Abstract
Objectives:
We present our initial clinical experience applying Natural Orifice Transluminal Endoscopic Surgical (NOTES) technique to perform cholecystectomy in ten patients at a military institution.
Methods:
A posterior colpotomy was created to accommodate a single site working port used to facilitate dissection and gallbladder mobilization under direct visualization via an infraumbilical port. The specimen was retrieved through the vagina and the colpotomy was closed with absorbable suture under direct visualization. Long-term follow up was performed over the phone to assess quality of life with 2 widely used health-related quality of life (HRQoL) surveys including RAND-36 Health Item Survey (Version 1.0),1 and the Female Sexual Function Index (FSFI).2
Results:
Ten women underwent a laparoscopic-assisted transvaginal cholecystectomy (TVC) with 7 available for long-term follow-up. The average age was 28.9 years (20–37) and the indications for surgery included symptomatic cholelithiasis (9) and biliary dyskinesia (1). The mean operative time was 129 mins (95–180), and median blood loss was 34 ml (5–400). There were no conversions and the average length of stay was 9.98 hours (2.4–28.8). Pain (analogue scale 1–10) on postoperative day three was minimal (mean 2.3) and was limited to the infraumbilical incision. On average patients returned to work by postoperative day six and resumed normal daily activities at seven days. Immediate postoperative complications included one incident of postoperative urinary retention requiring bladder catheterization. One intra-operative cholangiogram was successfully performed due to elevated preoperative liver enzymes without significant findings. Long-term complications included one asymptomatic incisional hernia repair at the infraumbilical port site. The RAND-36 survey demonstrated an average physical and mental health summary score of 82.2 and 63.7 with an average general health score of 63.6. The average FSFI total score was 21.8.
Conclusion:
TVC is safe and effective. Implementation may improve operational readiness by returning service members to normal activities more expeditiously than conventional laparoscopy.
Keywords: Endoscopic surgery, Natural orifice transluminal endoscopic surgery, NOTES, Transvaginal cholecystectomy
INTRODUCTION
Natural orifice transluminal endoscopic surgery (NOTES) is a technique defined by surgery performed through a natural orifice and has been successfully applied to many procedures including appendectomy, sigmoidectomy, peroral esophageal myotomy, necrosectomy, and cholecystectomy.3 NOTES was first described by Kalloo et al in 2004 in response to the 1998 meeting of the Apollo Group, intended to drive innovation in endoscopic therapies.4 In 2005, SAGES and the ASGE created the Natural Orifice Surgery Consortium for Assessment and Research (NOSCAR), a framework for advancement in the field.3 Shortly thereafter, the first successful transvaginal cholecystectomies (TVCs) were described by several pioneering groups.5–8
Since 2005, several large registries have demonstrated most NOTES procedures to be hybridized TVCs.9–12 While innovative in cholecystectomy, the TV route for specimen extraction, has historical precedent for both gynecologic and nongynecologic procedures.13–15 The first TV hysterectomy was reported 200 years ago16 and the technique of achieving entry to the abdominal cavity via posterior colpotomy has been described since the 1940s.17
Hybridized NOTES is differentiated from pure NOTES by virtue of a laparoscopic assist.3 While pure NOTES has been described,8,18–20 it is rarely performed due to concern for inadequate instruments and increased technical difficulty.21 The primary technical challenges are thought to be associated with inability to achieve triangulation to facilitate safe and effective retraction, exposure, and dissection.21 Several randomized controlled trials have demonstrated the safety, efficacy, and noninferiority of TVC, but have not proven a clear benefit over conventional laparoscopic cholecystectomy (CLC).22–25 TVC may cause less postoperative pain than CLC25–33 and has been associated with a shorter LOS9,26 and faster recovery,30,31,34–36 but this remains controversial in the literature.
We sought to evaluate the safety and efficacy of TVC performed in a population of active duty service members and their families at a military treatment facility. We studied the impact of TVC on patients returning to work. Our primary objective ascertained if this technique, as compared to CLC, can expedite the return of the patient to work – or the return of the warfighter to the battlefield, to improve operational readiness, reduce periods of vulnerability, and support military lethality.
MATERIALS AND METHODS
A prospective institutional review board (IRB) approved study of 10 women with nonurgent indications for cholecystectomy was performed. From Dec 2009 through Jan 2016 TVC was offered to female active duty, retired military personnel and their beneficiaries. There was significant delay in publishing these results due to war-time operational tempo, military training demands, and a recent pandemic. Inclusion criteria included between ages 18 to 50 years old, with a clinical indication for cholecystectomy and American Society of Anesthesiologists (ASA) classification of I. Exclusion criteria included radiographic evidence of possible gallbladder malignancy or choledocholithiasis, prior open abdominal or TV surgery, body mass index (BMI) ≥ 35, pregnancy, history of pelvic inflammatory disease, ectopic pregnancy, severe endometriosis, or use of anticoagulant therapy.
All patients participating in this protocol received counseling by the principal investigator (PI) on the TVC technique as well as potential risks and benefits as compared to CLC. The PI was the primary surgeon and had fellowship training in minimally invasive surgery as well as NOTES techniques. Prior to initiation of the study, the team, consisting of general surgery and support from the Department of Gynecology trained in the TV approach, honed the technique in a series of cadaver and swine training sessions. Postoperatively all patients maintained logs for one week following surgery and were questioned as to whether they would recommend the procedure to a friend.
Five year follow up included all patients also receiving a RAND 36-Item Health Survey (Version 1.0).1 The RAND is a widely used health-related quality of life (HRQoL) survey, which assesses the impact of health on an individual’s perceived well-being across 8 domains: physical functioning, bodily pain, role limitations due to physical health problems, role limitations due to personal or emotional problems, emotional well-being, social functioning, energy/fatigue, and general health perceptions.1 Each item is scored linearly from 0 to 100 such that a higher number represents a more desirable state of health.1 A physical health summary score is calculated by averaging the scores of physical functioning, physical role limitations, pain, and general health.37 A mental health summary score is calculated by averaging the scores of energy, social functioning, emotional role limitations, and mental health.37
The Female Sexual Function Index (FSFI) questionnaire first described by Rosen in 2000,38 is a 19-item self-report of female sexual function across 6 domains including arousal, desire, lubrication, orgasm, satisfaction, and pain. The sum of each domain is multiplied by a domain-specific factor to calculate the domain total.2 Domain totals are then summed to calculate the FSFI total, shown to be suggestive of female sexual dysfunction over the preceding 4 weeks if ≤26.55 (specificity 0.733, sensitivity 0.889).39 Of note, the FSFI cannot be used in isolation to diagnose female sexual dysfunction because there is no assessment of distress. It can give meaningful data over time reflecting response to intervention or treatment. The domain of desire can be evaluated independently using the established cutoff value of 5 to indicate hypoactive sexual disorder.40 All other domains do not have proven cutoff values and therefore cannot be assessed independently.2 The FSI has been validated on clinically diagnosed samples of women with female sexual arousal disorder (FSAD), female orgasmic disorder (FOD), and hypoactive sexual desire disorder (HSDD). All patients were also specifically examined for the presence of incisional hernia at 6 months postoperatively.
Operative Techniques
Following intubation, patients were placed in lithotomy (Figure 1) and a urinary catheter was inserted. The vaginal vault was prepared followed by the abdomen in the standard fashion.
Figure 1.
Patient and surgical team positioning. Endoscopic unit is a Stryker TowerTM.
