Abstract
Early detection measures for breast cancer, such as breast self-exams, clinical breast exams, and mammography, have considerable benefits in effectively reducing breast cancer-related mortality. As the incidence of breast cancer is steadily increasing, it is crucial to raise awareness on early detection. This scoping review assessed the current knowledge, attitudes, practices, and perceptions of breast cancer screening among female medical students. We used the six phases of Arksey and O'Malley's framework from the Joanna Briggs Institute Manual and the Preferred Reporting Items for Systematic Reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR) template. Our analysis included 43 articles from Google Scholar and PubMed search engines, focusing on female medical students. Our results showed that most female medical students had a satisfactory level of knowledge about the most common signs, symptoms, and early detection methods of breast cancer. Generally, their attitude and perceptions were positive regarding breast cancer-related preventive measures. However, the level of practice was reduced. Further efforts are necessary to promote and improve the practice of breast self-examination, clinical breast exams, and mammography among female medical students. Potential interventions could include modifications to the medical curriculum and social media campaigns to enhance engagement and adoption of these practices.
Keywords: medical students, breast cancer, breast self-exam, knowledge, practice
ABBREVIATIONS: BC – breast cancer, BSE – breast self-exam, BCS – breast cancer screening, CBE – clinical breast exam, DCIS- ductal carcinoma in situ, HBMS – Health Belief Model Scale, IMPC- invasive micropapillary carcinoma, MMG – mammography, MRI- magnetic resonance imaging, NST- non-specific type carcinoma, PRISMA-ScR – Preferred Reporting Items for Systematic Reviews and Meta-Analyses extension for scoping Reviews
INTRODUCTION
Globally, breast cancer (BC) is the most frequently identified disease, with more than 2.3 million new diagnoses and 685,000 deaths reported in 2020. Compared to developed countries, BC mortality continues to be disproportionately more prevalent in developing nations. Because of increasing populations and aging, the burden of BC is expected to rise to about three million new diagnoses and one million deaths annually by 2040 [1]. The rise in breast cancer mortality affects most age groups and regions worldwide. However, women under 50 are at the greatest risk [2]. In some Asian and African countries, the average age for breast cancer diagnosis is more than ten years earlier than that in European and American populations. Thus, raising health awareness and developing prevention measures is fundamental to reducing the incidence of BC, which is steadily rising, particularly in the most affected regions [3].
In the context of BC becoming a real public health concern, the importance of early detection measures such as breast self-exams (BSE), clinical breast exams (CBE), and mammography (MMG) is increasing. Regular BSE is an essential first step for early diagnosis, particularly for nations with poor access to healthcare. Furthermore, regular BSE is favorably linked with early BC detection in low and middle-income countries, which leads to improved treatment results. As a result, BSE practice and prompt medical evaluation when any abnormalities are detected could be an effective strategy for the early detection of breast cancer, which could boost survival rates [4]. Moreover, BSE holds particular significance, considering that young women cannot receive an MMG, often regarded as the gold standard in detecting BC. Nevertheless, mammography appearance is typically nonspecific for invasive micropapillary carcinoma (IMPC), with magnetic resonance imaging (MRI) evaluation being the best way to diagnose this BC [5]. Early detection for these patients is extremely important, as they typically tend to have considerable lesions diagnosed at an advanced stage with a worse prognosis due to the micropapillary aspect and the extension of lymph nodes compared to individuals with other kinds of breast cancer, particularly non-specific type carcinoma (NST) [6]. In this context, BSE is viewed as an unquestionable procedure when socioeconomic circumstances are also regarded, particularly in developing nations [7].
The progression of BC in younger women tends to be more aggressive than its development in older individuals. A subset of breast tumors with common patterns of gene expression is characterized by young age at diagnosis, which is correlated with a less favorable outcome. Likewise, a major contributing factor to the high death rate among young women is the lack of BC awareness [8]. Nowadays, various treatment options are available to improve the health status of patients. A wide range of scientific evidence is available on this subject. However, exercising caution is of great importance when interpreting the findings of studies that examined the clinical relevance of HER2 status in patients with ductal carcinoma in situ (DCIS). For patients with invasive breast cancer, a HER2 assessment holds an important status. However, this poses certain threats for patients exhibiting intermediate HER2 expression and/or intra-tumoral heterogeneity. Similarly, regarding Dductal carcinoma patients, the potential advantages of HER2 targeted therapy, including the clinical fundamental shifts, remain unclear [9].
Therefore, the main aim of our review was to map evidence in the existing scientific literature about knowledge, attitudes, practices, and perceptions of female medical students concerning BC screenings and to suggest future actions to improve the status quo. Since medical students have sufficient contact with health-related content, they might serve as informational resources for non-health students and other people in society, which makes this target group of particular interest [10]. Furthermore, students' ability to inform people about BC and BSE relies on their concurrent knowledge, practices, and health beliefs [7]. Achieving the mission of increasing cancer screening uptake is also shared with nurses and midwifery students [11]. Additionally, in developing nations where access to high-quality healthcare is still limited, nurses and midwives are typically the main sources of healthcare in remote rural communities where advanced cases of BC and mortality rates are higher compared to urban settings [12]. In these contexts, it is often their responsibility to instruct other women on performing BSE correctly [13].
MATERIAL AND METHODS
For this scoping review, we employed the six-phase framework outlined in the Joanna Briggs Institute Manual, as developed by Arksey and O'Malley, which included the following steps: (1) defining the research issue, (2) locating pertinent studies, (3) choosing surveys, (4) mapping data, (5) and (6) gathering, synthesizing, and recording the information [14]. In addressing the first phase of answering the research question, our primary goal was to investigate the level of knowledge among medical students regarding BC screenings. Secondary to this, we also focused on their attitudes, practices, and perceptions related to breast cancer screenings.
