Abstract
Objective
To compare long-term psychological symptoms and health-related quality of life (HRQOL) in intubated versus non-intubated ICU survivors.
Design
Prospective, multicentre observational cohort study.
Setting
Four tertiary medical-surgical ICUs in Australia.
Participants
Intubated and non-intubated adult ICU survivors.
Main outcome measures
Primary outcomes: clinically significant psychological symptoms at 3- and 12-month follow-up using Post-Traumatic Stress Syndrome-14 for post-traumatic stress disorder; Depression, Anxiety Stress Scales-21 for depression, anxiety, and stress. Secondary outcomes: HRQOL, using EuroQol-5D-5L questionnaire.
Results
Of the 133 ICU survivors, 54/116 (47 %) had at least one clinically significant psychological symptom (i.e., post-traumatic stress disorder, anxiety, depression, stress) at follow-up. Clinically significant scores for psychological symptoms were observed in 26 (39 %) versus 16 (32 %) at 3-months [odds ratio 1.4, 95 % confidence interval (0.66–3.13), p = 0.38]; 23 (37 %) versus 10 (31 %) at 12-months [odds ratio 1.3, 95 % confidence interval (0.53–3.31), p = 0.57] of intubated versus non-intubated survivors, respectively. Usual activities and mobility were the most commonly affected HRQOL dimension, with >30 % at 3 versus months and >20 % at 12-months of overall survivors reporting ≥ moderate problems. There was no difference between the groups in any of the EQ5D dimensions.
Conclusions
Nearly one-in-two (47 %) of the intubated and non-intubated ICU survivors reported clinically significant psychological symptoms at 3 and 12-month follow-ups. Overall, more than 30 % at 3-months and over 20 % at 12-months of the survivors in both groups had moderate or worse problems with their usual activities and mobility. The presence of psychological symptoms and HRQOL impairments was similar between the groups.
Keywords: Intensive care, Survivorship, Psychology, Quality of life
Graphical abstract
1. Introduction
Survivors of critical illness frequently have long-lasting physical and cognitive impairment, clinically important psychological symptoms, and reduced health-related quality of life (HRQOL).[1], [2], [3], [4], [5], [6] Such problems have been collectively termed, post intensive care syndrome (PICS).7
There is robust literature of longitudinal follow-up studies demonstrating persistent psychological symptom burden (e.g., post-traumatic stress disorder (PTSD), anxiety, and depression) and impaired HRQOL after mechanical ventilation in the intensive care unit (ICU),[8], [9], [10], [11] although few studies have evaluated these outcomes and compared results, with non-intubated patients. A small number of European studies indicate that anxiety, stress, and traumatic experiences occur in patients receiving non-invasive ventilation.12,13 Perhaps commonalities in the ICU environment (e.g., noise, poor sleep, unfamiliar clinical teams, loss of personal control, and isolation from family)14,15 and critical illness may produce similar psychological and HRQOL outcomes in ICU patients regardless of the use of invasive ventilation.
Thus, the psychological stress in intensive care survivors study aimed to describe and compare 3- and 12-month psychological symptoms and HRQOL in ICU survivors in patients managed with invasive ventilation (intubated) and without invasive ventilation (non-intubated).
2. Methods
Psychological stRess in Intensive CarE survivors (PRICE) was a multicentre prospective cohort study conducted in four tertiary ICUs across four hospitals in Australia from July 2015 until July 2019. The trial was registered (ACTRN12615000880549) and approved by the relevant human research ethics committees and a protocol, eligibility criteria, and statistical analysis plan were published.16 The study recruited intubated (invasive ventilation >24 h) and non-intubated (inotropic/vasopressor support and/or non-invasive ventilation) ICU survivors. Given the interest in new psychological symptoms occurring after the ICU, patients with pre-existing psychiatric disorders were excluded (detailed inclusion and exclusion criteria provided in Supplementary file 1). A consecutive sample of patients who met the study inclusion criteria was recruited contingent on research staff availability. Longitudinal follow-up (3-and 12-month) was initially conducted via post (mail), and if there was no response to two study letters, a telephone call was made by trained research staff.
The Strengthening the Reporting of Observational Studies in Epidemiology guidelines were followed in the reporting of the study results.17
2.1. Study objectives
The primary objective of the study was to compare psychological symptoms in intubated versus non-intubated ICU survivors at 3- and 12-month follow-up. The secondary objective was to compare HRQOL at 3- and 12-month follow-up.
Measurement instruments: Participants were asked to complete study questionnaires to assess psychological symptoms after discharge from ICU, but before hospital discharge (i.e. baseline) and at 3- and 12-month follow-up. These questionnaires included the Post-Traumatic Stress Syndrome-14 (PTSS-14); Depression, Anxiety Stress Scales-21 (DASS21).
