Abstract
Introduction:
In-hospital cardiac arrest (IHCA) remains a substantial cause of morbidity and mortality for hospitalized patients worldwide. This study aimed to identify associated factors of return of spontaneous circulation (ROSC) and survival with favorable neurological outcomes of IHCA patients.
Method:
A two-year retrospective cohort study was conducted at a university-based tertiary care hospital in Bangkok, Thailand, studying adult patients aged ≥ 18 years with IHCA from January 2021 to December 2022. The primary endpoint was sustained ROSC, and the secondary endpoint was survival with favorable neurological outcomes defined as Cerebral Performance Categories (CPC) Scale of 1 or 2 at discharge. Pre-arrest and intra-arrest variables were collected and analyzed using multivariable logistic regression to identify independent factors associated with the outcomes.
Results:
During the study period, 156 patients were included in the study. 105 (67.3%) patients achieved sustained ROSC after the CPR, 28 patients (18.0%) were discharged alive, and 15 patients (9.6%) survived with a favorable neurological outcome at hospital discharge. Overall, sustained ROSC was higher in patients who had IHCA during the day shift (odds ratio (OR): 4.11; 95% confidence interval (CI): 1.05-16.06) and electrocardiogram (ECG) monitoring prior to arrest (OR: 6.38; 95% CI: 1.18-34.54). In contrast, higher adrenaline doses administrated, and increased CPR duration reduced the odds of sustained ROSC (OR: 0.72; 95% CI: 0.54-0.94 and OR: 0.92; 95% CI: 0.85-0.98, respectively). Arrest due to cardiac etiology was associated with increased discharged survival with favorable neurological outcomes (OR: 13.43; 95% CI: 2.00-89.80), while a higher Good Outcome Following Attempted Resuscitation (GO-FAR) score reduced the odds of the secondary outcome (OR: 0.89; 95% CI: 0.81-0.98).
Conclusion:
The sustained ROSC was higher in IHCA during the daytime shift and under prior ECG monitoring. The administration of higher doses of adrenaline and prolonged CPR durations decreased the likelihood of achieving sustained ROSC. Furthermore, patients with cardiac-related causes of cardiac arrest exhibited a higher rate of survival to hospital discharge with favorable neurological outcomes.
Key Words: Heart arrest, Hospitalization, Prognosis, Survival, Outcome assessment, health care
1. Introduction:
In-hospital cardiac arrest (IHCA) is defined as a sudden cardiac arrest within the hospital setting. It is a condition commonly encountered in medical practice, particularly among patients in the intensive care unit (ICU) and emergency department (ED), where the patients often have significant disease severity and comorbidities (1). Many research studies from various countries have reported the incidence of IHCA in adults to be approximately 1-6 events per 1,000 hospital admissions. The outcomes after IHCA are generally heterogeneous among countries, with overall survival at discharge and 1-year survival of these patients reported to be only about 17.6% and 13.4%, respectively (2). For this reason, the IHCA is considered a substantial cause of various complications and undesired treatment outcomes, leading to morbidity and mortality for hospitalized patients.
The 2020 American Heart Association (AHA) Guidelines for Cardiopulmonary Resuscitation (CPR) and Emergency Cardiovascular Care (ECC) have highlighted the importance of the chain of survival in IHCA patients, which includes early recognition, prevention, activation of the emergency response team, high-quality chest compression, defibrillation if indicated, and post-cardiac arrest care in ICU and recovery (3). During the past decade, knowledge advancement and clinical practice update on each part of the chain of survival has significantly improved the outcome of CPR and resuscitation effort for patients with cardiac arrest (4, 5). Studies on intra-arrest medications, post-cardiac arrest treatment, and prognostication are lacking, especially in low-resource settings (6).
Therefore, this research intends to investigate pre- and intra-arrest factors associated with survival and favorable outcomes after sudden IHCA.
2. Methods:
2.1 Study design and setting
This study was a retrospective cohort study conducted at an ED, general ward, ICU, and any location that IHCA occurred in Ramathibodi Hospital, Bangkok, Thailand. Ramathibodi Hospital is a tertiary medical institution serving as a hub for training, education, and referral services in super-tertiary medical care. The hospital accommodates a substantial daily volume of outpatient visits, with a minimum of 5,600 daily visits, and provides in-patient care through over 1,300 beds distributed across specialized departments and units. In adherence to hospital protocols, all instances of IHCA were systematically documented and recorded in the Ramathibodi CPR unit's cardiac arrest registry. In this study the associated factors of IHCA outcomes were evaluated and reported.
The study was approved by the Committee on Human Rights Related to Research Involving Human Subjects, Ramathibodi Hospital, Mahidol University (COA. MURA2023/145). Due to the retrospective design, the ethics committee waived the need for informed consent.
2.2 Participants
The participants included adult patients aged ≥ 18 years old who experienced IHCA during the period between January 2021 and December 2022. We excluded those with the following criteria: out of hospital cardiac arrest (OHCA) prior to hospital arrival, pregnancy, incomplete data record including survival outcome, recurrent episode of arrest and CPR after initially sustained return of spontaneous circulation (ROSC), and patients with immediate do-not-resuscitate (DNR) order.
2.3 Data gathering
The prognostic factors in this study include pre-arrest factors and intra-arrest factors associated with a sustained ROSC for more than 20 minutes, neurological outcome, and survival to hospital discharge.
