ot. 4((new or novel or "19" or "2019" or Wuhan or Hubei or China or Chinese) adj3 (coronavirus* or corona virus* or betacoronavirus* or CoV or HCoV)).ti,ab,kw,hw,ot. 5(longCOVID* or postCOVID* or postcoronavirus* or postSARS*).ti,ab,kw,hw,ot. 6((coronavirus* or corona virus* or betacoronavirus*) adj3 (pandemic* or epidemic* or outbreak* or crisis)).ti,ab,kw,ot. 7((Wuhan or Hubei) adj5 pneumonia).ti,ab,kw,ot. 81 or 2 or 3 or 4 or 5 or 6 or 7 9limit 8 to yr="2019 -Current" 10pandemic*.ti,ab. 11palliative nursing/ or palliative therapy/ 12(palliative* or hospice* or "end of life").ti,ab. 1311 or 12 149 or 10 1513 and 14 16limit 15 to exclude medline journals |
454 | 666 |
|
CINAHL 1 (MH "COVID-19+") 2 (MH "Coronavirus+") OR (MH "COVID-19 Pandemic") 3 (MH "Disease Outbreaks+") 4 TI ( 2019-nCoV OR 2019nCoV OR COVID-19 OR SARS-CoV-2 OR coronavirus* or pandemic* ) OR AB ( 2019-nCoV OR 2019nCoV OR COVID-19 OR SARS-CoV-2 OR coronavirus* or pandemic* ) 5 S1 OR S2 OR S3 OR S4 6 (MH "Hospice and Palliative Nursing") OR (MH "Palliative Medicine") OR (MH "Hospice Care") OR (MH "Terminal Care+") 7 TI ( palliative* or hospice* or "end of life" ) OR AB ( palliative* or hospice* or "end of life" ) 8 S6 OR S7 9 S5 AND S8 10 S5 AND S8 Limit 2019-current 11 S5 AND S8 Exclude MEDLINE records |
942 | 419 |
|
Pubmed COVID-19 [mh] OR COVID-19 Testing[mh] OR COVID-19 Vaccines[mh] OR SARS-CoV-2[mh] OR spike glycoprotein, COVID-19 virus [Supplementary Concept] OR ((Coronavirus[mh:noexp] OR Betacoronavirus[mh:noexp] OR Coronavirus Infections[mh:noexp]) AND (Disease Outbreaks[mh:noexp] OR Epidemics[mh:noexp] OR Pandemics[mh])) OR nCoV[tiab] OR nCoV[tt] OR 2019nCoV[tiab] OR 2019nCoV[tt] OR 19nCoV[tiab] OR 19nCoV[tt] OR COVID19*[tiab] OR COVID19*[tt] OR COVID[tiab] OR COVID[tt] OR SARS-CoV-2[tiab] OR SARS-CoV-2[tt] OR SARSCOV-2[tiab] OR SARSCOV-2[tt] OR SARS-COV2[tiab] OR SARS-COV2[tt] OR SARSCOV2[tiab] OR SARSCOV2[tt] OR SARS coronavirus 2[tiab] OR SARS coronavirus 2[tt] OR Severe Acute Respiratory Syndrome Coronavirus 2[tiab] OR Severe Acute Respiratory Syndrome Coronavirus 2[tt] OR ((severe acute respiratory syndrome[tiab] OR severe acute respiratory syndrome[tt]) AND (corona virus 2[tiab] OR corona virus 2[tt])) OR new coronavirus[tiab] OR (new[tt] AND coronavirus[tt]) OR novel coronavirus[tiab] OR novel coronavirus[tt] OR novel corona virus[tiab] OR (novel[tt] AND corona virus[tt]) OR novel CoV[tiab] OR (novel[tt] AND CoV[tt]) OR novel HCoV[tiab] OR (novel[tt] AND HCoV[tt]) OR ((“19″[tiab] OR “19”[tt] OR “2019”[tiab] OR “2019”[tt] OR Wuhan[tiab] OR Wuhan[tt] OR Hubei[tiab] OR Hubei[tt]) AND (coronavirus*[tiab] OR coronavirus*[tt] OR corona virus*[tiab] OR corona virus*[tt] OR CoV[tiab] OR CoV[tt] OR HCoV[tiab] OR HCoV[tt])) OR longCOVID*[tiab] OR longCOVID*[tt] OR postCOVID*[tiab] OR postCOVID*[tt] OR postcoronavirus*[tiab] OR postcoronavirus*[tt] OR postSARS*[tiab] OR postSARS*[tt] OR ((coronavirus*[tiab] OR coronavirus*[tt] OR corona virus*[tiab] OR corona virus*[tt] OR betacoronavirus*[tiab] OR betacoronavirus*[tt]) AND (outbreak*[tiab] OR outbreak*[tt] OR epidemic*[tiab] OR epidemic*[tt] OR pandemic*[tiab] OR pandemic*[tt] OR crisis[tiab] OR crisis[tt])) OR ((Wuhan[tiab] OR Wuhan[tt] OR Hubei[tiab] OR Hubei[tt]) AND (pneumonia[tiab] OR pneumonia[tt])) AND 2019/10/31:3000/12/31[Date – Publication] AND palliative: "palliative"[All Fields] OR "palliatively"[All Fields] OR "palliatives"[All Fields] OR "hospice's"[All Fields] OR "hospices"[MeSH Terms] OR "hospices"[All Fields] OR "hospice"[All Fields] OR "hospice care"[MeSH Terms] OR ("hospice"[All Fields] AND "care"[All Fields]) OR "hospice care"[All Fields] OR "end of life"[All Fields] |
843 | 417 |
| Preprint | 37 | N/A |
Table 2.
Characteristics and Relative Contributions of Synthesized Publications
| Perspectives and sampling timeframe | Author | Year of publication | Research question(s) | Recruitment setting | Recruitment strategy | Qualitative data collection | Methodological orientation/approach to analysis | Percent of all coded quotes |
|---|---|---|---|---|---|---|---|---|
| Inpatient specialist palliative care providers (physician, nurse, nurse technician, chaplain), 2020–2021 | Boger | 2022 | To know the multidisciplinary palliative care team’s perception about stressors in the death and dying process | Brazil, hospitals | Convenience sampling | Semi-structured interviews | Content analysis | 1.12 |
| Inpatient specialist palliative care providers (physicians, nurses, healthcare assistants, senior manager, clinical manager) 2020–2021 | Bradshaw | 2022 | To explore the experiences of and impact on staff working in palliative care during the COVID-19 pandemic | UK, organizations providing specialist palliative services | Purposive sampling | Semi-structured interviews | Thematic analysis | 3.45 |
| Inpatient specialist palliative care providers (physicians, nurses, nursing assistants), not reported | Butkeviciene | 2021 | To understand professionals’ attitudes, experiences, and suggestions concerning end-of-life (EOL) dignity to provide knowledge upon which efforts to improve EOL care can be grounded | Lithuania, members of the Lithuanian Society of Palliative Medicine | Purposive sampling | Semi-structured interviews | Phenomenology, thematic analysis | 1.95 |
| Inpatient specialist palliative care providers (physicians, nurses, medical social worker, spiritual care provider, other), 2020 | Chan | 2021 | To examine the mental health of palliative care professionals in Hong Kong during the COVID-19 pandemic, the relationship of mental health with socio-demographic factors, and the impact of the pandemic on palliative care services | Hong Kong, public hospitals | Snowball sampling | Online survey | Thematic analysis | 0.53 |
| Inpatient specialist palliative care providers (chaplain, social workers, advanced practice nurses), 2020 | Currin-McCulloch | 2021 | To describe an innovative social work and nursing approach to brokering patient and family care amidst the social distancing and visitation restrictions of COVID-19 | USA, level 2 trauma center | Purposive sampling | Open-ended journal prompts | Thematic analysis | 1.95 |
| Inpatient specialist palliative care providers (nurses and nursing technicians) 2020 | deAzeredo Siqueira | 2021 | To identify the main stressors of the nursing staff in assisting patients in oncology palliative care with suspicions and confirmed for COVID-19 and to provide subsidies for measures of psychological interventions during the pandemic by COVID-19 and in the future | Brazil, hospital unit specialized in palliative oncology care | Convenience sampling | Semi-structured interviews | Psychodynamics; Christophe Dejours | 2.03 |
| Inpatient specialist palliative care providers (nurses, physician, psychologists, physiotherapists, spiritual support workers), 2020–2021 | DeLuca | 2023 | To understand the experiences of palliative care professionals deployed in supporting emergency and critical care staff during the COVID-19 first and second pandemic waves | Italy, urban hospital | Convenience, purposive, and snowball sampling | Semi-structured interviews | Thematic analysis | 3.67 |
| Inpatient specialist palliative care providers (physicians, nurses, social assistants), 2020–2021 | Figueiredo | 2021 | To capture the performance of the palliative care team in relation to patients with COVID-19 | Brazil, tertiary public hospital | Purposive sampling | Semi-structured interviews | Bardin’s thematic categorical analysis | 1.81 |
|
Inpatient specialist palliative care providers (physician, nurse practitioners, nurses, fellows, social workers, chaplains), 2020 |
Finuf | 2022 | To investigate how job resources and personal resources reduced perceptions of burnout and increased perceptions of well-being in palliative care teams | USA, urban academic hospitals | Purposive sampling | Anonymous electronic survey | Not reported | 0.26 |
| Inpatient specialist palliative care providers (physicians), 2020–2021 | Fish | 2022 | To explore the narratives of palliative care doctors working during the pandemic to understand their experiences at a personal and professional level | Scotland, hospice providing specialist inpatient and community-based palliative care | Convenience sampling | In-depth narrative interviews, video calls | Paradigmatic narrative analysis | 4.08 |
| Inpatient specialist palliative care providers (chaplains), 2020 | Galchutt | 2022 | To qualitatively capture the perceptions of inpatient palliative care chaplains and the patient–family experience as the pandemic emerged | USA, urban hospital | Convenience sampling | Semi-structured telephone interviews | Thematic analysis | 1.93 |
| Inpatient specialist palliative care providers (mesothelioma clinical nurse specialist), 2021 | Gardiner | 2022 | To explore perspectives of Mesothelioma clinical nurse specialists on their role in providing palliative care for patients with mesothelioma and their families | UK, Mesothelioma UK | Purposive sampling | Focus groups, interviews | Thematic analysis | 2.65 |
| Inpatient specialist palliative care providers (administrative, physician, nurse practitioner, consultant, spiritual worker), N/A | Holdsworth | 2022 | To understand how the pandemic impacted the implementation of new and existing palliative care programs in diverse hospital systems using the dynamic sustainability framework | USA, tertiary academic hospital | Not reported | Semi-structured interviews | Thematic analysis | 1.62 |
| Inpatient specialist palliative care providers (nurses), 2020 | Johnson | 2023 | To explore the caring experiences of palliative care nurses during the COVID-19 pandemic | Qatar, tertiary academic hospital | Purposive sampling | Semi-structured interviews | Content analysis | 2.10 |