Pneumoperitoneum was established using a Veress needle in an infraumbilical position followed by introduction of an optically guided 5 mm trocar. After an initial visual assessment, the patient was placed in Trendelenburg. With the assistance of the gynecology team, the uterus was manipulated anteriorly to expose the posterior vaginal fornix.
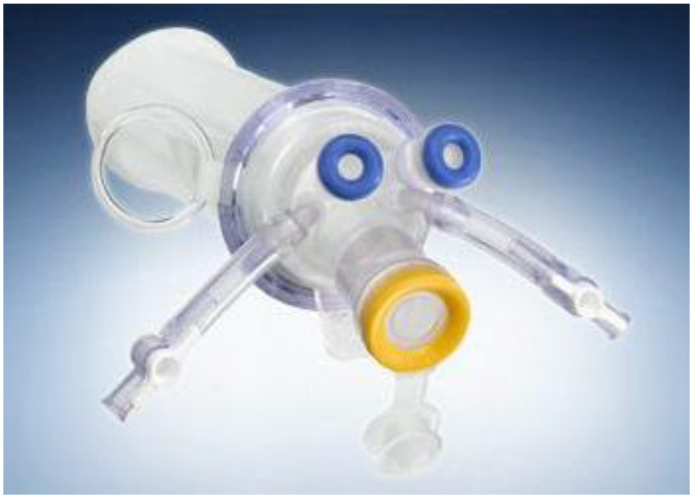
Under direct visualization, a posterior colpotomy was created using a 15-mm Ethicon Endopath XCEL Bladeness Trocar™ port, which was then removed and replaced with a Triport™ (TriPort, Olympus, Center Valley, PA) single site port (Figure 2). The patient was placed in the standard cholecystectomy left decubitus position with reverse Trendelenburg.
Figure 2.
Olympus Triport™ (TriPort, Olympus, Center Valley, PA) single site port.
Dissection proceeded via the umbilical trocar facilitated by retraction and optics using a 10-mm 45°F laparoscope via the TV port. After the critical view of safety was obtained, the cystic duct and artery were ligated and divided between 5-mm metallic clips placed through the 5-mm umbilical port. Standard bariatric-length rigid and reusable instruments were used except for the EndograbTM, intra-corporeal gallbladder retractor (Endograb, Virtual Ports, Caesarea, Israel). The specimen was removed transvaginally under laparoscopic visualization via the umbilical port. Colpotomy closure was performed with a running absorbable suture under direct visualization.
Patients were monitored for 2 hours postoperatively and were discharged in accordance with standard criteria. The patients were provided with a log to record their pain levels and medication use for 7 days postoperatively. Follow-up was arranged with the operating surgeon 1 and 2 weeks postoperatively and separately with the Department of Gynecology.
RESULTS
Successful TVC was performed in all ten patients although only 7 were able to be reached for long-term follow-up. There was one intra-operative cholangiogram for elevated preoperative liver enzymes without significant findings and one planned concomitant tubal ligation. The mean operating time was just over two hours and decreased over the course of the study. There was an average estimated blood loss of 34 mL and no intra-operative complications. The average length of stay was 9.98 hours. Postoperative complications were limited to one incident of urinary retention requiring bladder catheterization.
Patient logs were inventoried and supplemented with virtual interviews as well as the FSFI and RAND-36 surveys at one month and 5 years postoperatively respectively. The average pain on postoperative day 3 was 2.25 on a visual scale of 1–10 (Table 1). The average time to return to normal activities was reported as 7.33 days with an average time to return to work of 6 days. Postoperative pain patient logs did not quantify pain medication requirement. Complications included one asymptomatic umbilical port site hernia reported 1 year postoperatively. Of note, the patient who developed an umbilical hernia had a pre-existing hernia through which the 5-mm port was placed. There were no reports of postoperative fever or weight change.
Table 1.
Patient Outcomes
| Patient | f/u Years | Hernia | Pain |
|---|---|---|---|
| 1 | 5 | No | 6.0 |
| 2 | 5 | No | 6.0 |
| 3 | 5 | No | 3.6 |
| 4 | 5 | No | 3.6 |
| 5 | 5 | No | 0.0 |
| 6 | 5 | No | 5.6 |
| 7 | 4 | Yes | 5.2 |
The average FSFI total score was 21.8 (Table 2). The only independently assessable domain, desire, had an average score of 3.8. The RAND-36 survey demonstrated an average physical and mental health summary score of 82.2 and 63.7 with an average general health score of 63.6 (Table 3).
Table 2.
FSFI Questionnaire Results
| Patient | FSFI | Desire | Arousal | Lubrication | Orgasm | Satisfaction | Pain |
|---|---|---|---|---|---|---|---|
| 1 | 31.4 | 3.6 | 5.4 | 6 | 5.2 | 5.2 | 6 |
| 2 | 34.2 | 4.8 | 5.7 | 5.7 | 6 | 6 | 6 |
| 3 | 22.4 | 3.6 | 3.3 | 5.1 | 4 | 2.8 | 3.6 |
| 4 | 12.9 | 1.2 | 1.5 | 3 | 2 | 1.6 | 3.6 |
| 5 | 6 | 4.8 | 0 | 0 | 0 | 1.2 | 0 |
| 6 | 26 | 2.4 | 3.6 | 3.6 | 5.2 | 5.6 | 5.6 |
| 7 | 19.4 | 6 | 4.2 | 0 | 0 | 4 | 5.2 |
Table 3.
RAND 36 Health Survey (Version 1) Results
| Patient | PCS | MCS | Physical Function | Physical Role Limits | Emotional Role Limits | Energy | Emotional Well-Being | Social Function | Pain | General Health |
|---|---|---|---|---|---|---|---|---|---|---|
| 1 | 88.8 | 90.8 | 100.0 | 100.0 | 100.0 | 75.0 | 88.0 | 100.0 | 80.0 | 75.0 |
| 2 | 84.4 | 88.5 | 95.0 | 100.0 | 100.0 | 70.0 | 84.0 | 100.0 | 77.5 | 65.0 |
| 3 | 69.4 | 37.9 | 100.0 | 75.0 | 0.0 | 25.0 | 64.0 | 62.5 | 57.5 | 45.0 |
| 4 | 69.4 | 41.5 | 80.0 | 75.0 | 33.3 | 30.0 | 40.0 | 62.5 | 67.5 | 55.0 |
| 5 | 95.0 | 64.3 | 100.0 | 100.0 | 33.3 | 65.0 | 84.0 | 75.0 | 100.0 | 80.0 |
| 6 | 82.5 | 59.1 | 90.0 | 100.0 | 33.3 | 60.0 | 68.0 | 75.0 | 90.0 | 50.0 |
| 7 | 86.3 | 82.1 | 80.0 | 100.0 | 100.0 | 65.0 | 76.0 | 87.5 | 90.0 | 75.0 |
| Mean: | 82.2 | 63.7 | 92.1 | 92.9 | 57.1 | 55.7 | 55.7 | 80.4 | 80.4 | 63.6 |
Abbreviations: PCS, physical composite score, MCS, mental composite score.
