Abstract
Although both short and long sleep duration are associated with elevated hypertension risk, our understanding of their interplay with biological pathways governing blood pressure remains limited. To address this, we carried out genome-wide cross-population gene-by-short-sleep and long-sleep duration interaction analyses for three blood pressure traits (systolic, diastolic, and pulse pressure) in 811,405 individuals from diverse population groups. We discover 22 novel gene-sleep duration interaction loci for blood pressure, mapped to 23 genes. Investigating these genes’ functional implications shed light on neurological, thyroidal, bone metabolism, and hematopoietic pathways that necessitate future investigation for blood pressure management that caters to sleep health lifestyle. Non-overlap between short sleep (12) and long sleep (10) interactions underscores the plausible nature of distinct influences of both sleep duration extremes in cardiovascular health. Several of our loci are specific towards a particular population background or sex, emphasizing the importance of addressing heterogeneity entangled in gene-environment interactions, when considering precision medicine design approaches for blood pressure management.
INTRODUCTION
Abnormal sleep duration is detrimental to cardiovascular health – increasing the risk of incident cardiovascular disease (CVD) and mortality – and inherently complex, with suspected heterogeneous effects according to sex and race/ethnicity(1, 2). Deviation from healthy sleep can impact diurnal rhythms, hormone levels (e.g. ghrelin, cortisol), autonomous nervous system balance, and even remodel vascular structure - resulting in adverse consequences, such as reduced nocturnal blood pressure (BP) dipping and sustained daytime hypertension(1, 3).
Yet the mechanistic pathways underlying the biomolecular connection between short and long sleep with cardiovascular health remain unclear. Evidence implicates heightened sympathetic tone and metabolic dysfunction in the mechanism of short sleep, but there remains a gap in clarity with the added complexity of interwoven pathways like oxidative stress and endothelial dysfunction(1, 4). The role of long sleep is more elusive, with recent work highlighting the pertinence of inflammatory markers, underlying comorbidity burden (i.e. dyslipidemia, depression) and arterial stiffness metrics(5, 6). This incomplete understanding of the intersection between habitual sleep duration and cardiovascular health necessitates further investigation.
Hypertension is a major risk factor for CVD, with blood pressure traits known to have a strong genetic background. Recent genome-wide association analyses (GWASs) have discovered more than 2,000 loci explaining ~ 40% of systolic or diastolic BP heritability among European descent individuals(7). It is important to investigate the role of sleep health in such a polygenic landscape. This may both explain additional heritability of BP traits, as well as bring to the forefront novel genomic loci that inform perspective on sleep’s influence on biomolecular pathways underlying BP. Moreover, incorporating diverse population groups is essential – as this can reveal novel gene targets specific to particular subgroups or shared across – improving downstream therapeutic designs, and offering tangible insight to counter disparities in health. Our prior work in the Cohorts for Heart and Aging Research in Genomic Epidemiology (CHARGE) Gene-Lifestyle Interactions Working Group highlighted novel non-overlapping gene-sleep interactions for BP, suggesting distinct roles of influence for short and long sleep duration(8). Our current analysis advances the field by including a 12-fold larger sample size and additional sex-stratified analyses, yielding enhanced statistical power and granularity.
MATERIALS AND METHODS
This work was approved by the Institutional Review Board of Washington University in St. Louis and complies with all relevant ethical regulations. For each of the participating cohorts, the appropriate ethics review board approved the data collection and all participants provided informed consent.
Data Harmonization
Data from each cohort (Supplementary Tables S1-S2) were harmonized following this centralized protocol. Data were stratified by population group, based on self-reported ancestry and individual cohort definitions (AFR: African, EAS: East Asian, EUR: European, HIS: Hispanic/Latinos, SAS: South Asian), and sex (combined sex, female sex, male sex). Analyses considered 3 primary blood pressure (BP) traits as outcome variables (SBP: systolic, DBP: diastolic, PP: pulse pressure) and 2 dichotomous lifestyle exposures (LTST: long total sleep time, STST: short total sleep time). Genetic variants (G) were restricted to autosomal chromosomes 1–22 imputation quality≥0.3, and minor allele frequency≥0.1%. Age was restricted to ≥18 years, and reported total sleep time constrained within 3 and 14 hours. In scenarios of multiple visits, the single visit with largest sample size was utilized and in case-control study designs, cases and controls were required to be analyzed separately. For BP outcome measures, if multiple readings were taken in a single visit the mean was used. All BP values were winsorized at 6 standard deviations from the mean. BP values were adjusted for reported use of anti-hypertensive medications as follows: SBP (+ 15 mmHg) and DBP (+ 10 mmHg). PP was derived as SBP – DBP. In the case of studies with known between-sample relatedness, null model residuals (regressing BP traits on a kinship matrix/genetic covariance matrix) were denoted as the BP outcome. STST and LTST were derived from total sleep time (TST) by regressing TST on age, sex, age×sex and using the residuals’ 20th and 80th percentiles as cutoffs (STST = 1 if ≤ 20th percentile, LTST = 1 if ≥ 80th percentile, STST = 0 if > 20th percentile, LTST = 0 if < 80th percentile). Covariates included population-group specific principal components, cohort-specific confounders (study center), age, age2, sex, age×S/LTST, age2×S/LTST, and sex×S/LTST. Samples with missing data were excluded.
Genome-wide Gene-Sleep Interaction Analysis
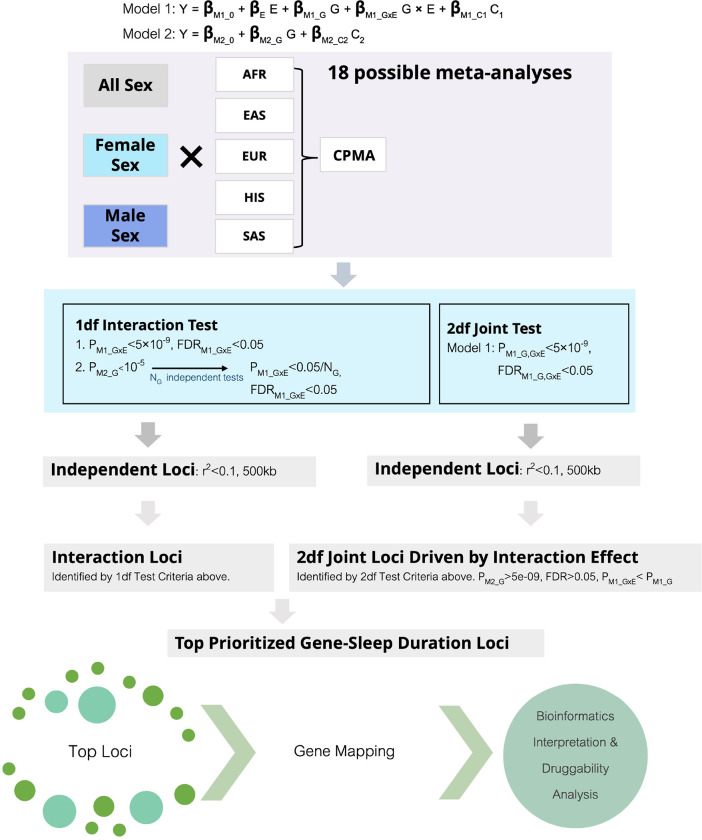
After data harmonization, each population-group specific cohort ran 2 regression models (M1 and M2) for 18 phenotype-exposure-sex combinations (3 phenotypes × 2 exposures × 3 sex groups: combined sex, female sex, male sex). Below E denotes the lifestyle exposure (STST or LTST), Y denotes the BP outcome (SBP, DBP, or PP), C1 denotes the vector of covariates incorporating E (age, age2, S/LTST, age*S/LTST, age2*S/LTST, sex, sex*S/LTST), and C2 denotes the subset without incorporating E (age, age2, sex). Female-specific and male-specific analyses were not adjusted for sex. Specialized software choice included LinGxEScanR v1.0 (https://github.com/USCbiostats/LinGxEScanR), GEM v1.4.1 (https://github.com/large-scale-gxe-methods/GEM), and/or MMAP (latest version available) (https://github.com/MMAP/MMAP.github.io) with robust standard errors (SEs) enforced(9). One degree of freedom (df) tests for the marginal effect (), the main effect (), and the interaction effect () were conducted; alongside the 2df joint test that simultaneously assesses the main effect and the interaction effect (, )(10).
Model 1 (Primary GxE Model of Interest)
| (1) |
Model 2 (Marginal Effect Model for Comparison)
| (2) |
Summary statistics were centrally processed after individual studies submitted results. EasyQC2 software (www.genepi-regensburg.de/easyqc2) was used to perform quality control (QC) on resultant data(11). Data were filtered for degrees of freedom≥20 calculated as minor allele count * imputation quality (e.g. MACxR2 provided by each cohort) within the unexposed, the exposed, and the total sample. Missing or invalid/out of range values for statistics and duplicated or monomorphic variants were discarded. hg19 genomic coordinates were lifted over to hg38 genomic coordinates. Allele frequency discrepancies relative to TOPMed-imputed 1000G reference panels (Trans-Omics for Precision Medicine imputed 1000Genomes) were assessed for each specific population group, along with genomic control (GC) lambda inflation. Meta-level quality control was conducted within groups based on population group, with evaluation of unwanted centering of the outcome variable, outlying cohorts highlighting unstable numerical computation, or alarming inflation.