| Inpatient specialist palliative care providers (nurse), not reported | Kirby | 2021 | To identify the main psychological influences on the perception of the Nursing staff in oncological palliative care during COVID-19 pandemic | Brazil, hospital specialized in oncological palliative care | Purposive sampling | Semi-structured interviews | Psychodynamics; Christophe Dejours | 1.13 |
| Inpatient specialist palliative care providers (physicians, nurses) 2020 | Luckett | 2021 | To solicit descriptions of, and responses to, ethical issues experienced as a result of COVID-19 related circumstances from the perspectives of nurses providing palliative care | Canada, specialist palliative care services (hospital, hospice, long-term care, community) | Purposive sampling | Video conferencing interviews | Thematic analysis | 0.22 |
| Inpatient specialist palliative care providers (nurses, nurse practitioners, practical nurse), 2020 | McMillan | 2021 | To solicit descriptions of, and responses to, ethical issues experienced as a result of COVID-19 related circumstances from the perspectives of nurses providing palliative care | Canada, specialist palliative care services (hospital, hospice, long-term care, community) | Purposive sampling | Video conferencing interviews | Thematic analysis | 2.39 |
| Inpatient specialist palliative care (physicians, nurses, social workers), 2021 | Okyere | 2022 | To explore palliative care providers’ perspectives on delivering PC services in the era of COVID-19 | Ghana, tertiary teaching hospital | Purposive sampling | Online survey | Content analysis | 3.30 |
| Inpatient specialist palliative care providers (residents), 2021 | Pfieifer | 2022 | To streamline clinical care and communication and improve patient and family experience through the integration of a Palliative Care Practitioner to a COVID-19 specific internal medicine physician team | USA, tertiary acute care teaching hospital and level 1 trauma center | Not reported | Semi-structured interviews | Not reported | 0.10 |
| Inpatient specialist palliative care providers (unknown), 2020 | Pastrana | 2021 | To explore how the COVID-19 pandemic has impacted palliative care workers around the world and describes the coping strategies they have adopted to face their specific situation | Global, IAHPC members | Purposive sampling | Free test questions — survey | Thematic analysis | 1.88 |
| Inpatient specialist palliative care providers (palliative program leaders), 2020–2021 | Rogers | 2023 | To explore palliative care program leaders’ perceptions of the future viability of their programs in the context of the pandemic and inform future educational and program development | USA, any specialist palliative care setting (hospital-based, home-based, other) | Purposive sampling | Online survey | Content analysis | 1.35 |
| Inpatient specialist palliative care providers (physicians, physician assistants, social workers, nurse practitioners) 2020 | Rosa | 2022 | To explore the experiences of an interdisciplinary palliative care team in meeting the holistic needs of oncology inpatients via telehealth over a 10-week period during the first COVID-19 surge | USA, urban comprehensive cancer center | Purposive sampling | Semi-structured interviews | Thematic analysis | 4.39 |
| Inpatient specialist palliative care providers (physicians, physician assistants, social workers, nurse practitioners) 2020–2021 | Rosa | 2022 | To explore the experiences of a multidisciplinary palliative care team delivering tele-palliative care for oncology inpatients during a 10-weeks COVID-19 surge in New York City | USA, urban comprehensive cancer center | Purposive sampling | Semi-structured interviews | Thematic analysis | 2.90 |
| Inpatient specialist palliative care providers (physicians, nurse practitioners, social workers, chaplains, advanced practice nurses), 2020 | Rowe | 2021 | To qualitatively explore the challenges presented by the COVID-19 pandemic from the perspective of palliative care clinicians. Specifically to (1) describe the strategies adopted by palliative care clinicians to cope with new challenges including patient and clinician isolation, prognostication of an emergent disease, and rapidly rising numbers of severely ill patients and (2) identify additions or adjustments to in-person and system-related palliative care training, methods, and tools made during pandemics | USA, specialist palliative care services (palliative care clinical sites, hospitals, academic medical centers) | Purposive sampling | Semi-structured interviews | Thematic analysis | 2.57 |
| Inpatient specialist palliative care providers (physicians, nurses, spiritual support counselor), 2020–2021 | Sena | 2022 | To explore palliative care health professionals and physicians perceptions of end-of-life care management in COVID units during the first two waves of the pandemic | Italy, hospitals | Convenience sampling | Semi-structured interviews | Thematic analysis | 3.23 |
| Inpatient specialist palliative care providers clinicians (physicians, nurses, physiotherapist, psychologist, pharmacist), 2020 | Tavares | 2021 | To explore the main challenges in providing PC during a pandemic and describe the strategies to be adopted to solve the identified difficulties | Portugal, urban academic hospital | Convenience sampling | Open-ended survey questions | Content analysis | 0.51 |
| Inpatient specialist palliative care providers (physicians, volunteer palliative care consultants), 2021 | Tong | 2022 | To understand the experiences of remote volunteer palliative care consultants during the initial COVID-19 surge | USA, urban academic hospital | Purposive sampling | Semi-structured interviews | Thematic analysis | 4.20 |
|
Inpatient specialist palliative care providers (physicians, nurses, consultants, residents), not reported Non-inpatient palliative care clinicians (nurses, physiotherapists, acute medicine consultants, respiratory consultants), not reported |
Wenzel | 2022 | To explore the experiences of healthcare workers providing non-invasive advanced respiratory support (NARS) to critically unwell patients with COVID-19 | UK, acute national health service trust across two hospitals | Purposive sampling | Semi-structured interviews | Thematic analysis | 1.29 |
|
Inpatient specialist palliative care providers (medical or nursing directors, other), 2020 Non-inpatient palliative care clinicians (medical or nursing directors, other) 2020 |
Bradshaw | 2021 | To describe the challenges UK specialist palliative care services experienced regarding advance care planning during COVID-19 and changes made to support timely conversations | UK, services providing specialist palliative care (inpatient palliative care, hospital palliative care, home palliative care, home nursing) | Purposive sampling | Cross-sectional online survey | Framework analysis | 3.08 |
|
Inpatient specialist palliative care providers (physicians, nurses) 2021 Non-inpatient palliative care clinicians (family members), 2021 |
Collier | 2022 | To investigate the experiences of any person — for example, patients, families and clinicians of restrictions to hospital visits for people with palliative and end-of-life care needs during COVID-19 restrictions in New Zealand | New Zealand, tertiary hospital | Purposive and snowball sampling | Semi-structured interviews | Not reported | 1.32 |
|
Inpatient specialist palliative care providers (medical directors, lead medical clinicians, nursing directors), 2020 Non-inpatient palliative care clinicians (medical directors, lead medical clinicians, nursing directors), 2020 |
Dunleavy | 2020 | To map and understand specialist palliative care services innovations and practice changes in response to COVID-19 | Global, services providing palliative care (inpatient palliative care, hospital palliative care, home palliative care, home nursing) | Purposive sampling | Online survey | Framework analysis | 4.95 |
|
Inpatient specialist palliative care providers (physicians), 2020 Non-inpatient palliative care clinicians (physicians), 2020 |
Gips | 2022 | To describe the perceived qualities of successful palliative care (PC) providers in the emergency department (ED), barriers and facilitators to ED–PC, and clinicians’ perspectives on the future of ED–PC | USA, urban academic EDs | Homogenous purposive | Semi-structured interviews | Two-step rapid analysis | 0.366 |
|
Inpatient specialist palliative care providers (physicians, nurses, social workers, chaplains, resident), 2020 Non-inpatient palliative care clinicians (nurses, consultants), 2021 |
Hanna | 2021 | To explore health and social care professionals’ experiences and perceptions of providing end-of-life care during the COVID-19 pandemic | UK, range of clinical settings (hospital care-home) | Purposive sampling | Semi-structured interviews | Thematic analysis | 1.63 |
|
Inpatient specialist palliative care providers (social workers), 2020 Non-inpatient palliative care clinicians (social workers), 2020 |
Latimer | 2022 | The main objectives of this study were (1) to assess palliative and hospice social workers’ experiences of moral distress during COVID-19 and (2) to identify and describe participants’ most morally distressing scenarios | USA, social work hospice palliative care network members | Snowball sampling | Online questionnaire | Thematic analysis | 1.13 |
|
Inpatient specialist palliative care providers (nurse, palliative consultants), 2020 Non-inpatient palliative care clinician (infection control nurse, consultant, anesthetist), 2020 |
Mitchinson | 2021 | To identify barriers to delivering end-of-life care, describe attempts to deliver care during the COVID-19 pandemic, and understand the impact this had on staff | UK, large teaching hospitals | Purposive sampling | Semi-structured interviews | Framework analysis | 0.647 |
|
Inpatient specialist palliative care providers (physician, nurses), 2020 Non-inpatient palliative care clinicians (pharmacist, supply chain and environmental service workers), 2020 |
