Abstract
Background
This study aimed to investigate the relationship between 3-dimensional (3D) alignment and postoperative bone mineral density (BMD) changes with Accolade II tapered wedge stems, which have a different proximal shape from other tapered wedge stems, up to 5 years after primary total hip arthroplasty.
Methods
We retrospectively analyzed the hips of 89 patients who underwent total hip arthroplasty using the second-generation proximally coated cementless stem (Accolade II; Stryker Orthopedics, Mahwah, NJ) at our institution from 2014 to 2018 over a 5-year follow-up. We evaluated the relationship between stem alignment, measured using 3D-templating software, and BMD changes in the 7 Gruen zones and compared the data with those from a former study using other short taper-wedge stems.
Results
BMDs in zones 1 and 7 continued to decrease gradually every year after surgery, and BMD in zone 7 showed the largest decrease (21%) from baseline over 5 years. No correlation was found between stem alignment (varus/valgus, flexion/extension, and anteversion/retroversion) and changes in BMD in each zone over 5 years.
Conclusions
Our data showed no correlation between 3D stem alignment and changes in BMD in each Gruen zone over 5 years. This suggests that the Accolade II stem may fit better into any shape of the proximal medullary canal because of its unique characteristics.
Keywords: Bone mineral density, Total hip arthroplasty, Stem alignment, Tapered wedge cementless stem
Introduction
Taper-wedge cementless stems have a long history, and good long-term (>20 years) results have been reported. Additionally, short taper-wedge stems have advantages including preserving bone stock, resisting stress shielding, and promoting periprosthetic bone formation, and they are suitable for minimally invasive total hip arthroplasty (THA) [[1], [2], [3], [4], [5], [6], [7], [8], [9], [10]].
The design of the stems can be a contributing factor in the decrease of bone mineral density (BMD), which results in postoperative aseptic loosening, stem subsidence, and periprosthetic fractures [11]. However, the proximal shape of each short taper-wedge stem is slightly different. The size of the conventional stem increases outward and the medial curve remains the same as the size increases; conversely, with the second-generation proximally coated cementless stem, Accolade II (Stryker Orthopedics, Mahwah, NJ), the medial curve gradually changes as the stem size becomes bigger, for better adaptation of the femoral canal shape thanks to a more anthropomorphic dimension ratio between its proximal and distal portions and to the variation in size of the radius of curvature of its medial side [12].
Not only the stem shape but also stem alignment affect stress shielding, aseptic loosening, or postoperative BMD [13,14]. A finite element method study reported that stress distribution in periprosthetic bone was dependent on stem alignment [15]. We have previously reported 3-dimensional (3D) stem alignment and BMD changes of 7 Gruen zones [16] with the conventional taper-wedge stem (Tri-Lock BPS; DePuy Synthes, Raynham, MA) up to 5 years postoperatively [14]. In that study, significant negative correlations between varus insertion and a decrease in BMD in zone 7 and between flexed insertion and decreases in BMD in zones 2, 3, and 4 were observed 5 years postoperatively.
The purpose of the present study was to (1) investigate the relationship between 3D alignment and postoperative BMD changes with Accolade II taper-wedge stems, which have a different proximal medial shape from other tapered wedge stems, up to 5 years after primary THA, and (2) discuss the difference between Accolade II and the other types of taper-wedge stems we have previously investigated.
Material and methods
Ethics statements
This study was approved by the institutional review board of our institution. The requirement for informed consent was waived because of the retrospective nature of the study. After approval, the patients’ medical records and radiologic data were retrospectively evaluated.
Study design and population
In this retrospective single-center cohort, we analyzed 115 hips of selected patients who had undergone THA using short taper-wedge cementless stems (Accolade II) at our institution between April 2014 and April 2018, with at least 5-year follow-up data. We performed THA by using only 2 stems (Tri-Lock BPS and Accolade II) randomly. In this study, only patients who had been followed up for at least 5 years and had available clinical and radiological data were included (K.I.). Eligible patients included those who had undergone primary THA performed by a single surgeon. The inclusion criterion was osteoarthritis (caused by primary osteoarthritis, developmental dysplasia of the hip, or idiopathic osteonecrosis of the femoral head) without prior hip surgery. The exclusion criteria were ipsilateral surgical history, THA for femoral neck fracture, and an inadequate follow-up period. Consequently, 89 hips from 89 patients (65 women and 24 men) were analyzed.