Duplicate records were removed before storage in the reference management tool, Zotero. The first phase consisted of screening the record titles and abstracts relevant to the aim of our review. Articles that were found to be outside the reach of the review reach were not taken into consideration, specifically grey literature. The full-text review was limited to articles considered relevant by at least one reviewer based on our predefined inclusion criteria. Our initial literature search was conducted on Google Scholar using keywords such as 'knowledge of students on BC screenings'. We specifically targeted articles related to our primary group of interest — students in medical and related health sciences fields — with a focus on BC screenings. Key search terms included: 'medical/nursing/midwifery students', 'undergraduates', or 'future health professionals', 'BC screenings', 'prevention strategies', 'early detection', and 'breast-self-examination'. Subsequently, we conducted a search on PubMed, utilizing a query that included terms like 'medical students' or 'medical university undergraduates' and 'BC screening' or 'breast self-exam'. This search was refined with filters for female sex, English language, and publications after the year 2009. We removed duplicates identified through Google Scholar and added only those relevant to our criteria, corresponding to the second phase from Figure 1.
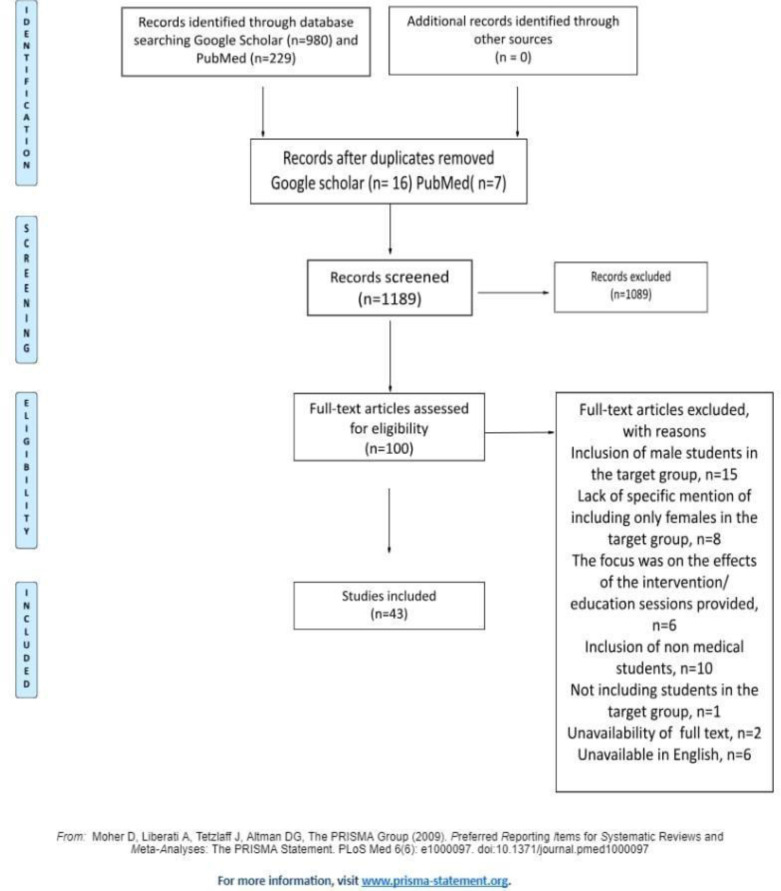
Figure 1.
PRISMA Flow Diagram
The following criteria were used to identify studies for this review: primary and secondary studies, published between January 2009 and August 2023, studies reporting evidence on female university students who study medicine or are related to medical fields such as nurses, midwives, pharmacists, public health and health sciences students, studies reporting evidence on BCS knowledge, attitude, practice, the perception among women, and articles in English. Exclusion criteria included studies focusing on health literacy, treatment, genetic counseling, awareness, studies reporting evidence on men, research published before 2009, studies published as reports, editorials, conference papers, book chapters, or reviews, research including other malignancies and articles generally focusing on cancer and having the target group college, high school, secondary school, and vocational school students, or students enrolled in other programs. We used the PRISMA-ScR template to report our review. Initially, we identified 980 records through Google Scholar and 229 through PubMed. However, we excluded certain articles for the following reasons: (a) inclusion of male students in the target group, n=15; (b) failure to specify the inclusion of only female participants in the target group, n=8; (c) focus on the effects of intervention/education sessions provided, n=6, (d) inclusion of non-medical students, n=10; (e) not including students in the target group, n=1, (f) unavailability of full text, n=2, (g) articles not available in English, n=6. Following these exclusions based on our eligibility criteria, the final analysis was conducted on 43 articles. This approach aligns with the third step of the PRISMA Flow Diagram, focusing on the selection process for the studies included in our review.
During the next step, researchers extracted and plotted the data. The data extraction framework included key elements such as the first author's name, publication date, study location and context, research design, objectives, study population, and main results (knowledge, attitudes, practices, perceptions, and awareness of BCS adoption). Two researchers independently evaluated each article, plotted information using the data extraction model, and adjusted the data extraction spreadsheet correspondingly.