PTSS-14 is a validated 14-item measure of post-traumatic symptoms. Scores range from 14 (least symptoms) to 98 (worst symptoms) with higher scores indicating worse symptoms. A published clinically relevant cut-off score of 45 is suggested for the measure.18
DASS21 is a 21-item scale that examines the presence and severity of depression, anxiety, and stress symptoms over the past month, with seven items examining each symptom state.19 Participants were asked to complete the items using 4-point frequency and impact scales (0–3), with higher scores indicating worse symptoms. Published cut-off scores are provided for the subscales to indicate the severity of each state from normal/mild, moderate, severe and extremely severe symptoms.20
HRQOL was assessed at 3- and 12-month follow-ups using the 5-level EuroQoL-5D version (EQ-5D-5L), in which survivors described their health across five dimensions: mobility, self-care, usual activities, pain, and anxiety/depression. Each dimension is scored from 1 to 5 (1 = no problems and 5 = extreme problem). Individual EQ5D-5L dimension scores were converted to a utility score using Australian normative data.21 Survivors were also asked to rate their overall health on a visual analog scale (VAS) ranging from 0 to 100, with a score of 100 indicating the best possible health.
2.2. Statistical analysis
A detailed statistical analysis plan was previously published.16 Patient demographics and baseline characteristics were summarised using means with standard deviations (S.D), medians, and 25 %–75 % quartiles (interquartile range) on continuous measures and frequencies (percentages) on categorical measures. An a priori sample size calculation indicated that 62 patients in each group would provide 80 % power to detect a 20 % difference between the groups for the presence of any psychological symptoms on follow-up at a significance level of 5 %. The study planned to recruit 75 patients in each group to account for a potential attrition rate of 20 % on longitudinal follow-up.
Clinically significant PTSD symptoms were indicated by a score of ≥45 on the PTSS-14. Individual DASS scores were dichotomized to normal/mild and at least moderate severity scores on each domain: depression (≥14), anxiety (≥10), and stress (≥19) and presented as a percentage of patients with clinically significant symptoms. EQ5D-5L dimensions were dichotomized as normal/mild problems and moderate or worse (extreme) problems and presented as the percentage of patients with ≥ moderate problems in HRQOL dimensions. Means with standard errors were used when reporting primary and secondary outcomes. Mean psychological symptom scores, EQ5D VAS, and utility scores were compared between groups at 3- and 12-months.
Patients who died at the time of hospital discharge (before any follow-up) were excluded from the analysis. Data for survivors were included and analysed as long as one of the follow-up assessments was completed. No imputation was conducted for incomplete or missing data (from incident mortality, dropout, or non-response), under the assumption of data being missing at random. A loss to follow-up analysis, including comparisons of baseline characteristics of participants with versus without follow-up data, was conducted. A linear mixed model, with follow-up time (3 and 12 months) and group (intubated vs non-intubated) and their interaction as fixed effects and patient as a random effect, was used to compare assessment scores between intubated and non-intubated survivors at both follow-up periods. Logistic regression analysis was used to compare the presence (prevalence) of individual clinically significant symptoms at each follow-up (3 or 12 months) between the groups, with the patient as a random effect. Measures of association were reported as odds ratio (OR) with 95 % confidence interval (CI). Pearson's chi-square test was used for categorical data, and the Wilcoxon rank sum test was used for continuous variables. All data analyses were performed using R statistical software (version 4.0.5) and R studio (version 1.4.1106) for Windows. P values of <0.05 were considered to be significant in the analyses, without adjustment for multiple comparisons.
3. Results
Of the 172 patients initially recruited, 21 (12 %) patients died at hospital discharge or withdrew consent before follow-up and 18 (12 %) survivors were lost to all follow-up (Fig. 1). Overall, 133 patients with a median age of 66 [57–73] years were included in the analyses. Most patients were males (61 %) and predominantly with medical admissions (62 %). The non-intubated patients had more medical comorbidities (55 % vs 30 %) and active malignancy/metastases (34 % vs 13 %). The intubated group had more patients with trauma (20 % vs 4 %), a higher prevalence of delirium in the ICU (32 % vs 4 %), and increased ICU and hospital length of stay (LOS) (Table 1).
Fig. 1.
Consort diagram. ICU: Intensive Care Unit.
Table 1.
Baseline patient characteristics stratified by intubation status.
| Characteristic | Intubated (n = 76) | Non-intubated (n = 57) |
|---|---|---|
| Age (years) | 65 [55–71] | 68 [60–75] |
| Male | 52 (68 %) | 29 (52 %) |
| Indigenous | 6 (8 %) | 7 (12 %) |
| Medical admission | 50 (66 %) | 33 (58 %) |
| Major admission categoryb | ||
| Respiratory | 24 (32 %) | 13 (23 %) |
| Cardiovascular | 17 (22 %) | 2 (4 %) |
| Trauma | 15 (20 %) | 2 (4 %) |
| Gastrointestinal | 8 (11 %) | 11 (19 %) |
| Neurological | 4 (5 %) | 2 (4 %) |
| Renal | 2 (3 %) | 8 (14 %) |
| Others | 6 (8 %) | 19 (33 %) |
| Major admission sub-category | ||
| Sepsis | 14 (18 %) | 19 (33 %) |
| Malignancy (active/metastases) | 10 (13 %) | 20 (35 %) |
| Any comorbidityc | 23 (30 %) | 32 (56 %) |
| Comorbidity count ≥2 | 5 (7 %) | 7 (12 %) |
| Deliriuma in ICU | 24 (32 %) | 2 (4 %) |
| Non-Invasive Ventilation in ICU | 6 (8 %) | 18 (32 %) |
| Any inotrope/vasopressor use | 64 (84 %) | 37 (66 %) |
| Inotrope/vasopressor ≥2 (concurrent) | 10 (13 %) | 1 (2 %) |
| APACHE II score | 19 (7.8) | 15 (5.5) |
| APACHE III score | 68 (31.2) | 57 (17.3) |
| Hospital LOS (days) | 25 [12.6–53.4] | 15 [8.3–24.7] |
| ICU LOS (days) | 7 [4.7–12] | 2 [1.6–2.7] |
| Hospital discharge destination | ||
| Home | 53 (70 %) | 52 (91 %) |
| Other hospital | 14 (18 %) | 4 (7 %) |
| Rehab | 9 (12 %) | 0 (0 %) |
| Nursing Home | 0 (0 %) | 1 (2 %) |
Data presented as number (%), mean (standard deviation) or median [interquartile range].
