Abstract
Background
Although women face a wide range of contraceptive options, globally, young women are at risk of unintended pregnancies. Our umbrella review aimed to determine the decisional needs of nulligravida women aged 11 to 30 considering contraceptive options and identify effective interventions to support their involvement in making decisions about contraceptive use.
Methods
We followed Joanna Briggs Institute methods for umbrella reviews, theoretically guided by the Ottawa Decision Support Framework. We searched six electronic databases. Two reviewers independently screened citations, extracted data, and appraised quality using AMSTAR2. We analysed findings descriptively.
Results
Of 124 citations, we identified 11 reviews of variable quality (critically low to moderate quality): Six reported decisional needs and 5 reported on interventions. Decisional needs of young women were: (a) information needs about contraceptive options (e.g., mechanism of actions, eligibility, administration, side effects); (b) unclear values (concerns about hormone use) and features of different options (based on their religious values); and (c) need for support and resources (support from society and need for privacy). Compared to controls, decision support interventions including patient decision aids and patient education material increased knowledge and improved discussion of options with their clinicians.
Conclusion
Young women making contraceptive decisions experience unmet decisional needs. Effective interventions such as patient decision aids and general patient education materials may address their decisional needs and enhance their level of participation in making contraception decisions. Implications and contribution to the field: Young women’s decisional needs when considering contraceptive use are informational needs, unclear values (including religious influences), need for support and resources when facing this decision. Interventions, such as patient decision aid and patient education material can, address decisional needs by improving young women’s knowledge about contraceptive options.
Supplementary Information
The online version contains supplementary material available at 10.1186/s12905-024-03172-2.
Keywords: Contraception, Decisional needs, Decision making, Decision support intervention, Young women, Patient decision aids
Introduction
Despite availability of numerous contraceptive options [1], there continues to be unintended pregnancies in young women. Younger women who become pregnant are at higher risk of mortality and morbidity [2,3], and are more likely to have social and economic consequences including dropping out of school or challenges with job stability [2].
According to the United Nations and World Health Organization (WHO), family planning with contraceptive counselling is a human right for all women and is pivotal for obtaining gender equality, decreasing poverty, and enhancing women’s bodily autonomy [1,4]. Young women are eligible for the same contraceptive options as older women [1]. However, only 60% of young women aged 15–19 receive modern contraceptives options compared to 75% of women over 30 years (2020) [5]. The decision about which contraceptive method to select presents unique challenges for young nulligravida women [6,7]. Common side effects of contraceptives include pain on insertion, changes in menstrual bleeding, deep vein thrombosis, acne, and headaches; some side effects may be considered positive such as less bleeding or reduced hormonally mediated premenstrual symptoms (e.g. headaches, bloating) [8].
Young women are more likely to have their decisions influenced by their changing cognitive abilities, emotions, risk taking behaviours, and physical characteristics [9]. Specific barriers limiting access to contraceptive options include lack of information about, cultural and societal stigmas, attitudes of healthcare professionals, and legal issues can limit access to contraceptives [2]. Other social factors such as gender, income, education, and inequality may also inhibit their access to contraceptive services [2]. Furthermore, misperceptions and myths about contraceptive options are common (e.g. need for a pelvic examination, concerns for future infertility, weight gain, cancer risk, among others) [7] interfere with young women using contraceptives and results in higher chance of unintended pregnancies [7,10].
There are international efforts to increase the use of modern, effective, and safe long-acting reversible contraceptives (LARC) such as intrauterine devices (IUD) and contraceptive implants. Yet, LARC may be more painful during the insertion especially for nulligravida women and potential risks that should be considered during the decision making process [11].
It is paramount to respect young women´s reproductive rights and avoid providing biased information or using coercion towards using specific types of contraceptives [11]. Engaging young women in making contraceptive decisions can enhance their understanding of the benefits and risk/harm (including side effects), identify potential barriers to accessing contraceptives, and augment their feeling of autonomy [12]. Thereby, supporting young women to select an option that is congruent with their informed values for features and outcomes of options. To support them in achieving this quality decisions, it is essential to understand their decisional needs and determine if effective decision support interventions are available to address their needs [13]. This includes their understanding of the benefits and risks/harms (including side effects), identifying potential barriers to accessing contraceptives, and selecting an option that is congruent with their own values for features and outcomes of options [12]. To achieve a quality decision, decisional needs can be addressed with tailored decision support interventions such as patient decision aids and decision coaching [13].
Although recent umbrella reviews investigated components of decisional needs and identify interventions to support decision making about contraceptives [14,15], none have focused on the perspectives of young women making this decision [2,13]. The overall aim of our umbrella review was to summarize the evidence specific the decisional needs and effective decision support interventions for young women (aged 11–30) considering contraceptive options.
Review questions
What are the decisional needs of young women facing contraceptive options?
What are the effects of interventions that support young women in making decisions about contraceptive options on their knowledge, participation in decision making and experiences?
Methods
We conducted an umbrella review following the Joanna Briggs Institute (JBI) methodology for umbrella reviews [16] and theoretically informed by the Ottawa Decision Support Framework (ODSF) [13]. The protocol was registered in Prospero 2023 CRD42023402147. We reported the findings using the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines [17].
According to the ODSF [13,18], there are three key elements to consider for supporting people to be involved in decision making: decisional needs, decision support interventions and decisional outcomes. Common decisional needs include decisional conflict, inadequate knowledge, unrealistic expectations, unclear values, inadequate support and resources, and clinical and personal needs [19]. Decision support interventions that can be used to address the decisional needs include clinical counselling, patient decision aids, or decision coaching [13]. Decisional outcomes are focused on enhancing the quality of the decision and quality of the decision making process, ultimately indicative of a reduction in decisional needs.
Eligibility criteria
The inclusion and exclusion criteria are described using JBI framework: Population, Intervention and phenomenon of Interest, Context, Outcomes of Interest, and Study design (PICOS) [16,20].
Population
We included reviews of young women after menarche and no previous pregnancy (i.e., approximately 11 to 30 years old). For reviews of women of all age groups considering contraception, we only included those who reported specific findings for young women (≤ 30 years). For reviews that included nulliparous and parous women, we included reviews if more than 50% of participants did not report being or ever having been pregnant. We excluded reviews that investigated the perspectives of males, significant others, family members, or healthcare professionals. We also excluded reviews of women postpartum, seeking abortion, or with a specific health condition (e.g., rheumatoid arthritis, cancer, psychiatric disorders).
Intervention and phenomena of interest
The phenomena of interest included decisional needs about contraception decision making (research question 1) and interventions to support decision making about contraceptive options (research questions 2). Interventions for example included patient decision aids or patient education materials. Reviews were excluded if they focused on emergency contraception, pregnancy decisions, abortion, human immunodeficiency virus (HIV) or sexually transmitted diseases (STD) prevention, actual use of contraceptives (e.g., prevalence studies), or sterilization.
Context
Eligible reviews for decisional needs were conducted in global north countries as indicated in the World Bank’s interactive map [21]. Reviews were excluded if they were conducted in global south countries given the differences in healthcare services supporting young women considering contraception (e.g., availability of contraceptives, cost, cultural practices) [22,23].
Eligible reviews for interventions to support decision making were from any country. That interventions may be universally applied across higher and lower income countries and decision support interventions may be adapted for use in other countries.
Outcomes of interest
Eligible reviews reported on any decisional needs (e.g., decisional conflict, inadequate knowledge, unrealistic expectations, unsupported, unclear values, clinical and personal needs and/or other outcomes indicating decisional needs).
Outcomes for interventions to support decision making included improved knowledge, participation in decision making, and their experiences (e.g., decisional conflict, satisfaction). Reviews were excluded if they exclusively reported uptake or use of options.