Data were retrieved from patients’ electronic medical records. THA was performed via the modified Watson-Jones approach in the lateral position by a single experienced surgeon. Cancellous bone removal in zone 7 was not performed, and conventional rasps, instead of compactors, were used during the femur-rasping procedure.
Outcome measurements
We evaluated the clinical results by comparing the preoperative Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC) score with the scores recorded at 3 months and at 1, 2, 3, 4, and 5 years after surgery. Occurrences of dislocations, infections, loosening, and all complications requiring revision arthroplasty were documented.
We further evaluated radiological outcomes based on the preoperative intramedullary canal shape (stovepipe-shaped, champagne flute-shaped, or standard shape) and results of computed tomography (from the pelvis to the femur) in the supine position before surgery and 3 months postoperatively, as previously reported [14].
All preoperative planning and postoperative evaluations of stem alignment had been completed using the computed tomography-based 3D templating software (LEXI, Tokyo, Japan), as previously reported [14]. The definitions of the femoral axis, varus or valgus, and flexion or extension axis used were previously reported [14]. The coordinate system recommended by the International Society of Biomechanics included 3 points: the center of the femoral head and the medial and lateral condyles of the femur. Anteversion was defined as the angle between the stem and the International Society of Biomechanics coordinate plane.
BMD around the stem was measured using dual-energy X-ray absorptiometry at 3 weeks (as a baseline), 3 months, and 1, 2, 3, and 5 years after surgery. The BMD changes in the Gruen zones [16] were calculated by the percentage change from baseline. Based on BMD at 3 weeks, we evaluated the correlation between stem alignment, measured using 3D templating software, and postoperative BMD changes in the 7 Gruen zones at 1, 2, 3, and 5 years.
Statistical analysis
Continuous variables are presented as means (ranges), whereas categorical variables are presented as absolute frequencies and percentages. The Mann-Whitney U test was used to compare the WOMAC scores and BMD changes between male and female patients. Bonferroni correction was used to account for the fact that there were multiple comparisons of BMD changes between male and female patients. The Spearman coefficient was used to analyze the relationship between postoperative stem alignment (flexion-extension, varus-valgus, and anteversion-retroversion) and changes in BMD levels in the 7 Gruen zones. Statistical significance was set at P < .05. Statistical analyses were performed using IBM SPSS Statistics for Windows (version 26.0; IBM Corp., Armonk, NY).
Results
Patients’ mean age at surgery, body mass index, and follow-up period were 67.9 (44-86) years, 23.8 (15.3-36.6) kg/m2, and 74.2 (60-108) months, respectively. The baseline BMD was significantly lower in females in each Gruen zone. In all 89 patients, the intramedullary canals were stovepipe-shaped in 6 hips, champagne flute-shaped in 18 hips, and standard in the other 65 hips.
The mean WOMAC score improved significantly from 43.2 (13-87) points preoperatively to 6.4 (0-40) points at 1 year postoperatively (P < .001); however, there were no significant differences between the scores at 1 and 5 years postoperatively (P = .817). No dislocation, infection, aseptic loosening, or other complications requiring a revision arthroplasty were observed.
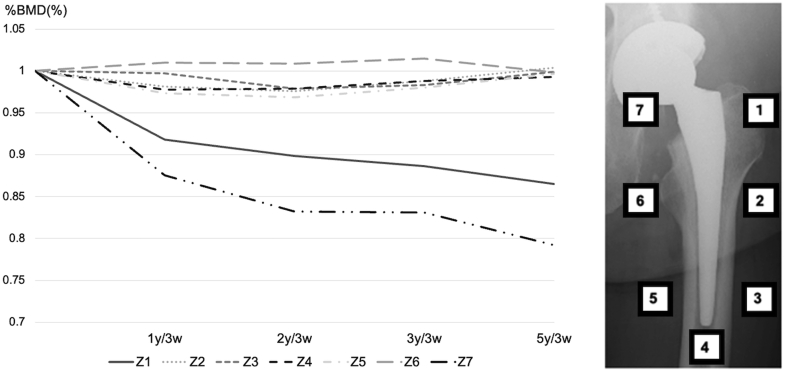
BMD in zone 7 showed the largest decrease from baseline over 5 years (3 months, 4%; 1 year, 13%; 2 years, 17%; 3 years, 17%; and 5 years, 21%). BMDs in zones 1 and 7 continued to decrease gradually every year after surgery (Table 1, Fig. 1). There were no differences in BMD change rates by gender except for Zone 1 at 5 years; females had significantly lower BMD than males. No correlation was found between stem alignment (varus/valgus, flexion/extension, and anteversion/retroversion) and changes in BMD in each zone over 5 years (Table 2).