The pre-arrest factors include gender, age, scene characteristics such as location and shifts, underlying diseases, neurological status based on Cerebral Performance Categories (CPC) Scale, primary diagnosis according to the International Classification of Diseases 10th Revision (ICD-10), intervention, vital signs, and laboratory findings before the event of cardiac arrest. We use the underlying diseases of each patient to calculate the Charlson Comorbidity Index (CCI) to demonstrate the severity of underlying diseases. The CCI is a prognostic score for predicting the 10-year survival rate in patients with multiple comorbidities (7).
We used the National Early Warning Score (NEWS) 2 score and Sequential Organ Failure Assessment (SOFA) score to identify the acute severity of illness for each included participant. NEWS2 is a simple aggregate scoring system combining six simple physiological parameters, including respiration rate, oxygen saturation, systolic blood pressure, pulse rate, level of consciousness, and temperature. NEWS2 was widely used to evaluate acute clinical illness severity and clinical deterioration in pre-hospital and hospital settings (8). SOFA score was initially introduced as a scoring system for evaluating the degree of organ dysfunction or failure. The score was later described as a potential tool for the prediction of mortality in critically ill patients (9). We also calculated the Good Outcome Following Attempted Resuscitation (GO-FAR) score for the data. The GO-FAR score was introduced in 2013 as a pre-arrest score to predict survival to discharge after CPR among IHCA cases with good neurological status (defined as a CPC score of 1) (10).
For intra-arrest factors, we recorded cardiac arrest etiology, CPR team activation, witness arrest, initial rhythm, total CPR time or time to ROSC, intervention, and laboratory test results if taken during cardiac arrest. We categorized ventricular fibrillation (VF) and ventricular tachycardia (VT) as shockable rhythms and pulseless electrical activity (PEA) and asystole as non-shockable rhythms. For the patients with sustained ROSC of more than 20 minutes, we collected the post-cardiac arrest parameters, including survival to discharge and neurological response and performance, to calculate the CPC score at discharge. All the data in this study was collected from the cardiac arrest registry, Ramathibodi CPR unit, and electronic emergency medical records (EMR).
2.4 Outcome measurement
We defined the primary outcome as sustained ROSC for over 20 minutes following CPR. The secondary outcome was survival at discharge with favorable neurological outcomes (a CPC score of 1 or 2).
2.5 Statistical analysis
The sample size for our study was calculated from Alnabels et al. research data, which was done as a single-center retrospective cohort study in patients older than 18 years with IHCA (11). In Alnabels et al.’s study, variables affecting survival to hospital discharge were studied. All factors that affected survival were considered, and the sample size was calculated using STATA version 16.1 (Alpha = 0.05, power = 0.8, and N2/N1 = 0.78). When calculating each variable to be used in our research, the lowest possible showed a statistically significant difference in the total number of patients (N), divided into 98 patients: 43 patients who survived until discharged from the hospital (N2) and 55 non-survivors (N1) from the minutes (time) to ROSC variable were obtained.
We used STATA version 17.0 to analyze our data. Univariable logistic analysis was used to compare the variables between sustained ROSC and non-sustained ROSC groups. Fisher’s exact test was used for categorical data with frequency and percentage, and the Student’s t-test results for continuous data was presented as mean ± standard deviation (SD). The power of discrimination was presented with 95% confidence intervals (CIs) and P-value.
In our analysis, we employed a multivariable logistic regression model to investigate potential confounding factors linked to the attainment of sustained ROSC and the likelihood of surviving to discharge while maintaining favorable neurological outcomes, denoted by a CPC score of 1 or 2. The results were presented in terms of odds ratios, accompanied by their respective 95% confidence intervals (CIs) and associated p-values. Additionally, we employed both backward elimination and stepwise selection techniques to iteratively refine the model by retaining only variables deemed statistically significant.
3. Results:
3.1. Baseline characteristics of studied cases
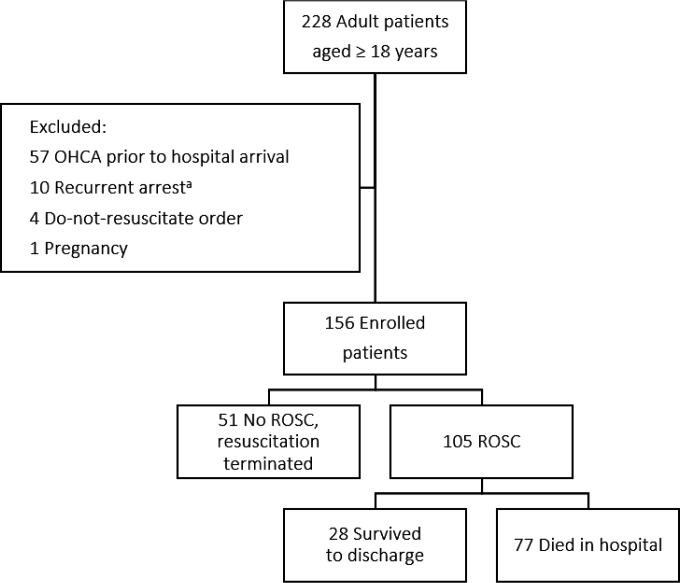
During the two-year study period, 228 adult patients aged ≥ 18 years experienced IHCA. After applying the exclusion criteria, 156 patients were entered into the study. From all enrolled participants, 105 (67.3%) patients achieved sustained ROSC after CPR, 28 patients (18.0%) were discharged alive, and 15 patients (9.6%) survived with a favorable neurological outcome (CPC scores 1 and 2) at hospital discharge, which accounts for 53.6% of the survivors (Figure 1).
