Abstract
Cardiac amyloidosis is a progressive disease characterized by the buildup of amyloid fibrils in the extracellular space of the heart. It is divided in 2 main types, immunoglobulin light chain amyloidosis and transthyretin amyloidosis (ATTR), and ATTR amyloidosis is further divided in 2 subtypes, non-hereditary wild type ATTR and hereditary mutant variant amyloidosis. Incidence and prevalence of ATTR cardiac amyloidosis is increasing over the last years due to the improvements in diagnostic methods. Survival rates are improving due to the development of novel therapeutic strategies. Tafamidis is the only disease-modifying approved therapy in ATTR amyloidosis so far. However, the most recent advances in medical therapies have added more options with the potential to become part of the therapeutic armamentarium of the disease. Agents including acoramidis, eplontersen, vutrisiran, patisiran and anti-monoclonal antibody NI006 are being investigated on cardiac function in large, multicenter controlled trials which are expected to be completed within the next 2-3 years, providing promising results in patients with ATTR cardiac amyloidosis. However, further and ongoing research is required in order to improve diagnostic methods that could provide an early diagnosis, as well as survival and quality of life of these patients.
Keywords: Transthyretin cardiac amyloidosis, Tafamidis, Acoramidis, Eplontersen, Vutrisiran, Patisiran
Core Tip: Transthyretin amyloidosis (ATTR) cardiac amyloidosis is a progressive disease, affecting patients’ functional capacity, survival and quality of life. Incidence and prevalence of ATTR cardiac amyloidosis is increasing over the last years while survival rates are improving. Tafamidis is the only disease-modifying approved therapy so far. Novel medical therapies including acoramidis, eplontersen, vutrisiran, patisiran and anti-monoclonal antibody NI006 are being investigated on cardiac function in large, multicenter controlled trials, with the potential to become part of the therapeutic armamentarium of the disease.
INTRODUCTION
Cardiac amyloidosis is a progressive disease characterized by the buildup of abnormal protein deposits, known as amyloid fibrils, in the extracellular space of the heart[1]. In systemic conditions, protein deposits in the peripheral nervous system can cause peripheral neuropathy, affecting the autonomic nervous system and therefore, blood pressure, heart rate, and cardiac function[1-3]. People with cardiac amyloidosis may have arrhythmias, cardiomegaly, or orthostatic hypertension, abnormalities that lead to progressive heart failure (HF) with increased rates of hospitalizations and mortality[1-3]. The age of the initial symptoms ranges from age 20 years to 70 years, varying widely among individuals[1-3].
Cardiac amyloidosis is divided into 2 main types; immunoglobulin light chain amyloidosis (AL) and transthyretin amyloidosis (ATTR)[2]. ATTR cardiac amyloidosis is further divided into 2 subtypes; non-hereditary wild type ATTR (ATTRwt) amyloidosis and hereditary mutant variant (ATTRv) amyloidosis[3]. Cardiac amyloidosis is a progressive disorder with significantly reduced survival and quality of life with ATTR type presenting a better prognosis than AL[4]. Tafamidis is the only approved disease-modifying therapy for ATTR cardiac amyloidosis so far. However, new experimental therapies are being developed through clinical phases worldwide.
The aim of the present editorial is to present all the recent advances on epidemiology, diagnostic techniques and therapeutic methods in ATTR cardiac amyloidosis.
EPIDEMIOLOGY OF ATTR CARDIAC AMYLOIDOSIS
The AC-TIVE study, a large prospective multicentric study that was conducted in Italy, investigated the prevalence of ATTR cardiac amyloidosis among patients with echocardiographic red flags and evaluated their diagnostic accuracy[5]. The main findings of this trial were that: (1) More than 7% of patients ≥ 55 years of age undergoing clinically-indicated echocardiography and 33% of patients with non-dilated, hypertrophic left ventricle (LV) with preserved ejection fraction (EF) have echocardiographic red-flags of cardiac amyloidosis; (2) Patients with a high echocardiographic suspicion of cardiac amyloidosis (≥ 3 red-flags) represent 1% of patients ≥ 55 years of age undergoing clinically-indicated echocardiography and 5% of patients with cardiac amyloidosis-compatible echocardiograms; (3) Patients with highly cardiac amyloidosis-suggestive echocardiograms are more frequently referred to echocardiographic laboratories due to HF with preserved EF (HFpEF); and (4) Thickened interatrial septal is the most frequent possible echocardiographic red-flag of cardiac amyloidosis[5]. The second phase of the study showed that the prevalence of cardiac amyloidosis was 29% in consecutive adults with echocardiographic findings suggestive of cardiac amyloidosis and LVEF ≥ 50%, while combined echocardiographic red flags usually present good diagnostic accuracy[5]. Similarly, Porcari et al[6] examined mortality rates between ATTR and AL cardiac amyloidosis over a 30-year period in Italy and found that incidence and prevalence rates of ATTR and AL cardiac amyloidosis are much higher the last decade compared to the previous ones, but the 2-year survival of ATTR amyloidosis has improved over the years compared to AL cardiac amyloidosis.
In a large national study in the French territory[7], authors investigated the prevalence and the incidence of ATTR cardiac amyloidosis between 2011 and 2019. Interestingly, incidence rate was increased from 0.6/100000 person-year to 3.6/100000 person-year within 8 years (P < 0.001). Moreover, men were more than women [sex ratios (males/females) increased from 1.52 in 2011 to 2.23 in 2019], as also confirmed from other studies in the French territory[8]. Median age at diagnosis was 85.5 years for women and 83.5 years for men. Finally, survival and prognosis were poor (median survival: 41.9 months [95% confidence interval (CI): (39.6, 44.1)].
A multicenter study in the United States[9] estimated the prevalence and incidence of ATTR cardiomyopathy in 1235 consecutive patients with HFpEF and ventricular wall thickening in southeastern Minnesota. Investigators showed that the prevalence was 2.5% (95%CI: 1.4%-4.0%) in men and 0% (95%CI: 0.0%-0.6%) in women. Moreover, prevalence increased with age from 0% in patients 60 years to 69 years of age to 21% in patients 90 years and older (P < 0.001).
In the United Kingdom, Ravichandran et al[10] obtained data from the United Kingdom National Amyloidosis Center database, identifying 11,006 patients who received a diagnosis of amyloidosis during the period from 1987 until 2019. Patients diagnosed with cardiac amyloidosis increased by 670% while the incidence of ATTRwt amyloidosis increased from less than 3% of all cases in 1987 to 25% in 2019.
In a cohort in Sweden[11], approximately 20% of 2238 HF patients with increased myocardial wall thickness were diagnosed with ATTRwt, estimating the prevalence for the whole population of HF patients at approximately 1.1% and in total population at 1:6000 people. Lauppe et al[12] investigated prevalence of patients with ATTR cardiac amyloidosis in Denmark, Finland, Norway, and Sweden during 2008-2018. The mean average prevalence in Scandinavia was 3.3 per 100000 people in 2018, and most specifically, cases of ATTRwt amyloidosis were higher in Sweden and Norway with 5.0 per 100000 and 3.7 per 100000, respectively, and lower in Finland and Denmark with 1.8 per 100000 and 1.4 per 100000, respectively. Prevalence increased in all of them during the following years. As far as sex is concerned, female patients were 20.3% in Denmark, 24.4% in Norway, 29.9% in Sweden, and 49.5% in Finland while overall, in the Nordic countries, 31.0% of patients were female[12]. Finally, median survival time after ATTR cardiac amyloidosis diagnosis was 25 (CI: 21-30) months in Denmark, 18 (CI: 16-22) months in Finland, 28 (CI: 25-36) months in Norway, and 37 (34-44) months in Sweden.