Study design
Eligible studies included any peer-reviewed knowledge synthesis studies including systematic reviews with or without meta-analysis, scoping reviews, qualitative systematic reviews, realist reviews, and rapid reviews [24]. Studies were excluded if they were individual studies, not peer-reviewed, brief reports, editorials, commentaries, protocols, conference abstracts, literature reviews, narrative reviews, dissertations, or theses.
Information sources
The search strategy was developed with a Research Librarian (VC) and peer reviewed by another information specialist (ND) using the PRESS guideline [25]. The search was conducted in six electronic databases: MEDLINE (OvidSP) (see supplement), Embase (OvidSP), PsycInfo (OvidSP), CINAHL(EBSCOHost), Cochrane Database of Systematic Reviews (CDSR) and Web of Science (Core Collection) from January 2000 to March 2023. The time limit of 2000 reflects the United States Food and Drug Administration approval of the IUD Mirena® (Berlex Laboratories, Wayne, NJ); the first levonorgestrel-releasing intrauterine system to be approved for use [26]. No language limits were applied to the search. To capture the breadth of research on this topic, we searched the following concepts using a combination of subject headings and keywords: contraception, decision making and childbearing populations. In drafting the search strategy, the concept of “contraception” was informed by Mack et al.’s Cochrane review [27]. Canada’s Drug and Health Technology Agency’s systematic review search filter was adapted to include scoping, rapid and realist reviews and used for searches in the electronic data bases [28,29].
Selection process
Using Covidence (Veritas Health Information, Melbourne, Australia, 2023), two independent reviewers (LP, MMDB) used a two-level screening process: (a) titles and abstracts; and (b) full text articles. All discrepancies were resolved through discussion and when unsure, a third reviewer was involved (DS). For identified umbrella reviews, included reviews were screened using the two-step process by two independent reviewers (MMDB, DS).
Data collection process
Two independent reviewers (MMDB, DS, SK, QZ) extracted the data using an electronic standardized data extraction form. The extraction form followed the JBI Data Extraction Form for Review for Systematic Reviews and Research Syntheses (e.g., authors, year, study design etc.) [16] and included relevant ODSF elements, specifically decisional needs and decision support interventions) [13,18]. If inadequate details were reported in the systematic reviews on the decision support interventions, we consulted the primary study to extract this additional data. We reviewed extracted data to determine whether the decision support interventions met qualifying criteria to be a patient decision aid according to the International Patient Decision Aid Standards [30,31]. If the intervention did not fulfil these criteria it was defined as patient education material.
Quality and risk of bias assessment
At least two review authors (MMDB, QZ, DS, TW) independently assessed the quality of included systematic reviews using the AMSTAR2 [32] and two additional items from the JBI Critical Appraisal Checklist for Systematic Reviews and Research Syntheses (e.g., recommendations for policy, directions for new research [33] (see supplement).
To determine confidence in the results from each included review, we relied on AMSTAR2 critical items 4, 7, 9, 11, 13, and 15 [32]. The other AMSTAR2 items were considered non-critical [32]. Results were then rated as follows: 4) critically low confidence if there were more than one critical flaw 3) low confidence if there was one critical flaw 2) moderate confidence if there was more than one non-critical weaknesses; and 1) high confidence if there was one or fewer non-critical weaknesses [32].
For the primary studies of decision support interventions, we used the risk of bias results as reported in the systematic review.
Synthesis methods
Decisional needs were deductively analysed using the coding manual for the ODSF [13,18]. The interventions were analysed according to JBI summary of evidence for umbrella reviews [16]. Results were reported with their confidence rating as described above [32]. Findings were descriptively reported and summarized in tables.
Patient and public involvement
We included, as part of the author group, three women in the target age group (< 30 years of age) to ensure the experiences of young women faced with these decisions were captured in our study design, conduct, and dissemination. They contributed to every step of the umbrella review conduct, from conceptualization to writing the manuscript.
Results
Characteristics of included reviews
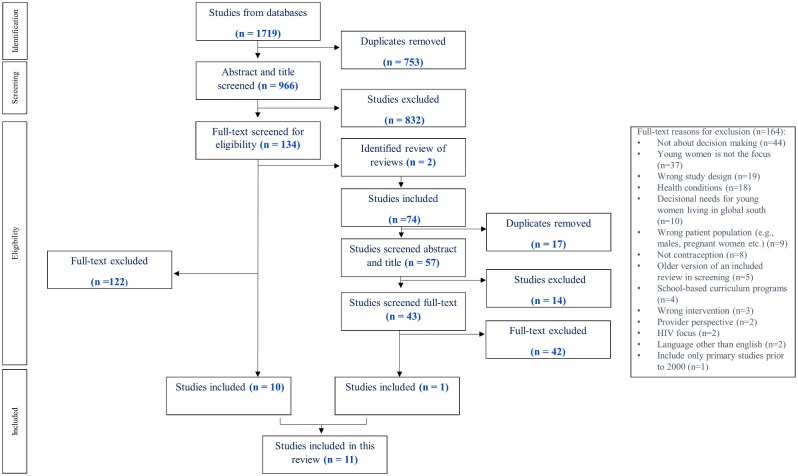
The database search identified 1719 records. After duplicates were removed, 966 records were screened resulting in 11 included reviews (see Fig. 1). The included reviews were conducted in the USA (n = 5), United Kingdom (n = 3), Canada (n = 1), Brazil (n = 1), and a multinational (UK, Belgium, United States of America, Switzerland) (n = 1). Most common reasons for excluding reviews at full text screening were: not focused on young women, not about decision making, limited to global south (decisional needs only), healthcare professional perspectives, male participants, post-partum (> 50% of sample), parent perspective, women undergoing abortion, women utilizing emergency contraception (see supplement S1). Some reviews reported on the same primary studies (see Table 1 and supplementS1).
Fig. 1.
Preferred Reporting Items for Systematic Reviews and Meta-Analyses flow diagram
Table 1.