Navuluri | 2023 | To understand the contours of distressed work faced by healthcare professionals during COVID-19 | USA, quaternary referral hospital | Purposive sampling | Semi-structured interviews and participant observations | Thematic analysis | 3.96 |
|
Inpatient specialist palliative care providers (physicians, nurses, administrative staff, other), 2020 Non-inpatient palliative care clinicians (physicians, nurses, administrative staff, other), 2020 |
Oluyase | 2020 | To study the response of and challenges for palliative care services during the COVID-19 pandemic | Global, specialist palliative care services (hospital, community-home based, nursing home) | Purposive sampling | Free-text questions in survey | Content analysis | 0.278 |
|
Inpatient specialist palliative care providers (physicians, nurses, psychologists, medical managers), 2020 Non-inpatient palliative care clinicians (nurses), 2020 |
Seibel | 2022 | To explore the experiences of stakeholders and staff in implementing and operating an ad hoc unit delivering acute palliative care | Germany, urban academic hospital | Purposive sampling | Semi-structured interviews | Content analysis | 1.13 |
|
Inpatient specialist palliative care providers (unknown), 2020 Non-inpatient palliative care clinicians (unknown), 2020 |
Singh | 2022 | To explore health professionals’ perspectives of the role of palliative care during the COVID-19 pandemic by analyzing their views and experiences expressed in articles and blogs located via Twitter | Convenience and/or snowball sampling | Online opinion articles (Tweets) | Content analysis | 1.09 | |
|
Inpatient specialist palliative care (physicians, internists), 2020–2021 Non-inpatient palliative care clinicians (physicians) 2020–2021 |
Wentlandt | 2022 | To explore the facilitators and barriers to palliative care integration in the care of patients with COVID-19 | Canada, primary, secondary, tertiary hospitals | Purposive and snowball sampling | Semi-structured, open-ended interview | Thematic analysis | 3.54 |
|
Inpatient specialist palliative care providers (physician), 2020–2021 Non-inpatient palliative care clinicians (physicians) 2020–2021 |
Wentlandt | 2023 | To describe physician experiences with (restrictive visitor) policies and reflections of their effects | Canada, primary, secondary, and tertiary hospitals | Snowball sampling | Semi-structured interviews | Template analysis | 4.45 |
|
Inpatient specialist palliative care providers (physician), 2020 Non-inpatient palliative care clinicians (physicians, nurse practitioner) 2020 |
Wiebe | 2021 | To document how the experience of providing medical assistance in dying (MAiD) changed during the COVID-19 pandemic | Canada, MAiD providers and coordinators | Convenience, purposive, and snowball sampling | Semi-structured interviews | Abductive reasoning | 1.41 |
|
Inpatient specialist palliative care providers (physicians, nurses, consultants, residents), not reported Non-inpatient palliative care clinicians (nurses, physiotherapists, acute medicine consultants, respiratory consultants), not reported |
Wenzel | 2022 | To explore the experiences of healthcare workers providing non-invasive advanced respiratory support (NARS) to critically unwell patients with COVID-19 | UK, acute national health service trust across two hospitals | Purposive sampling | Semi-structured interviews | Thematic analysis | 1.29 |
| Non-inpatient palliative clinicians (physician), 2020 | Aaronson | 2020 | To evaluate emergency department (ED) clinician’s experiences on embedding palliative care (PC) in the ED during COVID-19 | USA, urban academic ED | Voluntary response sampling | Survey | Inductive thematic analysis | 1.32 |
| Non-inpatient palliative clinicians (general public), 2019–2020 | Back | 2021 | To understand public perceptions of serious illness care to inform greater public engagement | USA, general public | Third-party recruitment | Focus groups | Not reported | 0.154 |
| Non-palliative clinicians (hospice medical directors, hospice directors of nursing), 2020 | Constantini | 2020 | To examine the preparedness for, and impact of, the COVID-19 pandemic on hospices in Italy to inform the response in other countries | Italy, hospices | Purposive sampling | Telephone interview | Descriptive analysis | 0.281 |
| Non-inpatient palliative care clinicians (hospice staff, family members), 2020 | Cross | 2022 | To explore how hospice admissions staff and caregivers of hospice patients perceive the hospice admission process and the transition to hospice at home | USA, hospice organization | Purposive sampling | Semi-structured interviews | Thematic analysis | 2.44 |
| Non-inpatient palliative care clinicians (directors of nursing), 2021 | Ninteau | 2022 | To capture how nursing homes addressed palliative care needs during the pandemic | USA, community nursing homes | Snowball sampling | Semi-structured interviews | Thematic analysis | 1.87 |
| Non-inpatient palliative care clinicians (physicians, nurses), 2020 | Schallenburger | 2022 | To examine challenges and possible solutions for general palliative care inpatients in relation to the care of seriously ill and dying patients and their relatives | Germany, primary, secondary, tertiary hospitals | Convenience sampling | Focus groups | Content analysis | 1.23 |
| Non-inpatient palliative care clinicians (physicians, hospital leader, spiritual care provider), 2020 | Vesel | 2021 | To explore the utilization, perceptions, and understanding of palliative care among critical care clinicians, hospital leaders, and spiritual care providers during the pandemic | USA, tertiary academic medical center | Purposive sampling | Semi-structured interviews | Thematic analysis | 3.39 |
| Non-inpatient palliative care clinicians (general public), 2020 | Vihvelin | 2022 | To gain insight into preferences for the end-of-life and end-of-life care from people experiencing homelessness | Canada, general public | Purposive sampling | Semi-structured telephone interviews | Thematic analysis | 0.179 |
| Non-inpatient palliative care clinicians (clinical oncologists), 2021–2022 | Wang | 2022 | To explore the current status of palliative care practice for cancer and the influence of COVID-19 from the perspective of oncologists | China, various settings (medical centers, palliative care institutions) | Not reported | Semi-structured interviews | Thematic analysis | 0.578 |
*Voices we abstracted for our study
Figure 1.
PRISMA flow diagram.
Quality Appraisal
The methodological quality of the studies was assessed independently by two co-authors (DWZ and SGR) using the Mixed Methods Appraisal Tool (MMAT).16 The MMAT is a 5-item assessment tool that allows for concurrent assessment of qualitative, quantitative, and mixed-method studies. The authors (DWZ, SGR) independently assigned quality ratings of high (***, 4–5 criteria met), moderate (**, 2–3 criteria met), and low (*, 0–1 criterion met) (Suppl Table 1). We neither weighted nor excluded articles from the review based on article quality as we extracted primary quotes for our independent analysis. We assessed the relative utility of each article to the purpose of the review and synthesis by calculating the percent of all coded data derived from each article15.
Data Extraction and Analysis
The data extraction and analysis process was informed by Thomas and Harden’s framework and Pozzar et al.’s approach.14,17 While Thomas and Harden provided a sequential, staged outline,14 Pozzar et al. provided the protocols and strategies for thematic analysis.17 The first stage was understanding the context of each study. Using Covidence,18 two authors independently (DWZ, SGR) extracted the main characteristics of each study: study type (qualitative, mixed method), research question, recruitment setting (country, setting), recruitment strategy, and relevant primary quotes. Additional details on study design were collected for qualitative studies and the qualitative arm of mixed-method studies (data collection strategy, methodological orientation/approach to analysis). Any disagreements were resolved through discussion or with a third reviewer (ZJ).
The second stage involved qualitative data analysis using a six-step thematic analysis approach.19 One author (DWZ) imported each manuscript into NVivo 12.20 In the first step, two authors (DWZ, SGR) read and reread the included articles to become familiarized with the primary quotes. Second, two authors (DWZ, SGR) performed inductive, line-by-line coding on all primary data that pertained to the perception and experience of inpatient palliative care specialists. Third, we developed a codebook using deductive (i.e., the socioecological model) and inductive approaches (open coding 100% of the transcripts). The fourth step involved two authors (DWZ, SGR) independently coding and recoding the primary data using the finalized codebook. During the coding process, authors met weekly to debrief and resolve conflicts, outliers, and refine codes and code definitions. We critiqued our application of these codes across studies through constant comparison.14 In the fifth step, similar codes were combined into descriptive themes. The sixth step involved generating analytical themes. We first considered the abstract concepts represented by the descriptive themes. We then generated a set of analytical themes by returning to the data and identifying the antecedents and consequents of each identified concept. With this approach, we aimed to ensure that our findings would expand upon (rather than simply summarize) the primary data.14 Our final set of analytical themes represents the relationships between concepts that were consistent across studies. No study was excluded based on quality as we extracted relevant primary data for thematic synthesis (Table 3).
