Abstract
BACKGROUND:
The interpretation of ventilator waveforms is essential for effective and safe mechanical ventilation but requires specialized training and expertise. This study aimed to investigate the ability of ICU professionals to interpret ventilator waveforms, identify areas requiring further education and training, and explore the factors influencing their interpretation skills.
METHODS:
We conducted an international online anonymous survey of ICU professionals (physicians, nurses, and respiratory therapists [RTs]), with ≥ 1 y of experience working in the ICU. The survey consisted of demographic information and 15 multiple-choice questions related to ventilator waveforms. Results were compared between professions using descriptive statistics, and logistic regression (expressed as odds ratios [ORs; 95% CI]) was performed to identify factors associated with high performance, which was defined by a threshold of 60% correct answers.
RESULTS:
A total of 1,832 professionals from 31 countries or regions completed the survey; 53% of respondents answered ≥ 60% of the questions correctly. The 3 questions with the most correct responses were related to waveforms that demonstrated condensation (90%), pressure overshoot (79%), and bronchospasm (75%). Conversely, the 3 questions with the fewest correct responses were waveforms that demonstrated early cycle leading to double trigger (43%), severe under assistance (flow starvation) (37%), and early/reverse trigger (31%). Factors significantly associated with ≥ 60% correct answers included years of ICU working experience (≥ 10 y, OR 1.6 [1.2–2.0], P < .001), profession (RT, OR 2.8 [2.1–3.7], P < .001), highest degree earned (graduate, OR 1.7 [1.3–2.2], P < .001), workplace (teaching hospital, OR 1.4 [1.1–1.7], P = .008), and prior ventilator waveforms training (OR 1.7 [1.3–2.2], P < .001).
CONCLUSIONS:
Slightly over half respondents correctly identified ≥ 60% of waveforms demonstrating patient-ventilator discordance. High performance was associated with ≥ 10 years of ICU working experience, RT profession, graduate degree, working in a teaching hospital, and prior ventilator waveforms training. Some discordances were poorly recognized across all groups of surveyed professionals.
Keywords: ICUs, mechanical ventilation, ventilator, patient-ventilator discordance, waveform interpretation
Introduction
Patient-ventilator discordance (PVD) refers to the mismatch between the patient’s respiratory demand and the ventilator settings in terms of timing (trigger and cycle) and support (tidal volume, pressure, flow). PVD can manifests as asynchrony, dyssynchrony, or work shifting between the patient and ventilator.1 PVD can occur at any stage of the respiratory cycle and at any time during the course of mechanical ventilation. Studies have reported varying incidence of PVD in mechanically ventilated subjects, ranging from 10–85%.2-8 Some studies have indicated rates as high as 80–100%,4,9-13 depending on factors such as subject characteristics and the method used to detect PVD.
PVD may increase the risk for ventilator-induced lung and diaphragm injury and worsen patient outcomes. For example, double trigger may lead to alveoli overdistention, potentially causing lung injury. Severe under assistance (flow starvation) results in increased work of breathing and patient discomfort. Early (reverse) trigger might lead to undue stretching of lung tissue, attributable to the Pendelluft effect.14 Additionally, Damiani et al15 found that the combination of reverse trigger with high inspiratory effort was associated with impaired diaphragm function and structure. Higher incidence of PVD has been consistently associated with increased patient discomfort, ventilator days, ICU and hospital length of stay, tracheostomies, morbidity, and mortality.16,17
As a consequence, ICU professionals must identify and address PVD promptly. However, only a small number of ICU professionals demonstrate the ability to accurately recognize abnormal ventilator waveforms.5,16-18 Several studies using videos of PVD reported that professionals recognized only 10–21% of the PVDs present.16-18 Moreover, training has been identified as a significant factor in accurately identifying PVD, whereas occupation and working experience have not consistently shown an association.
Existing studies on PVD recognition were primarily conducted in South America and the Middle East, with few respiratory therapists (RTs) included.16-18 RTs undergo comprehensive education, practical hands-on training in mechanical ventilation, and frequently manage mechanical ventilation in clinical practice. Therefore, the findings of these studies may not apply to regions where RTs play a more substantial role, such as North America, as well as China, where the RT profession has experienced rapid development in recent decades.19-21 Additionally, these studies included a limited number of PVD waveforms, typically ≤ 6.16-18 Consequently, the findings from these studies may not provide a comprehensive reflection of professionals’ ability to recognize PVD across all respiratory cycle phases, nor do they disclose the specific types of PVD that pose genuine challenges to ICU professionals.
We aimed to investigate the ability of ICU professionals, including RTs, physicians, and nurses, to identify the full spectrum of PVD. We aimed to identify specific areas of PVD that need to be targeted in educational programs and explore the factors that may influence the professionals’ ability in waveform interpretation.
