Chest pain has been a diagnostic problem for centuries. Heberden's superb clinical description of angina pectoris (and other chest pains) still stands, but today's doctors may be no better at diagnosing cardiac pain accurately than their predecessors 60 years ago. Even when a doctor is sure that the pain is non-cardiac, the more inquiring patient often wants a more specific label.
Much of the interest in this subject has arisen from the extensive investigation of patients concerned that their symptoms could be cardiac in origin. Given the associated and inevitable selection bias, there is little objective evidence on which to base practice, but the oesophagus is undoubtedly one of the organs that can generate problematic chest pain.
This article describes the oesophageal disorders responsible, and ways to diagnose them. Psychological factors are often important in patients with chest pain, so that common sense, understanding a patient and his or her problem, and good communication are usually more important than diagnostic tests and powerful drugs.
What does oesophageal pain feel like?
Oesophageal pain has many patterns: it is often described as burning, sometimes as gripping, and it can also be pressing, boring, or stabbing. Usually in the anterior chest, it tends to be felt mainly in the throat or epigastrium and sometimes radiates to the neck, back, or upper arms—all of which may equally apply to cardiac pain. The commonest patterns of cardiac and oesophageal pains are quite different and well recognised, but perhaps 20% of each are much harder to feel confident about.
Mechanisms of oesophageal pain
Discomfort or pain from the oesophagus may arise from irritant stimuli to the mucosa or from mechanical effects on the muscular wall, each with different sets of receptors.
Mucosal stimulation
Atypical chest pain arising from oesophageal mucosal irritation can be imitated by infusing hydrochloric acid into the oesophagus. This causes discomfort in most people eventually, but, for it to be truly acid induced, it must resolve rapidly when perfusion ceases (Bernstein test).
When the level of exposure of the lower oesophagus to acid is measured by a pH probe, two things can be seen. Firstly, atypical chest pain is usually associated with a drop in pH, but many episodes of acid reflux are painless. Secondly, there may be little relation between the amount of acid reflux and the severity and frequency of atypical chest pain. This parallels the longstanding observation that some patients with marked oesophagitis have little or no heartburn.
Other factors must therefore be involved in the threshold for experiencing pain, and these are discussed below.
Mechanical changes
Distension of the oesophagus, by swallowing a large food bolus or experimentally by inflating a balloon in its lumen, will cause pain in most people. However, individuals with recurrent spontaneous chest pain experience pain at much lower inflation volumes, suggesting that they have a “lowered threshold.” Others may have induced distension because they have a high threshold for belching.
Altered motility of the oesophagus (sometimes loosely referred to as “spasm”) can be a cause of chest pain. The rare condition of diffuse oesophageal spasm (seen radiologically as a “corkscrew oesophagus”) is associated with pain, and so is achalasia. Powerful, prolonged contractions can be induced by injection of edrophonium and may cause simultaneous pain, but similar contractions may also be seen in patients without chest pain. When pressures in the oesophagus are monitored continuously for 24 hours, a few patients with recurrent chest pain can be seen to have pain episodes associated with various abnormalities of oesophageal contractions, but this is surprisingly uncommon.
Pain threshold—psychological factors
Patients with other sorts of painful syndromes, such as irritable bowel syndrome or fibromyalgia, also feel pain induced by balloon distension of the oesophagus more readily than people without pain syndromes.
These observations led to the concept of “altered visceral receptor sensitivity.” When such individuals are given standard psychological tests many are found to have greater anxiety, depression, somatisation, neuroticism, or even panic disorder scores than control subjects, and some studies have shown improvement in pain with the use of antidepressants or anxiolytics.
Primary oesophageal motility disorders
Achalasia
Absent distal peristalsis
Abnormal relaxation of lower oesophageal sphincter
Diffuse oesophageal spasm
Simultaneous contractions
Intermittent peristalsis
Hypertensive (“nutcracker”) oesophagus
Increased contraction amplitude (mean >180 mm Hg)
Normal peristalsis
Ineffective oesophageal motility
Contractions of low amplitude or failed and non-transmitted
Moreover, some abnormalities of oesophageal motility— including “non-specific motility disorder” and “nutcracker oesophagus”—can be induced by the unconscious gulping and hyperventilation performed by some anxious individuals. Unfortunately, well intentioned but misguided medical interventions aimed at excluding cardiac disease may worsen this by raising patients' anxiety and medical dependency.