Figure 1.
Flow diagram of the study. OHCA: Out-of-hospital cardiac arrest; ROSC: Return of spontaneous circulation. a recurrent event of arrest and cardiopulmonary resuscitation after initially sustained ROSC
Table 1 demonstrates baseline demographics, clinical characteristics, and pre- and post-arrest factors categorized based on whether the participant achieved sustained ROSC after the CPR. The mean age of patients in the study was 68.00 ± 18.00 years (54.5% male). General wards were the most common location of arrest, which accounted for about 40.4% of all cardiac arrest events.
Table 1.
Characteristics of studied patients according to sustained ROSC after cardiopulmonary resuscitation
| Variables |
All patients
( n = 156) |
Sustained ROSC | P | |
|---|---|---|---|---|
| Yes ( n = 105) | No ( n = 51) | |||
| Pre-arrest factors | ||||
| Age (year) | ||||
| Mean (±SD) | 68.19 (±17.67) | 68.30 (±18.07) | 67.96 (±16.97) | 0.910 |
| Gender | ||||
| Male | 85 (54.49) | 54 (51.43) | 31 (60.78) | 0.271 |
| Day shift | ||||
| 8 a.m. - 4 p.m | 58 (37.18) | 40 (38.10) | 18 (35.29) | 0.734 |
| Location of arrest | ||||
| Intensive care unita | 33 (21.15) | 24 (22.86) | 9 (17.65) | 0.370 |
| Intermediate ward | 14 (8.97) | 9 (8.57) | 5 (9.80) | |
| General ward | 63 (40.38) | 43 (40.95) | 20 (39.22) | |
| Emergency department | 34 (21.79) | 24 (22.86) | 10 (19.61) | |
| Others | 12 (7.69) | 5 (4.76) | 7 (13.73) | |
| Charlson comorbidity index | ||||
| Mean (±SD) | 5.33 (±2.79) | 5.51 (±2.85) | 4.94 (±2.64) | 0.229 |
| CPC scale | 0.127 | |||
| Good CPC scale (1, 2) | 120 (76.92) | 77 (73.33) | 43 (84.31) | |
| Poor CPC scale (3-5) | 36 (23.08) | 28 (26.67) | 8 (15.69) | |
| NEWS2 | ||||
| Mean (±SD) | 7.37 (±4.24) | 7.63 (±4.00) | 6.82 (±4.70) | 0.268 |
| SOFA score (N = 103) | ||||
| Mean (±SD) | 7.13 (±4.73) | 7.13 (±4.43) | 7.20 (±5.45) | 0.997 |
| GO-FAR score (N = 126) | ||||
| Mean (±SD) | 16.82 (±13.25) | 17.53 (±13.59) | 15.23 (±12.48) | 0.370 |
| Primary diagnosis | ||||
| Circulatory | 51 (32.69) | 31 (29.52) | 20 (39.22) | 0.055 |
| Respiratory | 30 (19.23) | 20 (19.05) | 10 (19.61) | |
| Neoplasms | 27 (17.31) | 19 (18.10) | 8 (15.69) | |
| Infectious disease | 11 (7.05) | 11 (10.48) | 0 (0.00) | |
| Gastrointestinal | 9 (5.77) | 4 (3.81) | 5 (9.80) | |
| Genitourinary | 9 (5.77) | 9 (8.57) | 0 (0.00) | |
| Injury and external cause | 9 (5.77) | 5 (4.76) | 4 (7.84) | |
| Other b | 10 (6.41) | 6 (5.71) | 4 (7.84) | |
| Other factors | ||||
| Mechanical ventilator | 76 (48.72) | 52 (49.52) | 24 (47.06) | 0.773 |
| Any vasoactive agent | 33 (21.15) | 21 (20.00) | 12 (23.53) | 0.613 |
| ECG monitoring | 105 (67.31) | 73 (69.52) | 32 (62.75) | 0.397 |
| Witness arrest | 119 (76.28) | 82 (78.10) | 37 (72.55) | 0.445 |
| CPR team resuscitation | 48 (30.77) | 31 (29.52) | 17 (33.33) | 0.629 |
| Intra-arrest Factors | ||||
| Arrest etiology | ||||
| Cardiac | 42 (26.92) | 25 (23.81) | 17 (33.33) | 0.009 |
| Respiratory | 45 (28.85) | 40 (38.10) | 5 (9.80) | |
| Infection | 23 (14.74) | 13 (12.38) | 10 (19.61) | |
| Neurological/stroke | 10 (6.41) | 6 (5.71) | 4 (7.84) | |
| Other | 36 (23.08) | 21 (20.00) | 15 (29.41) | |
| CPR characteristics | ||||
| Initial rhythm with shockable | 31 (20.13) | 18 (17.48) | 13 (25.49) | 0.243 |
| ETT during CPR | 68 (43.59) | 40 (38.10) | 28 (54.90) | 0.047 |
| Defibrillation | 42 (26.92) | 23 (21.90) | 19 (37.25) | 0.043 |
| Total adrenaline doses | 5.30 (±5.76) | 3.11 (±3.18) | 9.80 (±7.15) | <0.001 |
| Total bicarbonate doses | 1.28 (±1.80) | 1.01 (±1.60) | 1.82 (±2.05) | 0.008 |
| Time to adrenaline (minute) | 3.15 (±3.66) | 2.96 (±3.03) | 3.49 (±4.58) | 0.405 |
| CPR time (minute) | 21.20 (±20.29) | 12.55 (±11.73) | 39.00 (±22.58) | <0.001 |
Data are presented as mean (± standard deviation (SD)) or number (%). CPC: Cerebral Performance Categories; CPR: Cardiopulmonary resuscitation; ECG: electrocardiogram; ETT: Endotracheal tube; GO-FAR: Good Outcome Following Attempted Resuscitation; NEWS2: National Early Warning Score 2; ROSC: Return of spontaneous circulation; SOFA: Sequential Organ Failure Assessment. a Intensive care unit includes coronary care unit and intensive care unit. b Other includes Catheterization laboratory, Operating room, Outpatient department, X-RAY department, Hemodialysis center, and private room.