Meta-Analysis
Meta-analysis was designed as the following paradigm. Cross-population meta-analysis (CPMA) was designed to be combine all population group results, with additional focused population-group specific and sex-specific analyses. This resulted in 18 total meta-analyses to be run: 6 population groups (CPMA, EUR, HIS, EAS, AFR, SAS) and 3 sex groups (combined sex, female sex, male sex). To accomplish this, METAL software was first used to run all meta-analyses within each specific population group for the marginal effect (), main effect (), interaction effect (), and joint effect (, ) with GC correction for inflation(12). Inverse-variance weights were used and Manning et. al’s method for the 2df joint test (13). CPMA was subsequently executed on the resultant population-group specific METAL output results with GC correction.
Genome-wide Significant Loci Identification
EasyStrata2 software was used to prioritize top loci from significant results identified from the 1df interaction and 2df joint tests(14). GC correction for population-group specific results was applied. Variants found within 1 Mb distance of the major histocompatibility complex (MHC) region were excluded. Either minimum sample size (N > 20000) or multiple cohorts (≥3) was required as necessary criteria for processing results from a specific sex-stratified, and/or population group-stratified meta-analysis.
Significant variants were identified using the following threshold criteria: (i) i variants with significant interaction effect (PM1_GxE<5e-9, FDR < 0.05); (ii) j variants with significant joint effect (PM1_G,GxE<5e-9, FDR < 0.05) were filtered as top variants; and (iii) k top variants for the interaction effect were identified using a 2-step method – identifying first z variants by the marginal effect (PM2_G<1e-5) and then filtering these by the interaction effect (PM1_GxE<0.05/NG, FDRGxE<0.05) where NG is the number of independent tests calculated using principal components analysis on the z variants. This 2-step method was incorporated to increase power for detecting interactions(15). This design was executed to maintain both stringent threshold criteria and incorporate false discovery correction implemented by the Benjamini-Hochberg method.
All such i + j + k significant variants were narrowed down to loci based on 500 kilobase (kb) regions. Finally, within these regions independent lead variants were identified as the top significant variant within the locus, subsequently defining variants in LD as those with linkage disequilibrium (LD) r2 threshold < 0.1 using TOPMed-imputed 1000G reference panels. If variants were missing in the LD panels, then the most significant variant within each 500kb region was retained for combined sex meta-analyses results.
Prioritizing Novel Sleep Duration Interaction Loci
Significant independent loci were subsequently filtered to prioritize gene-sleep duration interaction loci. From the 1df interaction test, X interaction loci were prioritized as those not found within 1Mb of previously identified gene-sleep duration loci for BP(8). Loci were annotated as whether novel for BP genetic architecture, or not, by checking for overlap with 1Mb of previous GWAS variants (Supplementary Table S3).
For the 2df test, first loci were filtered to those variants not found within 1Mb of previous GWAS identified variants for BP traits, and with insignificant marginal effect (PM2_G >5e-09, FDRM2_G >0.05). From these variants, Y loci were prioritized as driven by interaction if they harbored a stronger interaction effect relative to the main effect (PM1_GxE < PM1_G), and Z loci deemed as supported (but not driven) by interaction if this was not true.
Thus, collectively X + Y gene-sleep duration interaction loci were highlighted, alongside secondarily Z loci supported by interaction.
Heterogeneity by Sex
To test for interaction effects showing evidence of heterogeneity by sex (p < 0.05/Q), two-sample Z-tests assuming independence, were conducted for each of the top interaction loci and adjusted for multiple testing.
Mapped Protein Coding Genes
Gene mapping prioritized protein-coding genes for downstream interpretation. Variants directly overlapping protein-coding gene regions were top priority criteria for gene assignment. For intergenic variants nearest distance to transcription start site (TSS) or gene start/end site was queried from Open Target Genetics v22.10(16) or MyGene.Info using Python package mygene v3.2.2 (https://github.com/biothings/mygene.py). Variant mapping annotations were additionally noted from Open Target Genetics, Functional Annotation of Variants – Online Resource v2.0 (FAVOR)(17), HaploReg v4.2 (https://pubs.broadinstitute.org/mammals/haploreg/haploreg.php), BRAVO variant browser (https://bravo.sph.umich.edu/freeze8/hg38/), Functional Mapping and Annotation of Genome-wide Association Studies v1.5.6 (FUMA)(18), and MyGene.Info.
Variant Annotations
FAVOR was queried to annotate deleteriousness or functionality scores(17), and RegulomeDB v2.2 was used to extract aggregate regulatory function evidence scores, along with chromatin state, DNA accessibility, overlap with transcription factor (TF) binding sites or TF motifs, and expression quantitative trait loci (eQTL)(19). FUMA’s SNP2GENE pipeline was used to annotate a comprehensive list of genes for each top locus, incorporating positional, chromatin interaction (FDR < = 1e-6, 250bp upstream − 500 bp downstream of TSS), and GTEXv8 eQTL evidence (agreeing with RegulomeDB) with the top variant or its variants in LD (r2 > 0.1 within 500kb)(18).
At the variant level, PheWeb, Open Target Genetics, Common Metabolic Diseases Knowledge Portal (https://hugeamp.org/), and Oxford Brain Imaging Genetics Server (BIG40) were queried for significant trait associations (p < 5e-08) from past GWAS(16, 20, 21). At the gene level, International Mouse Phenotyping Consortium release 19.1 (IMPC), Online Mendelian Inheritance in Man (OMIM; https://omim.org/), PheWeb, Phenotype-Genotype Integrator (PheGenI), and Open Target Genetics were queried for phenotypic annotations from mice knockout study results, involvement in Mendelian disorders, and significant trait associations (p < 5e-08) (16, 20, 22, 23). All STST and LTST mapped protein-coding genes were then queried using FUMA’s GENE2FUNC pipeline to identify significant (adjusted p-value < 0.05) pathways and traits(18). STRING v12.0 was additionally queried using medium confidence threshold (0.4) to note significantly (FDR < 0.05) enriched traits or pathways to compare and contrast LTST and STST loci (24).
Druggability Analysis
The Drug-Gene Interaction database (v4.2.0) was first utilized to identify druggability potential, with genes also annotated for implicated pathways and functions using the Kyoto Encyclopedia of Genes and Genomes database. Druggability target categories were annotated and all interacting drugs queried from reports across 43 databases (BaderLabGenes, CarisMolecularIntelligence, dGene, FoundationOneGenes, GO, HingoraniCasas, HopkinsGroom, HumanProteinAtlas, IDG, MskImpact, Oncomine, Pharos, RussLampel, Tempus, CGI, CIViC, COSMIC, CancerCommons, ChemblDrugs, ChemblInteractions, ClearityFoundationBiomarkers, ClearityFoundationClinicalTrial, DTC, DoCM, DrugBank, Ensembl, Entrez, FDA, GuideToPharmacology, JACX-CKB, MyCancerGenome, MyCancerGenomeClinicalTrial, NCI, OncoKB, PharmGKB, TALC, TEND, TTD, TdgClinicalTrial, Wikidata). Protein targets for available active ligands in ChEMBL were also noted. Gene targets were looked up in the druggable genome using the most recent druggable genome list established from the NIH Illuminating the Druggable Genome Project (https://github.com/druggablegenome/IDGTargets) available through the Pharos web platform. Lastly, FDA-approved drugs, late-stage clinical trials and disease indications were queried in the DrugBank, ChEMBL, ClinicalTrials.gov databases to provide results for the top MESH and DrugBank indications and clinical trials.
RESULTS
Discovery of Novel Gene-Sleep Duration Interactions
From an initial source of 37 studies, 59 population-group specific cohorts (derived from self-reported ancestry) resulted in a pooled sample size of 811,405 individuals comprising of 5.9% AFR (12 cohorts), 6.0% EAS (5 cohorts), 83.4% EUR (34 cohorts), 3.7% HIS (7 cohorts), and 0.9% SAS (1 cohort) (Supplementary Tables S1-S2). The 1df test discovered seven loci and the 2-step method discovered one locus. The 2df joint test first identified 3629 significant loci, from which 18 were novel for BP (Supplementary Table S3) with insignificant marginal effect – revealing 14 loci driven by the interaction effect, and four not driven. Thus in total we discovered 22 gene-sleep duration interaction loci, and 4 secondary loci – of which 21 are novel for BP traits (Supplementary Table S4). Among the 22 prioritized interaction loci, four loci exhibited cross-population effects (Table 1, Supplementary Figures S1-S3) – one identified in combined sex, three in female sex-stratified analyses, and 18 identified specific to either one of the AFR, HIS, or EUR population groups (Table 2, Supplementary Figures S1-S3). Specifically, AFR analysis revealed one gene-sleep duration interaction locus, HIS analysis revealed 11 gene-sleep duration interaction loci, and EUR analysis revealed six gene-sleep duration loci (Table 2). Three variants identified in combined sex meta-analyses showed evidence of heterogeneous effect by sex (Table 2).