DISCUSSION
TVC has been widely demonstrated to be noninferior to CLC and may be associated with decreased postoperative pain,26–30 shorter length of stay,26 and possible faster return to work,30,34–36,41 as well as improved cosmesis.26,27,34 Additionally, complications have been comparable to CLC.22,24–26,28–30,34 Despite the potential advantages and proven safety profile, there has been declining interest over the almost 20 years since the technique was first described.9,42
In a systematic review of patient's perception of NOTES procedures, Pucher et al observed an overall 41%–41% acceptance rate suggesting strong interest.43 Of those patients who have had TVC, 93% would recommend the procedure to another patient.22 Motivating factors include the perception of reduced pain and recovery time, improved cosmesis, and reduced risk of hernia.43 Patient concerns, including those of male partners, have primarily centered on uncertainty regarding the effect on future pregnancies and sexual function particularly among younger women.44–48 Interestingly, patients with a medical education have been shown to be significantly less likely to choose NOTES procedures than those without.44 In a survey of 600 resident and attending surgeons, 91.5% reported they would not choose a single-incision or NOTES procedure for themselves.49
The primary patient concerns regarding sexual health and future pregnancies have been largely disproven in the literature. Colpotomy in the setting of TVC has not been shown to have any negative affect on female sexual function, quality of life,26,50–54 or pregnancy.54 In a retrospective cohort study of 88 patients, Bulian et al observed no significant changes in postoperative sexual function, menorrhea, or vaginal discharge at an average of two years postoperatively from TVC.35 A subsequent systematic review by Donatsky et al reported rates of de novo dyspareunia and vaginal pain or discomfort following TVC between 0% and 12.5% with no impairment of sexual function noted.53 Additionally, there is no evidence that NOTES procedures using TV access have any negative effect on conception, pregnancy, or delivery.54
NOTES procedures have also been shown to cause less pain than conventional laparoscopy,12 however, data pertaining to TVC specifically in support of this finding is limited to meta-analyses26–30 and prospective cohort studies31–33 and has not been reproduced in randomized controlled trials.22,24,25 The International Multicenter Trial on Clinical Natural Orifice Surgery (IMTN) Registry captured 362 patients from 16 centers across 9 countries having undergone NOTES procedures and demonstrated less pain in NOTES patients than in those having had conventional laparoscopy.12 While this study is inclusive of all NOTES procedures, Ghezzi et al demonstrated significantly less pain following TV specimen extraction than transumbilical extraction suggesting a consistent relationship.55 While randomized controlled trials comparing TVC to CLC have not detected a difference in postoperative pain, they may have been limited by inconsistent methods of pain assessment and ineffective poor blinding procedures.22,24,25 Furthermore, pain assessment methods such as having the patient cough while lying in bed may not accurately elicit pain which might be evident with activity.24
Incisional pain is of particular interest to our study because it is the primary factor related to delay of discharge and return to normal activity in patients after CVC.56 While some studies have shown a reduced length of stay26 and faster recovery,30,34–36,41 others have not.22,24,25,28,29 Of note, these findings may be confounded by institutional mandates such as the routine two-day hospital stay following laparoscopic cholecystectomy in Germany.34,57 Medication use, perhaps a better indicator of postoperative pain, may be reduced in patients following TVC as compared to CLC.26,31,33,41 Lehmann et al reported that 25% of NOTES patients captured in the German National Registry (GNR) had no pain medication requirement at all.10 While analgesia use has been inconsistently reported and not clearly associated with a universally decreased length of stay, there are multiple large series demonstrating no postoperative analgesia in significant portions of patients.10,12
Another factor potentially contributing to pain is variability in the number of additional abdominal trocars used beyond the single port for hybridized assist. Additional trocars have been reported in up to 8.6% of TVC26 with a mean of between 1.3 and 1.45 in large series.10,22,32 Although the conversion rate to conventional laparoscopy is between 2%–2%,22,26 the definition of conversion is unclear. Further studies are needed to determine if, given the known learning curve, experience with NOTES procedures is correlated with decreased number of additional abdominal trocars and perhaps reduced pain. Regardless, the overall patient satisfaction and cosmetic result has been shown to be significantly improved amongst TVC patients as compared to CLC.25–27,57–59
In addition to reduced or equivalent postoperative pain, there is no evidence of increased complications in TVC as compared to CLC.22,24–26,28–30,34 In a retrospective analysis of 571 TVCs over a 10-year period, Rössler et al observed a major complication rate of 1.6%.60 The incidence of bile duct injuries has been reported as 0.7%, slightly higher than in conventional laparoscopy.61 Interestingly, all bile duct injuries occurred in elective surgeries and were treated successfully with ERCP and stenting.60 In a systematic review and meta-analysis Sodergren et al did not note any significant differences in the rate of bile duct injury between TVC and CLC, although it is a rare event irrespective of approach and the studies included may not have been adequately powered to detect a difference.34 Minor complications such as vaginal bleeding have been reported but observed to stop spontaneously or with direct pressure.26 Theoretical complications include bowel herniation and vaginal cuff dehiscence,18 but have not been reported in the literature to our knowledge. Complication reporting in NOTES procedures has lacked standardization, which may create variability in interpretation.62
Access-related complications including injuries to the rectum, small bowel, and bladder have been reported,10 but there is significant data to support the safety of TV access.63 In a retrospective review of 102 TV access procedures, Woods et al reported an overall complication rate of 9.8% with a significant decrease after 50 cases.64 In a multinational retrospective study of 3,667 TV procedures performed by 44 gynecologists from 18 different countries, Gordts et al demonstrated a full thickness bowel injury rate of 0.65% which decreased to 0.25% after 50 cases and were all managed conservatively.63 A learning curve of 10–15 cases amongst laparoscopic surgeons performing TVC has been reported.65–67 Becerra et al noted greater improvement in those with less laparoscopic experience suggesting the importance of this skill and translation to NOTES using rigid instruments as opposed to flexible endoscopy.66 Van Den Boezem et al reported a decrease in operative time from 90 minutes to 55 minutes after 10 cases.65 The operative time has generally been shown to be longer in NOTES procedures and TVC specifically,22,24–26,28,29,34 but may decrease significantly with experience.