QUICK LOOK.
Current knowledge
Patient-ventilator discordance (PVD) can occur in a significant proportion of patients, ranging from 10–85%, and has been associated with adverse outcomes. However, studies assessing ICU professionals’ ability to recognize PVD using video recordings have reported relatively low rates of identification, ranging from 10–21%.
What this paper contributes to our knowledge
Of the 1,832 respondents from 31 countries or regions, slightly over half respondents correctly identified ≥ 60% of waveforms demonstrating PVD. High performance was associated with ≥ 10 years of ICU working experience, RT profession, graduate degree, working in a teaching hospital, and prior ventilator waveforms training. Some discordances were poorly recognized across all groups. To enhance professionals’ ability to interpret ventilator waveforms, it is crucial to implement targeted education and training programs.
Methods
We utilized an online anonymous survey in English and Chinese. The survey was distributed in the United States and China through two popular social media platforms from February 7, 2023–March 2, 2023. First, to reach a sufficient number of ICU professionals, we distributed questionnaires with informative titles emphasizing the research’s purpose and significance via commonly utilized social media platforms on our personal accounts, including Twitter and WeChat. Second, we invited ICU professionals to share the questionnaire on their social media accounts, employing the snowball sampling method.22 Third, to ensure continuous participation, reminders were posted weekly during the participant recruitment period. Lastly, to avoid duplicate responses from the same participant, each account could submit only one questionnaire response. Ethics approval was obtained by the ethics committee at Rush University (approval number 22091302-IRB01). It was deemed exempt from ethical review by the ethics committee at Peking University People’s Hospital in accordance with local regulations.
Study Subjects
ICU professionals, including physicians, nurses, and RTs, were invited to participate in the study if they met the following inclusion criteria: having ≥ 1 y of experience working in the ICU and caring for patients receiving mechanical ventilation in the month preceding the survey. If the respondents did not meet these criteria, the questionnaire would be promptly terminated and considered invalid.
Survey
Following a literature review, we developed the survey used in this study (see related supplementary materials at http://www.rcjournal.com). The survey comprised 3 sections. The first section contained an informed consent form that provided respondents with details about the survey’s objective, estimated completion time, and emphasized their participation’s voluntary and confidential nature. The second section collected demographic information, such as profession, years of ICU working experience, highest education degree, job title, affiliation with a teaching hospital, and whether respondents had received ventilator waveform training. The third section consisted of 15 multiple-choice questions featuring typical PVD waveforms. These waveforms, comprising pressure-time, flow-time, and volume-time scalars, were obtained from mechanically ventilated patients or generated through simulation using a high-fidelity simulator. In some cases, an extra waveform of the electrical activity of the diaphragm (EAdi)-time curve or the esophageal pressure-time curve was included to provide more information to the professional interpreting the waveforms.
The 15 questions focused primarily on the causes of PVD and identification of PVD types, which were categorized using a published taxonomy to identify the PVD,1 and usual terminology was provided in parenthesis if necessary. To comprehensively cover various PVD types, the questions were designed based on the 4 respiratory phases: trigger, inspiration, cycle, and expiration. Trigger discordances included questions on late trigger, false trigger caused by leaks, failed trigger, and early (reverse) trigger. Questions related to the inspiration phase included pressure overshoot, bronchospasm, increased abdominal pressure (decreased compliance), and severe under assistance (flow starvation). Cycle discordances involved late cycle caused by leaks or prolonged inspiratory time, early cycle, and early cycle leading to double trigger. Lastly, questions related to expiration included increased expiratory resistance due to emphysema, increased expiratory limb resistance, and presence of circuit condensation. Each question offered 5 options, including an “I don’t know” choice.
The validity and reliability of the survey were assessed. Six experts in ventilator waveforms were invited to evaluate the content validity, and inter-observer agreement was 100% after several revisions. To evaluate reliability, 10 subjects from each profession (physicians, nurses, and RTs) with varying work experience and education levels were invited to answer the questions twice, with a 2-week interval between completion. The survey demonstrated acceptable internal consistency with Cronbach alpha values of 0.79 and 0.78. The Pearson correlation coefficient between the accuracy of the first and the second survey was 0.83 (P < .001), indicating an excellent test-re-test reliability with high stability.
Translation Process
The translation process adhered to a standardized methodology encompassing 3 fundamental phases.23 Initially, an experienced investigator (JL) with 18 y of practice in respiratory care field, being a native Mandarin speaker and proficient in English, translated the original questionnaire into Mandarin. Subsequently, a professional translation service was engaged to perform the translation from Mandarin back to English. The back translator had no prior knowledge of the study’s objectives and was entirely unfamiliar with mechanical ventilation as a subject matter. The back-translated version and the original questionnaire were linguistically and conceptually similar. The final version was reviewed by 2 RTs (PL and SL) in China.