Finally, Ney et al[13] conducted a large retrospective study in Germany from 2009 to 2018, using health claims data of a statutory health insurance. Both prevalence and incidence increased from 15.5 to 47.6 per 100000 person-years and from 4.8 to 11.6 per 100000 person-years, respectively. Risk of death reduced by 9% (95%CI: 2%-15%, P = 0.008) in the second compared to the first 5 years of observation.
It seems clear that the incidence and prevalence of ATTR cardiac amyloidosis have significantly increased over time[5-13], due to advancements in non-invasive imaging techniques and heightened clinical awareness. This rise may also be influenced by the aging population, as the diagnosis is more prevalent in older adults. As a result, ATTR cardiac amyloidosis is now considered a critical factor in HF among the elderly, necessitating ongoing research and development of targeted therapies.
CURRENT GUIDELINES AND RECCOMENDATIONS IN DIAGNOSTIC METHODS
ATTR cardiac amyloidosis is a progressive and fatal condition without early diagnosis, leading to cardiomyopathy and end-stage cardiac failure. The main problems in the disease’s diagnosis are the increased number of misdiagnosed[14] and underdiagnosed cases[15], as well as the lack of awareness of this disease among healthcare professionals and the community in the United Kingdom and the United States[16,17], countries of South America[18], countries in the Middle East and Gulf Region[19], as well as European countries[20,21].
Diagnosis of cardiac amyloidosis includes two critical phases, the suspicious and the definite diagnosis phase[22]. The diagnostic process of ATTR cardiac amyloidosis begins with clinical history/examination, electrocardiogram (ECG), and transthoracic echocardiogram[3]. Cardiac magnetic resonance (CMR) imaging and endomyocardial biopsy are the diagnostic methods with the highest sensitivity and specificity that may be required in order to make the diagnosis[3].
ECG and echocardiography are primary diagnostic tools which can practically set the initial suspicions of cardiac amyloidosis[23]. Specifically, increased LV wall thickness with low-voltage QRS[24], the lack of progression of the R wave in the anterior precordial leads[25], left ventricular hypertrophy (LVH) morphology[26], and conduction defects including atrioventricular (AV) or bundle branch block and conduction delay[27] seem to be the most characteristic findings in the ECG so far. Ventricular tachycardia and ventricular fibrillation are those arrhythmias which can lead to sudden death in patients with ATTR amyloidosis[27]. However, the absence of these findings does not exclude the diagnosis[28]. The new insight in the ECG is the development of novel machine learning techniques with specific ECG algorithms which use patterns from detailed electroanatomic mappings of patients with cardiac amyloidosis[29]. Echocardiography includes standard diagnostic clues such as increased LV wall thickness (≥ 1.2 cm), thickening of AV valves, right ventricle free wall and interatrial septum, diastolic dysfunction, decreased mitral annular systolic velocity, enlargement of both atrials, and decreased global longitudinal strain with relative apical sparing[22,30-32]. However, neither this technique can set the diagnosis alone. Machine learning techniques combining ECG and echocardiography could present promising results in detecting ATTR cardiac amyloidosis in early stages, as shown through a large multicenter study where the machine learning model combining ECG and echo was capable to detect cardiac amyloidosis 1 year before diagnosis, and discriminate it from other differential diagnoses causing LVH[33].
CMR provides detailed cardiac tissue characterization and it is very useful in excluding amyloidosis from other diagnoses. The most characteristic findings are expansion of the extracellular volume, abnormal gadolinium contrast kinetics, and diffuse late gadolinium enhancement[30,31]. However, CMR has also disadvantages as it is not sufficient to establishing the diagnosis of cardiac amyloidosis alone, and cannot distinguish between AL and ATTR cardiac amyloidosis without endomyocardial biopsy[34].
Cardiac scintigraphy with intravenous injection of pyrophosphate, followed by the acquisition of planar and single-photon emission computed tomography (SPECT) or SPECT images after 1 and 3 hours, is considered as a cornerstone of ATTR amyloidosis diagnosis, especially in the absence of a monoclonal protein screen comprising 3 laboratory tests: Serum immunofixation electrophoresis (SIFE), urine immunofixation electrophoresis (UIFE) and serum free light chain (sFLC) assay[35,36]. Diagnostic criteria for positive planar scintigraphy include a Perugini score ≥ 2, and/or a heart/contralateral chest ratio ≥ 1.5 on a 1-hour scan or > 1.3 on a 3 hours scan[22,32,37,38]. In patients with suspected cardiac amyloidosis and an abnormal monoclonal protein screen, endomyocardial biopsy may be required to establish the diagnosis.
Finally, genetic testing for the presence or absence of a transthyretin (TTR) variant in the patient via TTR gene sequencing, in combination with genetic counseling and cascade testing of at-risk relatives, can distinguish ATTRv from ATTRwt, therefore, defining the appropriate treatment strategy[3].
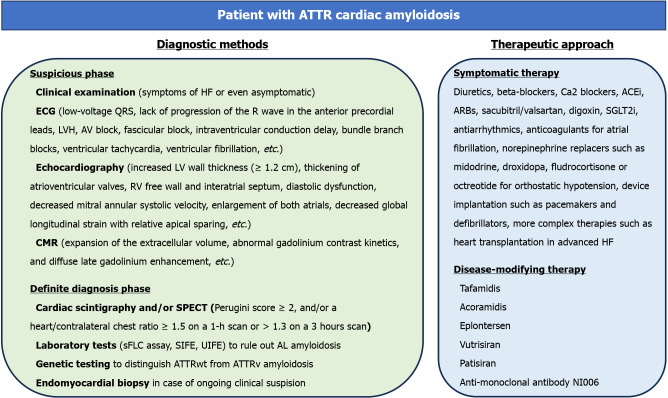
The appropriate diagnostic steps of ATTR cardiac amyloidosis after clinical or ECG/echo suspicions (Figure 1), according to the most updated recommendations are[3,22]: (1) Exclusion of AL amyloidosis by the absence of a monoclonal protein screen comprising sFLC assay, SIFE, and UIFE, with a negative predictive value of > 99%, or establishment of the diagnosis if present[32,35,37,38]; (2) Bone avid tracer scintigraphy to assess for ATTR amyloidosis and, if positive and grade 2 or 3 then TTR genetic testing so that to distinguish ATTRv from ATTRwt amyloidosis[2], or (3) Endomyocardial biopsy if there is ongoing clinical suspicion of cardiac amyloidosis including findings in the ECG, echocardiography and CMR, and low suspicion in the bone avid tracer scintigraphy[2].
Figure 1.