Characteristics of the included reviews for decisional needs (N = 6) and decision support interventions (N = 5)
| Study details | Review aim | Type of review with number of studies | Number of databases (years) | Population age range | # primary studies eligible (population) |
|---|---|---|---|---|---|
| Decisional needs | |||||
|
Baxter (2011) UK [34] |
Examine young women and health care professionals’ views on contraceptive services | Systematic review of 59 studies | 12 databases (1995–2008) | 15–25 | 4 studies (N = 243) |
|
Daley (2014) USA [38] |
Synthesize research on contraceptive decision-making among adolescents | Meta-ethnography with 14 studies | 8 databases (2000–2012) | 12–21 | 8 studies (N = 255)* |
|
Fox (2018) USA [42] |
Describe clients’ preferences regarding contraceptive counselling approaches in the family planning setting | Systematic review of 26 studies | 16 databases (1992–2011) | 14–29 | 9 studies (N = 177) |
|
Kirubarajan (2022) Canada [39] |
Determine awareness of LARCs in young people and characterize knowledge gaps, predictors of knowledge, information sources of adolescents | Systematic review and meta-analysis of 40 studies | 3 databases (2001–2021) | 12–25 | 32 studies (N = 8348) |
| Reis (2018) Brazil [36] | Review studies concerning the decision-making process of adolescents who use LARCs | Systematic review of 9 studies | 8 databases (prior to May 2018) | 12–19 | 7 studies (N = 3741) |
|
Ti (2022) USA [37] |
Describe values and preferences of adolescents and young adults related to contraception | Systematic review of 55 studies | 10 databases (2005–2020) | 10–25 | 36 studies (N = 4575) |
| Decision support interventions | |||||
|
Blank (2012) UK [43] |
Explore effectiveness of services which provide contraception to young people delivered in developed countries | Systematic review and narrative synthesis of 23 studies | 11 databases (1995–2008) | < 25 | 1 study (N = 949) |
| Cavallaro (2019) UK, Belgium, USA, Sw [41] | Investigate comparative effectiveness of contraceptive counselling strategies on contraceptive behaviour and satisfaction | Systematic review of 61 studies | 6 databases (1990–2018) | 11–29 | 2 studies (N = 1156) |
| Goueth (2022) USA [42] | Effectiveness of technology-based contraceptive decision aids | Systematic review and meta-analysis of 18 studies | 7 databases (2005–2022) | 12–30 | 7 studies (N = 3612) |
|
Jones (2022) USA [40] |
Explore how effective are currently available contraceptive decision aids | Systematic review of 10 studies | 2 databases (2011–2021) | 11–30 | 4 (N = 2886)** |
|
Walker (2020) UK [44] |
Resources for healthcare professionals to guide or structure the process of conducting an integrated sexual and reproductive health consultation | Scoping review of 17 studies | 8 databases (1998–2017) | 18–29 | 1 study (N = 21) |
LARC= Long-Acting Reversible Contraception; Sw= Switzerland; UK= United Kingdom; USA=United States of America *The authors refer to Noblit, G. W., & Hare, R. D. (1988). Meta-ethnography: Synthesizing qualitative studies. Newbury Park, CA: Sage Publications **The authors state that due to heterogeneity of outcomes and methods in primary studies, the authors has performed a qualitative synthesis
Young women’s decisional needs
Six reviews reported on decisional needs, of which five were qualitative systematic reviews [34–37] including a meta-ethnography [38], and one systematic review combined a meta-analysis with qualitative data [39] (see Table 2). The evidence on decisional needs of young women considering contraception options were based on two low [35,39], and four critical low [34,36–38] reviews (see Table 3). According to JBI critical appraisal checklist, only two reviews [37,39] included information on recommendations for policy, and four [34,35,37,39], proposed areas for future research (see supplement). The four broad decisional needs identified were informational, values, support and resources, and personal characteristics (see Table 4).
Table 2.
Quality rating of included reviews based on AMSTAR 2
| First author (year) | Item 1 PICO |
Item 2 Protocol |
Item 3 Selection of study design |
Item 4 Compre-hensive search |
Item 5 Duplicate study selection |
Item 6 Extract in duplicate |
Item 7 Justify exclusion |
Item 8 Detailed included studies |
Item 9 Risk of bias (RoB) assessed |
Item 10 Sources of funding |
Item 11 Meta-analysis performed |
Item 12 Meta-analysis; potential RoB |
Item 13 Account for RoB in discussion |
Item 14 Hetero-geneity |
Item 15 Publica-tion bias |
Item 16 Conflict of interest |
Overall rating | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Decisional needs | ||||||||||||||||||
| Baxter (2011) | No | No | No | Yes | No | No | No | Yes | Yes | No | N/A | N/A | No | No | N/A | Yes | Critical low | |
| Daley (2014) | Yes | No | Yes | Yes | No | No | No | Yes | No | No | N/A | N/A | No | No | N/A | Yes | Critical low | |
| Fox (2018) | No | No | No | Partial yes | Yes | Yes | No | Yes | Yes | Yes | N/A | N/A | Yes | No | N/A | Yes | Low | |
| Kirubarajan (2022) | Yes | No | Yes | Yes | Yes | Yes | No | No | Yes | No | Yes | Yes | Yes | Yes | Yes | Yes | Low | |
| Reis (2018) | Yes | No | Yes | Yes | Yes | Yes | No | Partial Yes | No | No | N/A | N/A | No | No | N/A | Yes | Critical low | |
| Ti (2022) | Yes | No | Yes | Yes | Yes | Yes | No | Yes | No | No | N/A | N/A | Yes | Yes | N/A | Yes | Critical low | |
| Decision support interventions | ||||||||||||||||||
| Blank (2012) | Yes | No | Yes | Partial Yes | No | No | No | Yes | Yes | No | N/A | N/A | Yes | No | N/A | Yes | Critical low | |
| Cavallaro (2020) | Yes | Yes | No | Yes | No | No | No | No | No | No | N/A | N/A | No | No | N/A | Yes | Critical low | |
| Goueth (2022) | Yes | Yes | Yes | Partial Yes | Yes | Yes | No | Yes | Yes | No | Yes | Yes | Yes | Yes | Yes | Yes | Low | |
| Jones (2022) | Yes | No | Yes | Yes | Yes | Yes | Partial yes | Yes | Yes | No | N/A | N/A | Yes | Yes | N/A | Yes | Moderate | |
| Walker (2020) | No | No | No | Yes | Yes | No | No | Partial Yes | No | No | N/A | N/A | No | No | N/A | Yes | Critical low | |
N/A= Not applicable
Table 3.
Decisional needs of young women considering contraception options (n=6 reviews)
| Review first author (year) | Countries of included primary studies | Data collection method(s) (n) | Information needs | Values | Support and resources | Personal characteristics | Confidence in results† |
|---|---|---|---|---|---|---|---|
|
Baxter (2011) [[34]] |
UK(n = 4) | Interview (n = 56), survey (n = 167), interview and survey (n = 20) | Yes | Yes | Yes | Critical low | |
|
Daley (2014) [[38]] |
USA (n = 8) | Interviews (n = 148), focus groups (n = 102), grounded theory (n = 5) | Yes | Yes | Yes | Yes | Critical low |
|
Fox (2018) [[35]] |
USA (n = 8), Belgium (n = 1) | Interviews (n = 100), focus group (n = 26), interview and survey (n = 35), interview and focus group (n = 16) | Yes | Low | |||
|
Kirubarajan (2022) †† [[39]] |
USA (n = 25) UK (n = 2), Norway (n = 1), Netherlands (n = 1), Australia (n = 2), New Zealand (n = 1) | Interviews (n = 310), focus group (n = 88), survey (n = 7340), interviews and survey (n = 14), focus group and survey (n = 596) | Yes | Low | |||
|
Reis (2018) †† [[36]] |
USA (n = 6), Greece (n = 1) | Cohort (n = 3441), survey (n = 300) | Yes | Yes | Critical low | ||
|
Ti (2022) [[37]] |
USA (n = 25), UK (n = 7), Canada (n = 1), Puerto Rico (n = 1), Australia (n = 2), Austria (n = 1), New Zealand (n = 1) | Interviews (n = 563), focus group (n = 15), survey (n = 3054), cohort (n = 731), case series (n = 20), RCT (n = 130), focus group and interviews (n = 62) | Yes | Yes | Yes | Critical low |
† AMSTAR2 total score= Measurement Tool to Assess systematic Reviews; UK= United Kingdom; USA=United States of America † † Exclusively about LARC; blank=not reported
Table 4.