Statistical Analysis
To evaluate the quality of individual questions and the overall performance of the test, we analyzed the responses provided by ICU professionals for each question using item analyses (University of Washington, Seattle, Washington).24 The average rate of correct responses for each question served as an indicator of its difficulty level. According to item analyses, item difficulty was classified as easy if the correct response rate was ≥ 85%, moderate if it was between 51–84%, and hard if it was ≤ 50%. Additionally, item discrimination was used to evaluate the questions’ discriminative power, which indicates how well the question separates the providers who can identify PVD from those who do not. Questions were classified as having good discrimination if the index was > 0.30, fair if it fell between 0.10–0.30, and poor if it was < 0.10.
Data analysis was performed using SPSS Statistics version 23.0 (IBM, Armonk, New York). Descriptive statistics were used to summarize the results, including mean ± SD for continuous variables and proportions for categorical variables. Differences among professions for continuous variables were assessed using analysis of variance test, while post hoc comparisons within groups were performed using the Games-Howell test. Categorical variables were compared using the chi-square test. A multivariate logistic regression model was employed to identify factors associated with achieving ≥ 60% correct answers. The results were presented as odds ratios (ORs) with corresponding 95% CIs, P values, and the area under the curve of the receiver operating characteristic (ROC) curve. Statistical significance was determined at a P value of < .05.
Results
Survey respondents
A total of 2,323 ICU professionals accessed the survey link to participate in the study. Among them, 491 (21%) professionals were excluded due to various reasons: 399 (17%) had < 1 y of experience in ICU settings; 55 (2%) had not been involved in the management of mechanical ventilation patients in the past month; 31 (1%) declined to participate, and 6 (0.3%) submitted incomplete responses. Ultimately, 1,832 respondents from 31 countries or regions completed valid questionnaires, yielding a completion rate of 79%. The distribution of respondents by profession was as follows: physicians (n = 895, 49%), nurses (n = 436, 24%), and RTs (n = 501, 27%). An overview of the distribution of ICU professionals across different countries or regions is shown in Supplementary Figure S1 (see related supplementary materials at http://www.rcjournal.com). Notably, the respondents were primarily from North America and Asia, where the ratios of physicians to RTs were comparable.
Table 1 presents demographic information of the study respondents. The mean years of ICU working experience were 7.0 ± 5.0 y, and no significant differences were observed among physicians, nurses, and RTs (P = .58). Of the 1,832 respondents, 1,214 (66%) held a bachelor’s degree; 388 (21%) held a master’s degree, and 106 (6%) held a doctorate degree. In terms of the professions, a greater percentage of physicians held graduate degrees (47%) than nurses (4%) and RTs (12%) (P < .001). A significant proportion of ICU professionals (75%) worked in teaching hospitals, with a higher percentage of nurses (83%) working in teaching hospitals compared to physicians (70%) and RTs (77%) (P < .001). The vast majority, 1,718 (94%), worked in adult ICUs, and 1,511 (83%) reported receiving ventilator waveform training. Notably, a higher percentage of RTs (96%) received ventilator waveform training compared to physicians (74%) and nurses (84%) (P < .001).
Table 1.
Respondents’ Demographic Information
Ventilator Waveform Interpretation
Of the 15 questions related to PVD, one question (regarding circuit condensation) was categorized as easy, while 8 questions were determined to possess a moderate level of difficulty, and 6 questions were classified as difficult (see related supplementary materials at http://www.rcjournal.com).
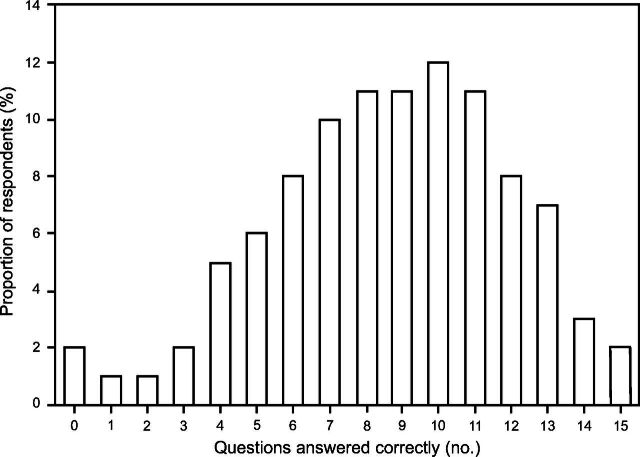
Among respondents, 53% answered ≥ 60% of the questions correctly (Fig. 1); 20% of respondents answered ≥ 80% of the questions correctly. Only 2% of the respondents managed to answer all questions correctly.