Table 1.
Novel Gene-Sleep Duration Interaction Loci Identified in Cross-Population Meta-Analysis All results herein are from the M1 model. Supplementary Table S21 provides summary statistics according to each population group identified in cross-population results. For the sex column, C denotes combined sex, and F denotes female sex-stratified meta-analysis. For the alleles column, E denotes effect allele, and O denotes other allele used as reference. Bold denotes significance.
| xposure | Variant | Nearest gene(s) | Position (hg38) |
Alleles (E/O) | AF | N | Sex | Population Groups | Trait | BM1_G (seM1_G) | BGxE (seGxE) | PM1_G | PGxE | PG,GxE | Psex_diff |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Loci Identified by 1df Interaction Test | |||||||||||||||
| STST | rs113144211 | WBP1L | 10:102808541 | C/CG | 0.551 | 279527 | F | AFR, EAS, EUR, HIS, SAS | PP | 0.12 (0.04) | 0.40 (0.09) | 1.60E-03 | 7.82E-06 | 3.54E-11 | 8.84E-05 |
| LTST | rs5384795532 | FAM98A | 2:33903659 | C/G | 0.102 | 41814 | F | AFR, EAS, EUR, HIS | SBP | 1.12 (0.40) | −5.09 (0.86) | 5.27E-03 | 3.32E-09 | 2.35E-08 | 3.59E-06 |
| Loci Identified by 2df Joint Test, Driven by Interaction Effect | |||||||||||||||
| STST | rs764584102 | YWHAB | 20:44851866 | G/A | 0.023 | 47678 | C | AFR,HIS | PP | 0.14 (0.34) | −3.65 (0.73) | 6.93E-01 | 6.38E-07 | 3.88E-09 | 6.87E-02 |
| LTST | rs14319996952 | ALG10B | 12:37297511 | T/C | 0.016 | 29473 | F | EUR, HIS | PP | −0.57 (0.44) | −3.28 (0.78) | 1.88E-01 | 2.46E-05 | 4.55E-09 | 4.07E-04 |
denotes the variant was identified using the two-step approach.
denotes variants novel for BP.
Table 2.
Novel Gene-Sleep Duration Interaction Loci Identified Specific to Certain Population Groups.
All results herein are from the M1 model. Supplementary Table S22 provides summary statistics according to each population group-specific cohort identified in these population-group specific results. For the sex column, C denotes combined sex meta-analysis, and M denotes male sex-stratified meta-analysis. For the alleles column, E denotes effect allele, and O denotes other allele used as reference. Bold denotes significance.
| Exposure | Variant | Nearest gene(s) | Position (hg38) |
Alleles (E/O) | Sex | AF | N | Population Groups | Trait | BM1_G (seM1_G) | BGxE (seGxE) | PM1_G | PGxE | PG,GxE | Psex_diff2 | |||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Loci Identified by 1df Interaction Test | ||||||||||||||||||
| STST | rs114831731 | AHCYL1 | 1:109970740 | A/T | C | 0.009 | 23897 | HIS | PP | 0.85 (0.64) | −6.27 (1.04) | 1.87E-01 | 1.57E-09 | 7.34E-11 | 5.67E-04 | |||
| rs144229676 | ZNF521 | 18:25303461 | A/C | C | 0.019 | 27119 | HIS | DBP | 2.32 (0.70) | −7.23 (1.18) | 8.70E-04 | 8.10E-10 | 1.80E-09 | 5.00e-01 | ||||
| rs1035064 | ZNF682 | 19:19997730 | T/C | M | 0.019 | 392939 | EUR | SBP | −0.27 (0.18) | 2.10 (0.36) | 1.62e-01 | 4.82E-09 | 5.76E-08 | 1.52E-04 | ||||
| rs1129580071 | PAK5 | 20:9805888 | C/T | C | 0.005 | 23897 | HIS | PP | 2.09 (0.97) | −10.83 (1.78) | 3.03E-02 | 1.28E-09 | 1.23E-08 | |||||
| rs7520866771 | KRTAP13-2 | 21:30362234 | C/G | C | 0.002 | 30009 | EUR | DBP | 2.12 (0.87) | −8.71 (1.23) | 1.47E-02 | 1.46E-12 | 5.68E-13 | |||||
| LTST | rs372262693 | TG, SLA | 8:133069499 | T/C | C | 0.023 | 23897 | HIS | PP | 0.62 (0.41) | −4.91 (0.82) | 1.34E-01 | 2.33E-09 | 7.11E-09 | 2.43E-01 | |||
| Loci Identified by 2df Joint Test, Driven by Interaction Effect | ||||||||||||||||||
| STST | rs1438637721 | MROH7 | 1:54707218 | T/G | C | 0.006 | 23902 | HIS | SBP | −1.56 (1.06) | −6.99 (1.74) | 1.47E-01 | 5.79E-05 | 1.84E-10 | ||||
| rs1411177151 | KCNJ3 | 2:155446948 | C/T | C | 0.021 | 23897 | HIS | PP | 0.51 (0.44) | −4.29 (0.76) | 2.53E-01 | 1.74E-08 | 2.45E-09 | 7.86E-02 | ||||
| rs170112821 | ZNF385D | 3:22386254 | C/G | C | 0.006 | 23897 | HIS | PP | −0.01 (0.79) | −6.00 (1.20) | 9.93E-01 | 5.86E-07 | 4.13E-10 | 1.97E-01 | ||||
| rs7649852491 | EFNA5 | 5:105713137 | T/C | C | 0.002 | 26230 | EUR | PP | 0.97 (1.48) | −11.78 (2.00) | 5.09E-01 | 4.06E-09 | 6.45E-12 | |||||
| rs5427451701 | WWOX | 16:78323227 | A/C | C | 0.009 | 23897 | HIS | PP | −0.36 (0.72) | −4.96 (1.19) | 6.20E-01 | 3.14E-05 | 5.00E-09 | 2.05E-03 | ||||
| LTST | rs5337240621 | BRINP3 | 1:190792851 | TA/T | C | 0.011 | 34442 | AFR | PP | 1.13 (0.60) | −4.40 (1.18) | 6.03E-02 | 1.92E-04 | 3.69E-09 | 3.56E-04 | |||
| rs1382886951 | CRBN | 3:3295965 | G/A | C | 0.006 | 23897 | HIS | DBP | 0.57 (0.68) | −5.50 (1.08) | 4.07E-01 | 3.46E-07 | 1.31E-09 | |||||
| rs1429661821 | ALCAM | 3:104791665 | T/C | C | 0.006 | 26230 | EUR | DBP | −0.20 (0.62) | −5.37 (1.01) | 7.50E-01 | 1.01E-07 | 1.21E-09 | |||||
| rs5400415831 | PAM | 5:103002447 | A/G | C | 0.003 | 26230 | EUR | PP | −1.54 (1.20) | −6.50 (1.66) | 1.99E-01 | 8.93E-05 | 6.93E-10 | |||||
| rs1139521421 | SDK1 | 7:3917121 | A/C | C | 0.005 | 23902 | HIS | SBP | −0.28 (1.20) | −9.07 (1.90) | 8.18E-01 | 1.81E-06 | 5.49E-10 | |||||
| rs1113924011 | JMJD1C | 10:65029197 | T/G | C | 0.007 | 23897 | HIS | DBP | 0.49 (0.63) | −5.71 (1.00) | 4.32E-01 | 1.27E-08 | 2.28E-10 | |||||
| rs7728629321 | ATP8A2 | 13:25395875 | T/C | C | 0.002 | 30009 | EUR | DBP | −0.11 (0.70) | −4.85 (1.00) | 8.70E-01 | 1.31E-06 | 1.28E-09 | |||||
denotes variants novel for BP.
Empty cell in Psex_diff indicates the variant, after quality control, was not found in both sex-stratified meta-analyses.
Prior Reported Gene-Sleep Interactions
In our current cross-population meta-analysis, rs10406644 showed interaction evidence with STST (PG×E=2.0×10−4 for PP), and rs7955964 with LTST (PG×E=6.6×10−3 for SBP, PG×E=1.7×10−2 for DBP) with direction of association agreeing with prior work(8), and non-significance (PGxE>0.05) for the opposite sleep duration exposure (Supplementary Table S5).