APACHE: Acute Physiology and Chronic Health Evaluation; LOS: length of stay.
Measured by Confusion Assessment Method for the ICU (CAM-ICU).
Admission ICU Diagnosis, based on APACHE III-J diagnostic codes.
Chronic co-morbidity: based on APACHE II (organ insufficiency prior to hospital admission).
At 3-months, 116 out of 127 survivors (91 %) and at 12-months, 94 out of 119 survivors (79 %) completed follow-up assessments.
3.1. Psychological symptoms at follow-up
Overall, 54/116 (47 %) survivors had clinically significant scores for one or more psychological symptoms (i.e., PTSD, anxiety, depression, and/or stress) at 3- or 12-month follow-up. In intubated vs. non-intubated survivors, a clinically significant score for one of the four psychological symptoms was observed in 26 (39 %) vs 16 (32 %) at 3-months [OR 1.4, 95 % CI (0.66–3.13), p = 0.38]; 23 (37 %) vs 10 (31 %) at 12-months [O.R. 1.3, 95 % CI (0.53–3.31), p = 0.57], respectively. Psychological assessment scores and the presence of clinically significant psychological symptoms in the two groups are described below.
PTSD: There was no difference in the PTSS-14 scores between the intubated and non-intubated survivors at either follow-up time point (Table 2) (Supplementary Figure 1). Clinically significant PTSD symptoms were evident in 11 % and 13 % of the overall survivors at 3- and 12-months, respectively. There was no difference in the presence of PTSD symptoms between the groups at 3 (p = 0.70) or 12 months (p = 0.23) (Fig. 2) (Supplementary Table 1).
Table 2.
Patient outcomes, stratified by intubation status.
| Follow-up screening | 3-months |
12-months |
||||
|---|---|---|---|---|---|---|
| Intubated (n = 66) |
Non-intubated (n = 50) | P value | Intubated (n = 62) |
Non-intubated (n = 32) | P value | |
| PTSS14 score | 30 (1.9) | 24 (2.3) | 0.07 | 30 (2.0) | 27 (2.5) | 0.29 |
| Depression score | 9 (1.3) | 7 (1.5) | 0.46 | 9 (1.3) | 8 (1.7) | 0.47 |
| Anxiety score | 8 (1.0) | 6 (1.2) | 0.21 | 6 (1.0) | 6 (1.3) | 0.74 |
| Stress score | 10 (1.1) | 7 (1.3) | 0.07 | 9 (1.1) | 7 (1.4) | 0.13 |
| EQ 5D 5L VAS | 63 (2.8) | 69 (3) | 0.13 | 70 (3) | 71 (3.5) | 0.71 |
| EQ 5D 5L utility score | 0.52 (0.04) | 0.67 (0.05) | 0.02∗ | 0.62 (0.04) | 0.68 (0.05) | 0.31 |
Scores provided as mean with standard errors.
PTSS14, Post Traumatic Stress Scale (14 items); EQ5D5L, EuroQOL 5 dimension, 5 level; VAS, Visual Analogue Scale.
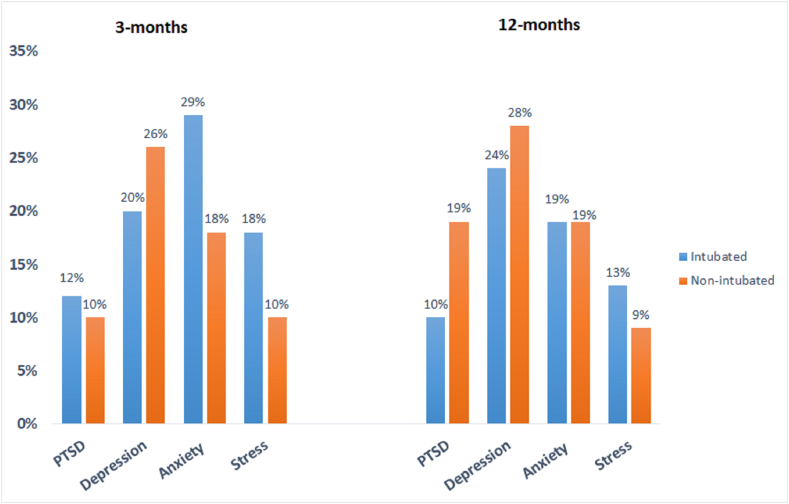
Fig. 2.
Clinically significant psychological symptoms at follow-up. PTSD: clinically significant symptoms as defined as PTSS14 ≥ 45. Depression/Anxiety/Stress: moderate to worse symptoms on DASS screening.