TV access has been further criticized for being limited to the female population, however, females are at increased risk of gallbladder pathology.68 Although universally available, transgastric (TG) access may be associated with a more difficult closure than TV access which can be performed under direct visualization.69–72 In the setting of cholecystectomy, TG access often involves visual inversion,58 retroflexion, and additional laparoscopic suturing to facilitate gastrostomy closure.12,71 There may be a greater learning curve in TG cholecystectomy due to the requirement for advanced endoscopic skills.12 In their review of the IMTN Registry, Zorron et al found that TG surgery was associated with a higher rate of complications and longer operative time than TV access procedures.12 The European clinical NOTES registry, captured an operative time in TG cholecystectomy almost double that of TVC and further associated with an increased requirement for additional trocar placement, and conversion to laparoscopy.9 TG surgery is also limited by the esophageal diameter to the extraction of relatively smaller specimens than the TV access.12 Conversely, extraction of pelvic masses up to 19 cm via posterior colpotomy has been reported without access-related morbidity.55
There has been additional hesitancy to pursue TV access as it requires incision of an otherwise uninvolved organ and was thought to potentially contaminate the peritoneum. While the colpotomy is typically five times as large as standard laparoscopic ports,28 there have been no reports to our knowledge of prolapse or complications associated with the incision itself. Peritoneal contamination following TV procedures has been demonstrated in preclinical models to be low.73–75 Lomanto et al specifically compared TV to TG access and found a lower risk of intra-abdominal contamination and sepsis in TV procedures.73 Preclinical studies have further demonstrated minimal and abridged systemic inflammation and a decreased immunologic response relative to CLC.75–77
Contraindications to TVC access are widely variable, but generally extend to infectious and inflammatory disease of the abdomen or pelvis to include acute cholecystitis, as well as prior surgery.12,18,34,65,78 TVC has also historically not been offered to patients with a BMI over 35,79 due to data associating obesity with increased operative time in laparoscopic cholecystectomy80–82 and increased risk of conversion from laparoscopic to open cholecystectomy,83,84 suggesting a more difficult procedure with an increased risk of complications. The safety and efficacy of NOTES TVC as an alternative to conventional laparoscopy in the morbidly obese has been proven.69,85–88 The available data suggest there is no increased risk of complications or pain in TVC performed in obese patients as compared to nonobese.10,85–87 Increasing BMI may be associated increased rates of conversion to open, longer operative time, higher number of percutaneous trocars, and increased length of stay.10,86 Some studies, however, observed no relationship between operative time and BMI.85
TVC has also been successfully performed in patients with prior abdominal surgery to include hysterectomy as well as gastric bypass and sleeve procedures.33,60,79,89 Given the altered anatomy and potential for adhesions especially in vicinity of the posterior vaginal vault, hysterectomy may increase the risk of complications particularly those related to access such as urinary bladder perforation.89 The GNR demonstrated an increased incidence of bladder injury amongst patients with prior hysterectomy.11 Rössler et al, however, in their review of 571 TVC’s over a 10-year period, found no difference.60 While the data are unclear regarding the incidence of bladder injury in this demographic, the overall complications have not been shown to be increased despite longer associated operating times.89
Key steps of TVC are the choice of endoscope, establishment of peritoneal access, dissection, extraction, and closure of the access site.90 Issues surrounding NOTES include poor operative field visibility, limited instrument maneuverability, increased grasping distances, and lack of specific suturing and anastomotic devices designed for NOTES.3 TVC typically requires adaptive curved instruments significantly longer than those for laparoscopic surgery.91,92 There is significant heterogeneity in procedural methodology and equipment. Both flexible6,69 and rigid8,79,93,94 instruments have been described as has the use of modified transanal endoscopic microsurgery equipment.91
The primary challenges associated with TVC and, pure NOTES TVC especially, are related to the colocation of instruments. Operative instruments and endoscopes working in parallel create the possibility for interferences, hinders effective manipulation, and does not facilitate triangulation as movement is constrained to the long axis.58,94–96 This may significantly limit exposure, dissection, and field of view potentially increasing the risk of injury while instruments are out of sight.97 In a task-analysis of CLC versus TVC, Nemani et al demonstrated increased errors in the TVC group due to instruments being out of sight whereas the CLC group had more errors due to lack of progress.98 It may also be more difficult to obtain the critical view of safety while working from a relatively more posterior angle.18
Hybridization is the predominant approach in TVC because it addresses many of these challenges.10 It also facilitates the passage of surgical clips, which is critical as historically available endoscopic clips are not intended and should not be used for full occlusion of the cystic artery and/or duct.18,58,72,96 Endoscopic clips may become dislodged99–101 and cannot achieve complete occlusion due to a hinge gap such that they are only occlusive at the distal tip.7,18,102 Some authors have described manual straightening of endoscopic clips to mitigate this issue and facilitate placement, however, while successful, this technique is inefficient and not ideal given that it requires modifying a manufactured product.18,95 Prototype flexible clip appliers capable of complete occlusion have been described103 including one with a zero-gap clip.97 Of note, clip placement using this prototype took 9 minutes, significantly longer than laparoscopic clip placement.97
In addition to the variable approach, there is also the choice of flexible or rigid instruments, both of which have been widely reported. Flexible endoscopes offer working ports for instruments, but require an additional skill set and potentially significant cost should equipment not be readily available.90 Furthermore, platform stability is sacrificed for maneuverability which may compromise the ability to create sufficient axial force, traction, and countertraction to facilitate efficient exposure and dissection.90,96 While the grasper allows for some traction, the endoscope is unable to simultaneously dissect.95 Rigid instruments allow for improved stability, resolution, field of view, and picture quality as well as independence of working instruments from visualization.90 Conversely, they are limited to access near natural orifices and dissection in-line with the direction of access.90 In a review of the EURO-NOTES Clinical Registry, inclusive of all NOTES procedures in the first five years of its clinical implementation, Arezzo et al demonstrated a significantly shorter operative time overall using rigid instruments as compared to flexible instruments.9
The lack of NOTES-specific instruments, a process significantly delayed by federal regulations, has been a major issue in limiting adoption.3 Additional issues with current procedural terminology (CPT), coding process, third-party-payer approvals, and hospital credentialing and purchasing processes as well as the requirement for IRB approval on all NOTES procedures, have also contributed to delayed integration.3 Instruments not only NOTES-compatible, but designed to address specific associated challenges, are available.104 Magnetic anchoring systems (MAS), for example, may allow for triangulation by improving the stability of flexible platforms facilitating multiaxial traction and countertraction in NOTES procedures by coupling internal components to external components.104–106 Preclinical studies of MAS experienced failures attributed to inadvertent magnetic coupling, but noted significant improvement over time as technique was refined.104 Even with appropriate equipment, however, it has been suggested that robotization may be necessary before more widespread adoption is possible.107 Robotic systems specific to endoluminal procedures have been developed108,109 and shown in randomized controlled trials to improve dissection and shorten operating time.110
There are several limitations to this study. This prospective study had a small sample size and the operations were completed over a decade ago. The population of patients was restricted to military personnel and their family members undergoing elective and highly selective cases. Lastly, the amount of pain medication taken postoperatively was not collected and therefore no comment on the relationship between TVC and postoperative pain medication requirement is available. Definitive conclusions from this data cannot be applied to the general population.
Importantly, the HRQoL surveys chosen for long-term follow up likely report results irrelevant to the index NOTES procedure. The results of the RAND-36 and the FSFI have limited relevance due to the collection in isolation and lack of established patient’s baseline, which make it difficult to assess the effect of the operation on these outcomes. Furthermore, the RAND-36 was conducted 5 years postoperatively at which time their quality of life as assessed by the survey was likely temporally separated from the effect of the operation because they had fully recovered. The FSFI was discordant from patient logs and showed most patients to have results suggestive of female sexual dysfunction and hypoactive sexual disorder. Importantly, FSFI is not diagnostic of female sexual dysfunction because it does not assess distress and, therefore, these findings are highly unlikely that all seven women had results objectively suggestive of this disorder without any endorsing symptoms elsewhere. We recommend future research efforts conduct both the RAND-36 and the FSFI prior to study initiation and at more than one time point postoperatively, to establish a baseline and better informed data interpretation.
The military relevant benefits of this technique are primarily related to the potential for expedited return of the warfighter back to the fight and limited restrictions for service member return to work. Future use of NOTES techniques in forward deployed environment may obviate the requirement for a sterile operating room environment, provide procedures that are less resource demanding and allow for broader implementation of invasive procedures performed closer to the point of injury as well as to service members in austere environments.
In conclusion, TVC is a novel technique which may improve operational readiness by returning service members to normal activities more expeditiously than traditional laparoscopy. Further research is to understand if there are significant decreases in pain, wound infection, complications, operative times associated with NOTES TVC.
Footnotes
Acknowledgements: The authors would like to express our appreciation for the support of Annissa Cromer, RN for her enthusiastic support of this study in the operating room and Amy Black, NP for her dedication to collecting the long-term follow up information. All individuals in acknowledgements have given written permission to be named.
All authors fulfill ICMJE authorship criteria.
Military disclaimer: the views expressed in this article reflect the results of research, opinions, interpretations, conclusions, and recommendations of the author and do not necessarily reflect the official policy or position of the Departments of the Army, Navy, Departments of Defense, nor the U.S. Government.
Disclosure: Drs Judge, Bandle, Wang, Gadbois, Simsiman, and Wood have no conflicts of interest to disclose. Dr Wisbach serves as a consultant for Intuitive Surgical Inc.