Effects of interventions to support decision making process for young women in regards of contraception
| First author (year) of primary study study; study design; (sample size); country | Review first author (year) Risk of bias of primary study reported in review‡ |
Intervention
Number of contraceptive methods included |
Comparator | Results | ||
|---|---|---|---|---|---|---|
| Knowledge | Participation in decision making | Experiences | ||||
|
Chewning (1999) Longitudinal (N = 949) USA [[48]] |
Cavallaro (2019) Risk of bias not reported Blank (2012) Good quality |
Contraceptive decision making programme, followed with clinic visit Control group (standard patient education and clinic visit) No details given |
NR | Compared to control: Increased knowledge (p ≤ 0.000) | NR | Compared to control: more confidence in oral contraceptive efficacy (p ≤ 0.000) |
|
Antonishak (2015) RCT (N = 2284) USA [[50]] |
Jones (2022) Medium risk of bias |
Online birth control support network; website Bedsider.org 17 methods |
Control group (no exposure) | Compared to control: more familiar with different methods (p = .00); no difference in knowledge of relative effectiveness. | NR | NR |
|
Marshall (2017) Qualitative interviews (N = 21) USA [[53]] |
Walker (2020) Risk of bias not reported |
Contraceptive decision support tool plus; website, LARC videos and counselling (My control navigator) “Birth Control Navigator” 16 methods |
No comparator | Informative; missed some information (e.g. sexual pleasure); narrowed down options; less biased information | NR | User experienced it to be useful before consultation |
|
Dehlendorf (2019) cRCT (N = 748 under 30 years) (73.2% of total participants aged 15–29) USA [[45]] |
Goueth (2022) Good overall rating |
Contraceptive decision support tool; website (“My Birth Control”) https://clinic.mybirthcontrol.org/ 11 methods |
Control group (standard counseling) | Compared to control: Increased knowledge; Answered question correctly on IUDs (OR, 2.47; CI, 1.75–3.49; p = < .01) | Compared to control: no difference on making the decision themselves (> 72% both groups) | Compared to control: no difference in overall decisional conflict 25.4% vs 22.6% (p = .41) |
| Patient education materials | ||||||
|
Gilliam (2014) Pilot RCT (N = 52) USA [[51]] |
Jones (2022) Medium risk of bias Goueth (2022) Fair overall rating |
Waiting-room application followed by standard counselling (provided with same day contraceptives) Not specified, but emphasized LARC (15 minute) |
Control group (standard contraceptive counselling care) | Compared to control: Increased knowledge; (p = .0001) | NR | Intervention group responded they would recommend app to a friend |
|
Mesheriakova, (2017) Prospective cohort study (N = 120) USA [[54]] |
Goueth, 2022 Risk of bias not reported |
Interactive, individually tailored application (“Health-E You”) Not specified |
No comparator | Increased knowledge (p ≤ .001) | NR | NR |
|
Hebert (2018) RCT (N = 207) USA [[55]] |
Cavallaro (2019) Risk of bias not reported Jones (2022) High risk of bias Goueth (2022) Fair overall rating |
Waiting-room application with LARC videos and counselling (“miPlan”) All method showing tiered effectiveness; focus on LARC (10 minutes) |
Control group (standard clinic visit) | Compared to control Increased knowledge (p < .001) | NR | NR |
|
Sridhar (2019) Pre-post test (N = 120) USA [[49]] |
Jones, 2022 Low risk of bias |
Comics paper format (www.birthcontroltales.com) Injection, IUD, implant, combined hormonal |
No comparator | Increased perceived knowledge (p = .001); 80% easy to understand | NR | 75% appreciated |
|
Tebb (2021) cRCT (18 sites, N = 1360 Latina/Hispanic girls) USA [[52]] |
Goueth, 2022 Fair overall rating |
Interactive, individually tailored application (“Health-E You/Salud iTu”) with tailored recommendations based on preference; printout for use in counselling with provider Not specified |
Control group (baseline survey on ipad, followed by standard counselling) |
Compared to control: Increased knowledge 3.3 (± 1.6) at baseline to 4.6 (± 1.7) after app use (p < 0.001); 43% too much information |
Compared to control: higher OR of discussing method with provider, (OR 2.22 (0.98, 5.01)); 70% intervention arm felt it helped quality of the health visit | High satisfaction with intervention |
|
Manlove (2020) Manlove (2021) RCT (N = 1124) Replication study (N = 871) USA |
Goueth, 2022 Good overall rating |
Reproductive health application (“Pulse”) to provide sexual and reproductive health content for young Black and Latinx women Not specified |
Control group (access to general health application) | Compared to control: increased knowledge (50% vs. 42%; p = 0.000)[47] | NR | NR |
CI= confidence interval; IUD=intrauterine device; LARC= Long-Acting Reversible Contraception; p= p value; NR= not reported; OR= Odds ratio; cRCT=cluster randomized control trial; RCT=Randomized control trial; USA=United States of America
‡ Instruments used for risk of bias assessment in primary studies: Blank (2012) utilized criteria developed by National Institute for Health and Clinical Excellene (2009); Jones (2022) utilized Cochrane Collaborative tool for risk of bias in RCTs and the ROBINS-I tool for non-RCT studies; Goueth (2022) utilized criteria developed by the US Preventative Services Task Force
The informational needs of young women were: safety concerns, mechanisms of actions, how it affected fertility (related to fear of becoming infertile), protection against sexual transmitted infection, eligibility, and insertion methods (with or without anesthesia) [37,39]. Further, young women expressed the importance of receiving hand-outs of personalized information, for example on side effects, as being complementary to counselling [35]. Specific to LARC, young women overestimated the risk of rare events and were challenged to understand how it worked [37]. Also, women described having a lack of knowledge on availability of contraception, misconceptions about the risk of unprotected sex, and fears about the side effects such as bleeding [38].
The features of contraception option that young women valued were: avoiding intake of hormones, menstrual related effects such as mood swings, and changes in body weight [37]. Furthermore, sexual behaviour related activities young women valued were intercourses as a spontaneous act, and avoiding pregnancy, and sexually transmitted infections [38]. Young women also reported being concerned about losing social standing and image, and not being stigmatized about their sexual activities [34].
Young women’s needs about support and resources was described as the influence of the social context in which contraceptive decisions are made such as wider society, religion, peers, parents, community, and partners, influenced values and preferences [37]. Furthermore, it was important for young women to experience privacy in the decision making process and also in option chosen [37]. Friends who had experienced a pregnancy were considered a source of support [38]. Young women wanted access to healthcare services with healthcare professionals providing fact based and a friendly approach that respected confidentiality [34,38]. Some young women experienced financial constraints that influenced their decision about contraception [38].
Personal characteristics that influenced their decisions about contraception were: feelings of embarrassment and their religious belief [34,38]. For example, young Muslim women were more likely than orthodox Christian women to favour the use of IUDs [36].
Effects of interventions to support young women’s contraceptive decisions
Five reviews reported on decision support interventions: two systematic reviews [40,41], one systematic review with meta-analysis [42], one systematic review with narrative synthesis [43], and one scoping review [44]. The evidence on interventions to support decision making for young women considering contraceptive options were primary studies (n = 11) reported in reviews rated as moderate [40], low [42], or critically low [41,43,44] according to AMSTAR 2 (see Table 3). According to the JBI critical appraisal items, two reviews offered information for policy [42,43], and two reviews included suggestions on priorities for future research [40,42]. Based on the risk of bias reported in the included reviews, the primary studies were rated as: low risk of bias [45–49], moderate risk of bias [50–52], not reported [53,54] and conflicting results [55]. All the interventions studies were conducted in USA. Detailed information on the interventions is in Table 4.
These reviews reported on two types of decision support interventions: patient decision aids and patient education materials. Four primary studies presented patient decision aids meeting qualifying criteria according to the International Patient Decision Aid Standards presented in the following formats: two websites [45,50], one website with videos and counselling [53], and one computer program [48]. Seven primary studies presented patient education materials in the following formats: one comic in paper format [49], four mobile applications [46,47,52,54] and two waiting room application followed with standard counselling [51,55].
Knowledge
Compared to controls, young women exposed to patient decision aids experienced increased knowledge [45,48]. In another study, compared to controls, young women exposed to patient decision aids were more familiar with contraceptive options, however, there was no difference in their knowledge of effectiveness of contraception methods [50]. Patient education material was found to increase knowledge in the intervention group [46,47,49,51,52,54,55]. Only one study reported 43% of participants thought the interventions had too much information [52].
Participation in decision making
When young women used a patient decision aid, there was no difference in their level of participation in decision making, compared to controls [45]. One study evaluating patient education material found the intervention group had a higher odds of discussing contraceptive options with their healthcare professional and 70% reported that the intervention aided the quality of the healthcare visit [52].