Table 3.
Themes, Subthemes, and Example Quotes
| Theme | Exemplary intrapersonal quote | Exemplary interpersonal quote; converging | Exemplary interpersonal quote; diverging |
|---|---|---|---|
| Theme 1: shifting foundations | |||
|
Subtheme 1.1: Systemic changes disrupted routines of palliative care |
“…when compare[d] to the year before, Our PCU had been 15 beds, we are now 10. We gave up 5 because we couldn’t fill them… And even the 10 that we had there was a reasonable balance. There was a while it was hard to fill even 10 ….” — Palliative Care Clinician, North America, Wentlandt et al., 2023 | “This means I may be faced with choices that, in my 20 years of clinical practice, I have never had to make .. . . These will be devastating decisions for all involved, including my colleagues.” Non-Palliative Care Clinician, Global, Singh et al., 2022 | |
|
Subtheme 1.2: Disruptions in clinical routines created confusion and misunderstandings of roles |
“I feel we did not know what to expect and had no plan of how we were going to do our jobs on a daily basis. We were reprimanded for not doing enough but had no direction on how to be helpful ... It added to the stress with an already difficult job. We are not expendable, it has left me feeling ambivalent about this job…” — Palliative Care Clinician, North America, Finuf et al., 2022 | “I found it difficult in part. In the sense of palliative thinking and working, it’s simply different from normal wards and surgery. And I sometimes had the feeling that the palliative care unit wanted you to work the way they know it and that they sometimes imposed their palliative thinking and acting on you.” — Non-palliative Nurse, Europe, Seibel et al., 2022 | “Well I don’t think [my perception] evolved. I said, ‘thank heaven we have that service running’… I think had it not been built up to the degree it was, I think we would have lost some ability to help some of these patients.” — Hospital Leader, North America, Vesel et al., 2021 |
|
Subtheme 1.3: Lack of presence spurred feelings of clinical ineffectiveness |
“[I] don’t feel comfortable prescribing something or making a recommendation for an opioid or medication … is it safe to escalate these medications when you’re not physically seeing the patient? And how do we know what we’re doing is right…” — Palliative Care Clinician, North America, Rosa et al., 2022 | “I mean, there’s no substitute for being in person with someone. When you’re with someone and they’re not there, you’re basically doing it blind when you’re on the phone, you’re robbing yourself of one of the most important senses, which is your visual, your body language. And body language gives off an energy where you can connect with someone you. It’s easier to empathize with someone when you can see what they look like and over the phone you just can’t, it’s a voice...” — Internist, North America, Wentlandt et al., 2023 | |
| Theme 2: reorienting to relationships | |||
|
Subtheme 2.1: Nimbleness and thoughtful risk-taking were essential for bridging relational gaps |
“I felt that it was really mean. The lady had two daughters and was unfair for them to decide who gets to see their mum before she died. I told them both to come and just blame it on me when they got to the hospital door.” — Palliative Care Resident, UK, Hanna et al., 2021 | “It’s not fair to treat everybody the same, it’s not reality. Reality is that there are certain family members and situations where they are essential to the wellbeing of that person...I’m willing to have more grey, more trying to work with exceptions” — Hospice Nurse, North America, McMillan et al., 2021 | |
|
Subtheme 2.2: Palliative care clinicians and enhanced interprofessional efficacy through compassionate presence |
“ED clinicians .. . said the reason they did not feel morally distressed is because we [palliative care clinicians] had their back. And that was really powerful.. .it just made me realize how many places there are in the institution that could benefit from partnership with us. I always knew they were there.” — Palliative Care Clinician, North America, Rowe et al., 2021 | “[There were] times when I disagreed with the family but palliative care was instrumental in advocating for them and listening in longer conversations that I would not have had time for, and they make me feel more confident that the clinical decisions are in line with the patients and families’ goals of care.” — Emergency Physician, North America, Aaronson et al., 2021 | “I found it difficult in part. In the sense of palliative thinking and working, it’s simply different from normal wards and surgery. And I sometimes had the feeling that the palliative care unit wanted you to work the way they know it and that they sometimes imposed their palliative thinking and acting on you.” — Non-palliative Nurse, Europe, Seibel et al., 2022 |
| Theme 3: evolving identities | |||
|
Subtheme 3.1: Rapid evolution of roles created emotional anguish for palliative care clinicians |
“I am the only member of the palliative care team at the hospital and I have resigned under the strain of the program. Currently, there are no plans to open the position and replace me.” Palliative Care Clinician, North America, Rogers et al., 2023 | “I was emotionally broken. I remember crying at the end of that weekend. I was, I was like ‘Oh my God’ and I had to, I had to actually reach out to my [palliative] consultant colleagues to say, ‘I feel broken’ and they were like, ‘that’s normal.’” Acute Medicine Consultant, Europe, Wenzel et al., 2022 | |
|
Subtheme 3.2: Decentralizing and expanding the tenets of palliative care |
“Palliative care is the medical specialty, but it’s also a set of principles and approaches to serious illness that are not consigned and should not be consigned to those who practice palliative care as a medical specialty. There are things that everybody should be doing... by hospitalists and cardiologists and oncologists and intensivists and surgeons and all of the different specialties.” — Palliative Care Clinician, North America, Rowe et al., 2021 | “All doctors are palliative care doctors now.” — Non-palliative clinician, Global, Singh et al., 2022 | |
RESULTS
Of the total 3869 unique articles, we assessed 246 for full texts and included 52 for the final analysis (Fig. 1). From the included articles, we extracted 877 primary quotes for analysis. Each article contributed between 0.11 and 4.95% of all coded data. The articles were then categorized based on the perspectives represented, geographical location, and timeframe of data collection. Most articles focused solely on the perspectives of inpatient palliative care clinicians (n = 28), some had mixed perspectives with non-inpatient palliative care clinicians (n = 14), and others solely focused on the perspectives of non-inpatient palliative care clinicians (n = 10). In terms of geographical representation, studies were conducted in North American (n = 23), European (n = 16), South American (n = 4), Oceanic (n = 2), Asian (n = 2), West African (n = 1), Middle Eastern (n = 1), and inter-continental settings (n = 3). Studies gathered data between 2019–2020 (n = 1), 2020 (n = 28), 2020–2021 (n = 11), 2021 (n = 7), and 2021–2022 (n = 1).
DESCRIPTIVE THEMES
Theme 1: Shifting Foundations
Subtheme 1.1: Systemic Changes Disrupted the Routines of Palliative Care
As COVID-19 rapidly spread across the globe, the routines of palliative care practices were challenged both at the system and institution level.3,21–45 Some clinicians experienced disrupted supply chains resulting in compromised access to medications (e.g., morphine powder)21 and personal protective equipment35 while many clinicians also scrambled to adjust to an increasingly “virtual” workplace.6,21,22,24,26,27,29,31,34,37,44 Many palliative clinicians experienced a dramatic decrease in workload,24,27,29,34,43,45,46 having “nothing to do”45 with beds being “hard to fill,”30 while others experienced a dramatic increase in workload,3,6,25,26,32,35–37,39,40,42 becoming engulfed within a “tsunami of death”42 and patients “swamping a bazillion beds.”40 As new rules and guidelines appeared “every hour,”6,23,35 palliative care clinicians felt that they became “disembodied professionals”40 constantly “reacting to threats”23 and “resigning”34 to new, more “complicated and lengthy”28 processes. Non-palliative care inpatient colleagues shared in the disruption of clinical routines, with virtual work becoming the new “norm,”12,30,32,43,47 and staff members working “overtime”4,30,48 and being “redeployed”48 to confront the threat of the pandemic.