Depression, Anxiety, and Stress: There were no significant differences between the groups at either time point for DASS-depression, DASS-anxiety, and DASS-stress scores (Table 2) (Supplementary Figure 1). The presence of clinically significant symptoms among the overall survivors was as follows: depression (22 % and 24 %), anxiety (24 % and 19 %), and stress (15 % and 12 %) at 3- and 12-months, respectively. There was no difference between the groups on the presence of symptoms at either 3 months (depression, p = 0.39; anxiety, p = 0.20; stress, p = 0.24) or 12 months (depression, p = 0.68; anxiety, p = 0.94; stress, p = 0.62) (Fig. 2) (Supplementary Table 1).
3.2. Health-related quality of life (HRQOL)
At 3- and 12-month follow-ups, respectively, 94 (81 %) and 90 (96 %) of overall survivors completed the EQ5D-5L assessments. Usual activities and mobility were the most commonly affected HRQOL dimensions in both groups, with >30 % at 3-months and >20 % at 12-months of overall survivors reporting ≥ moderate problems in the above HRQOL dimensions (Fig. 3). There was no difference between the groups on ≥ moderate problems in the EQ5D dimensions or mean EQ5D VAS scores at either follow-up point (Supplementary table 2) (Table 2). EQ5D utility score was worse in the intubated versus non-intubated patients at 3-months, but not at 12-months (Table 2).
Fig. 3.
EQ-5D-5L dimensions with ≥ moderate problems at follow-up.
3.3. Lost to follow-up analysis
Eighteen patients (12 %), nine from each group, were lost to all follow-up. Overall, they had similar demographics, baseline PTSS14 and DASS21 scores to participant responses at follow-up (Supplementary table 3 shows survivors stratified by loss to all follow-up). All surviving participants completed at least one psychological follow-up assessment. Of the 11 survivors who did not complete their 3-month assessment, all (except one from the non-intubated group, who did not survive until 12 months) later completed assessments at 12-months. All 25 survivors (12 intubated and 13 non-intubated) who did not complete their 12-month assessments had previously completed them at 3-months. These survivors (without 12-month assessments) had shorter ICU LOS, lower PTSS14, and depression and anxiety scores at baseline, but otherwise did not differ either at baseline or at 3-months relative to those who completed the 12-month assessments (Supplementary table 4 shows survivors stratified by 12-month follow-up completion).
4. Discussion
In this prospective multicentre follow-up study across 4 Australian ICUs, nearly one-in-two (47 %) of the ICU survivors experienced persistent clinically significant psychological symptoms at 3- and 12-months follow-up. Although there was a trend towards worse PTSD and stress symptoms in the intubated versus non-intubated survivors at 3-months, the overall severity of PTSD, anxiety, depression, and stress did not differ at follow-up. Further, at 3-months, >30 %, and at 12-months, >20 % of the overall survivors reported at least moderate HRQOL impairment with their usual activities and mobility. Although the self-rating of HRQOL was similar between groups, the intubated survivors had worse EQ-5D-5L utility scores at 3-months, but this difference did not persist at 12-months. Thus, we found that psychological symptoms were similar in intubated and non-intubated survivors, and although there was a tendency for intubated survivors to report worse HRQOL at 3-months, this difference had resolved by 12-months.
Our study results are consistent with prior findings of psychological outcomes in intubated ICU survivors. Our finding that 10 % of intubated ventilated survivors had symptoms of PTSD at 12 months is similar to recent Australian data showing possible PTSD symptoms in 8 % of intubated survivors at 6-months using the Impact of Events-revised Scale.22 Although few studies have evaluated non-intubated patients specifically, our results fit into the broader prevalence rates for PTSD symptoms in ICU survivors at long-term follow-up (5–64 %).11,[23], [24], [25], [26] However, no prior studies have directly compared psychological symptoms in intubated versus non-intubated ICU patients over time. In our study, we found that 10 % and 19 % of non-intubated ICU survivors reported PTSD symptoms at 3- and 12-months, respectively. Further, no robust differences were detected in the severity of psychological symptoms in intubated versus non-intubated ICU patients at 3- or 12-months. With reference to normed values, both survivor groups reported a higher prevalence of PTSD symptoms at 12-months, relative to Australian population norms (5.7 %).27
Furthermore, clinically significant symptoms (moderate or severe symptoms of depression, anxiety or stress) were similar between the intubated and non-intubated survivors. In our study, clinically significant depression was present in 24 % of the intubated versus 28 % of non-intubated survivors at 12-months, which is similar to published values in ICU survivors (8–57 %).9,23 In addition, 19 % of patients reported clinically significant anxiety at 12-months in our study, which is lower than Australian and international clinical data and published values (21–44 %).10,22,23 Although, at 12-months, psychological symptoms in the survivors in our study were much higher than the Australian population normed values for depression (4.8 %) and anxiety (16.8 %).27 Thus, the patient sample was comparable to values obtained in other ICU studies but much worse than in the Australian population. Any differences in our results and those of other ICU studies may be due to inherent differences in the timing of assessments, screening populations, and/or use of different screening tools. In addition, few studies have previously examined stress levels in ICU patients in the long-term ICU outcomes literature. We found that moderate to extremely severe symptoms of stress were present in 13 % of intubated and 9 % of non-intubated survivors at 12-months follow-up, demonstrating the persistence of psychological stress in some patients long after ICU discharge. It is unclear what contributed to their persistent feelings of stress, although our results add to the existing literature on acute stress in ICU survivors.