Ethical approval: All procedures performed in this study that involved human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Declarations: Awards – Second Place – 30th Annual Navy-wide Academic Research Competition, May 26, 2015.
Data availability: data are available upon request for the methods and materials related to this project.
Podium presentations: 5th Annual UCSD NOTES Surgical Symposium, San Diego, California in 2011; Society of American Gastrointestinal and Endoscopic Surgeons, San Diego, California in 2012; Academic Research Competition, Navy Medical Center San Diego in 2015; Third Military Surgical Symposium, SAGES in Boston, Massachusetts in 2016.
References:
- 1.Hays RD, Morales LS. The RAND-36 measure of health-related quality of life. Ann Med. 2001;33(5):350–357. [DOI] [PubMed] [Google Scholar]
- 2.Meston CM, Freihart BK, Handy AB, Kilimnik CD, Rosen RC. Scoring and interpretation of the FSFI: what can be learned from 20 years of use? J Sex Med. 2020;17(1):17–25. [DOI] [PubMed] [Google Scholar]
- 3.Rattner DW, Hawes R, Schwaitzberg S, Kochman M, Swanstrom L. The second SAGES/ASGE white paper on natural orifice transluminal endoscopic surgery: 5 years of progress. Surg Endosc. 2011;25(8):2441–2448. [DOI] [PubMed] [Google Scholar]
- 4.Kalloo AN, Singh VK, Jagannath SB, et al. Flexible transgastric peritoneoscopy: a novel approach to diagnostic and therapeutic interventions in the peritoneal cavity. Gastrointest Endosc. 2004;60(1):114–117. [DOI] [PubMed] [Google Scholar]
- 5.Zornig C, Emmermann A, Von Waldenfels HA, Mofid H. Laparoscopic cholecystectomy without visible scar: combined transvaginal and transumbilical approach. Endoscopy. 2007;39(10):913–915. [DOI] [PubMed] [Google Scholar]
- 6.Marescaux J, Dallemagne B, Perretta S, Wattiez A, Mutter D, Coumaros D. Surgery without scars: report of transluminal cholecystectomy in a human being. Arch Surg. 2007;142(9):823–826. [DOI] [PubMed] [Google Scholar]
- 7.Bessler M, Stevens PD, Milone L, Parikh M, Fowler D. Transvaginal laparoscopically assisted endoscopic cholecystectomy: a hybrid approach to natural orifice surgery. Gastrointest Endosc. 2007;66(6):1243–1245. [DOI] [PubMed] [Google Scholar]
- 8.Ramos AC, Murakami A, Galvão Neto M, et al. NOTES transvaginal video-assisted cholecystectomy: first series. Endoscopy. 2008;40(7):572–575. [DOI] [PubMed] [Google Scholar]
- 9.Arezzo A, Zornig C, Mofid H, et al. The EURO-NOTES clinical registry for natural orifice transluminal endoscopic surgery: a 2-year activity report. Surg Endosc. 2013;27(9):3073–3084. [DOI] [PubMed] [Google Scholar]
- 10.Lehmann KS, Zornig C, Arlt G, et al. Natural orifice transluminal endoscopic surgery in Germany: data from the German NOTES registry. Chirurg. 2015;86(6):577–586. [DOI] [PubMed] [Google Scholar]
- 11.Lehmann KS, Ritz JP, Wibmer A, et al. The German registry for natural orifice translumenal endoscopic surgery: report of the first 551 patients. Ann Surg. 2010;252(2):263–270. [DOI] [PubMed] [Google Scholar]
- 12.Zorron R, Palanivelu C, Galvão Neto MP, et al. International multicenter trial on clinical natural orifice surgery–NOTES IMTN study: preliminary results of 362 patients. Surg Innov. 2010;17(2):142–158. [DOI] [PubMed] [Google Scholar]
- 13.Childers JM, Huang D, Surwit EA. Laparoscopic trocar-assisted colpotomy. Obstet Gynecol. 1993;81(1):153–155. [PubMed] [Google Scholar]
- 14.Emmermann A, Zornig C, Peiper M, Weh HJ, Broelsch CE. Laparoscopic splenectomy: technique and results in a series of 27 cases. Surg Endosc. 1995;9(8):924–927. [PubMed] [Google Scholar]
- 15.Delvaux G, Devroey P, De Waele B, Willems G. Transvaginal removal of gallbladders with large stones after laparoscopic cholecystectomy. Surgical Laparoscopy & Endoscopy. 1993;3(4):307–309. [PubMed] [Google Scholar]
- 16.Sutton C. “The history of vaginal hysterectomy,” in Vaginal Hysterectomy, CRC Press. 2001:11–16. eBook ISBN: 9780429221040. [Google Scholar]
- 17.Decker A, Cherry TH. Culdoscopy: a new method in the diagnosis of pelvic disease—preliminary report. The Am J Surg. 1944;64(1):40–44. [Google Scholar]
- 18.Gumbs AA, Fowler D, Milone L, et al. Transvaginal natural orifice translumenal endoscopic surgery cholecystectomy: early evolution of the technique. Ann Surg. 2009;249(6):908–912. [DOI] [PubMed] [Google Scholar]
- 19.Bessler M, Gumbs AA, Milone L, Evanko JC, Stevens P, Fowler D. Video. Pure natural orifice transluminal endoscopic surgery (NOTES) cholecystectomy. Surg Endosc. 2010;24(9):2316–2317. [DOI] [PubMed] [Google Scholar]
- 20.de Sousa LH, de Sousa JAG, de Sousa Filho LH, et al. Totally NOTES (T-NOTES) transvaginal cholecystectomy using two endoscopes: preliminary report. Surg Endosc. 2009;23(11):2550–2555. [DOI] [PubMed] [Google Scholar]
- 21.Huang C, Huang R-X, Qiu Z-J. Natural orifice transluminal endoscopic surgery: new minimally invasive surgery come of age. World J Gastroenterol. 2011;17(39):4382–4388. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Borchert DH, Federlein M, Fritze-Büttner F, et al. Postoperative pain after transvaginal cholecystectomy: single-center, double-blind, randomized controlled trial. Surg Endosc. 2014;28(6):1886–1894. [DOI] [PubMed] [Google Scholar]
- 23.Bulian DR, Knuth J, Cerasani N, Sauerwald A, Lefering R, Heiss MM. Transvaginal/transumbilical hybrid–NOTES–versus 3-trocar needlescopic cholecystectomy: short-term results of a randomized clinical trial. Ann Surg. 2015;261(3):451–458. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Noguera JF, Cuadrado A, Dolz C, Olea JM, García JC. Prospective randomized clinical trial comparing laparoscopic cholecystectomy and hybrid natural orifice transluminal endoscopic surgery (NOTES)(NCT00835250. Surg Endosc. 2012;26(12):3435–3441. [DOI] [PubMed] [Google Scholar]
- 25.Schwaitzberg SD, Roberts K, Romanelli JR, et al. Natural Orifice Surgery Consortium for Assessment and Research® (NOSCAR®) Clinical Trial Group. The NOVEL trial: natural orifice versus laparoscopic cholecystectomy-a prospective, randomized evaluation. Surg Endosc. 2018;32(5):2505–2516. [DOI] [PubMed] [Google Scholar]