Functional Potential of Variants
Four variants (rs11483173, rs372262693, rs113952142, rs11314421) were marked by high transcription activity chromatin states and eight variants (rs114831731, rs372262693, rs143863772, rs533724062, rs11314421, rs1035064, rs538479553, rs13032423) were marked by accessible chromatin in heart tissue or blood (Supplementary Table S6). Six variants (rs114831731, rs542745170, rs533724062, rs11314421, rs1035064, rs538479553) reflected marked regulatory potential with RegulomeDB scores ≥2c (Supplementary Table S6).
Mapped Protein-Coding Genes
All 26 variants identified were either intronic or intergenic, and mapped to a primary set of 27 protein coding genes (Supplementary Table S7). Extended gene mapping revealed 292 genes highlighted for the 12 STST interaction loci, 67 genes for the 10 LTST interaction loci, and 35 genes for the four joint 2df loci not driven by interaction (Supplementary Tables S7-S9).
Expression Quantitative Trait Loci (eQTL)
Tissue-specific (GTEXv8) eQTL associations were observed at rs11314421, rs1035064, and rs34761985 in tissues of the heart, vasculature, or blood (Supplementary Table S8)(19). WBP1L-rs11314421 and ZNF682-rs1035064 gene mappings were corroborated by eQTL evidence identified in venous blood or the tibial artery. Beyond these primary mapped genes, MFSD13A, BORCS7, CALHM2, RPARP-AS1, AS3MT, and SFXN2 expression were mapped to rs11314421 by eQTL evidence in the ascending aorta, coronary artery, tibial artery, left ventricle myocardium, right atrium auricular region, venous blood, or lymphoblast. Similarly, ZNF56, ZNF253, ZNF93, ZNF90, and ZNF486 were mapped by coronary artery or venous blood eQTL evidence to rs1035064. UXS1 was mapped by rs34761985 eQTL data identified in the right atrium auricular region.
Variant-Level Cross-Trait Associations
Several variants show associations (P < 5×10−8) with other traits (Supplementary Table S10). Querying Open Target Genetics (https://genetics.opentargets.org) identified rs11314421 (WBP1L) to be associated with hypertension and testosterone levels, and rs13032423 (VRK2) with sleep duration and feeling miserable (Supplementary Table S11). Common Metabolic Diseases Knowledge Portal (https://hugeamp.org/) further identified rs13032423 (VRK2) to be associated with BMI and sleep duration (Supplementary Figure S4). Querying brain imaging phenotypes through the Oxford Brain Imaging Genetics Server (BIG40) revealed rs13032423’s (VRK2) connection to brain functional connectivity by its association with rfMRI connectivity (ICA100 edge 965) (Supplementary Table S12, Supplementary Figure S5)(21).
Gene Functional Implications
Mice knockout evidence highlighted genes important for heart morphology (BRINP3, CRBN, ALG10B, PRMT6), and cardiac rhythm (TG, WBP1L) (Supplementary Table S13). Open Target Genetics, PheWeb, and PheGenI revealed genes implicated in genetic associations (p < 5×10−8), with OMIM (https://omim.org/) identifying any linked Mendelian disorders (Supplementary Tables S14-S17)(16, 20, 23). Specifically, eight genes harbored links to the cardiovascular domain through association with traits identifying by genetic studies: WBP1L, EFNA5, ZNF521, WWOX, ZNF385D, FAM98A, PAM, and JMJD1C. ALG10B was identified to be implicated in the Mendelian disorder long QT syndrome. In the realm of sleep and circadian health, reported genetic associations corroborated the relevance of EFNA5, ZNF521, WWOX, ALG10B, PAM and SDK1 with insomnia, daytime napping, or chronotype traits. Genetic associations to other pertinent domains including kidney function, neurological health, liver function, thyroid function, metabolism, lifestyle choice, and inflammation, were also noted (Supplementary Table S10).
Gene Set Enrichment Analysis
We performed gene set enrichment analyses on the aforementioned extended gene sets in the FUMA GENE2FUNC platform and STRING database (Supplementary Tables S18-S19)(18, 24). STST-mapped genes highlighted pathways in antioxidant defense and neuron excitation, along with phenotypic connection to lipid levels, neurological health, cardiovascular health, metabolism and immune defense. LTST-mapped genes implicated traits involving inflammation, neurological health, and metabolism. A clearly distinctive pattern differentiating short and long sleep duration interaction loci was thus not observed.
Druggability
We investigated druggability of the primary mapped genes using an integrative approach to highlight drug repurposing potential (Supplementary Table S20) (25). Identified gene candidates revealed connections to serotonergic response (HTR1F, KCNJ3), proteasome-mediated ubiquitination (CRBN), thyroid hormone synthesis (TG), and axon guidance (PAK5, ALCAM) pathways. Of these, KCNJ3, CRBN, HTR1F, TG, PAK5, and ALCAM harbored links to reported drug interactions and active ligand interactions in the ChEMBL database. The following genes displayed evidence of pharmacological targeting: KCNJ3 (by small molecule inhibitors Atomoxetine and Dronedarone); CRBN (by thalidomide analogs Pomalidomide and Lenalidomide); HTR1F (by selective serotonin receptor agonists like Lasmiditan); and ALCAM (by chemotherapy agent Fluorouracil).
DISCUSSION
In this large-scale effort investigating the biomolecular mechanisms underpinning the intersecting roles of sleep health and blood pressure traits, we conducted genome-wide gene-by-sleep duration (short and long sleep) interaction analyses in 811,405 individuals of diverse population backgrounds (AFR, EAS, EUR, HIS, SAS) for systolic blood pressure, diastolic blood pressure, and pulse pressure. We report novel discovery of 22 gene-sleep duration interaction loci for BP traits – 12 for short sleep, and 10 for long sleep. Several of the identified variants are rare with allele frequency < = 1%, with four variants identified in sex-stratified meta-analyses, and 18 variants specific to either the AFR(1), EUR(6), or HIS (11) population groups. In line with our previous research, the identified genomic loci exhibiting interactions with short and long sleep are non-overlapping (with non-significance in the opposing sleep duration exposure), suggesting distinct mechanisms influencing cardiovascular health. Nonetheless, we did not observe a clear differentiating pattern in the biological pathways implicated when comparing short sleep and long sleep.
The functional annotation investigations of our prioritized genes point towards cardiovascular and neurological connections, along with revealing links to circadian rhythm, thyroid function, bone health, and hematopoiesis mechanisms. Our findings highlight potential pharmacological candidates and suggest pertinent pathways to consider when designing holistic therapeutic regimens for improving blood pressure control.
Firstly, at a broad level, several identified genes are tied to neurological mechanisms. KCNJ3 encodes Kir3.1 – the alpha subunit for the IKACh potassium channel – and is interestingly implicated in bradyarrhythmia by its missense variant inducing a gain of function of IKACh, as activation of this channel is tied to the negative chronotropic effect on heart rate exerted by the parasympathetic nervous system(29). CRBN is linked to cognitive function (30), SDK1 promotes synaptic connectivity (31), ZNF521 regulates neuron cell fate (32), and ATP8A2 is involved in both neuron vesicle transport and cardiac conduction (33). Further, KRTAP13-2, WWOX, EFNA5, and ALCAM are linked to nervous system development with additional roles for WWOX in myelination (34) and EFNA5 in vascular sympathetic innervation (35). These functional connections may suggest a potential nervous system-heart connection that could be influenced by sleep or circadian disturbances.
In fact neurological pathway connections to circadian rhythm reveal themselves through two enzymes - PAK5 and PAM. Given that circadian rhythm and clock gene expression is intimately connected to blood pressure patterns, of note is PAK5 – a serine/threonine kinase protective of adult neurons from injury and ischemic stress(36). PAK5 has both been shown to be targeted by clock gene-regulated miRNAs in the liver and identified to strongly bind to 14-3-3 proteins – a protein family connected to light-sensitive melatonin diurnal patterns and plausibly influential for sleep behavior(37, 38). This strong binding affinity to 14-3-3 proteins suggests an interesting connection, as YWHAB (one of this study’s primary genes mapped to a STST interaction locus), is part of this protein family. Another enzyme informing the neurological-sleep axis is PAM, encoding a copper-dependent enzyme important for synthesizing amidated neuropeptides like NPY – which regulates sleep through noradrenergic signals(39, 40).
Further, TG and JMJD1C, both encoding proteins intrinsically tied to thyroid hormone function (thyroglobulin and thyroid receptor-interacting protein 8 respectively) – present suggestive ties to the intersection between thyroid function and circadian rhythms. TG mRNA and protein expression levels have shown to increase in response to melatonin, along with its genetic variants associated with autoimmune thyroid diseases(41, 42). Gene silencing of JMJD1C’s paralog has shown arrhythmicity and prolonged sleep in Drosophila(43). Given that circadian clock and thyroid function are increasingly suggested to be interconnected, and sleep deprivation can disrupt temporal hormone profiles (e.g. increased morning plasma thyroid-stimulating hormone (TSH) levels), it may be valuable to investigate further the overlapping pathways between thyroid function, healthy sleep duration, and cardiovascular morbidity(44).