RESULTS
BCS knowledge among female medical students
General knowledge
A study that aimed to evaluate medical students’ knowledge about BC symptoms and risk factors illustrated the belief that tobacco use, hormone replacement therapy, oral contraceptives, as well as not practicing breastfeeding are risk factors for BC [15]. In contrast, the risk factors most frequently identified by female students included in another study were family history (82.9%), not breastfeeding (68.0%), oral contraceptive use (58.6%), and late menopause (50.9%) [16]. However, less than half recognized early menstruation (45.9%) and a high-fat diet (40.5%) as risk factors. A study focusing on female medical students' understanding, attitudes, and behavior toward BSE found that all participants had a solid understanding of BC, with 95% believing that BSE may be a useful technique for early diagnosis. Approximately 85% of the participants believed early BC screening enhances survival rates. Additionally, 65% of students were familiar with all three BC screening techniques: MMG, CBE, and BSE. Specifically, 52.2% had heard of MMG, 48.90% believed it was done in a clinical laboratory, and even a smaller percentage (40.4%) knew it was recommended after age 35. In addition, 66.7% of the participants reported that early BC screening is important [17]. Similar points were highlighted in another study [18], where 15.5% of respondents had a strong general understanding of BSE. Additionally, a similar level of good general knowledge about BSE was observed among third and fourth-year nursing students in a separate study [7]. Moreover, female nursing students were well-informed about BC screening techniques and practiced BSE [12]. Also, 94.4% of participants in another study recognized that early detection of BC can improve outcomes [15]. Overall, good knowledge was present in other studies as well, where all participants were aware of BC, 80% considered it a common disease [19], and 65.3% were familiar with the BSE technique, although 19% did not know the technique and 15.7% were uncertain [20]. However, a gap between knowledge and practice was also seen, as 45.1% knew about BSE, whereas only 33.3% performed it [17]. Likewise, 91% of students believed that BSE is essential, but only 87% of students could perform it [21]. Similarly to the finding that most participants (71%) had BSE-related knowledge, 60% knew how BSE must be performed, but only 16% performed it regularly [15].
Level of education and knowledge
Higher educational levels in medical studies have been linked to increased knowledge about BC screenings. For instance, a study that assessed how education affects the understanding and use of BSE among female medical students in the preclinical phase compared to female medical students in the clinical period showed that those in the clinical phase demonstrated a better understanding and more accurate practice of BSE. This highlights how strong education may affect appropriate levels of knowledge and perhaps result in optimal levels of BSE practice [22]. Similarly, in another study, many first-year and second-year students had low knowledge levels (28.9% and 10.3%), whereas fourth-year and third-year students had high knowledge levels (8.2% and 4.1%). Nevertheless, a study conducted in Turkey targeting third and fourth-year nursing students found that BSE and CBE were reasonably low, and the difference between the two groups was statistically negligible even though both groups had extremely high BSE knowledge. However, there was a statistically significant difference between the study year and the confidence level. Fourth-year students demonstrated greater confidence in performing BSE than third-year students [7]. Also, there was a highly statistically significant relationship between age groups and level of education with the total mean knowledge of BSE because 60% of the study population in the study were younger nursing students (first and second year) who did not yet get an in-depth BC curriculum [18]. Moreover, the level of study was a significant predictor of BC screening knowledge. Third-year students were 14 times more likely to have a strong understanding of BC screening techniques compared to first-year students (OR=13.9, 95% CI, 6.2–31.26) [12, 23]. Another study found that clinical exposure significantly improved female medical students' comprehension of BC signs, risks, and confidence in identifying warning signs [24].
Differences in knowledge were also influenced by the field of study. For example, medical students were more likely to recognize that breastfeeding reduces BC risk compared to students in pharmacy (62.5%), dental sciences (86.7%), and nursing sciences (70.0%), who showed uncertainty about this association [25]. Another study identified that students enrolled in clinical nutrition, health administration, and laboratory medicine departments showed differences in their awareness of BC symptoms: 36% of the health administration students believed that changes in breast shape and size are the most common signs of BC [26]. Likewise, 28% and 37% of laboratory medicine and clinical nutrition students reported a lump or a moving mass as the most frequently encountered sign. Another study showed that having a college education is not a predicting factor for BSE knowledge, as more than half of the 20-year-old female participants included did not know about BSE [23]. This finding aligns with another study where participants showed poor knowledge of certain BC signs and symptoms [27]. However, no significant associations were found between participants' knowledge and factors like marital status, residential area, faculty department, and academic year [28].
Jobs and knowledge
Health professionals shared common views regarding the importance of BC screening. Specifically, 85 doctors (n = 1,005) were aware of BSE, reporting its usefulness for early detection of BC [29]. Comparing midwives with midwifery students, the rate of performing BSE was higher among midwives (52.5% practicing BSE monthly) compared to students (45.4%) [30]. There was no difference in the technique used when performing BSE. Most students used their contralateral arm, yet <17% had two or more different positions, such as standing and raising their hands or lying and pressing against the waist. Most participants, both midwives and students, had a positive attitude and opinion concerning the evolution and success rate of detecting BC and treatment in the future. Likewise, most were willing to receive additional information, education, and support in performing BSE [31]. However, despite knowledge of BSE practice, some students did not perform it regularly [32].