- 26.Xu B, Xu B, Zheng W-Y, et al. Transvaginal cholecystectomy vs conventional laparoscopic cholecystectomy for gallbladder disease: a meta-analysis. World J Gastroenterol. 2015;21(17):5393–5406. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Bulian DR, Knuth J, Lehmann KS, Sauerwald A, Heiss MM. Systematic analysis of the safety and benefits of transvaginal hybrid-NOTES cholecystectomy. World J Gastroenterol. 2015;21(38):10915,–10925. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Peng C, Ling Y, Ma C, et al. Safety outcomes of NOTES cholecystectomy versus laparoscopic cholecystectomy: a systematic review and meta-analysis. Surg Laparosc Endosc Percutan Tech. 2016;26(5):347–353. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Xu J, Xu L, Li L, Zha S, Hu Z. Comparison of outcome and side effects between conventional and transvaginal laparoscopic cholecystectomy: a meta-analysis. Surg Laparosc Endosc Percutan Tech. 2014;24(5):395–399. [DOI] [PubMed] [Google Scholar]
- 30.Yang E, Nie D, Li Z. Comparison of major clinical outcomes between transvaginal notes and traditional laparoscopic surgery: a systematic review and meta-analysis. J Surg Res. 2019;244:278–290. [DOI] [PubMed] [Google Scholar]
- 31.Ansari AM, Kaushal G, Dhillon KS. An observational study comparing hybrid transvaginal notes and four-port laparoscopic cholecystectomy. Cureus. 2023;15(1):e33589. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Borchert DH, Federlein M, Rückbeil O, Schöpe J. Less pain after transvaginal cholecystectomy: single-center pooled analysis. Surg Endosc. 2017;31(6):2573–2576. [DOI] [PubMed] [Google Scholar]
- 33.Benhidjeb T, Kosmas IP, Hachem F, Mynbaev O, Stark M, Benhidjeb I. Laparoscopic cholecystectomy versus transvaginal natural orifice transluminal endoscopic surgery cholecystectomy: results of a prospective comparative single-center study. Gastrointest Endosc. 2018;87(2):509–516. [DOI] [PubMed] [Google Scholar]
- 34.Sodergren MH, Markar S, Pucher PH, Badran IA, Jiao LR, Darzi A. Safety of transvaginal hybrid NOTES cholecystectomy: a systematic review and meta-analysis. Surg Endosc. 2015;29(8):2077–2090. [DOI] [PubMed] [Google Scholar]
- 35.Bulian DR, Trump L, Knuth J, Cerasani N, Heiss MM. Long-term results of transvaginal/transumbilical versus classical laparoscopic cholecystectomy—an analysis of 88 patients. Langenbecks Arch Surg. 2013;398(4):571–579. [DOI] [PubMed] [Google Scholar]
- 36.Bulian DR, Trump L, Knuth J, et al. Less pain after transvaginal/transumbilical cholecystectomy than after the classical laparoscopic technique: short-term results of a matched-cohort study. Surg Endosc. 2013;27(2):580–586. [DOI] [PubMed] [Google Scholar]
- 37.Ware JE. “SF-36 physical and mental health summary scales: a user’s manual,” (No Title). 1994; ISBN: 1891810006. [Google Scholar]
- 38.Rosen R, Brown C, Heiman J, et al. The Female Sexual Function Index (FSFI): a multidimensional self-report instrument for the assessment of female sexual function. J Sex Marital Ther. 2000;26(2):191–208. [DOI] [PubMed] [Google Scholar]
- 39.Wiegel M, Meston C, Rosen R. The female sexual function index (FSFI): cross-validation and development of clinical cutoff scores. J Sex Marital Ther. 2005;31(1):1–20. [DOI] [PubMed] [Google Scholar]
- 40.Gerstenberger EP, Rosen RC, Brewer JV, et al. Sexual desire and the female sexual function index (FSFI): a sexual desire cutpoint for clinical interpretation of the FSFI in women with and without hypoactive sexual desire disorder. J Sex Med. 2010;7(9):3096–3103. [DOI] [PubMed] [Google Scholar]
- 41.Wood SG, Dabu-Bondoc S, Dai F, Mikhael H, Vadivelu N, Roberts KE. Comparison of immediate postoperative pain after transvaginal versus traditional laparoscopic cholecystectomy. Surg Endosc. 2014;28(4):1141–1145. [DOI] [PubMed] [Google Scholar]
- 42.Steinemann DC, Zerz A, Adamina M, et al. Single-incision and natural orifice translumenal endoscopic surgery in Switzerland. World J Surg. 2017;41(2):449–456. [DOI] [PubMed] [Google Scholar]
- 43.Pucher PH, Sodergren MH, Lord AC, Teare J, Yang G-Z, Darzi A. Consumer demand for surgical innovation: a systematic review of public perception of NOTES. Surg Endosc. 2015;29(4):774–780. [DOI] [PubMed] [Google Scholar]
- 44.Benhidjeb T, Benhidjeb I, Stark M, et al. Women’s perception of transgastric and transvaginal natural orifice transluminal endoscopic surgery (NOTES)–impact of medical education, stage of life and cross-cultural aspects. Int J Womens Health. 2022;14:1881–1895. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Behnia-Willison F, Nguyen T, Rezaeimotlagh A, Baekelandt J, Hewett PJ. Middle Eastern women’s attitudes and expectations towards vaginal natural orifice transluminal endoscopic surgery (vNOTES): a survey-based observational study. Surg Endosc. 2021;35(12):6865–6872. [DOI] [PubMed] [Google Scholar]
- 46.Strickland AD, Norwood MG, Behnia-Willison F, Olakkengil SA, Hewett PJ. Transvaginal natural orifice translumenal endoscopic surgery (NOTES): a survey of women’s views on a new technique. Surg Endosc. 2010;24(10):2424–2431. [DOI] [PubMed] [Google Scholar]
- 47.Bucher P, Ostermann S, Pugin F, Morel P. Female population perception of conventional laparoscopy, transumbilical LESS, and transvaginal NOTES for cholecystectomy. Surg Endosc. 2011;25(7):2308–2315. [DOI] [PubMed] [Google Scholar]
- 48.Kobiela J, Stefaniak T, Dobrowolski S, Makarewicz W, Lachiński AJ, Sledziński Z. Transvaginal NOTES cholecystectomy in my partner? No way! Wideochir Inne Tech Maloinwazyjne. 2011;6(4):236–241. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Lima DL, Lima RNC, Dos Santos DC, Shadduck PP, Carvalho GL, Malcher F. Which cholecystectomy technique would surgeons prefer on themselves? Surg Laparosc Endosc Percutan Tech. 2020;30(6):495–499. [DOI] [PubMed] [Google Scholar]
- 50.Wood SG, Solomon D, Panait L, Bell RL, Duffy AJ, Roberts KE. Transvaginal cholecystectomy: effect on quality of life and female sexual function. JAMA Surg. 2013;148(5):435–438. [DOI] [PubMed] [Google Scholar]
- 51.Tolcher MC, Kalogera E, Hopkins MR, Weaver AL, Bingener J, Dowdy SC. Safety of culdotomy as a surgical approach: implications for natural orifice transluminal endoscopic surgery. JSLS. 2012;16(3):413–420. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Long CY, Fang JH, Chen WC, Su JH, Hsu SC. Comparison of total laparoscopic hysterectomy and laparoscopically assisted vaginal hysterectomy. Gynecol Obstet Invest. 2002;53(4):214–219. [DOI] [PubMed] [Google Scholar]
- 53.Donatsky AM, Jørgensen LN, Meisner S, Vilmann P, Rosenberg J. Sexual function after transvaginal cholecystectomy: a systematic review. Surg Laparosc Endosc Percutan Tech. 2014;24(4):290–295. [DOI] [PubMed] [Google Scholar]