3.2. Univariable analysis
When comparing the two groups on the pre-arrest factors, there was no significant difference in age (p=0.910), gender (p=0.271), time of arrest (p=0.734), location of arrest (p=0.370), CCI (p=0.229), CPC scale (p=0.127), NEW2 score (p=0.268), SOFA score (p=0.997), GO-FAR score (p=0.370), mechanical ventilator use (p=0.773), vasoactive agent use (p=0.613), an electrocardiogram (ECG) monitoring (p =0.397), arrest being witnessed (p =0.445), or CPR team activation (p =0.629).
More than half of the causes of arrest were categorized as cardiac (26.92%) and respiratory (28.85%), followed by infection (14.74%). The patients with cardiac causes of arrest encompassed various clinical presentations, including acute coronary syndrome (19 patients), cardiac arrhythmias (12 patients), acute decompensation of chronic heart failure (9 patients), and cardiac tamponade (2 patients).
The arrest etiology significantly differed between the two groups, as the respiratory cause of arrest was more common in the sustained ROSC group than the non-ROSC group (38.10% vs. 9.80%, p = 0.009). Patients who achieved sustained ROSC also had fewer endotracheal tube (ETT) insertions during CPR (38.10% vs. 54.90%, p = 0.047) and fewer percentages of defibrillation (21.90% vs. 37.25%, p = 0.043) compared to the non-ROSC group. There were also significantly fewer doses of adrenaline (3.11± 3.18 vs. 9.80±7.15, p = <0.001) and bicarbonate (1.01±1.60 vs. 1.82±2.05, p = 0.008) used in sustained ROSC group with less total CPR time (12.55±11.73 minutes vs. 39.00±22.58 minutes, p ≤ 0.001). The two groups had no significant difference in initial rhythm and time to adrenaline.
3.3. Multivariable analysis
Sustained ROSC
The multivariable logistic regression analysis of factors associated with sustained ROSC following CPR is shown in Table 2. Patients who experienced IHCA during the day shift (8 a.m. - 4 p.m.) and patients who had ECG monitoring prior to arrest were independently associated with sustained ROSC (odds ratio (OR): 4.11; 95% CI :1.05-16.06 and OR: 6.38; 95% CI: 1.18-34.54, respectively). Higher total adrenaline dose and increased total CPR time in minutes were significantly negatively associated with sustained ROSC (OR: 0.72; 95% CI: 0.54-0.94 and OR: 0.92; 95% CI: 0.85-0.98, respectively). However, we found no significant association between GO-FAR score (p=0.271), arrest at the ICU (p=0.602), mechanical ventilator use (p=0.845), arrest being witnessed (p=0.470), CPR team activation (p=0.944), initial shockable rhythm (p=0.312), ETT during CPR (p=0.120), defibrillation during CPR (p=0.897), sodium bicarbonate dose provided during CPR (p=0.403), and time to first dose of adrenaline within 5 minutes after CPR initiation with sustained ROSC (p=0.425).
Table 2.
Independent associated factors of sustained return of spontaneous circulation (ROSC) in in-hospital cardiac arrest patients based on Multivariable analysis
| Prognostic Factors | Adjusted OR | 95% CI | P-value |
|---|---|---|---|
| GO-FAR score | 0.97 | 0.92-1.03 | 0.271 |
| Location (Intensive Care Unit) | 1.73 | 0.22-13.65 | 0.602 |
| Day shift | 4.11 | 1.05-16.06 | 0.042 |
| Mechanical ventilator | 1.19 | 0.20-7.07 | 0.845 |
| Vasopressor | 0.34 | 0.05-2.29 | 0.266 |
| ECG monitoring | 6.38 | 1.18-34.54 | 0.032 |
| Witness arrest | 0.57 | 0.12-2.62 | 0.470 |
| CPR team resuscitation | 0.95 | 0.24-3.81 | 0.944 |
| Initial shockable rhythm | 0.32 | 0.03-2.92 | 0.312 |
| Endotracheal intubation during CPR | 0.26 | 0.05-1.42 | 0.120 |
| Defibrillation | 1.12 | 0.20-6.21 | 0.897 |
| Total adrenaline dose during CPR | 0.72 | 0.54-0.94 | 0.017 |
| Total sodium bicarbonate dose during CPR | 1.15 | 0.83-1.57 | 0.403 |
| Time to first dose adrenaline within 5 minutes | 1.98 | 0.37-10.66 | 0.425 |
| Total CPR time | 0.92 | 0.85-0.98 | 0.015 |
OR: odds ratio; CI: confidence interval; ECG: electrocardiography; CPR: cardiopulmonary resuscitation; GO-FAR: Good Outcome Following Attempted Resuscitation.