Knowledge regarding the time of practicing BSE
Medical students from Baghdad University in Iraq demonstrated a higher level of knowledge about the appropriate timing for performing BSE compared to their colleagues from Haramaya University, Ethiopia. For instance, 67 female medical students from Baghdad University (44.67%) in the pre-clinical category and 77 students (51.33%) in the clinical group correctly identified that BSE should be performed five days following menstruation. Also, 85 students (56.65%) in the preclinical group recognized that the BSE should be conducted every month, compared to 116 students (77.33%) in the clinical group [22]. Contrastingly, fewer medical students, 34 (26.9%) from Haramaya University, Ethiopia, thought it should be performed a few days after menstruation, which is the recommended time according to existing guidelines, compared to 51.5% of the participants who thought that BSE should be performed a few days before menstruation [8]. Nonetheless, most nursing students from an Indian university had good knowledge regarding the time of practice but not the starting age. For instance, according to 50.4% and 56.3% of respondents, BSE must be performed monthly using the palm and a minimum of three fingers, and 47.5% said that BSE should be performed even <19 years, although the recommended time is after 20 years [19]. Limited knowledge was also reported among nursing students from Riyadh, Kingdom of Saudi Arabia, as 78% were unaware of the proper timing for executing BSE or its frequency (72%) [33]. Unsatisfactory knowledge of the frequency and the ideal time to perform BSE among final-year medical students were identified among students from Sudan as well [34]. Additionally, their findings regarding BSE knowledge were unexpected, as the target group consisted of final-year female medical students, with the main assumption that students should have acquired this knowledge within the educational training.
Sources of knowledge
A significant proportion of medical students (46.7%) in one study learned about BSE for the first time through seminars, classes, and tutorials, which highlights the reality that strong education may favorably affect high levels of knowledge and possibly result in high levels of BSE practice [22]. Along the same lines, another study found that 54% of medical students heard of BSE through lectures as their primary source of information. In addition, radio and television combined (35.7%) were significant in raising awareness about BC [8]. Likewise, the majority (73.2%) of the study sample claimed to have learned about BSE at school [30, 35], followed by printed materials (39.4%), medical personnel (30.7%) [33, 36], TV/internet (34.6%), and acquaintances (3.9%) [7]. The sources of knowledge of nursing students from a Nigerian hospital also ranged from official coaching (45.1%), media (33.3%), and individual learning (21.6%) [12]. Contrary to previously published studies, it was found that mass media was the main source of BSE information [18]. Mass media (TV, radio, and newspapers) made up the majority of information sources (35.1), as suggested by other studies as well [19, 37, 38], followed by contacts with medical staff (9.3%), family (2.1%), and other sources (14.4%). The two most frequent sources of BC knowledge, according to students, were media (TV/radio) and seminars on health topics (46.3% and 42.2%, respectively) [39]. Similar to the study conducted among medical students from Kenya, media, including television and radio, were the main sources of BSE-related information, as mentioned by 65% of the participants, whereas only 7% mentioned health professionals [25]. Nevertheless, acquaintances can also be a source of knowledge among those aware of BSE, 35.2% learned from family, friends, or teachers, 20.4% from communication tools and media, 21.2% from healthcare professionals, 14.4% from the internet, and 8.3% from articles and books [20].
Knowledge regarding symptoms and signs
Participants agreed that a palpable breast lump should be the first sign of BC (77.7%), followed by nipple drainage (7.1%), breast discoloration (9.5%), and a shift in breast dimensions (3.17%). However, over 65% of people claimed that MMG, CBE, and BSE can detect BC [8]. A stratified random cross-sectional study found that out of 423 female medical students, 35.2%, 14.7%, and 35.9% had no information about the causes and risk factors, early manifestation, and early BC detection methods [40].
Attitudes of female medical students regarding BCS
We detected a favorable attitude towards BSE in a majority of studies. Particularly, 63.9% of respondents mentioned that all women should participate in BSE, but 4.2% claimed BSE makes people feel embarrassed, and 29.9% said they were afraid to think about BC [17, 41]. Generally, more than three-quarters (75.3%) of nursing students at an Arab American University had a positive attitude towards BSE, whereas about 21.6% were not interested in participating in BCS, with no reports of unfavourable attitudes [18]. The findings revealed that most students held a positive attitude towards BSE, and 93.3% thought that performing BSE is required, but fear of developing BC in the future was also the primary driver behind BSE (84.8%) [19, 40]. Positive attitudes were related to being knowledgeable about BSE, seeking medical assistance in case of an abnormal breast or lump notice, and the monthly practice of BSE [42].
The practice of female medical students regarding BCS
Practice tendencies
The level of practice among students was generally low. For example, only 110 medical students (36.67%) from Baghdad University were practicing BSE, with 77 students (51.33%) in the clinical group never engaging in it [22]. Likewise, in another study, 62.9% of the students said they do not practice BSE monthly, and 42 students (43.3%) claimed that they had never been taught BSE by health professionals and had not studied the proper method for performing it [18]. This view was also supported by another paper, where the majority of participants (63.3%) refused to answer questions about the correct and complete method of performing BSE [22]. Another study [43] identified that 77.9% of female adolescents never engaged in any form of breast examination.
Despite the high percentage of public health students (89%, n=178) from Jimma University, Ethiopia, who had good BSE knowledge, only 21% (n=42) practiced it correctly. On the other hand, 25.5% (n=51) practiced it incorrectly, and more than half (107 students) did not practice it at all [44]. Furthermore, regardless of a good level of BSE knowledge, only 13.5% of monthly regular BSE cases and 10.3% of occasional CBE cases were detected among third and fourth-grade nursing students [7]. Only 33.3% routinely performed BSE throughout the year (12 times), and very few nursing students conducted an accurate and complete BSE [19]. Nevertheless, the existence of a physician in the family environment and the year of learning were both important mediators of BSE practice, according to multivariate analysis using binary logistic regression, which showed that about 90% of those who practiced BSE did so at least once a month [12].