Fig. 1.
The percentage of questions answered correctly by the respondents. The x axis represents the number of questions answered correctly by the respondents, ranging from 0–15. The y axis represents the proportion of respondents of the total number. Among all respondents, 2% answered all 15 questions correctly, while 2% did not answer any questions correctly. The remaining respondents fall within different ranges of correct answers, forming a distribution across the x axis.
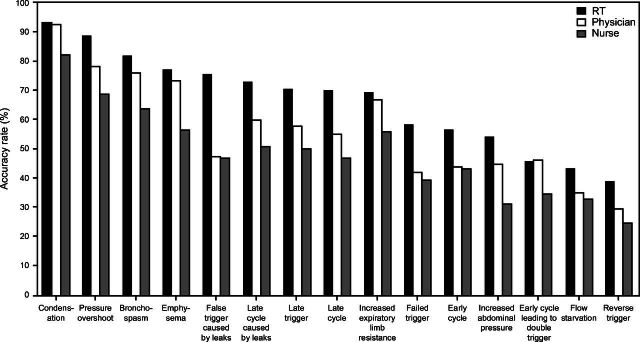
Regarding the questions categorized by respiratory phases, the questions related to expiration had the highest correct responses (68%), followed by those related to inspiration (59%), cycle (52%), and trigger (48%). The 3 questions with the most correct responses were condensation (90%) (supplementary file page 10, see related supplementary materials at http://www.rcjournal.com), pressure overshoot (79%) (supplementary file page 13), and bronchospasm (75%) (supplementary file page 18). Conversely, the 3 questions with the fewest correct responses were early cycle with double trigger (43%) (supplementary file page 21), severe under assistance (flow starvation) (37%) (supplementary file page 15), and early (reverse) trigger (31%) (supplementary file page 22) (Fig. 2). Furthermore, it is noteworthy that both the reverse trigger and late trigger questions exhibited a response trend where > 10% of respondents opted for the “I don’t know” option (Fig. 3).
Fig. 2.
The accuracy rate by the respondents from different professions. RT = respiratory therapist.
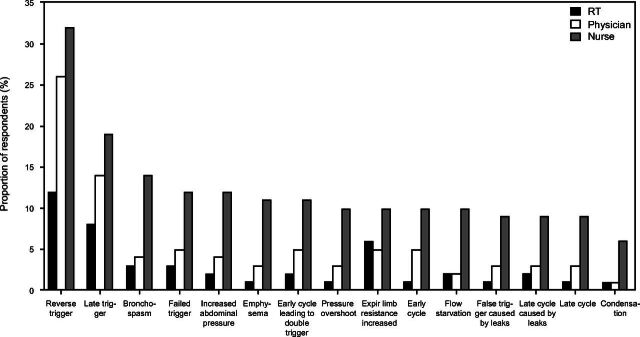
Fig. 3.
Proportion of respondents who chose “I don’t know” RT = respiratory therapist.
Among the 3 professions, RTs and physicians performed similarly in 4 of 15 questions including the early cycle leading to double trigger (46% and 46%, respectively) and the 3 expiratory abnormalities, namely condensation in the circuit (93% and 93%, respectively), emphysema (77% and 73%, respectively), and increased expiratory limb resistance (70% and 67%, respectively), while RTs outperformed physicians in the remaining 11 questions (Fig. 2). When compared to nurses, RTs showed better performance for all 15 questions. Physicians outperformed nurses for 10 questions, particularly in identifying the inspiration discordance (58% and 49%, respectively), cycle discordance (51% and 44%, respectively), and expiration discordance (73% and 65%, respectively). The percentage of respondents who selected “I don’t know” for each question was lowest among RTs and highest among nurses (Fig. 3).
Regarding the performance of professionals across distinct geographical regions, in Asia RTs had higher proportions of correct answers compared to physicians, whereas in North America RTs displayed either comparable or slightly lower percentages of correct answers than physicians (Supplementary Figures S2–S3, see related supplementary materials at http://www.rcjournal.com).
In the multivariable logistic regression model, several factors were found to be significantly associated with respondents’ performance of achieving ≥ 60% correct answers. These factors included years of ICU working experience (≥ 10 y, OR 1.6 [1.2–2.0], P < .001), profession (RT, OR 2.8 [2.1–3.7], P < .001), highest degree obtained (graduate, OR 1.7 [1.3–2.2], P < .001), workplace (teaching hospital, OR 1.4 [1.1–1.7], P = .008), and ventilator waveform training (OR 1.7 [1.3–2.2], P < .001) (Table 2). The multivariable logistic regression model demonstrated an overall accuracy rate of 62% in classifying the survey respondents. The sensitivity and specificity values were 0.64 and 0.60, respectively. The positive and negative predictive values were 0.65 and 0.59, respectively. Additionally, the area under the curve of the model’s ROC curve was 0.67. Upon inclusion of the country in the logistic regression model, we found no statistically significant differences.