Diagnostic approach and therapeutic strategies in transthyretin amyloidosis cardiac amyloidosis. ACEi: Angiotensin-converting enzyme inhibitors; AL: Immunoglobulin light chain amyloidosis; ARBs: Angiotensin receptor blockers; ATTR: Transthyretin amyloidosis; ATTRv: Mutant variant transthyretin amyloidosis; ATTRwt: Wild type transthyretin amyloidosis; AV: Atrioventricular; CMR: Cardiac magnetic resonance; ECG: Electrocardiogram; HCL: Heart/contralateral; HF: Heart failure; LV: Left ventricular; LVH: Left ventricular hypertrophy; RV: Right ventricular; sFLC: Serum free light chain; SGLT2i: Sodium-glucose cotransporter-2 inhibitors; SIFE: Serum immunofixation electrophoresis; SPECT: Single-photon emission computed tomography; UIFE: Urine immunofixation electrophoresis.
NEW INSIGHTS INTO THERAPEUTIC ARMAMENTARIUM OF ATTR CARDIAC AMYLOIDOSIS
Treatment management of ATTR cardiac amyloidosis is focused in either the symptoms of the clinical syndrome or its modification[22]. Classic symptom therapy may include HF medication such as diuretics, beta-blockers and calcium channel blockers, angiotensin-converting enzyme inhibitors, angiotensin II receptor blocker and sacubitril/valsartan, digoxin, sodium-glucose cotransporter type 2 inhibitors, antiarrhythmic treatment and anticoagulant therapy for atrial fibrillation, norepinephrine replacers such as midodrine, droxidopa, fludrocortisone or octreotide for orthostatic hypotension, device implantation such as pacemakers and defibrillators, and more complex therapies such as heart transplantation in advanced HF[2]. Disease-modifying therapy includes drugs that act on different phases of amyloidogenesis: (1) Silencing of the gene encoding TTR (small interfering RNA: Patisiran, vutrisiran; antisense oligonucleotides: Inotersen, eplontersen; new CRISPR Cas-9 drug technology for editing in vivo DNA); (2) Stabilization of circulating TTR to inhibit its dissociation and subsequent assembly of the resulting monomers in amyloidotic fibrils (tafamidis, acoramidis, and tolcapone), and (3) Destruction and re-absorption of already formed amyloid tissue deposits (monoclonal antibodies)[39].
The only approved medication for ATTR cardiac amyloidosis by the United States Food and Drug Administration (FDA) so far, is tafamidis at a dosage of 61 mg or tafamidis meglumine of 80 mg. Tafamidis acts as a TTR stabilizer, slowing the dissociation of TTR, and prevents amyloidogenesis and cardiac deposition by binding to transthyretin[3]. The beneficial effects of tafamidis were demonstrated through a large clinical trial in 2018, the ATTR-ACT trial (Tafamidis in Transthyretin Cardiomyopathy Clinical Trial)[40]. In this multicenter, international, double-blind, placebo-controlled, phase 3 trial, authors randomly assigned 441 patients with ATTR cardiomyopathy in a 2:1:2 ratio to receive 80 mg of tafamidis, 20 mg of tafamidis, or placebo for 30 months and assessed all-cause mortality, cardiovascular (CV)-related hospitalizations, changes in the 6-minute walk test and the score on the Kansas City Cardiomyopathy Questionnaire (KCCQ)-Overall Summary. Patients who received tafamidis presented lower all-cause mortality [78 of 264 (29.5%) vs 76 of 177 (42.9%); hazard ratio: 0.70; 95%CI: 0.51-0.96] and lower rates of CV-related hospitalizations [relative risk ratio 0.68 (0.48 per year vs 0.70 per year; 95%CI: 0.56-0.81)] compared to placebo. Moreover, tafamidis was associated with reduction in the decline of functional capacity and quality of life in these patients[41]. Benefits from tafamidis in mortality and functional decline are regardless of ATTR status, as shown by a subsequent analysis of the ATTR-ACT trial[42]. Moreover, Elliot et al[43] showed that patients initially treated with tafamidis in the ATTR-ACT trail, had better long-term survival up to 58 months than patients who were initially treated with placebo. As far as safety profile of tafamidis is concerned, adverse events were mild to moderate in severity[40], while monitoring is usually not necessary in the clinical environment.
The new insights in ATTR cardiac amyloidosis include promising targeted medical therapies which are being investigated in significant clinical trials (Table 1). Specifically, acoramidis, a novel TTR stabilizer, has currently been investigated in a phase 3 clinical trial, the ATTRIBUTE-CM trial[44]. In this double-blind trial, authors randomly assigned patients with ATTR cardiomyopathy in a 2:1 ratio to receive acoramidis hydrochloride at a dose of 800 mg twice daily or matching placebo for 30 months and evaluated 4 main outcomes; death from any cause, CV-related hospitalization, the change from baseline in the N-terminal pro-B-type natriuretic peptide (NT-proBNP) level, and the change from baseline in the 6-minute walk distance. Moreover, the score on the KCCQ-Overall Summary, and the serum TTR level were also evaluated. Acoramidis resulted in significantly improved rates of mortality, morbidity, and function compared to placebo [win ratio: 1.8 (95%CI: 1.4-2.2; P < 0.001), while adverse events were similar between the two groups (98.1% vs 97.6%, respectively][44]. The new insight in the treatment of cardiac amyloidosis is that the FDA has accepted a New Drug Application for acoramidis for the treatment of transthyretin amyloid cardiomyopathy and set a Prescription Drug User Fee Act action date of November 29, 2024.
Table 1.