Managing possible oesophageal pain
This can be a difficult problem, complicated by the fact that both oesophageal problems and ischaemic heart disease are relatively common in middle age and can coexist. Diagnosis of one does not exclude the other. However, first ensure that the patient is not taking sumatriptan for migraine; this drug causes chest pain in 3-5% of those taking it.
Sumatriptan causes chest pain in up to 5% of migraineurs
Atypical chest pain associated with heartburn
Patients with atypical chest pain and reflux symptoms need no investigation provided their symptoms respond to advice on diet and weight, stopping use of non-steroidal anti-inflammatory drugs, or to antacids or antisecretory drugs (see previous article). Endoscopy is desirable for anyone with alarm symptoms or a poor response to treatment.
“Pain like angina”
If the pain has elements that suggest a cardiac origin—such as an association with exercise, radiation to neck, jaw, or arms, or the presence of cardiac risk factors (family history, smoking, hypertension, obesity, hypercholesterolaemia, etc)—then the heart must first be investigated with resting and exercise electrocardiograms. If these are normal then the often difficult choice must be made between more invasive cardiac tests (such as coronary angiography, thallium scanning, etc) or oesophageal tests; specialist referral may be indicated, with the choice between cardiologist or gastroenterologist determined by the nature of the pain.
All tests create anxiety in patients and their family, and can lead to medical dependence. This is especially so when tests are “on the heart.” Studies show that, even when oesophageal tests are positive, patients and their family doctors often continue to believe that their pain originates from the heart.
Before referring any patient to a specialist, a general practitioner should have a clear idea of what may be achieved and explain the risks and benefits to the patient. A period of sympathetic and supportive observation may often be the best initial approach. This will not always be successful, and some patients can absorb substantial health resources in visits to doctors, use of drugs, and urgent “false alarm” admissions to coronary care units. Resident junior doctors wishing to consider an oesophageal cause for atypical chest pain should adopt the following approach.
Investigating the oesophagus as a cause of atypical chest pain
Some patterns of symptoms make it likely that chest pain is oesophageal in origin: an association with meals, dysphagia, relief by antacids, associated acid reflux, and a history of heartburn.
If reflux is suggested then an empiric approach may be appropriate. For patients with severe pain or dysphagia, endoscopy is the usual initial investigation (to look for oesophagitis, cancer, or other gastric disease), but a barium swallow (recorded on video by an experienced radiologist well briefed about the symptoms) will give more information about motility problems such as diffuse spasm or achalasia.
A “therapeutic trial” with high dose proton pump inhibitors (double healing doses) is an alternative approach with the attraction of simplicity, and if the pain disappears promptly and completely it is highly likely that reflux is the cause of the pain. However, it is important to remember that a misleading “placebo response” is common, particularly in anxious patients, and it is always an error to continue such drugs if the symptomatic response is only partial.
If endoscopy or barium swallow fail to confirm the diagnosis 24 hour pH monitoring is necessary to detect any abnormal acid reflux as the most likely treatable cause of “spasm.” If there is no abnormal reflux, and the pain continues as a significant problem, further tests are available to detect an oesophageal origin, although the treatment is far from effective.
Oesophageal manometry
Stationary—This may show subtle motility abnormalities not revealed by radiology, but all too often it shows only “non-specific” motility disorders, which are often clinically irrelevant.
Ambulatory—This is relatively simple for patients but involves complex technology in obtaining the records and analysing them. It can, however, be useful in patients with intractable problems, revealing abnormalities such as intermittent spasm and their association with episodes of pain, especially in patients with intermittent dysphagia.
Oesophageal provocation tests
Pharmacological—Edrophonium can be injected during stationary oesophageal manometry to provoke abnormal contractions and pain that patients can compare with their spontaneous symptoms. However, abnormal contractions can occur in normal individuals, and patients may anticipate symptoms.