We advance several possible reasons to explain the similar psychological symptom severity in intubated versus non-intubated survivors.1 ICUs are stressful environments for patients, with even healthy volunteers reporting symptoms of depression symptoms when admitted to ICU.2,28 There were a higher proportion of females in the non-intubated group in our study. A previous systematic review of risk factors for PICS has identified a three-fold higher risk of mental health issues in female sex.29 Also, the non-intubated group in our study had a higher comorbid disease burden and a higher proportion of underlying malignancy. Pre-ICU health status, including severe comorbidities, may have a non-modifiable impact on the long-term outcomes of ICU survivors.30 In cancer patients, prevalence rates for PTSD, depression, and anxiety vary on the type of malignancy and methodology of follow-up, but they are similar to those reported in the ICU literature.3,[31], [32], [33], [34] One-third of non-intubated patients in our study required non-invasive ventilation that may have been potentially distressing for them. Specifically, non-invasive ventilation can induce a psychological stress response, fear of dying, pain, and suffering;35 in part caused by mask discomfort, feelings of claustrophobia, and impaired awareness may contribute to psychological distress.36,37 Thus, psychological symptoms in ICU survivors are likely due to similarities in the ICU experience and may be based on their medical condition, although aspects of invasive ventilation may be uniquely stressful for some ICU patients.
Regarding HRQOL, >30 % at 3-months and at 12-months, >20 % of the overall survivors reported ≥ moderate and persistent HRQOL impairment with their usual activities, and mobility. Our results are similar to those observed in other intensive care survivors who were more likely to have persistent impairment in physical and mental domains of HRQOL, long after discharge from ICU.[38], [39], [40] A 6 -month follow-up study evaluating EQ5D scores in ICU survivors showed that ICU variables were not related to impairments in HRQOL suggesting that other determinants (e.g. pre-existing health) may be more important than the presence or absence of invasive ventilation.41 In particular, pre-existing co-morbidities and frailty can influence HRQOL outcomes in ICU survivors,[42], [43], [44] although we did not evaluate pre-existing frailty in our study. We did find that the EQ-5D utility score was significantly worse in intubated versus non-intubated survivors in the short-term (3-months), although any difference had disappeared by 12-months. The reasons underpinning the worse HRQOL in intubated patients at 3-months were not clear from the data available in this study.
There were several limitations in our study. First, due to a higher-than-expected mortality in the non-intubated group, the study may have been underpowered to detect differences between the groups. Second, although the overall loss to follow-up in this study was 12 %, almost all survivors completed at least one of the follow-up assessments. The higher mortality in the non-intubated group reflects the severity of illness of these patients. A poor response to multiple follow-up assessments in the non-intubated group may be reflective of survey fatigue in survivors with multiple co-morbidities. In addition, our results may be influenced by survivorship or selection bias. While a loss to follow-up is a challenge in long-term follow-up studies in ICU survivors,45 our rate compares favourably with other ICU survivor studies (e.g. 20–25 %).46 Further, we did not find any differences in the characteristics of patients lost/not lost to follow-up, suggesting that the loss of patients was not systematic (e.g. related to symptom severity). Third, the different baseline characteristics of the groups, in addition to the presence or absence of invasive ventilation (e.g., a higher proportion of females, co-morbidities, and malignancy in the non-invasive group versus a higher proportion of trauma patients, higher rates of ICU delirium and an increased ICU and hospital LOS in the intubated group) may have influenced the results. Fourth, we did not collect details on pre-ICU health status, which may have influenced long-term outcomes.41,47 And although we excluded patients with diagnosed pre-existing psychiatric disorders, undiagnosed pre-existing mental health disorders may have influenced the results. Finally, the patient sample was derived from Australian metropolitan teaching ICUs and the study results should be considered within this context.
Our study has numerous strengths. The multicentre, prospective design using validated screening tools and a mixed population of general ICU survivors allows wider generalisability. In addition, the study used two follow-up time points (3 and 12 months) allowing comparison with literature with varying follow-up time points and assessment for change over time. Furthermore, almost all the survivors completed at least one of their long-term psychological follow-up assessments. More importantly, due to the inclusion of non-intubated patients, the study creates insight into the long-term psychological and HRQOL outcomes of an increasing group of ICU survivors.
4.1. Implications
The complex myriad of psychological and HRQOL issues leaves a lasting legacy in some ICU survivors. The psychological and HRQOL outcomes of critically ill non-intubated ICU survivors are similar to those of intubated survivors, except that the short-term HRQOL of intubated patients may be worse than for non-intubated patients. Further long-term follow-up research with an emphasis on risk factors for PICS in critically ill non-intubated ICU survivors is required.
5. Conclusions
In this 4-site Australian study, nearly one-in-two of the ICU survivors reported clinically significant psychological symptoms at 3- and 12-month follow-ups. Over a third of the survivors at 3-months and over a fifth of the survivors at 12-months had moderate or worse impairments in their usual activities and mobility. There was no statistically significant difference in the presence of psychological symptoms and HRQOL impairments between the intubated and non-intubated survivors.
Conflict of interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Ethics approval and consent to participate
The study was approved by the relevant local human research ethics committees (HREC) of the Australian Capital Territory (ETH.11.14.315), New South Wales (HREC/16/HNE/64), South Australia (HREC/15/RAH/346). Written, informed consent was obtained from patients.