- 54.Thomaidis P, et al. Transvaginal Hybrid-NOTES procedures—do they have a negative impact on pregnancy and delivery? Langenbeck’s Arch Surg, pp. 2021:1–8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Ghezzi F, Raio L, Mueller MD, Gyr T, Buttarelli M, Franchi M. Vaginal extraction of pelvic masses following operative laparoscopy. Surg Endosc. 2002;16(12):1691–1696. [DOI] [PubMed] [Google Scholar]
- 56.Bisgaard T, Kehlet H, Rosenberg J. Pain and convalescence after laparoscopic cholecystectomy. Eur J Surg. 2001;167(2):84–96. [DOI] [PubMed] [Google Scholar]
- 57.Zornig C, Siemssen L, Emmermann A, et al. NOTES cholecystectomy: matched-pair analysis comparing the transvaginal hybrid and conventional laparoscopic techniques in a series of 216 patients. Surg Endosc. 2011;25(6):1822–1826. [DOI] [PubMed] [Google Scholar]
- 58.Niu J, Song W, Yan M, et al. Transvaginal laparoscopically assisted endoscopic cholecystectomy: preliminary clinical results for a series of 43 cases in China. Surg Endosc. 2011;25(4):1281–1286. [DOI] [PubMed] [Google Scholar]
- 59.Bulian DR, Knuth J, Cerasani N, et al. Transvaginal hybrid NOTES cholecystectomy–results of a randomized clinical trial after 6 months. Langenbecks Arch Surg. 2014;399(6):717–724. [DOI] [PubMed] [Google Scholar]
- 60.Rössler F, Keerl A, Bieri U, Slieker J, Nocito A. Natural orifice transluminal endoscopic surgery: long-term experience with hybrid transvaginal cholecystectomies. Surg Innov. 2020;27(6):594–601. [DOI] [PubMed] [Google Scholar]
- 61.Pesce A, Portale TR, Minutolo V, Scilletta R, Destri GL, Puleo S. Bile duct injury during laparoscopic cholecystectomy without intraoperative cholangiography: a retrospective study on 1,100 selected patients. Dig Surg. 2012;29(4):310–314. [DOI] [PubMed] [Google Scholar]
- 62.Borchert DH, Federlein M, Müller VA, Wagenpfeil S, Eisele RM. Comprehensive complication index for NOTES procedures: results from a randomized controlled trial and comparison to published NOTES complication data. Surg Endosc. 2015;29(10):2928–2933. [DOI] [PubMed] [Google Scholar]
- 63.Gordts S, Watrelot A, Campo R, Brosens I. Risk and outcome of bowel injury during transvaginal pelvic endoscopy. Fertil Steril. 2001;76(6):1238–1241. [DOI] [PubMed] [Google Scholar]
- 64.Wood SG, Panait L, Duffy AJ, Bell RL, Roberts KE. Complications of transvaginal natural orifice transluminal endoscopic surgery: a series of 102 patients. Ann Surg. 2014;259(4):744–749. [DOI] [PubMed] [Google Scholar]
- 65.van den Boezem PB, Velthuis S, Lourens HJ, Samlal RAK, Cuesta MA, Sietses C. Hybrid transvaginal cholecystectomy, clinical results and patient-reported outcomes of 50 consecutive cases. J Gastrointest Surg. 2013;17(5):907–912. [DOI] [PubMed] [Google Scholar]
- 66.Becerra Garcia FC, Misra MC, Bhattacharjee HK, Buess G. Experimental trial of transvaginal cholecystectomy: an ex vivo analysis of the learning process for a novel single-port technique. Surg Endosc. 2009;23(10):2242–2249. [DOI] [PubMed] [Google Scholar]
- 67.Wood SG, Dai F, Dabu-Bondoc S, et al. Transvaginal cholecystectomy learning curve. Surg Endosc. 2015;29(7):1837–1841. [DOI] [PubMed] [Google Scholar]
- 68.Afdhal N, Zakko S. Gallstones: epidemiology, risk factors and prevention. UpToDate. https://www.uptodate.com/contents/gallstones-epidemiology-risk-factors-and-prevention?search=gallstone%20risk%20factors&source=search_result&selectedTitle=1∼150&usage_type=default&display_rank=1 Accessed April 29, 2023.
- 69.Forgione A, Maggioni D, Sansonna F, et al. Transvaginal endoscopic cholecystectomy in human beings: preliminary results. J Laparoendosc Adv Surg Tech A. 2008;18(3):345–351. [DOI] [PubMed] [Google Scholar]
- 70.Rattner D, Kalloo A, ASGE/SAGES Working Group. ASGE/SAGES Working Group on natural orifice translumenal endoscopic surgery: October 2005. Surg Endosc. 2006;20(2):329–333. [DOI] [PubMed] [Google Scholar]
- 71.Zorron R, Maggioni LC, Pombo L, Oliveira AL, Carvalho GL, Filgueiras M. NOTES transvaginal cholecystectomy: preliminary clinical application. Surg Endosc. 2008;22(2):542–547. [DOI] [PubMed] [Google Scholar]
- 72.Liu L, Chiu PWY, Reddy N, et al. APNOTES Working Group. Natural orifice transluminal endoscopic surgery (NOTES) for clinical management of intra-abdominal diseases. Dig Endosc. 2013;25(6):565–577. [DOI] [PubMed] [Google Scholar]
- 73.Lomanto D, Chua HC, Myat MM, So J, Shabbir A, Ho L. Microbiological contamination during transgastric and transvaginal endoscopic techniques. J Laparoendosc Adv Surg Tech A. 2009;19(4):465–469. [DOI] [PubMed] [Google Scholar]
- 74.Linke GR, Tarantino I, Hoetzel R, et al. Transvaginal rigid-hybrid NOTES cholecystectomy: evaluation in routine clinical practice. Endoscopy. 2010;42(7):571–575. [DOI] [PubMed] [Google Scholar]
- 75.Fan JKM, Tong DKH, Ho DWY, Luk J, Law WL, Law S. Systemic inflammatory response after natural orifice translumenal surgery: transvaginal cholecystectomy in a porcine model. JSLS. 2009;13(1):9–13. [PMC free article] [PubMed] [Google Scholar]
- 76.Suzuki K, Yasuda K, Kawaguchi K, et al. Cardiopulmonary and immunologic effects of transvaginal natural-orifice transluminal endoscopic surgery cholecystectomy compared with laparoscopic cholecystectomy in a porcine survival model. Gastrointest Endosc. 2010;72(6):1241–1248. [DOI] [PubMed] [Google Scholar]
- 77.Vieira JP, Linhares MM, Caetano EM, et al. Evaluation of the clinical and inflammatory responses in exclusively NOTES transvaginal cholecystectomy versus laparoscopic routes: an experimental study in swine. Surg Endosc. 2012;26(11):3232–3244. [DOI] [PubMed] [Google Scholar]
- 78.Federlein M, Borchert D, Müller V, et al. Transvaginal video-assisted cholecystectomy in clinical practice. Surg Endosc. 2010;24(10):2444–2452. [DOI] [PubMed] [Google Scholar]
- 79.Zornig C, Mofid H, Siemssen L, et al. Transvaginal NOTES hybrid cholecystectomy: feasibility results in 68 cases with mid-term follow-up. Endoscopy. 2009;41(5):391–394. [DOI] [PubMed] [Google Scholar]
- 80.Gatsoulis N, Koulas S, Kiparos G, et al. Laparoscopic cholecystectomy in obese and nonobese patients. Obes Surg. 1999;9(5):459–461. [DOI] [PubMed] [Google Scholar]