Reasons for not performing BSE
Regarding the practice of BSE, 37.4% of medical students in Sudan said that they do not practice it because of negligence, whereas 26,2% do not know how to do it [45]. Lack of knowledge was also a barrier for female nursing students [19], and 20.8% of medical students relied on their poor performance due to the lack of familiarity with the technique [40]. There was a highly statistically significant correlation between BSE knowledge and practice, demonstrating the public’s willingness to get accurate BSE knowledge [18]. This aligns with findings from another study where students faced challenges accessing BSE information and lacked recommendations from others [46]. However, despite high levels of BSE knowledge, barriers to undergoing BSE were the lack of requirement to undertake the examination continuously, feeling healthy, and not having breast issues [37]. Other reasons included the lack of symptoms and the belief of not having BC [43], in line with about 45.7% of individuals who reported poor BSE performance attributed to the lack of breast issues [40]. Absence of symptoms or warning signs (28.8%), anxiety about seeing an anomaly (16.4%), and loss of intimacy (15.4%) were also causes for not performing BSE [8]. Also, a small percentage of the sample (4%) identified the absence of symptoms as a barrier to BSE practice [33]. This contrasts with the finding of another study [47], where 84.5% of the sample mentioned the importance and necessity of performing BSE despite the lack of symptoms. Another rationale cited as a cause for not practicing BSE was the failure to recall [7] (6.36% of individuals, as mentioned by two studies [35, 44]). Forgetfulness was mentioned by 17% of respondents [8] compared to 36.7% [36]. Not considering it necessary was also suggested by several studies. Specifically, 4.54% of medical students [21], contrasting to 13.3% of respondents, thought BSE was unnecessary and expressed fear of receiving a BC diagnosis [19]. This finding is similar to another study where 11.8% disagreed that BSE was essential [48] and did not consider it useful [49]. Lack of time was a commonly reported issue [49], mentioned by 22.0% of respondents in one study [36] and 11.5% in another [48]. A smaller proportion cited fear of the unknown [36], fear of detecting anomalies (2.3%), lack of expertise (22.7%), and lack of courage (6.8%) as reasons for not practicing BSE [48].
Female medical students’ perceptions of BCS
Risk perception, an essential component of the behavioral change framework, significantly impacts women's decisions to undergo breast cancer testing. Women who either did not perceive themselves at risk for BC or were unaware of their risk status were less likely to consistently perform BSE compared to those who had a pessimistic view of their risk of developing the illness. Our findings support the Health Belief Model, which suggests that women with a greater likelihood of developing BC are more likely to do routine BSE, as they view the disease as a severe danger, have fewer perception obstacles, and a greater perception of the advantages [10]. Similarly, it is believed that frequent BSE testing should consider women's health views. Another study used the Health Belief Model Scale (HBMS) to determine students' perceptions of BC screenings. A score close to five indicates susceptibility, paying attention, and health motivation. Likewise, it indicates that the advantages, barriers, and self-efficacy of BSE are highly acknowledged. The students' HBMS importance, health interest, and BSE value perception ratings were not significantly different from their BC knowledge and BSE competence scores across different academic years. Compared to students who participated in BSE infrequently or not at all, those who participated in BSE regularly perceived their vulnerability as being lower. Their BSE self-efficacy was stronger, their perception of BSE barriers was smaller, and a statistical difference was discovered [7]. Also, most studies indicated that medical students' perceptions of the major BC risk factors were generally positive [8].
DISCUSSION
The objective of this scoping review was to explore the existing research on the knowledge, attitudes, practices, and perceptions of female medical students and those in related medical fields regarding BCS, to influence public health and policy efforts, and to enhance screening procedures. It is important to analyze this paper in terms of the strengths and limitations it encompasses. Our research provided information on the level of knowledge, attitudes, and practices related to BCS among female medical students. The study offered broad perspectives, including a comprehensive analysis of 43 published scientific articles. On the other hand, as we limited our analysis to articles written only in English, this might impact the generalizability of our results, which could be an apparent limitation of our study.
We suggest utilizing the media and other channels to increase public awareness of the significance of BSE. First, appropriate health education initiatives are required to explain the risk factors and prevention of BC to medical students and the general population [8]. Intensified awareness projects and implementation of health campaigns among nursing university students are also required to supervise their current level of BC and BSE knowledge. Effective and coordinated implementation of awareness and health education programs can lead to beneficial behavioral changes. The use of media as a key tool for disseminating BSE information is essential for increasing public awareness [18]. These results agree with a study underlining the importance of promoting BSE awareness [19]. The study suggests that consistent information delivery and maintaining BSE practice can be improved with reminders and notifications. A unique and beneficial approach for students could be using a smartphone in conjunction with practical experience for BSE education. We suggest this teaching strategy be more widely applied to young women [46]. Therefore, the public must be actively informed about BSE and BC via the media. Medical professionals must use media more accurately and effectively [20].
Improving the current curricula for medical, midwifery, and nursing students should also be applied. For example, one study suggested that, as a substitute for regular training, specific training sessions need to be organized to enhance students' understanding, abilities, practices, and health convictions regarding BSE. The curricula should be updated to include information about BC [7]. In undergraduate nursing school curricula, changes are needed to support nurses' increasing involvement in cancer prevention screening. These reforms should encompass nurse education and training [35, 30, 46, 47]. Several studies have shown significant improvements in knowledge following educational activities. Specifically, there was a notable increase in the understanding of BCS techniques (i.e., CBE and BSE) among both basic science nursing (Group 1) and general nursing and midwifery students (Group 2) after educational interventions, compared to their initial knowledge levels. Moreover, following the presentation, 89% (n=31/35) of students in Group 2 and 96% (n=54/56) in Group 1 were prepared to catalyze the society for BC testing [11]. In addition, there was a statistical difference between the pre- and post-education programs for 67.3% of students [50]. However, in terms of attitudes towards BC and knowledge and proficiency in performing BSE, there was no statistically significant change in scores observed between the pre-education, 6-month, and 1-year follow-ups of the students [51, 52].