Survival to hospital discharge
The multivariable logistic regression for survival to hospital discharge with favorable neurological outcome is presented in Table 3. We found that arrest due to cardiac etiology was associated with a positive result on survival (OR: 13.43; 95% CI: 2.00-89.80), while a GO-FAR score was independently associated with the rate of discharged survival (OR: 0.89; 95% CI: 0.81-0.98). Conversely, we found no significant relationship between the total adrenaline dose during CPR (p=0.545) and total CPR time (p=0.530).
Table 3.
Independent associated factors of survival at discharge with good cerebral performance category scale (CPC1-2) following in-hospital cardiac arrest
| Prognostic factors | Adjusted OR | 95% CI | P-value |
|---|---|---|---|
| GO-FAR score | 0.89 | 0.81-0.98 | 0.015 |
| Total adrenaline dose during CPR | 0.72 | 0.26-2.06 | 0.545 |
| Total CPR time | 0.92 | 0.72-1.18 | 0.530 |
| Cardiac etiology | 13.43 | 2.00-89.80 | 0.007 |
OR: odds ratio; CI: confidence interval; CPR: cardiopulmonary resuscitation; GO-FAR: Good Outcome Following Attempted Resuscitation.
4. Discussion:
After IHCA in this study, the overall sustained ROSC was achieved at 18%, with overall survival to discharge with a favorable neurological outcome of 9.6%. Overall, sustained ROSC was higher in patients with IHCA during the day shift and ECG monitoring prior to arrest. In contrast, higher doses of epinephrine administrated and increased CPR duration reduced the odds of sustained ROSC. Arrest due to cardiac etiology was associated with increased survival to discharge with favorable neurological outcome.
According to various articles on IHCA, sustained ROSC after IHCA was achieved in 33% to 67% of IHCA patients, with overall survival to discharge ranging from 13% to 28% in high-resourced countries (12-14). One large cohort study from Sweden reported a 61% ROSC rate after IHCA and 28.5% survival at discharge, with 23.6% of all patients having a CPC score of 1 or 2 at discharge (14). Another study on cardiac arrest in the emergency department conducted in Korea reported a sustained ROSC rate of 68.6%, with about 35.2% of patients surviving to hospital discharge (15). Compared with the Swedish and Korean cohorts, our study demonstrates a comparable rate of sustained ROSC after IHCA at 67.2%. However, even with the comparable ROSC rate, survival and satisfactory neurological outcome at discharge are substantially lower (18% and 9.6%, respectively). Our results are similar to one previous study from another university-based hospital in Thailand, which also reported a high ROSC rate but a low percentage of survival to discharge(16). Additionally, the overall outcomes of IHCA in Thailand are expected to be poorer if accounted for the population in lower-resourced settings of non-referral and community hospitals across the country.
One of the explanations for this result could be the lack of advanced post-arrest neurocritical care according to the AHA guideline, including electroencephalogram (EEG), targeted temperature management (TTM), and multimodality neuroprognostication. Due to the shortage of ICU beds and intensive care staff, several essential components in neurocritical care are rarely available in Thailand and other low- to middle-income countries (17). For example, the EEG is not performed for most IHCA patients due to the lack of resources and skilled personnel to interpret the EEG result, potentially leading to undiagnosed and untreated non-convulsive seizures in post-arrest patients. As for the TTM, the AHA guideline 2020 recommends induced hypothermia at 32°C to 36 °C for all adults who do not follow commands after OHCA or IHCA in any cardiac rhythm, as evidence were found that the TTM improves survival and neurological outcomes, particularly in OHCAs with initial shockable rhythm. Nevertheless, more studies are needed for IHCA, as the current evidence supporting TTM in IHCA is still insufficient (18). Because the TTM requires accurate temperature control and cooling devices in the ICU, the procedure is not generally feasible in Thailand and many resource-limited areas due to a shortage of available ICU beds.
Insufficient advanced post-arrest management may contribute to poorer outcomes among IHCA patients in our study. Even comparisons of survival after IHCA between countries are limited due to variations in the populations, the definition for identifying IHCA in each country, and country-specific culture concerning CPR and do-not-resuscitate orders (2). Further studies exploring post-arrest management could be beneficial to improve the outcomes of IHCA in Thailand.
Our study provides interesting results on the factors associated with ROSC in IHCA. Firstly, patients who experienced cardiac arrest during daytime had significantly better odds of ROSC. This finding is consistent with previous studies on the relationship between time of arrest and survival (14, 19-21). Generally, more healthcare professionals are available for patient care during the day shift compared to the evening and night shifts. Some studies have also reported that healthcare staff during the night shift tend to be younger and less experienced. Night shift workers also reported decreased alertness and increased health-related problems, especially when longer consecutive night shifts are requested, affecting overall performance during the shift (22, 23).