Beyond thyroidal pathways, hematopoiesis presents a possible comprehensive perspective on the interconnectedness between sleep health and nervous system response. WBP1L, one of the primary genes identified (mapped to a STST interaction locus identified in female-specific CPMA) has suggestive connection to regulating the CXCL12-CXCR4 signaling pathway by its inhibitory role on CXCR4, the receptor for ligand CXCL12(45). This pathway is both influential for inflammation and hematopoietic state, reflects circadian control, and directly implicates the sympathetic nervous system response – pertinent as stressors are suspected to induce a more exacerbated response in females(46, 47). If stress factors (e.g. sleep loss) induce noradrenaline, this can downregulate CXCL12, with resultant increased cell proliferation of pro-inflammatory cells from the bone marrow, incurring vascular damage(46). For instance, fragmented sleep has shown to promote myelopoiesis and lower hypocretin release by the hypothalamus, in turn accelerating atherosclerosis progression(48). Thus perhaps WBP1L can offer insight into the intersections between sympathetic activation, neurological control, and unhealthy sleep impacting cardiovascular health, especially in women.
On a similar note of addressing sex-specificity, of relevance is FAM98A, a gene identified in female-specific CPMA for interaction with long sleep. FAM98A, harboring multiple arginine demethylation sites, is a substrate of PRMT1 - an enzyme which catalyzes the synthesis of asymmetric dimethylarginine (ADMA), a molecule associated with cardiovascular harm as it induces endothelial dysfunction(49). Thus seeking to lower harmful ADMA levels to counter harmful effects of sleep loss may be relevant in preservation of vascular integrity(50). FAM98A, encoding a microtubule-associated protein, is also functionally linked to osteoclast formation, which is key to bone resorption and involved in postmenopausal osteoporosis etiology(51). Given that osteoporosis and CVD share pathology, the FAM98A locus may shed light on the importance of considering holistic treatment for hypertensive women approaching or after menopause – an example being Felodipine, an antihypertensive found to additionally discourage osteoclast differentiation(52, 53).
Apart from FAM98A, specific genes highlight pathway connections to offer possible avenues for enhancing treatment efficacy for hypertension. Addressing the role of inflammation, SLA may lend promise as an immunosuppressant, with cytoplasm-specific delivery of specific domains of SLA shown to inhibit the T cell receptor functional cascade(54). ALG10B closely interacts with KCNH2 to protect it from inhibition by pharmaceuticals and thus prevent acquired long QT syndrome - interesting, as past work has identified KCNH2 genetic variation to associate with efficacy of specific antihypertensive drugs(55, 56). PAK5 is the effector protein of CDC42, vital for endothelial integrity and involved in the mechanism of Nebivolol, a third generation beta-blocker(57, 58). CRBN, due to its intrinsic role in ubiquitination, is recruited as an E3 ligase ligand in protease-targeted chimeras (PROTACs), which hold promise in cardiovascular therapeutics – an example being P22A shown to reduce collateral damage of HMGCR upregulation caused by statins(59). These findings point to the need for future preclinical and clinical studies to confirm the hypothesized mechanisms and test promising interventions.
Our druggability analysis specified genes acting as existing pharmacological targets of FDA-approved drugs, offering perspective for drug repurposing. HTR1F and KCNJ3 are linked to the serotonergic pathway and are targets of approved ADHD and antiarrhythmic drugs Atomoxetine and Dronedarone, respectively. This is potentially relevant given that serotonin may impact blood pressure regulation, and serotonin receptor desensitization is implicated in chronic sleep restriction(60, 61). HTR1F encodes for 5-HT1F, shown to function in smooth muscle and trigeminal nerves, with its selective agonists (i.e. Lasmiditan) offering greater efficacy for migraine treatment without the collateral harm of vasoconstrictive effects induced by non-selective triptans(62).
Noticeably all 22 gene-sleep duration interaction loci we identified were specific to a particular population group, a subset of population groups, or a particular sex. This may be due to substantial heterogeneity in BP architecture and sleep lifestyle as a result of cultural differences, uniquely varying stressors due to socioeconomics, and genetic risk that are both shaped by and influence lifestyle choices. For example, admixed African and Hispanic populations are more likely to have poorly controlled hypertension and circadian abnormalities in BP regulation, as well as higher prevalence of both short and long sleep duration relative to individuals of European ancestry(63, 64). Females generally sleep longer, have higher prevalence of insomnia, and experience an increased proinflammatory response to sleep deprivation compared to males(65). Such differential risk profiles are likely attributed to a myriad of social or environmental variables along with genetic and epigenetic susceptibility(8). Therefore, it is likely that the same duration of self-reported sleep has different etiologies and physiological effects across sex and population background. Future research incorporating extensive phenotyping may help clarify whether gender-specific or population-specific findings are explained by differences in sleep-related or other lifestyle behaviors, mechanisms underlying response to sleep disturbance, or are spurious.
This study has several strengths including its large-scale nature made possible by inclusion of several international biobanks and cohort studies, rigorous data harmonization and quality control protocols, and robust statistical analysis pipelines. Our findings are reinforced by multiple lines of evidence from bioinformatics analysis. Focused druggability analysis and interpretation of drug-gene interactions offer promising insight in drug repurposing and candidate targets for future pursuits.
Limitations of this study include the risk of unidentified misclassification of self-reported sleep duration (opposed to objective measurements from actigraphy or polysomnography) due to recall bias, sleep misperception, or other psychosocial factors. Sleep health is complex, with key dimensions beyond duration (e.g., timing, quality, satisfaction, and regularity)(66). Abnormality in these other sleep dimensions were not tested here due to lack of readily available data. Adding to the complexity, sleep duration itself reflects heterogeneous health effects influenced by genetic determinants. For example, genetic variation conducive to naturally short sleepers may even lend neuroprotection against harmful brain pathology(67). In addition, there may be residual confounding bias due to unadjusted comorbidities or environmental factors. Lastly, despite notable diversity of our sample, our data was dominated by individuals of European ancestry. It is striking that several of our loci are HIS-specific – which may be resultant of complex admixture present in this population group. Although we were able to delve into sex-specific interpretations for FAM98A, and WBP1L – future investigation is desired to understand the reasons behind heterogeneous effects by sex. Enrichment of sample sizes in minority populations is critical for future investigations.
In conclusion this study advances our understanding of the interaction between sleep duration extremes and genetic risk factors shaping the genetic landscape of blood pressure. Our novel discovery of 22 gene-sleep duration interaction loci both accentuates the relevance of proper sleep duration in cardiovascular health and the need to be conscious of heterogeneity present in specific sex or population groups, providing valuable perspective for therapeutic intervention strategies to address cardiovascular disease burden.
Figure 1.
Analysis Workflow
Figure 2.
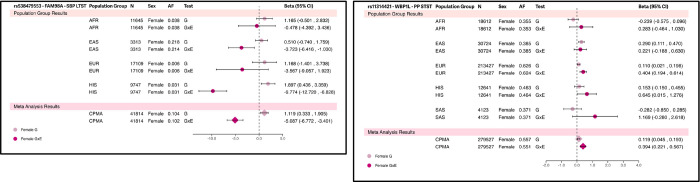
Forest Plots of Gene-Sleep Duration Loci Identified by the 1df Interaction Test in Female-Specific Cross-Population Meta-Analyses.
These are the prioritized 1df Interaction Test results from female-specific cross-population meta-analyses. Contributing female-specific population groups’ (if this variant is found in the particular population group, after quality control) summary statistics are depicted here that were pooled.
Figure 3.
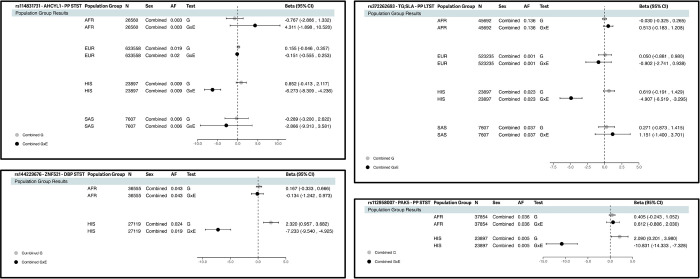
Forest Plots of Gene-Sleep Duration Loci Identified by the 1df Interaction Test in Combined Sex HIS-Specific Meta-Analyses
These are the prioritized 1df Interaction Test results from HIS-specific meta-analyses. Other population group data (if this variant is found in the particular population group, after quality control) are shown here to emphasize that these gene-sleep duration interaction loci were significant only in the HIS population group.
Table 3.