Chemical—Acid perfusion of the oesophagus can similarly reveal recognisable pain.
Mechanical—Balloon distension may show both an increased sensitivity to pain and that the pain is indeed oesophageal.
Treatment
The most important aspect of treating oesophageal pain is a sympathetic appraisal of patients' problems. Are they mainly worried about their heart or does their pain interfere with life in some other way, or is their family most concerned?
Treatments for oesophageal spasm
Reflux
Antisecretory drugs
Anxiety or depression
Explanation and reassurance
Psychotherapy
Anxiolytics
Tricyclic antidepressants
Achalasia
Balloon dilatation
Cardiomyotomy
Botulinum toxin
Other spasm disorders
Nitrites
Calcium channel blockers
Possibly balloon dilatation
Any reflux element is readily treated by the range of safe antisecretory drugs of different levels of power; “titrating upwards” is the best way to use them. If response seems inexplicably inadequate, pH monitoring while taking the drug can help.
Psychological problems need considerate management with both drugs and psychotherapy as appropriate. Tricyclic antidepressants (such as amitriptyline 25-75 mg at night) may be particularly useful because of their known value in functional somatic pain disorders such as irritable bowel syndrome.
When a true spasm disorder is demonstrated by manometry, physical treatment may have a place. Achalasia (and sometimes diffuse spasm) may be helped by judicious balloon dilatation of the gastro-oesophageal sphincter, but this carries the risk of perforation or subsequent gastro-oesophageal reflux. There are reports (all uncontrolled) of use of long oesophagomyotomy, but this is an invasive approach for a relatively benign disorder.
Nitrates and calcium channel blocking drugs can be tried— taken sublingually for episodes of pain or orally and regularly as a prophylactic. Separating useful effects from placebo ones is not easy, and these drugs have not been proved in randomised clinical trials. They have two disadvantages, however. One is that patients, reassured they do not have angina, may have their confidence undermined when they read the datasheet and realise they are taking antianginal drugs. The other is that any latent reflux may be accentuated.
Anticholinergic drugs (the traditional “antispasmodics”) have no useful effect, and it is illogical to prescribe metoclopramide or other prokinetic agents.
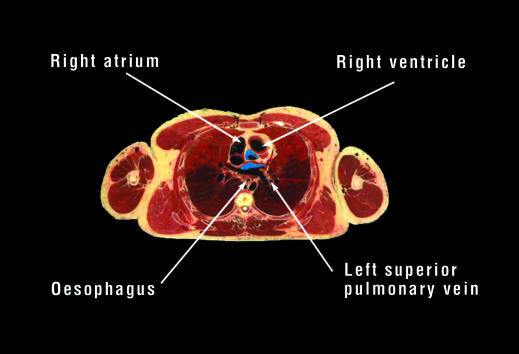
Figure.
The close proximity of the heart and oesophagus mean that distinguishing oesophageal from cardiac pain is often difficult
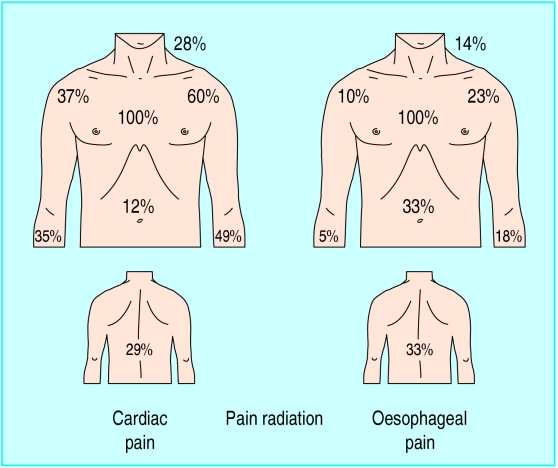
Figure.