Experiences
Young women who used the patient decision aid had increased confidence in oral contraceptives [48], and had less decisional conflict (not statistical significant) [45]. In one qualitative study, participants described the patient decision aid as informative, narrowing the options, presenting less biased information, and as more useful before the consultation with their healthcare professional [53]. In three studies, patient education materials were positively viewed by participants [49,52], and participants would recommend the patient education material to a friend [51].
Discussion
Our umbrella review identified 6 reviews describing decisional needs of young women and 5 reviews of interventions to support them making decisions about contraception options. The decisional needs identified were informational needs, young women’s values for features of contraception options, unmet needs for support and resources, and the influence of personal characteristics. Patient decision aids and patient education materials increased knowledge of contraceptive options, and the strength of their effectiveness was supported by primary studies with low risk of bias and reviews with moderate to critically low quality. Two new decisional needs identified by young women considering contraceptive options that were not yet reported in the ODSF were confidentiality and feelings of embarrassment. These needs were reported in other reviews about contraceptive healthcare services [14,56] and they should be considered in the design and delivery of interventions to support young women making these decision. Other decisional needs identified in our review were consistent with those reported by Hoefel et al., in their systematic review of 45 decisional needs assessment studies of adults making healthcare decisions [19]. Both our review and the Hoefel systematic review were based on the ODSF [13].
Lack of knowledge and misconceptions about contraceptive options is of concern given they are decisional needs interfering with achieving quality decisions and common barriers to contraception use [13,14]. Specifically, young women had misconception about insertion and removal of IUDs. Young women globally utilize IUDs to a lesser extent than older women [5]. Recent developments in the field of IUDs [57], may change young women’s attitudes towards IUDs. For example, a recent global survey among gynecologist found that removal is seen as easy, quick procedure which is contrary to some young women who believe removal requires anesthesia [58].
Although younger people tend to be more motivated to be involved in the decision making process, they also tend to lack confidence or even skills to make these decisions and their level of involvement is influenced by health literacy [59]. These personal characteristics were not identified in our review of decisional needs. However, our review of decision support interventions showed that patient education materials targeting young women improved communications about contraception options with their healthcare team and enhanced the quality of their visit [52].
Decision support interventions about contraceptive options identified in our review, patient decision aids and patient education materials, both were more effective than controls for improving knowledge [40–43]. These finding were reported in two reviews with low risk of bias [40,42] and are consistent with a systematic review of 209 patient decision aids [60]. We did not identify studies that evaluated other interventions known to support decision making such as decision coaching or question prompts [15,61,62]. A recent umbrella review investigated the effectiveness of interventions to increase contraceptive use and improve contraception choice among women of all ages [15]. The authors found that motivational interviewing, contraceptive counselling, school-based education, interventions promoting contraceptive access, demand-generation interventions (community and facility based, financial mechanisms and mass media), and mobile phone message interventions increased use of contraceptives [15]. Given that these interventions focused on increasing uptake of contraceptive rather than involving women in choosing the contraceptive option that fits best with their personal circumstances, this study was excluded from our umbrella review. Moreover, the focus on uptake may be an indication that decisional needs may be less prioritized in the research field, and outcomes such as uptake, interest or change in contraceptives are prioritized.
Decision support interventions must be non-directive to facilitate true shared decision making [12]. However, many interventions identified as supporting decision making focus mainly on LARC and were about increasing uptake of LARC options. Guiding young women in which options are most effective is an approach recommended by the WHO [1] and the patient education materials that presented options using a tiered approach did increase uptake of contraceptives [41]. However, there was limited information on these interventions reported in the included studies and it was not clear the extent to which these interventions, included counseling and/or presented balanced, non-directive, information on the options. A recent narrative review aimed to aid clinicians to develop an adolescent-centered, shared decision making approach that respects young women’s choices in regard of their reproductive autonomy [11]. The authors advocated for young women needing information, support, resources, and ways to engage in health care choices independently of their parents or social network. Bearing in mind that social media increasingly influences young women’s healthcare choices [63,64], future research could focus on the distinct decisional needs and digital decision making interventions for young women.
Interestingly, none of the included reviews reported on transgender men or young women with polycystic ovarian syndrome considering contraceptive options. Both groups may benefit from more research on the decision making process of contraceptive options due to the complexity of therapies. For example, transgender men may want to consider fertility preservation rather than permanent contraceptive options [65]. While women diagnosed with polycystic ovarian syndrome, may take medications that could interfere with the effectiveness of contraceptives, due to the altered metabolic function [66].
Our review findings lead to some implications for healthcare professionals and policymakers. Healthcare professionals can facilitate the involvement of young women in these healthcare decisions by recognizing decisional needs as discussed above and providing them with effective interventions such as patient decision aids and patient education materials. However, previous systematic reviews identified barriers to healthcare professionals involving patients in shared decision making and using patient decision aids in clinical practice. Common barriers for healthcare professionals are poor quality information, relational power imbalances, insufficient time, inadequate training, organizational culture that does not support patient involvement, and lack of leadership support [67–69]. Patient decision aids are effective interventions to address the poor-quality information and support patient involvement in decision making [70]. To successfully implement patient decision aids, decision aids should be co-produced with those who are target users such as young women considering contraceptive options, provide training to the whole healthcare team, prepare or invite patients to participate in the decision, get organizational support, and measure use of patient decision aids and patient outcomes as part of a quality improvement process [71]. From a policymaker perspective, patient decision aids are more likely to be used if they are endorsed by governments and healthcare organizations, kept in repositories endorsed by policymakers, and if there are financial incentives to use them [72–74].
Strengths and limitations
According to the AMSTAR2 the overall quality of evidence is based on reviews scoring low or critical low; only one review scored moderate for interventions to support decision making [40]. Ten of the 11 reviews included where rated critical low or low in accordance with AMSTAR2. This may affect the trustworthiness of the review’s findings and suggest there is a need for future rigorous research focused on young women aged 11–30. Another limitation of our study is the heterogeneity of the risk of bias assessment that we recounted from the primary intervention studies; making it challenging to compare risk of bias assessment findings across studies. Interestingly, the included interventions studies were all conducted in the United States. Due to different healthcare and legal systems globally, young women have different opportunities for access to contraceptives [14]. In most settings young females from lower socioeconomic backgrounds had greater challenges accessing any healthcare services including access to contraceptives [14]. Our findings may be less generalizable to other geographical setting and populations with lower socioeconomic status. Finally, having conducted an umbrella review, our findings were limited to the inclusion criteria of those reviews.
The strength of the current umbrella review is the that two independent reviewers screened both at abstract and full-text level for eligibility, as well as extracted data for the included studies. We conducted a comprehensive search of six databases with our search strategy PRESSed by another information specialist. Another strength is that our knowledge synthesis was theoretically grounded using the ODSF.
Conclusions
Our umbrella review identified six publications that reported on the decisional needs of young women considering contraceptive options and five publications of decision support interventions aimed at young women. Decisional needs of young women indicated the need for better sources of information on contraceptive options, confidential support from healthcare professionals, financial resources to access a broader range of contraceptive options, and important features of contraceptive options that young women value. Unique decisional needs for young women was having confidential contraceptive services to minimize feelings of embarrassment. Decision support interventions such as patient decision aids and general patient education materials improved knowledge, increased confidence in the chosen contraception option, and resulted in less decisional conflict. Further research should include more interventions aimed at supporting young women’s making contraceptive decisions, and exploring unique decisional needs of young women who have polycystic ovarian syndrome and transgender men.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Acknowledgements
We thank Nicholas Dehler, MIS, Research Librarian at the University of Ottawa for peer reviewing the MEDLINE search strategy, Meg Carley a Clinical Research Coordinator at the Ottawa Hospital Research Institute for providing guidance on the preparation of our article, and Mish Boutet, MIS, for creating the figures presented in our article.