Table 2.
Association of Training, Experience, and Profession With the Odds of Identifying ≥ 60% Correct Answers
Discussion
This survey assessed ICU professionals’ abilities to interpret ventilator waveforms. We found (1) among the 1,832 respondents, only 53% answered ≥ 60% of the questions correctly; (2) certain types of discordances were less frequently identified across all groups of respondents; and (3) profession, highest degree, working experience, workplace, and ventilator waveforms training were identified as significant factors affecting the correct identification.
We observed similar rates of correct identification for inspiration and cycle discordance as the prior study,17 and we found similar trigger discordance identification rates as reported in 2 other studies.16,18 However, a significant disparity emerged in trigger discordance when compared to Ramírez II et al,17 who reported trigger discordance as the highest correct response rate (71%). In contrast, we found that trigger discordance had the lowest correct response rate (48%). This discrepancy could be attributed to the inclusion of early (reverse) trigger questions, which had a high difficulty level and good discrimination (0.411) (supplementary file page 28, see related supplementary materials at http://www.rcjournal.com) and might have contributed to the increased difficulty of the trigger discordance questions in our study. However, it is noteworthy that the prevalence of reverse trigger (a type of early trigger) among patients has been reported to range between 3025–50%.26 To address this, we incorporated early (reverse) trigger questions and supplemented them with esophageal pressure-time curves. Despite this measure, reverse trigger still had the lowest rate of correct identification among all PVDs in our study. Moreover, the question pertaining to reverse trigger garnered the highest number of responses opting the choice of “I don’t know.” These findings indicate a persistent lack of understanding regarding reverse trigger.
The incorrect identification of PVD can be attributed to several factors. First, the lack of standardized terminology for describing PVD leads to the use of multiple names for the same type of PVD.1 For instance, premature cycling and short cycling, double trigger and double cycling, reverse trigger and early trigger are all used interchangeably. This inconsistency in terminology causes confusion and hinders accurate identification. Second, the reliance on invasive monitor tools to detect PVD, such as EAdi or esophageal pressure, poses a challenge for accurate identification of certain PVD subtypes like reverse trigger. These tools are limited to specific medical devices, which limits their widespread application in clinical settings. As a result, professionals may lack the tools, experience, and familiarity needed to identify these complex PVD patterns. For instance, in a randomized controlled study in Brazil, Silva et al27 found that the visualization of esophageal pressure in 49 simulated clinical scenarios only increased the sensitivity for PVD detection from 53% to 66% among experienced physicians and RTs. Considering that esophageal manometry provides visualization of the patient effort, this is a rather modest improvement in detection rate and can be attributed to the lack of specific training.
Recognizing and properly managing PVD require extensive clinical experience and specialized training. In line with other studies,16-18 we found that ventilator waveform training was significantly associated with correct identification of PVD. Despite the varying formats, from 1-h lectures to 1-d courses, studies consistently demonstrated that specialized training significantly improved the accuracy of PVD waveform analysis for professionals, particularly those with limited clinical experience.28-32 Previous studies16-18 reported that a significant percentage of ICU professionals, ranging from 29–56%, did not receive waveform training. Although our study observed a decrease in this proportion to 17%, the percentage of accurate responses in some questions remained remarkably low. This suggests that inadequate coverage of all PVD subtypes in training programs, especially challenging patterns, and the effectiveness of the training may contribute to the low accuracy rate. Additionally, a higher degree, such as a graduate degree, emerged as a significant factor correlated with accurate PVD identification. Notably, we did not ask the specific type of graduate degree; whether the types of graduate degree (eg, MSc, MBA, MHC) affect the respondents’ abilities to interpret the waveform remains unknown. Different from previous studies,16-18 we found an impact of other factors including profession (RT), ICU working experience (≥ 10 y), and hospital characteristics (teaching hospital) on the correct recognition of PVD. This discrepancy may be attributed to the larger sample size and the inclusion of more RTs in our study.
Recently, the integration of artificial intelligence (AI) has become an alternative approach to detect PVD.13,33-37 The performance of AI varies depending on the algorithms employed,38 necessitating validation on an independent data set to ensure the generalizability. Additionally, the performance of AI is linked to the subtypes of PVD. For instance, a previous study36 revealed that AI may miss the detection of failed trigger and late trigger combined with late cycle, underscoring the need for comprehensive training on an extensive data set to enhance detection accuracy and reliability. Therefore, whereas AI shows promise in PVD detection, it’s essential to acknowledge the existing limitations and challenges.