Table 1.
BMD changes in the Gruen zones.
| Zone | 1 Y | 2 Y | 3 Y | 5 Y |
|---|---|---|---|---|
| Zone 1 | ||||
| All patients | 0.92 | 0.90 | 0.89 | 0.87 |
| Male | 0.89 | 0.96 | 0.92 | 0.91 |
| Female | 0.91 | 0.89 | 0.87 | 0.86 |
| P-value | .93 | .06 | .24 | .02 |
| Zone 2 | ||||
| All patients | 0.98 | 0.98 | 0.99 | 1.00 |
| Male | 1.00 | 1.00 | 1.00 | 1.02 |
| Female | 0.97 | 0.97 | 0.98 | 1.00 |
| P-value | .13 | .13 | .37 | .46 |
| Zone 3 | ||||
| All patients | 1.00 | 0.98 | 0.98 | 1.00 |
| Male | 1.00 | 1.00 | 0.96 | 1.00 |
| Female | 0.99 | 0.97 | 0.98 | 1.00 |
| P-value | .46 | .95 | .46 | .18 |
| Zone 4 | ||||
| All patients | 0.98 | 0.98 | 0.99 | 0.99 |
| Male | 0.94 | 0.98 | 0.98 | 1.01 |
| Female | 0.98 | 0.98 | 0.99 | 0.99 |
| P-value | .89 | .85 | .46 | .28 |
| Zone 5 | ||||
| All patients | 0.97 | 0.97 | 0.98 | 1.00 |
| Male | 0.96 | 0,98 | 0.96 | 0.99 |
| Female | 0.98 | 0.97 | 0.98 | 1.00 |
| P-value | .49 | .16 | .62 | .78 |
| Zone 6 | ||||
| All patients | 1.01 | 1.01 | 1.01 | 1.00 |
| Male | 1.02 | 1.04 | 1.05 | 1.04 |
| Female | 1.01 | 1.00 | 1.01 | 0.99 |
| P-value | .33 | .24 | .36 | .17 |
| Zone 7 | ||||
| All patients | 0.88 | 0.83 | 0.83 | 0.79 |
| Male | 0.91 | 0.87 | 0.88 | 0.86 |
| Female | 0.87 | 0.83 | 0.82 | 0.78 |
| P-value | .76 | .10 | .17 | .10 |
The Mann-Whitney U test and Bonferroni correction were applied to compare the BMD changes in male and female patients. None of the statistical tests reached significance.
Values showing significant differences (P < .05) are shown in bold.
Figure 1.
Changes in BMD in each Gruen zone. Changes in BMD in zones 1 and 7 gradually decreased over time, and those in zone 3 were >100% at 5 years postoperatively. BMD, bone mineral density; Z, zone.
Table 2.
Correlation between 3D stem alignment and BMD changes in the Gruen zone.