Abbreviations
- IUD
Intrauterine devices
- JBI
Joanna Briggs Institute
- LARC
Long-acting reversible contraceptives
- ODSF
Ottawa Decision Support Framework
- PICOS
Population, Intervention and phenomenon of Interest, Context, Outcomes of Interest, and Study design
- PRISMA
Preferred Reporting Items for Systematic Reviews and Meta-Analyses
- WHO
World Health Organization
Author contributions
MMDB: conceptualization, data curation, formal analysis, methodology, validation, visualization, writing - original draft. SK: validation, writing - review & editing. LPB: conceptualization, formal analysis, validation, writing - review & editing. BD: conceptualization, writing - review & editing. EHH: conceptualization, writing - review & editing. KBL: conceptualization, writing - review & editing, QZ: formal analysis, validation, writing - review & editing. VC: investigation, data curation, writing - review & editing. TW: conceptualization, methodology, formal analysis, validation, visualization, writing - review & editing, co-supervision. DS: conceptualization, methodology, formal analysis, validation, visualization, writing - review & editing, co-supervision.
Funding
Partial funding for a research assistant was received from the University of Ottawa Research Chair in Knowledge Translation to Patients held by Dawn Stacey.
Open access funding provided by University Of South-Eastern Norway
Data availability
The datasets used and/or analysed during the current study is available from the corresponding author on reasonable request. Authors have no relevant financial relationships or perceived, potential or real conflicts of interest to disclose.
Declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Footnotes
The original online version of this article was revised: the affiliation details for author Elisabeth Holm Hansen and Dawn Stacey were incorrect and the figures were missing from the supplementary material of this article. It has been updated.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.World Health Organization. Selected practice recommendations for contraceptive use. 2016 [ https://apps.who.int/iris/bitstream/handle/10665/252267/9789241565400-eng.pdf. [PubMed]
- 2.Bitzer J, Abalos V, Apter D, Martin R, Black A. Targeting factors for change: contraceptive counselling and care of female adolescents. Eur J Contracept Reproductive Health Care. 2016;21(6):417–30. 10.1080/13625187.2016.1237629 [DOI] [PubMed] [Google Scholar]
- 3.World Health Organization. Adolescent pregnancy 2023 [2023 Jun 02:[ https://www.who.int/en/news-room/fact-sheets/detail/adolescent-pregnancy.
- 4.United Nations,Resolution XVIII. Human Rights Aspects of Family Planning, Final Act of the International Conference on Human Rights. Doc. A/CONF. 32/41, p.15, (1968).
- 5.United Nations Department of Economic and Social Affairs PD. World Family Planning. 2022. Meeting the changing needs forfamily planning: Contraceptiveuse by age and method 2022 [UN DESA/POP/2022/TR/NO. 4:[ https://www.un.org/development/desa/pd/sites/www.un.org.development.desa.pd/files/files/documents/2023/Feb/undesa_pd_2022_world-family-planning.pdf.
- 6.Marshall C, Kandahari N, Raine-Bennett T. Exploring young women’s decisional needs for contraceptive method choice: a qualitative study. Contraception. 2018;97(3):243–8. 10.1016/j.contraception.2017.10.004 [DOI] [PubMed] [Google Scholar]
- 7.Todd N, Black A. Contraception for adolescents. J Clin Res Pediatr Endocrinol. 2020;12(Suppl 1):28–40. 10.4274/jcrpe.galenos.2019.2019.S0003 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Teal S, Edelman A. Contraception Selection, Effectiveness, and adverse effects: a review. JAMA. 2021;326(24):2507–18. 10.1001/jama.2021.21392 [DOI] [PubMed] [Google Scholar]
- 9.Nucci-Sack A, Rojas M, Alpert IL, Lorde-Rollins E, Minguez M, Diaz A. Approach to and evaluation of the adolescent female. In: Altchek ADL, editor. Pediatric, adolescent & young adult gynecology. Chichester, UK: Wiley-Blackwell; 2009. pp. 134–40. [Google Scholar]
- 10.World Health Organization. Adolescent Sexual Reproductive Health. Overview 2023 [ https://www.who.int/southeastasia/activities/adolescent-sexual-reproductive-health.
- 11.Durante JC, Sims J, Jarin J, Gold MA, Messiah SE, Francis JKR. Long-acting reversible contraception for adolescents: a review of practices to support Better Communication, Counseling, and adherence. Adolesc Health Med Ther. 2023;14:97–114. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Stacey D, Hill S, McCaffery K, Boland L, Lewis KB, Horvat L. Shared decision making interventions: theoretical and empirical evidence with implications for health literacy. Stud Health Technol Inf. 2017;240:263–83. [PubMed] [Google Scholar]
- 13.Stacey D, Légaré F, Boland L, Lewis KB, Loiselle MC, Hoefel L, et al. 20th anniversary Ottawa decision support Framework: part 3 overview of systematic reviews and updated Framework. Med Decis Mak. 2020;40(3):379–98. 10.1177/0272989X20911870 [DOI] [PubMed] [Google Scholar]
- 14.D’Souza P, Bailey JV, Stephenson J, Oliver S. Factors influencing contraception choice and use globally: a synthesis of systematic reviews. Eur J Contracept Reprod Health Care. 2022;27(5):364–72. 10.1080/13625187.2022.2096215 [DOI] [PubMed] [Google Scholar]
- 15.D’Souza P, Phagdol T, D’Souza SRB, Anupama DS, Nayak BS, Velayudhan B, et al. Interventions to support contraceptive choice and use: a global systematic map of systematic reviews. Eur J Contracept Reprod Health Care. 2023;28(2):83–91. 10.1080/13625187.2022.2162337 [DOI] [PubMed] [Google Scholar]
- 16.Aromataris E, Fernandez R, Godfrey CHC, Khalil H, Tungpunkom P. Chapter 10: Umbrella Reviews. 2020 [ https://synthesismanual.jbi.global.
- 17.Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71. 10.1136/bmj.n71 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.O’Connor AM, Tugwell P, Wells GA, Elmslie T, Jolly E, Hollingworth G, et al. A decision aid for women considering hormone therapy after menopause: decision support framework and evaluation. Patient Educ Couns. 1998;33(3):267–79. 10.1016/S0738-3991(98)00026-3 [DOI] [PubMed] [Google Scholar]
- 19.Hoefel L, O’Connor AM, Lewis KB, Boland L, Sikora L, Hu J, Stacey D. 20th anniversary update of the Ottawa decision support Framework Part 1: a systematic review of the Decisional needs of people making Health or Social decisions. Med Decis Mak. 2020;40(5):555–81. 10.1177/0272989X20936209 [DOI] [PubMed] [Google Scholar]
- 20.Methley AM, Campbell S, Chew-Graham C, McNally R, Cheraghi-Sohi S. PICO, PICOS and SPIDER: a comparison study of specificity and sensitivity in three search tools for qualitative systematic reviews. BMC Health Serv Res. 2014;14:579. 10.1186/s12913-014-0579-0 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.The World Bank. The World by Income and Region 2022 [ https://datatopics.worldbank.org/world-development-indicators/the-world-by-income-and-region.html.