For these reasons, some countries require a mandatory sufficient time of rest for healthcare professionals before beginning a new shift. However, the situation is exacerbated in low-resourced countries with a shortage and maldistribution of healthcare workers, where most workers concentrate in central regions and large cities (24). In Thailand, the physician-to-patient ratio is about 7 per 10,000. The number is slightly lower than Southeast Asia's average density of 7.3 per 10,000 and about five times lower than 33.4 per 10,000 in high-income countries (25). Due to the shortage and maldistribution, healthcare workers must work overtime with frequent two consecutive shifts (16 hours), resulting in practice errors and decreased patient and worker satisfaction (26). From these findings, systemic approaches, strategies, and supportive policies are essential to improve patient outcomes during evening and night shifts. Further studies on workers' performance outside office hours are required to improve patient care.
Secondly, ECG monitoring prior to cardiac arrest increases the odds of ROSC. Monitor patients tend to be admitted to intermediate wards and ICU equipped with advanced hemodynamic monitoring devices and skilled staff experienced in CPR and resuscitation. ECG monitoring also leads to early detection of abnormal cardiac activity, resulting in immediate detection and response, which decreases CPR duration and improves outcomes (27).
Lastly, for intra-arrest factors, we found that the total adrenaline administration dose and increased CPR duration are associated with reduced ROSC. Various studies have demonstrated the association between the duration of resuscitation and patient outcomes. Most of the studies have confirmed that more favorable outcomes were related to shorter duration of CPR. The longer the CPR, the longer uncorrected underlying causes of arrest persist, resulting in increased organ ischemia and decreased chance of ROSC overtime (28-30).
However, the cut-point time for termination of resuscitation is unlikely to be determined based on the findings. Due to the numerous related clinical factors and differences in the CPR protocol of each hospital, the optimal time of resuscitation for any individual patient should be based on careful clinical judgment for each case (31).
Our study demonstrated the power of the GO-FAR score in predicting survival at discharge with satisfactory neurological outcomes after resuscitation in IHCA patients, which was consistent with the original article and various validation studies (10). The result confirmed the usefulness of the GO-FAR score as a potential tool for shared decisions regarding do-not-attempt-resuscitation orders, especially in critically ill patients who may not benefit from the CPR (32, 33).
We also found that patients whose arrest was due to cardiac etiology had better survival to hospital discharge with favorable neurological status. There are several explanations for this finding. Most arrest patients with cardiac etiology are admitted in ECG monitoring settings, which is associated with better survival after CPR. VF and VT arrest were also found to be higher in the cardiac etiology group, which could be potentially treated by defibrillation, resulting in early ROSC and less total CPR time. The effectiveness of percutaneous coronary intervention in patients with a myocardial infarction accounted for a considerable portion of IHCA with cardiac origin, also contributing to improvement in survival after the arrest (34).
Our present study has provided valuable information on the result of CPR on IHCA patients in Thailand, an upper-middle-income country in Southeastern Asia. The prognostic factors found in the study are helpful as supportive information for discussing the prognosis of IHCA with patients, relatives, and stakeholders to facilitate further clinical decisions. The findings also demonstrate the necessity of further strategies to improve CPR during out-of-office hours and post-cardiac arrest care for better patient outcomes. A more extensive prospective observational study on IHCA patients and their outcomes at the national level could be beneficial to evaluate the situation in lower-tier hospitals. The national cardiac registry database may help develop policies for supporting IHCA care nationwide in different hospital settings in Thailand, leading to an improvement in each component of the chain of survival for cardiac arrest patients.
5. Limitations
Our present study has several limitations which need consideration. Firstly, the study is retrospective with low sample size, which naturally leads to bias. Secondly, the study was conducted in a single, super-tertiary care, university-based hospital in Bangkok, Thailand. Patient characteristics and conditions are generally complicated as the hospital receives transfers from nearby lower-tier hospitals. Lastly, in our hospital, TTM is not yet a standard procedure in post-cardiac arrest patients. Since several studies have proved the benefit of TTM on patient outcomes, the result on the survival and neurological outcomes needed to be accounted for with the lack of TTM in this study before application.
6. Conclusion:
The sustained ROSC rate was higher in IHCA during the daytime shift and with prior ECG monitoring. The administration of higher doses of adrenaline and prolonged CPR durations decreased the likelihood of achieving sustained ROSC. Furthermore, patients with cardiac-related causes of cardiac arrest exhibited a higher rate of survival to hospital discharge with favorable neurological outcomes.
7. Declarations
7.1 Acknowledgment
None.
7.2 Funding Source
No fund was obtained for this study.
7.3 Authors’ contribution
All authors of this work have substantially participated in its development, encompassing the concept formation, study design, implementation, data collection, data analysis, and interpretation. Each author has been involved in the drafting and revision process, providing critical feedback on the manuscript. They have unanimously approved the final version for publication, concurred on the choice of journal for submission, and collectively accept responsibility for the integrity of all aspects of the work. All authors read and approved the final version of manuscript.
7.4 Ethical considerations
This study was approved by the Faculty of Medicine, Committee on Human Rights Related to Research Involving Human Subjects, Ramathibodi hospital, Mahidol university (COA. MURA2023/145).
7.5 Availability of data and material
The datasets used and/or analyzed during the current study are avilable form the corresponding author on reasonable request.
7.6 Conflict of interest
The authors declare that they have no competing interests.
7.7 Using artificial inteligence chatbots
None.