Novel promising targeted medical therapies of transthyretin amyloidosis cardiac amyloidosis which are being investigated in large clinical trials
|
Clinical trial
|
Intervention per group
|
Duration
|
Endpoints
|
Outcomes
|
| ATTR-ACT NCT01994889 | I1: 80 mg of tafamidis; I2: 20 mg of tafamidis; C: Placebo | 30 months | Primary: All-cause mortality; Frequency of CV-related hospitalizations. Secondary: 6MWT; KCCQ-OS; CV-related mortality; Stabilized TTR after 1 month | Tafamidis was associated with: (1) Lower all-cause mortality than placebo [78 of 264 (29.5%) vs 76 of 177 (42.9%); HR, 0.70; 95%CI: 0.51-0.96]; (2) Lower rate of cardiovascular-related hospitalizations [relative risk ratio of 0.68 (0.48 per year vs 0.70 per year; 95%CI: 0.56-0.81)]; (3) Lower rate of decline in distance for the 6-minute walk test (P < 0.001); (4) Lower rate of decline in KCCQ-OS score (P < 0.001); and (5) Similar incidence and types of adverse events between groups |
| ATTRIBUTE-CM NCT03860935 | I: 800 mg of acoramidis BID; C: Placebo | 30 months | Primary: (1) 6MWT after 12 months; (2) All-cause mortality; (3) CV-related hospitalizations; (4) NT-proBNP; (5) 6MWT after 30 months; and (6) KCCQ-OS | (1) All-cause mortality, cumulative frequency of CV-related hospitalization, change in NT-proBNP, and change in 6-6MWT, had an overall win ratio favoring acoramidis (win ratio 1.8, 95%CI: 1.4-2.2, P < 0.0001); (2) All-cause mortality: 25.7% vs 29.5%; HR: 0.77, 95%CI: 0.54-1.10 (P = 0.15); (3) Adjusted mean factor change in NT-proBNP from baseline: 0.529 (95%CI: 0.46-0.60, P < 0.05); (4) Improvement from baseline in 6-minute walk distance: 39.6 m (95%CI: 21.1-58.2, P < 0.001); (5) CV-related hospitalization: 26.7% vs 42.6% (P < 0.0001); (6) Least means square change in KCCQ-OS: 9.94 points (95%CI: 5.97-13.91, P < 0.001); and (7) Composite of all-cause mortality and CV-related hospitalization: HR: 0.65, 95%CI: 0.50-0.83 (P = 0.0008; number needed to treat = 7) |
| CARDIO-TTRansfor NCT04136171 | I: Eplontersen (sc) once every 4 weeks; C: Placebo | 140 weeks | Primary: CV mortality and recurrent CV clinical events up to week 140. Secondary: 6MWT at week 121; KCCQ at week 121; all-cause mortality up to week 140 | The trial is estimated to be completed by 2025 |
| HELIOS-B NCT04153149 |
I: 25 mg of vutrisiran (sc) once every 3 months C: Placebo |
30-36 months | Primary: All-cause mortality and recurrent CV clinical events at 30-36 months. Secondary: (1) 6MWT at month 30; (2) KCCQ at month 30; (3) Mean (LV) wall thickness at month 30; (4) GLS at month 30; (5) All-cause mortality; (6) Recurrent all-cause hospitalizations and urgent HF visits; and (7) NTproBNP at month 30 | The trial is estimated to be completed by 2026 |
| APOLLO-B NCT03997383 | I: 0.3 mg/kg of patisiran once every 3 weeks; C: Placebo | 12 months | Primary: 6MWT. Secondary: (1) KCCQ-OS; (2) Composite of death from any cause, CV events, and 6MWT; and (3) Composite of death from any cause, hospitalizations for any cause, and urgent HF visits | Patisiran was associated with: (1) Lower decline in the 6MWT (Hodges-Lehmann estimate of median difference, 14.69 m; 95%CI: 0.69-28.69; P = 0.02); (2) Increase of the KCCQ-OS (least-squares mean difference, 3.7 points; 95%CI: 0.2-7.2; P = 0.04); and (3) Infusion-related reactions, arthralgia, and muscle spasms more often in the patisiran group compared to placebo |
| NI006 phase 1 NCT04360434 | I: 0.3 to 60 mg/kg of NI006 IV every 4 weeks; C: Placebo | 4 months | Safety and pharmacokinetic profile; Cardiac imaging studies | NI006 was associated with no apparent drug-related serious adverse events in this phase 1 trial |
6MWT: 6-minute walk test; BID: Bis in die; C: Control group; CI: Confidence interval; CV: Cardiovascular; GLS: Global longitudinal strain; HF: Heart failure; HR: Hazard ratio; I: Intervention group; IV: Intravenous; KCCQ-OS: Kansas City Cardiomyopathy Questionnaire Overall Summary; LV: Left ventricular; NTproBNP: N-terminal prohormone B-type Natriuretic Peptide; SC: Subcutaneous; TTR: Transthyretin.
Eplontersen, a TTR silencer and antisense oligonucleotide, has also been assessed on cardiac structure and function in the NEURO-TTRansform trial[45]. This trial involved 144 adults with ATTRv polyneuropathy receiving eplontersen throughout and compared with a historical placebo group. Sixty-five weeks of eplontersen treatment was associated with improved LVEF by 4.3% (95%CI 1.40-21.01; P = 0.049) and stroke volume by 10.64 mL (95%CI 3.99-17.29; P = 0.002) while the remainder of echocardiographic parameters remained stable. Eplontersen’s effect on ATTR cardiomyopathy is being investigated in a global, double-blind, randomized, placebo-controlled Phase 3 CV outcome study in more than 1400 patients, the CARDIO-TTRansform trial (NCT04136171). This trial investigates CV mortality and recurrent CV clinical events up to week 140, change in the 6-minute walk test, the KCCQ scores at week 121, and the rates of CV mortality, CV clinical events and all-cause mortality at week 140 (NCT04136171). The trial is estimated to be completed by 2025.
Another targeted agent under investigation is vutrisiran, a TTR silencer and a small interfering RNA. HELIOS-B, a phase 3, randomized, double-blind, placebo-controlled, multicenter study will evaluate the efficacy and safety of vutrisiran 25 mg administered subcutaneously once every 3 months compared to placebo in patients with ATTR amyloidosis (NCT04153149). The major endpoints are all-cause mortality, recurrent CV events, CV hospitalizations and urgent HF visits at 30-36 months. Other endpoints are changes in the 6-minute walk test, the KCCQ Overall Summary, mean LV wall thickness by echocardiographic assessment, global longitudinal strain and NT-proBNP. The trial is estimated to be completed by 2026. However, an exploratory analysis with data from the HELIOS-A clinical trial[46] demonstrated evidence of the potential benefit of vutrisiran on cardiac manifestations in patients with ATTRv amyloidosis with polyneuropathy, with an acceptable safety profile. Specifically, vutrisiran showed improvements on NT-proBNP and echocardiographic parameters after 18 months compared to external placebo of the APOLLO study.
Patisiran is a molecule encapsulated in lipid nanoparticles, administered by intravenous infusion, and internalized specifically by hepatocytes, which was investigated in ATTR cardiac amyloidosis[47]. APOLLO-B trial (NCT03997383), a phase 3, double-blind, randomized trial, randomized patients with ATTRv or ATTRwt cardiac amyloidosis, in a 1:1 ratio, to receive patisiran (0.3 mg per kilogram of body weight) or placebo once every 3 weeks for 12 months. Authors assessed changes in the KCCQ-Overall Summary score, death from any cause, CV events, changes in the 6-minute walk test distance, hospitalizations for any cause, and urgent HF visits over 12 months. They concluded that patisiran was associated with a lower decline in the 6-minute walk distance (Hodges-Lehmann estimate of median difference, 14.69 m; 95%CI: 0.69-28.69; P = 0.02) and increased KCCQ-Overall Summary score (least-squares mean difference, 3.7 points; 95%CI: 0.2-7.2; P = 0.04) compared to the placebo.
Finally, anti-monoclonal antibody NI006 (ALXN2220), a recombinant human anti-ATTR antibody that was developed for the removal of ATTR by phagocytic immune cells, has been evaluated in a phase 1, double-blind trial in 40 patients with ATTRv or ATTRwt cardiomyopathy and chronic HF[48]. Authors compared intravenous infusions of either NI006 or placebo every 4 weeks for 4 months, assessing safety and pharmacokinetic profiles, and showed that the use of NI006 was associated with no apparent drug-related serious adverse events. Additionally, it seemed to reduce surrogate markers of cardiac amyloid load from scintigraphy and CMR imaging, median NT-proBNP and troponin T levels over a period of 12 months.