- 22.Sedgh G, Finer LB, Bankole A, Eilers MA, Singh S. Adolescent pregnancy, birth, and abortion rates across countries: levels and recent trends. J Adolesc Health. 2015;56(2):223–30. 10.1016/j.jadohealth.2014.09.007 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Munakampe MN, Zulu JM, Michelo C. Contraception and abortion knowledge, attitudes and practices among adolescents from low and middle-income countries: a systematic review. BMC Health Serv Res. 2018;18(1):909. 10.1186/s12913-018-3722-5 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Grant MJ, Booth A. A typology of reviews: an analysis of 14 review types and associated methodologies. Health Info Libr J. 2009;26(2):91–108. 10.1111/j.1471-1842.2009.00848.x [DOI] [PubMed] [Google Scholar]
- 25.McGowan J, Sampson M, Salzwedel DM, Cogo E, Foerster V, Lefebvre C. PRESS peer review of electronic search strategies: 2015 Guideline Statement. J Clin Epidemiol. 2016;75:40–6. 10.1016/j.jclinepi.2016.01.021 [DOI] [PubMed] [Google Scholar]
- 26.Gemzell-Danielsson K, Kubba A, Caetano C, Faustmann T, Lukkari-Lax E, Heikinheimo O. Thirty years of mirena: a story of innovation and change in women’s healthcare. Acta Obstet Gynecol Scand. 2021;100(4):614–8. 10.1111/aogs.14110 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Mack N, Crawford TJ, Guise JM, Chen M, Grey TW, Feldblum PJ, et al. Strategies to improve adherence and continuation of shorter-term hormonal methods of contraception. Cochrane Database Syst Rev. 2019;4(4):Cd004317. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.SR / MA / HTA / ITC - CINAHL. In: CADTH Search Filters Database. Ottawa: CADTH. 2023: 2023 Mar 07 [ https://searchfilters.cadth.ca/link/98].
- 29.SR / MA / HTA / ITC - MEDLINE, Embase. PsycInfo. In: CADTH Search Filters Database. Ottawa: CADTH; 2023: 2023 Mar 07 [ https://searchfilters.cadth.ca/link/33].
- 30.Joseph-Williams N, Newcombe R, Politi M, Durand MA, Sivell S, Stacey D, et al. Toward Minimum standards for certifying patient decision aids: a modified Delphi Consensus process. Med Decis Mak. 2014;34(6):699–710. 10.1177/0272989X13501721 [DOI] [PubMed] [Google Scholar]
- 31.Martin RW, Brogård Andersen S, O’Brien MA, Bravo P, Hoffmann T, Olling K, et al. Providing Balanced Information about options in patient decision aids: an update from the International patient decision Aid standards. Med Decis Mak. 2021;41(7):780–800. 10.1177/0272989X211021397 [DOI] [PubMed] [Google Scholar]
- 32.Shea BJ, Reeves BC, Wells G, Thuku M, Hamel C, Moran J, et al. AMSTAR 2: a critical appraisal tool for systematic reviews that include randomised or non-randomised studies of healthcare interventions, or both. BMJ. 2017;358:j4008. 10.1136/bmj.j4008 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Joanna Briggs Institute. The Joanna Briggs Institute Critical Appraisal tools for use in JBI Systematic Reviews 2017 [ https://jbi.global/sites/default/files/2019-05/JBI_Critical_Appraisal-Checklist_for_Systematic_Reviews2017_0.pdf.
- 34.Baxter S, Blank L, Guillaume L, Squires H, Payne N. Views of contraceptive service delivery to young people in the UK: a systematic review and thematic synthesis. J Fam Plann Reprod Health Care. 2011;37(2):71–84. 10.1136/jfprhc.2010.0014 [DOI] [PubMed] [Google Scholar]
- 35.Fox E, Reyna A, Malcolm NM, Rosmarin RB, Zapata LB, Frederiksen BN, et al. Client preferences for contraceptive counseling: a systematic review. Am J Prev Med. 2018;55(5):691–702. 10.1016/j.amepre.2018.06.006 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Reis YN, Vilela AL, de Souza Costa A, Andrade MRF, Filho ESF, de Abreu LC, et al. Factors Associated with adolescents’ choice to use long acting reversible contraceptives: a systematic review. Curr Obstet Gynecol Rep. 2018;7(4):153–62. 10.1007/s13669-018-0252-4 [DOI] [Google Scholar]
- 37.Ti A, Soin K, Rahman T, Dam A, Yeh PT. Contraceptive values and preferences of adolescents and young adults: a systematic review. Contraception. 2022;111:22–31. 10.1016/j.contraception.2021.05.018 [DOI] [PubMed] [Google Scholar]
- 38.Daley AM. What influences adolescents’ contraceptive decision-making? A meta-ethnography. J Pediatr Nurs. 2014;29(6):614–32. 10.1016/j.pedn.2014.05.001 [DOI] [PubMed] [Google Scholar]
- 39.Kirubarajan A, Li X, Yau M, Yu C, Got T, Li Q, et al. Awareness, knowledge, and misconceptions of adolescents and young people regarding long-acting reversible contraceptives: a systematic review and meta-analysis. Fertil Steril. 2022;118(1):168–79. 10.1016/j.fertnstert.2022.03.013 [DOI] [PubMed] [Google Scholar]
- 40.Jones A, Allison BA, Perry M. Effectiveness of contraceptive decision aids in adolescents and young adults: a systematic review. J Pediatr Adolesc Gynecol. 2022;35(1):7–17. 10.1016/j.jpag.2021.08.005 [DOI] [PubMed] [Google Scholar]
- 41.Cavallaro FL, Benova L, Owolabi OO, Ali M. A systematic review of the effectiveness of counselling strategies for modern contraceptive methods. what works and what doesn’t?; 2019. [DOI] [PMC free article] [PubMed]
- 42.Goueth RC, Maki KG, Babatunde A, Eden KB, Darney BG. Effects of technology-based contraceptive decision aids: a systematic review and meta-analysis. Am J Obstet Gynecol. 2022. [DOI] [PMC free article] [PubMed]
- 43.Blank L, Baxter SK, Payne N, Guillaume LR, Squires H. Systematic review and narrative synthesis of the effectiveness of contraceptive service interventions for young people, delivered in health care settings. Health Educ Res. 2012;27(6):1102–19. 10.1093/her/cys056 [DOI] [PubMed] [Google Scholar]
- 44.Walker S, Piercy H, Shearn K, Acton F. What consultation resources are available to support delivery of integrated sexual and reproductive health services? A scoping review. BMJ Sex Reproductive Health. 2020;46(2):88–99. 10.1136/bmjsrh-2019-200414 [DOI] [PubMed] [Google Scholar]
- 45.Dehlendorf C, Fitzpatrick J, Fox E, Holt K, Vittinghoff E, Reed R, et al. Cluster randomized trial of a patient-centered contraceptive decision support tool. My Birth Control Am J Obstet Gynecol. 2019;220(6):565..e1-.e12. [DOI] [PubMed] [Google Scholar]
- 46.Manlove J, Cook E, Whitfield B, Johnson M, Martínez-García G, Garrido M. Short-term impacts of pulse: an app-based Teen Pregnancy Prevention Program for Black and Latinx women. J Adolesc Health. 2020;66(2):224–32. 10.1016/j.jadohealth.2019.08.017 [DOI] [PubMed] [Google Scholar]
- 47.Manlove J, Whitfield B, Finocharo J, Cook E. Lessons learned from replicating a Randomized Control Trial evaluation of an app-based sexual Health Program. Int J Environ Res Public Health. 2021;18(6). [DOI] [PMC free article] [PubMed]
- 48.Chewning B, Mosena P, Wilson D, Erdman H, Potthoff S, Murphy A, Kuhnen KK. Evaluation of a computerized contraceptive decision aid for adolescent patients. Patient Educ Couns. 1999;38(3):227–39. 10.1016/S0738-3991(99)00014-2 [DOI] [PubMed] [Google Scholar]
- 49.Sridhar A, Friedman S, Grotts JF, Michael B. Effect of theory-based contraception comics on subjective contraceptive knowledge: a pilot study. Contraception. 2019;99(6):368–72. 10.1016/j.contraception.2019.02.010 [DOI] [PubMed] [Google Scholar]