Novel BP Loci Identified by the 2df Joint Test, Not Driven by the Interaction Effect
| Exposure | Variant | Nearest gene(s) | Position (hg38) |
Alleles (E/O) | Sex | AF | N | Population Groups | Trait | BM1_G (seM1_G) | BGxE (seGxE) | PM1_G | PGxE | PG,GxE | Psex_diff2 |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Loci Identified by 1df Interaction Test | |||||||||||||||
| STST | rs114831731 | AHCYL1 | 1:109970740 | A/T | C | 0.009 | 23897 | HIS | PP | 0.85 (0.64) | −6.27 (1.04) | 1.87E-01 | 1.57E-09 | 7.34E-11 | 5.67E-04 |
| rs144229676 | ZNF521 | 18:25303461 | A/C | C | 0.019 | 27119 | HIS | DBP | 2.32 (0.70) | −7.23 (1.18) | 8.70E-04 | 8.10E-10 | 1.80E-09 | 5.00e-01 | |
| rs1035064 | ZNF682 | 19:19997730 | T/C | M | 0.019 | 392939 | EUR | SBP | −0.27 (0.18) | 2.10 (0.36) | 1.62e-01 | 4.82E-09 | 5.76E-08 | 1.52E-04 | |
| rs1129580071 | PAK5 | 20:9805888 | C/T | C | 0.005 | 23897 | HIS | PP | 2.09 (0.97) | −10.83 (1.78) | 3.03E-02 | 1.28E-09 | 1.23E-08 | ||
| rs7520866771 | KRTAP13-2 | 21:30362234 | C/G | C | 0.002 | 30009 | EUR | DBP | 2.12 (0.87) | −8.71 (1.23) | 1.47E-02 | 1.46E-12 | 5.68E-13 | ||
| LTST | rs372262693 | TG, SLA | 8:133069499 | T/C | C | 0.023 | 23897 | HIS | PP | 0.62 (0.41) | −4.91 (0.82) | 1.34E-01 | 2.33E-09 | 7.11E-09 | 2.43E-01 |
| Loci Identified by 2df Joint Test, Driven by Interaction Effect | |||||||||||||||
| STST | rs1438637721 | MROH7 | 1:54707218 | T/G | C | 0.006 | 23902 | HIS | SBP | −1.56 (1.06) | −6.99 (1.74) | 1.47E-01 | 5.79E-05 | 1.84E-10 | |
| rs1411177151 | KCNJ3 | 2:155446948 | C/T | C | 0.021 | 23897 | HIS | PP | 0.51 (0.44) | −4.29 (0.76) | 2.53E-01 | 1.74E-08 | 2.45E-09 | 7.86E-02 | |
| rs170112821 | ZNF385D | 3:22386254 | C/G | C | 0.006 | 23897 | HIS | PP | −0.01 (0.79) | −6.00 (1.20) | 9.93E-01 | 5.86E-07 | 4.13E-10 | 1.97E-01 | |
| rs7649852491 | EFNA5 | 5:105713137 | T/C | C | 0.002 | 26230 | EUR | PP | 0.97 (1.48) | −11.78 (2.00) | 5.09E-01 | 4.06E-09 | 6.45E-12 | ||
| rs5427451701 | WWOX | 16:78323227 | A/C | C | 0.009 | 23897 | HIS | PP | −0.36 (0.72) | −4.96 (1.19) | 6.20E-01 | 3.14E-05 | 5.00E-09 | 2.05E-03 | |
| LTST | rs5337240621 | BRINP3 | 1:190792851 | TA/T | C | 0.011 | 34442 | AFR | PP | 1.13 (0.60) | −4.40 (1.18) | 6.03E-02 | 1.92E-04 | 3.69E-09 | 3.56E-04 |
| rs1382886951 | CRBN | 3:3295965 | G/A | C | 0.006 | 23897 | HIS | DBP | 0.57 (0.68) | −5.50 (1.08) | 4.07E-01 | 3.46E-07 | 1.31E-09 | ||
| rs1429661821 | ALCAM | 3:104791665 | T/C | C | 0.006 | 26230 | EUR | DBP | −0.20 (0.62) | −5.37 (1.01) | 7.50E-01 | 1.01E-07 | 1.21E-09 | ||
| rs5400415831 | PAM | 5:103002447 | A/G | C | 0.003 | 26230 | EUR | PP | −1.54 (1.20) | −6.50 (1.66) | 1.99E-01 | 8.93E-05 | 6.93E-10 | ||
| rs1139521421 | SDK1 | 7:3917121 | A/C | C | 0.005 | 23902 | HIS | SBP | −0.28 (1.20) | −9.07 (1.90) | 8.18E-01 | 1.81E-06 | 5.49E-10 | ||
| rs1113924011 | JMJD1C | 10:65029197 | T/G | C | 0.007 | 23897 | HIS | DBP | 0.49 (0.63) | −5.71 (1.00) | 4.32E-01 | 1.27E-08 | 2.28E-10 | ||
| rs7728629321 | ATP8A2 | 13:25395875 | T/C | C | 0.002 | 30009 | EUR | DBP | −0.11 (0.70) | −4.85 (1.00) | 8.70E-01 | 1.31E-06 | 1.28E-09 | ||
All results herein are from the M1 model. Supplementary Tables S21-S22 provides summary statistics according to each population group-specific cohort for rs59680540 and rs150586434, and according to each population group for rs34761985 and rs13032423 below. For the sex column, C denotes combined sex meta-analysis. For the alleles column, E denotes effect allele, and O denotes other allele used as reference. Bold denotes significance.
denotes variants novel for BP.
Empty cell in Psex_diff indicates the variant, after quality control, was not found in both sex-stratified meta-analyses.
ACKNOWLEDGMENTS
This project was largely supported by two grants from the U.S. National Heart, Lung, and Blood Institute (NHLBI), the National Institutes of Health, R01HL118305 and R01HL156991. Study-specific acknowledgements are included in the Supplementary Note. The research on the Million Veteran Program, was supported by award, CX001897 (PI A.M. Hung) from BLR&D, VA Office of R&D. This publication does not represent the views of the Department of Veteran Affairs or the United States Government. Acknowledgment of the Million Veteran Program leadership and staff contributions can be found in the Supplementary Note under MVP core acknowledgement.
Footnotes
Declarations
CONFLICT OF INTEREST
C.L.M. has received funding from AstraZeneca not related to the current study. B.M.P. serves on the steering committee of the Yale Open Data Access Project funded by Johnson & Johnson. D.C. receives consultancy fees from Roche Diagnostics and Trimedics and speaker fees from Servier. D.A.L. has received support from Medtronic LTD and Roche Diagnostics for biomarker research not related to the current study. The remaining authors declare no competing interests.
Contributor Information
Heming Wang, Brigham and Women’s Hospital.
Amy Bentley, National Institutes of Health, NHGRI.
Michael Brown, The University of Texas Health Science Center at Houston.
Lisa de las Fuentes, Washington University School of Medicine.
Xiuqing Guo, The Lundquist Institute.
Sarah Harris, The University of Edinburgh.
Jian’an Luan, University of Cambridge.
Leo-Pekka Lyytikäinen, Fimlab Laboratories and Finnish Cardiovascular Research Center.
Massimo Mangino, King’s College London.
Y Milaneschi, VU University Medical Center.
Nicholette Palmer, Department of Genetics and Genomic Sciences, Icahn School of Medicine at Mount Sinai.
Quan Sun, University of North Carolina, USA.
Stefan Weiss, University Medicine Greifswald & University of Greifswald.
Wei Zhao, University of Michigan.
Hugues Aschard, Institut Pasteur.
Lydia Bazzano, Louisiana State University.
Brian Cade, Brigham and Women’s Hospital.
Hung-hsin Chen, Vanderbilt University Medical Center.
Paul de Vries, Human Genetics Center.
Michele Evans, National Institute on Aging.
Mariaelisa Graff, University of North Carolina.
C. Charles Gu, Washington University
Iris Heid, University of Regensburg.
Sami Heikkinen, Institute of Biomedicine, School of Medicine, University of Eastern Finland, Kuopio Campus.
Heather Highland, University of North Carolina at Chapel Hill.
Mika Kähönen, Tampere University.
Kelly Tanika, University of Illinois Chicago.
Joseph McCormick, The University of Texas Health Science Center at Houston (UTHealth) School of Public Health.
Hao Mei, University of Mississippi Medical Center.
Cristina Menni, King’s College London.
Kisung Nam, Seoul National University.
Ilja Nolte, University of Groningen, University Medical Center Groningen.
Michael Province, Washington University.
Bruce Psaty, Cardiovascular Health Research Unit.
Olli Raitakari, Turku University Hospital and Research Centre of Applied and Preventive Cardiovascular Medicine, University of Turku.
Stephen Rich, University of Virginia.
Rodney Scott, University of Newcastle and the Hunter Medical Research Institute.
Jennifer Smith, University of Michigan.
Tamar Sofer, Harvard University.
Uwe Völker, University Medicine Greifswald.
Peter Vollenweider, Lausanne University Hospital (CHUV).
Ko WIllems van Dijk, Leiden University Medical Center.
Rui Xia, The Brown Foundation Institute of Molecular Medicine, McGovern Medical School, The University of Texas Health Science Center at Houston.