LIMITATIONS AND FUTURE PERSPECTIVES
Due to limited data in ATTR cardiac amyloidosis, more randomized controlled trials are required in order to demonstrate better diagnostics methods and more efficient therapeutic options. Although there are guidelines for cardiac amyloidosis management, there are still gaps in the awareness of this disease. The existing diagnostic methods cannot provide early diagnosis yet. It is characteristic that for ATTRwt amyloidosis, median time from symptoms to diagnosis remains similar during the last few years[49]. Therapeutically, the only disease-modifying therapy of ATTR-cardiomyopathy, tafamidis, is not available in most countries all over the world, even highly developed ones, due mainly to its high cost[50], resulting in missed opportunity for timely treatment or even no treatment in most patients.
There is need for educational programs and campaigns regarding cardiac amyloidosis in the future, in order to increase clinical awareness and early diagnosis, so that patients receive timely treatment[18]. It has been shown that healthcare professionals would benefit from information on the latest advances in ATTR cardiac amyloidosis as far as screening, diagnosis and therapy of patients is concerned[21]. Moreover, the development of cardiac amyloidosis networks and reference centers all over the world, as well as the creation of registries including patients’ demographics, clinical, imaging and laboratory exams, and medication, would also be helpful to increase scientific knowledge of this disease. The development and establishment of novel, more efficient therapeutic options would increase functional capacity, limit symptoms, improve prognosis, survival and, therefore, improve quality of life in patients with ATTR cardiac amyloidosis.
CONCLUSION
It seems that incidence and prevalence of ATTR cardiac amyloidosis is increasing over the last few years and patients who remained undiagnosed, are finally being diagnosed, probably due to the improvements in sensitivity of diagnostic methods and imaging techniques. Moreover, survival rates are getting higher due to the development of therapeutic strategies. Awareness of this disease still remains at low levels among healthcare professionals and within the community, but, with increasing trends during the last decade. The most recent advances in medical therapies have added more options with potential to become part of the therapeutic armamentarium of ATTR amyloidosis. However, tafamidis, as well as other potential disease modifying treatments, are widely unavailable in most countries due to their high cost, resulting in missed opportunities for timely treatment in most patients. Further and ongoing research is required in order to improve survival and quality of life for these patients.
Footnotes
Conflict-of-interest statement: The authors have no conflicts of interest to declare.
Provenance and peer review: Invited article; Externally peer reviewed.
Peer-review model: Single blind
Specialty type: Cardiac and cardiovascular systems
Country of origin: Greece
Peer-review report’s classification
Scientific Quality: Grade B
Novelty: Grade C
Creativity or Innovation: Grade C
Scientific Significance: Grade B
P-Reviewer: Castro J S-Editor: Qu XL L-Editor: Filipodia P-Editor: Yuan YY
Contributor Information
Christos Kourek, Clinical Ergospirometry, Exercise and Rehabilitation Laboratory, 1st Critical Care Medicine Department, Evangelismos Hospital, National and Kapodistrian University of Athens, Athens 10676, Greece.
Alexandros Briasoulis, Department of Clinical Therapeutics, Alexandra Hospital, Faculty of Medicine, National and Kapodistrian University of Athens, Athens 11528, Greece.
Dimitrios E Magouliotis, Department of Cardiothoracic Surgery, University of Thessaly, Larissa Biopolis, Larissa 41110, Greece.
Panagiotis Georgoulias, Department of Nuclear Medicine, University Hospital of Larissa, Larissa 41110, Greece.
Grigorios Giamouzis, Department of Cardiology, School of Medicine, University Hospital of Larissa, Larissa 41110, Greece.
Filippos Triposkiadis, Department of Cardiology, School of Medicine, University Hospital of Larissa, Larissa 41110, Greece.
John Skoularigis, Department of Cardiology, School of Medicine, University Hospital of Larissa, Larissa 41110, Greece.
Andrew Xanthopoulos, Department of Cardiology, School of Medicine, University Hospital of Larissa, Larissa 41110, Greece. andrewvxanth@gmail.com.
References
- 1.Rossi M, Varrà GG, Porcari A, Saro R, Pagura L, Lalario A, Dore F, Bussani R, Sinagra G, Merlo M. Re-Definition of the Epidemiology of Cardiac Amyloidosis. Biomedicines. 2022;10 doi: 10.3390/biomedicines10071566. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Brito D, Albrecht FC, de Arenaza DP, Bart N, Better N, Carvajal-Juarez I, Conceição I, Damy T, Dorbala S, Fidalgo JC, Garcia-Pavia P, Ge J, Gillmore JD, Grzybowski J, Obici L, Piñero D, Rapezzi C, Ueda M, Pinto FJ. World Heart Federation Consensus on Transthyretin Amyloidosis Cardiomyopathy (ATTR-CM) Glob Heart. 2023;18:59. doi: 10.5334/gh.1262. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Writing Committee. Kittleson MM, Ruberg FL, Ambardekar AV, Brannagan TH, Cheng RK, Clarke JO, Dember LM, Frantz JG, Hershberger RE, Maurer MS, Nativi-Nicolau J, Sanchorawala V, Sheikh FH. 2023 ACC Expert Consensus Decision Pathway on Comprehensive Multidisciplinary Care for the Patient With Cardiac Amyloidosis: A Report of the American College of Cardiology Solution Set Oversight Committee. J Am Coll Cardiol. 2023;81:1076–1126. doi: 10.1016/j.jacc.2022.11.022. [DOI] [PubMed] [Google Scholar]
- 4.Gillmore JD, Damy T, Fontana M, Hutchinson M, Lachmann HJ, Martinez-Naharro A, Quarta CC, Rezk T, Whelan CJ, Gonzalez-Lopez E, Lane T, Gilbertson JA, Rowczenio D, Petrie A, Hawkins PN. A new staging system for cardiac transthyretin amyloidosis. Eur Heart J. 2018;39:2799–2806. doi: 10.1093/eurheartj/ehx589. [DOI] [PubMed] [Google Scholar]