Frequency of pain experienced in different anatomical sites by patients with cardiac pain and oesophageal pain
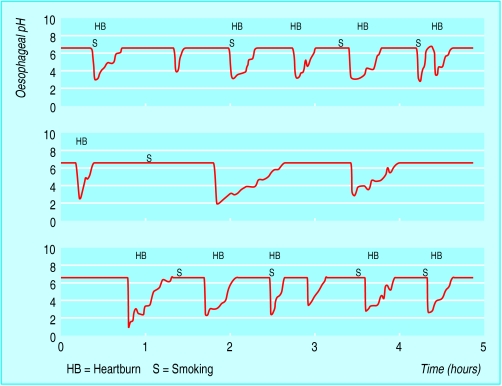
Figure.
Intraoesophageal pH tracing showing frequent episodes of acid reflux, some of them associated with heartburn
Figure.
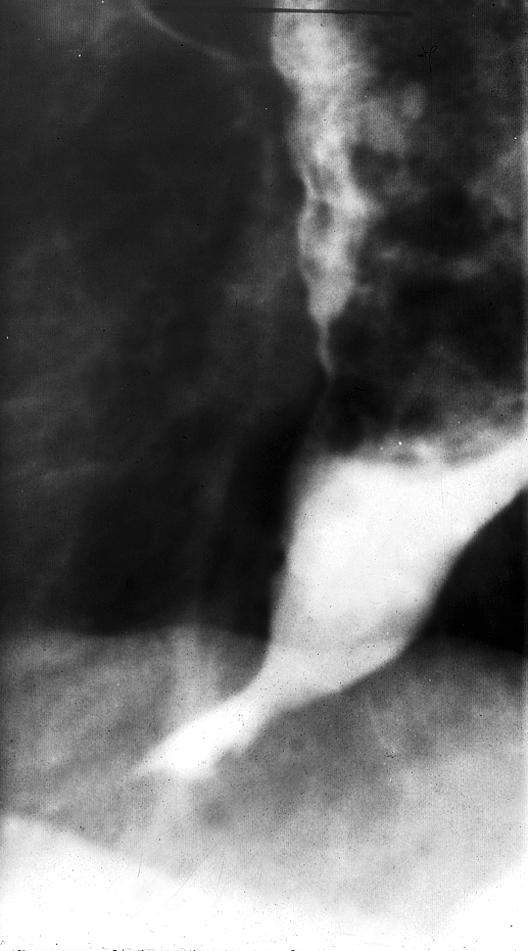
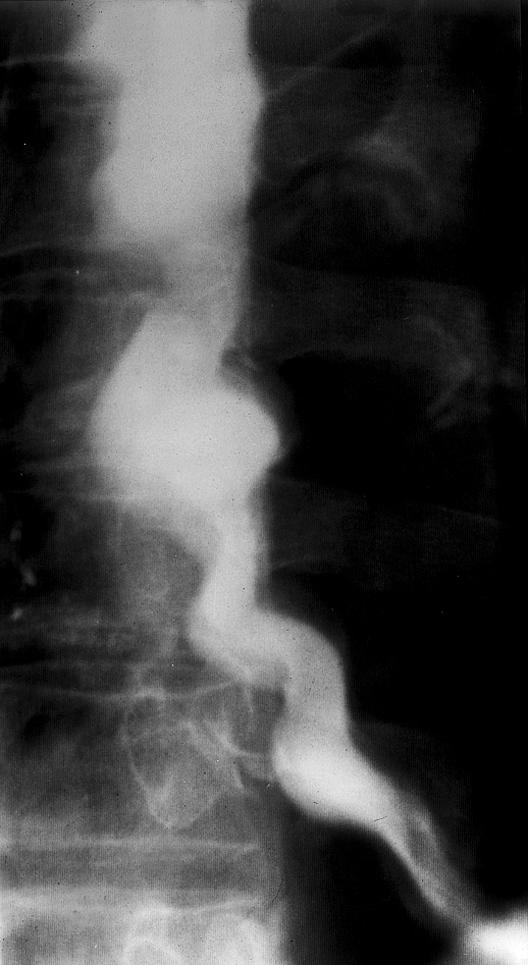
Barium swallow radiographs showing achalasia (left) and diffuse oesophageal spasm (“corkscrew oesophagus”) (right)
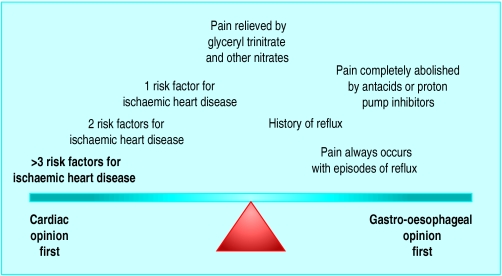
Figure.