Xiaofeng Zhu, Case Western Reserve University.
Jennifer Below, Vanderbilt University Medical Center.
Simon Cox, University of Edinburgh.
Marcus Dörr, University Medicine Greifswald.
Mary Feitosa, Washington University School of Medicine.
Sina Gharib, University of Washington.
Vilmundur Gudnason, Icelandic Heart Association.
Jiang He, Tulane University School of Public Health and Tropical Medicine.
Elizabeth Holliday, Hunter Medical Research Institute.
Deborah Lawlor, University of Bristol.
Terho Lehtimäki, Department of Clinical Chemistry, Fimlab Laboratories and Finnish Cardiovascular Research Center-Tampere, Faculty of Medicine and Health Technology, Tampere University.
Changwei Li, Department of Epidemiology, Tulane University School of Public Health and Tropical Medicine, New Orleans, LA, USA.
Ching-Ti Liu, Boston University School of Public Health.
Alanna Morrison, The University of Texas Health Science Center at Houston.
Patricia Peyser, Department of Epidemiology, School of Public Health, University of Michigan.
Jerome Rotter, The Lundquist Institute for Biomedical Innovation at Harbor-UCLA Medical Center.
Harold Snieder, University Medical Center Groningen.
Nicholas Wareham, University of Cambridge.
Alan Zonderman, National Institute on Aging, NIA/NIH/IRP.
Kari North, UNC Chapel Hill.
Myriam Fornage, 1. Institute of Molecular Medicine, McGovern Medical School, The University of Texas Health Science Center; 2. Human Genetics Center, Department of Epidemiology, School of Public Health.
Dabeeru Rao, Washington University in St. Louis.
Susan Redline, Brigham and Women’s Hospital.
Raymond Noordam, Leiden University Medical Center.
References
- 1.Makarem N, Shechter A, Carnethon MR, Mullington JM, Hall MH, Abdalla M. Sleep Duration and Blood Pressure: Recent Advances and Future Directions. Curr Hypertens Rep. 2019;21(5):33. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Kanki M, Nath AP, Xiang R, Yiallourou S, Fuller PJ, Cole TJ, et al. Poor sleep and shift work associate with increased blood pressure and inflammation in UK Biobank participants. Nat Commun. 2023;14(1):7096. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Kario K. Sleep and nocturnal hypertension: Genes, environment, and individual profiles. J Clin Hypertens (Greenwich). 2022;24(10):1263–5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Bock JM, Vungarala S, Covassin N, Somers VK. Sleep Duration and Hypertension: Epidemiological Evidence and Underlying Mechanisms. Am J Hypertens. 2022;35(1):3–11. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Matsubayashi H, Nagai M, Dote K, Turana Y, Siddique S, Chia YC, et al. Long sleep duration and cardiovascular disease: Associations with arterial stiffness and blood pressure variability. J Clin Hypertens (Greenwich). 2021;23(3):496–503. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Cui H, Xu R, Wan Y, Ling Y, Jiang Y, Wu Y, et al. Relationship of sleep duration with incident cardiovascular outcomes: a prospective study of 33,883 adults in a general population. BMC Public Health. 2023;23(1):124. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Warren H, Edwards T, Vaez A, Keaton J, Kamali Z, Xie T, et al. Genome-wide analysis in over 1 million individuals reveals over 2,000 independent genetic signals for blood pressure. Research Square; 2022. [Google Scholar]
- 8.Wang H, Noordam R, Cade BE, Schwander K, Winkler TW, Lee J, et al. Multi-ancestry genome-wide gene-sleep interactions identify novel loci for blood pressure. Mol Psychiatry. 2021;26(11):6293–304. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Westerman KE, Pham DT, Hong L, Chen Y, Sevilla-Gonzalez M, Sung YJ, et al. GEM: scalable and flexible gene-environment interaction analysis in millions of samples. Bioinformatics. 2021;37(20):3514–20. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Kraft P, Yen YC, Stram DO, Morrison J, Gauderman WJ. Exploiting gene-environment interaction to detect genetic associations. Hum Hered. 2007;63(2):111–9. [DOI] [PubMed] [Google Scholar]
- 11.Winkler TW, Day FR, Croteau-Chonka DC, Wood AR, Locke AE, Magi R, et al. Quality control and conduct of genome-wide association meta-analyses. Nat Protoc. 2014;9(5):1192–212. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Willer CJ, Li Y, Abecasis GR. METAL: fast and efficient meta-analysis of genomewide association scans. Bioinformatics. 2010;26(17):2190–1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Manning AK, LaValley M, Liu CT, Rice K, An P, Liu Y, et al. Meta-analysis of gene-environment interaction: joint estimation of SNP and SNP × environment regression coefficients. Genet Epidemiol. 2011;35(1):11–8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Winkler TW, Kutalik Z, Gorski M, Lottaz C, Kronenberg F, Heid IM. EasyStrata: evaluation and visualization of stratified genome-wide association meta-analysis data. Bioinformatics. 2015;31(2):259–61. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Gauderman WJ, Mukherjee B, Aschard H, Hsu L, Lewinger JP, Patel CJ, et al. Update on the State of the Science for Analytical Methods for Gene-Environment Interactions. Am J Epidemiol. 2017;186(7):762–70. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Ghoussaini M, Mountjoy E, Carmona M, Peat G, Schmidt EM, Hercules A, et al. Open Targets Genetics: systematic identification of trait-associated genes using large-scale genetics and functional genomics. Nucleic Acids Res. 2021;49(D1):D1311–D20. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Zhou H, Arapoglou T, Li X, Li Z, Zheng X, Moore J, et al. FAVOR: functional annotation of variants online resource and annotator for variation across the human genome. Nucleic Acids Res. 2023;51(D1):D1300–D11. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Watanabe K, Taskesen E, van Bochoven A, Posthuma D. Functional mapping and annotation of genetic associations with FUMA. Nat Commun. 2017;8(1):1826. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Boyle AP, Hong EL, Hariharan M, Cheng Y, Schaub MA, Kasowski M, et al. Annotation of functional variation in personal genomes using RegulomeDB. Genome Res. 2012;22(9):1790–7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Gagliano Taliun SA, VandeHaar P, Boughton AP, Welch RP, Taliun D, Schmidt EM, et al. Exploring and visualizing large-scale genetic associations by using PheWeb. Nat Genet. 2020;52(6):550–2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Smith SM, Douaud G, Chen W, Hanayik T, Alfaro-Almagro F, Sharp K, et al. An expanded set of genome-wide association studies of brain imaging phenotypes in UK Biobank. Nat Neurosci. 2021;24(5):737–45. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Groza T, Gomez FL, Mashhadi HH, Munoz-Fuentes V, Gunes O, Wilson R, et al. The International Mouse Phenotyping Consortium: comprehensive knockout phenotyping underpinning the study of human disease. Nucleic Acids Res. 2023;51(D1):D1038–D45. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Ramos EM, Hoffman D, Junkins HA, Maglott D, Phan L, Sherry ST, et al. Phenotype-Genotype Integrator (PheGenI): synthesizing genome-wide association study (GWAS) data with existing genomic resources. Eur J Hum Genet. 2014;22(1):144–7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Szklarczyk D, Gable AL, Lyon D, Junge A, Wyder S, Huerta-Cepas J, et al. STRING v11: protein-protein association networks with increased coverage, supporting functional discovery in genome-wide experimental datasets. Nucleic Acids Res. 2019;47(D1):D607–D13. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Kavousi M, Bos MM, Barnes HJ, Lino Cardenas CL, Wong D, Lu H, et al. Multi-ancestry genome-wide study identifies effector genes and druggable pathways for coronary artery calcification. Nat Genet. 2023;55(10):1651–64. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Freshour SL, Kiwala S, Cotto KC, Coffman AC, McMichael JF, Song JJ, et al. Integration of the Drug-Gene Interaction Database (DGIdb 4.0) with open crowdsource efforts. Nucleic Acids Res. 2021;49(D1):D1144–D51. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Zdrazil B, Felix E, Hunter F, Manners EJ, Blackshaw J, Corbett S, et al. The ChEMBL Database in 2023: a drug discovery platform spanning multiple bioactivity data types and time periods. Nucleic Acids Res. 2023. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Wishart DS, Feunang YD, Guo AC, Lo EJ, Marcu A, Grant JR, et al. DrugBank 5.0: a major update to the DrugBank database for 2018. Nucleic Acids Res. 2018;46(D1):D1074–D82. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Yamada N, Asano Y, Fujita M, Yamazaki S, Inanobe A, Matsuura N, et al. Mutant KCNJ3 and KCNJ5 Potassium Channels as Novel Molecular Targets in Bradyarrhythmias and Atrial Fibrillation. Circulation. 2019;139(18):2157–69. [DOI] [PubMed] [Google Scholar]