References
- 1.Virani SS, Alonso A, Benjamin EJ, Bittencourt MS, Callaway CW, Carson AP, et al. Heart Disease and Stroke Statistics-2020 Update: A Report From the American Heart Association. Circulation. 2020;141(9):e139–e596. doi: 10.1161/CIR.0000000000000757. [DOI] [PubMed] [Google Scholar]
- 2.Schluep M, Gravesteijn BY, Stolker RJ, Endeman H, Hoeks SE. One-year survival after in-hospital cardiac arrest: A systematic review and meta-analysis. Resuscitation. 2018;132:90–100. doi: 10.1016/j.resuscitation.2018.09.001. [DOI] [PubMed] [Google Scholar]
- 3.Berg KM, Cheng A, Panchal AR, Topjian AA, Aziz K, Bhanji F, et al. Part 7: Systems of Care: 2020 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2020;142(16_suppl_2):S580–s604. doi: 10.1161/CIR.0000000000000899. [DOI] [PubMed] [Google Scholar]
- 4.Girotra S, Nallamothu BK, Spertus JA, Li Y, Krumholz HM, Chan PS. Trends in Survival after In-Hospital Cardiac Arrest. New England Journal of Medicine. 2012;367(20):1912–20. doi: 10.1056/NEJMoa1109148. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Nas J, te Grotenhuis R, Bonnes JL, Furlaneto JM, van Royen N, Smeets JLRM, et al. Meta-Analysis Comparing Cardiac Arrest Outcomes Before and After Resuscitation Guideline Updates. The American Journal of Cardiology. 2020;125(4):618–29. doi: 10.1016/j.amjcard.2019.11.007. [DOI] [PubMed] [Google Scholar]
- 6.Andersen LW, Holmberg MJ, Berg KM, Donnino MW, Granfeldt A. In-Hospital Cardiac Arrest: A Review. Jama. 2019;321(12):1200–10. doi: 10.1001/jama.2019.1696. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis. 1987;40(5):373–83. doi: 10.1016/0021-9681(87)90171-8. [DOI] [PubMed] [Google Scholar]
- 8.Williams B. The National Early Warning Score: from concept to NHS implementation. Clinical Medicine. 2022;22(6):499–505. doi: 10.7861/clinmed.2022-news-concept. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Ferreira FL, Bota DP, Bross A, Mélot C, Vincent J-L. Serial Evaluation of the SOFA Score to Predict Outcome in Critically Ill Patients. Jama. 2001;286(14):1754–8. doi: 10.1001/jama.286.14.1754. [DOI] [PubMed] [Google Scholar]
- 10.Ebell MH, Jang W, Shen Y, Geocadin RG. Development and validation of the Good Outcome Following Attempted Resuscitation (GO-FAR) score to predict neurologically intact survival after in-hospital cardiopulmonary resuscitation. JAMA Intern Med. 2013;173(20):1872–8. doi: 10.1001/jamainternmed.2013.10037. [DOI] [PubMed] [Google Scholar]
- 11.Alnabelsi T, Annabathula R, Shelton J, Paranzino M, Faulkner SP, Cook M, et al. Predicting in-hospital mortality after an in-hospital cardiac arrest: A multivariate analysis. Resusc Plus. 2020;4:100039. doi: 10.1016/j.resplu.2020.100039. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Morrison LJ, Neumar RW, Zimmerman JL, Link MS, Newby LK, McMullan PW Jr, et al. Strategies for improving survival after in-hospital cardiac arrest in the United States: 2013 consensus recommendations: a consensus statement from the American Heart Association. Circulation. 2013;127(14):1538–63. doi: 10.1161/CIR.0b013e31828b2770. [DOI] [PubMed] [Google Scholar]
- 13.Ohbe H, Tagami T, Uda K, Matsui H, Yasunaga H. Incidence and outcomes of in-hospital cardiac arrest in Japan 2011–2017: a nationwide inpatient database study. Journal of Intensive Care. 2022;10(1):10. doi: 10.1186/s40560-022-00601-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Hessulf F, Karlsson T, Lundgren P, Aune S, Strömsöe A, Södersved Källestedt ML, et al. Factors of importance to 30-day survival after in-hospital cardiac arrest in Sweden - A population-based register study of more than 18,000 cases. Int J Cardiol. 2018;255:237–42. doi: 10.1016/j.ijcard.2017.12.068. [DOI] [PubMed] [Google Scholar]
- 15.Ko BS, Ahn R, Ryoo SM, Ahn S, Sohn CH, Seo DW, et al. Prevalence and outcomes of endotracheal intubation-related cardiac arrest in the ED. Am J Emerg Med. 2015;33(11):1642–5. doi: 10.1016/j.ajem.2015.07.083. [DOI] [PubMed] [Google Scholar]
- 16.Suraseranivongse S, Chawaruechai T, Saengsung P, Komoltri C. Outcome of cardiopulmonary resuscitation in a 2300-bed hospital in a developing country. Resuscitation. 2006;71(2):188–93. doi: 10.1016/j.resuscitation.2006.04.004. [DOI] [PubMed] [Google Scholar]
- 17.Viarasilpa T. Implementation of neurocritical care in Thailand. Front Neurol. 2022;13:990294. doi: 10.3389/fneur.2022.990294. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Panchal AR, Bartos JA, Cabañas JG, Donnino MW, Drennan IR, Hirsch KG, et al. Part 3: Adult Basic and Advanced Life Support: 2020 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2020;142(16_suppl_2):S366–S468. doi: 10.1161/CIR.0000000000000916. [DOI] [PubMed] [Google Scholar]