Funding
This work was supported by the Canberra Health Services Private Practice Fund (SR/IM) and Maurice Sando Foundation Sponsorship Scheme (KS/SR). The funders had no influence on the study design, analysis or interpretation of the results or manuscript development.
CRediT authorship contribution statement
SR conceptualised and was the chief investigator for the PRICE study. SR, RB, FVH, IM, DMN contributed to the study design. SR, KS, AR, MM, RP, MN supervised the conduct of the study and assisted with data collection and follow-up. SR and MN managed the data. TN provided statistical advice on study design and SR and TN conducted the data analysis. SR drafted the manuscript, and all authors contributed substantially to its revision. All authors have contributed substantially to the study and have approved the manuscript for submission.
Consent for publication
Not applicable.
Acknowledgements
We would like to acknowledge the research co-ordinator at each site: Shakira Spiller and Sarah Cummins (Canberra Hospital), Alexis Poole (Royal Adelaide Hospital), Kristy Masters (Nepean Hospital), Gail Brinkerhoff (John Hunter Hospital).
Footnotes
Supplementary data to this article can be found online at https://doi.org/10.1016/j.ccrj.2023.10.011.
Contributor Information
Sumeet Rai, Email: Sumeet.Rai@act.gov.au.
Imogen Mitchell, Email: Imogen.Mitchell@act.gov.au.
Appendix A. Supplementary data
The following is the Supplementary data to this article:
References
- 1.Herridge M.S., Cheung A.M., Tansey C.M., Matte-Martyn A., Diaz-Granados N., Al-Saidi F., et al. One-year outcomes in survivors of the acute respiratory distress syndrome. N Engl J Med. 2003;348(8):683–693. doi: 10.1056/NEJMoa022450. [DOI] [PubMed] [Google Scholar]
- 2.Cheung A.M., Tansey C.M., Tomlinson G., Diaz-Granados N., Matte A., Barr A., et al. Two-year outcomes, health care use, and costs of survivors of acute respiratory distress syndrome. Am J Respir Crit Care Med. 2006;174(5):538–544. doi: 10.1164/rccm.200505-693OC. [DOI] [PubMed] [Google Scholar]
- 3.Dowdy D.W., Eid M.P., Sedrakyan A., Mendez-Tellez P.A., Pronovost P.J., Herridge M.S., et al. Quality of life in adult survivors of critical illness: a systematic review of the literature. Intensive Care Med. 2005;31(5):611–620. doi: 10.1007/s00134-005-2592-6. [DOI] [PubMed] [Google Scholar]
- 4.Herridge M.S. Long-term outcomes after critical illness: past, present, future. Curr Opin Crit Care. 2007;13(5):473–475. doi: 10.1097/MCC.0b013e3282eff3af. [DOI] [PubMed] [Google Scholar]
- 5.Desai S.V., Law T.J., Needham D.M. Long-term complications of critical care. Crit Care Med. 2011;39(2):371–379. doi: 10.1097/CCM.0b013e3181fd66e5. [DOI] [PubMed] [Google Scholar]
- 6.Herridge M.S., Azoulay É. Outcomes after critical illness. N Engl J Med. 2023;388(10):913–924. doi: 10.1056/NEJMra2104669. [DOI] [PubMed] [Google Scholar]
- 7.Needham D.M., Davidson J., Cohen H., Hopkins R.O., Weinert C., Wunsch H., et al. Improving long-term outcomes after discharge from intensive care unit: report from a stakeholders' conference. Crit Care Med. 2012;40(2):502–509. doi: 10.1097/CCM.0b013e318232da75. [DOI] [PubMed] [Google Scholar]
- 8.Jackson J.C., Hart R.P., Gordon S.M., Hopkins R.O., Girard T.D., Ely E.W. Post-traumatic stress disorder and post-traumatic stress symptoms following critical illness in medical intensive care unit patients: assessing the magnitude of the problem. Crit Care. 2007;11(1) doi: 10.1186/cc5707. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Davydow D.S., Gifford J.M., Desai S.V., Bienvenu O.J., Needham D.M. Depression in general intensive care unit survivors: a systematic review. Intensive Care Med. 2009;35(5):796–809. doi: 10.1007/s00134-009-1396-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Nikayin S., Rabiee A., Hashem M.D., Huang M., Bienvenu O.J., Turnbull A.E., et al. Anxiety symptoms in survivors of critical illness: a systematic review and meta-analysis. Gen Hosp Psychiatr. 2016;43:23–29. doi: 10.1016/j.genhosppsych.2016.08.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Parker A.M., Sricharoenchai T., Raparla S., Schneck K.W., Bienvenu O.J., Needham D.M. Posttraumatic stress disorder in critical illness survivors. Crit Care Med. 2015;43(5):1121–1129. doi: 10.1097/CCM.0000000000000882. [DOI] [PubMed] [Google Scholar]
- 12.Schmidt M., Boutmy-Deslandes E., Perbet S., Mongardon N., Dres M., Razazi K., et al. Differential perceptions of noninvasive ventilation in intensive care among medical caregivers, patients, and their relatives: a multicenter prospective study-the PARVENIR study. Anesthesiology. 2016;124(6):1347–1359. doi: 10.1097/ALN.0000000000001124. [DOI] [PubMed] [Google Scholar]