CONCLUSION
This paper identified that the majority of students had good general knowledge regarding signs, symptoms, and early detection measures. Their information sources included family, friends, media, and TV, mainly classes and lectures. Most of them had a positive attitude and expressed an optimistic belief regarding BC preventive measures. Despite these, their practice level was poor. This supports the necessity of addressing this topic and finding a proper solution. Although the study successfully explored the existing literature on female medical students' knowledge, including signs and symptoms of BC and techniques of BSE, which are important to improve the detection of BC, it had certain limitations that need to be acknowledged. One limitation of the study is that it relied only on two databases, PubMed and Google Scholar, to identify scientific articles. Nevertheless, our analysis presented valuable insights into BCS, but more research is required to determine the optimal course of action for enhancing the adoption and application of BSE and other early BC detection techniques.
ACKNOWLEDGMENTS
Conflict of interest
The authors declare no conflict of interest.
Authorship
MT and MLV analyzed each article, plotted information using the data extraction model, and adjusted the data extraction spreadsheet correspondingly. MIU constantly analyzed, offered feedback and recommendations, and addressed inconsistencies and conflicts through additional assessment.
References
- 1.Arnold M, Morgan E, Rumgay H, Mafra A, et al. Current and future burden of breast cancer: Global statistics for 2020 and 2040. The Breast. 2022; 66:15–23. doi: 10.1016/j.breast.2022.08.010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Lima SM, Kehm RD, Terry MB. Global breast cancer incidence and mortality trends by region, age-groups, and fertility patterns. eClinicalMedicine. 2021;38 doi: 10.1016/j.eclinm.2021.100985. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Lei S, Zheng R, Zhang S, Wang S, et al. Global patterns of breast cancer incidence and mortality: A population-based cancer registry data analysis from 2000 to 2020. Cancer Commun (Lond) 2021;41(11):1183–1194. doi: 10.1002/cac2.12207. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Dewi TK, Ruiter RAC, Diering M, Ardi R, Massar K. Breast self-examination as a route to early detection in a lower-middle-income country: assessing psychosocial determinants among women in Surabaya, Indonesia. BMC Womens Health. 2022;22(1):179. doi: 10.1186/s12905-022-01748-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Verras GI, Tchabashvili L, Mulita F, Grypari IM, et al. Micropapillary Breast Carcinoma: From Molecular Pathogenesis to Prognosis. Breast Cancer (Dove Med Press) 2022;14:41–61. doi: 10.2147/BCTT.S346301. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Verras GI, Mulita F, Tchabashvili L, Grypari IM, et al. A rare case of invasive micropapillary carcinoma of the breast. Prz Menopauzalny. 2022;21(1):73–80. doi: 10.5114/pm.2022.113834. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Kıssal A, Kartal B, Çetin Ö. The Determination of Knowledge, Applications and Health Beliefs of Third-and Fourth-Grade Nursing Students Regarding Breast Self-Exam. J Breast Health. 2017;13(1):10–15. doi: 10.5152/tjbh.2016.3207. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Ameer K, Abdulie SM, Pal S, Arebo K, Kassa GG. Breast Cancer Awareness and Practice of Breast Self-Examination among Female Medical Students in Haramaya University, Harar, Ethiopia. 2014. Available from: https://www.semanticscholar.org/paper/Breast-Cancer-Awareness-and-Practice-of-Breast-in-Ameer-Abdulie/d1c25a1e63799f40bc5a3fc4fc07eb19fd63707e.
- 9.Akrida I, Mulita F. The clinical significance of HER2 expression in DCIS. Med Oncol. 2022;40(1):16. doi: 10.1007/s12032-022-01876-9. [DOI] [PubMed] [Google Scholar]
- 10.Osei-Afriyie S, Addae AK, Oppong S, Amu H, et al. Breast cancer awareness risk factors and screening practices among future health professionals in Ghana: A cross-sectional study. PLOS ONE. 2021;16(6):e0253373. doi: 10.1371/journal.pone.0253373. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Dhanasekaran K, Verma C, Sriram L, Kumar V, Hariprasad R. Educational intervention on cervical and breast cancer screening: Impact on nursing students involved in primary care. J Fam Med Prim Care. 2022;11(6):2846–2851. doi: 10.4103/jfmpc.jfmpc_1786_21. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Ighodaro EO, Akhigbe AO. Knowledge of breast cancer screening methods and the practice of breast self-examination among female nursing students in a Nigerian teaching hospital. East Afr Med J. 2016;93(11):599–605. doi: 10.4314/eamj.v93i11. [DOI] [Google Scholar]
- 13.Karadag M, Iseri O, Etiİkan İ. Determining Nursing Student Knowledge, Behavior and Beliefs for Breast Cancer and Breast Self-examination Receiving Courses with Two Different Approaches. ASIAN Pac J CANCER Prev. 2014;15(9) doi: 10.7314/apjcp.2014.15.9.3885. [DOI] [PubMed] [Google Scholar]