Subtheme 1.2: Disruptions in Routines Created Confusion and Misunderstandings of Roles
Accompanying the clinical disruptions were changes in how palliative care was regarded.21,22,25,28–32,36–40,44,46,48–57 At the institutional level, some palliative care clinicians felt they were “integral to the mission” and the “overall strategy”49 against COVID-19.22,36,51,53 However, many feared that as a “non-front-line service,”21,38 their program would be “chopped”49 as they were an “expendable”46 resource or an “easy target”49 for institutional financial restructuring.25,31,32,37 Between colleagues, some palliative care clinicians in the telehealth setting worried that they became an “annoyance”37 or an “outsider”25 while others felt “resented”37 for their absence and were “reprimanded for not doing enough.”46 The conflicting and competing expectations created internal existential distress40,44,48 for palliative care clinicians and a yearning for clear directions on how to be most effective.49 To non-palliative care clinicians and the general public, however, palliative care represented a pivotal and indispensable force in providing high-quality care.4,23,50,58 Although accounts of stigma and misunderstandings existed,9,30,54–56 many were overtaken by positive endorsements after interacting with palliative care clinicians.4,45,47,55–58
Subtheme 1.3: Lack of Presence Spurred Feelings of Clinical Ineffectiveness
Transmission-based precautions limited physical presence and challenged palliative care clinicians’ sense of clinical efficacy.3,21,22,25–27,30,31,34,37,39–41,43,44,48,52,59–62 For inpatient palliative clinicians, the sense of “inadequacy”25 arose from their “tools being taken away,”26,40 a lack of familial presence,21,23–25,30,31,34,36,37,39–41,43,44,50–54,58,63–65 and feeling “disengaged from their emotions.”48 Although some clinicians felt they were able to “successfully”27,37,59 adapt to the virtual environment, most palliative clinicians felt that virtual care limited their ability to deliver optimal care,21,22,27,30,31,37,39,40,43,44,61,62 leaving a few patients feeling “abandoned,”37 untouchable,41 and without a sense of “trust” in their clinicians.24,44 On a practical level, clinicians described feeling that they were “not doctoring,”44 that they lost their “psychosocial diagnostic skills,”37 and that they questioned their ability to safely prescribe medications.44 These sentiments of moral distress, loss of self-efficacy, and the feeling that “everything you do sets them up for failure”66 resonated with the experience of non-palliative care clinicians during the initial period of added hospital precautions.23,30,33,47,61–63,67
Theme 2: Reorienting to Relationships
Subtheme 2.1: Nimbleness and Thoughtful Risk-taking Were Essential for Bridging Relational Gaps
Inpatient palliative care clinicians recognized that policy changes “challenged”22 the relational aspects of high-quality serious illness care.21,23–25,30,31,34,36,37,39–41,43,44,50–54,58,63–65 Feeling responsible for ensuring that patients had access to healing relationships, many clinicians consciously chose to “transgress,”53 make “exceptions,”24 and shoulder any “blame”25 from allowing increased family presence,52,63 access to “home cooked food,”41 and more relaxed social distancing.34,61 To bridge the gap in familial presence, clinicians also invested in new technology to allow virtual goodbyes43,51 and to celebrate milestones.25,34,42,51 Palliative care clinicians’ efforts to maintain connection and to “support patients early, where possible”21,28,43 did not go unnoticed. Interdisciplinary team members consistently endorsed palliative care clinicians’ boldness to “negotiate”48 and to make “exceptions”61 as these actions exemplified “humanity over policy”61 during a period of unprecedented suffering.30,42,47,48,55,58,60,66
Subtheme 2.2: Palliative Care Clinicians Enhanced Interdisciplinary Efficacy Through Compassionate Presence
Beyond bridging relational care for patients and families, palliative care clinicians also adapted their skills to support their colleagues.4,9,23,24,29,32,34–37,39,42–45,47,49,50,55,57,58,60,66 This meant caring for their colleagues with the “same harmony”39 as they did with patients by actively offering colleagues a shoulder to “lean on.”37 Palliative care clinicians recognized that by bolstering interdisciplinary “resilience,”34 “preventing burnout,”49 and ameliorating “moral distress,”23 palliative care clinicians could enhance interdisciplinary camaraderie and team effectiveness.23,24,29,32,34–37,39,43,44,49 While the majority of colleagues expressed gratitude4,9,32,42,45,47,50,55,57,58,60,66 for palliative care clinicians’ ability to “take away uncertainties”45,57 and “bring calmness,”45 build “resilience,”58 “innovate,”47 and boost “confidence,”57 a few non-palliative clinicians also expressed feelings of being “imposed on”45 and that palliative care was “not useful.”9 Overall, the profound positive impact from collaborating with palliative care clinicians was shared by both palliative and non-palliative clinicians.4,9,23,24,29,32,34–37,39,42–45,47,49,50,55,57,58,60,66
Theme 3: Evolving Identities
Subtheme 3.1: Rapid Evolution of Roles Created Emotional Anguish for Palliative Care Clinicians
The sudden, volatile evolution of roles had profound physical and psychosocial impacts on inpatient palliative care clinicians.4,21,22,24–27,31–36,39,40,42–45,48,49,51,54,58,60,63,65,67 Beyond resolving conflicting expectations and building relational presence, palliative care clinicians embodied additional educational and novel leadership roles.4,21,24,26,32,36,42–45,49,51,54,58,60,65,67 This ranged from orchestrating “teaching sessions”26 on establishing trust, to regional committee meetings with public health,32 to disseminating best telehealth practices.24,44 A few palliative care clinicians also expressed how they took on more “active” roles in “advanced care” and “treatment escalation planning”24,26,36,65 for patients, and some felt they were delegated the roles of “infection prevention specialists.”21 Though one palliative clinician found their new roles to be “very satisfying,”63 for most clinicians, such abrupt role evolution was physically and emotionally “burdensome,”21,25,27,31,33,35,39,40,42,49 caused members to “resign,”49 and led to a constant state of emotional distress.22,27,31,40,42,44,48 The deep emotional anguish was shared by non-palliative care clinicians,42,61,63,68 consequently triggering both healthy and maladaptive coping mechanisms.22,27,34,35,39,51
Subtheme 3.2: Decentralizing and Expanding the Tenets of Palliative Care
As the presence and exposure of palliative care became more pronounced throughout the pandemic, widespread acknowledgment of the value of palliative care grew.3,17,18,21,23,34,39,41,43 In the eyes of inpatient palliative care clinicians, “palliative principles” and “approaches” to serious illness are ubiquitous and “should not be consigned to those who practice palliative care as a medical specialty.”3,17,18,21,23,34,39,41,43 For institutions that provided a concrete “bedrock”23 of primary palliative care skills to non-palliative clinicians, specialty services were less likely to be overburdened.23,29,40,47,53 Not only did non-palliative colleagues echo this protective need for palliative care,4,32,50,58,68 some also recognized that “all doctors are palliative care doctors”4,50 and wished they were “more skilled”60 in providing palliative care after challenging experiences with patients “already in the dying process.”24,45,50,53 Appreciating the profound benefits of a robust system of primary palliative care practitioners, policy-makers emerged from the pandemic to advocate27 for the expansion of palliative care capacity and an increase in palliative care training among “undergraduate and postgraduate trainees.”4 They saw these measures as a proactive step to help in case of future pandemics when palliative care skills would again be front and center.4,40,49
ANALYTICAL THEMES
Palliative Care Propagates Compassion Through a Healing Presence
In response to the disconnection and chaos inflicted by COVID-19, palliative care clinicians broke through institutional boundaries to maintain a healing presence. The impact of palliative care’s presence extended from patients and caregivers to interdisciplinary colleagues, where palliative care clinicians propagated compassion to combat sinking moral distress from traumatic psychosocial experiences. While palliative care’s presence was celebrated by most, the perception of an “imposing presence” necessitates a careful reflection of the changing clinical landscape.
Palliative Care Enhances Systemic Response to Suffering Through Nimble Leadership
The pandemic created unmet systemic needs that served as opportunities for palliative care clinicians to transcend their conventional roles and skillset in navigating uncertainty associated with loss and suffering. From becoming leaders in interdisciplinary palliative education to embracing new clinical duties, this plasticity allowed palliative care clinicians to bridge gaps in clinical spaces that were unaccustomed to loss and suffering, thereby enhancing the overall systemic response against COVID-19. Although these opportunities provided palliative care clinicians a platform to demonstrate their impact, a lack of formal guidelines and leadership training may have prevented some clinicians from harnessing these opportunities.
DISCUSSION
The unprecedented suffering caused by COVID-19 required a collaborative, interdisciplinary, and systemic response. Our systematic review of the global literature triangulated the roles that specialist palliative care providers played in responding to the distress and devastation across institutionalized settings. We found that in response to shifting foundations in systemic care, inpatient palliative care clinicians adapted their identity and reoriented towards mending relational gaps between patients, caregivers, the healthcare system, and among interdisciplinary colleagues. Together, these findings signal that palliative care clinicians can adapt their clinical skills in service of their colleagues, while emphasizing the need for leadership skill development within the field.
At the onset of the pandemic, palliative care received varying degrees of attention. Although international organizations (e.g., World Health Organization) and experts advocated for early integration of palliative care services into systemic responses,69 uptake of these recommendations was variable due to changing clinical needs and lack of primary data.70,71 As the pandemic unfolded, data emerged to describe the role and experiences of palliative care in non-institutional settings. Reviews of the role of palliative care in long-term care, hospice, and home-based settings identified a consistent need for palliative clinicians to be flexible and to adapt to the multidimensional needs of the system and interdisciplinary colleagues.70,72–77 The results of our systematic review are consistent with prior literature, but also expand it by triangulating the role(s), expectation(s), and experiences of inpatient palliative care clinicians through the perspectives of palliative care professionals, interdisciplinary colleagues, and caregivers.
The impact of inpatient palliative care specialists’ presence transcended direct clinical care to include interdisciplinary relationships as well. In our study, we triangulated the role of inpatient palliative clinicians in mitigating moral distress and propagating compassionate practices among colleagues, potentially alleviating burnout and compassion fatigue. Our findings resonate with prior research describing the benefits of collegial trust and collaboration in improving clinical outcomes.78–81 Palliative clinicians may facilitate interdisciplinary collaborations by creating a “holding space,” which is a theoretical relational space created for the referring clinicians by accompaniment, recognizing challenges, establishing expectations, and providing a clinical second look.82 These findings raise concerns that conventional metrics (e.g., relative value units) may not adequately capture the interdisciplinary and collaborative role that inpatient palliative clinicians may play during and beyond pandemic care.83 Innovations in patient-reported experience measures,84–86 particularly in the realm of perceived system compassion,87,88 represent an opportunity to demonstrate the interprofessional impact of palliative care prospectively. Future studies are also needed to elucidate the optimal process for building safe and effective interdisciplinary collaborations in response to systemic threats.