- 13.Iosifyan M., Schmidt M., Hurbault A., Mayaux J., Delafosse C., Mishenko M., et al. “I had the feeling that I was trapped”: a bedside qualitative study of cognitive and affective attitudes toward noninvasive ventilation in patients with acute respiratory failure. Ann Intensive Care. 2019;9(1) doi: 10.1186/s13613-019-0608-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Wenham T., Pittard A. Intensive care unit environment. Cont Educ Anaesth Crit Care Pain. 2009;9(6):178–183. [Google Scholar]
- 15.Gultekin Y., Ozcelik Z., Akinci S.B., Yorganci H.K. Evaluation of stressors in intensive care units. Turk J Surg. 2018;34(1):5–8. doi: 10.5152/turkjsurg.2017.3736. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Rai S., Brown R., van Haren F., Neeman T., Rajamani A., Sundararajan K., et al. Long-term follow-up for Psychological stRess in Intensive CarE (PRICE) survivors: study protocol for a multicentre, prospective observational cohort study in Australian intensive care units. BMJ Open. 2019;9(1) doi: 10.1136/bmjopen-2018-023310. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.von Elm E., Altman D.G., Egger M., Pocock S.J., Gøtzsche P.C., Vandenbroucke J.P. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet. 2007;370(9596):1453–1457. doi: 10.1016/S0140-6736(07)61602-X. [DOI] [PubMed] [Google Scholar]
- 18.Twigg E., Humphris G., Jones C., Bramwell R., Griffiths R.D. Use of a screening questionnaire for post-traumatic stress disorder (PTSD) on a sample of UK ICU patients. Acta Anaesthesiol Scand. 2008;52(2):202–208. doi: 10.1111/j.1399-6576.2007.01531.x. [DOI] [PubMed] [Google Scholar]
- 19.Henry J.D., Crawford J.R. The short-form version of the Depression Anxiety Stress Scales (DASS-21): construct validity and normative data in a large non-clinical sample. Br J Clin Psychol. 2005;44(Pt 2):227–239. doi: 10.1348/014466505X29657. [DOI] [PubMed] [Google Scholar]
- 20.Lovibond S.H., Lovibond P.F. 1995. Manual for the depression anxiety stress scales. [DOI] [PubMed] [Google Scholar]
- 21.Norman R., Cronin P., Viney R. A pilot discrete choice experiment to explore preferences for EQ-5D-5L health states. Appl Health Econ Health Pol. 2013;11(3):287–298. doi: 10.1007/s40258-013-0035-z. [DOI] [PubMed] [Google Scholar]
- 22.Hodgson C.L., Udy A.A., Bailey M., Barrett J., Bellomo R., Bucknall T., et al. The impact of disability in survivors of critical illness. Intensive Care Med. 2017;43(7):992–1001. doi: 10.1007/s00134-017-4830-0. [DOI] [PubMed] [Google Scholar]
- 23.Hatch R., Young D., Barber V., Griffiths J., Harrison D.A., Watkinson P. Anxiety, depression and post traumatic stress disorder after critical illness: a UK-wide prospective cohort study. Crit Care. 2018;22(1):310. doi: 10.1186/s13054-018-2223-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Righy C., Rosa R.G., da Silva R.T.A., Kochhann R., Migliavaca C.B., Robinson C.C., et al. Prevalence of post-traumatic stress disorder symptoms in adult critical care survivors: a systematic review and meta-analysis. Crit Care. 2019;23(1):213. doi: 10.1186/s13054-019-2489-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Davydow D.S., Gifford J.M., Desai S.V., Needham D.M., Bienvenu O.J. Posttraumatic stress disorder in general intensive care unit survivors: a systematic review. Gen Hosp Psychiatr. 2008;30(5):421–434. doi: 10.1016/j.genhosppsych.2008.05.006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Griffiths J., Fortune G., Barber V., Young J.D. The prevalence of post traumatic stress disorder in survivors of ICU treatment: a systematic review. Intensive Care Med. 2007;33(9):1506–1518. doi: 10.1007/s00134-007-0730-z. [DOI] [PubMed] [Google Scholar]
- 27.Australian Bureau of Statistics National study of mental health and wellbeing: summary results, 2020–21 [Internet] 2022. https://www.abs.gov.au/statistics/health/mental-health/national-study-mental-health-and-wellbeing/latest-release [cited 1st Mar 2023]. Available from:
- 28.Tanimoto S., Takayanagi K., Yokota H., Yamamoto Y. The psychological and physiological effects of an intensive-care unit environment on healthy individuals. Clin Perform Qual Health Care. 1999;7(2):77–82. [PubMed] [Google Scholar]
- 29.Lee M., Kang J., Jeong Y.J. Risk factors for post-intensive care syndrome: a systematic review and meta-analysis. Aust Crit Care Off J Confederat Austral Crit Care Nurses. 2020;33(3):287–294. doi: 10.1016/j.aucc.2019.10.004. [DOI] [PubMed] [Google Scholar]
- 30.Cuthbertson B.H., Wunsch H. Long-term outcomes after critical illness. The best predictor of the future is the past. Am J Respir Crit Care Med. 2016;194(2):132–134. doi: 10.1164/rccm.201602-0257ED. [DOI] [PubMed] [Google Scholar]
- 31.Kangas M., Henry J.L., Bryant R.A. Posttraumatic stress disorder following cancer. A conceptual and empirical review. Clin Psychol Rev. 2002;22(4):499–524. doi: 10.1016/s0272-7358(01)00118-0. [DOI] [PubMed] [Google Scholar]