| Alignment | Zone 1 | Zone 2 | Zone 3 | Zone 4 | Zone 5 | Zone 6 | Zone 7 |
|---|---|---|---|---|---|---|---|
| Varus | |||||||
| 1 y | |||||||
| correlation | 0.052 | −0.115 | −0.196 | 0.073 | −0.077 | −0.093 | 0.112 |
| P-value | .648 | .302 | 0.08 | .516 | .494 | .417 | .32 |
| 2 y | |||||||
| correlation | 0.102 | −0.161 | −0.039 | 0.221 | 0.152 | −0.033 | 0.054 |
| P-value | .375 | .153 | .734 | .054 | .186 | .774 | .641 |
| 3 y | |||||||
| correlation | 0.158 | −0.073 | −0.189 | −0.13 | −0.013 | 0.033 | 0.11 |
| P-value | .188 | .547 | .115 | .279 | .917 | .786 | .362 |
| 5 y | |||||||
| correlation | 0.047 | −0.148 | −0.138 | −0.028 | −0.129 | 0.171 | 0.179 |
| P-value | .698 | .225 | .257 | .817 | .291 | .16 | .141 |
| flexion | |||||||
| 1 y | |||||||
| correlation | 0.041 | −0.06 | −0.054 | 0.017 | 0.029 | 0.079 | 0.137 |
| P-value | .713 | .959 | .635 | .881 | .794 | .487 | .221 |
| 2 y | |||||||
| correlation | −0.147 | 0.04 | 0.021 | 0.043 | 0.082 | 0.195 | 0.185 |
| P-value | .688 | .722 | .858 | .709 | .48 | .089 | .107 |
| 3 y | |||||||
| correlation | 0.048 | −95 | 0.047 | −0.034 | 0.101 | 0.064 | 0.099 |
| P-value | .693 | .431 | .695 | .778 | 0.4 | .596 | .41 |
| 5 y | |||||||
| correlation | 0.207 | 0.042 | −0.61 | −0.042 | 0.092 | 0.189 | 0.176 |
| P-value | .086 | .735 | .621 | .729 | .453 | .12 | .147 |
| Anteversion | |||||||
| 1 y | |||||||
| correlation | 0.009 | 0.083 | −0.56 | −0.52 | −0.114 | −0.035 | 0.019 |
| P-value | .468 | .458 | .619 | .642 | .312 | .759 | .869 |
| 2 y | |||||||
| correlation | 0.113 | −0.152 | 0.032 | 0.089 | 0.065 | −0.2 | −0.212 |
| P-value | .165 | .174 | .785 | .442 | .573 | .082 | .064 |
| 3 y | |||||||
| correlation | 0.156 | 0.063 | 0.137 | 0.108 | 0.059 | −0.125 | −0.091 |
| P-value | .194 | .6 | .256 | .372 | .628 | .297 | .452 |
| 5 y | |||||||
| correlation | 0.057 | 0.076 | 0.121 | 0.119 | 0.085 | −0.022 | 0.038 |
| P-value | .64 | .536 | .321 | .332 | .485 | .859 | .757 |
The Spearman coefficient was used to analyze the correlation between 3D stem alignment and BMD changes.
P < .05 was considered statistically significant.
Discussion
In this study, BMD decreased most significantly in Gruen zone 7 at all postoperative follow-up points. This tendency has been reported by some researchers about many kinds of cementless stems [[17], [18], [19], [20]]. Inaba et al. [17] investigated the periprosthetic BMD changes in 3 types of stems (ie, fit-and-fill type stems, Zweymüller type stems, and short taper-wedge type stems) and similarly found the largest BMD decrease in zone 7 in all stem types at 3 years postoperatively. They reported that short taper-wedge stems showed a BMD loss of approximately 20% compared with 30% fit-and-fill and Zweymüller type stems in zone 7. With Accolade II, which has a different shape from other short taper-wedge stems, BMD loss was 17% in zone 7 at 3 years after surgery. This suggests that these stems result in lower BMD loss than fit-and-fill and Zweymüller-type stems in zone 7. We also reported that BMD decreased with other taper-wedge stems (Tri-Lock BPS; DePuy Synthes) at 5 years postoperatively. BMD loss in zone 7 at 5 years was approximately 31% for Tri-Lock BPS, compared with 21% for Accolade II. [14] This suggests that the different shape of Accolade II reduces stress shielding more strongly than traditional short taper-wedge stems do, although the short taper-wedge stem was originally designed to resist stress shielding.