- 30.Choi TY, Lee SH, Kim YJ, Bae JR, Lee KM, Jo Y, et al. Cereblon Maintains Synaptic and Cognitive Function by Regulating BK Channel. J Neurosci. 2018;38(14):3571–83. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.de Wit J, Ghosh A. Specification of synaptic connectivity by cell surface interactions. Nat Rev Neurosci. 2016;17(1):22–35. [DOI] [PubMed] [Google Scholar]
- 32.Bond HM, Mesuraca M, Amodio N, Mega T, Agosti V, Fanello D, et al. Early hematopoietic zinc finger protein-zinc finger protein 521: a candidate regulator of diverse immature cells. Int J Biochem Cell Biol. 2008;40(5):848–54. [DOI] [PubMed] [Google Scholar]
- 33.Sakuragi T, Nagata S. Publisher Correction: Regulation of phospholipid distribution in the lipid bilayer by flippases and scramblases. Nat Rev Mol Cell Biol. 2023;24(8):597. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Aldaz CM, Hussain T. WWOX Loss of Function in Neurodevelopmental and Neurodegenerative Disorders. Int J Mol Sci. 2020;21(23). [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Damon DH, teRiele JA, Marko SB. Eph/ephrin interactions modulate vascular sympathetic innervation. Auton Neurosci. 2010;158(1–2):65–70. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Huang N, Li S, Xie Y, Han Q, Xu XM, Sheng ZH. Reprogramming an energetic AKT-PAK5 axis boosts axon energy supply and facilitates neuron survival and regeneration after injury and ischemia. Curr Biol. 2021;31(14):3098–114 e7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Tinti M, Madeira F, Murugesan G, Hoxhaj G, Toth R, Mackintosh C. ANIA: ANnotation and Integrated Analysis of the 14-3-3 interactome. Database (Oxford). 2014;2014:bat085. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Klein DC, Ganguly S, Coon S, Weller JL, Obsil T, Hickman A, et al. 14-3-3 Proteins and photoneuroendocrine transduction: role in controlling the daily rhythm in melatonin. Biochem Soc Trans. 2002;30(4):365–73. [DOI] [PubMed] [Google Scholar]
- 39.Bousquet-Moore D, Mains RE, Eipper BA. Peptidylgycine alpha-amidating monooxygenase and copper: a gene-nutrient interaction critical to nervous system function. J Neurosci Res. 2010;88(12):2535–45. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Singh C, Rihel J, Prober DA. Neuropeptide Y Regulates Sleep by Modulating Noradrenergic Signaling. Curr Biol. 2017;27(24):3796–811 e5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Lee HJ, Stefan-Lifshitz M, Li CW, Tomer Y. Genetics and epigenetics of autoimmune thyroid diseases: Translational implications. Best Pract Res Clin Endocrinol Metab. 2023;37(2):101661. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Garcia-Marin R, Fernandez-Santos JM, Morillo-Bernal J, Gordillo-Martinez F, Vazquez-Roman V, Utrilla JC, et al. Melatonin in the thyroid gland: regulation by thyroid-stimulating hormone and role in thyroglobulin gene expression. J Physiol Pharmacol. 2015;66(5):643–52. [PubMed] [Google Scholar]
- 43.Shalaby NA, Pinzon JH, Narayanan AS, Jin EJ, Ritz MP, Dove RJ, et al. JmjC domain proteins modulate circadian behaviors and sleep in Drosophila. Sci Rep. 2018;8(1):815. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Ikegami K, Refetoff S, Van Cauter E, Yoshimura T. Interconnection between circadian clocks and thyroid function. Nat Rev Endocrinol. 2019;15(10):590–600. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Borna S, Drobek A, Kralova J, Glatzova D, Splichalova I, Fabisik M, et al. Transmembrane adaptor protein WBP1L regulates CXCR4 signalling and murine haematopoiesis. J Cell Mol Med. 2020;24(2):1980–92. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Poller WC, Nahrendorf M, Swirski FK. Hematopoiesis and Cardiovascular Disease. Circ Res. 2020;126(8):1061–85. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Greenlund IM, Carter JR. Sympathetic neural responses to sleep disorders and insufficiencies. Am J Physiol Heart Circ Physiol. 2022;322(3):H337–H49. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.McAlpine CS, Kiss MG, Rattik S, He S, Vassalli A, Valet C, et al. Sleep modulates haematopoiesis and protects against atherosclerosis. Nature. 2019;566(7744):383–7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Wang Q, Yan X, Fu B, Xu Y, Li L, Chang C, et al. mNeuCode Empowers Targeted Proteome Analysis of Arginine Dimethylation. Anal Chem. 2023;95(7):3684–93. [DOI] [PubMed] [Google Scholar]
- 50.Xiao HB, Wang YS, Luo ZF, Lu XY. SZSJ protects against insomnia by a decrease in ADMA level and an improvement in DDAH production in sleep-deprived rats. Life Sci. 2018;209:97–102. [DOI] [PubMed] [Google Scholar]
- 51.Fujiwara T, Ye S, Castro-Gomes T, Winchell CG, Andrews NW, Voth DE, et al. PLEKHM1/DEF8/RAB7 complex regulates lysosome positioning and bone homeostasis. JCI Insight. 2016;1(17):e86330. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Azeez TA. Osteoporosis and cardiovascular disease: a review. Mol Biol Rep. 2023;50(2):1753–63. [DOI] [PubMed] [Google Scholar]
- 53.Zhang S, Li H, Tang H, Huo S, Nie B, Qu X, et al. Felodipine blocks osteoclast differentiation and ameliorates estrogen-dependent bone loss in mice by modulating p38 signaling pathway. Exp Cell Res. 2020;387(2):111800. [DOI] [PubMed] [Google Scholar]
- 54.Kim JH, Moon JS, Yu J, Lee SK. Intracellular cytoplasm-specific delivery of SH3 and SH2 domains of SLAP inhibits TcR-mediated signaling. Biochem Biophys Res Commun. 2015;460(3):603–8. [DOI] [PubMed] [Google Scholar]
- 55.Nakajima T, Hayashi K, Viswanathan PC, Kim MY, Anghelescu M, Barksdale KA, et al. HERG is protected from pharmacological block by alpha-1,2-glucosyltransferase function. J Biol Chem. 2007;282(8):5506–13. [DOI] [PubMed] [Google Scholar]
- 56.He F, Luo J, Luo Z, Fan L, He Y, Zhu D, et al. The KCNH2 genetic polymorphism (1956, C>T) is a novel biomarker that is associated with CCB and alpha, beta-ADR blocker response in EH patients in China. PLoS One. 2013;8(4):e61317. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Ye H, Ling S, Castillo AC, Thomas B, Long B, Qian J, et al. Nebivolol induces distinct changes in profibrosis microRNA expression compared with atenolol, in salt-sensitive hypertensive rats. Hypertension. 2013;61(5):1008–13. [DOI] [PubMed] [Google Scholar]
- 58.Amado-Azevedo J, Reinhard NR, van Bezu J, de Menezes RX, van Beusechem VW, van Nieuw Amerongen GP, et al. A CDC42-centered signaling unit is a dominant positive regulator of endothelial integrity. Sci Rep. 2017;7(1):10132. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Wang C, Zhang Y, Wu Y, Xing D. Developments of CRBN-based PROTACs as potential therapeutic agents. Eur J Med Chem. 2021;225:113749. [DOI] [PubMed] [Google Scholar]
- 60.Roman V, Walstra I, Luiten PG, Meerlo P. Too little sleep gradually desensitizes the serotonin 1A receptor system. Sleep. 2005;28(12):1505–10. [PubMed] [Google Scholar]
- 61.Watts SW, Morrison SF, Davis RP, Barman SM. Serotonin and blood pressure regulation. Pharmacol Rev. 2012;64(2):359–88. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Vila-Pueyo M. Targeted 5-HT(1F) Therapies for Migraine. Neurotherapeutics. 2018;15(2):291–303. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63.Abrahamowicz AA, Ebinger J, Whelton SP, Commodore-Mensah Y, Yang E. Racial and Ethnic Disparities in Hypertension: Barriers and Opportunities to Improve Blood Pressure Control. Curr Cardiol Rep. 2023;25(1):17–27. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.Johnson DA, Jackson CL, Williams NJ, Alcantara C. Are sleep patterns influenced by race/ethnicity - a marker of relative advantage or disadvantage? Evidence to date. Nat Sci Sleep. 2019;11:79–95. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65.Irwin MR. Why sleep is important for health: a psychoneuroimmunology perspective. Annu Rev Psychol. 2015;66:143–72. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66.Buysse DJ. Sleep health: can we define it? Does it matter? Sleep. 2014;37(1):9–17. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67.Dong Q, Gentry NW, McMahon T, Yamazaki M, Benitez-Rivera L, Wang T, et al. Familial natural short sleep mutations reduce Alzheimer pathology in mice. iScience. 2022;25(4):103964. [DOI] [PMC free article] [PubMed] [Google Scholar]