Strengths and Limitations
Our study has several strengths. To the best of our knowledge, this is the largest international study of ventilator waveforms interpretation to date, representing several countries. Our respondents were primarily from North America and Asia, which can provide valuable data from regions that were previously underrepresented in the literature.16-18 Additionally, our inclusion of a substantial number of RTs better represents the regions where RTs play a significant role. We provide the item difficulty and discrimination of questions to better calibrate future studies on ventilator waveforms. More importantly, we included the “I don’t know” option in our survey; and by doing so, we might have mitigated any potential response bias stemming from mere speculation or guesswork. Lastly, we comprehensively evaluated PVD identification throughout the entire respiratory cycle. Specifically, we included identification of reverse trigger, late trigger, early cycle, late cycle, and the assessment of respiratory mechanics, which were not assessed in previous studies.16-18
However, our study has several limitations. First, respondents in our study were primarily from North America and Asia, which may limit the generalizability of our findings in other areas. Therefore, further research is warranted to investigate this aspect and provide additional insights. Second, open-ended questions are known to outperform multiple choice format for testing knowledge;39 and respondents in our study could still have guessed answers, although we provided the option of “I don’t know.” It also remains uncertain whether respondents consulted additional resources while answering the questions. Third, we did not specifically include the word physiotherapist in our survey; and by doing so, we may have excluded professionals responsible for ventilator management in certain regions. Therefore, our findings may not directly apply to these regions. Fourth, while we included PVD identification questions, we only included one related to PVD management. Consequently, our findings may not accurately reflect the PVD management abilities of ICU professionals. Lastly, although snowball sampling is particularly useful to locate members of specific populations, participation is voluntary and respondents are not randomly drawn; due to these potential biases, our study findings may not fully represent the entire professionals working in the ICU.
Conclusions
Slightly over half of respondents correctly identified ≥ 60% of waveform questions. Years of ICU working experience, profession, highest degree earned, workplace, and ventilator waveform training were significantly associated with improved interpretation skills. To enhance professionals’ ability in interpreting ventilator waveforms, and improve the safety and comfort of ventilated patients, it is crucial to implement targeted education and training programs, including professional training and continuing professional education. These programs should incorporate standardized nomenclature and specifically address PVD training with emphasis in the most commonly identified errors in ICU professionals.
Supplementary Material
Footnotes
Dr Li discloses relationships with Fisher & Paykel Healthcare, Aerogen, Vincent Medical, the Rice Foundation, the American Association for Respiratory Care, Vincent, and Heyer. Dr Li is a section editor for Respiratory Care. Mr Miller discloses relationships with Saxe Communications, S2N Health, and Fisher & Paykel. Mr Miller is a section editor for Respiratory Care. Dr Mireles-Cabodevila is a co-owner of a patent for mid-frequency ventilation. Dr Mireles-Cabodevila discloses relationships with IngMar Medical and Elsevier. The remaining authors have disclosed no conflicts of interest.
Ms Liu and Lyu contributed equally.
Supplementary material related to this paper is available at http://www.rcjournal.com.
See the Related Editorial on Page 902
REFERENCES
- 1.Mireles-Cabodevila E, Siuba MT, Chatburn RL. A taxonomy for patient-ventilator interactions and a method to read ventilator waveforms. Respir Care 2022;67(1):129-148. [DOI] [PubMed] [Google Scholar]
- 2.Chao DC, Scheinhorn DJ, Stearn-Hassenpflug M. Patient-ventilator trigger asynchrony in prolonged mechanical ventilation. Chest 1997;112(6):1592-1599. [DOI] [PubMed] [Google Scholar]
- 3.Thille AW, Rodriguez P, Cabello B, Lellouche F, Brochard L. Patient-ventilator asynchrony during assisted mechanical ventilation. Intensive Care Med 2006;32(10):1515-1522. [DOI] [PubMed] [Google Scholar]