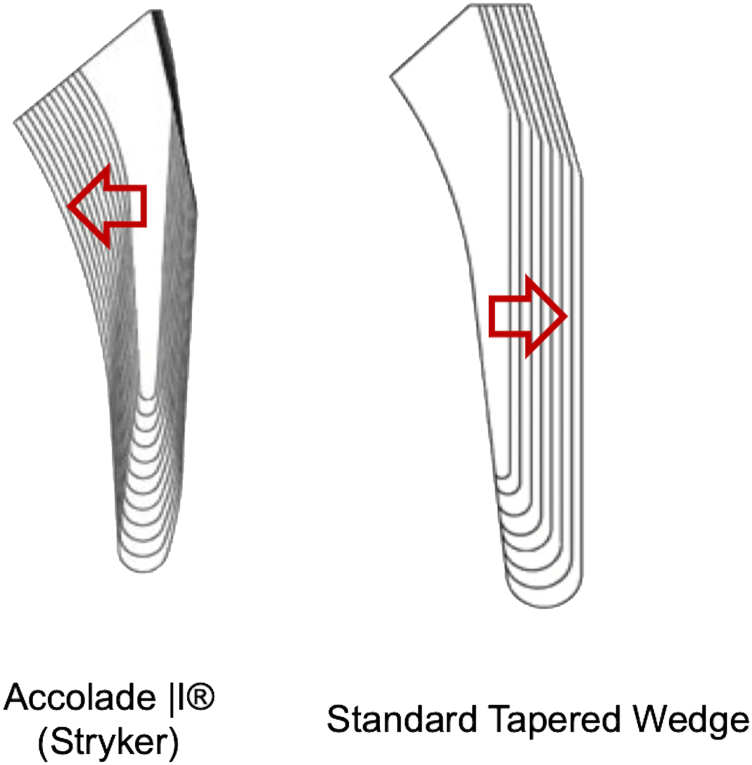
Moreover, we previously reported significant negative correlations between varus insertion and a decrease in BMD in zone 7 and between flexed insertion and decreases in BMD in zones 3 and 4 at 1 year. At 5 years in the present study, significant negative correlations were observed between varus insertion and a decrease in BMD in zone 7 and between flexed insertion and decreases in BMD in zones 2, 3, and 4. With increased varus/flexion stem alignment, BMD loss decreased. However, in this study, no correlation was found between stem alignment and changes in BMD in each zone over 5 years. This suggests that Accolade II may fit better into any shape of the proximal medullary canal because of its unique characteristics; the medial wedge angle decreases as the stem size increases (Fig. 2). Consequently, BMD in zones 1 and 7 was equally decreased compared to the remarkably decreased BMD in zone 7 for the conventional taper-wedge stem. Even if the stem was inserted in flexion, as the distal cortical bone in zones 2 and 3 is less loaded, we assumed that bone density at 5 years may not be affected by the stem alignment of Accolade II.
Figure 2.
Difference of the proximal medial shape between Accolade II and a standard taper-wedge stem.
Generally, femoral BMD in each Gruen zone of female patients was lower than the male’s. Liu et al. [21] reported that female patients older than 50 years lost significantly more BMD than male patients or patients younger than 50 years. In addition, female patients showed significantly more serious stress shielding than male patients. In our study, there were no differences in BMD change rates by gender except for Zone 1 at 5 years, but BMD baseline was lower in females and BMD decrease rates in zone 2-7 of female patients were bigger than male patients; it’s not statistically significant.
In this study, 6 hips were stovepipe-shaped, 18 hips were champagne flute-shaped, and 65 hips were standard. Some research has reported that there are more champagne flute-shaped hips than stovepipe-shaped hips in the Asian population [3,22,23]. Liu et al. [22] reported that the proportion of champagne flute-shaped hips was significantly larger in the Chinese population, whereas the proportion of standard hips was significantly smaller in the Western population. Umer et al. [3] found that in a Pakistani population, 67% of individuals had standard hips, whereas 1% and 33% of them had stovepipe-shaped and champagne flute-shaped hips, respectively. We assumed that Accolade II fit more champagne flute-shaped hips than stovepipe-shaped hips. In this study, we did not compare each BMD change and 3D stem alignment of the medullary canal shape because the number of stovepipe-shaped hips was too small.
There are some limitations to this study. First, only a single surgeon performed all operations, so the stem alignment may reflect the surgeon’s preference. However, the correlation between stem alignment and BMD was not affected by the surgical technique, so the outcome does not lose its generality. Second, we evaluated BMD only in the anteroposterior plane. If the sagittal plane was also evaluated, flexed or extended stem insertion might have influenced postoperative BMD. Third, this study had a retrospective study design, and 26 patients were excluded because complete data were unavailable, which introduced significant selection bias. Forth, a surgeon randomly selected the stem with his preference. So, we couldn’t rule out the possibility of selection bias. Sixth, overrepresentation of females may have influenced the results of this study, even though there were no complications related to BMD decrease or statistical significance in terms of gender, except for zone 1 at 5 years. Finally, the number of hips analyzed was small in this study; therefore, we were unable to analyze the relationship between stem size and periprosthetic BMD. Despite these limitations, we believe that these results showed the potential of 3D templating software to define the relationship between stem alignment and changes in BMD around the stem, which can be helpful after THA.