- 19.Hannen LEM, Toprak B, Weimann J, Mahmoodi B, Fluschnik N, Schrage B, et al. Clinical characteristics, causes and predictors of outcomes in patients with in-hospital cardiac arrest: results from the SURVIVE-ARREST study. Clin Res Cardiol. 2023;112(2):258–69. doi: 10.1007/s00392-022-02084-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Wang MT, Huang WC, Yen DH, Yeh EH, Wu SY, Liao HH. The Potential Risk Factors for Mortality in Patients After In-Hospital Cardiac Arrest: A Multicenter Study. Front Cardiovasc Med. 2021;8:630102. doi: 10.3389/fcvm.2021.630102. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Peberdy MA, Ornato JP, Larkin GL, Braithwaite RS, Kashner TM, Carey SM, et al. Survival From In-Hospital Cardiac Arrest During Nights and Weekends. Jama. 2008;299(7):785–92. doi: 10.1001/jama.299.7.785. [DOI] [PubMed] [Google Scholar]
- 22.Musy SN, Endrich O, Leichtle AB, Griffiths P, Nakas CT, Simon M. The association between nurse staffing and inpatient mortality: A shift-level retrospective longitudinal study. Int J Nurs Stud. 2021;120:103950. doi: 10.1016/j.ijnurstu.2021.103950. [DOI] [PubMed] [Google Scholar]
- 23.Ganesan S, Magee M, Stone JE, Mulhall MD, Collins A, Howard ME, et al. The Impact of Shift Work on Sleep, Alertness and Performance in Healthcare Workers. Scientific Reports. 2019;9(1):4635. doi: 10.1038/s41598-019-40914-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Boniol M, McCarthy C, Lawani D, Guillot G, McIsaac M, Diallo K. Inequal distribution of nursing personnel: a subnational analysis of the distribution of nurses across 58 countries. Hum Resour Health. 2022;20(1):22. doi: 10.1186/s12960-022-00720-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Measuring the availability of human resources for health and its relationship to universal health coverage for 204 countries and territories from 1990 to 2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet. 2022;399(10341):2129–54. doi: 10.1016/S0140-6736(22)00532-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Kunaviktikul W, Wichaikhum O, Nantsupawat A, Nantsupawat R, Chontawan R, Klunklin A, et al. Nurses' extended work hours: Patient, nurse and organizational outcomes. Int Nurs Rev. 2015;62(3):386–93. doi: 10.1111/inr.12195. [DOI] [PubMed] [Google Scholar]
- 27.Thorén A, Rawshani A, Herlitz J, Engdahl J, Kahan T, Gustafsson L, et al. ECG-monitoring of in-hospital cardiac arrest and factors associated with survival. Resuscitation. 2020;150:130–8. doi: 10.1016/j.resuscitation.2020.03.002. [DOI] [PubMed] [Google Scholar]
- 28.Yonis H, Andersen MP, Mills EHA, Winkel BG, Wissenberg M, Køber L, et al. Duration of resuscitation and long-term outcome after in-hospital cardiac arrest: A nationwide observational study. Resuscitation. 2022;179:267–73. doi: 10.1016/j.resuscitation.2022.08.011. [DOI] [PubMed] [Google Scholar]
- 29.Welbourn C, Efstathiou N. How does the length of cardiopulmonary resuscitation affect brain damage in patients surviving cardiac arrest? A systematic review. Scand J Trauma Resusc Emerg Med. 2018;26(1) doi: 10.1186/s13049-018-0476-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Matsuyama T, Ohta B, Kiyohara K, Kitamura T. Cardiopulmonary resuscitation duration and favorable neurological outcome after out-of-hospital cardiac arrest: a nationwide multicenter observational study in Japan (the JAAM-OHCA registry) Critical Care. 2022;26(1):120. doi: 10.1186/s13054-022-03994-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Goldberger ZD, Chan PS, Berg RA, Kronick SL, Cooke CR, Lu M, et al. Duration of resuscitation efforts and survival after in-hospital cardiac arrest: an observational study. Lancet. 2012;380(9852):1473–81. doi: 10.1016/S0140-6736(12)60862-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Thai TN, Ebell MH. Prospective validation of the Good Outcome Following Attempted Resuscitation (GO-FAR) score for in-hospital cardiac arrest prognosis. Resuscitation. 2019:140:2–8. doi: 10.1016/j.resuscitation.2019.05.002. [DOI] [PubMed] [Google Scholar]
- 33.Cho YJ, Kim YJ, Kim MY, Shin YJ, Lee J, Choi E, et al. Validation of the Good Outcome Following Attempted Resuscitation (GO-FAR) score in an East Asian population. Resuscitation. 2020;150:36–40. doi: 10.1016/j.resuscitation.2020.02.035. [DOI] [PubMed] [Google Scholar]
- 34.Wallmuller C, Meron G, Kurkciyan I, Schober A, Stratil P, Sterz F. Causes of in-hospital cardiac arrest and influence on outcome. Resuscitation. 2012;83(10):1206–11. doi: 10.1016/j.resuscitation.2012.05.001. [DOI] [PubMed] [Google Scholar]