- 5.Merlo M, Porcari A, Pagura L, Cameli M, Vergaro G, Musumeci B, Biagini E, Canepa M, Crotti L, Imazio M, Forleo C, Cappelli F, Favale S, Di Bella G, Dore F, Lombardi CM, Pavasini R, Rella V, Palmiero G, Caiazza M, Albanese M, Guaricci AI, Branzi G, Caponetti AG, Saturi G, La Malfa G, Merlo AC, Andreis A, Bruno F, Longo F, Sfriso E, Di Ienno L, De Carli G, Giacomin E, Spini V, Milidoni A, Limongelli G, Autore C, Olivotto I, Badano L, Parati G, Perlini S, Metra M, Emdin M, Rapezzi C, Sinagra G. A national survey on prevalence of possible echocardiographic red flags of amyloid cardiomyopathy in consecutive patients undergoing routine echocardiography: study design and patients characterization - the first insight from the AC-TIVE Study. Eur J Prev Cardiol. 2022;29:e173–e177. doi: 10.1093/eurjpc/zwab127. [DOI] [PubMed] [Google Scholar]
- 6.Porcari A, Allegro V, Saro R, Varrà GG, Pagura L, Rossi M, Lalario A, Longo F, Korcova R, Dal Ferro M, Perkan A, Dore F, Bussani R, De Sabbata GM, Zaja F, Merlo M, Sinagra G. Evolving trends in epidemiology and natural history of cardiac amyloidosis: 30-year experience from a tertiary referral center for cardiomyopathies. Front Cardiovasc Med. 2022;9:1026440. doi: 10.3389/fcvm.2022.1026440. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Damy T, Bourel G, Slama M, Algalarrondo V, Lairez O, Fournier P, Costa J, Pelcot F, Farrugia A, Zaleski ID, Lilliu H, Rault C, Bartoli M, Fievez S, Granghaud A, Rudant J, Coste A, Cosson CN, Squara PA, Narbeburu M, De Neuville B, Charron P. Incidence and survival of transthyretin amyloid cardiomyopathy from a French nationwide study of in- and out-patient databases. Orphanet J Rare Dis. 2023;18:345. doi: 10.1186/s13023-023-02933-w. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Adams D, Cintas P, Solé G, Tard C, Labeyrie C, Echaniz-Laguna A, Cauquil C, Pereon Y, Magy L, Morales RJ, Antoine JC, Lagrange E, Petiot P, Mallaret M, Francou B, Guiochon-Mantel A, Coste A, Demarcq O, Geffroy C, Famelart V, Rudant J, Bartoli M, Donal E, Lairez O, Eicher JC, Kharoubi M, Oghina S, Trochu JN, Inamo J, Habib G, Roubille F, Hagège A, Morio F, Cariou E, Adda J, Slama MS, Charron P, Algalarrondo V, Damy T, Attarian S. Transthyretin amyloid polyneuropathy in France: A cross-sectional study with 413 patients and real-world tafamidis meglumine use (2009-2019) Rev Neurol (Paris) 2024 doi: 10.1016/j.neurol.2024.02.393. [DOI] [PubMed] [Google Scholar]
- 9.AbouEzzeddine OF, Davies DR, Scott CG, Fayyaz AU, Askew JW, McKie PM, Noseworthy PA, Johnson GB, Dunlay SM, Borlaug BA, Chareonthaitawee P, Roger VL, Dispenzieri A, Grogan M, Redfield MM. Prevalence of Transthyretin Amyloid Cardiomyopathy in Heart Failure With Preserved Ejection Fraction. JAMA Cardiol. 2021;6:1267–1274. doi: 10.1001/jamacardio.2021.3070. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Ravichandran S, Lachmann HJ, Wechalekar AD. Epidemiologic and Survival Trends in Amyloidosis, 1987-2019. N Engl J Med. 2020;382:1567–1568. doi: 10.1056/NEJMc1917321. [DOI] [PubMed] [Google Scholar]
- 11.Lindmark K, Pilebro B, Sundström T, Lindqvist P. Prevalence of wild type transtyrethin cardiac amyloidosis in a heart failure clinic. ESC Heart Fail. 2021;8:745–749. doi: 10.1002/ehf2.13110. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Lauppe R, Liseth Hansen J, Fornwall A, Johansson K, Rozenbaum MH, Strand AM, Väkeväinen M, Kuusisto J, Gude E, Smith JG, Gustafsson F. Prevalence, characteristics, and mortality of patients with transthyretin amyloid cardiomyopathy in the Nordic countries. ESC Heart Fail. 2022;9:2528–2537. doi: 10.1002/ehf2.13961. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Ney S, Ihle P, Ruhnke T, Günster C, Michels G, Seuthe K, Hellmich M, Pfister R. Epidemiology of cardiac amyloidosis in Germany: a retrospective analysis from 2009 to 2018. Clin Res Cardiol. 2023;112:401–408. doi: 10.1007/s00392-022-02114-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Adams D, Gonzalez-Duarte A, O'Riordan WD, Yang CC, Ueda M, Kristen AV, Tournev I, Schmidt HH, Coelho T, Berk JL, Lin KP, Vita G, Attarian S, Planté-Bordeneuve V, Mezei MM, Campistol JM, Buades J, Brannagan TH 3rd, Kim BJ, Oh J, Parman Y, Sekijima Y, Hawkins PN, Solomon SD, Polydefkis M, Dyck PJ, Gandhi PJ, Goyal S, Chen J, Strahs AL, Nochur SV, Sweetser MT, Garg PP, Vaishnaw AK, Gollob JA, Suhr OB. Patisiran, an RNAi Therapeutic, for Hereditary Transthyretin Amyloidosis. N Engl J Med. 2018;379:11–21. doi: 10.1056/NEJMoa1716153. [DOI] [PubMed] [Google Scholar]
- 15.Ma C, Luo H, Fan L, Liu X, Gao C. Heart failure with preserved ejection fraction: an update on pathophysiology, diagnosis, treatment, and prognosis. Braz J Med Biol Res. 2020;53:e9646. doi: 10.1590/1414-431X20209646. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Vuong J, Singh A, Falk RH, Merchant R, Dorbala S. Geographic variation in public interest about amyloidosis in the United States and English speaking countries. Amyloid. 2020;27:210–212. doi: 10.1080/13506129.2020.1724941. [DOI] [PubMed] [Google Scholar]