Conclusions
Accolade II, with its unique characteristic of the medial wedge angle decreasing as the stem size increases, may be less likely to affect BMD around the stem regardless of its 3D alignment and reduce stress shielding over 5 years after THA. When THA is performed with Accolade II, there may be less need to be strict about stem alignment in terms of postoperative BMD changes. In the future, a prospective randomized controlled trial should be conducted, and comparing the results for each medullary cavity shape would clarify the indication of Accolade II.
Acknowledgments
We thank Yoshito Minami, Koji Mandai, Yuuki Shibata and Takashi Fujii for the assistants of the orthopaedic surgery in Shiraniwa Hospital.
Conflicts of interest
The authors declare there are no conflicts of interest.
For full disclosure statements refer to https://doi.org/10.1016/j.artd.2024.101433.
CRediT authorship contribution statement
Masashi Tsujino: Writing – original draft, Data curation. Kentaro Iwakiri: Supervision, Project administration. Yoichi Ohta: Writing – review & editing. Yukihide Minoda: Writing – review & editing. Akio Kobayashi: Formal analysis. Hiroaki Nakamura: Supervision.
Appendix A. Supplementary Data
References
- 1.Wacha H., Domsel G., Herrmann E. Long-term follow-up of 1217 consecutive short-stem total hip arthroplasty (THA): a retrospective single center experience. Eur J Trauma Emerg Surg. 2018;44:457–469. doi: 10.1007/s00068-017-0895-2. [DOI] [PubMed] [Google Scholar]
- 2.Ulivi M., Orlandini L.C., Meroni V., Lombardo M.D.M., Peretti G.M. Clinical performance, patient reported outcome, and radiological results of a short, tapered, porous, proximally coated cementless femoral stem results up to seven years of follow-up. J Arthroplasty. 2018;33:1133–1138. doi: 10.1016/j.arth.2017.11.046. [DOI] [PubMed] [Google Scholar]
- 3.Kaku N., Pramudita J.A., Yamamoto K., Tsumura H. Stress distributions of the short stem and the tapered wedge stem at different alignments: a finite element analysis study. J Orthop Surg Res. 2022;17:530. doi: 10.1186/s13018-022-03425-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Uçan V., Ezici V., Aliyev O., Uzer G., Tuncay İ., Yıldız F. Comparison of tapered-wedge short and standard-length femoral stems in single-stage bilateral direct anterior total hip arthroplasty. Int Orthop. 2021;45:3119–3127. doi: 10.1007/s00264-021-05152-9. [DOI] [PubMed] [Google Scholar]
- 5.Kolisek F.R., Chughtai M., Mont M.A. Outcomes of second-generation tapered wedge femoral stem. Surg Technol Int. 2016;28:275–279. [PubMed] [Google Scholar]
- 6.Ferguson R.J., Palmer A.J., Taylor A., Porter M.L., Malchau H., Glyn-Jones S. Hip replacement. Lancet. 2018;392:1662–1671. doi: 10.1016/S0140-6736(18)31777-X. [DOI] [PubMed] [Google Scholar]
- 7.Barrington J.W., Emerson R.H., Jr. The short and “shorter” of it: >1750 tapered titanium stems at 6- to 88-month follow-up. J Arthroplasty. 2013;28:38–40. doi: 10.1016/j.arth.2013.07.032. [DOI] [PubMed] [Google Scholar]
- 8.Zimmerer A., Slouka S., Kinkel S., Fritz T., Weiss S., Sobau C., et al. Comparison of short-stem with conventional-stem prostheses in total hip arthroplasty: an 8-year follow-up study. Arch Orthop Trauma Surg. 2020;140:1285–1291. doi: 10.1007/s00402-020-03519-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Hossain F., Konan S., Volpin A., Haddad F.S. Early performance-based and patient- reported outcomes of a contemporary taper fit bone-conserving short stem femoral component in total hip arthroplasty. Bone Joint J. 2017;99-B:49–55. doi: 10.1302/0301-620X.99B4.BJJ-2016-1291.R1. [DOI] [PubMed] [Google Scholar]