- 14.Peters MDJ, Godfrey CM, Khalil H, McInerney P, Parker D, Soares CB. Guidance for conducting systematic scoping reviews. International Journal of Evidence-Based Healthcare. 2015 Sep;13(3):141–6. doi: 10.1097/XEB.0000000000000050. [DOI] [PubMed] [Google Scholar]
- 15.Ansari AB, Shahzad N, Bota R, Ahmed M, et al. Medical Students’ Knowledge and Attitude towards Breast Cancer Risk Factors and Early Detection Practices. Austin Med Sci. 2018;3(1):1024. [Google Scholar]
- 16.Karthijekan K, Karunakaran KE. Knowledge on Breast Cancer and Practices on Breast Self-Examination among Female Students in Faculty of Health-Care Sciences, Eastern University, Sri Lanka. Int J Multidiscip Studies. 2017;4:17. doi: 10.4038/ijms.v4i1.33. [DOI] [Google Scholar]
- 17.Shah S, Rana S, Parvin T, Muraduzzaman S, Jalali M. Study on Awareness, Knowledge and Practice of Breast Screening Methods among the Female Students of Bangladesh University of Health Sciences. 2020;2(6):7. doi: 10.34104/ejmhs.020.01520158. [DOI] [Google Scholar]
- 18.Ayed A, Eqtait F, Harazneh L, Fashafsheh I, et al. Breast Self-Examination in Terms of Knowledge, Attitude, and Practice among Nursing Students of Arab American University/Jenin. J Educ Pract. 2015;6(4):37–47. [Google Scholar]
- 19.Sujindra E, Elamurugan TP. Knowledge, attitude, and practice of breast self-examination in female nursing students. IJEPR. 2015;1(2):71. doi: 10.4103/2395-2296.152216. [DOI] [Google Scholar]
- 20.Ardahan M, Dinc H, Yaman A, Aykir E, Aslan B. Health Beliefs of Nursing Faculty Students about Breast Cancer and Self Breast Examination. Asian Pac J Cancer Prev APJCP. 2015;16(17):7731–7736. doi: 10.7314/apjcp.2015.16.17.7731. [DOI] [PubMed] [Google Scholar]
- 21.Javaeed A, Rasheed I, Shafqat F. Knowledge, attitude, and practice of breast self-examination among female undergraduate medical students in Poonch Medical College, Azad Kashmir. JPMA. 2020;71:1–11. doi: 10.47391/JPMA.1046. [DOI] [PubMed] [Google Scholar]
- 22.Mizel R, Razzaq R, Al-Shahwani I. Knowledge and practice of breast self-examination among female medical students in clinical and pre-clinical stages at Al-Kindy College of Medicine/ Baghdad University. JABHS. 2020;21(1):19–26. [Google Scholar]
- 23.Beydağ DK, Yürügen B. The Effect of Breast Self-Examination (Bse) Education Given to Midwifery Students on Their Knowledge and Attitudes. APJCP. 2010;11(6):1761–1764. [PubMed] [Google Scholar]
- 24.Qasim S, Tayyab H, Zulqadar K, Masood S, et al. Breast Cancer knowledge and perceived barriers to help seeking among pre-clinical and clinical female medical students of King Edward Medical University, Lahore: a cross-sectional study. BMC Med Educ. 2020;20(1):222. doi: 10.1186/s12909-020-02132-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Kimani SM, Muthumbi E. Breast self examination and breast cancer: Knowledge and practice among female medical students in a Kenyan university. Ann Afr Surg. 2010;3(1):6. doi: 10.4314/aas.v3i1.53694. [DOI] [Google Scholar]
- 26.Abed H, Mohamed EA, El-Nagger N, Sayed H. Knowledge, Attitudes and Practices Regarding Breast Self-Examination among Female Undergraduate Students in the Faculty of Applied Medical Sciences at Umm Al-Qura University. 2013 Jan 1;9(4):622–32. [Google Scholar]
- 27.Moey SF, Saidin N. A survey on the knowledge of breast cancer and adoption of breast self-examination among female undergraduate students of Kulliyyah Allied Health Sciences, Iium Kuantan. Int J Allied Health Sci. 2018;2(2):368–376. [Google Scholar]
- 28.Hussein M, Qadir H, Ahmed H. Assessment of knowledge and practice of female students in Erbil Medical Technical Institute regarding breast self-examination. Polytechnic J. 2017;8:367–400. doi: 10.25156/ptj.2018.8.1.226. [DOI] [Google Scholar]
- 29.Ahmed S, Pulock OS, Chakraborty RR, Awal A. Breast Cancer Screening: Knowledge, Attitude and Practice Among Female Doctors and Medical Students in a Tertiary Care Hospital and Medical College in Bangladesh. RMCJ;2020; 3(1):11–16. [Google Scholar]
- 30.Dinas K, Moschaki V, Grammanikou K, Zepiridis L, et al. Breast self-examination in Greek midwives and midwifery students. Neoplasma. 2018;65(6):980–985. doi: 10.4149/neo_2018_171112N729. [DOI] [PubMed] [Google Scholar]
- 31.Plesnicar A, Golicnik M, Fazarinc IK, Kralj B, et al. Attitudes of midwifery students towards teaching breast-self examination. Radiol Oncol. 2010;44(1):52–56. doi: 10.2478/v10019-010-0009-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Erbil N, Bolukbas N. Health Beliefs and Breast Self-Examination among Female University Nursing Students in Turkey. APJCP. 2014;15:6525–6529. doi: 10.7314/APJCP.2014.15.16.6525. [DOI] [PubMed] [Google Scholar]
- 33.Yakout SM, El-shatbyMoursy AM, Moawad S, Salem O, Arabia S. Awareness Knowledge and Practice of Breast self examination among groups of Female nursing students, Riyadh, Kingdom of Saudi Arabia. 2014. Available from: https://www.semanticscholar.org/paper/Awareness%2C-Knowledge-and-Practice-of-Breast-self-of-Yakout-El-shatbyMoursy/b73db41033e36af8628e0f094270cfa41697481b.