- 50.Antonishak J, Kaye K, Swiader L. Impact of an online birth control support network on unintended pregnancy. Social Mark Q. 2015;21(1):23–36. 10.1177/1524500414566698 [DOI] [Google Scholar]
- 51.Gilliam ML, Martins SL, Bartlett E, Mistretta SQ, Holl JL. Development and testing of an iOS waiting room app for contraceptive counseling in a title X family planning clinic. Am J Obstet Gynecol. 2014;211(5):e4811–8. 10.1016/j.ajog.2014.05.034 [DOI] [PubMed] [Google Scholar]
- 52.Tebb KP, Rodriguez F, Pollack LM, Adams S, Rico R, Renteria R, et al. Improving contraceptive use among Latina adolescents: a cluster-randomized controlled trial evaluating an mHealth application, Health-E You/Salud iTu. Contraception. 2021;104(3):246–53. 10.1016/j.contraception.2021.03.004 [DOI] [PubMed] [Google Scholar]
- 53.Marshall C, Nuru-Jeter A, Guendelman S, Mauldon J, Raine-Bennett T. Patient perceptions of a decision support tool to assist with young women’s contraceptive choice. Patient Educ Couns. 2017;100(2):343–8. 10.1016/j.pec.2016.08.022 [DOI] [PubMed] [Google Scholar]
- 54.Mesheriakova VV, Tebb KP. Effect of an Ipad-based intervention to improve sexual health knowledge and intentions for contraceptive Use among adolescent females at School-Based Health centers. Clin Pediatr (Phila). 2017;56(13):1227–34. 10.1177/0009922816681135 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Hebert LE, Hill BJ, Quinn M, Holl JL, Whitaker AK, Gilliam ML. Mobile contraceptive application use in a clinical setting in addition to standard contraceptive counseling: a randomized controlled trial. Contraception. 2018;98(4):281–7. 10.1016/j.contraception.2018.07.001 [DOI] [PubMed] [Google Scholar]
- 56.Rea S, Zynda A, Allison B, Tolleson-Rinehart S. Adolescent perceptions of Technology-Based Sexual and Reproductive Health Services: a systematic review. J Adolesc Health. 2022;71(5):533–44. 10.1016/j.jadohealth.2022.05.012 [DOI] [PubMed] [Google Scholar]
- 57.Hsia JK, Creinin MD. Intrauterine contraception. Semin Reprod Med. 2016;34(3):175–82. 10.1055/s-0036-1571438 [DOI] [PubMed] [Google Scholar]
- 58.Vitale SG, Di Spiezio Sardo A, Riemma G, De Franciscis P, Alonso Pacheco L, Carugno J. In-office hysteroscopic removal of retained or fragmented intrauterine device without anesthesia: a cross-sectional analysis of an international survey. Updates Surg. 2022;74(3):1079–85. 10.1007/s13304-022-01246-0 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Keij SM, Lie HC, Laidsaar-Powell R, Kunneman M, de Boer JE, Moaddine S, et al. Patient-related characteristics considered to affect patient involvement in shared decision making about treatment: a scoping review of the qualitative literature. Patient Educ Couns. 2023;111:107677. 10.1016/j.pec.2023.107677 [DOI] [PubMed] [Google Scholar]
- 60.Stacey D. Cochrane Review of Patient Decision Aids – 2023 update adds 104 trials. https://www.isdmsociety.org/seminars/: Presentation to the International Shared Decision-Making Society,; 2023, Jun 7.
- 61.Jull J, Köpke S, Smith M, Carley M, Finderup J, Rahn AC, et al. Decision coaching for people making healthcare decisions. Cochrane Database Syst Rev. 2021;11(11):Cd013385. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Shepherd HL, Barratt A, Trevena LJ, McGeechan K, Carey K, Epstein RM, et al. Three questions that patients can ask to improve the quality of information physicians give about treatment options: a cross-over trial. Patient Educ Couns. 2011;84(3):379–85. 10.1016/j.pec.2011.07.022 [DOI] [PubMed] [Google Scholar]
- 63.Sewak A, Yousef M, Deshpande S, Seydel T, Hashemi N. The effectiveness of digital sexual health interventions for young adults: a systematic literature review (2010–2020). Health Promot Int. 2023;38(1). [DOI] [PubMed]
- 64.Wadham E, Green C, Debattista J, Somerset S, Sav A. New digital media interventions for sexual health promotion among young people: a systematic review. Sex Health. 2019;16(2):101–23. [DOI] [PubMed] [Google Scholar]
- 65.D’Amato A, Cascardi E, Etrusco A, Laganà AS, Schonauer LM, Cazzato G et al. Lights and shades of Fertility Preservation in Transgender men patients: a clinical and pathological review. Life (Basel). 2023;13(6). [DOI] [PMC free article] [PubMed]
- 66.Etrusco A, Mikuš M, D’Amato A, Barra F, Planinić P, Goluža T et al. Incretin hormone secretion in women with polycystic ovary syndrome: roles of obesity, insulin sensitivity and treatment with metformin and GLP-1s. Biomedicines. 2024;12(3). [DOI] [PMC free article] [PubMed]
- 67.Boland L, Lawson ML, Graham ID, Légaré F, Dorrance K, Shephard A, Stacey D. Post-training Shared decision making barriers and facilitators for Pediatric Healthcare providers: a mixed-methods study. Acad Pediatr. 2019;19(1):118–29. 10.1016/j.acap.2018.05.010 [DOI] [PubMed] [Google Scholar]
- 68.Légaré F, Ratté S, Gravel K, Graham ID. Barriers and facilitators to implementing shared decision-making in clinical practice: update of a systematic review of health professionals’ perceptions. Patient Educ Couns. 2008;73(3):526–35. 10.1016/j.pec.2008.07.018 [DOI] [PubMed] [Google Scholar]
- 69.Scholl I, LaRussa A, Hahlweg P, Kobrin S, Elwyn G. Organizational- and system-level characteristics that influence implementation of shared decision-making and strategies to address them - a scoping review. Implement Sci. 2018;13(1):40. 10.1186/s13012-018-0731-z [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Stacey D, Lewis KB, Smith M, Carley M, Volk R, Douglas EE, et al. Decision aids for people facing health treatment or screening decisions. Cochrane Database Syst Rev. 2024;1(1):Cd001431. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 71.Joseph-Williams N, Abhyankar P, Boland L, Bravo P, Brenner AT, Brodney S, et al. What works in implementing patient decision aids in routine clinical settings? A Rapid Realist Review and Update from the International patient decision Aid standards collaboration. Med Decis Mak. 2021;41(7):907–37. 10.1177/0272989X20978208 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 72.Stacey D, Suwalska V, Boland L, Lewis KB, Presseau J, Thomson R. Are patient decision aids used in clinical practice after rigorous evaluation? A Survey of Trial authors. Med Decis Mak. 2019;39(7):805–15. 10.1177/0272989X19868193 [DOI] [PubMed] [Google Scholar]
- 73.van der Weijden T, Pieterse AH, Koelewijn-van Loon MS, Knaapen L, Légaré F, Boivin A, et al. How can clinical practice guidelines be adapted to facilitate shared decision making? A qualitative key-informant study. BMJ Qual Saf. 2013;22(10):855–63. 10.1136/bmjqs-2012-001502 [DOI] [PubMed] [Google Scholar]
- 74.The National Institute for Health and Care Excellence. Shared decision making, NICE guideline [NG197] 2021 [2021 Jun 17:[ https://www.nice.org.uk/guidance/ng197. [PubMed]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Data Availability Statement
The datasets used and/or analysed during the current study is available from the corresponding author on reasonable request. Authors have no relevant financial relationships or perceived, potential or real conflicts of interest to disclose.