- 10.Albers A., Aoude A.A., Zukor D.J., Huk O.L., Antoniou J., Tanzer M. Favorable results of a short, tapered, highly porous, proximally coated cementless femoral stem at a minimum 4- year follow-up. J Arthroplasty. 2016;31:824–829. doi: 10.1016/j.arth.2015.08.020. [DOI] [PubMed] [Google Scholar]
- 11.Kröger H., Venesmaa P., Jurvelin J., Miettinen H., Suomalainen O., Alhava E., et al. Bone density at the proximal femur after total hip arthroplasty. Clin Orthop Relat Res. 1998;352:66–74. [PubMed] [Google Scholar]
- 12.Issa K., Pivec R., Wuestemann T., Tatevossian T., Nevelos J., Mont M.A. Radiographic fit and fill analysis of a new second- generation proximally coated cementless stem compared to its predicate design. J Arthroplasty. 2014;29:192–198. doi: 10.1016/j.arth.2013.04.029. [DOI] [PubMed] [Google Scholar]
- 13.Hayashi S., Hashimoto S., Kuroda R. Stem anteversion mismatch to the anatomical anteversion causes loss of periprosthetic bone density after THA. J Orthop Surg (Hong Kong) 2017;25 doi: 10.1177/2309499017739478. [DOI] [PubMed] [Google Scholar]
- 14.Masuda S., Iwakiri K., Nakamura H. Stem alignment with short tapered-wedge cementless stems affects bone mineral density continuously for at least 5 years after primary total hip arthroplasty. Hip Int. 2023;34:57–65. doi: 10.1177/11207000231178984. [DOI] [PubMed] [Google Scholar]
- 15.Bah M.T., Nair P.B., Taylor M., Browne M. Efficient computational method for assessing the effects of implant positioning in cementless total hip replacements. J Biomech. 2011;44:1417–1422. doi: 10.1016/j.jbiomech.2010.12.027. [DOI] [PubMed] [Google Scholar]
- 16.Gruen T.A., McNeice G.M., Amstutz H.C. ‘Modes of failure’ of cemented stem-type femoral components: a radiographic analysis of loosening. Clin Orthop Relat Res. 1979;141:17–27. [PubMed] [Google Scholar]
- 17.Inaba Y., Kobayashi N., Metal O., Ike H., Kubota S., Saito T. Difference in postoperative periprosthetic bone mineral density changes between 3 major designs of uncemented stems: a 3-year follow-up study. J Arthroplasty. 2016;31:1836–1841. doi: 10.1016/j.arth.2016.02.009. [DOI] [PubMed] [Google Scholar]
- 18.Sayyidmousavi A., Bougherara H. Investigation of stress shielding around the Stryker Omnifit and Exeter periprosthetic hip implants using an irreversible thermodynamic-based model. J Biomed Mater Res B Appl Biomater. 2012;100:1416–1424. doi: 10.1002/jbm.b.32500. [DOI] [PubMed] [Google Scholar]
- 19.de Waard S., van der Vis J., Haverkamp P.A.H.T., Sierevelt I.N., Kerkhoffs G.M.M.J., Haverkamp D. Short-term success of proximal bone stock preservation in short hip stems: a systematic review of the literature. EFORT Open Rev. 2021;6:1040–1051. doi: 10.1302/2058-5241.6.210030. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Bieger R., Ignatius A., Reichel H., Dürselen L. Biomechanics of a short stem: in vitro primary stability and stress shielding of a conservative cementless hip stem. J Orthop Res. 2013;31:1180–1186. doi: 10.1002/jor.22349. [DOI] [PubMed] [Google Scholar]
- 21.Liu Y., Wei W.X., Shen B. Comparison of femoral bone mineral density changes around 3 common designs of cementless stems after total hip arthroplasty-A retrospective cohort study. Orthop Surg. 2022;14:1059–1070. doi: 10.1111/os.13265. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Pi Y., Zhao Y., Wang W., He Z., Mao X. Measurement of proximal femoral morphology and analysis of 500 cases in Hunan Province. Zhong Nan Da Xue Xue Bao Yi Xue Ban. 2013;38:925–930. doi: 10.3969/j.issn.1672-7347.2013.09.010. [DOI] [PubMed] [Google Scholar]
- 23.Sevil-Kilimci F., Kara M.E. Canal flare index in the canine femur is influenced by the measurement method. Vet Comp Orthop Traumatol. 2020;33:198–204. doi: 10.1055/s-0040-1701501. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.