- 81.Hawn MT, Bian J, Leeth RR, et al. Impact of obesity on resource utilization for general surgical procedures. Ann Surg. 2005;241(5):821. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 82.Simopoulos C, Polychronidis A, Botaitis S, Perente S, Pitiakoudis M. Laparoscopic cholecystectomy in obese patients. Obes Surg. 2005;15(2):243–246. [DOI] [PubMed] [Google Scholar]
- 83.Rosen M, Brody F, Ponsky J. Predictive factors for conversion of laparoscopic cholecystectomy. Am J Surg. 2002;184(3):254–258. [DOI] [PubMed] [Google Scholar]
- 84.Livingston EH, Rege RV. A nationwide study of conversion from laparoscopic to open cholecystectomy. Am J Surg. 2004;188(3):205–211. [DOI] [PubMed] [Google Scholar]
- 85.Panait L, Wood SG, Bell RL, Duffy AJ, Roberts KE. Transvaginal natural orifice transluminal endoscopic surgery in the morbidly obese. Surg Endosc. 2013;27(7):2625–2629. [DOI] [PubMed] [Google Scholar]
- 86.Bulian DR, Knuth J, Thomaidis P, et al. Does obesity influence the results in transvaginal hybrid-NOTES cholecystectomy? Surg Endosc. 2018;32(11):4632–4638. [DOI] [PubMed] [Google Scholar]
- 87.Bulian DR, Walper S, Richards DC, et al. Comparative analysis of postoperative pain after transvaginal hybrid NOTES versus traditional laparoscopic cholecystectomy in obese patients. Surg Endosc. 2022;36(7):4983–4991. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 88.Decarli L, Zorron R, Branco A, et al. Natural orifice translumenal endoscopic surgery (NOTES) transvaginal cholecystectomy in a morbidly obese patient. Obes Surg. 2008;18(7):886–889. [DOI] [PubMed] [Google Scholar]
- 89.Bulian DR, Sauerwald A, Thomaidis P, et al. Does a prior hysterectomy complicate transvaginal/transumbilical hybrid NOTES cholecystectomy?—a comparative analysis of prospectively collected data. Langenbecks Arch Surg. 2022;407(2):655–662. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 90.Auyang ED, Santos BF, Enter DH, Hungness ES, Soper NJ. Natural orifice translumenal endoscopic surgery (NOTES(®)): a technical review. Surg Endosc. 2011;25(10):3135–3148. [DOI] [PubMed] [Google Scholar]
- 91.Buess G, Becerra-Garcia F, Misra MC. Instruments for transluminal laparoscopic surgery or ‘NOTES’.” Minim Invasive Ther Allied Technol. 2008;17(6):331–335. [DOI] [PubMed] [Google Scholar]
- 92.Brescia A, Masoni L, Gasparrini M, et al. Laparoscopic assisted transvaginal cholecystectomy: single centre preliminary experience. Surgeon. 2013;11 Suppl 1(1):S1–5. 10.1016/j.surge.2012.09.003. [DOI] [PubMed] [Google Scholar]
- 93.Roberts KE, Shetty S, Shariff AH, Silasi D-A, Duffy AJ, Bell RL. Transvaginal NOTES hybrid cholecystectomy. Surg Innov. 2012;19(3):230–235. [DOI] [PubMed] [Google Scholar]
- 94.Dhillon KS, Awasthi D, Dhillon AS. Natural orifice transluminal endoscopic surgery (hybrid) cholecystectomy: the Dhillon technique. J Minim Access Surg. 2017;13(3):176–181. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 95.Pulvirenti E, Toro A, Di Carlo I. Update on instrumentations for cholecystectomies performed via transvaginal route: state of the art and future prospectives. Diagn Ther Endosc. 2010;2010:405469. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 96.Pugliese R, Forgione A, Sansonna F, Ferrari GC, Di Lernia S, Magistro C. Hybrid NOTES transvaginal cholecystectomy: operative and long-term results after 18 cases. Langenbecks Arch Surg. 2010;395(3):241–245. [DOI] [PubMed] [Google Scholar]
- 97.Whang SH, Satgunam S, Miedema BW, Thaler K. Transvaginal cholecystectomy by using a prototype flexible clip applier. Gastrointest Endosc. 2010;72(2):351–357. [DOI] [PubMed] [Google Scholar]
- 98.Nemani A, Sankaranarayanan G, Olasky JS, et al. A comparison of NOTES transvaginal and laparoscopic cholecystectomy procedures based upon task analysis. Surg Endosc. 2014;28(8):2443–2451. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 99.Iida Y, Miura S, Munemoto Y, et al. Endoscopic resection of large colorectal polyps using a clipping method. Dis Colon Rectum. 1994;37(2):179–180. [DOI] [PubMed] [Google Scholar]
- 100.Jensen DM, Machicado GA. Hemoclipping of chronic canine ulcers: a randomized, prospective study of initial deployment success, clip retention rates, and ulcer healing. Gastrointest Endosc. 2009;70(5):969–975. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 101.Jensen DM, Machicado GA, Hirabayashi K. Randomized controlled study of 3 different types of hemoclips for hemostasis of bleeding canine acute gastric ulcers. Gastrointest Endosc. 2006;64(5):768–773. [DOI] [PubMed] [Google Scholar]
- 102.Bessler M, Stevens PD, Milone L, Hogle NJ, Durak E, Fowler D. Transvaginal laparoscopic cholecystectomy: laparoscopically assisted. Surg Endosc. 2008;22(7):1715–1716. [DOI] [PubMed] [Google Scholar]
- 103.Satgunam S, Miedema B, Whang S, Thaler K. Transvaginal cholecystectomy without laparoscopic support using prototype flexible endoscopic instruments in a porcine model. Surg Endosc. 2012;26(8):2331–2338. [DOI] [PubMed] [Google Scholar]
- 104.Scott DJ, Tang S-J, Fernandez R, et al. Completely transvaginal NOTES cholecystectomy using magnetically anchored instruments. Surg Endosc. 2007;21(12):2308–2316. [DOI] [PubMed] [Google Scholar]
- 105.Horgan S, Mintz Y, Jacobsen GR, et al. Video. Magnetic retraction for NOTES transvaginal cholecystectomy. Surg Endosc. 2010;24(9):2322. [DOI] [PubMed] [Google Scholar]
- 106.Ryou M, Thompson CC. Magnetic retraction in natural-orifice transluminal endoscopic surgery (NOTES): addressing the problem of traction and countertraction. Endoscopy. 2009;41(2):143–148. [DOI] [PubMed] [Google Scholar]
- 107.Gaillard M, Tranchart H, Lainas P, Dagher I. New minimally invasive approaches for cholecystectomy: review of literature. World J Gastrointest Surg. 2015;7(10):243–248. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 108.Sun Z, Ang RY, Lim EW, Wang Z, Ho KY, Phee SJ. Enhancement of a master-slave robotic system for natural orifice transluminal endoscopic surgery. Ann Acad Med Singap. 2167. 8013;40(5):223–230. [PubMed] [Google Scholar]
- 109.Rentschler ME, Dumpert J, Platt SR, Farritor SM, Oleynikov D. Natural orifice surgery with an endoluminal mobile robot. Surg Endosc. 2007;21(7):1212–1215. [DOI] [PubMed] [Google Scholar]
- 110.Phee SJ, Reddy N, Chiu PWY, et al. Robot-assisted endoscopic submucosal dissection is effective in treating patients with early-stage gastric neoplasia. Clin Gastroenterol Hepatol. 2012;10(10):1117–1121. [DOI] [PubMed] [Google Scholar]