- 17.Alexander KM, Orav J, Singh A, Jacob SA, Menon A, Padera RF, Kijewski MF, Liao R, Di Carli MF, Laubach JP, Falk RH, Dorbala S. Geographic Disparities in Reported US Amyloidosis Mortality From 1979 to 2015: Potential Underdetection of Cardiac Amyloidosis. JAMA Cardiol. 2018;3:865–870. doi: 10.1001/jamacardio.2018.2093. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Mut F, Carvajal I, Camilletti J, Erriest J, Alexanderson E, Grossman GB. Cardiac amyloidosis in Latin America: Gaps and opportunities to increase awareness of the disease. Findings from the AMILO-LATAM research group. J Nucl Cardiol. 2023;30:1592–1601. doi: 10.1007/s12350-022-03005-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Al Badarin F, Al-Humood K, Bader F, Alsaid S, Sulaiman K, Alzadjali M, Sabbour H, Shehab A, Bazargani N, Perlini S. Physician Knowledge and Awareness About Cardiac Amyloidosis in the Middle East and Gulf Region. JACC CardioOncol. 2022;4:421–424. doi: 10.1016/j.jaccao.2022.05.011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Adam R, Neculae G, Stan C, Jurcut R. Current Challenges of Cardiac Amyloidosis Awareness among Romanian Cardiologists. Diagnostics (Basel) 2021;11 doi: 10.3390/diagnostics11050834. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Mircsof D. Diagnosis of Amyloidosis: A Survey of Current Awareness and Clinical Challenges Among Cardiologists in Switzerland. Cardiol Ther. 2020;9:127–138. doi: 10.1007/s40119-019-00160-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Garcia-Pavia P, Rapezzi C, Adler Y, Arad M, Basso C, Brucato A, Burazor I, Caforio ALP, Damy T, Eriksson U, Fontana M, Gillmore JD, Gonzalez-Lopez E, Grogan M, Heymans S, Imazio M, Kindermann I, Kristen AV, Maurer MS, Merlini G, Pantazis A, Pankuweit S, Rigopoulos AG, Linhart A. Diagnosis and treatment of cardiac amyloidosis: a position statement of the ESC Working Group on Myocardial and Pericardial Diseases. Eur Heart J. 2021;42:1554–1568. doi: 10.1093/eurheartj/ehab072. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Hubert E, Dains JE. The Role of Echocardiogram and Cardiac Rhythm Analysis for Early Detection of Cardiac Amyloidosis. J Adv Pract Oncol. 2022;13:695–704. doi: 10.6004/jadpro.2022.13.7.5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Ruberg FL, Grogan M, Hanna M, Kelly JW, Maurer MS. Transthyretin Amyloid Cardiomyopathy: JACC State-of-the-Art Review. J Am Coll Cardiol. 2019;73:2872–2891. doi: 10.1016/j.jacc.2019.04.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Cheng Z, Zhu K, Tian Z, Zhao D, Cui Q, Fang Q. The findings of electrocardiography in patients with cardiac amyloidosis. Ann Noninvasive Electrocardiol. 2013;18:157–162. doi: 10.1111/anec.12018. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Dungu J, Sattianayagam PT, Whelan CJ, Gibbs SD, Pinney JH, Banypersad SM, Rowczenio D, Gilbertson JA, Lachmann HJ, Wechalekar A, Gillmore JD, Hawkins PN, Anderson LJ. The electrocardiographic features associated with cardiac amyloidosis of variant transthyretin isoleucine 122 type in Afro-Caribbean patients. Am Heart J. 2012;164:72–79. doi: 10.1016/j.ahj.2012.04.013. [DOI] [PubMed] [Google Scholar]
- 27.Cappelli F, Vignini E, Martone R, Perlini S, Mussinelli R, Sabena A, Morini S, Gabriele M, Taborchi G, Bartolini S, Lossi A, Nardi G, Marchionni N, Di Mario C, Olivotto I, Perfetto F. Baseline ECG Features and Arrhythmic Profile in Transthyretin Versus Light Chain Cardiac Amyloidosis. Circ Heart Fail. 2020;13:e006619. doi: 10.1161/CIRCHEARTFAILURE.119.006619. [DOI] [PubMed] [Google Scholar]
- 28.Cyrille NB, Goldsmith J, Alvarez J, Maurer MS. Prevalence and prognostic significance of low QRS voltage among the three main types of cardiac amyloidosis. Am J Cardiol. 2014;114:1089–1093. doi: 10.1016/j.amjcard.2014.07.026. [DOI] [PubMed] [Google Scholar]
- 29.Schrutka L, Anner P, Agibetov A, Seirer B, Dusik F, Rettl R, Duca F, Dalos D, Dachs TM, Binder C, Badr-Eslam R, Kastner J, Beitzke D, Loewe C, Hengstenberg C, Laufer G, Stix G, Dorffner G, Bonderman D. Machine learning-derived electrocardiographic algorithm for the detection of cardiac amyloidosis. Heart. 2022;108:1137–1147. doi: 10.1136/heartjnl-2021-319846. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Dorbala S, Ando Y, Bokhari S, Dispenzieri A, Falk RH, Ferrari VA, Fontana M, Gheysens O, Gillmore JD, Glaudemans AWJM, Hanna MA, Hazenberg BPC, Kristen AV, Kwong RY, Maurer MS, Merlini G, Miller EJ, Moon JC, Murthy VL, Quarta CC, Rapezzi C, Ruberg FL, Shah SJ, Slart RHJA, Verberne HJ, Bourque JM. ASNC/AHA/ASE/EANM/HFSA/ISA/SCMR/SNMMI expert consensus recommendations for multimodality imaging in cardiac amyloidosis: Part 1 of 2-evidence base and standardized methods of imaging. J Nucl Cardiol. 2019;26:2065–2123. doi: 10.1007/s12350-019-01760-6. [DOI] [PubMed] [Google Scholar]
- 31.Dorbala S, Ando Y, Bokhari S, Dispenzieri A, Falk RH, Ferrari VA, Fontana M, Gheysens O, Gillmore JD, Glaudemans AWJM, Hanna MA, Hazenberg BPC, Kristen AV, Kwong RY, Maurer MS, Merlini G, Miller EJ, Moon JC, Murthy VL, Quarta CC, Rapezzi C, Ruberg FL, Shah SJ, Slart RHJA, Verberne HJ, Bourque JM. ASNC/AHA/ASE/EANM/HFSA/ISA/SCMR/SNMMI expert consensus recommendations for multimodality imaging in cardiac amyloidosis: Part 2 of 2-Diagnostic criteria and appropriate utilization. J Nucl Cardiol. 2020;27:659–673. doi: 10.1007/s12350-019-01761-5. [DOI] [PubMed] [Google Scholar]
- 32.Kittleson MM, Maurer MS, Ambardekar AV, Bullock-Palmer RP, Chang PP, Eisen HJ, Nair AP, Nativi-Nicolau J, Ruberg FL American Heart Association Heart Failure and Transplantation Committee of the Council on Clinical Cardiology. Cardiac Amyloidosis: Evolving Diagnosis and Management: A Scientific Statement From the American Heart Association. Circulation. 2020;142:e7–e22. doi: 10.1161/CIR.0000000000000792. [DOI] [PubMed] [Google Scholar]
- 33.Goto S, Mahara K, Beussink-Nelson L, Ikura H, Katsumata Y, Endo J, Gaggin HK, Shah SJ, Itabashi Y, MacRae CA, Deo RC. Artificial intelligence-enabled fully automated detection of cardiac amyloidosis using electrocardiograms and echocardiograms. Nat Commun. 2021;12:2726. doi: 10.1038/s41467-021-22877-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Dorbala S, Cuddy S, Falk RH. How to Image Cardiac Amyloidosis: A Practical Approach. JACC Cardiovasc Imaging. 2020;13:1368–1383. doi: 10.1016/j.jcmg.2019.07.015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Hanna M, Ruberg FL, Maurer MS, Dispenzieri A, Dorbala S, Falk RH, Hoffman J, Jaber W, Soman P, Witteles RM, Grogan M. Cardiac Scintigraphy With Technetium-99m-Labeled Bone-Seeking Tracers for Suspected Amyloidosis: JACC Review Topic of the Week. J Am Coll Cardiol. 2020;75:2851–2862. doi: 10.1016/j.jacc.2020.04.022. [DOI] [PubMed] [Google Scholar]