- 4.de Wit M, Pedram S, Best AM, Epstein SK. Observational study of patient-ventilator asynchrony and relationship to sedation level. J Crit Care 2009;24(1):74-80. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Colombo D, Cammarota G, Alemani M, Carenzo L, Barra FL, Vaschetto R, et al. Efficacy of ventilator waveforms observation in detecting patient-ventilator asynchrony. Crit Care Med 2011;39(11):2452-2457. [DOI] [PubMed] [Google Scholar]
- 6.Alexopoulou C, Kondili E, Plataki M, Georgopoulos D. Patient-ventilator synchrony and sleep quality with proportional assist and pressure support ventilation. Intensive Care Med 2013;39(6):1040-1047. [DOI] [PubMed] [Google Scholar]
- 7.Holanda MA, Vasconcelos RDS, Ferreira JC, Pinheiro BV. Patient-ventilator asynchrony. J Bras Pneumol 2018;44(4):321-333. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Zhou Y, Holets SR, Li M, Cortes-Puentes GA, Meyer TJ, Hanson AC, et al. Etiology, incidence, and outcomes of patient-ventilator asynchrony in critically ill patients undergoing invasive mechanical ventilation. Sci Rep 2021;11(1):12390. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Nava S, Bruschi C, Fracchia C, Braschi A, Rubini F. Patient-ventilator interaction and inspiratory effort during pressure support ventilation in patients with different pathologies. Eur Respir J 1997;10(1):177-183. [DOI] [PubMed] [Google Scholar]
- 10.Blokpoel RGT, Burgerhof JGM, Markhorst DG, Kneyber MCJ. Patient-ventilator asynchrony during assisted ventilation in children. Pediatr Crit Care Med 2016;17(5):e204-e211. [DOI] [PubMed] [Google Scholar]
- 11.Ventre KM. The inscrutable signatures of patient-ventilator asynchrony: all the light we cannot see. Minerva Anestesiol 2021;87(3):278-282. [DOI] [PubMed] [Google Scholar]
- 12.Sousa MLdA, Magrans R, Hayashi FK, Blanch L, Kacmarek RM, Ferreira JC. Predictors of asynchronies during assisted ventilation and its impact on clinical outcomes: the EPISYNC cohort study. J Crit Care 2020;57:30-35. [DOI] [PubMed] [Google Scholar]
- 13.Blanch L, Villagra A, Sales B, Montanya J, Lucangelo U, Luján M, et al. Asynchronies during mechanical ventilation are associated with mortality. Intensive Care Med 2015;41(4):633-641. [DOI] [PubMed] [Google Scholar]
- 14.Yoshida T, Nakamura MAM, Morais CCA, Amato MBP, Kavanagh BP. Reverse triggering causes an injurious inflation pattern during mechanical ventilation. Am J Respir Crit Care Med 2018;198(8):1096-1099. [DOI] [PubMed] [Google Scholar]
- 15.Damiani LF, Engelberts D, Bastia L, Osada K, Katira BH, Otulakowski G, et al. Impact of reverse triggering dyssynchrony during lung-protective ventilation on diaphragm function: an experimental model. Am J Respir Crit Care Med 2022;205(6):663-673. [DOI] [PubMed] [Google Scholar]
- 16.Ramirez II, Arellano DH, Adasme RS, Landeros JM, Salinas FA, Vargas AG, et al. Ability of ICU health care professionals to identify patient-ventilator asynchrony using waveform analysis. Respir Care 2017;62(2):144-149. [DOI] [PubMed] [Google Scholar]
- 17.Ramírez II, Adasme RS, Arellano DH, Rocha ARM, Andrade FMD, Núñez-Silveira J, et al. Identifying and managing patient-ventilator asynchrony: an international survey. Med Intensiva (Engl Ed) 2019;45(3):138-146. [DOI] [PubMed] [Google Scholar]
- 18.Alqahtani JS, AlAhmari MD, Alshamrani KH, Alshehri AM, Althumayri MA, Ghazwani AA, et al. Patient-ventilator asynchrony in critical care settings: national outcomes of ventilator waveform analysis. Heart Lung 2020;49(5):630-636. [DOI] [PubMed] [Google Scholar]
- 19.Arabi YM, Phua J, Koh Y, Du B, Faruq MO, Nishimura M, et al. ; Asian Critical Care Clinical Trials Group. Structure, organization, and delivery of critical care in Asian ICUs. Crit Care Med 2016;44(10):e940-e948. [DOI] [PubMed] [Google Scholar]
- 20.Du B, Xi X, Chen D, Peng J; China Critical Care Clinical Trial Group (CCCCTG). Clinical review: critical care medicine in Mainland China. Crit Care 2010;14(1):206. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Li J, Ni Y, Tu M, Ni J, Ge H, Shi Y, et al. ; Respiratory Care Committee of Chinese Respiratory Disease Society. Respiratory care education and clinical practice in Mainland China. Respir Care 2018;63(10):1239-1245. [DOI] [PubMed] [Google Scholar]