Choices for proceeding with patients with chest pain and normal electrocardiograms
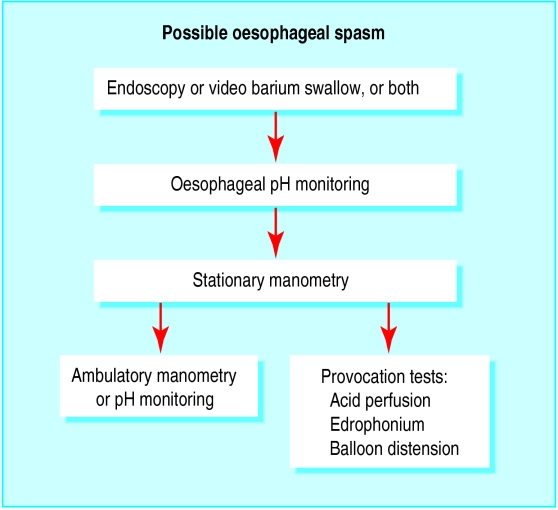
Figure.
Progression of tests for investigating the oesophagus as a cause of chest pain
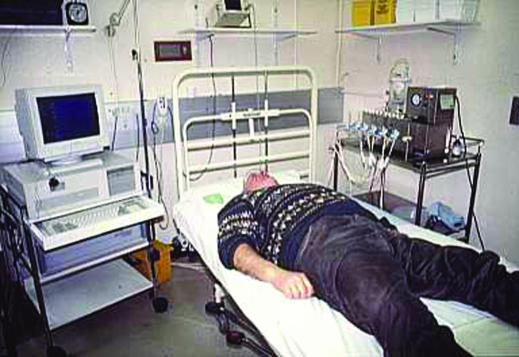
Figure.
Stationary oesophageal manometry is an outpatient procedure taking about 30 minutes to perform. A polyvinyl tube about 4 mm in diameter is passed pernasally after topical anaesthesia. The tube consists of several microcapillary tubes connected to external pressure transducers, which pass signals to a computer for real time display. Measurements of distal oseophageal pressure are taken during swallows of water while the tube is slowly withdrawn from the stomach
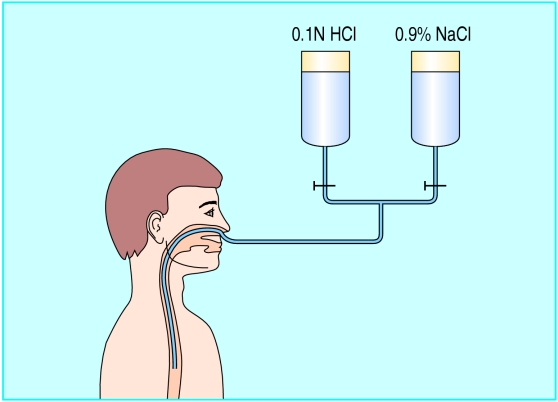
Figure.
The acid perfusion test for chemical provocation of the oesophagus
Acknowledgments
The cross sectional view of a human torso is adapted from the Visible Human Project. The list of primary oesophageal motility disorders is adapted from Richter JE. Lancet 2001;358:823-8.
Footnotes
John Bennett is treasurer at the Royal College of Physicians, London.
The ABC of upper gastrointestinal tract is edited by Robert Logan, senior lecturer in the division of gastroenterology, University Hospital, Nottingham, Adam Harris, consultant physician and gastroenterologist, Kent and Sussex Hospital, Tunbridge Wells, J J Misiewicz, honorary consultant physician and honorary joint director of the department of gastroenterology and nutrition, Central Middlesex Hospital, London, and J H Baron, honorary professorial lecturer at Mount Sinai School of Medicine, New York, USA, and former consultant gastroenterologist, St Mary's Hospital, London. The series will be published as a book in Spring 2002.