Building future pandemic preparedness requires attention to leadership development among palliative care clinicians. We found that inpatient palliative care clinicians demonstrated strong leadership qualities in effectively identifying and managing heightened uncertainty, loss, and suffering. This suggests that inpatient palliative care clinicians may play a central role in leading and directing systemic change to understand and address unprecedented suffering. Prior research recognizes that palliative leadership training and skill development represent a vital component to ensuring high-quality patient care.89–94 Simultaneously, many barriers exist which inhibit the integration of leadership training, including a lack of contextually relevant content and inequities in accessing leader mentors.80,90–103 Leadership education, possibly drawing from business literature and initiatives undertaken in other medical specialties, urgently needs to be developed and integrated throughout a palliative care clinician’s career.89,90,104–108
LIMITATIONS
Our study is the first theoretically framed, globally relevant systematic review that triangulated the roles and expectations of inpatient palliative care clinicians during the COVID-19 pandemic, but like any study it has limitations. First, our data predominantly represents Westernized healthcare teams, systems, and philosophies of care in high-income countries, with limited perspectives from Asian, African, and Middle Eastern contexts. This limits the transferability of our findings for inpatient palliative care clinicians who practice in non-Western medical settings. Secondly, the credibility of our study findings to direct clinical care may be limited by the lack of perspectives of the general public, patients, and caregivers. Finally, given that the included prospective studies were limited in their time frame, a future, retrospective analysis is needed to prioritize lessons learned from the pandemic.
CONCLUSION
This systematic review illustrates how inpatient, palliative care specialists played a complex, multifaceted role in the systemic response to suffering during the COVID-19 pandemic. Evidence suggests that palliative care clinicians prioritized and maintained relational presence despite disruptions in routines and interpersonal misunderstandings. In turn, inpatient palliative clinicians alleviated suffering faced by patients, families, and their colleagues. Future research is needed to characterize how inpatient palliative care clinicians are regarded within institutionalized settings and to foster leadership development among palliative care clinicians.
Supplementary Information
Below is the link to the electronic supplementary material.
Acknowledgements
The authors acknowledge Dr. Andrea C. Benites for her support with screening.
Author Contribution
Conception and design: all authors. Collection and assembly of data: DWZ, SGR. Data analysis and interpretation: all authors. Article writing: all authors. Final approval of article: all authors.
Declarations
Conflict of Interest
The authors declared no potential conflicts of interests with respect to the research, authorship, or publication of this article.
Footnotes
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.Krishnan A, Hamilton JP, Alqahtani SA, Woreta TA. COVID-19: An overview and a clinical update. World J Clin Cases. 2021;9:8–23. doi: 10.12998/wjcc.v9.i1.8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.McMahon M, Nadigel J, Thompson E, Glazier RH. Informing Canada’s Health System Response to COVID-19: Priorities for Health Services and Policy Research. Healthc Policy. 2020;16:112–124. doi: 10.12927/hcpol.2020.26249. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Tavares P, Rodrigues C, Neto IG. The Impact of COVID-19 on Palliative Care: Perspective of Healthcare Professionals. Cureus. 2021;13:e19522. doi: 10.7759/cureus.19522. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Singh GK, Rego J, Chambers S, Fox J. Health Professionals’ Perspectives of the Role of Palliative Care During COVID-19: Content Analysis of Articles and Blogs Posted on Twitter. Am J Hosp Palliat Care. 2022;39:487–493. doi: 10.1177/10499091211024202. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Al-Mahrezi A, Al-Mandhari Z. Palliative Care: Time for Action. Oman Med J. 2016;31:161–163. doi: 10.5001/omj.2016.32. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Dunleavy L, et al. ‘Necessity is the mother of invention’: Specialist palliative care service innovation and practice change in response to COVID-19. Results from a multinational survey (CovPall) Palliat Med. 2021;35:814–829. doi: 10.1177/02692163211000660. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Mojtahedi Z, Shen JJ. Home palliative Care during the COVID-19 pandemic: a scoping review. Am J Hosp Palliat Care. 2022;10499091221093314. [DOI] [PMC free article] [PubMed]
- 8.Etkind SN, et al. The Role and Response of Palliative Care and Hospice Services in Epidemics and Pandemics: A Rapid Review to Inform Practice During the COVID-19 Pandemic. J Pain Symptom Manage. 2020;60:e31–e40. doi: 10.1016/j.jpainsymman.2020.03.029. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Gips A, et al. Palliative care in the emergency department: A qualitative study exploring barriers, facilitators, desired clinician qualities, and future directions. Palliat Support Care. 2022;20:363–368. doi: 10.1017/S1478951521001012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Beng TS, et al. COVID-19, Suffering and Palliative Care: A Review. Am J Hosp Palliat Care. 2022;39:986–995. doi: 10.1177/10499091211046233. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Wentlandt K, et al. Palliative Care in Toronto During the COVID-19 Pandemic. J Pain Symptom Manag. 2021;62:615–618. doi: 10.1016/j.jpainsymman.2021.01.137. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Luckett T, et al. Australian specialist palliative care’s response to COVID-19: an anonymous online survey of service providers. Ann Palliat Med. 2021;10:2747–2757. doi: 10.21037/apm-20-1760. [DOI] [PubMed] [Google Scholar]
- 13.Fadul N, Elsayem AF, Bruera E. Integration of palliative care into COVID-19 pandemic planning. BMJ Support Palliat Care. 2021;11:40–44. doi: 10.1136/bmjspcare-2020-002364. [DOI] [PubMed] [Google Scholar]
- 14.Thomas J, Harden A. Methods for the thematic synthesis of qualitative research in systematic reviews. BMC Med Res Methodol. 2008;8:45. doi: 10.1186/1471-2288-8-45. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Tong A, Flemming K, McInnes E, Oliver S, Craig J. Enhancing transparency in reporting the synthesis of qualitative research: ENTREQ. BMC Med Res Methodol. 2012;12:181. doi: 10.1186/1471-2288-12-181. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Hong QN, Gonzalez-Reyes A, Pluye P. Improving the usefulness of a tool for appraising the quality of qualitative, quantitative and mixed methods studies, the Mixed Methods Appraisal Tool (MMAT) J Eval Clin Pract. 2018;24:459–467. doi: 10.1111/jep.12884. [DOI] [PubMed] [Google Scholar]
- 17.Pozzar RA, Berry DL. Communicating is analogous to caring: A systematic review and thematic synthesis of the patient-clinician communication experiences of individuals with ovarian cancer. Palliat Support Care. 2023;21:515–533. doi: 10.1017/S1478951522000621. [DOI] [PubMed] [Google Scholar]
- 18.Kellermeyer L, Harnke B, Knight S. Covidence and Rayyan. J Med Libr Assoc. 2018;106:580–583. doi: 10.5195/jmla.2018.513. [DOI] [Google Scholar]
- 19.Clarke V, Braun V, Hayfield N. Thematic analysis. Qual Psychol: A Pract Guide Res Methods. 2015;3:222–248. [Google Scholar]
- 20.Dhakal K. NVivo. J Med Libr Assoc: JMLA. 2022;110:270. doi: 10.5195/jmla.2022.1271. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Okyere J, Mensah ABB, Kissah-Korsah K. COVID-19 front-liners: Experiences of palliative care providers in a tertiary hospital. SAGE Open Nurs. 2022;8:23779608221132172. doi: 10.1177/23779608221132172. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Bradshaw A, et al. Experiences of staff providing specialist palliative care during COVID-19: a multiple qualitative case study. J R Soc Med. 2022;115:220–230. doi: 10.1177/01410768221077366. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Rowe JG, et al. Palliative care practice during the COVID-19 pandemic: a descriptive qualitative study of palliative care clinicians. J Pain Symptom Manag. 2021;62:1111–1116. doi: 10.1016/j.jpainsymman.2021.06.013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Holdsworth LM, Mui HZ, Winget M, Lorenz KA. “Never waste a good crisis”: A qualitative study of the impact of COVID-19 on palliative care in seven hospitals using the Dynamic Sustainability Framework. Palliat Med. 2022;36:1544–1551. doi: 10.1177/02692163221123966. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Hanna JR, et al. Health and social care professionals’ experiences of providing end of life care during the COVID-19 pandemic: A qualitative study. Palliat Med. 2021;35:1249–1257. doi: 10.1177/02692163211017808. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Bradshaw A, et al. Understanding and addressing challenges for advance care planning in the COVID-19 pandemic: an analysis of the UK CovPall survey data from specialist palliative care services. Palliat Med. 2021;35:1225–1237. doi: 10.1177/02692163211017387. [DOI] [PubMed] [Google Scholar]
- 27.Pastrana T, et al. The impact of COVID-19 on palliative care workers across the world: A qualitative analysis of responses to open-ended questions. Palliat Support Care. 2021;19:187–192. doi: 10.1017/S1478951521000298. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Chan WCH, Woo RKW, Kwok DK-S, Yu CTK, Chiu LM-H. Impact of COVID-19 on mental health of palliative care professionals and services: A mixed-methods survey study. Am J Hosp Palliat Med®. 2022;39:1227–1235. doi: 10.1177/10499091211057043. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Wang Y, et al. The impact of the COVID-19 pandemic on palliative care practice: A survey of clinical oncologists. Front Public Health. 2022;10:4447. doi: 10.3389/fpubh.2022.1020937. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Wentlandt K, et al. Physician perceptions of restrictive visitor policies during the COVID-19 pandemic: a qualitative study. Can Med Assoc Open Access J. 2023;11:E110–E117. doi: 10.9778/cmajo.20220048. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Latimer A, Fantus S, Pachner TM, Benner K, Leff V. Palliative and hospice social workers’ moral distress during the COVID-19 pandemic. Palliat Support Care. 2022;1-6. [DOI] [PubMed]
- 32.Wentlandt K, et al. Identifying barriers and facilitators to palliative care integration in the management of hospitalized patients with COVID-19: A qualitative study. Palliat Med. 2022;36:945–954. doi: 10.1177/02692163221087162. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Walshe C, et al. Understanding the role and deployment of volunteers within specialist palliative care services and organisations as they have adjusted to the COVID-19 pandemic: A multi-national EAPC volunteer taskforce survey. Palliat Med. 2023;37:203–214. doi: 10.1177/02692163221135349. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Fish EC, Lloyd A. Moral distress amongst palliative care doctors working during the COVID-19 pandemic: A narrative-focussed interview study. Palliat Med. 2022;36:955–963. doi: 10.1177/02692163221088930. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Kirby EEF, et al. COVID-19 an its psychical influences on the perception of the nursing staff of oncological palliative care. 2021.