- 34.Idris S, Hamza A, Hafiz M, Mohammed A, El shallaly G. Knowledge, attitude and practice of breast self examination among final years female medical students in Sudan. Int J Public Health Res. 2013;1:6–10. [Google Scholar]
- 35.Memis S, Akdolun Balkaya N, Demirkiran F. Knowledge, Attitudes, and Behaviors of Nursing and Midwifery Students Regarding Breast Self-Examination in Turkey. Oncol Nurs Forum. 2009;36:E39–46. doi: 10.1188/09.ONF.E39-E46. [DOI] [PubMed] [Google Scholar]
- 36.Haruna H, Chukwu EO, Ahmadu I, Teryila KR, et al. Knowledge and Practice of Breast Self-Examination Among Female Nursing Students in University of Maiduguri, Borno State, Nigeria. Int J Clin Oncol Cancer Res. 2017;2(3):57. doi: 10.11648/j.ijcocr.20170203.12. [DOI] [Google Scholar]
- 37.Abdul-Lateef SJ, Shabaan M. Assessment of Female Nursing Students knowledge and practice about Breast Self-Examination in Mosul University. Mosul J Nurs. 2019;7(1):30–36. doi: 10.33899/mjn.2019.162123. [DOI] [Google Scholar]
- 38.Zongo N, Sandrine SM, Aboubacar BH, Chantal S, et al. Screening and Early Diagnosis of Breast Cancer: Assessment of Knowledge and Practical Abilities of Final Year Nursing and Midwifery Students in Health Schools of Ouagadougou. Asian Pac J Cancer Care. 2017;2(3):47–47. doi: 10.31557/apjcc.2017.2.3.47. [DOI] [Google Scholar]
- 39.Nemenqani DM, Abdelmaqsoud SH, Al-Malki AHA, Oraija AA, Al-Otaibi EM. Knowledge, attitude and practice of breast self examination and breast cancer among female medical students in Taif, Saudi Arabia. Open J Prev Med. 2014;4(2):69–77. doi: 10.4236/ojpm.2014.42011. [DOI] [Google Scholar]
- 40.El-Sherbiny A, El-Shorbagy D, El-Shorbagy D, Zaid H. Knowledge, Attitude and Practice of Female Medical Students of Tanta University Towards Breast Cancer and Its Screening. EJCM. 2014;32(2):19. [Google Scholar]
- 41.Alrashid F, Idris S, Elamin AA, Alnajib A, Elmisbah H, Hussien T. Perspicacity of medical students towards breast self-examination. Medical Sci. 2021;25(108):7. [Google Scholar]
- 42.Ali A, Yuan F, Ying C, Ahmed N. Awareness, Knowledge and Attitude towards Breast Self-examination: A Cross-sectional Study among Female Pharmacy Students in Malaysia. Int J Oncol. 2020;2(4):1–10. [Google Scholar]
- 43.Malak AT, Yilmaz D, Tuna A, Gümüs AB, Turgay AS. Relations between breast and cervical cancer prevention behaviour of female students at a school of health and their healthy life style. Asian Pac J Cancer Prev. 2010;11(1):53–56. [PubMed] [Google Scholar]
- 44.Desta F, Workicho A, Atomsa A, Workneh D, Tebeje B. Knowledge, Practice and Associated Factors of Breast Self Examination Among Female Students of the College of Public Health and Medical Science, Jimma University, Ethiopia. Am J Health Res. 2018;6(2):44. doi: 10.11648/j.ajhr.20180602.12. [DOI] [Google Scholar]
- 45.Mohammed LA, Idris B, Bolis SM, Musa HH. Knowledge, attitudes and practices related to breast cancer self-examination among medical students at the University of Khartoum, Sudan. S Afr J Public Health. 2023:45–51. doi: 10.7196/SHS.2023.v6.i2.176. [DOI] [Google Scholar]
- 46.Kang SR, Shin H, Lee J, Kim SJ. Effects of smartphone application education combined with hands-on practice in breast self-examination on junior nursing students in South Korea. Jpn J Nurs Sci. 2020;17(3):e12318. doi: 10.1111/jjns.12318. [DOI] [PubMed] [Google Scholar]
- 47.Omar A, Bakr A, Ibrahim N. Female medical students’ awareness, attitudes, and knowledge about early detection of breast cancer in Syrian Private University, Syria. Heliyon. 2020;6(4):e03819. doi: 10.1016/j.heliyon.2020.e03819. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Parajuli P, Mandal GN. Knowledge about Breast Cancer and Breast Self Examination Practices among Medical, Dental and B.Sc Nursing Students of BPKIHS. Health Renaiss. 2011;8(3):166. [Google Scholar]
- 49.Kulundu CA. Thesis. International Health Sciences University: 2014. Prevalence and Factors Associated with Breast Self Examination for Breast Cancer Detection Among Female Students of International Health Sciences University. Available from: http://ir.ciu.ac.ug/xmlui/handle/123456789/683. [Google Scholar]
- 50.El-Mohsen ASA, El-Maksoud MMA. Improve Knowledge, Beliefs and Behavior of Undergraduate Female Nursing Students in Al-Alzhar University toward Breast Self-Examination Practice. J Educ Pract. 2015;6(8):102–110. [Google Scholar]
- 51.Kissal A, Kartal B. Effects of Health Belief Model-Based Education on Health Beliefs and Breast Self-Examination in Nursing Students. Asia-Pac J Oncol Nurs. 2019;6(4):403–410. doi: 10.4103/apjon.apjon_17_19. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Rezano A, Utama MS, Wiraswati HL, Ekawardhani S, et al. Knowledge Level towards Breast Cancer and Breast Self-Examination among Medical Students of Indonesia. Glob Med Health Commun. 2022;10(1):35–42. doi: 10.29313/gmhc.v10i1.8942. [DOI] [Google Scholar]