- 22.Goodfellow LT. An overview of survey research. Respir Care 2023;68(9):1309-1313. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Ferrer M, Alonso J, Prieto L, Plaza V, Monsó E, Marrades R, et al. Validity and reliability of the St George’s Respiratory Questionnaire after adaptation to a different language and culture: the Spanish example. Eur Respir J 1996;9(6):1160-1166. [DOI] [PubMed] [Google Scholar]
- 24.University of Washington. Understanding item analyses. Available at: https://www.washington.edu/assessment/scanning-scoring/scoring/reports/item-analysis. Accessed July 11, 2023. [Google Scholar]
- 25.Bourenne J, Guervilly C, Mechati M, Hraiech S, Fraisse M, Bisbal M, et al. Variability of reverse triggering in deeply sedated ARDS patients. Intensive Care Med 2019;45(5):725-726. [DOI] [PubMed] [Google Scholar]
- 26.Rodriguez PO, Tiribelli N, Fredes S, Gogniat E, Plotnikow G, Fernandez Ceballos I, et al. ; Grupo Argentino de Estudio de Asincronías en la Ventilación Mecánica Study Group. Prevalence of reverse triggering in early ARDS: results from a multi-center observational study. Chest 2021;159(1):186-195. [DOI] [PubMed] [Google Scholar]
- 27.Silva DO, de Souza PN, de Araujo Sousa ML, Morais CCA, Ferreira JC, Holanda MA, et al. Impact on the ability of health care professionals to correctly identify patient-ventilator asynchronies of the simultaneous visualization of estimated muscle pressure curves on the ventilator display: a randomized study (Pmus study). Crit Care 2023;27(1):128. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Chacón E, Estruga A, Murias G, Sales B, Montanya J, Lucangelo U, et al. Nurses’ detection of ineffective inspiratory efforts during mechanical ventilation. Am J Crit Care 2012;21(4):e89-e93. [DOI] [PubMed] [Google Scholar]
- 29.Lynch-Smith D, Thompson CL, Pickering RG, Wan JY. Education on patient-ventilator synchrony, clinicians’ knowledge level, and duration of mechanical ventilation. Am J Crit Care 2016;25(6):545-551. [DOI] [PubMed] [Google Scholar]
- 30.Acho M, Kriner E, Sartain NN, Chatterjee S, Sun J, Lee BW, et al. Impact of a mechanical ventilation curriculum on respiratory therapist recognition of patient-ventilator asynchrony. Respir Care 2022;67(12):1597-1602. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Gravante F, Crisci F, Palmieri L, Cecere L, Fusi C, Bulleri E, et al. The impact of a training intervention on detection of patient-ventilator asynchronies in nursing students. Acta Biomed 2022;93(S2):e2022144. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Seam N, Kriner E, Woods CJ, Shah NG, Acho M, McCurdy MT, et al. Impact of novel multi-institutional curriculum on critical care fellow ventilator knowledge. ATS Sch 2020;2(1):84-96. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.de Haro C, López-Aguilar J, Magrans R, Montanya J, Fernández-Gonzalo S, Turon M, et al. ; Asynchronies in the Intensive Care Unit (ASYNICU) Group. Double cycling during mechanical ventilation: frequency, mechanisms, and physiologic implications. Crit Care Med 2018;46(9):1385-1392. [DOI] [PubMed] [Google Scholar]
- 34.Blanch L, Sales B, Montanya J, Lucangelo U, Garcia-Esquirol O, Villagra A, et al. Validation of the Better Care system to detect ineffective efforts during expiration in mechanically ventilated patients: a pilot study. Intensive Care Med 2012;38(5):772-780. [DOI] [PubMed] [Google Scholar]
- 35.Adams JY, Lieng MK, Kuhn BT, Rehm GB, Guo EC, Taylor SL, et al. Development and validation of a multi-algorithm analytic platform to detect off-target mechanical ventilation. Sci Rep 2017;7(1):14980. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Bakkes THGF, Montree RJH, Mischi M, Mojoli F, Turco S. A machine learning method for automatic detection and classification of patient-ventilator asynchrony. Annu Int Conf IEEE Eng Med Biol Soc 2020;2020:150-153. [DOI] [PubMed] [Google Scholar]
- 37.Bakkes T, van Diepen A, De Bie A, Montenij L, Mojoli F, Bouwman A, et al. Automated detection and classification of patient-ventilator asynchrony by means of machine learning and simulated data. Comput Methods Programs Biomed 2023;230:107333. [DOI] [PubMed] [Google Scholar]
- 38.Esperanza JA, Sarlabous L, de Haro C, Magrans R, Lopez-Aguilar J, Blanch L. Monitoring asynchrony during invasive mechanical ventilation. Respir Care 2020;65(6):847-869. [DOI] [PubMed] [Google Scholar]
- 39.Sam AH, Westacott R, Gurnell M, Wilson R, Meeran K, Brown C. Comparing single-best-answer and very-short-answer questions for the assessment of applied medical knowledge in 20 UK medical schools: cross-sectional study. BMJ Open 2019;9(9):e032550. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.