- 36.Figueiredo SV, et al. Atuação da equipe de cuidados paliativos frente a pacientes com a covid-19. Enfermagem em Foco. 2021;12.
- 37.Rosa WE, Lynch KA, Hadler RA, Mahoney C, Parker PA. “Doing palliative care with my hands tied behind my back”: telepalliative care delivery for oncology inpatients during a COVID-19 surge. Transl Behav Med. 2022;12:816–824. doi: 10.1093/tbm/ibac044. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Oluyase AO, et al. The challenges of caring for people dying from COVID-19: a multinational, observational study (CovPall) J Pain Symptom Manag. 2021;62:460–470. doi: 10.1016/j.jpainsymman.2021.01.138. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Siqueira ASdA, et al. COVID-19 in oncology palliative care: psychological stress from the perspective of psychodynamics at work. 2021. [DOI] [PubMed]
- 40.Tong W, et al. Perspectives of Remote Volunteer Palliative Care Consultants During COVID: A Qualitative Study. J Pain Symptom Manag. 2022;63:321–329. doi: 10.1016/j.jpainsymman.2021.07.028. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Johnson J, Al Bulushi A, Idris Z, Essa ZA, Hassan A. The experience of palliative care nurses in qatar during the time of COVID-19: a qualitative study. J Nurs Res. 2023;10.1097. [DOI] [PubMed]
- 42.Wenzel D, Bleazard L, Wilson E, Faull C. Impact on staff of providing non-invasive advanced respiratory support during the COVID-19 pandemic: a qualitative study in an acute hospital. BMJ Open. 2022;12:e060674. doi: 10.1136/bmjopen-2021-060674. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Dunleavy L, et al. ‘Necessity is the mother of invention’: Specialist palliative care service innovation and practice change in response to COVID-19. Results from a multinational survey (CovPall) Palliat Med. 2021;35:814–829. doi: 10.1177/02692163211000660. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Rosa WE, Lynch KA, Hadler RA, Mahoney C, Parker PA. “It took away and stripped a part of myself”: Clinician distress and recommendations for future telepalliative care delivery in the cancer context. Am J Hosp Palliat Med®. 2023;40:235–243. doi: 10.1177/10499091221101883. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Seibel K, et al. Implementation of an acute palliative care unit for COVID-19 patients in a tertiary hospital: qualitative data on clinician perspectives. Palliat Med. 2022;36:332–341. doi: 10.1177/02692163211059690. [DOI] [PubMed] [Google Scholar]
- 46.Finuf KD, Lopez S, Carney MT. Coping through COVID-19: A mixed method approach to understand how palliative care teams managed the COVID-19 pandemic. Am J Hosp Palliat Med®. 2022;39:874–880. doi: 10.1177/10499091211045612. [DOI] [PubMed] [Google Scholar]
- 47.Gardiner C, Harrison M, Hargreaves S, Taylor B. Clinical nurse specialist role in providing generalist and specialist palliative care: A qualitative study of mesothelioma clinical nurse specialists. J Adv Nurs. 2022;78:2973–2982. doi: 10.1111/jan.15277. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Navuluri N, Solomon HS, Hargett CW, Kussin PS. Distressed Work: Chronic Imperatives and Distress in Covid-19 Critical Care. Hast Center Rep. 2023;53:33–45. doi: 10.1002/hast.1458. [DOI] [PubMed] [Google Scholar]
- 49.Rogers M, et al. Perceptions of palliative care program viability during the pandemic: qualitative results from a national survey. Am J Hosp Palliat Med®. 2023;10499091231152610. [DOI] [PMC free article] [PubMed]
- 50.Sena B, De Luca E. Managing the end of life in COVID patients. The role of palliative care in emergency departments during the pandemic. Front Sociol. 2022;7. [DOI] [PMC free article] [PubMed]
- 51.Currin-McCulloch J, et al. Hearts above water: Palliative care during a pandemic. Soc Work Health Care. 2021;60:93–105. doi: 10.1080/00981389.2021.1885562. [DOI] [PubMed] [Google Scholar]
- 52.Collier A, Balmer D, Gilder E, Parke R. Patient safety and hospital visiting at the end of life during COVID-19 restrictions in Aotearoa New Zealand: a qualitative study. BMJ Qual Saf. 2023. [DOI] [PubMed]
- 53.De Luca E, Sena B, Cataldi S. Supporting ethical end-of-life care during pandemic: palliative care team perspectives. Nurs Ethics. 2023;09697330231153684. [DOI] [PMC free article] [PubMed]
- 54.Butkevičienė R, et al. Being heard: A qualitative study of Lithuanian health care professionals’ perceptions of dignity at the end-of-life. Medicina. 2021;57:1318. doi: 10.3390/medicina57121318. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Schallenburger M, et al. Inpatient generalist palliative care during the SARS-CoV-2 pandemic–experiences, challenges and potential solutions. 2022. [DOI] [PMC free article] [PubMed]
- 56.Back AL, Grant MS, McCabe PJ. Public messaging for serious illness care in the age of coronavirus disease: cutting through misconceptions, mixed feelings, and distrust. J Palliat Med. 2021;24:816–819. doi: 10.1089/jpm.2020.0719. [DOI] [PubMed] [Google Scholar]
- 57.Aaronson EL, et al. The experience of emergency department providers with embedded palliative care during COVID. J Pain Symptom Manag. 2020;60:e35–e43. doi: 10.1016/j.jpainsymman.2020.08.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.Vesel T, Ernst E, Vesel L, McGowan K, Stopka TJ. A qualitative study of the role of palliative care during the COVID-19 pandemic: perceptions and experiences among critical care clinicians, hospital leaders, and spiritual care providers. Am J Hosp Palliat Care. 2021;10499091211055900. [DOI] [PMC free article] [PubMed]
- 59.Böger R, et al. Palliative professionals: stressors imposed on the team in the death and dying process. Texto & Contexto-Enfermagem. 2022;31.