- 36.Heidenreich PA, Bozkurt B, Aguilar D, Allen LA, Byun JJ, Colvin MM, Deswal A, Drazner MH, Dunlay SM, Evers LR, Fang JC, Fedson SE, Fonarow GC, Hayek SS, Hernandez AF, Khazanie P, Kittleson MM, Lee CS, Link MS, Milano CA, Nnacheta LC, Sandhu AT, Stevenson LW, Vardeny O, Vest AR, Yancy CW. 2022 AHA/ACC/HFSA Guideline for the Management of Heart Failure: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2022;145:e895–e1032. doi: 10.1161/CIR.0000000000001063. [DOI] [PubMed] [Google Scholar]
- 37.Kitaoka H, Izumi C, Izumiya Y, Inomata T, Ueda M, Kubo T, Koyama J, Sano M, Sekijima Y, Tahara N, Tsukada N, Tsujita K, Tsutsui H, Tomita T, Amano M, Endo J, Okada A, Oda S, Takashio S, Baba Y, Misumi Y, Yazaki M, Anzai T, Ando Y, Isobe M, Kimura T, Fukuda K Japanese Circulation Society Joint Working Group. JCS 2020 Guideline on Diagnosis and Treatment of Cardiac Amyloidosis. Circ J. 2020;84:1610–1671. doi: 10.1253/circj.CJ-20-0110. [DOI] [PubMed] [Google Scholar]
- 38.Witteles RM, Liedtke M. Avoiding Catastrophe: Understanding Free Light Chain Testing in the Evaluation of ATTR Amyloidosis. Circ Heart Fail. 2021;14:e008225. doi: 10.1161/CIRCHEARTFAILURE.120.008225. [DOI] [PubMed] [Google Scholar]
- 39.Cantone A, Sanguettoli F, Dal Passo B, Serenelli M, Rapezzi C. The treatment of amyloidosis is being refined. Eur Heart J Suppl. 2022;24:I131–I138. doi: 10.1093/eurheartjsupp/suac104. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Maurer MS, Schwartz JH, Gundapaneni B, Elliott PM, Merlini G, Waddington-Cruz M, Kristen AV, Grogan M, Witteles R, Damy T, Drachman BM, Shah SJ, Hanna M, Judge DP, Barsdorf AI, Huber P, Patterson TA, Riley S, Schumacher J, Stewart M, Sultan MB, Rapezzi C ATTR-ACT Study Investigators. Tafamidis Treatment for Patients with Transthyretin Amyloid Cardiomyopathy. N Engl J Med. 2018;379:1007–1016. doi: 10.1056/NEJMoa1805689. [DOI] [PubMed] [Google Scholar]
- 41.Hanna M, Damy T, Grogan M, Stewart M, Gundapaneni B, Patterson TA, Schwartz JH, Sultan MB, Maurer MS. Impact of Tafamidis on Health-Related Quality of Life in Patients With Transthyretin Amyloid Cardiomyopathy (from the Tafamidis in Transthyretin Cardiomyopathy Clinical Trial) Am J Cardiol. 2021;141:98–105. doi: 10.1016/j.amjcard.2020.10.066. [DOI] [PubMed] [Google Scholar]
- 42.Rapezzi C, Elliott P, Damy T, Nativi-Nicolau J, Berk JL, Velazquez EJ, Boman K, Gundapaneni B, Patterson TA, Schwartz JH, Sultan MB, Maurer MS. Efficacy of Tafamidis in Patients With Hereditary and Wild-Type Transthyretin Amyloid Cardiomyopathy: Further Analyses From ATTR-ACT. JACC Heart Fail. 2021;9:115–123. doi: 10.1016/j.jchf.2020.09.011. [DOI] [PubMed] [Google Scholar]
- 43.Elliott P, Drachman BM, Gottlieb SS, Hoffman JE, Hummel SL, Lenihan DJ, Ebede B, Gundapaneni B, Li B, Sultan MB, Shah SJ. Long-Term Survival With Tafamidis in Patients With Transthyretin Amyloid Cardiomyopathy. Circ Heart Fail. 2022;15:e008193. doi: 10.1161/CIRCHEARTFAILURE.120.008193. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Gillmore JD, Judge DP, Cappelli F, Fontana M, Garcia-Pavia P, Gibbs S, Grogan M, Hanna M, Hoffman J, Masri A, Maurer MS, Nativi-Nicolau J, Obici L, Poulsen SH, Rockhold F, Shah KB, Soman P, Garg J, Chiswell K, Xu H, Cao X, Lystig T, Sinha U, Fox JC ATTRibute-CM Investigators. Efficacy and Safety of Acoramidis in Transthyretin Amyloid Cardiomyopathy. N Engl J Med. 2024;390:132–142. doi: 10.1056/NEJMoa2305434. [DOI] [PubMed] [Google Scholar]
- 45.Masri A, Maurer MS, Claggett BL, Kulac I, Waddington Cruz M, Conceição I, Weiler M, Berk JL, Gertz M, Gillmore JD, Rush S, Chen J, Zhou W, Kwoh J, Duran JM, Tsimikas S, Solomon SD. Effect of Eplontersen on Cardiac Structure and Function in Patients With Hereditary Transthyretin Amyloidosis. J Card Fail. 2023 doi: 10.1016/j.cardfail.2023.11.016. [DOI] [PubMed] [Google Scholar]
- 46.Garcia-Pavia P, Grogan M, Kale P, Berk JL, Maurer MS, Conceição I, Di Carli M, Solomon SD, Chen C, Yureneva E, Vest J, Gillmore JD. Impact of vutrisiran on exploratory cardiac parameters in hereditary transthyretin-mediated amyloidosis with polyneuropathy. Eur J Heart Fail. 2024;26:397–410. doi: 10.1002/ejhf.3138. [DOI] [PubMed] [Google Scholar]
- 47.Maurer MS, Kale P, Fontana M, Berk JL, Grogan M, Gustafsson F, Hung RR, Gottlieb RL, Damy T, González-Duarte A, Sarswat N, Sekijima Y, Tahara N, Taylor MS, Kubanek M, Donal E, Palecek T, Tsujita K, Tang WHW, Yu WC, Obici L, Simões M, Fernandes F, Poulsen SH, Diemberger I, Perfetto F, Solomon SD, Di Carli M, Badri P, White MT, Chen J, Yureneva E, Sweetser MT, Jay PY, Garg PP, Vest J, Gillmore JD APOLLO-B Trial Investigators. Patisiran Treatment in Patients with Transthyretin Cardiac Amyloidosis. N Engl J Med. 2023;389:1553–1565. doi: 10.1056/NEJMoa2300757. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Garcia-Pavia P, Aus dem Siepen F, Donal E, Lairez O, van der Meer P, Kristen AV, Mercuri MF, Michalon A, Frost RJA, Grimm J, Nitsch RM, Hock C, Kahr PC, Damy T. Phase 1 Trial of Antibody NI006 for Depletion of Cardiac Transthyretin Amyloid. N Engl J Med. 2023;389:239–250. doi: 10.1056/NEJMoa2303765. [DOI] [PubMed] [Google Scholar]
- 49.Nativi-Nicolau J, Siu A, Dispenzieri A, Maurer MS, Rapezzi C, Kristen AV, Garcia-Pavia P, LoRusso S, Waddington-Cruz M, Lairez O, Witteles R, Chapman D, Amass L, Grogan M THAOS Investigators. Temporal Trends of Wild-Type Transthyretin Amyloid Cardiomyopathy in the Transthyretin Amyloidosis Outcomes Survey. JACC CardioOncol. 2021;3:537–546. doi: 10.1016/j.jaccao.2021.08.009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Kazi DS, Bellows BK, Baron SJ, Shen C, Cohen DJ, Spertus JA, Yeh RW, Arnold SV, Sperry BW, Maurer MS, Shah SJ. Cost-Effectiveness of Tafamidis Therapy for Transthyretin Amyloid Cardiomyopathy. Circulation. 2020;141:1214–1224. doi: 10.1161/CIRCULATIONAHA.119.045093. [DOI] [PMC free article] [PubMed] [Google Scholar]