- 32.Mehnert A., Koch U. Psychological comorbidity and health-related quality of life and its association with awareness, utilization, and need for psychosocial support in a cancer register-based sample of long-term breast cancer survivors. J Psychosom Res. 2008;64(4):383–391. doi: 10.1016/j.jpsychores.2007.12.005. [DOI] [PubMed] [Google Scholar]
- 33.Ostovar S., Modarresi Chahardehi A., Mohd Hashim I.H., Othman A., Kruk J., Griffiths M.D. Prevalence of psychological distress among cancer patients in Southeast Asian countries: a systematic review. Eur J Cancer Care. 2022;31(6) doi: 10.1111/ecc.13669. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Stein K.D., Syrjala K.L., Andrykowski M.A. Physical and psychological long-term and late effects of cancer. Cancer. 2008;112(11 Suppl):2577–2592. doi: 10.1002/cncr.23448. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Ngandu H., Gale N., Hopkinson J.B. Experiences of noninvasive ventilation in adults with hypercapnic respiratory failure: a review of evidence. Eur Respir Rev. 2016;25(142):451–471. doi: 10.1183/16000617.0002-2016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.McCormick J.L., Clark T.A., Shea C.M., Hess D.R., Lindenauer P.K., Hill N.S., et al. Exploring the patient experience with noninvasive ventilation: a human-centered design analysis to inform planning for better tolerance. Chronic Obstr Pulm Dis. 2022;9(1):80–94. doi: 10.15326/jcopdf.2021.0274. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Beckert L., Wiseman R., Pitama S., Landers A. What can we learn from patients to improve their non-invasive ventilation experience? 'It was unpleasant; if I was offered it again, I would do what I was told'. BMJ Support Palliat Care. 2020;10(1):e7. doi: 10.1136/bmjspcare-2016-001151. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Chaboyer W., Elliott D. Health-related quality of life of ICU survivors: review of the literature. Intensive Crit Care Nurs Off J Br Assoc Crit Care Nurses. 2000;16(2):88–97. doi: 10.1054/iccn.1999.1582. [DOI] [PubMed] [Google Scholar]
- 39.Gerth A.M.J., Hatch R.A., Young J.D., Watkinson P.J. Changes in health-related quality of life after discharge from an intensive care unit: a systematic review. Anaesthesia. 2019;74(1):100–108. doi: 10.1111/anae.14444. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Alam N., Nannan Panday R.S., Heijnen J.R., van Galen L.S., Kramer M.H.H., Nanayakkara P.W.B. Long-term health related quality of life in patients with sepsis after intensive care stay: a systematic review. Acute Med. 2017;16(4):164–169. [PubMed] [Google Scholar]
- 41.Granja C., Teixeira-Pinto A., Costa-Pereira A. Quality of life after intensive care--evaluation with EQ-5D questionnaire. Intensive Care Med. 2002;28(7):898–907. doi: 10.1007/s00134-002-1345-z. [DOI] [PubMed] [Google Scholar]
- 42.Bagshaw S.M., Stelfox H.T., Johnson J.A., McDermid R.C., Rolfson D.B., Tsuyuki R.T., et al. Long-term association between frailty and health-related quality of life among survivors of critical illness: a prospective multicenter cohort study∗. Crit Care Med. 2015;43(5):973–982. doi: 10.1097/CCM.0000000000000860. [DOI] [PubMed] [Google Scholar]
- 43.Sjoberg F., Orwelius L., Berg S. Health-related quality of life after critical care-the emperor's new clothes. Crit Care. 2020;24(1):308. doi: 10.1186/s13054-020-03012-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Beumeler L.F.E., van Wieren A., Buter H., van Zutphen T., Navis G.J., Boerma E.C. Long-term health-related quality of life, healthcare utilisation and back-to-work activities in intensive care unit survivors: prospective confirmatory study from the Frisian aftercare cohort. PLoS One. 2022;17(9) doi: 10.1371/journal.pone.0273348. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Davies H., McKenzie N., Williams T.A., Leslie G.D., McConigley R., Dobb G.J., et al. Challenges during long-term follow-up of ICU patients with and without chronic disease. Aust Crit Care Off J Confederat Austral Crit Care Nurses. 2016;29(1):27–34. doi: 10.1016/j.aucc.2015.04.002. [DOI] [PubMed] [Google Scholar]
- 46.Williams T.A., Leslie G.D. Challenges and possible solutions for long-term follow-up of patients surviving critical illness. Aust Crit Care Off J Confederat Austral Crit Care Nurses. 2011;24(3):175–185. doi: 10.1016/j.aucc.2011.03.001. [DOI] [PubMed] [Google Scholar]
- 47.Geense W.W., van den Boogaard M., Peters M.A.A., Simons K.S., Ewalds E., Vermeulen H., et al. Physical, mental, and cognitive health status of ICU survivors before ICU admission: a cohort study. Crit Care Med. 2020;48(9):1271–1279. doi: 10.1097/CCM.0000000000004443. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.