- 60.Ninteau K, Bishop CE. Nursing home palliative care during the pandemic: Directions for the future. Innov Aging. 2022;6:igac030. doi: 10.1093/geroni/igac030. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.McMillan K, Wright DK, McPherson CJ, Ma K, Bitzas V. Visitor Restrictions, Palliative Care, and Epistemic Agency: A Qualitative Study of Nurses’ Relational Practice During the Coronavirus Pandemic. Glob Qual Nurs Res. 2021;8:23333936211051702. doi: 10.1177/23333936211051702. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Wiebe E, et al. How the experience of medical assistance in dying changed during the COVID-19 pandemic in Canada: a qualitative study of providers. Can Med Assoc Open Access J. 2021;9:E400–E405. doi: 10.9778/cmajo.20200163. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63.Mitchinson L, et al. Missing the human connection: A rapid appraisal of healthcare workers’ perceptions and experiences of providing palliative care during the COVID-19 pandemic. Palliat Med. 2021;35:852–861. doi: 10.1177/02692163211004228. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.Tavares P, Rodrigues C, Neto IG, Rodrigues Sr C, Neto I. The impact of COVID-19 on palliative care: Perspective of healthcare professionals. Cureus. 2021;13. [DOI] [PMC free article] [PubMed]
- 65.Pfeifer L, Lwin T, Fitzgibbons L, Gillette S, Melton E. Joining forces: the addition of a palliative care practitioner to a resident teaching service during COVID-19 pandemic as a tool to improve patient care and provider communication. Am J Hosp Palliat Med®. 2022;10499091221121809. [DOI] [PMC free article] [PubMed]
- 66.Cross SH, Ramkalawan JR, Ring JF, Boucher NA. “That Little Bit of Time”: Transition-to-Hospice Perspectives From Hospice Staff and Bereaved Family. Innov Aging. 2022;6:igab057. doi: 10.1093/geroni/igab057. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67.Galchutt P, Labuschagne D, Usset T. Patient-Family Experience at the Onset of COVID-19: Interviews with Ten Palliative Chaplains. J Palliat Med. 2022;25:1222–1227. doi: 10.1089/jpm.2021.0550. [DOI] [PubMed] [Google Scholar]
- 68.Costantini M, Sleeman KE, Peruselli C, Higginson IJ. Response and role of palliative care during the COVID-19 pandemic: a national telephone survey of hospices in Italy. Palliat Med. 2020;34:889–895. doi: 10.1177/0269216320920780. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Janssen DJA. Palliative care in COVID-19. Curr Opin Support Palliat Care. 2021;15:199–204. doi: 10.1097/SPC.0000000000000567. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Etkind SN, et al. The role and response of palliative care and hospice services in epidemics and pandemics: a rapid review to inform practice during the COVID-19 pandemic. J Pain Symptom Manag. 2020;60:e31–e40. doi: 10.1016/j.jpainsymman.2020.03.029. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 71.Edmonds PM, et al. The impact of and response to the COVID-19 pandemic on a hospital palliative care team. Futur Healthc J. 2021;8:62–64. doi: 10.7861/fhj.2020-0131. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 72.Mitchell S, Maynard V, Lyons V, Jones N, Gardiner C. The role and response of primary healthcare services in the delivery of palliative care in epidemics and pandemics: A rapid review to inform practice and service delivery during the COVID-19 pandemic. Palliat Med. 2020;34:1182–1192. doi: 10.1177/0269216320947623. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73.de Boer M, Coghlan RJ, Russell B, Philip JA. The underrepresentation of palliative care in global guidelines for responding to infectious disease outbreaks: a systematic narrative review. Int Health. 2022;14:453–467. doi: 10.1093/inthealth/ihab075. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 74.Davies A, Hayes J. Palliative care in the context of a pandemic: similar but different. Clin Med. 2020;20:274. doi: 10.7861/clinmed.2020-0157. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 75.Bolt SR, et al. Practical nursing recommendations for palliative care for people with dementia living in long-term care facilities during the COVID-19 pandemic: A rapid scoping review. Int J Nurs Stud. 2021;113:103781. doi: 10.1016/j.ijnurstu.2020.103781. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Koffman J, Shapiro GK, Schulz-Quach C. Enhancing equity and diversity in palliative care clinical practice, research and education. BioMed Central. 2023;22:1–3. doi: 10.1186/s12904-023-01185-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77.Mojtahedi Z, Shen JJ. Home palliative care during the COVID-19 pandemic: a scoping review. Am J Hosp Palliat Med®. 2023;40:216–224. doi: 10.1177/10499091221093314. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 78.Tseng H-C, Chen T-F, Chou S-M. SARS: Key factors in crisis management. J Nurs Res. 2005;13:58–65. doi: 10.1097/01.JNR.0000387526.99770.1e. [DOI] [PubMed] [Google Scholar]
- 79.Honey M, Wang WY. New Zealand nurses perceptions of caring for patients with influenza A (H1N1) Nurs Crit Care. 2013;18:63–69. doi: 10.1111/j.1478-5153.2012.00520.x. [DOI] [PubMed] [Google Scholar]
- 80.Al Knawy BA, et al. Perceptions of postoutbreak management by management and healthcare workers of a Middle East respiratory syndrome outbreak in a tertiary care hospital: a qualitative study. BMJ Open. 2019;9:e017476. doi: 10.1136/bmjopen-2017-017476. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 81.Reeves S, Pelone F, Harrison R, Goldman J, Zwarenstein M. Interprofessional collaboration to improve professional practice and healthcare outcomes. Cochrane Database Syst Rev. 2017. [DOI] [PMC free article] [PubMed]
- 82.Brenner KO, et al. Referral relationship: illuminating the ways palliative care creates a holding environment for referring clinicians. J Palliat Med. 2022;25:185–192. doi: 10.1089/jpm.2021.0527. [DOI] [PubMed] [Google Scholar]
- 83.Jones CA, Bull J, Acevedo J, Kamal AH. Top ten inpatient palliative medicine billing and coding mistakes (and how to fix them this week) J Palliat Med. 2015;18:211–216. doi: 10.1089/jpm.2015.0005.18.3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 84.Bull C, Byrnes J, Hettiarachchi R, Downes M. A systematic review of the validity and reliability of patient-reported experience measures. Health Serv Res. 2019;54:1023–1035. doi: 10.1111/1475-6773.13187. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 85.Walling AM, et al. Patient-reported quality measures for palliative care: the time is now. J Pain Symptom Manag. 2023;65:87–100. doi: 10.1016/j.jpainsymman.2022.11.001. [DOI] [PubMed] [Google Scholar]
- 86.Gilmore KJ, Corazza I, Coletta L, Allin S. The uses of patient reported experience measures in health systems: a systematic narrative review. Health Policy. 2023;128:1–10. doi: 10.1016/j.healthpol.2022.07.008. [DOI] [PubMed] [Google Scholar]
- 87.Roberts BW, Roberts MB, Mazzarelli A, Trzeciak S. Validation of a 5-Item tool to measure patient assessment of clinician compassion in hospitals. J Gen Int Med. 2021. [DOI] [PMC free article] [PubMed]
- 88.Sinclair S, et al. Development and validation of a patient-reported measure of compassion in healthcare: the Sinclair Compassion Questionnaire (SCQ) BMJ Open. 2021;11:e045988–e045988. doi: 10.1136/bmjopen-2020-045988. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 89.Beldick SR, et al. Physician Executive Leadership Plus: An Approach to Business and Management Education for Medical Students. J Med Educ Curricular Dev. 2021;8:23821205211051803. doi: 10.1177/23821205211051803. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 90.Collins-Nakai R. Leadership in medicine. McGill J Med: MJM. 2006;9:68. [PMC free article] [PubMed] [Google Scholar]
- 91.Till A, McKimm J, Swanwick T. The importance of leadership development in medical curricula: a UK perspective (stars are aligning). J Healthc Leadersh. 2020;19-25. [DOI] [PMC free article] [PubMed]
- 92.Dahlin C, Coyne P, Goldberg J, Vaughan L. Palliative care leadership. J Palliat Care. 2019;34:21–28. doi: 10.1177/0825859718791427. [DOI] [PubMed] [Google Scholar]
- 93.Dahlin C, et al. The Cambia Sojourns Scholars Leadership Program: Projects and Reflections on Leadership in Palliative Care. J Palliat Med. 2019;22:823–829. doi: 10.1089/jpm.2018.0523. [DOI] [PubMed] [Google Scholar]
- 94.Hewison A, Sawbridge Y, Tooley L. Compassionate leadership in palliative and end-of-life care: A focus group study. Leadersh Health Serv. 2019;32:264–279. doi: 10.1108/LHS-09-2018-0044. [DOI] [PubMed] [Google Scholar]
- 95.Honey M, Wang WY. New Zealand nurses perceptions of caring for patients with influenza A (H1N1) Nurs Crit Care. 2013;18:63–69. doi: 10.1111/j.1478-5153.2012.00520.x. [DOI] [PubMed] [Google Scholar]
- 96.Li WW, Chhabra J, Singh S. Palliative care education and its effectiveness: a systematic review. Public Health. 2021;194:96–108. doi: 10.1016/j.puhe.2021.02.033. [DOI] [PubMed] [Google Scholar]
- 97.Scholz B, Bevan A, Georgousopoulou E, Collier A, Mitchell I. Consumer and carer leadership in palliative care academia and practice: A systematic review with narrative synthesis. Palliat Med. 2019;33:959–968. doi: 10.1177/0269216319854012. [DOI] [PubMed] [Google Scholar]
- 98.Lyons O, et al. Evidence-based medical leadership development: a systematic review. BMJ Lead. 2021;5. [DOI] [PubMed]
- 99.Lerman C, Jameson JL. Leadership development in medicine. N Engl J Med. 2018;378:1862. doi: 10.1056/NEJMp1801610. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 100.van Diggele C, Burgess A, Roberts C, Mellis C. Leadership in healthcare education. BMC Med Educ. 2020;20:1–6. doi: 10.1186/s12909-020-02288-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 101.Hjiej G, et al. Knowledge, attitudes, and practice of leadership skills among undergraduate medical students. Acta Bio Medica: Atenei Parmensis. 2023;94. [DOI] [PMC free article] [PubMed]
- 102.Ferris FD, Moore SY, Callaway MV, Foley KM. Leadership development initiative: Growing global leaders… advancing palliative care. J Pain Symptom Manag. 2018;55:S146–S156. doi: 10.1016/j.jpainsymman.2017.05.011. [DOI] [PubMed] [Google Scholar]
- 103.Barker L. Effective leadership within hospice and specialist palliative care units. J Manag Med. 2000;14:291–309. doi: 10.1108/02689230010362909. [DOI] [PubMed] [Google Scholar]
- 104.Angood P, Birk S. The value of physician leadership. Physician Exec. 2014;40:6–20. [PubMed] [Google Scholar]
- 105.Kotter JP. Leading change, (Harvard business press, 2012).
- 106.Chrislip DD. The collaborative leadership fieldbook, (John Wiley & Sons, 2002).
- 107.Linden RM. Working across boundaries: Making collaboration work in government and nonprofit organizations, (John Wiley & Sons, 2003).
- 108.Parapini M, Hirpara D, Scott T, Sidhu R, Karimuddin A. Leadership Development Programs for Surgical Residents: A Narrative Review of the Literature. Health Sci Rev. 2022;3:100025. [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.